Abstract
Objective
Negative affect has been purported to play an important role in the etiology and maintenance of bulimic behaviors. The objective of this study was to identify daily mood patterns in the natural environment exhibited by individuals with bulimia nervosa and to examine the relationship between these patterns and bulimic behaviors.
Method
One hundred thirty-three women aged 18–55 meeting DSM-IV criteria for bulimia nervosa were recruited through clinical referrals and community advertisements. Ecological momentary assessment was used to collect multiple ratings of negative affect, binge eating and purging each day for a two-week period using palmtop computers. Latent growth mixture modeling was used to identify daily mood patterns.
Results
Nine distinct daily mood patterns were identified. The highest rates of binge eating and purging episodes occurred on days characterized by stable high negative affect or increasing negative affect over the course of the day.
Conclusions
These findings support the conclusion that negative mood states are intimately tied to bulimic behaviors and may in fact precipitate such behavior.
Keywords: bulimia nervosa, ecological momentary assessment, latent growth mixture model
A number of sources of information converge to suggest that negative affect is an antecedent to binge eating and purging. Several theoretical models contend that negative affect plays an important role in the etiology and maintenance of bulimic behaviors. Heatherton and Baumeister (1991) proposed that binge eating serves as a mechanism to “escape from self-awareness,” thereby allowing an individual with bulimia nervosa (BN) to reduce the subjective experience of negative affect. Masking theory (Polivy & Herman, 1999) contends that BN patients avoid dealing with the actual source of their negative affect by engaging in binge eating, which provides a more acceptable source to which they can attribute negative affect.
Regardless of the specific model to which one adheres, increasing empirical evidence suggests that negative affect plays a role in the etiology and maintenance of eating disorders. For example, there is neurobiological support for the notion that patients with anorexia nervosa (AN) engage in extreme dietary restriction in an effort to regulate central serotonin levels, thereby allowing them to reduce negative affect (Kaye, Weltzin, & Hsu, 1991). BN participants, in comparison to normal controls, also report significantly higher negative affect and mood variability following acute tryptophan depletion (Kaye, Gendall, Fernstrom, Fernstrom, McConaha, & Weltzin, 2000). These findings suggest that BN patients may be particularly impacted by low central serotonin levels and therefore more likely to engage in extreme behaviors (e.g., binge eating and purging) in an effort to alleviate their negative mood.
Other lines of research have also supported a link between negative affect and eating disorder behavior. For example, Waller and colleagues (Waller, Babbs, Milligan, Meyer, Ohanian, & Leung, 2003) found that individuals with eating disorder symptomatology report greater levels of state anger and anger suppression. Negative affect has also been shown to predict the onset of eating disorder behavior (Stice, 2002) and a poorer course for AN (Strober, Freeman, & Morrell, 1997). Depressive symptoms and negative affect have been found to predict increases in bulimic symptoms and psychopathology associated with BN (Stice, 2001; Cooley & Toray, 2001; Killen, Taylor, Hayward, Haydel, Wilson, Hammer, Kraemer, Blair-Greiner, & Strachowski, 1996; Stice & Agras, 1998; Stice, Burton, & Shaw, 1994). Further, it has been reported that treatment of depressive symptoms can produce longitudinal decreases in bulimic symptoms (Burton, Stice, Bearman, & Rohde, 2007). Finally, negative affect has been shown to covary predictably with bulimic behaviors in naturalistic studies (Smyth et al., 2007).
In the current paper we attempt to further examine the relationship between negative affect and bulimic behaviors. Specifically, we evaluate the extent to which patterns of mood experienced by bulimic individuals over the course of the day are associated with binge eating and purging behaviors. We employ a sophisticated naturalistic data collection technique (ecological momentary assessment) with bulimic women to obtain multiple assessments per day over a two-week period. We then use latent growth mixture modeling to develop a classification of daily mood patterns experienced by BN participants. While previous studies have classified eating disordered patients on the basis of symptom patterns (Grilo, Masheb, & Berman, 2001; Stice & Agras, 1999) and personality traits (Goldner, Srikameswaran, Schroeder, Livesley, & Birmingham; 1999; Espelage, Mazzeo, Sherman, & Thompson, 2002; Westen & Harnden-Fischer, 2001), no study to date has attempted to classify daily mood patterns commonly experienced by BN patients. Finally, we compare rates of binge eating and purging across different classes of days. We hypothesized that bulimic behaviors would be more likely to occur on days characterized by higher levels and greater variability in negative affect. This study provides a significant contribution to the literature by evaluating bulimic behaviors in the natural environment and describing a typology of daily mood patterns and its relationship to bulimic behaviors.
METHODS
Participants and Recruitment
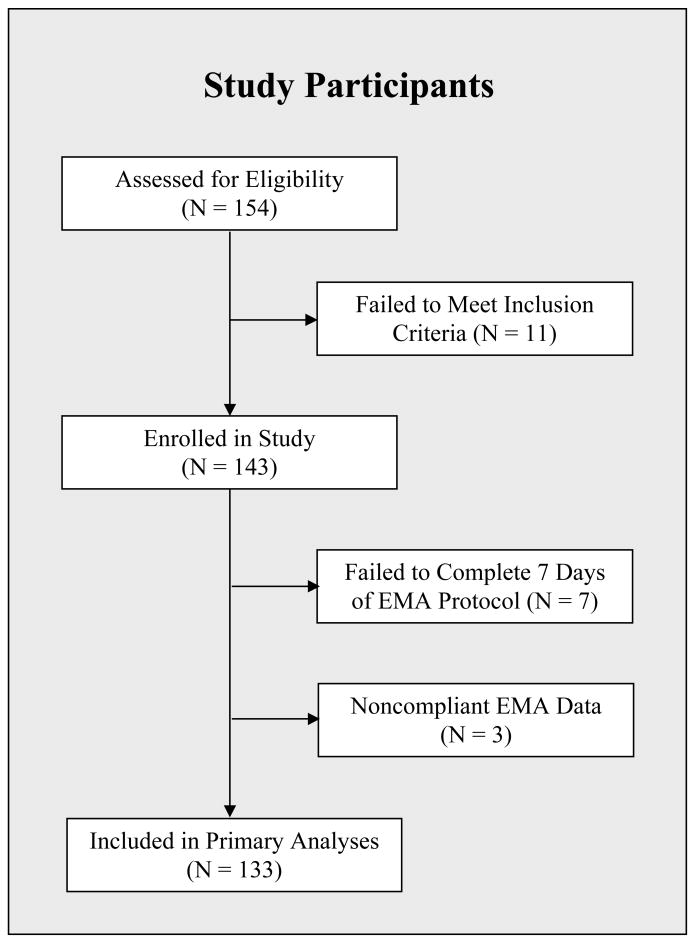
Participants were eligible for the present study if they were female, at least 18 years of age, and met DSM-IV criteria for BN (American Psychiatric Association, 1994). Participants were recruited through clinical referrals, as well as through community and campus advertisements. Figure 1 presents a flowchart of study participants. A total of 154 prospective participants completed a phone screen to determine initial eligibility for the study. Eleven individuals failed to meet inclusion criteria and were excluded, resulting in 143 participants who were enrolled in the protocol. Seven participants dropped out of the protocol prior to completing at least seven days of EMA data and 3 participants were not compliant with the EMA protocol, resulting in 10 participants excluded from analysis. EMA data from the remaining 133 participants are reported in the current manuscript.
