Invasive meningococcal disease (IMD) is an epidemic infectious disease highly influenced by climatic factors. Climate plays an important role in both the spatial distribution of the disease and in the seasonality of IMD as seen all over the world (1). It is mentioned as one of the infectious diseases likely to be affected by climate change in the Fourth Assessment report of the Intergovernmental Panel on Climate Change (IPCC) (2).
IMD is an airborne disease with humans as its only reservoir. Global warming will change precipitation levels with a combination of more severe droughts in some areas and more frequent heavy precipitation events in others (2), and these are events likely to affect the incidence and geographical distribution of IMD (1). Effects suspected to be the result of climate change are already evident on the distribution of IMD epidemics in Africa (1, 3).
Research in the field of infectious diseases and climate has focused on vector-borne diseases like malaria and dengue fever (1, 4–8). Less is known about the effects of climate on airborne diseases like IMD.
The aim of this review is to give an overview of the current knowledge of how climate affects IMD and to more thoroughly investigate the climate research concerning IMD that has been published in the last decade.
The disease and its prevention
IMD includes meningococcal septicaemia and meningococcal meningitis. The disease is prevalent all over the world. It is caused by Neisseria meningitidis, a gram-negative coccoid bacteria. Treatment of IMD is still not a major problem as N. meningitidis is sensitive to a number of antibiotics, although betalactamase resistance is seen in some parts of the world (9–12). Despite treatment, 4–17% of the patients die (13–18) and 8–20% of the survivors will suffer from lifelong sequelae like deafness, cognitive impairment and other central nervous system complications (19–22). The age groups most susceptible to the disease are young children, adolescents and young adults (23, 24).
N. meningitidis can be divided into serogroups on the basis of polysaccharide capsular antigens. The major pathogenic serogroups are A, B, C, W135, X and Y (24, 25). There are differences between the serogroups, both in virulence and in their capacity to cause epidemics. Large-scale epidemics are mainly caused by serogroup A, although serogroups W135 and C have also been implicated in epidemics. Smaller outbreaks and singular cases of the disease are more commonly caused by serogroups B and C and less frequently by other serogroups (24, 26, 27).
IMD is transmitted through respiratory secretion or saliva. N. meningitidis is found mainly in the upper respiratory tract (URT). Acquisition of the bacteria can either be transient or result in colonisation of the URT epithelium (carriage) or in invasive disease (24). The epidemiology of IMD is complex due to the great number of symptom-free carriers of the bacteria. In populations studied, 2–70% of people have been found to be carriers of the bacteria in their airways (24, 28–30). In Africa, carrier rates have been shown to be higher during epidemics than in the endemic situation (24, 28, 30, 31) and less frequent in small children than in adolescents and adults (24, 31). Carriage of Neisseria plays an important role in the epidemiology of the disease, a role that is still not well understood (29, 32).
Vaccines exist for serogroups A, C, W135, X and Y but no commercial vaccine has yet been produced for serogroup B. Limitations of the vaccines are short duration of immunity, 3–5 years, low immunogenity in children under two years and no effect on carriage of the bacteria (24, 25). New conjugate vaccines have been developed for serogroups A and C, with prolonged immunity, better immunological effect in young children and with protective effects against carriage (24, 33–36).
Epidemiology of invasive meningococcal disease (IMD)
Meningitis belt
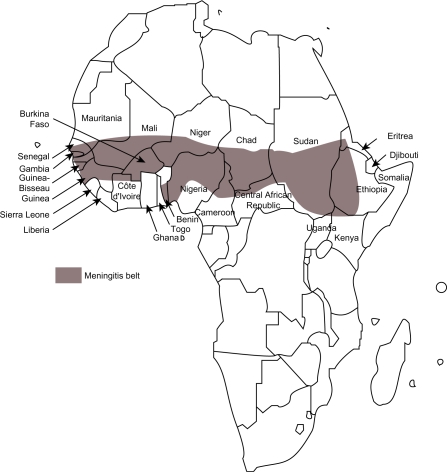
In 1963, the French physician Lapeyssonnie described a geographically well-defined area in Sub-Saharan Africa with an exceptionally high incidence of meningococcal meningitis (37). This area, the classical meningitis belt (Fig. 1), has seen epidemics of the disease at intervals of 5–10 years during the last 100 years (38). The first well-described epidemic in Africa was in Nigeria in 1905 (38). The meningitis belt stretches from Ethiopia and the Sudan in East Africa to Mali, Senegal and Guinea in the west (38). The most common cause of these epidemics is N. meningitidis serogroup A (37, 38). In the epidemic years of 2002–2003, serogroup A was substituted by serogroup W135 that caused a large epidemic with its main focus in Burkina Faso (39–42), but since then serogroup A has been the dominant pathogen again (38). In the 2002–2003 serogroup W135 epidemic, as well as in a serogroup A epidemic starting in the Sudan and Chad in 1988, it has been demonstrated that one likely source of introduction of new meningococcal bacterial strains in the meningitis belt is pilgrims returning from the Hajj in Saudi Arabia (43–45).
Fig. 1.
The classic African meningitis belt.
Source: Control of epidemic meningococcal disease. WHO practical guidelines. 2nd edition 1998 WHO/EMC/BAC/98.3. Available from: http://www.who.int/csr/resources/publications/meningitis/whoemcbac983.pdf
In the last decades, African countries south of the belt have experienced large IMD epidemics and there has been an extension of the belt into countries like Togo, Cameroon, Côte d'Ivoire and Benin (3, 46, 47). In East Africa, Kenya, Uganda and Tanzania have suffered large-scale IMD epidemics (3, 18, 38, 47–49). The health impact of IMD in Africa makes the disease a main focus for interventions by health agencies in the countries of the meningitis belt. During epidemics in the 1990s an incidence of 1,000 cases per 100,000 was seen (24). An estimated 200,000 people were hit by the disease in the serogroup A epidemic of 1996 (32, 49).
