Abstract
Objective
Epidemiologic studies of air pollution effects on respiratory health report significant modification by sex, although results are not uniform. Importantly, it remains unclear whether modifications are attributable to socially derived gendered exposures, to sex-linked physiological differences, or to some interplay thereof. Gender analysis, which aims to disaggregate social from biological differences between males and females, may help to elucidate these possible sources of effect modification.
Data sources and data extraction
A PubMed literature search was performed in July 2009, using the terms “respiratory” and any of “sex” or “gender” or “men and women” or “boys and girls” and either “PM2.5” (particulate matter ≥ 2.5 μm in aerodynamic diameter) or “NO2” (nitrogen dioxide). I reviewed the identified studies, and others cited therein, to summarize current evidence of effect modification, with attention to authors’ interpretation of observed differences. Owing to broad differences in exposure mixes, outcomes, and analytic techniques, with few studies examining any given combination thereof, meta-analysis was not deemed appropriate at this time.
Data synthesis
More studies of adults report stronger effects among women, particularly for older persons or where using residential exposure assessment. Studies of children suggest stronger effects among boys in early life and among girls in later childhood.
Conclusions
The qualitative review describes possible sources of difference in air pollution response between women and men, which may vary by life stage, coexposures, hormonal status, or other factors. The sources of observed effect modifications remain unclear, although gender analytic approaches may help to disentangle gender and sex differences in pollution response. A framework for incorporating gender analysis into environmental epidemiology is offered, along with several potentially useful methods from gender analysis.
Keywords: air pollution, effect modification, epidemiology, gender, sex
There is growing epidemiologic evidence of differing associations between air pollution and respiratory health for females and males. More studies report stronger effects among women and girls than among men and boys, but the literature is far from consistent. Importantly, it is unknown whether observed modification is attributable primarily to biological differences between men and women, to exposure differences (e.g., work-related coexposures), or to some interplay thereof. Gender analysis, which aims to disaggregate social and biological differences between men and women (e.g., hormonal status), may help to elucidate this modification, identify key mechanisms, and design more effective interventions.
The distinction between gender (i.e., self-representation, socially derived activities and roles) and sex (i.e., biological differences by chromosomal complement, including reproductive organs and hormonal composition) (Krieger 2003) speaks to the distinction between exposure and susceptibility. Gender analysis is more common in occupational epidemiology (Arbuckle 2006; Messing and Stellman 2006; Messing et al. 2003; Schachter et al. 2009) than in environmental health (Keitt et al. 2004), because persistent job stratification by sex (Alexanderson and Östlin 2001) has produced marked differences in occupational exposures to chemical agents (Hursidic-Radulovic et al. 2002; London et al. 2002), ergonomic demands (Silverstein et al. 1986), injury (Salminen et al. 1992), and psychosocial stressors (Arcand et al. 2000; Bourbonnais et al. 2000; Gutek 2001; Hall 1989).
Gender, a social construct, includes cultural norms, roles, and behaviors shaped by relations among women and men and among girls and boys (Krieger 2003). Gender, inherently social, varies continuously over multiple dimensions over the life course, whereas sex is normally dichotomous. Gender is shaped at the societal level and varies across nation, culture, class, race, ethnicity, nationality, sexuality, and religion. Gender describes patterns of behavior, place, and role, determining where people spend time and their activities, thereby shaping exposure distributions.
Sex, a biological construct, is based on physiologic differences enabling reproduction, defined by physiologic characteristics (especially reproductive organs) or chromosomal complement (Krieger 2003). Sex-linked traits (e.g., hormonal status, body size) influence biological transport of environmentally derived chemicals. Lung size and growth, deposition of fine particles [particulate matter ≥ 2.5 μm in aerodynamic diameter (PM2.5)] (Kim and Hu 1998, 2006), gas absorption (Jones and Lam 2006), gas–blood barrier permeability (Brauner et al. 2009), airway hyperresponsiveness (Kanner et al. 1994), vascular response (Prisby et al. 2008), and inflammation (Hermes et al. 2006; Sood et al. 2008) all differ, on average, by sex.
Sex and gender can be difficult to distinguish in epidemiologic data; they are tightly intertwined, with reciprocal effects. Biological characteristics (e.g., body size) become engendered as occupational and family roles, which are gendered expressions of biology. Likewise, gendered work and caregiving roles, smoking, and alcohol consumption influence muscle mass, adiposity, and chemical body burden—collectively, these are socially derived biological expressions of gender (Krieger 2003).
In this review I present a framework for incorporating gender analysis into air pollution epidemiology, describing pathways through which gender and sex, separately and multiplicatively, may influence pollution response. Current evidence of effect modification in air pollution respiratory epidemiology is summarized, and potentially useful nascent analytic methods from gender analysis are offered.
Gender analysis explores topics far beyond those addressed here, including sexuality and transgender issues. Here I consider only those constructs and tools that may directly inform mean differences between men and women in air pollution epidemiology.
A Framework for Incorporating Gender Analysis into Environmental Epidemiology
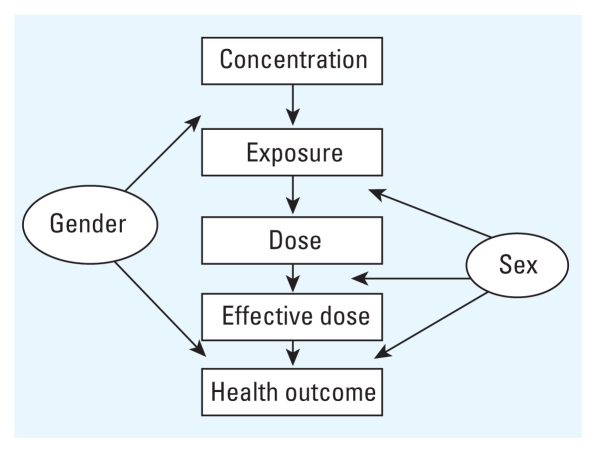
Incorporating aspects of gender analysis into the environmental health paradigm (Figure 1) actualizes this distinction between gender and sex. The framework is elucidated by drawing examples broadly from environmental epidemiology, elucidating pathways through which gender and sex may, individually and recursively, shape population exposure and susceptibility.
Figure 1.
Possible roles of gender and sex in shaping observed relationships between air pollution and health. Gender affects the presence of the exposure itself (e.g., cosmetic use), whereas biological sex differences determine the consequent dose (e.g., through dermal thickness and permeability). Sex differences in biological transport and target organs determine health outcomes, potentially modified by gendered (behavioral) coexposures and their sequelae.
Concentration to exposure
Gender shapes where people spend time and activity patterns—for example, sports participation, work-related chemical and ergonomic exposures, and use of personal care and cleaning products. Nickel dermatitis and hand eczema are far more prevalent among women than men in Western countries, likely because of chronic exposures from jewelry (Meding 2000). Indoor fossil fuel burning for cooking in developing countries drastically increases kitchen PM2.5 concentrations (Dionisio et al. 2008; Rumchev et al. 2007); because women generally perform more cooking in these societies, they suffer elevated respiratory symptoms (Behera 1997), asthma (Qureshi 1994), chronic bronchitis (Pandey 1984), chronic obstructive pulmonary disease (COPD) (Ramirez-Venegas et al. 2006), pneumoconiosis (Grobbelaar and Bateman 1991), tuberculosis, lung cancer (Behera and Balamugesh 2005), and mortality (Lopez et al. 2006). Accordingly, stove-replacement interventions have effectively reduced exposures and improved women’s health in these settings (Khushk et al. 2005; McCracken et al. 2007). Gendered home activities shape exposures to cooking exhaust and cleaning products, behaviors and home characteristics that vary by social class, climate, and culture. Residence-based exposure estimates may better capture exposures among homemakers and thus may be more accurate for women than men in most societies.
Exposure to dose
Sex differences in dermal absorption and lung function (Becklake and Kauffmann 1999; Ernstgard et al. 2002) influence contaminant uptake. Skin metabolizes some xenobiotics, modifying their toxicity (Bashir and Maibach 2002); this characteristic differs by sex and is influenced by gendered dermal exposures (e.g., topical creams, cosmetics, jewelry). Respiratory absorption of airborne gases (Jones and Lam 2006) and gas–blood barrier permeability (Brauner et al. 2009) also differ by sex.
Dose to effective dose
Sex determines the availability of target organs and hormonal systemic regulation. Only in women are patterns in ovarian cancer or pregnancy outcomes observable; only in men can testicular cancer patterns be observed. Kinetics and toxicity of chemicals in women’s bodies vary across the life course, during menarche, pregnancy, lactation, and menopause (Roberts and Silbergeld 1995; Silbergeld et al. 1988); gastrointestinal cadmium accumulation increases with low iron stores (Åkesson et al. 2002), common during pregnancy and among women of reproductive age (Gunshin et al. 1997). Estradiol and testosterone influence transport of environmentally derived chemicals and accumulation in the brain, kidney, liver, and intestines (Morris et al. 2003); mercury retention in kidneys can be three times higher among women than men (Barregård et al. 1999; Hultman and Nielsen 2001). During pregnancy (a sex-linked state), activity and exposure patterns change (Nethery et al. 2009), and hormonal changes affect toxicant transport throughout the body.
Effective dose to health outcome
Sex-linked biological differences influence disease etiology after organ exposure. Women have more arsenic-induced kidney and bladder cancers than do men in regions with arsenic in drinking water, likely because of reduced chemical excretion during pregnancy and lactation (Concha et al. 1998). Sex-linked hormonal status alters vascular effects of diesel exhaust (Prisby et al. 2008). Coexposures from gendered behaviors (e.g., alcohol and tobacco use, cardiovascular exercise) modify the biological fate of environmentally derived chemicals and organ resiliency. Sex and gender effects can interact; sex-linked pregnancy outcomes (observable only among women) are modified by gendered behaviors (e.g., smoking, occupational endocrine disruptors, hairspray exposures) (Ormond et al. 2008). Gender differences in health-care seeking and illness behaviors influence the progression of environmentally derived illness.
Current Evidence of Effect Modification by Sex in Air Pollution Epidemiology
Search Methods
A PubMed (National Library of Medicine 2009) search, performed in July 2009, retrieved all publications in the database identifiable using the terms “respiratory” and “nitrogen dioxide” (or “NO2”) and any of the following terms: “sex” (n = 41 citations), “gender” (n = 8), “women and men” (or “men and women”) (n = 243), or “girls and boys” (or vice versa) (n = 8). Another search retrieved all publications identifiable using “fine particulate matter” (“PM2.5”) and “respiratory” and any of the following terms: “sex” (n = 11), “gender” (n = 5), “women and men” (or vice versa) (n = 65), or “girls and boys” (or vice versa) (n = 2). Only respiratory outcomes were considered (i.e., diagnosed respiratory illness, symptoms, lung function, respiratory mortality), although the findings and models may apply to other outcomes. Papers examining noninhalation pathways were also excluded; thus, effects of prenatal air pollution exposures on infant and child health (which may differentially affect boys) are not considered here.
Of the 383 publications identified, seven review articles were eliminated, along with 30 duplicate citations identified by multiple search criteria, 42 publications not available in English, 50 publications on noninhalation pathways or nonrespiratory outcomes, 13 publications on nonhuman species, and 32 publications not primarily examining air pollution exposures. Abstracts of the remaining 209 publications were reviewed to determine whether effect modification by sex was tested; if the abstract was unclear, the original publication was consulted.
