Abstract
Children with type 1 diabetes are at risk for negative psychosocial and physiological outcomes, particularly as they enter adolescence. The purpose of this randomized trial (n=82) was to determine the effects, mediators, and moderators of a coping skills training intervention (n=53) for school-aged children compared to general diabetes education (n=29). Both groups improved over time, reporting lower impact of diabetes, better coping with diabetes, better diabetes self-efficacy, fewer depressive symptoms, and less parental control. Treatment modality (pump vs. injections) moderated intervention efficacy on select outcomes. Findings suggest that group-based interventions may be beneficial for this age group.
Keywords: coping skills training, child, type 1 diabetes
Effects of Coping Skills Training in School-age Children with Type 1 Diabetes
Type 1 diabetes (T1D) is one of the most common severe chronic illnesses in children, affecting 1 in every 400 individuals under the age of 20, over 176,000 American youth (National Institute of Diabetes and Digestive and Kidney Disease, 2002). Diabetes is the seventh leading cause of death in the United States, and adults with T1D are twice as likely to die prematurely from complications compared to adults without T1D National Institute of Diabetes and Digestive and Kidney Disease, 2007). Management of T1D is demanding, requiring frequent monitoring of blood glucose levels, monitoring and controlling carbohydrate intake, daily insulin treatment (3-4 injections/day or infusion from a pump), and adjusting insulin dose to match diet and activity patterns (American Diabetes Association, 2008). Such an intensive treatment regimen and maintenance of near-normal glycemic control may delay or prevent long-term complications of T1D by 27-76% (Diabetes Control and Complications Trial [DCCT] Research Group, 1994). Interventions are needed to assist children and families in coping with the considerable demands of living with T1D. The purpose of this study was to evaluate the efficacy of a coping skills training (CST) intervention, specific to school-aged children and their parents, on metabolic control and psychosocial outcomes, and to examine mediators and moderators of these outcomes.
Tasks of childhood development can compromise diabetes management. Metabolic control declines during adolescence (Travis, Brouhard, & Schreiner, 1987). Although the physiological changes of puberty contribute to insulin resistance, a premature transfer of responsibility for diabetes-related tasks from parents to children also may result in poor adherence and metabolic control (Anderson, Ho, Brackett, Finkelstein, & Laffel, 1997; Holmes et al., 2006; Schilling, Knafl, & Grey, 2006). As children enter adolescence and strive for autonomy, parents' attempts to monitor or control their child's treatment may be viewed as intrusive or nagging, which may result in adolescents becoming resistant, defiant, and noncompliant (Berg et al., 2007; Cameron et al., 2008; Weinger, O'Donnell, & Ritholz, 2001). Low levels of family support and increased family conflict have been consistently associated with poor diabetes self-management, metabolic control, psychosocial adaptation, and quality of life (QOL) in adolescents with T1D (Pendley et al., 2002; Whittemore, Kanner, & Grey, 2004; Wysocki, 1993). In addition, T1D is a risk factor for depression in youth, with the prevalence of clinically significant depressive symptoms ranging from 12-15% in children to 15-27% in adolescents with T1D (Hood et al., 2006; Kokkonen, Lautala, & Salmela, 1997; Kovacs, Goldston, Obrosky, & Bonar, 1997; Whittemore et al., 2002).
Due to the risks associated with poor metabolic control and psychosocial adjustment for adolescents with T1D, increasing attention is being paid to the developmental transition between pre-adolescence and adolescence for the promotion of better health outcomes. Parents may need to adjust their level of involvement, so that children can exercise developmentally-appropriate gains in autonomy, while continuing to rely upon parents for support, guidance, and encouragement (Anderson, Auslander, Jung, Miller, & Santiago, 1990). Research supports the need for children and parents to work cooperatively with open communication and flexible problem-solving skills in order to negotiate shared responsibility for treatment management (Schilling et al., 2006; Wysocki, 1993). Parental guidance, warm and caring family behaviors, open communication, and expression of feelings have demonstrated protective effects on metabolic control and psychosocial adjustment (Davis et al., 2001; Faulkner & Chang, 2007; Grey, Boland, Davidson, & Tamborlane 2001).
Family-based psychosocial interventions have been developed to improve family interactions and enhance the well-being of youth with T1D. In several randomized trials family-based interventions improved family relations, communication, problem-solving skills, treatment adherence, and metabolic control. For example, Anderson and colleagues showed that a low-intensity office-based, family intervention increased parental involvement, while decreasing diabetes-related family conflict (Anderson, Brackett, Ho, & Laffel, 1999; Laffel et al., 2003). Other researchers have targeted families at high risk for problems. Wysocki and colleagues (2008) demonstrated that intensive behavior family systems therapy improved outcomes in families with high levels of conflict. Ellis and colleagues (2007) demonstrated that a comprehensive home- and community-based intervention improved outcomes in families with low socioeconomic status. The majority of these family-based interventions targeted adolescents and were focused primarily on problem solving and communication. However, variables such as coping and self-efficacy also have been associated with improved adherence, family functioning, psychosocial adjustment, and metabolic control in youth with T1D (Graue, Wentzel-Larsen, Bru, Hanestad, & Sovik, 2004; Grey, Lipman, Cameron, & Thurber, 1997; Griva, Myers, & Newman, 2000).
Coping skills training (CST) is based on social cognitive theory, which proposes that individuals can actively influence many areas of their lives, particularly coping and health behaviors (Bandura, 1997). A major premise of this approach is that practicing and rehearsing a new behavior, such as learning how to cope successfully with a problem situation, can enhance self-efficacy and promote positive behaviors (Marlott & Gordon, 1985). The goal of CST is to increase competence and mastery by retraining non-constructive coping styles and behaviors into more constructive behaviors. There is evidence supporting the potential efficacy of CST to promote positive health outcomes in youth with and without a chronic illness (see review by Davidson, Boland, & Grey, 1997). A randomized clinical trial of a CST program, based on Forman's (1993) protocol, and modified for adolescents with T1D (Grey, Boland, Davidson, Yu, & Tamborlane, 1999), demonstrated improvements in metabolic control, psychosocial adjustment, and QOL at 6 and 12 month follow-up (Grey, Boland, Davidson, Li, & Tamborlane, 2000). Because a CST intervention demonstrated efficacy for adolescents with T1D, the potential to provide the intervention to other developmental phases, such as school-aged children, seems warranted.
In this study, we report long-term treatment effects of a coping skills training (CST) program for school age children (8-12 years old) and their parents compared to an attention control group who received supplemental diabetes education. A report of the preliminary short-term efficacy indicated that children and parents who received CST showed promising trends for more adaptive family functioning and greater life satisfaction than those families in group education (Ambrosino et al., 2008). These results support the potential application of CST in the developmental phase of 8-12 year olds. If school-aged children and parents can learn effective coping skills, a positive transition to adolescence may occur, one in which parents and children collaborate to maintain effective diabetes management.
