Abstract
Little is known about the effective elements of Interactive Cancer Communication Systems (ICCSs). A randomized trial explored which types of services of a multifaceted ICCS benefited patients and the nature of the benefit. Women with breast cancer (N = 450) were randomized to different types of ICCS services or to a control condition that provided internet access. The Comprehensive Health Enhancement Support System (CHESS), served as the ICCS. ICCS services providing information and support, but not coaching such as cognitive behavior therapy, produced significant benefits in health information competence and emotional processing. Provision of Information and Support ICCS services significantly benefited women with breast cancer. More complex and interactive services designed to train the user had negligible effects.
Keywords: Breast cancer, eHealth, Quality of life, Cognitive behavior therapy
Consumer-focused eHealth interventions are intended to help the public deal with health issues, particularly during illness. It is clear that people turn to the internet with health questions. For example, the Health Information National Trends Survey [HINTS; cited in [1]] showed that 48% of people who sought cancer information went first to the internet. Similarly, about two thirds of people with cancer who called the National Cancer Institute’s Cancer Information Service reported using the internet to obtain cancer information, and family and friends were slightly more likely to do so [1]. The HINTS also found that after doctors and other health care providers, the internet was the most trusted source of information [cited in [1]]. Surveys show that most users of eHealth cancer resources report success in finding the information they were seeking [2].
eHealth comprises a variety of possible resources for cancer patients, including Websites or CD’s presenting basic information, email notices to list serves of individuals with common health interests, and also interactive cancer communication services (ICCSs). ICCSs are computer-based, usually Web-based, providing information about cancer and its treatment, and also other services such as social support services, decision-making support, and/or behavior change or emotional coping support [3]. Should such interventions be effective, they have great potential to play a major role in modern health care, since they are highly accessible (including 24 h/day access), have relatively low delivery and maintenance costs, have high quality assurance in that intervention fidelity is built-in, can be tailored to different patient groups [4], and can deliver multiple types of interventions. These features make ICCSs attractive in today’s health care setting that faces cost and personnel constraints, and concerns about the consistent application of evidence-based medicine and psychosocial interventions (e.g., [5]). Also, ICCSs can be viewed as one element in the increasing effort to enhance the infrastructure and support for electronic medical communication systems (e.g., electronic medical records). The future of ICCSs, however, depends upon evidence that they actually produce benefit.
Mounting and varied evidence confirms that eHealth use is generally beneficial to patients, producing benefits on measures ranging from increased knowledge to improved coping (e.g., [4, 6]). However, considerable gaps remain in the evidence. For instance, randomized controlled trials (RCTs) yield the strongest inferences regarding treatment effects, but relatively few RCTs have analyzed eHealth interventions for a given disease. A Cochrane review of eHealth for chronic disease [3] found only 24 acceptable RCTs on interactive health communication strategies, of which only three addressed ICCSs, and these studies differed by type of cancer, age of the population, and types of outcome measures. A more recent review [7] detected six randomized trials involving computer-based cancer interventions that passed the review’s screening criteria, but these trials varied on the types of services offered in the interventions, the populations involved, the outcome measures used, and the results. Thus, while there is mounting evidence that eHealth interventions, in general, can be effective, we know little about ICCSs in particular, e.g., how effective they are and how to use them most effectively.
As noted above, ICCSs tend to offer a broad range of services, such as answers to frequently asked questions, expert responses to personalized questions, chat rooms, discussion groups, decision-making aids, and information search services. One open question concerns how effective these different services are. Simply assuming that anything “interactive” will be beneficial overlooks opportunities for improving ICCSs and may obscure real weaknesses. One recent study showed that giving breast cancer patients open access (with training) to the internet showed no benefits relative to a control group that received an informative book [8], although provision of an integrated set of ICCS services (i.e., CHESS) showed greater benefits than either of those groups.
The current study addresses three central questions: (1) How effective is a “model” ICCS? (2) Which types of services produce significant benefit? (3) What types of benefits are observed? Therefore, this study addresses issues that are critical to health care decisions about providing eHealth resources to cancer patients: (1) Should the health care system provide patients with an integrated set of eHealth resources or just promote access to the internet? And, (2) If the health care system provides an integrated program of services, which types of services should be provided? It is important to establish ICCS effectiveness, but it is also vital to discover how to structure or engineer such systems so that ICCSs can be most beneficial to cancer patients.
The ICSS used in this research, the Comprehensive Health Enhancement and Support System (CHESS), was selected as the ICSS for study because, relative to other candidate ICCSs, it comprises a comprehensive array of services, allowing good services coverage, and there is evidence that its services are of high quality [8–10].
TYPES OF ICSS (CHESS) SERVICES
A recent review by Strecher [4]; also see [3] suggested that eHealth could improve health outcomes by serving several different functions. First, eHealth may function as a vast available library by providing ready and organized access to information. Second, eHealth may function as a communication and support channel by linking people together (via online discussion groups, for example). Finally, eHealth may function as an interactive coach. That is, the expert system can gather information from a user, apply algorithms or decision rules, and provide feedback or prompts appropriate to the individual user’s characteristics or problems. For instance, computer-delivered cognitive behavior therapy would constitute a type of coaching service. Unfortunately, it is unclear which of these functions of eHealth is responsible for reported benefits because RCTs typically test systems that combine all of these attributes against non-ICCS or generic internet conditions. Some evidence supporting [27] distinctions comes from researchers inferring benefit from correlations between eHealth use patterns and outcomes [11]. Such correlations, however, do not permit strong inferences about the directionality of causal paths [3, 4, 6, 12]. Identifying the most useful services could allow researchers to hone ICCSs to enhance effectiveness, reduce complexity and burden on users, and reduce development costs.
