Abstract
Background
Cetuximab has demonstrated significant clinical activity in metastatic colon cancer. However, cetuximab-containing neoadjuvant chemoradiation has not been shown to improve tumor response in locally advanced rectal cancer patients in recent phase I/II trials. We evaluated functional germline polymorphisms of genes involved in EGFR pathway, angiogenesis, ADCC, DNA repair, and drug metabolism, for their potential role as molecular predictors for clinical outcome in locally advanced rectal cancer patients treated with preoperative cetuximab-based chemoradiation.
Methods
130 patients (74 men and 56 women) with locally advanced rectal cancer (4 with stage II, 109 with stage III and 15 with stage IV, 2 unknown) who were enrolled in phase I/II clinical trials treated with cetuximab-based chemoradiation in European cancer centers were included. Genomic DNA was extracted from formalin-fixed paraffin-embedded tumor samples and genotyping was performed using PCR-RFLP assays. Fisher’s exact test was used to examine associations between polymorphisms and complete pathologic response (pCR) that was determined by a modified Dworak classification system (grade 0-III vs grade IV: complete response).
Results
Patients with the EGF 61 G/G genotype had pCR of 45% (5/11), compared with 21% (11/53) in patients heterozygous, and 2% (1/54) in patients homozygous for the A/A allele (P <0.001). In addition, this association between EGF 61 G allele and pCR remained significant (p=0.019) in the 59 patients with wild type KRAS.
Conclusions
This study suggests EGF A+61G polymorphism to be a predictive marker for pCR, independent of KRAS mutation status, to cetuximab-based neoadjuvant chemoradiation of patients with locally advanced rectal cancer.
Keywords: colorectal cancer, EGF 61, complete pathologic response (pCR), KRAS, cetuximab
Introduction
It is estimated that 142,570 Americans will be diagnosed with colorectal cancer (CRC) in 2010, of which 39,670 are rectal cancers. The incidence rate of rectal cancer has decreased from 18.42 to 12.77 per 100,000 over the past 20 years, largely attributed to the improved screening programs. From 1999 to 2006, 77% of diagnosed rectal cancer patients had localized or regional advanced disease and these patients had significant 5 year survival advantage (88.6% and 67.1%) compared to 12.3% for distantly metastasized patients (SEER’s data). Similar trend has been observed in western Europe. The widely used surgical technique, total mesorectal excision (TME) alone, has decreased the local recurrence rate from 39.4% to 9.8% and improved the observed 5-year survival rate from 50% to 71% (1). In addition, preoperative therapy with concurrent radiation and infusion of 5FU has shown to further decrease the local recurrence rate in stage II and III rectal cancer (2–4). Therefore neoadjuvant chemoradiation is now a standard of care for locally advanced rectal cancer patients. Interestingly, neither pelvic radiation nor chemotherapy before surgery has demonstrated significant survival benefits. Ongoing clinical trials are examining newer agents such as capecitabine, oxaliplatin, irinotecan, cetuximab or bevacizumab, to further optimize local control, reduce distant metastases and ultimately improve survival. Epidermal growth factor receptor (EGFR) signals through two major pathways, the RAS-MAPK and the PI3K-AKT pathway. Hyperactivity of the EGFR pathways is associated with more aggressive phenotype and poor prognosis of cancers (5), and can render cancer cells resistant to radiation(6). Cetuximab is an EGFR monoclonal antibody and has demonstrated significant clinical activity in metastatic colon cancer (7, 8). In addition, concomitant high-dose radiotherapy plus cetuximab has been shown to improve locoregional control and reduce mortality in squamous carcinoma of the head and neck (9). Recent phase I/II clinical trials have evaluated EGFR inhibitors as a radiosensitizer in CRC and demonstrated that cetuximab can be safely given without unexpected toxicity (10, 11). However, cetuximab-containing neoadjuvant chemoradiation has not been shown to improve tumor response and complete pathologic response (pCR) rates in locally advanced rectal cancer patients (12–14). In order to identify the subgroup of patients who may benefit from the cetuximab protocol, we designed a retrospective study within a cohort of 4 prospectively conducted phase I/II clinical trials. We evaluated functional germline polymorphisms of genes involved in the EGFR signaling pathway (EGF, EGFR, COX-2, KRAS, CyclinD1), angiogenesis (VEGF, IL-8), ADCC (FCGR2A/3A), DNA repair (XRCC3, Rad51), and drug metabolism (TS, MTHFR), for their potential role as molecular predictors for clinical outcome in locally advanced rectal cancer patients treated with preoperative cetuximab-based chemoradiation followed by surgery.
Materials and Methods
Patients
130 patients (74 men and 56 women, median age 61) with locally advanced rectal cancer (4 with stage II, 109 with stage III and 15 with stage IV, 2 unknown) who were enrolled in phase I/II clinical trials treated with cetuximab-based chemoradiation in 4 European cancer centers (Brussels /Leuven, Belgium; Ljubljana, Slovenia; Halle/Erlangen /Göttingen /Regensburg, Germany and Cologne, Germany) were included (table 1) (15, 16). Informed consent was obtained from each patient and the studies were approved by the Institutional Review Boards of the participating centers. Clinical staging was based on results from endoscopy, endoscopic ultrasound, and computed tomography/magnetic resonance imaging (MRI) of the chest and abdomen. Patients underwent radical resection within 4–8 weeks after completion of chemoradiation by either a low anterior resection or an abdomino-perineal rectal amputation with total mesorectal excision.
Table 1.
Patient characteristics and treatments
| N =130 | % | |
|---|---|---|
| Age, years | ||
| Median | 61 | |
| Range | 33–83 | |
|
| ||
| Sex | ||
| Male | 74 | 57 |
| Female | 56 | 43 |
|
| ||
| Stage | ||
| II | 4 | 3 |
| III | 109 | 85 |
| IV | 15 | 12 |
|
| ||
| Type of neoadjuvant therapy | ||
| 5-FU/Cetuximab/Radiation (Cologne, Germany) | 16 | 12 |
| Capecitabine/Cetuximab/Radiation (Belgium/Slovenia) | 72 | 56 |
| Capecitabine/Oxaliplatin/Cetuximab/Radiation (Halle/Erlangen/Göttingen/Regensburg, Germany) | 42 | 32 |
Treatment protocols
Brussels/Leuven, Belgium
Patients (n=41) received capecitabine (4 patients at first dose level of 650 mg/m2 twice a day; 37 patients at second dose level of 825 mg/m2 twice a day) and intravenous cetuximab (400 mg/m2 as initial dose 1 week before CRT followed by 250 mg/m2/week for 5 weeks) and 45 Gy of radiation (25 × 1.8 Gy).
