Abstract
PTEN Hamartoma Tumour Syndrome (PHTS) includes Cowden syndrome (CS), Bannayan-Riley-Ruvalcaba syndrome (BRRS), and other conditions resulting from germline mutation of the PTEN tumour suppressor gene. Although macrocephaly, presumably due to megencephaly, is found in both CS and BRRS, the prevalence and degree have not been formally assessed in PHTS. We evaluated head size in a prospective nested series of 181 patients found to have pathogenic germline PTEN mutations. Clinical data including occipital-frontal circumference (OFC) measurement were requested for all participants. Macrocephaly was present in 94% of 161 evaluable PHTS individuals. In patients ≤18 years, mean OFC was +4.89 standard deviations (SD) above the population mean with no difference between genders (P=0.7). Among patients >18 years, average OFC was 60.0 cm in females and 62.8 cm in males (P<0.0001). To systematically determine whether macrocephaly was due to megencephaly, we examined PtenM3M4 missense mutant mice generated and maintained on mixed backgrounds. Mice were killed at various ages, brains were dissected out and weighed. Average brain weight for PtenM3M4 homozygous mice (N=15) was 1.02 g compared with 0.57 g for heterozygous mice (N=29) and 0.49 g for wild-type littermates (N=24) (P<0.0001). Macrocephaly, secondary to megencephaly, is an important component of PHTS and more prevalent than previously appreciated. Patients with PHTS have increased risks for breast and thyroid cancers, and early diagnosis is key to initiating timely screening to reduce patient morbidity and mortality. Clinicians should consider germline PTEN testing at an early point in the diagnostic work-up for patients with extreme macrocephaly.
Keywords: PTEN Hamartoma Tumour syndrome, Cowden syndrome, Bannayan-Riley-Ruvalcaba syndrome
Introduction
PTEN Hamartoma Tumour Syndrome (PHTS) is a molecularly-defined umbrella term used to describe individuals with Cowden Syndrome (CS, OMIM 158350), Bannayan-Riley-Ruvalcaba Syndrome (BRRS, OMIM 153480), and other conditions with germline mutations of the PTEN tumour suppressor gene, localised to 10q23. CS is an autosomal dominant disorder which is difficult to recognise and is characterised by multiple hamartomas and an up to 50% lifetime risk of female breast cancer and 10% risk of epithelial thyroid cancer.1, 2 It is assumed that individuals carrying broad clinical diagnoses and germline PTEN mutations, that is, PHTS, carry similar risks but this has not been formally assessed. The central nervous system in PHTS is also affected, causing increased risks for Lhermitte-Duclos disease, developmental disabilities, and autism spectrum disorders.3, 4 For purposes of initial gene discovery, strict phenotypic criteria for ascertainment were developed, and if followed closely, resulted in an 80% PTEN mutation frequency.5 Unfortunately, CS is difficult to recognise and the complex criteria developed for the gene discovery phase are challenging to use in a clinical setting. For purposes of clinical care, therefore, operational diagnostic criteria for CS have been developed which include macrocephaly as a major feature;6 macrocephaly has also long been recognised as a hallmark characteristic of BRRS.7, 8 However, the true prevalence of macrocephaly is uncertain. A population-based study in Amsterdam including a review of the literature at that time cited a weighted prevalence of 21%,2 whereas two other retrospective studies from tertiary referral centers found macrocephaly in 100% of patients studied.9, 10
In addition to PHTS, macrocephaly is a component of many other genetic syndromes, a few of which have had occipital-frontal circumference (OFC) norms ascertained and published. However, the systematic ascertainment and characterisation of head circumference has not been performed in CS or BRRS nor in the molecularly defined PHTS. Furthermore, while it is presumed that the aetiology of the macrocephaly is megencephaly from single case-report imaging,11 we do not know if this is the case. Therefore, we sought to systematically measure and characterise the OFC from our adult and paediatric research participants found to have germline pathogenic PTEN mutations. In addition, we weighed the brains of a mouse model with mono-allelic and biallelic knock-in Pten mutations in order to ascertain whether the macrocephaly actually reflects megencephaly.
