Abstract
An 18-year-old Asian girl was referred to the nephrology unit with rapidly progressive renal failure. At the age of 15 she was diagnosed as having systemic lupus erythematosus but had defaulted treatment. Her renal functions improved with cyclophosphamide pulse treatment but she continued to have central nervous system vasculitis, gastrointestinal vasculitis and opportunistic infections making her a unique and challenging case of systemic lupus erythematosus.
BACKGROUND
This case report highlights how difficult it can be to manage a multisystem disorder and how prognosis can be improved with multidisciplinary specialist management. Also, it describes some unique features observed in this patient.
CASE PRESENTATION
An 18-year-old girl of Pakistani origin was seen at the tertiary care renal unit with fluid overload and worsening renal functions (creatinine rising from 77 μmol/l to 225 μmol/l in 3 days). She was diagnosed as having systemic lupus erythematosus (SLE). Her symptoms began at the age of 15 when she presented to a rheumatologist with tiredness, joint pains and loss of weight. Distal interphalangeal, proximal interphalangeal, wrist, shoulder and ankle joints were symmetrically involved and appeared clinically normal. She was a product of a consanguineous marriage and had a strong family history of SLE with both male and female members affected in the past four generations. A diagnosis of SLE was confirmed based on clinical features and positive antinuclear antibodies and anti-double-stranded DNA antibodies. She showed a good response to prednisolone and methotrexate but as an adolescent she defaulted on treatment and opted for homeopathic treatment. Symptoms soon recurred and she was readmitted with shortness of breath and rapidly progressive renal failure. She had an erythrocyte sedimentation rate of 131 mm/h, raised immunoglobulins and reduced complement levels. Serum autoantibody studies showed positive antinuclear antibodies, anti-double-stranded-DNA antibodies and antiphospholipid antibodies. Anti-extractable nuclear antigen antibodies and antineutrophil cytoplasmic antibodies were negative. A renal biopsy showed a medium vessel vasculitis. Her renal functions improved with cyclophosphamide/methylprednisolone pulse therapy but she developed generalised muscular weakness and inability to walk. An obvious thought was mononeuritis multiplex but a magnetic resonance angiogram of the brain showed tiny punctuate infarcts suggestive of CNS vasculitis. On the 10th day of starting immunosuppressive treatment she developed acute respiratory distress syndrome secondary to pneumonitis caused by parainfluenza virus and she required ventilation.
It was difficult to provide further pulse therapy because of an ongoing chest infection and being on ventilator. However, she was finally weaned off the ventilator but developed severe watery diarrhoea, the cause of which remained unknown until a chest x-ray revealed gas under the diaphragm. There were no clinical signs of peritonitis presumably because of the high-dose steroids she was receiving. Investigations revealed intestinal perforation at rectosigmoid junction. She required total colectomy and ileostomy. Histology of the colon showed widespread vascular changes affecting large, medium and small sized arteries in keeping with lupus vasculitis. Luckily she pulled through this major surgery but developed neutropenia and stoma site infection. It was treated with antibiotics and granulocyte colony-stimulating factor. With good high dependency and multidisciplinary care she made a steady recovery and was finally sent for rehabilitation with the plan to continue cyclophosphamide pulse therapy for a year. The results of IV cyclophosphamide were promising with her creatinine improving to 76 μmol/l but her future is difficult to predict as she has poor prognostic factors. It is worth mentioning that with simple prophylactic measures she did not develop deep vein thrombosis despite being lupus anticoagulant positive and bed ridden.
DIFFERENTIAL DIAGNOSIS
Polyarteritis nodosa causing medium vessel vasculitis.
Catastrophic antiphospholipid syndrome causing multiple arterial thromboses.
TREATMENT
Corticosteroids±cytotoxic/immunosuppressive agents.
OUTCOME AND FOLLOW-UP
Although the patient showed a good response to treatment, the disease is likely to run a remitting and relapsing course.
DISCUSSION
This case of SLE had several uncommon features.
Age of onset: peak age at diagnosis is 30–40 years.
Strong family history: only 10% of relatives of patients with SLE are affected.
