Abstract
Originally aimed at treating degenerative syndromes of the lumbar spine, percutaneous minimally invasive posterior fixation is nowadays even more frequently used to treat some thoracolumbar fractures. According to the modern principles of saving segment of motion, a short implant (one level above and one level below the injured vertebra) is generally used to stabilise the injured spine. Although the authors generally use a short percutaneous fixation in treating thoracolumbar fractures with good results, they observed some cases in which the high fragmentation of the vertebral body and the presence of other associated diseases (co-morbidities) did not recommend the use of a short construct. The authors identified nine cases, in which a long implant (two levels above and two levels below the injured vertebra) was performed by a percutaneous minimally invasive approach. Seven patients (five males/two females) were affected by thoracolumbar fractures. T12 vertebra was involved in three cases, L1 in two cases, T10 and L2 in one case, respectively. Two fractures were classified as type A 3.1, two as A 3.2, two as A 3.3 and one as B 2.3, according to Magerl. In the present series, there were also two patients affected by a severe osteolysis of the spine (T9 and T12) due to tumoral localisation. All patients operated on with long instrumentation had a good outcome with prompt and uneventful clinical recovery. At the 1-year follow-up, all patients except one, who died 11 months after the operation, did not show any radiologic signs of mobilisation or failure of the implant. Based on the results of the present series, the long percutaneous fixation seems to represent an effective and safe system to treat particular cases of vertebral lesions. In conclusion, the authors believe that a long implant might be an alternative surgical method compared to more aggressive or demanding procedures, which in a few patients could represent an overtreatment.
Keywords: Minimally invasive spinal surgery, Percutaneous fixation, Short implant, Long implant, Thoracolumbar fractures
Introduction
Originally aimed at treating degenerative pathologies, the minimally invasive posterior pedicle screwing is even more frequently used to treat other pathologies of the spine, such as some types of thoracolumbar fractures.
The most important advantages of minimally invasive spinal surgery are the prompt recovery of the patient and the decrease in the complications by minimising iatrogenic tissue injury typical of that encountered following open spine surgery. Following the introduction of such a method as a daily practice, it has become evident that it was possible to obtain better results in patients affected by thoracolumbar fractures by using a minimally invasive posterior approach.
From 2003, we have started to use the minimally invasive approach to the lumbar spine affected by degenerative pathologies and soon after extended the indications to the treatment of well-defined spinal pathologies, such as particular types of thoracolumbar fractures and tumour lesions. According to the intrinsic characteristics of each lesion, we have always carried out the shortest possible implant with the aim of saving segments of motion. In some particular cases, we have adopted an unusually long construct. This kind of implant, unavoidably sacrifices further segments of motion, yet, on the other hand, it is able to grant a primary greater stability, which is particularly desirable in certain unstable or potentially unstable lesions. In this paper, we focused our attention only on patients treated with long implant stabilisation that represents, under some aspects, the personal modification of the minimally invasive Pathfinder (Abbott Spine) system. Technical notes and results are presented and discussed.
Materials and methods
We performed a long construct by using a minimally invasive posterior approach in nine patients (seven males, two females). Seven patients were affected by thoracolumbar fractures and two had tumours. In the fracture group, there were five males and two females with a minimum age of 48, a maximum age of 68 and an average age of 60. The affected levels were T10 (n = 1), T12 (n = 3), L1 (n = 2) and L2 (n = 1). Two fractures were classified as being type A 3.1, two as A 3.2, two as A 3.3 and one as B 2.3, according to the Magerl et al. classification [1]. Two patients were affected by tumours; one had a T12 metastasis of urothelial carcinoma (83 years old) and the other a single localisation of myeloma in T9 (81 years old).
