Abstract
It has been reported that 4-1BB triggering in vivo selectively suppressed the recall response of staphylococcal enterotoxin A (SEA)-specific CD4+ T cells, in which CD8+ T-derived TGF-β was involved. Here, we have examined an alternative mechanism for the 4-1BB-mediated CD4+ T suppression, as the neutralization of TGF-β is only effective in rescuing the SEA-specific recall response at high cellular concentrations. We show that this selective suppression of CD4+ T cells by 4-1BB triggering in vivo is mediated mainly by induction of indoleamine 2,3-dioxygenase (IDO) in an IFN-γ-dependent manner. SEA-specific CD4+ T responses were suppressed partly by TGF-β-expressing CD8+ T cells, particularly CD11c+CD8+ T cells, but strongly inhibited by dendritic cells (DCs) expressing IDO. IFN-γ that increased IDO in DCs was produced primarily from CD11c+CD8+ T cells, which were expanded selectively by 4-1BB stimulation. CD4+, CD8+, and plasmacytoid DCs exerted a similar suppressive activity toward the SEA-specific CD4+ T cells. Neutralization of IFN-γ or IDO activity in vivo largely reversed the 4-1BB-mediated CD4+ T suppression. Collectively, these data indicate that 4-1BB-dependent suppression of SEA-specific CD4+ T responses was mediated mainly by IFN-γ-dependent IDO induction and partially by TGF-β.
Keywords: SEA, T cells, costimulation
INTRODUCTION
4-1BB, an inducible T cell surface receptor present on CD4+, CD8+, NK 1.1, and dendritic cells (DCs), provides CD28-independent costimulation of T cell activation [1,2,3]. 4-1BB-mediated signaling plays a critical role in preventing activation-induced cell death, promoting the rejection of cardiac allografts and skin transplants, enhancing integrin-mediated cell adhesion, and increasing T cell cytolytic potential [1, 3, 4], as well as in eradicating established tumors [3, 5,6,7]. However, recent studies suggest that in vivo 4-1BB stimulation can have immune-boosting and immune-suppressing effects at the same time [8, 9]. In vivo 4-1BB stimulation suppresses CD4+ T cell responses and ameliorates autoimmune diseases such as systemic lupus erythematosus and rheumatoid arthritis [10,11,12,13]. We showed previously that 4-1BB-mediated suppression of collagen-induced arthritis (CIA) is caused by an expansion of CD11c+CD8+ T cells and that the IFN-γ produced by these cells suppresses antigen-specific CD4+ T cells through the induction of indoleamine 2,3-dioxygenase (IDO) in DCs [11].
The tryptophan-catabolizing enzyme, IDO, contributes to maternal tolerance during pregnancy [14], the suppression of anti-tumor response by tumor cells [15], autoimmune diseases [11] and allergic inflammation [16, 17], and control of hyperinflammatory responses [18]. In infection, IDO plays a critical role in controlling the balance between Th cells and T regulatory cells (Tregs) to prevent excessive inflammation [19]. During inflammation, IDO is induced in DCs by stimulation via TLR9 [20], CD80 [21], CD40 [22], and glucocorticoid-induced TNFR ligand (GITRL) [17] as well as proinflammatory cytokine IFN-γ [11]. This process contributed to IDO-mediated Treg generation through nocanonical NF-κB signaling [23]. Tregs induce the IDO production in plasmacytoid DCs (pDCs) by using reverse signaling [17, 21, 23]. As IDO-mediated immune regulation has been implicated in suppressing the T cell responses and promoting the immune tolerance, it is interesting that the marked enhancement of the CD8+ T cell response by 4-1BB triggering is linked with the IDO-dependent suppression of CD4+ T cell immunity.
Superantigens stimulate strong proliferative responses in CD4+ and CD8+ T cells through specific interactions with the Vβ-chains of their TCRs [24]. The injection of staphylococcal enterotoxin A (SEA) is a well-established model that induces T cell unresponsiveness after immune hyperactivity in vivo [25]. However, in vitro exposure of SEA induces IL-17 secretion from T cells with effector cell generation [26]. In vivo injection of SEA is also known to lead to induction of highly suppressive Tregs [25, 27]. Using the SEA model, Myers et al. [28] showed that 4-1BB costimulation with TLR triggering could generate suppressor CD8+ T cells, of which suppressive activity was involved with TGF-β. Although this report stated that the suppressive effect on CD4+ T cells was mediated directly by CD8+ T cells expressing TGF-β, we thought it possible that an alternative mechanism could be involved in 4-1BB-mediated CD4+ T suppression, as the neutralization of TGF-β is only effective to rescue the SEA-specific recall proliferation at high cellular concentrations.
Therefore, we examined the roles of TGF-β and IDO in 4-1BB-mediated suppression of CD4+ T cells in the SEA model. By treating SEA-challenged mice with agonistic anti-4-1BB mAb as well as with neutralizing anti-IFN-γ mAb, IDO inhibitor 1-methyl-DL-tryptophan (1-MT), and anti-TGF-β mAb, we examined whether the 4-1BB-mediated suppression of CD4+ T cells was mediated mainly by IFN-γ-dependent IDO induction or TGF-β. We found that the neutralization of IFN-γ or IDO activity reversed the proliferation of SEA-specific CD4+ T cells profoundly but that anti-TGF-β mAb treatment produced only marginal recovery in the SEA-specific CD4+ T cells after 4-1BB-mediated suppression in vitro and in vivo. These results indicate that IFN-γ-dependent IDO induction and not TGF-β is the major factor in CD4+ T suppression.
MATERIALS AND METHODS
Mice and reagents
C57BL/6 mice (6–8 weeks old) were purchased from The Jackson Laboratory (Bar Harbor, ME, USA). 4-1BB−/− (H-2Kb) C57BL/6 mice were bred in a specific pathogen-free facility at the University of Ulsan (Ulsan, Korea). IDO−/− C57BL/6 mice were kindly provided by Dr. Andrew L. Mellor (Medical College of Georgia, Augusta, GA, USA). SEA was purchased from Toxin Technology (Madison, WI, USA). BrdUrd was purchased from Sigma-Aldrich (St. Louis, MO, USA). The IDO inhibitor, 1-MT, was purchased from Innovative Research of America (Sarasota, FL, USA) and Sigma-Aldrich.
Antibodies and microbeads
Agonistic anti-mouse 4-1BB mAb-producing hybridoma (3H3) was a generous gift from Dr. Robert Mittler (Emory University, Atlanta, GA, USA). The antibody was produced from ascites and was purified by a protein G-column (Sigma-Aldrich). Purified rat IgG was purchased from Sigma-Aldrich and served as a control antibody. The following mAb were purchased from BD PharMingen (San Diego, CA, USA) for flow cytometry: FITC-, PE-, PE-Cy4-, or biotin-anti-CD8α (53-6.7); FITC- or PE-anti-CD8β (Ly-3.2, 53-5.8); PE- or PE-Cy5-anti-CD4 (H129.19); FITC-, PE-, or biotin-anti-CD11c (HL3); FITC-Vβ3 (KJ25); PE-anti-Fas ligand (FasL; MFL3); PE- or biotin-anti-CD11b (M1/70); biotin-anti-CD25 (7D4); biotin-anti-CD40 (3/23); biotin-anti-B220 (RA3-6B2); anti-IFN-γ (XMG1.2); biotin-anti-TGF-β1 (A75-3.1); purified anti-CD16/CD32 (2.4G2); and PE- or FITC-streptavidin. PE-Cy5-anti-CD8β (Ly3.2, 53-5.8) and biotin-anti-F4/80 (BM8) were purchased from eBioscience (San Diego, CA, USA). CD4-, CD8-, CD11c-, and streptavidin-conjugated microbeads were purchased from Miltenyi Biotec (Auburn, CA, USA).
