Abstract
Objectives The purpose of this pilot study was to determine the association of observed parenting behaviors with adjustment in adolescents with type 1 diabetes (T1D) and their mothers. Methods Adolescents with T1D (n = 30) and their mothers provided data on psychosocial adjustment and engaged in a discussion task about diabetes stress, which was coded for parenting behavior. Clinical data (i.e., HbA1c) was obtained from adolescents’ medical records. Results Mothers’ symptoms of anxiety and depression were related to lower levels of child-centered parenting. Higher levels of observed child-centered parenting and positive reinforcement and lower levels of maternal hostility and parental influence were related to better psychosocial adjustment in adolescents (i.e., fewer depressive symptoms, better quality of life) and better metabolic control. Conclusions Results support the use of observational data in this population and provide estimates of effect sizes between parenting variables, maternal and adolescent psychosocial adjustment, and metabolic control.
Keywords: adjustment, adolescents, diabetes, parent-adolescent communication, parenting
Type 1 diabetes (T1D) is one of the most common chronic childhood illnesses, affecting 2.28 in every 1,000 youth in the U.S. aged 10–19 years, and research suggests that the incidence of T1D is increasing (Gale, 2002; Liese, 2006). Diabetes requires the child and his/her family to be responsible for the majority of disease management, including multiple daily injections/boluses, monitoring carbohydrate intake, and frequent blood glucose monitoring (ADA, 2008). This intensive level of responsibility is likely to increase family stress and conflict, particularly when children reach adolescence (Anderson et al., 2002). Adolescence is also a time of increased risk for psychological disorders and deteriorating metabolic control (Hocking & Lochman, 2005). Because T1D is a chronic illness that requires continuous supervision by parents, as well as ongoing communication between parents and adolescents around treatment management, it becomes particularly important to understand specific parenting behaviors that promote this collaboration.
Parenting and Adjustment to T1D
Family functioning has been strongly linked to adjustment in adolescents with T1D, including both metabolic control and psychosocial functioning (Whittemore, Kanner, & Grey, 2004). Diabetes-specific family conflict has been related to poorer adherence and metabolic control, as well as lower quality of life in youth (Anderson et al., 2002; Laffel et al., 2003; Lewin et al., 2006). On the other hand, higher levels of family cohesion have been related to better adherence to treatment and better metabolic control in youth (Cohen, Lumley, Naar-King, Partridge, & Cakan, 2004; Jacobson et al., 1994). More warmth and caring behaviors by families have also been related to better quality of life in adolescents (Grey, Boland, Yu, Sullivan-Bolyai, & Tamborlane, 1998). Although these findings underscore the importance of parenting behaviors to adolescents’ adjustment to T1D, previous studies have been limited by the absence of observational studies as an objective measure of parenting behaviors.
Direct observational methods allow researchers to study relationships between individuals, and they provide information independent of self- and other-reports and unaffected by reporting biases that may influence the reports of parents and children (Kerig, 2001). However, the majority of research on family functioning in children with T1D has relied on mothers’, and occasionally children's, reports of parenting and family environment (Drotar, 1997). In addition, some of the observational research on youth with T1D was conducted decades ago (Bobrow, AvRuskin, & Siller, 1985; Hauser et al., 1986), before the intensive treatment regimen was recommended for youth with T1D (DCCT Research Group, 1994).
The few studies of parent–child interactions in adolescents with T1D have produced promising results. For example, one study of adolescent girls with T1D and their mothers found that more emotionally charged and confrontational discussions of conflict (based on transcripts of the parent–child interaction) were related to poorer adherence to treatment (Bobrow et al., 1985). One of the only studies that coded observed behavior during a diabetes-related task found that higher levels of observed parental emotional support, acceptance, and conflict resolution were related to better metabolic control, while higher levels of observed parental anger and sadness were related to poorer metabolic control (Martin, Miller-Johnson, Kitzmann, & Emery, 1998). Other researchers have used observed parent-child interactions as an outcome measure in intervention studies of adolescents with T1D and their parents, finding that improvements in parent–child communication were associated with better adherence and adjustment to T1D (Wysocki et al., 1999), as well as decreased family conflict, and improved metabolic control (Wysocki et al., 2008).These findings suggest the important implications for parenting on adolescents’ metabolic control. More research is needed, however, to determine the impact of specific parenting behaviors on adolescents’ psychosocial adjustment.
