Abstract
Angiocidin, a matrix bound and tumor associated protein, has been shown to inhibit tumor progression and angiogenesis. We previously demonstrated that angiocidin binds to thrombospondin-1 and alpha2beta1 integrin. We now show that angiocidin binds and is a preferred substrate for tissue transglutaminase-2 (tTgase). Angiocidin bound tissue tTgase saturably with a Kd of 26 nM, while an angiocidin deletion mutant missing the matrix binding domain of angiocidin failed to bind tTgase. tTgase colocalized with angiocidin on endothelial cells. tTgase bound anti-angiocidin immunoprecipitates of endothelial cell lysates. Breast cancer cells expressing high levels of tTgase attached to angiocidin immobilized on tissue culture plates. Angiocidin was a preferred substrate for tTgase forming high molecular weight cross-linked multimers when treated with tTgase. Cross-linked angiocidin contained iso-peptide bonds as demonstrated by Western blotting and immunohistochemical colocalization studies using endothelial cells treated with angiocidin. Cross-linked angiocidin inhibited cell migration in contrast to monomeric angiocidin and inhibited localization of fibronectin (FN), a pro-tumorigenic matrix protein, into the extracellular matrix (ECM) of tumor and HUVE cells. Our studies provide an additional explanation for the anti- tumor activity of angiocidin suggesting that cross-linked angiocidin disrupts the tumor ECM making it less permissive for tumor growth.
Keywords: angiocidin, angiogenesis, endothelial cells, tumor progression, tissue transglutaminase
Introduction
Angiogenesis is the formation of new blood vessels from the endothelium of pre-existing vasculature and is the main mechanism of vascularization during physiological processes such as embryonic development, growth, regeneration, and wound healing (Folkman, 2006). This tightly controlled process in healthy tissues differs greatly from the perpetuation of neovascularization involved in a number of pathological processes including tumor growth, metastasis, diabetic retinopathy, and arthritis (Folkman, 2002).
We isolated a protein from lung carcinoma by peptide affinity chromatography using a highly hydrophobic sequence from the type 1 repeat domain of thrombospondin-1, a matrix protein over-expressed in tumor stroma (Tuszynski et al., 1993). The immunohistochemical localization of this protein showed selective expression on invasive cancer cells and capillary endothelial cells (Arnoletti et al., 1994; Tuszynski and Nicosia, 1994; Wakiyama et al., 2001). These results suggested that the protein could function in mechanisms of metastasis and angiogenesis.
We cloned the full-length cDNA for this protein and expressed the protein in bacteria (Zhou et al., 2004). The recombinant protein, referred to as angiocidin, had potent anti-angiogenic and anti-tumor activity. The recombinant angiocidin induced endothelial apoptosis when added to growth cultures of endothelial cells in full media or when cells were plated on angiocidin adsorbed on tissue culture plastic. Antibodies prepared against the recombinant angiocidin showed over-expression of angiocidin in hepatocellular carcinoma (Poon et al., 2004), prostate, lung, bladder, and melanoma cancers (Zhou et al., 2004). Angiocidin showed both matrix and cytoplasmic distribution. A Blast search of the full-length cDNA of angiocidin revealed that the protein sequence had a high degree of homology with S5a (Young et al., 1998) and antisecretory factor (Nilsson et al., 1992) but differed from them by three additional amino acids in its carboxyl terminus (G255ER257). Since it is not clear how many genes encode for angiocidin and its homologues, we have elected to call our recombinant protein, angiocidin, based on its observed functional activity in inhibiting angiogenesis.
While the anti-angiogenic mechanism of action of angiocidin has not been fully characterized, we have observed that the exogenous application of the recombinant protein to endothelial cell culture inhibits adhesion, migration, and proliferation and that these activities are related to the ability of angiocidin to inhibit cell proteasome activity and cell-extracellular matrix interactions (Dimitrov et al., 2005; Sabherwal et al., 2006). In a previous study, we made the interesting observation that angiocidin bound tissue transglutaminase-2 (tTgase) from endothelial cell lysates when passed over columns containing immobilized angiocidin (Dimitrov et al., 2005). Establishing the significance of this observation is the topic of the present paper.
tTgase is an enzyme that catalyzes the cross-linking of proteins through an acyl transfer reaction between the c-carboxamide group of peptide-bound glutamine and the epsilon -amino group of peptide-bound lysine, resulting in an epsilon - lysine - carboxy glutamyl isopeptide bond (Pisano et al., 1968). The chemical bond formed by tTgase catalysis is highly stable and is resistant to mechanical and proteolytic degradation.
tTgase is ubiquitously expressed in various tissue types, occurs in both an intracellular and extracellular form, and is highly expressed in endothelial cells and smooth muscle cells in the vasculature (Sane et al., 2007). tTgase recognizes both intracellular and extracellular proteins with both intracellular and extracellular proteins modified post-translationally by tTgase. Despite the lack of a leader sequence, tTgase is secreted from cells externally and binds to the cell surface or extracellular matrix (ECM). Here, it has been implicated in the stabilization of the extracellular matrix and in cell–ECM interactions important in angiogenesis and cancer by cross-linking matrix proteins (Belkin et al., 2001; Mehta, 2009). Under normal physiological conditions, tTgase externalized from cells becomes tightly bound to fibronectin (FN) and forms ternary complexes with collagens that function as a cementing substance in the ECM. This mechanism probably serves to clear the enzyme from the circulation to prevent it inducing adverse effects (Esposito et al., 2005). The interactions between molecules that form heteromeric complexes in the ECM of specific tissues are stabilized by tTgase like FN, thrombospondin-1(TSP-1) and collagen (Bale and Mosher, 1986; Mosher and Johnson, 1983).
Based on the ability of tTgase to remodel ECM and the importance of tumor matrix in mechanisms of angiogenesis and tumor progression, we postulate that the interaction of angiocidin with tTgase may contribute to the anti-angiogenic activity of angiocidin by remodeling the ECM. In this report, we provide evidence that angiocidin not only binds tTgase, but is a preferred substrate for tTgase forming a cross-linked angiocidin product both in the presence of cultured endothelial cells and in the tumor stroma. We show that cross-linked angiocidin inhibits the ECM incorporation of FN, an important component of the basement membrane that promotes tumor progession and angiogenesis (Akerman et al., 2005). These results suggest that tTgase cross-linked angiocidin may significantly contribute to the anti-angiogenic activity of monomeric angiocidin by generating an ECM that is less permissive for tumor progression.
Materials and methods
Materials
All reagents, unless specified otherwise, were reagent grade and purchased from Sigma Chemical Co. (St. Louis, MO). Tissue culture supplies were purchased from Fisher Scientific (Malvern, PA). Fluoroblock inserts were purchased from Falcon, Pittsburgh, PA. Human umbilical vein endothelial cell cells (HUVE) were grown in EBM-2 media purchased from Lonza, Allendale, NJ. Reagents for sodium dodecyl sulfate polyacrylamide gel electrophoresis (SDS-PAGE) were purchased from Bio-Rad Laboratories (Richmond, CA). 5-chloromethylfluorescein diacetate (CMFDA) was purchased from Invitrogen, Carlsbad, CA. Vectastain Elite ABC peroxidase kit and anti-rabbit and anti-mouse IgG labeled with horse radish peroxidase (HRP), fluorescene-labeled goat anti-mouse and anti-rabbit IgG and Texas Red labeled anti-mouse IgG were purchased from Vector Laboratories Inc., Burlingame, CA. Laminin (LM) and type IV collagen and FN were purchased from Collaborative Research, Bedford, MA. Anti-tTgase neutralizing mouse monoclonal antibody clone CUB 7402 and mouse monoclonal FN antibody were purchased from Thermo Scientific (Fisher Scientific, Pittsburgh, PA). Mouse monoclonal anti-penta-his tag antibody was purchased from Qiagen Inc, Valencia, CA. Mouse monoclonal antibody to the isopeptide bond clone 81D1C2 was purchased from Abcam Inc., Cambridge, MA.
