Abstract
The existence of complications of suppurative otitis media and efforts to control it go far back into history. Early diagnosis and management have been greatly modified by the extensive use of CT scan and higher antibiotics. Despite an overall decline in the incidence of complications of otitis media, severe complications still exist with high mortality. Suggested reasons are decrease in physician’s experience and changing of the virulence and susceptibility of causative organism. This series is a prospective study of 18 cases of otogenic brain abscess, carried out in Department of ENT and Head & Neck Surgery, SSG Hospital, Baroda from June 2005 to June 2008. We emphasize on confirmation of resolution of brain abscess by CT scan. This will eliminate recurrent/residual abscess and help in reduced overall mortality and morbidity.
Keywords: Otitis media, Brain abscess, CT scan, Mastoidectomy
Introduction
In the five-year period preceding the introduction of antibiotics, approximately one in every 40 deaths in a large general hospital was caused by an intracranial complication of otitis media [1]. The complications of chronic suppurative otitis media develop when middle ear infection spreads from its confines to an adjacent space or structures from which it is usually separated. Middle ear cleft and mastoid air cells are separated from the dura and the sigmoid sinus by very thin plates of bone, the dural plate and the sinus plate, respectively. Thus, the potential for serious intracranial complications is present in every patient with chronic suppurative otitis media. The symptomatology of these complications is slow in development and the clinical diagnosis is at times difficult. Although, the mortality rate has been reduced, the incidence of brain abscess has remained almost unchanged [2]. CT scan has formed the mainstay in the diagnosis of patients of brain abscess in recent years. It offers a highly accurate, relatively noninvasive and rapid means of establishing the diagnosis and following the course of disease.
Materials and Methods
All cases with history suggestive of CSOM and having additional symptoms of fever, earache, vertigo, headache, vomiting or altered sensorium giving suspicion of intracranial complications, were studied in detail. All such patients were investigated with CT scan. Patients with otogenic brain abscess were included in our study.
All patients were infused with injectable antibiotics in meningitic dose covering a broad spectrum which includes most gram positive, gram negative and anaerobes (triple antibiotics). The antibiotics were changed depending upon culture sensitivity report. Mannitol, dexamethasone and anticonvulsants were used when needed.
Most of the surgical intervention was carried out under pre-operative antibiotic cover of at least 48–72 h except in life threatening cases which needed urgent intervention. Usually transmastoid route was used to drain the abscess. Cortical mastoidectomy was done, pus and disease was cleared from the mastoid cavity. Status of the dural/sinus plate was observed. Usually it was found eroded, if it was found intact then it was drilled. Suspected site was opened and incised, drained or aspirated with brain cannula. It was kept open for self drainage till pus stopped. Burr hole or craniotomy as an approach was used in case where abscess was not approachable through transmastoid route and where patient was unable to tolerate prolonged general anesthesia. Advice of a neurosurgeon was sought when needed.
Repeat CT scan was done after 10–14 days of injectable antibiotics to confirm the resolution of abscess. If there was residual abscess of size more than 1.5 cm in maximum diameter then patient was taken for re-aspiration procedure. The same protocol was repeated after next drainage.
The middle ear disease clearing and canal wall down mastoidectomy was done once the repeat CT scan showed resolution of abscess or if the size of the abscess was insignificant. Suitable tympanoplasty and meatoplasty was done depending upon the middle ear disease and regular follow up was done.
Results and Observations
13 males and 5 females were included in our study. Most of them were young and had short duration of ear discharge. Bilateral disease was seen in 11 patients. Clinical diagnosis with the help of CT scan confirmed the offending ear in case of bilateral CSOM. Routine blood investigations and fundus examination was done pre-operatively. 11 patients were anemic (Hb ≤ 10 gm) out of which 6 also had lateral sinus thrombophlebitis.
Symptoms and signs suggestive of cerebellar abscess were present in 4 cases but 8 cases of cerebellar abscess were diagnosed on CT scan. One of them had multiple abscesses. Clinical features suggestive of Temporal lobe abscess were present in 5 cases but 7 cases were diagnosed on CT scan. One patient of extradural abscess was found intraoperatively and then confirmed by post-operative CT scan in which we had not suspected any intracranial complication pre-operatively. One case of perisinus abscess was reported only as sigmoid sinus thrombosis in CT scan. Another case of extradural abscess was reported in CT scan which was very small and managed conservatively.
12 patients had other intracranial complications in our study which could be detected by CT scan. 8 patients had meningitis and 6 patients had sigmoid sinus thrombosis. 2 patients had both meningitis and sigmoid sinus thrombosis. This emphasizes the need for CT scan in diagnosis of multiple complications.
