Abstract
Coronary artery ectasia (CAE) is defined as a localized or diffuse non-obstructive lesion of the epicardial coronary arteries with a luminal dilation exceeding 1.5-fold the diameter of the normal adjacent arterial segment. The incidence of CAE has been reported to range between 2% and 4%, which might be an overestimation of the true frequency. The coincidence of CAE with other systemic vascular dilatations has suggested that the mechanism underlying CAE is not only localized to coronary arteries, but also to other vascular compartments such as aorta or peripheral veins. Although the pathophysiology of CAE remains largely unknown, it was supposed to represent a variant of coronary atherosclerosis. This review focuses on this controversy of whether CAE and coronary artery disease (CAD) are two manifestations of the same underlying process. There are clear differences between CAD and CAE with respect to cardiovascular risk factors such as diabetes mellitus, and pathogenic steps in disease progress such as inflammation or extracellular matrix remodeling. As this review will underscore, the current knowledge of the field is insufficient to finally clarify the causative interrelation between CAE and CAD. The clinical course and treatment of CAE mainly depends on its coexistence with CAD. When coexisting with CAD, the prognosis and treatment of CAE are the same as for CAD alone. In isolated CAE, prognosis is better and anti-platelet drugs are the mainstay of treatment. Surgical treatment can be considered in selected patients. For clarifying the mechanism underlying CAE, additional clinical, histopathological and pathophysiological investigations are required. In fact, every patient with CAE should be evaluated systematically for pathological changes in other vascular territories, both in the arterial system as well as in the venous system, which might occur in the disease process.
Key words: coronary artery ectasia, coronary artery disease, atherosclerosis
Introduction
The clinical relevance and the pathophysiology of coronary artery ectasia (CAE) have received increasing attention in the last decades. The most commonly used angiographic definition of CAE is the diameter of the ectatic segment measuring more than 1.5 times the diameter of an adjacent healthy reference segment (Fig. 1) [21, 82]. The main coronary angiographic characteristics of CAE are impaired coronary blood flow, delayed antegrade coronary dye filling, segmental back flow phenomenon (milking phenomenon) and stasis with local deposition of dye in dilated coronary segments [48]. CAE was classified into four distinct types by Markis et al. [53]. These are in decreasing order of severity: Type I, diffuse ectasia of two or three vessels; Type II, diffuse disease in one vessel and localized disease in another vessel; Type III, diffuse ectasia of one vessel only; Type IV, localized or segmental ectasia. Although the etiology of CAE is not fully understood, it has been associated with a diverse spectrum of pathologies (Table 1).
Fig. 1.
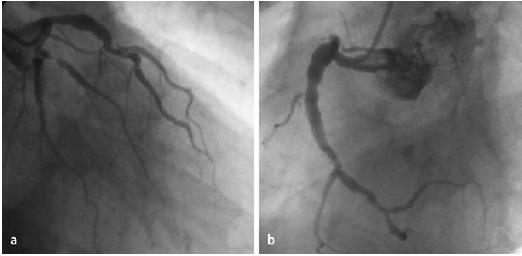
Coronary angiogram showing ectasia affecting the proximal portion of the left anterior descending coronary artery (a) and right coronary artery (b) of the same patient
Table 1.
Pathological entities associated with coronary artery ectasia
| Coronary atherosclerosis [21, 53, 82] |
| Kawasaki disease [18, 39] |
| Congenital [16, 17, 71, 90, 100] |
| Familial hypercholesterolemia [80] |
| Infections [20, 36] |
| Collagen vascular disease |
| Ehler-Danlos syndrome [75] |
| Systemic Lupus erythematosus [54] |
| Polyarteritis Nodosa [83] |
| Sclerodema [15] |
| Juvenile idiopathic arthritis [12] |
| Takayasu’s disease [59] |
| Cardiac lymphoma [31] |
| Cocain use [67] |
The incidence of CAE ranges from 0.2% to 10% [2, 10, 19, 26, 38, 65, 74, 81, 82, 86] with the largest ante mortem series found in the Coronary Artery Surgery Study (CASS) registry (4.9% of 20 087 patients referred for coronary angiography) [82]. The incidence of CAE in an Indian patient cohort with ischemic heart disease has been reported to exceed 10% [74]. It is reasonable to expect that the incidence of CAE reported in the literature overestimates the true frequency in the general population, since the current gold standard for diagnosis of CAE is coronary angiography, and patients referred to coronary angiography are pre-selected.
Cardiovascular risk factors and coronary artery ectasia
Several studies have evaluated the traditional cardiovascular risk factors in patients with CAE and compared them in those with CAD. Giannoglu et al. [32] have reported a male dominance in patients with CAE. This gender difference has been reported previously [38, 81] and supposed due to the lower incidence of CAD in women, although the relation between CAE and CAD is not fully understood [32]. Moreover, the higher likelihood of males having CAE compared with women is generally consistent with a study in Spain in which male gender was demonstrated as an independent factor that increased the hazard of CAE [11]. Age has been shown to constitute a significant factor that is inversely associated with the presence of CAE [32]. A similar finding of significantly younger age among patients with CAE compared to those without CAE has previously been reported [11, 21, 82]. On the other hand, Markis et al. [53] have reported comparable sex and mean age in patients with CAE and patients with CAD. Although contradictory results were reported [21], hypertension and dyslipidemia were also reported to be implicated in the pathogenesis of CAE [10, 31, 53]. Smoking was found to be more common in patients with CAE than in those with CAD [11]. Cocain use was also found to be an independent predictor of CAE in which smoking was excluded from the model [67].