Ljubljana, Slovenia
Patients (n=31) received capecitabine 1250 mg/m2 twice daily for 2 weeks followed by intravenous cetuximab 400 mg/m2 at week 3, then weekly intravenous 250 mg/m2 cetuximab plus CRT including capecitabine 825 mg/m2 twice daily (including weekends during radiotherapy) with radiotherapy of 45 Gy (25 × 1.8 Gy), 5 days a week for 5 weeks.
Halle/Erlangen/Göttingen/Regensburg, Germany
Patients (n=42) received cetuximab given as an initial dose of 400 mg/m2 7 days before the start of RT, and then at 250 mg/m2 once weekly during RT (50.4 Gy, 28 × 1.8 Gy). Capecitabine and oxaliplatin were administered according to an established schedule of oxaliplatin (50 mg/m2 on Days 1, 8, 22, and 29) and capecitabine (Days 1–14 and 22–35) at three dose levels: 1,000, 1,300, and 1,650 mg/m2/d.
Cologne, Germany
Patients (n=16) where treated with 45 Gy of radiation (25 × 1.8 Gy) and cetuximab (400 mg/m2 as initial dose 1 week before CRT followed by 250 mg/m2/wk for 5 weeks) in combination with 5-FU.
Tissue samples and pathologic response evaluation
Tumor biopsies from the study patients were obtained at the time of diagnosis (pre-therapeutic biopsy), and at the time of surgery (post-therapeutic biopsy). Pre-treatment biopsies from 109 (84%) patients and post-treatment biopsies from 117 (90%) patients were collected and analyzed in this study. For diagnosis, three sections representative of the beginning, middle and end of the tissue were collected. The resected specimens were fixed in 10% formalin, embedded in paraffin and cut into 5μm thick slices. The sections were then stained with hematoxylin and eosin stain (H&E) and all samples were reviewed by a staff pathologist in each study center. To determine pathologic response, Dworak’s regression grading system (grade 0: no regression; grade 1: minimal regression; grade 2: moderate regression; grade 3: good regression; and grade 4: total regression) was used in all of the participating centers (17). Grade 4 was defined as complete pathological response (pCR).
DNA extraction
Formalin-fixed paraffin-embedded (FFPE) tissues from the patients were dissected as described previously. Ten micrometer thick slides were obtained from the identified areas with the highest tumor concentration and were mounted on uncoated glass slides. Sections were deparafinized in xylene for 10 minutes, hydrated with 100%, 95% and 70% ethanol and then washed in H2O for 30 seconds. The sections were then stained with nuclear fast red (NFR, American Master Tech Scientific, Inc., Lodi, CA) for 20 seconds and rinsed in H2O for 30 seconds, dehydrated with 70% ethanol, 95% ethanol and 100% ethanol for 30 seconds each, followed by xylene for 10 minutes and then completely air-dried. Laser capture microdissection (P.A.L.M. Microlaser Technologies AG, Munich, Germany) was used in all tumor samples. Genomic DNA was then extracted from the dissected tumor samples using the QIAamp kit (Qiagen, CA) according to manufacture’s instructions.
KRAS analysis
KRAS analysis of 7 KRAS mutations (codon 12 and codon 13) was performed according to a proprietary procedure defined by Response Genetics Inc. (Los Angeles, CA; United States patent number 6, 248, 535).
PCR- RFLP
Genotyping was performed using PCR-RFLP assays. Briefly, forward primers and reverse primers (table 2) were used for PCR amplification, PCR products were digested by restriction enzymes (New England Biolab, Ipswich, MA, USA), and alleles were separated on 4% NuSieve ethidium bromide-stained agarose gel.
Table 2.
Primers and Enzymes for PCR-RFLP
| Gene | Forward-Primer (5′L-3′L) | Reverse-Primer (5′L-3′L) | Enzyme | Annealing |
|---|---|---|---|---|
| FCGR2A H131R | GGAAAATCCCAGAAATTCTCGC | CAACAGCCTGACTACCTATTACGCGGG | BstU I | 55° |
| FCGR3A V158F | CTGAAGACACATTTTTACTCCCAAA/C | TCCAAAAGCCACACTCAAAGAC | n.a. | 64° |
| VEGF C+936T | AAGGAAGAGGAGACTCTGCGCAGAGC | TAAATGTATGTATGTGGGTGGGTGTGTCTACAGG | Nla III | 60° |
| EGF A+61G | CATTTGCAAACAGAGGCTCA | TGTGACAGAGCAAGGCAAAG | Alu I | 60° |
| EGFR (CA)n Repeat | ACCCCAGGGCTCTATGGGAA | TGAGGGCACAAGAAGCCCCT | n.a. | 55° |
| EGFR G+497A | TGCTGTGACCCACTCTGTCT | CCAGAAGGTTGCACTTGTCC | Bst-N I | 59° |
| MTHFR C677T | GCACTTGAAGGAGAAGGTGTCT | TGTGTCAGCCTCGAAAGAAAAGCT | Hin fI | 68° |
| IL8 T-251A | TTGTTCTAACACCTGCCACTCT | GGCAAACCTGAGTCTCACA | Mfe I | 60° |
| MTHFR A-1298C | GGAGGAGCTGCTGAAGATGTG | CCCGAGAGGTAAAGAACAAAGACTT | Mbo II | 68° |
| COX-2 G-765C | ATTCTGGCCATCGCCGCTTC | CTCCTTGTTTCTTGGAAA GAGACG | Aci I | 55° |
| Cyclin D1A+870G | GTGAAGTTCATTTCCAATCCGC | GGGACATCACCCTCACTTAC | ScrF I | 61° |
| COX-2 G-765C | ATTCTGGCCATCGCCGCTTC | CTCCTTGTTTCTTGGAAA GAGACG | Aci I | 55° |
| XRCC3Thr241Met | GCCTGGTGGTCATCGACTC | ACAGGGCTCTGGAAGGCACTGCTCAGCTCACGCACC | Nco I | 60° |
| TS 3′UTR 6bp+/− | CAAATCTGAGGGAGCTGAGT | CAGATAAGTGGCAGTACAGA | Dra I | 58° |
| TS 5′UTR 2R/3R | GAAAAGGCGCGCGGAAGG | GCTCCGAGCCGGCCACA | n.a | 62° |
| RAD G51C | TGGGAACTGCAACTCATCTGG | GCGCTCCTCTCTCCAGCAG | Mva I | 60° |
| KRAS let-7 lcs6 | TGACTGAATATAAACTTGTGGTAGTTG | TCGTCCACAAAATGATTCTGAA | Tfi I | 60° |
Statistical analysis
Tumor response to neoadjuvant chemoradiotherapy evaluated by Dworak criteria was the primary endpoint. Patients with grade 4 Dworak response were classified as having pCR. Patients having grade 0–3 Dworak response were categorized as not having pCR. Fisher’s exact test was used to examine associations between polymorphisms and pCR or KRAS mutation status and pCR. The exact conditional test was used to evaluate the associations between polymorphisms and ordinal Dworak response. The independent effects of polymorphisms on pCR were examined using the Logistic regression model when stratifying the study center and patient baseline characteristics.