Treatment
SEA was administered i.p. at a dose of 0.30 μg/mice. For 4-1BB stimulation, SEA-injected mice were injected i.p. with 200 mg anti-4-1BB mAb (3H3, rat IgG2a) or rat IgG as control on postinjection (PI) Days 0 and 2. To neutralize IFN-γ or TGF-β, mice were injected i.p with 500 mg purified R4-6A2 [American Type Culture Collection (ATCC), Manassas, VA, USA] or 1D11 (ATCC) on Days –1, 4, and 7. To inhibit IDO activity, slow-release polymer pellets (10 mg/day 1-MT for 10 days) or placebo pellets were implanted under the dorsal skin 1 day before SEA injection.
Flow cytometry
SEA-injected C57BL/6 mice were injected i.p. with anti-4-1BB mAb or rat IgG on PI Days 0 and 2. The inguinal lymph node (ILN) cells were collected and preincubated with Fc blocker 2.4G2 for 10 min. To determine the phenotype of CD8+ T cells, the cells were stained with PE-Cy5-conjugated anti-CD8, PE-conjugated anti-CD11c, and FITC-conjugated Vβ3-TCR or FITC-conjugated anti-FasL. To examine IFN-γ and TGF-β, spleen and ILN cells were stimulated with 50 ng/ml PMA and 500 ng/ml ionomycin in the presence of 1 mM brefeldin A (Golgiplug, BD PharMingen) for 5 h. The incubated cells were first stained with PE-Cy5-conjugated anti-CD8 and PE-conjugated anti-CD11c and then fixed and permeabilized with the Cytofix/cytoperm kit (BD PharMingen) according to the manufacturer’s instructions. The permeabilized cells were incubated further with FITC-conjugated anti-IFN-γ or anti-TGF-β mAb. All samples were analyzed subsequently on a FACScan.
Calculation of absolute numbers (AN) of CD4+, CD8+, and Vβ3+ T cells
Viable cells were recovered from the draining lymph nodes (DLN) and counted by hemacytometer; aliquots were stained with fluorescent antibodies specific for Vβ3, CD4+, and CD8+ T cell markers. The AN of each cell subset were calculated by multiplying the percentage of a given cell type, measured by flow cytometry, by the total number of viable cells (AN=percent×total cells recovered).
BrdU incorporation assay
To measure the proliferation of T cells, spleen and ILN cells were prepared from rat IgG- or anti-4-1BB mAb-treated mice on PI Day 10, restimulated with 0.1 μg/ml SEA for 3 days, and labeled with BrdU for the final hour. The cells were surface-stained with PE-conjugated anti-CD4 or anti-CD8 mAb and then stained intracellularly with FITC-conjugated anti-BrdU according to the manufacturer’s instructions (BD Biosciences, San Jose, CA, USA).
RT-PCR
For IDO and inducible NO synthetase (iNOS) RT-PCR, total cellular RNA was prepared from DCs or macrophages using Trizol (Invitrogen, Carlsbad, CA, USA) following the manufacturer’s instructions. First-strand cDNA was synthesized from total RNA using Superscript II (Invitrogen) and oligo(dT)12–18. PCR was performed in a 20-μl reaction mixture with 0.5 mg/ml cDNA and 0.5 mM each of the following primers: IDO (sense, 5′-CACTGTATCCAGTGCAGTAG-3′, and antisense, 5′-ACCATTCACACACTCGTTAT-3′), iNOS (sense, 5′-AAGTCAAATCCTACCAAAGTGA-3′, and antisense, 5′-CCATAATATGGTTGATGAACT-3′), and GAPDH (sense, 5′-GAACGGGAAGCTTGTCATCAA-3′, and antisense, 5′-CTAAGCAGTTGGTGGTGCAG-3′). PCR amplification was done for 40 cycles to detect IDO and iNOS for 45 s at 94°C, 45 s at 47°C, and 1 min at 72°C and 30 cycles for GAPDH for 45 s at 94°C, 45 s at 68°C, and 1 min at 72°C.
Purification of macrophages and DCs
Spleen and ILN were collected from SEA-injected mice on PI Day 10, cut into small pieces, and incubated with collagenase type II (1 mg/ml; Sigma-Aldrich) and DNase I (15 mg/ml; Roche Biotech, Switzerland) at 37°C for 40 min. To purify CD11c+ DCs, T cells were depleted with CD90 microbeads (Miltenyi Biotec) twice, and the T cell-depleted cell fraction was incubated further with CD11c microbeads. Macrophages were isolated from ILN cells using CD11b microbeads. Subpopulations of DCs were isolated for T–DC coculture experiments. To purify pDCs, ILN cells were incubated with pDC antigen 1 (PDCA-1) microbeads. The CD90-depleted cell fraction was depleted further with CD4 microbeads to isolate CD4-CD11c+ DCs or with CD8 microbeads to isolate CD8-CD11c+ DCs. CD4-CD11c+ and CD8-CD11c+ DCs were then purified by incubating the CD4-depleted or CD8-depleted cell fraction with CD11c microbeads. The purity of DCs and macrophages was >92% by FACScan.
Purification of CD4+ and CD8+ T cells
Spleen and ILN cells were collected from SEA-injected mice on PI Day 10, and CD8+ T cells were purified using the MACS magnetic separation system according to the manufacturer’s instructions (Miltenyi Biotec). In brief, the single-cell suspension was preincubated with 2.4G2 for 10 min at 4°C and then incubated with CD8 microbeads. CD8+ T cells were isolated by loading the cells on an LS column. To isolate CD25–CD4+ T cells, CD25+ cells were depleted by adding a biotinylated anti-CD25 mAb and streptavidin microbeads, and then CD4+ cells were purified from the negatively selected cell fraction with CD4 microbeads. The CD8+ and CD4+ populations were >95% pure by flow cytometry.
Isolation of CD11c+CD8+ and CD11c–CD8+ T cells
Single-cell suspensions were prepared from spleens and ILN of anti-4-1BB mAb-treated mice. CD11c+CD8+ T cells and CD11c–CD8+ T cells were separated by MACS separation columns (Miltenyi Biotec). CD11c+CD8+ T cells were purified by immunomagnetically deleting CD4+, F4/80+, CD40+, and B220+ cell populations by incubation with the relevant antibodies. Negatively selected cells were incubated further with anti-mouse CD11c (N418)-conjugated microbeads: CD11c+CD8+ T cells were purified positively from the negatively selected cells with CD11c microbeads, and CD11c–CD8+ T cells were isolated further from the remaining cells with CD8 microbeads (Miltenyi Biotec). The purity of the isolated cells was >95% on flow cytometry.
T–DC coculture
CD4+ T cells were isolated from spleens and ILN of SEA-injected mice on PI Day 10. The purified CD4+ T cells were cocultured with the CD11c+, PDCA-1+, CD4–CD11c+, or CD8–CD11c+ DCs at a 5:1 ratio in the presence or absence of 0.1 mg/ml SEA. The cultures were incubated for 72 h and pulsed with [3H]-thymidine (1.0 mCi/well) (Amersham Pharmacia, Piscataway, NJ, USA) during the last 12 h. The incorporated radioactivity was counted (Wallac, Perkin Elmer, Wellesley, MA, USA).
Statistical analysis
All data were analyzed using a statistical program (Prism 4.0, GraphPad, San Diego, CA, USA). Student’s t-test was used to determine statistical significance between groups, and P < 0.05 was considered significant.