Maternal Psychosocial Adjustment and Parenting
Given that mothers of youth with T1D are likely to experience symptoms of depression and anxiety related to their child's illness (Kovacs et al., 1990; Mullins et al., 2004), observational studies of depressed and anxious mothers with their healthy children are relevant to this population. A meta-analytic review of observational studies found that depressed mothers are more likely to exhibit negative/critical behavior (ES =.40) and disengaged behavior (ES =.29), and less likely to exhibit positive behavior (ES =.16) than nondepressed mothers in interactions with their children (Lovejoy, Graczyk, O'Hare, & Neuman, 2000). Similarly, a review of observational studies with anxious parents and their children (Wood, McLeod, Sigman, Hwang, & Chu, 2003) indicated that anxious mothers exhibit higher levels of controlling and intrusive behaviors, and lower levels of warmth during interactions with their children. We would expect to see similar parent behaviors in anxious and depressed mothers of adolescents with T1D; however, this has not been evaluated in this population. Taken together, these findings suggest a need for more observational studies of adolescents with T1D and their parents, with a particular focus on parenting behaviors that may be related to the stress of treatment management, such as intrusiveness and support.
The Current Study
The current study is a pilot study of parenting behaviors and adjustment in adolescents with T1D and their mothers. The purpose of this study was to determine the feasibility of conducting observational research including a discussion of diabetes-related stress in this population. An additional objective was to provide estimates of the effect sizes of the relationships between specific observed parenting variables with maternal anxiety and depression, and adolescents’ depressive symptoms, quality of life, and metabolic control. Adolescents and their mothers completed questionnaires and engaged in a 15-min discussion of stress related to diabetes management, which was coded for parenting behaviors. Clinical data (i.e., HbA1c) were obtained from adolescents’ medical records. We expected, first, that greater symptoms of maternal anxiety and depression would be related to higher levels of negative parenting behaviors (i.e., observed hostility and intrusiveness) and lower levels of positive parenting (i.e., warmth, positive reinforcement). Next, we expected that higher levels of negative parenting would be related to poorer adjustment in adolescents (i.e., higher rates of depressive symptoms, poorer quality of life, and poorer metabolic control), and that higher rates of positive parenting behaviors would be related to better adjustment in adolescents.
Methods
Participants and Procedures
Adolescents with T1D and their mothers were recruited from the pediatric diabetes clinic of a university medical center. Adolescents were eligible if they had no major health problems other than T1D; had been diagnosed for at least 6 months; were currently living with their mothers; were age-appropriate for their grade within 1 year; were able to speak and read English; and were between the ages of 10 and 16 years. This age range was chosen because it encompasses a developmental stage when adolescents typically show a decline in diabetes management, and 10 is the age at which the American Diabetes Association recommends regular screening for depression (Anderson et al., 2002; Silverstein et al., 2005). Using Lerner and Steinberg's (2004) definition, children in the second decade of life (ages 10–19 years) are considered adolescents. Mothers were eligible if they were living with the child and were able to speak and read English. Demographic characteristics are presented in Table I.
Table I.
Demographic Characteristics (n = 30)
| Variable | |
|---|---|
| Child age, M ± SD (range), years | 12.6 ± 1.6 (10–16) |
| Child gender (%) | |
| Female | 52 |
| Male | 48 |
| Race/Ethnicity (%) | |
| White | 74 |
| Black | 13 |
| Hispanic | 13 |
| Duration of diabetes, M ± SD (range), months | 69.1 ± 56.2 (7–249) |
| Treatment type (%) | |
| Insulin pump | 74 |
| Multiple injections | 26 |
| HbA1c, M ± SD | 7.9 ± 1.5 (5.5–13.4) |
| Maternal age, M ± SD (range), years | 43.47 ± 6.7 (30–57) |
| Maternal education (%) | |
| Less than high school | 7 |
| High school/GED | 16 |
| Associates/some college | 17 |
| College degree | 32 |
| Graduate degree | 29 |
| Annual family income (%) | |
| <$40,000/year | 17 |
| $40,000–$80,000/year | 34 |
| >$80,000/year | 48 |
During the recruitment period, 82% of the 85 families approached expressed interest in participating. The most frequent reason given for declining participation was the time commitment (69%), with only a few families citing distance or lack of interest. Of those who expressed interest, 57% were unable to be contacted or scheduled (as this was a pilot study, there was limited time and resources to follow up with families). There were no significant differences in race/ethnicity or marital status between families who participated and those who did not.
Measures
Demographics
Demographic information was obtained from a questionnaire completed by the mother including questions about race/ethnicity, annual family income, marital status, maternal education, religious affiliation, and adults living in the home.
Diabetes-related Stress
Mothers’ and adolescents’ reported on diabetes-related stress using the T1D version of the Responses to Stress Questionnaire (RSQ, Connor-Smith, Compas, Wadsworth, Thomsen, & Saltzman, 2000). The first 10 items of the measure list topics that are stressful for adolescents with T1D (Davidson, Penney, Muller, & Grey, 2004), such as feeling different from others or having to deal with diabetes care (e.g., remembering to give shots/bolus). Respondents reported on the recent (i.e., past 6 months) occurrence of each of the stressors on a four-point Likert scale (0 = never, 1 = a few times, 2 = many times, and 3 = almost every day). For the purposes of this study, these items were used to determine a topic for the parent–child interaction (see below).