All patients were surgically stabilised by the long implant fixation system Pathfinder (Abbott Spine) applied through a minimally invasive posterior approach. The long implant was carried out by positioning two pairs of screws in the pedicles of the two proximal vertebrae next to the injured vertebrae and another two pairs of screws in the distal vertebrae. In one case (T9 myeloma), the proximal screws were positioned in the T7 and T8 pedicles, and the distal ones in the T11 and T12 pedicles with the aim of carrying out a longer construct (Fig. 1). The implantation technique does not differ significantly from that utilised in the case of the classic short implant, except for some technical details that we refer to. The first detail is the positioning of the patient on the surgical table. The patient has to be carefully positioned on the table in order to obtain the best pre-operative reduction of the kyphotic acquired deformity, because the system employed allows only some distraction–compression manoeuvres that could be ineffective in producing a good fracture reduction. The screws are positioned at the planned pre-operative levels, under fluoroscopy, through small skin incisions centred above the projection of the pedicles. One of the most interesting aspects of the present fixation system is the availability of smaller diameter pedicular screws for use in the thoracic tract that is notoriously more demanding for well-known anatomical reasons. A very important technical detail concerns the modelling of the rod before its final positioning. As the system does not allow in situ correction, a careful bending of the rod before its implantation, according to the level of the lesion, is required. The localisation of the fractures at the transition zone, such as the fractures of T12 and L1 vertebral bodies, requires a careful bending of the rod, on the sagittal plane, in the opposite direction in order to respect proximal kyphosis and distal lordosis (Fig. 2). A careful modelling of the rod is required in the thoracic region to preserve the pre-existing kyphotic angle of the patients. In one case (T10 fracture), the patient had a significant degree of hyperkyphosis of the thoracic spine (Fig. 3).
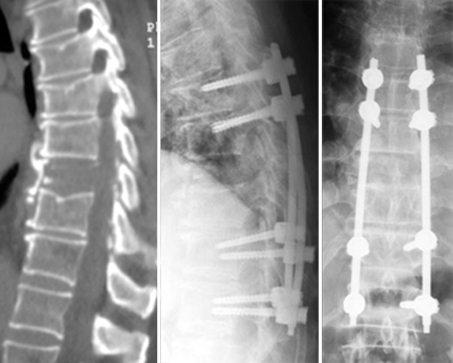
Fig. 1.
An 81-year-old male affected by T9 localisation of myeloma before operation and at 1-year follow-up. The patient was operated on with long posterior minimally invasive stabilisation system extended from T7 to T12. Pedicular screws were positioned percutaneously in the pedicles of T7/T8 proximally and in the pedicles of T11/T12 distally
Fig. 2.
A 48-year-old male who reported fracture of L1 as well as a bilateral wrist fracture. Because the fractures of the wrists made it impossible for him to conduct a normal daily life, he refused any conservative treatment or open access to the spine. He was operated on with percutaneous long implant extended from T11 to L3. He started to ambulate the day after the operation. At 1-year follow-up, he was pain free; no changes in the implant imaging was observed
Fig. 3.
A 68-year-old farmer reported a fracture of the T10, rib fractures and pulmonary contusion with breathing dysfunction, after falling from an olive tree. He was operated on with long posterior percutaneuos fixation with rapid improving of his breathing. The implant was extended from T8 proximally to T12 distally. Because the system does not allow in situ modelling, the rod was carefully bent to adapt to the hyperkyphosis of the patient before its final positioning. At 1-year follow-up, there were no modifications of the implant and the patient returned to his job
The decision to carry out a long stabilisation in the present series of patients, instead of a short implant, was strongly influenced by a lot of clinical aspects, which have been illustrated in Table 1 as co-morbidities. One of the most recurrent co-morbidities is the very low compliance of the patients to any type of conservative treatment or bed rest. In no. 1, the female patient was affected by epilepsy and had a serious postural problem and walking disability as a consequence of congenital brain malformation, which was operated on in childhood. She used a crutch to improve her static balance. Any kind of orthosis caused the worsening of her postural problem and walking ability. Another female patient (case no. 2) was affected by Parkinson’s disease and osteoporosis. Her camptocormic posture was dramatically worsened by regional kyphosis induced by the L1 fracture. She lived alone and had a serious walking disability. In patient no. 3 (Fig. 3), all kinds of conservative treatment were contraindicated due to the presence of multiple rib fractures and breathing difficulties. The patient was suddenly mobilised soon after the operation with an evident improvement of lung functioning. The no. 5 patient (Fig. 2) was affected by L1 fracture as well as a bilateral wrist fracture. The spinal fracture was assessed to be treated by means of conservative method, but the patient refused any kind of orthosis and bed rest due to the fact that the fractures of the wrists made it impossible for him to conduct a normal daily life.