Most publications reported only sex-adjusted effects or examined only one sex. Only 37 unique publications examined air pollution effect modification by sex (summarized in Tables 1 and 2). Given vast differences in analytic methods, outcomes, exposure intensities, and durations—with few studies exploring any combination thereof—meta-analysis was not appropriate. It is beyond the scope of this review to assess the magnitude of effect modification, which varies by study design and outcome measure. Most (not all) of the reviewed publications reported odds ratios or risk ratios, with interactions on the multiplicative scale. Authors also used varying statistical criteria for “significant” interactions (here, p < 0.05 unless otherwise stated). Issues in assessment of interactions for epidemiology have been detailed elsewhere (Knol et al. 2009).
Table 1.
Studies examining effect modification by sex among adults.
| Study | Population | Exposure metric(s) | Outcome(s) | Risk among males | Risk among females |
|---|---|---|---|---|---|
| Studies reporting stronger effects among women | |||||
| Franklin et al. 2007 | 1.3 million deaths, 27 U.S. cities 1997–2002 | Prior day PM2.5 > 10 μg/m3 | Percent increase in respiratory mortality All-cause mortality |
1.90 (0.14–3.65) 1.06% (0.07–2.6) |
1.57% (−0.22 to −3.35) 1.34% (0.40–2.27) |
| Ito and Thurston 1996 | Daily deaths in Chicago, IL 1985–1990 | Daily PM10, O3 at nearest regulatory monitor | RR for respiratory mortality | RR = 1.10 (0.97–1.26) | RR = 1.17 (1.02–1.35) |
| Kan et al. 2007 | 15,792 middle-age U.S. adults, 1987–1989 (ARIC cohort) | Quartiles of residential traffic density | Lung function: FEV1 FVC |
β (Q4, age adjusted) = 19.6 (−34.9 to 74.1); p-trend = 0.66 β (Q4, multivariate) = 11.7 (−40.2 to 63.5); p-trend = 0.86 |
β (Q4, age adjusted) = −34.8 (−66.5 to −3.1); p-trend = 0.01 β (Q4, multivariate) = −34.8 (−66.5 to −3.1); p-trend = 0.01 |
| Kan et al. 2008 | Adult population of Shanghai, China (population, 13.1 million) | 10-μg/m3 increase in daily PM10, SO2, NO2, O3 | Percent increase in respiratory mortality | β (PM10) = 0.17% (0.03 to 0.32) β (SO2) = 0.85% (0.43 to 1.28) β (NO2) = 0.88% (0.49 to 1.28) β (O3) = 0.19% (−0.16 to 0.55) |
β (PM10) = 0.33% (0.18–0.48) β (SO2) = 1.06% (0.62–1.51) β (NO2) = 1.10% (0.69–1.51) β (O3) = 0.40% (0.03–0.76) |
| Luginaah et al. 2005 | 1,602 adults (15–64 years) in Windsor, Ontario, Canada 1995–2000 | IQR increase in 1-, 2-, 3-day lag NO2, SO2, CO, COH, O3, PM10, TRS | Risk of respiratory hospitalization | RR (2-day COH) = 1.04 (0.82–1.32) RR (3-day COH) = 0.95 (0.80–1.13) |
RR (2-day COH) = 1.20 (1.00–1.43), by case crossover RR (3-day COH) = 1.15 (1.02–1.30), by time series |
| Sunyer et al. 2000 | 2,305 adults (≥ 35 years of age) Spain, 1985–1989 | 20-μg/m3 increase in same-day ambient black smoke | Respiratory mortality | OR = 1.14 (0.98–1.33) | OR = 1.52 (0.99, 2.31) |
| Sunyer et al. 2006 | 3,232 men and 3,592 women in Europe | Constant traffic density NO2 > 50 μg/m3 |
Prevalence of chronic phlegm | β (traffic) = 6.13% (4.37–8.32); p-trend = 0.47 β (NO2) = 6.67% (3.49–11.36); p-trend = 0.98 |
β (traffic) = 7.69% (5.95–9.75); p-trend = 0.002 β (NO2) = 8.68% (5.30–13.22); p-trend = 0.05 |
| Thaller et al. 2008a | 142 lifeguards 16–27 years of age (79% male) | 10-μg/m3 increase daily average PM2.5, maximum O3 | FVC FEV1/FVC |
β (PM2.5) = −0.1% (−0.8 to 0.5) β (O3) = −0.006% (−0.2 to 0.05) |
β (PM2.5) = −2.1% (−3.2 to −1.0) β (O3) = −0.3% (−0.4 to −0.6) |
| Studies reporting stronger effects among men | |||||
| Abbey et al. 1998 | 1,391 nonsmoking U.S. adults | IQR difference of 54.2 days/year > 100 μg/m3 PM10 | PPFEV1 FEV1/FVC |
β = −7.2 (−11.5 to −2.7) (males w/parental respiratory illness) β = −1.5 (−2.7 to −0.4) |
β = 0.9 (−0.8 to 2.5) β = −0.2 (−0.9 to 0.5) |
| Galizia and Kinney 1999 | 520 nonsmoking undergraduate students in New Haven, CT | Lived ≥ 4 years in U.S. county with summer 1-hr O3 ≥ 80 ppb | Percent change in FEV1 FEF25–75 FEF75 symptoms |
β = −4.7% (−0.7 to −8.8) β = −13.0% (−4.9 to −21.1) β = −10.0% (1.3 to −21.3) OR = 2.30 (1.15–3.46) |
β = −0.26% (3.79 to −4.31) β = −1.96% (5.39 to −10.30) β = −2.08% (9.94 to −13.9) OR = 1.79 (0.83–3.89) |
| Korrick et al. 1998 | 530 hikers (18–64 years), Mt. Washington, NH | Ambient O3, PM2.5, aerosol acidity | Percent change in FEV1 FVC |
β = −0.055 (SE = 0.025) β = −0.051 (SE = 0.016) |
β = −0.039 (SE = 0.039) β = −0.019 (SE = 0.025) |
| Wang et al. 1999 | 1,075 Chinese adults (35–60 years) | Ambient PM2.5 and SO2 (rural vs. urban area) | Mean change FEV1 | 199 mL (SE = 50 mL) | 87 mL (SE = 30 mL) |
| Studies reporting null or mixed modification | |||||
| Ackermann-Liebrich et al. 1997 | 9,651 adults 18–60 years of age in Switzerland (SAPALDIA cohort) | 10-μg/m3 change in annual mean PM10 | FVC | β = 3.4% (p < 0.05)b | Effects did not differ by sex |
| Chestnut et al. 1991 | 6,913 adults (25–75 years) (NHANES I) | 1-SD increase in TSP (about 34 μg/m3) | Percent change in FVC | β = 2.25% (p < 0.05) | Effects did not differ by sex (p > 0.75) |
| Jedrychowski and Krzyzanowski 1989 | 584 men, 830 women in Krakow, Poland | Residence in area with higher sulfate or sulfur transformation ratio | Lung function, symptoms | FEV1 decline faster by 11 mL/year in high- vs. low-sulfate areas | High-sulfate area predicted symptoms, not lung function |
| Oosterlee et al. 1996 | 1,485 Haarlem, Netherlands, adults | Living on heavy (vs. light) trafficked streets | Wheeze (ever) Wheeze (2-year) |
OR = 1.1 (0.8–1.3) OR = 1.1 (0.6–1.8) |
Effects did not differ by sex |
| Zeka et al. 2006 | 1.9 million deaths in 20 U.S. cities, 1989–2000 | 10-μg/m3 change in daily PM10 concentrations | Percent increase in respiratory mortality | β = 0.71 (0.004–1.42) | β = 1.04 (0.33–1.75) |
Abbreviations: IQR, interquartile range; NHANES, National Health and Nutrition Examination Survey; NR, not reported; OR, odds ratio; PPFEV1, percent predicted FEV1; RR, relative risk; Q, quartile; SAPALDIA, Study on Air Pollution and Lung Diseases in Adults; TRS, total reduced sulfur; VC%, vital capacity percent. Key results demonstrate observed effect modification, and are not exhaustive of results reported for each study. Values in parentheses are 95% confidence intervals, unless otherwise indicated.
Other outcomes showed no significant effect modification by sex.
Effects did not differ by sex, and therefore are reported here in only one column.
Table 2.
Studies examining effect modification by sex among children.
| Study | Population | Exposure metric(s) | Outcome(s) of interest | Risk among males | Risk among females |
|---|---|---|---|---|---|
| Studies reporting stronger effects among girls | |||||
| Brunekreef et al. 1997 | 877 Dutch children (7–12 years of age) in 1995 | Truck traffic density (for children within 300 m of motorway) | Change in FVC FEV1 |
β = −1.1 (−6.7 to 4.9) β = −1.8 (−7.5 to 4.2) |
β = −6.3 (−11.4 to −0.8) β = −6.2 (−11.5 to −0.6) |
| Luginaah et al. 2005 | 883 children (0–14 years of age) in Windsor, Ontario, Canada 1995–2000 | IQR increase in 1-, 2-, 3-day lag NO2, SO2, CO, COH, O3, PM10, TRS | RR of respiratory hospitalization | RR(lag1 SO2) = 0.95 (0.87 to 1.04) RR(lag2 CO) = 0.996 (0.93 to 1.06) RR(lag2 CO) = 0.997 (0.87 to 1.14) RR(lag1 NO2) = 0.93 (0.81 to 1.07) |
RR(lag1 SO2) = 1.11 (1.01 to 1.22) RR(lag2 CO) = 1.07 (1.00 to 1.14) RR(lag2 CO) = 1.19 (1.02 to 1.38) RR(lag1 NO2) = 1.19 (1.002 to 1.41) |
| Oftedal et al. 2008 | 2,307 9- and 10-year-old children in Oslo, Norway | IQR increase in lifetime NO2, PM2.5, PM10 | Change in PEF FEF25 FEF50 |
β (NO2) = −69.1 mL/sec (−135.3 to −3.0) β (PM10) = −57.9 mL/sec (−116.2 to 0.4) β (PM2.5) = −30.1 mL/sec (−79.7 to 19.5) |
β (NO2) = −94.5 mL/sec (−166.6 to −22.4) β (PM10) = −77.9 mL/sec (−141.9 to −14.0) β (PM2.5) = −68.9 mL/sec (−120.8 to −16.9) |
| Oosterlee et al. 1996 | 291 Haarlem, Netherlands, children (0–15 years of age) | Living on heavy (vs. light) trafficked streets | Wheeze (ever) Wheeze (1-year) Dyspnea (ever) Dyspnea (1-year) |
OR = 1.2 (0.4–3.7) OR = 0.7 (0.2–2.5) OR = 0.9 (0.2–3.2) OR = 0.4 (0.1–2.6) |
OR = 4.4 (1.4–13.6) OR = 5.3 (1.1–25.0) OR = 4.8 (1.3–17.7) OR = 15.8 (1.4–174.4) |
| Pershagen et al. 1995 | 197 children (4 months to 4 years) hospitalized with wheeze, 350 controls | Residential outdoor NO2, presence of gas stove | RR of wheezing bronchitis | RR (NO2 > 0.7) = 0.7 (0.4–1.3); p-trend = 0.10 RR (gas stove) = 0.9 (0.5–1.8) |
RR (NO2 > 70) = 2.7 (1.1–6.8); p-trend= 0.02 RR (gas stove) = 2.4 (1.0–5.9) |
| Peters et al. 1999 | 3,293 children in 12 Southern California communities | Lifetime ambient NO2, PM2.5, and O3 | FVC FEV1 PEFR MMEF |
β (NO2) = −29.9 L/min (SE = 29.5) β (PM2.5) = 8.3 L/min (SE = 24.5) β (03) = 52.0 L/min (SE = 65.8) β (PM2.5) = 32.0 L/min (SE = 30.1) |
β (NO2) = −63.8 (SE = 18.3) β (PM2.5) = −47.6 (SE = 14.4) β (03) = −250.9 (SE = 69.9) β (PM2.5) = −130.0 (SE = 30.3) |
| Rojas-Martinez et al. 2007 | 3,170 children (8 years of age) in Mexico City, 1996–1999 | IQR increase in mean O3, PM10, NO2 | Change in FEV1 | β (O3) = −4 mL (−10 to 2) β (PM10) = −15 mL (−23 to −6) β (NO2) = −25 mL (−33 to −18) |
β (O3) = −12 mL (−18 to −6) β (PM10) = −11 mL (−20 to −3) β (NO2) = −30 mL (−37 to −22) |
| Rosenlund et al. 2009 | 2,107 children 9–14 years of age in 40 Rome schools | Residential traffic Distance to busy road Modeled NO2 |
Percent difference in FEV1 FEF25–75 |
β = −4% (−29 to 21) β = −26% (−81 to 29) |
β = −23% (−49 to 2); p for difference = 0.25 β = −103% (−163 to −43); p for difference = 0.06 |
| Stern et al. 1989 | 1,630 children (7–12 years of age) in rural Canada | High- vs. low-exposure community | Percent difference in FVC FEV1.0 |
β = 1.45% (p < 0.05) β = 1.41% (p < 0.01) |
