Abstract
A 35-year-old woman was seen as an outpatient with a 3-month history of pain in the right iliac fossa. A CT scan of her abdomen revealed the presence of a mucocele of the appendix. Intra-operatively, an appendico-appendicular intussusception was found. Histology confirmed the presence of a mucinous cystadenoma with the presence of acellular mucin on the serosal surface of the appendix. This association has rarely been described in the literature. Prompt surgical intervention is advocated to prevent the subsequent development of pseudomyxoma peritonei. We present a case of intussusception of the appendix with a mucinous cystadenoma as its lead point.
Keywords: Appendix, Intussusception, Mucinous cystadenoma, Pseudomyxoma peritonei
1. Introduction
Intussusception of the appendix is an uncommon presentation with an incidence of 0.01% of human appendix specimens.1 Symptoms associated with an appendicial intussusception include chronic, remitting lower abdominal pain, gastrointestinal disturbances, and bleeding per rectum. It is very difficult to diagnose the presence of an intussuscepted appendix pre-operatively and investigations will usually include colonoscopy and CT scan.2 We present a case of intussusception of the appendix with a mucinous cystadenoma as its lead point.
2. Case history
A 35-year-old woman was referred to our out patient clinic complaining of a three-month history of abdominal pain and an altered bowel habit. The pain was central and episodic in nature. Associated symptoms included diarrhoea, vomiting, and abdominal distension. She also complained of anorexia and had unintentional weight loss. There was no family history of colorectal cancer or inflammatory bowel disease. Examination revealed a soft abdomen with no palpable abdominal mass and no organomegaly. Both digital rectal examination and rigid sigmoidoscopy were unremarkable. Her full blood count and serum biochemistry taken one month prior to referral were normal. Both upper and lower gastrointestinal endoscopy were arranged to investigate her symptoms further.
Upper gastrointestinal endoscopy was normal. At colonoscopy, an extramucosal lesion was seen bulging into the caecum, with a normal overlying mucosa. Biopsies were taken and histopathological examination confirmed normal large bowel mucosa and no evidence of dysplasia or neoplasia. CT colonography was subsequently undertaken and this confirmed the presence of an appendicular mucocele, the base of which was bulging into the lumen of the caecum. The patient was then admitted into hospital for elective surgery.
A Lanz incision and typical dissection for standard appendicectomy was performed. The patient was found to have a mucocele of the appendix with appendicular intussusception (Fig. 1). Reduction of the intussusception was not attempted. A partial caecectomy was performed, leaving the ileo-caecal valve intact. No peritoneal deposits were found. Histological examination of the resected specimen confirmed the presence of an appendicular intussusception with copious amounts of mucinous material and luminal dilatation. Histology showed a mucinous cystadenoma with low-grade dysplasia at the base of the appendix. Acellular mucin was seen on the serosal surface of the appendix.
Fig. 1.
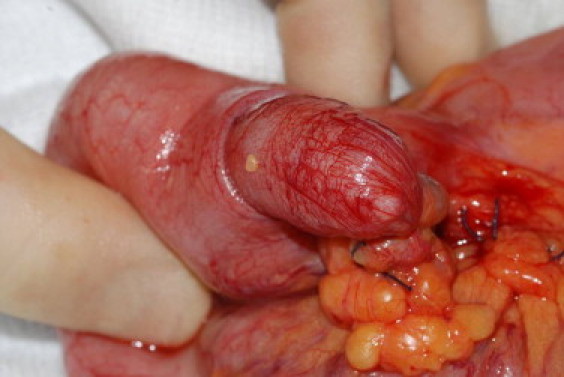
Intra-operative view of an appendico-appendicular intussusception.
The postoperative period was uneventful, and the patient was well on discharge two days following her procedure.