Table 1.
Minimally invasive long-implant stabilisation comprehensive data
| Patient no. | Age/sex | Level | Cause | Type | Proximal screws | Distal screws | Co-morbidity |
|---|---|---|---|---|---|---|---|
| 1 | 58/female | T12 misdiagnosed fracture (5 months previously) | Fall | A 3.1 | T10/T11 | L1/L2 | Severe Parkinson’s disease, osteoporosis, severe kyphotic disalignment |
| 2 | 60/female | L1 misdiagnosed fracture (3 months previously) | Fall | A 3.1 | T11/T12 | L2/L3 | Emiplegia, severe walking disability, hip fracture, osteoporosis |
| 3 | 68/male | T 10 | Fall from olive tree | B 2.3 | T8/T9 | T11/T12 | Rib fractures, pulmonary contusion, wide area of skin sufferance on the dorsum |
| 4 | 72/male | L2 misdiagnosed fracture (6 months previously) | Fall from 3 m height | A 3.2 | T12/L1 | L3/L4 | Claustrophobic syndrome, no collaborating patient, osteoporosis |
| 5 | 48/male | L1 | Car accident | A 3.2 | T11/T12 | L2/L3 | Bilateral wrist fracture, extremely low compliance to conservative treatment |
| 6 | 52/male | T12 | Fall | A 3.3 | T10/T11 | L1/L2 | Left heel fracture, right wrist fracture |
| 7 | 63/male | T12 | Vehicle accident | A 3.3 | T10/T11 | L1/L2 | Rib fracture, head injury |
Two patients were affected by tumours. The first case was that of an old man (83 years old), who was operated on 6 months previously for a urothelial bladder carcinoma and had a short lifespan prognosis. A CT scan of the chest revealed multiple lung metastases and an osteolytic lesion of the pedicle and half the T12 on the right side of the body. A long implant extending from T10 to L2 was carried out. The patient started to walk the day after the operation without pain. He remained pain free till 11 months later when he died. The second case refers to an old man (81 years) who was sent to our department due to a severe T9 osteolysis (Fig. 1). He was not able to walk and had been confined to bed 2 months previously due to this condition. A CT percutaneous biopsy diagnosed a solitary myeloma. In view of the poor clinical conditions and the bad prognosis, we decided to perform a long, percutaneous stabilisation in a first step further delaying more demanding surgical procedures depending on the post-operative recovery of the patient. The patient’s general clinical condition improved rapidly. At the 1-year follow-up, he was pain free, walking without the aid of a crutch and refused other surgical treatments.
Clinical assessment was carried out pre-operatively and then before discharging the patients from hospital and at 3 month, 6 month and 1-year intervals. Pre-operative and early post-operative imaging studies of the spine included standard X-rays, CT scans and, in the two patients suffering from tumours, also MR imaging. The assessment included implant imaging evaluation and the clinical outcome of the patients. The accuracy of pedicle screws placement, and the presence of radiolucency around the screws or its breakage was assessed. Pain was graded according to the Visual Analogue Pain Scale (VAS, 0–10).
Results
All patients had a very fast and uneventful post-operative recovery. No complications related to the surgical technique were seen. The long-term results of all patients except one (affected by a tumour and who died 11 months after the operation) were assessed 1 year following the operation. Clinical outcome was satisfactory in all the cases. Patients were able to walk without external aid (except case no.1) and three of them returned to their occupation. Pain was referred to be absent or very mild (VAS > 8–9), although the data have no statistic relevance. The careful examination of the imaging, at 1-year follow-up, showed no radiolucency around the screws, which are recognised as early signs of implant failure, or breakage of the implants.