Parenting Behaviors
The Iowa Family Interaction Rating Scales (IFIRS; Melby & Conger, 2001) was used as an observational measure of parenting behaviors. The IFIRS is a well-established, widely used global coding system, applicable across racial and ethnic groups (Alderfer et al., 2008). The validity of the IFIRS system has been established against reports from self and other family members using correlational and confirmatory factor analyses (Melby & Conger, 2001). Although this system was developed to code interactions in families with healthy adolescents, it has been used successfully to study parenting in other pediatric populations, including children with cystic fibrosis (DeLambo, Iever-Landis, Drotar, & Quittner, 2004) and asthma (Celano et al., 2008).
The IFIRS coding system requires that each interaction be viewed a total of five times: once for an overall impression, and twice per focal (mother and adolescent). Each interaction was coded by the first author, who received intensive training from the authors of the IFIRS, and double-coded by another trained research assistant (RA). Behavior is scored on a scale from 1 to 9, with 1 being “not at all characteristic” of the subject during the 15-min interaction, and 9 being “mainly characteristic” of the subject during the interaction. Frequency of behaviors, context and affect, as well as intensity and proportion are all considered when scoring each subject on the level of “characteristicness” of the scale. The following Parenting Codes, which rate mothers’ observed and reported childrearing behaviors displayed during the interaction, were used in the current study: Hostility (the extent to which the mother displays hostile, angry, critical, disapproving, and/or rejecting behavior toward her child), Parental Influence (the extent to which the mother attempts to regulate, control, or influence the child's behavior), Sensitive/Child Centered (the extent to which the mother displays awareness of the child's needs, moods, interests, and capabilities), and Positive Reinforcement (the extent to which the mother responds to her child's desired behavior with praise, approval, rewards, or smiles) (Melby et al., 1998). Inter-rater reliability (Intraclass correlations) for the current study were.67 for Hostility,.61 for Parental Influence,.73 for Child Centered, and.79 for Positive Reinforcement. These levels indicate moderate agreement between coders (Shrout, 1998).
Maternal Depression
The Center for Epidemiologic Studies of Depression Scale (CES-D) was used as a brief self-report measure of depressive symptoms in mothers (Radloff, 1977). A total score is calculated from 20 items and ranges from 0 to 60. Higher scores indicate more depressive symptoms, and a score of 16 or higher suggests clinical depression. This measure is widely used with both clinical samples and community surveys, with excellent reliability. Internal consistency (Chronbach's α) for the current sample was.88.
Maternal Anxiety
The State Trait Anxiety Inventory (STAI) was used to assess mothers’ symptoms of anxiety (Spielberg, Gorsuch, & Lushene, 1970). The STAI is the most widely used measure of anxiety in adults and has established reliability and validity. The 20 items measuring state anxiety by asking how respondents “feel right now” were used to assess current symptoms of anxiety. Scores range from 20 to 80, with higher scores indicating a greater level of anxiety. The cutoff score for high anxiety for the age range that includes the mean age of mothers in the study (40–49 years) is 44. Internal consistency (Chronbach's α) for this scale was.91.
Adolescent Depressive Symptoms
The Child Depression Inventory (CDI; Kovacs, 1985) was used to measure adolescents’ current depressive symptoms. The CDI consists of 21 items, and higher scores indicate higher current levels of depression, with a score of greater than or equal to 13 suggesting clinical levels of depression. Internal consistency is good, and the measure meets criteria for test-retest reliability and stability over time. The CDI has been used frequently with children and adolescents with T1D (e.g., Whittemore et al., 2002). Internal consistency (Chronbach's α) for the current sample was.85.
Quality of Life
The Pediatric Quality of Life Inventory (PedsQL) was developed to evaluate quality of life in children with chronic health conditions (Varni et al., 1999). The PedsQL consists of a 23-item core measure of global health-related quality of life, for which higher scores reflect better quality of life. High reliability and validity have been established in samples of children with type 1 diabetes, and discriminant validity was demonstrated for children with T1D and healthy children (Varni et al., 2003). Internal consistency for the current sample (Chronbach's α) was.84.
Metabolic Control
Glycosylated hemoglobin (HbA1c) was used as a measure of adolescents’ metabolic control. The glycosylation of the hemoglobin molecule provides objective criteria of metabolic control over the most recent 8–12 weeks, and it is routinely measured quarterly in patients with T1D (ADA, 2008). Those without diabetes have an HbA1c of <6.3%, and an HbA1c of <8% is considered acceptable control for school-aged children and adolescents (ADA, 2008). Analyses were performed using the Bayer Diagnostics DCA2000® machine, which provides results on a fingerstick blood sample (normal range = 4.2–6.3%).