3. Discussion
In adults, the lead point of an intestinal intussusception is usually due to an identifiable cause, such as, intestinal tumours, gastroenteritis, cystic fibrosis or an iatrogenic cause. An association between an appendicular mucocele and an intussusception of the appendix, although rare, has been reported. Mucocele of the appendix is a descriptive term for several pathological processes of which the commonest being mucinous cystadenoma. The presence of a mucinous cystadenoma can lead to malignant transformation and spontaneous or iatrogenic rupture. This can result in implantation of mucin-producing cells inside the peritoneal cavity, and subsequent pseudomyxoma peritonei.3 Early intervention aims to reduce these risks. An appendicular intussusception should not be reduced to avoid exposing the peritoneal cavity to these mucin-producing cells.2
Patients with benign mucinous cystadenomas have an excellent prognosis, with five-year survival rates of greater than 90%. However, those with malignant cystadenocarcimonas and pseudomyxoma peritonei have a five-year survival rate of 25%, signifying the need for early recognition, management and follow-up.4
Small, uncomplicated lesions of the appendix are usually treated by simple appendicectomy, whereas larger lesions, due to the higher potential for malignancy, are treated by right hemicolectomy.3 Alternatively laparoscopic approach allows the benefits of minimal access surgery as well as allowing further diagnostic exploration of the abdominal cavity,5 however it also carries the increased risk of iatrogenic rupture. Therefore certain precautions should be taken including avoidance of grasping of the lesion and removal from the abdominal cavity in a bag.6 In our case, although the lesion was small, it was intussuscepting, thus making an appendicectomy impossible unless resorting to a reduction of the intussusception. Mcswain classified appendiceal intussusceptions into four basic types7 (Table 1). During the procedure a type IV intussusception was identified. Therefore the caecal pole was removed with the appendix to ensure good clearance of its base. Clear resection margins were confirmed histologically.
Table 1.
McSwain classification of appendiceal intussusception.
| Type | |
|---|---|
| I | Tip of the appendix invaginates into the proximal lumen |
| II | Distal appendix invaginates into the lumen of the proximal appendix |
| III | Proximal appendix invaginates into the distal appendix |
| IV | Complete intussusception of the appendix within the caecum |
Following surgery patients require follow-up to identify patients at risk of developing pseudomyxoma peritonei as further intervention may be indicated for this condition. This includes cytoreductive surgery and intraperitoneal chemotherapy, which may help eradicate the metastatic spread of mucinous neoplastic cells in the peritoneum and increase five-year survival rates from 20% to more than 50% with complete cytoreductive surgery.8 Follow-up should also include colonoscopy as 20% of benign mucinous cystadenomas are associated with colorectal cancer.3
Conflicts of interest
None.
Funding
None.
Ethical approval statement
Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal on request.
References
- 1.Langsam L.B., Raj P.K., Galang C.F. Intussusception of the appendix. Dis Colon Rectum. 1984;27:387–392. doi: 10.1007/BF02553007. [DOI] [PubMed] [Google Scholar]
- 2.Chaar C., Wexelman B., Zuckerman K. Intussusception of the appendix: comprehensive review of the literature. Am J Surg. 2009;198:122–128. doi: 10.1016/j.amjsurg.2008.08.023. [DOI] [PubMed] [Google Scholar]
- 3.Zagrodnik D.F., Rose D.M. Mucinous cystadenoma of the appendix: diagnosis, surgical management, and follow-up. Curr Surg. 2003;60(3):341–343. doi: 10.1016/S0149-7944(02)00728-6. [DOI] [PubMed] [Google Scholar]
- 4.Aho A.J., Heinonen R., Lauren P. Benign and malignant mucocele of the appendix: histological types and prognosis. Acta Chir Scand. 1973;139:392–400. [PubMed] [Google Scholar]
- 5.Lau H., Yuen W.K., Loong F., Lee F. Laparoscopic resection of an appendiceal mucocele. Surg Laparosc Endosc Percutan Tech. 2002;12:367–370. doi: 10.1097/00129689-200210000-00014. [DOI] [PubMed] [Google Scholar]
- 6.Navarra G., Asopa V., Basaglia E., Jones M., Jiao L.R., Habib N.A. Mucous cystadenoma of the appendix: is it safe to remove it by a laparoscopic approach? Surg Endosc. 2003;17(5):833–834. doi: 10.1007/s00464-002-4266-6. [DOI] [PubMed] [Google Scholar]
- 7.McSwain B. Intussusception of the appendix: review of the literature and report of a case. South Med J. 1941;34:263–271. [Google Scholar]
- 8.Sugarbaker P.H., Chang D. Results of treatment of 385 patients with peritoneal surface spread of appendiceal malignancy. Ann Surg Oncol. 1999;6:727–731. doi: 10.1007/s10434-999-0727-7. [DOI] [PubMed] [Google Scholar]