Conceptual Framework
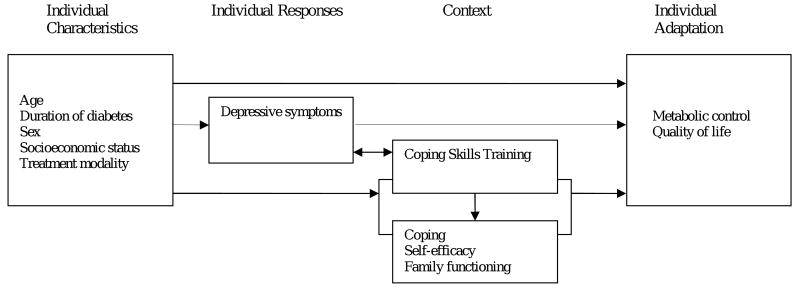
Stress-adaptation models provide a framework for the study of interventions to promote adaptation to chronic illness and posit that adaptation may be viewed as an active process whereby the individual adjusts to the environment and the challenges of a chronic illness. (Grey et al., 2001; Grey & Thurber, 1991; Pollock, 1993). Adaptation, in this framework, is the degree to which an individual adjusts both physiologically and psychosocially to the stress of living with a long-term illness. The framework suggests that individual characteristics, such as age, socioeconomic status, and in children with T1D, treatment modality (pump vs. injections), individual responses (depressive symptoms), and context (coping, self-efficacy, family functioning) influence the level of individual adaptation. In this model, adaptation has both physiologic (metabolic control) and psychosocial (QOL) components (see Figure 1). The CST was hypothesized to influence the individual's responses (depressive symptoms) and context (coping, self-efficacy, family functioning) directly and level of adaptation (metabolic control, QOL) both indirectly and directly.
Figure 1. Conceptual Framework.
Purpose
The primary aim of this randomized clinical trial was to determine the effect of group-based CST for school-aged children with T1D and their parents compared to an attention-control group receiving supplemental general diabetes education (GE) over a period of a year on children's metabolic control, QOL, depressive symptoms, coping, self-efficacy, and family functioning at 12-month follow-up. The data in this analysis include only child outcomes. The secondary aim was to explore mediators (coping, self-efficacy, family functioning) and moderators (age, sex, socioeconomic status, treatment modality) of intervention efficacy based on the conceptual framework. The following hypotheses were tested:
Children with T1D who participate in CST will demonstrate better metabolic control (lower HbA1c levels), better QOL, fewer depressive symptoms, fewer issues in coping, better diabetes self-efficacy, and better family functioning (stable or less family guidance and control and more family warmth and caring) compared to children with T1D who participate in GE.
Age, sex, socioeconomic status, and treatment modality will moderate the intervention effect on metabolic control and QOL.
Changes in coping, self-efficacy, and family functioning will mediate the intervention effect on metabolic control and QOL.
Method
Design and Sample
A two-group experimental design was used. Data were collected at baseline and 1, 3, 6, and 12 months post-randomization by trained research assistants who were blinded to group assignment. Children were eligible to participate if they were: (a) between the ages of 8 and 12 years; (b) diagnosed with T1D and treated with insulin for at least 6 months; (c) free of other significant health problems; and, (d) in school grade appropriate to within 1 year of child's age.
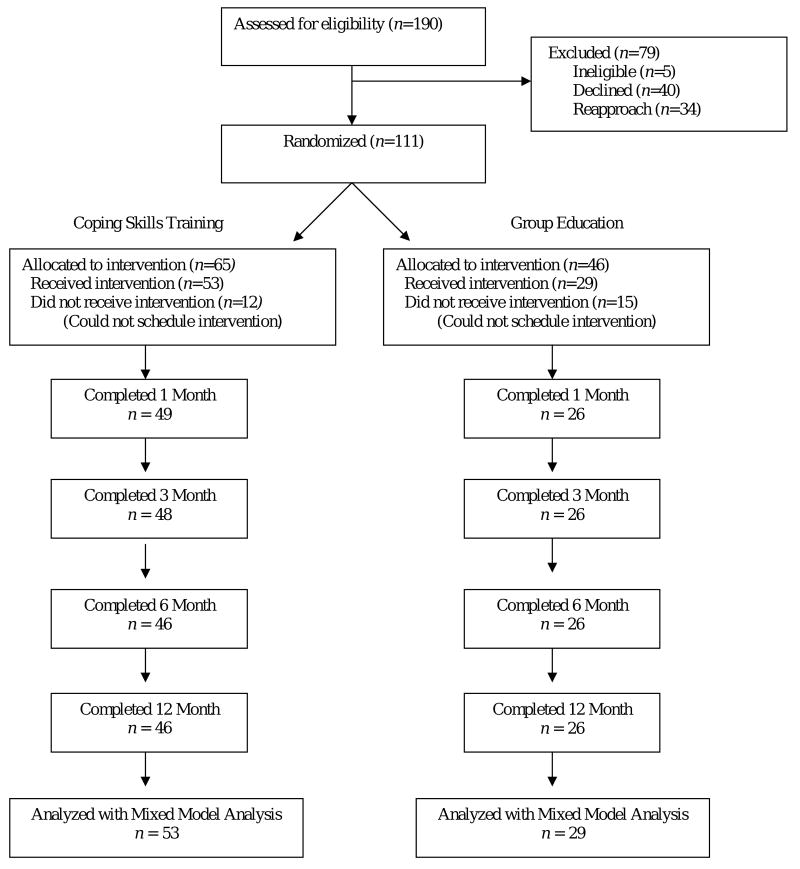
A sample of 100 subjects was determined by a power analysis based on the effect size seen in our adolescent study (Grey et al., 2000) and in our pilot work with younger children (difference in HbA1c was .7%). A two‐way analysis of variance with 100 subjects with a .05 significance level would have 98% power to detect a variance among the 2 group means of .04, 99% power to detect a variance among the 3 time means of .051, and 80% power to detect a interaction among the 2 group levels and the 3 time levels of .022, assuming that the common standard deviation is .04, when the sample size in each group is 50 (Elashoff, 1995). Due to problems scheduling groups, we were unable to meet our projected goal of 100 subjects (Figure 2).
Figure 2. Consort Table.
Of those approached for participation, approximately 58% agreed; 18% expressed interest and asked to be approached later, and 21% refused (e.g., too busy). Twenty-four percent of participants were unable to be scheduled for the group-based intervention and were excluded from the analysis due to lack of exposure to any aspects of the intervention (18% in the CST group and 33% in the GE group). This report is based on the 82 children who were exposed to the interventions. There were 53 children in the CST group and 20 in the GE group. Comparison of those who received the intervention (CST or GE) to those who enrolled but did not receive either intervention demonstrated that groups were comparable on baseline measures, other than an increased likelihood for white children and children whose mothers had higher education to receive the intervention. Data comparing attenders to nonattenders has previously been reported (Ambrosino et al., 2008). Attrition was low with only 10 participants dropping out or lost to follow up over the 1-year period (14%). Once scheduled, attendance at sessions was good. Participants of CST attended an average of 4.6 of 6 sessions (range=1-6; SD = 1.21); those in GE attended on average 3.3 of 4 sessions (range=1-4; SD = .75).
Descriptive statistics for the sample are provided in Table 1. Children were predominately white and of high income, which is consistent with the overall clinic composition. On average, children's duration of diabetes was 3.5 years; most were on pump therapy and had metabolic control comparable with the ADA's recommendations for age.