Analysis of isopeptide bonds in crosslinked angiocidin
Recombinant monomeric angiocidin dialyzed against 20mM (4-(2-hydroxyethyl)-1-piperazineethanesulfonic acid (HEPES buffer) was incubated in the presence or absence of tissue 10 milli-units of guinea pig tTgase in a buffer containing 20mM HEPES, 10 mM CaCl2, and 10mM dithiothreitol (DTT) at 37°C for one hour. 10μl aliquots of the mixtures incubated in the presence or absence of tTgase were heated with 2X sodium dodecyl sulfate (SDS) sample buffer at 95°C for 5 minutes. Samples of the mixtures incubated in the presence or absence of tTgase were analyzed by SDS-PAGE. A western blot was performed with mouse monoclonal 81D1C2 to isopeptide antibody at a concentration of 25μg/ml followed by incubation of the blot with 0.01 μg/ml HRP-labeled rabbit anti-mouse. The blot was then developed using chemoluminesence.
Binding of tTgase to angiocidin and its mutants
In a 96-well plate, 1 μg of guinea pig tTgase in a 20mM HEPES buffer was adsorbed to the well in duplicate overnight at 4°C. Remaining buffer was aspirated and the wells were washed with phosphate-buffered saline (PBS). The plate was then blocked in 1% (w/v) BSA in PBS for 30 minutes without shaking. Serial dilutions of recombinant angiocidin or it mutants with final protein concentrations of 0.0312μg/ml, 0.0625μg/ml, 0.125μg/ml, 0.25μg/ml, 0.5μg/ml, and 1μg/ml in a 20mM HEPES buffer were added to the wells. The 96 well plate was incubated at room temperature with shaking for two hours. Remaining proteins were aspirated and then was washed with tris-buffered saline containing 0.1% Tween 20 (TBST) three times. Biotinylated rabbit anti-angiocidin antibody prepared as previously described (Sabherwal et al., 2007) at a concentration of 0.01 μg/ml in TBST was added for one hour with shaking. Remaining antibody was aspirated and then the wells were washed with TBST three times. An aliquot of 100 μl of a 0.05 μg/ml streptavidin horseradish peroxidase in TBST was added for 30 minutes with shaking. Remaining reagent was then aspirated and the wells were washed three times with TBST. Ultra 3,3′,5,5′-tetramethylbenzidine (TMB) was added to each well for 15 minutes and 100 μl of 0.5M H2SO4 was added to stop the reaction and the plate read in an ELISA plate reader at 450nm.
Biotin cadaverine incorporation into extracellular matrix proteins
HUVE cells grown in T75 culture flasks in normal media were either not treated, or treated for 30 min with either 5 μg/ml biotin cadaverine, 5μg/ml biotin cadaverine and 10μg/ml angiocidin, or 5 μg/ml biotin-cadaverine and 10 μg/ml neutralizing tTgase antibody. Cells were lysed on ice with a radioImmuno precipitation assay (RIPA) buffer lysis buffer containing 1% NP-40, 1% sodium deoxycholate, 0.1% SDS, 0.15 molar NaCl, 0.01 molar sodium phosphate, pH 7.2, supplemented with a general mammalian protease inhibitor cocktail. Samples containing 20μg of total protein were analyzed on 10% SDS-PAGE, blotted, and the blots probed with 0.01μg/ml of horse radish perioxidase-labeled streptavidin (HRP-streptavidin) in Tris-buffered saline containing 1% Tween 20 and developed using chemoluminesence. Blots were then stripped and re-probed for fibronectin and β-actin.
Cell culture
HUVE cells were grown in EBM-2 media supplemented with 10% fetal bovine serum (FBS) and a bullet kit containing growth factors, cytokines, and supplements including hEGF, hydrocortisone, GA-1000 (gentamicin, amphotericin-B), vascular endothelial growth factor (VEGF), human follicular growth factor (hFGF-B), insulin growth factor (R3-IGF-1), ascorbic acid, and heparin. Cells were maintained in a humidified atmosphere containing 5% CO2 at 37°C. MD-MBA-231 breast carcinoma subclones expressing various levels of tTgase kindly provided by Dr. Kapil Mehta from the MD Anderson Cancer Center, University of Texas were grown at 37°C and 5% CO2 in Dulbecco’s Modified Eagle Medium (DMEM) supplemented with 10% FBS, 50 U/ml of penicillin, 50 μg/ml of streptomycin, and 50 μg/ml of gentamicin sulfate.
Co-immunoprecipitation
HUVE cell lysate was incubated with a rabbit anti-angiocidin polyclonal antibody raised in our laboratory and previously characterized by us (Sabherwal et al., 2007) and immunoprecipitated with protein A/G beads and the immunoprecipitate probed with an anti- tTgase monoclonal antibody. Briefly, HUVE cells were grown in 6 well plates as described above and when cells were 75% confluent they were lysed and scraped with lysis buffer consisting of 20 mM HEPES buffer pH 7.5, containing 150 mM NaCl, 0.1% Triton X-100, 10% glycerol supplemented with protease inhibitor cocktail (Sigma) for use with mammalian cell and tissue extracts. Whole cell lysates were centrifuged at 4°C for 15 minutes at 15,000 revolutions per minute to pellet insoluble material. Protein A/G-Sepharose beads were gently washed in lysis buffer three times. One milligram of total cell proteins were incubated with 20 μl of washed protein A/G-Sepharose beads to pre-clear the cell lysates. Pre-cleared cell lysates, containing 10 μg/ml primary rabbit anti-angiocidin antibody, and 20 μl of protein A/G-Sepharose beads were incubated with gentle mixing overnight at 4°C. A negative control of pre-cleared cell lysates, 10 μg/ml rabbit anti-IgG and 20 μl of protein G-Sepharose beads were incubated in parallel. The complexes were washed three times with lysis buffer. The complexes were boiled in 20 μl of SDS-PAGE sample buffer containing 0.5M Tris-HCl pH 6.8, 5% glycerol, 2% sodium dodecyl sulfate (SDS) and 100 mM DTT prior to loading on the gel, with a lane containing recombinant angiocidin protein as a positive control. Samples were run on 10% SDS-PAGE, transferred to polyvinylidene fluoride (PVDF) membrane, blocked with 5% milk in Tris-buffered saline with TBST, immunoblotted with the mouse anti- tTgase antibody at a 1μg/ml concentration. The membrane was then washed three times in TBST for five minutes. The membrane was then incubated with HRP coupled anti-mouse secondary IgG (H+L) antibody at a concentration of 0.01 μg/ml for one hour at 4°C. The membrane was then washed three times in TBST for five minutes. The membrane was incubated with ECL Plus Detection System (Amersham) for chemiluminescence detection.
Cell adhesion assay of MDA- MB-231 subclones to recombinant angiocidin
Using MDA-MB-231 breast cancer cell subclones containing different levels of tTgase obtained from Dr. Kapil Mehta from the MD Anderson Cancer Center, University of Texas, cell adhesion of these cells to recombinant angiocidin was tested. Each well of the 96-well microplates was coated with 1 μg of recombinant angiocidin as previously described (Zhou et al., 2004). Cells were labeled with 5-chloromethylfluorescein diacetate (CMFDA) as previously described (Brown et al., 2008). CMFDA-labeled cells (5×105) were added to each well of the plates, incubated, and lysed. The amount of fluorescence associated with the wells was quantified with a Cytofluor 2350 fluorescence plate reader (Millipore, Bedford, MA, U.S.A.) and the proportion of the number of attached cells to fluorescence was determined.