RESULTS
In vivo 4-1BB triggering leads to the selective expansion of CD8+ T cells and the suppression of CD4+ T cells specific for SEA
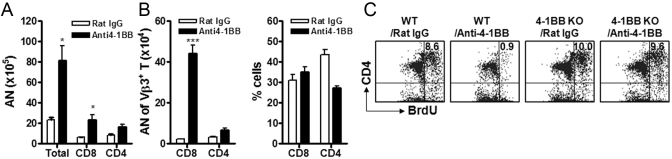
Previous reports suggested that 4-1BB triggering actively induces suppression of SEA-specific CD4+ T cells in B10BR mice by increasing TGF-β on CD8+ T cells [28]. However, the same treatment with anti-4-1BB mAb also induced strong suppression of antigen-specific CD4+ T cells in autoimmune disease models [11]. We therefore evaluated the contributions of TGF-β and IDO to 4-1BB-mediated CD4+ T cell suppression. C57BL/6 mice were injected i.p. with 0.3 μg SEA and then received 200 μg anti-4-1BB mAb or rat IgG on PI Days 0 and 2. We analyzed the AN of total lymphocytes, CD4+ T cells, and CD8+ T cells in the ILN to determine whether 4-1BB triggering rescued the peripheral deletion of CD4+ and CD8+ T cells. It is known that injection of peptides or superantigens into mice leads to significant clonal expansion followed by peripheral deletion of the responding T cells [29,30,31]. Consistent with a previous report [28], treatment with anti-4-1BB mAb in vivo increased not only the AN but also the percentage of CD8+ T cells (Fig. 1A). In particular, SEA-specific Vβ3, TCR-positive CD8+ T cells were increased 45-fold by 4-1BB triggering (0.9×104±0.2×104 cells in IgG-treated mice vs. 44.1×104±1.2×104 in anti-4-1BB mAb-treated mice; Fig. 1A). In the case of CD4+ T cells, the AN were increased slightly, but the proportion was decreased, which indicated that in vivo 4-1BB triggering reversed the ratio of CD4+ and CD8+ T cells (Fig. 1B).
Fig. 1.
In vivo 4-1BB triggering blocks the peripheral deletion of CD4+ T and CD8+ T cells but suppresses the recall proliferative response of CD4+ T cells. C57BL/6 mice were injected i.p. with 0.3 μg SEA. Anti-4-1BB mAb or rat IgG was administered i.p. (200 μg/injection) on PI Days 0 and 2. (A, B) Viable cells were recovered from the DLN, total numbers were counted by hemacytometer, and DLN cells were stained with FITC-conjugated anti-CD8 and PE-conjugated anti-CD4 and FITC-conjugated anti-Vβ3 and PE-conjugated anti-CD4 or anti-CD8. The AN of CD4+ and CD8+ T cell subsets were calculated by multiplying the percentage measured by flow cytometry by the total number of viable cells recovered from the same culture (AN=percent×total cells recovered). (C) For BrdU incorporation, cells were isolated from DLN on Day 10 and incubated with 0.1 μg/ml SEA for 3 days. The incubated cells were stained with PE-conjugated anti-CD4, intracellularly stained with FITC-conjugated anti-BrdU, according to the manufacturer’s instructions (BD Biosciences), and analyzed on FACScan. The plotted data are means ± sd (*, P<0.05; ***, P<0.001). The results are representative of three independent experiments. WT, Wild-type; KO, knockout.
To assess the role of 4-1BB in the recall response of SEA-specific CD4+ T cells on PI Day 10, ILN cells were isolated from WT and 4-1BB-deficient mice that had been treated with rat IgG or anti-4-1BB mAb as well as SEA. By restimulating ILN cells with SEA and labeling the proliferating cells with BrdU for last 1 h of the 3-day incubation, SEA-specific CD4+ T responses were examined in each group of mice. We found that the SEA-specific CD4+ T response was only suppressed in the mice receiving anti-4-1BB mAb but not in the other experimental groups (Fig. 1C). These results indicate that in vivo 4-1BB triggering blocks the peripheral deletion of CD4+ and CD8+ T cells but inhibits the recall response of SEA-specific CD4+ T cells along with massive expansion of SEA-specific CD8+ T cells.
4-1BB triggering leads to the expansion of CD11c+CD8+ T cells producing IFN-γ and TGF-β and induction of IDO in APCs
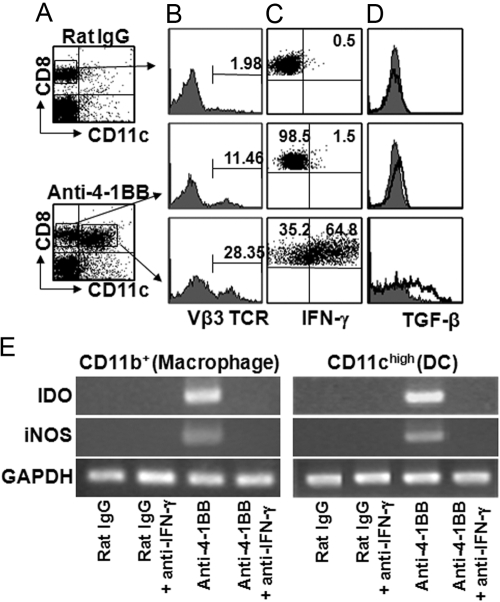
As changes in CD11c+CD8+ T cells are the most prominent cellular effect resulting from the treatment with anti-4-1BB mAb [8, 11], we examined whether CD11c+CD8+ T cells were expanded in SEA-injected mice by triggering with 4-1BB. ILN cells were collected from rat IgG- or anti-4-1BB mAb-treated mice on PI Day 10 and stained with fluorescence-conjugated anti-CD8 and anti-CD11c mAb. 4-1BB triggering induced the expansion of CD11c+CD8+ T cells (Fig. 2A). To determine whether the CD11c+CD8+ T cells included SEA-specific CD8+ T cells, CD11c+CD8+ T cells were stained with an anti-Vβ3-TCR mAb, which was known to be specific for SEA-reactive T cells. In rat IgG-treated mice, 1.98 ± 0.21% Vβ3-positive CD8+ T cells were found. In anti-4-1BB mAb-treated mice, 11.4 ± 1.2% Vβ3-positive T cells were found in CD11c–CD8+ T cells, and 28.4 ± 0.37% were found in CD11c+CD8+ T cells. These results indicate that >75% of the Vβ3-positive CD8+ T cells in anti-4-1BB mAb-treated mice are included in the CD11c+CD8+ T cells (Fig. 2B).
Fig. 2.
4-1BB triggering induces IFN-γ and TGF-β in CD11c+CD8+ T cells and IDO in APCs. SEA-injected C57BL/6 mice were injected i.p. with 200 μg rat IgG or anti-4-1BB mAb on PI Days 0 and 2. (A, B) On PI Day 10, ILN cells were stained with fluorescent antibodies specific for CD8β, CD11c, and TCR-Vβ3. (C, D) ILN cells were incubated with 0.1 μg SEA for 6 h in the presence of brefeldin A. The incubated cells were stained for cell-surface molecules (CD8 and CD11c) and further, stained intracellularly against IFN-γ and TGF-β. All samples were analyzed on FACScan. The data are representative of three independent experiments. (E) C57BL/6 mice received SEA as well as rat IgG or anti-4-1BB mAb, and some mice were additionally treated with anti-IFN-γ mAb on PI Days –1, 4, and 7. CD11b+ macrophages or CD11c+ DCs were purified from each group of mice on PI Day 10. cDNA was synthesized from the RNA of the purified macrophages and DCs, and transcript levels of IDO and iNOS were confirmed by PCR. The data are representative of three independent experiments.
4-1BB triggering is known to increase IFN-γ and TGF-β in CD8+ T cells that are involved in CD4+ T suppression [11, 28] and also massively increases CD11c+CD8+ T cells. Therefore, we examined whether the CD11c+CD8+ T cells would express TGF-β. When IFN-γ and TGF-β were stained intracellularly in CD11c–CD8+ and CD11c+CD8+ T cells, IFN-γ was preferentially produced from CD11c+CD8+ T cells rather than CD11c–CD8+ T cells in anti-4-1BB mAb-treated mice. IFN-γ production by CD11c+CD8+ T cells was ∼43-fold higher than that of CD11c–CD8+ T cells (64.8±0.8% vs. 1.5±0.13%; Fig. 2C). TGF-β was also induced on CD8+ T cells by anti-4-1BB mAb treatment, which was restricted in CD11c+CD8+ T cells (Fig. 2D).
Expansion of CD11c+CD8+ T cells and massive IFN-γ production were similar to that seen in 4-1BB-mediated CD4+ T suppression in CIA [11]. Therefore, we next tested whether the increased IFN-γ induced the expression of IDO in APCs such as macrophages and DCs. C57BL/6 mice were treated with SEA as well as rat IgG or anti-4-1BB mAb and additionally, with 500 μg anti-IFN-γ mAb on PI Days –1, 4, and 7. On PI Day 10, IDO and iNOS mRNAs were assessed in DCs and macrophages of DLN. 4-1BB triggering induced transcripts of IDO and iNOS in DCs and macrophages; this effect was reversed by neutralizing IFN-γ (Fig. 2E) but not by blockade of TGF-β (Supplemental Fig. 1).