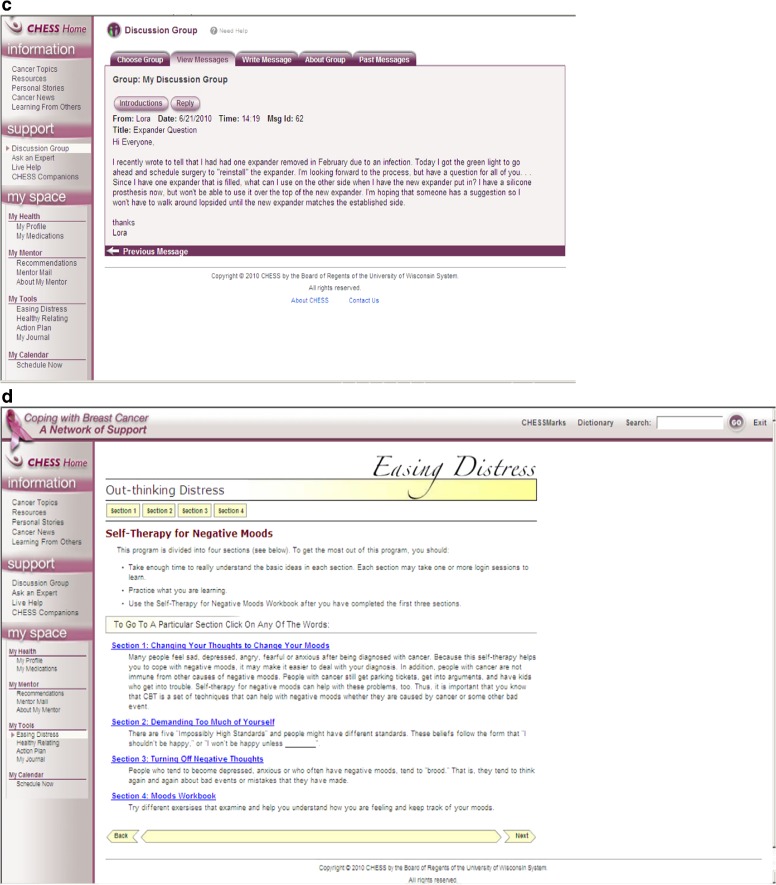
To achieve the aims of this study, breast cancer patients recruited in three different cancer care facilities were randomly assigned to either a control condition (with internet access) or to one of three versions of an ICCS. This experiment employed a stacked design in which each of the three CHESS conditions received different numbers and types of CHESS services. The first CHESS condition (CHESS Information) received only the Information services; the second condition (CHESS Information and Support) received both the Information and Support services, while the third condition received all three types of CHESS services (Information, Support, and Coaching: Full CHESS). This stacked design reflected the distinct natures and mechanisms of the service types and also reflected pragmatic dimensions, such as the greater costs of creating and maintaining Support and Coaching services. The particular services comprised by the various versions of CHESS and their intended functions are listed in Table 1, and Fig. 1a–d shows representative screen shots from the home page and from the three major service types.
Table 1.
CHESS service separation
| CHESS information services | CHESS information+support services | CHESS information+support+coaching servicesa |
|---|---|---|
| Cancer Topics: Basic information about breast cancer, symptoms, treatment, self-care, and navigating the health care system | All CHESS Information Services | All CHESS Information and Support Services |
| PLUS ↓ | PLUS: ↓ | |
| Frequently Asked Questions: Answers to commonly asked questions related to breast cancer | Discussion Groups: Provides access to anonymous, facilitated message boards to share information and support with other breast cancer survivors | Easing Distress: Helps users learn to manage affective distress through cognitive behavioral or mindfulness coaching, feedback and exercises. |
| Library Articles: Links to full articles from scientific and popular press | Ask an Expert: Allows users to ask questions and get a personal answer from a cancer information expert | Healthy Relating: Helps users learn more effective ways of relating with close others through interactive assessments, skills training, and assigned exercises |
| Web Links: Links to reliable cancer, general health, and interest websites. | Live Help: Link to the National Cancer Institute chat line | Action Plan: Offers direction and feedback to users to develop a plan for lifestyle change |
| Resource Guide: Helps users be better informed, more efficient health care consumers | My Profile: Allows the user to manage a health profile on personal demographics, treatments, and current concerns | |
| Personal Stories and Video Gallery: Collection of written and video accounts of breast cancer survivors’ experiences and how they coped | ||
| My Journal: Online journal to record thoughts and experiences. Encourages emotionally expressive coping. | ||
| Resource Directory: Links to local and national community resources | ||
| Cancer News: Provides links to recently released cancer news | ||
| Medications Manager: Allows users to track current medications and related concerns | ||
| CHESS Calendar: Allows users to keep track of appointments, tests, and other important dates |
In addition, all CHESS users had word and information search and bookmarking services
aThe coaching services involve some service tailoring based on user identification of concerns or ongoing treatment
Fig. 1.
a–d Screen shots of the CHESS home page (a), and representative pages from the three major types of services: Information, Support, and Coaching (b–d)
The Information services were viewed as “base” services because they are highly available, relatively inexpensive to develop, and are expected by patients and clinicians. Communication Support services are relatively easy to add to Information services, but require some management. Coaching services, however, require considerably more development effort and also more effort and commitment by the user who is asked to actively participate in exercises involving self-assessment, analysis, and practice.
Previous research has shown that CHESS has produced benefit relative to two kinds of control conditions, i.e., provision of a comprehensive book about breast cancer, or training and access to the internet plus provision of Web addresses of selected, high-quality internet sites. In theory, CHESS offers certain advantages over internet access per se. The internet offers a great deal of useful information, but much of it is unedited; it may be punctuated by intrusions (e.g., pop-ups), some information is inaccurate and biased, variations in interfaces can make searches tedious and confusing, and because the different Websites are not integrated with one another, searches may yield redundant or conflicting information. CHESS is designed to address these limitations by providing accurate (vetted) information, a single easy-to-use interface, and information that is integrated across services to reduce redundancy and conflicting messages. Through extensive and ongoing development via focus groups and process and outcome evaluations in clinical trials, CHESS has become a good representative of an integrated ICCS [8, 13, 14]. Virtually all of the services offered in the Full CHESS intervention were included in the versions of CHESS that have been experimentally validated in previous research with breast cancer patients [8, 13, 14]. However, the Coaching services have received considerably less evaluation. For instance, the Easing Distress and the Healthy Relating services had not been included in the prior successful applications of CHESS with breast cancer patients, increasing the importance of determining whether these services do indeed benefit such patients.
