Abstract
Background and objectives: The Chronic Renal Insufficiency Cohort (CRIC) Study was established to examine risk factors for the progression of chronic kidney disease (CKD) and cardiovascular disease (CVD) in patients with CKD. We examined baseline demographic and clinical characteristics.
Design, setting, participants, & measurements: Seven clinical centers recruited adults who were aged 21 to 74 yr and had CKD using age-based estimated GFR (eGFR) inclusion criteria. At baseline, blood and urine specimens were collected and information regarding health behaviors, diet, quality of life, and functional status was obtained. GFR was measured using radiolabeled iothalamate in one third of participants.
Results: A total of 3612 participants were enrolled with mean age ± SD of 58.2 ± 11.0 yr; 46% were women, and 47% had diabetes. Overall, 45% were non-Hispanic white, 46% were non-Hispanic black, and 5% were Hispanic. Eighty-six percent reported hypertension, 22% coronary disease, and 10% heart failure. Mean body mass index was 32.1 ± 7.9 kg/m2, and 47% had a BP >130/80 mmHg. Mean eGFR was 43.4 ± 13.5 ml/min per 1.73 m2, and median (interquartile range) protein excretion was 0.17 g/24 h (0.07 to 0.81 g/24 h). Lower eGFR was associated with older age, lower socioeconomic and educational level, cigarette smoking, self-reported CVD, peripheral arterial disease, and elevated BP.
Conclusions: Lower level of eGFR was associated with a greater burden of CVD as well as lower socioeconomic and educational status. Long-term follow-up of participants will provide critical insights into the epidemiology of CKD and its relationship to adverse outcomes.
The prevalence of ESRD that requires renal replacement therapy has risen dramatically in the United States during the past three decades (1). Non–dialysis-requiring chronic kidney disease (CKD) is substantially more common than ESRD, with an estimated 15 million adults in the United States having CKD of stage 3 or worse (as defined by an estimated GFR [eGFR] of <60 ml/min per 1.73 m2) (2) Furthermore, CKD frequently progresses in severity, but the factors that are responsible for accelerated decline need further elucidation. In addition, recent studies have highlighted an important association between even mild CKD and increased risk for cardiovascular disease (CVD) (3), but the mechanisms for this association remain unclear.
In response to the epidemic of CKD and our incomplete understanding of factors that govern its progression and associated morbidity, the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) established the Chronic Renal Insufficiency Cohort (CRIC) Study in 2001. The broad aims of the CRIC Study are to examine risk factors for the progression of kidney disease and CVD in patients with CKD and to develop predictive models to identify high-risk subgroups. The design and methods of the CRIC Study have been previously reported (4). In this article, we characterize the eligibility and recruitment methods, describe the baseline characteristics of patients enrolled in the cohort, and report initial analyses of correlates of level of eGFR.
Materials and Methods
Study Organization
The CRIC Study consists of a Scientific and Data Coordinating Center; seven clinical centers, central laboratories, and reading centers; a Scientific Advisory Committee; and NIDDK project scientists as described previously (4). The study protocol was approved by institutional review boards at participating institutions, and the research was conducted in accordance with the ethical principles of the Declaration of Helsinki.
Study Design
The CRIC Study was designed as a prospective cohort of approximately 3600 participants who were enrolled through seven clinical centers. A weighted random sample of approximately one third of the cohort (referred to as the subcohort) was assigned to undergo additional, more intensive testing (including iothalamate clearance studies to measure GFR and electron-beam tomography) that would also facilitate use of nested case-cohort substudies (4). CRIC participants are followed until death or withdrawal of informed consent. Follow-up continues even after ESRD occurs with initiation of chronic dialysis or receipt of a kidney transplant. Outcomes regarding progression of kidney dysfunction will focus principally on reductions in GFR as well as the occurrence of clinically relevant declines in renal function. Evaluation of subclinical CVD is assessed annually (via standard 12-lead electrocardiography and measurements of ankle-brachial index [ABI]), and transthoracic echocardiography is performed at years 1 and 4 of follow-up for all participants. Coronary artery calcium burden assessment using electron-beam tomography or multidetector computed tomography will be performed in the subcohort at years 1 and 4. Clinical cardiovascular outcomes (including acute myocardial infarction, heart failure, arrhythmias, stroke, and peripheral arterial disease [PAD]) will be ascertained every 6 mo during follow-up, and relevant medical records will be centrally adjudicated. Hypertension at entry was defined as either systolic BP ≥140 mmHg, diastolic BP ≥90 mmHg, or use of antihypertensive medications (5). Diabetes was defined as either fasting glucose ≥126 mg/dl, random glucose ≥200 mg/dl, or use of insulin or antidiabetic medication (6).
Study Population and Recruitment
Eligibility criteria.
The CRIC Study was designed to include a racially and ethnically diverse group of adult patients who were aged 21 to 74 yr and had mild to moderate CKD and approximately half of whom had diabetes (Table 1). The age and eGFR criteria were specifically designed to facilitate evaluation of the progression and implications of CKD across a wide spectrum of mild to moderate kidney dysfunction and age. Age-based eGFR entry criteria were established to limit the proportion of older individuals who were recruited with age-related diminutions of GFR but otherwise nonprogressive CKD. The level of eGFR used to define eligibility was based on the four-variable Modification of Diet in Renal Disease (MDRD) estimating equation (7), using locally measured serum creatinine calibrated to the Cleveland Clinic laboratory (8).
Table 1.
Sequence and schedule of CRIC Study clinic visits/contacts and proceduresa
| Parameter | Visit |
|||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Screening | Baseline | 6 mo | 12 mo | 18 mo | 24 mo | 30 mo | 36 mo | 42 mo | 48 mo | 54 mo | 60 mo | |
| Type of contact | Visit | Visit | Phone | Visit | Phone | Visit | Phone | Visit | Phone | Visit | Phone | Visit |
| Informed consent | • | |||||||||||
| Medical record consent | • | • | • | • | ||||||||
| Contact information | • | • | • | • | • | • | • | • | • | • | • | • |
| Labs: creatinine, glucose | • | |||||||||||
| Demographic information | • | |||||||||||
| Eligibility confirmation | • | |||||||||||
| Medical history | • | • | • | • | • | • | ||||||
| Genetic blood sample | • | • | • | • | • | • | ||||||
| Labs: CBC, metabolic panel, lipids | • | • | • | • | • | • | ||||||
| 24-h urine | • | • | • | • | • | • | ||||||
| BP | • | • | • | • | • | • | ||||||
| Anthropometric measures | • | • | • | • | • | • | ||||||
| Ankle brachial index | • | • | • | • | • | • | ||||||
| Bioelectric impedance assessment | • | • | • | • | • | • | ||||||
| Nail clippings | • | • | • | • | • | • | ||||||
| Electrocardiogram | • | • | • | • | • | • | ||||||
| Echocardiogram | • | • | ||||||||||
| EBT or MDCT (one third subcohort) | • | • | ||||||||||
| Iothalamate-GFR (one third subcohort) | • | • | • | |||||||||
| Pulse wave velocity | • | • | ||||||||||
| Physical assessment | • | • | • | |||||||||
| Medications | • | • | • | • | • | • | • | |||||
| KDQOL quality of life (43) | • | • | • | • | • | • | ||||||
| Diet History Questionnaire (44) | • | • | • | |||||||||
| Mini Mental Status Exam (45) | • | • | • | |||||||||
| MDRD Symptom Index (46) | • | • | • | • | • | • | ||||||
| Beck Depression Inventory (47) | • | • | • | |||||||||
| Physical Activity (48,49) | • | • | • | |||||||||
| Kansas City Questionnaire (50) | • | • | • | • | • | |||||||
| Recent medical history | • | • | • | • | • | • | • | • | • | • | • | |
CBC, complete blood count; CRIC, Chronic Renal Insufficiency Cohort; EBT, electron-beam tomography; MDCT, multidetector computed tomography; MDRD, Modification of Diet in Renal Disease; KDQOL, Kidney Disease Quality of Life.
Exclusion criteria.