β = 2.52% (p < 0.001) β = 2.03% (p < 0.001) |
| Van Vliet et al. 1997 | 1,498 children in 13 schools | Residence within 100 m of freeway | Chronic cough Wheeze | OR = 1.05 (0.50–2.22) OR = 1.29 (0.45–3.68) |
OR = 2.45 (1.16–5.16) OR = 3.05 (1.11–8.41) |
| Studies reporting stronger effects among boys | |||||
| Delfino et al. 2004 | 14 boys and 5 girls with asthma, 9–17 years of age | IQR increase in 4-day personal PM2.5 | FEV1 | β = −16% (−26 to −6) | β = −1% (−16 to 14) |
| Gehring et al. 2002 | 1,756 German infants | Outdoor residential exposure gradient 1.5 μg/m3 in PM2.5, 0.4 × 10−5/m abs, 8.5 μg/m3 NO2 | Cough without infection Dry cough at night |
OR (PM2.5) = 1.43 (1.14–1.80) OR (abs) = 1.38 (1.11–1.71) OR (NO2) = 1.52 (1.16–2.00) OR (PM2.5) = 1.39 (1.08–1.78) OR (abs) = 1.31 (1.04–1.67) OR (NO2) = 1.45 (1.07–1.98) |
OR (PM2.5) = 1.19 (0.84–1.70) OR (abs) = 1.25 (0.87–1.78) OR (NO2) = 1.22 (0.81–1.85) OR (PM2.5) = 1.17 (0.81–1.68) OR (abs) = 1.16 (0.79–1.71) OR (NO2) = 1.20 (0.78–1.84) |
| Jedrychowski et al. (1999) | 1,001 children in Krakow, Poland | Residence in high- vs. low-pollution area | Slower growth in FVC FEV1 |
OR (FVC) = 2.15 (1.25–3.69) OR (FEV1) = 1.90 (1.12–3.25) |
OR (FVC) = 1.50 (0.84–2.68) OR (FEV1) = 1.39 (0.78–2.44) |
| Peters et al. 1999 | 3,676 children in 12 Southern California communities | IQR difference in community lifetime ambient acid, NO2, PM2.5, O3 | Prevalence of wheeze | OR (NO2) = 1.47 (1.04–2.09) OR (acid) = 1.55 (1.03–2.32) |
OR (NO2) = 0.85 (0.59–1.21) OR (acid) = 1.08 (0.71–1.66) |
| Studies reporting null or mixed modification | |||||
| Emenius et al. 2003 | 540 Stockholm children (0–2 years of age) | Indoor and outdoor residential NO2 | OR for recurrent wheeze (high vs. low quartile) | OR (outdoor NO2) = 1.60 (0.78–3.26)a OR (indoor NO2) = 1.51 (0.81–2.82) |
NR; effects did not differ by sex |
| Gauderman et al. 2004 | 1,759 children in 12 Southern California communities | Lifetime community annual average NO2, PM2.5, EC (most vs. least polluted) | Growth in FVC FEV1 MMEF |
β (NO2) = −95.0 (−189.4 to −0.6)a β (NO2) = −101.4 (−164.5 to −38.4) β (NO2) = −211.0 (−377.6 to −44.4) |
NR; effects did not differ by sex |
| Lin et al. 2005 | 6,782 Toronto, Canada children, 0–14 years of age | 6.5 μg/m3 increase in 6-day PM10–2.5 exposure | Hospitalizations for respiratory infections | β = 1.15% ( 1.02–1.30) | β = 1.18% (1.01–1.36) |
| Liu et al. 2009 | 182 asthmatic children 9–14 years of age in Windsor, Ontario, Canada | IQR change in same-day, lagged SO2, NO2, O3, PM2.5 | Percent change in FEF25–75 | β (same-day NO2 ) = −2.4 (−4.3 to −0.4) β (same-day PM2.5) = 1.9 (−3.5 to −0.3) |
NR; effects did not differ by sex |
| Roemer et al. 1999 | 1,621 children in 14 European centers, 1993–1994 | 24-hr measures of PM10, BS, SO2, NO2 | Change in evening PEF per 100 μg/m3 | β (lag 0 SO2) = 1.9 L/min (p < 0.05) β (lag 0 BS) = 0.7 L/min (p < 0.10) β (lag 2 PM2.5) = −0.5 L/min (NS) |
β (lag 0 SO2) = 1.4 (NS) β (lag 0 BS) = 0.2 (NS) β (lag 2 PM2.5) = 1.2 (p < 0.05) |
| Schwartz 1989 | 4,300 youths (6–24 years of age), NHANES II, 1976–1980 | Annual average SO2, NO2, TSP, O3 at monitors | Change in FVC FEV1 PEF |
β (NO2) = −2.94 (p = 0.0004) β (NO2) = −3.09 (p = 0.0003) β (NO2) = −3.23 (p = 0.0019) |
NR; effects did not differ by sex |
| Smith et al. 2000 | 44 asthmatic children (< 14 years of age) | Daily personal NO2 exposure | Chest tightness | OR = 1.29 (1.16, 1.43) | NR; effects did not differ by sex |
| Zhao et al. 2008 | 1,993 pupils (11–15 years of age) in urban China | School indoor and outdoor SO2, NO2, O3 | Asthma, wheeze | OR (wheeze, indoor SO2) = 1.18 (1.03–1.35)a OR (wheeze, indoor CH2O) = 1.24 (1.03–1.48) |
NR; effects did not differ by sex |
Abbreviations: abs, absorbance; BS, black smoke; CH2O, formaldehyde; EC, elemental carbon; IQR, interquartile range; MMEF, median mid-expiratory flow; NR, not reported; NS, not significant; OR, odds ratio; PEFR, peak expiratory flow rate; RR, relative risk; TRS, total reduced sulfur. Key results demonstrate observed effect modification, and are not exhaustive of results reported for each study. Values in parentheses are 95% confidence interval, unless otherwise indicated.
Effects did not differ by sex, and therefore are reported here in only one column.
The qualitative review documents the widely varying explanations offered to explain observed modifications—as such, only papers in which authors offered such interpretations are included. Accordingly, the results described here, and summarized in Tables 1 and 2, are not exhaustive, but represent effect modification as reported by the authors. Only a few studies took additional analytic steps to examine sources of difference that may account for observed effect modification.
Search Results
Because gender differences in behaviors, exposures, or coexposures (e.g., diet, smoking) and biological factors (e.g., hormonal composition) change over the life course, studies are summarized separately for adults and children.
Gender and sex differences in respiratory health effects among adults
Studies reporting stronger effects among women
Studies of residential air pollution exposures suggest stronger associations among women. In the Atherosclerosis Risk in Communities (ARIC) study, Kan et al. (2007) found that living near a major road predicted lower forced expiratory volume in 1 sec (FEV1) and forced vital capacity (FVC) only among women. The authors pointed to women’s greater airway reactivity, citing stronger responses to smoking (Lodrup Carlsen et al. 2006; Vollmer et al. 1994; Yunginger et al. 1992), or better accuracy in residential exposure assessment for homemakers (35% of ARIC women vs. 17% of men).
Franklin et al. (2007) studied 130,000 respiratory deaths in 27 U.S. communities, using case–crossover methods and meta-analysis, and found that community air pollution better predicted death among women than among men. The authors proposed sex-differing respiratory anatomy and physiology, or PM deposition patterns.
In a comprehensive study of daily air pollution and respiratory hospitalization among adults and children in Windsor, Ontario, using time-series and case–crossover methods, Luginaah et al. (2005) reported a larger number of significant associations among women and girls than among men and boys. Two-day lagged coefficient of haze (COH) exposures predicted increased risks among women. For girls 0–14 years of age, 1- to 2-day lagged NO2, sulfur dioxide (SO2), and carbon monoxide (CO) exposures predicted elevated risks. Among males, only 1-day lagged PM10 predicted increased risks among adults. The authors proposed sex-differing biological explanations (e.g., hormonally affected inflammation, smooth muscle and vascular function, lung growth and decline, airway and parenchymal size), citing evidence of sex-differing airway PM2.5 deposition (Kim and Hu 1998; Kohlhaufl et al. 1999) and greater responsivity to tobacco smoke among females (Chen et al. 1999, 2005; Gold et al. 1996; Hursidic-Radulovic et al. 2002; Prescott et al. 1997; Varkev 2004; Xu et al. 1994a, 1994b). They considered gendered explanations; women are, on average, poorer and may experience greater (or different) psychosocial stressors, perform more household tasks (increasing exposures to viral infection, indoor allergens, combustion exhaust, cleaning solvent, and aeroallergens) (Redline and Gold 1994), and may differ from men in health-care seeking and illness management behaviors (Goodman et al. 1994).
One Chicago cohort studied by Ito and Thurston (1996) showed greater all-cause and respiratory mortality with same- and previous-day PM10 among black women than among other sex/race groups. The authors observed that physiologic differences and gender differences in activities, occupation, and class may shape pollution response, noting that race and gender were yet unexplored in environmental epidemiology.
In the Public Health and Air Pollution in Asia (PAPA) study, Kan et al. (2008) reported stronger associations between pollutants [PM10 (PM with aerodynamic diameter < 10 μm) SO2, NO2, ozone (O3)] and daily respiratory mortality among women, elderly, and lower socioeconomic status (SES) persons. The authors offered gendered explanations (e.g., smoking among men may obscure pollution effects; Shanghai women’s lower average education may confound gender and SES) and considered biological explanations, including women’s smaller airways, greater airway reactivity (Yunginger et al. 1992), and greater deposition of PM2.5 (Kohlhaufl et al. 1999; Sunyer et al. 2000).
Among 6,824 adults in 10 European countries in the European Community Health Survey 2000–2002 (ECRHS I), Sunyer et al. (2006) found that home traffic intensity and outdoor NO2 better predicted chronic bronchitis among women than among men. The authors also examined occupational exposures, which better predicted outcomes among men, separating some gendered activity pattern effects. The authors suggested sex-linked differences in hormonal status, and gender differences in coexposures, disease perception, health care access and use and differing perceptions of environmental quality and symptoms by gender and education.
Sunyer et al. (2000) found that older and female Barcelona adults with COPD showed greater all-cause, respiratory, and cardiovascular mortality with same-day black smoke than did younger persons and men. The authors suggested the reasons were a higher prevalence of frail persons among the elderly and women than among men, or biological differences, including inflammatory response [given women’s stronger response to smoking (Xu et al. 1994a, 1994b)], lung size, and airway diameter influencing PM deposition, respiratory patterns, and airway resistance (Bennett et al. 1996).