It is important to recognize that the control conditions that have been used in CHESS research occur in addition to usual care support for cancer patients, which typically includes access to physicians (typically oncologists, radiologists, and surgeons), nurses, literature supplied by the health care system, and often access to a cancer care counselor (e.g., a medical educator with relevant training). These sorts of cancer care resources were available in the programs from which patients were recruited in the current research. Past research has shown that CHESS has produced benefit over and above these usual care resources, and control condition (e.g., provision of internet access and training), with effects usually being seen in such outcomes as perceived competence in dealing with health care information, quality of life, perceived social support, confidence in or satisfaction with health care, and emotional status or confidence in dealing with emotions (e.g., [8, 14]).
Based on an evaluation of the goals of the different types of CHESS services and clinical relevance, we identified four types of measures as primary [15]: Cancer Information Competence, Social Support, Emotional Processing, and Functional Well-Being (Quality of Life), at 3 months follow-up. These measures assess effects of each type of service (Information, Support, and Coaching [cognitive behavior therapy (CBT)]) as well as the general or overall effects of CHESS (Quality of Life).1 The 3-month mark was chosen because it permitted sufficient time for women to access and learn to use CHESS, and it tapped a time period of considerable stress, anxiety, and coping with breast cancer.
Thus, this study addresses the question of how complex ICCSs must be in order to yield optimal effects. If cancer patients benefit only from access to information per se, then the Information CHESS condition should show as much benefit as the other CHESS conditions. However, if cancer patients are aided by communication links with other patients and cancer experts, then the Information and Communication condition should be superior on some outcomes. The Full CHESS condition will reveal whether outcomes are further enhanced by coaching/training services provided by the expert system that tailors information on the basis of patient needs, concerns, and treatment status. Thus, this design tested whether “more” is better, with “more” being reflected in greater numbers and more complex types of services.
Patients receiving CHESS were compared with patients who were randomly assigned to a condition (Internet Only) in which they were provided internet access. This was done to equate groups with regard to internet access and to distinguish them on the basis of provision of a high-quality, integrated ICCS. Thus, this design tests whether different versions of an integrated high-quality ICCS are effective relative to unstructured internet access.
METHOD
Recruitment
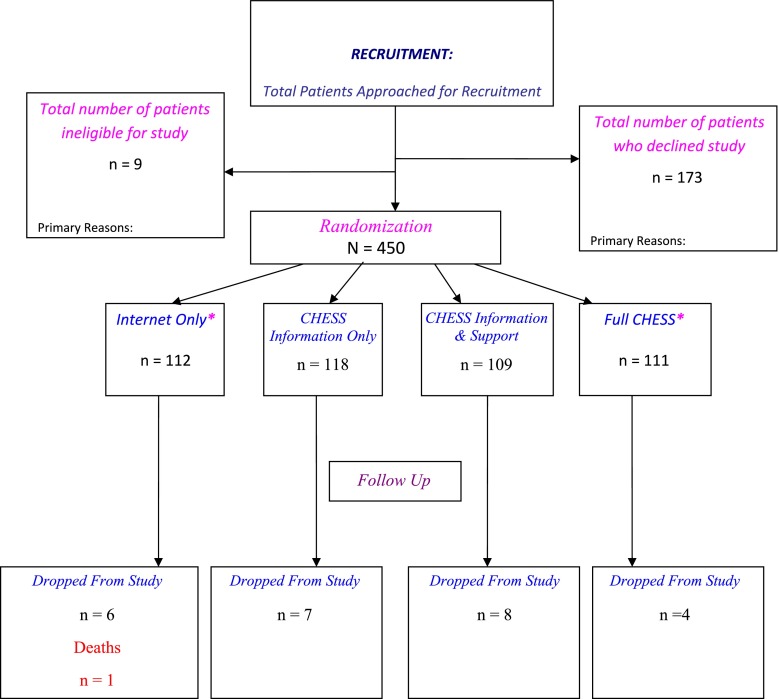
Study recruitment was conducted from April 1, 2005 through May 31, 2007 at the University of Wisconsin Paul P. Carbone Comprehensive Cancer Center (UWCCC), Hartford Hospital’s Helen and Harry Gray Cancer Center, and The University of Texas M.D. Anderson Cancer Center. Recruitment was conducted for two different studies that shared two experimental conditions (the internet control condition and the Full CHESS condition were included in both experiments; see [15]. A total of 1,034 women from patient pools at the three sites were approached for study participation in the two experiments; women were approached for participation in either the current experiment or the companion experiment [15] on a predetermined, random basis. Six hundred thirty-two women were ultimately positively screened and randomized to one of the treatment conditions in the two experiments with 450 patients participating in the current experiment (see Fig. 2 for Consort diagram). Each experiment randomly assigned women to the shared conditions: with each study contributing about half of the women to each condition (but, for clarity, all subjects ultimately assigned to all four conditions are depicted in Fig. 2). This sample size provided adequate power (>0.80) for effects of moderate size. Participants were randomized via a computer-generated list that was accessed by site study managers on a patient-by-patient basis, with experimental conditions blocked within sites.
Fig. 2.
Components experiment: comprehensive cancer communication study. Sites UW Comprehensive Cancer Center, M.D. Anderson Cancer Center, Hartford Hospital; Recruitment Dates: 4/1/2005–5/31/2007
Recruitment occurred via brochures at relevant locations, training of clinical staff, and standardized recruitment scripts. Staff at all sites approached potentially eligible patients and asked if they would be interested in learning more about the study. As appropriate, staff members then reviewed the informed consent and HIPAA information, explained the nature of the interventions, answered patient questions, obtained written consent, collected complete patient contact and computer access information, and provided patients the baseline questionnaires. Standard inclusion criteria were used at all sites: women were >17 years old, able to read and understand English, and were within 2 months of a diagnosis of primary breast cancer or recurrence at the time of recruitment.
