Abstract
Background
In spite of recent advances in post-operative pain relief, pain following orthopedic surgery remains an ongoing challenge for clinicians. We examined whether a well known and frequently prescribed homeopathic preparation could mitigate post-operative pain.
Method
We performed a randomized, double blind, placebo-controlled trial to evaluate the efficacy of the homeopathic preparation Traumeel S® in minimizing post-operative pain and analgesic consumption following surgical correction of hallux valgus. Eighty consecutive patients were randomized to receive either Traumeel tablets or an indistinguishable placebo, and took primary and rescue oral analgesics as needed. Maximum numerical pain scores at rest and consumption of oral analgesics were recorded on day of surgery and for 13 days following surgery.
Results
Traumeel was not found superior to placebo in minimizing pain or analgesic consumption over the 14 days of the trial, however a transient reduction in the daily maximum post-operative pain score favoring the Traumeel arm was observed on the day of surgery, a finding supported by a treatment-time interaction test (p = 0.04).
Conclusions
Traumeel was not superior to placebo in minimizing pain or analgesic consumption over the 14 days of the trial. A transient reduction in the daily maximum post-operative pain score on the day of surgery is of questionable clinical importance.
Trial Registration
This study was registered at ClinicalTrials.gov. # NCT00279513
Background
The management of postoperative pain following ambulatory orthopedic surgery is an issue of ongoing concern for patients and for physicians performing these procedures. Numerous studies have found pain control to be inadequate [1-6]. Pain is the most frequent cause of delayed discharge and unanticipated readmission following ambulatory surgery [7,8], as well as for contacting the family physician after discharge [9]. Nearly a third of patients have moderate to severe pain 24 hours after ambulatory surgery [10], while eleven percent experience severe pain [11]. Both moderate and severe pain can last for up to a week after surgery [9]. Treatment for post-operative pain typically includes anti-inflammatory medications and opiates, both of which are associated with adverse effects, limiting patient compliance and effectiveness.
Traumeel S® is an over-the-counter homeopathic preparation composed of extracts from a combination of plants and minerals that have been highly-diluted, though not beyond Avogadro's number (see Table 1). It has been widely sold in German, Switzerland and Austria for over 50 years, and is one of the most popular alternative medications in these countries, selling approximately four million doses a year [manufacturer information]. Earlier studies have suggested that Traumeel may be effective in trauma [12-15], acute tendinopathy [16] and in the spinal syndrome [17], though these studies were either non-randomized or used poorly chosen controls. A small RCT found Traumeel to be effective in post-chemotherapy stomatitis [18]. While the mechanism of action of this preparation remains unknown, recent research has shown that Traumeel reduces secretion of pro-inflammatory cytokines from various human immune cells in vitro, both at rest and when activated by PHA-, PMA-, or TNF-α. Interleukin-1β secretion was reduced by 70%, TNF-α by 65% and 54% (resting and activated), and IL-8 by 50% (P < 0.01 for all comparisons) [19].
Table 1.
Composition of the homeopathic-complex Traumeel S®.
| Component | Homeopathic dilution | Quantity per tablet |
|---|---|---|
| Arnica Montana | D2 | 150 μg |
| Calendula officinalis | D2 | 150 μg |
| Atropa belladonna | D4 | 7.5 μg |
| Aconitum napellus | D3 | 30 μg |
| Bellis perennis | D2 | 60 μg |
| Hypericum perforatum | D2 | 30 μg |
| Echinacea angustifolia | D2 | 60 μg |
| Echinacea purpurea | D2 | 60 μg |
| Hepar sulfuris | D8 | 300 pg |
| Symphytum officinale | D8 | 240 pg |
| Matricaria Chamomilla | D3 | 24 μg |
| Achillea millefolium | D3 | 15 μg |
| Mercurius solubilis Hahnemanni | D8 | 300 pg |
μg = microgram (1/1,000,000 g), pg = picogram (1/1,000,000,000 g)
Unpublished data from a manufacturer safety survey indicated adverse events in 0.0035% of 3.5 million cases [personal communication]. These appeared almost entirely in cases where Traumeel was injected, with the most common of these events being local irritation at the site of injection that resolved spontaneously after discontinuation of treatment. No drug interactions are known with this preparation [manufacturer information].