Studies reporting stronger effects among men
In the 20-year prospective California Adventists Health Study, Abbey et al. (1998) linked PM10 to reduced lung function (FEV1/FVC) among nonsmoking males, and decreased FEV1 among men with parental respiratory illness. Women and never-smoking males displayed increased peak expiratory flow (PEF) lability. Among males, sulfate exposures predicted reduced FEV1, and O3 exposures predicted reduced FEV1 among men with parental respiratory illness. The authors suggested gender differences in work-related exposures or possible stronger healthy worker effects among women. They confirmed that cohort men spent more time outdoors (16.1 hr/week vs. 9.2 hr/week; p < 0.0005) and suggested that outdoor exposures may trigger responses in males with genetic predisposition to respiratory illness.
Galizia and Kinney (1999) found that, among Yale freshmen, growing up in areas with high (vs. low) O3 was associated with symptoms and reduced lung function among males but not among females. The authors suggested the gendered explanation that men may accumulate greater O3 exposures through outdoor physical activity.
Studies reporting null or mixed modification
Zeka et al. (2006) found that ambient PM10 was associated with respiratory and all-cause mortality across 20 U.S. cities, using case–crossover analysis. Although modification was nonsignificant, the authors posited that sex, race, and age may indicate SES, increasing susceptibility through lesser health care access, poorer nutrition, greater stress or violence exposures, or increasing actual exposures through residential proximity to highways or occupational coexposures. Finally, they suggest sex-linked biological differences in PM deposition.
In a 13-year follow-up of Krakow adults, Jedrychowski and Krzyzanowski (1989) found that residence in higher sulfate areas better predicted FEV1 decrements among men than among women. Among women, SO2 and PM correlated with symptoms; the authors suggested that women’s greater average spent time near home produced better accuracy in exposure assessment.
Gender and sex differences in respiratory health effects among children
Disentangling gender and sex effects in air pollution–health associations among children may be more complicated, because lung function growth rates (critical periods for pollution effects) differ by sex (Berhane et al. 2000). Most air pollution epidemiology studies among children examine chronic exposures, although outcomes considered vary widely, including lung function growth, wheeze, asthma onset and exacerbation, and symptoms.
Studies reporting stronger effects among girls
Using baseline cross-sectional results from the Southern California Children’s Health Study (CHS) of children in grades 4, 7, and 10 in 12 communities, Peters et al. (1999) reported that air pollutants (PM10, PM2.5, acid vapor, NO2, O3) were more strongly inversely associated with lung function among girls than among boys. The authors suggested gender differences in time outdoors and play activities, and sex differences in growth rates, hormonal factors, and respiratory mechanisms. Using longitudinal CHS analyses, Gauderman et al. (2004) found deficits in FEV1 growth from 10 to 18 years of age associated with community NO2, PM2.5, and acid vapor not significantly differing by sex. McConnell et al. (2002) reported higher asthma risk with outdoor sports participation in higher O3 areas in the CHS cohort, especially among girls, and suggested that higher ventilation during play may increase exposures.
In a U.S. study, Neas et al. (1991) reported stronger associations between home indoor NO2 and respiratory symptoms among girls than among boys 7–11 years of age. The authors cited reports of stronger effects among girls, including a British study linking gas stove use to symptoms among girls (Melia et al. 1977), a paper reporting FEV75 (75th percentile) decrements of 1.1% among girls 9–13 years of age but slight increases among boys (Hasselblad et al. 1981), and a British study linking kitchen NO2 and gas stoves to greater reductions in PEF and forced expiratory flow between 25th and 75th percentile (FEF25–75) among girls (Florey et al. 1979).
Among Dutch children 7–12 years of age, Brunekreef et al. (1997) found that truck traffic and black smoke at schools were associated with lung function reductions only among girls, and van Vliet et al. (1997) found that residential distance from freeway, truck traffic density, and school black smoke measures better predicted chronic respiratory symptoms among girls than among boys, after accounting for SES and home exposures. In both studies, the authors contrast their results with evidence of stronger passive smoke effects among boys. However, these studies examine in utero exposures and noninhalation pathways (Cuijpers et al. 1995; Cunningham et al. 1994), and suggest that, because boys exhibit more symptoms overall, air pollution effects may be obscured by other respiratory “noise” (Pershagen et al. 1995).
Among 673 adults and 106 children in Haarlem, the Netherlands, Oosterlee et al. (1996) reported significant associations between living along busy (vs. quiet) streets and asthma or dyspnea only among girls. They suggested that boys’ higher total respiratory symptoms may mask pollution effects, and considered gendered factors (e.g., passive smoking, activity patterns, coexposures) in their analysis.
In Oslo, Norway, Oftedal et al. (2008) found that lifetime residential NO2, PM10, and PM2.5 among 9- and 10-year-old children was associated with lower PEF, more strongly among girls, only slightly attenuated by SES adjustment. The authors suggested biological explanations (e.g., girls experience growth spurts earlier, captured within this follow-up, or hormonal status may alter girls’ responses) and suggested unmeasured SES-related confounders (e.g., gendered sports participation).
In a case–control study in Stockholm, Pershagen et al. (1995) reported significant associations between outdoor home NO2 and gas stove use on wheezing bronchitis only among girls, despite boys’ higher wheezing prevalence. Outdoor NO2, gas stove use, and smoking conferred multiplicative risks in girls but not in boys, after SES adjustment. The authors reported consistency with prior studies, indicated that results were unlikely due to selection bias or misclassification, and acknowledged a need for activity data to explore gender differences.
Rosenlund et al. (2009) found associations between chronic residential NO2 exposure and lung function to be stronger among Roman girls than boys 9–14 years of age; mean FEV1 and FEF25–75 decrements were approximately four times greater in girls than boys, corroborating other studies (Cesaroni et al. 2008; Kulkarni et al. 2006; Li et al. 2003; Neas et al. 1991; Nordling et al. 2008; Oftedal et al. 2008; Pershagen et al. 1995). The authors indicated complexities in comparing childhood cohorts differing by age, pubertal status, pollution mixtures, study designs, and susceptibilities and noted that the consistency of results across Europe reporting stronger air pollution effects among girls, meriting further investigation.
Studies reporting stronger effects among boys
In the Traffic-Related Air Pollution on Childhood Asthma (TRAPCA) study, Gehring et al. (2002) reported stronger associations between residential PM2.5 and symptoms (e.g., cough without infection, cough at night) among boys than among girls 0–2 years of age. The authors suggested that differences in total symptoms, masking pollution effects, were important or that, given sex differences in lung development, infant girls have larger airways relative to body size and lesser airway resistance.
In a prospective cohort study of annual mean total suspended particle (TSP) and SO2 exposures among preadolescent children in Krakow, Poland, Jedrychowski et al. (1999) reported stronger associations with FVC and FEV1 among boys than among girls. The authors noted sex-differing lung growth rates, producing different critical periods for pollution effects.
Studies reporting null or mixed effect modification
In a 3-year prospective study of children in Mexico City, Mexico, Rojas-Martinez et al. (2007) associated elevated PM10, NO2, and O3 with reduced lung function among boys and girls. Interquartile range increases in NO2 predicted FEV1 declines in girls, whereas increases in PM10 predicted FEV1 declines among boys. Elevated O3 predicted FEV1 decreases three times larger among girls than among boys, unexplained by SES. The authors compared these findings with CHS results on sex-differing lung function growth and suggested higher O3 exposures among children spending time outdoors (Gauderman et al. 2000; McConnell et al. 2002).
In Toronto (Ontario, Canada), respiratory hospitalizations were significantly associated with PM2.5–10 among boys and girls, with PM10 among boys, and with NO2 among girls (Lin et al. 2005). The authors proposed sex-linked explanations: Boys have smaller airways relative to lung volume and differ in smooth muscle, vascular function, and hormonal status.
Discussion
Among adults, evidence of effect modification by sex remains uncertain; studies of older adults and those using residential exposure estimates suggest stronger effects among women. The range of plausible explanations is very broad, including sex-linked biological factors related to lung volume, deposition, reactivity, and hormonal influences on chemical transport and systemic regulation. Gendered explanations include confounding or modification by smoking behaviors, job-related chemical exposures, differential accuracy in residence-based exposure assignment, exposures to indoor allergens and cleaning agents, and differing exposure and response to psychosocial stressors. Refined distinction between sex and gender may elucidate these associations.
Studies of younger children suggest stronger associations among boys; older childhood cohorts suggest the opposite. Age-related trends may be linked to sex-differing lung function growth rates (Gold et al. 1994) and differences in airway function at birth, which suggest lower respiratory volumes and greater airway resistance among boys (Stocks et al. 1997). At older ages, gendered activities may also shape pollution response.
Gender, sex, and multiple exposures
Environmental exposures are complex. Traffic-related air pollution includes gaseous species and PM from combustion, tire and brake wear, resuspended roadway dusts, and salts (Schauer et al. 2006). Pollution exposures occur in multiplicity, and polluted neighborhoods often also suffer poverty, crime, and lower access to health-related resources (Morello-Frosch and Shenassa 2006). In workplaces, chemical exposures co-vary with heat, noise, and strain, acting recursively and synergistically on workers’ health (MacDonald et al. 2001). Gender analysis fits into environmental health under this multiple exposures framework. There is growing interest in pollution effect modification by SES (Jerrett et al. 2004; O’Neill et al. 2003) and chronic stress (Chen et al. 2008; Clougherty et al. 2006, 2007; Morello-Frosch and Shenassa 2006). Likewise, SES is a complex mix of social and physical stressors accumulating over the life course (Romieu et al. 2005), shaping health and susceptibility. Behavioral and physiologic responses to SES and stressors may vary by gender (Seeman et al. 2002); women, on average, may respond more strongly to interpersonal stressors (Davis et al. 1999) and experience different physiologic sequelae (Hermes et al. 2006; Iwasaki-Sekino et al. 2009; Seeman et al. 1995). Women’s behavioral responses may emphasize social support, caregiving, and child tending (Taylor et al. 2000), whereas better known “fight-or-flight” responses emphasize sympathetic–adrenal–medullary enervation and activities linked to traditionally male roles (Powell and Matthews 2002; Taylor et al. 2000). Stress may be a gendered factor (i.e., exposures differ by gender) and a sex-differing factor as well, if physiologic responses to stress differ (e.g., sex-differing epinephrine responses). If stress modifies pollution response, then understanding gendered stress responses is likely important for accurately characterizing gendered pollution responses.
Research from social geography may help to better elucidate gendered spatial and behavioral exposure patterns. Gendered use of space and exposure patterns in urban communities is evident in the example of fear of violence. One large U.S. survey reported that 26% of women “never” leave home after dark (vs. 9% of men), 51% “always” bring friends for protection (vs. 4% of men), and 71% consider safety when parking (vs. 33% of men) (Gordon and Riger 1991). Strong gender differences in perceived safety shape activity and exercise patterns; parents’ greater restriction of girls’ geographic range in U.S. cities shapes exposure paradigms, exercise, experience, and developmental opportunity (Katz 1993). Better understanding the gendered environment can improve exposure assessment, better isolate biological responses, and provide a model for examining other social effect modifiers (Clougherty and Kubzansky 2009).
Analytic approaches for disentangling effects of gender and sex
Because gender and sex are tightly intertwined, their effects can be difficult to distinguish in epidemiologic data. “Gender” and “sex” have commonly been conflated in epidemiologic research (Krieger 2003). Most important, careful use of language distinguishing these constructs will enable researchers to better describe and understand sources of difference in exposure–health relationships. Methodology for gender analysis is an evolving field, although the methods described here may help to disentangle some effects of sex and gender and may merit further exploration in environmental epidemiology.
