Abstract
OBJECTIVE:
The purpose of this study was to compare spirometry data between patients who underwent single-lung or double-lung transplantation the first year after transplantation.
INTRODUCTION:
Lung transplantation, which was initially described as an experimental method in 1963, has become a therapeutic option for patients with advanced pulmonary diseases due to improvements in organ conservation, surgical technique, immunosuppressive therapy and treatment of post-operative infections.
METHODS:
We retrospectively reviewed the records of the 39 patients who received lung transplantation in our institution between August 2003 and August 2006. Twenty-nine patients survived one year post-transplantation, and all of them were followed.
RESULTS:
The increase in lung function in the double-lung transplant group was more substantial than that of the single-lung transplant group, exhibiting a statistical difference from the 1st month in both the forced expiratory volume in one second (FEV1) and the forced vital capacity (FVC) in comparison to the pre-transplant values (p <0.05).
Comparison between double-lung transplant and single lung-transplant groups of emphysema patients demonstrated a significant difference in lung function beginning in the 3rd month after transplantation.
DISCUSSION:
The analyses of the whole group of transplant recipients and the sub-group of emphysema patients suggest the superiority of bilateral transplant over the unilateral alternative. Although the pre-transplant values of lung function were worse in the double-lung group, this difference was no longer significant in the subsequent months after surgery.
CONCLUSION:
Although both groups demonstrated functional improvement after transplantation, there was a clear tendency to greater improvement in FVC and FEV1 in the bilateral transplant group. Among our subjects, double-lung transplantation improved lung function.
Keywords: Lung transplantation, Spirometry, Respiratory function tests, Emphysema, Insufflation
INTRODUCTION
Lung transplantation, which was initially described as an experimental method in 1963, has become a therapeutic option for patients with advanced pulmonary diseases due to improvements in organ conservation, surgical technique, immunosuppressive therapy and treatment of post-operative infections.
In agreement with the International Society for Heart and Lung Transplantation, the procedure is indicated for patients with advanced chronic pulmonary disease without control in spite of maximal medical therapy or for those for whom there is no efficient medical treatment.1
Initially, pulmonary fibrosis was the only indication for lung transplantation;2 however, indications have expanded to include cystic fibrosis, primary and secondary forms of pulmonary hypertension (PH), bronchiectasis and chronic obstructive pulmonary disease (COPD), primarily of the emphysema phenotype.3
Chronic obstructive pulmonary disease (COPD) is expected to be the fifth leading cause of death in the world by 20204. For many years, the only treatment that improved survival in patients with advanced COPD was chronic home oxygen therapy.5,6 Since the 1990s, orthotopic lung transplantation has proved to be an effective therapeutic alternative, although the indication for this procedure is restricted by criteria of age, comorbidity, and feasibility of the surgery.7
There is a clear post-transplant survival benefit in patients with advanced pulmonary fibrosis and PH. In patients with cystic fibrosis and COPD a clear survival benefit has not yet been demonstrated, but the post-transplantation gain in quality of life and in physical activities tolerance appears to be more important.8–12 We have also demonstrated that post-transplantation bronchial stenosis can be corrected with a self-expandable silicone stent.13
The lung transplant program at our institution began in 1990. This program has experienced irregular patient turnover and inactive periods. Between 1990 and 2003, 20 single-lung transplantations were performed. Between 2003 and 2007, when a permanent and exclusive team was created, our institution performed 60 transplants. Of those 60 procedures, 36 were double-lung transplants. We performed an annual mean of 15 transplants between 2006 and 2007.
When lung transplantation is indicated, a unilateral or bilateral transplantation may be carried out. Single-lung surgery maintains a native lung, whereas double-lung transplants require the removal of both native lungs from the receiver.
Double lung transplant is a necessity for suppurative diseases that attack both native lungs. In these cases, the persistence of an infected lung in a transplanted individual who needs immunosuppressive therapy can lead to infectious exacerbations and risk of respiratory complications, such as chronic sputum production and progressive physical limitation after the operation.
