Abstract
Hereditary neuropathies form a heterogeneous group of disorders for which over 40 causal genes have been identified to date. Recently, dominant mutations in the transient receptor potential vanilloid 4 gene were found to be associated with three distinct neuromuscular phenotypes: hereditary motor and sensory neuropathy 2C, scapuloperoneal spinal muscular atrophy and congenital distal spinal muscular atrophy. Transient receptor potential vanilloid 4 encodes a cation channel previously implicated in several types of dominantly inherited bone dysplasia syndromes. We performed DNA sequencing of the coding regions of transient receptor potential vanilloid 4 in a cohort of 145 patients with various types of hereditary neuropathy and identified five different heterozygous missense mutations in eight unrelated families. One mutation arose de novo in an isolated patient, and the remainder segregated in families. Two of the mutations were recurrent in unrelated families. Four mutations in transient receptor potential vanilloid 4 targeted conserved arginine residues in the ankyrin repeat domain, which is believed to be important in protein–protein interactions. Striking phenotypic variability between and within families was observed. The majority of patients displayed a predominantly, or pure, motor neuropathy with axonal characteristics observed on electrophysiological testing. The age of onset varied widely, ranging from congenital to late adulthood onset. Various combinations of additional features were present in most patients including vocal fold paralysis, scapular weakness, contractures and hearing loss. We identified six asymptomatic mutation carriers, indicating reduced penetrance of the transient receptor potential vanilloid 4 defects. This finding is relatively unusual in the context of hereditary neuropathies and has important implications for diagnostic testing and genetic counselling.
Keywords: transient receptor potential vanilloid 4 gene, hereditary motor and sensory neuropathy type 2C, scapuloperoneal spinal muscular atrophy, congenital distal spinal muscular atrophy, skeletal dysplasia
Introduction
The long arm of human chromosome 12 harbours a region (12q21–q24) that is rich in disease-causing loci for neurological disorders (Klein et al., 2003). It contains the heat shock 22kDa protein 8 (HSPB8) gene linked to distal hereditary motor neuropathy type II (distal HMN II) (Irobi et al., 2004), the Ataxin 2 gene associated with spinocerebellar ataxia type 2 (Pulst et al., 1996), and loci for scapuloperoneal muscular dystrophy (Wilhelmsen et al., 1996) and hereditary spastic paraplegia (Schule et al., 2009). In addition, loci for three other dominantly inherited peripheral neuropathies have been reported in this region, namely hereditary motor and sensory neuropathy type 2C (HMSN2C), scapuloperoneal spinal muscular atrophy (SMA) and congenital distal SMA (Isozumi et al., 1996; van der Vleuten et al., 1998; Klein et al., 2003).
Patients with HMSN2C or Charcot–Marie–Tooth type 2C are clinically characterized by distal muscle weakness and wasting in the limbs, distal sensory loss, vocal fold paralysis and weakness of the diaphragm and intercostal muscles. The age of onset varies widely from early childhood to the third decade. Lifespan may be decreased due to respiratory complications (Dyck et al., 1994; Donaghy and Kennett, 1999; Santoro et al., 2002; McEntagart et al., 2005). Scapuloperoneal SMA was originally described in a large New England family (DeLong and Siddique, 1992). As the name implies, patients with scapuloperoneal SMA have no detectable involvement of sensory nerves. The distribution of scapuloperoneal muscle atrophy and weakness in patients with scapuloperoneal SMA is highly unusual within the disease spectrum of hereditary neuropathies. As in HMSN2C, patients affected with scapuloperoneal SMA often have vocal fold paralysis. Congenital distal SMA is a neurological condition with prenatal onset affecting the lower motor neurons. In a four-generation Dutch pedigree linked to the 12q23–q24 chromosomal region, the disease severity varied from congenital muscle weakness restricted to the distal lower limbs, to more severe phenotypes with weakness of pelvic girdle and trunk muscles with associated scoliosis; 15 affected members presented with arthrogryposis (Fleury and Hageman, 1985; van der Vleuten et al., 1998).
Three recent studies showed that mutations in the transient receptor potential vanilloid 4 gene (TRPV4) underlie these three clinically diverse hereditary neuropathies (HMSN2C, scapuloperoneal SMA and congenital distal SMA) (Auer-Grumbach et al., 2010; Deng et al., 2010; Landoure et al., 2010). Four different mutations in eight unrelated families were reported in these studies: Arg269His, Arg269Cys, Arg315Trp and Arg316Cys. All mutations except Arg269Cys were found to be recurrent in at least two unrelated families.
Mutations were found in previously reported families including an HMSN2C family of New Zealand descent (McEntagart et al., 2005) that carries the Arg315Trp mutation (Auer-Grumbach et al., 2010); a HMSN2C family from the USA (Dyck et al., 1994) that carries the Arg269Cys mutation as was independently shown by two studies (Deng et al., 2010; Landoure et al., 2010); a scapuloperoneal SMA family from the USA (DeLong and Siddique, 1992) that carries the Arg316Cys mutation (DeLong and Siddique, 1992; Deng et al., 2010); and the Dutch family with congenital distal SMA (van der Vleuten et al., 1998) that carries the Arg269His mutation (Auer-Grumbach et al., 2010).
TRPV4 contains 15 exons and encodes a non-selective cation channel modestly permeable to Ca2+ (Liedtke et al., 2000; Plant and Strotmann, 2007). TRPV4 was initially identified as a vertebrate osmosensor but can in fact be activated by a wide variety of stimuli including cell shearing, heat, endogenous agonists (e.g. endocannabinoid anandamide, arachidonic acid) and synthetic agonists like 4α-phorbol-12,13-didecanoate (4αPDD) (Liedtke et al., 2000; Nilius et al., 2003; Watanabe et al., 2003; Plant and Strotmann, 2007; Everaerts et al., 2009). TRPV4 shares structural features with other TRPV family members, including six putative transmembrane α-helices (TM) with a channel pore between TM5 and TM6 and intracellular domains at the N- and C- termini (Everaerts et al., 2009). Based on the recently determined crystal structure of the corresponding domain from the chicken orthologue (Landoure et al., 2010), TRPV4 contains an N-terminal ankyrin repeat domain (ARD) with six repeats. Such repeats have been found to be important for oligomerization, proper trafficking to the plasma membrane and interaction with other proteins (Erler et al., 2004; Hellwig et al., 2005; Arniges et al., 2006; Everaerts et al., 2009; Phelps et al., 2009). A proline-rich domain is located upstream of the ARD and has been shown to be involved in mechanosensation and interaction with protein kinase C and casein kinase substrate in neurons, proteins implicated in synaptic vesicular trafficking and regulation of endocytotic processes (Cuajungco et al., 2006; D'Hoedt et al., 2008). A putative calmodulin-binding domain at the C-terminus is involved in Ca2+-dependent activation of the channel. A DAPL motif formed by four amino acids at the C-terminal end of the sequence is similar to a PDZ-binding motif (PSD95/Dlg/ZO-1), and might be responsible for interaction with proteins containing PDZ-like domains (Everaerts et al., 2009).
Interestingly, TRPV4 was previously shown to be involved in human disease, as dominant mutations were reported to cause various skeletal dysplasia syndromes including brachyolmia (Rock et al., 2008), spondylometaphyseal dysplasia Kozlowski type and metatropic dysplasia (Krakow et al., 2009). The mutations causing these different skeletal dysplasia syndromes were shown to result in a gain of channel function (Rock et al., 2008; Krakow et al., 2009).
For the neuropathy-associated TRPV4 mutations there is less consensus regarding the underlying disease mechanism. Four mutations (Arg269Cys, Arg269His, Arg315Trp and Arg316Cys) were studied functionally in different cell systems (Auer-Grumbach et al., 2010; Deng et al., 2010; Landoure et al., 2010). Two studies showed that mutant TRPV4 causes a gain of channel function with increased calcium influx compared to wild-type protein, both under basal conditions and after stimulation (Deng et al., 2010; Landoure et al., 2010). In contrast, the third study postulated a loss-of-function mechanism (Auer-Grumbach et al., 2010).