Table 1. Baseline Demographic and Clinical Characteristics.
| CST (N=53) n (%) or mean (SD) |
GE (N=29) n (%) or mean (SD) |
|
|---|---|---|
| Racial Group | ||
| White | 44 (83%) | 26 (90%) |
| Sex | ||
| Girls | 30(57%) | 20 (69%) |
| Treatment modality at study entry | ||
| Pump | 38 (72%) | 22 (76%) |
| Family Income | ||
| <$39 999 | 8 (15%) | 1 (4%) |
| $40 000-$79 999 | 13 (25%) | 7 (24%) |
| >$80 000 | 32 (60%) | 21 (72%) |
| Parent's relationship (mother) | 49 (92%) | 28 (97%) |
| Age (yr) | 9.9 (1.5) | 9.9 (1.4) |
| Diabetes duration (yr) | 3.7 (2.78) | 3.6 (3.0) |
| Mother's education(yr) | 15.4 (2.2) | 15.9 (2.4) |
Using Fisher's Exact test for categorical variables and t-test for continuous variables, there were no significant differences between groups.
Setting and Procedures
Children and their parents were approached for participation in the trial during regularly scheduled visits at a pediatric diabetes clinic in the northeast. Families interested in the study completed a consent/assent process approved by the university's Human Subjects Research Review Committee, as well as baseline questionnaires. Children who scored above criteria for elevated depressive symptoms on standardized questionnaires were referred for follow up, but not excluded from the intervention unless they required hospitalization for suicidality. After consent, participants were randomized by a sealed envelope technique to either CST or GE. Both groups received diabetes team care throughout the course of the study, and clinicians at the recruitment site were blinded to study group assignment.
Interventions
Coping Skills Training (CST)
The goal of CST in this age group is to increase a child's and his or her parents' sense of competence and mastery by retraining inappropriate or non-constructive coping styles and forming more positive styles and patterns of behavior. Unlike previous research with CST in T1D where the intervention was provided only to youth, CST in this study was provided as a family intervention, to both parents and youth. Specific coping skills that were addressed in the intervention included: communication, social problem solving, recognition of associations between thoughts, feelings, and behavior and guided self-dialogue, stress management, and conflict resolution around diabetes-specific stressors (Table 2). Six weekly sessions were conducted in small groups of 2-6 children; parents met simultaneously but separately. At the end of each session, children and their parents met together to share salient issues and discuss possible connections between group themes and family concerns.
Table 2. Coping Skills Training (CST) Session Content.
| Session | Description |
|---|---|
| 1. Introduction to CST | Session content, structure, rules, CST framework. Diabetes experience – discussion of commonalities and differences. |
| 2. Communication Skills | Forms of communication, including verbal and non-verbal cues. Puzzle game to explore styles of communication (passive, aggressive, and assertive) and assumptions about others. Skill practice and discussion to probe for managing difficult or embarrassing moments. |
| 3. Social Problem Solving | Use of a step-by-step model with diabetes specific situations including possible responses and alternatives to explore steps through role-playing. |
| 4. Conflict Resolution | Discussion about different conflict styles (avoidance, giving in, confrontation, being humorous, and problem solving). Animal photos depicting styles, participants identifying style. Situation role-playing to discover the most positive ways to handle conflict and difficult situations. |
| 5. Stress Management | Teaching of a variety of stress management techniques, including deep breathing, muscle relaxation, and guided imagery. |
| 6. Self-Talk | Identification of feelings to understand associations between feelings, thoughts, and behaviors. Presentation of a cognitive model to help further explore links and responses. Role-play of specific situations and discussion to encourage application of self-talk skills. |
Within each session, coping skills were presented and discussed. Role-play also was used for participants to practice a specific coping skill in a potentially difficult social situation. Trainers provided coaching on child or parent responses to the situation to enable participants to learn more skillful responses. All participants were encouraged to practice the specific skills at home in between sessions. Each 1.5 hour session was facilitated by a mental health professional. All CST groups were audio taped and reviewed for treatment fidelity.
Group Education (GE)
Because the usual method of working with youth with T1D is education, GE was provided as an attention-control condition, supplementing the individual diabetes education provided in clinic to all study participants. All children in this study received ongoing diabetes education within the context of quarterly clinic visits. The session content of the control condition provided a review of intensive insulin regimens (multiple daily injections and pump), carbohydrate counting and nutrition, sports and sick days, and updates on diabetes care and technology (Table 3). Age-appropriate written materials were provided at each session. Participants were encouraged to discuss the materials in each session and apply it to their individual family situations. Four weekly sessions were conducted in small groups of 2-6 children and their parent(s). Each 1.5 hour session was taught by an advanced practice nurse, and all sessions were audio taped and reviewed for treatment fidelity.
Table 3. Group Education (GE) Session Content.
| Session | Description |
|---|---|
| 1. Intensive Insulin Regimen | Glucose control, target glucose, and blood sugar trends Emphasis on how participants feel when blood sugar is well controlled, and how good blood sugar control prevents health complications Instruction in adjusting insulin when using multiple daily injections or the pump with examples |
| 2. Nutrition | Carbohydrate counting Three basic food groups (carbohydrates, protein, and fats) and the value of fiber Discussion of choosing food wisely (limiting sugar, reading food labels, and increasing intake of fruits and vegetables) Healthy recipes |
| 3. Sports and Sick Days | Health benefits of exercise Consideration of diabetes and exercise Sick day guidelines for pump and injection users Discussion of the importance of sleep Review of exercise and sick-day problem solving. |
| 4. Updates and Technology | New developments in diabetes technology and research (meters, pumps and pump features, continuous glucose monitoring systems, real-time glucose monitoring systems, pump and real-time glucose monitoring systems) Diabetes organizations that could be used as resources for information or referral. |
Measures
Data were collected from children on metabolic control, QOL, depressive symptoms, coping, self-efficacy, and family functioning. Self-report instruments were completed by the children, and demographic data were collected from a parent. The HbA1c and other treatment-related values were extracted from medical charts.
Metabolic control was assessed with HbA1c, a measure of the glycosylation of the hemoglobin molecule that reflects the child's average blood sugar over the past 3 months. Analyses were performed using the Bayer Diagnostics DCA2000®, which has evidence of high reliability (Tarrytown, NY, normal range = 4.2-6.3%). The ADA recommendation for the treatment goal for children age 6-12 years is <8% (Silverstein et al., 2005).
Child QOL was measured by the Diabetes Quality of Life Scale which has 3 subscales to assess youth perceptions of the impact of T1D management (21 items), their general satisfaction with life (18 items), and worries related to T1D (8 items). Scores range from 21-84 for impact, 18-72 for satisfaction, and 8-32 for worry. Higher scores indicate greater impact of diabetes on child's life (poorer QOL), more worry (poorer QOL), and greater life satisfaction (better QOL). The scale has evidence of adequate construct validity and internal consistency reliability (.82 – .85 for subscales; Ingersoll & Marrero, 1991). In our sample, alpha = .90 for impact, .84 for satisfaction, and .89 for worries.
Child depressive symptoms were measured with the Children's Depression Inventory (CDI) which assesses disturbance in mood and hedonic capacity, self-evaluation, vegetative functions, and interpersonal behaviors (Kovacs, 1985). The scale has 27 multiple choice items that yield total scores from 0 to 54 with higher scores reflecting more symptoms. The CDI has been used extensively in studies of school-aged children and adolescents, in groups with known mental health problems (Kovacs, Brent, Feinberg, Paulauskas, & Reid, 1986; Kovacs et al., 1990). Reliability estimates have been adequate, with internal consistency reliability between .71 and .87 (.84 in our data) and test‐retest reliability at .80 to .87. The inventory has concurrent and discriminant validity, and a score of 13 may be interpreted as the criterion score for elevated depressive symptoms (Smucker, Craighead, Craighead & Green, 1986). As in other studies, because depression is not normally distributed, CDI scores were treated with a square root transformation prior to analysis.
