Abstract
An increased risk of tuberculosis has been documented in humans treated with tumor necrosis factor alpha (TNF) neutralizing agents. In murine models, impaired signaling by TNF caused exacerbation of both acute and chronic infection associated with aberrant granuloma formation and maintenance. The non-human primate model of tuberculosis provides an opportunity to study immune modulation in the setting of TNF neutralization during primary and latent tuberculosis. Administration of TNF neutralizing agents prior to M. tuberculosis infection resulted in fulminant and disseminated disease by 8 weeks post-infection. Neutralization of TNF in latently infected cynomolgus macaques caused reactivation in a majority of animals as determined by gross pathology and bacterial burden. A spectrum of dissemination was noted including extrapulmonary disease. Surprisingly, monkeys who developed primary and reactivation tuberculosis after TNF neutralization had similar granuloma structure and composition compared to active control monkeys. TNF neutralization was associated with increased IL-12, decreased CCL4, increased chemokine receptor expression and reduced mycobacteria-specific IFN-γ production in blood but not to the affected mediastinal lymph nodes. Finally, the first signs of reactivation often occurred in thoracic lymph nodes. These findings have important clinical implications for determining the mechanism of TNF-neutralization-related tuberculosis.
Abstract: TNF, tuberculosis, non-human primate
Introduction
In humans, an increased incidence of tuberculosis (presumably reactivation of latent infection) is observed in patients receiving TNF neutralizing agents for inflammatory conditions [1, 2]. The granuloma, the histopathological hallmark of M. tuberculosis infection, represents both an immunological and physical barrier by which to contain the infection. Poor granuloma structure has been associated with disseminated disease [3]. Tumor necrosis factor alpha (TNF) plays a critical role in control of acute and chronic M. tuberculosis infection in murine models, characterized by disorganized granuloma structure contributing to poor control of infection [4, 5]. Other mechanisms by which TNF affects the response to M. tuberculosis include macrophage activation [6], apoptosis [7, 8], chemokine [9, 10] and adhesion molecule expression [11, 12]. These patients often had few clinical signs of tuberculosis, leading to difficulty in diagnosis and ultimately poor outcome. There was a striking predominance of extrapulmonary and disseminated tuberculosis unlike the more typical (pulmonary) pattern of reactivation [13]. As TNF-neutralizing agents are introduced in countries with higher endemic rates of tuberculosis, the potential risk of tuberculosis, both primary and reactivation, may be greatly increased.
The standard murine models used for study of tuberculosis are inbred strains, with varying patterns of resistance and pathology [14]. While the mouse is crucial for investigating immune responses and pathogenesis, there are two major limitations to this model. First, unlike humans, mice do not establish latent infection, but instead develop chronic disease and will eventually die of progressive primary tuberculosis. Second, the common inbred strains of mice produce granulomas that are best termed granulomatous infiltrations: collections of macrophages and lymphocytes that lack the architectural organization seen in humans. No mouse strains generate the spectrum of granulomas observed in humans.
Here we demonstrate that cynomolgus macaques receiving TNF neutralizing agents had uncontrolled and disseminated disease by 8 weeks after M. tuberculosis infection. TNF neutralizing agents also induced a high rate of reactivation tuberculosis among latently infected macaques [15]. Extrapulmonary disease occurred in both acute and reactivation tuberculosis. In sharp contrast to murine data, normal granuloma architecture, similar to that seen in active tuberculosis, was observed in TNF-neutralized monkeys, suggesting that mechanisms of TNF-associated susceptibility to tuberculosis may be different than in murine models [16].
Materials and Methods
Animals
Cynomolgus macaques (Macacca fasicularis) ≥ 4 years of age were used (Labs of Virginia Inc. [Yemassee, SC], Shin Nippon Biomedical Laboratory [Summerville, SC], Valley Biosystems [Sacramento, CA], Covance [Vienna, VA]) within a biosafety level 3 primate facility [17]. All animal protocols and procedures were approved by University of Pittsburgh’s Institutional Animal Care and Use Committee.
Monkeys were infected with M. tuberculosis (Erdman strain) via bronchoscopic instillation of ~25 colony forming units to the lower lung lobe [17]. Infection was confirmed by Tuberculin skin test conversion [18] and/or lymphocyte proliferation assay. Serial clinical, microbiologic, immunologic and radiographic examinations were performed [15]. Based on defined clinical criteria [15], monkeys were classified as having latent or active disease at 6–8 months post infection. Monkeys with active disease have abnormal chest radiographs, M. tuberculosis growth from gastric aspirate or bronchoalveolar lavage, cough, weight loss and/or elevated erythrocyte sedimentation rate beyond 3 months post-infection [15,19]. In contrast, latently infected monkeys have no radiographic, microbiologic, or clinical signs of disease [15,19]. Historical latent and active disease control monkeys were used for comparison (some data on these monkeys were previously published)[19].
Anti-TNF Agents
For acute infections, monkeys were given adalimumab (Humira®, Abbott Labs, Abbott Park, IL), a humanized monoclonal antibody obtained via pharmacy, at 4mg/kg subcutaneously, two days prior to infection and every 10 days until necropsy. This dose is ~1.8 fold higher than loading dose for a human with Crohn’s disease. Latently infected monkeys were given either an inhibitor of soluble TNF, recombinant methionyl human soluble TNF-type 1 receptor (p55-TNFR1) (Amgen, Inc, Thousand Oaks, CA) [20] (monkeys 7104, 6604) or adalimumab (monkeys 17905, 9605, 16605, 10605, 12102, 23802, 25503). Adalimumab was administered every 10 days for 4–8 weeks. p55-TNFR1 was given at 10 mg/kg subcutaneously weekly for 19 weeks. Latent control monkeys were given saline or no treatment.
Immunological assays
Immunogenicity against TNF agents
Monkey derived antibody against the humanized neutralizing agent was assayed by ELISA. Plates were coated with the anti-TNF agent and serial plasma dilutions used to estimate the anti-neutralizing agent present (http://www.bidmc.harvard.edu/display.asp?node_id=3770). To determine if the macaque-derived antibody neutralized the effects of the anti-TNF agent, a functional assay was developed using WEHIvar 13 cells [21], with the following conditions: positive control (recombinant human TNF (rhTNF), 10–10,000 pcg/ml), negative control (media alone), rhTNF (10–10,000 pcg/ml) pre-incubated with monkey serum (dilutions 1:100 and 1:1000) and adalimumab (10ug/ml), as well as rhTNF (10–10,000 pcg/ml) with adalimumab (10ug/ml). Sera from control monkeys were compared to those who received adalimumab. In this assay, no biologically active TNF could be detected after adalimumab and rhTNF were added together, and the presence of anti-adalimumab antibody would neutralize these effects resulting in detectable levels of TNF by WEHI assay.