Reporting sex-stratified results is more informative than is adjustment for sex (Arbuckle 2006) and can identify associations differing broadly between males and females. However, sex stratification often confounds tightly correlated gender and sex effects, obscuring true sources of difference. Preferably, researchers may stratify data separately by multiple sex- and gender-associated factors (e.g., body size, working outside the home, time spent on household tasks) to elucidate sources of difference. Most epidemiologic data sets are not adequately powered to perform multiple stratifications simultaneously, so these multiple stratifications usually need be performed separately. Stratification variables should reflect time–activity patterns or meaningful biological factors, rather than stereotypical attributes, to identify true factors relevant to the cohort under study.
Population-specific exposure modeling may improve culturally and behaviorally specific exposure assessment, clarifying gendered exposure differences. Residential exposure metrics may be more accurate for women, who spend more time near home on average, especially when caring for children or other family members (Gilliand et al. 2005; Kingsley 2003; Maziak et al. 2005; Payne-Sturges et al. 2004). Residential activities may require microenvironmental exposure assessment (LaRosa et al. 2002), because gendered activities (e.g., cooking, cleaning, lawn care) produce different exposure patterns. Exposure measurement may benefit from gendered exposure measurement, comparison of gendered activities across communities (Berhane et al. 2004), or foci on temporal exposure characteristics (e.g., diurnal trends in residential exposures and activities, critical life-course periods related to hormonal composition or roles) (Gilliand et al. 2005). Assignment of gendered exposures broadly to sex-stratified groups, however, should be generally avoided, because this practice obscures sources of variability between men and women, further confounding sex effects in subsequent epidemiologic analyses.
Temporally refined exposure assessment may elucidate gendered activity distributions. Recent approaches include probabilistic modeling of personal exposures (Zidek et al. 2005). Techniques from the social sciences may be useful; the experience sampling method (Csikszentmihalyi and Larson 1987) uses cell phones or pagers to prompt individuals throughout the day to record their location, activities, and well-being. The technique improves upon diary entries, which suffer recall bias, and allows more detail in activity reports (e.g., cleaning activity with duration and product name) with contemporaneous physiological or psychological conditions that may modify effects. Aggregated, the data provide population-specific activity distributions and capture mean daily activity and exposure differences between men and women.
Physiologically based pharmacokinetic (PBPK) modeling may help to distinguish sex differences in dermal absorption, body size, and toxicity (Arbuckle 2006; Meibohm et al. 2002) from gendered exposures. PBPK models may facilitate analysis of biological processes across multiple life stages (e.g., infancy, childhood, puberty, adulthood) and, among women, by reproductive cycle and hormonal status (e.g., menarche, pregnancy, lactation, menopause). Better understanding of sex and life-stage aspects of bodily chemical transport may help to elucidate differences in effective dose or chemical interactions in the body.
Propensity analysis incorporates predictive modeling for both exposures and responses, enabling researchers to predict subjects’ propensity (likelihood) of exposure, given preexposure characteristics and population exposure distributions. Researchers can then examine health responses among individuals with comparable exposure likelihoods, using propensity matching or propensity stratification (Kurth et al. 2006). For example, sex-stratified propensity models can estimate effects of education, work history, SES, family structure, and home demands on exposure assignment (e.g., job, neighborhood of residence) for men and women. Then researchers can better observe health responses by sex, reasonably isolating effects of mean biological differences from those of gendered exposure assignment. One recent occupational study examined blue-collar status and hypertension among employees of a large U.S. manufacturing company (Clougherty et al. 2009). Family structure influenced exposure (job) assignment for men and women; single mothers were more likely to be blue-collar workers than were other women. Men with partners and children were more likely to be white-collar workers than were other men. Blue-collar status increased risks solely among women predicted to be blue collar, suggesting interaction effects between SES (which predicted job assignment) and on-the-job exposures.
Finally, researchers have proposed variants of multilevel modeling (Phillips 2005) to disaggregate variability between and within the sexes. Researchers may differentiate sex-linked biological effects (e.g., target organs, hormonal composition), which can differ substantially between men and women, from gendered exposures, which generally display more variability among men and women. The technique may be applicable, however, only to illnesses directly involving biological parameters (e.g., sex organs, hormonal composition) which differ strongly by sex. A different method for employing multilevel modeling stems from the societal-level construction of gender, whereas sex is an individual-level biological construct. Examining men’s and women’s exposure and disease patterns across and within societies that vary in measures of gender equity (e.g., income disparities, female education, reproductive rights) may offer important clues toward understanding root causes of exposure and susceptibility differences (Phillips 2008).
Conclusions
Studies suggest that health responses to air pollution may differ between women and men and between girls and boys. It remains unclear, however, whether observed modification is a result of sex-linked biological differences (e.g., hormonal complement, body size) or gender differences in activity patterns, coexposures, or exposure measurement accuracy. Most modification likely consists of some combination of these two factors (exposure patterns and biological response); disentangling these effects is challenging yet necessary toward fully understanding the relevant pathways for differential air pollution effects on health.
Because gender varies by state and society, designing effective localized health interventions requires clarity about these distinct sources of difference (gender and sex), with an aim of improving population health. Careful consideration of gender and sex effects and exploration of nascent methods for quantitative gender analysis may help to elucidate sources of difference. More broadly, exploring the role for gender analysis in environmental epidemiology may provide a model for exploring other social factors that can shape population responses to air pollution.
Footnotes
Many thanks to N. Krieger, M. Perry, J. Dennerlein, J. Levy, and C. Katz for helpful suggestions in the early development of the manuscript and to N. Jeffrey and M. Simons for reviewing the manuscript.
References
- Abbey DE, Burchette RJ, Knutsen SF. Long-term particulates and other air pollutants and lung function in nonsmokers. Am J Resp Crit Care Med. 1998;158:289–298. doi: 10.1164/ajrccm.158.1.9710101. [DOI] [PubMed] [Google Scholar]
- Ackermann-Liebrich U, Leuenberger P, Schwartz J, Schindler C, Monn C, Bolognini G, et al. Lung function and long term exposure to air pollutants in Switzerland. Study on Air Pollution and Lung Diseases in Adults (SAPALDIA) team. Am J Respir Crit Care Med. 1997;155(1):122–129. doi: 10.1164/ajrccm.155.1.9001300. [DOI] [PubMed] [Google Scholar]
- Åkesson A, Berglund M, Schütz A, Bjellerup P, Bremme K, Vahter M. Cadmium exposure in pregnancy and lactation in relation to iron status. Am J Public Health. 2002;92(2):284–287. doi: 10.2105/ajph.92.2.284. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Alexanderson K, Östlin P. Work and Ill-Health among Men and Women in Sweden. In: Markland S, editor. Worklife and Health in Sweden. Stockholm: National Institute for Working Life; 2001. pp. 119–134. [Google Scholar]
- Arbuckle TE. Are there sex and gender differences in acute exposure to chemicals in the same setting? Environ Res. 2006;101:195–204. doi: 10.1016/j.envres.2005.08.015. [DOI] [PubMed] [Google Scholar]
- Arcand R, Labreche F, Messing K, Stock S, Tissot F. Enquete sociale et de sante 1998 (Social and Health Survey 1998) [in French] Quebec: Institute de la statistique du Quebec; 2000. Work environment and health [Environnement de travail et santé] pp. 525–570. [Google Scholar]
- Barregård L, Svalander C, Schütz A, Westberg G, Sällsten G, Blohmé I, et al. Cadmium, mercury, and lead in kidney cortex of the general Swedish population: a study of biopsies from living kidney donors. Environ Health Perspect. 1999;107:867–871. doi: 10.1289/ehp.107-1566723. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bashir SJ, Maibach HI. Cutaneous metabolism of xenobiotics. In: Bronaugh RL, Maibach HI, editors. Topical Absorption of Dermatological Products. New York: Marcel Dekker; 2002. pp. 77–92. [Google Scholar]
- Becklake MR, Kauffmann F. Gender differences in air-way behaviour over the human life span. Thorax. 1999;54:1119–1138. doi: 10.1136/thx.54.12.1119. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Behera D. An analysis of effect of common domestic fuels on respiratory function. Indian J Chest Dis Allied Sci. 1997;39:235–243. [PubMed] [Google Scholar]
- Behera D, Balamugesh T. Indoor air pollution as a risk factor for lung cancer in women. J Assoc Physicians India. 2005;53:190–192. [PubMed] [Google Scholar]
- Bennett WD, Zeman KL, Kim C. Variability of fine particle deposition in healthy subjects: effect of age and gender. Am J Resp Crit Care Med. 1996;153:1641–1647. doi: 10.1164/ajrccm.153.5.8630615. [DOI] [PubMed] [Google Scholar]
- Berhane K, Gauderman WJ, Stram DO, Thomas DC. Statistical issues in studies of the long term effects of air pollution: the Southern California Children’s Health Study. Stat Sci. 2004;19(3):414–449. [Google Scholar]