While the genetic model of inheritance for the polymorphisms had not established, a co-dominant model was considered first. A dominant model was used whenever the patients carrying the genotype of variant/variant were too few (<5%).
The false discovery rate (FDR) of multiple testing was controlled using the Benjamini and Hochberg method (18). The FDR adjusted p values < 15% were considered as significant.
An internal validation method, leave-one-out cross validation was used to evaluate the process of polymorphism selection to predict pCR.
All statistical tests were 2-sided and performed using the SAS statistical package version 9.2 (SAS Institute Inc. Cary, North Carolina, USA).
Results
Pathologic response
Data from 125 out of the 130 patients were available to evaluate pathologic response with cetuximab based chemoradiation after surgery. Among them, 21 (17%) patients had grade 0/1, 55 (44%) patients had grade 2, 30 (24%) patients had grade 3, and 19 (15%) patients had grade 4 response.
EGF 61 polymorphism and complete pathologic response
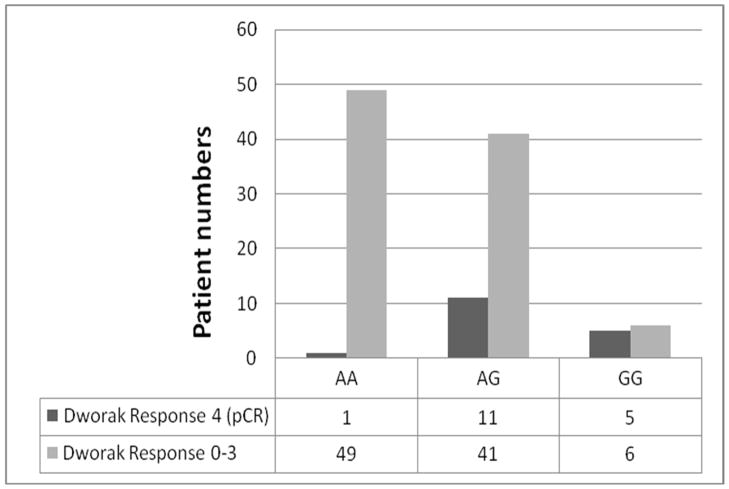
Genotyping for EGF 61 was successful in 118 (91%) of 130 cases. In 12 patients (9%) genotyping was not successful because of limited quantity and quality of extracted genomic DNA or biopsy samples. Forty-six percent (54/118) of patients were homozygous for A/A allele, 45% (53/118) were heterozygous A/G, and 9% (11/118) were homozygous for the G/G allele. Patients with the EGF G/G genotype had a pCR of 45% (5/11), compared with 21% (11/53) in patients heterozygous, and 2% (1/54) in patients homozygous for the A/A allele, respectively (Figure 1). There was statistically significant association between EGF A61G polymorphism and pCR after treatment of these patients (P <0.001, Fisher’s exact test, Table 3). EGF A61G polymorphism remained significantly associated with pCR in the multivariable logistic regression model stratified by the study center and age (Table 4).
Figure 1.
EGF 61 polymorphism status and pCR.
Table 3.
