Abstract
The majority of prostate cancers harbor recurrent gene fusions between the hormone-regulated TMPRSS2 and members of the ETS family of transcription factors, most commonly ERG. Prostate cancer with ERG rearrangements represent a distinct subclass of tumor based on studies reporting associations with histomorphologic features, characteristic somatic copy number alterations, and gene expression signatures. The current study describes the frequency of ERG rearrangement prostate cancer and three 5 prime (5') gene fusion partners (i.e., TMPRSS2, SLC45A3 and NDRG1) in a large prostatectomy cohort.
ERG gene rearrangements and mechanism of rearrangement, as well as rearrangements of TMPRSS2, SLC45A3, and NDRG1 were assessed using fluorescence in-situ hybridization (FISH) on prostate cancer samples from 614 patients treated by radical prostatectomy. ERG rearrangement occurred in 53% of the 540 assessable cases. TMPRSS2 and SLC45A3 were the only 5' partner in 78% and 6% of these ERG rearranged cases, respectively. Interestingly, 11% of the ERG rearranged cases demonstrated concurrent TMPRSS2 and SLC45A3 rearrangements. TMPRSS2 or SLC45A3 rearrangements could not be identified for 5% of the ERG rearranged cases. From these remaining cases we identified one case with NDRG1 rearrangement. We did not observe any associations with pathologic parameters or clinical outcome.
This is the first study to describe the frequency of SLC45A3-ERG fusions in a large clinical cohort. Most studies have assumed that all ERG rearrangement prostate cancers harbor TMPRSS2-ERG fusions. This is also the first study to report concurrent TMPRSS2 and SLC45A3 rearrangements in the same tumor focus suggesting additional complexity that had not been previously appreciated. This study has important clinical implications for the development of diagnostic assays to detect ETS rearrangement prostate cancer. Incorporation of these less common ERG rearrangement prostate cancer fusion assays could further increase the sensitivity of these PCR-based approaches.
Keywords: Prostate cancer, ETS rearrangements, prevalence
INTRODUCTION
Since the original description of recurrent gene fusions in prostate cancer involving TMPRSS2 and ETV1 or ERG (1), the list of putative recurrent gene fusions continues to grow (2). As initially observed, these fusions most commonly involve an ETS family member gene fused to a 5 prime (5') hormonally regulated promoter, most often TMPRSS2(3). Few reports have focused on trying to determine how common a particular gene fusion occurs in a population. Over twenty studies from independent research groups (recently reviewed by Tomlins et al. (4) and Clark and Cooper (5)) suggest that ERG rearrangement can be observed in 40–60% of prostate cancers identified through prostate-specific antigen (PSA) screening. These studies were predominately based on the evaluation of tumor samples from men who underwent surgery for clinically localized disease. Mosquera et al. recently reported a frequency of ERG rearrangement in 46% of cases in a prospective PSA-screened prostate cancer biopsy cohort (6).
There is mounting data suggesting that ERG rearranged prostate cancer has several distinct features defining a sub-class of this common epithelial neoplasm. First, mouse model studies over expressing ERG alone (7, 8) or in the context of PTEN loss (9, 10) demonstrate a neoplastic phenotype. Second, associations between histomorphologic features and ERG rearrangement have been observed (6, 11). Third, molecular profiles suggest distinct alterations in pathways, specifically estrogenic signaling, in ERG rearranged prostate cancer (12, 13). Forth, distinct somatic copy number alterations are enriched in ERG rearranged prostate cancers (14). Fifth, if left untreated, ERG rearranged prostate cancers are associated with an unfavorable clinical course as compared to non-ERG rearranged prostate cancer (15, 16). Finally, Attard et al. have demonstrated an ERG rearrangement status dependent response to abiraterone acetate, a CYP17 inhibitor (17). Taken together, ERG rearrangement prostate cancer appears to represent a distinct molecular and clinical sub-class of prostate cancer.
Most studies have taken a shorthand to define the TMPRSS2-ERG fusion cancers. This is based on the use of a fluorescence in situ hybridization (FISH) break apart assay to identify ERG rearrangement as indirect evidence for TMPRSS2-ERG gene fusion(1, 18). A priori knowledge of possible 5' partners involved in ETS rearranged prostate cancers led Han et al. to discover an ERG rearranged case to be fused with SLC45A3 (Solute carrier family 45, member 3, also known as Prostein) as the 5' partner(19). This was the first study to identify an alternate 5' fusion partner of ERG, other than TMPRSS2. Up until then, all cases harboring the ERG rearrangement were believed to contain the TMPRSS2-ERG fusion. To explore for other potential 5' partners of ERG, we recently evaluated all ERG rearranged and ERG over-expressing cases from a population of 101 samples and confirmed the recurrent nature of SLC45A3-ERG fusions. In addition, we discovered NDRG1 (N-myc Downstream Regulated Gene 1) as a novel 5' fusion partner by whole transcriptome sequencing NDRG1 (20).