Among cardiovascular risk factors, diabetes mellitus has taken our attention by independently and inversely associating with CAE. Diabetes mellitus is a well known risk factor positively associated with coronary atherosclerosis and its complications, i.e. cardiovascular events [7, 29, 45]. Effects of diabetes mellitus on progression of atherosclerosis have been shown by the demonstration of increased carotid artery intima-media thickness [64, 95]. Androulakis et al. [5] and Bermudez et al. [11] have reported significant independent and inverse association between CAE and diabetes mellitus. Supporting this inverse association, relative demographic data have already been provided in many studies referring to patients with CAE, in whom a low prevalence of diabetes was noticed [81, 94]. Diabetes mellitus is known to promote negative remodeling in the arterial wall and impairs compensatory arterial enlargement during the course of the atherosclerotic process [47, 91]. It is reasonable to expect such an inverse association between diabetes mellitus and CAE. On the other hand, this makes a contradictory situation being positively associated with atherosclerosis and negatively associated with CAE. This contradiction also suggests that the pathogenesis underlying CAE is not simply a variant of coronary atherosclerosis. In accordance with these observations, increased prevalence of abdominal aortic aneurysm (AAA) has been reported in patients without diabetes mellitus [13, 44]. Blanchard et al. [13] have reported that neither clinical hypercholesterolemia nor serum levels of total cholesterol, low density lipoprotein cholesterol, and high density lipoprotein cholesterol is associated with AAA. However they have reported an inverse association between diabetes mellitus and abdominal aortic aneurysm. The results of this study suggest that the risk factors for AAA may differ from those for atherosclerosis and that atherosclerosis per se is not an adequate explanation as the cause of AAA [13].
A rare variant of CAE can be found as a congenital anomaly, independent of any cardiovascular risk factor. Congenital CAE is frequently associated with other cardiac anomalies such as bicuspid aortic valve, aortic root dilatation, ventricular septal defect or pulmonary stenosis [17, 90]. In addition, CAE have been well documented in patients with cyanotic congenital heart disease. These necropsy specimens of dilated and tortuous coronary arteries showed medial smooth muscle cell loss, increased medial collagen and disrupted internal elastic lamina [17].
Comparison of angiographic findings in CAE and CAD
CAE has a high coexistence with CAD. Approximately 85% of patients with CAE also have concomitant stenosing CAD [21, 27, 77, 82]. In patients with concomitant CAD, the right coronary artery is most frequently involved in the ectatic process, followed by the left anterior descending artery and the circumflex artery [21, 82]. The right coronary artery is also the most commonly involved coronary artery in patients with isolated CAE ranging from 45% to 75% [10, 14, 21, 50, 82].
However, with regard to CAD, the LAD is most commonly affected, followed by the right coronary and left circumflex artery [32]. Furthermore involvement of the right coronary artery by the stenotic lesion is the least compared to left anterior descending and left circumflex artery in Demopoulos’s report [21]. In patients with CAD coexisting with CAE, 34% of the stenotic lesions were in the vessels affected by the ectatic process, while 65% were in the non-ectatic vessels [21]. p ]It has also been demonstrated that total CAD severity, expressed as the number of coronary stenotic lesions per patient, is found to be equivalent in patients with CAD coexisting with and without CAE. The two patient groups have a similar incidence of one vessel, two vessel, and three vessel disease [21]. Patients with coronary ectasia and coronary obstructive disease are similar in any respect to those with similar coronary obstructive disease, but without ectasia [53]. On the other hand, Giannoglou et al. found that patients with CAE exhibited higher rates of CAD than those without CAE, a difference that was statistically significant [32]. However, over the 9 year study period, burden of CAD increased markedly in the same study in contrast to CAE whose prevalence remained the same [32].
Underlying pathology of CAE in relation to CAD
The frequent coexistence of CAE with CAD and histopathological findings resembling those of atherosclerosis have led to the conclusion that the mechanism underlying the pathogenesis of CAE is a variant of atherosclerosis. However, there are some differences in the proven association with CAE compared to CAD. These issues are summarized in Table 2.
Table 2.
Differences between CAE and CAD with regard to disease characteristics
| Coronary artery ectasia CAE | Coronary artery disease CAD | |
|---|---|---|
| Inversely associated risk factors | ||
| Diabetes mellitus | + | − |
| Age | + | − |
| More pronounced inflammatory parameters | + | − |
| Changes in extracellular matrix remodeling | ||
| MMP-3 5A polymorphism | + | − |
| Increased plasma levels of MMP-3 | + | − |
| Involvement of coronary artery | ||
| Right coronary artery | + | − |
| Left anterior descending | − | + |
| Increased carotid intima-media thickness | ± | + |
| Decreased endothelium independent dilatation | + | − |
| Possible association with vein involvement | + | ± |
| Possible hazardous effect of nitrate treatment | + | − |
Histological examination has been performed in only a minority of studies [19, 53, 81, 94] typically revealing marked destruction and reduction of the medial elastic fibers with disruption of the internal and external elastic laminae, usually out of proportion to the degree of the intimal involvement. However, as the histopathological characteristics are similar to coronary atherosclerosis, there are obvious similarities between the pathogenesis of CAE and CAD. On the other hand, the loss of musculoelastic arterial wall components in CAE was noticed to be unrelated to local atheromatous burden [10, 94]. Nonatherosclerotic forms of CEA have been described with an intact vessel intima, but with extensive media degeneration (smooth muscle cell replacement by hyalinized collagen) [55, 65]. Thus, a functional loss of the musculoelastic components of the coronary artery media is considered to be the predominant aspect in the pathogenesis of CAE [10, 53, 81].