Taken together, these results indicate that 4-1BB triggering increases the expression of IFN-γ and TGF-β, which is restricted to the CD11c+CD8+ T cells, and also induces the expression of IDO in APCs.
4-1BB triggering suppresses CD4+ T cells through CD8+ T cells and APCs
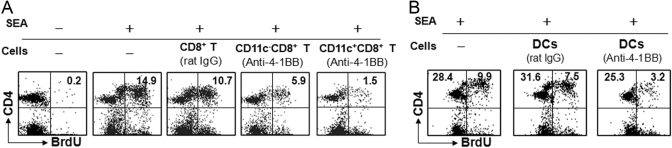
Having found the induction of TGF-β in CD8+ T cells and IDO in APCs, we sought to determine if both cells would suppress SEA-specific CD4+ T cells. SEA-experienced CD4+ T cells were cocultured with CD11c–CD8+ T cells, CD11c+CD8+ T cells, or DCs from IgG- or anti-4-1BB mAb-treated mice in the presence of SEA. The recall proliferation of CD4+ T cells was analyzed by BrdU incorporation. CD4+ T proliferation was suppressed strongly by CD11c+CD8+ T cells from anti-4-1BB mAb-treated mice (1.5±0.2%) and modestly by CD11c–CD8+ T cells (5.9±0.9%). However, CD8+ T cells from rat IgG-treated mice did not suppress the proliferation of CD4+ T cells (10.7±1.6%; Fig. 3A). In a separate experiment, when the CD11c+CD8+ T cells were cocultured with freshly isolated CD11c+ DCs in vitro, those DCs induced IDO transcripts that suppress the recall proliferation of CD4+ T cells (data not shown). The proliferation of CD4+ T cells was also suppressed by CD11chigh DCs from anti-4-1BB mAb-treated mice (3.2±0.1%) but not by DCs from rat IgG-treated mice (7.5±0.9%; Fig. 3B). CD11b+ macrophages from anti-4-1BB mAb-treated mice suppressed proliferation of CD4+ T cells in coculture (data not shown).
Fig. 3.
CD8+ T cells and DCs mediate the suppressive effects of 4-1BB triggering. SEA-injected C57BL/6 mice were injected i.p. with rat IgG or anti-4-1BB mAb on PI Days 0 and 2. Cells were isolated from ILN on PI Day 10, and then populations, including CD11c+CD8+ T cells, CD11c–CD8+ T cells, and CD11chigh DCs, were purified. Responder CD4+ T cells were purified from rat IgG-treated mice. (A) CD11c+CD8+ T or CD11c–CD8+ T cells were cultured with CD4+ T cells in the presence or absence of 0.1 μg/ml SEA for 3 days, and CD11c+ DCs from naïve mice were added to each well at 10% of cultured whole cells. (B) CD11chigh DCs from the rat IgG- or anti-4-1BB-treated group were cultured with CD4+ T cells in the presence of 0.1 μg/ml SEA for 3 days. The incubated cells were stained with PE-conjugated anti-CD4 and intracellularly stained with FITC-conjugated anti-BrdU according to the manufacturer’s instructions (BD Biosciences). All samples were analyzed on FACScan. The data are representative of three independent experiments.
Taken together, these results suggest that CD11c+CD8+ T cells and APCs are involved in the 4-1BB-mediated suppression of CD4+ T cells.
Minor involvement of TGF-β in 4-1BB-mediated suppression of CD4+ T cells
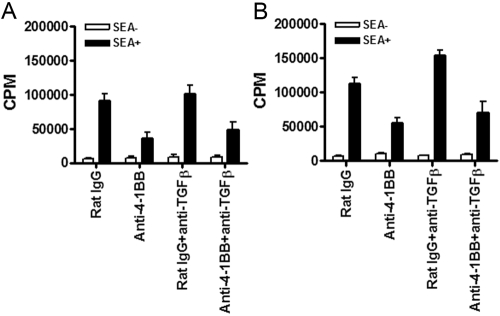
In that CD8+ T cells increased TGF-β by 4-1BB triggering and suppressed SEA-specific CD4+ T cells, we tested the involvement of TGF-β in 4-1BB-mediated suppression of CD4+ T cells in vitro and in vivo. C57BL/6 mice were given SEA as well as rat IgG or anti-4-1BB mAb. ILN cells were restimulated with SEA in the presence or absence of anti-TGF-β mAb (1D11) in vitro for 3 days. Neutralization of TGF-β in vitro only marginally reversed the 4-1BB-mediated suppression (Fig. 4A). This experiment was repeated many times; all experiments showed similar results. In vivo neutralization of TGF-β with anti-TGF-β mAb treatment of rat IgG- or anti-4-1BB mAb-treated mice also demonstrated that TGF-β did not make a critical contribution to the 4-1BB-mediated suppression, as the neutralization of TGF-β did not reverse >20% of the 4-1BB-mediated suppression (Fig. 4B).
Fig. 4.
Minor effects of TGF-β neutralization in vitro and in vivo. C57BL/6 mice received SEA along with rat IgG or anti-4-1BB mAb. (A) In vitro neutralization of TGF-β. Beginning on PI Day 10, ILN cells were restimulated with SEA in the presence or absence of 10 μg/ml anti-TGF-β mAb for 3 days. (B) In vivo neutralization of TGF-β. SEA-challenged mice were additionally treated with 500 μg anti-TGF-β mAb on PI Days –1, 4, and 7. Beginning on PI Day 10, ILN cells were restimulated with SEA for 3 days and labeled with [3H]-thymidine for the last 8 h.
These results imply that CD11c+CD8+ T cells suppress CD4+ T cells by alternative mechanisms. Therefore, we conclude that 4-1BB-triggered CD8+ T cells suppress SEA-reactive CD4+ T cells, which may be mediated by IFN-γ-induced IDO expression from DCs, but TGF-β is not the major suppressive factor.
IFN-γ and IDO mediate the suppression of SEA-specific CD4+ T cells by anti-4-1BB treatment
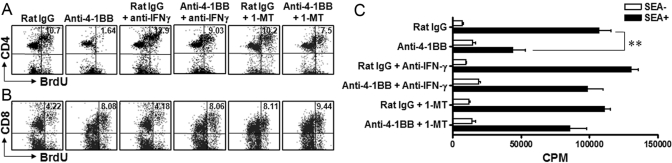
We showed that DCs from anti-4-1BB mAb-treated mice suppress the proliferation of CD4+ T cells in the recall response (Fig. 3B). Therefore, we examined whether IFN-γ and IDO are involved in 4-1BB-mediated suppression of CD4+ T cells. To inhibit IFN-γ or IDO activity, rat IgG- or anti-4-1BB mAb-treated mice received the neutralizing anti-IFN-γ mAb or were implanted with slow-release polymer pellets containing 1-MT (a pharmacological inhibitor of IDO) or placebo under the dorsal skin.
On PI Day 10, spleen and ILN cells were prepared from each group of mice and stimulated with SEA. SEA-specific recall proliferation of CD4+ T cells was measured by the incorporation of BrdU or [3H]-thymidine. 4-1BB-mediated suppression of SEA-specific CD4+ T cells was reversed by treating with the neutralizing anti-IFN-γ mAb or 1-MT. The incorporation of BrdU in CD4+ T cells was 10.7 ± 2.7% in the group treated with rat IgG and decreased to 1.6 ± 0.5% in 4-1BB-treated mice (Fig. 5A). With inhibition of IFN-γ or IDO, CD4+ T proliferation was restored to 9.0 ± 1.2% or 7.5 ± 0.8%, respectively (Fig. 5A). However, CD8+ T cell responses were not affected significantly by treatment with anti-IFN-γ or 1-MT (Fig. 5B). The expansion of CD11c+CD8+ T cells was also increased by anti-4-1BB mAb in WT and IFN-γ-deficient mice, indicating that IFN-γ did not affect the expansion of the double-positive T cells (Supplemental Fig. 2). Consistent with the BrdU incorporation, we obtained similar results using the [3H]-thymidine incorporation assay, demonstrating reversal of the 4-1BB-mediated suppression following treatment with anti-IFN-γ or 1-MT (Fig. 5C).
