Abstract
Background
Pulmonary tuberculosis, the most common clinical form of mycobacterial diseases, is a granulomatous disease of the lungs caused by Mycobaterium tuberculosis. A number of genes have been identified in studies of diverse origins to be important in tuberculosis. Of these, both tumor necrosis factor α (TNF-α) and lymphotoxin α (LT-α) play important immunoregulatory roles.
Methods
To investigate the association of TNF polymorphisms with tuberculosis in the Asian Indians, we genotyped five potentially functional promoter polymorphisms in the TNFA gene and a LTA_NcoI polymorphism (+252 position) of the LTA gene in a clinically well-defined cohort of North-Indian patients with tuberculosis (N = 185) and their regional controls (N = 155). Serum TNF-α (sTNF-α) levels were measured and correlated with genotypes and haplotypes.
Results
The comparison of the allele frequencies for the various loci investigated revealed no significant differences between the tuberculosis patients and controls. Also, when the patients were sub-grouped into minimal, moderately advanced and far advanced disease on the basis of chest radiographs, TST and the presence/absence of cavitary lesions, none of the polymorphisms showed a significant association with any of the patient sub-groups. Although a significant difference was observed in the serum TNF-α levels in the patients and the controls, none of the investigated polymorphisms were found to affect the sTNF-α levels. Interestingly, it was observed that patients with minimal severity were associated with lower log sTNF-α levels when compared to the patients with moderately advanced and far advanced severity. However, none of these differences were found to be statistically significant. Furthermore, when haplotypes were analyzed, no significant difference was observed.
Conclusions
Thus, our findings exclude the TNF genes as major risk factor for tuberculosis in the North Indians.
Background
Mycobacterial diseases are a major health concern, with an estimate of approximately one-third of the world's population being affected by them [1,2]. Pulmonary tuberculosis, the most common clinical form of the disease, is a granulomatous disease of the lungs caused by Mycobaterium tuberculosis. However, only 5-10% of the infected people ever develop the disease. The genetic contribution of the host plays a significant role in determining susceptibility to developing the active form of the disease, the severity of infection and the health outcome of the patient [3,4]. A number of genes have been identified in studies of diverse origins to be important in tuberculosis [5-7].
The genes for tumor necrosis factor-α (TNF-α; TNFA) and lymphotoxin-α (LT-α; LTA), located within the MHC III region of chromosome 6, shows close linkage to the HLA class I (HLA-B) and class II (HLA-DR) genes [8]. Both TNF-α, produced mainly by monocytes and activated macrophages; and LT-α, produced mainly by activated T-cells, play important immunoregulatory roles [9]. Of these, TNF-α contributes to the pathogenesis of tuberculosis due to its role in the formation and maintenance of granulomas [10]. Additionally, it also plays a major role in host defense to M. tuberculosis by its synergistic action with interferon-γ (IFN-γ) to activate macrophages and thereby impacts on disease perpetuation [11,12]. Elevated serum TNF-α (sTNF-α) levels have been reported in advanced tuberculosis patients when compared to those with mild tuberculosis and healthy individuals [13].
Studies on monozygotic twins and their first-degree relatives, using ex vivo endotoxin stimulated whole blood samples, have provided evidence that 60% of variation in the production capacity of TNF-α appears to be genetically determined [14]. Several polymorphisms within the promoter region of TNFA and the intron 1 polymorphism of LTA, in particular, have been associated with altered levels of circulating TNF-α [15,16]. A few of these polymorphisms have been also studied for determining susceptibility or resistance towards tuberculosis in several ethnic groups, the results of which have been inconclusive [17-26].
The aim of this study was to determine associations, if any, of potentially functional TNFA and LTA polymorphism(s), both individually and at the haplotype level, with tuberculosis in patients from North-India. In addition, we have attempted to explore whether any of these polymorphisms may be related to the severity and the associated features of the disease. We also attempt to correlate these polymorphisms with sTNF-α levels in the patients and the controls.
Methods
Study Subjects
185 unrelated tuberculosis patients (mean age 32.16 ± 13.8 years; male:female 0.42:0.58), who presented to the Medical Outpatient Department or were admitted at the All India Institute of Medical Sciences hospital, New Delhi, between 1996 and 2006 were recruited. The study was approved by the ethical committee of the hospital and informed consent was obtained from all participants. Patients with chronic illness such as cirrhosis of liver, chronic hepatitis, acute viral hepatitis, and/or gastrointestinal, renal, or cardiac diseases and those who were tested positive for HIV using ELISA were excluded during the preliminary evaluations.
Pulmonary tuberculosis
There were 149 patients in this group (Table 1). The diagnosis of pulmonary TB was based on the presence of acid-fast bacilli on sputum smear or M. tuberculosis on sputum culture. In patients with smear-positive TB, culture was not done unless multidrug- resistant TB was strongly suspected. Sputum cultures were done in all patients with smear-negative pulmonary TB. In patients with negative smears and cultures (N = 17), the diagnosis of TB was based on symptoms, chest radiographic infiltrates in the upper lobes, and clinical and radiographic response to antituberculosis drugs. In addition, high resolution computed tomography (HRCT) for the patients showed tree-in-bud appearance compatible with the clinical diagnosis of pulmonary TB. Also, all 149 pulmonary TB patients showed a good clinical and radiographic response to anti-TB treatment. The severity of the pulmonary lesions was graded by studying the chest radiographs following the guidelines of the American Thoracic Society [27].