Since the unilateral transplant technique is easier and requires less surgical time, patients with non-suppurative diseases like emphysema and pulmonary fibrosis often initially undergo this procedure.14 However, even in non-suppurative diseases, there seems to be prolonged improvement when bilateral transplants are performed. For example, in patients with COPD who underwent bilateral lung transplantation, superior lung function and a trend towards improved long-term survival were observed despite apparent equity between the two methods when exercise tolerance and quality of life were assessed.3,15
Since its initial description, the survival of lung transplantation patients has increased. At present, some centers report one-year survival in excess of 80%, with an average of 60% survival after 3 years. With this increase in life expectancy, it is important to study the methods of follow-up and long-term control in order to quickly and precisely diagnose infectious complications and rejection.16
Spirometry is used in the follow-up of transplanted patients. The evaluation of FEV1 and FVC is a reproducible method for screening for complications including rejection, bronchiolitis obliterans and infection. This method has a low diagnosis specificity regarding the type of complication.
In case of unilateral transplants, there is an additional pitfall in the interpretation of spirometric data. An observed decrease in FEV1 can be a consequence of complications in the transplanted lung as well as progression of the disease or hyperinsufflation in the native lung.
Decreases in FVC and FEV1 greater than 11% and 12%, respectively, are considered significant for bilateral transplantation. In comparison, decreases in the FVC and FEV1 of greater than 12% and 13%, respectively, are considered significant for unilateral transplantation. Such decreases mandate investigation of rejection or infection of the organ.17
As noted previously, the surgical technique for bilateral transplantation is more laborious than that for unilateral transplantation. However, if this procedure presents long-term advantages for the transplanted patient, this operation is indicated. The advantages of bilateral transplantation in patients with non-suppurative pulmonary diseases have not been confirmed. Recent data show that spirometry following double-lung transplantation is marginally superior to that following single-lung transplantation in patients with emphysema.18
The purpose of this study was to compare spirometry data between patients who underwent single-lung and double-lung transplantation at the first year after the transplant procedure. We intend to determine whether bilateral lung transplantation conveys a larger gain in pulmonary function and whether this advantage persists after one year of follow-up. These results will contribute to the growing evidence that bilateral lung transplantation is superior to the unilateral alternative.
METHODS
We retrospectively reviewed the records of the 39 patients who underwent lung transplantation in our institution between August 2003 and August 2006. Twenty-nine of the patients survived to one year after surgery, and all of them were followed. Another 10 patients (9 single-lung transplantation and 1 double-lung transplantation) died within the first post-operative year. These patients were excluded from the study.
The follow-up after hospital discharge was carried out weekly until the end of the third month, after which it was conducted monthly or twice-monthly. In all visits, the patient was evaluated by the performance of pulmonary function tests, a radiological examination and blood tests.
The immunosuppressive therapy regimen used by our group consists of induction with Basiliximab (Simulect) for suppurative patients and 1 gram of metilprednisolone intraoperatively for all patients. The maintenance regimen consists of tacrolimus, azathioprine and steroids. If the patient is intolerant to tacrolimus, they receive cyclosporine instead. In addition, azathioprine can be replaced with mycophenolate mofetil. The standard treatment for acute rejection is 10 mg/kg pulse therapy with metilprednisolone.
All patients underwent monthly vigilance bronchoscopies for the first twelve months after transplantation. We collected biopsies and bronchoalveolar lavage in order to identify rejection and infections. After this period, the bronchoscopies were performed according to clinical indication.
The spirometric values of these 29 patients who achieved more than 1 year survival after lung transplantation were analyzed. The FVC and FEV1 values were analyzed as the percent of predicted value from the last test performed before transplantation. These tests were performed at 1 month, 3 months, 6 months, 9 months and one year following transplantation.
All spirometric measurements were carried out in accordance with the guidelines of the International Proceedings in Portable Spirometer (Koko Spirometry; Pulmonary Data Services Instrumentation, Inc, Louisville, Lap) or Pletsmograph (MedGraphics Elite Dx System, St Paul, MN). The results are expressed in absolute values and percentage of the predicted value using the equations reported by Knudson et al.19 All tests were carried out in the morning (Mondays from 8:30 to 11:30 am).20
The patients were divided into two groups according to the type of lung transplant. The single-lung group included 11 patients, and the double-lung group included 18 patients.