Cell transmigration assay
HUVE cells were grown in EBM-2 media. Using a 24-well plate, 1μg of monomeric or polymeric angiocidin prepared as described above was plated in the upper chamber of the fluoroblock insert and incubated at 37° C in 5% CO2 for 4 hours. Then, 10μg/ml of collagen IV in 0.2M acetic acid was plated in the upper chamber of the fluoroblock insert on top of the immobilized monomeric and polymeric angiocidin and incubated at 37° C in 5% CO2 for 4 hours. HUVE cells were then labeled with 3μg/ml CMFDA as previously described (Brown et al., 2008) in EGM-2 media without FBS and growth factors and incubated for 30 minutes at 37°C in 5% CO2. The collagen IV coated-fluoroblock insert was then washed three times with 1x PBS and then the chemoattractent was added into the lower chamber, which was EGM-2 media containing 2% FBS and no growth factors. HUVE cells were then added to the upper chamber at a density of 2 × 105 cells. To measure the random migration of HUVE cells, HUVE cells were added to wells with fluoroblock coated inserts without chemoattractant in the lower chamber. The plate was read at different time points from 30 min to 6 hours using a Cytofluor 2350 florescence plate reader (Millipore, Bedford, MA) using a 485 nm excitation filter and 530 nm emission filter.
Cellular localization of FN in HUVE cells
HUVE cells were plated onto glass chamber slides, allowed to re-attach for one hour, and either treated with 10 μg/ml angiocidin, 10μg/ml neutralizing anti-tissue tTgase antibody, or buffer control. Fixed cells were then incubated with mouse anti-FN antibody at 1 μg/ml and incubated with 0.01 μg/ml of fluorescene-labeled goat anti-mouse IgG. Cells were mounted and cover-slipped. Images were captured using a Nikon fluorescent microscope.
Immunocytochemistry of FITC labeled angiocidin and tTgase in human umbilical vein endothelial cells
HUVE cells, serum-starved for 24 hours, were treated with 10 μg/ml of fluorescein isothiocyanate (FITC)-conjugated recombinant angiocidin in phosphate-buffered saline (PBS) as previously described (Zhou et al., 2004) or PBS alone for one hour. Fixed cells were then incubated with the primary antibody, 10 μg/ml mouse anti-tTgase antibody and with a fluorescent secondary antibody, Texas Red anti-mouse IgG at a concentration of 0.1μg/ml. Cells were mounted with Vectashield mounting medium for fluorescence containing 4′,6-diamidino-2-phenylindole (DAPI) and cover-slipped. Images were captured using a Nikon fluorescent microscope at 400X.
Localization of isopeptide expression in angiocidin-treated human umbilical vein endothelial cells
HUVE cells, serum-starved for 24 hours, were treated with 10 μg/ml of recombinant angiocidin in PBS or PBS alone for one hour. Fixed cells were then incubated with 1 of mouse monoclonal 81D1C2 to isopeptide antibody followed by 0.1 μg/ml fluorescene-labeled goat anti-mouse IgG. Cells were cover-slipped and viewed under fluorescence microscopy.
ECM composition of tumors from control and angiocidin-treated mice
Formalin-fixed, paraffin-embedded tissue was obtained from a previously published study (Sabherwal et al., 2006). Tissues were cut into 4-μm thick sections and stained with hematoxylin and eosin (H&E) for routine histological diagnosis and characterization. Immunohistochemistry was performed using the avidin-biotin-peroxidase complex system according to the manufacturer’s instructions (Vectastain Elite ABC peroxidase kit; Vector Laboratories Inc., Burlingame, CA). Briefly, slides were deparaffinized in xylenes, rehydrated through descending grades of alcohol up to water, and nonenzymatic antigen retrieval was performed in 0.01 molar sodium citrate buffer (pH 6.0) by heating the slides to 95°C for 30 minutes in a vacuum oven. After a cooling period of 20 minutes, the slides were rinsed in phosphate-buffered saline (PBS) and treated with 3% H2O2 in methanol for 25 minutes to quench endogenous peroxidase. Sections were then rinsed with PBS and blocked with 5% normal horse serum (for mouse monoclonal antibodies) or goat serum (for rabbit polyclonal antibodies) in 0.1% BSA in PBS for 2 hours at room temperature. In this assay, the tissue sections were incubated with primary antibodies at a concentration of 5 μg/ml which included anti-penta his antibody, anti-isopeptide, and rabbit polyclonal anti-fibronectin antibody overnight at room temperature in a humidifier chamber. After washing with PBS, the sections were incubated with the appropriate secondary antibodies at concentrations of 0.01 μg/ml for one hour at room temperature. All secondary antibodies were HRP-labeled except for fluorescene-labeled goat anti-rabbit IgG. Finally, sections were rinsed with PBS and mounted with mounting medium.
Purification of recombinant angiocidin, its deletion mutants, and TSP-1
Recombinant his-tagged angiocidin and its deletion mutants M1 and M2 were expressed in E. coli and purified on a nickel-Sepharose column as previously described (Zhou et al., 2004). TSP-1 was purified from human platelets as previously described (Tuszynski et al., 1985).
tTgase mediated crosslinking of different extracellular matrix substrates
Purified FN, purified TSP-1, purified laminin, and recombinant angiocidin were dialyzed against a 20mM HEPES buffer. These proteins were then incubated in a buffer containing 20mM HEPES, 10 mM CaCl2, and 10mM DTT at 37°C at equal molar concentrations. 10 milliunits of tTgase was added to each protein sample and samples containing approximately 1 μg of the protein mixtures were collected at various time points (0 minutes, 2 minutes, 5 minutes, 10 minutes, 20 minutes, 30 minutes, and 60 minutes) heated in 2X SDS-PAGE sample buffer at 95°C for 5 minutes. Samples were analyzed by SDS-PAGE gel and gels stained with Coomassie Brilliant Blue stain.
Treatment of recombinant angiocidin, FN, TSP-1 and laminin with tTgase
100 μl aliquots of a 0.1mg/ml solution of recombinant monomeric angiocidin, purified TSP-1, FN, and laminin were dialyzed against a 20mM HEPES buffer. Dialyzed samples were incubated in the presence or absence of 10 milli-units of tTgase in a buffer containing 10 mM CaCl2, and 10mM DTT at 37°C for one hour. 10μl samples containing approximately 1μg of the mixtures were incubated in the presence or absence of tTgase were heated in SDS sample buffer at 95°C for 5 minutes. Samples were analyzed by 10% SDS-PAGE and gels stained with Coomassie Brilliant Blue.
Western blot analysis
Cell lysates and protein samples were fractionated on 8–12% SDS-PAGE and then transferred to PVD membranes using a Pharmacia Phast gel electrophoresis system. Nonspecific sites of the membranes were blocked with 5% skimmed milk in TBST. The immunoblots were incubated with primary antibodies diluted in TBS-T for 1 h at a concentration of 1 μg/ml. After washing, the immunoblots were incubated in TBST with 0.1 μg/ml of the appropriate horseradish peroxidase-conjugated secondary antibody for 1 hour. After washing, the immunoreactivity was detected using enhanced chemoluminesence (ECL) system (Amersham, Arlington Heights, IL).
Results
Binding of tTgase to angiocidin
We previously reported that tTgase present in HUVE cell extracts bound to recombinant angiocidin immobilized on Sepharose beads (Dimitrov et al., 2005). The peptide eluted from the angiocidin-Sepharose beads was identified by mass spectral analysis of its tryptic peptides. In this study we further substantiated these results by performing a number of experimental approaches designed to demonstrate tTgase angiocidin interaction (Fig. 1).