Table 1.
Clinical characteristics of the tuberculosis patients used for the study
| PTB | DTB | LNTB | |
|---|---|---|---|
| No. of patients | 149 | 11 | 25 |
| Age (years; ± SD) | 32.50 ± 13.3 | 34.36 ± 12.9 | 29.12 ± 11.6 |
| Sex (M:F) | 0.37:0.63 | 0.27:0.73 | 0.76: 0.24 |
| Sputum smear | 129 | 0 | 0 |
| Sputum culture | 47 | 0 | 0 |
| Lymph node FNAC | ND | 2 | 7 |
| Lymph node biopsy | ND | 3 | 20 |
| Pus smear | ND | 4 | 0 |
| Pus culture | ND | 6 | 0 |
| Positive TST response | 79 | 8 | 17 |
| Response to treatment | 149 | 11 | 25 |
Some patients in the PTB group had both smears and cultures positive while in the LNTB group, two patients had positive FNAC as well as biopsy positive. Similarly, in the DTB group 4 patients had both smear and cultures positive from the cold abscesses.
DTB: disseminated tuberculosis; PTB: pulmonary tuberculosis; LNTB = lymph node tuberculosis; FNAC= fine needle aspiration cytology
Disseminated tuberculosis
Focal disseminated tuberculosis (DTB) was diagnosed based on the criteria including i) clinical features suggestive of tuberculosis; ii) concurrent involvement of at least two non-contiguous organ sites of the body or involvement of the bone marrow; iii) microbiological and/or histopathological evidence of tuberculosis; (iv) evidence of marked improvement on antituberculosis treatment. The presence of all criteria was required for the diagnosis of disseminated tuberculosis and there were 11 patients in this group (Table 1). Of these, 2 patients had positive Ziehl-Neelsen (ZN) staining on fine needle aspiration cytology (FNAC) of the lymph nodes; 3 patients had histopathology of lymph nodes compatible with the diagnosis of TB; 4 patients had both positive ZN staining and Mycobacterium tuberculosis (Mtb) culture positivity in the pus from cold abscess and additional 2 patients had only Mtb culture positivity. All patients showed a good clinical response to anti-TB treatment.
Lymph node tuberculosis
Lymph node tuberculosis (LNTB) was diagnosed based on the following criteria i) clinical presentation compatible with tuberculosis; ii) fine needle aspiration cytology presenting evidence of tuberculosis with positive staining for acid-fast bacilli; iii) histopathological evidence of caseating granulomas on lymph node biopsy specimens; iv) evidence of marked improvement on antituberculosis treatment. The presence of i), and either ii) or iii) and iv) was required for the diagnosis of lymph node tuberculosis and there were 25 patients in this group (Table 1). Of these, 7 patients had positive ZN staining on FNAC and 20 had histopathology of the lymph nodes compatible with the diagnosis of tuberculosis of the lymph nodes (2 of these also had positive FNAC). All these patients showed a good clinical response to anti-TB treatment.
Normal Controls
Healthy Volunteers (referred to as normal controls, N = 155; mean age 28.16 ± 13.6 years; male:female 0.46:0.54) were randomly recruited from the general population with the same socio-economic status and ethnic background as that of the patients. All individuals gave informed consent and were screened negative for HIV infection and a family history of tuberculosis or any other related disease. In addition, these individuals had a negative tuberculin test (to exclude a possibility of a latent tuberculosis infection) and their chest radiographs as well as peripheral blood counts and blood chemistries were normal.
All patients with TB and normal controls recruited for the study represented a fairly homogeneous ethnic group of north Indian Hindu population from the states of Punjab, Haryana, Uttar Pradesh and Delhi. All these individuals come under the Indo-European linguistic group and belong to the same ethnic group (group 1) [28,29].
Tuberculin Skin Test (TST)
The TST was done using 5 tuberculin purified protein derivative (PPD) units (5 TU Tuberculin PPD/0.1 ml; Span Diagnostics Ltd., India); and the indurations were measured after 48 hours. A cut-off of 10 mm was used for a positive TST.
Serum TNF-α measurement
Serum TNF-α levels were determined for 107 tuberculosis patients and 112 normal controls using the OPTEIA™ ELISA kit (BD Biosciences), as per the manufacturer's instruction.
