Abstract
Objective
This exploratory study examined psychiatric symptom severity as a moderator of outcomes among women receiving either the Women’s Recovery Group (WRG), a new manualized group treatment for substance use disorders combining single-gender group composition and women-focused content, or Group Drug Counseling (GDC), an empirically supported mixed-gender group treatment.
Methods
We used a mixed model analysis of variance.
Results
We found a significant 3-way interaction effect of treatment condition, time, and baseline Brief Symptom Inventory scores as well as Beck Depression Inventory scores.
Conclusion
Single-gender group treatment may confer added benefit for women with substance abuse and high psychiatric symptom severity than mixed-gender treatment.
Women with substance use disorders (SUDs) differ from their male counterparts in their risk factors, presenting problems, co-occurring psychiatric disorders, medical consequences, and reasons for relapse; these differences may not be adequately addressed in mixed-gender settings (1). Some of these gender differences may be better addressed in women-focused treatment. In addition, women often endorse preferences for women-only SUD treatment because of their perceptions of enhanced comfort (2). The Women’s Recovery Group (WRG) was designed to combine single-gender group composition and women-focused content. It is the first manual-based recovery group for women that is not specific for type of substance abused (e.g., opioids, alcohol, cocaine, etc.) or specific co-occurring psychiatric disorders (e.g., post-traumatic stress disorder, borderline disorder).
The 12-weekly WRG sessions examined triggers to relapse with demonstrated relevance to treatment-seeking women with SUDs, including managing symptoms associated with psychiatric disorders (e.g., depression and anxiety) (3). Comparable reductions in substance use were achieved in a Stage 1 randomized controlled trial comparing outcomes of women receiving WRG (n=29) to women receiving an empirically supported mixed-gender treatment Group Drug Counseling (GDC) (n=7) (4). However, during the 6-month post-treatment follow-up, WRG members continued to reduce their substance use while GDC members did not (4). As depression, anxiety, and other psychiatric disorders (5) predict resumed substance use following SUD treatment, we conducted the current study to examine whether psychiatric symptom severity moderates substance use treatment outcomes. Specifically, we examined whether baseline psychiatric symptom severity, and depressive symptom severity, were associated with differential post-treatment outcomes among women enrolled in WRG and GDC.
METHODS
The Women’s Recovery Group (WRG) is a 12-session manual-based relapse-prevention group therapy that utilizes a cognitive-behavioral approach developed for this study by the principal investigator (4). The WRG study hypothesized that both the single-gender group composition and women-focused content would result in better outcomes than standard mixed-gender group treatment (4). A detailed description of the study design and WRG intervention manual are available (4). Briefly, content areas for individual sessions were based on gender-specific substance abuse antecedents, consequences, and treatment outcomes (1, 6–8). Because of the high prevalence of co-occurring psychiatric disorders, one session specifically addresses mood, anxiety, and eating disorders. In addition, the need for self-care is emphasized including seeking appropriate care and treatment for any co-occurring psychiatric disorders. Our comparison treatment, Group Drug Counseling (GDC) (9), is an empirically supported group treatment delivered typically to mixed-gender groups with no explicit attention to gender-specific issues. Both groups used a 90 minute structured format and covered common recovery topics such as triggers to use, relapse prevention, use of self-help, among others.
After obtaining approval from the McLean Hospital Institutional Review Board, written informed consent was obtained from all study participants. Individuals with co-occurring bipolar, psychotic, or post-traumatic stress disorders were excluded. In the pre-pilot phase of the study, of the 13 enrolled subjects, 100% completed treatment and 6-month post-treatment follow-up. At the end of both pre-pilot rounds, the WRG manual was revised based on patient, counselor, and outside consultant feedback. However, such revisions were minimal and included some reworking and rewording of bulletin board materials and take home messages. In the pilot RCT, 23 subjects were randomized either to WRG (N = 16) or GDC (N = 7), of which 18 (78.3%) completed all treatment sessions and 20 (87.0%) completed the 6-month post-treatment follow-up. In order to gain the broadest assessment of the experience of WRG versus GDC, we compared outcomes for all WRG subjects (n=29) to those women enrolled in GDC (n=7) (4).