IFN-γ enzyme-linked immunospot assay (ELISPOT)
Mycobacteria-specific production of IFN-γ was measured by ELISPOT with peripheral blood mononuclear cells (PBMC) and bronchoalveolar lavage (BAL) cells at baseline and serial intervals, and at necropsy. Briefly, PBMC or BAL cells were co-cultured with autologous PBMC-derived dendritic cells and mycobacterial antigen peptide pools [17], and the frequency of IFN-γ producing cells measured (spot forming units (SFU) per well).
Assays at necropsy
At necropsy, monkeys were maximally bled, terminal BAL performed, and euthanized with pentobarbital and phenytoin (Beuthanasia, Schering-Plough). Gross pathologic findings were described by a board certified veterinary pathologist (E.K.). To quantify gross pathologic disease, we developed a necropsy score worksheet in which tuberculosis disease from each lung lobe, lymph node and visceral organ is recorded and enumerated and an overall score determined [19]. Points are given for number, size and pattern of granulomas distributed in each lung lobe, mediastinal lymph node and other organs [19]. Representative sections of each tissue were placed in formalin for histology or homogenized into single cell suspensions for immunologic studies, flow cytometric analysis and bacterial burden as described previously [15, 17].
Histology
Microscopic histopathology of tissue sections was reviewed by a veterinary pathologist (E.K.) with specific focus on granuloma characteristics: overall architectural appearance, type of granuloma (caseous [local organization of lymphocytes and epithelioid macrophages with a central core of eosinophilic protein, caseum], non-necrotizing (solid) [regional area of inflammatory cells like caseous granulomas but with a central area of macrophages instead of caseum], suppurative [a caseous granuloma with >50% of caseous area filled with neutrophils]), distribution pattern (focal, multifocal, coalescing, invasive) and cellular composition [19]. Microscopic histopathology was compared blind between acute, latent, active and TNF neutralized groups.
ELISPOT and phenotypic expression
At necropsy, PBMCs and cells from BAL, granulomatous and non-granulomatous lung tissue, and mediastinal lymph nodes were used in for ELISPOT assays [15, 17]. Flow cytometry using markers for T cells (CD3, CD8, CD4), T cell activation (CD69, CD29), chemokine receptors (CCR5, CXCR3) and macrophages (CD14, CD11b, CD11c) [17], was performed using CellQuest Software (BD Immunocytometry systems, San Jose, CA) and analyzed with Flow Jo software (Treestar, Inc, Ashland, OR).
Cytokine analysis of tissue homogenates
Luminex-Beadlyte human multi-cytokine detection system (Upstate, Millipore, Billerica, MA) was performed on tissue homogenates of lung and mediastinal lymph node per manufacturer’s recommendation[22].
Bacterial burden
Bacterial burden from BAL (monthly and at necropsy) and 20–40 tissue samples at necropsy was serially diluted, plated on 7H10 media and colony forming units (CFU) enumerated at 21 days [17]. A “CFU score” was derived (as a summation of the log transformation of CFU/gram of each sample obtained from each tissue) as a measure of overall bacterial burden [19]. Bacterial dissemination was reflected as the percentage of samples that grew M. tuberculosis from tissues obtained at necropsy. These two methods of bacterial burden were validated to distinguish latent and active disease monkeys [19].
Statistical analysis
Pair-wise analysis between TNF neutralized and control monkeys was performed using Student’s T test (normal distributed data) and Mann-Whitney (non-normal data). Statistical significance was designated as p –value ≤ 0.05. Statistical analysis was performed on GraphPad PRISM software (GraphPad Software, Inc, San Diego, CA). When more than 2 groups were compared, one-way ANOVA analysis was used with Bonferroni post-hoc analysis or other non-parametric equivalent.
Results
TNF is important for control of initial M. tuberculosis infection
Clinical parameters
To address whether TNF was necessary for control of initial infection, control (n=4) and TNF neutralized (n=4) groups were euthanized at 8 weeks post-infection (p.i.). Early indications of disease progression among the anti-TNF group included persistent growth of M. tuberculosis from BAL or gastric aspirate (monkeys 2107 and 2807), elevated ESR (monkeys 2807 and 17107) and development of bilateral lower lobe pneumonia (monkey 2107). Control monkeys had no microbiologic or radiographic evidence of disease. Elevated ESR was noted in 2 anti-TNF monkeys (2107: 30.5mm and 2807:16 mm [Normal range 0–2.0 mm]) at necropsy.
TNF neutralization results in disseminated disease during acute infection with intact granulomas
At necropsy, three of four adalimumab-treated monkeys had more severe disease compared to control monkeys (Figure 1). Average necropsy scores were higher in adalimumab-treated monkeys compared to controls, reflecting increased frequency of lesions in lung lobes and spread of disease to liver and spleen, although this did not reach statistical significance because one monkey was apparently unaffected by anti-TNF treatment (Figures 1, 2). Gross evidence of invasive tuberculous pneumonia was noted in monkeys 2807 and 2107. Control monkeys had enlarged, granulomatous lymph nodes and fewer grossly visible lung granulomas.
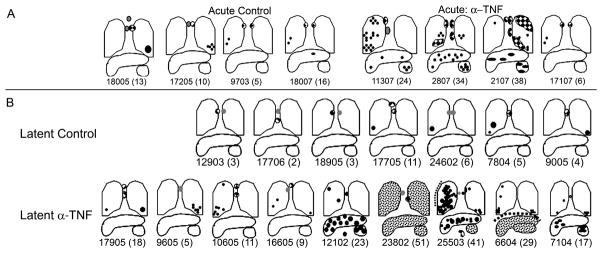
Figure 1.
TNF is necessary to control initial and latent M. tuberculosis infection. A) Gross disease pathology in macaques infected with low dose M. tuberculosis with or without TNF neutralizing antibody for 8 weeks. Control monkeys show granulomas (black circles) localized to a single lung lobe and mediastinal lymph node enlargement (grey circles) with or without granulomas (checkered circles). In 3 of 4 monkeys treated with anti-TNF reagent, aggressive and disseminated disease was observed including multiple granulomas in lungs, liver and spleen and tuberculous pneumonia (checkered areas in the lungs). B) Latently infected monkeys have limited gross pathology: a few granulomas in the lung, and mediastinal lymph node enlargement with or without granulomas. In contrast, gross pathology of latent monkeys treated with TNF neutralizing agents ranged from normal to severe disseminated disease. Liver and spleen (monkeys 12102, 23802, 25503, 6604 and 7104) had multiple granulomas to miliary disease (speckled pattern). Disseminated miliary disease was observed in all lung lobes, liver and spleen of 23802. Multiple granulomas were observed on the diaphragm (dotted line) of 6604 and extensive pleural disease (dotted line) in 25503. Individual monkey identifiers are below each schema with necropsy score in parentheses.