Genotyping
Isolation of the genomic DNA from the peripheral blood leukocytes was carried out using the modified salting out procedure as described elsewhere [16]. Polymorphisms in the TNF genes, namely TNFA-1031T > C, TNFA-863C > A, TNFA-857T > C, TNFA-308G > A, TNFA-238G > A and the LTA_NcoI polymorphism were genotyped using primer pairs as described elsewhere [16]. Briefly, the TNFA-1031T > C, TNFA-863C > A, TNFA-857T > C, TNFA-308G > A and the TNFA-238G > A were studied using SNaPshot ddNTP Primer Extension Kit (Applied Biosystems, Foster City, USA) as per the manufacturer's instructions. To clean up the primer extension reaction, 1U of calf intestinal phosphatase (CIP) (New England Biolabs) was added to the reaction mixture and the mixture was incubated at 37°C for 1 hour, followed by 15 minutes at 72°C for enzyme inactivation. These samples were subsequently electrophoresed using the ABI Prism 3100 Genetic Analyzer as per the manufacturer's instructions. The results were analyzed using the GeneMapper software (Applied Biosystems, Foster City, USA). The LTA_NcoI polymorphism was assessed using NcoI restriction endonuclease digestion. The accuracy of genotyping was confirmed by direct sequencing of the DNA samples (N = 5) for all three respective genotypes for all the loci investigated.
Statistical Analysis
The allele frequencies were calculated and agreement with Hardy-Weinberg equilibrium was tested using a χ2 goodness-of-fit test for each locus. The association between two categorical variables was evaluated by likelihood ratio (LR) χ2 and Fishers exact tests. All statistical tests performed were two-tailed. ANOVA was performed to test the effect of the polymorphisms and haplotypes on sTNF-α levels and F-ratio statistics were calculated to study the variation in sTNF-α levels in different groups. PHASE was used to infer haplotypes for each individual [30]. Clump22 software was used with 1,000,000 Monte-Carlo simulations to determine the primary difference in the haplotype frequencies [31]. Normal (T1) χ2 values, calculated from the 2 × N raw data, and maximum (T4) χ2 values, calculated by simulating 2 × N data followed by clumping into 2-by-2 tables to produce maximal chi-squared values, have been reported.
Results
Association of TNF polymorphisms with tuberculosis
The genotype frequencies for all the polymorphisms investigated did not deviate significantly from Hardy-Weinberg expectations in both the patient and the control populations (p > 0.05). Table 2 and Table 3 enlist the allele and the genotype frequencies for all the polymorphisms genotyped in the TNF genes, respectively. The comparison of the allele and genotype frequencies for all the loci investigated revealed no significant differences between the tuberculosis patients and controls (p > 0.05; Table 2 and Table 3, respectively).
Table 2.
Allele frequencies of the polymorphisms investigated in the TNFA and LTA genes.
| Polymorphism | Allele | Tuberculosis Patients (2N = 370) |
Normal Controls (2N = 310) |
FET p-value |
|---|---|---|---|---|
| NcoI | A | 270 (72.97) | 244 (78.71) | 0.09 |
| G | 100 (27.03) | 66 (21.29) | ||
| -1031 | C | 136 (36.76) | 110 (35.48) | 0.79 |
| T | 234 (63.24) | 200 (64.52) | ||
| -863 | A | 119 (32.16) | 100 (32.26) | >0.99 |
| C | 251 (67.84) | 210 (67.74) | ||
| -857 | C | 339 (91.62) | 276 (89.03) | 0.29 |
| T | 31 (8.38) | 34 (10.97) | ||
| -308 | A | 36 (9.73) | 27 (8.71) | 0.69 |
| G | 334 (90.27) | 283 (91.29) | ||
| -238 | A | 23 (6.22) | 14 (4.52) | 0.40 |
| G | 347 (93.78) | 296 (95.48) | ||
Numbers in parentheses indicate the frequency (%).
Table 3.
Genotype frequencies of the polymorphisms investigated in the TNFA and LTA genes.
| Polymorphism | Allele | Tuberculosis Patients (2N = 185) |
Normal Controls (2N = 155) |
LR χ2 | p-value (df = 2) |
|---|---|---|---|---|---|
| NcoI | AA | 94 (50.81) | 97 (62.58) | 3.43 | |
| AG | 82 (44.32) | 50 (32.26) | 0.18 | ||
| GG | 9 (4.86) | 8 (5.16) | |||
| -1031 | CC | 25 (13.51) | 20 (12.90) | 0.13 | |
| CT | 86 (46.49) | 70 (45.16) | 0.94 | ||
| TT | 74 (40.0) | 65 (41.94) | |||
| -863 | AA | 17 (9.19) | 17 (10.97) | 0.53 | |
| AC | 85 (45.95) | 66 (42.58) | 0.77 | ||
| CC | 83 (44.86) | 72 (46.45) | |||
| -857 | CC | 154 (83.24) | 123 (79.35) | NC | |
| CT | 31 (16.76) | 30 (19.35) | NS | ||
| TT | 0 (0) | 2 (1.29) | |||
| -308 | AA | 3 (1.62) | 2 (1.29) | NC | |
| AG | 30 (16.22) | 23 (14.84) | NS | ||
| GG | 152 (82.16) | 130 (83.87) | |||
| -238 | AA | 2 (1.08) | 0 (0) | NC | |
| AG | 19 (10.27) | 14 (9.03) | NS | ||
| GG | 164 (88.65) | 141 (90.97) | |||
Numbers in parentheses indicate the frequency (%).
df: Degrees of freedom; NC - Test not conducted as counts are less than 5 for a few categories; NS - Non-significant.