Each measurement passed a normality test (Kolmogorov-Smirnov). The spirometric evolution of each group from pre-transplant up to one year post-operation was compared using analysis of variance (ANOVA). The comparative analysis between unilateral and bilateral transplants at each time point was performed by a students t-test for comparison of averages. The value of significance was alpha = 0.05.
The sub-group of pulmonary emphysema patients (five unilateral transplants and four bilateral transplants) was analyzed separately with the same statistical methodology. The statistical calculations were carried out by use of Sigma Plot V10.0 (SPSS, Chicago, IL).
RESULTS
Demographic characteristics and lung function pre-transplantation
The lung function of eighteen patients who underwent bilateral lung transplantation and eleven patients who received unilateral transplants were analyzed. Table 1 shows the baseline data of each group of patients. There was a difference in the FVC and FEV1 on the pre-transplant spirometry between unilateral and bilateral transplant recipients (p=0.002 and p<0.001, respectively). The patients who underwent double-lung transplantation had worse lung function pre-transplantation. The FVC of transplanted double-lung recipients was, on average, 14% less than in the unilateral transplant group. The difference of the preoperative FEV1 was 11%. The median age of the two groups was also different; unilateral transplant recipients averaged 13 years older than bilateral recipients (p=0.005).
Table 1 -.
Demographic data of lung transplant recipients: Single- vs. Double-lung transplant. (alpha = 0.05)
| Single Lung N=11 | Double Lung N=18 | ||
|---|---|---|---|
| Sex | 4F, 7M | 5F, 13M | p = 0.694 |
| Age (y) | 53.9 +/− 7.10 | 40.83 +/− 12.86 | p = 0.005 |
| Height (cm) | 160 +/− 9.06 | 164 +/− 8.0 | p = 0.206 |
| Weight (Kg) | 61.09 +/− 10.75 | 58.55 +/− 12.32 | p = 0.578 |
| FVC % | 54.27 +/− 7.70 | 40.23 +/− 12.45 | p = 0.002 |
| FEV1% | 44.11 +/− 18.59 | 23.68 +/− 9.18 | p < 0.001 |
| Disease | p = 0.007 | ||
| Emphysema | 5 | 4 | |
| Pulmonary Fibrosis | 6 | 1 | |
| Bronchiectasis | 6 | ||
| Cystic Fibrosis | 5 | ||
| Lymphangioleiomyomatosis | 1 | ||
| Pulmonary | 1 | ||
| Hypertension | |||
Regarding the underlying disease, the single-lung transplant group contained a higher number of pulmonary fibrosis patients, while the double-lung transplant group consisted of more patients with cystic fibrosis, bronchiectasis, lymphangioleiomyomatosis and PH. Pulmonary emphysema was the only condition with similar numbers of unilateral and bilateral recipients in our cohort.
Post-transplant lung function evolution
Table 3 shows the mean values for FVC and FEV1 percent predicted in both single- and double-lung transplant recipients during follow-up.
Table 3 -.
Lung Function values in all single and double lung transplant recipients during follow-up
| Single Lung N=5 | Double Lung N=4 | ||
|---|---|---|---|
| Sex | 3F, 2M | 4M | p = 1.000 |
| Age (y) | 52.2 +/− 8.13 | 56.25 +/− 6.39 | p = 0.444 |
| Height (cm) | 155 +/− 9.0 | 165 +/− 7.1 | p = 0.128 |
| Weight (Kg) | 55.4 +/− 7.4 | 63.8 +/− 16.2 | p = 0.331 |
| FVC % | 52.98 +/− 8.70 | 51.02 +/− 11.73 | p = 0.781 |
| FEV1% | 27.15 +/− 5.58 | 21.08 +/− 4.75 | p = 0.128 |
Values expressed in % predicted value.
Statistically significant difference between single and double transplant groups.