In the current study we report one new and four previously known TRPV4 mutations. The associated phenotypic spectrum is described in eight families presenting with various forms of hereditary neuropathy. Detailed genotype–phenotype correlations giving insight into the complexity of TRPV4 neuropathies are presented.
Patients and methods
Patient cohort
To ascertain the phenotypic variability of TRPV4-related neuropathies a heterogeneous cohort was selected consisting of 145 unrelated index patients with various types of hereditary neuropathies. For a subgroup of 83 patients, criteria for inclusion were based on the unusual clinical characteristics of the phenotypes recently described in families with TRPV4 mutations (Auer-Grumbach et al., 2010; Deng et al., 2010; Landoure et al., 2010). Patients in this subgroup of 83 individuals were included if they were diagnosed with either hereditary motor sensory neuropathy (HMSN) or HMN with at least one of the following additional features: congenital onset (in the case of HMN diagnosis), scapular or other proximal weakness, contractures, vocal fold paralysis, diaphragmatic weakness, respiratory difficulty or pronounced scoliosis. In addition to the above-mentioned cohort of 83 patients, a second group of 62 patients with axonal forms of HMSN without specific additional features were also included.
Patients were referred from various European countries and the USA by neurologists who are well acquainted with rare neuromuscular disorders. All patients or their legal representatives signed an informed consent form prior to enrolment. The local Institutional Review Board approved this study.
Molecular genetic analysis
Genomic DNA from total blood samples obtained from patients with hereditary neuropathy and control persons was isolated using standard extraction protocols. The coding regions and exon–intron boundaries of TRPV4 were amplified by polymerase chain reaction (PCR) using primer oligonucleotides designed with Primer3 (Rozen and Skaletsky, 2000) (Supplementary Table 1, PCR conditions are available upon request). PCR products were purified with the exonuclease I-shrimp alkaline phosphatase enzyme (USB, Cleveland, USA). Mutation screening was performed by bidirectional sequencing using the BigDye® Terminator v3.1 Cycle Sequencing Kit (Applied Biosystems, Foster City, USA). Fragments were electrophoretically separated on an ABI3730xl DNA Analyser (Applied Biosystems, Foster City, USA). Sequence analysis was performed with the SeqMan™II (DNASTAR Inc., Madison, USA) program. The nucleotide numbering was based on the published online protein (NP_067638) and mRNA (NM_021625) sequence of TRPV4 (http://www.ncbi.nlm.nih.gov). For the description of the mutations we used the latest conventions of the Human Genome Variation Society nomenclature (http://www.hgvs.org/mutnomen). Sequence variants were confirmed by an independent PCR and sequencing of the original or new stock DNA samples. Segregation of the mutations with the disease phenotype was analysed in all families. For the Arg232Cys and Val620Ile mutations, 280 controls of European descent were screened.
Haplotype sharing and paternity testing
In order to investigate haplotype-sharing among the families carrying the Arg232Cys or Arg269Cys mutation and confirm the de novo character of the Val620Ile mutation, genotyping was performed using five highly informative short tandem repeat markers surrounding the TRPV4 gene (D12S105, D12S1583, D12S1645, D12S1343 and D12S1344). Short tandem repeats were PCR-amplified with fluorescently labelled primer pairs; sequences are available at http://www.ncbi.nlm.nih.gov. The PCR fragments were mixed with formamide and the GeneScanTM 500 Liz® Size Standard (Applied Biosystems, Foster City, USA) and subsequently size-separated on an ABI3730xl DNA Analyser. Genotypes were analysed using Local Genotype Viewer, an in-house developed software program (http://www.vibgeneticservicefacility.be/).
Paternity was tested using 15 highly informative short tandem repeats distributed throughout the genome (ATA38A05, D1S1646, D1S1653, D1S1360, D2S2256, D3S3037, D4S2382, D4S3240, D7S509, D8S1759, D9S1118, D12S1056, D12S2082, D16S2619 and GATA152H04). The short tandem repeat fragment analysis was processed with the same equipment and software.
Results
Genetic findings
Mutation screening in a large cohort of 145 unrelated patients with various types of hereditary neuropathies revealed eight families with five different heterozygous missense mutations in TRPV4 (Table 1 and Fig. 1) including the American ‘Family 1’ (F1) (Landoure et al., 2010). The other seven families were not previously reported to carry a TRPV4 mutation. Autosomal dominant segregation of the mutations was found in seven families; the remaining index patient (PN-1394.1) was sporadic and carried a de novo mutation (Fig. 2). Affected members in a UK family (CMT-455), a Swiss family (CMT-456) and one patient from a UK pedigree (CMT-1100) carried a novel sequence variation in exon 4 (c.694C>T) resulting in an Arg232Cys transition in the TRPV4 protein. The Arg269Cys (c.805C>T) mutation in exon 5 was present in the previously reported American family (F1) (Landoure et al., 2010) and in a new Spanish family (CMT-858). Three other previously identified mutations were found: Arg269His (exon 5) in an Italian kindred (CMT-165) and Arg315Trp (exon 6) in a third UK family (CMT-149) (Auer-Grumbach et al., 2010; Deng et al., 2010; Landoure et al., 2010). Finally the Val620Ile (c.1958G>A) mutation in exon 12, which was previously reported to cause autosomal dominant brachyolmia (Rock et al., 2008), was identified in an isolated Croatian patient (PN-1394.1). The Arg232Cys and Val620Ile mutations were absent from 280 control individuals of European descent.
Table 1.
Families with TRPV4 mutations identified in this study
| Mutation | Amino acid change | Exon | Known phenotypes | Familya | Country of origin | Familial history | Number affected | Additional remarks |
|---|---|---|---|---|---|---|---|---|
| c.694C>T | Arg232Cys | 4 | HMN with vocal fold paralysis, SPSMA, HMSN2 | CMT-455 | UK | AD | 3 | One unaffected mutation carrier (CMT-455), new mutation. CMT-455 and CMT-1100 share the same haplotype (Table 2) |
| CMT-456 | Switzerland | AD | 4 | |||||
| CMT-1100 | UK | AD | 2 | |||||
| c.805C>T | Arg269Cys | 5 | HMSN2C, SPSMA, congenital distal SMA | CMT-858 | Spain | AD | 2 | Three unaffected mutation carriers. |
| F1 | USA | AD | 7 | Two unaffected mutations carriers. | ||||
| c.806G>A | Arg269His | 5 | HMSN2C, SPSMA, congenital distal SMA | CMT-165 | Italy | AD | 3 | |
| c.943C>T | Arg315Trp | 6 | HMSN2C, SPSMA, congenital distal SMA | CMT-149 | UK | AD | 5 | |
| c.1858G>A | Val620Ile | 12 | HMSN2, autosomal dominant brachyolmia | PN-1394 | Croatia | IC | 1 |
AD = autosomal dominant; IC = isolated case; SPSMA = scapuloperoneal spinal muscular atrophy.
a: This study.
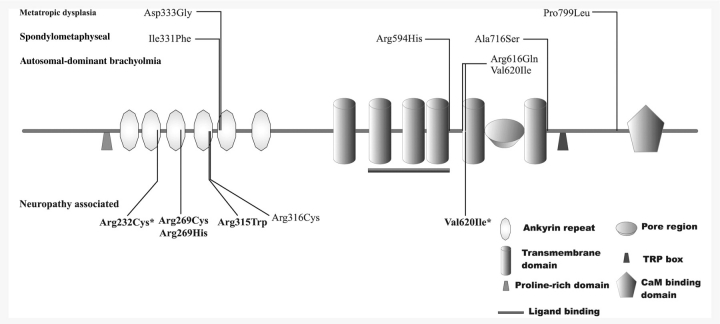
Figure 1.
Location of mutations in the different domains of TRPV4 protein. Neuropathy causing mutations are indicated as well as previously described mutations for autosomal-dominant brachyolmia, spondylometaphyseal dysplasia (SMDK), Kozlowski type and metatropic dysplasia. Mutations identified in this study are in bold. The new neuropathy associated mutations are indicated by asterisks.