Materials and methods
From October 15, 2005 to May 27, 2010, 2827 eligible patients were enrolled into Cleveland Clinic IRB# 8458 (as approved by the Cleveland Clinic Human Subjects' Protection Committee) if they minimally met the following: ‘relaxed' criteria for the diagnosis of CS (presence of two major/pathognomonic, one major/pathognomonic + two minor, or three minor characteristics of Cowden syndrome per the International Cowden Consortium diagnostic criteria6); presence of macrocephaly and developmental disability/autism; presence of penile freckling; or presence of a known germline PTEN alteration. Clinical data including OFC measurement were requested for all participants. OFC was measured by either the referring provider or a physician member of the patient's healthcare team.
Mutation analysis for all subjects included promoter sequencing and mutation scanning by denaturing gel gradient electrophoresis (DGGE) or LightScanner; variants detected by DGGE or LightScanner were confirmed with single exon Sanger sequencing as per routine of the Eng lab. Samples from patients meeting ICC criteria, those with macrocephaly and developmental disability/autism, and those with a personal/family history of a known large PTEN rearrangement also underwent multiplex ligation probe assay (MLPA); identified rearrangements were confirmed with quantitative PCR.
Macrocephaly was defined as greater than or equal to 2 standard deviations (SD) above the mean. SD data for patients were calculated using norms derived from the Nellhaus charts for males and females12 due to their common use in clinical genetics and paediatrics. Pearson's correlation was used to assess the strength and direction of linear association between height and OFC. The association between OFC and height was assessed with a linear regression model. Differences between groups were analysed by unpaired t-test.
PtenM3M4 missense mutant mice were generated in our lab and maintained on mixed 129/CD-1, 129/AJ/C57BL/6J, or 129/CD-1/C57BL/6J backgrounds for these studies (Eng et al, unpublished). Mice were killed at various ages; brains were dissected out and weighed before further processing (n=68). All protocols involving mice were approved by the Institutional Animal Care and Use Committee at the Cleveland Clinic. ANOVA was used to compare brain weight across genotypes, and mixed-effects regression models were computed using brain weight as the dependent variable. Genotype, sex, age, and background were independent variables. Models were estimated using SPSS Version 18.
Results
In our series of 2827 research participants, 181 were found to have pathogenic germline PTEN mutations. To be rigorous, participants with variants of unknown significance and promoter variants that were not functionally validated were not used for this study. Of the 161 individuals with germline pathogenic mutations with OFC information reported, 152 (94.4%) were macrocephalic as defined by an OFC measurement ≥2 SD over the mean (Table 1). There were no significant differences in age or gender between the patients with known and unknown OFC data.
Table 1. OFC status by gender and age.
| Females | Males | |
|---|---|---|
| All patients | ||
| Macrocephalic | 75 | 77 |
| Normocephalic | 6 | 3 |
| OFC status unknown | 13 | 7 |
| Patients ⩽18 years | ||
| Macrocephalic | 17 | 36 |
| Exact OFC and date measured confirmed | 15 | 30 |
| Normocephalic | 0 | 2 |
| Exact OFC and date measured confirmed | — | 2 |
| OFC status unknown | 0 | 0 |
| Mean SD of OFC | +5.04 | +4.83 |
| SD | 1.70 | 1.82 |
| SEM | 0.44 | 0.31 |
| Patients >18 years | ||
| Macrocephalic | 58 | 41 |
| Exact OFC known | 50 | 30 |
| Exact OFC and height known | 40 | 23 |
| Normocephalic | 6 | 1 |
| Exact OFC known | 5 | 1 |
| Exact OFC and height known | 4 | 1 |
| OFC status unknown | 13 | 7 |
| Mean OFC (cm) | 60 | 62.8 |
| SD | 2.47 | 2.23 |
| SEM | 0.33 | 0.40 |
| Mean SD of OFC | +3.54 | +5.24 |
| SD | 1.77 | 1.72 |
| SEM | 0.24 | 0.31 |
Of our 86 adults with germline PTEN mutations and OFC measurements, OFC for adult females averaged 60.0 cm (SD 2.47 cm, 95% CI 59.3–60.6) and for males averaged 62.8 cm (SD 2.23 cm, 95% CI 62.0–63.6) (P<0.0001). There was a significant correlation between OFC and height in adult men (r=0.563, P=0.004) and to a lesser extent, adult women (r=0.346, P=0.021) (Figures 1a and b).