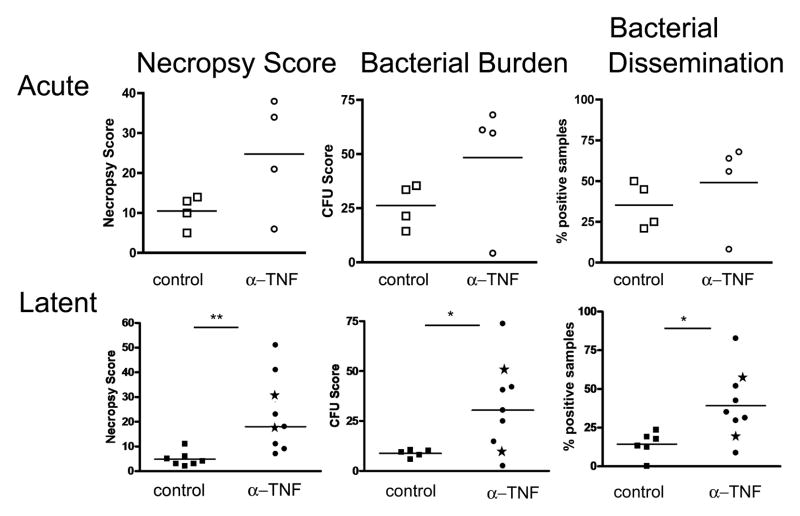
Figure 2.
Gross pathology and bacterial burden of acute and latent control and TNF neutralized monkeys. (A) During acute infection, gross pathology as quantified by necropsy score appeared greater among TNF neutralized (open circles) compared to control monkeys (open squares) though this did not reach statistical significance. Overall bacterial burden (CFU score) and distribution of bacterial burden (percent of positive samples) appeared higher in anti-TNF treated monkeys, but not statistically different due to variability in the groups. (B) Latently infected monkeys treated with TNF neutralization agents (closed circles) results in greater gross pathology, bacterial burden, and dissemination (percent positive samples) compared to latent control monkeys (closed squares) (Mann Whitney or Student’s T test). Latently infected monkeys treated with adalimumab are indicated by solid circles whereas monkeys treated with p55-TNFR1 are indicated in solid stars. (* is p<0.05, ** is p<0.01).
The architecture of individual granulomas (caseous and non-necrotizing) in mediastinal lymph nodes and lungs was indistinguishable between control (Figure 3A,B) and TNF neutralized groups (Figures 3C-F) by microscopic histopathology. However, overall the TNF neutralized group had a more aggressive and invasive disease pattern with granuloma invasion into nearby vessels and airways. This pattern was not observed among control monkeys 5–8 weeks post-infection, but has been observed in monkeys with active tuberculosis, which usually takes >3 months to develop. Despite normal granuloma formation with TNF neutralization, function of the granulomas was apparently impaired, since disease was much more aggressive and disseminated.
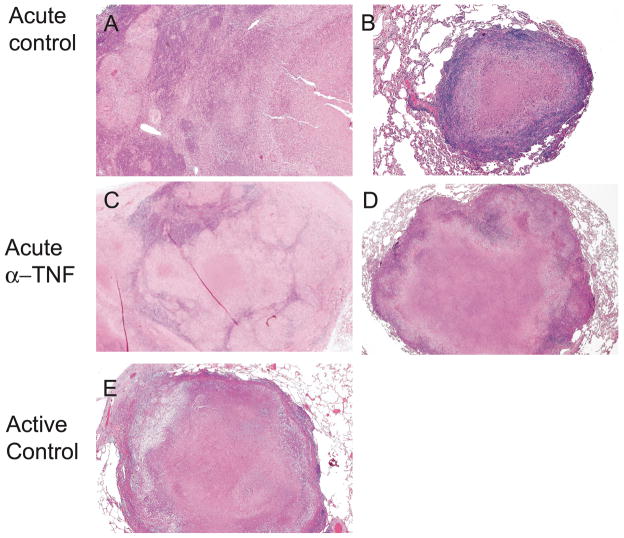
Figure 3.
More aggressive disease is seen in TNF neutralized monkeys with normal granuloma structure. (A) Caseous granuloma with adjacent non-necrotizing granulomas (left side) present in the hilar lymph node of an 8 week control monkey (18007), 5×; (B) Caseous granuloma in the accessory lobe of acute control monkey (9703) consisting of a central area of eosinophilic proteinaceous material (caseum) surrounded by epithelioid macrophages and the lymphocytes along the outmost periphery, 5×; (C) Massive effacement of carinal lymph node with both caseous and non-necrotizing granulomas in a TNF neutralized monkey 8 weeks after infection, 2×; (D) Large caseous granuloma in the lung of TNF neutralized monkey (2807) with normal architecture, 2×; (E) Large caseous granuloma in the lung lobe of a monkey with active tuberculosis. The architectural structure of the granuloma appears similar to granulomas observed in monkeys treated with TNF neutralizing agents, 2×. All slides stained with H&E.
Bacterial burden
Adalimumab-treated monkeys had slightly higher bacterial burden (CFU score) and dissemination (percent of tissue with growth) compared to control monkeys (Figure 2). One adalimumab-treated monkey (monkey17107) did not have exacerbated disease, leading to a large standard deviation in both measurements.
Immunologic responses
Percentages of CD4 and CD8 T cells within PBMC, lung, lymph node and BAL at necropsy between control and acute TNF neutralized groups were similar as was chemokine receptor (CXCR3 or CCR5) and activation marker (CD69 and CD29) expression. The absolute number of CD4 or CD8 T cells in tissues was similar between groups. Mycobacteria-specific production of IFN-γ by ELISPOT of PBMC, BAL, mediastinal lymph node and lung was also similar between both groups. At necropsy, all monkeys treated with adalimumab had detectable levels of macaque generated antibody against adalimumab though this did not abrogate the ability of adalimumab to neutralize TNF in vitro (Table 1) and did not correlate with disease outcome.
Table 1.