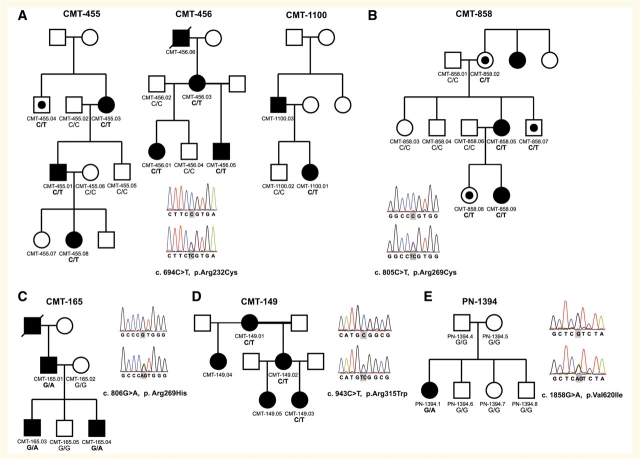
Figure 2.
Pedigrees of families with TRPV4 mutations. Segregation analysis and sequence trace files is shown for seven families, the pedigree of family F1 is shown elsewhere (Landoure et al., 2010). (A) Families CMT-455, CMT-456 and CMT-1100 carrying the Arg232Cys mutation. (B) Family CMT-858 with the Arg269Cys mutation. (C) Family CMT-165 with the Arg269His mutation. (D) Family CMT-149 with the Arg315Trp mutation. (E) Family PN-1394 with the Val620Ile mutation. Square = male; circle = female; black filled symbol = affected; empty symbol = unaffected; empty symbol with black dot = unaffected mutation carrier. Genotype is indicated under each individual from whom the DNA was available for testing.
Segregation analysis was performed in all families and TRPV4 mutations were present in all available affected individuals (Fig. 2). Genetic testing revealed three asymptomatic carriers of the Arg269Cys mutation in pedigree CMT-858. These individuals (CMT-858.02, CMT-858.07 and CMT-858.08) were clinically unaffected at the age of 79, 36 and 6 years, respectively. Furthermore, two unaffected members from the F1 family (II.4 and IV.6 in the original paper) also carried the Arg269Cys mutation (Landoure et al., 2010). In family CMT-455 one individual (CMT-455.04) carrying the Arg232Cys mutation was clinically unaffected at the age of 69 years.
Additional short tandem repeat marker and single nucleotide polymorphism analysis for the recurrent Arg232Cys mutation (families CMT-455, CMT-456 and CMT-1100) and Arg269Cys mutation (CMT-858 and F1) showed that the Arg232Cys mutation in families CMT-455 and CMT-1100 resides on a common haplotype. The other families do not share haplotypes (Table 2).
Table 2.
Haplotype analysis of 12q markers in patients with Arg232Cys and Arg269Cys mutations in TRPV4
|
Arg232Cys |
Arg269Cys |
||||
|---|---|---|---|---|---|
| Patient Marker | CMT-455.01 | CMT-456.01 | CMT-1100.01 | CMT-858.09 | F1.IV.4 |
| D12S105 | 143 | 147 | 145 | 145 | 143 |
| D12S1583 | 237 | 225 | 237 | 221 | 239 |
| D121645 | 212 | 216 | 212 | 218 | 212 |
| rs3742032 (T/C) | C | T | C | C | T |
| rs3825394 (A/C) | C | A | C | C | A |
| D12S1343 | 206 | 206 | 206 | 206 | 208 |
| D12S1344 | 239 | 235 | 239 | 239 | 227 |
The alleles of the short tandem repeats are sized in base pairs. The position of the markers is according to the reference assembly of NCBI genome build 36.3.
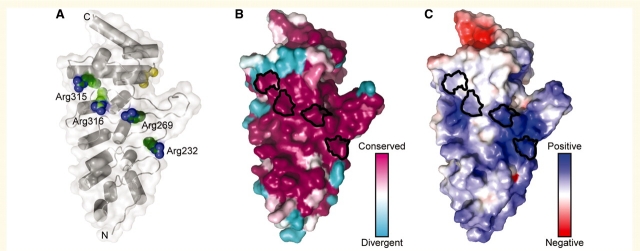
Four of the five mutations identified in this study target conserved residues in the ARD of TRPV4 based on the crystal structure of ARD of the TRPV4 chicken orthologue (Landoure et al., 2010). The mutant residues Arg232, Arg269 and Arg315, and previously identified Arg316 (Auer-Grumbach et al., 2010; Deng et al., 2010) are situated on the convex surface of ARD in the loops of finger 2, 3 and 4, respectively (Fig. 3A). Mapping of the sequence conservation among 27 TRPV4 orthologues on the molecular surface demonstrate that the convex face of the ARD is very highly conserved (Fig. 3B). The solvent-accessible electrostatic surface properties show that the convex surface is also highly positively charged (Fig. 3C).
Figure 3.
The four mutations at arginine residues in the TRPV4 ARD localize to the same conserved, positively charged protein surface. (A) A ribbon representation of the structure of the TRPV4 ARD from chicken (Landoure et al., 2010), with a transparent molecular surface. The side chains of Arg232, Arg269 and Arg315 (Arg218, Arg255 and Arg301, respectively, in chicken) are shown in green ‘van der Waals’ sphere representation, and the previously identified Arg316 (Arg302 in chicken) (Deng et al., 2010) is shown in light green. The backbone positions of the skeletal dysplasia mutations at Ile331 and Asp333 (Krakow et al., 2009) are shown as yellow spheres for reference. (B) The sequence conservation in TRPV4, using an alignment of 27 TRPV4 orthologues, is mapped onto the surface of the structure. Note that Arg232, Arg269, Arg315 and Arg316 are strictly conserved as arginine residues in available TRPV4 orthologues. (C) The solvent-accessible electrostatic properties of the protein are mapped onto the molecular surface, with blue representing positively charged surfaces (+5 kT) and red, negatively charged surfaces (–5 kT). In (B) and (C) the surface regions corresponding to Arg232, Arg269, Arg315 and Arg316 are outlined in black.
Clinical findings
The first subgroup of the screening cohort consisted of 83 patients presenting with various hereditary neuropathies with at least one of the additional features as described above. For 15 patients of this subgroup, a formal diagnosis of HMN was made; HMSN1 for 26 and HMSN2 for 16. For the remaining 26 patients of the first group of 83, no detailed electrophysiological information was available so no clear distinction between HMN, HMSN1 and HMSN2 could be made. Disease onset ranged widely from childhood through adulthood; nine HMN patients had a congenital onset. Scapular or other proximal upper limb weakness was encountered in eight patients and contractures were present in 17 patients. In this cohort 14 patients were diagnosed with vocal fold paralysis, five with diaphragmatic paralysis and 36 with scoliosis. The second subgroup of the screening cohort consisted of 62 patients with a diagnosis of HMSN2 without additional features.
The detailed clinical and electrophysiological findings in the eight families are shown in Tables 3 and 4. Data from 27 patients were included; 23 had genetically confirmed TRPV4 mutations, the remaining 4 were affected by history but DNA for molecular testing was not available. Clinical findings and linkage data in family CMT-456 were reported earlier (Boltshauser et al., 1989; McEntagart et al., 2002).
Table 3.