Figure 1.
Adult PHTS patients' OFCs plotted against height for (a) female and (b) male patients, with trendline demonstrating positive correlation between OFC and height. Diamonds represent individual patient measures.
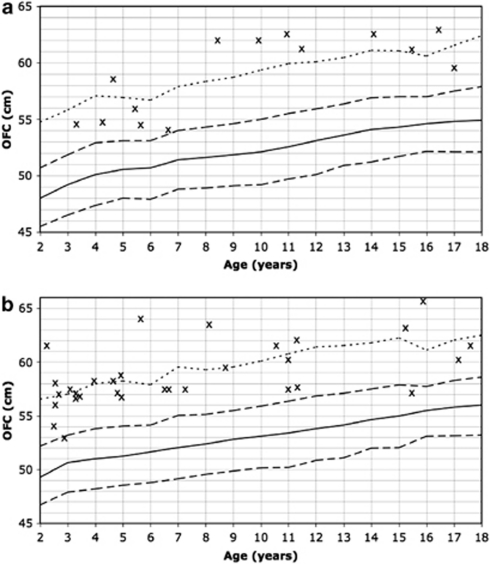
Of the 47 research participants aged 18 years and younger with germline PTEN mutations and OFC measurements, OFC averaged +4.89 SD (SD 1.76; 95% CI 4.4–5.4) above the mean, with no difference between genders (P=0.7). Of the 15 females, none were within +2 SD of the mean, whereas 8 (53%) had OFC beyond +5 SD above the mean (Figure 2a). Of the 32 males, 2 (6%) were within +2 SD of the mean, whereas 13 (40%) had OFC above +5 SD (Figure 2b). We also observed a significant difference in mean OFC by SD values over population norms between paediatric and adult females (P=0.0047), but the difference between paediatric and adult males was not significant (P=0.36).
Figure 2.
Measured OFC in PTEN mutation-positive patients aged 18 and under plotted on the Nellhaus curves for (a) females and (b) males. Solid line=50th centile; dashed line=+/− 2 SD; dotted line=+5 SD; x=individual patient measures.
We then examined whether macrocephaly was associated with any particular PTEN genotype. Among the 86 adults with OFC data known, 36 (42%) had missense mutations. Adults with missense mutations had an average OFC of +3.7 SD compared to adults with truncating or whole gene deletion mutations (average OFC +4.5 SD, P=0.07). Among the nine patients with normal OFC (Table 2), missense mutations seemed slightly overrepresented compared with truncating mutations; however, this association was not significant (P=0.28). Five of these adult patients had missense mutations in exon 9 (Table 3).
Table 2. Clinical features and PTEN genotype for patients with normal OFC.
| ID | M/F | Age | OFC (cm) | SD | Mutation | Exon | Protein | PHTS Features | Meets ICC criteria |
|---|---|---|---|---|---|---|---|---|---|
| 0780 | M | 3 | 53 | +1.85 | c.44ins16 | 1 | FS | GM, HH, L, DD | No: PLS |
| 2610 | M | 15 | 57 | +1.38 | c.586insT | 6 | FS | DD, L, OMP, PF, TN | No: BRRS |
| 5153 | M | 41 | 57 | +0.77 | c.441insAdelGG | 5 | FS | L, F, Ham, OMP, PF, TN | Yes |
| 0004 | F | 26 | ? | ? | c.655C>T | 7 | p.G219X | AK, GT, F, L, ThyCA | Yes |
| 4340 | F | 47 | 53 | −1.43 | c.235G>A | 4 | p.A79T | FBD, BrCA, L, OMP, TN, UF | Yes |
| 1509 | F | 48 | 56 | +0.71 | c.1066A>G | 9 | p.N356D | FBD, TN, ThyCA | No |
| 2094 | F | 48 | 53.3 | −1.21 | c.1061C>A | 9 | p.P354Q | BrCA, FBD, UF | No |
| 2438 | F | 49 | 57 | +1.43 | c.1033C>G | 9 | p.L345V | FBD, BrCA, TN, UtCA, UF | Yes |
| 0622 | F | 52 | 57.2 | +1.57 | c.406T>C | 5 | p.C136R | TN, FBD, BrCA, L, ThyCA, UtCA | Yes |
Age, age at measurement of OFC; ?, unknown.