In 2007 we published the results of an open pilot study to evaluate the efficacy of Traumeel in mitigating post-operative pain following ambulatory hallus valgus surgery [20]. In this study, treatment allocation was by week of surgery rather than by strict randomization. This study found significantly lower post-operative pain scores in patients treated with supplementary Traumeel as compared with standard care alone. To the best of our knowledge, no randomized controlled trial has yet assessed the effectiveness of Traumeel for the relief of acute pain in patients following ambulatory surgery. We therefore performed a randomized, double-blind, placebo-controlled clinical trial to evaluate the efficacy of Traumeel in controlling post-operative pain after ambulatory hallus valgus correction.
Methods
Study design
The study was designed, conducted, and reported according to the Consolidated Standards of Reporting Trials (CONSORT) guidelines [21], and approved by the ethics committees of the Shaare Zedek Medical Center (SZMC) and the Meir Medical Centers (MMC). All patients scheduled for ambulatory hallus valgus surgery at the Shaare Zedek Medical Center department of orthopedics between 12 September 2006 and 19 November 2007, and at Meir Medical Center between 1 August 2007 and 19 November 2007 were screened for inclusion in the trial. The exclusion criteria were as follows: age under 18 years, bilateral surgery, previous hallus valgus surgery on the ipsilateral foot, diseases possibly effecting wound healing or pain sensation (uncontrolled diabetes mellitus, Berger's disease, deep vein thrombosis, peripheral vascular disease), sensitivity to any of the study medications and technical or cognitive inability to comply with the study protocol. Eighty consecutive patients who fulfilled all inclusion and no exclusion criteria and who signed informed consent were enrolled in the trial.
Study design was randomized and double-blind. Randomization blocks of four subjects were created, and then selected using random number sequence. The HEEL Company (Baden-Baden, Germany) prepared and supplied the study medication or an indistinguishable placebo in 100 consecutively numbered, sealed boxes, according to the randomization list. Sealed copies of the randomization list were held by the manufacturer and a hospital physician not otherwise involved in the trial. These were to be opened only in the event of a medical emergency necessitating knowledge of the treatment allocation of a given patient. Otherwise, patient and all study personnel remained unaware of treatment allocation until the trail was completed and the database sealed, at which point the allocation envelopes were to be opened and the randomization code unveiled. Each eligible patient was assigned the lowest numbered box available. Surgery was performed as orthopedically indicated, with all patients anesthetized using an ankle block of 20 cc Lidocaine 1% and Marcaine 0.5%. Upon completion of surgery, patients were instructed to take two tablets of the study medication five times daily for the first three days, and three times daily afterwards. The composition of Traumeel tablets is displayed in Table 1. Patients also received tablets of paracetamol 325 mg with codeine 15 mg (Cod-Acamol Forte, Teva Pharmaceutical Industries, Israel) as primary analgesic, to be taken in a two-tablet dose up to six times daily, as needed. Patients additionally received a prescription for Tramadol tablets 100 mg (Tramadex, Dexcel Pharma, Israel) as rescue analgesic to be taken as needed, up to a maximum of four tablets a day. The choice of a primary analgesic including a mild opiate was based upon the necessity for standardized primary analgesia while offering patients adequate pain relief over the course of the trial. Previous experience had indicated that non-opiate analgesics were insufficient for this purpose. Patients were instructed to record maximal daily pain scores at rest using a self-administered, horizontal 11-point numerical rating score (NRS-11), graded from 0 (no pain) to 10 (worst imaginable pain). Patients were further requested to record in the patient diary the number of primary and rescue analgesic tablets taken, and the maximum level of pain at rest they had experienced during that day.
Patients were contacted by telephone every evening by a study nurse, who recorded the reported NSR and analgesic consumption values in the case report form. The nurse also encouraged study compliance. Patients were instructed to withhold study medication if the NRS score was three or less and no other analgesics had been consumed for two consecutive days. Patients were examined by a surgeon on days 6 and 13 days after surgery, and any adverse events, related or unrelated to treatment, were registered. On post-operative day 13, all study materials were collected from the patient.
Efficacy measures
The primary outcome measure was maximum daily pain at rest, as measured by a horizontal, 11-point numerical rating scale (NRS-11) filled out on the day of surgery (day 0) and for 13 post-operative days. Secondary outcomes were total consumption of primary analgesics and number of days requiring rescue analgesics. Adverse events were monitored throughout the study.