Outside the belt
IMD is a global disease seen in most countries of the world. The incidence of the disease is however lower than in the meningitis belt. In Europe it ranges between 0.2 and 14 cases per 100,000 and 0.2–4 per 100,000 in USA (51). In most countries the disease is endemic with small outbreaks, mainly in crowded settings like schools and military establishments and is mainly caused by serogroups B and C (24, 52). Changes in the epidemiology of IMD due to the introduction of the serogroup C conjugate vaccine are expected to be seen in the future (51). Infrequently epidemics of serogroup A meningitis have been seen outside Africa, for example, in China (53), Nepal (54), India (55) and Russia (56).
Climate and invasive meningococcal disease (IMD)
Two main features of the IMD are influenced by climatic factors: the geographical distribution of high disease incidence with large epidemics in the meningitis belt and the seasonality of the disease seen globally. During the last decade, with growing interest in the effects of climate on health, a number of studies, spatial as well as temporal, of climatic effects on IMD have been conducted and models for predicting epidemics have been proposed. The majority of these studies have concerned IMD in Africa (3, 50, 58–62).
Geographical distribution
Lapeyssonnie described the boundaries of the meningitis belt as equivalent to the annual rainfall isohyets of 300 mm in the north, and 1,100 mm in the south, thereby indicating that climatic factors are involved in the geographical distribution (37). Subsequent research in the meningitis belt have found that the optimal climate for transmission of the disease is the savannah climate south of the Sahel, with an annual precipitation index of 300–1,100 mm, extremely dry but warm winter seasons and a relatively abrupt onset of the rainy season (3, 57). During the last decade climate research concerning the geographical distribution of IMD in Africa has made important progress and has resulted in risk mapping models.
Risk mapping
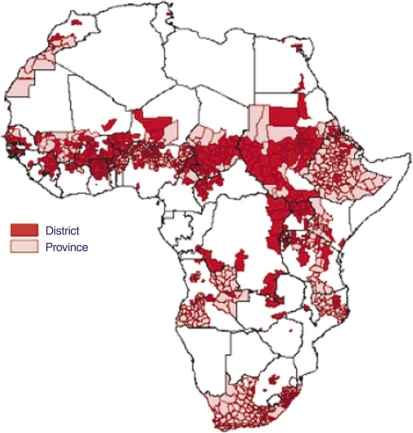
In a study by Molesworth and colleagues (3) in 2002, the spatial distribution of IMD epidemics in Africa occurring between 1980 and 1999 was mapped using a dataset with published and unpublished epidemics and surveillance data of number of cases reported to the WHO (Fig. 2). Maps showing the location and maximum incidence rates of 144 epidemics in Africa were constructed. The maps demonstrated that the risk of IMD epidemics is almost as high in many geographical areas south of the meningitis belt, like the Rift Valley and the Great Lakes region, but that the maximum number of cases is higher in the countries in the belt as compared to countries outside the belt. In accordance with the suggested boundaries of the meningitis belt proposed by Lapeyssonnie 40 years previously, the risk map also demonstrated a striking association between IMD epidemics and the 300–1,100 rainfall isohyets in all of Africa, also outside the belt.
Fig. 2.
Risk map for IMD. Districts and provinces experiencing meningococcal meningitis epidemics in Africa 1980–1999. After Molesworth et al. (3). Available from: http://www.liv.ac.uk/researchintelligence/issue15/graphics/15/meningitis_01.gif
The risk models constructed by Molesworth and colleagues have been further developed to investigate the environmental factors driving the IMD epidemics in Africa. In a study by Molesworth and colleagues published in 2003 (58), they analysed the same IMD epidemic and surveillance data as in (3) together with information on climate variables like absolute humidity, dust and rainfall, and data on land-cover type and population density. They found that absolute humidity and land-cover type were the climatic factors that best correlated to IMD epidemics. Among other factors found to be independently associated with IMD epidemics, dust was especially interesting as the dustiness in the meningitis belt increased dramatically due to the Sahelian droughts of the 1970s and 1980s (58). The model also demonstrated that climate zones not having distinct wet and dry seasons, such as deserts and the humid and often forested parts of coastal and central Africa, are less likely to have epidemics than those with contrasting seasons like the semi-arid savannah and grassland found in the Sahel and eastern and southern Africa.
The risk model of Molesworth and colleagues was evaluated in a prospective study of IMD epidemics in Africa 2002–2004 by Savory and colleagues (59). They found that only 59% of the 71 epidemics that occurred during the time period were located within the meningitis belt. Most of the new epidemic districts were however located in areas geographically contiguous to the belt. The epidemics in the meningitis belt had a significantly higher mean number of cases than epidemics outside the belt. The authors concluded that there is an extension of the meningitis belt particularly into districts in Côte d'Ivoire, Togo, the Central African Republic and Cameroon (59). The risk mapping of IMD provides a tool for priority planning of vaccination campaigns, for further research on climate effects on IMD in Africa and a model that can be suitable for the development of early warning systems (EWS) for the disease. It will also be an important instrument for surveillance of the impact of future climate change (57).
Seasonality
Lapeyssonnie also described the seasonality of the disease, with the peak of epidemics during the dry winter season. Frequently the epidemics ceased when the rainy season started, to be resumed in the dry season of the next year (37, 63, 64).
Subsequent studies have suggested low absolute humidity (58) and the dry Harmattan winter winds (62) as the main climatic driver behind the seasonality in the meningitis belt. Sultan and colleagues found a strong correlation between the maximum Harmattan wind index and the onset of IMD epidemics in a study in Mali during 1994–2002 (62). They concluded that the seasonal rise in meningitis cases corresponded to large-scale atmospheric phenomena associated with the Sahelian dry season (62).