Statistically significant difference compared to pre-transplant values. Alpha = 0.05
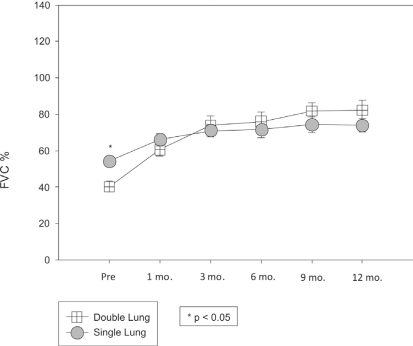
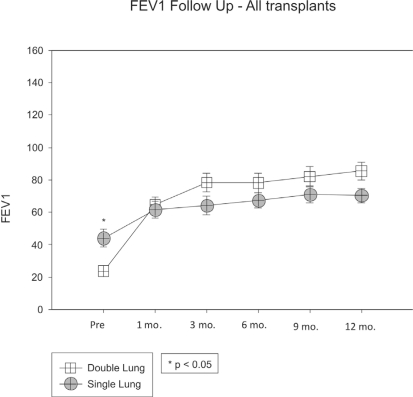
The increase in lung function in the double-lung transplant group was more marked, showing a statistical difference from the 1st month in both the FEV1 (Figure 1) and FVC (Figure 2) in comparison to the pre-transplant values (p <0.05). The FVC of this group continued to increase during the first postoperative year. We observed a significant increase between the values in the 9th and 12th month as compared with the first post-operative month (p <0.05).
Figure 1 -.
Forced vital capacity of lung transplant recipients (Single- vs. Double-lung transplant group)
Figure 2 -.
Forced expiratory volume in one second of lung transplant recipients (Single- vs. Double-lung transplant group)
In the single-lung transplant group, there was significant increase of FVC after 3 months (p=0.002) and FEV1 after 6 months (p=0.004). After 3° and 6° months, the FVC and FEV1 of the unilateral group did not vary significantly, respectively.
Comparison of FEV1 and FVC post-transplant values (1, 3, 6, 9 and 12 months) between the unilateral and bilateral transplant groups did not show any statistically significant differences. Both groups improved from a functional point of view.
The bilateral transplant group had a proportionally higher gain since their pre-transplant lung function was more compromised. In double-lung transplant recipients, the FEV1 increased 3.75-fold from pre-transplantation values at 12 months post-transplantation. By contrast, a 1.66-fold increase was observed in the single-lung group over the same period of time (p<0.001). The FVC increased 2.14-fold in the bilateral group versus a 1.37-fold increase in the unilateral group (p<0.001).
Sub-group of emphysema patients
During the period analyzed in our study, nine patients with pulmonary emphysema underwent pulmonary transplantation, five single-lung and four double-lung transplants. We compared the two techniques in this sub-group of patients.
When the pre-transplant variables of each group were compared, there was no observed difference in age, height, weight or pulmonary function (Table 2).
Table 2 -.
Demographic data of lung transplant emphysema recipients: Single- vs. Double-lung transplant (alpha=0.05)
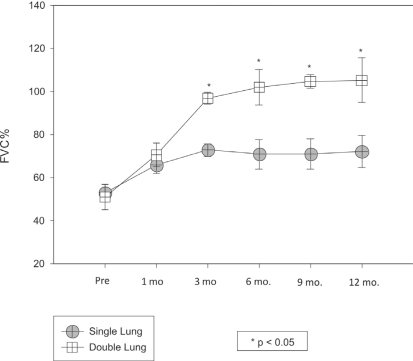
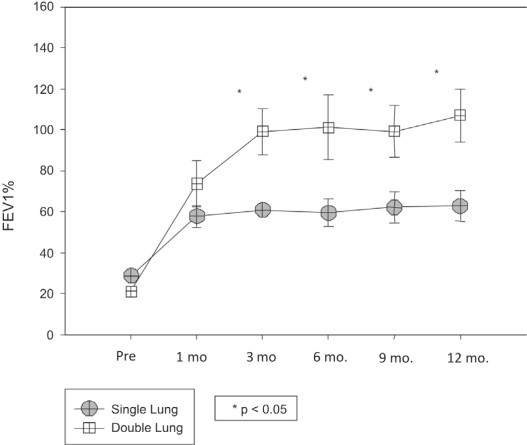
Figures 3 and 4 show the evolution of the functional data (FVC and FEV1) during the one year follow-up of the emphysema patients subjected to lung transplantation. There was no significant variation in the FVC in the unilateral group during the post-transplant months in comparison with pre-transplant values (p=0.861). For the same group, the post-transplant FEV1 values increased from the sixth month post-transplantation onwards (p=0.002). The double-lung transplant group showed significant increases in FVC and FEV1 from the third month post-transplantation onwards (p <0.001 and p=0.002).