Association of TNF polymorphisms in tuberculosis sub-groups
The severity of the pulmonary lesions was graded by studying the chest radiographs following the guidelines of the American Thoracic Society [27]; the patients were sub-grouped into minimal, moderately advanced and far advanced. Further, the patients were also sub-grouped on the basis of response to TST (negative/positive) and the presence/absence of cavitary lesions. However, none of the studied polymorphisms showed a significant association with any of the patient sub-groups (p > 0.05; data not shown).
Association of TNF haplotypes with tuberculosis
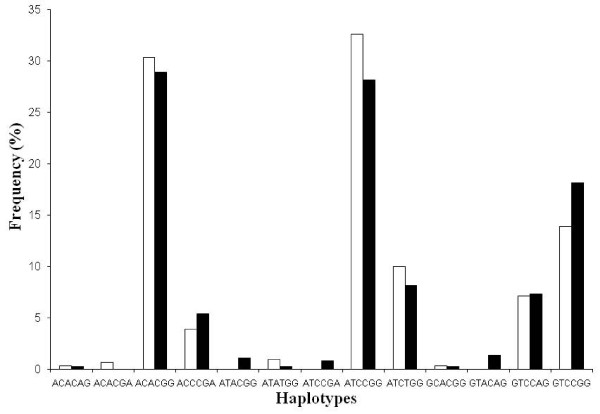
To study the combined effects of the six SNPs in the TNF genes, haplotypes were estimated by the statistical software PHASE. Of the 13 haplotypes observed in the 185 TB patients and 155 controls recruited for the study, only five haplotypes were represented at frequencies >5% (Figure 1). These accounted for >87% of the total haplotypes. As the count per haplotype was very low, Clump22 with 1,000,000 Monte-Carlo simulations was used to estimate differences in the haplotype frequencies in the patients and controls. However, no significant differences were observed in the haplotype counts in the two groups [normal (T1) χ2 = 18.498, df = 12, P = 0.78; and maximum (T4) χ2 = 7.825, P = 0.214]. Therefore, it may be concluded that haplotypes in the TNF genes were not associated with tuberculosis in the studied population.
Figure 1.
The frequency distribution of the haplotypes of the TNFA and LTA genes. The frequency distribution of the haplotypes of the TNFA and LTA genes in tuberculosis patients (dark bars) and unrelated controls (light bars). The haplotypes have been plotted on the x-axis and their respective relative frequencies (%) on the y-axis.
Association analyses of TNF polymorphisms with its serum levels
TNF-α levels were measured in the serum samples of 107 tuberculosis patients and 112 unrelated controls. A difference with borderline significance was observed in the serum TNF-α levels in the patients and the controls (F-ratio = 3.84, df = 1, p = 0.051); a higher levels of the cytokine was observed in the patients sera [log sTNF-α ± standard deviation (s.d.) = 1.89 ± 0.87] when compared with the control population [log sTNF-α ± s.d. = 1.65 ± 0.89].
Although, none of the investigated polymorphisms were found to affect the sTNF-α levels in both the patient and the control populations and in the patient sub-groups (p > 0.05), a few interesting observations were made. Of the 107 patients, 39 patients with positive TST showed higher log sTNF-α levels (2.10 ± 0.91) while 68 patients with negative TST showed lower log sTNF-α levels (1.75 ± 0.84) [F-ratio = 3.92, df = 1, p = 0.05]. Furthermore, when the patients were graded on the basis of severity into minimal severity, moderately advanced and far advanced sub-groups, it was observed that patients with minimal severity had lower log sTNF-α levels (1.54 ± 0.73) when compared to the patients with moderately advanced (1.86 ± 0.98) and far advanced severity (1.96 ± 0.71). However, none of these differences were statistically significant (p > 0.05). Additionally, no difference was observed in the log sTNF-α levels when patients were sub-grouped on the basis of presence/absence of cavitary lesions in the X-rays (p > 0.05).
Furthermore, when haplotypes (counts ≥ 2) were analyzed with respect to sTNF-α levels in the patient samples (case-only analysis), no significant difference were observed (p-value > 0.05), thereby negating the influence of any of the studied polymorphisms on sTNF-α levels in the study population.
Discussion
TNF-α plays an important role in granuloma formation in tuberculosis. Previous studies have shown that mice deficient in TNF-α exhibit poorly formed granulomas with areas of extensive necrosis, resulting in widespread dissemination of M. tuberculosis and rapid death of animals [32]. Earlier data obtained from the rheumatoid arthritis patients treated with TNF-α antagonists showed that blocking TNF-α could lead to reactivation of tuberculosis [33]. All these points hint towards TNFA as an important candidate gene for tuberculosis.