Fig. 1.
The interaction of angiocidin with tTgase. A- Direct binding of angiocidin to immobilized tTgase; B- tTgase Western blot of anti-angiocidin HUVE cell immunoprecipitates; C – Immunohistochemical localization of tTgase and his-tag angiocidin in cultured HUVE cells; D- Adhesion to angiocidin of MDA-MB-231 breast expressing low, medium, and high levels of tTgase. Low expressors are designated Low, medium expressors are designated wildtype (WT) and high expressors are designated High. The lower panel in D shows the cell lines Western blotted for tTgase. All experiments were repeated three times to establish reproducibility. The experiments shown are representative of three experiments performed for each panel.
Purified recombinant angiocidin bound to tTgase immobilized on wells of a microtiter dish in a dose-dependent and saturable manner, showing an apparent binding constant of 26 nM (Fig. 1A). Direct angiocidin binding was measured by an ELISA procedure using biotinylated rabbit anti-angiocidin antibody and HRP-streptavidin as previously described (Sabherwal et al., 2005).
To confirm this protein-protein interaction, a co-immunoprecipitation assay was performed to determine whether endogenous angiocidin bound tTgase in HUVE cell lysates (Fig. 1B). Anti-angiocidin HUVE cell immunoprecipitates were Western blotted for tTgase. Fig 1B, lane 1 shows tTgase present in the anti-angiocidin immunoprecipitates while little or no tTgase was detected in the control IgG immunoprecipitate (Fig 1B, lane 2). As expected, whole cell lysates contained tTgase as revealed by Western blot analysis (Fig. 1B, lane 3).
To ascertain if exogenously added recombinant angiocidin interacts with tTgase on the cell surface or ECM of HUVE cells, cells were treated with FITC-labeled angiocidin and immunocytochemically stained with tTgase antibody and visualized with a Texas-Red secondary antibody (Fig. 1C). HUVE cells were treated with FITC conjugated angiocidin for five minutes and then washed with PBS to remove unbound protein. As a negative control, untreated fixed cells were incubated with secondary antibody alone for background. Images captured microscopically show a pattern of binding of the FITC labeled angiocidin to the cell. In Figure 1C, panel B the recombinant angiocidin labeled with FITC showed two patterns of staining, larger punctuates in the cytoplasm and diffuse staining through out the cell. In Figure 1C, panel C, staining for tTgase shows a similar pattern to that of FITC-labeled angiocidin. Overlay of the images from panel B and C shown in panel D of Fig 1C show considerable overlap as indicated by the yellow punctuates, suggesting that angiocidin and tTgase co-localize. A negative control included secondary antibody staining alone to confirm the working antibody concentration and that there was no overlap of fluorophore wavelengths (data not shown).
MDA-MB-231 breast cancer cell subclones containing different levels of tTgase obtained from Dr. Kapil Mehta of M.D. Anderson, University of Texas were used in an adhesion assay to determine if different levels of tTgase could be reflected in the adhesion of the cells to recombinant angiocidin. The different subclones of MDA-MB-231 cells included over-expressing clone 16W cells with high levels of tTgase, under-expressing clone 9H cells with low levels of tTgase, and the wild type cells with moderate levels of tTgase. As shown in Figure 1D, western blot confirmed the levels of tTgase in the subclones. The cells were labeled with CMFDA to better quantify cellular adhesion and serial dilutions of CMFDA-labeled cells were prepared to make a standard curve from which the number of adhered cells were calculated (data not shown). These adhesion studies show that cell adhesion was proportional to the level of tTgase expressed by the subclones and wild type cells. These studies provide a separate proof that angiocidin interacts with tTgase.
Angiocidin is a substate for tTgase
Having established that tTgase binds to recombinant angiocidin, we next determined if angiocidin could act as a substrate for tTgase. Recombinant monomeric angiocidin was incubated in the presence or absence of tTgase and calcium at 37°C for one hour and 1μg of the mixture was analyzed by SDS-PAGE (Fig. 2A). In the first lane, monomeric angiocidin was visible as a 55 kDa band. When the recombinant angiocidin was incubated with tTgase in the presence of calcium, the recombinant protein crosslinked and was visible at the top of the gel. We estimate that the crosslinked product was in excess of 106 molecular weight as evaluated by size exclusion chromatography (data not shown). To rule out that the cross-linked product was not just aggregated by tTgase but covalently cross-linked, tTgase-treated angiocidin was Western blotted with an antibody against the isopeptide bond, the major covalent bond generated by tTgase in its cross-linked products. As seen in Fig. 2A, the cross-linked angiocidin is detected by the iso-peptide antibody while the monomeric angiocidin starting material shows no reactivity. The cross-linking of angiocidin is rapid and is largely complete in 20 min under our experimental conditions (Fig 2B, panel 1). Similarly, TSP-1 and FN, known substrates for tTgase (Bale and Mosher, 1986; Barsigian et al., 1991), was also rapidly cross-linked (Fig. 2B, panels 2and 3), while laminin (LM), a protein that is has not been reported to be a preferred substrate for tTgase in the absence of other proteins (Aeschlimann and Paulsson, 1991), showed no cross-linking under our reaction conditions (Fig. 2B, panel 4). These experiments suggest that angiocidin is a preferred substrate for tTgase.
Fig. 2.
tTgase-mediated cross-linking of angiocidin and matrix proteins. A- left panel monomeric and cross-linked angiocidin analyzed by SDS-PAGE, right panel- Anti-isopeptide bond blot of monomeric and cross-linked angiocidin. B- SDS-gels of angiocidin, TSP-1, FN, and laminin treated with tTgase for various times. All experiments were repeated three times to establish reproducibility. The experiments shown are representative of three experiments performed for each panel.
To further establish the specificity of tTgase-mediated cross-linking of angiocidin and identify important structural components of angiocidin that participate in the cross-linking reaction, we evaluated the ability of tTgase to cross-link two deletion mutants of angiocidin, M1 and M2. Mutant M1 missing the 20 amino residues F86-H105 has been shown by us to lose its anti-tumor activity and matrix binding activity (Sabherwal et al., 2006; Zhou et al., 2004), while M2 missing the eight amino residues I36-S43 reported to be the active site of anti-secretory factor (Johansson et al., 1997), a close structural homologue of angiocidin, retains its matrix binding and anti-tumor activities (unpublished observations). We found that mutant M1 failed to crosslink in an hour under our experimental conditions while M2 and angiocidin were completely cross-linked (Fig. 3A). These results suggest that residues F86-H105 of angiocidin are required for cross-linking. In support of this conclusion, we also found that a 25 mer peptide of angiocidin K81-H105 containing the 20 amino residues F86-H105 matrix binding domain of angiocidin significantly inhibited tTgase catalyzed cross-linking of angiocidin (Fig. 3B).
Fig. 3.
Angiocidin sequence requirements for tTgase-mediated cross-linking of angiocidinA-Comparison of tTgase mediated cross-linking of angiocidin and two deletion mutants of angiocidin, M1 and M2 as assessed by SDS-PAGE B-The effect of M1 peptide on tTgase mediated cross-linking of angiocidin as assessed by SDS-PAGE. All experiments were repeated three times to establish reproducibility. The experiments shown are representative of three experiments performed for each panel.
Angiocidin is cross-linked by HUVE cells
To determine if recombinant angiocidin is cross-linked by HUVE cells, HUVE cells were treated with different concentrations of angiocidin (1μg/ml, 10μg/ml, and 100μg/ml) for 10 minutes. Immunocytochemical analysis using an anti-isopeptide antibody showed faint background isopeptide staining of the serum and supplement starved cells with no treatment (Fig. 4A). However, with increasing recombinant angiocidin treatment, there is was a dramatic increase in isopeptide staining. This diffuse pattern of staining is consistent with small isopeptide bonds, in contrast to large structural aggregates. The angiocidin-dependent isopeptide staining suggests that recombinant angiocidin is being cross-linked by the endothelial cells.