In the present study, we analyze a large prostatectomy cohort for the presence of TMPRSS2-ERG, SLC45A3-ERG, and NDRG1-ERG fusion events to determine their frequency and potential association with clinical parameters.
MATERIAL AND METHODS
Case Selection and Pathologic Analysis
The cohort consisted of 614 prostate cancer patients who underwent radical prostatectomy between 1999 and 2005 at the Charité Hospital (Berlin, Germany) (Table 1). The demographics of this cohort were recently described (21). In brief, patient age ranged from 43 and 74 years (median 62 years). Preoperative PSA levels ranged from 0.8 to 39 ng/ml (median 7.2 ng/ml). Forty-four patients (7%) had received gonadotropin-releasing hormone analogues at the discretion of the referring urologist, prior to surgery (median 4 weeks, range 2–16 weeks). Clinical follow-up data were reviewed annually. PSA relapse-free survival time was available for 609 patients from this cohort. The median follow-up time of all the cases was 48 months (range 1–108 months) and 89 patients (15%) experienced a PSA relapse after a median time of 13 months (range 1–68). The Gleason scores were distributed as follows: Gleason score 4–6: 217 (35%); Gleason score 7: 291 (48%) Gleason score 8–10: 106 (17%). Organ-confined carcinoma (pT2) was found in 420 patients; 191 showed extraprostatic tumor extension (pT3).
Table 1.
Demographic and clinical characteristics of 540 men (all assessable cases) with clinically localized prostate cancer patients by ERG rearrangement status and mechanism.
| ERG rearranged n= 284 | ERG not rearranged n= 256 | ||
|---|---|---|---|
|
|
|||
| Translocation through deletion | Translocation through insertion | ||
| All assessable cases (540) | 178 (63%) | 106 (37%) | 256 (47%) |
| Age | |||
| ≤ 62 | 86 (32%) | 63 (23%) | 120 (45%) |
| > 62 | 92 (34%) | 43 (16%) | 136 (50%) |
| Preoperative PSA (533) | |||
| ≤ 10 ng/ml | 130 (24%) | 80 (15%) | 173 (33%) |
| > 10 ng/ml | 47 (9%) | 26 (5%) | 77 (14%) |
| pT stage (540) | |||
| pT2 | 111 (30%) | 72 (20%) | 186 (50%) |
| pT3/T4 | 67 (39%) | 34 (20%) | 70 (41%) |
| Gleason score (540) | |||
| 3–6 | 59 (11%) | 36 (7%) | 89 (16%) |
| 7 | 94 (17% | 51 (9%) | 115 (21% |
| 8–10 | 25 (5%) | 19 (4%) | 52 (10%) |
| Biochemical recurrence (515) | |||
| Yes | 146 (28%) | 86 (17%) | 208 (40%) |
| No | 25 (5%) | 16 (3%) | 34 (7%) |
| Anti-androgen therapy (538) | |||
| Yes | 165 (33%) | 102 (20%) | 232 (47%) |
| No | 11 (28%) | 4 (10%) | 24 (62%) |
Tissue microarray construction
Formalin-fixed paraffin-embedded tissue blocks from radical prostatectomy specimens were used for tissue microarray construction (21). Two cores (1.0mm) of invasive prostate cancer were chosen, reflecting the primary and secondary Gleason pattern. In addition, normal prostatic tissue was selected for each case.