Intervention
Once consent and the baseline survey were received by the research staff, the participant was randomized and her particular needs regarding internet access, hardware, etc., were assessed. Research staff informed the patient about the resources to which she had been randomized and asked whether she needed a laptop computer or internet service. Any patient who did not have access to a computer with internet access was provided a computer and access by the research program. Fifty-eight individuals were given both internet access connection and a computer, while five were given only the internet access.
Every study participant was offered training on using the CHESS system or Google’s Web search engine depending on group assignment. Training typically took about 30 min and was usually conducted by telephone, but occasionally was done in person if the individual required hands-on instruction. All women had no-cost access to the internet, including those in the experimental CHESS conditions.
Assessment methods
Patients were given surveys at the baseline visit and mailed the surveys back to research staff before randomization. Follow-up surveys were mailed to patients at 2, 6, 12, and 24 weeks post-intervention access, and patients returned the surveys by mail. Patient withdrawal rates were about 8% [16].
Demographics and patient characteristics
Demographic information reported by participants is depicted in Table 2.
Table 2.
Baseline characteristics for participants: mean and (SD)
| Internet only n = 112 | CHESS info only n = 118 | CHESS info+support n = 109 | Full CHESS info+support+coaching n = 111 | |
|---|---|---|---|---|
| Age (years) | 52.3 (10.2) | 52.2 (9.8) | 50.6 (10.8) | 50.9 (9.0) |
| Education | 4.9 (1.3) | 5.1 (1.4) | 4.8 (1.5) | 4.9 (1.4) |
| Income | 3.9 (1.6) | 4.0 (1.7) | 3.7 (1.7)a | 4.3 (1.5)b |
| Minority | 11% | 12% | 15% | 10% |
| Uninsured | 0% | 2% | 1% | 0% |
| Live alone | 17% | 14% | 20% | 9% |
| Days since diagnosis | 42.9 (25.5) | 44.6 (29.1) | 51.3 (30.3) | 42.9 (24.8) |
| Computer comfort | 3.0 (1.1) | 3.1 (1.0) | 3.1 (1.1) | 3.2 (0.9) |
| Internet comfort | 3.0 (1.1) | 3.0 (1.1) | 3.0 (1.2) | 3.1 (1.1) |
Means with different superscripts differ significantly (p < .05). Response scales were, for Education: 1=did not complete Junior High; 2=did not complete High School; 3=High School degree; 4=some college; 5=Bachelors degree; 6=some graduate school; and 7=graduate degree. For Income: 1 < $20 K; 2=$20 K to $40 K; 3=$40 K to $60 K; 4=$60 K to $80 K; 5=$80 k to $100 K; and 6 > $100 K. For Comfort with Computer and the Internet: 0=not at all comfortable, 1=a little bit comfortable, 2=somewhat comfortable, 3=quite comfortable, 4=very comfortable
Outcomes
Primary outcome measures were selected to reflect effects that were both suggested by prior research and that were intended to reflect effects of the three major service types. Secondary measures targeted constructs or outcomes that were exploratory in nature (e.g., measures of quality of life comprising physical health system and mobility items). These were selected to serve as pilot measures that could suggest new CHESS services or outcomes for future research.
Cancer Information Competence, a primary outcome measure, was with a five-item scale used in past CHESS studies (alpha = 0.80). Items assessed patients’ perceived ability to obtain and use health care information they felt they needed [13].
Health care competence was a five-item, shortened version of an eight-item scale used in previous CHESS research (alpha = 0.83; [8], assessing a woman’s comfort and activation level dealing with physicians and health care situations [14].
Emotional processing, another primary outcome measure, was a nine-item assessment developed for this research. It was designed to tap two domains we believed would be affected by CHESS: women’s reactions to their emotions and their appraisal of their emotion-coping skills. While other measures target emotional reaction, some CHESS services stress acceptance of negative emotions, and measures of this construct were not well-represented among extant, brief measures. Factor analysis indicated that the items on this measure should be treated as assessing a single dimension. High scores reflected reduced fear and greater acceptance of negative emotions, and improved coping. Using data from both studies at pretest revealed a coefficient alpha = 0.88 for this scale.
Positive coping was calculated by taking the mean (alpha = 0.76) of the eight positive items from Carver’s Brief Cope [17]; the humor, active coping, positive reframing, and planning subscales).
Functional well-being, another primary outcome measure, was assessed with the seven-item subscale of the FACT-B (the Functional Assessment of Cancer Therapy scale, [18] assessing a woman’s ability to carry out everyday activities (alpha = 0.87 from pretest data for these two studies).
Breast cancer concerns were measured with a FACT-B subscale on which women report their degree of concern about nine individual physical or social consequences of breast cancer and its treatment. Because these individual issues can occur independently of each other, their interdependence is modest (alpha = 0.59). Nevertheless, the scale reflects cumulative cancer-related burden.
Wisconsin social support scale
This six-item scale measures perceived and expected support (emotional, informational, and instrumental), and constitutes the fourth and final primary outcome. This instrument had high internal consistency in previous CHESS studies. In addition, access to CHESS has typically been associated with greater perceived support (alpha at pretest = 0.89).
Satisfaction with professionals
This single confidence-in-doctor item was taken from the FACT-B that was also used in prior CHESS studies.
RESULTS
The groups did not differ significantly on the characteristics listed in Table 2 (p > 0.14), except for income (p = 0.025), with one condition (Information+Support) showing slightly lower incomes than the Full CHESS condition, p < .05. These differences were not significant when using Shaffer’s correction for multiple tests [19].
Outcomes were analyzed with analyses of covariance in which baseline score on the outcome measures served as a covariate, along with factors selected on an a priori basis: age, education, minority status, and days since diagnosis. Separate tests were conducted at three different time points: 6 weeks, 3 and 6 months post-intervention access.2 Experimental condition (treatment group) served as the independent variable and dummy coding was used to compare each of the CHESS groups with the Internet control group. Given the weight of prior evidence on CHESS effects [8, 13, 14] and clear a priori directional hypotheses based on adding resources across the conditions of the design, we employed significance tests using one-tailed alpha = 0.05 (two-tailed values are indicated in tabular presentations for comparison with other studies using two-tailed tests.)