Abbreviations: AK, Acral keratoses; BrCA, Breast cancer; BRRS, Bannayan-Riley-Ruvalcaba syndrome; DD, Developmental delay; FCBD, Fibrocystic breast disease, F, Fibroma; FS, frameshifting mutation; GM, Genitourinary malformation; GT, Genitourinary tumour; Ham, Hamartomatous GI polyp; HH, Hemihyperplasia; L, lipoma; OMP, oral mucosal papillomatosis; PF, penile freckling; PLS, Proteus-like phenotype; ThyCA, epithelial thyroid carcinoma; TN, Thyroid nodules or goiter; Trich, Trichilemmomas; UF, uterine fibroids; UtCA, Uterine carcinoma.
Table 3. Clinical features and PTEN genotype for patients with exon 9 missense mutations.
| ID | Age | M/F | Mutation | Protein | Macrocephaly | Other CS features | Meets ICC Criteria |
|---|---|---|---|---|---|---|---|
| 2438 | 57 | F | c.1033C>G | p.L345V | No | BrCA, UtCA, FCBD, TN, UF | Yes |
| 1509 | 49 | F | c.1066A>G | p.N356D | No | ThyCA, FCBD, TN | No |
| 2094/1 | 49 | F | c.1061C>A | p.P354Q | No | BrCA, FCBD, UF | No |
| 2094/2 | 56 | F | c.1061C>A | p.P354Q | Unknown | FCBD, GT | No |
| 294 | 43 | F | c.1027-2A>C | Splice | Yes | OMP, Trich, FCBD, TN, L | Yes |
Age, age at measurement of OFC.
Abbreviations: AK, Acral keratoses; BrCA, Breast cancer; FCBD, Fibrocystic breast disease, GT, Genitourinary tumour; L, lipoma; OMP, oral mucosal papillomatosis; ThyCA, epithelial thyroid carcinoma; TN, Thyroid nodules or goiter; Trich, Trichilemmomas; UF, uterine fibroids; UtCA, Uterine carcinoma.
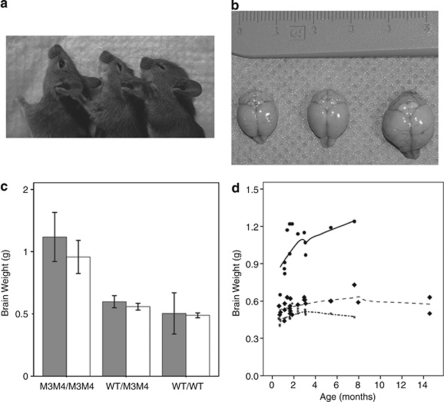
Mice that are homozygous or heterozygous for missense Pten mutation have obvious macrocephaly by inspection (Figure 3a). To directly determine whether their macrocephaly is secondary to megencephaly, we measured brain weight for 44 mice, which were either homozygous (N=15) or heterozygous (N=29) for germline missense mutation in Pten under the endogenous promoter, along with 24 wild-type littermates. Average brain weight for PtenM3M4 mutant mice was 1.02 g (SD 0.19g, 95% CI 0.9–1.1), compared with 0.57g (SD 0.06 g, 95% CI 0.55–0.60) for heterozygous mice and 0.49 g (SD 0.04 g, 95% CI 0.47–0.51) for wild-type mice (F2, 65=139.96 (P<0.0001), Figures 3a and b). Older age and male sex also independently predicted brain weight (F1, 52=5.34, P=0.025; F1, 52=4.99, P=0.030). A trend toward an interaction between sex and genotype (F2, 52=2.73, P=0.075) (Figures 3b and c) was also observed; male PtenM3M4 mutant and heterozygous mice trended toward even larger brain weights relative to female mice. Importantly, the genetic background of the mice did not predict brain weight (F3, 52=0.386, P=0.76).
Figure 3.
