Abstract
OBJECTIVE: To determine the ability of carotid intima-media thickness (CIMT) and coronary artery calcium score (CACS) to detect subclinical atherosclerosis in a young to middle-aged, low-risk, primary-prevention population.
PATIENTS AND METHODS: Patients aged 36 to 59 years who underwent determination of CIMT and CACS at our institution between May 1, 2004, and April 1, 2008, were included in the study. Those with diabetes mellitus or a history of coronary, peripheral, or cerebral vascular disease were excluded. Other information, such as Framingham risk score (FRS), was obtained by a review of clinical and laboratory data.
RESULTS: Of 118 patients, 89 (75%) had a CACS of zero and 94 (80%) were men; mean ± SD age was 48.9±5.7 years. The mean FRS of this group was 4.0; 86 patients (97%) were considered at low risk (<1% annualized rate) of cardiovascular events. Evidence of carotid atherosclerosis was found in 42 (47%; 95% confidence interval, 37%-58%) of these 89 patients; carotid plaque was found in 30 (34%); and CIMT above the 75th percentile was found in 12 (13%) of age-, sex-, and race-matched control patients. Of the 40 patients with low-risk CIMT (below the 50th percentile), 4 (10%) had a CACS at or above the 50th percentile.
CONCLUSION: Subclinical vascular disease can be detected by CIMT evaluation in young to middle-aged patients with a low FRS and a CACS of zero. These findings have important implications for vascular disease screening and the implementation of primary-prevention strategies.
Subclinical vascular disease can be detected by carotid intima-media thickness evaluation in young to middle-aged patients with a low Framingham risk score and a coronary artery calcium score of zero; these findings have important implications for vascular disease screening and the implementation of primary-prevention strategies.
ARIC = Atherosclerosis Risk in Communities; CACS = coronary artery calcium score; CIMT = carotid intima-media thickness; CT = computed tomography; CVD = cardiovascular disease; FRS = Framingham risk score
…at the beginning a disease is easy to cure but difficult to diagnose; but as time passes, not having been recognized or treated at the outset, it becomes easy to diagnose but difficult to cure.
Niccolò Machiavelli (1469-1527)1
Cardiovascular disease (CVD) is the number one cause of mortality worldwide.2 Identifying the “vulnerable patient” is clinically important because the initial manifestation of CVD is sudden death in approximately 20% of patients,3 the prognosis of those who survive a vascular event is poor,4 and effective primary prevention strategies are available.5-7 However, it can be challenging to identify which patients will most benefit from a primary-prevention strategy beyond therapeutic lifestyle change. Population-based screening tools that assign a risk probability, such as the Framingham risk score (FRS), are effective in assigning risk to populations but are limited in their ability to characterize the risk of an individual.8-10
If subclinical atherosclerosis could be detected, risk could be individualized and insight gained into the interaction between a multitude of risk factors for vascular disease and a patient's unique genetic makeup. Two procedures that can identify sub-clinical atherosclerosis are ultrasonography of the carotid artery, which can detect plaque and determine carotid intima-media thickness (CIMT), and computed tomography (CT), which can assess calcification of the coronary arteries and determine a coronary artery calcium score (CACS). These measures not only characterize disease but also provide information predictive of a graded risk for adverse vascular events.11-18 Although both CIMT and CACS can characterize subclinical atherosclerosis, the correlation between the 2 measures is weak, probably because coronary calcification is a more advanced stage of vascular disease.19,20 Therefore, for young to middle-aged patients with plaque that has not yet calcified, a CACS of zero may be falsely reassuring. The purpose of this study was to determine whether CIMT and CACS would be useful in detecting subclinical vascular disease in a cohort of young to middle-aged patients in a primary-prevention population.