- Berhane K, McConnell R, Gilliand F, Islam T, Gauderman WJ, Avol E, et al. Sex-specific effects of asthma on pulmonary function in children. Am J Resp Crit Care Med. 2000;162:1723–1730. doi: 10.1164/ajrccm.162.5.2001116. [DOI] [PubMed] [Google Scholar]
- Bourbonnais R, Larocque B, Brisson C, Vezina M, Laliberte D, Courtemanche N. Environnement psychosocial du travail (The psychosocial environment of work) [in French] In: Daveluy C, Audet R, Lapointe F, editors. Enquete sociale et de sante (Social and Health Survey 2000) Quebec: Institut de la statistique; 2000. pp. 571–583. [Google Scholar]
- Brauner EV, Mortensen J, Moller P, Bernard A, Vinzents P, Wahlin P, et al. Effects of ambient air particulate exposure on blood-gas barrier permeability and lung function. Inhal Toxicol. 2009;21(1):38–47. doi: 10.1080/08958370802304735. [DOI] [PubMed] [Google Scholar]
- Brunekreef B, Janssen NAH, Hartog J, Harssema H, Knape M, van Vliet P. Air pollution from truck traffic and lung function in children living near motorways. Epidemiology. 1997;8(3):298–303. doi: 10.1097/00001648-199705000-00012. [DOI] [PubMed] [Google Scholar]
- Cesaroni G, Badaloni C, Porta D, Forastiere F, Perucci CA. Comparison between several indices of exposure to traffic-related air pollution and their respiratory health impact in adults. Occup Environ Med. 2008;65(10):683–690. doi: 10.1136/oem.2007.037846. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Chen E, Schreier HMC, Strunk R, Brauer M. Chronic traffic-related air pollution and stress interact to predict biologic and clinical outcomes in asthma. Environ Health Perspect. 2008;116:970–975. doi: 10.1289/ehp.11076. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Chen Y, Dales R, Krewski D, Breithaupt K. Increased effects of smoking and obesity on asthma among female Canadians: the National Population Health Survey, 1994–1995. Am J Epidemiol. 1999;150:255–262. doi: 10.1093/oxfordjournals.aje.a009996. [DOI] [PubMed] [Google Scholar]
- Chen Y, Rennie DC, Lockinger LA, Dosman JA. Gender, environmental tobacco smoke, and pulmonary function in rural children and adolescents: the Humboldt study. J Agric Saf Health. 2005;11(2):167–173. doi: 10.13031/2013.18183. [DOI] [PubMed] [Google Scholar]
- Chestnut LG, Schwartz J, Savitz DA, Burchfiel CM. Pulmonary function and ambient particulate matter: Epidemiological evidence from NHANES I. Arch Environ Health. 1991;46(3):135–144. doi: 10.1080/00039896.1991.9937440. [DOI] [PubMed] [Google Scholar]
- Clougherty JE, Eisen EA, Slade MD, Kawachi I, Cullen MR. Workplace status and risk of hypertension among hourly and salaried aluminum manufacturing employees. Soc Sci Med. 2009;68(2):304–313. doi: 10.1016/j.socscimed.2008.10.014. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Clougherty JE, Kubzansky LD. A framework for examining social stress and susceptibility to air pollution in respiratory health. Environ Health Perspect. 2009;117:1351–1358. doi: 10.1289/ehp.0900612. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Clougherty JE, Levy JI, Hynes HP, Spengler JD. A longitudinal analysis of the efficacy of environmental interventions on asthma-related quality of life and symptoms among children in urban public housing. J Asthma. 2006;43:335–343. doi: 10.1080/02770900600701408. [DOI] [PubMed] [Google Scholar]
- Clougherty JE, Levy JI, Kubzansky LD, Ryan PB, Suglia SF, Canner MJ, et al. Synergistic effects of traffic-related air pollution and exposure to violence on urban asthma etiology. Environ Health Perspect. 2007;115:1140–1146. doi: 10.1289/ehp.9863. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Concha G, Vogler G, Nermell B, Vahter M. Low-level arsenic excretion in breast milk of native Andean women exposed to high levels of arsenic in drinking water. Int Arch Occup Environ Health. 1998;71:42–46. doi: 10.1007/s004200050248. [DOI] [PubMed] [Google Scholar]
- Csikszentmihalyi M, Larson R. Validity and reliability of the experience-sampling method. J Nerv Ment Dis. 1987;175(9):526–536. doi: 10.1097/00005053-198709000-00004. [DOI] [PubMed] [Google Scholar]
- Cuijpers CEJ, Swaen GMH, Wessling G, Sturmans F, Wouters EFM. Adverse effects of the indoor environment on respiratory health in primary school children. Environ Res. 1995;86:11–23. doi: 10.1006/enrs.1995.1003. [DOI] [PubMed] [Google Scholar]
- Cunningham J, Dockery DW, Speizer FE. Maternal smoking during pregnancy as a predictor of lung function in children. Am J Epidemiol. 1994;139:1139–1152. doi: 10.1093/oxfordjournals.aje.a116961. [DOI] [PubMed] [Google Scholar]
- Davis MC, Matthews KA, Twamley EW. Is life more difficult on Mars or Venus? A meta-analytic review of sex differences in major and minor life events. Ann Behav Med. 1999;21(1):83–97. doi: 10.1007/BF02895038. [DOI] [PubMed] [Google Scholar]
- Delfino RJ, Quintana PJE, Floro J, Gastanaga VM, Samini BS, Kleinman MT, et al. Association of FEV1 in asthmatic children with personal and microenvironmental exposure to airborne particulate matter. Environ Health Perspect. 2004;112:932–941. doi: 10.1289/ehp.6815. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dionisio KL, Howie S, Fornace KM, Chimah O, Adegbola RA, Ezzati M. Measuring the exposure of infants and children to indoor air pollution from biomass fuels in the Gambia. Indoor Air. 2008;18(4):317–327. doi: 10.1111/j.1600-0668.2008.00533.x. [DOI] [PubMed] [Google Scholar]
- Emenius G, Pershagen G, Berglind N, Kwon H-J, Lewne M, Nordvall SL, et al. NO2, as a marker of air pollution, and recurrent wheezing in children: a nested case-control study within the BAMSE birth cohort. Occup Environ Med. 2003;60:876–881. doi: 10.1136/oem.60.11.876. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ernstgard L, Gullstrand E, Lof A, Johansson J. Are women more sensitive than men to 2-propanol and m-xylene vapours? Occup Environ Med. 2002;59:759–767. doi: 10.1136/oem.59.11.759. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Florey CV, Melia RJW, Chinn S. The relation between respiratory illness in primary schoolchildren and the use of gas for cooking. III. Nitrogen dioxide, respiratory illness, and lung function. Int J Epidemiol. 1979;8:347–353. doi: 10.1093/ije/8.4.347. [DOI] [PubMed] [Google Scholar]
- Franklin M, Zeka A, Schwartz J. Association between PM2.5 and all-cause and specific-cause mortality in 27 US communities. J Expo Sci Environ Epidemiol. 2007;17:279–287. doi: 10.1038/sj.jes.7500530. [DOI] [PubMed] [Google Scholar]
- Galizia A, Kinney PL. Long-term residence in areas of high ozone associations with respiratory health in a nationwide sample of nonsmoking young adults. Environ Health Perspect. 1999;107:675–679. doi: 10.1289/ehp.99107675. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gauderman WJ, Avol E, Gilliand F. The effect of air pollution on lung development from 10 to 18 years of age. N Eng J Med. 2004;351:1057–1067. doi: 10.1056/NEJMoa040610. [DOI] [PubMed] [Google Scholar]
- Gauderman WJ, McConnell R, Gilliand F. Association between air pollution and lung function growth in Southern California children. Am J Resp Crit Care Med. 2000;162(pt 1):1383–1390. doi: 10.1164/ajrccm.162.4.9909096. [DOI] [PubMed] [Google Scholar]
- Gehring U, Cyrys J, Sedlmeir G, Brunekreef B, Bellander T, Fischer P, et al. Traffic-related air pollution and respiratory health during the first 3 years of life. Eur Respir J. 2002;19:690–698. doi: 10.1183/09031936.02.01182001. [DOI] [PubMed] [Google Scholar]
- Gilliand F, Avol E, Kinney PL, Jerrett M, Dvonch T, Lurmann F, et al. Air pollution exposure assessment for epidemiologic studies of pregnant women and children: lessons learned from the Centers for Children’s Environmental Health and Disease Prevention Research. Environ Health Perspect. 2005;113:1447–1454. doi: 10.1289/ehp.7673. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gold DR, Wang X, Wypij D, Speizer FE, Ware JH, Dockery DW. Effects of cigarette smoking on lung function in adolescent boys and girls. N Eng J Med. 1996;335(13):931–937. doi: 10.1056/NEJM199609263351304. [DOI] [PubMed] [Google Scholar]
- Gold DR, Wypij D, Wang X, Speizer FE, Pugh M, Ware JH, et al. Gender- and race-specific effects of asthma and wheeze on level and growth of lung function in children in six U.S. cities. Am J Resp Crit Care Med. 1994;149(5):1198–1208. doi: 10.1164/ajrccm.149.5.8173760. [DOI] [PubMed] [Google Scholar]
- Goodman DE, Israel E, Rosenberg M, Johnston R, Weiss ST, Drazen JM. The influence of age, diagnosis, and gender on proper use of metered-dose inhalers. Am J Resp Crit Care Med. 1994;150(5):1256–1261. doi: 10.1164/ajrccm.150.5.7952549. [DOI] [PubMed] [Google Scholar]
- Gordon MT, Riger S. The Female Fear: The Social Cost of Rape. Chicago: University of Illinois Press; 1991. [Google Scholar]
- Grobbelaar JJ, Bateman ED. Hut lung: a domestically acquired pneumoconiosis of mixed aetiology in rural women. Thorax. 1991;46:334–340. doi: 10.1136/thx.46.5.334. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gunshin H, Mackenzie B, Berger UV, Gunshin Y, Romero MF, Boron WF, et al. Cloning and characterization of a mammalian proton-coupled metal-ion transporter. Nature. 1997;338:482–488. doi: 10.1038/41343. [DOI] [PubMed] [Google Scholar]
- Gutek BA. Women and paid work. Psychol Women Q. 2001;25(4):379–393. [Google Scholar]
- Hall EM. Gender, work control, and stress: a theoretical discussion and an empirical test. Int J Health Serv. 1989;19:725–745. doi: 10.2190/5MYW-PGP9-4M72-TPXF. [DOI] [PubMed] [Google Scholar]
- Hasselblad V, Humble CG, Graham MG. Indoor environmental determinants of lung function in children. Am Rev Respir Dis. 1981;123:479–485. doi: 10.1164/arrd.1981.123.5.479. [DOI] [PubMed] [Google Scholar]
- Hermes G, Rosenthal L, Montag A, McClintock MK. Social isolation and the inflammatory response: sex differences in the enduring effects of a prior stressor. Am J Physiol Regul Integr Comp Physiol. 2006;290:R273–R282. doi: 10.1152/ajpregu.00368.2005. [DOI] [PubMed] [Google Scholar]
- Hultman P, Nielsen JB. The effect of dose, gender, and non-H-2 genes in murine mercury-induced autoimmunity. J Autoimmun. 2001;17:27–37. doi: 10.1006/jaut.2001.0521. [DOI] [PubMed] [Google Scholar]
- Hursidic-Radulovic A, Mustajbegovic J, Zuskin E, Ivankovic D, Schachter EN. Gender related differences of low level exposure to occupational irritants—a three-year follow-up of chemical industry workers. Coll Antropol. 2002;26(suppl 1):109–118. [PubMed] [Google Scholar]