Selected exclusion criteria were implemented (Table 2). Patients with polycystic kidney disease were excluded because of its distinct pathophysiology and its exclusive focus by another ongoing NIDDK-sponsored study (9). Patients with additional primary renal diseases were excluded when active immunosuppression had been used within 6 mo of enrollment. Patients with significant coexisting illnesses were also excluded, as detailed in Table 2.
Table 2.
Eligibility and exclusion criteria
| Eligibility criteria |
| Age stratum (yr)/eligible eGFR range (ml/min per 1.73 m2)a |
| 21 to 44/20 to 70 |
| 45 to 64/20 to 60 |
| 65 to 74/20 to 50 |
| Exclusion criteria |
| institutionalized (e.g., prisoner, nursing home or skilled nursing facility resident) |
| unable or unwilling to give consent |
| unlikely or unable to participate in required study procedures |
| New York Heart Association class III or IV heart failure (baseline) |
| known cirrhosis |
| known HIV infection and/or AIDS |
| pregnant women |
| previously received dialysis for {my]1 mo |
| previous organ or bone marrow transplant |
| received immunosuppressive or other immunotherapy for primary renal disease or systemic vasculitis within the past 6 mo |
| previous chemotherapy or alkylating agents for systemic cancer other than non-melanoma skin cancer within 2 yr |
| previous diagnosis of multiple myeloma or renal carcinoma |
| polycystic kidney disease |
| current participation in interventional clinical trial or in a research study |
Based on simplified Modification of Diet in Renal Disease (MDRD) equation.
Recruitment.
The initial protocol called for each of the seven clinical centers to enroll approximately 450 participants each during a 33-mo period (May 2003 through March 2006). In August 2005, after Hurricane Katrina, enrollment at Tulane was halted after 405 participants had been enrolled. Consequently, the recruitment period was extended and recruitment targets at the other six clinical centers were increased. Study enrollment was completed on March 31, 2007. Recruitment strategies varied from center to center and included computerized searches of laboratory databases and hand searches of medical records and referrals from health care providers.
Screening, Enrollment, Follow-up, and Study Data Collection
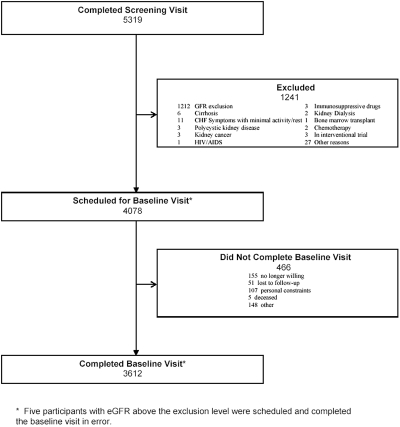
A total of 5319 participants completed screening visits, at which time consent was obtained and eligibility was determined (Figure 1, Table 1). Of those screened, 4073 were found to be eligible and 3612 completed a baseline visit, defining membership in the cohort. Five individuals with an eGFR above the exclusion level completed the baseline visit in error and are included in our analyses. At the baseline visit, sociodemographic characteristics, medical history, lifestyle behaviors, and current medications were recorded. Standardized BP measurements were obtained using a previously validated protocol (10). Anthropometric measures (height, weight, and mid-abdominal waist circumference) were obtained, and body composition was assessed using bioelectrical impedance analysis techniques. ABI was measured using standard methods (11). A 12-lead electrocardiogram was obtained using standardized methods (12). GFR was assessed by the renal clearance of 125-iodine iothalamate (13) in the subcohort. As detailed in Table 1, a series of questionnaires were administered regarding quality of life, diet, cognitive function, depressive symptoms, and physical activity level. Plasma, urine, and nail samples were collected for initial study measures, and aliquots were also stored for future studies. Additional details regarding visit and contact schedule are provided in Table 1.
Figure 1.
Particpant recruitment and follow-up flow diagram. *Five participants with estimated GFR above the exclusion level were scheduled and completed the baseline visit in error.
Statistical Analysis
The analytical plan for the CRIC Study has been previously described (4). Baseline characteristics are described using means with SD or medians and interquartile ranges for continuous variables, and frequency distribution is described with percentages for categorical variables. Missing values occurred when a participant failed to answer a question on a case report form or when a physical measure was not obtained or a laboratory test was not performed. The analysis for each variable is based on the observed values only. Baseline characteristics are compared between groups using t tests, ANOVA, or χ2 tests, as appropriate. A two-sided P ≤ 0.05 was considered statistically significant.
Results
Baseline Demographic and Clinical Characteristics of Participants
The final enrolled cohort has a mean ± SD age of 58.2 ± 11.0 yr with excellent representation of women (46%) and patients with diabetes (47%), consistent with the targeted enrollment goals (Table 3). The cohort is racially and ethnically diverse with 1638 (45%) non-Hispanic white patients, 1651 (46%) non-Hispanic black/African American patients, 169 (5%) Hispanic patients, and 154 (4%) Asian/Pacific Islander/Native American patients. Approximately 33% of the cohort had completed a college education, and 28% had annual incomes <$20,000 (US). Nearly 90% of the cohort had a history of hypertension. Fewer than 25% of the cohort had a self-reported history of coronary disease or PAD. Although the mean systolic and diastolic BPs were approximately 128 mmHg and approximately 71 mmHg, respectively, 47% of participants had a baseline BP >130/80 mmHg at entry. Mean body mass index (BMI) was elevated at 32.1 ± 7.9 kg/m2 with more than one half of all participants having a BMI >30 kg/m2. Mean eGFR for the entire cohort was 43.4 ± 13.5 ml/min per 1.73 m2, and median (IQR) proteinuria was 0.17 g per 24 h (0.07 to 0.81 g per 24 h). Almost 70% of the cohort was taking an angiotensin-converting enzyme inhibitor or an angiotensin receptor blocker. Most participants had an eGFR consistent with National Kidney Foundation's stages 3 and 4 CKD (70 and 18%, respectively) (14).
Table 3.