For editorial comment, see page 218
PATIENTS AND METHODS
This study enrolled patients aged 36 to 59 years who reported 1 or more cardiovascular risk factors (smoking, hyperlipidemia, hypertension, family history of premature coronary artery disease) and were seeking primary prevention but who did not exhibit symptoms of CVD. To be included in the study, patients had to have undergone determination of CACS and CIMT at our institution between May 1, 2004, and April 1, 2008; those determinations had to have occurred within 3 years of each other. All patients originally underwent CACS determination as a screening tool for identifying subclinical atherosclerosis; when CIMT evaluation became available, the patients underwent this test for further characterization of their cardiovascular risk. Patients were excluded from the study if they had diabetes mellitus or a history of coronary, peripheral, or cerebral vascular disease. Patients with a CACS of zero were placed into one group; patients with a low-risk CIMT score were placed into a second group. A low-risk CIMT score was defined as a score below the 50th percentile score of an age-, sex-, and race-matched control group, as determined by the Atherosclerosis Risk in Communities (ARIC) study.14 The study protocol was approved by the Mayo Clinic Institutional Review Board.
Coronary Artery Calcium Score
Electron-beam CT was used to evaluate coronary artery calcification. We obtained a CT scout image to determine the location of the heart. We then obtained a prospective electrocardiogram-gated scan with a 3-mm slice thickness from the level of the carina through the bottom of the heart. When coronary calcium was detected, we used an automated program based on the Agatston method21 to compute the CACS. The CACS percentiles were based on the scores of age- and sex-matched control patients.22
Carotid Intima-Media Thickness
The carotid arteries were imaged with a Siemens Sequoia ultrasonography system (Siemens Medical Solutions, Mountain View, CA) with an 8- to 15-MHz linear-array transducer). A depth of 4 cm was used. The examination included a thorough scan of the extracranial carotid arteries to detect carotid plaque, defined either as a thickening of the focal wall that was at least 50% greater than the thickening of the surrounding vessel wall or as a focal region with a CIMT of more than 1.2 mm. In the absence of identified plaque, the CIMT of the distal 1 cm of the far wall of the common carotid artery was measured by using a semiautomated border-detection program. The mean CIMT was calculated by averaging 3 measurements of CIMT at each of 3 scan planes (anterior, lateral, and posterior) from both the right and left common carotid arteries (18 total measurements). Using data from the ARIC Study, we calculated an age-, sex-, and race-matched percentile from the composite CIMT of the left and right common carotid arteries.14 If the quartile was discrepant between the right and left common carotid arteries, the highest quartile was assigned.
Framingham Risk Score
We performed a retrospective review of each patient's clinical chart to extract information and to calculate the FRS.23
Statistical Analyses
Data are summarized as mean ± SD or as frequencies and percentages. Using the exact binomial method, we calculated a 95% confidence interval for the proportion of patients who were found to have atherosclerosis by carotid examination. A McNemar association test comparing results from CIMT and CACS methods yielded a 2-tailed P value. Statistical significance was set at P<.05.
RESULTS
Baseline Characteristics
A total of 118 patients, of whom 94 (80%) were men, met the inclusion criteria for the study and underwent both CIMT and CACS evaluation. Of these, 89 (75%) had a CACS of zero. The mean ± SD age was 48.9±5.7 years. Vascular risk factors used in calculating the FRS included smoking (30%), hypertension (21%), and hyperlipidemia (47%). The patients' mean FRS was 4.0; according to the Framingham criteria, 86 (97%) of the patients were considered to be at low risk (<1% annualized cardiovascular event rate), whereas 3 had an FRS higher than 10 (>6% annualized cardiovascular event rate). For 80 patients (68%), CACS and CIMT evaluations were completed within 1 year of each other.
Carotid Intima-Media Thickness
Of the 89 patients with a CACS of zero, 42 (47%; 95% confidence interval, 37%-58%) had evidence of atherosclerosis by carotid examination. Of these patients, 30 (34%) had carotid plaque, and 12 (13%) had a CIMT higher than the 75th percentile for age-, sex-, and race-matched control patients. The mean FRS was 4.5 for patients with carotid plaque and 2.8 for those with a CIMT higher than the 75th percentile (Table; Figure 1). The McNemar 2-tailed P value for CIMT and CACS methods was less than .001. These findings were not statistically different when we compared the group of patients for whom CACS and CIMT evaluations were performed more than 1 year apart and those for whom the 2 studies were performed within 1 year.
TABLE.
CIMT Characteristics of 89 Patients With CACS of Zeroa
FIGURE 1.
Carotid intima-media thickness (CIMT) findings in 89 patients with a coronary artery calcium score of zero.