Statistical analysis
Statistical analysis was performed following the intention-to-treat principle. To compare the post-operative pain between the study groups, the area-under-the-curve (AUC) of the NRS pain scores recorded daily over the 2 weeks post-operative was used. We chose the AUC for both clinical and statistical reasons. Clinically, it summarizes the strength of pain and the number of days the patient experienced pain. Statistically, it is a summary measure which allows one to deal with repeated measurements with no need to adjust for the type 1 error rate. For each patient, an AUC was obtained by graphing the NRS pain scores recorded every day during follow-up, linking time-adjacent points by a straight line and calculating the area under the resulting polygon. When all 14 pain scores are available, this is equivalent to the sum of the 14 scores. Linear interpolation was performed to estimate the NRS score on those days that were missing. The mean AUCs were compared between study groups using the Mann-Whitney test. The repeated measures mixed model was used to test for an interaction between time and treatment allocation. Mann-Whitney tests were used to compare the total amount of primary analgesics consumed and the total number of days taking rescue analgesics. Post-hoc subgroup analysis was performed to assess the influence of type of surgery on post-operative pain scores. Surgical procedures were characterized as 'Chevron only', 'Additional osteotomy', or 'Triple or proximal osteotomy', and Mann-Whitney tests were performed in each subgroup to compare the area-under-the-curve of the NRS pain scores between treatment arms. Frequency of the main adverse events was compared using Fisher's exact test. Sample size was calculated using a conservative interpretation of the data obtained in our previous pilot study [20], a type I error of 0.05, a power of 90% and a 15% loss to follow-up.
Results
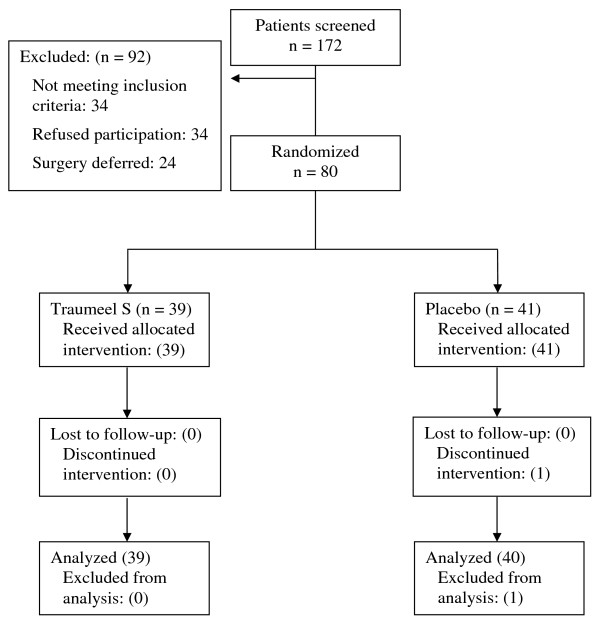
Patient flow throughout the study is presented in Figure 1. Of the 80 patients who participated in the trial, 79 were evaluable for intention-to-treat analysis. The remaining patient withdrew consent on the third day of the trial because of nausea, vomiting and abdominal pain. He did not provide sufficient data points to be included in the final analysis. Patient groups were balanced with respect to all baseline parameters except for laterality of surgery (Table 2).
Figure 1.
Flow chart of patients through study. 172 patients were screened for participation in the trial. Of 80 patients randomized, one discontinued treatment and was excluded from analysis.
Table 2.
Baseline demographic and clinical variables of the Traumeel S® and placebo treatment groups.
