Abstract
Antifungal effects of iron chelators (lactoferrin, deferoxamine, deferiprone, and ciclopirox) were tested alone and in combination with antifungal drugs against Aspergillus fumigatus B5233 conidia. Lactoferrin, ciclopirox, and deferiprone inhibited whereas deferoxamine enhanced fungal growth. Antifungal synergy against conidia was observed for combinations of ketoconazole with ciclopirox or deferiprone, lactoferrin with amphotericin B, and fluconazole with deferiprone. Iron chelation alone or combined with antifungal drugs may be useful for prevention and treatment of mycosis.
Invasive aspergillosis in neutropenic and immunocompromised patients is a serious therapeutic challenge (2, 4, 7, 16). Prophylaxis using antifungal drugs has markedly reduced the occurrence of these infections (8, 19, 23, 24); however, mortality for aspergillosis remains high (17). Most clinically deployed antifungal drugs target ergosterol, a membrane sterol present in plants and fungi (19), leaving a great need for drugs with alternative mechanisms of action. In vitro demonstration that lactoferrin inhibits the growth Aspergillus fumigatus conidia by iron deprivation (25) and the topical use of the iron chelator ciclopirox for superficial fungal infections (11) suggest that inhibition of fungal iron acquisition may provide an alternative drug target. Furthermore, transfusional siderosis and iron overload in malignancy and liver and stem cell transplantation are associated with an increased risk of aspergillosis (1, 3, 15).
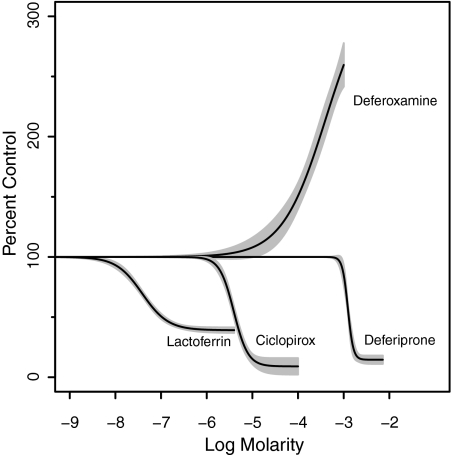
To assay the effects of iron chelators and antifungal drugs on the growth of Aspergillus fumigatus strain B5233 (provided by June Kwon-Chung, NIAID), conidia (105) were cultured in 90 μl RPMI 1640 without phenol red, buffered with 25 mM HEPES (pH 7.2), in the presence of drugs or buffer (final volume, 100 μl). After 16 h at 37°C in a humidified 5% CO2 incubator, 100 μl of RPMI with 5 μM 5-chloromethylfluorescein diacetate (Invitrogen) was added, followed by incubation for 30 min, and fluorescence measured as described previously (5, 25). As shown in Fig. 1, lactoferrin (partially saturated native human; Sigma Chemicals, St. Louis, MO) was most potent on a molar basis, requiring only 105 ± 9 nM to reduce untreated control growth by 50% (50% inhibitory concentration [IC50]), followed by ciclopirox (6-cyclohexyl-1-hydroxy-4-methyl-2(1H)-pyridinone; Toronto Research Chemicals, North York, Ontario, Canada) (IC50 = 4.22 ± 0.18 μM) and deferiprone (1,2-dimethyl-3-hydroxypyrid-4-one; Toronto Research Chemicals) (IC50 = 1.29 ± 0.2 mM). Deferoxamine mesylate (Sigma) promoted A. fumigatus growth, as has been reported for Rhizopus (6, 9).
FIG. 1.
Iron chelator effect on Aspergillus fumigatus conidial growth. Fungal growth inhibition was performed as described in the text, and the data are expressed as percentages of control growth in vehicle alone. Dose-response curves were estimated from multiple experiments (for deferoxamine, n = 3; for deferiprone, n = 38; for ciclopirox, n = 40; for lactoferrin, n = 43) using three-parameter logistic models and are plotted with 95% confidence intervals.