- Ito K, Thurston GD. Daily PM10/ mortality associations: an investigation of at-risk populations. J Expo Anal Environ Epidemiol. 1996;6(1):79–95. [PubMed] [Google Scholar]
- Iwasaki-Sekino A, Mano-Otagiri A, Ohata H, Yamauchi N, Shibasaki T. Gender differences in corticotropin and corticosterone secretion and corticotropin-releasing factor mRNA expression in the paraventricular nucleus of the hypothalamus and the central nucleus of the amygdala in response to footshock stress or psychological stress in rats. Psychoneuroendocrinology. 2009;34:226–237. doi: 10.1016/j.psyneuen.2008.09.003. [DOI] [PubMed] [Google Scholar]
- Jedrychowski W, Flak E, Mroz E. The adverse effect of low levels of ambient air pollutants on lung function growth in preadolescent children. Environ Health Perspect. 1999;107:669–674. doi: 10.1289/ehp.99107669. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jedrychowski W, Krzyzanowski M. Ventilatory lung function and chronic chest symptoms among the inhabitants of urban areas with various levels of acid aerosols: prospective study in Cracow. Environ Health Perspect. 1989;79:101–107. doi: 10.1289/ehp.8979101. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jerrett M, Burnett R, Brook J, Kanaraglou P, Giovis C, Finkelstein J, et al. Do socioeconomic characteristics modify the short term association between air pollution and mortality? Evidence from a zonal time series in Hamilton, Canada. J Epidemiol Community Health. 2004;58:31–40. doi: 10.1136/jech.58.1.31. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Jones AY, Lam PK. End-expiratory carbon monoxide levels in healthy subjects living in a densely populated urban environment. Sci Total Environ. 2006;354(2–3):150–156. doi: 10.1016/j.scitotenv.2005.02.018. [DOI] [PubMed] [Google Scholar]
- Kan H, Heiss G, Rose KM. Traffic exposure and lung function in adults: the Atherosclerosis in Communities study. Thorax. 2007;62:873–879. doi: 10.1136/thx.2006.073015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kan H, London SJ, Chen G, Zhang Y, Song G, Zhao N, et al. Season, sex, age, and education as modifiers of the effects of outdoor air pollution on daily mortality in Shanghai, China: the Public Health and Air Pollution in Asia (PAPA) study. Environ Health Perspect. 2008;116:1183–1188. doi: 10.1289/ehp.10851. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kanner RE, Connett JE, Altose MD, Buist AS, Lee WW, Tashkin DP, et al. Gender difference in airway hyperresponsiveness in smokers with mild COPD. The Lung Health Study. Am J Resp Crit Care Med. 1994;150(4):956–961. doi: 10.1164/ajrccm.150.4.7921469. [DOI] [PubMed] [Google Scholar]
- Katz C. Growing girls/closing circles: limits on the spaces of knowing in rural Sudan and US cities. In: Katz C, Monk J, editors. Full Circles: Geographies of Women over the Lifecourse. New York: Routledge; 1993. pp. 88–106. [Google Scholar]
- Keitt SK, Fagan TF, Marts SA. Understanding sex differences in environmental health: a thought leaders’ roundtable. Environ Health Perspect. 2004;112:604–609. doi: 10.1289/ehp.6714. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Khushk WA, Fatmi Z, White F, Kadir MM. Health and social impacts of improved stoves on rural women: a pilot intervention in Sindh, Pakistan. Indoor Air. 2005;15:311–316. doi: 10.1111/j.1600-0668.2005.00367.x. [DOI] [PubMed] [Google Scholar]
- Kim CS, Hu SC. Regional deposition of inhaled particles in human lungs: comparison between men and women. J Appl Physiol. 1998;84(6):1834–1844. doi: 10.1152/jappl.1998.84.6.1834. [DOI] [PubMed] [Google Scholar]
- Kim CS, Hu SC. Total respiratory tract deposition of fine micrometer-sized particles in healthy adults: empirical equations for sex and breathing pattern. J Appl Physiol. 2006;101:401–412. doi: 10.1152/japplphysiol.00026.2006. [DOI] [PubMed] [Google Scholar]
- Kingsley G. Housing, health, and the neighborhood context. Am J Prev Med. 2003;24(3 suppl):6–7. doi: 10.1016/s0749-3797(02)00651-7. [DOI] [PubMed] [Google Scholar]
- Knol MJ, Egger M, Scott P, Geerlings MI, Vandenbroucke JP. When one depends on the other: reporting of interactions in case-control and cohort studies. Epidemiology. 2009;20(2):161–166. doi: 10.1097/EDE.0b013e31818f6651. [DOI] [PubMed] [Google Scholar]
- Kohlhaufl M, Brand P, Scheuch G, Meyer TS, Schulz H, Haussinger K. Increased fine particle deposition in women with asymptomatic nonspecific airway hyperresponsiveness. Am J Resp Crit Care Med. 1999;159(3):902–906. doi: 10.1164/ajrccm.159.3.9805036. [DOI] [PubMed] [Google Scholar]
- Korrick SA, Neas LM, Dockery DW, Gold DR, Allen GA, Hill LB, et al. Effects of ozone and other pollutants on the pulmonary function of adult hikers. Environ Health Perspect. 1998;106:93–99. doi: 10.1289/ehp.9810693. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Krieger N. Genders, sexes, and health: what are the differences, and why does it matter? Int J Epidemiol. 2003;32:652–657. doi: 10.1093/ije/dyg156. [DOI] [PubMed] [Google Scholar]
- Kulkarni N, Pierse N, Rushton L, Grigg J. Carbon in airway macrophages and lung function in children. N Engl J Med. 2006;355(1):21–30. doi: 10.1056/NEJMoa052972. [DOI] [PubMed] [Google Scholar]
- Kurth T, Walker A, Glynn R, Chan K, Gaziano J, Berger K, et al. Results of multivariable logistic regression, propensity matching, propensity adjustment, and propensity-based weighting under conditions of non-uniform effect. Am J Epidemiol. 2006;163(3):262–270. doi: 10.1093/aje/kwj047. [DOI] [PubMed] [Google Scholar]
- LaRosa LE, Buckley TJ, Wallace LA. Real-time indoor and outdoor measurements of black carbon in an occupied house: an examination of sources. J Air Waste Manag Assoc. 2002;52:41–49. doi: 10.1080/10473289.2002.10470758. [DOI] [PubMed] [Google Scholar]
- Li N, Phalen RF, Hinds WC, Nel AE. Particulate air pollutants and asthma: a paradigm for the role of oxidative stress in PM-induced adverse health effects. Clin Immunol. 2003;109:250–265. doi: 10.1016/j.clim.2003.08.006. [DOI] [PubMed] [Google Scholar]
- Lin M, Steib DM, Chen Y. Coarse particulate matter and hospitalization for respiratory infections in children younger than 15 years in Toronto: a case-crossover analysis. Pediatrics. 2005;116:2004–2012. doi: 10.1542/peds.2004-2012. [DOI] [PubMed] [Google Scholar]
- Liu L, Poon R, Chen L, Frescura AM, Montuschi P, Ciabattoni G, et al. Acute effects of air pollution on pulmonary function, airway inflammation, and oxidative stress in asthmatic children. Environ Health Perspect. 2009;117:668–674. doi: 10.1289/ehp11813. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lodrup Carlsen KC, Lovik M, Granum B, Mowinckel P, Carlsen KH. Soluble CD14 at 2 yr of age: gender-related effects of tobacco smoke exposure, recurrent infections and atopic diseases. Pediatr Allergy Immunol. 2006;17(4):304–312. doi: 10.1111/j.1399-3038.2006.00412.x. [DOI] [PubMed] [Google Scholar]
- London L, de Grosbois S, Wesseling C, Kisting S, Rother HA, Mergler D. Pesticide usage and health consequences for women in developing countries: out of sight, out of mind? Int J Occup Environ Health. 2002;8(1):46–59. doi: 10.1179/oeh.2002.8.1.46. [DOI] [PubMed] [Google Scholar]
- Lopez AD, Mathers CD, Ezzati M, Jamison DT, Murray CJL. Global Burden of Disease and Risk Factors. Washington, DC: World Bank Publications; 2006. [PubMed] [Google Scholar]
- Luginaah IN, Fung KY, Gorey KM, Webster G, Wills C. Association of ambient air pollution with respiratory hospitalization in a government-designated “area of concern”: the case of Windsor, Ontario. Environ Health Perspect. 2005;113:290–296. doi: 10.1289/ehp.7300. [DOI] [PMC free article] [PubMed] [Google Scholar]
- MacDonald L, Karasek R, Punnett L, Scharf T. Covariation between workplace physical and psychosocial stressors: evidence and implications for occupational health research and prevention. Ergonomics. 2001;44(7):696–718. doi: 10.1080/00140130119943. [DOI] [PubMed] [Google Scholar]
- Maziak W, Ward KD, Mzavek F, Rastam S, Bachir ME, Fouad MF, et al. Mapping the health and environmental situation in informal zones in Aleppo, Syria: report from the Aleppo household survey. Int Arch Occup Environ Health. 2005;78(7):547–558. doi: 10.1007/s00420-005-0625-7. [DOI] [PubMed] [Google Scholar]
- McConnell R, Berhane K, Gilliand F, London SJ, Islam T, Gauderman WJ, et al. Asthma in exercising children exposed to ozone: a cohort study. Lancet. 2002;359:386–391. doi: 10.1016/S0140-6736(02)07597-9. [DOI] [PubMed] [Google Scholar]
- McCracken JP, Smith KR, Diaz A, Mittleman M, Schwartz J. Chimney stove intervention to reduce long-term wood smoke exposure lowers blood pressure among Guatemalan women. Environ Health Perspect. 2007;115:996–1001. doi: 10.1289/ehp.9888. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Meding B. Differences between sexes with regard to work-related skin disease. Contact Derm. 2000;43:65–71. doi: 10.1034/j.1600-0536.2000.043002065.x. [DOI] [PubMed] [Google Scholar]
- Meibohm B, Beierle I, Derendorf H. How important are gender differences in pharmacokinetics? Clin Pharmacokinet. 2002;41(5):329–342. doi: 10.2165/00003088-200241050-00002. [DOI] [PubMed] [Google Scholar]
- Melia JW, Florey CV, Altman DG. Association between gas cooking and respiratory disease in children. Br Med J. 1977;2:149–152. doi: 10.1136/bmj.2.6080.149. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Messing K, Punnett L, Bond M, Alexanderson K, Pyle J, Zahm S, et al. Be the fairest of them all: challenges and recommendations for the treatment of gender in occupational health research. Am J Ind Med. 2003;43:618–619. doi: 10.1002/ajim.10225. [DOI] [PubMed] [Google Scholar]
- Messing K, Stellman JM. Sex, gender, and women’s occupational health: the importance of considering mechanism. Environ Res. 2006;101:146–162. doi: 10.1016/j.envres.2005.03.015. [DOI] [PubMed] [Google Scholar]
- Morello-Frosch R, Shenassa ED. The environmental “riskscape” and social inequality: implications for explaining maternal and child disparities. Environ Health Perspect. 2006;114:1150–1153. doi: 10.1289/ehp.8930. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Morris ME, Lee HJ, Predko LM. Gender differences in the membrane transport of endogenous and exogenous compounds. Pharmacol Rev. 2003;55:229–240. doi: 10.1124/pr.55.2.1. [DOI] [PubMed] [Google Scholar]
- National Library of Medicine. PubMed. 2009. [[accessed 17 July 2009]]. Available: http://www.ncbi.nlm.nih.gov/sites/entrez?db=pubmed.