Discussion
To date, the management of traumatic thoracolumbar fractures remains controversial. Despite a considerable amount of relevant literature, clear evidence regarding the most suitable treatment for traumatic thoracolumbar spine fractures is lacking. [2, 3] A great number of thoracolumbar burst fractures may be treated in the traditional manner by means of posterior fixation implants. In the last few decades, efforts have been made to improve the clinical outcome of the patients undergoing operations, essentially by minimising the invasive nature of the open approach and by reducing the segments of motion involved in the fusion area, although a high failure rate has also been reported with short-segment constructs. Several factors are regarded as being potential causes of short implant failure, among which the most important seems to be the inadequate anterior column support. Therefore, in cases of real or impending anterior column deficiency, such as in the case of severe comminution of the vertebral body, a short construct alone could prove to be an almost certain failure. The real problem approaching an unstable or potentially unstable vertebral lesion seems to be the choice of the best way in which to support the spine by avoiding either extremely demanding or invasive procedures or too simple constructs, which could be at high risk of implant failure. Although the modern trend is to use short spinal instrumentation systems, no guidelines exist in literature for the proper selection of patients suitable for their use. Parker et al. [4] used the Load-Sharing Classification [5] prospectively to determine the approach for short-segment instrumentation. In their opinion, a general assessment of comminution is the most important way to clinically predict successful short-segment thoracolumbar spinal fracture repair. Only fractures with mild comminution can be successfully repaired from the posterior approach with pedicle screw-based implants, while long-segment fracture repair is used for patients with unpredictable post-operative compliance. Altay et al. [6], in a retrospective study, compared the outcomes of the short-segment posterior fixation (SSPF) and long-segment posterior fixation (LSPF) in unstable thoracolumbar junction burst fractures (T12-L2) in Magerl Type-A fractures. A solid fixation, without implant failure, was achieved with SSPF in patients, with Load-Sharing Classification (LSC) point 7 or less with Magerl Type A3.1 and A3.2 fractures (LSC point 6 or less in Magerl Type A3.3), while LSPF was more beneficial in Magerl Type A3.3 fractures with LSC point 7 or more (LSC points 8–9 in Magerl Type A3.1 and A3.2). Recently, minimally invasive posterior approach has been suggested for the treatment of thoracolumbar fractures. Barbanti Brodano et al. [7] operated on 23 type-A (6 A1, 6 A2 and 11 A3) and 2 B2 fractures according to Magerl et al. classification with good clinical outcomes and with no significant complications. They suggest a mini-invasive short construct in type-A thoracolumbar spinal fractures as an alternative to the traditional treatment method. Other authors, with the aim of preventing the loss of height of the vertebral body, suggested the association of a short-segment percutaneous instrumentation and kyphoplasty carried out in the same time to reinforce the anterior column [8–10] or as reported by Maciejczak et al. too [11], which proposed a vertebral corpectomy and pedicular fixation to treat burst fractures, but only relating to sub-type B fractures according to the Denis classification [12] or subtype A 3.1 according to Magerl’s classification. The advantage of the method is the possibility of carrying out a corpectomy without having to use an anterior approach, whilst the main disadvantage is that it is a particularly demanding technique and requires great surgical expertise.
Right from the first experiences using the percutaneous pedicular fixation method in the treatment of degenerative lumbar pathologies, we have hypothesised the possible extension of the indications of such a method also to the treatment of thoracolumbar type A fractures. Although we generally use a short implant pedicular fixation with a minimally invasive approach, in a few cases we preferred to use a long construct because of the presence of a high grade of comminution of the fractured vertebral body and/or the association of other pathologies. In fact although certain type-A Magerl fractures are assessed to be stable, their grade of comminution is such that they can represent a real risk of failure of a short implant due to the lack of adequate anterior support. Moreover, in a few patients, we have observed the concomitance of other extrarachideal diseases (co-morbidities), which strongly advise against the use of short implants. Therefore, in a few well-selected cases, we considered that it was better to use a long multi-level implant, which is always carried out by means of a minimally invasive percutaneous method, rather than resorting to an open surgery technique or methods, which are particularly complex or demanding. We used the Pathfinder (Abbott Spine) pedicle instrumentation system, which is one of the most recent minimally invasive systems that allows multiple-level instrumentation. The system was used in two more patients, who were affected by tumour localised to the spine. In both cases, there was a high risk of further collapse of the spine, following neurologic complications. Both patients were very old and, at the first observation, in bad general clinical condition that did not recommend demanding surgical procedures. They were stabilised with minimally invasive procedures with a fast clinical recovery after the operation. The patient affected by T12 urothelial metastasis started to walk the day after the operation and he was discharged from the hospital in the 4th postoperative day. The patient affected by T9 myeloma was transferred to the rehabilitation department soon after spine stabilisation.