Assessment of ERG, TMPRSS2, SLC45A3 and NDRG1 rearrangements using two-color FISH break apart (b/a) assays
Four-micron thick tissue microarray sections were used for interphase FISH analysis. Rearrangement status was determined using a dual-color break-apart interphase FISH assay as described previously (1, 18, 22). In brief, two differentially labeled probes were designed to span the telomeric and centromeric neighboring regions of each locus. The following telomeric/centromeric BAC clones were selected to design break-apart assays to assess for rearrangement status (i.e., rearrangement versus no rearrangement): ERG (RP11-372O17 and RP11-24A11), TMPRSS2 (RP11-120C17 and RP11-35C4), SLC45A3 (RP11-131E5 and RP11-249H15), and NDRG1 (RP11-1145H17 and RP11-185E14). In the case of rearrangement, the assay was also capable of differentiating between two different rearrangement mechanisms (i.e., rearrangement through insertion or rearrangement through deletion) as previously described (18). A nucleus without a gene rearrangement demonstrates two pairs of juxtaposed red and green signals (mostly forming two yellow signals). A nucleus with a rearrangement through insertion shows the split of one red-green (yellow) signal pair, resulting in a single red and green signal for the rearranged allele, and a still combined (yellow) signal for the non-rearranged allele in each nucleus. Finally, a nucleus with a gene rearrangement through deletion shows one juxtaposed red-green signal pair (yellow) for the non-rearranged allele, and a single red or green signal for the allele involved in the rearrangement. Slides were analyzed under a x60 oil immersion objective using an Olympus (Center Valley, PA) BX-51 fluorescence microscope equipped with appropriate filters and a charge-coupled device camera, and the CytoVision FISH imaging and capturing software (Applied Imaging, San Jose, CA). Evaluation was independently performed by a minimum of two evaluators (RE, CJL, SP and VS). For each case a minimum of 100 nuclei were assessed.
In cases with co-occurring ERG rearrangement and rearrangement of one of the three 5' partners (i.e., TMPRSS2, SLC45A3, or NDRG1), we defined these cases harboring a fusion of the rearranged genes.
Statistical analysis
We investigated for significant association between rearrangement status and clinical parameters including patient age, preoperative PSA serum levels, Gleason score, pathological stage using Pearson Chi-square test. We also investigated for associations between biochemical failure and gene fusion status using Kaplan Meier estimates and log rank test.
RESULTS
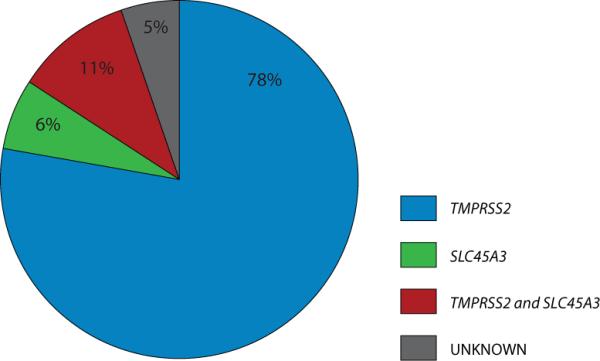
We were able to assess 540 out of 614 cases for ERG rearrangement status. ERG rearrangement was identified in 53% (284/540) of the cases (Figure 1). We then characterized TMPRSS2 and SLC45A3 rearrangement status in the ERG rearrangement positive cases as these are known to be the most common fusion partner for ERG. Out of 284, 254 cases were assessable for both ERG 5' partners (i.e., TMPRSS2 and SLC45A3) in addition to the ERG rearrangement. TMPRSS2 rearrangement was observed in 78% (198/254) of the ERG rearranged cases. SLC45A3 was rearranged in 6% (16/254) of these cases. Interestingly, 11% of the ERG rearranged cases (27/254) harbored concurrent rearrangements of SLC45A3 and TMPRSS2 (Figure 1 and Figure 2).
Figure 1. Pie chart summary of study results.
Frequencies of the most common 5' partners of ERG rearranged prostate cancer cases are given in percentages (number of rearranged cases/evaluable cases)
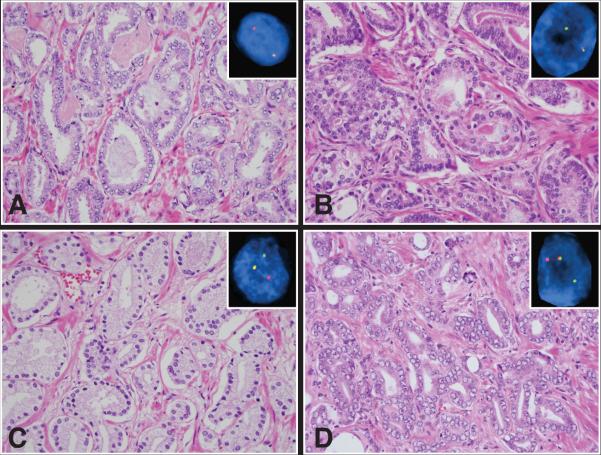
Figure 2. Representative example of four similar prostate cancer cases harboring gene rearrangement.
ERG rearrangement through deletion (a) TMPRSS2 rearrangement through deletion (b) SCL45A3 rearrangement (c) and NDRG1 rearrangement (d) (H&E images are taken at 40x objective magnification and FISH images are taken at 60x objective magnification).