Baseline demographic and clinical characteristics of participantsa
| Variable | Cohort(n = 3612) | Subcohort with iGFR (n = 1288) | Diabetes(n = 1683) | No Diabetes(n = 1929) | P for Diabetes versus No Diabetes |
|---|---|---|---|---|---|
| Age (yr; mean ± SD) | 58.2 ± 11.0 | 56.1 ± 12.5 | 59.5 ± 9.8 | 57.1 ± 11.8 | 0.0001 |
| Gender (n [%]) | 0.2516 | ||||
| male | 1959 (54) | 713 (55) | 931 (55) | 1028 (53) | |
| female | 1653 (46) | 575 (45) | 754 (45) | 899 (47) | |
| Racial/ethnic group (n [%]) | 0.0001 | ||||
| non-Hispanic white | 1638 (45) | 713 (46) | 931 (39) | 1028 (51) | 0.2516 |
| non-Hispanic black/African American | 1651 (46) | 532 (41) | 849 (50) | 802 (42) | |
| Hispanic | 169 (5) | 69 (5) | 111 (7) | 58 (3) | |
| otherb | 154 (4) | 99 (8) | 76 (5) | 78 (4) | 0.0001 |
| Annual household income (n [%]) | 0.0001 | ||||
| ≤$20,000 | 1009 (28) | 297 (23) | 565 (34) | 444 (23) | |
| $20,001 to $50,000 | 906 (25) | 338 (26) | 432 (26) | 474 (24) | |
| $50,001 to $100,000 | 725 (20) | 306 (24) | 281 (17) | 444 (23) | |
| >$100,000 | 389 (11) | 153 (12) | 134 (8) | 255 (13) | |
| no response | 583 (16) | 193 (15) | 271 (16) | 312 (16) | |
| Educational attainment (n [%]) | 0.0001 | ||||
| <7th grade | 60 (2) | 16 (1) | 41 (2) | 19 (1) | |
| 7th to 12th grade | 545 (15) | 153 (12) | 319 (19) | 226 (12) | |
| high school diploma | 695 (19) | 239 (19) | 339 (20) | 356 (18) | |
| vocational degree | 184 (5) | 64 (5) | 98 (6) | 86 (4) | |
| some college | 921 (26) | 319 (25) | 440 (26) | 481 (25) | |
| college graduate | 696 (19) | 298 (23) | 281 (17) | 415 (22) | |
| graduate degree | 510 (14) | 198 (15) | 167 (10) | 343 (18) | |
| Tobacco use (n [%]) | |||||
| current smoker | 494 (14) | 151 (12) | 212 (13) | 282 (15) | 0.0733 |
| >100 cigarettes during lifetime | 2019 (56) | 667 (52) | 983 (58) | 1036 (54) | 0.0057 |
| Medical history (n [%]) | |||||
| hypertension | 3094 (86) | 1091 (85) | 1552 (92) | 1542 (80) | 0.0001 |
| MI or coronary revascularization | 810 (22) | 225 (17) | 493 (29) | 317 (17) | 0.0001 |
| chronic heart failure | 357 (10) | 86 (7) | 245 (15) | 112 (6) | 0.0001 |
| PAD | 250 (7) | 80 (6) | 181 (11) | 69 (4) | 0.0001 |
| BP variables | |||||
| SBP (mmHg; mean ± SD) | 127.7 ± 21.9 | 127.8 ± 21.3 | 132.4 ± 22.5 | 123.6 ± 20.5 | 0.0001 |
| DBP (mmHg; mean ± SD) | 71.4 ± 12.8 | 72.4 ± 12.7 | 69.4 ± 12.9 | 73.1 ± 12.8 | 0.0001 |
| MAP (mmHg; mean ± SD) | 90.2 ± 13.8 | 90.9 ±13.2 | 90.4 ± 13.9 | 89.9 ± 13.6 | 0.3113 |
| BP >130/80 mmHg (n [%]) | 1686 (47) | 626 (49) | 882 (53) | 804 (42) | 0.0001 |
| Weight (kg; mean ± SD) | 92.0 ± 23.7 | 89.9 ± 21.2 | 97.7 ± 24.2 | 87.1 ± 22.1 | 0.0001 |
| BMI (kg/m2; mean ± SD) | 32.1 ± 7.9 | 31.3 ± 7.0 | 34.1 ± 8.2 | 30.3 ± 7.2 | 0.0001 |
| BMI (kg/m2; n [%]) | 0.0001 | ||||
| <25.0 | 607 (17) | 234 (18) | 179 (11) | 428 (22) | |
| 25.0 to 29.9 | 1017 (28) | 380 (30) | 388 (23) | 629 (33) | 0.0001 |
| >30.0 | 1987 (55) | 673 (52) | 1118 (67) | 869 (45) | |
| ABI<0.9 (n [%]) | 526 (15) | 173 (14) | 335 (20) | 191 (10) | 0.0001 |
| Kidney function measures | |||||
| adjusted serum creatinine(mg/dl; mean ± SD) | 1.73 ± 0.57 | 1.68 ± 0.56 | 1.80 ± 0.56 | 1.66 ± 0.56 | 0.0001 |
| eGFR (ml/min/1.73 m2; mean ± SD) | 43.4 ± 13.5 | 45.2 ± 14.1 | 41.4 ± 12.9 | 45.1 ± 13.8 | 0.0001 |
| eGFR (ml/min/1.73 m2; n [%]) | |||||
| <15 | 3 (0) | 2 (0) | 1 (0) | 2 (0) | 0.0001 |
| 15 to 29 | 664 (18) | 206 (16) | 351 (21) | 313 (16) | |
| 30 to 59 | 2532 (70) | 887 (69) | 1197 (71) | 1335 (70) | |
| 60 to 89 | 389 (11) | 187 (15) | 126 (8) | 263 (14) | |
| >90 | 8 (0) | 4 (0) | 4 (0) | 4 (0) | |
| urine protein/24 h (g; median (IQR) | 0.17 (0.07 to 0.81) | 0.18 (0.07 to 0.90) | 0.32 (0.09 to 1.49) | 0.11 (0.06 to 0.43) | 0.0001 |
| ACEI or ARB therapy (n [%]) | 2462 (68) | 880 (68) | 1336 (79) | 1126 (58) | 0.0001 |
| Lipoproteins (mg/dl; mean ± SD) | |||||
| total cholesterol | 183.0 ± 44.5 | 183.8 ± 47.1 | 177.0 ± 47.2 | 188.2 ± 41.3 | 0.0001 |
| LDL cholesterol | 102.5 ± 35.0 | 103.4 ± 36.6 | 96.4 ± 36.4 | 107.8 ± 33.7 | 0.0001 |
| HDL cholesterol | 48.1 ± 15.6 | 47.5 ± 15.7 | 45.7 ± 13.9 | 50.2 ± 16.8 | 0.0001 |
| triglycerides | 154.2 ± 115.6 | 152.2 ± 112.5 | 166.2 ± 130.3 | 143.6 ± 99.8 | 0.0001 |
| Hemoglobin (g/dl; mean ± SD) | 12.7 ± 1.8 | 12.6 ± 1.7 | 12.1 ± 1.7 | 13.2 ± 1.7 | 0.0001 |
| Serum calcium (mg/dl; mean ± SD) | 9.2 ± 0.5 | 9.2 ± 0.5 | 9.1 ± 0.5 | 9.2 ± 0.5 | 0.0001 |
| Serum phosphorus (mg/dl; mean ± SD) | 3.7 ± 0.7 | 3.7 ± 0.7 | 3.9 ± 0.7 | 3.6 ± 0.6 | 0.0001 |
| Total PTH (pg/ml; median [IQR]) | 53.0 (34.0 to 88.0) | 52.9 (34.0 to 85.0) | 60.0 (37.1 to 102.4) | 48.5 (32.5 to 78.0) | 0.0001 |
| Blood glucose (mg/dl; median [IQR]) | 97.0 (86.0 to 124.0) | 97.0 (86.0 to 121.0) | 127.0 (100.0 to 163.0) | 90.0 (84.0 to 98.0) | 0.0001 |
| Glycosylated hemoglobin (%; mean ± SD | 6.6 ± 1.6 | 6.6 ± 1.6 | 7.7 ± 1.7 | 5.7 ± 0.5 | 0.0001 |
ABI, ankle-brachial index; ACEI, angiotensin-converting enzyme inhibitor; ARB, angiotensin receptor blocker; BMI, body mass index; DBP, diastolic BP; eGFR, estimated GFR; iPTH, intact parathyroid hormone; IQR, interquartile range; MAP, mean arterial pressure; MI, myocardial infarction; PAD, peripheral arterial disease; SB{, systolic BP.
Includes Asian/Pacific Islander and Native American individuals.
Several differences also existed between participants with and without diabetes (Table 3). Compared with participants without diabetes, those with diabetes were more likely to be nonwhite and Hispanic and to earn annual incomes <$20,000 but were less likely to have a college education (P = 0.0001). Self-reported myocardial infarction/coronary revascularization, congestive heart failure, and PAD were nearly twice as common among participants with diabetes. Participants with diabetes were also more likely to have a history of hypertension, have mean baseline BP >130/80 mmHg, and have a BMI ≥30 (P = 0.0001). Furthermore, these participants had a two-fold greater prevalence of an ABI <0.9. Mean eGFR was lower and urine protein higher among participants with diabetes than among those without diabetes.
Baseline Characteristics by eGFR Level
As a result of enrollment strategies, there was relatively even distribution by race across eGFR strata (Table 4). In comparison with those who had higher eGFR, participants with lower eGFR tended to older, female, and Hispanic (P = 0.0001). Also, a trend existed between lower eGFR and a higher proportion of annual incomes <$20,000, having only high school level education, BMI >30 kg/m2, and history of >100 cigarettes. The prevalence of hypertension (and those with mean BP >130/80 mmHg), diabetes, CVD, PAD, and proteinuria were also significantly higher in lower eGFR groups (P = 0.0001). With lower eGFR, there were progressive decreases in mean hemoglobin and increases in mean serum phosphorus and total parathyroid hormone (P = 0.0001).
Table 4.