Coping was measured by the Issues in Coping with T1D- Child Scale which has two subscales that assess child perceptions of how hard or difficult it is to handle T1D management (14 items, range 0-42) or how upsetting T1D management is (12 items, range 12-36; Kovacs et al., 1986). Items are rated with a 4-point Likert-type scale, with higher scores indicating that children find it more difficult or upsetting to cope with diabetes. The scale has been used in previous studies of adaptation to diabetes over time, and internal reliability has ranged from .78-.90 (alpha = .72 for the How Hard subscale and .66 for the How Upsetting subscale in our sample).
Self-efficacy was measured by the Self-Efficacy for Diabetes Scale, which evaluates self-perceptions or expectations held by children with T1D about their personal competence, power, and resourcefulness for successfully managing their T1D (Grossman, Brink, & Hauser, 1987). The scale consists of 35 items in three subscales: diabetes-specific self-efficacy (24 items), medical situations self-efficacy (5 items), and, general situations (6 items). Participants are asked to rate their degree of confidence for all items on a 5-point scale (very sure I can to very sure I can't), with higher scores indicating lower self-efficacy. Only the diabetes-specific subscale was used in this analysis. Scores for his subscale range from 24-120. Reliability coefficient for the diabetes-specific subscale has been reported at .92 and validity studies demonstrate that the scale has content and discriminant validity (Grossman et al., 1987). The alpha coefficient for the diabetes-specific subscale was .84 in our data.
Family functioning was measured by the Diabetes Family Behavior Scale (DFBS; McKelvey et al., 1993) that evaluates diabetes-specific family behaviors thought to be important in helping or hindering a child in following a T1D regimen. The scale has two subscales measuring specific areas of family support: guidance-control (15 items) and warmth-caring (15 items). Higher scores on the guidance-control subscale indicate greater parental involvement in diabetes care (range 15-75), and higher scores on the warmth-caring subscale indicate more warmth and support with interactions related to diabetes care (range 15-75). Previous reliability coefficients were .81 for the guidance and control subscale and .79 for the warmth and caring subscale (McKelvey et al., 1993). Internal consistency for the present sample was .40 for guidance-control and .73 for warmth-caring.
Demographic and clinical data consisted of family sociodemographic data (i.e., race/ethnicity, education, socioeconomic status), child sex, child duration of illness, and treatment modality (pump vs. injections).
Data Analysis
All data were double-entered into a database and checked for accuracy. Analyses were conducted using SAS 9.2 (SAS Institute, Cary, NC). Groups were compared on baseline characteristics using t-tests for continuous variables and Fisher's Exact tests for categorical variables.
Comparison of CST with GE
To determine the effect of CST for children with T1D compared to the attention-control group (GE), a random coefficient regression analysis was used with an intent-to-treat approach (ITT). The ITT approach included all subjects in the data analysis, as randomized, regardless of whether they withdrew or deviated from the protocol (Fisher, et. al., 1990). The purpose is to preserve balance in the characteristics of groups achieved by randomization, and to guard against a potential bias in the outcomes from differential drop-outs.
SAS Proc Mixed was used to perform the random coefficient regression analysis, in which missing outcome data are treated as missing at random (MAR, i.e. given the previous outcome values and covariables, the missingness is independent of unobserved outcomes; Rubin, 1976). Outcomes of interest included metabolic control (HbA1c), diabetes QOL (impact, worry, and satisfaction), depressive symptoms, coping, self-efficacy, and family functioning (warmth/caring and guidance/control). Random coefficient models included intervention group, time, and the group by time interaction as fixed effects, along with random effects for subject-specific intercepts and slopes. This allowed each participant to have his or her own initial value of the outcome and the trajectory of change in the outcome. Differences in slopes (rates of change) between the two treatment groups, obtained from an interaction of treatment group-by-time in the regression model, were used to evaluate intervention efficacy. For an overall effect of time on each outcome of interest, regardless of group assignment, the group-by-time interaction was removed, and we evaluated the main effect of time. Analyses were adjusted for duration of diabetes diagnosis, child's sex, diabetes treatment modality (i.e., insulin injections or pump), and parental income. Results were presented as annual rates of change for each intervention group and combined across both groups. For outcomes that demonstrated differences at baseline an alternative mixed model was used to evaluate group differences at 3 months, 6 months, and 12 months, adjusting for the baseline value in the outcome. Additional analyses were performed using the last observation carried forward (LOCF; Hollis & Campbell, 1999) but did not result in substantial alterations in conclusions and are therefore not presented.
Mediators and Moderators of Intervention Efficacy
To explore mediators and moderators of intervention efficacy, additional analyses of rates of change in the outcomes were conducted to determine for whom and how the treatment may have worked (Kraemer, Wilson, Fairburn, & Agras, 2002). Based on previous research and the conceptual framework, the pre-existing characteristics of child age, sex, socioeconomic status, and treatment modality (i.e., insulin injections or pump) were evaluated as moderators of treatment by including their two and three-way interaction with treatment group and time in the regression models. Proposed mediators (coping, diabetes self-efficacy, and family functioning) of changes in outcomes (HbA1c and QOL) were evaluated by correlating 3-month changes in mediators (post intervention) with 1-year changes in outcomes using Pearson correlation coefficients. Associations among the 3-month changes and 6- and 12-month outcomes were further examined using random effect models and adjusting for baseline outcome(s), treatment modality, sex, income and group.
Results
Psychosocial variables
For psychosocial variables, children reported good coping, self-efficacy, family functioning and QOL. At baseline 11% of the children demonstrated elevated depressive symptoms. Children randomized to CST reported lower QOL and less family warmth and caring compared to children in GE (Table 4).
Table 4. Clinical and Psychosocial Variables at Baseline.
| CST (N=53) Mean (SD) |
GE (N=29) Mean (SD) |
p-value* | ||||
|---|---|---|---|---|---|---|
| HbA1c | 6.98 | (1.33) | 7.11 | (1.21) | .67 | |
| Diabetes QOL | ||||||
| Impact (Range 21-84) | 37.8 | (9.8) | 33.6 | (4.9) | .04 | |
| Satisfaction (Range 18-72) | 57.3 | (7.4) | 61.7 | (4.6) | .01 | |
| Worry (Range 8-32) | 12.5 | (5.0) | 10.3 | (2.1) | .03 | |
| CDI** (Range 0-54) | 7.0 | (6.1) | 5.5 | (4.5) | .30 | |
|
|
2.4 | (1.2) | 2.1 | (1.0) | ||
| Coping | ||||||
| How hard to (Range 0-42) | 18.5 | (4.2) | 18.0 | (4.1) | .57 | |
| Coping upsets me (Range 12-36) | 18.0 | (3.7) | 17.0 | (3.1) | .26 | |
| Self-Efficacy- Diabetes (Range 24-120) | 88.1 | (13.2) | 91.0 | (13.5) | .35 | |
| Family | ||||||
| Guidance and Control (Range 15-75) | 47.7 | (6.4) | 46.4 | (6.0) | .38 | |
| Warmth and Caring (Range 15-75) | 57.7 | (8.1) | 61.4 | (6.8) | .05 | |
t-test analysis
Transformed by square-root transformation to satisfy normal distribution
CST = Coping Skills Training Group; GE = General Education Group; HbA1c = Hemoglobin A1c; QOL = quality of life; CDI = Children's Depressive Inventory
Intervention Efficacy
There were no significant differences between CST and GE groups over time on metabolic control, QOL, depressive symptoms, coping, self-efficacy or family functioning. Group effect sizes at 12 months indicated a small effect of CST on QOL Impact (ES = .32) and a small effect of GE on one coping subscale (Upsets, ES =.41). No significant effects of treatment were observed for metabolic control, self-efficacy, or family outcomes.