Procedures
Adolescents and their mothers were recruited from the university medical center's pediatric diabetes clinic during their regular quarterly clinic visits. Interested families were scheduled for a visit, which was conducted in a private laboratory space, including comfortable chairs and a video camera. In line with the university Institutional Board Review requirements, consent forms were read to the adolescent and his/her mother and any additional questions regarding the study were answered. If the mother consented (and adolescent assented), the mother and adolescent completed the questionnaires and participated in a 15-min videotaped interaction (see below for description). Mothers provided demographic data and completed self-report measures of current symptoms of anxiety and depression, as well as stress related to diabetes management. Adolescents completed measures of their own depressive symptoms, quality of life, and diabetes-related stress. If an adolescent indicated that he/she was experiencing significant distress on the depression inventory (i.e., total Child Depression Inventory score ≥13, or endorsed the item “I want to kill myself”), or a mother indicated that she was experiencing significant distress (i.e., total CES-D score ≥ 16), a licensed clinical psychologist screened the individual to determine if a referral was necessary to ensure the participant's safety. Clinical data, including HbA1c, was obtained from the child's medical record from the clinic visit closest to completing the questionnaire data.
The topic for the interaction was chosen by comparing mothers’ and adolescents’ responses to the stressor items on the T1D version of the Responses to Stress Questionnaire (RSQ, Connor-Smith et al., 2000). A common stressor was chosen by summing the mother's and adolescent's scores for each item to determine the highest-rated issue per mother and child report. The family was given a cue card with standardized questions to prompt discussion on this issue (e.g., What happened the last time [we had to deal with diabetes care (e.g., checking blood sugar)]? When [we have to deal with diabetes care], what usually happens? What kind of feelings or emotions do we usually have when [we have to deal with diabetes care]? What can we do to reduce this stress?). After the 15-min period, the participants had the opportunity to discuss what happened during the procedure, feelings or thoughts about diabetes that may have surfaced, and how each participant felt about the discussions. Adolescents and their mothers were compensated for their time ($20 each).
Data Analysis Plan
Analyses were performed using SPSS (v. 16.0, Chicago, IL, USA) statistical packages. Descriptive analyses were conducted to determine the frequency and distribution of each variable. Next, we tested for effects of child age and gender on key variables. To test our hypotheses, we conducted bivariate correlations to determine the association between maternal distress (i.e., CES-D, STAI), parenting variables (i.e., Hostility, Parental Influence, Child Centered, and Positive Reinforcement), and adolescent adjustment (i.e., CDI, PedsQL, HbA1c).
Results
Descriptive Statistics
Table II presents the descriptive statistics for mothers’ reports of current symptoms of anxiety and depression, observed parenting behaviors, and adolescents’ reports of current depressive symptoms and quality of life, as well as HbA1c. In general, adolescents reported fairly high quality of life and few symptoms of depression. Average metabolic control was within the recommended range for this age group (< 8%, ADA, 2008). In terms of depression, 6.5% (n = 2) of the adolescents in the sample met the cutoff score for symptoms of depression (CDI score ≥ 13), and 22.6% (n = 7) of the mothers met the cutoff score for symptoms of depression (CES-D score ≥ 16). In addition, 12.9% (n = 4) of the mothers met the cutoff score for symptoms of anxiety (STAI ≥ 44).
Table II.
Descriptive Statistics and Correlations for Parenting Behaviors and Adjustment in Adolescents with T1D and their Mothers
| 1. | 2. | 3. | 4. | 5. | 6. | 7. | 8. | 9. | 10. | 11. | |
|---|---|---|---|---|---|---|---|---|---|---|---|
| 1. CES-D M = 10.83 (8.50) | – | ||||||||||
| 2. State Anxiety M = 32.58 (9.08) | .80*** | – | |||||||||
| 3. Hostility M = 3.20 (1.55) | .20 | .33+ | – | ||||||||
| 4. Parental Influence M = 5.65 (1.18) | .12 | .19 | .17 | – | |||||||
| 5. Child Centered M = 6.20 (1.12) | −.45* | −.50** | −.77*** | .00 | – | ||||||
| 6. Pos. Reinforcement M = 3.63 (1.90) | −.27 | −.27 | −.57*** | .21 | .62*** | – | |||||
| 7. CDI M = 3.87 (4.50) | −.00 | .26 | .52** | .44* | −.37* | −.22 | – | ||||
| 8. PedsQL M = 86.71 (8.85) | .03 | −.19 | −.13 | −.37* | −.01 | .13 | −.71*** | – | |||
| 9. HbA1c M = 7.9 (1.5) | .20 | .35+ | .45* | .05 | −.53** | −.56*** | .36* | −.11 | – | ||
| 10. Child Age M = 12.6 (1.6) | −.07 | −.12 | .17 | −.37* | −.10 | −.06 | −.30 | .28 | .13 | – | |
| 11. Duration M = 69.1 (56.2) | −.21 | −.34+ | .31 | −.11 | −.09 | −.24 | .10 | −.09 | .12 | .26 | – |
Values in parentheses are standard deviations.