Figure 1. Flowchart of study participants.
All participants were female with a mean age of 25.3 (SD = 7.6, range = 18–55). The majority of participants were Caucasian (n = 127, 95.5%), never married (n = 85, 63.9%), students (n = 74, 55.6%), currently employed (n = 96, 73.3%), and all but one (n = 132, 99.2%) had completed high school. The mean BMI for participants was 23.9 (SD = 5.2, range = 17.1–47.6). All participants were at least 85% of ideal body weight. The majority of participants (n = 115, 85.5%) met lifetime criteria for a DSM-IV mood disorder, and over half (n = 71, 53.4%) met criteria for a mood disorder in the past month. Similarly, 78 participants (58.6%) met lifetime criteria for a DSM-IV anxiety disorder and approximately half of the participants (n = 67, 50.4%) met criteria for an anxiety disorder in the past month. Lifetime rates of substance abuse or dependence were 36.8% (n = 49), and 15.8% (n = 21) met criteria for substance abuse or dependence in the past month.
Assessment and Procedures
This study was approved by the Institutional Review Boards of the University of North Dakota and MeritCare Hospital (Fargo, ND). Eligible participants attended a meeting where they received information about the study and provided written informed consent. Participants were then scheduled for two assessment visits that lasted a total of 3–4 hours. During these visits a blood sample was collected for electrolyte screening to ensure medical stability, a series of structured interviews were conducted by doctoral-level psychologists (described below), and several self-report measures were completed. Only those measures used for the current study are described below.
A trained doctoral-level psychologist administered the Structured Clinical Interview for DSM-IV Axis I Disorders (SCID-I/P; First, Spitzer, Gibbon, & Williams, 1995). The SCID-I/P was used to determine current (i.e., eating disorders) and lifetime (i.e., mood, anxiety, substance abuse/dependence) psychiatric diagnoses. The Eating Disorder module of the SCID-I/P was used to establish a current DSM-IV diagnosis of bulimia nervosa, from which study eligibility was determined. All SCID-I/P interviews were audio-taped, and twenty-five (18.8%) of these tapes were randomly selected to be rated by a second doctoral-level psychologist for the purposes of determining interrater reliability. The kappa coefficient for current DSM-IV bulimia nervosa based upon these 25 cases was 1.0.
At the end of the first assessment session, participants were trained to use palmtop computers to complete their EMA recordings. Participants were instructed that they should not complete ratings at inconvenient times (e.g., while in class) or if safety was a concern (e.g., while driving), and were encouraged to delay responding until a more convenient time in those circumstances. Participants were provided palmtop computers and were instructed to complete ratings for two practice days. When participants returned for the second assessment session, these data were reviewed with the participant and feedback regarding compliance rates was provided. These practice data were not used for analysis purposes. At the completion of second assessment session, participants were given palmtop computers to complete EMA assessments over the course of the next two weeks. Two visits were scheduled for each participant during the two-week interval to collect palmtop computer data in order to minimize the amount of lost data in the event of technical problems. Participants were given feedback about their compliance rates at each visit. Participants received $200 for the completing two weeks of EMA assessments and were given a $50 bonus for compliance rates of 85% or greater.
Participants were signaled by the palmtop computer to complete ratings at six semi-random times throughout the day. The time of the signal was determined randomly to be within +/− 20 minutes of each of six “anchor” times distributed evenly throughout the day: 8:30 a.m., 11:10 a.m., 1:50 p.m., 4:30 p.m., 7:10 p.m., and 9:50 p.m. When signaled, participants were asked to rate their current mood and any recent behaviors not yet recorded (described in detail below). Participants were also asked to complete ratings of mood, stress and specific eating disorder behaviors (see below).
EMA mood ratings for the current analyses were based upon the Negative Affect (NA) scale from the Positive and Negative Affect Scale (PANAS; Watson, Clark, & Tellegen, 1988). Eleven items from the NA scale (afraid, lonely, irritable, ashamed, disgusted, nervous, dissatisfied with self, jittery, sad, distressed, angry with self) were rated on a 5-point scale (1 = “Not at All”; 5 = “Extremely”). Watson and colleagues (Watson et al., 1988) have reported an alpha coefficient of .85 for NA. The coefficient alpha for NA based upon the 11 items used in the current study was .92.
Participants were asked to record whenever they engaged in binge eating, vomiting, or used laxatives for the purpose of controlling weight. Participants could record these behaviors either immediately after they occurred (i.e., event contingent recording) or when they were next signaled to complete ratings (i.e., signal contingent recording). During training participants were provided with standard definitions of binge eating (“an amount of food that you consider excessive, or an amount of food that other people would consider excessive, with an associated loss of control or the feeling of being compelled to eat”) and vomiting (“intentionally making yourself throw up for the purposes of controlling your weight”). Thus binge eating assessments included eating episodes involving both subjectively and objectively large amounts of food. Participants were also provided with examples of what constituted objectively large amounts of food.
Statistical Analysis
Latent growth mixture modeling (Muthén & Khoo, 1998; Muthén & Muthén, 2000) (LGMM) was used to identify distinct trajectories of daily mood patterns as reported during EMA assessments. The LGMM approach assumes that the sample is composed of a mixture of distinct subgroups, each defined by a prototypical growth curve or trajectory (Wiesner, Weichold & Silbereisen, 2007). LGMM has typically been used to classify individuals in terms of their distinct trajectories; in contrast, the current study uses LGMM to classify days in terms of mood patterns, with each class representing a prototypical pattern of mood for that day.