The presence of macaque generated antibody against adalimumab does not neutralize the effects of adalimumab in vitro or influence disease outcome.
| Monkey ID | Anti-adalimumab titer by ELISA | Percent expected TNF activity | Disseminated disease |
|---|---|---|---|
| 17107 | 1:30,000 | 0% | No |
| 2107 | 1:20,000 | 0% | Yes |
| 2807 | 1:15,000 | N/A | Yes |
| 11307 | 1:20,000 | 0% | Yes |
| 9605 | 1:40,000. | 0% | No |
| 10605 | 1:40,000. | 0% | No |
| 16605 | 1:40,000. | 0% | No |
| 17905 | 1:20,000. | 0.24% | No * |
| 23802 | 1:40,000. | 0% | Yes |
| 12102 | 1:40,000. | 0% | Yes |
| 25503 | 1:40,000. | 0% | Yes |
The presence of macaque derived anti-adalimumab antibodies among monkeys treated during acute (monkeys 17107, 2107, 2807, and 11307) and latent M. tuberculosis infection (9605, 10605, 16605, 17905, 23802, 12102, 25503) was measured by ELISA. The minimum detectable antibody titer is shown. To determine if the production of macaque-derived antibody against adalimumab abrogated the effects of adalimumab induced TNF neutralization, TNF bioactivity was measured with recombinant human TNF, adalimumab and serum of control and adalimumab treated monkeys. The percent expected TNF activity is based amount of biologically active TNF when adalimumab, monkey serum and recombinant TNF in the presence of WEHI var 13 cells (numerator) compared to recombinant TNF and serum alone without adalimumab (denominator). We theorized that macaque derived functionally neutralizing antibody against adalimumab would result in bioavailable TNF and this was not seen in our studies.
evidence of microscopic reactivation based on histopathology.
TNF neutralization alters IL-2 and IL-8 production in lungs during acute infection
Production of cytokines was measured in tissue homogenates of lung and hilar lymph nodes (Figure 4). Lung samples from adalimumab-treated monkeys had ~10 fold more IL-2 compared to controls (p=0.04). Within granulomatous lung, IL-8 levels were 30% lower among adalimumab-treated monkeys compared to controls (p=0.02). This cytokine plays a role in recruitment of neutrophils and has been identified within granulomas (specifically fibroblasts) [23, 24]. TNF neutralization reduces IL-8 secretion in response to M. tuberculosis infected fibroblasts in vitro [24]. However, by histopathology, more neutrophils were observed in lung tissue from adalimumab treated monkeys compared to controls. The paucity of detectable IL-8 in TNF-neutralized lungs may be a direct result of TNF neutralization or from increased neutrophils binding to free IL-8. Levels of CCL2, CCL3, CCL4, CCL5, IL-12, IL-6 and GM-CSF were similar between anti-TNF and control groups.
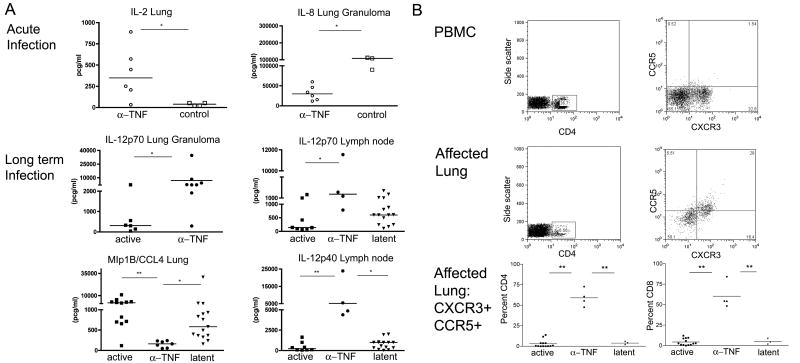
Figure 4.
TNF neutralization alters cytokine and chemokine receptor expression during acute and latent infection. (A) Lung and lymph node homogenates were analyzed for cytokine production. During acute infection, TNF neutralization (open circles) resulted in more IL-2 in lungs and less IL-8 in lung granuloma compared to control groups (open squares). Increased IL-12p70 was observed in lung and hilar lymph nodes among latently infected monkeys treated with TNF neutralizing agents (closed circles) compared to active (closed squares) and latent (closed triangles) controls. CCL4 was reduced in TNF neutralized groups compared to active and latent controls. (Kruskal-Wallis with Dunn’s multiple comparison). (B) Flow cytometry dot plots of CD4 T cell gate and CXCR3+CCR5+ dual positive cells in PBMC and affected lung samples. Significantly greater percentages of CXCR3+CCR5+ CD4 and CD8 T cells are observed among TNF neutralized monkeys compared to active and latent groups. (ANOVA with Bonferroni post hoc analysis.) * p<0.05, ** p<0.001
Treatment of latently infected monkeys with TNF-neutralizing agents reactivates tuberculosis
Monkeys can remain latently infected for many months to years [15]. The control group of latently infected monkeys for the current study (monkeys 7804, 24602, 17706, 17705, 12903, 18905, 17706) remained clinically stable, with no evidence of reactivation, until necropsy (10–15 months p.i.). Latently infected monkeys were infected for 13–32 months prior to adalimumab administration (N=7) or, 12–14 months prior to p55-TNFR1 treatment (N=2). No monkeys developed cough, anorexia, or respiratory distress. However, after 14 weeks of p55-TNFR1, monkey 6604 had gastric aspirates positive for M. tuberculosis, and an elevated ESR at necropsy. Of those treated with adalimumab, monkey 23802 developed 10% weight loss and elevated ESR (35mm) at 4 weeks post treatment, and monkey 25503 had a positive gastric aspirate after 2 weeks of treatment.
Humoral response against TNF agent
Monkeys did not develop detectable antibodies against sTNFR1. All monkeys treated with adalimumab developed anti-adalimumab antibodies by the time of necropsy (Table 1). Again, the presence of anti-adalimumab antibodies did not abrogate the ability of adalimumab to neutralize TNF activity in vitro (Table 1), and did not correlate with disease outcome.
Reactivation and disseminated disease observed in TNF-neutralized monkeys
Among latent control monkeys, limited gross pathologic findings were observed at necropsy including none to few granulomas in a single lung lobe, and thoracic lymph node enlargement with or without granulomas (Figure 1B)[19], and with no extrapulmonary lesions. Both monkeys who received p55-TNFR1 had gross evidence of reactivation characterized by multiple granulomas in liver and spleen or other organs with limited lung involvement. Three of 7 adalimumab-treated monkeys developed gross evidence of reactivation that included miliary disease throughout lungs, liver and spleen (23802), multiple granulomas in liver, spleen and extrapulmonary lymph nodes (12102), and granulomas in multiple lung lobes with dissemination along the pleura of the chest, liver, spleen and kidney (25503). Two monkeys (9605 and 10605) had multiple granulomas in one or more lung lobes (more than latent controls) suggesting early reactivation. Necropsy scores of monkeys treated with anti-TNF agents were significantly higher than latent controls (Figure 2).