Genomic Polymorphisms and Tumor Response in Patients with Rectal Cancer Treated with Neoadjuvant Chemoradiation
| Polymorphism | N‡ | pCR
|
Dworak Response
|
||||
|---|---|---|---|---|---|---|---|
| Yes | No | 1 | 2 | 3 | 4 | ||
| IL-8 T-251A | |||||||
| TT | 38 | 8 (22%) | 28 | 7 | 12 | 9 | 8 |
| TA | 62 | 7 (12%) | 53 | 9 | 29 | 15 | 7 |
| AA | 26 | 4 (16%) | 21 | 4 | 12 | 5 | 4 |
| P value* | 0.37 (0.74) | 0.54 (0.70) | |||||
| MTHFR C677T | |||||||
| CC | 59 | 12 (20%) | 47 | 9 | 23 | 15 | 12 |
| CT | 56 | 4 (8%) | 48 | 9 | 27 | 12 | 4 |
| TT | 11 | 3 (30%) | 7 | 2 | 3 | 2 | 3 |
| P value* | 0.070 (0.37) | 0.50 (0.70) | |||||
| MTHFR A-1298C | |||||||
| AA | 54 | 8 (16%) | 43 | 7 | 26 | 10 | 8 |
| CA | 62 | 8 (13%) | 52 | 12 | 25 | 15 | 8 |
| CC | 8 | 3 (38%) | 5 | 0 | 2 | 3 | 3 |
| P value* | 0.18 (0.72) | 0.30 (0.70) | |||||
| FCGR2A H131R | |||||||
| HH | 35 | 4 (12%) | 30 | 6 | 13 | 11 | 4 |
| HR | 69 | 11 (17%) | 55 | 11 | 31 | 13 | 11 |
| RR | 19 | 4 (22%) | 14 | 2 | 9 | 3 | 4 |
| P value* | 0.61 (0.85) | 0.77 (0.82) | |||||
| FCGR3A V158F | |||||||
| VV | 49 | 6 (12%) | 43 | 7 | 23 | 13 | 6 |
| VF | 37 | 3 (9%) | 32 | 8 | 15 | 9 | 3 |
| FF | 15 | 3 (20%) | 12 | 3 | 8 | 1 | 3 |
| P value* | 0.49 (0.85) | 0.55 (0.70) | |||||
| CYCLIND1 A870G | |||||||
| AA | 32 | 5 (17%) | 25 | 6 | 15 | 4 | 5 |
| AG | 58 | 7 (12%) | 49 | 9 | 23 | 17 | 7 |
| GG | 34 | 6 (18%) | 27 | 5 | 15 | 7 | 6 |
| P value* | 0.76 (0.85) | 0.55 (0.70) | |||||
| XRCC3 Thr241Met | |||||||
| TT | 51 | 6 (12%) | 42 | 11 | 21 | 10 | 6 |
| CT | 55 | 9 (17%) | 45 | 7 | 26 | 12 | 9 |
| CC | 12 | 2 (18%) | 9 | 0 | 4 | 5 | 2 |
| P value* | 0.74 (0.85) | 0.059 (0.24) | |||||
| VEGF C936T | |||||||
| CC | 93 | 13 (15%) | 75 | 16 | 40 | 19 | 13 |
| CT† | 30 | 6 (19%) | 26 | 4 | 13 | 9 | 6 |
| TT† | 2 | ||||||
| P value* | 0.58 (0.85) | 0.33 (0.70) | |||||
| EGFR G497A | |||||||
| GG | 71 | 10 (15%) | 57 | 13 | 24 | 20 | 10 |
| AG | 42 | 8 (19%) | 34 | 5 | 23 | 6 | 8 |
| AA | 12 | 1 (9%) | 10 | 2 | 6 | 2 | 1 |
| P value* | 0.75 (0.85) | 0.61 (0.70) | |||||
| EGFR (CA)n repeat | |||||||
| Both <20 | 58 | 10 (18%) | 47 | 9 | 23 | 15 | 10 |
| Any ≥20 | 47 | 9 (21%) | 34 | 5 | 20 | 9 | 9 |
| P value* | 0.80 (0.85) | 0.83 (0.83) | |||||
| EGF A61G | |||||||
| AA | 54 | 1 (2%) | 49 | 14 | 24 | 11 | 1 |
| AG | 53 | 11 (21%) | 41 | 4 | 25 | 12 | 11 |
| GG | 11 | 5 (45%) | 6 | 2 | 1 | 3 | 5 |
| P value* | <0.001 (0.002) | <0.001 (<0.001) | |||||
| TS 3′ UTR | |||||||
| +/+ | 55 | 8 (15%) | 44 | 7 | 21 | 16 | 8 |
| +/− | 56 | 9 (16%) | 46 | 10 | 25 | 11 | 9 |
| −/− | 14 | 2 (15%) | 11 | 3 | 7 | 1 | 2 |
| P value* | 1.00 (1.00) | 0.24 (0.70) | |||||
| TS 5′ UTR | |||||||
| 2R/2R | 15 | 5 (36%) | 9 | 3 | 1 | 5 | 5 |
| 2R/3R | 56 | 9 (16%) | 46 | 11 | 23 | 12 | 9 |
| 3R/3R | 24 | 0 (0%) | 23 | 4 | 14 | 5 | 0 |
| P value* | 0.006 (0.045) | 0.015 (0.12) | |||||
| COX-2 G-765C | |||||||
| GG | 84 | 15 (19%) | 66 | 12 | 37 | 17 | 15 |
| GC† | 38 | 4 (10%) | 35 | 8 | 16 | 11 | 4 |
| CC† | 3 | ||||||
| P value* | 0.30 (0.72) | 0.47 (0.70) | |||||
| RAD G51C | |||||||
| GG | 102 | 14 (14%) | 84 | 16 | 43 | 25 | 14 |
| GC | 21 | 5 (25%) | 15 | 3 | 9 | 3 | 5 |
| P value* | 0.31 (0.72) | 0.61 (0.70) | |||||
| KRAS let-7 lcs6 poly | |||||||
| TT | 109 | 15 (14%) | 92 | 20 | 48 | 24 | 15 |
| TG† | 14 | 4 (29%) | 10 | 0 | 5 | 5 | 4 |
| GG† | 3 | ||||||
| P value* | 0.23 (0.72) | 0.024 (0.13) | |||||
Nominal P values werebased on Fisher’s exact test for pCR and exact conditional test for Dworak response. FDR-adjusted P values were shown in parentheses.
Combined in the analysis
Number of patients by each genotype. Some of the patients had response not evaluable.
Table 4.
Logistic regression model of EGF A61G and TS 5′ UTR polymorphisms and pCR
| Polymorphism | Univariate analysis
|
Multivariate analysis† |
|---|---|---|
| OR (95%CI) | OR (95%CI) | |
| EGF A61G | ||
| AA | 1 (reference) | 1 (reference) |
| AG or GG | 16.68 (95%CI: 2.13 – 130.82) | 13.08 (95%CI: 1.51 – 113.54) |
| P value* | 0.007 | 0.020 |
| TS 5′ UTR | ||
| 2R/2R | 1 (reference) | 1 (reference) |
| 2R/3R or 3R/3R | 0.24 (95%CI: 0.06 – 0.86) | 0.30 (95%CI: 0.06 – 1.52) |
| P value* | 0.028 | 0.14 |
Based on Wald test
Stratified by study center and age (<60 vs 60+ years old)
TS 5′UTR polymorphism and complete pathologic response
Genotyping for TS 5′UTR was successful in 95 (73%) of 130 cases. In 35 patients (27%) genotyping was not successful because of limited quantity and quality of extracted genomic DNA or biopsy samples. Sixteen percent (15/95) of patients were homozygous for 2R/2R allele, 59% (56/95) were heterozygous 2R/3R, and 25% (24/95) were homozygous for the 3R/3R allele. Patients with the TS 5′UTR 2R/2R genotype had a pCR of 33% (5/15), compared with 16% (9/56) in patients heterozygous, and 0% (0/24) in patients homozygous for the 3R/3R genotype, respectively. There was statistically significant association between TS 5′UTR 2R allele and pCR after treatment of these patients (P = 0.006, Fisher’s exact test, Table 3). The association was no longer statistically significant in the multivariate logistic regression model (Table 4).