Brain weight from mice with wild-type Pten, or homozygous and heterozygous missense mutations in Pten. (a) Wild-type (left), heterozygote (center), and homozygous mutant (right) littermate female mice at 5 weeks of age, demonstrating obvious macrocephaly in the homozygote. (b) A representative image of wild-type (left), heterozygous (center), and homozygous mutant (right) brains from littermate mice at 2 months of age. (c) Brain weight increases with dose of mutant Pten, potentially interacting with sex (males – grey, females – white). (d) Brain weight with age in PtenM3M4/M3M4 (circles), PtenWT/M3M4 (diamonds), and PtenWT/WT mice (stars). Note that brain weights of heterozygotes begin to differ from wild-type mice only by 3 months of age.
Discussion
By clinical anecdote, macrocephaly is an accepted component of CS and BRRS. In the only population-based clinical epidemiologic study of CS in the Amsterdam area in the 1980's, the prevalence of macrocephaly was estimated at 25%.2 This epidemiologic study was undertaken before PTEN was identified as the CS predisposition gene. Taken together with review studies, prevalence estimates for macrocephaly in CS range from 25 to 38%.1, 13, 14 However, a systematic prospective study of OFC in a series of individuals carrying germline PTEN mutations has never been undertaken. We found that 94% of our prospective series of individuals with PHTS have OFC +2.0 to +6.9 SD (mean +3.5 SD) over population norms. In the paediatric PHTS patients, average OFC was almost +5 SD over population norms. In our prospective series of 3042 probands accrued with classic CS or Cowden-like features, macrocephaly was identified in only 33% of PTEN mutation-negative research participants (compared with 83% in mutation-positive individuals; P<0.0001). We concluded that macrocephaly was a necessary, but not sufficient, criterion for PTEN mutation testing in the paediatric population and carried significant weight towards recommending testing in the adult population.15
OFC is a straightforward measurement that can be easily performed by any health caregiver. However, our understanding of its relationship to height in the adult population and ethnic background remains rudimentary. Studies of paediatric populations in different countries find differences in OFC norms that one would think would continue into adulthood. Interestingly, the data from our murine model show little variation in brain weight despite different genetic backgrounds for each Pten genotype. Therefore, data from a large study of adult human head circumference and correlation with height and ethnicity would be helpful to have for more accurate comparative purposes and to better understand whether differences in ethnic background contributes to significant differences in OFC measurement in an adult population.
In the patient presenting to genetics clinic with macrocephaly as a chief complaint, the clinician's syndromic differential diagnosis is extensive. An OMIM search for syndromes with ‘macrocephaly' within the clinical synopsis reveals 103 syndromes for which clinical testing is available or a diagnosis could be made based on clinical and laboratory assessment. Head circumference has been systematically assessed in patients with Fragile X,16 Nevoid Basal Cell Carcinoma (NBCCS),17 Neurofibromatosis 1,18 and Sotos19, 20 syndromes. In Fragile X syndrome, OFC for most patients falls into the normal range, with the 5th, 50th, and 95th centiles for the patient population being consistently just slightly above the respective normal centiles. A small series of patients with NBCCS found only probands to be macrocephalic, with many family members having an OFC that fell within the normal range, leading the authors to conclude that NBCCS is more consistent with a generalised overgrowth disorder than a true macrocephaly syndrome. A study of 436 patients from the National NF Foundation Database found macrocephaly in 24%, with the remainder falling into the normal range.
OFC parameters in patients with Sotos syndrome revealed the greatest similarity to our patients with PHTS. An early paper found macrocephaly in all 33 patients with a clinical diagnosis studied, with OFC ranging from +2.0 to +6.9 SD with a mean of +3.5 SD.19 A larger analysis of patients with NSD1 mutations found macrocephaly in 146/192 (76%) of patients.20 The characteristic facial appearance of patients with Sotos syndrome was observed in 99% of mutation-positive patients; to date, similar studies have not been carried out to determine whether a particular facies exists in PHTS patients. Other common findings in Sotos syndrome include advanced bone age (76%), neonatal problems (70%), seizures (25%), and cardiac anomalies (21%); these are all findings not known to be associated with PHTS, but their precise frequencies have not been investigated in a large patient series.