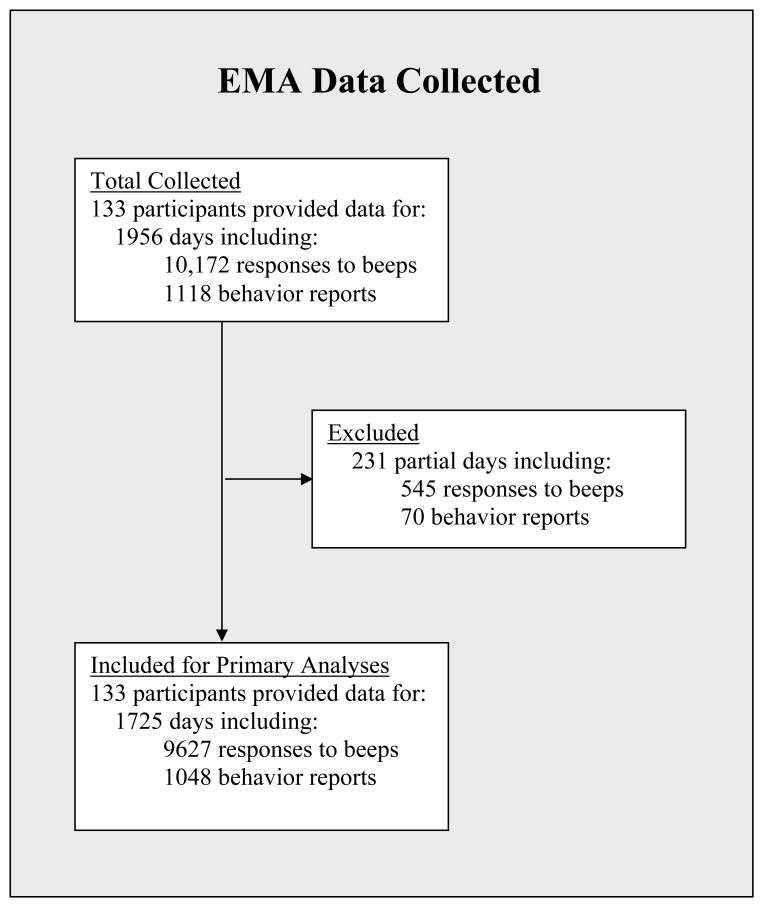
A flowchart of EMA data collected and used in the current analyses is presented in Figure 2. First, a decision was made to use mood data only from ratings completed when signaled (i.e., 6 possible ratings per day). Although mood ratings were also made when behaviors were recorded and at end-of-day ratings, the number and timing of these recordings varied dramatically across individuals and days. We elected to use mood data only from ratings completed when signaled because of the comparable timeframe and frequency of ratings across participants. Second, a decision was made to exclude mood ratings from days where less than four mood ratings in response to a signal were completed. The majority of these “partial” days with 3 or less mood ratings were participants’ first and last day of EMA recording. Partial and full days did not differ significantly in terms of mean negative affect. While LGMM does allow for missing data (see below), it seemed unsound to include days where half or more of the mood ratings were missing. Thus, from the 1956 total participant days of EMA recordings, those days with 1 (n = 45, 2.3%), 2 (n = 58, 3.0%), or 3 (n = 128; 6.5%) valid mood ratings were excluded, leaving 1725 participant days of EMA mood recordings. Of this total, 1167 (67.7%) included all 6 valid mood ratings, 393 (22.8%) included 5 valid ratings, and 165 (9.6%) included 4 valid ratings. In total, LGMM was performed on 1725 participant days of observation containing 9627 separate mood assessments in response to random signals.
Figure 2. Flowchart of EMA data collected.
The LGMM models were estimated using Mplus 3.12 software (Muthén & Muthén, 1998–2004). Preliminary analyses revealed that models required an intercept, as well as linear and quadratic components to adequately characterize daily mood patterns. Separate model components were estimated for each class, and individual variation within class was allowed for both the intercept and the linear components. The variance of the quadratic components was set to zero to facilitate model convergence. As a result, the LGMM models estimated both mean growth curves for each class as well as individual variation around these growth curves (Muthén & Muthén, 2000). Missing responses to random signals (maximum of 2 per day) were estimated with full information maximum-likelihood estimation. The LGMM models included participant as a clustering variable to account for the multiple observations provided by each participant.
The optimal number of classes was determined based upon four separate fit indices. The Bayesian information criterion (BIC; Schwartz, 1978) expresses model fit as a function of log-likelihood, sample size, and the number of parameters in the model. An alternative form of the BIC has been developed, referred to as the adjusted BIC (aBIC), which includes a correction for large sample size (Sclove, 1987). The Akaike information criterion (AIC; Akaike, 1987) determines model fit on the basis of the log-likelihood of the model and the number of estimated parameters. A derivation of the AIC has been suggested, referred to as the Consistent Akaike information criterion (cAIC), which includes a penalty for models having larger number of parameters (Bozdogman, 1987). All of the information criterion indices above were used for comparing plausible models with the lowest values indicating the best fitting model. In addition, the entropy index (Ramaswamy, DeSarbo, Reibstein, & Robinson, 1993) was calculated for each model. Although not a fit index per se, entropy represents the average classification accuracy of a given model, and can be informative for evaluating competing models.
General estimating equations (GEE; Liang & Zeger, 1986) were used to compare latent classes in terms of the proportion of days with binge eating and purging (i.e., vomiting or laxative use). Overall comparisons between groups were based upon the Wald chi-square statistic. Odds ratios and 95% confidence intervals were computed between Class 1 (Stable Low Negative Affect) and all other classes.
RESULTS
Identification of Daily Mood Trajectories
LGMM models varying in the number of latent classes between 1 and 10 were evaluated. A summary of these models is presented in Table 1. Three of the four information criterion indices (BIC, aBIC, and cAIC) were at their minimum for the 9-class model. The AIC reached its minimum for the 10-class model. Given the agreement amongst these three indicators, and considering the higher entropy value for the 9-class versus the 10-class model (.816 vs. .786), the 9-class model of daily mood patterns was selected as the best fitting model. A summary of the model parameters is presented in Table 2. Figure 3 presents the mean negative affect scores at each time point separately by class. A summary description of these classes is provided below.
Table 1.