When rates of change over time were examined across both groups, the following outcomes indicated improvement: diabetes QOL Worry (p=.013), depression (p<.001), both coping scales (How Hard, p=.003; How Upsetting, p=.008), and self-efficacy (p<.001). These improvements were observed although children were taking on additional responsibility for their diabetes care as evidenced by a significant reduction over time in both groups in parental guidance and control (p<.001).
Moderators
Child age, sex, socioeconomic status (income), and treatment modality (insulin pump vs. injections) were included as interaction terms in the model to test for moderation. Children on a pump had lower HbA1c across all time points (p<.05) and there was a significant treatment group-by-modality–by-time interaction (p=.007). Nevertheless treatment group differences were not apparent at 6 and 12 months. Among children on the pump, there were no significant group by time interactions with HbA1c.
There was a significant difference between groups on the Warmth and Caring subscale of the DFBS and treatment modality. Children receiving injections reported a decrease in warmth and caring over time; children on a pump reported stable warmth and caring (p<.05). There was also a treatment group-by-treatment modality-by-time interaction (p=.004). Stratified analysis by modality revealed that at 6 months Warmth and Caring was not significantly higher in GE compared to CST among children using the pump (p=.07). Child age, sex, and socioeconomic status were not significant moderators of treatment effects on outcomes.
Mediators
Based on our conceptual model, coping, self-efficacy, and family functioning were tested as potential mediators of the intervention on QOL and metabolic control. Although we did not find significant effects of the intervention on these outcomes or the proposed mediators (Table 5), in line with Kraemer and colleagues (2002), we tested whether changes in the proposed mediators (i.e., difficulty coping, upset related to coping, self-efficacy for diabetes, family warmth/caring, and family guidance/control) were related to changes in outcomes (i.e. QOL impact, QOL worry, and HbA1c) across intervention groups. Correlation analyses revealed that 3-month increases in family warmth/caring were associated with lower 1-year changes in worry QOL (r = -.29, p = .02) and impact on QOL (r = -.42, p < .001). No significant correlations were observed between changes in self-efficacy, upset related to coping, or family guidance/control and any of the outcome variables. Further, none of the potential mediators were associated with change in HbA1c.
Table 5. One Year Changes in Outcomes Following Intervention*.
| Comparison of Treatment Groups Rate of Change per Year |
Analysis Combining Both Groups Rate of Change per Year† |
||||
|---|---|---|---|---|---|
| CST | GE | Group* Time (p) | Combined Groups | Time (p) | |
| HbA1c | .52 | .29 | .265 | .43 | .001 |
| Diabetes QOL | |||||
| Impact | -1.84 | -1.96 | .957 | -1.88 | .054 |
| Worry | -1.10 | .33 | .080 | -1.00 | .013 |
| Satisfaction | 1.72 | 1.00 | .758 | 1.46 | .188 |
| Depression – (√CDI) | -.47 | -.612 | .574 | -.52 | .001 |
| Coping | |||||
| How hard to | -1.46 | -1.58 | .911 | -1.51 | .002 |
| Coping upsets me | -1.01 | -1.62 | .448 | -1.19 | .006 |
| Self-Efficacy | |||||
| Diabetes | 5.98 | 5.93 | .984 | 5.95 | .001 |
| Family | |||||
| Guidance & Control | -2.17 | -2.39 | .867 | -2.24 | .001 |
| Warmth & Caring | .24 | -.16 | .821 | .10 | .906 |
Rates of change were estimated using a random effects regression model adjusted for child gender, median time between diagnosis and study entry, parental income and treatment modality; baseline outcome values were entered as fixed effects for the models of Diabetes QOL and Family
Estimated rate of change in the combined intervention groups corresponds to the fixed effect for time in random regression model excluding the group by time interaction.
CST = Coping Skills Training Group; GE = General Education Group; HbA1c = Hemoglobin A1c; QOL = quality of life; CDI = Children's Depressive Inventory
The change from baseline to 3 months post-intervention for each of the mediators also was entered into a mixed model predicting outcomes at 6 months and 12 months, after adjusting for baseline outcome, treatment modality, sex, income and group. Three-month changes in family warmth/caring significantly predicted QOL impact (B = -.26, p = .02); each 1 unit increase in family warmth/caring over 3-months was associated with a .26 reduction at 6 and 12 months for QOL impact. None of the other proposed mediators were significant predictors of outcomes in these adjusted analyses.
Discussion
The purpose of this study was to examine the efficacy of a group-based CST intervention for school-aged children with T1D and their parents compared to an attention control group (GE). The primary hypothesis, that children of the CST intervention would demonstrate better metabolic control, QOL, depressive symptoms, coping, self efficacy, and family functioning, was not supported.
The intention of this intervention was to provide a preventive intervention for school-aged children and their parents, prior to adolescence, when metabolic control typically worsens and psychosocial and family issues arise. The International Society for Pediatric and Adolescent Diabetes (ISPAD) clinical consensus guidelines advocate for preventive interventions for youth with T1D (Delamater, 2007). A considerable research challenge with a prevention intervention, however, is that improvement may be difficult to demonstrate in a population with good physiological and psychosocial adjustment, such as the current sample. However, equivalence or lack of decline over time may be equally important. School-aged children in this sample demonstrated excellent metabolic control and good psychosocial adjustment at baseline and across the intervention period. Recruitment yield for this sample of school-aged children was less than in previous studies with adolescents, and scheduling of the group sessions was more difficult, which may indicate that families were not experiencing significant challenges warranting participation in a psycho-educational intervention.
The lack of differential effects of CST may be due to the small sample size and significant time effects demonstrated in this study. Children who received either CST or GE reported significantly better QOL, fewer depressive symptoms, fewer issues in coping, less parental guidance and control over diabetes management, and better diabetes self-efficacy over time. Perceptions of family warmth remained stable over time. These are important findings, as increased psychosocial difficulties would be expected as children transition into adolescence, particularly with depressive symptoms and family functioning (Anderson, et al., 2002; Kovacs et al., 1997). Although further research is indicated, group-based interventions during pre-adolescence for both children and their parents may be warranted. It is possible that receiving T1D education in a group format at this developmental phase is equally as beneficial as CST, because there are considerable challenges to successful management of T1D in a maturing child such as the transfer of responsibility from a parent to a teen that may be addressed in an educational group setting. Providing education in a group context may also expose participants to peer-identified coping skills and peer social support. Indeed, anecdotal reports from parents and the study interventionist for the GE sessions indicated that a supportive group process occurred within the context of providing diabetes-specific education.
The lack of support for the proposed mediators of coping, self-efficacy, and family functioning on intervention efficacy could also be attributable to the small sample size and significant time effects without a differential intervention effect. Recent advocates for evaluating mediation effects in clinical trials recommend exploring mediation effects despite non-significant intervention effects, as such analysis could still identify mechanisms of change (Kraemer et al., 2002). Although exploratory in nature, results of this mediation analysis did not support coping or self-efficacy as mediators of change in metabolic control or QOL in this school-aged sample. However, across intervention groups, there was support for improvement in coping and family warmth/caring as mediators of improved QOL. It is possible that unmeasured factors such as social support which were present in both interventions, may influence metabolic control and psychosocial adjustment in school-aged children living with T1D. Previous research supports the beneficial effect of peer support, such as that experienced in the groups for parents and children with T1D (La Greca et al., 1995; Sullivan Bolyai et al., 2004).