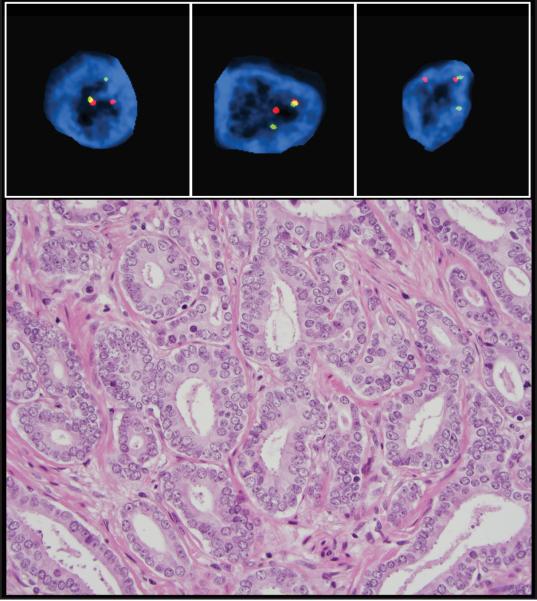
Seven of these 27 cases harbored simultaneous TMPRSS2 and SLC45A3 rearrangements within the same tissue microarray core. We evaluated by FISH the original standard tissue block in four of these seven cases. We could confirm that one of them harbored ERG rearrangement and coexisting rearrangement of TMPRSS2 and SLC45A3 in the same tumor glands (Figure 3). The three remaining cases harbored a mixture of tumor glands with both normal and rearrangement pattern.
Figure 3. Representative example of a case with simultaneous rearrangements of two 5' fusion partners. Prostatic tissue with prostatic adenocarcinoma (Gleason 3+3=6) and FISH images.
Within the same gland almost all cells harbor ERG rearrangement (translocation trough insertion) (a) and both 5' gene rearrangements, TMPRSS2 (b) and SLC45A3 (c). (H&E images are taken at 40x objective magnification and FISH images are taken at 60x objective magnification)
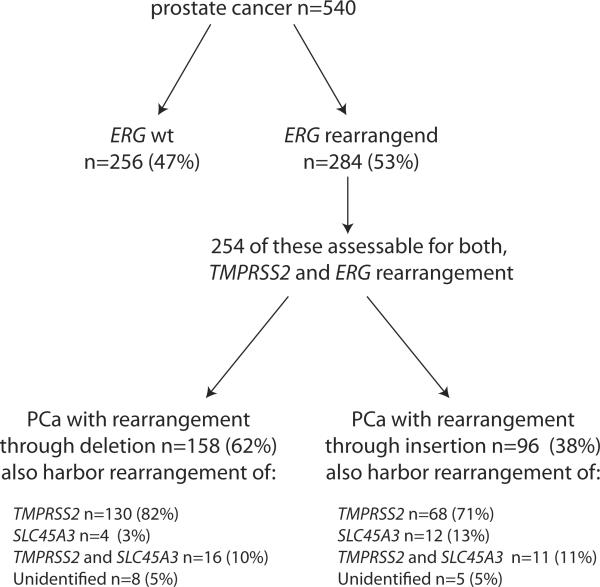
ERG with rearrangement through deletion mechanism was seen in 62% (158/254) of the ERG rearranged cases. TMPRSS2 was the fusion partner in 82% (130/158) and SLC45A3 in around 3% (4/158) of these cases, and both 5' fusion partners were simultaneous rearranged in 10% (16/158) of these ERG rearranged cases. ERG rearrangement through insertion was detected in 38% (96/254) of cases, with TMPRSS2 as 5' fusion partner in 71% (68/96), and SLC45A3 as 5' fusion partner in 12% of cases (12/96) (Figure 4). Simultaneous TMPRSS2 and SLC45A3 gene rearrangement were identified in 11% of cases (11/96) (Figure 4).
Figure 4. Schematic of ERG rearrangement.
In the 13/254 (5%) ERG rearranged cases without a TMPRSS2 or SLC45A3 rearrangement, we next sought for NDRG1 rearrangement. We could assess NDRG1 in 10 of these 13 cases and one case demonstrated NDRG1 rearrangement. The 5' partner of the remaining ERG rearranged cases could not accounted for by the three 5' partners. None of the normal prostatic tissue harbored a rearrangement of ERG, TMPRSS2, SLC45A3 or NDRG1.
Statistical analysis revealed no significant association between any of the assessed gene rearrangements and clinical features such as Gleason grade, stage, or PSA recurrence-free survival (Table 1).