Celik et al. [14] have shown an association between increased carotid intima-media-thickness and isolated CAE, suggesting that atherosclerosis may be involved in the pathogenesis of isolated CAE. However, they did not study patients with concomitant CAE and CAD. Another ultrasonographic study has shown that patients with CAE coexisting with CAD have a significantly lower carotid intima-media thickness compared those with CAD and without CAE indicating that the mechanism underlying CAE might differ from the ones observed in atherosclerosis [99]. Interestingly, decreased endothelium-independent vasodilatation has been shown in patients with CAE and CAD compared to those with CAD alone [3].
Some authors have suggested NO to play a role in the formation of CAE, which is distinct from atherogenesis. England [24, 25] has reported an increased frequency of CAE in individuals who had been exposed to herbicide sprays. A herbicide containing acetylcholinesterase inhibitor directly stimulates NO production by increasing acetylcholine. It has been proposed that chronic nitrite exposure may cause hyaline degeneration of the coronary artery intimamedia resulting in abnormal coronary dilatation. Johanning et al. [43] and Fukuda et al. [30] have experimentally shown that NO production plays a major role in inflammation and aneurysm pathogenesis. The overexpression of iNOS has been shown in varicose veins together with an increased expression of TGF-β1 and the presence of macrophages [41]. It is therefore interesting to note that the association of peripheral varicose veins with CAE and varicocele has been documented recently [46, 100].
NO production by iNOS occurs primarily by inflammatory cells resulting in high NO levels and toxic products that degrade elastin and disrupt the extracellular matrix [9, 60]. Inhibition of NO has been shown to limit aneurysmal dilatation of the aorta [43].
In accordance with these findings, Turhan et al. have reported increased levels of C-reactive protein and adhesion molecules indicating an increased inflammatory process in patients with isolated CAE compared with both patients with and patients without CAD [87, 88]. Furthermore, regarding the extracellular matrix, Lamblin et al. [50] found that MMP-3 5A/5A genotype was significantly more frequent in patients with CAE than in the control group of CAD patients. Increased MMP-3 activity is known to be associated with structural alterations in the vessel wall through the degradation of extracellular matrix proteins such as proteoglycans, laminin, fibronectin and collagen types III, IV, V and IX [23, 97]. Additionally, MMP-3 activity is increased in the wall of aortic aneurysms [57, 100]. Finally, the recent observation that high circulating levels of MMP-3 are associated with coronary lesions in Kawasaki disease, which is one of the underlying potential etiologies of CAE [73], also supports an important role for MMP-3 in the pathogenesis of CAE.
Arterial remodeling and CAE
Regarding the high coexistence of CAE and CAD, positive remodeling described as enlargement of the area within the external elastic membrane [34] may play a role in the pathogenesis of CAE. Atherosclerotic coronary arteries undergo expansive remodeling to accommodate an increasing plaque burden, especially during early stages of plaque accumulation and following plaque rupture [34, 69]. One can regard CAE as a consequence of extensive positive remodeling. However, this hypothesis remains to be proven.
Systemic vascular involvement in patients with CAE
Williams and Stewart [96] have suggested that, in most patients, coronary ectasia is a diffuse disease of the coronary arteries rather than a localized abnormality of a single arterial segment. Increased ‘thrombolysis in myocardial infarction’ (TIMI) frame count, which is an angiographic definition describing the number of cineangiographic frames from initial contrast opacification of the proximal coronary artery segment to opacification of distal arterial landmarks [33], has been shown in both ectatic and nonectatic coronary arteries [62, 72]. A similar finding has also been reported using magnetic resonance flow velocity [56]. Angiographic signs of turbulent and stagnant flow include delayed antegrade dye filling, a segmental back flow phenomenon and local deposition of dye (stasis) in the dilated coronary segment [48, 53]. Slow flow has also been demonstrated in the non-ectatic vessels of the same patients with CAE. Additionally, Akyurek et al. [4] have demonstrated lower resting blood flow velocity and coronary flow reserve by using the Doppler wire (Flowire) in patients with isolated CAE. Following intracoronary administration of papaverine, a potent hyperemic stimulus, the coronary flow reserve was 1.51 in CAE compared with 2.67 in control arteries (p<0.001), suggesting a combination of epicardial flow disturbances and microvascular dysfunction as the cause of myocardial ischaemia.
A generalized deficit of the wall of the entire arterial system has already been assumed, as associations have been found between CAE and ectasias or aneurysms in other parts of the arterial tree including the abdominal aorta and peripheral arteries [51, 66, 76, 85]. Papadakis et al. [61] reported an association between CAE and aneurysm of the ascending aorta. They have found increased incidence of CAE in patients with aneurysm of ascending aorta (26%) compared to age-matched control group (5%). On the contrary the incidence of CAD is significantly lower in patients with aneurysm of ascending aorta (26%) than in control group (73%). Additionally, Stajduhar et al. [70] reported that all patients with CAE and abdominal aneurysms had obstructive CAD, whereas Papadakis et al. found this in only 38% of patients (8 out of 21) with CAE and ascending aortic aneurysms. A possible explanation for this discrepancy may be that aneurysms of the ascending aorta most often result from the process of cystic medial degeneration, whereas atherosclerotic aneurysms occur infrequently in this segment of the aorta [61].