Clinical characteristics of patients with proven TRPV4 mutations
| Patient | Age at onset | Age at last examination | Symptoms at onset | Weakness lower limbs | Weakness upper limbs | Weakness | Vocal fold paresis | Scoliosis | Contractures | Sensory involvement | Additional features | Diagnosis | ||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| (years) | Distal | Proximal | Distal | Proximal | Other | |||||||||
| CMT-455.01 | 14 y | 33 | Stridor | + | − | − | − | Left diaphragmatic paralysis | + | − | − | − | Respiratory insufficiency, pes cavus | Distal HMN with vocal fold paresis |
| CMT-456.01 | 6 m | 30 | Stridor | + | + | + | − | Scapular winging | + Unilateral L | + | − | − | Sensorineural hearing loss, arythenoidectomy L at 10 y | Scapuloperoneal SMA |
| CMT-456.03 | Childh | 52 | Weakness hands | + | + | + | − | − | + Unilateral L, asymptomatic | − | − | − | Sensorineural hearing loss, loss of myelinated fibres on sural nerve biopsy | Distal HMN with vocal fold paresis |
| CMT-456.05 | Childh | 36 | Distal weakness upper/lower limbs | + | − | + | − | − | + Unilateral, dysphonia | − | − | − | Sensorineural hearing loss | Distal HMN with vocal fold paresis |
| CMT-456.06 | Adol | 65 | Weakness hands | + | − | + | − | − | + 40 y, unilateral L | − | − | − | Bilateral hearing aids at 40 y | Distal HMN with vocal fold paresis |
| CMT-1100.01 | 14 y | 27 | Scoliosis | + (4) | − | + (4) | − | − | − | + | − | + Distal↓ vibration sense | − | HMSN2 |
| CMT-1100.03 | 11 y | 43 | Tripping with feet | + | + (4) | + | + (4) | Truncal | − | − | − | + Distal UL/LL | Wasting shoulders and mid thigh, pes cavus, restless legs syndrome | HMSN2 |
| CMT-858.05 | Childh | 39 | Scapular winging | + (2) | − | + (3) | − | Scapular winging, mild facial weakness | + Asymptomatic | − | − | + Distal↓ vibration sense | Pes cavus, hammertoes | Scapuloperoneal SMA |
| CMT-858.09 | Cong | 6 | Arthrogryposis lower limbs | + (2) | + (2) | + (3) | + (2) | Shoulder amyotrophy | + 1 y, unilateral L | + | Arthrogryposis lower limbs | − | Respiratory insufficiency, tracheostomy, bladder incontinence | Congenital distal SMA |
| F1 III.2 | 44 y | 71 | Distal weakness lower limbs | + (3, 4) | − | + (4) | − | − | + | − | − | + Minimal | Sensorineural hearing loss, bladder urgency | HMSN2C |
| F1 IV2 | 5 y | 48 | Distal weakness lower limbs | + (1) | + (4) | + (3) | + (4) | − | + Asymmetric | NA | − | + Mild | Pes cavus, bladder incontinence, CS | HMSN2C |
| F1 IV3 | 5 y | 46 | Stridor | + (2) | + (4) | + (3) | + (4) | Neck flexor (4) | + Asymmetric | NA | − | + Mild | Mild dysphagia, postural tremor, bladder urgency and incontinence, mild pes cavus, CS | HMSN2C/distal HMN |
| F1 IV4 | 3 y | 44 | Distal weakness lower limbs | + (0) | + (1) | + (0) | + (0) | Neck, truncal, diaphragm, tongue muscles, facial | + With dysphagia | + (9 y) | + (Elbow, fingers, wrists, knees, hips) | + Moderate | Sensorineural hearing loss, bladder incontinence, CS | HMSN2C |
| F1 V1 | 7 y | 24 | Distal weakness lower limbs | + (4) | − | + (4) | − | Neck flexor (4) | + (Intermittent hoarseness) | − | − | + Mild | Pes cavus, hammertoes | HMSN2C |
| F1 V3 | 5 y | 20 | Stridor | + (4) | − | + (4/5–) | − | Neck flexor (4) | + | − | − | + Mild | Bladder urgency, pes cavus, hammertoes, CS | HMSN2C |
| F1 V8 | 2 y | 18 | Stridor | + (4) | − | − | − | − | + | + Mild | − | + Minimal | Pes cavus | HMSN2C/HMN |
| CMT-165.01 | Childh | 52 | Distal weakness lower limbs | + | + | + (mild) | − | Scapular winging SCM, trapezius, | − | − | − | − | − | Scapuloperoneal SMA |
| CMT-165.03 | Cong | 27 | Club feet | + (1) | + (3) | − | − | SCM, trapezius | − | − | Talipes equinovarus, knees | − | Mild lumbar hyperlordosis, muscle hypertrophy UL plus deltoids and pectoralis, finger tremor | Congenital distal SMA |
| CMT-165.04 | 8 y | 10 | Distal weakness lower limbs | + (1, 2) | − | − | − | SCM, trapezius, neck flexors 10 y | − | − | Ankles | − | − | Scapuloperoneal SMA |
| CMT-149.01 | >20 y | 51 | Scoliosis | + | − | − | Scapular winging R, neck flexors | + | + (Thoracic) | − | − | Facial asymmetry | Scapuloperoneal SMA | |
| CMT-149.02 | Cong | 28 | Club feet | + (0) | + | + | − | Scapular winging, neck flexors | NA | + (Lumbar) | Talipes equinovarus | − | Facial asymmetry, tongue fasciculations, dorsal hyperlordosis | Congenital distal SMA |
| CMT-149.03 | Cong | 11 | Club feet | + (L>R) | + | − | − | Scapular winging, neck flexors, | − | − | Talipes equinovarus, knee L | − | Congenital distal SMA | |
| CMT-149.04 | Child | 12 | Pain lower limbs | + | − | − | − | Scapular winging (mild) | − | − | − | − | Scapuloperoneal SMA | |
| CMT-149.05 | Cong | 4 | Club feet, stridor | + | − | − | − | Scapular winging | + (Bilateral) | − | Talipes equinovarus | − | Gastrostomy | Congenital distal SMA |
| PN-1394.1 | 6 y | 15 | Distal weakness lower limbs | + | − | − | − | − | − | + | Ankles and knees | − | Short stature | HMSN2 |
+ = present; – = absent; y = year; m = month; childh = childhood; cong = congenital; adol = adolescence; L = left, R = right; SCM = sternocleidomastoideus muscle; NA = information not available; CS = cold sensitivity with worsening of weakness in hands; UL = upper limbs; LL = lower limbs.
Table 4.
Nerve conduction studies in patients with proven TRPV4 mutation
| Patient | Age (years) |
Median motor |
Ulnar motor |
Peroneal motor |
Tibial motor |
Median sensory |
Ulnar sensory |
Sural sensory |
|||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Normal values | Amp | CV | Amp | CV | Amp | CV | Amp | CV | Amp | CV | Amp | CV | Amp | CV | |
| 4.0 | 49.0 | 4.0 | 49.0 | 3.0 | 41.0 | 3.0 | 41.0 | 7.0 | 46.0 | 2.0 | 47.0 | 1.0 | 44.0 | ||
| CMT-455.01 | 33 | − | − | 7.6 | 55.0 | − | − | 4.2 | 49.0 | 9.4 | N | 10.3 | N | 11.0 | N |
| CMT-455.08 | 10 | − | − | − | − | − | − | 0.9 | 39.7 | − | − | − | − | 12.8 | N |
| CMT-456.01 | 13 | 7.0 | 50.0 | − | − | − | − | 12.0 | 45.0 | 10.0 | 55.0 | − | − | − | − |
| CMT-456.03 | 35 | 13.0 | 61.0 | − | − | − | 52.0 | 10.0 | 49.0 | 10.0 | 52.0 | 10.0 | 49.0 | 8.0 | 54.0 |
| CMT-456.05 | 33 | 5.3 | 54.0 | − | − | 1.6 | 49.0 | − | − | − | − | − | − | 1.6 | 45.0 |
| CMT-1100.01 | 23 | 7.2 | 57.0 | 4.2 | 65.0 | 1.6 | 55.0 | 3.9 | − | 7.0 | 54.0 | 5.0 | 58.5 | 5.0 | 50.0 |
| CMT-1100.03 | 42 | – | 60.0 | – | 66.0 | 0.4 | − | – | − | A | − | − | − | A | – |
| CMT-858.05 | 40 | 3.8 | 52.9 | 3.6 | 51.4 | 0.9 | 53.7 | 0.5 | 52.3 | 8.4 | 56.9 | − | − | 18.1 | 56.3 |
| CMT-858.09 | 4 | 4.6 | 49.1 | 1.6 | 52.4 | 0.4 | 48.8 | 0.4 | 44.7 | 9.0 | 47.8 | − | − | 6.5 | 48.1 |
| F1 III2 | 71 | 4.9 | 57.0 | 7.0 | 51 | 2.1 | 46.0 | 4.5 | 41.0 | 13.0 | 36.0 | 18.0 | 46.0 | − | – |
| F1 IV3 | 45 | 0.4 | 50.0 | A | A | A | A | 1.4 | 40.0 | 5.0 | 56.0 | 3.0 | 52.0 | 9.0 | 41.0 |
| 27 | 3.4 | 53.6 | 1.8 | 62.5 | 0.3 | 51.6 | − | − | 10.0 | 60.0 | 5.0 | 52.3 | 9.0 | 46.1 | |
| F1 IV8 | 19 | 12.4 | 56.0 | − | − | 4.1 | 40.0 | 6.5 | 45.0 | 20.0 | 50.0 | − | − | 13.0 | 41.0 |
| CMT-165.03 | 22 | − | − | − | − | 0.6 | 45.0 | − | − | − | − | − | − | 23.0 | 47.0 |
| CMT-165.04 | 8 | 1.7 | 52.0 | − | − | − | − | − | − | − | − | − | − | − | – |
| CMT-149.01 | 47 | 3.0 | 59.0 | − | − | − | − | 5.2 | 50.7 | N | N | N | N | N | N |
| CMT-149.02 | 29 | 7.0 | 51.0 | − | − | − | − | − | − | 4.5 | N | 3.2 | N | ||
| CMT-149.03 | 1 | − | 53.3 | − | − | − | − | − | − | − | − | − | − | − | – |
| CMT-149.04 | 12 | − | − | − | − | − | − | 11.9 | − | − | − | − | − | 6.9 | N |
| PN-1394.1 | 16 | 8.0 | 55.7 | N | N | 0.05 | 33.3 | − | − | 10.0 | 50.0 | N | N | A | A |
A = absent response; Age = age at examination; Amp = amplitude (motor: in mV; sensory: in µV); CV = conduction velocity (in m/s); - = not measured; N = normal. Bold indicates abnormal values.