Fig. 4.
The effect of cross-linked angiocidin on HUVE cell migration. The migration through of HUVE cells through collagen, cross-linked angiocidin plus collagen or as a control in the presence of tTgase was measured as described in Materials and methods. All experiments were repeated three times to establish reproducibility. The experiments shown are representative of three experiments performed.
To show that angiocidin is a substrate for tTgase in situ and that cross-linked recombinant angiocidin is the source of isopeptide bond formation observed in Fig. 4A, immunocytochemical staining HUVE cells was performed. HUVE cells were treated with recombinant angiocidin or buffer alone for ten minutes. In Fig. 4B, fixed cells were then incubated with primary antibodies, monoclonal isopeptide antibody for detection of the tTgase –mediated isopeptide bond and anti-penta-His antibody which reacts with the recombinant his-tagged angiocidin. After appropriate secondary antibodies and DAPI counterstain, fluorescent images were captured showing that only minor background staining of the anti-His antibody occurs in the untreated cells. In the untreated cells, some isopeptide bond formation is detected. In contast with recombinant angiocidin treatment, the His-tagged protein appears to bind to the cell surface and localize with the isopeptide in the extracellular matrix surrounding the cell. Overlay of the isopeptide staining and His-tag staining further shows co-localization, suggesting that the His-tagged angiocidin was cross-linked.
Cross-linked- angiocidin inhibits HUVE cell migration
A transmigration assay was performed to evaluate the ability of endothelial cells to migrate through monomeric angiocidin or polymeric angiocidin. Controls included adsorbing the same concentration of tTgase onto the fluoroblock insert with an overlay of collagen IV, a fluoroblock insert with an overlay of collagen IV alone, and a fluoroblock insert with no overlay to measure the random migration of HUVE cells. A chemoattractant of 2% FBS was added to the bottom chambers. HUVE cells were labeled with the fluorophore calcein to label the cells to facilitate quantification by using a Cytofluor 2350 fluorescence plate. In Fig. 5C, the bar graph shows HUVE cells migrating through the tissue tTgase, a known adhesive substrate (Akimov et al., 2000) and the monomeric angiocidin coated wells. In the polymeric angiocidin assay, a thirty-fold decrease in migration occurs through the chamber. Therefore, HUVE cell migration was inhibited through collagen sandwiched with polymeric angiocidin.
Fig. 5.
The co-localization of angiocidin and isopeptide bond formation in HUVE cells treated with angiocidin. A- Immunohisto-localization of isopeptide bond formation in HUVE cells treated with different concentrations angiocidin B-Co- immunohisto-localization of isopeptide bond formation and his-tagged angiocidin in HUVE cells treated with his-tagged recombinant angiocidin. All experiments were repeated three times to establish reproducibility. The experiments shown are representative of three experiments performed for each panel.
Angiocidin inhibits incorporation of FN into the ECM of HUVE cells
To better understand recombinant angiocidin’s role in tTgase mediated remodeling of the ECM, endothelial cells were treated with biotin cadaverine, a polyamine substrate for tTgase that is used to identify protein substrates of tTgase. Using a biotin cadaverine incorporation assay and tracking the biotin- labeled amine protein adduct by SDS-PAGE and probing membrane blots with HRP-streptavidin, an alteration of amine incorporation into cellular proteins with recombinant angiocidin or a neutralizing tissue tTgase antibody can be monitored. Re-probing the membrane blots with antibodies for specific extracellular matrix proteins identifies the proteins amidated with cadaverine. The positive control had only biotin-cadaverine added to the cells for 30 minutes and the blot with HRP-streptavidin showed one major band of approximately 220 kD (Fig 6A). With recombinant angiocidin treatment and treatment with an anti- tTgase antibody, the major band diminished significantly. The membrane was probed for extracellular matrix proteins by Western blot and the major band was identified as fibronectin. The blot was subsequently re-probed for β actin to check for loading gel loading. Total fibronectin in all the treatment groups was constant. These results suggest that angiocidin inhibits tTgase-dependent incorporation of FN into the ECM.
Fig. 6.
The effect of angiocidin on fibronectin incorporation into ECM of HUVE cells. A- The effect of angiocidin and anti-tTgase antibody on biotin-cadaverine incorporation in HUVE-cells. The major band labeled with biotin-cadaverine was identified as fibronectin by Western-blot analysis. B- Immunohisto localization of fibronectin in untreated or HUVE cells treated with angiocidin or anti-tTgase antibody. Cells photographed at 100× magnification. C. Immunohisto localization of fibronectin in untreated or HUVE cells treated with angiocidin. Cells photographed at 400× magnification. All experiments were repeated three times to establish reproducibility. The experiments shown are representative of three experiments performed for each panel.
To confirm the inhibitory effects of recombinant angiocidin on the assembly of fibronectin into ECM, HUVE cells were detached and re-plated in the presence or absence of angiocidin. As these cells actively secrete extracellular matrix while re-attaching to the surface, alterations in the de novo assembly of FN can be visualized. HUVE cells were plated onto glass chamber slides and allowed to re-attach for one hour. After initial attachment, the cells were either treated with 10 μg/ml angiocidin, neutralizing tTgase antibody, or buffer. Fixed cells were then incubated with mouse anti-fibronectin antibody with the appropriate fluorescein secondary antibody to visualize the fibronectin localization. Figure 6B shows a series of panels in which cells were treated with buffer control, recombinant angiocidin, or neutralizing antibody. In the untreated control, fibronectin was assembled outside of the cell while treatment with recombinant angiocidin or neutralizing antibody caused the FN to remain associated within the cell. A higher magnification image in Fig. 6C illustrates the difference in localization of FN in the buffer and angiocidin-treated samples.
Angiocidin inhibits FN incorporation into the ECM of tumors from mice treated with angiocidin
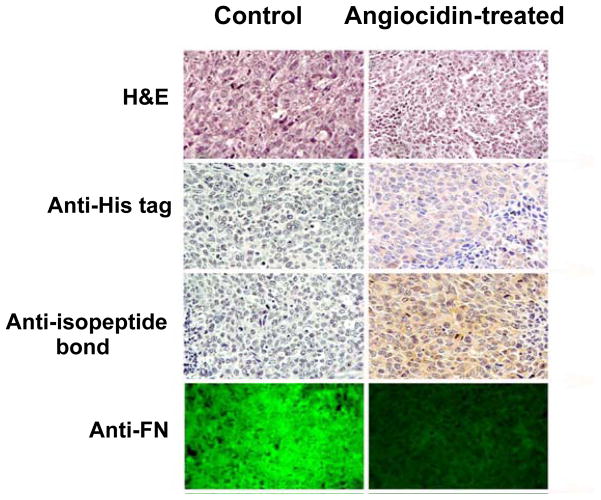
To determine if angiocidin administered to tumor bearing animals remodels the tumor ECM in a manner similar to that observed with HUVE cells, we analyzed paraffin embedded tumor tissue obtained from mice engrafted with Lewis lung carcinoma. Tumor sections from control and angiocidin-treated animals were stained for the presence of isopeptide bonds, His-tagged angiocidin, and FN. These animals were treated with intravenous injections of 1 mg/kg doses of angiocidin every other day for two weeks (Sabherwal et al., 2006). Tumor growth in the angiocidin-treated animals was significantly decreased showing reductions in excess of 70% as compared to controls (Sabherwal et al., 2006). Formalin-fixed, paraffin-embedded tumor tissue from these studies was cut into 4-μm thick sections and stained with hematoxylin and eosin (H&E) for routine histological diagnosis and characterization (top panel Fig. 7). Hematoxylin and eosin staining showed the basic histological features characteristic of these mouse tumors. In the tumors samples stained for His-tagged angiocidin, diffuse staining of the ECM around the tumor cells was observed in the angiocidin-treated mice, but not in the control animals (second panel, Fig. 7). In the tumor tissue stained for isopeptide antibody, more intense staining as compared to tumor tissue from control animals, indicating an increase in tTgase activity in the angiocidin-treated animals. Immunofluorescent staining was performed to evaluate the ECM composition of FN in these tumor samples. In the last panel of Fig. 7, the angiocidin-treated animals showed a significantly lower expression of FN as compared to tumors from control animals. These experiments provide further evidence suggesting that angiocidin is cross-linked in the tumor tissue and disrupts FN in ECM.