Missense germline mutations in PTEN have, to date, been far less prevalent than truncating mutations; thus, it is notable that there is a trend demonstrating less dramatic macrocephaly in adults with missense mutations compared with those with other mutation types. Interestingly, a subset of these missense mutations affect one of the two ATP-binding motifs of PTEN, which results in inability of PTEN to bind ATP and inability to exit the nucleus.21, 22, 23 These types of mutants result in relative instability of PTEN, increased double-strand DNA breaks and increased reactive oxygen species.23 Our Pten constitutional knock-in mouse was created to model defective nuclear–cytoplasmic localisation, and one of its phenotypes is megencephaly. The life span for the homozygous mutant mice averages 8 weeks or less, with very few of these mice surviving past this point. Among the advantages of our model compared with tissue-specific or heterozygous models of Pten loss24, 25 is the fact that this is a germline mutation expressed under the endogenous promoter, leading to a functional disruption also observed in a subset of PHTS patients. This advantage allows exploration of the impacts of a missense mutation expressed from the earliest embryonic time points through adulthood, a situation where protein function is reduced but absolute levels are not as low as in murine models of heterozygous or tissue-specific deletion.
We also found it notable that 5 of our 181 mutation-positive patients have missense mutations in exon 9, an exon that is rarely affected by mutations.5, 26, 27 As the final exon in PTEN, missense mutations in this region would be predicted to only cause a slight alteration in protein structure and function. All three patients with exon 9 missense mutations and normal OFC had an invasive cancer that led their clinicians to consider a diagnosis of PHTS, but none had a family history that would have caused increased suspicion for PHTS before their cancers were diagnosed. It is plausible that exon 9 missense mutations may result in an attenuated PHTS phenotype.
Finding macrocephaly in 94% of our PHTS series confirms that this feature should be considered a major component phenotype in this population. It is possible that selection bias could lead to the identification of an abundance of PHTS patients with extreme macrocephaly, particularly as a presenting feature within the paediatric or young adult population who have not yet developed the full phenotypic features of PHTS. This was supported among the females in this study, where OFC SD values were significantly greater for patients ≤18 years (P=0.0047). However, a similar pattern was not identified in males (P=0.36).
Identifying nine patients with PHTS and normal head circumference should remind clinicians not to exclude this diagnosis in a patient with normal OFC. Among our seven normocephalic adult patients, all but two adult females would meet clinical diagnostic criteria for Cowden syndrome based on their other features. One of the two male children would be diagnosed with BRRS based on the finding of tan macules on the glans penis; the other would likely be considered Proteus-like because of the findings of hemihyperplasia and lipomas, leading their clinicians to consider PTEN molecular analysis despite the absence of macrocephaly. Notably all nine normocephalic patients were probands, implying that selecting patients for analysis based on macrocephaly did not confound these findings.
In any hereditary syndrome, early diagnosis is critical to provide optimal screening and medical recommendations. In particular, recognising extreme macrocephaly as a hallmark feature of PHTS should encourage clinicians to consider germline PTEN testing at an early point in the diagnostic work-up for patients with this characteristic, and should prompt them to investigate for other features of PHTS within the personal and family histories. Evaluation by both a geneticist and dermatologist is ideal to fully investigate patients for subtle syndromic manifestations and to rule out other syndromes associated with macrocephaly. Current recommendations by the National Comprehensive Cancer Network (http://www.nccn.org) advocate for increased surveillance for breast and thyroid cancers in patients with CS. Appropriately, these same recommendations are made for any patient with a known PTEN mutation regardless of whether they meet CS diagnostic criteria. Early diagnosis of PHTS can lead to the patient and their family members gaining the ability to take advantage of this high-risk screening, thereby reducing potential morbidity and mortality of this difficult-to-recognise syndrome. Because the clinical manifestation of PHTS is protean and broad, finding straightforward ‘most frequent' phenotypes associated with PTEN germline mutations is helpful. In this study, we provide evidence that macrocephaly, likely secondary to megencephaly, is an important component of PHTS and is more prevalent than previously appreciated, with extreme macrocephaly being a defining phenotype caused by germline PTEN mutations.