Table 3 shows results obtained for the targeted outcomes, including the four deemed as primary. The results show no significant effects for several of the outcomes (Functional Well-Being, Breast Cancer Concerns, and the Wisconsin Social Support Scale) but do show significant effects for the other five measures. However, these measures showed effects for only two of the three sets of group contrasts and then primarily at relatively brief follow-up intervals. Specifically, only the comparisons of the Internet Only condition with CHESS Information and with CHESS Information+Support yielded significant effects, and these occurred primarily at 6 weeks and 3 months. No significant effects were found when Full CHESS (Information + Support+Coaching) was compared with the Internet Only condition at any time point. The CHESS Information group significantly exceeded the Internet Only condition for Cancer Information Competence (6 weeks and 3 months), Health Care Competence (3 months), and Emotional Processing (6 weeks and 3 months). The CHESS Information and Support condition produced significantly higher ratings than did the Internet control group on Cancer Information Competence (6 weeks), Health Care Competence (6 weeks), Emotional Processing (3 months), Positive Coping (3 months), and Satisfaction with Professionals (6 weeks and 6 months).
Table 3.
Results
| Internet only | CHESS info only | CHESS info+support | Full CHESS info+support+coach | CHESS info>internet | CHESS info+support>internet | Full CHESS>internet | |
|---|---|---|---|---|---|---|---|
| Cancer information competence | |||||||
| 6 weeks | 2.92 | 3.13 | 3.15 | 2.98 | 0.01*, ** | 0.01*, ** | 0.27 |
| 3 months | 2.98 | 3.13 | 3.12 | 3.00 | 0.04* | 0.08 | 0.41 |
| 6 months | 3.11 | 3.14 | 3.15 | 3.01 | 0.38 | 0.33 | |
| Health care competence | |||||||
| 6 weeks | 2.93 | 3.07 | 3.17 | 2.93 | 0.08 | 0.01*, ** | |
| 3 months | 2.96 | 3.14 | 3.06 | 3.01 | 0.02*, ** | 0.15 | 0.27 |
| 6 months | 3.02 | 3.06 | 2.97 | 3.13 | 0.36 | 0.15 | |
| Emotional processing | |||||||
| 6 weeks | 2.42 | 2.56 | 2.54 | 2.51 | 0.02*, ** | 0.05 | 0.10 |
| 3 months | 2.47 | 2.65 | 2.66 | 2.57 | 0.02*, ** | 0.02*, ** | 0.12 |
| 6 months | 2.59 | 2.58 | 2.69 | 2.67 | 0.12 | 0.16 | |
| Positive coping | |||||||
| 6 weeks | 1.64 | 1.62 | 1.63 | 1.60 | |||
| 3 months | 1.50 | 1.58 | 1.65 | 1.60 | 0.15 | 0.03* | 0.08 |
| 6 months | 1.60 | 1.62 | 1.55 | 1.56 | 0.38 | ||
| Functional well-being | |||||||
| 6 weeks | 2.62 | 2.58 | 2.53 | 2.46 | |||
| 3 months | 2.62 | 2.70 | 2.67 | 2.50 | 0.20 | 0.31 | |
| 6 months | 2.83 | 2.85 | 2.80 | 2.85 | 0.40 | 0.42 | |
| Breast cancer concerns | |||||||
| 6 weeks | 1.17 | 1.16 | 1.28 | 1.22 | 0.43 | ||
| 3 months | 1.20 | 1.21 | 1.15 | 1.25 | 0.29 | ||
| 6 months | 1.14 | 1.19 | 1.10 | 1.20 | 0.33 | ||
| Social support | |||||||
| 6 weeks | 3.23 | 3.29 | 3.32 | 3.28 | 0.24 | 0.14 | 0.28 |
| 3 months | 3.16 | 3.28 | 3.28 | 3.22 | 0.09 | 0.09 | 0.26 |
| 6 months | 3.26 | 3.28 | 3.28 | 3.23 | 0.38 | 0.38 | |
| Satisfaction with professionals | |||||||
| 6 weeks | 3.17 | 3.28 | 3.46 | 3.32 | 0.16 | 0.01*, ** | 0.10 |
| 3 months | 3.26 | 3.30 | 3.40 | 3.17 | 0.38 | 0.14 | |
| 6 months | 3.28 | 3.38 | 3.48 | 3.31 | 0.15 | 0.03* | 0.37 |
Means are covariate-adjusted for age, education, minority status, days since diagnosis, and pretest level of the dependent variable. The primary outcome measures were Cancer Information Competence, Emotional Processing, Functional Well-Being, and Social Support
*p < 0.05, one-tailed; **p < 0.05, two-tailed
DISCUSSION
These results are consistent with prior research showing beneficial effects of eHealth interventions for people with a cancer diagnosis (e.g., [3]; [7]). More specifically, the results replicate earlier research showing that CHESS can positively affect the cancer patient’s sense of competence in dealing with cancer and health care information [13, 14]. It is noteworthy that CHESS benefits were obtained relative to a control condition that provided internet access (a loaned computer if needed and payment for 6 months internet access) and training in internet searching, in addition to usual care resources. In short, patients in the control group had ready access to multiple extensive eHealth and other resources. This makes the test of CHESS impact fairly conservative.
That some CHESS conditions proved superior to such a set of additional treatments replicates earlier research [8], suggesting that quality variations, navigation differences, and the appearance of redundancy across internet sites may limit the benefits patients derive from unstructured internet access. However, the present results do not isolate whether CHESS superiority over unstructured access to the internet stems from its content, its navigation, or its structure.
In addition to showing effects on cancer and health care information competence, findings showed that some CHESS interventions increased the patient’s sense that she could cope with emotions and positively affected the patient’s satisfaction with her health care professionals. We had expected that the patient’s appraisal of her emotional coping would be most affected by the Full CHESS condition, which offered emotion focused skill training; but, the effects were significant only for the other two versions of CHESS (Information and Information and Support). Also, contrary to our hypotheses, there was little evidence that CHESS positively affected patients’ general sense of quality of life or that it increased perceived social support, both of which were identified a priori as important outcomes of intervention.