DISCUSSION
Most studies to date are using a FISH break apart assay to determine TMPRSS2-ERG fusion status. Therefore, the prevalence of ERG rearrangement is well characterized at approximately 40–60% of PSA screened prostate cancer cases. This study confirms that in the vast majority of cases, ERG rearrangement is due to TMPRSS2-ERG gene fusion either through deletion or insertion. As suggested in a recently published study of 101 prostate cancer cases (20) and now demonstrated in a significantly larger population of 540 prostate cancer cases, SLC45A3-ERG and NDRG1-ERG fusion account for around 10% of the ERG rearranged tumors. It is yet to be determined if there are any significant implications to these other less common gene fusions. As suggested by Pflueger et al (20), TMPRSS2, SLC45A3, and NDRG1 are all exquisitely driven by both Androgen and Estrogen. A potential difference is that NDRG1-ERG fusions do encode for a chimeric protein product (20), whereas TMPRSS2-ERG and SLC45A3-ERG fusions encode for a truncated ERG protein. To date no study has addressed the clinical implications of this observation but given that expression profiling of ERG and non-ERG rearranged prostate cancer samples (n=455) did not reveal any clear subclasses within the ERG rearranged category(13), we can speculate that ERG over expression is the main alteration associated with the molecular phenotype. From a practical perspective, the current study suggests that performing the ERG and TMPRSS2 rearrangement assays should help classify around 90% of the ERG rearranged prostate cancer cases.
The current study focused only on ERG rearrangement prostate cancer and did not explore for the frequency of other known ETS rearrangements. Mehra et al systematically interrogated all 27 other ETS rearrangements in a cohort of 96 prostate cancer cases and found that after ERG, ETV1 was the most commonly rearranged prostate cancer suggesting that TMPRSS2-ETV1 fusion may in around 2% of prostate cancer cases (23). Attard et al. examining a cohort of 429 prostate cancer cases found that ETV1 was rearranged in slightly over 5% of the cases (24). The Attard study also identified other novel 5' fusion partners besides TMPRSS2 for ETV1. In a recent unpublished study exploring ETV1, ETV4, and ETV5 rearrangements in 88 prostate cancer cases, we identified similar rearrangement frequencies (Svensson et al, unpublished data). Therefore, ERG and ETV1 appear to be rearranged in around 40–60% and 2–5% of PSA screened prostate cancer cases, respectively. Other ETS genes such as ETV4 and ETV5 may have rearrangement frequencies at or below 1–2%. There appears to be a wider range of recurrent 5' partners besides the originally described TMPRSS2 (1) including SLC45A3 and NDRG1. Only large systematic studies will be able to define any clinical significance to the less common rearrangements.
Consistent with some of the initial descriptions of ERG rearranged prostate cancer cases assessed by FISH (1, 18, 25), we found approximately 53% of cases harbored an ERG rearrangement with 62% of these being rearranged through deletion and 38% being rearranged through insertion. To date there is no known clinical implication associated with these two types of ERG rearrangements. However, we did initially speculate that the region between TMPRSS2 and ERG on chromosome 21 does harbor candidate tumor suppressor genes that might be lost in ERG rearrangements through deletion(18).
This is the first study to systematically evaluate for the SLC45A3-ERG rearrangement in a large population. Han et al first described this fusion (19) and the recurrent nature was confirmed more recently by Pflueger et al. (20). By systematically interrogating 540 prostate cancers, we observe a 6% frequency of SLC45A3-ERG fusion prostate cancer. As this study has shown and future studies are sure to observe, that there is more complexity to ETS rearrangements than initially appreciated. Specifically, in our current study around 11% of the individuals harboring ERG rearranged, showed coexisting rearrangement of two 5' fusion partners (i.e., TMPRSS2 and SLC45A3) and seven of them in the same tissue microarray core. This would suggest different possible gene fusion combinations (TMPRSS2-ERG, SLC45A3-ERG and/or other potentially not yet identified fusions). We were able to evaluate four of these seven specific cases harboring multiple rearrangements on the original tissue block and could confirm that one of them harbored ERG rearrangement and both 5' partners TMPRSS2 and SLC45A3 rearrangements in the same tumor glands. One important limitation of our study is that we did not have fresh frozen material from these cases to perform assays that would allow us to characterize the nature of these fusions or explore for novel 5' fusion partners.