Fig. 7.
Immunohistochemical analysis of isopeptide bond formation and his-tag angiocidin localization in control and angiocidin-treated tumor-bearing mice Tumor tissue of Lewis lung engrafted mice either treated with buffer or angiocidin was examined immunohistochemically for the presence of isopeptide bonds, His-tagged angiocidin and FN. Images were photographed at 100× magnification. All experiments were repeated three times to establish reproducibility. The experiments shown are representative of three experiments performed for each panel.
Discussion
Several experimental observations support the hypothesis that tTgase plays a role in the development of certain types of cancer. First, multiple studies have shown that the tTgase protein is up-regulated in cancerous tissue relative to adjacent healthy tissue such as glioblastomas (Yuan et al., 2005), malignant melanomas (Fok et al., 2006), and pancreatic ductal adenocarcinomas (Verma et al., 2006). Additionally, chemotherapeutic resistance and metastatic potential of certain cancers with tTgase expression levels have been correlated with therapeutic outcomes (Verma and Mehta, 2007). tTgase has been shown to exert anti-apoptotic effects on cells while its down-regulation by siRNA inhibition or treatment with tTgase inhibitors makes these cells more sensitive to apoptosis (Mangala and Mehta, 2005). In neoplasia, tTgase has been implicated in cancer progression with several different players, even though no unifying molecular mechanism has been established. Recent data suggest that intracellular tTgase is able to crosslink nuclear factor of kappa light polypeptide gene enhancer in B-cells inhibitor, IκBα, an inhibitory subunit of nuclear factor kappa-light-chain-enhancer of activated B cells, NF-κB. This would constitutively activate the transcription factor NF-κB and promote expression of anti-apoptotic proteins such as Bcl-xL and BFL1 (Lee et al., 2004; Mann et al., 2006). Other data suggest that tTgase expression activates focal adhesion kinase, FAK, through a mechanism independent of its enzymatic activity. Activated FAK subsequently activates anti-apoptotic pathways and promotes a pro-survival PI3K/Akt pathway. The activation of FAK may lead to uncontrolled cell growth if constitutively activated (Verma et al., 2006). Therefore, with the underlying molecular connection between tTgase expression and cancer poorly characterized, it is difficult to ascertain if tTgase inhibition has therapeutic potential in hindering tumorigenesis and metastatic spread (Siegel and Khosla, 2007).
We isolated a tumor-associated protein from lung carcinoma extracts by affinity chromatography with CSVTCG, peptide fragment of thrombospondin-1 (TSP-1), a matrix protein that has been implicated in mechanisms of tumor progression (Tuszynski et al., 1993). The CSVTCG type I peptide repeats of TSP-1 are essential for many of the adhesive interactions that mediate cell adhesion, platelet aggregation, and tumor cell metastasis (Tuszynski et al., 1992). The full-length cDNA of this binding protein was isolated from a prostate cancer cell (PC3-NI) cDNA library and the recombinant protein termed angiocidin was shown to be a potent inhibitor of angiogenesis and tumor progression (Zhou et al., 2004). Monoclonal and polyclonal antibodies prepared against the recombinant protein showed cellular distribution in both the ECM and cytoplasm. With these antibodies, immunohistochemical analysis of different tissues showed an over-expression of angiocidin in melanoma, breast, prostate, colon tumors (Zhou et al., 2004). The full-length protein sequence angiocidin revealed that the protein sequence was nearly homologous with S5a, the major polyubiquitin recognition subunit of the eukaryotic 26S proteasome enzyme complex that binds polyubiquitin chains (Deveraux et al., 1995) and anti-secretory factor, a regulatory protein which inhibits the intestinal fluid secretion induced by cholera toxin (Johansson et al., 1995).
Our laboratory has been actively investigating the anti-tumor activity of angiocidin. We have discovered that the protein binds not only TSP-1 but other matrix proteins such as FN and type 1 collagen and the cell surface type 1 collagen receptor α2β1 (Sabherwal et al., 2006). A 20 amino residue in the amino terminal end of angiocidin is necessary for its anti-tumor as well as its matrix and integrin binding activities (Sabherwal et al., 2006). This domain may also signal activation of the NFκβ pathway which can initiate pathways of cell differentiation through the production of cytokines (Gaurnier-Hausser et al., 2008).
While investigating the interaction of angiocidin with potential HUVE cell protein binding partners using angiocidin-affinity chromatography (Dimitrov et al., 2005), we discovered that one of the protein bands that was eluted from the column was a 150 kDa protein whose tryptic fragments matched those of tissue transglutaminase 2 (tTgase) as revealed by mass spectral fingerprinting. In this study we have attempted to investigate the significance of this finding as it relates to the anti-tumor activity of recombinant angiocidin. We show here for the first time that angiocidin binds to purified tTgase and in endogenous tTgase present in cell extracts of HUVE cells (Fig. 1A and B). When added to growing cultures of HUVE cells, recombinant angiocidin rapidly co-localized with tTgase (Fig. 1C). The interaction of tTgase with angiocidin was further confirmed by adhesion studies with MDA-MB-231 breast cancer cells expressing various levels of tTgase. We found that adhesion of these cells to angiocidin increased with increasing expression of tTgase (Fig. 1D).
Now that the interaction of angiocidin with tTgase has been established, the question then arises as to what the consequences of this interaction are? To answer this question we investigated whether recombinant angiocidin could act as a substrate for tTgase. We found that angiocidin could be rapidly crosslinked by tTgase forming a large molecular weight multimer that could not be resolved by SDS-PAGE and was observed at the top of the resolving gel or in the sample well (Fig. 2A). Using size exclusion chromatography, we estimate that the angiocidin multimer is in excess of 106 daltons (data not shown). The cross-linked angiocidin is truly an poly-isopeptide product of tTgase since it is recognized by an antibody against the isopeptide bond (Fig. 2A) and will not be generated by tTgase unless calcium ion, a divalent cation requirement for tTgase catalyzed isopeptide bond formation, is present. We also found that angiocidin is a preferred substrate for tTgase as is TSP-1 and FN showing complete cross-linking in 30 min under our experimental conditions, whereas laminin was not appreciably cross-linked under these conditions (Fig. 2B). A deletion mutant M1 of angiocidin missing residues F86-H105 was not appreciably cross-linked by tTgase whereas another mutant missing residues I36-S43 cross-linked as well as angiocidin (Fig. 3A). We conclude that Q101 contained in the 20 residues F86-H105 may be acting as the Q donor in the cross-linking reaction since a peptide containing residues F86-H105 effectively inhibited tTgase-mediated cross-linking of angiocidin (Fig. 3B). These results are particularly significant and strongly suggest that tTgase-dependent cross-linking of angiocidin to the ECM may play a role in the anti-tumor activity of angiocidin because M1 has been shown not to bind to extracellular matrix or have anti-tumor activity(Sabherwal et al., 2006; Zhou et al., 2004).