The promoter region of the TNFA gene is highly polymorphic. In this case-control study, conducted in tuberculosis patients and normal controls recruited from Northern India, we focused on potential functional polymorphisms in the transcriptional region of TNFA and a LTA_NcoI (+252) polymorphism in the first intron of LTA gene a few of which have earlier been associated with TNF-α levels [15,16]. Individually, none of the polymorphisms showed any significant association with tuberculosis or sTNF-α levels. An earlier study carried out in HLA-A, B and DR typed pulmonary tuberculosis patients (N = 210) and healthy control subjects (N = 120) from South India also failed to detect any significant differences between the LTA_NcoI and TNFA_-308 and TNFA_-238 polymorphisms and tuberculosis [20]. These included active and cured tuberculosis patients as well as controls of Indo-dravidian origin, an ethnicity different from ours, recruited from North-India and belonging to the Indo-European linguistic group. Additionally, another recent study carried out in the north-Indian populations also failed to find any association of TNFA -308 promoter polymorphism with tuberculosis [34]. This study was conducted in ethnically matched 145 physician diagnosed tuberculosis patients and 211 normal healthy controls recruited from the state of Punjab from North India. However, in both these studies no attempts were made to correlate these and the other promoter polymorphisms individually and at the level of haplotype with sTNF-α levels. Also, the normal controls recruited for our study were tested negative by the TST test and had normal blood chemistries, peripheral blood counts and normal chest radiographs. Additionally, all patients and controls recruited for our study were HIV-negative. Our study also gains support from others which report a lack of association between TNF gene polymorphisms and tuberculosis in different populations (Table 4). On the other hand, a few studies reported association between the TNFA_-308 polymorphism and tuberculosis [22,35-37]. However, these differences in results could be attributed to ethnic variations that persist in different populations, study design and patient selection criteria. Additionally, the association observed in the later studies may be explained on the basis of linkage disequilibrium that exists between the TNF genes and HLA [38].
Table 4.
Association studies of the TNF genes with tuberculosis.
| S. No | Reference | Polymorphisms Investigated | Location | Population | Sample size | Results |
|---|---|---|---|---|---|---|
| 1. | Selvaraj et al. [20] | TNFA -238, -308 and LTA (Nco I) | Promoter; Intron 1 | South Indian | 210 PTB patients and 120 normal controls (NC) | No association with pulmonary TB (PTB). |
| 2. | Ates et al. [17] | TNFA -308 G/A, -238 G/A, -376 G/A | Promoter | Turkish | 128 TB patients and 80 NC | No association with TB. |
| 3. | Vejbaesya et al. [21] | TNFA +488, -238, and -308 | Promoter | Thai | 149 TB patients and 147 NC | No association with TB. |
| 4. | Amirzargar et al. [37] | TNFA -308, G/A -238 | Promoter | Iranian | 41 PTB and 123 NC | -238 polymorphism was associated with pulmonary TB (p = 0.0009). |
| 5. | Shaw et al. [42] | Linkage study | Markers across the genome | Northern Brazilian | 98 pedigrees, with 704 individuals | Minor role of TNFA in control of TB. |
| 6. | Correa et al. [35,36] | TNFA -308, G/A -238 | Promoter | Columbia | 138 TB and 419 NC | Association of TNF1 with TB (OR: 1.9, 95%C.I. 1.2-3.1, p = 0.02) |
| 7. | Wu et al. [24] | TNFA -308 | Promoter | Chinese | 61 PTB patients and 122 PTB-free miners. | Lack of association with TB. |
| 8. | Larcombe et al. [26] | TNFA -308 | Promoter | Canadian Aboriginal | Three cohorts n = 61, 42 and 91 for Dené, Cree and healthy Caucasians, respectively | Lack of association with TB. |
| 9. | Henao et al. [25] | TNFA -308 | Promoter | Colombian | 54 tuberculin-negative NC, 81 tuberculin-positive NC, 140 PTB patients, 30 with pleural TB and 20 with miliary TB | Lack of association with TB. |
| 10. | Kumar et al. [34] | TNFA -308 | Promoter | Indian | 145 TB and 211 NC | Lack of association with TB. |
| 11. | Oh et al. [18] | TNFA -308 | Promoter | Korean | 117 NC, 80 newly diagnosed TB patients and 65 patients with recurrent TB | TNFA gene does not affect differential TB susceptibility. |
| 12. | Sharma et al. [Current] | LTA_NcoI; TNFA -238, -308, -857, -863, -1031 | Intron 1; Promoter | North Indian | 185 TB patients and 155 NC | Lack of association with TB. |
PTB = pulmonary tuberculosis; NC = normal controls
Our study also failed to detect any effect of the TNF polymorphisms on sTNF-α levels in the tuberculosis patients. The results from previous in vivo and in vitro studies conducted for the TNFA-308G > A polymorphism have rather been conflicting. Whereas there are studies which report the minor TNFA-308A allele (allele 2) to be associated with higher inducible levels of gene transcription and TNF-α production [39,40], our earlier study in sarcoidosis patients found the G allele for this polymorphism to be associated with high sTNF-α levels [16]. It is also evident from the study by Knight et al that the TNFA-308 SNP does not regulate TNF-α levels and is not likely to be the functionally important SNP as previously hypothesized [41]. Thus, it may be possible that another SNP in LD is involved in this phenomenon. Further high resolution HLA typing data in addition to fine mapping of the TNF genes would be of help in resolving these problems.