18 brain abscess patients were included in the study. 2 of them, one temporal lobe and another small extradural abscess were managed conservatively as they were less than 1.5 cm in size. Remaining 16 otogenic brain abscess were drained.
All 8 cerebellar abscesses were drained by transmastoid route. One patient died immediate post operatively due to coning. Depending upon site, 2 out of 6 temporal lobe abscess were drained by transmastoid route and rest four through burr hole operation which were placed high up in temporal lobe. One case of extradural abscess and one case of perisinus abscess were drained by transmastoid route.
Repeat CT scan after clinical improvement and cessation of pus was done in 15 patients. One cerebellar abscess patient had died post operatively, one had very small extradural abscess and one with intra operative detection of extradural abscess was not submitted for 2nd CT scan.
In repeat CT scan, resolution of abscess was confirmed in 10 patients, but 5 patients (33%) showed residual abscess and required redrainage procedure. One of residual temporal lobe abscess pt died after redrainage through transmastoid route due to intracerebral hemorrhage. 2 patients of residual temporal lobe abscess required craniotomy for complete excision of abscess as there was repeated refilling of abscess after drainage by burr hole approach. Both residual cerebellar abscesses were redrained through transmastoid route. All 4 patients were subjected again for CT scan and resolution of abscess confirmed.
After final confirmation of resolution of abscess middle ear surgery was done and all of them underwent canal wall down mastoidectomy as all had extensive atticoantral type CSOM.
The minimum follow-up period was 6 months and maximum follow-up period was 3 years. On an average the follow-up period was 14 months. Minor complications like post aural wound gaping and discharging cavities were present in some patients which resolved in due course of time. No patient reported with recurrence of intracranial complication. Patients stayed in hospital for 20–45 days and intravenous antibiotics was given for a minimum period of 3–5 weeks Figs. 1, 2, 3, 4, 5 and 6.
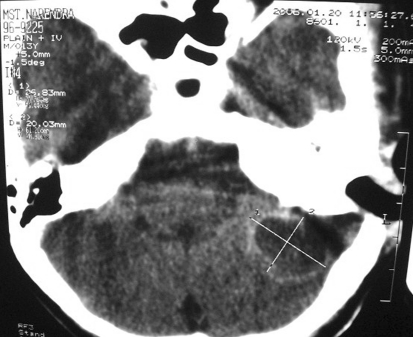
Fig. 1.
Large cerebellar abscess (pre-operative)
Fig. 2.
Residual abscess on 18th day of drainage
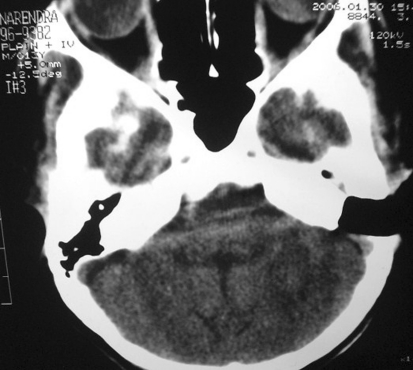
Fig. 3.
Fully resolved cerebellar abscess 10 days after redrainage
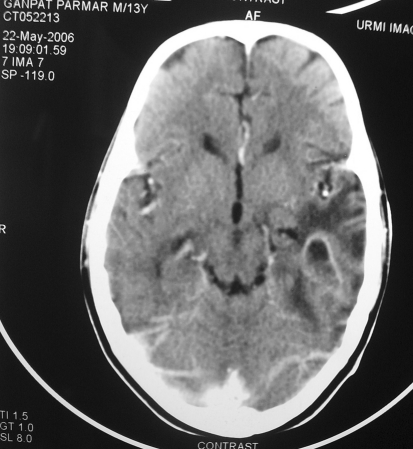
Fig. 4.
Patient of LT temporal lobe abscess
Fig. 5.
14 Days after transmastoid drainage showing reduction in size
Fig. 6.
26 Days after 1st drainage with fully resolved abscess shown in Fig. 5
Discussion
Role of CT Scan in Management of Otogenic Brain Abscesses
Role of CT scan is well documented for size, site and number of otogenic brain abscesses. It is essential for selection, treatment and follow-up of patients [3]. Small abscesses can be treated with high doses of intravenous antibiotics and observing improvement by serial CT studies [4, 5]. Large abscess should be drained. If the abscess is seen in connection to temporal bone, it should be drained by transmastoid route. Transmastoid route clears the offending mastoid cavity, at the same time it drains the brain abscess in the same route as it has spread. So recovery is achieved by reversal of disease process. When the abscess is not seen in continuity of temporal bone, drainage procedure should be designed by burr hole or craniotomy in such a way as to minimize trauma to normal brain tissue. Exact mapping can be done with 3D reconstruction of CT scan [6].