Baseline characteristics by eGFR level
| Variable | eGFR (ml/min per 1.73 m2) |
P | ||||
|---|---|---|---|---|---|---|
| <30 | 30 to <40 | 40 to <50 | 50 to <60 | ≥60 | ||
| n | 667 | 844 | 968 | 720 | 397 | |
| Age (yr; mean ± SD) | 58.7 ± 11.2 | 59.6 ± 11.0 | 60.0 ± 10.4 | 57.7 ± 10.1 | 51.5 ± 11.0 | 0.0001 |
| Gender (n [%]) | 0.0001 | |||||
| male | 311 (47) | 440 (52) | 568 (59) | 406 (56) | 226 (57) | |
| female | 356 (53) | 404 (48) | 400 (41) | 314 (44) | 171 (43) | |
| Racial/ethnic group (n [%]) | 0.0673 | |||||
| non-Hispanic white | 277 (42) | 386 (46) | 461 (48) | 348 (48) | 160 (40) | |
| non-Hispanic black/African American | 303 (45) | 387 (46) | 430 (44) | 319 (44) | 202 (51) | |
| Hispanic | 55 (8) | 43 (5) | 32 (3) | 21 (3) | 18 (5) | |
| othera | 32 (5) | 28 (3) | 45 (5) | 32 (4) | 17 (4) | 0.0001 |
| Annual household income (n [%]) | 0.1435 | |||||
| ≤$20,000 | 249 (37) | 292 (35) | 232 (24) | 155 (22) | 72 (18) | |
| $20,001 to $50,000 | 179 (27) | 199 (24) | 267 (28) | 162 (23) | 96 (24) | |
| $50,001 to $100,000 | 103 (17) | 150 (18) | 187 (19) | 171 (24) | 108 (27) | |
| >$100,000 | 38 (6) | 69 (8) | 117 (12) | 115 (16) | 49 (12) | |
| no response | 93 (14) | 134 (16) | 165 (17) | 117 (16) | 72 (18) | |
| Educational attainment (n [%]) | 0.0001 | |||||
| <7th grade | 27 (4) | 15 (2) | 10 (1) | 4 (1) | 2 (1) | |
| 7th to 12th grade | 126 (18) | 160 (19) | 143 (15) | 82 (11) | 27 (7) | |
| high school diploma | 145 (22) | 177 (21) | 189 (20) | 112 (16) | 69 (17) | |
| vocational degree | 36 (5) | 38 (5) | 48 (5) | 36 (5) | 26 (7) | |
| some college | 162 (24) | 224 (27) | 228 (24) | 192 (27) | 112 (28) | |
| college graduate | 106 (16) | 146 (17) | 188 (19) | 172 (24) | 82 (21) | |
| graduate degree | 65 (10) | 84 (10) | 162 (17) | 122 (17) | 76 (19) | |
| Tobacco use (n [%]) | ||||||
| current smoker | 110 (16) | 122 (15) | 117 (12) | 84 (12) | 54 (14) | 0.0001 |
| >100 cigarettes during lifetime | 405 (61) | 500 (59) | 542 (56) | 375 (52) | 139 (48) | 0.0189 |
| Medical history (n [%]) | ||||||
| hypertension | 612 (92) | 767 (91) | 848 (88) | 587 (82) | 267 (67) | 0.0001 |
| diabetes | 352 (53) | 459 (54) | 448 (46) | 290 (40) | 130 (33) | 0.0001 |
| MI or coronary revascularization | 170 (26) | 227 (27) | 227 (23) | 131 (18) | 51 (13) | 0.0001 |
| chronic heart failure | 97 (15) | 103 (12) | 91 (10) | 43 (6) | 19 (5) | 0.0001 |
| PAD | 75 (11) | 85 (10) | 47 (5) | 31 (4) | 11 (4) | 0.0001 |
| BP variables | . | |||||
| SBP (mmHg; mean ± SD) | 130.5 ± 23.6 | 129.4 ± 23.2 | 127.7 ± 21.3 | 125.4 ± 20.2 | 123.5 ± 20.0 | 0.0001 |
| DBP (mmHg; mean ± SD) | 69.9 ± 13.3 | 70.0 ± 12.6 | 71.5 ± 12.7 | 72.3 ± 12.3 | 74.9 ± 12.8 | 0.0001 |
| MAP (mmHg; mean ± SD) | 90.1 ± 14.4 | 89.8 ± 14.0 | 90.2 ± 13.7 | 90.0 ± 13.1 | 91.1 ± 13.6 | 0.6042 |
| BP >130/80 (mmHg; n [%]) | 335 (50) | 394 (47) | 466 (48) | 319 (45) | 164 (42) | 0.0001 |
| Weight (kg; mean ± SD) | 89.8 ± 24.8 | 92.3 ± 23.2 | 92.5 ± 23.3 | 93.3 ± 24.1 | 92.4 ± 22.6 | 0.0311 |
| BMI (kg/m2; mean ± SD) | 31.9 ± 8.4 | 32.5 ± 7.9 | 32.1 ± 7.8 | 32.2 ± 8.1 | 31.3 ± 7.1 | 0.2313 |
| BMI category (kg/m2; n [%]) | 0.9367 | |||||
| <25.0 | 134 (20) | 128 (15) | 150 (15) | 121 (17) | 74 (19) | |
| 25.0 to 29.9 | 182 (27) | 238 (28) | 275 (28) | 206 (29) | 112 (28) | 0.0001 |
| >30 | 353 (53) | 480 (57) | 544 (56) | 392 (55) | 212 (54) | |
| ABI <0.9 | 142 (22) | 149 (18) | 125 (13) | 93 (13) | 15 (4) | 0.0001 |
| Roche adjusted creatinine (mean ± SD) | 2.56 ± 0.56 | 1.90 ± 0.32 | 1.56 ± 0.23 | 1.32 ± 0.20 | 1.14 ± 0.20 | 0.0001 |
| Urine protein/24 h (g; median [IQR]) | 0.58 (0.15 to 2.14) | 0.26 (0.08 to 1.22) | 0.13 (0.07 to 0.60) | 0.10 (0.06 to 0.36) | 0.10 (0.06 to 0.22) | 0.0001 |
| Lipoproteins | ||||||
| total cholesterol (mg/dl; mean ± SD) | 183.3 ± 51.2 | 182.5 ± 46.2 | 183.1 ± 42.1 | 183.2 ± 41.3 | 183.5 ± 39.6 | 0.8297 |
| LDL cholesterol (mg/dl; mean ± SD) | 99.7 ± 37.9 | 100.2 ± 35.3 | 103.1 ± 34.6 | 104.4 ± 33.3 | 107.3 ± 32.6 | 0.0001 |
| HDL cholesterol (mg/dl; mean ± SD) | 46.9 ± 15.5 | 47.4 ± 15.8 | 48.2 ± 14.9 | 48.8 ±16.0 | 50.2 ± 16.4 | 0.0004 |
| triglycerides (mg/dl; mean ± SD) | 168.1 ± 127.2 | 163.0 ± 123.4 | 151.4 ± 99.6 | 148.5 ± 127.2 | 129.9 ± 81.6 | 0.0001 |
| Hemoglobin (g/dl; mean ± SD) | 11.8 ± 1.7 | 12.3 ± 1.7 | 12.8 ± 1.7 | 13.2 ± 1.6 | 13.4 ± 1.6 | 0.0001 |
| Serum calcium (mg/dl; mean ± SD) | 9.1 ± 0.6 | 9.2 ± 0.5 | 9.2 ± 0.5 | 9.2 ± 0.5 | 9.2 ± 0.4 | 0.0002 |
| Total iPTH (pg/ml; median [IQR]) | 105.0 (64.0 to 172.0) | 63.9 (41.0 to 100.0) | 47.5 (32.0 to 74.0) | 41.0 (29.7 to 59.1) | 36.0 (27.3 to 50.3) | 0.0001 |
| Serum phosphorus(mg/dl; mean ± SD) | 4.1 ± 0.8 | 3.8 ± 0.6 | 3.6 ± 0.6 | 3.5 ± 0.6 | 3.4 ± 0.5 | 0.0001 |
| Blood glucose (mg/dl; median [IQR]) | 97.0 (85.0 to 124.0) | 98.0 (87.0 to 131.0) | 100.0 (88.0 to 127.0) | 95.0 (85.0 to 119.0) | 94.0 (84.0 to 110.0) | 0.0003 |
| Glycosylated hemoglobin(%; mean ± SD) | 6.7 ± 1.5 | 6.8 ± 1.6 | 6.7 ± 1.5 | 6.5 ± 1.4 | 6.3 ± 1.7 | 0.0001 |
| Serum uric acid (mg/dl; mean ± SD) | 8.2 ± 2.0 | 7.9 ± 1.9 | 7.3 ± 1.8 | 6.8 ± 1.6 | 6.2 ± 1.7 | 0.0001 |
Includes Asian/Pacific Islander and Native American individuals.