The present study has potential clinical implications for the development of cancer specific diagnostic assays. Pioneering work in prostate cancer biomarker development demonstrated that the PCA3 transcript could be used as a prostate cancer diagnostic test in the urine of men at risk of prostate cancer (26–30). This assay is now being offered for clinical use at several national commertial laboratories. Extending this type of assay, several studies have explored using the TMPRSS2-ERG fusion transcript as a prostate cancer specific urine biomarker either alone or in combination with other assays (31–33). The presence of TMPRSS2-ERG fusion transcripts is highly specific for prostate cancer when detected (31, 32, 34). However, the sensitivity approaches the theoretical limitations of 40–50% reflecting the prevalence of TMRPSS2-ERG fusions in the prostate cancer population. The current study suggests that this sensitivity might be improved by incorporating other common recurrent gene fusions such as SLC45A3-ERG, TMPRSS2-ETV1, SLC45A3-ETV1, and NDRG1-ERG. As the next generations of these assays are developed, perhaps incorporations of all known gene fusions would be feasable.
Our study of 540 men with clinically localized prostate cancer did not observe any clinical associations between ETS rearrangement status and pathology or clinical parameters. There is considerable controversy and confusion regarding the clinical implications of ETS rearangement prostate cancer (See Tomlins et al. for a review on this subject (4)). Associations with cancer specific death and ERG rearrangment prostate cancer were described in two Watchful Waiting cohorts (15, 16). These studies are particular because patients were diagnosed and then followed with prostate cancer without undergoing initial definitive treatment. These studies therefore might represent the natural clinical course of ETS rearrangement prostate cancer. A number of other studies has explored for associations for between PSA biochemical recurrence and ETS rearrangement and have failed to demonstrate any consistent findings (See Tomlins et al. for a review on this subject(4). We posit that these studies can not be used as evidence that ETS rearrangement prostate cancers do not have a more or less aggressive natural history as the course of the tumor progression was interrupted by clinical intervention. In addition, PSA biochemical recurrence has not been demonstrated to be an accurate predictor of cancer cancer specific death (35). Some have suggested that the frequency of ETS rearrangement prostate cancer cases (40–60%) is too high to represent an aggressive sub-population. This is an imporant observation given the relative low mortality rate of prostate cancer. More recent work by Carver et al. (10) and King et al. (9), using animal models suggests that ERG over expression alone is insufficient for disease progression and the concurrent PTEN loss or alteration of the PI3/AKT/PTEN pathway is required. These studies would suggest that ETS rearragements and other molecular concurrent events may best describe an aggressive clinical cancer. Numerous studies are underway to explore this hypothesis.
In summary, we were able to confirm in a large cohort that around 80% of prostate cancer cases with ERG rearrangement have TMPRSS2-ERG gene fusions. We also demonstrate the recurrent nature of SLC45A3-ERG and NDRG1-ERG fusions in approximately 7% of ERG rearranged cases. Interestingly in 11% of the cases, we observed prostate cancer cases where individuals harbored more than one type of ERG rearrangement and rarely where two ERG fusions appear to occur in the same tumor focus. For the remaining ERG rearranged cases we could not confirm the 5' partner. This study has important clinical implications for the development of diagnostic assays to detect ETS rearrangement prostate cancer. Incorporation of these less common ERG rearrangement prostate cancer fusion assays could further increase the sensitivity of these PCR-based approaches.
ACKNOWLEDGEMENTS
This study was supported by NCI grant CA125612 (SP and MAR), by the German Research Foundation grant (Deutsche Forschungsgemeinschaft, DFG, Emmy-Noether Programme, PE1179/2-1) and the University Hospital of Tuebingen (Fortuene Programme, No. 1809-1-0) to S.P. and by a grant of the Spanish Government (“Rio Hortega” Expte No. CMO8/0006) from both the Instituto de Salud Carlos III and the Institut Municipal d'Investigacio Medica of Barcelona to R.E.
Footnotes
DISCLOSURE/CONFLICT OF INTEREST S. Perner and M. A. Rubin are listed as co-inventors on a patent filed by The University of Michigan and The Brigham and Women's Hospital covering the diagnostic and therapeutic fields for ETS fusions in prostate cancer. The diagnostic field has been licensed to Gen-Probe, Inc. Gen-Probe has not played a role in the design and conduct of the study, in the collection, analysis or interpretation of the data, or in the preparation, review, or approval of the article. The authors mentioned disclose any financial interest.