The peak of the IMD epidemics comes when the absolute humidity is at its lowest and the epidemics subside with rising humidity before the annual rain period begins (28). In a study in Niger, Jackou-Boulama and colleagues (65) found a negative correlation between rainfall and IMD incidence. The IMD incidence fell when the rain season began. In contrast, incidence of meningococcal carriage has been found to rise with increasing atmospheric humidity in a study by Mueller and colleagues (66) where they investigated carriage rates in the non-epidemic year of 2003 in Burkina Faso. This result stresses the complex role of carriers in the understanding of IMD.
Many countries outside Africa, especially in the Northern hemisphere, show a similar seasonal incidence of the disease as in the meningitis belt (67–71) with peak incidence during the dry winter months, but the relation between high incidence and low humidity seen in the meningitis belt is not a consistent finding outside the belt. In New Zealand a study showed that the incidence of IMD increased with increasing humidity and cooler temperatures, but declined, as in the meningitis belt, with heavy rain (72). UK studies have shown that IMD outbreaks are correlated with high humidity and rapid changes in relative humidity before outbreaks (73, 74).
The proposed biological explanation for the climate effects on IMD is that low humidity, dry winds and high levels of dust in the air injures the barriers of the URT mucosa, thus facilitating IMD (18, 48). N. meningitidis can more easily penetrate injured mucosal membranes and access the blood stream and the meninges, where it causes disease (18). The mechanisms of interaction between N. meningitidis and the mucosal epithelial cells are well known (18, 75), but to my knowledge no studies concerning the effects of climatic factors on the pathogenesis and transmission of N. meningitidis in vivo have been done, perhaps mainly due to the lack of a reliable animal model for the bacteria (76).
Early warning systems (EWSs)
One of the main aims of EWSs for IMD is to predict epidemics so that mass vaccination can begin in time to curb the spread of disease (57, 59, 61). One tool for identifying epidemics is the IMD case number thresholds presented by WHO as an EWS in the year 2000. It distinguishes between the usual annual rise in IMD incidence and epidemics (77). To find climatic factors that can predict IMD epidemics, Thomson and colleagues investigated a large number of environmental factors in a study in Burkina Faso, Niger, Mali and Togo (61). They found that land-cover type (savannah, grassland and barren areas) was associated with IMD incidence, rainfall and dust. Areas with barren land had the lowest IMD incidence and highest dust levels, and in savannah areas the rainy season started earlier and was more intense than in grassland and barren areas. They could also demonstrate that excess dust in October and a rainfall deficit in January were the best predictors for epidemics. Annual meningitis incidence anomalies (e.g. early cases) at district level were significantly correlated with monthly climate anomalies for rainfall and dust in the pre, post and epidemic seasons, with stronger relationship in savannah areas (57).
The performance of an EWS based on climate indices has recently been investigated in a study by Yaka and colleagues (60). They identified Burkina Faso and Niger as the two countries with the highest risk of IMD epidemics using data from a previously published study by Broutin and colleagues (50). By computing meningitis cases in the two countries with climate variables, they found a significant correlation between IMD incidence and climatic factors during the winter period, October–January, in Niger. In Burkina Faso the correlation was not significant. This study stresses the importance of including other variables than climate in future EWSs to be able to predict epidemics.
Climate is a driving factor in the seasonality of the disease and in the geographical distribution of IMD in the meningitis belt, but climatic factors alone cannot explain the high disease incidence in the meningitis belt or the periodicity of epidemics. Immunity in the population, carriage rates, vaccination coverage, social interactions and the introduction of new strains of meningococci are other main factors to be considered to fully understand the dynamics of IMD in the meningitis belt (57, 61).
Discussion
The epidemiology of IMD is closely related to climatic factors like air humidity, rainfall and dust (3, 58, 61, 65). The disease is a special challenge to research in the field of disease and climate change as it is spread all over the world and in almost all types of climate zones. The meningitis belt in the Sahel region of Africa has the highest IMD incidence and large epidemics mainly caused by serogroup A meningococci is one of the main health issues for the countries in the belt (30, 78).
Pre-epidemic vaccination against serogroups A and W135, the most common serogroups causing epidemics in the meningitis belt, is feasible, but the vaccine effect only lasts for three to five years, although the new conjugate vaccines now in the pipeline may improve that duration (79, 80). To keep the population constantly immune to the disease is too costly and demands a vaccination infrastructure that does not yet exist in the countries involved. Mass vaccination in the face of a current epidemic is often done too late (81).
In Africa, 350 million people lives in areas at risk for IMD epidemics (57, 58)s. Only 40 million doses of the new conjugate A vaccine will be available during the first years. Risk models could guide selection of priority areas and demonstrate vaccination efficacy through surveillance. They could also provide support for the control of epidemics in areas where the population has not had access to new vaccines (57).
Meteorological surveillance offers a possibility for developing EWSs for epidemic preparedness (55–59). With the aid of EWSs, vaccination could be made more effective. Attempts at EWSs have been promising but need further refinement (55–57). For future predictive models to be effective, meteorological data must be included in computations together with data on population immunity, changes in population structure and the dynamics of N. meningitidis carriers (57, 61). There also needs to be an improvement of disease surveillance data and weather forecasting data in the African continent (57). It is also crucial that health authorities in the countries at most risk for IMD epidemics are interested in the implementation of EWSs and that economic resources are allocated for them (82, 83, 85). In 2008, the University Corporation for Atmospheric Research (UCAR), working with an international team of health and weather organisations, launched the Meningitis forecast project. The aim of the project is to provide long-term weather forecasts to medical officials in Africa to help reduce outbreaks of meningitis. The forecasts will enable local health providers to target vaccination programmes more effectively (see http://www.ucar.edu/news/releases/2008/meningitis.jsp).