The results suggest the benefits of CHESS are produced largely by the Information and Support services. The more complex Coaching services, and the attempt to tailor content to the patient’s treatment status and concerns, produced little or no benefit beyond effects obtained from internet access per se. In fact, the data suggest the more complex CHESS Coaching services may have reduced the benefit of the otherwise beneficial services, although this was not formally tested.
The relatively poor results observed with Full CHESS could be due to the increased complexity of the combined service, inadequacies in the Coaching services, or a reduced breadth of information and services to which full CHESS patients were exposed because of the tailoring (i.e., because it may have prematurely narrowed women’s information search activities).
Other research shows that computer coaching can produce benefit across numerous health conditions. For instance, there is considerable evidence that computer-delivered CBT has been effective for conditions such as bulimia, anxiety disorders, substance abuse disorders, and depression [20–24]. This raises the question of why such coaching services were not effective in the current study (which comprised CBT among other services). It is always possible that the coaching services were not as well-executed in this study as in others. However, these services went through the same intensive development and vetting as the other CHESS services, and they had proved popular with other types of patients [25]. It may be that the effectiveness of the Coaching services was attenuated in this research because: (1) They were offered with a host of other services, and (2) They were offered at a time when women were not receptive to new learning and mastering their relatively complex content in order to achieve behavior change. With regard to the first point, most successful uses of coaching services have not presented those services along with multiple other services (e.g., extensive information services). In the current research, the availability of so many services may have overwhelmed users or caused them to ignore the more complex services. In fact, other research has produced evidence that more complex eHealth interventions can produce decreased use [26] or effects [27]. Thus, there is supportive evidence that complexity may interfere with impact [6]. With regards to the second point, women who are newly diagnosed with breast cancer are often suffering from emotional turmoil, having to make great changes in their lives, and having to make momentous decisions with life-altering consequences. It may be that women newly diagnosed with breast cancer are less able or willing than other patient groups to devote the energy, time, and cognitive resources that are required to derive benefit from such coaching. This suggests that blanket judgments about eHealth services are inappropriate; rather, services should be evaluated within context comprising information about patient type, disease status, competing demands, patient goals, emotional state, and so on.
While there was evidence of superiority of some CHESS services over internet access, it is important to recognize that the evidence of this superiority was found on only some measures and primarily early in the treatment period (e.g., not at 6 months), consistent with earlier reports that CHESS effects are larger early in the course of intervention [8]. An examination of effect sizes for some of the tests in the present study revealed smaller effects relative to effects obtained in some earlier research with CHESS. For instance, earlier experimental evaluations of CHESS relative to internet access yielded an effect size of 0.47 on a social support measure [8], in contrast to effect sizes here <0.20. We obtained fairly weak effects on two of the four measures that were identified as primary in this research (Social Support and Function Well-Being [quality of life]).
If CHESS effects have diminished over time, relative to internet access per se, this may be because internet resources have improved over time and CHESS no longer holds such an edge with regard to integration, ease of navigation, and so on. Or this may reflect increasing population sophistication in internet use, so that internet shortcomings are no longer significant barriers to benefit.
As noted, the results also suggest that CHESS effects tend to be strongest early in the course of the patient’s illness. This suggests that CHESS or similar ICCSs may provide their greatest benefits while patients are in the midst of early struggles with their illness and treatments, but may produce little residual advantage over internet use. However, it is important to recognize that CHESS might produce longer-lasting benefit in comparison to a noninteractive (i.e., non-ICCS) intervention. Research has shown that CHESS effects relative to a usual care control (only book or audio tape resources provided) were strongest 6 and 9 months post-intervention [8]. In contrast, the advantage over an internet access control was large initially (after 2 months, in that study) but decreased to nonsignificance by 9 months [8]. Thus, the current results may actually underestimate the size and durability of ICCS effects because the internet access control condition gave women access to some high-quality ICCS resources, and the benefits of such access may increase over time (there is evidence of some improvement over time on several measures among individuals in the Internet Only condition, perhaps because women learn to navigate the complex Internet environment).
To summarize, to the extent that CHESS services represent high-quality ICCS services, the results suggest that, relative to internet access: (a) ICCS-delivered information produces significant benefit to patients; (b) there is modest evidence that provision of Support services adds to the benefits of Information services (e.g., with regards to satisfaction with health care professionals), but this finding must be tempered by the fact that Support services did not appear to affect ratings of perceived support, a primary target of this type of service; (c) the benefits of Information and Support services primarily occur with regard to patients’ sense that they can cope competently with health care information and their emotions (e.g., learning to be less afraid of emotions); (d) the interactive Coaching services did not appear to aid these newly diagnosed women, and there was some suggestion that these services might have reduced the benefit yielded by the Information and Support services; and (e) ICCS benefits are greatest within the first several months of the cancer diagnosis and treatment.
One question arising from these results concerns the clinical significance of the findings. How meaningful is it that the best CHESS intervention (Information+Support) produced relatively transitory effects on information and healthcare competence, emotional coping, and satisfaction with professionals? First, for the average patient significant effects occurred over 3–4.5 months after diagnosis (given that CHESS access lagged diagnosis by about 6–8 weeks), when many patients were highly concerned about the ultimate course of their illness and were struggling with stressful effects of treatment. In this light, the transitory nature of the effects may not be terribly concerning because the treatment had an effect when the women may have most needed support. Second, the value of these effects may be gauged by the specific questions from the measures upon which the treatments differed. Questions from some of these measures include: “I feel that I am in control over how and what I learn about my health” (Cancer Information Competence); “I knew the right question to ask” and “I felt comfortable with how actively I participated in my care” (Health Care Competence); “Since I learned I had cancer I have seen some worth in negative emotions” and, “Since I had cancer I have gained some control over my negative emotions” (Emotional Process Assay); and “I had confidence in my doctor” (Satisfaction with Professionals). These outcomes seem of clear clinical importance for patients coping with breast cancer and for their clinicians. It is less clear from these results how important these ICCS effects are to other stakeholders such as insurers and health care systems. As noted in previous reviews [3], future research should address whether ICCS availability and use affects a broad array of outcomes such as health economic endpoints.