CT scan gives fare idea about size of brain abscess. So we know the amount of pus that should be drained. After adequate drainage of brain abscess, usually there is dramatic improvement in patient’s clinical condition which is augmented by intravenous antibiotics and steroids. This gives assurance of cure to patient and also ourselves which is often erroneous. There is always a possibility of refilling of abscess cavity. It may be due to persistence of inflammatory process due to high virulence of causative organisms or seepage of blood and CSF in dead space of abscess cavity getting secondarily infected. Repeated attempts to drain anticipated refilling of abscess is not recommended as there are potential complications for it. Instead repeat CT scan after clinical cure is advised to confirm resolution of brain abscess. In case there is residual abscess, exact size and amount of pus can be estimated. Also the site and approach for abscess drainage can be revised if needed.
In our study 33% of patients had residual brain abscess in 2nd CT scan. All of them had improved symptoms and signs after first drainage. These patients would represent back as recurrent abscess later when antibiotics will be stopped. Most of the patients with complicated CSOM are from poor socioeconomic background. Recurrence of brain abscess will be dangerous. They will lose faith in treating physician, may go for alternate therapy or may refuse any treatment. We should educate them regarding disease process and treatment plan and should discharge the patient from hospital after confirming cure from intracranial complication.
The procedure of Computed Tomography is non invasive, easily available at most centers, relatively cheap and can be repeated without any hazards to the patient. We recommend repeat CT scans till confirmation of abscess resolution in all cases of otogenic brain abscess.
The uses of CT scan in a case of otogenic brain abscess are
In coma patient or patient who is irritable, where history, signs and symptoms are unreliable it helps in accurate diagnosis.
In case of bilateral disease it helps in deciding which ear to operate first.
In case of brain abscess associated with other intracranial complications it helps in deciding which complication to be given priority [7].
By delineating the exact size and multiplicity of abscess it avoids unnecessary surgery in case of small abscess.
By knowing the stage of the abscess and the surrounding edema or hydrocephalus it helps in deciding the timing of surgical treatment.
By knowing the size and position of the abscess we come to know the best approach for the drainage of abscess.
Follow up CT scan helps in confirming the resolution of abscess. We can detect residual abscess and treat them adequately in time, thus reducing overall mortality and morbidity.
Conclusion
All the complications of CSOM including brain abscess are decreasing with increasing use of antibiotics. Otogenic brain abscess can be successfully managed by various modalities of treatment. Treatment plan should be tailored according to patient’s clinical condition and facilities available. It is recommended to confirm the resolution of brain abscess by follow up CT scan in all patients irrespective of treatment procedure used. This will eliminate recurrent/residual abscess and help in reduced overall mortality and morbidity.
Footnotes
CT scan has formed the mainstay in the diagnosis of patients of brain abscess in recent years. It offers a highly accurate, relatively noninvasive and rapid means of establishing the diagnosis and following the course of disease. We emphasize on confirmation of resolution of brain abscess by CT scan.
References
- 1.Wolfowitz B. Otogenic intracranial complications. Arch Otolaryngol. 1972;96:220–222. doi: 10.1001/archotol.1972.00770090342003. [DOI] [PubMed] [Google Scholar]
- 2.Kulah A. Otogenic intracranial abscesses. Acta Neurochir. 1990;107:140–146. doi: 10.1007/BF01405793. [DOI] [PubMed] [Google Scholar]
- 3.Rosenblum ML, et al. Decreased mortality from brain abscess since advent of computerized tomography. J Neurosurg. 1978;49:658–667. doi: 10.3171/jns.1978.49.5.0658. [DOI] [PubMed] [Google Scholar]
- 4.Rosenblum ML, Hoff JT, et al. Non operative treatment of brain abscess in selected high risk patients. J Neurosurg. 1980;52:217–225. doi: 10.3171/jns.1980.52.2.0217. [DOI] [PubMed] [Google Scholar]
- 5.Bidzinski J, Koszevski W. The value of different methods of treatment of brain abscess in the CT era. Acta Neurochir. 1990;105:117–120. doi: 10.1007/BF01669993. [DOI] [PubMed] [Google Scholar]
- 6.Samuel C Levin, Chris De Souza (2003) In: George E Sham Baugh (ed) Intracranial complications of otitis media, Surgery of the ear, pp 443–462
- 7.Kurien M. Otogenic intracranial abscess—changing trends in developing country. Arch Otolaryngol. 1998;124(12):1353–1356. doi: 10.1001/archotol.124.12.1353. [DOI] [PubMed] [Google Scholar]