Granuloma structure and formation is intact in latently infected TNF-neutralized monkeys
Latently infected monkeys demonstrated lung granulomas with typical cellular architecture consisting of scarce peripherally located lymphoplasmacytic cells surrounding a zone of epithelioid macrophages with a core of caseous necrosis (Figure 5D). Some granulomas had peripheral fibrosis and centrally located mineralization (Figure 5B). One or several isolated caseous granulomas with or without mineralization could be seen within normal lymph node architecture (Figure 5A).
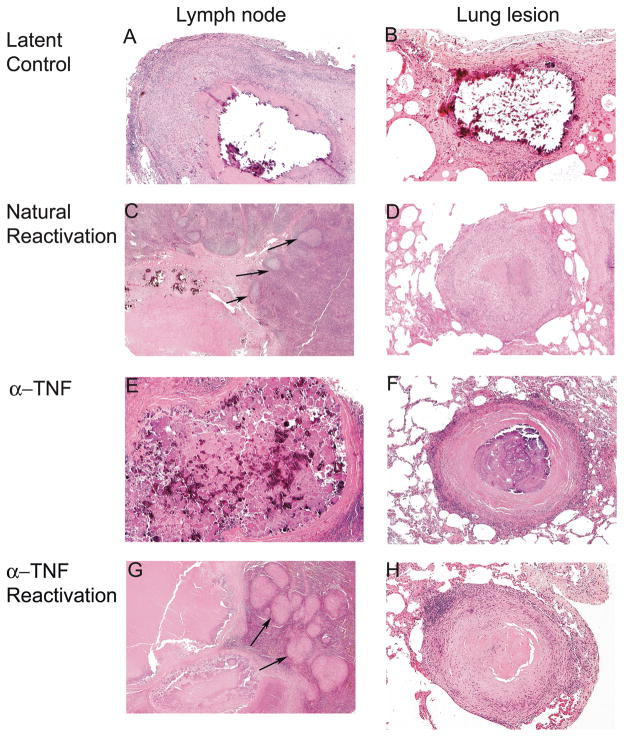
Figure 5.
Normal granuloma structure after TNF neutralization despite reactivation tuberculosis. Latently infected monkeys have caseous and/or mineralized granulomas in lungs and mediastinal lymph nodes. (A) Mineralized granuloma (central core of mineral has artifactually dropped out of section) surrounded by a fibrotic rim within a mediastinal lymph node, 5×; (B) Focal mineralized granulomas (mineral shattered during cutting) in lung of latent monkey, 5×; (C) Non-necrotizing granulomas (arrow) emanating from caseous granuloma (left) with mineralization suggesting reactivation is occurring from carinal lymph node of this natural reactivation monkey, 2×; (D) Classic caseous granuloma in lung with a proteinaceous central area of necrosis surrounded by epithelioid macrophages and lymphocytes in a natural reactivation monkey, 5×; (E) Mineralized granulomas (and caseous granulomas) in carinal lymph node of a TNF neutralized monkey. (F) Caseous granuoloma with fibrocalcific changes in TNF neutralized monkey, indistinguishable from a latent control granuloma, 5×; (G) Non-necrotizing granulomas (arrow) emerging from a caseous granulomas (with mineralization) in TNF neutralized monkey suggesting reactivation from carinal lymph node, similar to (C), 2×; (H) Classic caseous granuloma structure in lung of 25503 who had disseminated disease throughout the lung, liver and spleen.5×. All slides stained with H&E.
Microscopic histopathology of granulomas in adalimumab-treated monkeys demonstrated both non-necrotizing and caseous granulomas (Figures 5E-H) with typical cellular architecture observed in monkeys with active disease (Figures 5C,D)[19]. Even the extrapulmonary granulomas, likely to be newly formed as a result of dissemination, had normal cellular architecture. A miliary pattern of disease, both grossly and microscopically, was observed in some monkeys. Although granulomas in anti-TNF treated monkeys were clearly not identical to latent granulomas, since these monkeys developed reactivation, in fact we found no evidence of disorganized or abnormal granuloma structure compared to monkeys with active disease.
Histolopathologic evidence of reactivation in thoracic lymph nodes of TNF-neutralized monkeys
Mineralized granulomas were observed in lung and lymph nodes of both groups consistent with latent infection. In contrast, early reactivation lesions adjacent to established granulomas were observed in TNF-neutralized monkeys. Analysis of tissues from latent and active tuberculosis monkeys suggested that non-necrotizing granulomas are found only during early or active disease [19]. This pattern of “satellite” non-necrotizing granulomas in mediastinal lymph nodes of anti-TNF treated monkeys (Figure 5G) is similar to lesions identified in mediastinal lymph nodes of monkeys who developed spontaneous reactivation of latent infection (Figure 5C) [19]. This pattern suggests early reactivation in response to TNF neutralization originates from latent lesions in thoracic lymph nodes, and this may lead to rapid dissemination. Based on this, monkey 17905 (adalimumab) had evidence of microscopic reactivation in lymph nodes without gross evidence of reactivation.
Bacterial burden is increased in TNF-neutralized latently infected monkeys
Bacterial burden and dissemination was greater among TNF-neutralized monkeys compared to latent controls (Figure 2B), The gross pathology, histology, and microbiologic data together demonstrate that neutralization of TNF can lead to overwhelming reactivation and dissemination of latent M. tuberculosis infection, while maintaining apparently normal granuloma architecture.
IFN-γ in hilar lymph nodes is not altered by TNF neutralization
Greater bacterial burden and production of mycobacterial specific IFN-γ was observed among active monkeys compared to latent controls [19]. In hilar lymph nodes, TNF neutralized monkeys had greater IFN-γ production compared to latent controls (p<0.01) and similar responses to active controls indicating appropriate IFN-γ responses. Given the limited lung disease, too few samples were available for meaningful comparison. Taken as a whole, these data suggest that IFN-γ production is not altered by TNF neutralization at the site of disease in contrast to blood (23,[25]
TNF neutralization impairs cellular recruitment and alters chemokine receptor expression
Despite similar bacterial burden in TNF neutralized monkeys compared to active controls, the absolute numbers of CD4 and CD8 T cells per gram tissue in hilar lymph nodes and lung were similar to latent controls as determined by flow cytometry (data not shown). We previously reported that increased T cell numbers in lungs are associated with increased bacterial burden [19]. These data suggest that despite similar bacterial burdens between monkeys with active disease and or TNF neutralized, TNF neutralization may impair cellular recruitment of T cells to the lungs. However, such results may also be explained by the disproportionate degree of extrapulmonary disease in TNF neutralized monkeys.