+p <.10; *p <.05; **p <.01; ***p <.001.
Preliminary Analyses
Preliminary analyses were conducted to test for effects of child age and gender on key variables. There were no significant gender differences on any key variables, and child age was significantly associated with only one of the parenting variables: mothers of older children exhibited significantly less parental influence (r = −.37, p <.05).
Maternal Psychosocial Distress and Observed Parenting
As seen in Table I, mothers who reported greater symptoms of depression exhibited lower levels of child centered parenting (r = −.45, p =.012). There was not a significant association between maternal symptoms of depression and any other parenting behaviors. Mothers who reported higher levels of anxiety exhibited lower levels of child centered parenting (r = −.50, p =.005), and somewhat higher levels of hostility (r =.33, p =.073). Maternal anxiety was not related to observed parental influence or positive reinforcement.
Observed Parenting and Adolescent Adjustment
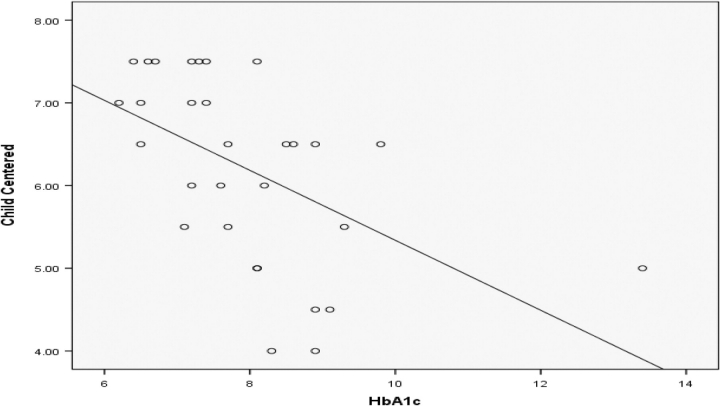
Bivariate correlations between observed parenting and adolescent adjustment revealed that higher levels of observed maternal hostility were related to greater symptoms of depression (r =.52, p =.003) and poorer metabolic control (r =.45, p =.012) in adolescents (Figure 1). Further, higher levels of observed parental influence (i.e., attempts to regulate or control child's behavior) were related to greater symptoms of depression (r =.44, p =.015) and poorer quality of life (r = −.37, p =.047) in adolescents. In contrast, higher levels of child centered parenting (i.e., demonstrations of sensitivity of child's needs) were related to fewer depressive symptoms (r = −.37, p =.043), and better metabolic control (r = −.53, p =.003) in adolescents (Figure 2). Finally, as seen in Figure 3, higher levels of positive reinforcement were related to better metabolic control (r = −.56, p =.001).
Fig. 1.
Scatterplot of maternal hostility with HbA1c.
Fig. 2.
Scatterplot of child centered parenting with HbA1c.
Fig. 3.
Scatterplot of positive reinforcement with HbA1c.
Discussion
The current study is one of the first studies of adolescents with T1D to use direct observational methods to measure specific parenting variables in relation to maternal psychosocial distress, adolescent adjustment, and metabolic control. Maternal depression and anxiety were related to lower levels of positive parenting, and observed parenting was related to both psychosocial adjustment and metabolic control in adolescents. Specifically, sensitive, child-centered parenting and positive reinforcement were related to better psychosocial adjustment and better metabolic control, whereas maternal hostility was related to poorer metabolic control in adolescents.
In our sample, 23% of the mothers scored above the clinical cutoff for depressive symptoms and 13% for symptoms of anxiety. These results are in line with findings from a recent study of mothers of children ages 8–12 years with T1D, in which 22% of mothers scored above the clinical cutoff for depressive symptoms (Jaser, Whittemore, Ambrosino, Lindemann, & Grey, 2008). Results from the current study suggest that maternal symptoms of depression and anxiety were most strongly correlated with positive parenting behaviors (i.e., sensitive/child centered parenting). However, the small sample size limited our power to detect smaller effects, and the correlation between maternal anxiety and observed hostility approached significance. Larger sample sizes may be needed to determine the relationship between maternal anxiety/depression and negative parenting behaviors, including intrusiveness (Cameron, Young, & Wiebe, 2007).