| Traumeel S® (n = 39) |
Placebo (n = 40) |
|
|---|---|---|
| Clinical Center: | ||
| SZMC* | 33 | 34 |
| MMC** | 6 | 6 |
| Age (y) | ||
| Mean (SD) | 48.1 (16.7) | 45.2 (18.7) |
| < 50 | 17 | 19 |
| ≥ 50 | 22 | 21 |
| Sex (%) | ||
| M | 8 (20.5) | 8 (20.0) |
| F | 31 (79.5) | 32 (80.0) |
| Ethnicity/Origin (%) | ||
| Europe/America | 12 (30.8) | 9 (22.5) |
| Asia/Africa | 21 (53.9) | 25 (62.5) |
| Israeli Arab | 2 (5.1) | 0 |
| Mixed | 2 (5.1) | 2 (5.0) |
| Other | 2 (5.1) | 4 (10.0) |
| BMI | ||
| Mean (SD) | 24.7 (4.1)† | 24.3 (4.0)† |
| < 24 | 20 | 23 |
| ≥ 24 | 18 | 16 |
| Pain before surgery | ||
| Mean (SD) | 5.4 (2.8) | 5.7 (2.6)† |
| < 6 | 19 | 18 |
| ≥ 6 | 20 | 21 |
| Laterality (%) | ||
| Right | 21 (53.9) | 14 (35.9)† |
| Left | 16 (41.0) | 24 (61.5) |
| Bilateral# | 2 (5.1) | 1 (2.6) |
| Type of surgery (%) | ||
| Chevron - only | 9† (23.0) | 10†† (26.3) |
| Additional | 17 (43.5) | 18 (47.3) |
| osteotomy | ||
| Triple or | 13 (33.3) | 10 (26.3) |
| proximal | ||
| osteotomy | ||
* SZMC -- Shaare Zedek Medical Center
**MMC -- Meir Medical Center
#3 patients had a bilateral hallux valgus but underwent surgery on only one foot.
† - includes 1 patient with missing data.
††-includes 2 patients with missing data.
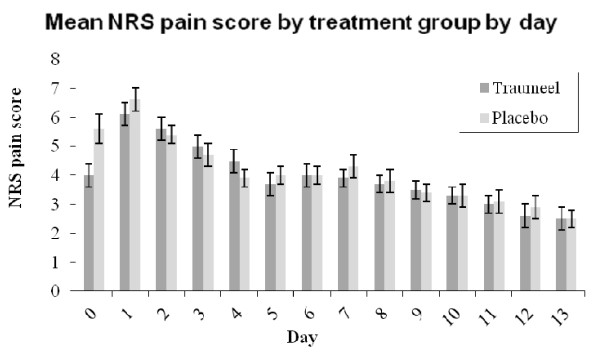
Overall, the mean area-under-the-curve pain scores during the 14 days of the trial were not significantly different between the groups (55.4 ± 25.5 in Traumeel group vs. 57.4 ± 25.7 for placebo, p = 0.89). However, the mean pain score on the day of surgery appeared lower in the Traumeel group than placebo (4.0 vs. 5.6, Figure 2). This difference is supported by the test for interaction between time and treatment group (p = 0.04).
Figure 2.
Mean pain score over the 14 days of the trial. Mean NRS pain scores over 14 days for 79 patients receiving Traumeel S® or Placebo. The error bars indicate the mean plus or minus 1 standard error.
When stratified for type of surgery, in the Chevron-only strata the mean pain score appeared lower in the Traumeel group than in the placebo group, however this difference was not found statistically significant (Traumeel - 46.1, Placebo - 61.8, p = 0.35). In the 'Additional osteotomy' and ' Triple or proximal osteotomy' groups, differences in mean pain between the verum and placebo groups were negligible (Table 3).
Table 3.
Pain score stratified for type of surgery.
| Chevron-only | Additional osteotomy | Triple or proximal osteotomy | ||||
|---|---|---|---|---|---|---|
| AUC | Traumeel (n = 9) | Placebo (n = 10) | Traumeel (n = 17) | Placebo (n = 18) | Traumeel (n = 13) | Placebo (n = 10) |
| Mean | 46.1 | 61.8 | 63.1 | 59.5 | 51.6 | 49.2 |
| SD | 23.4 | 34.1 | 25.6 | 55.5 | 49.0 | 49.0 |
| p-value | 0.35 | 0.69 | 0.88 | |||
AUC -- Area Under the Curve
There was little difference between the two arms in the total number of tablets of primary analgesics consumed (15.6 ± 12.2 for Traumeel vs. 16.0 ± 11.9 for placebo, p = 0.74) and in the number of days on which rescue analgesics were required (mean ± SD: 1.0 ± 3.1 for Traumeel and 1.5 ± 2.0 for Placebo, p = 0.99).