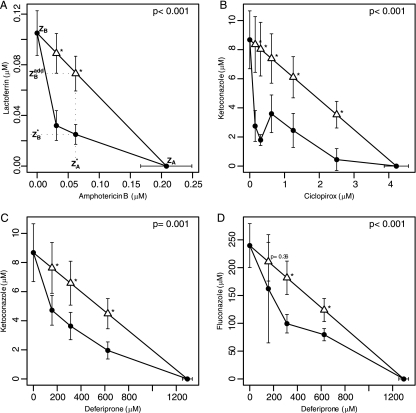
Analysis of the combined effects of different drugs is clinically important since synergistic combinations of drugs may be more efficacious and less toxic than single agents (14, 20, 21). Checkerboard assays of the three active iron chelators alone and in combination with itraconazole, fluconazole, ketoconazole (Sigma), or amphotericin B (Toronto Research Chemicals) were performed. The respective IC50s (± standard errors) for these drugs were 0.29 ± 0.04, 239.65 ± 20.16, 8.68 ± 1.01, and 0.21 ± 0.02 μM. Isobolic analysis (18, 22) was employed to assess departure from Loewe's additivity. An isobologram consists of doses of individual drugs and the combined doses required to achieve a particular effect, in this case a 50% decrease in fungal growth compared to that of untreated controls. The dose (denoted by IC50) was estimated by fitting a three-parameter or four-parameter logistic regression model for drugs tested alone or in combination. Combinations are considered synergistic (or antagonistic) if the drug dose pair is significantly lower (or higher) than the additivity line formed by connecting the IC50 of the individual drugs. Of the 12 combinations tested, only 4 demonstrated significant synergy; these are shown in Fig. 2. As an example of the analysis, Fig. 2A shows two dose pairs of amphotericin B and lactoferrin that are more active than predicted by Loewe's additivity model. Formal statistical testing can be conducted by comparing the estimated dose (illustrated by 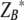 in Fig. 2A) to the expected dose (
in Fig. 2A) to the expected dose (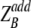 ) under additivity, with the standard error of the difference estimated by applying the delta method. To efficiently combine the evidence against additivity using all dose combinations, a global chi-square test was carried out by combining the test statistics for all drug pairs and accounting for the correlation between test statistics. For the combinations shown in Fig. 2A to D, the combined doses are significantly (global P ≤ 0.05) more active than expected, suggesting that the combination is synergistic. In contrast, significant antagonism was noted between amphotericin B and deferiprone and between lactoferrin and fluconazole. The remaining combinations were indifferent; that is, the combined effects were not significantly different from additivity. All P values were two-sided, and P values of less than 0.05 were considered to be statistically significant. Data analyses were performed using the R software program (www.r-project.org) (version 2.7.2).
) under additivity, with the standard error of the difference estimated by applying the delta method. To efficiently combine the evidence against additivity using all dose combinations, a global chi-square test was carried out by combining the test statistics for all drug pairs and accounting for the correlation between test statistics. For the combinations shown in Fig. 2A to D, the combined doses are significantly (global P ≤ 0.05) more active than expected, suggesting that the combination is synergistic. In contrast, significant antagonism was noted between amphotericin B and deferiprone and between lactoferrin and fluconazole. The remaining combinations were indifferent; that is, the combined effects were not significantly different from additivity. All P values were two-sided, and P values of less than 0.05 were considered to be statistically significant. Data analyses were performed using the R software program (www.r-project.org) (version 2.7.2).
FIG. 2.
Isobolograms of combined antifungal effects. The doses of each agent alone (indicated by ZA and ZB) and in combination, indicated by (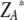 ,
, 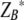 ), required to achieve a 50% reduction in growth compared to that of untreated controls are plotted along with the 95% confidence intervals. Under additivity, the dose pair (
), required to achieve a 50% reduction in growth compared to that of untreated controls are plotted along with the 95% confidence intervals. Under additivity, the dose pair (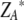 ,
, 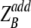 ) is expected to yield the same effect. Lines of additivity are indicated by open triangles, and measured drug combinations are indicated by filled circles. Statistical significance (P < 0.05) is indicated by an asterisk, and the P value of the global chi-square test is given in the upper right corner of each graph. Panels A to D show examples of synergistic combinations of chelators with antifungal drugs. The figures are generated from between four and eight checkerboard experiments for each combination of drugs.
) is expected to yield the same effect. Lines of additivity are indicated by open triangles, and measured drug combinations are indicated by filled circles. Statistical significance (P < 0.05) is indicated by an asterisk, and the P value of the global chi-square test is given in the upper right corner of each graph. Panels A to D show examples of synergistic combinations of chelators with antifungal drugs. The figures are generated from between four and eight checkerboard experiments for each combination of drugs.