Assessment of substance use was conducted at baseline and at months 1–6 and 9 (months 1–3 were in-treatment assessments and months 4–6 and 9 were post-treatment follow-up assessments). Outcome analyses were conducted by treatment phase and compared to change from baseline with the “in-treatment” phase comprising months 1–3, and the “post-treatment” phase comprising months 4–9 (4). The Timeline Follow-Back technique (10) was used to obtain substance use data. Psychiatric symptoms were assessed using the Brief Symptom Inventory (BSI)(11) and the Beck Depression Inventory (BDI)(12).
As described previously (4), a general mixed model analysis of variance (MMANOVA) was used to maximize the information provided from the available data (13). This framework models the means per group over the respective time period and the covariance between the repeated measures over the assessments. We focused on the difference between groups across phase (i.e., within treatment phase for months 1–3 and post-treatment phase for months 4–9) as modeled by the interaction of treatment and phase (4). MMANOVA requires continuous outcome measures with near normal distributions. Subtracting the baseline from all outcomes resulted in near normality for each outcome measure (14) Effect size derivation for all effects of interest were derived based on the F-test for compound symmetry models discussed by (15, 16).
Utilizing the standard cut-off score (12), baseline BSI scores were categorized as high (BSI≥63) and low (BSI<63). To examine the effect of baseline BSI (high or low) on treatment outcome across time, we included all two-way and three-way interactions of baseline BSI (high or low), treatment condition (WRG vs. GDC), and time (in-treatment or post-treatment assessment) in our MMANOVA. This analysis was repeated using BDI scores, which were also categorized with a score of 0–18 indicates no to mild depression and a score of 19 or above indicates moderate to severe depression (17). Age was included as a covariate in all analyses as randomization did not achieve equivalence between conditions as a function of age.
RESULTS
Baseline Characteristics
There were 29 women enrolled in pre-pilot and pilot WRG groups with 13 women in the pre-pilot WRG groups, 16 women randomized to the pilot WRG and 7 women to the pilot GDC (n=7) groups. Baseline characteristics of this sample have been previously reported (4), but overall, the sample was predominantly white (e.g., one subject endorsed a Native American ethnicity) and alcohol dependent [86.2% (n=25) of WRG and 100.0% (n=7) GDC women]. The mean age for women enrolled in GDC was 58.3 years (SD=7.18) and 45.0 years (SD = 10.73) for women in WRG. There were no other statistically significant differences in baseline characteristics.
Over one-third of participants were diagnosed with other current co-occurring psychiatric disorders, including mood disorders (i.e., 37.9% WRG and 42.9% GDC), anxiety disorders (i.e., 31.0% WRG and 42.9% GDC), eating disorders (i.e., 3.4% WRG and 0.0% GDC), other Axis I disorder (i.e., 3.4% WRG and 0.0% (GDC), and Axis II personality disorders (i.e., 34.5% all WRG, 37.5% pilot WRG, and 57.1% GDC). Approximately three-fourths of participants were diagnosed with lifetime co-occurring psychiatric disorders including mood disorders (75.9% WRG and 85.7% GDC), anxiety disorders (i.e., 44.8% WRG and 42.9% GDC), eating disorders (i.e., 20.7% WRG and 0.0% GDC), and other Axis I disorders (i.e., 3.4% WRG and 0.0% GDC). None of these differences were statistically significant.
Psychiatric Symptoms and Outcome
The mean BSI score for women in the WRG condition was 36.17 (sd= 28.88) and for women in the GDC was 42.43 (sd= 35.08), which was not significantly different (t(34)=0.49, p=0.62). The analysis of baseline psychiatric severity (BSI) as a moderator of outcomes assessed during treatment and in the 6 months post-treatment found a significant 3-way interaction effect of treatment condition, time, and BSI on days of any substance use (F(1,194)=8.31, p=.0044) and number of drinking days per month (F(1,194)=10.42, p=.0015) (see Table 1).