Model Fit Indices of Latent Growth Mixture Models for 1725 EMA Mood Assessment Days.
| Number of Classes | BIC | a BIC | AIC | cAIC | LL | Entropy |
|---|---|---|---|---|---|---|
| 1 | 63751.1 | 63713.0 | 63685.7 | 63763.1 | −31830.8 | --- |
| 2 | 63598.7 | 63547.9 | 63511.5 | 63614.7 | −31739.7 | .862 |
| 3 | 63398.2 | 63334.6 | 63289.2 | 63418.2 | −31624.6 | .781 |
| 4 | 63281.3 | 63205.1 | 63150.4 | 63305.3 | −31551.2 | .811 |
| 5 | 63246.1 | 63157.2 | 63093.5 | 63274.1 | −31518.7 | .838 |
| 6 | 63129.7 | 63028.1 | 62955.2 | 63161.7 | −31445.6 | .802 |
| 7 | 63076.2 | 62961.8 | 62879.9 | 63112.2 | −31403.9 | .813 |
| 8 | 63041.2 | 62914.2 | 62823.2 | 63081.3 | −31371.6 | .815 |
| 9 | 62998.0 | 62858.2 | 62758.1 | 63042.0 | −31335.0 | .816 |
| 10 | 63012.6 | 62860.2 | 62750.9 | 63060.6 | −31327.5 | .786 |
Abbreviations: BIC = Bayesian information criterion; aBIC = sample size-adjusted Bayesian information criterion; AIC = Akaike information criterion; cAIC = Consistent Akaike information criterion; LL = log likelihood.
Darkened cells indicate lowest value of fit index in column.
Table 2.
Relative Proportion, Parameter Estimates, and Standard Errors for 9-Class Latent Growth Mixture Model.
| Intercept | Linear | Quadratic | ||||||
|---|---|---|---|---|---|---|---|---|
| Class | Description | n (Proportion1) | Est. | SE | Est. | SE | Est. | SE |
| Class 1 | Stable Low NA | 941 (.546) | 17.16*** | 0.53 | 0.20 | 0.15 | −0.03 | 0.03 |
| Class 2 | Stable Moderate NA | 303 (.176) | 31.65*** | 1.33 | 0.71 | 0.82 | −0.13 | 0.10 |
| Class 3 | Stable High NA | 71 (.041) | 42.88*** | 2.24 | 0.14 | 0.89 | 0.10 | 0.17 |
| Class 4 | Late Increasing NA | 107 (.062) | 19.96*** | 1.37 | −2.44** | 0.91 | 0.98*** | 0.22 |
| Class 5 | Early Increasing NA | 119 (.069) | 22.79*** | 2.77 | 4.95** | 2.14 | −0.47 | 0.36 |
| Class 6 | Late Decreasing NA | 24 (.014) | 38.07*** | 2.30 | 6.15*** | 1.60 | −1.92*** | 0.28 |
| Class 7 | Early Decreasing NA | 90 (.052) | 34.87*** | 1.75 | −4.76*** | 0.95 | .432*** | 0.15 |
| Class 8 | Inverted U-Shaped NA | 50 (.029) | 18.57*** | 1.24 | 11.27*** | 1.43 | −2.11*** | 0.22 |
| Class 9 | U-Shaped NA | 20 (.012) | 37.09*** | 2.85 | −12.11*** | 1.80 | 2.55*** | 0.29 |
Abbreviations: NA = Negative Affect; Est. = Estimate; SE = Standard Error
p < .05;
p < .01;
p < .001
Proportions based upon most likely latent class membership.
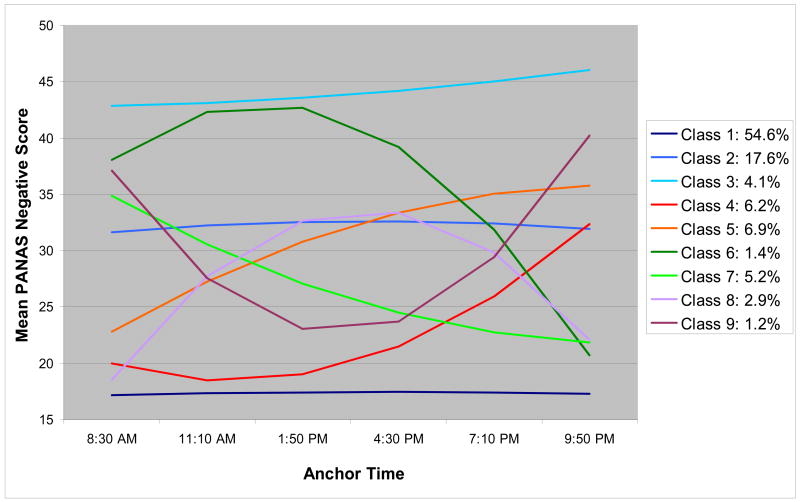
Figure 3. Latent classes of daily negative affect patterns.
Three classes involve stable mood patterns across the day. Class 1, labeled “Stable Low Negative Affect,” is characterized by low negative affect throughout the day. This class accounts for over half (54.6%) of all days classified. Class 2, labeled “Stable Moderate Negative Affect,” accounts for 17.6% of all classified days, and is characterized by moderate levels of negative affect. Class 3, labeled “Stable High Negative Affect,” accounts for 4.1% of all days, and is characterized by high levels of negative affect throughout the day. These classes represent unchanging mood trajectories (as indicated in Table 2 by non-significant linear and quadratic components) that differ in overall level of negative affect.
Two latent classes involve increasing negative affect over the course of the day. Class 4, labeled “Late Increasing Negative Affect,” is characterized by low negative affect for the first three ratings, followed by steady increases thereafter, culminating in moderate levels of negative affect at the last rating. Class 4 accounts for 6.2% of all days classified. Class 5, labeled “Early Increasing Negative Affect,” is characterized by relatively low negative affect at the first rating which increases steadily to moderate levels by the last ratings. This class accounts for 6.9% of all classified days.
Two latent classes involve decreasing negative affect over the course of the day. Class 6, labeled “Late Decreasing Negative Affect,” is characterized by high levels of negative affect which increase slightly over the first three ratings, and dramatically decline thereafter. This class accounts for only 1.4% of all classified days. In contrast, Class 7, labeled “Early Decreasing Negative Affect,” is characterized by moderate levels of negative affect at the first rating which decline steadily over the course of the day. This class accounts for 5.2% of all days classified.