Future climate change and invasive meningococcal disease (IMD)
In the 21st century the main projected climate changes in Africa are warming, especially in sub-tropical regions and a decrease in annual rainfall, especially in North Africa and the northern parts of Sahara. By 2080, an increase of 5–8% of arid and semi-arid land in Africa is projected (78). The Sahel, where the meningitis belt is situated, is one of the regions in Africa most vulnerable to climate change. The factors that determine the southern boundary of t he Sahara and rainfall in the Sahel have attracted special interest among climate scientists because of the extended drought experienced in this region in the 1970s and 1980s (84). Not only warming and decreased rainfall but also complex feedback mechanisms due to deforestation, land-cover change and changes is atmospheric dust-loading are also playing a role, particularly for drought persistence in the Sahel and its surrounding areas(78).
A likely scenario for the projected increase in temperature and decrease in rainfall is more frequent and longer droughts and thereby a likely increase in the amount of dust in the surface air, together with alterations of atmospheric humidity. These climatic factors will most likely have negative effects on IMD in the meningitis belt, with epidemics of longer duration and maybe also higher incidence. But the effects these climate changes may have on the incidence of meningococcal carriage must also be considered, as carriage incidence plays an important role in the dynamics of IMD epidemics (24, 29, 31). This makes constructing scenarios for IMD more complex, especially as some previous studies have shown negative correlations between carriage and air humidity (66).
Warming and reduced rainfall will also affect the land-cover types in the region with extension of the savannah southwards. Populations at the margin of the current distribution of IMD will be particularly affected (3, 58). The meningitis belt has already expanded (48, 58, 85, 86) and countries south of the belt have suffered from epidemics to an extent not previously reported, for example, in Cameroon (46), Ghana (87) and Togo (88). The population at risk of IMD epidemics is likely to expand, but this prediction is uncertain as droughts also play a role in human migration and population dislocation (78).
Future research and surveillance
Expansion of the meningitis belt is already evident and is likely to progress with climate change in Africa. Close surveillance of IMD incidence in the areas bordering the meningitis belt, and of other African countries with similar climates, for early detection of climate change effects is therefore of uttermost importance (3). Further development of existing EWSs with inclusion of more demographic data, data on vaccination coverage and natural immunity in the populations and bacteriological surveillance data on meningococcal strains, is necessary for predicting epidemics in time for massvaccination campaigns to be effective (60). Further studies on the relation between climatic factors and IMD, both in the meningitis belt in Africa and in countries outside the belt in the Northern and Southern hemisphere are needed, to be able to refine knowledge on how climate affects both the carrier state and the disease. Of special interest are epidemics outside Africa within the 300–1,100 mm rainfall isohyets (57).
There are differences between different serogroups of meningococci, both in virulence and in their ability to cause epidemics, that need to be investigated to a greater extent to better understand differences in epidemiology between serogroup A in the meningitis belt and other serogroups, mainly C and B in countries outside the belt (24, 26, 27). Molecular biology studies are needed to better understand the effects of climate on the binding and penetration of N. meningitidis in mucosal membranes. This includes development of tissue models and animal models for N. meningitidis.
Conflict of interest and funding
The author has not received any funding or benefits from industry to conduct this study.
References
- 1.IPCC. Climate change 2007: impacts, adaptation and vulnerability. In: Parry ML, Canziani OF, Palutikof JP, van der Linden PJ, Hanson CE, editors. Contribution of Working Group II to the fourth assessment. Report of the Intergovernmental Panel on Climate Change. Cambridge, UK: Cambridge University Press; 2007. p. 976. Available from: http://www.ipcc.ch/publications_and_data/publications_ipcc_fourth_assessment_report_wg2_report_impacts_adaptation_and_vulnerability.htm [cited 12 September 2009] [Google Scholar]
- 2.Confalonieri U, Menne B, Akhtar R, Ebi KL, Hauengue M, Kovats RS. Human health. In: Parry ML, Canziani OF, Palutikof JP, van der Linden PJ, Hanson CE, editors. Climate change 2007: impacts, adaptation and vulnerability. Contribution of Working Group II to the fourth assessment report of the Intergovernmental Panel on Climate Change. Cambridge, UK: Cambridge University Press; 2007. pp. 391–431. Available from: http://www.ipcc.ch/pdf/assessment-report/ar4/wg2/ar4-wg2-chapter8.pdf [cited 12 September 2009] [Google Scholar]