Coexistence of CAE with venous dilatation has been described, including varicosities of the coronary venous tree [10] and of the leg veins [85]. Recently, increased prevalence of peripheral varicous vein has been reported by Androulakis et al. [6] in patients with CAE compared to those with CAD. Histological examination of the varicosities usually shows degeneration, fragmentation and loss of the medial elastic tissue, fragmentation and reshape of the collagen fiber network, accumulation of extracellular matrix widely separating the hypertrophied medial VSMC and thickening of the intima [58, 68, 84]. Recently, we have shown increased prevalence of varicocele, which is pathologic dilatation of pampiniform plexus in patients with CAE compared to patients with CAD [99]. These findings have also suggested that the mechanism underlying CAE might affect not only the arterial system, but also the venous system in the body. Although some preexisting intimal hyperplasia has been shown in the saphenous veins of the patients who underwent coronary bypass surgery [28], atherosclerosis is known to be a disease of elastic arteries and medium and large size muscular arteries [35]. The coexistence of CAE and venous system dilatation raises the possibility that there might be different pathogenic mechanism or mechanisms between the pathogenesis of CAE and atherosclerosis.
Clinical course and treatment of CAE
The clinical course of CAE mainly depends on whether it is isolated or coexisted with CAD. No significant differences existed between the patients with CAD coexisting with CAE during a follow-up of 5 years [82]. Patients with coronary ectasia and coronary obstructive disease are similar in every respect to those with similar coronary obstructive disease but without ectasia. Demopoulos et al. [21] have reported comparable 2-year survival in patients with and without CAE (96.7% vs 94.8%). Although there is a measurable incidence of previous myocardial infarction, patients with pure ectasia have a good prognosis [21].
Pure ectasia is not completely innocuous, since there is an appreciable incidence of a previous myocardial infarction and angina [21]. On the other hand Baman et al. [8] used more stringent criteria for identifying patients with CAE, reported a significant adverse outcome among 276 patients they studied, with a 5-year survival of 71%.
Treatment modalities of CAE have been well reviewed by Manginas and Cokkinos [52]. Coronary artery bypass grafting has been used for many years for the treatment of significant CAD co-existing with ectatic coronary segments. The presence of thrombus within the CAE and the question of the necessity to remove large aneurysms have led to the introduction of a variety of operative procedures, including proximal and distal ligation, aneurysmorrhectomy and even aneurysm resection [1, 92]. The post-operative outcome, however, was uniformly good [37]. Autologous venous graft-covered stent was applied in a patient with an aneurysm in the right coronary artery. Although the immediate and long-term angiographic evaluation after the covered stent implantation showed complete sealing of the aneurysm without restenosis [79], long-term benefits have not been confirmed by trials.
Unlike the concomitant CAD and CAE, medical treatment for isolated CAE is not readily described. Since patients with isolated CAE or dilated coronaropathy have considerable risk of myocardial infarction due to microemboli and thrombotic occlusion [65], the application of platelet inhibitors as prophylaxis against ischemic syndromes is indispensable in all forms of CEA [48, 89]. Although some authors previously suggested use of anticoagulant drugs in patients with CAE, there is no available data to date [52]. Concerning the medical treatment of CAE, nitroglycerin should be discussed in details. In contrast to the NTG effect in stenotic CAD, where the drug had been proven to restore myocardial ischemia in coronary sinus studies [78], nitroglycerin can lead to aggravation of myocardial ischemia in patients with CAE and without obstructive lesions [48]. Kruger et al. demonstrated that nitroglycerin (0.8 mg) provoked a further significant deterioration of myocardial ischemia and a frank cardiac lactate production. The results of their study strongly suggest that nitroglycerin has no therapeutic benefit in “dilated coronaropathy,” but it may lower the ischemic threshold [48]. Consequently, the administration of nitrates in “dilated coronaropathy” should be avoided. Myocardial ischemia development in patients with isolated CAE has been shown to be depended on heart rate; therefore, a reasonable therapeutic approach might be the administration of beta-blockers due to their negative chronotropic effect and reduction of myocardial oxygen consumption in the absence of vasodilation [40, 48].
Conclusion
Patients with CAE coexisting with CAD do not have any known additional risk compared to those with CAD only. However, even patients with isolated CAE have an enhanced risk for cardiovascular events secondary to slow coronary blood flow, microemboli or thrombosis. Based on the current knowledge on CAE, it is not fully justified to conclude that CAE is a definite variant of coronary atherosclerosis. Regarding the slow progression and complex manifestation pattern of atherosclerosis, CAD at a certain stage might result in aneurysmal dilatation, i.e. CAE formation. This transition is unpredictable based on our current knowledge. Alternatively, the atherosclerotic process may be triggered at sites of CAE.
Because of the discrepancies between CAE and CAD, and because of the association of CAE with other dilating arterial and even venous vascular disease, we tend to regard CAE as a systemic vascular wall abnormality rather then a simple variation of atherosclerosis. In order to further clarify the mechanisms underlying the pathogenesis of CAE, more clinical and histopathological studies are required. In fact, every patient with CAE should be rigorously evaluated for the involvement of other vascular territories in the dilating disease process, both in the arterial as well as in the venous vascular system.
Acknowledgment
The authors wish to thank Dr Hasan Turhan, Inonu University, Malatya, Turkey, for discussion.