Within granulomatous lung, a greater percentage of CD4 and CD8 T cells expressing both CXCR3 and CCR5 were present in TNF-neutralized monkeys compared to both latent and active control monkeys (p<0.01) (Figure 4B). These data suggest that TNF neutralization is associated with altered chemokine receptor expression, perhaps contributing to extrapulmonary spread.
TNF neutralization alters IL-12 and CCL4 levels in lung and lymph node
Within lymph nodes, IL-12p70 levels were significantly greater in TNF-neutralized compared to active but not latent control monkeys (p<0.05)(Figure 4). IL-12p40 in hilar lymph nodes was higher in anti-TNF treated monkeys compared to latent and active controls. Within granulomatous lung, IL-12p70 (Figure 4) and IL-12p40 (data not shown) levels among TNF neutralized monkeys were significantly higher than active controls (p=0.02). CCL4 in lung tissue was significantly reduced among TNF neutralized monkeys compared to active and latent controls (p<0.05). This finding may be associated with the disproportionate degree of extrapulmonary disease seen. There were insufficient samples of granulomatous lung tissue available from latent monkeys for this comparison.
Discussion
Humans treated with TNF neutralizing agents are at substantially higher risk of developing tuberculosis. To date, this appears to be reactivation of latent infection. However, as these immunomodulatory agents begin to be used in developing countries with higher endemic tuberculosis rates, the risk of primary tuberculosis in these patients is likely to increase. This study investigated the host response to M. tuberculosis following TNF neutralization in macaques, the only established model of latent tuberculosis that provides a spectrum of granuloma histopathology that is most similar to humans. We demonstrate that TNF neutralization leads to exacerbation of primary disease and reactivation of latent infection with increased bacterial burden, pathology and extrapulmonary spread. Importantly, normal granuloma structure was observed despite TNF neutralization during both primary infection (granuloma formation) and latent infection (granuloma maintenance). The overall granuloma architecture was similar in TNF-neutralized monkeys to that seen in monkeys with active tuberculosis. This is consistent with data from the zebrafish model of M. marinum infection in which normal and accelerated granuloma formation was observed in the absence of TNF despite increased bacterial growth suggesting that early granuloma formation is independent of TNF signaling [26]. These data challenge the current presumption that tuberculosis associated with TNF neutralization in humans is due to impaired granuloma organization. In murine models, we and others reported that granuloma structure was disrupted during both primary and chronic disease without functional TNF [4], suggesting that TNF was not only necessary for macrophage activation, but also for signals leading to formation and maintenance of granulomas. This disparity in findings may be due to the inherent nature of murine granulomas, which are loosely organized aggregates of inflammatory cells, compared to the distinct architecture of tightly localized inflammatory cells seen in zebrafish and primates [1, 2]. Simulations of a granuloma in a mathematical model and dissection of the various functions of TNF in control of M. tuberculosis predicted that granuloma formation or maintenance was not dependent on TNF, but instead that the primary role for TNF in the granuloma was macrophage activation and stimulation of chemokine production [27]. This model also demonstrated that granuloma size, and to some degree structure, depended primarily on bacterial numbers. This correlates well with the data presented here.
The murine studies resulted in speculation regarding granuloma structure among patients with anti-TNF associated tuberculosis. Iliopoulous et al [28] reviewed anti-TNF associated tuberculosis reports and found only 2 cases in which tuberculosis was diagnosed by culture with negative biopsy evidence [2, 29]. The authors contend that this notion of “granuloma free tuberculosis” may have dissuaded physicians from performing diagnostic biopsy. Likewise, the majority of published cases describe a range of disease involvement (pulmonary, extrapulmonary [2], or miliary disease [28, 30]) yet no cases of aberrant granuloma structure. A high proportion of disseminated and/or extrapulmonary disease, as seen in our model, occurs in human cases compared to reactivation tuberculosis in the general population [2, 31] in which mediastinal disease is the most common manifestation [13]. The unusual presentation of tuberculosis in these cases likely contributes to difficulty in diagnosis but should not dissuade physicians from obtaining diagnostic biopsy or culture.
The presence of normal granuloma structure suggests that the mechanism of disease exacerbation in humans may differ from the murine model. No differences in cell number, cellular phenotype or mycobacterial specific production of IFN-γ could be identified in acutely infected monkeys despite the disseminated disease seen in TNF neutralized monkeys. The greater production of IL-2 in lungs of TNF neutralized monkeys is likely to be the result of more severe disease. Less IL-8 was detected in lung granulomas of TNF neutralized monkeys during acute infection compared to controls, although more neutrophils were present in granulomas these monkeys.
TNF neutralized latently infected monkeys had greater disease burden and bacterial load compared to latent controls. Human studies of PBMCs have suggested that TNF neutralizing agents decrease mycobacteria-specific IFN-γ production [32, 33] and proliferative responses [25]. In contrast, our data suggest that TNF neutralization does not alter IFN-γ responses at the site of disease. While differences in chemokine expression due to TNF neutralization in mice were described [9, 10, 34], CCL4 was the only chemokine altered during TNF neutralization in monkeys. Substantially more T cells expressing both CXCR3 and CCR5 were observed in lungs of TNF neutralized monkeys compared to controls. Increased expression of chemokine receptors may reflect changes in cytokine or chemokine concentrations, and affect appropriate cell trafficking within tissues or granulomas. IL-12 was higher in TNF neutralized hilar lymph nodes and lungs, supporting that TNF plays a role in regulation of IL-12 expression as in in vitro models [35, 36]. Overall, it appears that TNF neutralization (whether directly or indirectly) results in dysregulation of critical cytokines and chemotactic factors that ultimately contributes to disseminated disease. Thus, TNF may still affect localization of cells [26, 37] and the integrity of cellular interactions within the granuloma, rather than at the level of overall granuloma structure.
TNF has multiple effector mechanisms that may be important in control of tuberculosis including influence of cytokine [6] and chemokine responses [9, 10], macrophage activation [6], and apoptosis [7, 8]. Macrophage function is likely altered by TNF neutralization as others have reported [26, 27, 37, 38]. Anti-TNF antibody has been associated with reduction in a subset of CD8 memory effector cells that have tuberculocidal activity [39]. Our current efforts are focused on these aspects.