The final two latent classes involve dramatic changes in negative affect over the course of the day. Class 8, labeled “Inverted U-Shaped Negative Affect,” is characterized by low negative affect at the first rating that increases to moderate levels by late afternoon and declines dramatically thereafter. This class accounts for 2.9% of classified days. In contrast, Class 9, labeled “U-Shaped Negative Affect,” is characterized by moderately high levels of negative affect at the first and last rating, with lower levels of negative affect in between. This is the most infrequent class, accounting for only 1.2% of all classified days.
One important question is the distribution of the latent classes within individuals. That is, do individuals consistently report the same pattern of mood (resulting in the same latent class) across days? If so, then the classification of days would be largely redundant with a classification of individuals. On the other hand, if individuals tend to report many different patterns of mood (resulting in many different classes for a given individual), then the classification of days might have unique relevance apart from a classification of individuals. In the current study, the number of different classes of days for individual participants ranged from 1–7 (out of 9 possible), with a median of 3. Eighty-two percent (n = 109) of participants had at least two different classes, and almost half (n = 66) reported four or more. Among the 24 participants with only a single class across all days of recording, 22 had all Class 1 (“Stable Low Negative Affect”) days, one participant had all Class 2 (“Stable Moderate Negative Affect”) days, and the remaining participant had all Class 3 (“Stable High Negative Affect”) days. These data suggest that the classification of days does capture some variability in mood pattern within individuals.
Daily Mood Trajectories and Eating Disordered Behaviors
Significant differences between classes were found in rates of both binge eating (Wald chi-square = 68.5; df = 8; p < .001) and purging (Wald chi-square = 43.3; df = 8; p < .001). Table 3 presents the percentage of days on which binge eating and purging were reported by latent class. In comparison to Class 1 (Stable Low NA), where binge eating was reported on 32.2% of days, the highest rates of binge eating were reported for Class 5 (Early Increasing NA; 67.2%), Class 3 (Stable High NA; 66.2%), and Class 9 (U-Shaped NA; 65.0%). Interestingly, rates of binge eating were significantly higher for all classes in comparison to the reference class (Class 1) except for the two classes (Classes 6 & 7) characterized by decreasing negative affect over the course of the day. Those classes with significantly higher rates of purging behavior compared to Class 1 include Class 3 (Stable High NA; 76.1%), Class 5 (Early Increasing NA; 73.9%), and Class 2 (Stable Moderate NA; 59.1%).
Table 3.
Binge Eating and Purging Behaviors by Daily Mood Patterns.
| Binge Eating | Purging | ||||||
|---|---|---|---|---|---|---|---|
| Class | Description | % | OR | 95% CI | % | OR | 95% CI |
| Class 1 | Stable Low NA | 32.2% | --- | --- | 43.4% | --- | --- |
| Class 2 | Stable Moderate NA | 50.2% | 1.20*** | 1.09–1.31 | 59.1% | 1.17** | 1.06–1.30 |
| Class 3 | Stable High NA | 66.2% | 1.41*** | 1.18–1.67 | 76.1% | 1.39*** | 1.15–1.68 |
| Class 4 | Late Increasing NA | 55.1% | 1.26*** | 1.13–1.40 | 52.3% | 1.09 | 0.99–1.20 |
| Class 5 | Early Increasing NA | 67.2% | 1.42*** | 1.27–1.59 | 73.9% | 1.36*** | 1.22–1.50 |
| Class 6 | Late Decreasing NA | 41.7% | 1.10 | 0.86–1.40 | 58.3% | 1.16 | 0.90–1.49 |
| Class 7 | Early Decreasing NA | 28.9% | 0.97 | 0.88–1.07 | 43.3% | 1.00 | 0.89–1.13 |
| Class 8 | Inverted U-Shaped NA | 50.0% | 1.20* | 1.02–1.40 | 58.0% | 1.16 | 0.98–1.37 |
| Class 9 | U-Shaped NA | 65.0% | 1.39*** | 1.18–1.63 | 55.0% | 1.12 | 0.93–1.36 |
Abbreviations: NA = Negative Affect; OR = Odds ratio in comparison to Class 1; 95% CI = 95% Confidence Interval for Odds Ratio.
p < .05;
p < .01;
p < .001
Secondary Analysis
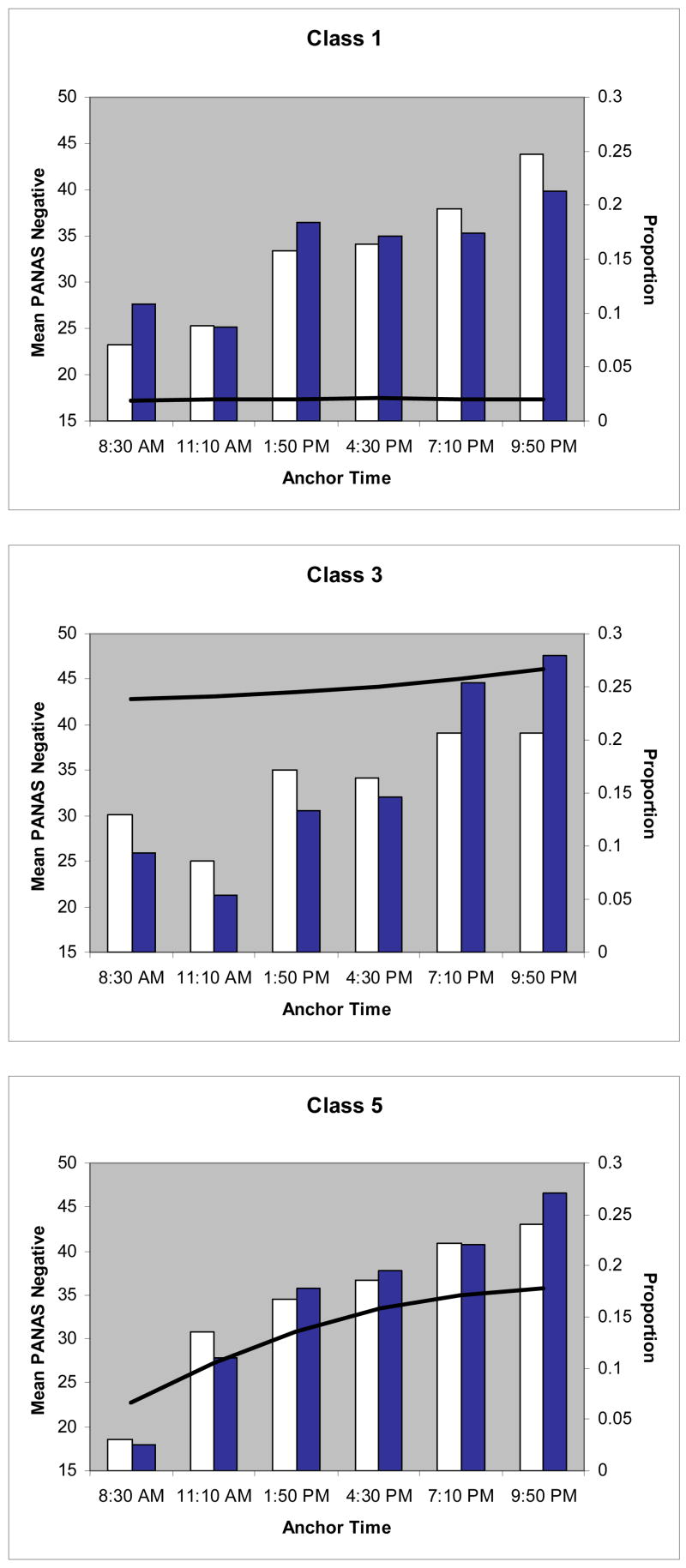
In order to examine the temporal distribution of eating disordered behaviors within days, we calculated separately for Class 1, 3 and 5, the percentage of binge eating and purging behaviors that were reported at each of the six random assessment intervals. Class 3 (Stable High NA) and Class 5 (Early Increasing NA) represent the daily mood patterns with the highest rates of binge eating and purging, while Class 1 (Stable Low NA) was chosen as the most relevant comparison condition. These data are presented in Figure 4. For each graph, the line represents the mean negative affect pattern over the course of the day. The light bars represent the proportion all purging episodes that occurred at each of the six random assessment points, while the dark bars represent the proportion of binge eating episodes.1 For example, for Class 1, 24.7% of all purge episodes and 21.3% of all binge eating episodes were reported at the last random assessment of the day (9:50 PM). There are few notable differences in the timing of eating disordered behaviors across the three classes. The highest proportion of purging and binge eating episodes were reported at the last random assessment for all 3 classes. Likewise, the majority of both purging and binge eating episodes were reported in the final three random assessments (4:50 PM or later) for all 3 classes.
Figure 4. Daily patterns of binge eating and mood by latent class.
Lines represent the mean negative affect (left axis), light bars the proportion of purging episodes (right axis), and dark bars the proportion of binge eating episodes at each assessment time by class.
DISCUSSION