- Neas LM, Dockery DW, Ware JH, Spengler JD, Speizer FE, Ferris BG., Jr Association of indoor nitrogen dioxide with respiratory symptoms and pulmonary function in children. Am J Epidemiol. 1991;134:204–219. doi: 10.1093/oxfordjournals.aje.a116073. [DOI] [PubMed] [Google Scholar]
- Nethery E, Brauer M, Janssen P. Time-activity patterns of pregnant women and changes during the course of pregnancy. J Expo Sci Environ Epidemiol. 2009;19:317–324. doi: 10.1038/jes.2008.24. [DOI] [PubMed] [Google Scholar]
- Nordling E, Berglind N, Melen E, Emenius G, Hallberg J, Nyberg F, et al. Traffic-related air pollution and childhood respiratory symptoms, function, and allergies. Epidemiology. 2008;19(3):401–408. doi: 10.1097/EDE.0b013e31816a1ce3. [DOI] [PubMed] [Google Scholar]
- O’Neill M, Jerrett M, Kawachi I, Levy J, Cohen A, Gouveia N, et al. Health, wealth, and air pollution: advancing theory and method. Environ Health Perspect. 2003;111:1861–1870. doi: 10.1289/ehp.6334. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Oftedal B, Brunekreef B, Nystad W, Madsen C, Walker S-E, Nafstad P. Residential outdoor air pollution and lung function in schoolchildren. Epidemiology. 2008;19(1):129–137. doi: 10.1097/EDE.0b013e31815c0827. [DOI] [PubMed] [Google Scholar]
- Oosterlee A, Drijver M, Lebret E, Brunekreef B. Chronic respiratory symptoms in children and adults living along streets with high traffic density. Occup Environ Med. 1996;53:241–247. doi: 10.1136/oem.53.4.241. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ormond G, Nieuwenhuijsen MJ, Nelson P, Toledano MB, Iszatt N, Geneletti S, et al. Endocrine disruptors in the workplace, hair spray, folate supplementation, and risk of hypospadias: case–control study. Environ Health Perspect. 2008;117:303–307. doi: 10.1289/ehp.11933. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pandey MR. Domestic smoke pollution and chronic bronchitis in a rural community of the Hille region of Nepal. Thorax. 1984;39:337–339. doi: 10.1136/thx.39.5.337. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Payne-Sturges DC, Burke TA, Breysse PN, Diener-West M, Buckley TJ. Personal exposure meets risk assessment: a comparison of measured and modeled exposures and risks in an urban community. Environ Health Perspect. 2004;112:589–598. doi: 10.1289/ehp.6496. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pershagen G, Rylander E, Norberg S, Eriksson M, Nordvall SL. Air pollution involving nitrogen dioxide exposure and wheezing bronchitis in children. Int J Epidemiol. 1995;24(6):1147–1153. doi: 10.1093/ije/24.6.1147. [DOI] [PubMed] [Google Scholar]
- Peters JM, Avol E, Gauderman WJ. A study of twelve Southern California communities with differing levels and types of air pollution. II. Effects on pulmonary function. Am J Resp Crit Care Med. 1999;159:768–775. doi: 10.1164/ajrccm.159.3.9804144. [DOI] [PubMed] [Google Scholar]
- Phillips SP. Defining and measuring gender: a social determinant of health whose time has come. Int J Equity Health. 2005;4:11. doi: 10.1186/1475-9276-4-11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Phillips SP. Measuring the health effects of gender. J Epidemiol Commun Health. 2008;62:368–371. doi: 10.1136/jech.2007.062158. [DOI] [PubMed] [Google Scholar]
- Powell LH, Matthews KA. New directions in understanding the link between stress and health in women. Int J Behav Med. 2002;9(3):173–175. doi: 10.1207/s15327558ijbm0903_01. [DOI] [PubMed] [Google Scholar]
- Prescott E, Bjerg AM, Anderson PK, Lange P, Vestbo J. Gender differences in smoking effects on lung function and risk of hospitalization for COPD: results from a Danish longitudinal population study. Eur Respir J. 1997;10:822–827. [PubMed] [Google Scholar]
- Prisby RD, Muller-Delp J, Delp MD, Nurkiewicz TR. Age, gender, and hormonal status modulate the vascular toxicity of the diesel exhaust extract phenanthraquinone. J Toxicol Environ Health A. 2008;71(7):464–470. doi: 10.1080/15287390701839349. [DOI] [PubMed] [Google Scholar]
- Qureshi KA. Domestic smoke pollution and prevalence of chronic bronchitis/asthma in a rural area of Kashmir. Indian J Chest Dis Allied Sci. 1994;36:61–72. [PubMed] [Google Scholar]
- Ramirez-Venegas A, Sansores RH, Perez-Padilla R, Regalado J, Valazquez A, Sanchez C, et al. Survival of patients with chronic obstructive pulmonary disease due to biomass smoke and tobacco. Am J Resp Crit Care Med. 2006;173:393–397. doi: 10.1164/rccm.200504-568OC. [DOI] [PubMed] [Google Scholar]
- Redline S, Gold DR. Challenges in interpreting gender differences in asthma. Am J Resp Crit Care Med. 1994;150:1219–1221. doi: 10.1164/ajrccm.150.5.7952543. [DOI] [PubMed] [Google Scholar]
- Roberts JS, Silbergeld EK. Pregnancy, lactation, and menopause: how physiology and gender affect the toxicity of chemicals. Mt Sinai J Med. 1995;62:343–355. [PubMed] [Google Scholar]
- Roemer W, Clench-Aas J, Englert N, Hoek G, Katsouyanni K, Pekkanen J, et al. Inhomogeneity in response to air pollution in European children (PEACE project) Occup Environ Med. 1999;56:86–92. doi: 10.1136/oem.56.2.86. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rojas-Martinez R, Perez-Padilla R, Olaiz-Fernandez G, Mendoza-Alvarado L, Moreno-Macias H, Fortoul T, et al. Lung function growth in children with long-term exposure to air pollutants in Mexico City. Am J Resp Crit Care Med. 2007;176:377–384. doi: 10.1164/rccm.200510-1678OC. [DOI] [PubMed] [Google Scholar]
- Romieu I, Tellez-Rojo MM, Lazo M, Manzano-Patino A, Cortez-Lugo M, Julien P. Omega-3 fatty acid prevents heart rate variability reductions associated with particulate matter. Am J Resp Crit Care Med. 2005;172(12):1534–1540. doi: 10.1164/rccm.200503-372OC. [DOI] [PubMed] [Google Scholar]
- Rosenlund M, Forastiere F, Porta D, De Sario M, Badaloni C, Perucci CA. Traffic-related air pollution in relation to respiratory symptoms, allergic sensitization, and lung function in school children. Thorax. 2009;64(7):573–580. doi: 10.1136/thx.2007.094953. [DOI] [PubMed] [Google Scholar]
- Rumchev K, Spickett JT, Brown HL, Mkhweli B. Indoor air pollution from biomass combustion and respiratory symptoms of women and children in a Zimbabwean village. Indoor Air. 2007;17(6):468–474. doi: 10.1111/j.1600-0668.2007.00494.x. [DOI] [PubMed] [Google Scholar]
- Salminen S, Saari J, Saarela KL, Rasasen T. Risk factors for women in serious occupational accidents. Occup Health Safety (Austral NZ) 1992;8(4):341–347. [Google Scholar]
- Schachter EN, Zuskin E, Moshler EL, Godbold J, Mustajbegovic J, Pucarin-Cvetkovic J, et al. Gender and respiratory findings in workers occupationally exposed to organic aerosols: a meta analysis of 12 cross-sectional studies. Environ Health. 2009;8(1):1–33. doi: 10.1186/1476-069X-8-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Schauer JJ, Lough GC, Schafer MM, Christensen WF, Arndt MF, DeMinter JT, et al. HEI Research Report 133. Boston: Health Effects Institute; 2006. Characterization of Metals Emitted from Motor Vehicles. [PubMed] [Google Scholar]
- Schwartz J. Lung function and chronic exposure to air pollution: a cross-sectional analyses of NHANES II. Environ Res. 1989;50:309–321. doi: 10.1016/s0013-9351(89)80012-x. [DOI] [PubMed] [Google Scholar]
- Seeman TE, Singer B, Charpentier P. Gender differences in patterns of HPA response to challenge: MacArthur Studies of Successful Aging. Psychoneuroendocrinology. 1995;20:711–725. doi: 10.1016/0306-4530(95)00024-0. [DOI] [PubMed] [Google Scholar]
- Seeman TE, Singer BH, Ryff CD, Dienberg Love G, Levy-Storms L. Social relationships, gender, and allostatic load across two age cohorts. Psychosom Med. 2002;64:395–406. doi: 10.1097/00006842-200205000-00004. [DOI] [PubMed] [Google Scholar]
- Silbergeld EK, Schwartz J, Mahaffey K. Lead and osteoporosis: mobilization of lead from bone in postmenopausal women. Environ Res. 1988;47:79–94. doi: 10.1016/s0013-9351(88)80023-9. [DOI] [PubMed] [Google Scholar]
- Silverstein BA, Fine LJ, Armstrong TJ. Hand wrist cumulative trauma disorders in industry. Br J Ind Med. 1986;43:779–784. doi: 10.1136/oem.43.11.779. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Smith BJ, Nitschke M, Pilotto LS, Ruffin RE, Pisaniello DL, Willson KJ. Health effects of daily indoor nitrogen dioxide exposure in people with asthma. Eur Respir J. 2000;16:879–885. doi: 10.1183/09031936.00.16587900. [DOI] [PubMed] [Google Scholar]
- Sood A, Cui X, Qualis C, Beckett WS, Gross MD, Steffes MW, et al. Association between asthma and serum adiponectin concentration in women. Thorax. 2008;63:877–882. doi: 10.1136/thx.2007.090803. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Stern B, Jones L, Raizenne M, Burnett R, Meranger JC, Franklin CA. Respiratory health effects associated with ambient sulfates and ozone in two rural Canadian communities. Environ Res. 1989;49:20–39. doi: 10.1016/s0013-9351(89)80019-2. [DOI] [PubMed] [Google Scholar]
- Stocks J, Henschen M, Hoo A-F, Costeloe K, Dezateux C. Influence of ethnicity and gender on airway function in preterm infants. Am J Resp Crit Care Med. 1997;156(6):1855–1862. doi: 10.1164/ajrccm.156.6.9607056. [DOI] [PubMed] [Google Scholar]
- Sunyer J, Jarvis D, Gotschi T, Garcia-Esteban R, Jacquemin B, Aguilera I, et al. Chronic bronchitis and urban air pollution in an international study. Occup Environ Med. 2006;63:836–843. doi: 10.1136/oem.2006.027995. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sunyer J, Schwartz J, Tobias A, Macfarlane D, Garcia J, Anto JM. Patients with chronic obstructive pulmonary disease are at increased risk of death associated with urban particulate air pollution: a case-crossover analysis. Am J Epidemiol. 2000;151(1):50–56. doi: 10.1093/oxfordjournals.aje.a010121. [DOI] [PubMed] [Google Scholar]
- Taylor SE, Klein LC, Lewis BP, Gruenewald TL, Gurung RAR, Updegraff JA. Biobehavioral responses to stress in females; tend-and-befriend, not fight-or-flight. Psychol Rev. 2000;107(3):411–429. doi: 10.1037/0033-295x.107.3.411. [DOI] [PubMed] [Google Scholar]
- Thaller EI, Petronella SA, Hochman D, Howard S, Chhikara RS, Brooks EG. Moderate increases in abient PM2.5 and ozone are associated with lung function decreases in beach lifeguards. J Occup Environ Med. 2008;50:202–211. doi: 10.1097/JOM.0b013e31816386b4. [DOI] [PubMed] [Google Scholar]
- van Vliet P, Knape M, de Hartog J, Janssen N, Harssema H, Brunekreef B. Motor exhaust and chronic respiratory symptoms in children living near freeways. Environ Res. 1997;74(2):122–132. doi: 10.1006/enrs.1997.3757. [DOI] [PubMed] [Google Scholar]
- Varkev AB. Chronic obstructive pulmonary disease in women: exploring gender differences. Curr Opin Pulm Med. 2004;10(2):98–103. doi: 10.1097/00063198-200403000-00003. [DOI] [PubMed] [Google Scholar]
- Vollmer WM, Enright PL, Pedula KL, Speizer F, Kuller LH, Kiley J. Race and gender differences in smoking effects on adult pulmonary function. Eur Respir J. 1994;7(3):477–483. doi: 10.1183/09031936.94.07030477. [DOI] [PubMed] [Google Scholar]
- Wang B, Peng Z, Zhang X, Xu Y, Wang H, Allen G, et al. Particulate matter, sulfur dioxide, and pulmonary function in never-smoking adults in Chongqing, China. Int J Occup Environ Health. 1999;5(1):14–19. doi: 10.1179/oeh.1999.5.1.14. [DOI] [PubMed] [Google Scholar]
- Xu X, Li B, Wang L. Gender differences in smoking effects on adult pulmonary function. Eur Respir J. 1994a;7:477–483. doi: 10.1183/09031936.94.07030477. [DOI] [PubMed] [Google Scholar]
- Xu X, Weiss ST, Rijcken B. Smoking, changes in smoking habits, and the rate of decline in FEV1: new insight into gender differences. Eur Respir J. 1994b;7:1056–1061. [PubMed] [Google Scholar]
- Yunginger JW, Reed CE, O’Connell EJ, Melton LJI, O’Fallon WM, Silverstein MD. A community-based study of the epidemiology of asthma. Incidence rates, 1964–1983. Am Rev Respir Dis. 1992;146(4):888–894. doi: 10.1164/ajrccm/146.4.888. [DOI] [PubMed] [Google Scholar]
- Zeka A, Zanobetti A, Schwartz J. Individual modifiers of the effects of particulate matter on daily mortality. Am J Epidemiol. 2006;163:849–859. doi: 10.1093/aje/kwj116. [DOI] [PubMed] [Google Scholar]
- Zhao Z, Zhang Z, Wang Z, Ferm M, Liang Y, Norback D. Asthmatic symptoms among pupils in relation to winter indoor and outdoor air pollution in schools in Taiyuan, China. Environ Health Perspect. 2008;116:90–97. doi: 10.1289/ehp.10576. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zidek JV, Shaddick G, White R, Meloche J, Chatfield C. Using a probabilistic model (pCNEM) to estimate personal exposure to air pollution. Environmetrics. 2005;16:481–493. [Google Scholar]