- 3.Molesworth AM, Thomson MC, Connor SJ, Cresswell MP, Morse AP, Shears P, et al. Where is the meningitis belt? Defining an area at risk of epidemic meningitis in Africa. Trans R Soc Trop Med Hyg. 2002;96:242–9. doi: 10.1016/s0035-9203(02)90089-1. [DOI] [PubMed] [Google Scholar]
- 4.Patz JA, Epstein PR, Burke TA, Balbus JM. Global climate change and emerging infectious diseases. JAMA. 1996;275:217–23. [PubMed] [Google Scholar]
- 5.Githeko AK, Lindsay SW, Confalonieri UE, Patz JA. Climate change and vector-borne diseases: a regional analysis. Bull World Health Organ. 2000;78:1136–47. [PMC free article] [PubMed] [Google Scholar]
- 6.Semenza JC, Menne B. Climate change and infectious diseases in Europe. Lancet Infect Dis. 2009;9:365–75. doi: 10.1016/S1473-3099(09)70104-5. [DOI] [PubMed] [Google Scholar]
- 7.Zell R. Global climate change and the emergence/re-emergence of infectious diseases. Int J Med Microbiol. 2004;293:16–26. doi: 10.1016/s1433-1128(04)80005-6. [DOI] [PubMed] [Google Scholar]
- 8.Reiter P. Climate change and mosquito-borne disease: knowing the horse before hitching the cart. Rev Sci Tech. 2008;27:383–98. [PubMed] [Google Scholar]
- 9.Sáez-Nieto JA, Lujan R, Berrón S, Campos J, Viñas M, Fusté C, et al. Epidemiology and molecular basis of penicillin-resistant Neisseria meningitidis in Spain: a 5-year history (1985–1989) Clin Infect Dis. 1992;14:394–402. doi: 10.1093/clinids/14.2.394. [DOI] [PubMed] [Google Scholar]
- 10.Hedberg ST, Fredlund H, Nicolas P, Caugant DA, Olcén P, Unemo M. Antibiotic susceptibility and characteristics of Neisseria meningitidis isolates from the African meningitis belt, 2000 to 2006: phenotypic and genotypic perspectives. Antimicrob Agents Chemother. 2009;53:1561–6. doi: 10.1128/AAC.00994-08. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.du Plessis M, von Gottberg A, Cohen C, de Gouveia L, Klugman KP. Neisseria meningitidis intermediately resistant to penicillin and causing invasive disease in South Africa in 2001 to 2005. J Clin Microbiol. 2008;46:3208–14. doi: 10.1128/JCM.00221-08. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Jorgensen JH, Crawford SA, Fiebelkorn KR. Susceptibility of Neisseria meningitidis to 16 antimicrobial agents and characterization of resistance mechanisms affecting some agents. J Clin Microbiol. 2005;43:3162–71. doi: 10.1128/JCM.43.7.3162-3171.2005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Olivares R, Bouyer J, Hubert B. Risk factors for death in meningococcal disease. Pathol Biol (Paris) 1993;41:164–8. [PubMed] [Google Scholar]
- 14.Baraff LJ, Lee SI, Schriger DL. Outcomes of bacterial meningitis in children: a meta-analysis. Pediatr Infect Dis J. 1993;12:389–94. doi: 10.1097/00006454-199305000-00008. [DOI] [PubMed] [Google Scholar]
- 15.Domínguez A, Cardeñosa N, Pañella H, Orcau A, Companys M, Alseda M, et al. The case-fatality rate of meningococcal disease in Catalonia, 1990–1997. Scand J Infect Dis. 2004;36:274–9. doi: 10.1080/00365540410020163. [DOI] [PubMed] [Google Scholar]
- 16.Smith I, Bjørnevik AT, Augland IM, Berstad A, Wentzel-Larsen T, Halstensen A. Variations in case fatality and fatality risk factors of meningococcal disease in Western Norway, 1985–2002. Epidemiol Infect. 2006;134:103–10. doi: 10.1017/S0950268805004553. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Veeken H, Ritmeijer K, Hausman B. Priority during a meningitis epidemic: vaccination or treatment? Bull World Health Organ. 1998;76:135–41. [PMC free article] [PubMed] [Google Scholar]
- 18.van Deuren M, Brandtzaeg P, van der Meer JWM. Update on meningococcal disease with emphasis on pathogenesis and clinical management. Clin Microbiol Rev. 2000;13:144–66. doi: 10.1128/cmr.13.1.144-166.2000. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Smith AW, Bradley AK, Wall RA, McPherson B, Secka A, Dunn DT, et al. Sequelae of epidemic meningococcal meningitis in Africa. Trans R Soc Trop Med Hyg. 1988;82:312–20. doi: 10.1016/0035-9203(88)90459-2. [DOI] [PubMed] [Google Scholar]
- 20.Pomeroy SL, Holmes SJ, Dodge PR, Feigin RD. Seizures and other neurologic sequelae of bacterial meningitis in children. N Engl J Med. 1990;323:1651–7. doi: 10.1056/NEJM199012133232402. [DOI] [PubMed] [Google Scholar]
- 21.Al Khorasani A, Banajeh S. Bacterial profile and clinical outcome of childhood meningitis in rural Yemen: a 2-year hospital-based study. J Infect. 2006;53:228–34. doi: 10.1016/j.jinf.2005.12.004. [DOI] [PubMed] [Google Scholar]
- 22.Schildkamp RL, Lodder MC, Bijlmer HA, Dankert J, Scholten RJ. Clinical manifestations and course of meningococcal disease in 562 patients. Scand J Infect Dis. 1996;28:47–51. doi: 10.3109/00365549609027149. [DOI] [PubMed] [Google Scholar]
- 23.Peltola H. Meningococcal disease: still with us? Rev Infect Dis. 1983;5:71–91. doi: 10.1093/clinids/5.1.71. [DOI] [PubMed] [Google Scholar]