Four patients in the placebo group (10%) and two in the Traumeel group (5.1%) developed wound infection. Six patients in the Traumeel group (15%) and four patients in the placebo group (10%) developed nausea and/or vomiting, though these differences were not statistically significant (p = 0.51 and p = 0.68 respectively). In the Traumeel group, one 82-year-old patient with type II diabetes developed cellulitis following wound infection. He was hospitalized for intravenous antibiotic treatment, but did not require further surgery. This was deemed a serious adverse event unrelated to the study medication.
Discussion
Traumeel was not superior to placebo in minimizing pain or analgesic consumption over the 14 days of the trial, however a transient reduction in the daily maximum post-operative pain score was observed on the day of surgery. Our statistical design did not allow for a significance test specific to that day, however a test for interaction was significant. Stratification by type of surgery did not alter these results. Because post-operative pain is maximal in the period immediately following surgery, this finding may be of clinical importance. Wound infection was more prevalent in the placebo group, but the difference was not statistically significant. Other adverse effects were too rare to analyze statistically.
Our findings do not support those of a pilot study published in 2007 that suggested a 30% improvement in pain over 14 post-operative days, and a non-significant trend towards lower analgesic consumption. In that non-blinded study, 30 subjects were allocated by week of surgery to intraoperative injection of Traumeel, injection plus oral Traumeel, or no treatment. Both treatment arms were found superior to no treatment [20]. Differences in study methodology could explain the differences in outcome. We believe that future research should focus on the early post-operative period.
Homeopathy is frequently attacked for its use of solutions diluted beyond Avogadro's number, and hence physical-chemical implausibility. That criticism was circumvented in this trial by employing a preparation of solutions that were dilute, but well within the material range.
Relief of post-operative pain remains an ongoing challenge. While other treatment modalities have been examined, each has its own limitations. Valdecoxib and rofecoxib have both been found effective for relief of pain following hallux valgus surgery [22,23] but were removed from the market amid concerns of excessive risk of heart attack and stroke. Betamethasone has been found to reduce post-operative pain and nausea [24], but concerns remain regarding the effect of corticosteroids on post-operative healing [25]. Parenteral routes for delivery of opiates are available, but they entail greater cost, complexity, and possible need for hospitalization [26].
This trial has several limitations. By choosing a cumulative 14-day measure for our primary outcome, we may have inadvertently diluted any effect that may have been present in the first days after surgery - those with the greatest pain. Homeopathic purists may find fault in the administration of a standardized combination homeopathic formula to all patients, based upon clinical diagnosis - as opposed to the individualized manner dictated by standard homeopathic practice. We were aware of this limitation at the outset; however, performing an individualized RCT would be far more complex, time-consuming, and fraught with methodological pitfalls. The mode of administration of the remedy may have played a role as well. In contrast to our pilot study, in the current study, for the sake of simplicity we chose to use only oral administration of the study medication, under the assumption that its effect would be similar to that of injection followed by oral therapy. In retrospect, that assumption may have been mistaken.
Conclusions
The homeopathic complex Traumeel S® was not found superior to placebo in mitigating post-operative pain or analgesic consumption over the 14 days of the trial. A transient reduction in the daily maximum post-operative pain score, observed on the day of surgery, is of questionable importance. We recommend repetition of this trial, but using injected Traumeel and focusing on the early post-operative period.
Abbreviations
CONSORT: Consolidated Standards of Reporting Trials; MMC: Meir Medical Center, Kefar Saba, Israel; NRS: Numerical Rating Scale; SZMC: Shaare Zedek Medical Center, Jerusalem, Israel.
Competing interests
The HEEL Company (Baden-Baden, Germany) has funded previous research at the Shaare Zedek Center for Integrative Complementary Medicine, and provided funding for the performance and monitoring of this project, supplied the study medication and placebo, and prepared the randomization list. However, it had by contractual agreement no control over the flow of the study, the data analysis, or the decision when and where to publish the study findings. The authors have full control over the primary data, and agree to allow the journal to review the data if requested.
Authors' contributions
MO conceived the trial, and was central to its design, performance, and reporting.
SRS was PI, participated in drafting the protocol, oversaw performance of the trial and participated in drafting the manuscript. NS and OP participated in study design and drafting of protocol and manuscript. MAK, SW, JR, GM, MI and MN screened patients and performed surgery and follow-ups. EL and LF participated in design of the trial, data management and analysis. All authors have read and approved the final manuscript.