The findings of this study are significant in several ways. First, the present findings offer a classification of days based on patterns of mood rather than a classification of individuals, which is unique in the eating disorder research field. Second, the findings provide further support for the idea that negative mood states are intimately tied to bulimic behaviors and may in fact precipitate such behavior. Finally, the findings demonstrate that EMA technologies provide a uniquely fine-grained, time-sensitive approach to measuring bulimic behavior that research participants reliably complete. Each of these will be reviewed below.
One innovative feature of the current study is the identification of distinct mood patterns in the lives of bulimic individuals. Whereas previous classification studies (Keel, Fichter, Quadflieg, Bulik, Baxter, Thornton et al., 2004; Wonderlich, Crosby, Joiner, Peterson, Bardone-Cone, Klein et al., 2005) have attempted to identify different subgroups of individuals, those studies do not acknowledge variability in the types of days that any bulimic individual may experience. Highly affective and impulsive bulimic individuals may in fact have days in which their emotions are relatively positive and stable, and anxious bulimic individuals may have fairly calm days, but such variability is not included in between-subjects research designs.
The present effort to identify different types of days based on patterns of emotions, regardless of between-subject differences, may prove clinically useful. From the perspective of the patient, it may be useful for them to learn strategies in treatment to identify and cope with the different kinds of days they experience. Psychotherapeutic treatments may benefit from developing strategies for identifying and managing the different kinds of days that bulimic individuals may experience. Educating patients about the days which are most risky for bulimic behavior could serve as a helpful clinical intervention. EMA technology could also be used in treatment to inform bulimic individuals about the patterns of their moods over the course of a day and the risk of binge-purge behavior. Intervention strategies ultimately could be delivered both in face-to-face psychotherapy, as well as through portable electronic devices which simultaneously serve to identify mood patterns and deliver daily interventions (Wonderlich, Peterson, Mitchell, & Crow, 2001).
The second major implication of the present study is the significant daily co-variance of emotions and behavior in bulimia nervosa. Similar to studies which have simply modeled the overall relationship of mood ratings and bulimic behavior (e.g., Smyth et al., 2007), the present findings suggest that days high in negative emotion tend to be days on which bulimic behavior occurs. Although we are unable to ascertain, in the present findings, whether such emotional days beget bulimic behavior or are a consequence of bulimic behavior, the finding that such high negative mood days (e.g., Class 3, Class 5) are characterized by a tendency for bulimic behaviors to occur in the later portion of the day is consistent with the idea that negative mood states ultimately drive bulimic behavior. Perhaps after a day of prolonged, or escalating negative mood, a threshold point is reached (late in the day) which increases the likelihood of bulimic behavior. Furthermore, other factors may also increase the risk of bulimic behaviors late in the day, such as prolonged episodes of dietary restriction or a decrease in structured activity (e.g., job is done, school is over).
Of course, it is also possible that the elevated negative mood states seen early on Class 3 days are precipitated by bulimic behaviors which occur early in the day. However, such negative mood states may then precipitate bulimic behavior later in the day. Clearly, the relationship of emotion and bulimic behavior is likely to be complex and reciprocal and raises the possibility that such negative mood states may be both consequence and cause of bulimic behavior. Nonetheless, clinicians may benefit from monitoring the mood-behavior relationship and targeting high risk times later in a given day, especially when negative mood is escalated.
Finally, the current study underscores the utility of EMA in the study of eating disorders. EMA technology overcomes significant methodological research problems associated with the retrospective recall of behaviors and associated states (e.g., mood). Behavior is gathered in the moment, thus reducing errors in recall and biases which commonly plague behavioral research. Thus, when the subjects in the present study reported binge eating or purging behaviors, they did so within minutes, or at most hours from when the behaviors occurred. Similarly, mood measurements were assessed in the moment, thus providing a contemporaneous assessment of a mood state. Furthermore, particularly when hand-held computers are used for the assessment of such behaviors and moods, we are able to identify the temporal-longitudinal patterns of these variables. For example, the data in this study demonstrate that although bulimic behaviors occur over the entire course of a typical day, they are much more likely to occur in the evenings. These data support clinical reports which often characterize evenings and weekends as the most vulnerable time for such behavior (Crosby, Wonderlich, Smyth, Miltenberger, Steiger, Engel, & Mitchell, 2004) and may be particularly informative in efforts to enhance psychosocial interventions which attempt to decrease the likelihood of bulimic behavior in the outpatient setting. These data also provide empirical support for BN treatments, such as cognitive behavioral therapy (Fairburn, Marcus, & Wilson, 1993) or newer treatments (Fairburn, Cooper,& Shafran, 2003; Wonderlich, Peterson, Mitchell, & Crow, 2001), that focus on high risk times over the course of the day.