References
- 1.Aboud A, Bossert T, Siggusch HH, Gummert J (2006) Surgical treatment o fmultiple atherosclerotic coronary artery aneurysms in a patient with acute myocardial infarction. Clin Res Cardiol 95:1–10 [DOI] [PubMed]
- 2.Aintablian A, Hamby RI, Hoffman I, Kramer RJ (1978) Coronary ectasia: incidence and results of coronary bypass surgery. Am Heart J 96:309–315 [DOI] [PubMed]
- 3.Aksoy Y, Acikgoz N, Sivri N, et al (2006) Decreased nitrate-mediated dilatation in patients with coronary artery ectasia: an ultrasonographic evaluation of brachial artery. Coron Artery Dis 17:365–369 [DOI] [PubMed]
- 4.Akyurek O, Berkalp B, Sayin T, et al (2003) Altered coronary flow properties in diffuse coronary artery ectasia. Am Heart J 145:66–152 [DOI] [PubMed]
- 5.Androulakis AE, Andrikopoulos GK, Kartalis AN, et al (2004) Relation of coronary artery ectasia to diabetes mellitus. Am J Cardiol. 93:1165–1167 [DOI] [PubMed]
- 6.Androulakis AE, Katsaros AA, Kartalis AN, et al (2004) Varicose veins are common in patients with coronary artery ectasia. Just a coincidence or a systemic deficit of the vascular wall? Eur J Vasc Endovasc Surg 27:519–524 [DOI] [PubMed]
- 7.Assmann G, Cullen P, Schulte H (2002) Simple scoring scheme for calculating the risk of acute coronary events based on the 10-year follow-up of the Prospective Cardiovascular Münster (PROCAM) study. Circulation 105:310–315 [DOI] [PubMed]
- 8.Baman TS, Cole JH, Devireddy CM, Sperling LS (2004) Risk factors and outcomes in patients with coronary artery aneurysms. Am J Cardiol 93:1549–1551 [DOI] [PubMed]
- 9.Beckman JS, Koppenol WH (1996) Nitric oxide, superoxide, and peroxynitrite: the good, the bad, and the ugly. Am J Physiol 271:C1424–C1437 [DOI] [PubMed]
- 10.Befeler B, Aranda MJ, Embi A et al (1977) Coronary artery aneurysms: study of their etiology, clinical course, and effect on left ventricular function and prognosis. Am J Med 62:597–607 [DOI] [PubMed]
- 11.Bermúdez P, Palop EL, Martínez- Luengas RL et al (2003) Coronary ectasia: prevalence, and clinical and angiographic characteristics. Revista Espanola De Cardiologia 56:473–479 [DOI] [PubMed]
- 12.Binstadt BA, Levine JC, Nigrovic PA, et al (2005) Coronary artery dilation among patients presenting with systemic- onset juvenile idiopathic arthritis. Pediatrics 116:e89–e93 [DOI] [PubMed]
- 13.Blanchard JF, Armenian HK, Friesen PP (2000) Risk factors for abdominal aortic aneurysm: results of a casecontrol study. Am J Epidemiol 151:575–583 [DOI] [PubMed]
- 14.Celik S, Erdogan T, Kasap H, et al (2007) Carotid intima-media thickness in patients with isolated coronary artery ectasia. Atherosclerosis 190:385–387 [DOI] [PubMed]
- 15.Chaithiraphan S, Goldberg E, O’Reilly M (1973) Multiple aneurysms of coronary artery in sclerodermal heart disease. Angiology 24:86–93 [DOI] [PubMed]
- 16.Chakrabarti S, Thomas E, Wright JG, Vettukattil JJ (2003) Congenital coronary artery dilatation. Heart 89:595–596 [DOI] [PMC free article] [PubMed]
- 17.Chugh R, Perloff JK, Fishbein M, Child JS (2004) Extramural coronary arteries in adults with cyanotic congenital heart disease. Am J Cardiol 94:1355–1357 [DOI] [PubMed]
- 18.Dahdah NS, Fournier A, Jaeggi E, et al (1999) Segmental myocardial contractility versus perfusion in Kawasaki disease with coronary arterial aneurysm. Am J Cardiol 83:48–51 [DOI] [PubMed]
- 19.Daoud AS, Pankin D, Tulgan H, Florentin RA (1963) Aneurysms of the coronary artery: report of ten cases and review of the literature. Am J Cardiol 11:228–237 [DOI] [PubMed]
- 20.Davidson A, Eshaghpour E, Young N, Mintz GS (1991) Late thrombosis of a coronary artery mycotic aneurysm. Am Heart J 121:1549–1550 [DOI] [PubMed]
- 21.Demopoulos V, Olympios C, Fakiolas C, et al (1997) The natural history of aneurysmal coronary artery disease. Heart 78:136–141 [DOI] [PMC free article] [PubMed]
- 22.Dietl RH, Seggewiss H, Ohlmeier H, et al (1996) Congenital coronary artery aneurysm: a rare cause of acute myocardial infarct. Z Kardiol 85(3):188–192 [PubMed]
- 23.Dollery CM, McEwan JR, Henney AM (1995) Matrix metalloproteinases and cardiovascular disease. Circ Res 77:863–868 [DOI] [PubMed]
- 24.England JF (1981) Herbicides and coronary artery ectasia. Med J Aust 1:140 [DOI] [PubMed]
- 25.England JF (1981) Herbicides and coronary artery ectasia. Med J Aust 2:260 [DOI] [PubMed]
- 26.Falsetti HL, Carrol RJ (1976) Coronary artery aneurysm: a review of the literature with a report of 11 new cases. Chest 69:630–636 [DOI] [PubMed]
- 27.Farto-e-Abreu P, Mesquita A, Silva JA, Seabra Comez R (1993) Coronary artery ectasia: clinical and angiographic characteristics and prognosis. Rev Port Cardiol 12:305–310 [PubMed]