Patients With Low-Risk CIMT
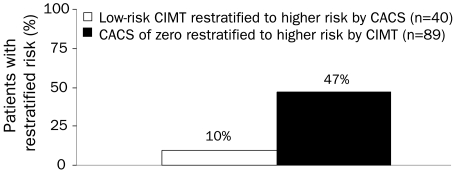
Forty patients had a low-risk CIMT (less than the 50th percentile for age-, sex-, and race-matched control patients from the ARIC Study and no plaque). The mean FRS for this group was 4.2. Four patients (10%) had a CACS at or higher than the 50th percentile, and 34 (85%) had a CACS of zero. Only 4 patients (10%) with a low-risk CIMT were placed into a higher risk category because of their CACS, whereas 47% of patients with a CACS of zero were placed into a higher risk category because their CIMT indicated atherosclerosis (Figure 2).
FIGURE 2.
Percentage of patients whose risk of cardiovascular disease was restratified to a higher level because of evaluations of either carotid intima-media thickness (CIMT) or coronary artery calcium score (CACS).
Patients With CACS Higher Than Zero
For the 29 patients with a CACS higher than zero, the average FRS was 5.9. Of these patients, 4 (14%) had carotid plaque, 14 (48%) had a CIMT higher than the 75th percentile, 6 (21%) had a CIMT between the 50th and 75th percentile, and 5 (17%) had a CIMT lower than the 50th percentile.
DISCUSSION
The principal finding of this study is that a substantial percentage of patients who have no clinically apparent atherosclerosis and a CACS of zero in fact have atherosclerotic disease, as determined by ultrasonography of the carotid arteries. The importance of this finding is emphasized by the well-established principle that atherosclerosis detected by ultrasonography of the carotid artery is a strong predictor of adverse cardiovascular events.12-15 This principle has been corroborated by investigators from Cedars-Sinai Medical Center, who found that 55% of a primary-prevention population with no calcification in the coronary arteries or the thoracic aorta had carotid artery plaque as demonstrated by ultrasonography.24 Most of our patients who had a low-risk CIMT (below the 50th percentile) also had a low-risk CACS (85% had a CACS below the 50th percentile). Only 15% of patients with a low-risk CIMT were placed into a higher risk category because of their CACS, whereas 47% of patients with a CACS of zero had a CIMT indicative of atherosclerosis. These findings support the notion that CIMT is a more sensitive test than CACS for the detection of subclinical atherosclerosis.
The goal of clinical medicine should be not only to treat but also to prevent disease. How best to determine which patients may benefit from more aggressive CVD prevention strategies before the occurrence of an adverse atherosclerotic event remains an enigma. Both CACS25 and CIMT26 have been advocated as clinical tools that can add incremental information for CVD risk stratification. A high CACS is helpful in determining that a patient is at an increased risk of adverse CVD events, but a CACS of zero suggests only that the patient's risk of a CVD event is low to intermediate over the ensuing 3 to 7 years.16-18,27,28 For young to middle-aged patients, this information may not be particularly helpful clinically. Certainly, short-term outcomes are important, but, given the substantial lifetime burden and the decades-long evolution of CVD, a more sensitive measure of subclinical atherosclerosis with a higher negative predictive value would be more relevant.
Whether screening for subclinical atherosclerosis decreases the incidence of future cardiovascular events has not yet been determined, but clinical guidelines recommend more aggressive preventive interventions for patients with an FRS indicating a high probability of disease.29 Therefore, until more data are available, a judgment-based approach to clinical medicine would support a strategy of early identification and treatment of disease. This strategy is similar to that supporting successful screening programs for breast, colon, and prostate cancer, programs that have become the expected standard of care.
Screening for CVD should not be limited merely to determining probability; ideally, it should detect early subclinical disease. The results of this study indicate that CIMT is more sensitive than CACS in detecting subclinical atherosclerosis in a young to middle-aged population for whom early identification and intervention would probably be most beneficial. The value of CACS is probably limited for this group; although arterial calcification indicates a later stage of vascular disease, its absence does not exclude the presence of noncalcified “vulnerable” plaque.