Fig. 5.
IFN-γ and IDO mediate 4-1BB suppression of SEA-specific CD4+ T cells. SEA-injected C57BL/6 mice were treated with rat IgG or anti-4-1BB on PI Days 0 and 2. The mice were additionally treated with 500 μg anti-IFN-γ on PI Days –1, 4, and 7 or given 3 mg/ml 1-MT in drinking water beginning 1 day before SEA injection. (A, B) The DLN cells were prepared from each group of mice on PI Day 10 and cultured with 0.1 μg/ml SEA for 3 days. The cells were labeled with BrdU for the last hour, stained with PE-conjugated anti-CD4 (A) or anti-CD8 (B), and stained intracellularly with FITC-conjugated anti-BrdU. (C) To assess [3H]-thymidine incorporation, DLN cells were incubated with 0.1 μg/ml SEA for 3 days at 37°C in a 5% CO2 atmosphere, pulsed with [3H]-thymidine (1 μCi/well) during the last 12 h, harvested onto glass fiber filter mats, and analyzed for [3H]-thymidine incorporation by liquid scintillation counting. The plotted data are means ± sd (**, P<0.01). The results are representative of three independent experiments.
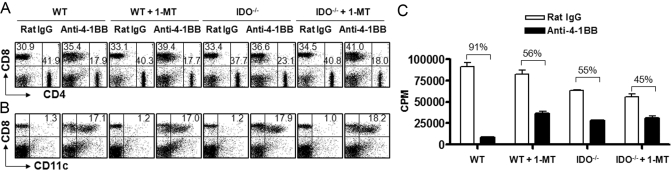
To further confirm the role of IDO in 4-1BB-mediated suppression of CD4+ T cells, WT and IDO-deficient C57BL/6 mice were injected with SEA and treated with anti-4-1BB mAb or rat IgG as described above; some of the mice were given 1-MT in their drinking water. Lymphocytes were prepared from ILN of each group of mice on PI Day 10, and the ratio of CD4+ to CD8+ T cells was analyzed. Treatment with anti-4-1BB mAb preferentially increased the CD8+ T cells, which resulted in the reversal of the CD4+ versus CD8+ T cell ratio in WT C57BL/6 mice (Fig. 6A). In IDO-deficient C57BL/6 mice, the ratio of CD4+ vs. CD8+ T cells was reversed by treating with anti-4-1BB mAb even in the presence of 1-MT (Fig. 6A). CD11c+CD8+ T cells were also increased by anti-4-1BB mAb in WT and IDO-deficient mice, independent of 1-MT treatment (Fig. 6B).
Fig. 6.
IDO as a mediator of 4-1BB-dependent suppression of SEA-specific CD4+ T cells. C57BL/6 and IDO-deficient C57BL/6 mice were injected with SEA as described previously, and some mice were given 3 mg/ml 1-MT in drinking water beginning 1 day before SEA injection. The mice were treated further with rat IgG or anti-4-1BB mAb on PI Days 0 and 2. The ILN cells were prepared from each group of mice on PI Day 10 and stained with anti-CD4 and anti-CD8 mAb (A) or anti-CD8 and anti-CD11c mAb (B). (C) ILN cells were cultured with 0.1 μg/ml SEA for 3 days and labeled with 1 μCi [3H]-thymidine for the last 8 h, and the incorporation of [3H]-thymidine was assessed by liquid scintillation counting. The plotted data are means ± sd. The results are representative of three independent experiments.
ILN cells were restimulated with SEA in vitro for 3 days to determine SEA-specific proliferation. Treatment with anti-4-1BB mAb again inhibited >90% of SEA-specific proliferation in WT mice that received the placebo pellet, but the 4-1BB-mediated inhibition rate was 40–60% in IDO-deficient mice or 1-MT-treated WT and IDO-deficient mice (Fig. 6C). Contrary to our expectations, IDO-deficient C57BL/6 mice showed hyporesponsiveness compared with WT mice, although the reason was not clear. However, these results indicate that treatment with anti-4-1BB mAb suppresses SEA-specific CD4+ T cell responses through IFN-γ, which is produced mainly by CD11c+CD8+ T cells and the induction of IDO in macrophages and DCs as a downstream effector molecule.
Subpopulations of DCs responsible for 4-1BB-mediated suppression of CD4+ T cells
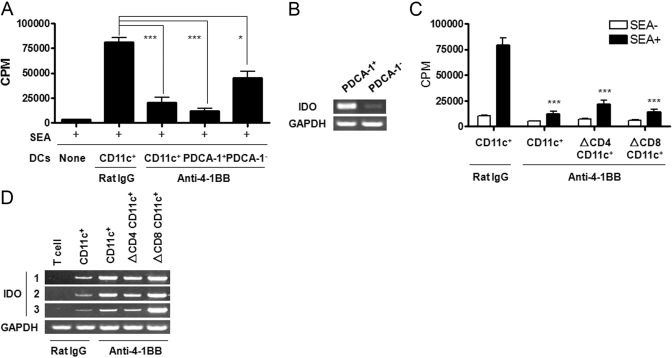
To characterize DC subpopulations responsible for CD4+ T suppression and IDO expression, DC populations including CD8–CD11c+, CD4–CD11c+, and pDCs were prepared from spleens and ILN of rat IgG- or anti-4-1BB mAb-treated mice on PI Day 10. We first purified CD11c+ DCs from the rat IgG- and anti-4-1BB mAb-treated groups and PDCA-1+ pDCs and PDCA-1– CD11c+ DCs from the anti-4-1BB mAb group. By coculturing CD4+ T cells from rat IgG-treated mice with the purified DCs at a 5:1 ratio, we determined the suppressive activity of each type of DC. CD11c+ DCs from the rat IgG-treated group induced CD4+ T cell proliferation rather than suppression, whereas CD11c+ DCs from the anti-4-1BB mAb-treated group suppressed the CD4+ T cell response markedly compared with DCs from rat IgG-treated mice (Fig. 7A). The purified PDCA-1+ pDCs from the anti-4-1BB mAb group also showed a strong, suppressive activity on the CD4+ T cell response that was comparable with or even stronger than that of CD11c+ DCs (Fig. 7A). PDCA-1-depleted CD11c+ DCs (PDCA-1–CD11c+) also exerted suppressive activity but less significantly than that of CD11c+ or PDCA-1+ DCs (Fig. 7A). When the level of the IDO transcript was assessed in PDCA-1+ and PDCA-1–CD11c+ DCs from anti-4-1BB mAb-treated mice, the expression of IDO mRNA was higher in PDCA-1+ DCs than PDCA-1–CD11c+ DCs (Fig. 7B). When the T–DC coculture was performed using CD4-depleted or CD8-depleted CD11c+ DCs, both DC subsets showed similarly suppressed SEA-specific CD4+ T cell responses (Fig. 7C). However, IDO expression was higher in CD8–CD11c+ DCs than CD4–CD11c+ DCs (Fig. 7D).
Fig. 7.
4-1BB-dependent suppression of CD4+ T cells by IDO-expressing DC subpopulations. SEA-injected C57BL/6 mice were treated with rat IgG or anti-4-1BB mAb on PI Days 0 and 2. DLN cells were prepared from rat IgG- or anti-4-1BB mAb-treated mice on PI Day 10 and then used for the purification of each population including CD11c+, PDCA-1+, and PDCA-1– DCs and CD4–CD11c+ and CD8–CD11c+ DCs. Responder CD4+ T cells were purified from rat IgG-treated mice on PI Day 10. (A) CD11c+, PDCA-1+, and PDCA-1– DCs were cultured with CD4+ T cells in the presence or absence of 0.1 μg/ml SEA for 3 days. CD11c+, CD4-depleted (ΔCD4) CD11c+, and CD8-depleted CD11c+ DCs were also mixed with CD4+ T cells in coculture (C). Cultured cells were pulsed with [3H]-thymidine (1 μCi/well) during the last 12 h, harvested onto glass fiber filter mats, and analyzed for [3H]-thymidine incorporation by liquid scintillation counting. (B, D). IDO expression in freshly purified DC population on Day 10. Expression level of IDO was confirmed by RT-PCR. The plotted data are means ± sd (*, P<0.05; ***, P<0.001). The results are representative of three independent experiments.