- 28.Friedl R, Li J, Schumacher B, et al (2004) Intimal hyperplasia and expression of transforming growth factor- beta1 in saphenous veins and internal mammary arteries before coronary artery surgery. Ann Thorac Surg 78:1312–1318 [DOI] [PubMed]
- 29.Fujiwara S, Emoto M, Komatsu M, et al (2003) Arterial wall thickness is associated with insulin resistance in type 2 diabetic patients. J Atheroscler Thromb 10:246–252 [DOI] [PubMed]
- 30.Fukuda S, Hashimoto N, Naritomi H, et al (2000) Prevention of rat cerebral pseudoaneurysm formation by inhibition of nitric oxide synthase. Circulation 101:2532–2538 [DOI] [PubMed]
- 31.Gardiner DS, Lindop GB (1989) Coronary artery aneurysm due to primary cardiac lymphoma. Histopathology 15:537–540 [DOI] [PubMed]
- 32.Giannoglou GD, Antoniadis AP, Chatzizisis YS, et al (2006) Prevalence of Ectasia in Human Coronary Arteries in Patients in Northern Greece Referred for Coronary Angiography. Am J Cardiol 98:314–318 [DOI] [PubMed]
- 33.Gibson CM, Cannon CP and Daley WL, et al (1996) TIMI frame count: a quantitative method of assessing coronary artery flow. Circulation 93:879–888 [DOI] [PubMed]
- 34.Glagov S, Weisenberg E, Zarins CK, et al (1987) Compensatory enlargement of human atherosclerotic coronary arteries. N Engl J Med 316:1371–1375 [DOI] [PubMed]
- 35.Goran KH, Jan H (2001) Pathogenesis of atherosclerosis. In: Crawford MH, DiMarco JP (eds) Cardiology. Mosby, London Edinburg, pp 1–22
- 36.Harada H, Yamamoto N, Ueda M, Abe T (1997) A clinical investigation of Bentall’s operation for annuloaortic ectasia in the elderly. Kyobu Geka 50(8 Suppl):632–636 [PubMed]
- 37.Harandi S, Johnston SB, Wood RE, Roberts WC (1999) Operative therapy of coronary arterial aneurysm. Am J Cardiol 83:1290–1293 [DOI] [PubMed]
- 38.Hartnell GG, Parnell BM, Pridie RB (1985) Coronary artery ectasia: its prevalence and clinical significance in 4993 patients. Br Heart J 54:392–395 [DOI] [PMC free article] [PubMed]
- 39.Hiraishi S, Yashiro K, Oguchi K, et al (1981) Clinical course of cardiovascular involvement in the mucocutaneous lymph node syndrome-relation between the clinical signs of carditis and development of coronary arterial aneurysm. Am J Cardiol 47:323–330 [DOI] [PubMed]
- 40.Jackson G, Atkinson L and Oram S (1977) Improvement of myocardial metabolism in coronary arterial disease by beta-blockade. Br Heart J 39:829–833 [DOI] [PMC free article] [PubMed]
- 41.Jacob T, Hingorani A, Ascher E (2005) Overexpression of transforming growth factor-beta1 correlates with increased synthesis of nitric oxide synthase in varicose veins. J Vasc Surg 41:523–530 [DOI] [PubMed]
- 42.Johanning JM, Armstrong PJ, Franklin DP, et al (2002) Nitric oxide in experimental aneurysm formation: early events and consequences of nitric oxide inhibition. Ann Vasc Surg 16:65–72 [DOI] [PubMed]
- 43.Johanning JM, Franklin DP, Han DC, et al (2001) Inhibition of inducible nitric oxide synthase limits nitric oxide production and experimental aneurysm expansion. J Vasc Surg 33:579–586 [DOI] [PubMed]
- 44.Kang SS, Littooy FN, Gupta SR, et al (1999) Higher prevalence of abdominal aortic aneurysms in patients with carotid stenosis but without diabetes. Surgery 126:687–691 [PubMed]
- 45.Kannel WB, McGee DL (1979) Diabetes and cardiovascular disease: the Framingham study. JAMA 241:2035–2038 [DOI] [PubMed]
- 46.Kilic S, Aksoy Y, Sincer I, et al (2007) Cardiovascular evaluation of young patients with varicocele. Fertility and Sterility (published online on Feb 16) [DOI] [PubMed]
- 47.Kornowski R, Mintz GS, Lansky J, et al (1998) Paradoxic decreases in atherosclerotic plaque mass in insulintreated diabetic patients. Am J Cardiol 81:1298–1304 [DOI] [PubMed]
- 48.Krueger D, Stierle U, Herrmann G, et al (1999) Exercise-induced myocardial ischaemia in isolated coronary artery ectasias and aneurysms (‘Dilated Coronaropathy’. J Am Coll Cardiol 34:1461–1470 [DOI] [PubMed]
- 49.Lam CSP and Ho KT (2004) Coronary artery ectasia: a ten year experience in a tertiary hospital in Singapore, Ann Acad Med Singapore 33:419–422 [PubMed]
- 50.Lamblin N, Bauters C, Hermant X, et al (2002) Polymorphisms in the promoter regions of MMP-2, MMP-3, MMP-9 and MMP-12 genes as determinants of aneurysmal coronary artery disease. J Am Coll Cardiol 40:43–48 [DOI] [PubMed]
- 51.LaMendola CL, Culliford AT, Harris LJ, Amendo MT (1990) Multiple aneurysms of the coronary arteries in a patient with systemic aneurysmal disease. Ann Thorac Surg 49:1009–1010 [DOI] [PubMed]