To enhance our understanding about the contribution of these genetic variants further to tuberculosis, six-locus haplotypes were constructed and their distribution was compared in the patients and the control population. None of the haplotype showed significant association with tuberculosis in the study population.
Conclusions
In summary, our findings suggest that the polymorphisms present in and around the TNF genes are unlikely to be the major risk factors for tuberculosis in Asian Indians. However, as the present study was performed with relatively small sample size, further studies with larger sample sizes would be necessary to elucidate the role of TNF polymorphisms in tuberculosis.
Abbreviations
HLA: Human leukocyte antigen; LR: Likelihood ratio; LTA: Lymphotoxin α; PPD: Purified protein derivative; TB: Tuberculosis; TNF: Tumor necrosis factor; TST: Tuberculin skin test
Competing interests
The authors declare that they have no competing interests.
Authors' contributions
SS, BG and SKS conceived and designed the study. SS and JR were involved in collection of the data. SS, JR, BG and SKS were involved in the analysis and interpretation of the data. SS, BG and SKS were involved in preparation and critical revision of the manuscript. All authors have approved the final version of the manuscript.
Pre-publication history
The pre-publication history for this paper can be accessed here:
Contributor Information
Shilpy Sharma, Email: shilpy.sharma@gmail.com.
Jaishriram Rathored, Email: jaishriz@gmail.com.
Balaram Ghosh, Email: bghosh@igib.res.in.
Surendra K Sharma, Email: surensk@gmail.com.
Acknowledgements
We thank all patients and healthy volunteers for participating in this study. The authors acknowledge the help extended by Ms. Yogita Dixit and Ms. Shweta Tamta during the course of this work. The work was supported by Department of Biotechnology, Govt. of India on Program Support for "Immunoproteomics Based Diagnostic of Infectious Disease" (BT/PR5100/MED/12/2005/2004). Shilpy Sharma acknowledges CSIR, Govt. of India, for her fellowship.
References
- Raviglione MC, Snider DE Jr, Kochi A. Global epidemiology of tuberculosis. Morbidity and mortality of a worldwide epidemic. JAMA. 1995;273:220–226. doi: 10.1001/jama.273.3.220. [DOI] [PubMed] [Google Scholar]
- Global tuberculosis control: key findings from the December 2009 WHO report. Wkly Epidemiol Rec. 2010;85:69–80. [PubMed] [Google Scholar]
- Comstock GW. Tuberculosis in twins: a re-analysis of the Prophit survey. Am Rev Respir Dis. 1978;117:621–624. doi: 10.1164/arrd.1978.117.4.621. [DOI] [PubMed] [Google Scholar]
- Schurr E. Is susceptibility to tuberculosis acquired or inherited? J Intern Med. 2007;261:106–111. doi: 10.1111/j.1365-2796.2006.01741.x. [DOI] [PubMed] [Google Scholar]
- Fernando SL, Britton WJ. Genetic susceptibility to mycobacterial disease in humans. Immunol Cell Biol. 2006;84:125–137. doi: 10.1111/j.1440-1711.2006.01420.x. [DOI] [PubMed] [Google Scholar]
- Hoal EG. Human genetic susceptibility to tuberculosis and other mycobacterial diseases. IUBMB Life. 2002;53:225–229. doi: 10.1080/15216540212644. [DOI] [PubMed] [Google Scholar]
- Malik S, Schurr E. Genetic susceptibility to tuberculosis. Clin Chem Lab Med. 2002;40:863–868. doi: 10.1515/CCLM.2002.153. [DOI] [PubMed] [Google Scholar]
- Nedwin GE, Naylor SL, Sakaguchi AY, Smith D, Jarrett-Nedwin J, Pennica D, Goeddel DV, Gray PW. Human lymphotoxin and tumor necrosis factor genes: structure, homology and chromosomal localization. Nucleic Acids Res. 1985;13:6361–6373. doi: 10.1093/nar/13.17.6361. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cuturi MC, Murphy M, Costa-Giomi MP, Weinmann R, Perussia B, Trinchieri G. Independent regulation of tumor necrosis factor and lymphotoxin production by human peripheral blood lymphocytes. J Exp Med. 1987;165:1581–1594. doi: 10.1084/jem.165.6.1581. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Flynn JL, Chan J. Immunology of tuberculosis. Annu Rev Immunol. 2001;19:93–129. doi: 10.1146/annurev.immunol.19.1.93. [DOI] [PubMed] [Google Scholar]