Select Anticipated and Actual Recruitment Targets
Recruitment by racial and ethnic groups was similar to anticipated target goals (Table 5). In contrast, the actual recruitment of young participants with (3.99%) and without diabetes (9.51%) was less than the targeted goal of 12.5% for both subgroups (Table 6).
Table 5.
Select anticipated and actual recruitment targets: Race/ethnic target distribution in CRIC Study
| Race/Ethnic Group | Anticipated (%) | Actual (%) |
|---|---|---|
| Non-Hispanic white | 47.50 | 45.34 |
| Non-Hispanic black | 47.50 | 45.92 |
| Othera | 5.00 | 8.75 |
For the purposes of recruitment goal, other group includes Hispanic, Asian/Pacific Islander, and Native American individuals.
Table 6.
Select anticipated and actual recruitment targets: Age- and diabetes-status distribution in CRIC Study
| Age Stratum (yr) | Anticipated Recruitment (%) |
Actual Recruitment Cohort (%) |
||
|---|---|---|---|---|
| No Diabetes | Diabetes | No Diabetes | Diabetes | |
| 21 to 44 | 12.50 | 12.50 | 9.51 | 3.99 |
| 45 to 64 | 25.00 | 25.00 | 29.72 | 27.75 |
| 65 to 74 | 12.50 | 12.50 | 14.56 | 14.47 |
Discussion
The CRIC Study was designed to examine risk factors for CKD progression and CVD incidence and progression among a large, representative cohort of individuals with CKD. The CRIC cohort enrolled a diverse set of participants who had CKD and possessed a broad range of kidney dysfunction and other potentially important prognostic attributes. Recruitment goals regarding race/ethnicity, gender, age, and diabetes status were largely met. The strength of the CRIC Study lies in the diverse characteristics of the assembled cohort and the comprehensive data collection activities that have been designed to address gaps in our understanding of CKD-associated morbidity and mortality and to identify potential targets for trials of preventive therapies.
The baseline findings regarding diabetic status and level of kidney function support that the assembled cohort has characteristics representative of the broader CKD population. As expected, participants with diabetes in the cohort were more likely to have self-reported CVD than those without diabetes. The findings in the CRIC subgroup with diabetes reinforce the findings from clinical trials that indicate that the CVD burden in the ESRD population with diabetes has its beginnings earlier during the course of CKD (15,16). In addition, lower levels of eGFR were associated with a greater burden of CVD. This is consistent with the increasing evidence for the presence and severity of CKD as an independent and graded risk factor for CVD events (3). By using sophisticated measurements of kidney function and subclinical CVD, the CRIC Study will provide insights into the pathophysiology of this relationship and will enable an assessment of both traditional and nontraditional risk factors.
Noteworthy is the high prevalence of several potentially modifiable risk factors in this CKD cohort. Almost half of all participants had a BP level above the recommended goal (17). Suboptimal levels of BP control have been reported in other CKD cohorts (18,19), and the findings in the CRIC cohort reinforce the need to raise awareness of effective BP management in CKD as a public health priority. As well, we observed a high prevalence of obesity among participants with and without diabetes. It has been suggested that higher BMI may be an independent risk factor for CKD (20–22) and progression to ESRD that requires dialysis (23). The modest association between lower eGFR and previous cigarette exposure is consistent with the previously described association of smoking with CKD (24). This relationship is also of particular interest because it may represent another potential risk factor. Longitudinal follow-up of CRIC participants will afford a more rigorous assessment of these newly recognized but less studied risk factors on CVD and CKD outcomes.
We also observed an important association between lower eGFR and both lower socioeconomic status (SES) and lesser educational attainment. It is known that lower SES is associated with ESRD (25,26). Analyses of several cohorts found an association between lower SES and progressive CKD (27–29). The CRIC Study will facilitate evaluation of the impact of SES and educational level in individuals with more advanced stages of CKD and potential mediating pathways that could have important health policy implications.
Previous epidemiologic studies of the relationship between CKD and CVD have come from various sources, including post hoc analyses of clinical trials (30–33), large cohort studies focused on non-CKD populations (34–37), and analyses of large datasets from major health care providers (3,38). Despite the important contributions made by these studies, major gaps in our knowledge remain. The CRIC Study will occupy a unique niche because of its use of observational epidemiology in a large cohort of patients with CKD and its use of longitudinal state-of-the-art measurements of kidney function and subclinical CVD. In addition to examining risk factors for CKD and CVD progression, the CRIC Study will facilitate the development of predictive models that identify high-risk groups; the determination of exposure–outcome relationships; and the evaluation of the impact of CKD and progressive CKD on quality of life, functional status, and resource use. Unlike most previous studies, the CRIC Study continues to follow participants after progression to ESRD, thereby providing an important opportunity to study the critical period when patients transition from CKD to ESRD.
Concurrent with the CRIC Study, several ongoing studies are examining risk factors for CKD. The National Health and Nutrition Examination Survey (NHANES) monitors CKD prevalence and risk factors over time (2,39). The National Kidney Foundation's Kidney Evaluation Education Program (KEEP) collects data characterizing CKD in the community among at-risk subgroups (40). The African American Study of Kidney Disease and Hypertension (AASK) (41) is investigating factors that influence CKD progression among black individuals with hypertensive kidney disease. Internationally, the CKD-Japan Cohort Study (CKD-JAC) is in the early stages of follow-up. The information gained from the CRIC Study will be complementary to and extend the important work accomplished by these studies. As an example, compared with the population-based NHANES CKD cohort (2), the CRIC cohort is older and by design has more advanced CKD with more even distribution across eGFR strata, a larger percentage of individuals with diabetes, and a larger representation of black participants to facilitate more robust subgroup analyses.
As with all prospective observational studies, inferences regarding causality will be limited by potential biases and residual confounding. Numerous methodologic strategies have been adopted to minimize these limitations and enhance the robustness of etiologic inferences drawn from this study. Another potential limitation is underrepresentation of young individuals with diabetes. To adapt to this, this group was oversampled for recruitment into the subcohort from which more detailed assessments of kidney function and cardiovascular health will be obtained. In addition, the less-than-anticipated recruitment of Hispanic individuals will be addressed by the ongoing supplemental recruitment of >330 Hispanic participants at the University of Illinois at Chicago.
The observed low level of proteinuria could also have potential implications for future risk of cardiovascular and renal events; however, the high prevalence of self-reported comorbidities suggests that the cohort is at increased risk for adverse events. Furthermore, in the AASK, there was significant progression of CKD despite relatively low levels of baseline proteinuria (42). It is also important to note that findings from the CRIC Study may not be generalizable to certain types of kidney disease that was poorly represented in the cohort, such as glomerulonephritis. It was not intended for the study to be representative of all patients with CKD; rather, it was designed to be broadly representative of the ESRD population in which diabetes and hypertension are reported as the primary diagnoses for >70% of patients (1). Finally, analyses included self-reported comorbidities, which are subject to inherent limitations with regard to accuracy.
The CRIC Study has assembled a large and diverse CKD cohort with characteristics that area generalizable to CKD populations managed in different practice settings in the United States. Analogous to the Framingham Heart and Atherosclerosis Risk in Communities Studies, the CRIC Study will use observational epidemiology to answer key questions about the cause, prognosis, management, clinical outcomes, health service use, and quality of life in CKD. The knowledge generated from the CRIC Study will lead to the formulation of hypotheses regarding potentially modifiable pathways that will serve as the basis for targeted interventional trials that focus on reducing the burden of CKD and CVD.
Disclosures
None.