- 52.Manginas A, Cokkinos DV (2006) Coronary artery ectasias: imaging, functional assessment and clinical implications. Eur Heart J 27:1026–1031 [DOI] [PubMed]
- 53.Markis JE, Joffe CD, Cohn PF, Feen et al (1976) Clinical significance of coronary arterial ectasia. Am J Cardiol 37:217–222 [DOI] [PubMed]
- 54.Matayoshi AH, Dhond MR, Laslett LJ (1999) Multiple coronary aneurysms in a case of systemic lupus erythematosus. Chest 116:1116–1168 [DOI] [PubMed]
- 55.Mattern AL, Baker WP, McHale JJ, Lee DE (1972) Congenital coronary aneurysms with angina pectoris and myocardial infarction treated with saphenous vein bypass graft. Am J Cardiol 30:906–909 [DOI] [PubMed]
- 56.Mavrogeni SI, Manginas A, Papadakis E, et al (2005) Coronary flow evaluation by TIMI frame count and magnetic resonance flow velocity in patients with coronary artery ectasia. J Cardiovasc Magn Reson 7:545–550 [DOI] [PubMed]
- 57.Newman KM, Ogata Y, Malon AM, et al (1994) Identification of matrix metalloproteinases 3 (stromelysin-1) and 9 (gelatinase B) in abdominal aortic aneurysm. Arterioscler Thromb 14:1315–1320 [DOI] [PubMed]
- 58.Niebes P (1996) Vessel wall modification in venous pathology. Application to the study of phlebotonic drugs. Int Angiol 15:88–92 [PubMed]
- 59.Noma M, Kikuchi Y, Yoshimura H, et al (1993) Coronary ectasia in Takayasu’s arteritis. Am Heart J 126:459–461 [DOI] [PubMed]
- 60.Paik DC, Ramey WG, Dillon J, Tilson MD (1997) The nitrite/elastin reaction: implication for in vivo degenerative effects. Connect Tissue Res 36:241–251 [DOI] [PubMed]
- 61.Papadakis MC, Leontiadis E, Manginas A, et al (2004) Frequency of coronary artery ectasia in patients undergoing surgery for ascending aortic aneurysms. Am J Cardiol 94:1433–1435 [DOI] [PubMed]
- 62.Papadakis MC, Manginas A, Cotileas P, et al (2001) Documentation of slow coronary flow by the TIMI frame count in patients with coronary ectasia. Am J Cardiol 88:1030–1032 [DOI] [PubMed]
- 63.Pasterkamp G, Schoneveld AH, van der Wal AC, et al (1998) Relation of arterial geometry to luminal narrowing and histologic markers for plaque vulnerability: the remodeling paradox. J Am Coll Cardiol 32:655–662 [DOI] [PubMed]
- 64.Rajaram V, Pandhya S, Patel S, et al (2004) Role of surrogate markers in assessing patients with diabetes mellitus and the metabolic syndrome and in evaluating lipid-lowering therapy. Am J Cardiol 93:32C–48C [DOI] [PubMed]
- 65.Rath S, Har-Zahav Y, Battler A, et al (1985) Fate of non-obstructive aneurysmatic coronary artery disease: angiographic and clinical follow-up report. Am Heart J 109:785–791 [DOI] [PubMed]
- 66.Ruttimann M, Perez JP, Richard R, et al (1997) Intracranial aneurysm and coronary ectasia. Presse Med 26:1141–1143 [PubMed]
- 67.Satran A, Bart BA, Henry CR, et al (2005) Increased prevalence of coronary artery aneurysms among cocaine users.Circulation 111:2424–2429 [DOI] [PubMed]
- 68.Schoen FJ and Cotran RS (1999) Blood vessels (varicose veins) In: Robbins SL, Cotran RS, Kumar V (eds) Pathologic basis of disease (6th ed), Saunders, London, pp 529
- 69.Schoenhagen P, Ziada KM, Kapadia SR, et al (2000) Extent and direction of arterial remodeling in stable versus unstable coronary syndromes: an intravascular ultrasound study. Circulation 101:598–603 [DOI] [PubMed]
- 70.Schoenhagen P, Vince DG, Ziada K, et al (2000) Increased presence of matrix-metalloproteinase 3 in human coronary lesions with positive arterial remodeling (abstr). J Am Coll Cardiol 35 Suppl A:58A–59A
- 71.Seabra-Gomes R, Somerville J, Ross DN, et al (1974) Congenital coronary artery aneurysms. Br Heart J 36:329–335 [DOI] [PMC free article] [PubMed]
- 72.Senen K, Yetkin E, Turhan H, et al (2004) Increased thrombolysis in myocardial infarction frame counts in patients with isolated coronary artery ectasia. Heart Vessels 19:23–26 [DOI] [PubMed]
- 73.Senzaki H, Masutani S, Kobayashi J, et al (2001) Circulating matrix metalloproteinases and their inhibitors in patients with Kawasaki disease. Circulation 104:860–863 [DOI] [PubMed]
- 74.Sharma SN, Kaul U, Sharma S, et al (1990) Coronary arteriographic profile in young and old Indian patients with ischaemic heart disease: a comparative study. Indian Heart J 42:365–369 [PubMed]
- 75.Shiro I, Bannerman RM, Graf CJ, Brennan JC (1969) Ehlers–Danlos syndrome with multiple arterial lesions. Am J Med 47:967–977 [DOI] [PubMed]
- 76.Stajduhar KC, Laird JR, Rogan KM and Wortham DC (1993) Coronary arterial ectasia: increased prevalence in patients with abdominal aortic aneurysm as compared to occlusive atherosclerotic peripheral vascular disease. Am Heart J 125:86–92 [DOI] [PubMed]