Moderators considered in evaluating intervention efficacy in children with T1D included age, sex, and socioeconomic status as well as treatment modality (pump or injections). Only treatment modality moderated intervention efficacy, and only with certain outcomes (HbA1c, family warmth and caring). Children using the pump, regardless of group assignment, had better metabolic control and reported more family warmth and caring compared to children treated with multiple injections. Results of the moderation analysis indicated that children exposed to GE who were treated with injections had a greater increase in HbA1c at 3 months. Children exposed to GE who were treated with a pump had greater family warmth and caring at 6 months. Although previous research has demonstrated better metabolic control and QOL in children treated with a pump vs. injections (Doyle et al., 2004; Hilliard, Goeke-Morey, Cogen, Henderson, & Streisand, 2008; Nimri et al., 2006), more information is needed on the impact of treatment modality on family functioning.
It is important to note that the lack of variability in this sample in socioeconomic status also may have influenced results of this study. The sample was predominately of middle to upper income, reflective of the clinic population. Previous research supports considerable variation in metabolic control and psychosocial adjustment with differences in socioeconomic status. For example, youth with lower socioeconomic status have demonstrated poorer metabolic control, greater stress, and lower adherence compared to youth of higher socioeconomic status (Naar-King et al., 2006; Overstreet, Holmes, Dunlap, & Frentz, 1997). Future research with more diverse samples is indicated.
Findings of this study must also be interpreted in light of several limitations. In addition to the small sample of primarily white and upper socioeconomic status families and the fact that the majority of children demonstrated excellent metabolic control and good psychosocial adjustment at baseline, the majority also were using an insulin pump. This is not reflective of other studies of youth with T1D (Valenzuela et al., 2006), and may be because pump therapy is strongly encouraged at our clinic recruitment site. Also, several subscales (DFBS Guidance and Control, Coping How Upsetting) had low internal consistency reliability, leading to increased measurement variance. Lastly, inability to schedule groups in a substantial number of children that enrolled in the study may have also created a selection bias, in that participants who were able to be scheduled for groups may have been more motivated with overall better adjustment to T1D.
Despite these limitations and the primarily non-significant findings, there are several important clinical and research implications. School-aged children and their parents were successful in implementing intensive treatment of T1D as evidenced by excellent metabolic control. Although the children generally demonstrated good psychosocial adjustment, 11% reported elevated depressive symptoms at baseline. Thus, these findings highlight the importance of screening for depressive symptoms in school-aged children with T1D, as recommended by the American Diabetes Association (Silverstein et al., 2005).
Positive outcomes associated with the use of the insulin pump provide some evidence for the benefit of the pump modality as an option for school-aged children with T1D. In our sample, treatment type was a moderator of metabolic control on family warmth/caring, suggesting that children on the pump may have better family functioning in addition to better metabolic control. These findings may be a result of decreased need for parental reminders for children using insulin pumps.
Lastly, findings of this study also lend support to group-based psycho-educational interventions for school-aged children with T1D and parents. Children participating in both programs demonstrated improvements on important psychosocial outcomes, particularly in self-efficacy, coping, depressive symptoms, worry, and impact of diabetes on QOL. Perhaps the non-specific factor of social support (received by both groups) is one of the mediators of the treatment. Further research is indicated.
Conclusion
CST did not have the expected effect on child and family outcomes in this relatively well-adjusted sample of school-aged children with T1D. Both CST and GE improved psychosocial outcomes for children. A better understanding of the potential moderation of pump therapy in school-age children has been elucidated. Further research is indicated on preventive interventions with longer follow-up to capture the targeted transition to adolescence. In addition, future research is indicated to determine the intervention efficacy in children of more diverse race, ethnicity, and socioeconomic status; children with higher HbA1c levels; and children with more variable psychosocial adjustment and family functioning.
Acknowledgments
Supported by a grant from the National Institute for Nursing Research (National Institute of Health R01NR004009; PI: Margaret Grey, DrPH, RN, FAAN).
Contributor Information
Margaret Grey, Yale School of Nursing, New Haven, CT.
Robin Whittemore, Yale School of Nursing.
Sarah Jaser, Yale School of Nursing.
Jodie Ambrosino, Department of Pediatrics, Yale School of Medicine.
Evie Lindemann, Albertus Magnus College, New Haven, CT.
Lauren Liberti, Yale School of Nursing.
Veronika Northrup, Yale Center for Clinical Investigations, New Haven, CT.
James Dziura, Yale Center for Clinical Investigations, New Haven, CT.
References
- Ambrosino JM, Fennie K, Whittemore R, Jaser S, Dowd MF, Grey M. Short-term effects of coping skills training in school-age children with type 1 diabetes. Pediatric Diabetes. 2008;9:74–82. doi: 10.1111/j.1399-5448.2007.00356.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- American Diabetes Association. Standards of medical care in diabetes. Diabetes Care. 2005;28(Suppl 1):s4–s36. [PubMed] [Google Scholar]
- Anderson BJ, Auslander WF, Jung KC, Miller JP, Santiago JV. Assessing family sharing of diabetes responsibilities. Journal of Pediatric Psychology. 1990;15:477–492. doi: 10.1093/jpepsy/15.4.477. [DOI] [PubMed] [Google Scholar]
- Anderson BJ, Brackett J, Ho J, Laffel LM. An office-based intervention to maintain parent-adolescent teamwork in diabetes management. Impact on parent involvement, family conflict, and subsequent glycemic control. Diabetes Care. 1999;22:713–721. doi: 10.2337/diacare.22.5.713. [DOI] [PubMed] [Google Scholar]
- Anderson BJ, Ho J, Brackett J, Finkelstein D, Laffel LM. Parental involvement in diabetes management tasks: Relationships to blood glucose monitoring adherence and metabolic control in young adolescents with insulin-dependent diabetes mellitus. Journal of Pediatrics. 1997;130:257–265. doi: 10.1016/s0022-3476(97)70352-4. [DOI] [PubMed] [Google Scholar]