Acknowledgments
We are grateful to our patients and their families who have taken part in our research over the last many years. We wish to acknowledge all the genetic counselors, physicians, and other healthcare providers who have referred patients to our study. This study is funded, in part, by the National Cancer Institute, Bethesda, MD (R01CA118980 and P01CA124570 to CE) and the William Randolph Hearst Foundations, New York (to CE). AKT is a predoctoral fellow of the HHMI Program in Molecular Medicine at the Cleveland Clinic Lerner College of Medicine. CE is the Sondra J and Stephen R Hardis Chair of Cancer Genomic Medicine at the Cleveland Clinic, and an American Cancer Society Clinical Research Professor, generously funded, in part by the FM Kirby Foundation.
The authors declare no conflict of interest.
References
- Zbuk KM, Eng C. Cancer phenomics: RET and PTEN as illustrative models. Nat Rev Cancer. 2007;7:35–45. doi: 10.1038/nrc2037. [DOI] [PubMed] [Google Scholar]
- Starink TM, van der Veen JP, Arwert F, et al. The Cowden syndrome: a clinical and genetic study in 21 patients. Clin Genet. 1986;29:222–233. doi: 10.1111/j.1399-0004.1986.tb00816.x. [DOI] [PubMed] [Google Scholar]
- Butler MG, Dasouki MJ, Zhou XP, et al. Subset of individuals with autism spectrum disorders and extreme macrocephaly associated with germline PTEN tumour suppressor gene mutations. J Med Genet. 2005;42:318–321. doi: 10.1136/jmg.2004.024646. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zhou XP, Marsh DJ, Morrison CD, et al. Germline inactivation of PTEN and dysregulation of the phosphoinositol-3-kinase/Akt pathway cause human Lhermitte-Duclos disease in adults. Am J Hum Genet. 2003;73:1191–1198. doi: 10.1086/379382. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Marsh DJ, Coulon V, Lunetta KL, et al. Mutation spectrum and genotype-phenotype analyses in Cowden disease and Bannayan-Zonana syndrome, two hamartoma syndromes with germline PTEN mutation. Hum Mol Genet. 1998;7:507–515. doi: 10.1093/hmg/7.3.507. [DOI] [PubMed] [Google Scholar]
- Pilarski R, Eng C. Will the real Cowden syndrome please stand up (again)? Expanding mutational and clinical spectra of the PTEN hamartoma tumour syndrome. J Med Genet. 2004;41:323–326. doi: 10.1136/jmg.2004.018036. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gorlin RJ, Cohen MM, Jr, Condon LM, Burke BA. Bannayan-Riley-Ruvalcaba syndrome. Am J Med Genet. 1992;44:307–314. doi: 10.1002/ajmg.1320440309. [DOI] [PubMed] [Google Scholar]
- Fargnoli MC, Orlow SJ, Semel-Concepcion J, Bolognia JL. Clinicopathologic findings in the Bannayan-Riley-Ruvalcaba syndrome. Arch Dermatol. 1996;132:1214–1218. [PubMed] [Google Scholar]
- Lachlan KL, Lucassen AM, Bunyan D, Temple IK. Cowden syndrome and Bannayan Riley Ruvalcaba syndrome represent one condition with variable expression and age-related penetrance: results of a clinical study of PTEN mutation carriers. J Med Genet. 2007;44:579–585. doi: 10.1136/jmg.2007.049981. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tan WH, Baris HN, Burrows PE, et al. The spectrum of vascular anomalies in patients with PTEN mutations: implications for diagnosis and management. J Med Genet. 2007;44:594–602. doi: 10.1136/jmg.2007.048934. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Padberg GW, Schot JD, Vielvoye GJ, Bots GT, de Beer FC. Lhermitte-Duclos disease and Cowden disease: a single phakomatosis. Ann Neurol. 1991;29:517–523. doi: 10.1002/ana.410290511. [DOI] [PubMed] [Google Scholar]
- Nellhaus G. Head circumference from birth to eighteen years. Practical composite international and interracial graphs. Pediatrics. 1968;41:106–114. [PubMed] [Google Scholar]