Table 1.
Tests of Fixed Effects: Baseline BSI and BDI × Group × Time
| Test of Fixed Effects for Baseline BSI × Group × Time | |||
|---|---|---|---|
| During-Treatment (months 1–3) Group contrasts for patients with high baseline BSI | t | DF | p |
| Days of any substance use | 2.37 | 194 | .019 |
| Drinking days per month | 1.77 | 194 | .078 |
| Post-treatment Follow-up (months 4–9) Group contrasts for patients with high baseline BSI | |||
| Days of any substance use | 4.22 | 194 | <.0001 |
| Drinking days per month | 4.11 | 194 | <.0001 |
| Test of Fixed Effects for Baseline BDI × Group × Time | |||
| During-Treatment (months 1–3) Group contrasts for patients with high baseline BDI | |||
| Days of any substance use | .14 | 194 | .893 |
| Drinking days per month | .05 | 194 | .961 |
| Post-treatment follow-up (months 4–9) Group contrasts for patients with high baseline BDI | |||
| Days of any substance use | 1.76 | 194 | .080 |
| Drinking days per month | 2.09 | 194 | .036 |
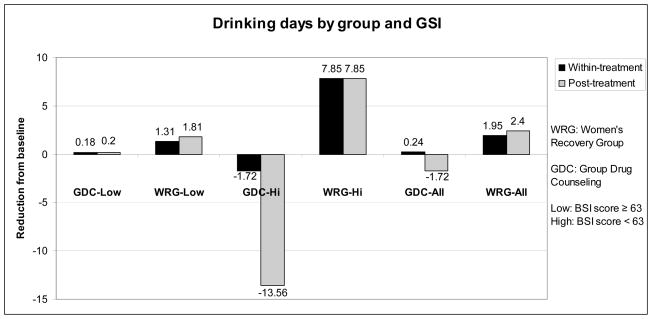
Specifically, during treatment, women in WRG with high baseline psychiatric symptom severity (i.e. a BSI score of 63 or greater) were more likely than women in GDC with high BSI scores to reduce their drinking days (t(194)=1.77, p=.078) and days of any substance use (t(194)=2.37, p=.019). The magnitude and significance of the reductions were even greater in the post-treatment phase; women in WRG with high BSI scores endorsed significantly fewer drinking days (t(194)=4.11, p<.0001) and days of any substance use post-treatment (t(194)=4.22, p<.0001) than women with high BSI scores in GDC (see Figure 1).
Figure 1.
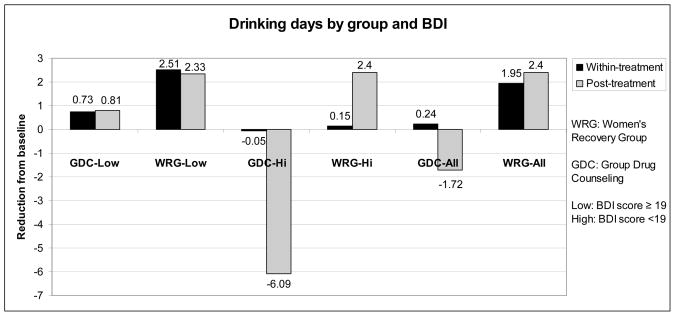
There was also a significant 3-way interaction effect of treatment condition, time, and baseline BDI on days of any substance use (F(1,194)=11.29, p=.0009) and number of drinking days per month (F(194)=13.17, p=.0004) (see Table 1). During treatment, women with high levels of depression (i.e. a BDI score of 19 or above) in WRG demonstrated similar substance use reductions in comparison to their GDC counterparts; in the post-treatment phase, however, women with high levels of depression in WRG endorsed significantly fewer drinking days (t(194)=2.09, p = .036) and a trend toward fewer days of any substance use (t(194)=1.76, p=.080) compared to women with high BDI scores enrolled in GDC (see Figure 2).
Figure 2.