- 24.Stephens DS, Greenwood B, Brandtzaeg P. Epidemic meningitis, meningococcaemia, and Neisseria meningitides . Lancet. 2007;369:2196–210. doi: 10.1016/S0140-6736(07)61016-2. [DOI] [PubMed] [Google Scholar]
- 25.Rosenstein NE, Bradley BA, Stephens DS, Popovic T, Hughes JM. Meningococcal disease. N Engl J Med. 2001;344:1378–88. doi: 10.1056/NEJM200105033441807. [DOI] [PubMed] [Google Scholar]
- 26.Noah N. Surveillance of bacterial meningitis in Europe 1999–2000. Eurosurveillance. 2002;6 Available from: http://www.eurosurveillance.org/ViewArticle.aspx?ArticleId=2116 [cited 11 October 2009].2116 [Google Scholar]
- 27.Shigematsu M, Davison KL, Charlett A, Crowcroft NS. National enhanced surveillance of meningococcal disease in England, Wales and Northern Ireland, January 1999–June 2001. Epidemiol Infect. 2002;129:459–70. doi: 10.1017/s0950268802007549. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Greenwood BM, Greenwood AM, Bradley AK, Williams K, Hassan-King M, Shenton FC, et al. Factors influencing susceptibility to meningococcal disease during an epidemic in The Gambia, West Africa. J Infect. 1987;14:167–84. doi: 10.1016/s0163-4453(87)92052-4. [DOI] [PubMed] [Google Scholar]
- 29.Trotter C, Greenwood B. Meningococcal carriage in the meningitis belt. Lancet Infect Dis. 2007;7:797–803. doi: 10.1016/S1473-3099(07)70288-8. [DOI] [PubMed] [Google Scholar]
- 30.Roberts L. An ill wind, bringing meningitis. Science. 2008;320:1710–5. doi: 10.1126/science.320.5884.1710. [DOI] [PubMed] [Google Scholar]
- 31.Yazdankhah SP, Caugant DA. Neisseria meningitidis: an overview of the carriage state. J Med Microbiol. 2004;53:821–32. doi: 10.1099/jmm.0.45529-0. [DOI] [PubMed] [Google Scholar]
- 32.Greenwood B. Meningococcal meningitis in Africa. Trans R Soc Trop Med Hyg. 1999;93:341–53. doi: 10.1016/s0035-9203(99)90106-2. [DOI] [PubMed] [Google Scholar]
- 33.Jódar L, LaForce FM, Ceccarini C, Aguado T, Granoff DM. Meningococcal conjugate vaccine for Africa: a model for development of new vaccines for the poorest countries. Lancet. 2003;361:1902–4. doi: 10.1016/S0140-6736(03)13494-0. [DOI] [PubMed] [Google Scholar]
- 34.Trotter CL, Andrews NJ, Kaczmarski EB, Miller E, Ramsay ME. Effectiveness of meningococcal serogroup C conjugate vaccine 4 years after introduction. Lancet. 2004;364:365–7. doi: 10.1016/S0140-6736(04)16725-1. [DOI] [PubMed] [Google Scholar]
- 35.Snape MD, Pollard AJ. Meningococcal polysaccharide–protein conjugate vaccines. Lancet Infect Dis. 2005;5:21–30. doi: 10.1016/S1473-3099(04)01251-4. [DOI] [PubMed] [Google Scholar]
- 36.Siu T, Tang W, Dawar M, Patrick DM. Impact of routine immunization using meningococcal C conjugate vaccine on invasive meningococcal disease in British Columbia. Can J Public Health. 2008;99:380–2. doi: 10.1007/BF03405245. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Lapeyssonnie L. La méningitite cérebrospinale en Afrique. Bull World Health Organ. 1963;28:3–114. [PMC free article] [PubMed] [Google Scholar]
- 38.Greenwood B. 100 years of epidemic meningitis in West Africa – has anything changed? Trop Med Int Health. 2006;11:773–80. doi: 10.1111/j.1365-3156.2006.01639.x. [DOI] [PubMed] [Google Scholar]
- 39.Decosas J, Koama JB. Chronicle of an outbreak foretold: meningococcal meningitis W135 in Burkina Faso. Lancet Inf Dis. 2002;2:763–5. doi: 10.1016/s1473-3099(02)00455-3. [DOI] [PubMed] [Google Scholar]
- 40.Nathan N, Rose AM, Legros D, Tiendrebeogo SR, Bachy C, Bjørløw E, et al. Meningitis serogroup W135 outbreak, Burkina Faso, 2002. Emerg Infect Dis. 2007;13:920–3. doi: 10.3201/eid1306.060940. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Kelly D, Pollard AJ. W135 in Africa: origins, problems and perspectives. Travel Med Infect Dis. 2003;1:19–28. doi: 10.1016/S1477-8939(03)00019-X. [DOI] [PubMed] [Google Scholar]
- 42.Zombré S, Hacen MM, Ouango G, Sanou S, Adamou Y, Koumaré B, et al. The outbreak of meningitis due to Neisseria meningitidis W135 in 2003 in Burkina Faso and the national response: main lessons learnt. Vaccine. 2007;25:A69–71. doi: 10.1016/j.vaccine.2007.04.044. [DOI] [PubMed] [Google Scholar]
- 43.Moore PS, Harrison LH, Telzak EE, Ajello GW, Broome CV. Group A meningococcal carriage in travelers returning from Saudi Arabia. JAMA. 1988;260:2686–9. [PubMed] [Google Scholar]
- 44.Salih MA, Danielsson D, Bäckman A, Caugant DA, Achtman M, Olcén P. Characterization of epidemic and non-epidemic Neisseria meningitidis serogroup A strains from Sudan and Sweden. J Clin Microbiol. 1990;28:1711–9. doi: 10.1128/jcm.28.8.1711-1719.1990. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Lingappa JR, Al-Rabeah AM, Hajjeh R, Mustafa T, Fatani A, Al-Bassam T, et al. Serogroup W-135 meningococcal disease during the Hajj, 2000. Emerg Infect Dis. 2003;9:665–71. doi: 10.3201/eid0906.020565. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Cunin P, Fonkoua M-C, Kollo B, Bedifeh AB, Bayanak P, Martin PMV. Serogroup A Neisseria meningitidis outside meningitis belt in Southwest Cameroon. Emerg Inf Dis. 2003;9:1351–3. doi: 10.3201/eid0910.030170. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Anonymous. Outbreak news. Meningococcal disease, African meningitis belt, epidemic season 2006. Wkly Epidemiol Rec. 2006;81:119–20. [PubMed] [Google Scholar]