It is interesting to note that, in our sample, both positive parenting behaviors (i.e., child-centered parenting and positive reinforcement) and negative parenting behaviors (i.e., hostility) were significantly associated with adolescents’ depressive symptoms and metabolic control. For example, positive reinforcement, which included statements such as, “you’re doing a good job remembering to check your sugar at school,” had a fairly strong association with metabolic control (r = −.56). These associations are in line with—but somewhat stronger than—those found in a previous study linking adolescents’ metabolic control with observed parental emotional support (r = −.39) and acceptance (r = −.37). It is possible that the specific parenting behaviors measured in the IFIRS coding system (e.g., positive reinforcement) are better predictors of metabolic control than more general indicators of emotional support. These findings suggest the need to consider both positive and negative parenting behaviors in research and practice.
Similar to previous studies using questionnaire data (Cameron et al., 2007), we found that observed intrusive parenting (i.e., parental influence) was related to adolescents’ quality of life and depressive symptoms. These results are in line with the view that, as children enter adolescence and strive for autonomy, parents’ attempts to monitor or control their child's treatment may be perceived as intrusive or “nagging,” which may result in adolescents becoming depressed and withdrawn (Berg et al., 2007; Cameron et al., 2008; Weinger et al., 2001). On the other hand, parental monitoring of diabetes management and involvement that is perceived as supportive and collaborative by adolescents has been related to better metabolic control and fewer depressive symptoms (Ellis et al., 2007; Whittemore et al., 2002; Wiebe et al., 2005). Taken together, these findings suggest that the goal may be for adolescents to gradually assume independence with continued parental monitoring (Wiebe et al., 2005). More research is needed to tease out the differences between parental monitoring and intrusiveness, and observational studies may play an important role in determining effective ways for parents to monitor adolescents’ self-care without intruding on their independence.
Limitations
As a pilot study, it is important to note that the current results may be limited in their generalizability; our sample is limited by the demographics and treatment practices of the clinic from which it was drawn. In addition, the relatively low rate of participation may bias the results. Further, the inter-rater reliability was at a moderate, albeit acceptable level (Shrout, 1998), which may impact the results. Finally, the small sample size of the current study precluded testing for possible interactions with child age or gender. These data, however, provide estimates of the effect sizes between variables that may be used to determine the sample size needed to fully test these relationships.
Implications
Despite these limitations, the strong relationship between observed parenting variables with both psychosocial (i.e., depressive symptoms, quality of life) and physiological (i.e., metabolic control) indicators of adjustment support the use of observational methods to study parenting in this population. Although coding of interactions is time consuming and parent–child interactions in the laboratory may not reflect behavior at home (Kerig, 2001), our results support that this type of data provides an important perspective on family functioning in adolescents with T1D. The next step is to conduct larger, longitudinal studies using similar methods to test parenting as a mediator of maternal and child psychosocial distress. Ultimately, such studies could inform interventions to relieve maternal distress and promote positive parenting practices among families of adolescents with T1D.
Funding
Funding for the current study was provided by a Pilot/Feasibility Studies Program Award from the National Institute of Nursing Research (P30 NR008999) and the Intramural Small Grant Program from the Yale University School of Nursing.
References
- American Diabetes Association. Standards of medical care in diabetes – 2008. Diabetes Care. 2008;31:S12–S54. doi: 10.2337/dc08-S012. [DOI] [PubMed] [Google Scholar]
- Alderfer MA, Fiese BH, Gold JI, Cutuli JJ, Holmbeck GN, Goldbeck L, et al. Evidence-based assessment in pediatric psychology: Family measures. Journal of Pediatric Psychology. 2008;33(9):1046–1061. doi: 10.1093/jpepsy/jsm083. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Anderson BJ, Vangsness L, Connell A, Butler D, Goebel-Fabbri A, Laffel LMB. Family conflict, adherence, and glycaemic control in youth with short duration Type 1 diabetes. Diabetic Medicine. 2002;19:635–642. doi: 10.1046/j.1464-5491.2002.00752.x. [DOI] [PubMed] [Google Scholar]