Figure 3 -.
Forced vital capacity of lung transplant recipients with emphysema (Single- vs. Double-lung transplant group)
Figure 4 -.
Forced expiratory volume in one second of lung transplant recipients with emphysema (Single- vs. Double-lung transplant group)
Comparisons between the two groups show a difference in lung function beginning in the third month post-transplantation. The unilateral transplant group had an average FVC of 72.7 ± 5.8% of the predicted value, and the bilateral group had an average of 96.8 ± 5.6% (p=0.001) of the predicted value. This finding is reproducible when comparing FEV1: the value for the unilateral group was 53.4 ± 15.1 % of predicted value and the value for the bilateral group was 99.1 ± 22.2% of the predicted value (p=0.015). The difference in lung function between the groups was maintained in all follow up measurements.
DISCUSSION
This study compared the spirometric evolution of single- and double-lung transplant patients in the first year after surgery. The results of the analyses of the whole group and the sub-group of emphysema patients suggest the superiority of bilateral transplantation over the unilateral alternative.
The values of the FVC and FEV1 pre-transplantation were lower in patients who underwent double-lung transplantation when compared to unilateral transplantation. This difference is explained by the selection of younger and more functionally impaired patients, such as those with cystic fibrosis and bronchiectasis, for the bilateral procedure.
Although the pre-transplant lung function values were worse in the double-lung transplantation group, this difference was not observed in the months following surgery. After one year of follow-up, we observed an average 2.14-fold gain in the initial value of the FVC and a 3.75-fold increase in the FEV1 in bilateral transplant patients. By contrast, we observed a 1.37-fold increase in the initial FVC value and a 1.66-fold increase in the FEV1 in unilateral transplant recipients. (P=0.004 and P=0.001, respectively).
Despite the initial disparities in lung function, we demonstrated equality between the groups at one month post-transplantation. This equality persisted through the end of the first year. There were no statistically or clinically significant differences between these groups. In summary, in spite of worse initial lung function, double-lung transplant patients exhibited functional performance, as measured by spirometry, that was equal to or better than the single-lung recipients during the observed period of follow-up.
In our analysis of the group of emphysema patients, we compared the two transplant modalities in patients with similar anthropometric characteristics and preoperative function. In those patients with similar characteristics, the double-lung transplant patients showed greater increase in lung function relative to the single-lung recipients from the 3rd month post-transplantation.
There is no consensus on the ideal timing of transplantation in patients with COPD. The current recommendation is to include only patients with severe COPD and respiratory insufficiency. This suggestion is the most appropriate because of the high rate of associated mortality in this population.10,11
Approximately 40% of pulmonary transplants are currently carried out for advanced pulmonary emphysema.16 It is not clearly established whether bilateral transplantation is advantageous in this group. However, for single-lung transplantation, evidence suggests that hyperinsufflation of the native lung can lead to an imbalance in the ventilation/perfusion ratio and serious negative hemodynamic consequences.21 The literature indicates that single-lung transplantation has a higher mortality rate than double-lung transplantation. The risk of death in emphysema patients receiving a single-lung transplant was nine-fold higher than in the patients who underwent the bilateral procedure.15 In addition, the improved long-term survival of double-lung over single-lung recipients among patients with emphysema remains a favorable prognostic factor in the International Society of Heart and Lung Transplantation (ISHLT) registry.16
In our study, patients with emphysema presented with pre-operative values for FVC and FEV1 that were similar to those reported in the literature. A series of 306 recipients reported by Cassivi et al showed mean FVC and FEV1 of 51% and 16% of the predicted values, respectively.22 In the study above cited, the mean values increased to 84% and 79% of the predicted values at the end of the 1 year follow-up. The difference in these values is significant. Our study demonstrated a significant increase of the same values, but the increases in FEV1 and FVC in double-lung transplantation were observed from the third month post-transplantation onwards. In single-lung transplants, six months were required before a significant difference in FEV1 was observed. Ferrer et al7 reported that mean values for FVC and FEV1 were 41.8% and 21.1% of the predicted values in a sample of 65 patients with emphysema. One must consider, however, that patients who underwent single-lung transplant may have exhibited worse performance in the post-operative examinations due to persistence and progression of disease in the native lung .