- 48.Moore PS. Meningococcal meningitis in sub-Saharan Africa: a model for the epidemic process. Clin Infect Dis. 1992;14:515–25. doi: 10.1093/clinids/14.2.515. [DOI] [PubMed] [Google Scholar]
- 49.Anonymous. Response to epidemic meningitis in Africa, 1997. Wkly Epidemiol Rec. 1997;72:313–18. [PubMed] [Google Scholar]
- 50.Broutin H, Philippon S, Constantin de Magny G, Courel F, Sultan B, Guegan JF. Comparative study of meningitis dynamics across nine African countries: a global perspective. Int J Health Geo. 2007;6 doi: 10.1186/1476-072X-6-29. Available from: http://www.ij-healthgeographics.com/content/6/1/29 [cited 12 September 2009]. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Harrison LH, Trotter CL, Ramsay ME. Global epidemiology of meningococcal disease. Vaccine. 2009;27:B51–63. doi: 10.1016/j.vaccine.2009.04.063. [DOI] [PubMed] [Google Scholar]
- 52.Thikomirov E, Santamaria M, Esteves K. Meningococcal disease: public health burden and control. World Health Stat Q. 1997;50:170–7. [PubMed] [Google Scholar]
- 53.Wang JF, Caugant DA, Li X, Hu X, Poolman JT, Crowe BA, et al. Clonal and antigenic analysis of serogroup A Neisseria meningitidis with particular reference to epidemiological features of epidemic meningitis in the People's Republic of China. Infect Immun. 1992;60:5267–82. doi: 10.1128/iai.60.12.5267-5282.1992. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Cochi SL, Markowitz LE, Joshi DD, Owens RC, Jr, Stenhouse DH, Regmi DN, et al. Control of epidemic serogroup A meningococcal meningitis in Nepal. Int J Epidemiology. 1987;16:91–7. doi: 10.1093/ije/16.1.91. [DOI] [PubMed] [Google Scholar]
- 55.Bhatia SL, Sharma KB, Natarajan R. An outbreak of meningococcal meningitis in Delhi, India. J Med Res. 1968;56:259–63. [PubMed] [Google Scholar]
- 56.Achtman M, van der Ende A, Zhu P, Koroleva IS, Kusecek B, Morelli G, et al. Molecular epidemiology of serogroup a meningitis in Moscow, 1969 to 1997. Emerg Infect Dis. 2001;7:420–7. doi: 10.3201/eid0703.010309. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Cuevas LE, Jeanne I, Molesworth A, Bell M, Savory EC, Connor SJ, et al. Risk mapping and early warning systems for the control of meningitis in Africa. Vaccine. 2007;25:A12–7. doi: 10.1016/j.vaccine.2007.04.034. [DOI] [PubMed] [Google Scholar]
- 58.Molesworth AM, Cuevas LE, Connor SJ, Morse AP, Thomson MC. Environmental risk and meningitis epidemics in Africa. Emerg Inf Dis. 2003;9:1287–93. doi: 10.3201/eid0910.030182. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Savory EC, Cuevas LE, Yassin MA, Hart CA, Molesworth AM, Thomson MC. Evaluation of the meningitis epidemics risk model in Africa. Epidemiol Infect. 2006;134:1047–51. doi: 10.1017/S0950268806005929. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Yaka P, Sultan B, Broutin H, Janicot S, Philippon S, Fourquet N. Relationship between climate and year to year variability in meningitis outbreaks: a case study in Burkina Faso and Niger. Int J Health Geogr. 2008;7:34. doi: 10.1186/1476-072X-7-34. Available from: http://www.ij-healthgeographics.com/content/7/1/34 [cited 12 September 2009] [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Thomson MC, Molesworth AM, Djingarey MH, Yameogo KR, Belanger F, Cuevas LE. Potential of environmental models to predict meningitis epidemics in Africa. Trop Med Int Health. 2006;11:781–8. doi: 10.1111/j.1365-3156.2006.01630.x. [DOI] [PubMed] [Google Scholar]
- 62.Sultan B, Labadi K, Guégan J-F, Janicot S. Climate drives the meningitis epidemics onset in West Africa. PLoS. 2005;2:43–9. doi: 10.1371/journal.pmed.0020006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Greenwood BM, Bradley AK, Wall RA. Meningococcal disease and season in sub-Saharan Africa. Lancet. 1985;2:829–30. doi: 10.1016/s0140-6736(85)90812-8. [DOI] [PubMed] [Google Scholar]
- 64.Salih MA, Ahmed HS, Karrar ZA, Kamil I, Osman KA, Palmgren H, et al. Features of a large epidemic of group A meningococcal meningitis in Khartoum, Sudan in 1988. Scand J Infect Dis. 1990;22:161–70. doi: 10.3109/00365549009037897. [DOI] [PubMed] [Google Scholar]
- 65.Jackou-Boulama M, Michel R, Ollivier L, Meynard JB, Nicolas P, Boutin JP. Correlation between rainfall and meningococcal meningitis in Niger. Med Trop (Mars) 2005;65:329–33. [PubMed] [Google Scholar]
- 66.Mueller JE, Yaro S, Madec Y, Somda PK, Idohou RS, Lafourcade BM, et al. Association of respiratory tract infection symptoms and air humidity with meningococcal carriage in Burkina Faso. Trop Med Int Health. 2008;13:1543–52. doi: 10.1111/j.1365-3156.2008.02165.x. [DOI] [PubMed] [Google Scholar]
- 67.Block C, Roitman M, Bogokowsky B, Meizlin S, Slater PE. Forty years of meningococcal disease in Israel: 1951–1990. Clin Infect Dis. 1993;17:126–32. doi: 10.1093/clinids/17.1.126. [DOI] [PubMed] [Google Scholar]