Acknowledgments
In addition to funding under a cooperative agreement from National Institute of Diabetes and Digestive and Kidney Diseases (5U01DK060990, 5U01DK060984, 5U01DK06102, 5U01DK061021, 5U01DK061028, 5U01DK60980, 5U01DK060963, and 5U01DK060902), this work was supported in part by the following institutional Clinical Translational Science Awards and other National Institutes of Health grants: Johns Hopkins University UL1 RR-025005, University of Maryland GRCR M01 RR-16500, Case Western Reserve University Clinical and Translational Science Collaborative (University Hospitals of Cleveland, Cleveland Clinic Foundation, and MetroHealth) UL1 RR-024989, University of Michigan GCRC M01 RR-000042 and CTSA UL1 RR-024986, University of Illinois at Chicago Clinical Research Center, M01 RR-013987-06, Tulane/LSU/Charity Hospital General Clinical Research Center RR-05096, and Kaiser NIH/NCRR UCSF-CTSI UL1 RR-024131 and 5K24DK002651. Additional support provided by the National Center for Minority Health and Health Disparities, National Institutes of Health, and Department of Veterans Affairs (Career Development Award to M.J.F.).
University of Pennsylvania, Scientific & Data Coordinating Center: Harold I. Feldman, MD, MSCE (principal investigator), J. Richard Landis, PhD, Shawn Ballard, MS, Zhen Chen, PhD, Denise Cifelli, Robert M. Curley, MS, James Dattilo, Marie Durborow, Stephen Durborow, Susan Eachus, PhD, Melanie Glenn, MPH, Asaf Hanish, MPH, Christopher Helker, MSPH, Maximilan Herlim, Amanda Hyre, PhD, MPH, Marshall Joffe, MD, PhD, MPH, Hopiy Kim, Stephen E. Kimmel, MD, Shiriki Kumanyika, PhD, MPH, Lisa Nessel, MSS, MLSP, Emile R. Mohler, III, MD, Gargi Parikh, MS, Amy Praestgard, MS, Nancy Robinson, MS, Leigh Rosen, MUEP, J. Sanford Schwartz, MD, Sandra Smith, Joan Stahl, MS, Valerie L. Teal, MS, Dawei Xie, PhD, Peter Yang, PhD; University of Pennsylvania Medical Center: Raymond R. Townsend, MD (principal investigator), Thomas Capolla, MD, ScM (ancillary investigator), Debbie Cohen, MD, Magdalena Cuevas, Mark J. Duckworth, Virginia Ford, MSN, CRNP, Colin M. Gorman, Juan Grunwald, MD (ancillary investigator), Lucy Kibe, MS, Mary B. Leonard, MD, MSCE (ancillary investigator), Maureen Maguire, PhD (ancillary investigator), Stephanie McDowell, John Murphy, MD, Muredach Reilly, MB (ancillary investigator), Sylvia E. Rosas, MD (ancillary investigator), Wanda M. Seamon, Angie Sheridan, MPH, Karen Teff, MD; The Johns Hopkins University: Lawrence J. Appel, MD, MPH (principal investigator), Cheryl Anderson, PhD, MPH, Brad Astor, PhD, MPH, Jeanne Charleston, RN, Bernard Jaar, MD, MPH, Edgar “Pete” Miller, MD, Patience Ngoh, Hemalatha Venkatesh, J. Hunter Young, MD, MHS; University of Maryland: Jeffrey Fink, MD, MS (co-principal investigator), Wanda Fink, RN, BSN, Afshin Parsa, MD, MPH, Beth Scism, Stephen Seliger, MD, MS, Matthew Weir, MD; University Hospitals of Cleveland Case Medical Center: Mahboob Rahman, MD (principal investigator), Renita Brooks, Valori Corrigan, RN, Genya Kisin, MA, Radhika Kanthety, Louise Strauss, RN, Jackson T. Wright, Jr., MD, PhD; MetroHealth Medical Center: Patricia Kao (co-principal investigator), Kim Bauchens, RN, Jacqui Bjaloncik, Jeffrey Schelling, MD, John R. Sedor, MD, Mary Ann Shella, RN, BSN, Jacqueline Theurer, J. Daryl Thornton, MD, MPH; Cleveland Clinical Foundation: Martin J. Schreiber, MD (co-principal investigator), Martha Coleman, RN, Richard Fatica, MD, David Frey, Darla Greenwald, Sandra Halliburton, PhD, Carol Horner, BSN, RN, Teresa Markle, BS, Sandra Pangonis, RN, Carmen Paradis, MD, Mohammed A. Rafey, MD, MS, Annette Russo, Stephanie Slattery, RN, Jackie Soos, Rita Spirko, RN, MSN, Kay Stelmach, RN, Velma Stephens, LPN; University of Michigan at Ann Arbor: Akinlolu Ojo, MD, PhD (principal investigator), Anil Attili, MD, Jeff Briesmiester, Tonya L. Corbin, MD, Denise Cornish-Zirker, BSN, Crystal Gadegbeku, MD, Nancy Hill, Kenneth Jamerson, MD, Bruce Robinson, MD, Rajiv Saran, MD, Bonnie Welliver, BSN, CNN, Jillian Wilson, Eric Young, MD, MS; St. John's Health System: Susan P. Steigerwalt, MD, FACP (co-principal investigator), Keith Bellovich, DO, Jennifer DeLuca, Sherry Gasko, BSRN, Gail Makos, RN, MSN, Chantal Parmelee, Shahan Smith, Kathleen Walls; Wayne State University: John M. Flack, MD, MPH (co-principal investigator), Andrew Johnson III, RN, Mary Maysura, Barbara Lloyd, MA, RD, Stephen Migdal, MD, M. Jena Mohanty, MD, Yanni Zhuang, BSN; University of Illinois at Chicago: James P. Lash, MD (principal investigator), Jose Arruda, MD, Carolyn Brecklin, MD, Janet Cohan, MSN, Michael Fischer, MD, MSPH, Leon Fogelfeld, Anne Frydrych, MS, RD, Claudia Lora (ancillary investigator), MD, Onesema Martinez, Patricia Meslar, MSN, Kalyani Perumal, MD, Thomas Stamos, MD, Gregg Vachon, Paul Vaitkus, MD, Eve Van Cauter (ancillary investigator), PhD, Julio C. Vijil, MD (ancillary investigator); Tulane University Health Science Center: Jiang He, MD, PhD (principal investigator), Brent Alper, MD, Vecihi Batuman, MD, Lydia A. Bazzano, MD, PhD, Bernadette Borja, Adriana Burridge, Jing Chen, MD, MSc, Catherine Cooke, Patrice Delafontaine, MD, Karen B. DeSalvo, MD, MPH, MSc, Vivian A. Fonseca, MD, Lee Hamm, MD, Michelle R. Hurly, RN, BSN, Eva Lustigova, MPH, Paul Muntner, PhD (ancillary investigator), Lindsey Powers, Paul Whelton, MD, MSc; Kaiser Permanente of Northern California: Alan S. Go, MD (principal investigator), Lynn M. Ackerson, PhD, Pete Dorin, MPA, Daniel Fernandez, Rosy Fox, Nancy G. Jensvold, MPH, Joan C. Lo, MD, Juan D. Ordonez, MD, MPH, Rachel Perloff, Thida Tan, MPH, Daphne Thompson, Gina M. Valladares, Annette Wiggins, RN, Diana B. Wong, RN, MPH, Jingrong (Michelle) Yang, MA; University of California, San Francisco: Chi-yuan Hsu, MD, MSc (co-principal investigator), Glenn M. Chertow, MD, MPH, Nisha Bansal, MD, Irina Gorodetskaya, Vanessa Grubbs, MD (ancillary investigator), Manju Kurella, MD, MPH (ancillary investigator), Lowell Lo, MD, Michael G. Shlipak, MD, MPH (ancillary investigator), Kristine Yaffe, MD (ancillary investigator); NIDDK: John W. Kusek, PhD, Andrew S. Narva, MD; Scientific Advisory Committee: Kathy Faber-Langendoen, MD, Bryce A. Kiberd, MD, Elisa T. Lee, PhD, Julia Lewis, MD, William McClellan, MD, MPH, Timothy Meyer, MD, David Nathan, MD, John B. Stokes, MD, Herman Taylor, MD, Peter W. Wilson, MD; University of New Mexico: Dominic Raj, MD, DM (ancillary investigator), Vallabh Shah, PhD (ancillary investigator); Consultants- Harvard School of Med: Paul M. Ridker, MD; Central Lab-University of Pennsylvania: Daniel J. Rader, MD, Anna DiFlorio, Ted Mifflin, Linda Morrell, Megan L. Wolfe; GFR Lab-Cleveland Clinic: Phillip Hall, MD, Sue Saunders; EBT Reading Center- UCLA: Mathew Budoff, MD, Chris Dailing; ECG Reading Center- Wake Forest: Ronald Prineas, MD, PhD, Elsayed Soliman, MD, Zhu-Ming Zhang, MD; Echo Reading Center-University of Pennsylvania: Martin St. John Sutton, MBBS, Martin G. Keane, MD, FACC, FAHA
We thank the CRIC participants for time and commitment to the study.