Preventive interventions that have been shown to decrease the incidence of adverse CVD events and death have not been effective in reducing CACS; however, they have been shown to slow the progression of CIMT and even to result in limited regression.30-32 In fact, on November 8, 2007, the US Food and Drug Administration approved rosuvastatin as an adjunct to diet to slow the progression of atherosclerosis, a decision based largely on the demonstration that the medication could slow the progression of atherosclerosis as defined by CIMT.30 Additionally, aggressive lipid lowering with atorvastatin has been shown to be more effective in reducing CIMT than conventional lipid-lowering therapy.31,32 Although ultrafast CT coronary angiography may also detect soft, noncalcified plaque, its use violates a fundamental tenet of preventive screening because it results in harmful exposures to radiation or contrast dye. On the basis of these concepts, the use of CIMT to clarify cardiovascular risk for selected patients is supported by the American Society of Echocardiography, the Society for Vascular Medicine,26 and the American Heart Association Prevention Conference V.33
The findings of this study are based on a relatively small sample size and are observational; the definitive effect of an intervention was not tested. However, large primary-prevention trials involving young to middle-aged patients with atherosclerosis as defined by CIMT will be both costly and lengthy. Until such trials are performed, clinicians must use a judgment-based approach to individual patient care. Such a judgment-based approach should use tools that can determine the presence or absence of early, “easy-to-treat” disease so that interventions can be performed. Some of our patients underwent CACS and CIMT evaluations that were as long as 36 months apart; however, this fact should not detract from the observation that those with a CACS of zero may have demonstrable disease as defined by CIMT. Another limitation of this study is that inclusion required that patients undergo evaluations of both CACS and CIMT; thus, the results may not be generalizable to a population with similar demographic characteristics. Nevertheless, CACS and CIMT evaluations were performed only at the request of the patient's physician as part of what was deemed an appropriate primary-prevention screening evaluation.
The Agatston method of measuring coronary calcium uses attenuation cofactors determined at a slice thickness of 3 mm. It is now possible to obtain subcentimeter resolution, which may detect very low levels of coronary calcium in some individuals with a CACS of zero as determined by the Agatston method. However, given the large volume of published studies based on the Agatston method, we continue to use this method of calcium scoring in our clinical practice.
CONCLUSION
A CIMT evaluation can detect subclinical vascular disease in young to middle-aged patients with a low FRS and a CACS of zero. These findings have important implications for vascular disease screening and the implementation of primary-prevention strategies.
REFERENCES
- 1.Machiavelli N. The Portable Machiavelli Bondanella PE, Musa M, trans-eds. London, England: Penguin; 2005. [Google Scholar]
- 2.World Health Organization Web site http://www.who.int/dietphysicalactivity/publications/facts/cvd/en/ Cardiovascular disease: prevention and control. 2003 Accessed January 6, 2009.
- 3.Thom T, Haase N, Rosamond W, et al. Heart disease and stroke statistics—2006 update: a report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee [published corrections appear in Circulation. 2006;113(14):e696 and 2006;114(23):e630] Circulation 2006February14;113(6):e85-e151 Epub 2006 Jan 11 [DOI] [PubMed] [Google Scholar]
- 4.Cannon CP, Braunwald E, McCabe CH, et al. Pravastatin or Atorvastatin Evaluation and Infection Therapy-Thrombolysis in Myocardial Infarction 22 Investigators Intensive versus moderate lipid lowering with statins after acute coronary syndromes [published correction appears in N Engl J Med. 2006; 354(7):778] N Engl J Med. 2004April8;350(15):1495-1504 Epub 2004 Mar 8 [DOI] [PubMed] [Google Scholar]