Another factor associated with the single lung transplant functional performance might be hyperinflation of the remaining lung. Hyperinflation of the native lung is defined as swinging of the mediastinum towards the grafted lung with rectification of the ipsilateral diaphragm. Hyperinflation leads to a mechanical disadvantage for ventilation and can cause hemodynamic worsening due to increased thoracic pressure. Hyperinflation is associated with low FVC and FEV1 values in unilateral transplantation, especially in patients with obstructive diseases.23
Better spirometry results were obtained for bilateral-lung transplant recipients. Hyperinflation of the native lung may explain the reduced functional values observed for single-lung recipients. Pulmonary fibrosis is another disease that was treated with double-lung transplantation. Based on the results of this study, it is unclear whether patients with PF exhibit similar functional outcomes to those observed in patients with emphysema, as our cohort contained six patients who underwent double-lung transplantation and only one who underwent single-lung transplantation.
However, when both lungs are replaced in bilateral transplantation, the influence of the pulmonary disease on post-operative functional performance is reduced.
In conclusion, we observed significant improvement of lung function in unilateral and bilateral transplant recipients after one year of follow-up. There was a clear tendency of greater improvement in FVC and FEV1 in the bilateral transplant group. Evaluation of a larger patient population and longer follow-up are necessary in order to confirm these observations.
REFERENCES
- 1.Maurer JR, Frost AE, Estenne M, Higenbottam T, Glanville AR. International guidelines for the selection of lung transplant candidates. The International Society for Heart and Lung Transplantation, the American Thoracic Society, the American Society of Transplant Physicians, the European Respiratory Society. Transplantation. 1998;15(66):951–6. doi: 10.1097/00007890-199810150-00033. [DOI] [PubMed] [Google Scholar]
- 2.The Toronto Lung Transplant Group Experience with single-lung transplantation for pulmonary fibrosis JAMA 1988152592258–62. [PubMed] [Google Scholar]
- 3.Pochettino A, Kotloff RM, Rosengard BR, Arcasoy SM, Blumenthal NP, Kaiser LR, et al. Bilateral versus single lung transplantation for chronic obstructive pulmonary disease: intermediate-term results Ann Thorac Surg 2000701813–8.discussion 1818–9 [DOI] [PubMed] [Google Scholar]
- 4.Murray CJ, Lopez AD.Alternative projections of mortality and disability by cause 1990–2020: Global Burden of Disease Study Lancet 1997243491498–504. [DOI] [PubMed] [Google Scholar]
- 5.Nocturnal Oxygen Therapy Trial Group Continuous or nocturnal oxygen therapy in hypoxemic chronic obstructive lung disease: a clinical trial. Ann Intern Med. 1980;93:391–8. doi: 10.7326/0003-4819-93-3-391. [DOI] [PubMed] [Google Scholar]
- 6.Long term domiciliary oxygen therapy in chronic hypoxic cor pulmonale complicating chronic bronchitis and emphysema Report of the Medical Research Council Working Party. Lancet. 1981;28(1):681–6. [PubMed] [Google Scholar]
- 7.Ferrer J, Rodriguez E, Roman A, Bravo C, Roldan J, Hermosilla E, et al. Factors related to postoperative mortality in lung transplantation for emphysema. Transplant Proc. 2007;39:3317–22. doi: 10.1016/j.transproceed.2007.09.006. [DOI] [PubMed] [Google Scholar]
- 8.Chu CM, Chan VL, Lin AW, Wong IW, Leung WS, Lai CK. Readmission rates and life threatening events in COPD survivors treated with non-invasive ventilation for acute hypercapnic respiratory failure. Thorax. 2004;59:1020–5. doi: 10.1136/thx.2004.024307. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Geertsma A, Ten Vergert EM, Bonsel GJ, de Boer WJ, van der Bij W. Does lung transplantation prolong life? A comparison of survival with and without transplantation. J Heart Lung Transplant. 1998;17:511–6. [PubMed] [Google Scholar]