These findings have important implications in studying the complexity of reactivation. The presence of non-necrotizing granulomas (seen exclusively in active disease) in hilar lymph nodes of both natural and TNF neutralized reactivation monkeys suggests that this process begins in hilar lymph nodes. While the rate of reactivation among TNF neutralized monkeys was not 100%, it was certainly very high as reflected by human data. In our model, a spectrum of latent infection can be observed [19] suggesting that risk of reactivation likely depends on a complex combination of factors, including state of infection, severity and duration of immune suppression. Currently patients with latent tuberculosis are recommended anti-tuberculosis medications prior to starting a TNF inhibitor. Despite this, tuberculosis cases still occur during TNF treatment [40] demonstrating that TNF plays a critical role in control of tuberculosis for some patients.
In summary, the high rate and rapid onset of reactivation that can occur during TNF neutralization and presence of normal granuloma structure should remind clinicians to maintain a high level of clinical suspicion and low threshold for culture and biopsy in such patients. Our data strongly support that use of TNF-neutralizing agents in areas of endemic tuberculosis should be carefully monitored, as the incidence of both primary and reactivation tuberculosis is likely to increase dramatically and may be difficult to diagnose, due to unusual presentation.
Acknowledgments
This study was supported by NIH K08AI063101-05 (P.L.L.), Harold Bayer-Neu Award of the Infectious Disease Society of America (P.L.L.), Otis H. Childs Charitable Trust (P.L.L.), NIH RO1 HL075845-04 (J.L.F.), NIH R33 HL092883 (J.L.F.), the Bill and Melinda Gates Foundation Grand Challenges in Global Health (J.L.F.), and the Ellison Foundation (J.L.F). Amgen provided the p55-TNFR1 agent used for these experiments and a small research grant for purchase of adalimumab. We gratefully acknowledge the technical help of Stephanie Casino, Andre Samuels, and David Litvin. We thank Santosh Pawarfor initial flow cytometry analyses, and James S. Louie for helpful discussions. We thank Corixa, Inc, and the NIH Tuberculosis Reagent Contract (NIH NIAID NO1-AI-40091) for supplying antigens Dr. Keith Reimann for insight on use of humanized antibodies in primates, and Michael Schearer for use of the B3 anti-macaque antibody for ELISA.
References
- 1.Wallis RS. Reconsidering adjuvant immunotherapy for tuberculosis. Clin Infect Dis. 2005;41(2):201–8. doi: 10.1086/430914. [DOI] [PubMed] [Google Scholar]
- 2.Keane J, et al. Tuberculosis associated with infliximab, a tumor necrosis factor alpha-neutralizing agent. N Engl J Med. 2001;345(15):1098–104. doi: 10.1056/NEJMoa011110. [DOI] [PubMed] [Google Scholar]
- 3.Emile JF, et al. Correlation of granuloma structure with clinical outcome defines two types of idiopathic disseminated BCG infection. J Pathol. 1997;181(1):25–30. doi: 10.1002/(SICI)1096-9896(199701)181:1<25::AID-PATH747>3.0.CO;2-Z. [DOI] [PubMed] [Google Scholar]
- 4.Plessner HL, et al. Neutralization of tumor necrosis factor (TNF) by antibody but not TNF receptor fusion molecule exacerbates chronic murine tuberculosis. J Infect Dis. 2007;195(11):1643–50. doi: 10.1086/517519. [DOI] [PubMed] [Google Scholar]
- 5.Mohan VP, et al. Effects of tumor necrosis factor alpha on host immune response in chronic persistent tuberculosis: possible role for limiting pathology. Infect Immun. 2001;69(3):1847–55. doi: 10.1128/IAI.69.3.1847-1855.2001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Flynn JL, et al. Tumor necrosis factor-alpha is required in the protective immune response against Mycobacterium tuberculosis in mice. Immunity. 1995;2(6):561–72. doi: 10.1016/1074-7613(95)90001-2. [DOI] [PubMed] [Google Scholar]
- 7.Keane J, Shurtleff B, Kornfeld H. TNF-dependent BALB/c murine macrophage apoptosis following Mycobacterium tuberculosis infection inhibits bacillary growth in an IFN-gamma independent manner. Tuberculosis (Edinb) 2002;82(2–3):55–61. doi: 10.1054/tube.2002.0322. [DOI] [PubMed] [Google Scholar]
- 8.Keane J, et al. Infection by Mycobacterium tuberculosis promotes human alveolar macrophage apoptosis. Infect Immun. 1997;65(1):298–304. doi: 10.1128/iai.65.1.298-304.1997. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Algood HM, et al. TNF influences chemokine expression of macrophages in vitro and that of CD11b+ cells in vivo during Mycobacterium tuberculosis infection. J Immunol. 2004;172(11):6846–57. doi: 10.4049/jimmunol.172.11.6846. [DOI] [PubMed] [Google Scholar]
- 10.Saunders BM, Frank AA, Orme IM. Granuloma formation is required to contain bacillus growth and delay mortality in mice chronically infected with Mycobacterium tuberculosis. Immunology. 1999;98(3):324–8. doi: 10.1046/j.1365-2567.1999.00877.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Schreiber T, et al. Selectin ligand-independent priming and maintenance of T cell immunity during airborne tuberculosis. J Immunol. 2006;176(2):1131–40. doi: 10.4049/jimmunol.176.2.1131. [DOI] [PubMed] [Google Scholar]
- 12.Lopez Ramirez GM, et al. Mycobacterium tuberculosis alters expression of adhesion molecules on monocytic cells. Infect Immun. 1994;62(6):2515–20. doi: 10.1128/iai.62.6.2515-2520.1994. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Rieder HL, Snider DE, Jr, Cauthen GM. Extrapulmonary tuberculosis in the United States. Am Rev Respir Dis. 1990;141(2):347–51. doi: 10.1164/ajrccm/141.2.347. [DOI] [PubMed] [Google Scholar]
- 14.North RJ, Jung YJ. Immunity to tuberculosis. Annu Rev Immunol. 2004;22:599–623. doi: 10.1146/annurev.immunol.22.012703.104635. [DOI] [PubMed] [Google Scholar]