Detailed laryngoscopy assessment of vocal fold function was performed in the F1 family showing that the vocal fold involvement was often asymmetric (Table 5). A video fragment from the laryngoscopic evaluation of vocal fold dysfunction in patient F1 III.2 is provided in the Supplementary material.
Table 5.
Laryngoscopic findings in family F1
| Patient | Dyspnoea | Aspiration | Dysphonia | Vocal fold adduction |
Vocal fold abduction |
Comments | ||
|---|---|---|---|---|---|---|---|---|
| Left | Right | Left | Right | |||||
| F1 III2 | − | + | − | 1 | 1 | 1 | 1 | Raspy voice |
| F1 IV3 | + | + | + | 2 | 1 | 2 | 1 | High-pitched voice |
| F1 V8 | + | − | + | 2 | 2 | 2 | 1 | Husky voice, arytenoidectomy at age 2 years |
+ = present; – = absent. Vocal fold movement: 0 = normal; 1 = impaired mobility; 2 = immobile.
The clinical phenotype of the patients described in the current study is highly variable both between and within families. The majority of patients seem to fall in the category of pure or predominantly motor nerve disorders. Nerve conduction studies showed an axonal neuropathy with preserved or only slightly attenuated nerve conduction velocities in all studied patients (Table 4).
Of special interest is the isolated Croatian patient PN-1394.1 who developed symptoms of a predominantly motor neuropathy in early childhood. Nerve conduction studies were compatible with an axonal neuropathy and concentric needle EMG showed chronic neurogenic changes in distal muscles (Tables 3 and 4). Because scoliosis and short stature in this patient might resemble a brachyolmia phenotype, additional radiographic studies were performed. A right convex kyphoscoliosis with flattened vertebrae in the mid-thoracic segment was found and the necks of both femurs were shortened, wide and slightly irregular. There was no brachydactyly or delay of the carpal bone ossification. Genetic testing for other more common causes of hereditary neuropathy (CMT1A duplication and point mutations in PMP22, MPZ, GJB1 and SH3TC2) was unremarkable in this patient.
Discussion
In this study we report clinical and genetic findings in eight unrelated families with hereditary neuropathies caused by TRPV4 mutations identified during mutation screening of a heterogeneous cohort of 145 unrelated index patients. The F1 family was already reported to carry a mutation in TRPV4 but is described in detail here (Landoure et al., 2010). In the current literature there are at least two more families that may link to the 12q-locus, however they were not yet reported to carry a TRPV4 mutation. One is of UK origin (Donaghy and Kennett, 1999; McEntagart et al., 2005); the second is of Italian descent (Santoro et al., 2002). Five different heterozygous mutations were identified in the current study, of which four (Arg269Cys, Arg269His, Arg315Trp and Val620Ile) were previously reported in other families (Rock et al., 2008; Auer-Grumbach et al., 2010; Deng et al., 2010; Landoure et al., 2010) (Table 1). The novel Arg232Cys mutation was found in three families who were unrelated by history. Two of these (CMT-455 and CMT-1100) are probably distantly related since they share the same disease haplotype. The third family with the Arg232Cys mutation does not share this haplotype. No common haplotype could be found in pedigrees CMT-858 and F1, both carrying the Arg269Cys mutation (Table 2). Thus, all mutations in this study are recurrent in at least two families pointing to the presence of mutation hotspots in exons 4, 5, 6 and 12 of TRPV4 (Rock et al., 2008; Auer-Grumbach et al., 2010; Deng et al., 2010; Landoure et al., 2010). In addition, the recurrent Arg594His mutation was described in spondylometaphyseal dysplasia Kozlowski type. This points to another mutational hotspot in exon 11 (Krakow et al., 2009).
Reduced penetrance was observed in six asymptomatic mutation carriers, for the Arg232Cys mutation in family CMT-455 and for the Arg269Cys mutation in families CMT-858 and F1 (Landoure et al., 2010) (Fig. 2). It was also reported previously for the Arg315Trp mutation (Auer-Grumbach et al., 2010). Incomplete penetrance is a relatively uncommon event in the context of hereditary peripheral neuropathies, although it has been observed before for glycyl-tRNA synthetase (GARS) (Sivakumar et al., 2005), myelin protein zero (MPZ) (De Jonghe et al., 1999) and Berardinelli-Seip congenital lipodystrophy 2 (BSCL2) (Auer-Grumbach et al., 2005). In TRPV4-associated neuropathy, however, reduced penetrance seems to be a relatively common feature that is not mutation-specific.
In accordance with previous descriptions, further phenotypic subdivision could be made: congenital distal SMA with contractures, scapuloperoneal SMA, HMSN2C (Auer-Grumbach et al., 2010; Deng et al., 2010; Landoure et al., 2010), but also HMN with vocal fold paralysis and ‘generic’ HMSN2 (Table 3). Taking the previously described mutations and phenotypes into account and the fact that different phenotypes can arise even within one family, no clear correlations can be made between the various TRPV4 mutations and the associated phenotypes (Table 1). Although the separate disease entities of TRPV4-associated neuropathies could still serve a purpose from a semiological point of view, they are actually elements of a neuropathy disease spectrum that is exceptionally broad.
Mutations in TRPV4 were mainly identified in complex phenotypes. Index patients from seven out of our eight families presented with neuropathies with additional features, as opposed to one index (family CMT-1100), who was diagnosed with HMSN2 without clear additional features. The mutation frequency can therefore be estimated at 8.4% in the subgroup of the complex neuropathies (7 out of 83) and only 1.6% in the subgroup of the HMSN2 neuropathies without additional features (1 out of 62). The unifying feature however of all identified neuropathy patients with TRPV4 mutations is the axonal electrophysiology. This is further underscored by the fact that our screening cohort also contained 26 index patients with an electrophysiological diagnosis of demyelinating neuropathy (HMSN1), none of which was found to have a TRPV4 mutation.