The most important criticisms that could be made on this kind of orientation guideline in treating thoracolumbar burst fractures with long percutaneous implants are the lack of spine fusion and the greater sacrifice of segments of motion. With regard to the need for a fusion, recently, a prospective randomised study compared the clinical and radiographic outcome of two groups of patients affected by surgically open stabilised burst fracture [13]. The non-fusion group had a greater loss of correction in the sagittal curve, although the residual deformity did not correlate with the symptoms encountered during the checkup, while the percentage of vertebral body height loss was significantly higher in the fusion group. Segmental motion was significantly greater in the non-fusion group, but did not reach the criteria of instability. No significant differences in low back outcome score were observed on long-term follow-up, on comparing the groups with and without fusion. Screw breakage was encountered at an overall incidence of 13.7–16.6% for the fusion group and 10.7% of the non-fusion group. Especially from the clinical point of view, this paper seems to encourage percutaneous fixation without fusion, although from a biomechanical point of view, quite a few doubts remain concerning the survival of the implant. Although the follow-up is too short to draw any conclusion, in our little series of long posterior percutaneous stabilisation without fusion, we did not recognise any case of rod–screws breakages, any mobilisation of the implant or painful implant-related syndrome. Among the minimally invasive technique users, the need to remove the implant once the fracture heals may be a matter of discussion in the future.
With regard to the sacrificing of segments of motion, it is evident that the problem specifically affects the lumbar spine area. In fact, the proximal lengthening of the fixation to the thoracic tract is not biomechanically so relevant due to the fact that the thoracic segments are barely mobile; therefore, a longer fixation does not influence significantly the overall movement of the spine. Quite a different matter, for biomechanical considerations, is the distal lengthening of the implant to a lower lumbar motion segment. If we compare the short and long constructs, the real difference between the two systems, in terms of global movement of the spine, is the loss of only one more distal segment of motion that is suppressed in the long stabilisation. In this case, there is an obvious loss of a certain degree of lumbar spine motion, although the patients operated on by long implants did not refer to symptoms related to spinal stiffness. We think that, in particular patients, it could be more reasonable to choose to sacrifice one or more segments of motion than to perform a demanding surgical procedure.
However, further investigations will be required to assess the efficacy of the procedure. At present, the long construct, carried out by means of the percutaneous approach, proved to be effective in providing good primary correction of the sagittal balance of the spine, to prevent further loss of the correction and to ensure a prompt recovery with good clinical outcome.
Conclusion
New techniques of surgical percutaneous pedicle screw stabilisation of the spine have become popular as immediate primary stability of the spine is achieved with a short bed rest and brief hospitalisation. To date, percutaneous short-segment fixation reveals an effective and safe method to cure stable thoracolumbar fractures, if properly indicated. In fact, careful attention has to be paid to the correct indication for short-segment fixation due to the high failure rate of the implant that occurs in patients who are not properly selected. In a few cases, there are some patient-specific co-morbidities, which are too relevant to ignore in the decision-making process. In these cases, an aggressive surgical approach could represent an overtreatment, while a long posterior screw fixation could represent an effective alternative option. In these well-selected cases, it is possible to perform a percutaneous multi-level construct, obtaining the same advantages that are typical of the minimally invasive techniques. A long implant is then realised by applying percutaneous pedicle screws two levels below and two levels above the injured vertebra. The good results obtained in our small series encourage the use of a long percutaneous implant as an alternative method to short-segment fixation, when the patient’s co-morbidities do not require more aggressive surgery such as open anterior or posterior surgery procedures or combined anterior–posterior approaches.