Medium vessel vasculitis: vasculitis in SLE is usually limited to small vessels alone.1
Multi-organ vasculitis: reports on SLE with medium vessel vasculitis generally describe involvement of a single vascular bed.2
Intestinal vasculitis in SLE is quite rare. In the literature only two similar cases are reported.2
LEARNING POINTS
SLE is a heterogeneous disorder and can take a variety of clinical and pathological forms.
Patients with SLE and renal failure may have a pathological finding other than lupus nephritis and hence a thorough renal biopsy examination is absolutely essential.
Medium vessel vasculitis can occasionally be seen in a patient with SLE; when present it is associated with a higher incidence of visceral vasculitis.3
Pulsed cyclophosphamide has been the treatment of choice for patients with moderate to severe lupus nephritis.4 However, recent randomised open-label trials have proved mycophenolate mofetil to be superior to cyclophosphamide in achieving remission of lupus nephritis and appear to be better tolerated.5
SLE in its severe form presents a therapeutic challenge, treatment being associated with serious and potentially life-threatening side-effects. None the less, good multidisciplinary specialist care can improve the prognosis.
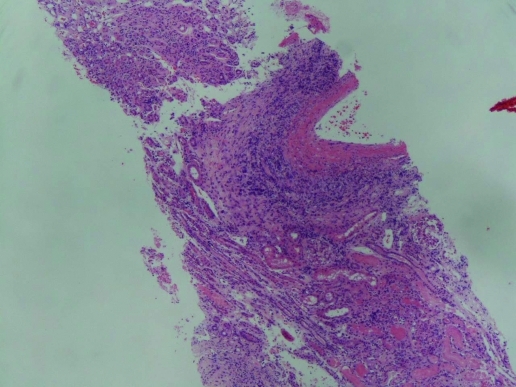
Figure 1.
Transmural neutrophilic infiltration of a medium-sized artery.
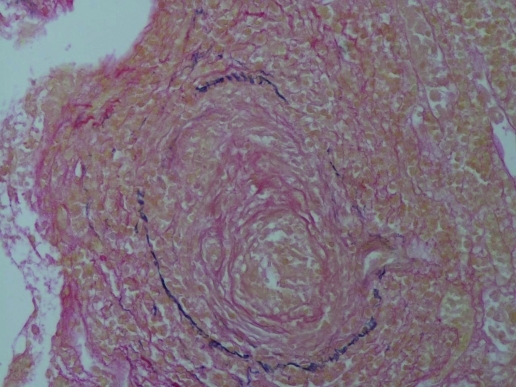
Figure 2.
Glomerulus is spared.
Acknowledgments
Patient and her parents for giving her consent.
Footnotes
Competing interests: none.
Patient consent: Patient/guardian consent was obtained for publication.
REFERENCES
- 1.Kumar N, Choudhary N, Agarwal G, et al. Extensive medium vessel vasculitis with SLE: an unusual association. J Clin Rheumatol 2007; 13: 140–2 [DOI] [PubMed] [Google Scholar]
- 2.Grimbacher B, Huber M, Von Kempis J, et al. Successful treatment of gastrointestinal vasculitis due to systemic lupus erythematosus with intravenous pulse cyclophosphamide: a clinical case report and review of literature. Br J Rheumatol 1998; 37: 1023–8 [DOI] [PubMed] [Google Scholar]
- 3.Ramos-casals M, Nardi N, Lagrutta M, et al. Vasculitis in systemic lupus erythematosus: prevalence and clinical characteristics in 670 patients. Medicine (Baltimore) 2006; 85: 95–104 [DOI] [PubMed] [Google Scholar]
- 4.Takada K, Illei GG, Boumpas DT. Cyclophosphamide for the treatment of systemic lupus erythematosus. Lupus 2001; 10: 154–61 [DOI] [PubMed] [Google Scholar]
- 5.Ginzler EM, Dooley MA, Aranow C, et al. Mycophenolate mofetil or intravenous cyclophosphamide for lupus nephritis. N Engl J Med 2005; 353: 2219–28 [DOI] [PubMed] [Google Scholar]