Of special importance for the prognosis of patients is the frequently observed vocal fold involvement. Nearly all families that have been reported to date with TRPV4 mutations contained patients with vocal fold dysfunction (Auer-Grumbach et al., 2010; Deng et al., 2010; Landoure et al., 2010). In five out of eight families in our series, vocal fold dysfunction was observed, often unilateral or asymmetric with the left more affected than the right vocal fold (families F1, CMT-456 and CMT-858) and ranging in severity from asymptomatic in patients CMT-456.03 and CMT-858.05 to clear respiratory insufficiency requiring tracheostomy in patient CMT-858.09 (Tables 3 and 5 and Supplementary video fragment). Some patients underwent surgical procedures of the vocal folds (families F1 and CMT-456). Vocal fold involvement is not a typical feature of hereditary neuropathy in general, but it has occasionally been associated with recessive ganglioside-induced differentiation-associated protein 1 (GDAP1) mutations (Sevilla et al., 2003; Stojkovic et al., 2004), dominant early growth response 2 (EGR2) mutation (Pareyson et al., 2000), dynactin 1 (DCTN1) mutation (Puls et al., 2003, 2005), distal HMN type VII linked to chromosome 2q14 (McEntagart et al., 2001) and a few patients with CMT1A duplication (Thomas et al., 1997). In our screening cohort, 5 out of the 14 patients who initially presented with vocal fold paralysis were shown to have a TRPV4 mutation (36%). This indicates that TRPV4 is likely to be a major gene for hereditary neuropathies with vocal fold paralysis. Why the recurrent laryngeal nerve innervating the vocal folds is so vulnerable for the effects of TRPV4 mutations remains unclear at this point. However, the predominant involvement of the left vocal fold could result from length dependency since the left recurrent laryngeal nerve descends around the aortic arch before turning to go up to the larynx, making it much longer than its counterpart on the right.
The additional feature of bladder urgency and urinary incontinence was observed in members of family F1 and in patient CMT-858.09. This finding is more commonly seen in the context of spinal cord disorders and autonomic neuropathies, but is highly unusual in the context of hereditary (non-autonomic) neuropathies. Therefore, more patient observations and systematic bladder function studies are needed in order to attribute this feature to the TRPV4 disease spectrum. No other autonomic disturbances were noted in any of the patients.
In the context of the broad phenotypic variability of TRPV4 mutations, special interest goes to patient PN-1394.1 carrying the de novo Val620Ile mutation, which was previously shown to cause autosomal dominant brachyolmia (Rock et al., 2008). None of the TRPV4-associated skeletal dysplasia syndromes are known to feature peripheral neuropathy or other neurological involvement. The skeletal abnormalities in patient PN-1394.1 were obvious but too limited to make a formal diagnosis of a skeletal dysplasia. Particularly the abnormalities of the spine could also be secondary to the longstanding neuropathy as was previously suggested (Auer-Grumbach et al., 2010). None of the more common neuropathy genes were mutated in this individual, making the incidental co-occurrence of a mutation in another neuropathy-associated gene unlikely. Taking the overall variability of TRPV4-associated disorders into account, patient PN-1394.1 may represent an overlap syndrome between skeletal dysplasia and neuropathy. Skeletal abnormalities such as congenital hip dysplasia, scoliosis, small hands and limb shortening have been observed in the scapuloperoneal SMA family with the Arg316Cys mutation (DeLong and Siddique, 1992; Deng et al., 2010). The authors already suggested a TRPV4 disease spectrum encompassing both peripheral neuropathy and skeletal dysplasia (Deng et al., 2010). Our patient PN-1394.1 might be a first confirmation of this intriguing hypothesis.
All known neuropathy-causing TRPV4 mutations (except Val620Ile) are surface mutations not expected to affect protein folding. They cluster on the highly positively charged convex surface of the ARD and target arginine residues that are strictly conserved throughout 27 available TRPV4 orthologues, suggesting their importance in TRPV4 function (Auer-Grumbach et al., 2010; Deng et al., 2010; Landoure et al., 2010) (Table 1 and Fig. 3B). These mutations are located in three consecutive finger loops of the protein, Arg232Cys in finger 2, Arg269Cys/Arg269His in finger 3 and Arg315Trp/Arg316Cys in finger 4 (Fig. 3A–C). In contrast, the bone dysplasia mutations (Ile331Phe and Asp333Gly) (Krakow et al., 2009) are situated on the opposing concave side (Fig. 3A). This concave surface of ankyrin repeats is commonly used in protein–protein interactions, whereas few ankyrin-repeat-containing proteins have ligands known to bind to the convex surface (Gaudet, 2008).
TRPV4 mutations causing skeletal dysplasias probably act through a gain of function mechanism (Rock et al., 2008; Krakow et al., 2009). For the neuropathy-causing mutations however, discrepancies exist in the current reports. In one study, three TRPV4 mutations (Arg269His, Arg315Trp and Arg316Cys) influenced proper localization of the ion channel to the plasma membrane (Auer-Grumbach et al., 2010) with the formation of cytoplasmic aggregates. Mutant TRPV4 was shown to cause loss of normal channel function (Auer-Grumbach et al., 2010). The results from two other studies differed substantially (Deng et al., 2010; Landoure et al., 2010); both showed increased intracellular calcium levels caused by abnormal activity of the TRPV4 ion channel in the presence of either the Arg269His, Arg269Cys or Arg316Cys mutation. The use of various cell systems in the above-mentioned studies may underlie the differences in results (Nilius and Owsianik, 2010). Nevertheless, it remains uncertain whether changes in TRPV4 channel function alone are causing the peripheral neuropathy. Further studies are definitely needed to shed light on the disease mechanism.
Since the majority of neuropathy-causing TRPV4 mutations cluster on one face of the ARD, disturbances in protein–protein interactions specific to nervous system form an interesting pathophysiological hypothesis; however, this has not been proven so far (Landoure et al., 2010). The only mutation outside of the ARD in this study is the de novo Val620Ile mutation in patient PN-1394.1, which may argue against this hypothesis. Alternatively, it may only imply that this mutation works through a different disease mechanism. Although the neuropathy-associated mutations seem to cluster in well-defined residues of the ARD, the skeletal dysplasia mutations are more spread out over the protein including two in the ARD, Asp333Gly and Ile331Phe (Krakow et al., 2009). This means that an absolute distinction between the two groups of phenotypes cannot be made based on the position of the mutation in the primary structure of the protein alone. The skeletal abnormalities in the original scapuloperoneal SMA family (Deng et al., 2010) with the Arg316Cys mutation and patient PN-1394.1 with the Val620Ile mutation seem to strengthen this point further.
A parallel could be made with dominant mutations in dynamin 2 (DNM2) causing an intermediate form of HMSN and centronuclear myopathy. Overall, mutations causing one of the two phenotypes cluster in different domains of the protein but the distinction is not absolute (Claeys et al., 2009). Likewise, the majority of lamin A/C (LMNA) mutations causing one of the many laminopathies cluster together in certain domains of the protein; however, some mutations have been reported to cause distinct phenotypes in different patients (Rankin and Ellard, 2006). Given the substantial phenotypic variability of TRPV4-related disorders, additional modulating factors, both genetic and environmental, may be at play (Auer-Grumbach et al., 2010; Deng et al., 2010; Landoure et al., 2010).
In addition to the substantial phenotypic heterogeneity of TRPV4-associated neuropathy, genetic heterogeneity in pedigrees with similar phenotypes has also been reported (Landoure et al., 2010). In a second family with congenital distal SMA, linkage to the 12q23–q24 locus was excluded (van der Vleuten et al., 1998). A distal HMN type VII with vocal fold paresis was suggested to be allelic with HMSN2C, however the disease-causing locus was mapped to chromosome 2q14 (McEntagart et al., 2001).
In this study we enlarge the genetic spectrum of TRPV4-related disorders and report considerable phenotypic variability of hereditary neuropathies caused by TRPV4 mutations. Nearly all patients in our series have one or more features that are rather unusual for the most commonly encountered hereditary neuropathies. Conversely, screening of 62 HMSN2 phenotypes revealed only one family with a TRPV4 mutation (CMT-1100). Therefore we propose to direct diagnostic screening of TRPV4 towards patients presenting with either pure motor, or motor and sensory neuropathies, with clear axonal electrophysiology and at least one of the following additional clinical features: vocal fold paralysis, proximal weakness in the upper limbs, pronounced scoliosis or contractures. While performing mutation analysis of TRPV4, the extensive phenotypic variability and reduced penetrance should be taken into account, especially in the context of genetic counselling.