- Bobrow ES, AvRuskin TW, Siller J. Mother-daughter interaction and adherence to diabetes regimens. Diabetes Care. 1985;8:146–151. doi: 10.2337/diacare.8.2.146. [DOI] [PubMed] [Google Scholar]
- Cameron LD, Young MJ, Wiebe DJ. Maternal trait anxiety and diabetes control in adolescents with type 1 diabetes. Journal of Pediatric Psychology. 2007;32:733–744. doi: 10.1093/jpepsy/jsl053. [DOI] [PubMed] [Google Scholar]
- Celano M, Bakeman R, Gaytan O, Smith CO, Koci A, Henderson S. Caregiver depressive symptoms and observed family interaction in low-income children with persistent asthma. Family Process. 2008;47:7–20. doi: 10.1111/j.1545-5300.2008.00236.x. [DOI] [PubMed] [Google Scholar]
- Cohen DM, Lumley MA, Naar-King S, Partridge T, Cakan N. Child behavior problems and family functioning as predictors of adherence and glycemic control in economically disadvantaged children with Type I diabetes: A prospective study. Journal of Pediatric Psychology. 2004;29:171–184. doi: 10.1093/jpepsy/jsh019. [DOI] [PubMed] [Google Scholar]
- Connor-Smith JK, Compas BE, Wadsworth ME, Thomsen AH, Saltzman H. Responses to stress in adolescence: Measurement of coping and involuntary stress responses. Journal of Consulting and Clinical Psychology. 2000;68:976–992. [PubMed] [Google Scholar]
- Davidson M, Penney EA, Muller B, Grey M. Stressors and self-care challenges faced by adolescents living with type 1 diabetes. Applied Nursing Research. 2004;17:72–80. doi: 10.1016/j.apnr.2004.02.006. [DOI] [PubMed] [Google Scholar]
- DCCT Research Group. Effect of intensive insulin treatment on the development and progression of long-term complications in adolescents with insulin-dependent diabetes mellitus: Diabetes Control and Complications Trial. Journal of Pediatrics. 1994;125:177–188. doi: 10.1016/s0022-3476(94)70190-3. [DOI] [PubMed] [Google Scholar]
- DeLambo KE, Iever-Landis CE, Drotar D, Quittner AL. Association of observed family relationship quality and problem-solving skills with treatment adherence in older children and adolescents with cystic fibrosis. Journal of Pediatric Psychology. 2004;29:343–353. doi: 10.1093/jpepsy/jsh038. [DOI] [PubMed] [Google Scholar]
- Drotar D. Relating parent and family functioning to the psychological adjustment of children and with chronic health conditions: What have we learned? What do we need to know? Journal of Pediatric Psychology. 1997;22:149–165. doi: 10.1093/jpepsy/22.2.149. [DOI] [PubMed] [Google Scholar]
- Gale EAM. The Rise of Childhood Type 1 Diabetes in the 20th Century. Diabetes. 2002;51(12):3353–3361. doi: 10.2337/diabetes.51.12.3353. [DOI] [PubMed] [Google Scholar]
- Grey M, Boland EA, Yu C, Sullivan-Bolyai S, Tamborlane WV. Personal and family factors associated with quality of life in adolescents with diabetes. Diabetes Care. 1998;21:909–914. doi: 10.2337/diacare.21.6.909. [DOI] [PubMed] [Google Scholar]
- Hauser ST, Jacobson AM, Wertlieb D, Weiss-Perry B, Follansbee D, Wolfsdorf JI, et al. Children with recently diagnosed diabetes: Interactions within their families. Health Psychology. 1986;5:273–296. doi: 10.1037//0278-6133.5.3.273. [DOI] [PubMed] [Google Scholar]
- Hocking MC, Lochman JE. Applying the transactional stress and coping model to sickle cell disorder and insulin-dependent diabetes mellitus: Identifying psychosocial variables related to adjustment and intervention. Clinical Child and Family Psychology Review. 2005;8:221–246. doi: 10.1007/s10567-005-6667-2. [DOI] [PubMed] [Google Scholar]
- Jacobson AM, Hauser ST, Lavori P, Willett JB, Cole CF, Wofsdorf JI, et al. Family environment and glycemic control: A four-year prospective study of children and adolescents with insulin-dependent diabetes mellitus. Psychosomatic Medicine. 1994;56:401–409. doi: 10.1097/00006842-199409000-00004. [DOI] [PubMed] [Google Scholar]
- Jaser SS, Whittemore R, Ambrosino J, Lindemann E, Grey M. Mediators of depressive symptoms in children with type 1 diabetes and their mothers. Journal of Pediatric Psychology. 2008;33:509–519. doi: 10.1093/jpepsy/jsm104. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kerig PK. Introduction and overview: Conceptual issues in family observational research. In: Kerig PK, Lindahl KM, editors. Family observational coding systems. Mahway, NJ: Lawrence Erlbaum; 2001. pp. 1–22. [Google Scholar]
- Kovacs M. The Children's Depression Inventory (CDI) Psychopharmacology Bulletin. 1985;21:995–998. [PubMed] [Google Scholar]