The present findings are not without limitations. First, it is likely that participants did not report all occurrences of binge eating and purging. It is not known the extent of these omissions or the impact of these omissions on the current findings. Second, although these data suggest a relationship between negative affect and eating disordered behaviors, a causal connection cannot be established. Third, it is possible that self-monitoring of mood and behaviors in the current study somehow biased or influenced these results. Previous EMA studies with BN participants have found little evidence for reactivity (Stein & Corty, 2003). In the current study, the frequency of mood patterns was not significantly different between the first and second week of EMA recording, suggesting that affective reactivity to EMA may have been minimal. Finally, future research is needed to determine whether the daily mood patterns identified in the current study and their relative rates of occurrence are specific to bulimic individuals, or whether they are generalizable to other psychiatric and healthy populations.
These limitations notwithstanding, however, the current study used an innovative assessment strategy to investigate the role of mood in bulimia nervosa. We identified distinct daily patterns of mood experienced by bulimic individuals and established an association between these mood patterns and bulimic behaviors. As such, the current study provides strong evidence of the relationship between daily mood patterns and bulimic behaviors that may have relevance for the development of more effective treatments.
Acknowledgments
Raymond G. Miltenberger, Ph.D., Howard Steiger, Ph.D., Marjorie H. Klein, Ph.D., Dean D. Krahn, M.D. and Marsha Rorty, Ph.D. provided consultation on this project. Tricia Myers-Cook, Ph.D. and Lorraine Swan-Kremeier, Ph.D. conducted assessments. Maisley Paxton-Jones, Ph.D., Jennifer Redlin, M.A., and Jessica Severson, B.A. contributed to the execution of this study. Nancy Monson, B.A., Jodi Swanson, B.A., and Traci L. Kalberer, B.A. helped to manage data. Tammy L. Root provided helpful comments and feedback on an early version of this manuscript.
Funding Support: This project was funded by grant R01-MH-59674 from the National Institute of Mental Health awarded to the Neuropsychiatric Research Institute (Dr. Wonderlich).
Footnotes
A relatively small percentage of purging (5.8%) and binge eating (5.0%) episodes were reported after the last random beep of the day. These behaviors are not shown in the graphs but are reflected in terms of the percentages reported for the random assessments.
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
References
- Akaike H. Factor analysis and AIC. Psychometrika. 1987;52:317–332. [Google Scholar]
- American Psychiatric Association (APA) Diagnostic and statistical manual of mental disorders. 4. Washington, DC: American Psychiatric Association; 1994. [Google Scholar]
- Bozdogman H. Model selection and Akaike’s information criterion: The general theory and its analytical extensions. Psychometrika. 1987;52:345–370. [Google Scholar]
- Burton E, Stice E, Bearman SK, Rohde P. Experimental test of the affect-regulation theory of bulimic symptoms and substance use: A randomized trial. International Journal of Eating Disorders. 2007;40(1):27–36. doi: 10.1002/eat.20292. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cooley E, Toray T. Body image and personality predictors of eating disorder symptoms during the college years. International Journal of Eating Disorders. 2001;30(1):28–36. doi: 10.1002/eat.1051. [DOI] [PubMed] [Google Scholar]
- Crosby RD, Wonderlich SA, Smyth J, Miltenberger R, Steiger H, Engel SG, Mitchell JE. A day in the life of... a description of the temporal patterns of bulimic behaviors and mood based on intensive electronic diary recordings. Presented at the annual meeting of the Eating Disorders Research Society; Amsterdam, Netherlands. October 8.2004. [Google Scholar]
- Espelage DL, Mazzeo SE, Sherman R, Thompson R. MCMI-II profiles of women with eating disorders: A cluster analytic investigation. Journal of Personality Disorders. 2002;16:453–463. doi: 10.1521/pedi.16.5.453.22127. [DOI] [PubMed] [Google Scholar]
- Fairburn CG, Cooper Z, Shafran R. Cognitive behaviour therapy for eating disorders: A ‘transdiagnostic’ theory and treatment. Behaviour Research and Therapy. 2003;41(5):509–528. doi: 10.1016/s0005-7967(02)00088-8. [DOI] [PubMed] [Google Scholar]
- Fairburn CG, Marcus MD, Wilson GT. Cognitive-behavioral therapy for binge eating and bulimia nervosa: A comprehensive treatment manual. In: Fairburn CG, Wilson GT, editors. Binge eating: Nature, assessment, and treatment. New York, NY: Guilford Press; 1993. pp. 361–404. [Google Scholar]
- First M, Spitzer R, Gibbon M, Williams J. Structured Clinical Interview for DSM-IV Axis I Disorders: Patient Edition (SCID-I/P) New York: Biometrics; 1995. [Google Scholar]
- Goldner EM, Srikameswaran S, Schroeder ML, Livesley WJ, Birmingham CL. Dimensional assessment of personality pathology in patients with eating disorders. Psychiatry Research. 1999;85:151–159. doi: 10.1016/s0165-1781(98)00145-0. [DOI] [PubMed] [Google Scholar]
- Grilo CM, Masheb RM, Berman RM. Subtyping women with bulimia nervosa along dietary and negative affect dimensions: A replication in a treatment-seeking sample. Eating and Weight Disorders. 2001;6(1):53–8. doi: 10.1007/BF03339753. [DOI] [PubMed] [Google Scholar]
- Heatherton TF, Baumeister RF. Binge eating as escape from self-awareness. Psychological Bulletin. 1991;110(1):86–108. doi: 10.1037/0033-2909.110.1.86. [DOI] [PubMed] [Google Scholar]
- Kaye WH, Gendall KA, Fernstrom MH, Fernstrom JD, McConaha CW, Weltzin TE. Effects of acute tryptophan depletion on mood in bulimia nervosa. Biological Psychiatry. 2000;47(2):151–157. doi: 10.1016/s0006-3223(99)00108-0. [DOI] [PubMed] [Google Scholar]