In sum, this research suggests that a comprehensive ICCS should probably include both information and support services that link patients with one another and with health experts. The results suggest that more complex ICCS services involving Coaching/skills training (at least of the sorts tested) along with tailoring (to encourage patients to focus on the most relevant information) do not enhance outcomes, at least not when added to Information and Support services provided to newly diagnosed breast cancer patients. The results also suggest that most ICCS effects are maximal within a few months of study entry. However, interpretation of this effect must be tempered by recognition that the patients did not have access to the tested services for 6–8 weeks, on average, after their diagnoses; this delay in access to CHESS may have caused all women to spend their first 1–2 months post-diagnosis searching for answers on the internet. This delay may have seriously reduced CHESS benefit as women did not have access to CHESS when they needed it most. A critical goal of future research would be to test the effects of CHESS when patients have almost immediate access to it after receiving their diagnosis. This research also suggests that ICCS effects tend to occur in the domains of information competence, emotional processing, and satisfaction with health care.
Limitations
The limitations of this research include the use of multiple tests at three follow-up intervals, which increased the odds of experiment-wise error. We decided it was vital to include three follow-up occasions in the analysis to show the temporal pattern of effects. Concerns with experiment-wise error caused us not to make all possible inter-group tests (e.g., experimental groups were not directly compared with one another). Also, while some recommend that only a single primary measure be used for analyses [28], we thought it was important to include a general measure, and also measures designed to assess each of the major service types. This approach reflects both the multi-attribute nature of the CHESS intervention and the diversity of women’s experiences of and responses to breast cancer. Other concerns are that even with the range of outcome measures used, some important outcomes were not assessed (e.g., health system utilization and economic impact). And, type of CHESS service was inextricably confounded with complexity of the CHESS intervention; e.g., Coaching services were always added to the other two types of services. Therefore, the data may reflect reactions to the total package of services and not just to the added service.
We did not gather precise measures of the other communication, psychosocial, and eHealth resources that women used outside of the experimental ones, and we did not control such use, which no doubt increases error and reduces power. Because the types and numbers of eHealth and psychosocial services in this area are constantly evolving, it is likely that control conditions reflect the impacts of multiple, evolving interventions available via usual care or internet searches, thereby creating a constantly shifting benchmark against which experimental interventions are evaluated. Furthermore, the present results are generalizable only to the extent that CHESS and its services are representative of the types of intervention services they are designed to model. Finally, in the current paper, we did not examine moderation of CHESS effects to determine if some types of patients benefitted more than others, and we did not relate outcomes to CHESS use patterns. Both of these topics will be addressed in subsequent reports of this work.
In closing, despite all the internet resources available for cancer patients, it nevertheless appears that there is some incremental benefit to being provided with, and directed to, a single comprehensive and integrated ICCS (in this case, CHESS). It is unknown why these resources provided relative benefit over unstructured internet access. However, the results of this research may provide a clue—as resource complexity increases, the signal-to-noise ratio declines and it may become more difficult to use and benefit from eHealth resources. Thus, the results suggest that integrated, focused cancer information and communication services may best support a broad range of women newly diagnosed with breast cancer and that additional sorts of service types do not necessarily add benefit.
Acknowledgements
We thank the women who agreed to participate in our study. Additionally, we thank Haile Berhe and Gina Landucci for technical contributions.
The study was funded by P50 CA095817-05 from the National Cancer Institute. Dr. Baker was supported in part by grant #1K05CA139871 from the National Institutes of Health. No other author had potential conflicts to disclose.
Footnotes
Two other measures were originally viewed as primary (a measure of health care utilization and marital satisfaction), but these are no longer viewed as primary due to limitations in the quality of the utilization measure and changes in the development of the relationship intervention.
All randomized subjects with data at a follow-up time point were included in analyses. Also, data were gathered at 12 months post-treatment but are not reported. We did not expect significant treatment effects to persist for 12 months [8], and they did not. In fact, as will be apparent from the data to be presented, the significant effects tended to occur early in the course of treatment.
Implications
Practice: Patients can derive significant benefit from this ICCS and its use may enhance patients’ satisfaction with their health care professional. While this issue was not studied formally, informal reports and observations produced no evidence that CHESS interfered with the clinician-patient relationship.
Policy: Health care systems should support the development or adoption of well-designed, integrated ICCSs for breast cancer, as evidence shows that such systems yield more benefit than simple access to the internet.
Research: This paper suggests that it is wise to take a nuanced or contextualized perspective when drawing conclusions about the effects of eHealth interventions. Such effects may differ with regard to type of service, intensity, time periods appraised, type of outcome, and probably type of clinical problem and population.