- Kovacs M, Iyengar S, Goldston D, Obrosky DS, Steward J, Marsh J. Psychological functioning among mothers of children with insulin-dependent diabetes mellitus: A longitudinal study. Journal of Consulting and Clinical Psychology. 1990;58:189–195. doi: 10.1037//0022-006x.58.2.189. [DOI] [PubMed] [Google Scholar]
- Laffel LM, Connell A, Vangness L, Goebel-Fabbri A, Mansfield A, Anderson BJ. General quality of life in youth with Type 1 Diabetes: Relationship to patient management and diabetes-specific family conflict. Diabetes Care. 2003;26:3067–3073. doi: 10.2337/diacare.26.11.3067. [DOI] [PubMed] [Google Scholar]
- Lerner RM, Steinberg L. Handbook of adolescent psychology. 2nd. Hoboken, NJ: John Wiley & Sons; 2004. [Google Scholar]
- Lewin AB, Heidgerken AD, Geffken GR, Williams LB, Storch EA, Gelfand KM, et al. The relation between family factors and metabolic control: The role of diabetes adherence. Journal of Pediatric Psychology. 2006;31:174–183. doi: 10.1093/jpepsy/jsj004. [DOI] [PubMed] [Google Scholar]
- Liese AD. The burden of diabetes mellitus among US youth: Prevalence estimates from the SEARCH for Diabetes in Youth Study. Pediatrics. 2006;118:1510–1518. doi: 10.1542/peds.2006-0690. [DOI] [PubMed] [Google Scholar]
- Lovejoy MC, Graczyk PA, O'Hare E, Neuman G. Maternal depression and parenting behavior: A meta-analytic review. Clinical Psychology Review. 2000;20:561–592. doi: 10.1016/s0272-7358(98)00100-7. [DOI] [PubMed] [Google Scholar]
- Martin MT, Miller-Johnson S, Kitzmann KM, Emery RE. Parent-child relationships and insulin-dependent diabetes mellitus: Observational ratings of clinically relevant dimensions. Journal of Family Psychology. 1998;12:102–111. [Google Scholar]
- Melby JN, Conger RD. The Iowa Family Interaction Rating Scales: Instrument summary. In: Kerig PK, Lindahl KM, editors. Family observational coding systems. Mahway, NJ: Lawrence Erlbaum; 2001. pp. 33–58. [Google Scholar]
- Melby JN, Conger RD, Book R, Reuter M, Lucy L, Repinski D. The Iowa Family Interaction Rating Scales. 5th. Iowa State University: Unpublished manuscript, Ames Institute for Social and Behavioral Research; 1998. [Google Scholar]
- Mullins LL, Fuemmeler BF, Hoff A, Chaney JM, Van Pelt J, Ewing CA. The relationship of parental overprotection and perceived child vulnerability to depressive symptomotology in children with type 1 diabetes mellitus: The moderating influence of parenting stress. Children's Health Care. 2004;33:21–34. [Google Scholar]
- Radloff LS. The CES-D Scale: A self-report depression scale for research in the general population. Applied Psychological Measurement. 1977;1:385–401. [Google Scholar]
- Shrout PE. Measurement reliability and agreement in psychiatry. Statistical Methods in Medical Research. 1998;7:301–317. doi: 10.1177/096228029800700306. [DOI] [PubMed] [Google Scholar]
- Silverstein JH, Klingensmith G, Copeland K, Plotnick L, Kaufman F, Laffel LMB, et al. Care of children and adolescents with type 1 diabetes. Diabetes Care. 2005;28:184–212. doi: 10.2337/diacare.28.1.186. [DOI] [PubMed] [Google Scholar]
- Spielberg CD, Gorsuch RL, Lushene RE. Test manual for the State-Trait Anxiety Inventory. Palo Alto, California: Consulting Psychologists Press; 1970. [Google Scholar]
- Whittemore R, Kanner S, Grey M. The influence of family on physiological and psychosocial health in youth with type 1 diabetes: A systematic review. In: Melnyk B, Fineat-Overholt E, editors. Evidence-based practice in nursing and healthcare: A guide to best practice. Philadelphia, PA: Lippincott Williams & Wilkins; 2004. pp. CD22-73–CD22-87. [Google Scholar]
- Whittemore R, Kanner S, Singleton S, Hamrin V, Chiu J, Grey M. Correlates of depressive symptoms in adolescents with type 1 diabetes. Pediatric Diabetes. 2002;3:135–143. doi: 10.1034/j.1399-5448.2002.30303.x. [DOI] [PubMed] [Google Scholar]
- Wood JJ, McLeod BD, Sigman M, Hwang W-C, Chu BC. Parenting and childhood anxiety: Theory, empirical findings, and future directions. Journal of Child Psychology and Psychiatry. 2003;44:134–151. doi: 10.1111/1469-7610.00106. [DOI] [PubMed] [Google Scholar]
- Wysocki T, Harris MA, Buckloh LM, Mertlich D, Lochrie AS, Taylor A, et al. Randomized, controlled trial of behavioral family systems therapy for diabetes: Maintenance and generalization of effects on parent-adolescent communication. Behavior Therapy. 2008;39:33–46. doi: 10.1016/j.beth.2007.04.001. [DOI] [PubMed] [Google Scholar]
- Wysocki T, Miller KM, Greco P, Harris MA, Harvey LM, Taylor A, et al. Behavior therapy for families of adolescents with diabetes: Effects on directly observed family interactions. Behavior Therapy. 1999;30:507–525. [Google Scholar]