These results indicate that IDO expression is up-regulated in several DC subpopulations including PDCA-1+, CD4+, and CD8+ DCs following treatment with anti-4-1BB mAb. Despite the different levels of IDO expression in each DC subpopulation, they suppressed SEA-specific CD4+ T responses similarly. As the expression and suppressive activity of IDO are known to be regulated by different factors [32], the suppressive activity of IDO in DCs appears to be regulated in at least two different ways: the induction of IDO and maturation of the expressed IDO protein.
DISCUSSION
It has been reported that costimulation of T cells through 4-1BB receptors increases the proliferation, cytokine production, and cytolytic activity of T cells [1, 3,4,5,6,7]. However, recent studies suggest that in vivo triggering of 4-1BB not only increases the effector function of CD8+ T cells but also suppresses CD4+ T cell responses [11]. For example, 4-1BB triggering enhanced CD8+ T cell responses against tumors and viruses, and the same agonistic anti-4-1BB mAb may ameliorate autoimmune diseases such as experimental autoimmune encephalomyelitis, CIA, and lupus-like syndrome [5,6,7, 10,11,12,13, 33,34,35,36]. Therefore, the suppressive mechanism resulting from anti-4-1BB mAb treatment becomes an interesting issue, as the signaling through nonpolymorphic 4-1BB molecules exerts contradictory responses on CD4+ and CD8+ T cells. Myers et al. [28] demonstrated that TLR ligands and 4-1BB costimulation massively enhance the clonal expansion of antigen-specific T cells in vivo but profoundly suppress CD4+ T cell responses for which CD8+ T-derived TGF-β was involved. Other reports suggest that IFN-γ plays a critical role in 4-1BB-mediated suppression and that IDO expression by IFN-γ functions as a final effector molecule to ameliorate autoimmune disease [10, 11].
Here, we provide evidence that 4-1BB-dependent suppression of CD4+ T cells in the SEA model is mediated mainly by CD8+ T cells and IDO-expressing APCs. In a previous report [28], 4-1BB triggering blocked the peripheral deletion of CD4+ and CD8+ T cells but suppressed the recall-proliferative response of CD4+ T cells. This suppression was provoked in WT mice that were given anti-4-1BB mAb with SEA but not in 4-1BB-deficient mice or rat IgG-treated WT mice, indicating that the suppression of the CD4+ T cell response is dependent on 4-1BB signaling with the antigen (Fig. 1). The expansion of CD11c+CD8+ T cells, which has been suggested as a regulator for the suppression of CIA [11], was found in SEA-injected mice treated with anti-4-1BB mAb, and this unique population produced IFN-γ and TGF-β (Fig. 2, C and D). In vitro coculture experiments showed that SEA-specific CD4+ T responses could be suppressed by CD11c+CD8+ T cells (Fig. 3A). Consistent with our previous report [11], DCs from anti-4-1BB mAb-treated mice also suppressed the SEA-specific CD4+ T cell response profoundly, which was restored largely by neutralizing IFN-γ or IDO activity in vivo (Figs. 5 and 6). These results indicate that IFN-γ and IDO are the major suppressive factors in the 4-1BB-mediated suppression. IFN-γ neutralization effectively restored the 4-1BB-mediated suppression in vivo but marginally in vitro (Supplemental Fig. 3). However, in vitro inhibition of IDO with 1-MT restored the recall proliferation significantly, and the recovery rate was comparable with the effect of blocking IDO in vivo. The ineffective restoration of the recall responses in in vitro IFN-γ neutralization may be because the IDO was already induced in the DLN APCs. These results support the idea that the IFN-γ-IDO axis mediated the suppressive effects of anti-4-1BB treatment.
Although the anti-TGF-β mAb 1D11.16 is known to be the mAb that can neutralize all three isoforms of TGF-β and inhibit receptor cross-linking [37,38,39], we may need to confirm further whether all of the TGF-β activities have been inhibited completely in our assays.
We examined a potential contamination of DCs in the CD11c+CD8+ T cell preparation in the in vitro CD4+ T cell suppression assays (Figs. 3B and 7). Lymphocytes were isolated from ILN and treated with collagenase type IV and DNase I. Single-cell suspensions were stained with surface antigen-specific antibodies against CD8β, CD11c, I-Ab, and CD3 (Supplemental Fig. 4). As CD11chigh DCs express the CD8α in the cell surface, but not CD8β, we could exclude the contamination of CD11c+CD8α+ DCs from CD11c+CD8+ T cells by staining CD8β in FACS analysis of SEA injected- and anti-4-1BB-treated mice. Consistent with previous reports, the CD11c+CD8+ cell population was not DCs but CD8+ T cells, which expressed a low level of Class II on their surface [11]. When we analyzed the expression of cell-surface antigens in purified cell populations, CD11c+CD8+ cells contained 6.4% of I-Ab-positive and 94.1% of CD3-positive cells. These results indicate that the purified CD11c+CD8+ T cell population was contaminated with some lymphoid DCs of the anti-4-1BB-treated group. As DCs were added in the in vitro suppression assays with purified CD8+ T cells (Fig. 3A), the contaminated lymphoid DCs might produce an added suppressive effect.
4-1BB triggering has been known to selectively enhance the proliferation of CD8+ T cells rather than CD4+ T cells in vivo even after similar induction with 4-1BB on both kinds of T cells [10, 40, 41]. When anti-4-1BB mAb were used to treat mice that received OVA-specific CD4+ T (OT-II) or CD8+ T cells (OT-I) as well as OVA antigen, only CD8+ T cells massively proliferated (data not shown) [42,43,44]. Therefore, there could be intrinsic differences in intracellular 4-1BB signaling between CD4+ and CD8+ T cells, which provide a possible explanation for the selective suppression of CD4+ T cells by IDO; CD8+ T cells, but not CD4+ T cells, receiving 4-1BB signaling seem to be more resistant to IDO-dependent suppression.
Among the DC subpopulations, the transcript level of IDO was higher in PDCA-1+ pDCs compared with that of CD4+ or CD8+ DCs following treatment with anti-4-1BB mAb (Fig. 7B). However, these DC subpopulations similarly suppressed SEA-specific CD4+ T cells in vitro (Fig. 7, A and C). IFN-γ is known to induce the IDO transcript in CD8α– and CD8α+ DCs but only enhances the IDO activity in CD8α+ DCs [45]. The reverse and noncanonical NF-κB signaling through CD80, CD40, and GITRL also induces the IDO expression on DCs [19,20,21,22], which mediate the generation of Tregs by combination effects of tryptophan starvation and tryptophan catabolites [46]. Conversely, Tregs promote the IDO production in pDCs by reverse signaling via CD80 and GITRL [17, 21, 23]. Both cells may be involved in suppression of SEA-specific CD4+ T cells. In the current setting, TGF-β produced by CD11c+CD8+ T cells following 4-1BB stimulation may also contribute to the generation of suppressive Tregs. Therefore, it seems that 4-1BB triggering primarily induces IDO expression in CD8a+ DCs and pDCs in an IFN-γ-dependent manner, but the other DCs seem to induce IDO expression through other factors such as CTLA-4, which might be expressed abundantly on the activated T cells and Tregs. In summary, our data suggest that 4-1BB-mediated suppression of the CD4+ T response in the SEA model is regulated mainly by the IFN-γ-IDO axis and partially by TGF-β on CD8+ T cells.
Supplementary Material
Acknowledgments
This work was supported in part by grants from the National Cancer Center, Korea (NCC-0810720-1 and NCCF-0890830-1), Korean Research Foundation (KRF-2005-084-E00001), Arthritis Foundation (Innovative Research Award to B. S. K.), National Institutes of Health grant (R001EY013325 to B. S. K.), MEST-2006-04212, Korea Health 21 R&D (A050260), and KOSEF-M1087006009-08N7006-00910.