Conflict of interest statement
None of the authors has any potential conflict of interest.
References
- 1.Magerl F, Aebi M, Gertzbein SB, et al. A comprehensive classification of thoracic and lumbar injuries. Eur Spine J. 1994;3:184–201. doi: 10.1007/BF02221591. [DOI] [PubMed] [Google Scholar]
- 2.Verlaan JJ, Diekerhof CH, Buskens E, et al. Surgical treatment of traumatic fractures of the thoracic and lumbar spine: a systematic review of the literature on techniques, complications, and outcome. Spine. 2004;29:803–814. doi: 10.1097/01.BRS.0000116990.31984.A9. [DOI] [PubMed] [Google Scholar]
- 3.Stadhouder A, Buskens E, Klerk LW, et al. Traumatic thoracic and lumbar spinal fractures: operative or nonoperative treatment: comparison of two treatment strategies by means of surgeon equipoise. Spine. 2008;33:1006–1017. doi: 10.1097/BRS.0b013e31816c8b32. [DOI] [PubMed] [Google Scholar]
- 4.Parker JW, Lane JR, Karaikovic EE, et al. Successful short-segment instrumentation and fusion for thoracolumbar spine fractures: a consecutive 41/2-year series. Spine. 2000;25:1157–1170. doi: 10.1097/00007632-200005010-00018. [DOI] [PubMed] [Google Scholar]
- 5.McCormack T, Karaikovic E, Gaines RW. The load sharing classification of spine fractures. Spine. 1994;19:1741–1744. doi: 10.1097/00007632-199408000-00014. [DOI] [PubMed] [Google Scholar]
- 6.Altay M, Ozkurt B, Aktekin CN, et al. Treatment of unstable thoracolumbar junction burst fractures with short- or long-segment posterior fixation in Magerl type A fractures. Eur Spine J. 2007;16:1145–1155. doi: 10.1007/s00586-007-0310-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Barbanti Brodano G, Iure F, Cappuccio M, et al. Osteosintesi con tecnica percutanea mininvasiva nel trattamento delle fratture vertebrali toraciche e lombari. Esperienza preliminare. GIOT. 2007;33:78–85. [Google Scholar]
- 8.Cho DY, Lee WY, Sheu PC. Treatment of thoracolumbar burst fractures with polymethyl methacrylate vertebroplasty and short-segment pedicle screw fixation. Neurosurgery. 2003;53:1354–1360. doi: 10.1227/01.NEU.0000093200.74828.2F. [DOI] [PubMed] [Google Scholar]
- 9.Verlaan JJ, Dhert WJ, Verbout AJ, et al. Balloon vertebroplasty in combination with pedicle screw instrumentation: a novel technique to treat thoracic and lumbar burst fractures. Spine. 2005;30:E73–E79. doi: 10.1097/01.brs.0000152162.64015.fb. [DOI] [PubMed] [Google Scholar]
- 10.Fuentes S, Metellus P, Fondop J, et al. Percutaneous pedicle screw fixation and kyphoplasty for management of thoracolumbar burst fractures. Neurochirurgie. 2007;53:272–276. doi: 10.1016/j.neuchi.2007.04.006. [DOI] [PubMed] [Google Scholar]
- 11.Maciejczak A, Barnas P, Dudziak P, et al. Posterior keyhole corpectomy with percutaneous pedicle screw stabilization in the surgical management of lumbar burst fractures. Neurosurgery. 2007;60:232–242. doi: 10.1227/01.NEU.0000255399.08033.B3. [DOI] [PubMed] [Google Scholar]
- 12.Denis F. Spinal instability as defined by the three-column spine concept in acute spinal trauma. Clin Orthop Relat Res. 1984;189:65–76. [PubMed] [Google Scholar]
- 13.Wang ST, Ma HL, Liu CL, et al. Is fusion necessary for surgically treated burst fractures of the thoracolumbar and lumbar spine? A prospective, randomized study. Spine. 2006;31:2646–2652. doi: 10.1097/01.brs.0000244555.28310.40. [DOI] [PubMed] [Google Scholar]