- Berner MD, Sura ME, Alves BN, Hunter KW Jr. IFN-gamma primes macrophages for enhanced TNF-alpha expression in response to stimulatory and non-stimulatory amounts of microparticulate beta-glucan. Immunol Lett. 2005;98:115–122. doi: 10.1016/j.imlet.2004.10.020. [DOI] [PubMed] [Google Scholar]
- Mohan VP, Scanga CA, Yu K, Scott HM, Tanaka KE, Tsang E, Tsai MM, Flynn JL, Chan J. Effects of tumor necrosis factor alpha on host immune response in chronic persistent tuberculosis: possible role for limiting pathology. Infect Immun. 2001;69:1847–1855. doi: 10.1128/IAI.69.3.1847-1855.2001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Fiorenza G, Rateni L, Farroni MA, Bogue C, Dlugovitzky DG. TNF-alpha, TGF-beta and NO relationship in sera from tuberculosis (TB) patients of different severity. Immunol Lett. 2005;98:45–48. doi: 10.1016/j.imlet.2004.09.008. [DOI] [PubMed] [Google Scholar]
- Westendorp RG, Langermans JA, Huizinga TW, Elouali AH, Verweij CL, Boomsma DI, Vandenbroucke JP. Genetic influence on cytokine production and fatal meningococcal disease. Lancet. 1997;349:170–173. doi: 10.1016/S0140-6736(96)06413-6. [DOI] [PubMed] [Google Scholar]
- Sharma S, Sharma A, Kumar S, Sharma SK, Ghosh B. Association of TNF haplotypes with asthma, serum IgE levels, and correlation with serum TNF-alpha levels. Am J Respir Cell Mol Biol. 2006;35:488–495. doi: 10.1165/rcmb.2006-0084OC. [DOI] [PubMed] [Google Scholar]
- Sharma S, Ghosh B, Sharma SK. Association of TNF polymorphisms with sarcoidosis, its prognosis and tumour necrosis factor (TNF)-alpha levels in Asian Indians. Clin Exp Immunol. 2008;151:251–259. doi: 10.1111/j.1365-2249.2007.03564.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ates O, Musellim B, Ongen G, Topal-Sarikaya A. Interleukin-10 and tumor necrosis factor-alpha gene polymorphisms in tuberculosis. J Clin Immunol. 2008;28:232–236. doi: 10.1007/s10875-007-9155-2. [DOI] [PubMed] [Google Scholar]
- Oh JH, Yang CS, Noh YK, Kweon YM, Jung SS, Son JW, Kong SJ, Yoon JU, Lee JS, Kim HJ, Park JK, Jo EK, Song CH. Polymorphisms of interleukin-10 and tumour necrosis factor-alpha genes are associated with newly diagnosed and recurrent pulmonary tuberculosis. Respirology. 2007;12:594–598. doi: 10.1111/j.1440-1843.2007.01108.x. [DOI] [PubMed] [Google Scholar]
- Qu Y, Tang Y, Cao D, Wu F, Liu J, Lu G, Zhang Z, Xia Z. Genetic polymorphisms in alveolar macrophage response-related genes, and risk of silicosis and pulmonary tuberculosis in Chinese iron miners. Int J Hyg Environ Health. 2007;210:679–689. doi: 10.1016/j.ijheh.2006.11.010. [DOI] [PubMed] [Google Scholar]
- Selvaraj P, Sriram U, Mathan KS, Reetha AM, Narayanan PR. Tumour necrosis factor alpha (-238 and -308) and beta gene polymorphisms in pulmonary tuberculosis: haplotype analysis with HLA-A, B and DR genes. Tuberculosis (Edinb) 2001;81:335–341. doi: 10.1054/tube.2001.0307. [DOI] [PubMed] [Google Scholar]
- Vejbaesya S, Chierakul N, Luangtrakool P, Sermduangprateep C. NRAMP1 and TNF-alpha polymorphisms and susceptibility to tuberculosis in Thais. Respirology. 2007;12:202–206. doi: 10.1111/j.1440-1843.2006.01037.x. [DOI] [PubMed] [Google Scholar]
- Scola L, Crivello A, Marino V, Gioia V, Serauto A, Candore G, Colonna-Romano G, Caruso C, Lio D. IL-10 and TNF-alpha polymorphisms in a sample of Sicilian patients affected by tuberculosis: implication for ageing and life span expectancy. Mech Ageing Dev. 2003;124:569–572. doi: 10.1016/S0047-6374(03)00038-1. [DOI] [PubMed] [Google Scholar]
- Oral HB, Budak F, Uzaslan EK, Basturk B, Bekar A, Akalin H, Ege E, Ener B, Göral G. Interleukin-10 (IL-10) gene polymorphism as a potential host susceptibility factor in tuberculosis. Cytokine. 2006;35:143–147. doi: 10.1016/j.cyto.2006.07.015. [DOI] [PubMed] [Google Scholar]
- Wu F, Qu Y, Tang Y, Cao D, Sun P, Xia Z. Lack of association between cytokine gene polymorphisms and silicosis and pulmonary tuberculosis in Chinese iron miners. J Occup Health. 2008;50:445–454. doi: 10.1539/joh.L8006. [DOI] [PubMed] [Google Scholar]
- Henao MI, Montes C, Paris SC, Garcia LF. Cytokine gene polymorphisms in Colombian patients with different clinical presentations of tuberculosis. Tuberculosis (Edinb) 2006;86:11–19. doi: 10.1016/j.tube.2005.03.001. [DOI] [PubMed] [Google Scholar]