References
- Vinay D S, Kwon B S. Role of 4-1BB in immune responses. Semin Immunol. 1998;10:481–489. doi: 10.1006/smim.1998.0157. [DOI] [PubMed] [Google Scholar]
- Melero I, Johnston J V, Shufford W W, Mittler R S, Chen L. NK1.1 cells express 4-1BB (CDw137) costimulatory molecule and are required for tumor immunity elicited by anti-4-1BB monoclonal antibodies. Cell Immunol. 1998;190:167–172. doi: 10.1006/cimm.1998.1396. [DOI] [PubMed] [Google Scholar]
- Kwon B, Moon C H, Kang S, Seo S K, Kwon B S. 4-1BB: still in the midst of darkness. Mol Cells. 2000;10:119–126. doi: 10.1007/s10059-000-0119-0. [DOI] [PubMed] [Google Scholar]
- Lee H W, Park S J, Choi B K, Kim H H, Nam K O, Kwon B S. 4-1BB promotes the survival of CD8+ T lymphocytes by increasing expression of Bcl-xL and Bfl-1. J Immunol. 2002;169:4882–4888. doi: 10.4049/jimmunol.169.9.4882. [DOI] [PubMed] [Google Scholar]
- Miller R E, Jones J, Le T, Whitmore J, Boiani N, Gliniak B, Lynch D H. 4-1BB-specific monoclonal antibody promotes the generation of tumor-specific immune responses by direct activation of CD8 T cells in a CD40-dependent manner. J Immunol. 2002;169:1792–1800. doi: 10.4049/jimmunol.169.4.1792. [DOI] [PubMed] [Google Scholar]
- Ye Z, Hellstrom I, Hayden-Ledbetter M, Dahlin A, Ledbetter J A, Hellstrom K E. Gene therapy for cancer using single-chain Fv fragments specific for 4-1BB. Nat Med. 2002;8:343–348. doi: 10.1038/nm0402-343. [DOI] [PubMed] [Google Scholar]
- Wilcox R A, Flies D B, Zhu G, Johnson A J, Tamada K, Chapoval A I, Strome S E, Pease L R, Chen L. Provision of antigen and CD137 signaling breaks immunological ignorance, promoting regression of poorly immunogenic tumors. J Clin Invest. 2002;109:651–659. doi: 10.1172/JCI14184. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Vinay D S, Kwon B S. Immunotherapy targeting 4-1BB and its ligand. Int J Hematol. 2006;83:23–28. doi: 10.1532/IJH97.05125. [DOI] [PubMed] [Google Scholar]
- Myers L M, Vella A T. Interfacing T-cell effector and regulatory function through CD137 (4-1BB) co-stimulation. Trends Immunol. 2005;26:440–446. doi: 10.1016/j.it.2005.06.003. [DOI] [PubMed] [Google Scholar]
- Foell J, Strahotin S, O'Neil S P, McCausland M M, Suwyn C, Haber M, Chander P N, Bapat A S, Yan X J, Chiorazzi N, Hoffmann M K, Mittler R S. CD137 costimulatory T cell receptor engagement reverses acute disease in lupus-prone NZB × NZW F1 mice. J Clin Invest. 2003;111:1505–1518. doi: 10.1172/JCI17662. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Seo S K, Choi J H, Kim Y H, Kang W J, Park H Y, Suh J H, Choi B K, Vinay D S, Kwon B S. 4-1BB-mediated immunotherapy of rheumatoid arthritis. Nat Med. 2004;10:1088–1094. doi: 10.1038/nm1107. [DOI] [PubMed] [Google Scholar]
- Foell J L, Diez-Mendiondo B I, Diez O H, Holzer U, Ruck P, Bapat A S, Hoffmann M K, Mittler R S, Dannecker G E. Engagement of the CD137 (4-1BB) costimulatory molecule inhibits and reverses the autoimmune process in collagen-induced arthritis and establishes lasting disease resistance. Immunology. 2004;113:89–98. doi: 10.1111/j.1365-2567.2004.01952.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sun Y, Lin X, Chen H M, Wu Q, Subudhi S K, Chen L, Fu Y X. Administration of agonistic anti-4-1BB monoclonal antibody leads to the amelioration of experimental autoimmune encephalomyelitis. J Immunol. 2002;168:1457–1465. doi: 10.4049/jimmunol.168.3.1457. [DOI] [PubMed] [Google Scholar]
- Munn D H, Zhou M, Attwood J T, Bondarev I, Conway S J, Marshall B, Brown C, Mellor A L. Prevention of allogeneic fetal rejection by tryptophan catabolism. Science. 1998;281:1191–1193. doi: 10.1126/science.281.5380.1191. [DOI] [PubMed] [Google Scholar]
- Munn D H, Sharma M D, Hou D, Baban B, Lee J R, Antonia S J, Messina J L, Chandler P, Koni P A, Mellor A L. Expression of indoleamine 2,3-dioxygenase by plasmacytoid dendritic cells in tumor-draining lymph nodes. J Clin Invest. 2004;114:280–290. doi: 10.1172/JCI21583. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hayashi T, Beck L, Rossetto C, Gong X, Takikawa O, Takabayashi K, Broide D H, Carson D A, Raz E. Inhibition of experimental asthma by indoleamine 2,3-dioxygenase. J Clin Invest. 2004;114:270–279. doi: 10.1172/JCI21275. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Grohmann U, Volpi C, Fallarino F, Bozza S, Bianchi R, Vacca C, Orabona C, Belladonna M L, Ayroldi E, Nocentini G, Boon L, Bistoni F, Fioretti M C, Romani L, Riccardi C, Puccetti P. Reverse signaling through GITR ligand enables dexamethasone to activate IDO in allergy. Nat Med. 2007;13:579–586. doi: 10.1038/nm1563. [DOI] [PubMed] [Google Scholar]
- Romani L, Fallarino F, De Luca A, Montagnoli C, D'Angelo C, Zelante T, Vacca C, Bistoni F, Fioretti M C, Grohmann U, Segal B H, Puccetti P. Defective tryptophan catabolism underlies inflammation in mouse chronic granulomatous disease. Nature. 2008;451:211–215. doi: 10.1038/nature06471. [DOI] [PubMed] [Google Scholar]
- De Luca A, Montagnoli C, Zelante T, Bonifazi P, Bozza S, Moretti S, D'Angelo C, Vacca C, Boon L, Bistoni F, Puccetti P, Fallarino F, Romani L. Functional yet balanced reactivity to Candida albicans requires TRIF, MyD88, and IDO-dependent inhibition of Rorc. J Immunol. 2007;179:5999–6008. doi: 10.4049/jimmunol.179.9.5999. [DOI] [PubMed] [Google Scholar]
- Fallarino F, Puccetti P. Toll-like receptor 9-mediated induction of the immunosuppressive pathway of tryptophan catabolism. Eur J Immunol. 2006;36:8–11. doi: 10.1002/eji.200535667. [DOI] [PubMed] [Google Scholar]
- Grohmann U, Orabona C, Fallarino F, Vacca C, Calcinaro F, Falorni A, Candeloro P, Belladonna M L, Bianchi R, Fioretti M C, Pucetti P. CTLA-4-Ig regulates tryptophan catabolism in vivo. Nat Immunol. 2002;3:1097–1101. doi: 10.1038/ni846. [DOI] [PubMed] [Google Scholar]
- Tas S W, Vervoordeldonk M J, Hajji N, Schuitemaker J H, van der Sluijs K F, May M J, Ghosh S, Kapsenberg M L, Tak P P, de Jong E C. Noncanonical NF-κB signaling in dendritic cells is required for indoleamine 2,3-dioxygenase (IDO) induction and immune regulation. Blood. 2007;110:1540–1549. doi: 10.1182/blood-2006-11-056010. [DOI] [PubMed] [Google Scholar]
- Puccetti P, Grohmann U. IDO and regulatory T cells: a role for reverse signaling and non-canonical NF-κB activation. Nat Rev Immunol. 2007;7:817–823. doi: 10.1038/nri2163. [DOI] [PubMed] [Google Scholar]