KRAS mutation status and pCR
KRAS mutation status was available from pre-therapeutic tumor biopsies of 101 patients, 42% of which (42/101) had KRAS mutation, 58% (59/101) had wild type KRAS. The mutation status (wild type vs. mutant) was not significantly correlated with pCR (p=0.214, Fischer Exact Test). KRAS mutant patients showed 15% (5/34) pCR to cetuximab based neoadjuvant CRT compared to KRAS wild type patients with 10% (5/52) pCR.
Gene polymorphisms in patients with wild-type KRAS
When gene polymorphism and tumor response were analyzed in the 59 patients with wild type KRAS, EGF 61 remains to be significantly associated with the pCR, with the EGF G/G genotype had a pCR of 40% (2/5), compared with 12% (3/25) in patients heterozygous, and 0% (0/24) in patients homozygous for the A/A allele (P = 0.019, Fisher’s exact test). On the other hand, TS 5′UTR polymorphism was no longer significantly associated with pCR (p=0.67, data not shown).
Analysis of other tested germline polymorphisms
We did not observe statistically significant associations between other tested gene polymorphisms and pCR (Table 3).
EGF A61G SNP was the only polymorphism predicted pCR, which was validated by the leave-one-out cross validation method (118 of 121 leave-one-out datasets) through all the steps of analyses including the univariate, multivariate analysis, and subgroup analysis among Kras wildtype patients.
Discussion
With the development of the total mesorectal excision technique and the current neoadjuvant chemo-radiation regimen, the local recurrence rate in locally advanced rectal cancer patients has decreased significantly from 20–30% to less than 10%, and is no longer the reason for poor survival in these patients (19). Interestingly this drop in local recurrence has not been correlated with better survival, and the high rate of distant metastasis appeared to be the problem for this failure (20). Therefore, targeted therapies have been added to the standard care of neoadjuvant chemoradiation for better local control and survival. Complete pathologic response (pCR) has been shown to be strongly associated with the effectiveness of treatments and has been used to predict survival following neoadjuvant therapy (21). However, recent phase I/II clinical trials with cetuximab-based chemoradiation therapy have failed to demonstrate improved pCR or survival in locally advanced rectal cancer patients. Question has been raised whether a subset of patients might benefit from this treatment. Our study suggests EGF A+61G polymorphism is significantly associated with pCR to cetuximab-based neoadjuvant chemoradiation in locally advanced rectal cancer patients, independent of KRAS mutation status. This is the first study suggesting this polymorphism might be a predictive marker for response to cetuximab-based therapy.
The EGF/EGFR pathway plays important roles in the pathogenesis and progression of human cancers (22) and both EGF and EGFR are commonly over-expressed in CRC. Epidermal growth factor (EGF) is encoded by a single gene on chromosome 4q25–q27. In 2002, Shahbazi et al. identified a G to A polymorphism at position 61 in the 5′ untranslated region of EGF that is significantly correlated with production of EGF (23). Individuals with the G/G or A/G genotypes had higher EGF production in vitro than individuals with the A/A genotype, and homozygosity of the G allele was shown to be associated with the risk of developing malignant melanoma and several other malignancies, including gastric cancer (24), glioma (25), hepatocellular carcinoma in cirrhotic patients(26), colorectal cancer, and recurrence of liver metastasis from colorectal cancer (27), although subsequent studies showed conflicting results (28–31). On the other hand, several recent studies have shown that the G/G genotype is associated with improved OS and progression-free survival or less tumor recurrence in patients with metastatic colorectal and esophageal cancers (32–34). Graziano et al investigated 110 metastatic CRC patients who were treated with cetuximab-irinotecan salvage therapy and found significant association between EGF 61 G/G genotype and a favorable OS in these patients. In another group of 130 mCRC patients who were treated with single agent cetuximab, EGF +61 G/G genotype was associated with better progression free survival (35). These apparently paradoxical results are possibly due to the different effect of increased EGF activity in different stages of cancer development. Overproduction of the EGF can impose an increased risk to develop cancer on normal cells, however, it might also increase cancer cells’ susceptibility to treatment, especially targeted therapy such as cetuximab. Indeed, in our study, EGF61 G allele is strongly associated with pCR in this group of locally advanced rectal patients treated with cetuximab-based neoadjuvant chemoradiation. Our data is in line with the result of Khambata-Ford, et al that mCRC patients whose tumors with increased expression of EGF ligands epiregulin and amphiregulin are more likely to have disease control and progression free survival when treated with cetuximab (36). Whether this association of EGF 61 polymorphism and pCR is due to enhanced inhibition of the EGFR pathway or increased sensitivity to radiation therapy requires further investigation. KRAS mutation status has been shown to predict response to cetuximab-based therapy in mCRC patients (37) and mCRC patients with mutant-type KRAS are more likely to have a worse response, PFS, and OS when treated with cetuximab (38). On the other hand, studies of cetuximab- based neoadjuvant therapy in rectal cancer patients are few and have generated inconclusive results regarding the significance of KRAS mutation status and response to cetuximab therapy (39), likely due to small patient numbers of these studies. Our data showed that the KRAS mutation status is not statically significantly associated with the pCR. However, only 10 of the 101 patients with known KRAS mutation status had pCR to cetuximab based neoadjuvant chemoradiation therapy. This small sample size limited our ability to interpret the result and larger trials are required to make the conclusion. However, our data showed that the EGF61 A>G polymorphism has significant association with pCR to the cetuximab based therapy in patients with both KRAS wild type and mutant tumors.