- Anderson BJ, Vangsness L, Connell A, Butler D, Goebel-Fabbri A, Laffel LMB. Family conflict, adherence, and glycaemic control in youth with short duration Type 1 diabetes. Diabetic Medicine. 2002;19:635–642. doi: 10.1046/j.1464-5491.2002.00752.x. [DOI] [PubMed] [Google Scholar]
- Bandura A. The anatomy of stages of change. American Journal of Health Promotion. 1997;12:8–10. doi: 10.4278/0890-1171-12.1.8. [DOI] [PubMed] [Google Scholar]
- Berg CA, Wiebe DJ, Beveridge RM, Palmer DL, Korbel CD, Upchurch R, et al. Mother child appraisal involvement in coping with diabetes stressors and emotional adjustment. Journal of Pediatric Psychology. 2007;32:995–1005. doi: 10.1093/jpepsy/jsm043. [DOI] [PubMed] [Google Scholar]
- Cameron FJ, Skinner TC, de Beaufort CE, Hoey H, Swift PG, Aanstoot H, et al. Are family factors universally related to metabolic outcomes in adolescents with Type 1 Diabetes? Diabetes Medicine. 2008;25:463–468. doi: 10.1111/j.1464-5491.2008.02399.x. [DOI] [PubMed] [Google Scholar]
- Davidson M, Boland EA, Grey M. Teaching teens to cope: Coping skills training for adolescents with insulin-dependent diabetes mellitus. Journal of the Society of Pediatric Nurses. 1997;2:65–72. doi: 10.1111/j.1744-6155.1997.tb00062.x. [DOI] [PubMed] [Google Scholar]
- Davis CL, Delamater AM, Shaw KH, La Greca AM, Eidson MS, Perez-Rodriguez JE, et al. Parenting styles, regimen adherence, and glycemic control in 4- to 10-year-old children with diabetes. Journal of Pediatric Psychology. 2001;26:123–129. doi: 10.1093/jpepsy/26.2.123. [DOI] [PubMed] [Google Scholar]
- Delamater AM. Psychological care of children and adolescents with type 1 diabetes. Pediatric Diabetes. 2007;8:340–348. doi: 10.1111/j.1399-5448.2007.00318.x. [DOI] [PubMed] [Google Scholar]
- Diabetes Control and Complications Trial Research Group. Effect of intensive insulin treatment on the development and progression of long-term complications in adolescents with insulin-dependent diabetes mellitus: Diabetes Control and Complications Trial. Journal of Pediatrics. 1994;125:177–188. doi: 10.1016/s0022-3476(94)70190-3. [DOI] [PubMed] [Google Scholar]
- Doyle EA, Weinzimer SA, Steffen AT, Ahern JA, Vincent M, Tamborlane WV. A randomized, prospective trial comparing the efficacy of continuous insulin infusion with multiple daily injections using insulin glargine. Diabetes Care. 2004;27:1554–1558. doi: 10.2337/diacare.27.7.1554. [DOI] [PubMed] [Google Scholar]
- Elastoff JD. nQuery Advisor (Version 1.0) Boston: Statistical Solutions; 1995. [Google Scholar]
- Ellis DA, Yopp J, Templin T, Naar-King S, Frey MA, Cunningham PB, et al. Family mediators and moderators of treatment outcomes among youths with poorly controlled type 1 diabetes: Results from a randomized controlled trial. Journal of Pediatric Psychology. 2007;32:194–205. doi: 10.1093/jpepsy/jsj116. [DOI] [PubMed] [Google Scholar]
- Faulkner MS, Chang LI. Family influence on self-care, quality of life, and metabolic control in school-age children and adolescents with type 1 diabetes. Journal of Pediatric Nursing. 2007;22:59–68. doi: 10.1016/j.pedn.2006.02.008. [DOI] [PubMed] [Google Scholar]
- Fisher L, Dixon D, Herson J, Frankowski RK, Hearron MS, Peace KE. Intention to treat in clinical trials. In: Peace K, editor. Statistical issues in drug research and development. New York: Marcel Dekker; 1990. pp. 331–349. [Google Scholar]
- Forman SG. Coping skills interventions for children and adolescents. San Francisco: Jossey-Bass; 1993. [Google Scholar]
- Graue M, Wentzel-Larsen T, Bru E, Hanestad BR, Sovik O. The coping styles of adolescents with type 1 diabetes are associated with degree of metabolic control. Diabetes Care. 2004;27:1313–1317. doi: 10.2337/diacare.27.6.1313. [DOI] [PubMed] [Google Scholar]
- Grey M, Boland EA, Davidson M, Tamborlane WV. Clinical and psychosocial factors associated with achievement of treatment goals in adolescents with diabetes. Journal of Adolescent Health. 2001;28:377–385. doi: 10.1016/s1054-139x(00)00211-1. [DOI] [PubMed] [Google Scholar]
- Grey M, Boland EA, Davidson M, Yu C, Tamborlane WV. Coping skills training for youths with diabetes on intensive therapy. Applied Nursing Research. 1999;12:3–12. doi: 10.1016/s0897-1897(99)80123-2. [DOI] [PubMed] [Google Scholar]
- Grey M, Boland EA, Davidson M, Li J, Tamborlane WV. Coping skills training for youth with diabetes mellitus has long-lasting effects on metabolic control and quality of life. Journal of Pediatrics. 2000;137:107–113. doi: 10.1067/mpd.2000.106568. [DOI] [PubMed] [Google Scholar]
- Grey M, Lipman T, Cameron ME, Thurber FW. Coping behaviors at diagnosis and in adjustment one year later in children with diabetes. Nursing Research. 1997;46:312–317. doi: 10.1097/00006199-199711000-00003. [DOI] [PubMed] [Google Scholar]
- Grey M, Thurber FW. Adaptation to chronic illness in childhood: Diabetes mellitus. Journal of Pediatric Nursing. 1991;6:302–309. [PubMed] [Google Scholar]
- Griva K, Myers LB, Newman S. Illness perceptions and self efficacy beliefs in adolescents and young adults with insulin dependent diabetes mellitus. Psychology & Health. 2000;15:733–750. [Google Scholar]
- Grossman HY, Brink S, Hauser ST. Self-efficacy in adolescent girls and boys with insulin-dependent diabetes mellitus. Diabetes Care. 1987;10:324–329. doi: 10.2337/diacare.10.3.324. [DOI] [PubMed] [Google Scholar]
- Hilliard ME, Goeke-Morey M, Cogen FR, Henderson C, Streisand R. Predictors of diabetes-related quality of life after transitioning to the insulin pump. Journal of Pediatric Psychology. 2008;62:1–10. doi: 10.1093/jpepsy/jsn062. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hollis S, Campbell F. What is meant by intention to treat analysis? Survey of published randomised controlled trials. British Medical Journal. 1999;319:670–674. doi: 10.1136/bmj.319.7211.670. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Holmes CS, Chen R, Streisand R, Marschall DE, Souter S, Swift EE, et al. Predictors of youth diabetes care behaviors and metabolic control: A structural equation modeling approach. Journal of Pediatric Psychology. 2006;31:770–784. doi: 10.1093/jpepsy/jsj083. [DOI] [PubMed] [Google Scholar]
- Hood KK, Huestis S, Maher A, Butler D, Volkening L, Laffel LM. Depressive symptoms in children and adolescents with type 1 diabetes: Association with diabetes-specific characteristics. Diabetes Care. 2006;29:1389–1391. doi: 10.2337/dc06-0087. [DOI] [PubMed] [Google Scholar]
- Ingersoll GM, Marrero DG. A modified Quality of Life Measure for youths: Psychometric properties. The Diabetes Educator. 1991;17:114–118. doi: 10.1177/014572179101700219. [DOI] [PubMed] [Google Scholar]