Footnotes
Published online ahead of print. Publication date available at www.cjasn.org.
This trial has been registered at www.clinicaltrials.gov (identifier NCT00304148).
References
- 1.US Renal Data System: Excerpts from the United States Renal Data System 2006 Annual Data Report. Am J Kidney Dis 49: A6–A296, 2007 [DOI] [PubMed] [Google Scholar]
- 2.Coresh J, Selvin E, Stevens LA, Manzi J, Kusek JW, Eggers P, Van Lente F, Levey AS: Prevalence of chronic kidney disease in the United States. JAMA 298: 2038–2047, 2007 [DOI] [PubMed] [Google Scholar]
- 3.Go AS, Chertow GM, Fan D, McCulloch CE, Hsu CY: Chronic kidney disease and the risks of death, cardiovascular events, and hospitalization. N Engl J Med 351: 1296–1305, 2004 [DOI] [PubMed] [Google Scholar]
- 4.Feldman HI, Appel LJ, Chertow GM, Cifelli D, Cizman B, Daugirdas J, Fink JC, Franklin-Becker ED, Go AS, Hamm LL, He J, Hostetter T, Hsu CY, Jamerson K, Joffe M, Kusek JW, Landis JR, Lash JP, Miller ER, Mohler ER, III, Muntner P, Ojo AO, Rahman M, Townsend RR, Wright JT: The Chronic Renal Insufficiency Cohort (CRIC) Study: Design and methods. J Am Soc Nephrol 14[Suppl]: S148–S153, 2003 [DOI] [PubMed] [Google Scholar]
- 5.Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL, Jr, Jones DW, Materson BJ, Oparil S, Wright JT, Jr, Roccella EJ: The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: The JNC 7 report. JAMA 289: 2560–2572, 2003 [DOI] [PubMed] [Google Scholar]
- 6.Diagnosis and classification of diabetes mellitus. Diabetes Care 29[Suppl 1]: S43–S48, 2006 [PubMed] [Google Scholar]
- 7.Levey AS, Bosch JP, Lewis JB, Greene T, Rogers N, Roth D: A more accurate method to estimate glomerular filtration rate from serum creatinine: A new prediction equation. Modification of Diet in Renal Disease Study Group. Ann Intern Med 130: 461–470, 1999 [DOI] [PubMed] [Google Scholar]
- 8.Coresh J, Astor BC, McQuillan G, Kusek J, Greene T, Van Lente F, Levey AS: Calibration and random variation of the serum creatinine assay as critical elements of using equations to estimate glomerular filtration rate. Am J Kidney Dis 39: 920–929, 2002 [DOI] [PubMed] [Google Scholar]
- 9.Grantham JJ, Torres VE, Chapman AB, Guay-Woodford LM, Bae KT, King BF, Jr, Wetzel LH, Baumgarten DA, Kenney PJ, Harris PC, Klahr S, Bennett WM, Hirschman GN, Meyers CM, Zhang X, Zhu F, Miller JP: Volume progression in polycystic kidney disease. N Engl J Med 354: 2122–2130, 2006 [DOI] [PubMed] [Google Scholar]
- 10.Perloff D, Grim C, Flack J, Frohlich ED, Hill M, McDonald M, Morgenstern BZ: Human blood pressure determination by sphygmomanometry. Circulation 88: 2460–2470, 1993 [DOI] [PubMed] [Google Scholar]
- 11.McDermott MM, Criqui MH, Liu K, Guralnik JM, Greenland P, Martin GJ, Pearce W: Lower ankle/brachial index, as calculated by averaging the dorsalis pedis and posterior tibial arterial pressures, and association with leg functioning in peripheral arterial disease. J VascSurg 32: 1164–1171, 2000 [DOI] [PubMed] [Google Scholar]
- 12.Vitelli LL, Crow RS, Shahar E, Hutchinson RG, Rautaharju PM, Folsom AR: Electrocardiographic findings in a healthy biracial population. Atherosclerosis Risk in Communities (ARIC) Study Investigators. AmJCardiol 81: 453–459, 1998 [DOI] [PubMed] [Google Scholar]
- 13.Hall PM, Rolin H: Iothalamate clearance and its use in large-scale clinical trials. Curr Opin Nephrol Hypertens 4: 510–513, 1995 [DOI] [PubMed] [Google Scholar]
- 14.National Kidney Foundation (NKF) Kidney Disease Outcome Quality Initiative (K/DOQI): Clinical practice guidelines for chronic kidney disease: Evaluation, classification, and stratification. Am J Kidney Dis 39: S1–S246, 2002 [PubMed] [Google Scholar]
- 15.Brenner BM, Cooper ME, De Zeeuw D, Keane WF, Mitch WE, Parving HH, Remuzzi G, Snapinn SM, Zhang Z, Shahinfar S: Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med 345: 861–869, 2001 [DOI] [PubMed] [Google Scholar]
- 16.Lewis EJ, Hunsicker LG, Clarke WR, Berl T, Pohl MA, Lewis JB, Ritz E, Atkins RC, Rohde R, Raz I: Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N Engl J Med 345: 851–860, 2001 [DOI] [PubMed] [Google Scholar]
- 17.K/DOQI clinical practice guidelines on hypertension and antihypertensive agents in chronic kidney disease. Am J Kidney Dis 43: S1–S290, 2004 [PubMed] [Google Scholar]
- 18.Duru OK, Li S, Jurkovitz C, Bakris G, Brown W, Chen SC, Collins A, Klag M, McCullough PA, McGill J, Narva A, Pergola P, Singh A, Norris K: Race and sex differences in hypertension control in CKD: Results from the Kidney Early Evaluation Program (KEEP). Am J Kidney Dis 51: 192–198, 2008 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Parikh NI, Hwang SJ, Larson MG, Meigs JB, Levy D, Fox CS: Cardiovascular disease risk factors in chronic kidney disease: Overall burden and rates of treatment and control. Arch Intern Med 166: 1884–1891, 2006 [DOI] [PubMed] [Google Scholar]
- 20.Chen J, Muntner P, Hamm LL, Jones DW, Batuman V, Fonseca V, Whelton PK, He J: The metabolic syndrome and chronic kidney disease in U.S. adults. Ann Intern Med 140: 167–174, 2004 [DOI] [PubMed] [Google Scholar]
- 21.Fox CS, Larson MG, Leip EP, Culleton B, Wilson PW, Levy D: Predictors of new-onset kidney disease in a community-based population. JAMA 291: 844–850, 2004 [DOI] [PubMed] [Google Scholar]
- 22.Kramer H, Luke A, Bidani A, Cao G, Cooper R, McGee D: Obesity and prevalent and incident CKD: The Hypertension Detection and Follow-Up Program. Am J Kidney Dis 46: 587–594, 2005 [DOI] [PubMed] [Google Scholar]
- 23.Hsu CY, McCulloch CE, Iribarren C, Darbinian J, Go AS: Body mass index and risk for end-stage renal disease. Ann Intern Med 144: 21–28, 2006 [DOI] [PubMed] [Google Scholar]
- 24.Orth SR: Smoking and the kidney. J Am Soc Nephrol 13: 1663–1672, 2002 [DOI] [PubMed] [Google Scholar]
- 25.Young EW, Mauger EA, Jiang KH, Port FK, Wolfe RA: Socioeconomic status and end-stage renal disease in the United States. Kidney Int 45: 907–911, 1994 [DOI] [PubMed] [Google Scholar]
- 26.Perneger TV, Whelton PK, Klag MJ: Race and end-stage renal disease: Socioeconomic status and access to health care as mediating factors. Arch Intern Med 155: 1201–1208, 1995 [PubMed] [Google Scholar]