- 68.Jensen ES, Lundbye-Christensen S, Pedersen L, Sørensen HT, Schønheyder HC. Seasonal variation in meningococcal disease in Denmark: relation to age and meningococcal phenotype. Scand J Infect Dis. 2003;35:226–9. [PubMed] [Google Scholar]
- 69.Michele MM, Alberto M, Liana S, Francesco D. Do environmental factors influence the occurrence of acute meningitis in industrialized countries? An epidemic of varying aetiology in northern Italy. Eur J Epidemiol. 2006;21:465–8. doi: 10.1007/s10654-006-9013-1. [DOI] [PubMed] [Google Scholar]
- 70.Fisman DN. Seasonality of infectious diseases. Annu Rev Public Health. 2007;28:127–43. doi: 10.1146/annurev.publhealth.28.021406.144128. [DOI] [PubMed] [Google Scholar]
- 71.Kinlin LM, Spain CV, Ng V, Johnson CC, White AN, Fisman DN. Environmental exposures and invasive meningococcal disease: an evaluation of effects on varying time scales. Am J Epidemiol. 2009;169:588–95. doi: 10.1093/aje/kwn383. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Lindsay AP, Hope V, Marshall RJ, Salinger J. Meningococcal disease and meteorological conditions in Auckland, New Zealand. Aust N Z J Public Health. 2002;26:212–8. doi: 10.1111/j.1467-842x.2002.tb00676.x. [DOI] [PubMed] [Google Scholar]
- 73.Millon C. BA Thesis. Oford, UK: School of Geography, University of Oxford; 1983. When and where are we at risk? The geographical distribution of meningococcal meningitis in England and Wales. [Google Scholar]
- 74.Collier CG. Weather conditions prior to major outbreaks of meningococcal meningitis in the United Kingdom. Int J Biometeorol. 1992;36:18–29. doi: 10.1007/BF01208730. [DOI] [PubMed] [Google Scholar]
- 75.Plant L, Jonsson AB. Contacting the host: insight and implications of pathogenic Neisseria cell interactions. Scand J Infect Dis. 2003;35:608–13. doi: 10.1080/00365540310016349. [DOI] [PubMed] [Google Scholar]
- 76.Zarantonelli ML, Szatanik M, Giorgini D, Hong E, Huerre M, Guillou F, et al. Transgenic mice expressing human transferrin as a model for meningococcal infection. Infect Immun. 2007;75:5609–14. doi: 10.1128/IAI.00781-07. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Anonymous. Detecting meningococcal meningitis epidemics in highly-endemic African countries. WER. 2000;28:306–9. [PubMed] [Google Scholar]
- 78.IPCC. Climate change 2007: synthesis report. In: Core Writing Team; Pachauri RK, Reisinger A, editors. Contribution of Working Groups I, II and III to the fourth assessment report of the Intergovernmental Panel on Climate Change. Geneva, Switzerland: IPCC; 2007. p. 104. Available from: http://www.ipcc.ch/publications_and_data/publications_ipcc_fourth_assessment_report_synthesis_report.htm [cited 12 September 2009] [Google Scholar]
- 79.Vogel G. Shortage of meningitis vaccine forces triage in Burkina Faso. Science. 2003;299:1499–501. doi: 10.1126/science.299.5612.1499a. [DOI] [PubMed] [Google Scholar]
- 80.LaForce FM, Konde K, Viviani S, Préziosi MP. The meningitis vaccine project. Vaccine. 2007;25:A97–100. doi: 10.1016/j.vaccine.2007.04.049. [DOI] [PubMed] [Google Scholar]
- 81.LaForce FM, Ravenscroft N, Djingarey M, Viviani S. Epidemic meningitis due to group A Neisseria meningitidis in the African meningitis belt: a persistent problem with an imminent solution. Vaccine. 2009;27:B13–9. doi: 10.1016/j.vaccine.2009.04.062. [DOI] [PubMed] [Google Scholar]
- 82.Armstrong G, Sackey SO, Tetteh C, Bugri S, Perkins BA, Rosenstein NE, et al. Emergency vaccination against epidemic meningitis in Ghana: implications for the control of meningococcal disease in West Africa. Lancet. 2000;355:30–3. doi: 10.1016/S0140-6736(99)03366-8. [DOI] [PubMed] [Google Scholar]
- 83.Cox J, Abeku TA. Early warning systems for malaria in Africa: from blueprint to practice. Trends Parasitol. 2007;23:243–6. doi: 10.1016/j.pt.2007.03.008. [DOI] [PubMed] [Google Scholar]
- 84.Guibourdenche M, Høiby EA, Riou JY, Varaine F, Joguet C, Caugant DA. Epidemics of serogroup A Neisseria meningitidis of subgroup III in Africa, 1989–94. Epidemiol Infect. 1996;116:115–20. doi: 10.1017/s095026880005233x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.DaSilva J, Connor SJ, Mason SJ, Thomson MC. Response to Cox and Abeku: early warning systems for malaria in Africa: from blueprint to practice. Trends Parasitol. 2007;23:243–6. doi: 10.1016/j.pt.2007.04.008. [DOI] [PubMed] [Google Scholar]
- 86.Varaine F, Caugant DA, Riou JY, Kondé MK, Soga G, Nshimirimana D, et al. Meningitis outbreaks and vaccination strategy. Trans R Soc Trop Med Hyg. 1997;91:3–7. doi: 10.1016/s0035-9203(97)90371-0. [DOI] [PubMed] [Google Scholar]
- 87.Leimkugel J, Hodgson A, Forgor AA, Pflüger V, Dangy JP, Smith T, et al. Clonal waves of Neisseria colonisation and disease in the African meningitis belt: eight-year longitudinal study in northern Ghana. PLoS Med. 2007;4:e101. doi: 10.1371/journal.pmed.0040101. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88.Aplogan A, Batchassi E, Yakoua Y, Croisier A, Aleki A, Schlumberger M, et al. An epidemic of meningococcal meningitis in the region of Savanes in Togo in 1997: research and control strategies. Sante. 1997;7:384–90. [PubMed] [Google Scholar]