- Kaye WH, Weltzin TE, Hsu GL. An open trial of fluoxetine in patients with anorexia nervosa. Journal of Clinical Psychiatry. 1991;52:464–471. [PubMed] [Google Scholar]
- Keel PK, Fichter M, Quadflieg N, Bulik CM, Baxter MG, Thornton L, et al. Application of a latent class analysis to empirically define eating disorder phenotypes. Archives of General Psychiatry. 2004;61:192–200. doi: 10.1001/archpsyc.61.2.192. [DOI] [PubMed] [Google Scholar]
- Killen JD, Taylor CB, Hayward C, Haydel KF, Wilson DM, Hammer L, et al. Weight concerns influence the development of eating disorders: a 4-year prospective study. Journal of Consulting and Clinical Psychology. 1996;64(5):936–940. doi: 10.1037//0022-006x.64.5.936. [DOI] [PubMed] [Google Scholar]
- Liang KY, Zeger SL. Longitudinal analysis using generalized linear models. Biometrika. 1986;73:13–22. [Google Scholar]
- Muthén B, Khoo ST. Longitudinal studies of achievement growth using latent variable modeling. Learning and Individual Differences. 1998;10:73–101. [Google Scholar]
- Muthén B, Muthén LK. Integrating person-centered and variable-centered analyses: growth mixture modeling with latent trajectory classes. Alcoholism, Clinical and Experimental Research. 2000;24(6):882–891. [PubMed] [Google Scholar]
- Muthén LK, Muthén B. Mplus user’s guide. Los Angeles: Muthén & Muthén; 1999–2004. [Google Scholar]
- Polivy J, Herman CP. Distress and eating: why do dieters overeat? International Journal of Eating Disorders. 1999;26:153–164. doi: 10.1002/(sici)1098-108x(199909)26:2<153::aid-eat4>3.0.co;2-r. [DOI] [PubMed] [Google Scholar]
- Ramaswamy V, DeSarbo W, Reibstein D, Robinson W. An empirical pooling approach for estimating marketing mix elasticities with PIMS data. Marketing Science. 1993;12:103–124. [Google Scholar]
- Schwartz G. Estimating the dimension of a model. Annals of Statistics. 1978;6:461–464. [Google Scholar]
- Sclove LS. Application of model-section criteria to some problems in multivariate analysis. Psychometrika. 1987;52:333–343. [Google Scholar]
- Smyth J, Wonderlich SA, Heron KE, Sliwinski MJ, Crosby RD, Mitchell JE, et al. Daily and momentary mood and stress are associated with binge eating and vomiting in bulimia nervosa patients in the natural environment. Journal of Consulting and Clinical Psychology. 2007;75(4):629–638. doi: 10.1037/0022-006X.75.4.629. [DOI] [PubMed] [Google Scholar]
- Stein KF, Corty CM. Ecological momentary assessment of eating-disordered behaviors. International Journal of Eating Disorders. 2003;34:349–360. doi: 10.1002/eat.10194. [DOI] [PubMed] [Google Scholar]
- Stice E. A prospective test of the dual-pathway model of bulimic pathology: Mediating effects of dieting and negative affect. Journal of Abnormal Psychology. 2001;110(1):124–135. doi: 10.1037//0021-843x.110.1.124. [DOI] [PubMed] [Google Scholar]
- Stice E. Risk and maintenance factors for eating pathology: A meta-analytic review. Psychological Bulletin. 2002;128(5):825–848. doi: 10.1037/0033-2909.128.5.825. [DOI] [PubMed] [Google Scholar]
- Stice E, Agras WS. Predicting onset and cessation of bulimic behaviors during adolescence: A longitudinal grouping analysis. Behavior Therapy. 1998;29:257–276. [Google Scholar]
- Stice E, Agras WS. Subtyping bulimic women along dietary restraint and negative affect dimensions. Journal of Consulting and Clinical Psychology. 1999;67(4):460–469. doi: 10.1037//0022-006x.67.4.460. [DOI] [PubMed] [Google Scholar]
- Stice E, Burton EM, Shaw H. Prospective relations between bulimic pathology, depression, and substance abuse: Unpacking comorbidity in adolescent girls. Journal of Consulting and Clinical Psychology. 2004;72(1):62–71. doi: 10.1037/0022-006X.72.1.62. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Strober M, Freeman R, Morrell W. The long-term course of severe anorexia nervosa in adolescents: Survival analysis of recovery, relapse, and outcome predictors over 10–15 years in a prospective study. International Journal of Eating Disorders. 1997;22(4):339–360. doi: 10.1002/(sici)1098-108x(199712)22:4<339::aid-eat1>3.0.co;2-n. [DOI] [PubMed] [Google Scholar]
- Waller G, Babbs M, Milligan R, Meyer C, Ohanian V, Leung N. Anger and core beliefs in the eating disorders. International Journal of Eating Disorders. 2003;34(1):118–124. doi: 10.1002/eat.10163. [DOI] [PubMed] [Google Scholar]
- Watson D, Clark LA, Tellegen A. Development and validation of brief measures of positive and negative affect: The PANAS scales. Journal of Personality and Social Psychology. 1988;54:1063–1070. doi: 10.1037//0022-3514.54.6.1063. [DOI] [PubMed] [Google Scholar]
- Westen D, Harnden-Fischer J. Personality profiles in eating disorders: Rethinking the distinction between Axis I and Axis II. American Journal of Psychiatry. 2001;158:547–562. doi: 10.1176/appi.ajp.158.4.547. [DOI] [PubMed] [Google Scholar]
- Wiesner M, Weichold K, Silbereisen RK. Trajectories of alcohol use among adolescent boys and girls: Identification, validation, and sociodemographic characteristics. Psychology of Addictive Behaviors. 2007;21(1):62–75. doi: 10.1037/0893-164X.21.1.62. [DOI] [PubMed] [Google Scholar]
- Wonderlich S, Crosby R, Joiner T, Peterson C, Bardone-Cone A, Klein M, et al. Personality subtyping and bulimia nervosa: Psychological and genetic correlates. Psychological Medicine. 2005;35:649–657. doi: 10.1017/s0033291704004234. [DOI] [PubMed] [Google Scholar]
- Wonderlich SA, Peterson C, Mitchell JE, Crow S. Integrative cognitive therapy for bulimia nervosa. In: Striegel-Moore R, Smolak L, editors. Eating disorders: New directions for research and practice. New York: American Psychological Association Press; 2001. pp. 173–196. [Google Scholar]