References
- 1.Baker TB, McFall RM, Shoham V. Current status and future prospects of clinical psychology: toward a scientifically principled approach to mental and behavioral health care. Psychol Sci Public Interest. 2009;9(2):67–103. doi: 10.1111/j.1539-6053.2009.01036.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Bright MA, Fleisher L, Thomsen C, Morra ME, Marcus A, Gehring W. Exploring e-Health usage and interest among cancer information service users: the need for personalized interactions and multiple channels remains. J Health Commun. 2005;10(Suppl 1):35–52. doi: 10.1080/10810730500265609. [DOI] [PubMed] [Google Scholar]
- 3.Butler LH, Correia CJ. Brief alcohol intervention with college student drinkers: face-to-face versus computerized feedback. Psychol Addict Behav. 2009;23(1):163–167. doi: 10.1037/a0014892. [DOI] [PubMed] [Google Scholar]
- 4.Cartreine JA, Ahern DK, Locke SE. A roadmap to computer-based psychotherapy in the United States. Harv Rev Psychiatry. 2010;18(2):80–95. doi: 10.3109/10673221003707702. [DOI] [PubMed] [Google Scholar]
- 5.Carver SJ. You want to measure coping but your protocol is too long: consider the Brief COPE. Int J Behav Med. 1997;4:92–100. doi: 10.1207/s15327558ijbm0401_6. [DOI] [PubMed] [Google Scholar]
- 6.Cella DF, Tulsky DS, Gray G, et al. The functional assessment of cancer therapy scale: development and validation of the general measure. J Clin Oncol. 1993;11(3):570–579. doi: 10.1200/JCO.1993.11.3.570. [DOI] [PubMed] [Google Scholar]
- 7.Danaher BG, Seeley JR. Methodological issues in research on web-based behavioral interventions. Ann Behav Med. 2009;38(1):28–39. doi: 10.1007/s12160-009-9129-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Glasgow RE, Nelson CC, Kearney KA, et al. Reach, engagement, and retention in an Internet-based weight loss program in a multi-site randomized controlled trial. J Med Internet Res. 2007;9(2):e11. doi: 10.2196/jmir.9.2.e11. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Gustafson DH, Hawkins R, Boberg E, et al. Impact of a patient-centered, computer-based health information/support system. Am J Prev Med. 1999;16(1):1–9. doi: 10.1016/S0749-3797(98)00108-1. [DOI] [PubMed] [Google Scholar]
- 10.Gustafson DH, McTavish FM, Boberg E, et al. Empowering patients using computer based health support systems. Qual Health Care. 1999;8(1):49–56. doi: 10.1136/qshc.8.1.49. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Gustafson DH, Hawkins RP, Boberg EW, et al. CHESS: ten years of research and development in consumer health informatics for broad populations, including the underserved. Stud Health Technol Inform. 2001;84(Pt 2):1459–1563. [PubMed] [Google Scholar]
- 12.Gustafson DH, Hawkins R, Pingree S, et al. Effect of computer support on younger women with breast cancer. J Gen Intern Med. 2001;16(7):435–445. doi: 10.1046/j.1525-1497.2001.016007435.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Gustafson DH, Hawkins R, McTavish F, et al. Internet-based interactive support for cancer patients: are integrated systems better? J Commun. 2008;58(2):238–257. doi: 10.1111/j.1460-2466.2008.00383.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Gysels M, Higginson IJ. Interactive technologies and videotapes for patient education in cancer care: systematic review and meta-analysis of randomised trials. Support Care Cancer. 2007;15(1):7–20. doi: 10.1007/s00520-006-0112-z. [DOI] [PubMed] [Google Scholar]
- 15.Hawkins R. Integrating eHealth with human services for breast cancer patients. Patient Educ Couns. in press [DOI] [PMC free article] [PubMed]
- 16.Horrigan, J., & Raine, L. (2002). Counting on the internet. Washington, DC: Pew Internet and American Life Project.
- 17.Japuntich SJ, Zehner ME, Smith SS, et al. Smoking cessation via the internet: a randomized clinical trial of an internet intervention as adjuvant treatment in a smoking cessation intervention. Nicotine Tob Res. 2006;8(Suppl 1):S59–S67. doi: 10.1080/14622200601047900. [DOI] [PubMed] [Google Scholar]
- 18.Kay-Lambkin FJ, Baker AL, Lewin TJ, Carr VJ. Computer-based psychological treatment for comorbid depression and problematic alcohol and/or cannabis use: a randomized controlled trial of clinical efficacy. Addiction. 2009;104(3):378–388. doi: 10.1111/j.1360-0443.2008.02444.x. [DOI] [PubMed] [Google Scholar]
- 19.Lenert L. Automating smoking cessation on the web. WATI: Web-assisted Tobacco Intervention. Available at: http://www.wati.net/presentations/watiII.lenert.pres.20050607.pdf. Accessed July 14, 2010
- 20.Moher D, Hopewell S, Schulz KF, CONSORT et al. Explanation and elaboration: updated guidelines for reporting parallel group randomised trials. BMJ. 2010;340:c869. doi: 10.1136/bmj.c869. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Murray E, Burns J, See TS, Lai R, Nazareth I (2005) Interactive Health communication applications for people with chronic disease. Cochrane Database Syst Rev (4):CD004274 [DOI] [PubMed]
- 22.Reger MA, Gahm GA. A meta-analysis of the effects of internet- and computer-based cognitive-behavioral treatments for anxiety. J Clin Psychol. 2009;65(1):53–75. doi: 10.1002/jclp.20536. [DOI] [PubMed] [Google Scholar]
- 23.Serlin RC. Confidence intervals and the scientific method: a case for Holm on the range. J Exp Educ. 1993;61:350–360. [Google Scholar]
- 24.Shapiro JR, Reba-Harrelson L, Dymek-Valentine M, Woolson SL, Hamer RM, Bulik CM. Feasibility and acceptability of CD-ROM-based cognitive–behavioural treatment for binge-eating disorder. Eur Eat Disord Rev. 2007;15(3):175–184. doi: 10.1002/erv.787. [DOI] [PubMed] [Google Scholar]
- 25.Smaglik P, Hawkins RP, Pingree S, Gustafson DH, Boberg E, Bricker E. The quality of interactive computer use among HIV-infected individuals. J Health Commun. 1998;3(1):53–68. doi: 10.1080/108107398127508. [DOI] [PubMed] [Google Scholar]
- 26.Spring B, Pagoto S, Knatterud G, Kozak A, Hedeker D. Examination of the analytic quality of behavioral health randomized clinical trials. J Clin Psychol. 2007;63(1):53–71. doi: 10.1002/jclp.20334. [DOI] [PubMed] [Google Scholar]
- 27.Strecher V. Internet methods for delivering behavioral and health-related interventions (eHealth) Annu Rev Clin Psychol. 2007;3:53–76. doi: 10.1146/annurev.clinpsy.3.022806.091428. [DOI] [PubMed] [Google Scholar]
- 28.Tate DF, Zabinski MF. Computer and Internet applications for psychological treatment: update for clinicians. J Clin Psychol. 2004;60(2):209–220. doi: 10.1002/jclp.10247. [DOI] [PubMed] [Google Scholar]