The functional significance of tTgase –dependent cross-linking of angiocidin in HUVE cells was investigated using a motility assay. We found that monomeric angiocidin caused some inhibition of migration while in marked contrast cross-linked angiocidin was an effective barrier to cell migration when added to collagen causing an almost complete inhibition in cell migration (Fig. 4). These results suggested that matrix barriers containing cross-linked angiocidin might inhibit tumor progression. To provide further evidence in support of this idea, we investigated whether exogenous recombinant angiocidin added to growing HUVE cultures was cross-linked. We found that addition of angiocidin to HUVE cultures promoted isopeptide bond formation (Fig. 5A) and that recombinant angiocidin appeared to contain isopeptide bonds based on co-localization of angiocidin and isopeptide bond staining (Fig 5B).
Since angiocidin appeared to be cross-linked by HUVE cells, we wanted to know if angiocidin competed with other matrix proteins for tTgase thereby changing the composition of the ECM. To answer this question, we treated HUVE cells with biotin cadaverine, a polyamine substrate for tTgase, which catalyzes the amination of an appropriate Q donor protein. The incorporation of labeled cadaverine into cells has been used to identify tTgase targets and activity in cell-based assays (Summey et al., 2002). When HUVE cells were treated with biotin- cadaverine for 30 min and the cell lysate analyzed by SDS- PAGE and the blots subsequently probed with HRP-streptavidin, a major labeled band at 220 kDa was observed (Fig 6A). This band was identified as FN by Western blot analysis. When cells were treated with biotin-cadaverine in the presence of angiocidin or with an antibody against tTgase, cadaverine incorporation into FN decreased significantly while total FN levels were unchanged (Fig. 6A). When cells were stained for FN, we observed a decrease FN incorporation into the ECM with increased focal staining of FN in the cell cytoplasm either after treatment with angiocidin or after treatment with anti-tTgase antibody (Fig. 6B and C). These results suggested that angiocidin or anti-tTgase antibody disrupted incorporation of FN into the ECM, replacing an ECM rich in FN with one rich in angiocidin. Loss of FN from the ECM would be expected to be less permissive for microvessel formation and tumor and endothelial cell migration (Ruoslahti, 1999).
To further investigate if such a mechanism might be operative in vivo, we compared the expression of FN, isopeptide bond formation, His-tag angiocidin in tumor tissue harvested from mice treated with angiocidin or buffer as described in a previously published study (Sabherwal et al., 2006). We found that tumor tissue obtained from animals treated with an iv. injection of 1 mg/kg recombinant angiocidin every other day for two weeks expressed significantly more isopeptide bond formation, and less FN than controls (Fig. 7). As expected His-tag angiocidin was only present in the angiocidin-treated animals and the pattern of isopeptide bond expression and His-tag angiocidin localization was very similar suggesting that angiocidin was cross-linked and sequestered in the tumor ECM.
Taken together the data presented in this paper suggest that recombinant angiocidin is a preferred substrate for tTgase and consequently can alter the tumor matrix making it less permissive for angiogenesis and cell migration. This activity together with its capacity to stimulate innate immunity (Gaurnier-Hausser and Tuszynski, 2009) and differentiate tumor cells (Gaurnier-Hausser et al., 2008) makes angiocidin an attractive candidate for development as a therapeutic for the inhibition of tumor progression.
Acknowledgments
This work was supported in part by NIH grant R01 CA88931 and a grant from the Pennsylvania State Tobacco Settlement Act.
Abbreviations
- CMFDA
5-chloromethylfluorescein diacetate
- cDNA
complimentary DNA
- DAPI
4′,6-diamidino-2-phenylindole
- DTT
dithiothreitol
- DMEM
dulbecco’s Modified Eagle Medium
- ECL
enhanced chemoluminesence
- ECM
extracellular matrix
- FN
fibronectin
- FITC
fluorescein isothiocyanate
- HEPES
4-(2-hydroxyethyl)-1-piperazineethanesulfonic acid
- HRP
horse radish peroxidase
- HUVE cells
human umbilical vein endothelial
- hFGF-B
cells human follicular growth factor
- (R3-IGF-1)
insulin growth factor
- LM
laminin
- MMP
metalloproteinase
- PBS
phosphate-buffered saline
- PVDF
polyvinylidene fluoride
- SDS
sodium dodecyl sulfate
- SDS-PAGE
sodium dodecyl sulfate-polyacylamide gel electrophoresis
- TMB
3,3′,5,5′-tetramethylbenzidine
- TIMP
tissue inhibitor of metalloproteinase
- tTgase
tissue transglutaminase-2
- TSP-1
thrombospondin-1
- TBST
tris-buffered saline containing 0.1% Tween 20
- VEGF
vascular endothelial growth factor
Footnotes
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
References
- Aeschlimann D, Paulsson M. Cross-linking of laminin-nidogen complexes by tissue transglutaminase. A novel mechanism for basement membrane stabilization. J Biol Chem. 1991;266:15308–17. [PubMed] [Google Scholar]
- Akerman ME, et al. Angiostatic peptides use plasma fibronectin to home to angiogenic vasculature. Proc Natl Acad Sci U S A. 2005;102:2040–5. doi: 10.1073/pnas.0409844102. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Akimov SS, et al. Tissue transglutaminase is an integrin-binding adhesion coreceptor for fibronectin. J Cell Biol. 2000;148:825–38. doi: 10.1083/jcb.148.4.825. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Arnoletti JP, et al. Computer-assisted image analysis of tumor sections for a new thrombospondin receptor. Am J Surg. 1994;168:433–6. doi: 10.1016/s0002-9610(05)80093-5. [DOI] [PubMed] [Google Scholar]
- Bale MD, Mosher DF. Thrombospondin is a substrate for blood coagulation factor XIIIa. Biochemistry. 1986;25:5667–73. doi: 10.1021/bi00367a048. [DOI] [PubMed] [Google Scholar]
- Barsigian C, et al. Tissue (type II) transglutaminase covalently incorporates itself, fibrinogen, or fibronectin into high molecular weight complexes on the extracellular surface of isolated hepatocytes. Use of 2-[(2-oxopropyl)thio] imidazolium derivatives as cellular transglutaminase inactivators. J Biol Chem. 1991;266:22501–9. [PubMed] [Google Scholar]
- Belkin AM, et al. Matrix-dependent proteolysis of surface transglutaminase by membrane-type metalloproteinase regulates cancer cell adhesion and locomotion. J Biol Chem. 2001;276:18415–22. doi: 10.1074/jbc.M010135200. [DOI] [PubMed] [Google Scholar]
- Brown MC, et al. Angiostatic activity of obtustatin as alpha1beta1 integrin inhibitor in experimental melanoma growth. Int J Cancer. 2008;123:2195–203. doi: 10.1002/ijc.23777. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Deveraux Q, et al. Molecular cloning and expression of a 26 S protease subunit enriched in dileucine repeats. J Biol Chem. 1995;270:23726–9. doi: 10.1074/jbc.270.40.23726. [DOI] [PubMed] [Google Scholar]