- 10.Thabut G, Mal H, Castier Y, Groussard O, Brugiere O, Marrash-Chahla R, et al. Survival benefit of lung transplantation for patients with idiopathic pulmonary fibrosis. J Thorac Cardiovasc Surg. 2003;126:469–75. doi: 10.1016/s0022-5223(03)00600-7. [DOI] [PubMed] [Google Scholar]
- 11.Charman SC, Sharples LD, McNeil KD, Wallwork J. Assessment of survival benefit after lung transplantation by patient diagnosis. J Heart Lung Transplant. 2002;21:226–32. doi: 10.1016/s1053-2498(01)00352-7. [DOI] [PubMed] [Google Scholar]
- 12.Hosenpud JD, Bennett LE, Keck BM, Edwards EB, Novick RJ.Effect of diagnosis on survival benefit of lung transplantation for end-stage lung disease Lancet 1998335124–7. [DOI] [PubMed] [Google Scholar]
- 13.Samano MN, Minamoto H, Oliveira EQ, Caramori ML, Pêgo-Fernandes PM, Jatene FB. Bronchial stenosis treatment after lung transplantation with a self-expandable silicone stent. Clinics. 2007;62:643–644. doi: 10.1590/s1807-59322007000500019. [DOI] [PubMed] [Google Scholar]
- 14.Mal H, Andreassian B, Pamela F, Duchatelle JP, Rondeau E, Dubois F, et al. Unilateral lung transplantation in end-stage pulmonary emphysema. Am Rev Respir Dis. 1989;140:797–802. doi: 10.1164/ajrccm/140.3.797. [DOI] [PubMed] [Google Scholar]
- 15.Angles R, Tenorio L, Roman A, Soler J, Rochera M, de Latorre FJ. Lung transplantation for emphysema. Lung hyperinflation: incidence and outcome. Transpl Int. 2005;17:810–4. doi: 10.1007/s00147-004-0714-7. [DOI] [PubMed] [Google Scholar]
- 16.Trulock EP, Christie JD, Edwards LB, Boucek MM, Aurora P, Taylor DO, et al. Registry of the International Society for Heart and Lung Transplantation: twenty-fourth official adult lung and heart-lung transplantation report-2007. J Heart Lung Transplant. 2007;26:782–95. doi: 10.1016/j.healun.2007.06.003. [DOI] [PubMed] [Google Scholar]
- 17.Martinez JA, Paradis IL, Dauber JH, Grgurich W, Richards T, Yousem SA, et al. Spirometry values in stable lung transplant recipients. Am J Respir Crit Care Med. 1997;155:285–90. doi: 10.1164/ajrccm.155.1.9001326. [DOI] [PubMed] [Google Scholar]
- 18.Mason DP, Rajeswaran J, Murthy SC, McNeill AM, Budev MM, Mehta AC, et al. Spirometry after transplantation: how much better are two lungs than one. Ann Thorac Surg. 2008;85:1193–201. 201, e1–2. doi: 10.1016/j.athoracsur.2007.12.023. [DOI] [PubMed] [Google Scholar]
- 19.Knudson RJ, Lebowitz MD, Holberg CJ, Burrows B. Changes in the normal maximal expiratory flow-volume curve with growth and aging. Am Rev Respir Dis. 1983;127:725–34. doi: 10.1164/arrd.1983.127.6.725. [DOI] [PubMed] [Google Scholar]
- 20.Miller MR, Crapo R, Hankinson J, Brusasco V, Burgos F, Casaburi R, et al. General considerations for lung function testing. Eur Respir J. 2005;26:153–61. doi: 10.1183/09031936.05.00034505. [DOI] [PubMed] [Google Scholar]
- 21.Stevens PM, Johnson PC, Bell RL, Beall AC, Jr, Jenkins DE.Regional ventilation and perfusion after lung transplantation in patients with emphysema N Engl J Med 197029282245–9. [DOI] [PubMed] [Google Scholar]
- 22.Cassivi SD, Meyers BF, Battafarano RJ, Guthrie TJ, Trulock EP, Lynch JP, et al. Thirteen-year experience in lung transplantation for emphysema Ann Thorac Surg 2002741663–9.discussion 9–70 [DOI] [PubMed] [Google Scholar]
- 23.Yonan NA, el-Gamel A, Egan J, Kakadellis J, Rahman A, Deiraniya AK. Single lung transplantation for emphysema: predictors for native lung hyperinflation. J Heart Lung Transplant. 1998;17:192–201. [PubMed] [Google Scholar]