SRS and MAK are joint first authors.
Pre-publication history
The pre-publication history for this paper can be accessed here:
Contributor Information
Shepherd R Singer, Email: singer2@013.net.
Michal Amit-Kohn, Email: muak@bezeqint.net.
Samuel Weiss, Email: weisssh@zahav.net.il.
Jonathan Rosenblum, Email: jrosenb@bezeqint.net.
Guy Maoz, Email: guy.maoz@clalit.org.il.
Noah Samuels, Email: refplus@netvision.net.il.
Esther Lukasiewicz, Email: estherhagai@live.com.
Laurence Freedman, Email: lsf@actcom.co.il.
Ora Paltiel, Email: ora@vms.huji.ac.il.
Menachem Itzchaki, Email: m_itzcha@netvision.net.il.
Meir Niska, Email: nyska@internet-zahav.net.
Menachem Oberbaum, Email: oberbaum@szmc.org.il.
References
- Rawal N, Hylander J, Nydahl PA, Olofsson I, Gupta A. Survey of postoperative analgesia following ambulatory surgery. Acta Anaesthesiol Scand. 1997;41:1017–22. doi: 10.1111/j.1399-6576.1997.tb04829.x. [DOI] [PubMed] [Google Scholar]
- Beauregard L, Pomp A, Choiniere M. Severity and impact of pain after day surgery. Can J Anaesth. 1998;45:304–11. doi: 10.1007/BF03012019. [DOI] [PubMed] [Google Scholar]
- Chung F, Ritchie E, Su J. Postoperative pain in ambulatory surgery. Anesth Analg. 1997;85:808–16. doi: 10.1097/00000539-199710000-00017. [DOI] [PubMed] [Google Scholar]
- McHugh GA, Thomas GMM. The management of pain following day-case surgery. Anaesthesia. 2002;57:266–83. doi: 10.1046/j.1365-2044.2002.2366_2.x. [DOI] [PubMed] [Google Scholar]
- Rocchi A, Chung F, Forte L. Canadian survey of postsurgical pain and pain medication experiences. Can J Anaesth. 2002;49:1053–6. doi: 10.1007/BF03017901. [DOI] [PubMed] [Google Scholar]
- Huang N, Cunningham F, Laurito CE, Chen C. Can we do better with postoperative pain management? Am J Surg. 2001;182(5):440–8. doi: 10.1016/S0002-9610(01)00766-8. [DOI] [PubMed] [Google Scholar]
- Chung F. Home-readiness after ambulatory surgery. Anesth Analg. 2002;80:896–902. doi: 10.1097/00000539-199505000-00008. [DOI] [PubMed] [Google Scholar]
- Coley KC, Williams BA, DaPos SV, Chen C, Smith RB. Retrospective evaluation of unanticipated admissions and readmissions after same day surgery and associated costs. J Clin Anesth. 2002;14:349–53. doi: 10.1016/S0952-8180(02)00371-9. [DOI] [PubMed] [Google Scholar]
- Ghosh S, Sallam S. Patient satisfaction and postoperative demands on hospital and community services. Br J Surg. 1994;81:1635–8. doi: 10.1002/bjs.1800811124. [DOI] [PubMed] [Google Scholar]
- McGrath B, Elgendy H, Chung F, Kamming D, Curti B, King S. Thirty percent of patients have moderate to severe pain 24 h after ambulatory surgery: a survey of 5,703 patients. Can J Anaesth. 2004;51:886–91. doi: 10.1007/BF03018885. [DOI] [PubMed] [Google Scholar]
- Dolin SJ, Cashman JN, Bland JM. Effectiveness of acute postoperative pain management. I. Evidence from published data. Br J Anaesth. 2002;89:409–23. doi: 10.1093/bja/aef207. [DOI] [PubMed] [Google Scholar]
- Thiel W, Borho B. Die Therapie von frischen, traumatischen Blutergüssen der Kniegelenke (Hämarthros) mit Traumeel N Injektionslösung. Biol Med. 1991;20:506–15. [German] [Google Scholar]
- Bohmer D, Ambrus P. Behandlung von Sportverletzungen mit Traumeel-Salbe-Kontrollierte Doppelblindstudie. Biol Med. 1992;21:260–8. [German] [Google Scholar]