- Dimitrov S, et al. The endothelial apoptotic activity of angiocidin is dependent on its polyubiquitin binding activity. Br J Cancer. 2005;93:662–669. doi: 10.1038/sj.bjc.6602773. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Esposito C, et al. Tissue transglutaminase and celiac disease. Prog Exp Tumor Res. 2005;38:158–73. doi: 10.1159/000084239. [DOI] [PubMed] [Google Scholar]
- Fok JY, et al. Implications of tissue transglutaminase expression in malignant melanoma. Mol Cancer Ther. 2006;5:1493–503. doi: 10.1158/1535-7163.MCT-06-0083. [DOI] [PubMed] [Google Scholar]
- Folkman J. Role of angiogenesis in tumor growth and metastasis. Semin Oncol. 2002;29:15–8. doi: 10.1053/sonc.2002.37263. [DOI] [PubMed] [Google Scholar]
- Folkman J. Angiogenesis. Annu Rev Med. 2006;57:1–18. doi: 10.1146/annurev.med.57.121304.131306. [DOI] [PubMed] [Google Scholar]
- Gaurnier-Hausser A, et al. The novel angiogenic inhibitor, angiocidin, induces differentiation of monocytes to macrophages. Cancer Res. 2008;68:5905–14. doi: 10.1158/0008-5472.CAN-07-6179. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gaurnier-Hausser A, Tuszynski GP. The immunomodulatory role of angiocidin, a novel angiogenesis inhibitor. Curr Pharm Des. 2009;15:1937–48. doi: 10.2174/138161209788453149. [DOI] [PubMed] [Google Scholar]
- Johansson E, et al. Identification of an active site in the antisecretory factor protein. Biochim Biophys Acta. 1997;1362:177–82. doi: 10.1016/s0925-4439(97)00066-5. [DOI] [PubMed] [Google Scholar]
- Johansson E, et al. Molecular cloning and expression of a pituitary gland protein modulating intestinal fluid secretion. J Biol Chem. 1995;270:20615–20. doi: 10.1074/jbc.270.35.20615. [DOI] [PubMed] [Google Scholar]
- Lee J, et al. Transglutaminase 2 induces nuclear factor-kappaB activation via a novel pathway in BV-2 microglia. J Biol Chem. 2004;279:53725–35. doi: 10.1074/jbc.M407627200. [DOI] [PubMed] [Google Scholar]
- Mangala LS, Mehta K. Tissue transglutaminase (TG2) in cancer biology. Prog Exp Tumor Res. 2005;38:125–38. doi: 10.1159/000084237. [DOI] [PubMed] [Google Scholar]
- Mann AP, et al. Overexpression of tissue transglutaminase leads to constitutive activation of nuclear factor-kappaB in cancer cells: delineation of a novel pathway. Cancer Res. 2006;66:8788–95. doi: 10.1158/0008-5472.CAN-06-1457. [DOI] [PubMed] [Google Scholar]
- Mehta K. Biological and therapeutic significance of tissue transglutaminase in pancreatic cancer. Amino Acids. 2009;36:709–16. doi: 10.1007/s00726-008-0128-4. [DOI] [PubMed] [Google Scholar]
- Mosher DF, Johnson RB. Specificity of fibronectin--fibrin cross-linking. Ann N Y Acad Sci. 1983;408:583–94. doi: 10.1111/j.1749-6632.1983.tb23275.x. [DOI] [PubMed] [Google Scholar]
- Nilsson LA, et al. Induction of anti-secretory factor in mice by the nonintestinal parasite Schistosoma mansoni. J Parasitol. 1992;78:1055–8. [PubMed] [Google Scholar]
- Pisano JJ, et al. [Cross-link in fibrin polymerized by factor 13: epsilon-(gamma-glutamyl)lysine.] Science. 1968;160:892–3. doi: 10.1126/science.160.3830.892. [DOI] [PubMed] [Google Scholar]
- Poon RT, et al. Clinical significance of thrombospondin 1 expression in hepatocellular carcinoma. Clin Cancer Res. 2004;10:4150–7. doi: 10.1158/1078-0432.CCR-03-0435. [DOI] [PubMed] [Google Scholar]
- Ruoslahti E. Fibronectin and its integrin receptors in cancer. Adv Cancer Res. 1999;76:1–20. doi: 10.1016/s0065-230x(08)60772-1. [DOI] [PubMed] [Google Scholar]
- Sabherwal Y, et al. Integrin alpha2beta1 mediates the anti-angiogenic and anti-tumor activities of angiocidin, a novel tumor-associated protein. Exp Cell Res. 2006;312:2443–53. doi: 10.1016/j.yexcr.2006.04.009. [DOI] [PubMed] [Google Scholar]
- Sabherwal Y, et al. Clinical significace of serum angiocidin levels in hepatocellular carcinoma. Proceedings of the American Association for Cancer Research; 2005. p. 1319. [Google Scholar]
- Sabherwal Y, et al. Clinical significance of serum angiocidin levels in hepatocellular carcinoma. Cancer Lett. 2007;251:28–35. doi: 10.1016/j.canlet.2006.10.023. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sane DC, et al. Roles of transglutaminases in cardiac and vascular diseases. Front Biosci. 2007;12:2530–45. doi: 10.2741/2253. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Siegel M, Khosla C. Transglutaminase 2 inhibitors and their therapeutic role in disease states. Pharmacol Ther. 2007;115:232–45. doi: 10.1016/j.pharmthera.2007.05.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Summey BT, Jr, et al. Tissue transglutaminase localization and activity regulation in the extracellular matrix of articular cartilage. J Orthop Res. 2002;20:76–82. doi: 10.1016/S0736-0266(01)00064-X. [DOI] [PubMed] [Google Scholar]
- Tuszynski GP, Nicosia RF. Localization of thrombospondin and its cysteine-serine-valine-threonine-cysteine-glycine-specific receptor in human breast carcinoma. Lab Invest. 1994;70:228–33. [PubMed] [Google Scholar]
- Tuszynski GP, et al. Biological activities of peptides and peptide analogues derived from common sequences present in thrombospondin, properdin, and malarial proteins. J Cell Biol. 1992;116:209–17. doi: 10.1083/jcb.116.1.209. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tuszynski GP, et al. Identification and characterization of a tumor cell receptor for CSVTCG, a thrombospondin adhesive domain. J Cell Biol. 1993;120:513–21. doi: 10.1083/jcb.120.2.513. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tuszynski GP, et al. The interaction of human platelet thrombospondin with fibrinogen. Thrombospondin purification and specificity of interaction. J Biol Chem. 1985;260:12240–5. [PubMed] [Google Scholar]
- Verma A, Mehta K. Tissue transglutaminase-mediated chemoresistance in cancer cells. Drug Resist Updat. 2007;10:144–51. doi: 10.1016/j.drup.2007.06.002. [DOI] [PubMed] [Google Scholar]
- Verma A, et al. Increased expression of tissue transglutaminase in pancreatic ductal adenocarcinoma and its implications in drug resistance and metastasis. Cancer Res. 2006;66:10525–33. doi: 10.1158/0008-5472.CAN-06-2387. [DOI] [PubMed] [Google Scholar]
- Wakiyama T, et al. The localization of thrombospondin-1 (TSP-1), cysteine-serine-valine-threonine-cysteine-glycine (CSVTCG) TSP receptor, and matrix metalloproteinase-9 (MMP-9) in colorectal cancer. Histol Histopathol. 2001;16:345–51. doi: 10.14670/HH-16.345. [DOI] [PubMed] [Google Scholar]
- Young P, et al. Characterization of two polyubiquitin binding sites in the 26 S protease subunit 5a. J Biol Chem. 1998;273:5461–7. doi: 10.1074/jbc.273.10.5461. [DOI] [PubMed] [Google Scholar]
- Yuan L, et al. Tissue transglutaminase 2 inhibition promotes cell death and chemosensitivity in glioblastomas. Mol Cancer Ther. 2005;4:1293–302. doi: 10.1158/1535-7163.MCT-04-0328. [DOI] [PubMed] [Google Scholar]
- Zhou J, et al. Cloning and characterization of angiocidin, a tumor cell binding protein for thrombospondin-1. J Cell Biochem. 2004;92:125–46. doi: 10.1002/jcb.20076. [DOI] [PubMed] [Google Scholar]