- Larcombe LA, Orr PH, Lodge AM, Brown JS, Dembinski IJ, Milligan LC, Larcombe EA, Martin BD, Nickerson PW. Functional gene polymorphisms in canadian aboriginal populations with high rates of tuberculosis. J Infect Dis. 2008;198:1175–1179. doi: 10.1086/592049. [DOI] [PubMed] [Google Scholar]
- Diagnostics standards and classification of tuberculosis. New York: National Tuberculosis Association; 1961. National Tuberculosis Association of the USA. [Google Scholar]
- The Indian Genome Variation database (IGVdb): a project overview. Hum Genet. 2005;118:1–11. doi: 10.1007/s00439-005-0009-9. [DOI] [PubMed] [Google Scholar]
- Genetic landscape of the people of India: a canvas for disease gene exploration. J Genet. 2008;87:3–20. doi: 10.1007/s12041-008-0002-x. [DOI] [PubMed] [Google Scholar]
- Stephens M, Smith NJ, Donnelly P. A new statistical method for haplotype reconstruction from population data. Am J Hum Genet. 2001;68:978–989. doi: 10.1086/319501. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sham PC, Curtis D. Monte Carlo tests for associations between disease and alleles at highly polymorphic loci. Ann Hum Genet. 1995;59:97–105. doi: 10.1111/j.1469-1809.1995.tb01608.x. [DOI] [PubMed] [Google Scholar]
- Bean AG, Roach DR, Briscoe H, France MP, Korner H, Sedgwick JD, Britton WJ. Structural deficiencies in granuloma formation in TNF gene-targeted mice underlie the heightened susceptibility to aerosol Mycobacterium tuberculosis infection, which is not compensated for by lymphotoxin. J Immunol. 1999;162:3504–3511. [PubMed] [Google Scholar]
- Gomez-Reino JJ, Carmona L, Valverde VR, Mola EM, Montero MD. Treatment of rheumatoid arthritis with tumor necrosis factor inhibitors may predispose to significant increase in tuberculosis risk: a multicenter active-surveillance report. Arthritis Rheum. 2003;48:2122–2127. doi: 10.1002/art.11137. [DOI] [PubMed] [Google Scholar]
- Kumar V, Khosla R, Gupta V, Sarin BC, Sehajpal PK. Differential association of tumour necrosis factor-alpha single nucleotide polymorphism (-308) with tuberculosis and bronchial asthma. Natl Med J India. 2008;21:120–122. [PubMed] [Google Scholar]
- Correa PA, Gomez LM, Cadena J, Anaya JM. Autoimmunity and tuberculosis. Opposite association with TNF polymorphism. J Rheumatol. 2005;32:219–224. [PubMed] [Google Scholar]
- Correa PA, Gomez LM, Anaya JM. Polymorphism of TNF-alpha in autoimmunity and tuberculosis. Biomedica. 2004;24(Supp 1):43–51. [PubMed] [Google Scholar]
- Amirzargar AA, Rezaei N, Jabbari H, Danesh AA, Khosravi F, Hajabdolbaghi M, Yalda A, Nikbin B. Cytokine single nucleotide polymorphisms in Iranian patients with pulmonary tuberculosis. Eur Cytokine Netw. 2006;17:84–89. [PubMed] [Google Scholar]
- Price P, Witt C, Allcock R, Sayer D, Garlepp M, Kok CC, French M, Mallal S, Christiansen F. The genetic basis for the association of the 8.1 ancestral haplotype (A1, B8, DR3) with multiple immunopathological diseases. Immunol Rev. 1999;167:257–274. doi: 10.1111/j.1600-065X.1999.tb01398.x. [DOI] [PubMed] [Google Scholar]
- Kroeger KM, Carville KS, Abraham LJ. The -308 tumor necrosis factor-alpha promoter polymorphism effects transcription. Mol Immunol. 1997;34:391–399. doi: 10.1016/S0161-5890(97)00052-7. [DOI] [PubMed] [Google Scholar]
- Wilson AG, Symons JA, McDowell TL, McDevitt HO, Duff GW. Effects of a polymorphism in the human tumor necrosis factor alpha promoter on transcriptional activation. Proc Natl Acad Sci USA. 1997;94:3195–3199. doi: 10.1073/pnas.94.7.3195. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Knight JC, Keating BJ, Rockett KA, Kwiatkowski DP. In vivo characterization of regulatory polymorphisms by allele-specific quantification of RNA polymerase loading. Nat Genet. 2003;33:469–475. doi: 10.1038/ng1124. [DOI] [PubMed] [Google Scholar]
- Shaw MA, Collins A, Peacock CS, Miller EN, Black GF, Sibthorpe D, Lins-Lainson Z, Shaw JJ, Ramos F, Silveira F, Blackwell JM. Evidence that genetic susceptibility to Mycobacterium tuberculosis in a Brazilian population is under oligogenic control: linkage study of the candidate genes NRAMP1 and TNFA. Tuber Lung Dis. 1997;78:35–45. doi: 10.1016/S0962-8479(97)90014-9. [DOI] [PubMed] [Google Scholar]