DISCUSSION
In this exploratory study, women with high psychiatric symptom severity made greater reductions in substance use at the end of 12 weeks of group therapy treatment when they were assigned to WRG, a single-gender, women-focused treatment, as opposed to a mixed gender GDC treatment. Perhaps even more striking, however, is that substance abuse treatment outcomes for women with high psychiatric severity enrolled in WRG continued to improve in the six month post-treatment follow-up compared with those enrolled in GDC.
While substance abuse treatment in an all-women’s group context has been proposed to be more effective for women (1) (18) this study is unique in that it examines treatment outcomes for women enrolled in either all-women’s or mixed-gender group treatment who are heterogeneous with respect to their primary substance of abuse and co-occurring other psychiatric disorders (4). Consistent with the general population of treatment-seeking women (19), a significant proportion of women in our sample had co-occurring mood, anxiety, and personality disorders. Our findings are consistent with prior research demonstrating that psychiatric symptoms moderate drinking outcomes in treatment-seeking women (19, 20) and alcohol consumption in women in community based samples (21, 22). Sex-specific effects of depression on elevated alcohol consumption have been demonstrated for women in the community (21, 22), for women at treatment entry (23), and for post-treatment outcomes in women with alcohol dependence (5). In addition, high psychiatric severity was predictive of decreased retention of women in substance abuse outpatient treatment (24) and treatment retention may be an especially important predictor of substance abuse outcome among women (1).
The WRG provides education about sex-specific factors in women’s recovery including the role of co-occurring psychiatric disorders, especially mood and anxiety disorders, in maintaining abstinence from substances. In particular, the WRG directly supports women’s self-care including seeking effective treatment for other psychiatric disorders (4). Enhanced comfort experienced by women in all-women’s group treatment has been proposed as a mechanism to enhance treatment outcomes (25, 26). The continued improvement of women with high psychiatric severity in WRG may be attributable to increased coping skills (27) and enhanced self-efficacy (28) achieved by these women through skills learned and enhanced support in an all-women’s context. This study hypothesized synergy between women-focused content and all-female group composition and we are unable to differentiate the relative effects of these two elements on treatment outcome. Future research will be necessary to elucidate the relative contributions of these elements.
This study is limited by its small sample size. It is also important to note that only a small proportion of women had a primary drug use disorder and the findings may not generalize to women with other clinical or demographic characteristics. Nevertheless, we are aware of no research examining potential moderators of differential treatment outcomes for women participating in women-only treatment groups versus mixed-gender groups. As such, our findings extend previous reports regarding the treatment of women with substance use disorders and provide the basis for future hypothesis driven research (29). While further research is necessary to confirm the results described here, the identification of clinical characteristics of women most likely to benefit from single gender treatment approaches represents an important step in improving SUD treatment for women. In addition, WRG may prove to be appealing to clinical programs managing scarce resources in that it may be appropriate for women with a range of co-occurring psychiatric disorders and symptoms as well as different primary substances of abuse.