- Kokkonen J, Lautala P, Salmela P. The state of young adults with juvenile onset diabetes. International Journal of Circumpolar Health. 1997;56:76–85. [PubMed] [Google Scholar]
- Kovacs M. The Children's Depression Inventory (CDI) Psychopharmacology Bulletin. 1985;21:995–998. [PubMed] [Google Scholar]
- Kovacs M, Brent D, Feinberg TF, Paulauskas S, Reid J. Children's self-reports of psychologic adjustment and coping strategies during the first year of insulin-dependent diabetes mellitus. Diabetes Care. 1986;9:472–479. doi: 10.2337/diacare.9.5.472. [DOI] [PubMed] [Google Scholar]
- Kovacs M, Goldston D, Obrosky DS, Bonar LK. Psychiatric disorders in youth with IDDM: Rates and risk factors. Diabetes Care. 1997;20:36–44. doi: 10.2337/diacare.20.1.36. [DOI] [PubMed] [Google Scholar]
- Kovacs M, Iyengar S, Goldston D, Stewart J, Obrosky DS, Marsh J. Psychological functioning of children with insulin-dependent diabetes mellitus: A longitudinal study. Journal of Pediatric Psychology. 1990;15:619–632. doi: 10.1093/jpepsy/15.5.619. [DOI] [PubMed] [Google Scholar]
- Kraemer HC, Wilson GT, Fairburn CG, Agras WS. Mediators and moderators of treatment effects in randomized clinical trials. Archives of General Psychiatry. 2002;59:877–883. doi: 10.1001/archpsyc.59.10.877. [DOI] [PubMed] [Google Scholar]
- La Greca AM, Auslander WF, Greco P, Spetter D, Fisher EB, Santiago JV. I get by with a little help from my family and friends: Adolescents' support for diabetes care. Journal of Pediatric Psychology. 1995;20:449–476. doi: 10.1093/jpepsy/20.4.449. [DOI] [PubMed] [Google Scholar]
- Laffel LMB, Connell A, Vangness L, Goebel-Fabbri A, Mansfield A, Anderson BJ. General quality of life in youth with Type 1 Diabetes: Relationship to patient management and diabetes-specific family conflict. Diabetes Care. 2003;26:3067–3073. doi: 10.2337/diacare.26.11.3067. [DOI] [PubMed] [Google Scholar]
- Marlott GA, Gordon JR. Relapse prevention: Maintenance strategies in addictive behavior change. New York: Guilford; 1985. [Google Scholar]
- McKelvey J, Waller DA, North AJ, Marks J, Schreiner B, Travis L, et al. Reliability and validity of the Diabetes Family Behavior Scale. The Diabetes Educator. 1993;19:125–132. doi: 10.1177/014572179301900206. [DOI] [PubMed] [Google Scholar]
- Naar-King S, Idalski A, Ellis D, Frey M, Templin T, Cunningham PB, et al. Gender differences in adherence and metabolic control in urban youth with poorly controlled type 1 diabetes: The mediating role of mental health symptoms. Journal of Pediatric Psychology. 2006;31:793–802. doi: 10.1093/jpepsy/jsj090. [DOI] [PubMed] [Google Scholar]
- National Institute of Diabetes and Digestive and Kidney Diseases. Diabetes in America. Bethesda, MD: 2002. NIH publication No 02-3892. [Google Scholar]
- National Institute of Diabetes and Digestive and Kidney Diseases. National Diabetes Statistics. Deaths among people with diabetes, United States, 2006. 2007 Retrieved January 19, 2009 from http://diabetes.niddk.nih.gov/dm/pubs/statistics/index.htm.
- Nimri R, Weintrob N, Benzaquen H, Ofan R, Fayman G, Phillip M. Insulin pump therapy in youth with type 1 diabetes: A retrospective paired study. Pediatrics. 2006;117:2126–2131. doi: 10.1542/peds.2005-2621. [DOI] [PubMed] [Google Scholar]
- Overstreet S, Holmes CS, Dunlap WP, Frentz J. Sociodemographic risk factors to disease control in children with diabetes. Diabetic Medicine. 1997;14:153–157. doi: 10.1002/(SICI)1096-9136(199702)14:2<153::AID-DIA318>3.0.CO;2-K. [DOI] [PubMed] [Google Scholar]
- Pendley JS, Kasmen LJ, Miller DL, Donze J, Swenson C, Reeves G. Peer and family support in children and adolescents with type 1 diabetes. Journal of Pediatric Psychology. 2002;27:429–438. doi: 10.1093/jpepsy/27.5.429. [DOI] [PubMed] [Google Scholar]
- Pollack SE. Adaptation to chronic illness: A program of research for testing nursing theory. Nursing Science Quarterly. 1993;6:86–92. doi: 10.1177/089431849300600208. [DOI] [PubMed] [Google Scholar]
- Rubin DB. Inference and missing data. Biometrika. 1976;63:581–592. [Google Scholar]
- Schilling LS, Knafl KA, Grey M. Changing patterns of self-management in youth with type I diabetes. Journal of Pediatric Nursing. 2006;21:412–424. doi: 10.1016/j.pedn.2006.01.034. [DOI] [PubMed] [Google Scholar]
- Silverstein JH, Klingensmith G, Copeland K, Plotnick L, Kaufman F, Laffel LMB, et al. Care of children and adolescents with type 1 diabetes. Diabetes Care. 2005;28:184–212. doi: 10.2337/diacare.28.1.186. [DOI] [PubMed] [Google Scholar]
- Smucker MR, Craighead WE, Craighead LW, Green BJ. Normative and reliability data for the Children's Depression Inventory. Journal of Abnormal Child Psychology. 1986;14:25–29. doi: 10.1007/BF00917219. [DOI] [PubMed] [Google Scholar]
- Sullivan-Bolyai S, Grey M, Deatrick J, Gruppuso P, Giraritis P, Tamborlane W. Helping other mothers effectively work at raising young children with type 1 diabetes. Diabetes Educator. 2004;30:476–484. doi: 10.1177/014572170403000319. [DOI] [PubMed] [Google Scholar]
- Travis LB, Brouhard BH, Schreiner BJ. Diabetes mellitus in children and adolescents. Philadelphia: W. B. Saunders; 1987. [Google Scholar]
- Valenzuela JM, Patino AM, McCullough J, Ring C, Sanchez J, Eidson M, et al. Insulin pump therapy and health-related quality of life in children and adolescents with type 1 diabetes. Journal of Pediatric Psychology. 2006;31:650–660. doi: 10.1093/jpepsy/jsj088. [DOI] [PubMed] [Google Scholar]
- Weinger K, O'Donnell KA, Ritholz MD. Adolescent views of diabetes-related parent conflict and support: a focus group analysis. Journal of Adolescent Health. 2001;29:330–336. doi: 10.1016/s1054-139x(01)00270-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Whittemore R, Kanner S, Grey M. The influence of family on physiological and psychosocial health in youth with type 1 diabetes: A systematic review. In: Melnyk B, Fineout-Overholt E, editors. Evidence-based practice in nursing and healthcare: A guide to best practice. Philadelphia: Lippincott Williams & Wilkins; 2004. pp. CD 22-73–CD 22-87. [Google Scholar]
- Whittemore R, Kanner S, Singleton S, Hamrin V, Chiu J, Grey M. Correlates of depressive symptoms in adolescents with type 1 diabetes. Pediatric Diabetes. 2002;3:135–143. doi: 10.1034/j.1399-5448.2002.30303.x. [DOI] [PubMed] [Google Scholar]
- Wysocki T. Associations among teen-parent relationships, metabolic control, and adjustment to diabetes in adolescents. Journal of Pediatric Psychology. 1993;18:441–452. doi: 10.1093/jpepsy/18.4.441. [DOI] [PubMed] [Google Scholar]
- Wysocki T, Harris MA, Buckloh LM, Mertlich D, Lochrie AS, Taylor A, et al. Randomized, controlled trial of behavioral family systems therapy for diabetes: Maintenance and generalization of effects on parent-adolescent communication. Behavior Therapy. 2008;39:33–46. doi: 10.1016/j.beth.2007.04.001. [DOI] [PubMed] [Google Scholar]