- 77.Starc R, Janezic AS, Cijan A (1991) Angiographic evidence of coronary arteryectasia: our experience. Cor Vasa 33:288–293 [PubMed]
- 78.Steele RJ, Burggraf GW and Parker JO (1975) Effects of isosorbide dinitrate on response to atrial pacing in coronary heart disease. Am J Cardiol 33:206–11 [DOI] [PubMed]
- 79.Stefanadis C, Toutouzas K, Tsiamis E, Toutouzas P (2000) New stent design for autologous venous graft-covered stent preparation: first human application for sealing of a coronary aneurysm. Catheter Cardiovasc Interv 55:222–227 [DOI] [PubMed]
- 80.Sudhir K, Ports TA, Amidon TM, et al (1995) Circulation. Increased prevalence of coronary ectasia in heterozygous familial hypercholesterolemia 91(5):1375–1380 [DOI] [PubMed]
- 81.Swanton RH, Thomas ML, Coltart DJ, et al (1978) Coronary artery ectasia: a variant of occlusive coronary arteriosclerosis. Br Heart J 40:393–400 [DOI] [PMC free article] [PubMed]
- 82.Swaye PS, Fisher LD, Litwin P, et al (1983) Aneurysmal coronary artery disease. Circulation 67:134–138 [DOI] [PubMed]
- 83.Tang PHL, Segal AJ (1970) Polyarteritis nodosa of infancy: fatal late complications. JAMA 217:666–670 [PubMed]
- 84.Travers P, Brookes CE, Evans J et al (1996) Assessment of wall structure and composition of varicose veins with reference to collagen, elastin and smooth muscle content. Eur J Vasc Endovasc Surg 11:230–237 [DOI] [PubMed]
- 85.Triantafillidi H, Rizos I, Androulakis A, et al (2001) Coronary artery ectasia, aneurysm of the basilar artery and varicose veins. Common presentation or generalized defect of the vessel wall? Angiology 52:287–291 [DOI] [PubMed]
- 86.Tunick PA, Slater J, Kronzon I, Glassman E (1990) Discrete atherosclerotic coronary artery aneurysms: a study of 20 patients. J Am Coll Cardiol 15:279–282 [DOI] [PubMed]
- 87.Turhan H, Erbay AR, Yasar AS, et al (2004) Comparison of C-reactive protein levels in patients with coronary artery ectasia ‘ vs ’ patients with obstructive coronary artery disease. Am J Cardiol 94:1303–1306 [DOI] [PubMed]
- 88.Turhan H, Erbay AR, Yasar AS, et al (2005) Plasma soluble adhesion molecules; intercellular adhesion molecule- 1, vascular cell adhesion molecule- 1 and E-selectin levels in patients with isolated coronary artery ectasia. Coron Artery Dis 16:45–50 [DOI] [PubMed]
- 89.Turhan H, Yetkin E (2007) What is the plausible strategy for the management of patients with isolated coronary artery ectasia and myocardial ischemia? Int J Cardiol 117:285–286 [DOI] [PubMed]
- 90.Ucar T, Atalay S, Tekin M, Tutar E (2005) Bilateral coronary artery dilatation and supravalvular pulmonary stenosis in a child with noonan syndrome. Pediatr Cardiol 26:848–850 [DOI] [PubMed]
- 91.Vavuranakis M, Stefanadis C, Toutouzas K, et al (1997) Impaired compensatory coronary artery enlargement in atherosclerosis contributes to the development of coronary artery stenosis in diabetic patients. An in vivo intravascular ultrasound study. Eur Heart J 18:1090–1094 [DOI] [PubMed]
- 92.Vijayanagar R, Shafii E, DeSantis M, et al (1994) Surgical treatment of coronary aneurysms with and without rupture. J Thorac Cardiovasc Surg 107:1532–1535 [PubMed]
- 93.Vine N, Powell JT (1991) Metalloproteinases in degenerative aortic disease. Clin Sci (Colch) 81:233–239 [DOI] [PubMed]
- 94.Virmani R, Robinowitz M, Atkinson JB, et al (1986) Acquired coronary arterial aneurysms: an autopsy study of 52 patients. Hum Pathol 17:575–583 [DOI] [PubMed]
- 95.Wagenknecht LE, Zaccaro D, Espeland MA, et al (2003) Diabetes and progression of carotid atherosclerosis: the insulin resistance atherosclerosis study. Arterioscler Thromb Vasc Biol 23:1035–1041 [DOI] [PubMed]
- 96.Williams MJA, Stewart RAH (1994) Coronary artery ectasia: local pathology or diffuse disease. Cathet Cardiovasc Diagn 33:116–119 [DOI] [PubMed]
- 97.Ye S, Eriksson P, Hamsten A, et al (1996) Progression of coronary atherosclerosis is associated with a common genetic variant of the human stromelysin-1 promoter which results in reduced gene expression. J Biol Chem 271:13055–13060 [DOI] [PubMed]
- 98.Yetkin E, Acikgoz N, Aksoy Y, et al (2005) Decreased carotid intima–media thickness in patients with coronary artery ectasia compared to patients with coronary artery disease. Coron Artery Dis 16:495–498 [DOI] [PubMed]
- 99.Yetkin E, Kilic S, Acikgoz N, et al (2005) Increased prevalence of varicocele in patients with coronary artery ectasia. Coron Artery Dis 16:261–264 [DOI] [PubMed]
- 100.Zankl AR, Schumacher H, Katus HA, et al (2007) Pathology, natural history and treatment of abdominal aortic aneurysms. Clin Res Cardiol 96:1–12 [DOI] [PubMed]