REFERENCES
- 1.Tomlins SA, Rhodes DR, Perner S, et al. Recurrent fusion of TMPRSS2 and ETS transcription factor genes in prostate cancer. Science. 2005;310:644–648. doi: 10.1126/science.1117679. [DOI] [PubMed] [Google Scholar]
- 2.Kumar-Sinha C, Tomlins SA, Chinnaiyan AM. Recurrent gene fusions in prostate cancer. Nat Rev Cancer. 2008 doi: 10.1038/nrc2402. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Tomlins SA, Laxman B, Dhanasekaran SM, et al. Distinct classes of chromosomal rearrangements create oncogenic ETS gene fusions in prostate cancer. Nature. 2007;448:595–599. doi: 10.1038/nature06024. [DOI] [PubMed] [Google Scholar]
- 4.Tomlins SA, Bjartell A, Chinnaiyan AM, et al. ETS Gene Fusions in Prostate Cancer: From Discovery to Daily Clinical Practice. Eur Urol. 2009 doi: 10.1016/j.eururo.2009.04.036. [DOI] [PubMed] [Google Scholar]
- 5.Clark JP, Cooper CS. ETS gene fusions in prostate cancer. Nat Rev Urol. 2009;6:429–439. doi: 10.1038/nrurol.2009.127. [DOI] [PubMed] [Google Scholar]
- 6.Mosquera JM, Mehra R, Regan MM, et al. Prevalence of TMPRSS2-ERG Fusion Prostate Cancer among Men Undergoing Prostate Biopsy in the United States. Clin Cancer Res. 2009 doi: 10.1158/1078-0432.CCR-08-2927. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Tomlins SA, Laxman B, Varambally S, et al. Role of the TMPRSS2-ERG gene fusion in prostate cancer. Neoplasia. 2008;10:177–188. doi: 10.1593/neo.07822. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Klezovitch O, Risk M, Coleman I, et al. A causal role for ERG in neoplastic transformation of prostate epithelium. Proc Natl Acad Sci U S A. 2008;105:2105–2110. doi: 10.1073/pnas.0711711105. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.King JC, Xu J, Wongvipat J, et al. Cooperativity of TMPRSS2-ERG with PI3-kinase pathway activation in prostate oncogenesis. Nat Genet. 2009;41:524–526. doi: 10.1038/ng.371. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Carver BS, Tran J, Gopalan A, et al. Aberrant ERG expression cooperates with loss of PTEN to promote cancer progression in the prostate. Nat Genet. 2009;41:619–624. doi: 10.1038/ng.370. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Mosquera JM, Perner S, Demichelis F, et al. Morphological features of TMPRSS2-ERG gene fusion prostate cancer. J Pathol. 2007;212:91–101. doi: 10.1002/path.2154. [DOI] [PubMed] [Google Scholar]
- 12.Jhavar S, Brewer D, Edwards S, et al. Integration of ERG gene mapping and gene-expression profiling identifies distinct categories of human prostate cancer. BJU Int. 2009;103:1256–1269. doi: 10.1111/j.1464-410X.2008.08200.x. [DOI] [PubMed] [Google Scholar]
- 13.Setlur SR, Mertz KD, Hoshida Y, et al. Estrogen-dependent signaling in a molecularly distinct subclass of aggressive prostate cancer. J Natl Cancer Inst. 2008;100:815–825. doi: 10.1093/jnci/djn150. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Demichelis F, Setlur SR, Beroukhim R, et al. Distinct genomic aberrations associated with ERG rearranged prostate cancer. Genes Chromosomes Cancer. 2009;48:366–380. doi: 10.1002/gcc.20647. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Attard G, Clark J, Ambroisine L, et al. Duplication of the fusion of TMPRSS2 to ERG sequences identifies fatal human prostate cancer. Oncogene. 2008;27:253–263. doi: 10.1038/sj.onc.1210640. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Demichelis F, Fall K, Perner S, et al. TMPRSS2:ERG gene fusion associated with lethal prostate cancer in a watchful waiting cohort. Oncogene. 2007;26:4596–4599. doi: 10.1038/sj.onc.1210237. [DOI] [PubMed] [Google Scholar]
- 17.Attard G, Swennenhuis JF, Olmos D, et al. Characterization of ERG, AR and PTEN gene status in circulating tumor cells from patients with castration-resistant prostate cancer. Cancer Res. 2009;69:2912–2918. doi: 10.1158/0008-5472.CAN-08-3667. [DOI] [PubMed] [Google Scholar]
- 18.Perner S, Demichelis F, Beroukhim R, et al. TMPRSS2:ERG Fusion-Associated Deletions Provide Insight into the Heterogeneity of Prostate Cancer. Cancer Res. 2006;66:8337–8341. doi: 10.1158/0008-5472.CAN-06-1482. [DOI] [PubMed] [Google Scholar]