In order to shed more light on the underlying pathomechanism through which TRPV4 mutations work, further research into the extent of the associated disease spectrum is warranted. This could include the study of the contribution of TRPV4 in patients with distal HMN without additional features or patients with milder skeletal abnormalities in the absence of neuropathy (e.g. idiopathic scoliosis). Also the degree of phenotypic overlap between skeletal dysplasia and peripheral neuropathy could be explored further by means of systematic nerve conduction exams in TRPV4 skeletal dysplasia patients, a study that has not yet been performed to our knowledge.
Funding
University of Antwerp, the Fund for Scientific Research (FWO-Flanders); Medical Foundation Queen Elisabeth (GSKE);‘Association Belge contre les Maladies Neuromusculaires’ (ABMM);Interuniversity Attraction Poles P6/43 program of the Belgian Federal Science Policy Office (BELSPO); ‘Methusalem excellence grant’ of the Flemish Government; Austrian Science Fond (FWF; P19455-B05); McKnight Scholar Award and NIH grant (RG; R01GM081340); PhD fellowships of the FWO-Flanders to M.Z. and J.B.; Medical Research Council (MRC) and the Muscular Dystrophy Campaign support to M.M.R. and H.H. The work of M.M.R. and H.H. was undertaken at University College London Hospitals/University College London, which received a proportion of funding from the Department of Health's National Institute for Health Research Biomedical Research Centres funding scheme; intramural research funds from NINDS.
Supplementary material
Supplementary material is available at Brain online.
Supplementary Material
Acknowledgements
The authors are grateful to the patients and their families for their willingness to cooperate in this research project. The authors also wish to thank the Genetic Service Facility (VIB) for the sequencing support (http://www.vibgeneticservicefacility.be/) and Dr Robert Kleta for support and encouragement.
Glossary
Abbreviations
- ARD
ankyrin repeat domain
- HMN
hereditary motor neuropathy
- HMSN
hereditary motor and sensory neuropathy
- PCR
polymerase chain reaction
- SMA
spinal muscular atrophy
- TRPV4
transient receptor potential vanilloid 4 gene
References
- Arniges M, Fernandez-Fernandez JM, Albrecht N, Schaefer M, Valverde MA. Human TRPV4 channel splice variants revealed a key role of ankyrin domains in multimerization and trafficking. J Biol Chem. 2006;281:1580–6. doi: 10.1074/jbc.M511456200. [DOI] [PubMed] [Google Scholar]
- Auer-Grumbach M, Schlotter-Weigel B, Lochmuller H, Strobl-Wildemann G, Auer-Grumbach P, Fischer R, et al. Phenotypes of the N88S Berardinelli-Seip congenital lipodystrophy 2 mutation. Ann Neurol. 2005;57:415–24. doi: 10.1002/ana.20410. [DOI] [PubMed] [Google Scholar]
- Auer-Grumbach M, Olschewski A, Papic L, Kremer H, McEntagart ME, Uhrig S, et al. Alterations in the ankyrin domain of TRPV4 cause congenital distal SMA, scapuloperoneal SMA and HMSN2C. Nat Genet. 2010;42:160–4. doi: 10.1038/ng.508. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Boltshauser E, Lang W, Spillmann T, Hof E. Hereditary distal muscular atrophy with vocal cord paralysis and sensorineural hearing loss: a dominant form of spinal muscular atrophy? J Med Genet. 1989;26:105–8. doi: 10.1136/jmg.26.2.105. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Claeys KG, Zuchner S, Kennerson M, Berciano J, Garcia A, Verhoeven K, et al. Phenotypic spectrum of dynamin 2 mutations in Charcot-Marie-Tooth neuropathy. Brain. 2009;132:1741–52. doi: 10.1093/brain/awp115. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cuajungco MP, Grimm C, Oshima K, D'Hoedt D, Nilius B, Mensenkamp AR, et al. PACSINs bind to the TRPV4 cation channel. PACSIN 3 modulates the subcellular localization of TRPV4. J Biol Chem. 2006;281:18753–62. doi: 10.1074/jbc.M602452200. [DOI] [PubMed] [Google Scholar]
- D'Hoedt D, Owsianik G, Prenen J, Cuajungco MP, Grimm C, Heller S, et al. Stimulus-specific modulation of the cation channel TRPV4 by PACSIN 3. J Biol Chem. 2008;283:6272–80. doi: 10.1074/jbc.M706386200. [DOI] [PubMed] [Google Scholar]
- De Jonghe P, Timmerman V, Ceuterick C, Nelis E, De Vriendt E, Lofgren A, et al. The Thr124Met mutation in the peripheral myelin protein zero (MPZ) gene is associated with a clinically distinct Charcot-Marie-Tooth phenotype. Brain. 1999;122:281–90. doi: 10.1093/brain/122.2.281. [DOI] [PubMed] [Google Scholar]
- DeLong R, Siddique T. A large New England kindred with autosomal dominant neurogenic scapuloperoneal amyotrophy with unique features. Arch Neurol. 1992;49:905–8. doi: 10.1001/archneur.1992.00530330027010. [DOI] [PubMed] [Google Scholar]
- Deng HX, Klein CJ, Yan J, Shi Y, Wu Y, Fecto F, et al. Scapuloperoneal spinal muscular atrophy and CMT2C are allelic disorders caused by alterations in TRPV4. Nat Genet. 2010;42:165–9. doi: 10.1038/ng.509. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Donaghy M, Kennett R. Varying occurrence of vocal cord paralysis in a family with autosomal dominant hereditary motor and sensory neuropathy. J Neurol. 1999;246:552–5. doi: 10.1007/s004150050402. [DOI] [PubMed] [Google Scholar]
- Dyck PJ, Litchy WJ, Minnerath S, Bird TD, Chance PF, Schaid DJ, et al. Hereditary motor and sensory neuropathy with diaphragm and vocal cord paresis. Ann Neurol. 1994;35:608–15. doi: 10.1002/ana.410350515. [DOI] [PubMed] [Google Scholar]
- Erler I, Hirnet D, Wissenbach U, Flockerzi V, Niemeyer BA. Ca2+-selective transient receptor potential V channel architecture and function require a specific ankyrin repeat. J Biol Chem. 2004;279:34456–63. doi: 10.1074/jbc.M404778200. [DOI] [PubMed] [Google Scholar]
- Everaerts W, Nilius B, Owsianik G. The vallinoid transient receptor potential channel Trpv4: from structure to disease. Prog Biophys Mol Biol. 2009 doi: 10.1016/j.pbiomolbio.2009.10.002. [Epub ahead of print] [DOI] [PubMed] [Google Scholar]
- Fleury P, Hageman G. A dominantly inherited lower motor neuron disorder presenting at birth with associated arthrogryposis. J Neurol Neurosurg Psychiatry. 1985;48:1037–48. doi: 10.1136/jnnp.48.10.1037. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gaudet R. A primer on ankyrin repeat function in TRP channels and beyond. Mol Biosyst. 2008;4:372–9. doi: 10.1039/b801481g. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hellwig N, Albrecht N, Harteneck C, Schultz G, Schaefer M. Homo- and heteromeric assembly of TRPV channel subunits. J Cell Sci. 2005;118:917–28. doi: 10.1242/jcs.01675. [DOI] [PubMed] [Google Scholar]
- Irobi J, Van Impe K, Seeman P, Jordanova A, Dierick I, Verpoorten N, et al. Hot-spot residue in small heat-shock protein 22 causes distal motor neuropathy. Nat Genet. 2004;36:597–601. doi: 10.1038/ng1328. [DOI] [PubMed] [Google Scholar]
- Isozumi K, DeLong R, Kaplan J, Deng HX, Iqbal Z, Hung WY, et al. Linkage of scapuloperoneal spinal muscular atrophy to chromosome 12q24.1-q24.31. Hum Mol Genet. 1996;5:1377–82. doi: 10.1093/hmg/5.9.1377. [DOI] [PubMed] [Google Scholar]