Thymidylate synthase catalyze the reaction from dUMP to dTMP, the only de novo source of dTMP in cells, and is the therapeutic target for 5FU and its derivatives. High TS expression levels and activity have been associated with poor prognosis and response rates in colorectal cancer patients (40). The variable number of tandem repeats (VNTR) of a 28-bp sequence (2R and 3R) located within the 5′ untranslated region (5′UTR) is one of the three polymorphisms identified to affect the expression of TS gene, located at 18p11.32. Studies have shown that the wild-type 3R enhance TS protein translation and elevates enzyme activity (41). However, data on the prognostic and predictive value of the VNTR has been mixed and conflicting. TS 5′ UTR 3R genotype was linked to lower response rate (42), better survival outcome (43), better response to chemotherapy, or no significant difference in outcome (44) in advanced CRC patients treated with 5FU. On the other hand, heterozygous 2R/3R genotype was associated with worse overall survival in one study (45) and was a favorable marker in others (46). Possible explanations for these inconsistent results include the multiple polymorphisms existing in the TS gene including the G/C SNP in the 3G allele (47), the 6bp deletion within the 3′UTR (48), and variations of TS gene copy number due to loss of heterozygosis (LOH) (49) or gene amplification. In our study, TS 5′UTR 3R/3R genotype was significantly associated with the worst response rate (0% pCR) to cetuximab based neoadjuvant chemoradiation therapy, compared to 33% pCR in patients with 2R/2R genotype, and 16% pCR in patients with heterozygous 2R/3R genotype (P = 0.006). Interestingly, this association is not significant in patients with wild type KRAS. This result might be confounded by the treatment of all patients with 5FU or capecitabine.
In conclusion, our study suggests intratumoral EGF61 A/G polymorphism to be a potential predictive marker for pCR to cetuximab-based neoadjuvant chemoradiation in patients with locally advanced rectal cancer. The retrospective nature and relatively small sample size limited the significance of this study. Further, the patients all received cetuximab based therapy and there is no untreated control group. Therefore the results of this study should be interpreted carefully and validated in larger prospective trials.
Statement of translational relevance.
Our study suggests EGF A+61G polymorphism is significantly associated with pCR to cetuximab-based neoadjuvant chemoradiation in locally advanced rectal cancer patients, independent of KRAS mutation status. This is the first study suggesting this polymorphism might be predictive marker for response to cetuximab-based therapy.
Acknowledgments
Financial support: This study was performed in the Sharon A. Carpenter Laboratory at USC/Norris Comprehensive Cancer Center. The study was previously presented at American Society of Clinical Oncology 2010 (Abstract ID 3641). This work was funded by the NIH grant 5 P30CA14089-27I and the Dhont Family Foundation. This work was also funded by the Deutsche Forschungsgemeinschfat (DFG), Grant No. VA 506/1-1; 535112 and Cologne Fortune.
References
- 1.Kockerling F, Reymond MA, Altendorf-Hofmann A, Dworak O, Hohenberger W. Influence of surgery on metachronous distant metastases and survival in rectal cancer. J Clin Oncol. 1998;16:324–9. doi: 10.1200/JCO.1998.16.1.324. [DOI] [PubMed] [Google Scholar]
- 2.Kapiteijn E, Marijnen CA, Nagtegaal ID, et al. Preoperative radiotherapy combined with total mesorectal excision for resectable rectal cancer. N Engl J Med. 2001;345:638–46. doi: 10.1056/NEJMoa010580. [DOI] [PubMed] [Google Scholar]
- 3.Sauer R, Becker H, Hohenberger W, et al. Preoperative versus postoperative chemoradiotherapy for rectal cancer. N Engl J Med. 2004;351:1731–40. doi: 10.1056/NEJMoa040694. [DOI] [PubMed] [Google Scholar]
- 4.Bosset JF, Collette L, Calais G, et al. Chemotherapy with preoperative radiotherapy in rectal cancer. N Engl J Med. 2006;355:1114–23. doi: 10.1056/NEJMoa060829. [DOI] [PubMed] [Google Scholar]
- 5.Kopp R, Rothbauer E, Mueller E, Schildberg FW, Jauch KW, Pfeiffer A. Reduced survival of rectal cancer patients with increased tumor epidermal growth factor receptor levels. Dis Colon Rectum. 2003;46:1391–9. doi: 10.1007/s10350-004-6756-1. [DOI] [PubMed] [Google Scholar]
- 6.Wollman R, Yahalom J, Maxy R, Pinto J, Fuks Z. Effect of epidermal growth factor on the growth and radiation sensitivity of human breast cancer cells in vitro. Int J Radiat Oncol Biol Phys. 1994;30:91–8. doi: 10.1016/0360-3016(94)90523-1. [DOI] [PubMed] [Google Scholar]
- 7.Van Cutsem E, Kohne CH, Hitre E, et al. Cetuximab and chemotherapy as initial treatment for metastatic colorectal cancer. N Engl J Med. 2009;360:1408–17. doi: 10.1056/NEJMoa0805019. [DOI] [PubMed] [Google Scholar]
- 8.Bokemeyer C, Bondarenko I, Makhson A, et al. Fluorouracil, leucovorin, and oxaliplatin with and without cetuximab in the first-line treatment of metastatic colorectal cancer. J Clin Oncol. 2009;27:663–71. doi: 10.1200/JCO.2008.20.8397. [DOI] [PubMed] [Google Scholar]
- 9.Bonner JA, Harari PM, Giralt J, et al. Radiotherapy plus cetuximab for squamous-cell carcinoma of the head and neck. N Engl J Med. 2006;354:567–78. doi: 10.1056/NEJMoa053422. [DOI] [PubMed] [Google Scholar]