Acknowledgments
Support for this study was provided by the National Institute on Drug Abuse R01 DA015434 (SFG) and K24 DA019855 (SFG)
Footnotes
Presented in part at the annual meeting of the College of Problems on Drug Dependence, Quebec City, Canada, June 19, 2007
Works Cited
- 1.Greenfield S, Brooks A, Gordon S, Green C, Kropp F, McHugh R, Lincoln M, Hien D, Miele G. Substance abuse treatment entry, retention, and outcome in women: A review of the literature. Drug Alcohol Depend. 2007;86(1):1–21. doi: 10.1016/j.drugalcdep.2006.05.012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Kauffman E, Dore MM, Nelson-Zlupko L. The role of women’s therapy groups in the treatment of chemical dependence. Am J Orthopsychiatry. 1995;65(3):355–63. doi: 10.1037/h0079657. [DOI] [PubMed] [Google Scholar]
- 3.Benishek LA, Bieschke KJ, Staffelmayr BE, Mavis BE. Gender differences in depression and anxiety among alcoholics. J Subst Abuse. 1992;4(3):235–245. doi: 10.1016/0899-3289(92)90032-s. [DOI] [PubMed] [Google Scholar]
- 4.Greenfield S, Trucco E, McHugh R, Lincoln M, Gallop R. The Women’s Recovery Group study: A stage I trial of women-focused group therapy for substance use disorders versus mixed-gender Group Drug Counseling. Drug Alcohol Depend. 2007;90:39–47. doi: 10.1016/j.drugalcdep.2007.02.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Greenfield S, Weiss R, Muenz L, Vagge L, Kelly J, Bello L, Michael J. The effect of depression on return to drinking: A prospective study. Arch Gen Psychiatry. 1998;55(3):259–265. doi: 10.1001/archpsyc.55.3.259. [DOI] [PubMed] [Google Scholar]
- 6.Greenfield S, Weiss R, Kelly J, Bello L, Muenz L, Michael J. Gender differences in 12-month course of depression and anxiety symptoms. Harvard Consolidated Department of Psychiatry Research Day; Boston. 1996. [Google Scholar]
- 7.Hernandez-Avila CA, Rounsaville BJ, Kranzler HR. Opioid-, cannabis- and alcohol-dependent women show more rapid progression to substance abuse treatment. Drug Alcohol Depend. 2004;74(3):265–72. doi: 10.1016/j.drugalcdep.2004.02.001. [DOI] [PubMed] [Google Scholar]
- 8.Lex B. Gender differences and substance abuse. In: Mello N, editor. Advances in Substance Abuse: Behavioral and Biological Research. Vol. 4. Jessica Kingsley; London: 1991. pp. 225–96. [Google Scholar]
- 9.Crits-Christoph P, Siqueland L, Blaine J, Frank A, Luborsky L, Onken L, Muenz L, Thase M, Weiss R, Gasfriend D, Woody G, Barber J, Butler S, Daley D, Salloum I, Bishop S, Najavits L, Lis J, Mercer D, Griffin M, Moras K, Beck A. Psychosocial treatments for cocaine dependence: Results of the National Institute on Drug Abuse Collaborative Cocaine Treatment Study. Arch Gen Psychiatry. 1999;56(6):493–502. doi: 10.1001/archpsyc.56.6.493. [DOI] [PubMed] [Google Scholar]
- 10.Sobell LC, Sobell MB, Litten RZ, Allen JP. Measuring Alcohol Consumption: Psychosocial and Biochemical Methods. Humana Press; 1992. Timeline follow-back: A technique for assessing self-reported alcohol consumption; pp. 41–72. [Google Scholar]
- 11.Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J. An inventory for measuring depression. Arch Gen Psychiatry. 1961;4:561–571. doi: 10.1001/archpsyc.1961.01710120031004. [DOI] [PubMed] [Google Scholar]
- 12.Derogatis LR. Brief Symptom Inventory. Administration, Scoring, and Procedures Manual. National Computer Systems, Inc; Minneapolis, MN: 1993. [Google Scholar]
- 13.Schwarz CJ. The MIxed-Model ANOVA: The truth, the computer packages, the books. The American Statistician. 1993;47:48–59. [Google Scholar]
- 14.Keselman HJ, Algina J, Kowalchuk RK, Wolfinger RD. A comparison of two approaches for selecting covariance structures in the analysis of repeated measurements. Communications in Statistics: Simulations and Computation. 1998;27:591–604. [Google Scholar]