- 5.Downs JR, Clearfield M, Weis S, et al. AFCAPS/TexCAPS Research Group Primary prevention of acute coronary events with lovastatin in men and women with average cholesterol levels: results of AFCAPS/TexCAPS. JAMA 1998;279(20):1615-1622 [DOI] [PubMed] [Google Scholar]
- 6.Sever PS, Dahlöf B, Poulter NR, et al. ASCOT Investigators Prevention of coronary and stroke events with atorvastatin in hypertensive patients who have average or lower-than-average cholesterol concentrations, in the Anglo-Scandinavian Cardiac Outcomes Trial—Lipid Lowering Arm (ASCOT-LLA): a multicentre randomised controlled trial. Lancet 2003;361(9364):1149-1158 [DOI] [PubMed] [Google Scholar]
- 7.Shepherd J, Cobbe SM, Ford I, et al. West of Scotland Coronary Prevention Study Group Prevention of coronary heart disease with pravastatin in men with hypercholesterolemia. N Engl J Med. 1995;333(20):1301-1307 [DOI] [PubMed] [Google Scholar]
- 8.Khot UN, Khot MB, Bajzer CT, et al. Prevalence of conventional risk factors in patients with coronary heart disease. JAMA 2003;290(7):898-904 [DOI] [PubMed] [Google Scholar]
- 9.Magnus P, Beaglehole R. The real contribution of the major risk factors to the coronary epidemics: time to end the “only-50%” myth. Arch Intern Med. 2001;161(22):2657-2660 [DOI] [PubMed] [Google Scholar]
- 10.Nissen SE, Tuzcu EM, Schoenhagen P, et al. REVERSAL Investigators Effect of intensive compared with moderate lipid-lowering therapy on progression of coronary atherosclerosis: a randomized controlled trial. JAMA 2004;291(9):1071-1080 [DOI] [PubMed] [Google Scholar]
- 11.Ali YS, Rembold KE, Weaver B, et al. Prediction of major adverse cardiovascular events by age-normalized carotid intimal medial thickness. Atherosclerosis 2006July;187(1):186-190 Epub 2005 Oct 17 [DOI] [PubMed] [Google Scholar]
- 12.O'Leary DH, Polak JF, Kronmal RA, Manolio TA, Burke GL, Wolfson SK, Jr, Cardiovascular Health Study Collaborative Research Group Carotidartery intima and media thickness as a risk factor for myocardial infarction and stroke in older adults. N Engl J Med. 1999;340(1):14-22 [DOI] [PubMed] [Google Scholar]
- 13.Salonen JT, Salonen R. Ultrasound B-mode imaging in observational studies of atherosclerotic progression. Circulation 1993;87(3)(suppl):II56-II65 [PubMed] [Google Scholar]
- 14.Chambless LE, Heiss G, Folsom AR, et al. Association of coronary heart disease incidence with carotid arterial wall thickness and major risk factors: the Atherosclerosis Risk in Communities (ARIC) Study, 1987-1993. Am J Epidemiol. 1997;146(6):483-494 [DOI] [PubMed] [Google Scholar]
- 15.Salonen R, Salonen JT. Progression of carotid atherosclerosis and its determinants: a population-based ultrasonography study. Atherosclerosis 1990;81(1):33-40 [DOI] [PubMed] [Google Scholar]
- 16.Budoff MJ, Shaw LJ, Liu ST, et al. Long-term prognosis associated with coronary calcification: observations from a registry of 25,253 patients. J Am Coll Cardiol. 2007May8;49(18):1860-1870 Epub 2007 Apr 20 [DOI] [PubMed] [Google Scholar]
- 17.Greenland P, LaBree L, Azen SP, Doherty TM, Detrano RC. Coronary artery calcium score combined with Framingham score for risk prediction in asymptomatic individuals [published correction appears in JAMA. 2004; 291(5):563] JAMA 2004;291(2):210-215 [DOI] [PubMed] [Google Scholar]
- 18.Kondos GT, Hoff JA, Sevrukov A, et al. Electron-beam tomography coronary artery calcium and cardiac events: a 37-month follow-up of 5635 initially asymptomatic low- to intermediate-risk adults. Circulation 2003May27;107(20):2571-2576 Epub 2003 May 12 [DOI] [PubMed] [Google Scholar]
- 19.Davis PH, Dawson JD, Mahoney LT, Lauer RM. Increased carotid intimal-medial thickness and coronary calcification are related in young and middle-aged adults: the Muscatine study. Circulation 1999;100(8):838-842 [DOI] [PubMed] [Google Scholar]