- 10.Hofheinz RD, Horisberger K, Woernle C, et al. Phase I trial of cetuximab in combination with capecitabine, weekly irinotecan, and radiotherapy as neoadjuvant therapy for rectal cancer. Int J Radiat Oncol Biol Phys. 2006;66:1384–90. doi: 10.1016/j.ijrobp.2006.07.005. [DOI] [PubMed] [Google Scholar]
- 11.Machiels JP, Sempoux C, Scalliet P, et al. Phase I/II study of preoperative cetuximab, capecitabine, and external beam radiotherapy in patients with rectal cancer. Ann Oncol. 2007;18:738–44. doi: 10.1093/annonc/mdl460. [DOI] [PubMed] [Google Scholar]
- 12.Bertolini F, Chiara S, Bengala C, et al. Neoadjuvant treatment with single-agent cetuximab followed by 5-FU, cetuximab, and pelvic radiotherapy: a phase II study in locally advanced rectal cancer. Int J Radiat Oncol Biol Phys. 2009;73:466–72. doi: 10.1016/j.ijrobp.2008.04.065. [DOI] [PubMed] [Google Scholar]
- 13.Bengala C, Bettelli S, Bertolini F, et al. Epidermal growth factor receptor gene copy number, K-ras mutation and pathological response to preoperative cetuximab, 5-FU and radiation therapy in locally advanced rectal cancer. Ann Oncol. 2009;20:469–74. doi: 10.1093/annonc/mdn647. [DOI] [PubMed] [Google Scholar]
- 14.Rodel C, Arnold D, Hipp M, et al. Phase I–II trial of cetuximab, capecitabine, oxaliplatin, and radiotherapy as preoperative treatment in rectal cancer. Int J Radiat Oncol Biol Phys. 2008;70:1081–6. doi: 10.1016/j.ijrobp.2007.07.2356. [DOI] [PubMed] [Google Scholar]
- 15.Velenik V, Ocvirk J, Oblak I, Anderluh F. A phase II study of cetuximab, capecitabine and radiotherapy in neoadjuvant treatment of patients with locally advanced resectable rectal cancer. Eur J Surg Oncol. 36:244–50. doi: 10.1016/j.ejso.2009.12.002. [DOI] [PubMed] [Google Scholar]
- 16.Semrau RVD, Kocher M, et al. Pre-operative radio-chemo-immunotherapy with cetuximab and 5-FU in patients with locally advanced rectal cancer. First results of a phase I/II trial. Annual meeting of the German and Austrian Society of Radiooncology; Vienna. 2008; abstract 169. [Google Scholar]
- 17.Dworak O, Keilholz L, Hoffmann A. Pathological features of rectal cancer after preoperative radiochemotherapy. Int J Colorectal Dis. 1997;12:19–23. doi: 10.1007/s003840050072. [DOI] [PubMed] [Google Scholar]
- 18.Benjamini Y, Hochberg Y. Controlling the false discovery rate: A practical and powerful approach to multiple testing. Journal of the Royal Statistical Society. 1995;57:289–300. [Google Scholar]
- 19.Peeters KC, Marijnen CA, Nagtegaal ID, et al. The TME trial after a median follow-up of 6 years: increased local control but no survival benefit in irradiated patients with resectable rectal carcinoma. Ann Surg. 2007;246:693–701. doi: 10.1097/01.sla.0000257358.56863.ce. [DOI] [PubMed] [Google Scholar]
- 20.Collette L, Bosset JF, den Dulk M, et al. Patients with curative resection of cT3–4 rectal cancer after preoperative radiotherapy or radiochemotherapy: does anybody benefit from adjuvant fluorouracil-based chemotherapy? A trial of the European Organisation for Research and Treatment of Cancer Radiation Oncology Group. J Clin Oncol. 2007;25:4379–86. doi: 10.1200/JCO.2007.11.9685. [DOI] [PubMed] [Google Scholar]
- 21.Rodel C, Martus P, Papadoupolos T, et al. Prognostic significance of tumor regression after preoperative chemoradiotherapy for rectal cancer. J Clin Oncol. 2005;23:8688–96. doi: 10.1200/JCO.2005.02.1329. [DOI] [PubMed] [Google Scholar]
- 22.Fisher DA, Lakshmanan J. Metabolism and effects of epidermal growth factor and related growth factors in mammals. Endocr Rev. 1990;11:418–42. doi: 10.1210/edrv-11-3-418. [DOI] [PubMed] [Google Scholar]
- 23.Shahbazi M, Pravica V, Nasreen N, et al. Association between functional polymorphism in EGF gene and malignant melanoma. Lancet. 2002;359:397–401. doi: 10.1016/S0140-6736(02)07600-6. [DOI] [PubMed] [Google Scholar]
- 24.Hamai Y, Matsumura S, Matsusaki K, et al. A single nucleotide polymorphism in the 5′ untranslated region of the EGF gene is associated with occurrence and malignant progression of gastric cancer. Pathobiology. 2005;72:133–8. doi: 10.1159/000084116. [DOI] [PubMed] [Google Scholar]
- 25.Costa BM, Ferreira P, Costa S, et al. Association between functional EGF+61 polymorphism and glioma risk. Clin Cancer Res. 2007;13:2621–6. doi: 10.1158/1078-0432.CCR-06-2606. [DOI] [PubMed] [Google Scholar]
- 26.Tanabe KK, Lemoine A, Finkelstein DM, et al. Epidermal growth factor gene functional polymorphism and the risk of hepatocellular carcinoma in patients with cirrhosis. JAMA. 2008;299:53–60. doi: 10.1001/jama.2007.65. [DOI] [PubMed] [Google Scholar]
- 27.Kovar FM, Thallinger C, Marsik CL, et al. The EGF 61A/G polymorphism - a predictive marker for recurrence of liver metastasesfrom colorectal cancer. Wien Klin Wochenschr. 2009;121:638–43. doi: 10.1007/s00508-009-1250-3. [DOI] [PubMed] [Google Scholar]
- 28.Randerson-Moor JA, Gaut R, Turner F, et al. The relationship between the epidermal growth factor (EGF) 5′UTR variant A61G and melanoma/nevus susceptibility. J Invest Dermatol. 2004;123:755–9. doi: 10.1111/j.0022-202X.2004.23304.x. [DOI] [PubMed] [Google Scholar]
- 29.Goto Y, Ando T, Goto H, Hamajima N. No association between EGF gene polymorphism and gastric cancer. Cancer Epidemiol Biomarkers Prev. 2005;14:2454–6. doi: 10.1158/1055-9965.EPI-05-0401. [DOI] [PubMed] [Google Scholar]