- 19.Han B, Mehra R, Dhanasekaran SM, et al. A fluorescence in situ hybridization screen for E26 transformation-specific aberrations: identification of DDX5-ETV4 fusion protein in prostate cancer. Cancer Res. 2008;68:7629–7637. doi: 10.1158/0008-5472.CAN-08-2014. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Pflueger D, Rickman DS, Sboner A, et al. N-myc downstream regulated gene 1 (NDRG1) is fused to ERG in prostate cancer. Neoplasia. 2009;11:804–811. doi: 10.1593/neo.09572. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Kristiansen G, Fritzsche FR, Wassermann K, et al. GOLPH2 protein expression as a novel tissue biomarker for prostate cancer: implications for tissue-based diagnostics. Br J Cancer. 2008;99:939–948. doi: 10.1038/sj.bjc.6604614. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Perner S, Mosquera JM, Demichelis F, et al. TMPRSS2-ERG fusion prostate cancer: an early molecular event associated with invasion. Am J Surg Pathol. 2007;31:882–888. doi: 10.1097/01.pas.0000213424.38503.aa. [DOI] [PubMed] [Google Scholar]
- 23.Mehra R, Tomlins SA, Shen R, et al. Comprehensive assessment of TMPRSS2 and ETS family gene aberrations in clinically localized prostate cancer. Mod Pathol. 2007;20:538–544. doi: 10.1038/modpathol.3800769. [DOI] [PubMed] [Google Scholar]
- 24.Attard G, Clark J, Ambroisine L, et al. Heterogeneity and clinical significance of ETV1 translocations in human prostate cancer. Br J Cancer. 2008;99:314–320. doi: 10.1038/sj.bjc.6604472. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Barry M, Perner S, Demichelis F, Rubin MA. TMPRSS2-ERG fusion heterogeneity in multifocal prostate cancer: clinical and biologic implications. Urology. 2007;70:630–633. doi: 10.1016/j.urology.2007.08.032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Bussemakers MJ, van Bokhoven A, Verhaegh GW, et al. DD3: a new prostate-specific gene, highly overexpressed in prostate cancer. Cancer Res. 1999;59:5975–5979. [PubMed] [Google Scholar]
- 27.de Kok JB, Verhaegh GW, Roelofs RW, et al. DD3(PCA3), a very sensitive and specific marker to detect prostate tumors. Cancer Res. 2002;62:2695–2698. [PubMed] [Google Scholar]
- 28.Hessels D, Klein Gunnewiek JM, van Oort I, et al. DD3(PCA3)-based molecular urine analysis for the diagnosis of prostate cancer. Eur Urol. 2003;44:8–15. doi: 10.1016/s0302-2838(03)00201-x. discussion 15–16. [DOI] [PubMed] [Google Scholar]
- 29.Schalken JA, Hessels D, Verhaegh G. New targets for therapy in prostate cancer: differential display code 3 (DD3(PCA3)), a highly prostate cancer-specific gene. Urology. 2003;62:34–43. doi: 10.1016/s0090-4295(03)00759-3. [DOI] [PubMed] [Google Scholar]
- 30.Groskopf J, Aubin SM, Deras IL, et al. APTIMA PCA3 molecular urine test: development of a method to aid in the diagnosis of prostate cancer. Clin Chem. 2006;52:1089–1095. doi: 10.1373/clinchem.2005.063289. [DOI] [PubMed] [Google Scholar]
- 31.Laxman B, Tomlins SA, Mehra R, et al. Noninvasive detection of TMPRSS2:ERG fusion transcripts in the urine of men with prostate cancer. Neoplasia. 2006;8:885–888. doi: 10.1593/neo.06625. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Laxman B, Morris DS, Yu J, et al. A first-generation multiplex biomarker analysis of urine for the early detection of prostate cancer. Cancer Res. 2008;68:645–649. doi: 10.1158/0008-5472.CAN-07-3224. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Rostad K, Hellwinkel OJ, Haukaas SA, et al. TMPRSS2:ERG fusion transcripts in urine from prostate cancer patients correlate with a less favorable prognosis. APMIS. 2009;117:575–582. doi: 10.1111/j.1600-0463.2009.02517.x. [DOI] [PubMed] [Google Scholar]
- 34.Hessels D, Smit FP, Verhaegh GW, et al. Detection of TMPRSS2-ERG fusion transcripts and prostate cancer antigen 3 in urinary sediments may improve diagnosis of prostate cancer. Clin Cancer Res. 2007;13:5103–5108. doi: 10.1158/1078-0432.CCR-07-0700. [DOI] [PubMed] [Google Scholar]
- 35.Porter CR, Kodama K, Gibbons RP, et al. 25-year prostate cancer control and survival outcomes: a 40-year radical prostatectomy single institution series. J Urol. 2006;176:569–574. doi: 10.1016/j.juro.2006.03.094. [DOI] [PubMed] [Google Scholar]