- 15.Capuano SV, 3rd, et al. Experimental Mycobacterium tuberculosis infection of cynomolgus macaques closely resembles the various manifestations of human M. tuberculosis infection. Infect Immun. 2003;71(10):5831–44. doi: 10.1128/IAI.71.10.5831-5844.2003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Botha T, Ryffel B. Reactivation of latent tuberculosis infection in TNF-deficient mice. J Immunol. 2003;171(6):3110–8. doi: 10.4049/jimmunol.171.6.3110. [DOI] [PubMed] [Google Scholar]
- 17.Lin PL, et al. Early events in Mycobacterium tuberculosis infection in cynomolgus macaques. Infect Immun. 2006;74(7):3790–803. doi: 10.1128/IAI.00064-06. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Richter CB, Lehner NDM, Hendrickson RV. Primates. In: Fox JG, Cohren BJ, Loew FM, editors. Laboratory animal medicine. San Diego, Calif: Academic Press, Inc; 1984. [Google Scholar]
- 19.Lin PL, et al. Quantitative comparison of active and latent tuberculosis in the cynomolgus macaque model. Infect Immun. 2009 doi: 10.1128/IAI.00592-09. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Edwards CK, 3rd, et al. Design of PEGylated soluble tumor necrosis factor receptor type I (PEG sTNF-RI) for chronic inflammatory diseases. Adv Drug Deliv Rev. 2003;55(10):1315–36. doi: 10.1016/s0169-409x(03)00112-1. [DOI] [PubMed] [Google Scholar]
- 21.Espevik T, Nissen-Meyer J. A highly sensitive cell line, WEHI 164 clone 13, for measuring cytotoxic factor/tumor necrosis factor from human monocytes. J Immunol Methods. 1986;95(1):99–105. doi: 10.1016/0022-1759(86)90322-4. [DOI] [PubMed] [Google Scholar]
- 22.Giavedoni LD. Simultaneous detection of multiple cytokines and chemokines from nonhuman primates using luminex technology. J Immunol Methods. 2005;301(1–2):89–101. doi: 10.1016/j.jim.2005.03.015. [DOI] [PubMed] [Google Scholar]
- 23.Bergeron A, et al. Cytokine patterns in tuberculous and sarcoid granulomas: correlations with histopathologic features of the granulomatous response. J Immunol. 1997;159(6):3034–43. [PubMed] [Google Scholar]
- 24.O’Kane CM, et al. Monocyte-dependent fibroblast CXCL8 secretion occurs in tuberculosis and limits survival of mycobacteria within macrophages. J Immunol. 2007;178(6):3767–76. doi: 10.4049/jimmunol.178.6.3767. [DOI] [PubMed] [Google Scholar]
- 25.Hamdi H, et al. Inhibition of anti-tuberculosis T-lymphocyte function with tumour necrosis factor antagonists. Arthritis Res Ther. 2006;8(4):R114. doi: 10.1186/ar1994. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Clay H, Volkman HE, Ramakrishnan L. Tumor necrosis factor signaling mediates resistance to mycobacteria by inhibiting bacterial growth and macrophage death. Immunity. 2008;29(2):283–94. doi: 10.1016/j.immuni.2008.06.011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Ray JC, Flynn JL, Kirschner DE. Synergy between individual TNF-dependent functions determines granuloma performance for controlling Mycobacterium tuberculosis infection. J Immunol. 2009;182(6):3706–17. doi: 10.4049/jimmunol.0802297. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Iliopoulos A, et al. A case of tuberculous meningoencephalitis in a patient with Behcet’s disease. Clin Rheumatol. 2006;25(1):121–2. doi: 10.1007/s10067-005-1135-4. [DOI] [PubMed] [Google Scholar]
- 29.Liberopoulos EN, Drosos AA, Elisaf MS. Exacerbation of tuberculosis enteritis after treatment with infliximab. Am J Med. 2002;113(7):615. doi: 10.1016/s0002-9343(02)01205-6. [DOI] [PubMed] [Google Scholar]
- 30.Verhave JC, et al. Tuberculous peritonitis during infliximab therapy. Neth J Med. 2008;66(2):77–80. [PubMed] [Google Scholar]
- 31.Dimakou K, et al. Disseminated tuberculosis complicating anti-TNF-alpha treatment. Int J Clin Pract. 2004;58(11):1052–5. doi: 10.1111/j.1742-1241.2004.00061.x. [DOI] [PubMed] [Google Scholar]
- 32.Giardina AR, et al. Blocking TNF in vitro with infliximab determines the inhibition of expansion and interferon gamma production of Vgamma9/Vdelta2 T lymphocytes from patients with active rheumatoid arthritis. A role in the susceptibility to tuberculosis’. Reumatismo. 2009;61(1):21–6. doi: 10.4081/reumatismo.2009.21. [DOI] [PubMed] [Google Scholar]
- 33.Saliu OY, et al. Tumor-necrosis-factor blockers: differential effects on mycobacterial immunity. J Infect Dis. 2006;194(4):486–92. doi: 10.1086/505430. [DOI] [PubMed] [Google Scholar]
- 34.Saukkonen JJ, et al. Beta-chemokines are induced by Mycobacterium tuberculosis and inhibit its growth. Infect Immun. 2002;70(4):1684–93. doi: 10.1128/IAI.70.4.1684-1693.2002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Masli S, Turpie B. Anti-inflammatory effects of tumour necrosis factor (TNF)-alpha are mediated via TNF-R2 (p75) in tolerogenic transforming growth factor-beta-treated antigen-presenting cells. Immunology. 2009;127(1):62–72. doi: 10.1111/j.1365-2567.2008.02933.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Ma X, et al. Inhibition of IL-12 production in human monocyte-derived macrophages by TNF. J Immunol. 2000;164(4):1722–9. doi: 10.4049/jimmunol.164.4.1722. [DOI] [PubMed] [Google Scholar]
- 37.Egen JG, et al. Macrophage and T cell dynamics during the development and disintegration of mycobacterial granulomas. Immunity. 2008;28(2):271–84. doi: 10.1016/j.immuni.2007.12.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Harris J, Hope JC, Keane J. Tumor necrosis factor blockers influence macrophage responses to Mycobacterium tuberculosis. J Infect Dis. 2008;198(12):1842–50. doi: 10.1086/593174. [DOI] [PubMed] [Google Scholar]
- 39.Bruns H, et al. Anti-TNF immunotherapy reduces CD8+ T cell-mediated antimicrobial activity against Mycobacterium tuberculosis in humans. J Clin Invest. 2009 doi: 10.1172/JCI38482. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Sichletidis L, et al. Tuberculosis in patients receiving anti-TNF agents despite chemoprophylaxis. Int J Tuberc Lung Dis. 2006;10(10):1127–32. [PubMed] [Google Scholar]