Given the abundance of Aspergillus conidia in the environment, prophylactic antifungal therapy is a standard clinical practice for neutropenic patients (8, 24) or patients with chronic granulomatous disease who experience frequent life-threatening infections (10). The differences in efficacies of chelators against particular organisms and, indeed, the ability of some organisms to acquire iron through chelators such as deferoxamine demand that in vitro and in vivo studies be performed for each drug against each organism. In support of the potential use of iron chelators in antifungal therapy, deferiprone (12) and deferasirox (13) protected mice from Rhizopus oryzae infection. Importantly, since both synergistic and antagonistic interactions have been observed between specific combinations of chelators and antifungals, it should not be assumed that independently effective antifungal drugs can be combined without in vitro and in vivo validation. Despite these limitations, transition metal chelators may be a potentially useful addition to the otherwise sparse repertoire of antifungal drugs.
Acknowledgments
We thank Dean Follman, June Kwon-Chung, and Janyce Sugui (NIAID) for useful discussions and suggestions.
This work was supported by the Division of Intramural Research of the NIAID and the NIH Clinical Center.
Footnotes
Published ahead of print on 23 March 2009.
REFERENCES
- 1.Alexander, J., A. P. Limaye, C. W. Ko, M. P. Bronner, and K. V. Kowdley. 2006. Association of hepatic iron overload with invasive fungal infection in liver transplant recipients. Liver Transpl. 12:1799-1804. [DOI] [PubMed] [Google Scholar]
- 2.Almyroudis, N. G., S. M. Holland, and B. H. Segal. 2005. Invasive aspergillosis in primary immunodeficiencies. Med. Mycol. 43(Suppl. 1):S247-S259. [DOI] [PubMed] [Google Scholar]
- 3.Altes, A., A. F. Remacha, P. Sarda, F. J. Sancho, A. Sureda, R. Martino, J. Briones, S. Brunet, C. Canals, and J. Sierra. 2004. Frequent severe liver iron overload after stem cell transplantation and its possible association with invasive aspergillosis. Bone Marrow Transplant. 34:505-509. [DOI] [PubMed] [Google Scholar]
- 4.Antachopoulos, C., T. J. Walsh, and E. Roilides. 2007. Fungal infections in primary immunodeficiencies. Eur. J. Pediatr. 166:1099-1117. [DOI] [PubMed] [Google Scholar]
- 5.Balajee, S. A., A. Imhof, J. L. Gribskov, and K. A. Marr. 2005. Determination of antifungal drug susceptibilities of Aspergillus species by a fluorescence-based microplate assay. J. Antimicrob. Chemother. 55:102-105. [DOI] [PubMed] [Google Scholar]
- 6.Boelaert, J. R., M. de Locht, J. Van Cutsem, V. Kerrels, B. Cantinieaux, A. Verdonck, H. W. Van Landuyt, and Y. J. Schneider. 1993. Mucormycosis during deferoxamine therapy is a siderophore-mediated infection. In vitro and in vivo animal studies. J. Clin. Investig. 91:1979-1986. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Brakhage, A. A. 2005. Systemic fungal infections caused by Aspergillus species: epidemiology, infection process and virulence determinants. Curr. Drug Targets 6:875-886. [DOI] [PubMed] [Google Scholar]
- 8.Cornely, O. A., J. Maertens, D. J. Winston, J. Perfect, A. J. Ullmann, T. J. Walsh, D. Helfgott, J. Holowiecki, D. Stockelberg, Y. T. Goh, M. Petrini, C. Hardalo, R. Suresh, and D. Angulo-Gonzalez. 2007. Posaconazole vs. fluconazole or itraconazole prophylaxis in patients with neutropenia. N. Engl. J. Med. 356:348-359. [DOI] [PubMed] [Google Scholar]
- 9.de Locht, M., J. R. Boelaert, and Y. J. Schneider. 1994. Iron uptake from ferrioxamine and from ferrirhizoferrin by germinating spores of Rhizopus microsporus. Biochem. Pharmacol. 47:1843-1850. [DOI] [PubMed] [Google Scholar]