- Kappler J, Kotzin B, Herron L, Gelfand E W, Bigler R D, Boylston A, Carrel S, Posnett D N, Choi Y, Marrack P. V β-specific stimulation of human T cells by staphylococcal toxins. Science. 1989;244:811–813. doi: 10.1126/science.2524876. [DOI] [PubMed] [Google Scholar]
- Ivars F. Superantigen-induced regulatory T cells in vivo. Chem Immunol Allergy. 2007;93:137–160. doi: 10.1159/000100862. [DOI] [PubMed] [Google Scholar]
- Li H, Nooh M M, Kotb M, Re F. Commercial peptidoglycan preparations are contaminated with superantigen-like activity that stimulates IL-17 production. J Leukoc Biol. 2008;83:409–418. doi: 10.1189/jlb.0807588. [DOI] [PubMed] [Google Scholar]
- Schartner J M, Singh A M, Dahlberg P E, Nettenstrom L, Seroogy C M. Recurrent superantigen exposure in vivo leads to highly suppressive CD4(+)CD25(+) and CD4(+)CD25(–) T cells with anergic and suppressive genetic signatures. Clin Exp Immunol. 2009;155:348–356. doi: 10.1111/j.1365-2249.2008.03827.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Myers L, Takahashi C, Mittler R S, Rossi R J, Vella A T. Effector CD8 T cells possess suppressor function after 4-1BB and Toll-like receptor triggering. Proc Natl Acad Sci USA. 2003;100:5348–5353. doi: 10.1073/pnas.0837611100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Liblau R S, Tisch R, Shokat K, Yang X, Dumont N, Goodnow C C, McDevitt H O. Intravenous injection of soluble antigen induces thymic and peripheral T-cells apoptosis. Proc Natl Acad Sci USA. 1996;93:3031–3036. doi: 10.1073/pnas.93.7.3031. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McCormack J E, Callahan J E, Kappler J, Marrack P C. Profound deletion of mature T cells in vivo by chronic exposure to exogenous superantigen. J Immunol. 1993;150:3785–3792. [PubMed] [Google Scholar]
- MacDonald H R, Baschieri S, Lees R K. Clonal expansion precedes anergy and death of V β 8+ peripheral T cells responding to staphylococcal enterotoxin B in vivo. Eur J Immunol. 1991;21:1963–1966. doi: 10.1002/eji.1830210827. [DOI] [PubMed] [Google Scholar]
- Braun D, Longman R S, Albert M L. A two-step induction of indoleamine 2,3 dioxygenase (IDO) activity during dendritic-cell maturation. Blood. 2005;106:2375–2381. doi: 10.1182/blood-2005-03-0979. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Xu D, Gu P, Pan P Y, Li Q, Sato A I, Chen S H. NK and CD8+ T cell-mediated eradication of poorly immunogenic B16–F10 melanoma by the combined action of IL-12 gene therapy and 4-1BB costimulation. Int J Cancer. 2004;109:499–506. doi: 10.1002/ijc.11696. [DOI] [PubMed] [Google Scholar]
- Ito F, Li Q, Shreiner A B, Okuyama R, Jure-Kunkel M N, Teitz-Tennenbaum S, Chang A E. Anti-CD137 monoclonal antibody administration augments the antitumor efficacy of dendritic cell-based vaccines. Cancer Res. 2004;64:8411–8419. doi: 10.1158/0008-5472.CAN-04-0590. [DOI] [PubMed] [Google Scholar]
- Halstead E S, Mueller Y M, Altman J D, Katsikis P D. In vivo stimulation of CD137 broadens primary antiviral CD8+ T cell responses. Nat Immunol. 2002;3:536–541. doi: 10.1038/ni798. [DOI] [PubMed] [Google Scholar]
- Kim Y H, Seo S K, Choi B K, Kang W J, Kim C H, Lee S K, Kwon B S. 4-1BB costimulation enhances HSV-1-specific CD8+ T cell responses by the induction of CD11c+CD8+ T cells. Cell Immunol. 2005;238:76–86. doi: 10.1016/j.cellimm.2006.01.004. [DOI] [PubMed] [Google Scholar]
- Dasch J R, Pace D R, Waegell W, Inenaga D, Ellingsworth L. Monoclonal antibodies recognizing transforming growth factor-β. Bioactivity neutralization and transforming growth factor β 2 affinity purification. J Immunol. 1989;142:1536–1541. [PubMed] [Google Scholar]
- Myers L, Croft M, Kwon B S, Mittler R S, Vella A T. Peptide-specific CD8 T regulatory cells use IFN-γ to elaborate TGF-β-based suppression. J Immunol. 2005;174:7625–7632. doi: 10.4049/jimmunol.174.12.7625. [DOI] [PubMed] [Google Scholar]
- Nam J S, Terabe M, Mamura M, Kang M J, Chae H, Stuelten C, Kohn E, Tang B, Sabzevari H, Anver M R, Lawrence S, Danielpour D, Lonning S, Berzofsky J A, Wakefield L M. An anti-transforming growth factor β antibody suppresses metastasis via cooperative effects on multiple cell compartments. Cancer Res. 2008;68:3835–3843. doi: 10.1158/0008-5472.CAN-08-0215. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Shuford W W, Klussman K, Tritchler D D, Loo D T, Chalupny J, Siadak A W, Brown T J, Emswiler J, Raecho H, Larsen C P, Pearson T C, Ledbetter J A, Aruffo A, Mittler R S. 4-1BB costimulatory signals preferentially induce CD8+ T cell proliferation and lead to the amplification in vivo of cytotoxic T cell responses. J Exp Med. 1997;186:47–55. doi: 10.1084/jem.186.1.47. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kim Y J, Kim S H, Mantel P, Kwon B S. Human 4-1BB regulates CD28 co-stimulation to promote Th1 cell responses. Eur J Immunol. 1998;28:881–890. doi: 10.1002/(SICI)1521-4141(199803)28:03<881::AID-IMMU881>3.0.CO;2-0. [DOI] [PubMed] [Google Scholar]
- Cooper D, Bansal-Pakala P, Croft M. 4-1BB (CD137) controls the clonal expansion and survival of CD8 T cells in vivo but does not contribute to the development of cytotoxicity. Eur J Immunol. 2002;32:521–529. doi: 10.1002/1521-4141(200202)32:2<521::AID-IMMU521>3.0.CO;2-X. [DOI] [PubMed] [Google Scholar]
- Dawicki W, Watts T H. Expression and function of 4-1BB during CD4 versus CD8 T cell responses in vivo. Eur J Immunol. 2004;34:743–751. doi: 10.1002/eji.200324278. [DOI] [PubMed] [Google Scholar]
- Lee S J, Myers L, Muralimohan G, Dai J, Qiao Y, Li Z, Mittler R S, Vella A T. 4-1BB and OX40 dual costimulation synergistically stimulate primary specific CD8 T cells for robust effector function. J Immunol. 2004;173:3002–3012. doi: 10.4049/jimmunol.173.5.3002. [DOI] [PubMed] [Google Scholar]
- Fallarino F, Vacca C, Orabona C, Belladonna M L, Bianchi R, Marshall B, Keskin D B, Mellor A L, Fioretti M C, Grohmann U, Pucetti P. Functional expression of indoleamine 2,3-dioxygenase by murine CD8 α(+) dendritic cells. Int Immunol. 2002;14:65–68. doi: 10.1093/intimm/14.1.65. [DOI] [PubMed] [Google Scholar]
- Fallarino F, Grohmann U, You S, McGrath B C, Cavener D R, Vacca C, Orabona C, Bianchi R, Belladonna M L, Volpi C, Santamaria P, Fioretti M C, Puccetti P. The combined effects of tryptophan starvation and tryptophan catabolites down-regulate T cell receptor ζ-chain and induce a regulatory phenotype in naive T cells. J Immunol. 2006;176:6752–6761. doi: 10.4049/jimmunol.176.11.6752. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.