- 30.Vauleon E, Auger N, Benouaich-Amiel A, et al. The 61 A/G EGF polymorphism is functional but is neither a prognostic marker nor a risk factor for glioblastoma. Cancer Genet Cytogenet. 2007;172:33–7. doi: 10.1016/j.cancergencyto.2006.07.013. [DOI] [PubMed] [Google Scholar]
- 31.Qi P, Wang H, Chen YM, Sun XJ, Liu Y, Gao CF. No association of EGF 5′UTR variant A61G and hepatocellular carcinoma in Chinese patients with chronic hepatitis B virus infection. Pathology. 2009;41:555–60. doi: 10.1080/00313020903071603. [DOI] [PubMed] [Google Scholar]
- 32.Lanuti M, Liu G, Goodwin JM, et al. A functional epidermal growth factor (EGF) polymorphism, EGF serum levels, and esophageal adenocarcinoma risk and outcome. Clin Cancer Res. 2008;14:3216–22. doi: 10.1158/1078-0432.CCR-07-4932. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Graziano F, Ruzzo A, Loupakis F, et al. Pharmacogenetic profiling for cetuximab plus irinotecan therapy in patients with refractory advanced colorectal cancer. J Clin Oncol. 2008;26:1427–34. doi: 10.1200/JCO.2007.12.4602. [DOI] [PubMed] [Google Scholar]
- 34.Lurje G, Leers JM, Pohl A, et al. Genetic variations in angiogenesis pathway genes predict tumor recurrence in localized adenocarcinoma of the esophagus. Ann Surg. 251:857–64. doi: 10.1097/SLA.0b013e3181c97fcf. [DOI] [PubMed] [Google Scholar]
- 35.Lurje G, Nagashima F, Zhang W, et al. Polymorphisms in cyclooxygenase-2 and epidermal growth factor receptor are associated with progression-free survival independent of K-ras in metastatic colorectal cancer patients treated with single-agent cetuximab. Clin Cancer Res. 2008;14:7884–95. doi: 10.1158/1078-0432.CCR-07-5165. [DOI] [PubMed] [Google Scholar]
- 36.Khambata-Ford S, Garrett CR, Meropol NJ, et al. Expression of epiregulin and amphiregulin and K-ras mutation status predict disease control in metastatic colorectal cancer patients treated with cetuximab. J Clin Oncol. 2007;25:3230–7. doi: 10.1200/JCO.2006.10.5437. [DOI] [PubMed] [Google Scholar]
- 37.Lievre A, Bachet JB, Boige V, et al. KRAS mutations as an independent prognostic factor in patients with advanced colorectal cancer treated with cetuximab. J Clin Oncol. 2008;26:374–9. doi: 10.1200/JCO.2007.12.5906. [DOI] [PubMed] [Google Scholar]
- 38.Qiu LX, Mao C, Zhang J, et al. Predictive and prognostic value of KRAS mutations in metastatic colorectal cancer patients treated with cetuximab: A meta-analysis of 22 studies. Eur JCancer. doi: 10.1016/j.ejca.2010.05.022. [DOI] [PubMed] [Google Scholar]
- 39.Debucquoy A, Haustermans K, Daemen A, et al. Molecular response to cetuximab and efficacy of preoperative cetuximab-based chemoradiation in rectal cancer. J Clin Oncol. 2009;27:2751–7. doi: 10.1200/JCO.2008.18.5033. [DOI] [PubMed] [Google Scholar]
- 40.Popat S, Matakidou A, Houlston RS. Thymidylate synthase expression and prognosis in colorectal cancer: a systematic review and meta-analysis. J Clin Oncol. 2004;22:529–36. doi: 10.1200/JCO.2004.05.064. [DOI] [PubMed] [Google Scholar]
- 41.Morganti M, Ciantelli M, Giglioni B, et al. Relationships between promoter polymorphisms in the thymidylate synthase gene and mRNA levels in colorectal cancers. Eur J Cancer. 2005;41:2176–83. doi: 10.1016/j.ejca.2005.06.016. [DOI] [PubMed] [Google Scholar]
- 42.Pullarkat ST, Stoehlmacher J, Ghaderi V, et al. Thymidylate synthase gene polymorphism determines response and toxicity of 5-FU chemotherapy. Pharmacogenomics J. 2001;1:65–70. doi: 10.1038/sj.tpj.6500012. [DOI] [PubMed] [Google Scholar]
- 43.Dotor E, Cuatrecases M, Martinez-Iniesta M, et al. Tumor thymidylate synthase 1494del6 genotype as a prognostic factor in colorectal cancer patients receiving fluorouracil-based adjuvant treatment. J Clin Oncol. 2006;24:1603–11. doi: 10.1200/JCO.2005.03.5253. [DOI] [PubMed] [Google Scholar]
- 44.Stoehlmacher J, Park DJ, Zhang W, et al. A multivariate analysis of genomic polymorphisms: prediction of clinical outcome to 5-FU/oxaliplatin combination chemotherapy in refractory colorectal cancer. Br J Cancer. 2004;91:344–54. doi: 10.1038/sj.bjc.6601975. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Fernandez-Contreras ME, Sanchez-Hernandez JJ, Gonzalez E, et al. Combination of polymorphisms within 5′ and 3′ untranslated regions of thymidylate synthase gene modulates survival in 5 fluorouracil-treated colorectal cancer patients. Int J Oncol. 2009;34:219–29. [PubMed] [Google Scholar]
- 46.Suh KW, Kim JH, Kim YB, Kim J, Jeong S. Thymidylate synthase gene polymorphism as a prognostic factor for colon cancer. J Gastrointest Surg. 2005;9:336–42. doi: 10.1016/j.gassur.2004.09.030. [DOI] [PubMed] [Google Scholar]
- 47.Mandola MV, Stoehlmacher J, Muller-Weeks S, et al. A novel single nucleotide polymorphism within the 5′ tandem repeat polymorphism of the thymidylate synthase gene abolishes USF-1 binding and alters transcriptional activity. Cancer Res. 2003;63:2898–904. [PubMed] [Google Scholar]
- 48.Ulrich CM, Bigler J, Velicer CM, Greene EA, Farin FM, Potter JD. Searching expressed sequence tag databases: discovery and confirmation of a common polymorphism in the thymidylate synthase gene. Cancer Epidemiol Biomarkers Prev. 2000;9:1381–5. [PubMed] [Google Scholar]
- 49.Uchida K, Hayashi K, Kawakami K, et al. Loss of heterozygosity at the thymidylate synthase (TS) locus on chromosome 18 affects tumor response and survival in individuals heterozygous for a 28-bp polymorphism in the TS gene. Clin Cancer Res. 2004;10:433–9. doi: 10.1158/1078-0432.ccr-0200-03. [DOI] [PubMed] [Google Scholar]