- 10.Gallin, J. I., D. W. Alling, H. L. Malech, R. Wesley, D. Koziol, B. Marciano, E. M. Eisenstein, M. L. Turner, E. S. DeCarlo, J. M. Starling, and S. M. Holland. 2003. Itraconazole to prevent fungal infections in chronic granulomatous disease. N. Engl. J. Med. 348:2416-2422. [DOI] [PubMed] [Google Scholar]
- 11.Gupta, A. K., and A. R. Skinner. 2003. Ciclopirox for the treatment of superficial fungal infections: a review. Int. J. Dermatol. 42(Suppl. 1):3-9. [DOI] [PubMed] [Google Scholar]
- 12.Ibrahim, A. S., J. E. Edwards, Jr., Y. Fu, and B. Spellberg. 2006. Deferiprone iron chelation as a novel therapy for experimental mucormycosis. J. Antimicrob. Chemother. 58:1070-1073. [DOI] [PubMed] [Google Scholar]
- 13.Ibrahim, A. S., T. Gebermariam, Y. Fu, L. Lin, M. I. Husseiny, S. W. French, J. Schwartz, C. D. Skory, J. E. Edwards, Jr., and B. J. Spellberg. 2007. The iron chelator deferasirox protects mice from mucormycosis through iron starvation. J. Clin. Investig. 117:2649-2657. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Johnson, M. D., C. MacDougall, L. Ostrosky-Zeichner, J. R. Perfect, and J. H. Rex. 2004. Combination antifungal therapy. Antimicrob. Agents Chemother. 48:693-715. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Kontoyiannis, D. P., G. Chamilos, R. E. Lewis, S. Giralt, J. Cortes, I. I. Raad, J. T. Manning, and X. Han. 2007. Increased bone marrow iron stores is an independent risk factor for invasive aspergillosis in patients with high-risk hematologic malignancies and recipients of allogeneic hematopoietic stem cell transplantation. Cancer 110:1303-1306. [DOI] [PubMed] [Google Scholar]
- 16.Latge, J. P. 1999. Aspergillus fumigatus and aspergillosis. Clin. Microbiol. Rev. 12:310-350. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Lin, S. J., J. Schranz, and S. M. Teutsch. 2001. Aspergillosis case-fatality rate: systematic review of the literature. Clin. Infect. Dis. 32:358-366. [DOI] [PubMed] [Google Scholar]
- 18.Loewe, S. 1927. Die Mischarznei. Versuch einer allgemeinen Pharmakologie der Arzneikombinationen. Klin. Wochenschr. 23:1077-1085. [Google Scholar]
- 19.Mohr, J., M. Johnson, T. Cooper, J. S. Lewis, and L. Ostrosky-Zeichner. 2008. Current options in antifungal pharmacotherapy. Pharmacotherapy 28:614-645. [DOI] [PubMed] [Google Scholar]
- 20.Ostrosky-Zeichner, L. 2008. Combination antifungal therapy: a critical review of the evidence. Clin. Microbiol. Infect. 14(Suppl. 4):65-70. [DOI] [PubMed] [Google Scholar]
- 21.Segal, B. H., and W. J. Steinbach. 2007. Combination antifungals: an update. Expert Rev. Anti-Infect. Ther. 5:883-892. [DOI] [PubMed] [Google Scholar]
- 22.Tallarida, R. J. 2006. An overview of drug combination analysis with isobolograms. J. Pharmacol. Exp. Ther. 319:1-7. [DOI] [PubMed] [Google Scholar]
- 23.Ullmann, A. J., J. H. Lipton, D. H. Vesole, P. Chandrasekar, A. Langston, S. R. Tarantolo, H. Greinix, W. Morais de Azevedo, V. Reddy, N. Boparai, L. Pedicone, H. Patino, and S. Durrant. 2007. Posaconazole or fluconazole for prophylaxis in severe graft-versus-host disease. N. Engl. J. Med. 356:335-347. [DOI] [PubMed] [Google Scholar]
- 24.Walsh, T. J., H. Teppler, G. R. Donowitz, J. A. Maertens, L. R. Baden, A. Dmoszynska, O. A. Cornely, M. R. Bourque, R. J. Lupinacci, C. A. Sable, and B. E. dePauw. 2004. Caspofungin versus liposomal amphotericin B for empirical antifungal therapy in patients with persistent fever and neutropenia. N. Engl. J. Med. 351:1391-1402. [DOI] [PubMed] [Google Scholar]
- 25.Zarember, K. A., J. A. Sugui, Y. C. Chang, K. J. Kwon-Chung, and J. I. Gallin. 2007. Human polymorphonuclear leukocytes inhibit Aspergillus fumigatus conidial growth by lactoferrin-mediated iron depletion. J. Immunol. 178:6367-6373. [DOI] [PubMed] [Google Scholar]