- 27.Klag MJ, Whelton PK, Randall BL, Neaton JD, Brancati FL, Stamler J: End-stage renal disease in African-American and white men: 16-year MRFIT findings. JAMA 277: 1293–1298, 1997 [PubMed] [Google Scholar]
- 28.Krop JS, Coresh J, Chambless LE, Shahar E, Watson RL, Szklo M, Brancati FL: A community-based study of explanatory factors for the excess risk for early renal function decline in blacks vs whites with diabetes: The Atherosclerosis Risk in Communities study. Arch Intern Med 159: 1777–1783, 1999 [DOI] [PubMed] [Google Scholar]
- 29.Merkin SS, Diez Roux AV, Coresh J, Fried LF, Jackson SA, Powe NR: Individual and neighborhood socioeconomic status and progressive chronic kidney disease in an elderly population: The Cardiovascular Health Study. Soc Sci Med 65: 809–821, 2007 [DOI] [PubMed] [Google Scholar]
- 30.Hunsicker LG, Adler S, Caggiula A, England BK, Greene T, Kusek JW, Rogers NL, Teschan PE: Predictors of the progression of renal disease in the Modification of Diet in Renal Disease Study. Kidney Int 51: 1908–1919, 1997 [DOI] [PubMed] [Google Scholar]
- 31.Jafar TH, Stark PC, Schmid CH, Landa M, Maschio G, De Jong PE, De Zeeuw D, Shahinfar S, Toto R, Levey AS: Progression of chronic kidney disease: The role of blood pressure control, proteinuria, and angiotensin-converting enzyme inhibition—A patient-level meta-analysis. Ann Intern Med 139: 244–252, 2003 [DOI] [PubMed] [Google Scholar]
- 32.Norris KC, Greene T, Kopple J, Lea J, Lewis J, Lipkowitz M, Miller P, Richardson A, Rostand S, Wang X, Appel LJ: Baseline predictors of renal disease progression in the African American Study of Hypertension and Kidney Disease. J Am Soc Nephrol 17: 2928–2936, 2006 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Keane WF, Brenner BM, De Zeeuw D, Grunfeld J-P, Lash JP, Lyle PA, McGill J, Mitch WE, Remuzzi G, Shahinfar S, Snapinn SM, Toto R, Zhang Z.RENAAL Study Investigators: A risk score for predicting end-stage renal disease in patients with type 2 diabetes and nephropathy. Clin J Am Soc Nephrol 1: 761–767, 2006 [DOI] [PubMed] [Google Scholar]
- 34.Culleton BF, Larson MG, Evans JC, Wilson PW, Barrett BJ, Parfrey PS, Levy D: Prevalence and correlates of elevated serum creatinine levels: The Framingham Heart Study. Arch Intern Med 159: 1785–1790, 1999 [DOI] [PubMed] [Google Scholar]
- 35.Stehman-Breen CO, Gillen D, Steffes M, Jacobs DR, Jr, Lewis CE, Kiefe CI, Siscovick D: Racial differences in early-onset renal disease among young adults: The coronary artery risk development in young adults (CARDIA) study. J Am Soc Nephrol 14: 2352–2357, 2003 [DOI] [PubMed] [Google Scholar]
- 36.Fried LF, Shlipak MG, Crump C, Bleyer AJ, Gottdiener JS, Kronmal RA, Kuller LH, Newman AB: Renal insufficiency as a predictor of cardiovascular outcomes and mortality in elderly individuals. J Am Coll Cardiol 41: 1364–1372, 2003 [DOI] [PubMed] [Google Scholar]
- 37.Muntner P, He J, Astor BC, Folsom AR, Coresh J: Traditional and nontraditional risk factors predict coronary heart disease in chronic kidney disease: Results from the Atherosclerosis Risk in Communities Study. J Am Soc Nephrol 16: 529–538, 2005 [DOI] [PubMed] [Google Scholar]
- 38.Patel UD, Young EW, Ojo AO, Hayward RA: CKD progression and mortality among older patients with diabetes. Am J Kidney Dis 46: 406–414, 2005 [DOI] [PubMed] [Google Scholar]
- 39.Muntner P, Hamm LL, Kusek JW, Chen J, Whelton PK, He J: The prevalence of nontraditional risk factors for coronary heart disease in patients with chronic kidney disease. Ann Intern Med 140: 9–17, 2004 [DOI] [PubMed] [Google Scholar]
- 40.National Kidney Foundation Kidney Early Evaluation Program (KEEP) 2006 Annual Data Report Am J Kidney Dis 49: S3–S160, 2007 [Google Scholar]
- 41.Sika M, Lewis J, Douglas J, Erlinger T, Dowie D, Lipkowitz M, Lash J, Cornish-Zirker D, Peterson G, Toto R, Kusek J, Appel L, Kendrick C, Gassman J: Baseline characteristics of participants in the African American Study of Kidney Disease and Hypertension (AASK) Clinical Trial and Cohort Study. Am J Kidney Dis 50: 78–89, 89.e1, 2007 [DOI] [PubMed] [Google Scholar]
- 42.Wright JT, Jr, Bakris G, Greene T, Agodoa LY, Appel LJ, Charleston J, Cheek D, Douglas-Baltimore JG, Gassman J, Glassock R, Hebert L, Jamerson K, Lewis J, Phillips RA, Toto RD, Middleton JP, Rostand SG: Effect of blood pressure lowering and antihypertensive drug class on progression of hypertensive kidney disease: Results from the AASK trial. JAMA 288: 2421–2431, 2002 [DOI] [PubMed] [Google Scholar]
- 43.Korevaar JC, Merkus MP, Jansen MA, Dekker FW, Boeschoten EW, Krediet RT: Validation of the KDQOL-SF: A dialysis-targeted health measure. Qual Life Res 11: 437–447, 2002 [DOI] [PubMed] [Google Scholar]
- 44.Diet History Questionnaire, Version 1. [Accessed June 4, 2009];National Institutes of Health, Applied Research Program, National Cancer Institute. Available at: http://riskfactor.cancer.gov/DHQ/
- 45.Folstein MF, Folstein SE, McHugh PR: “Mini-mental state”: A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12: 189–198, 1975 [DOI] [PubMed] [Google Scholar]
- 46.Rocco MV, Gassman JJ, Wang SR, Kaplan RM: Cross-sectional study of quality of life and symptoms in chronic renal disease patients: The Modification of Diet in Renal Disease Study. Am J Kidney Dis 29: 888–896, 1997 [DOI] [PubMed] [Google Scholar]
- 47.Beck AT, Steer RA, Garbin MG: Psychometric properties of the Beck Depression Inventory: 25 years of evaluation. Clin Psychol Rev 8: 77–100, 1988 [Google Scholar]
- 48.Ainsworth BE, Irwin ML, Addy CL, Whitt MC, Stolarczyk LM: Moderate physical activity patterns of minority women: The Cross-Cultural Activity Participation Study. J Womens Health Gend Based Med 8: 805–813, 1999 [DOI] [PubMed] [Google Scholar]
- 49.Bild DE, Bluemke DA, Burke GL, Detrano R, Diez Roux AV, Folsom AR, Greenland P, Jacob DR, Jr, Kronmal R, Liu K, Nelson JC, O'Leary D, Saad MF, Shea S, Szklo M, Tracy RP: Multi-ethnic study of atherosclerosis: Objectives and design. Am J Epidemiol 156: 871–881, 2002 [DOI] [PubMed] [Google Scholar]
- 50.Green CP, Porter CB, Bresnahan DR, Spertus JA: Development and evaluation of the Kansas City Cardiomyopathy Questionnaire: A new health status measure for heart failure. J Am Coll Cardiol 35: 1245–1255, 2000 [DOI] [PubMed] [Google Scholar]