- Klein CJ, Cunningham JM, Atkinson EJ, Schaid DJ, Hebbring SJ, Anderson SA, et al. The gene for HMSN2C maps to 12q23-24: a region of neuromuscular disorders. Neurology. 2003;60:1151–6. doi: 10.1212/01.wnl.0000055900.30217.ea. [DOI] [PubMed] [Google Scholar]
- Krakow D, Vriens J, Camacho N, Luong P, Deixler H, Funari TL, et al. Mutations in the gene encoding the calcium-permeable ion channel TRPV4 produce spondylometaphyseal dysplasia, Kozlowski type and metatropic dysplasia. Am J Hum Genet. 2009;84:307–15. doi: 10.1016/j.ajhg.2009.01.021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Landoure G, Zdebik AA, Martinez TL, Burnett BG, Stanescu HC, Inada H, et al. Mutations in TRPV4 cause Charcot-Marie-Tooth disease type 2C. Nat Genet. 2010;42:170–4. doi: 10.1038/ng.512. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Liedtke W, Choe Y, Marti-Renom MA, Bell AM, Denis CS, Sali A, et al. Vanilloid receptor-related osmotically activated channel (VR-OAC), a candidate vertebrate osmoreceptor. Cell. 2000;103:525–35. doi: 10.1016/s0092-8674(00)00143-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McEntagart M, Dunstan M, Bell C, Boltshauser E, Donaghy M, Harper PS, et al. Clinical and genetic heterogeneity in peroneal muscular atrophy associated with vocal cord weakness. J Neurol Neurosurg Psychiatry. 2002;73:762–5. doi: 10.1136/jnnp.73.6.762. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McEntagart M, Norton N, Williams H, Teare MD, Dunstan M, Baker P, et al. Localization of the gene for distal hereditary motor neuronopathy VII (dHMN-VII) to chromosome 2q14. Am J Hum Genet. 2001;68:1270–6. doi: 10.1086/320122. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McEntagart ME, Reid SL, Irrthum A, Douglas JB, Eyre KE, Donaghy MJ, et al. Confirmation of a hereditary motor and sensory neuropathy IIC locus at chromosome 12q23-q24. Ann Neurol. 2005;57:293–7. doi: 10.1002/ana.20375. [DOI] [PubMed] [Google Scholar]
- Nilius B, Owsianik G. Channelopathies converge on TRPV4. Nat Genet. 2010;42:98–100. doi: 10.1038/ng0210-98. [DOI] [PubMed] [Google Scholar]
- Nilius B, Watanabe H, Vriens J. The TRPV4 channel: structure-function relationship and promiscuous gating behaviour. Pflugers Arch. 2003;446:298–303. doi: 10.1007/s00424-003-1028-9. [DOI] [PubMed] [Google Scholar]
- Pareyson D, Taroni F, Botti S, Morbin M, Baratta S, Lauria G, et al. Cranial nerve involvement in CMT disease type 1 due to early growth response 2 gene mutation. Neurology. 2000;54:1696–8. doi: 10.1212/wnl.54.8.1696. [DOI] [PubMed] [Google Scholar]
- Phelps CB, Wang RR, Choo SS, Gaudet R. Differential regulation of TRPV1, TRPV3, and TRPV4 sensitivity through a conserved binding site on the ankyrin repeat domain. J Biol Chem. 2009;285:731–40. doi: 10.1074/jbc.M109.052548. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Plant TD, Strotmann R. Trpv4. Handb Exp Pharmacol. 2007:189–205. doi: 10.1007/978-3-540-34891-7_11. [DOI] [PubMed] [Google Scholar]
- Puls I, Jonnakuty C, LaMonte BH, Holzbaur EL, Tokito M, Mann E, et al. Mutant dynactin in motor neuron disease. Nat Genet. 2003;33:455–6. doi: 10.1038/ng1123. [DOI] [PubMed] [Google Scholar]
- Puls I, Oh SJ, Sumner CJ, Wallace KE, Floeter MK, Mann EA, et al. Distal spinal and bulbar muscular atrophy caused by dynactin mutation. Ann Neurol. 2005;57:687–94. doi: 10.1002/ana.20468. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pulst SM, Nechiporuk A, Nechiporuk T, Gispert S, Chen XN, Lopes-Cendes I, et al. Moderate expansion of a normally biallelic trinucleotide repeat in spinocerebellar ataxia type 2. Nat Genet. 1996;14:269–76. doi: 10.1038/ng1196-269. [DOI] [PubMed] [Google Scholar]
- Rankin J, Ellard S. The laminopathies: a clinical review. Clin Genet. 2006;70:261–74. doi: 10.1111/j.1399-0004.2006.00677.x. [DOI] [PubMed] [Google Scholar]
- Rock MJ, Prenen J, Funari VA, Funari TL, Merriman B, Nelson SF, et al. Gain-of-function mutations in TRPV4 cause autosomal dominant brachyolmia. Nat Genet. 2008;40:999–1003. doi: 10.1038/ng.166. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rozen S, Skaletsky H. Primer3 on the WWW for general users and for biologist programmers. Methods Mol Biol. 2000;132:365–86. doi: 10.1385/1-59259-192-2:365. [DOI] [PubMed] [Google Scholar]
- Santoro L, Manganelli F, Di Maio L, Barbieri F, Carella M, D'Adamo P, et al. Charcot-Marie-Tooth disease type 2C: a distinct genetic entity. Clinical and molecular characterization of the first European family. Neuromuscul Disord. 2002;12:399–404. doi: 10.1016/s0960-8966(01)00305-4. [DOI] [PubMed] [Google Scholar]
- Schule R, Bonin M, Durr A, Forlani S, Sperfeld AD, Klimpe S, et al. Autosomal dominant spastic paraplegia with peripheral neuropathy maps to chr12q23-24. Neurology. 2009;72:1893–8. doi: 10.1212/WNL.0b013e3181a6086c. [DOI] [PubMed] [Google Scholar]
- Sevilla T, Cuesta A, Chumillas MJ, Mayordomo F, Pedrola L, Palau F, et al. Clinical, electrophysiological and morphological findings of Charcot-Marie-Tooth neuropathy with vocal cord palsy and mutations in the GDAP1 gene. Brain. 2003;126:2023–33. doi: 10.1093/brain/awg202. [DOI] [PubMed] [Google Scholar]
- Sivakumar K, Kyriakides T, Puls I, Nicholson GA, Funalot B, Antonellis A, et al. Phenotypic spectrum of disorders associated with glycyl-tRNA synthetase mutations. Brain. 2005;128:2304–14. doi: 10.1093/brain/awh590. [DOI] [PubMed] [Google Scholar]
- Stojkovic T, Latour P, Viet G, de Seze J, Hurtevent JF, Vandenberghe A, et al. Vocal cord and diaphragm paralysis, as clinical features of a French family with autosomal recessive Charcot-Marie-Tooth disease, associated with a new mutation in the GDAP1 gene. Neuromuscul Disord. 2004;14:261–4. doi: 10.1016/j.nmd.2004.01.003. [DOI] [PubMed] [Google Scholar]
- Thomas PK, Marques W, Jr, Davis MB, Sweeney MG, King RH, Bradley JL, et al. The phenotypic manifestations of chromosome 17p11.2 duplication. Brain. 1997;120(Pt 3):465–78. doi: 10.1093/brain/120.3.465. [DOI] [PubMed] [Google Scholar]
- van der Vleuten AJ, van Ravenswaaij-Arts CM, Frijns CJ, Smits AP, Hageman G, Padberg GW, et al. Localisation of the gene for a dominant congenital spinal muscular atrophy predominantly affecting the lower limbs to chromosome 12q23-q24. Eur J Hum Genet. 1998;6:376–82. doi: 10.1038/sj.ejhg.5200229. [DOI] [PubMed] [Google Scholar]
- Watanabe H, Vriens J, Prenen J, Droogmans G, Voets T, Nilius B. Anandamide and arachidonic acid use epoxyeicosatrienoic acids to activate TRPV4 channels. Nature. 2003;424:434–8. doi: 10.1038/nature01807. [DOI] [PubMed] [Google Scholar]
- Wilhelmsen KC, Blake DM, Lynch T, Mabutas J, De Vera M, Neystat M, et al. Chromosome 12-linked autosomal dominant scapuloperoneal muscular dystrophy. Ann Neurol. 1996;39:507–20. doi: 10.1002/ana.410390413. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.