- Mergen H. Behandlung einer post mit Traumeel. Ein Beitrag zur "Dosisefekt" eines Kombinationspraeparates. Munch Med Wochenschr. 1969;111:298–300. [German] [PubMed] [Google Scholar]
- Zell J, Connert WD, Mau J, Feuerstake G. Behandlung von akuten Sprunggelenksdistorsionen. Fortschr Med. 1988;106:96–100. [German] [PubMed] [Google Scholar]
- Schneider C, Klein P, Stolt P, Oberbaum M. A homeopathic ointment preparation compared with 1% diclofenac gel for acute symptomatic treatment of tendinopathy. Explore. 2005;1(6):446–52. doi: 10.1016/j.explore.2005.08.010. [DOI] [PubMed] [Google Scholar]
- Vorstoffel E. Behandlung eines Spinalsyndromes mit paravertebrale Traumeelinfiltrationen. Munch Med Wochenschr. 1971;113:440–3. [German] [PubMed] [Google Scholar]
- Oberbaum M, Yaniv I, Ben-Gal Y, Stein J, Ben-Zvi N, Freedman LS, Branski D. A randomized, controlled clinical trial of the homeopathic medication TRAUMEEL S® in the treatment of chemotherapy-induced stomatitis in children undergoing stem cell transplantation. Cancer. 2001;92:684–90. doi: 10.1002/1097-0142(20010801)92:3<684::AID-CNCR1371>3.0.CO;2-#. [DOI] [PubMed] [Google Scholar]
- Porozov S, Cahalon L, Weiser M, Branski D, Lider O, Oberbaum M. Inhibition of IL-1beta and TNF-alpha secretion from resting and activated human immunocytes by the homeopathic medication Traumeel S®. Clin Dev Immunol. 2004;11:143–9. doi: 10.1080/10446670410001722203. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Singer SR, Amit-Kohn M, Weiss S, Rosenblum J, Lukasiewiczc E, Itzchaki M, Oberbaum M. Efficacy of a homeopathic preparation in control of post-operative pain-A pilot clinical trial. Acute Pain. 2007;9:7–12. doi: 10.1016/j.acpain.2006.11.005. [DOI] [Google Scholar]
- Moher D, Schulz KF, Altman DG. The CONSORT statement: revised recommendations for improving the quality of reports of parallel-group randomised trials. Lancet. 2001;357:1191–4. doi: 10.1016/S0140-6736(00)04337-3. [DOI] [PubMed] [Google Scholar]
- Pollak R, Raymond GA, Jay RM, Hillstrom HJ, Mahan KT, Riff D, Jacobs EL, Brown MT, Verburg KM. Analgesic efficacy of valdecoxib for acute postoperative pain after bunionectomy. J Am Podiatr Med Assoc. 2006;96(5):393–407. doi: 10.7547/0960393. [DOI] [PubMed] [Google Scholar]
- Desjardins PJ, Black PM, Daniels S, Bird SR, Fitzgerald BJ, Petruschke RA, Tershakovec A, Chang DJ. A randomized controlled study comparing rofecoxib, diclofenac sodium, and placebo in post-bunionectomy pain. Curr Med Res Opin. 2004;20(10):1523–37. doi: 10.1185/030079904X3069. [DOI] [PubMed] [Google Scholar]
- Aasboe V, Raeder JC, Groegaard B. Betamethasone reduces postoperative pain and nausea after ambulatory surgery. Anesth Analg. 1998;87(2):319–23. doi: 10.1097/00000539-199808000-00015. [DOI] [PubMed] [Google Scholar]
- Gaston MS, Simpson AHRW. Inhibition of fracture healing. J Bone Joint Surg Br. 2007;89-B:1553–1560. doi: 10.1302/0301-620X.89B12.19671. [DOI] [PubMed] [Google Scholar]
- Thipphawong JB, Babul N, Morishige RJ, Findlay HK, Reber KR, Millward GJ, Otulana BA. Analgesic efficacy of inhaled morphine in patients after bunionectomy surgery. Anesthesiology. 2003;99(3):693–700. doi: 10.1097/00000542-200309000-00026. [DOI] [PubMed] [Google Scholar]