- Hanssen AM, Werquin H, Suys E, Fryns JP. Cowden syndrome: report of a large family with macrocephaly and increased severity of signs in subsequent generations. Clin Genet. 1993;44:281–286. doi: 10.1111/j.1399-0004.1993.tb03901.x. [DOI] [PubMed] [Google Scholar]
- Eng C. Role of PTEN, a lipid phosphatase upstream effector of protein kinase B, in epithelial thyroid carcinogenesis. Ann N Y Acad Sci. 2002;968:213–221. doi: 10.1111/j.1749-6632.2002.tb04337.x. [DOI] [PubMed] [Google Scholar]
- Tan MH, Mester J, Peterson C, et al. A clinical scoring system for selection of patients for PTEN mutation testing is proposed on the basis of a prospective study of 3042 probands. Am J Hum Genet. 2010;88:42–56. doi: 10.1016/j.ajhg.2010.11.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Butler MG, Brunschwig A, Miller LK, Hagerman RJ. Standards for selected anthropometric measurements in males with the fragile X syndrome. Pediatrics. 1992;89:1059–1062. [PMC free article] [PubMed] [Google Scholar]
- Bale SJ, Amos CI, Parry DM, Bale AE. Relationship between head circumference and height in normal adults and in the nevoid basal cell carcinoma syndrome and neurofibromatosis type I. Am J Med Genet. 1991;40:206–210. doi: 10.1002/ajmg.1320400217. [DOI] [PubMed] [Google Scholar]
- Szudek J, Birch P, Friedman JM. Growth in North American white children with neurofibromatosis 1 (NF1) J Med Genet. 2000;37:933–938. doi: 10.1136/jmg.37.12.933. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Cole TR, Hughes HE. Sotos syndrome: a study of the diagnostic criteria and natural history. J Med Genet. 1994;31:20–32. doi: 10.1136/jmg.31.1.20. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tatton-Brown K, Douglas J, Coleman K, et al. Genotype-phenotype associations in Sotos syndrome: an analysis of 266 individuals with NSD1 aberrations. Am J Hum Genet. 2005;77:193–204. doi: 10.1086/432082. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lobo GP, Waite KA, Planchon SM, Romigh T, Houghton JA, Eng C. ATP modulates PTEN subcellular localization in multiple cancer cell lines. Hum Mol Genet. 2008;17:2877–2885. doi: 10.1093/hmg/ddn185. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lobo GP, Waite KA, Planchon SM, Romigh T, Nassif NT, Eng C. Germline and somatic cancer-associated mutations in the ATP-binding motifs of PTEN influence its subcellular localization and tumor suppressive function. Hum Mol Genet. 2009;18:2851–2862. doi: 10.1093/hmg/ddp220. [DOI] [PMC free article] [PubMed] [Google Scholar]
- He X, Ni Y, Wang Y, Romigh T, Eng C. Naturally-occurring germline and tumor-associated mutations within the ATP-binding motifs of PTEN lead to oxidative damage of DNA associated with decreased nuclear p53. Hum Mol Genet. 2010;20:80–89. doi: 10.1093/hmg/ddq434. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kwon CH, Zhu X, Zhang J, et al. Pten regulates neuronal soma size: a mouse model of Lhermitte-Duclos disease. Nat Genet. 2001;29:404–411. doi: 10.1038/ng781. [DOI] [PubMed] [Google Scholar]
- Podsypanina K, Ellenson LH, Nemes A, et al. Mutation of Pten/Mmac1 in mice causes neoplasia in multiple organ systems. Proc Natl Acad Sci USA. 1999;96:1563–1568. doi: 10.1073/pnas.96.4.1563. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Marsh DJ, Kum JB, Lunetta KL, et al. PTEN mutation spectrum and genotype-phenotype correlations in Bannayan-Riley-Ruvalcaba syndrome suggest a single entity with Cowden syndrome. Hum Mol Genet. 1999;8:1461–1472. doi: 10.1093/hmg/8.8.1461. [DOI] [PubMed] [Google Scholar]
- Varga EA, Pastore M, Prior T, Herman GE, McBride KL. The prevalence of PTEN mutations in a clinical pediatric cohort with autism spectrum disorders, developmental delay, and macrocephaly. Genet Med. 2009;11:111–117. doi: 10.1097/GIM.0b013e31818fd762. [DOI] [PubMed] [Google Scholar]