- 20.Oei HH, Vliegenthart R, Hak AE, et al. The association between coronary calcification assessed by electron beam computed tomography and measures of extracoronary atherosclerosis: the Rotterdam Coronary Calcification Study. J Am Coll Cardiol. 2002;39(11):1745-1751 [DOI] [PubMed] [Google Scholar]
- 21.Agatston AS, Janowitz WR, Hildner FJ, Zusmer NR, Viamonte M, Jr, Detrano R. Quantification of coronary artery calcium using ultrafast computed tomography. J Am Coll Cardiol. 1990;15(4):827-832 [DOI] [PubMed] [Google Scholar]
- 22.Hoff JA, Chomka EV, Krainik AJ, Daviglus M, Rich S, Kondos GT. Age and gender distributions of coronary artery calcium detected by electron beam tomography in 35,246 adults. Am J Cardiol. 2001;87(12):1335-1339 [DOI] [PubMed] [Google Scholar]
- 23.Wilson PW, D'Agostino RB, Levy D, Belanger AM, Silbershatz H, Kannel WB. Prediction of coronary heart disease using risk factor categories. Circulation 1998;97(18):1837-1847 [DOI] [PubMed] [Google Scholar]
- 24.Mendoza F, Berman DS, Rafii F, et al. Does zero coronary or aortic calcium score predict the absence of carotid plaque [abstract 907-255]? J Am Coll Cardiol. 2008;51(10):A152 [Google Scholar]
- 25.Nasir K, Vasamreddy C, Blumenthal RS, Rumberger JA. Comprehensive coronary risk determination in primary prevention: an imaging and clinical based definition combining computed tomographic coronary artery calcium score and National Cholesterol Education Program risk score. Int J Cardiol. 2006June16;110(2):129-136 Epub 2005 Nov 21 [DOI] [PubMed] [Google Scholar]
- 26.Stein JH, Korcarz CE, Hurst RT, et al. Use of carotid ultrasound to identify subclinical vascular disease and evaluate cardiovascular disease risk: a consensus statement from the American Society of Echocardiography Carotid Intima-Media Thickness Task Force: endorsed by the Society for Vascular Medicine [published correction appears in J Am Soc Echocardiogr. 2008; 21(4):376] J Am Soc Echocardiogr. 2008;21(2):93-111 [DOI] [PubMed] [Google Scholar]
- 27.Arad Y, Goodman KJ, Roth M, Newstein D, Guerci AD. Coronary calcification, coronary disease risk factors, C-reactive protein, and atherosclerotic cardiovascular disease events: the St. Francis Heart Study. J Am Coll Cardiol. 2005;46(1):158-165 [DOI] [PubMed] [Google Scholar]
- 28.Detrano R, Guerci AD, Carr JJ, et al. Coronary calcium as a predictor of coronary events in four racial or ethnic groups. N Engl J Med. 2008;358(13):1336-1345 [DOI] [PubMed] [Google Scholar]
- 29.Grundy SM, Cleeman JI, Merz CN, et al. Implications of recent clinical trials for the National Cholesterol Education Program Adult Treatment Panel III guidelines [published correction appears in Circulation. 2004;110(6):763] Circulation 2004;110(2):227-239 [DOI] [PubMed] [Google Scholar]
- 30.Crouse JR, III, Raichlen JS, Riley WA, et al. METEOR Study Group Effect of rosuvastatin on progression of carotid intima-media thickness in low-risk individuals with subclinical atherosclerosis: the METEOR Trial. JAMA 2007March28;297(12):1344-1353 Epub 2007 Mar 25 [DOI] [PubMed] [Google Scholar]
- 31.Taylor AJ, Kent SM, Flaherty PJ, Coyle LC, Markwood TT, Vernalis MN. ARBITER: Arterial Biology for the Investigation of the Treatment Effects of Reducing Cholesterol: a randomized trial comparing the effects of atorvastatin and pravastatin on carotid intima media thickness. Circulation 2002;106(16):2055-2060 [DOI] [PubMed] [Google Scholar]
- 32.Smilde TJ, van Wissen S, Wollersheim H, Trip MD, Kastelein JJ, Stalenhoef AF. Effect of aggressive versus conventional lipid lowering on atherosclerosis progression in familial hypercholesterolaemia (ASAP): a prospective, randomised, double-blind trial. Lancet 2001;357(9256):577-581 [DOI] [PubMed] [Google Scholar]
- 33.Smith SC, Jr, Greenland P, Grundy SM. AHA Conference Proceedings: prevention conference, V: beyond secondary prevention: identifying the high-risk patient for primary prevention: executive summary. Circulation 2000;101(1):111-116 [DOI] [PubMed] [Google Scholar]