- 15.Rosnow RL, Rosenthal R. If you’re looking at the cell means, you’re not looking at only the interaction (unless all main effects are zero) Psychol Bull. 1991;110(3):574–576. [Google Scholar]
- 16.Verbeke G, Molenberghs G. Linear Mixed Models for Longitudinal Data. Springer-Verlag; New York: 2000. [Google Scholar]
- 17.DeRubeis RJ, Hollon SD, Amsterdam JD, Shelton RC, Young PR, Salomon RM, O’Reardon JP, Lovett ML, Gladis MM, Brown LL, Gallop R. Cognitive Therapy vs Medications in the Treatment of Moderate to Severe Depression. Arch Gen Psychiatry. 2005;62(4):409–416. doi: 10.1001/archpsyc.62.4.409. [DOI] [PubMed] [Google Scholar]
- 18.Hien DA, Cohen LR, Miele GM, Litt LC, Capstick C. Promising treatments for women with comorbid PTSD and substance use disorders. Am J Psychiatry. 2004;161(8):1426–1432. doi: 10.1176/appi.ajp.161.8.1426. [DOI] [PubMed] [Google Scholar]
- 19.Zilberman ML, Tavares H, Blume SB, el-Guebaly N. Substance use disorders: Sex differences and psychiatric comorbidities. The Canadian Journal of Psychiatry/La Revue canadienne de psychiatrie. 2003;48(1):5–13. doi: 10.1177/070674370304800103. [DOI] [PubMed] [Google Scholar]
- 20.Hasin DS, Tsai W, Endicott J. The effects of major depression on alcoholism: Five-year course. Am J Addict. 1996;5(2):144–155. doi: 10.1016/0165-0327(96)00068-7. [DOI] [PubMed] [Google Scholar]
- 21.Dixit AR, Crum RM. Prospective study of depression and the risk of heavy alcohol use in women. Am J Psychiatry. 2000;157(5):751–758. doi: 10.1176/appi.ajp.157.5.751. [DOI] [PubMed] [Google Scholar]
- 22.Wang J, Patten SB. A Prospective Study of Sex-Specific Effects of Major Depression on Alcohol Consumption. The Canadian Journal of Psychiatry/La Revue canadienne de psychiatrie. 2001;46(5):422–425. doi: 10.1177/070674370104600507. [DOI] [PubMed] [Google Scholar]
- 23.Pettinati HM, Pierce JD, Jr, Wolf AL, Rukstalis MR, O’Brien CP. Gender differences in comorbidly depressed alcohol-dependent outpatients. Alcohol Clin Exp Res. 1997;21(9):1742–1746. [PubMed] [Google Scholar]
- 24.Mertens JR, Weisner CM. Predictors of substance abuse treatment retention among women and men in an HMO. Alcoholism, Clinical and Experimental Research. 2000;24(10):1525–33. [PubMed] [Google Scholar]
- 25.Swift W, Copeland J. Treatment needs and experiences of Australian women with alcohol and other drug problems. Drug Alcohol Depend. 1996;40(3):211–9. doi: 10.1016/0376-8716(95)01209-5. [DOI] [PubMed] [Google Scholar]
- 26.Nelson-Zlupko L, Dore M, Kauffman E, Kaltenbach K. Women in recovery: Their perceptions of treatment effectiveness. J Subst Abuse Treat. 1996;13(1):51–59. doi: 10.1016/0740-5472(95)02061-6. [DOI] [PubMed] [Google Scholar]
- 27.Carroll KM, Rounsaville BJ, Nich C, Gordon LT, Wirtz PW, Gawin F. One-year follow-up of psychotherapy and pharmacotherapy for cocaine dependence: delayed emergence of psychotherapy effects. Arch Gen Psychiatry. 1994;51(12):989–997. doi: 10.1001/archpsyc.1994.03950120061010. [DOI] [PubMed] [Google Scholar]
- 28.Greenfield SF, Hufford MR, Vagge LM, Muenz LR, Costello ME, Weiss RD. The relationship of self-efficacy expectancies to relapse among alcohol dependent men and women: A prospective study. J Stud Alcohol. 2000;61(2):345–351. doi: 10.15288/jsa.2000.61.345. [DOI] [PubMed] [Google Scholar]
- 29.Kraemer HC, Mintz J, Noda A, Tinklenberg J, Yesavage JA. Caution Regarding the Use of Pilot Studies to Guide Power Calculations for Study Proposals. Arch Gen Psychiatry. 2006;63(5):484–489. doi: 10.1001/archpsyc.63.5.484. [DOI] [PubMed] [Google Scholar]