Abstract
A 57-year-old morbidly obese (160 kg) man presented with a 12 h history of severe bilateral scrotal pain and swelling. His scrotum was erythematous, with cellulitis advancing superiorly along the anterior abdominal wall. He was in septic shock. Following resuscitation with intravenous fluids, commencement of vasopressor infusion and broad-spectrum antimicrobials, he underwent surgical exploration and debridement. This revealed a devitalised gangrenous scrotum with abscess formation noted in the ischio-rectal spaces. This was debrided posteriorly to the wall of the rectum. The penis was de-gloved. Both testicles were spared. A colostomy was performed on day 3 to maintain a clean environment for healing. Subsequent scrotal reconstruction and grafting was performed with a pedicled gracilis flap and split skin grafting. The colostomy was reversed at 5 months.
Background
Fournier’s gangrene is a rare, necrotising fasciitis of the genitals, perineum and perianal region caused by a mixture of aerobic and anaerobic microorganisms. This rapidly progressive synergistic infection can lead to multiple organ failure and death within hours of onset, meaning that ability among clinicians to recognise and treat the disease promptly is essential. Broad-spectrum antimicrobials, aggressive surgical debridement and septic shock resuscitation are the mainstay of treatment. Mortality averages 20–30% in most series.1 We report a case of Fournier’s gangrene and discuss the diagnosis (with images), immediate resuscitation and intensive care management, antimicrobial therapy, immediate surgical debridement and long-term surgical repair.
Case presentation
A 57-year-old morbidly obese (160 kg) retired farmer presented with a 12 h history of severe bilateral scrotal pain and swelling. He described his scrotum as being ‘the size of a melon’ and intensely painful to touch. He had a history of rate controlled atrial fibrillation, for which he was on a β blocker, but denied any symptoms of cardiorespiratory disease. He was a non-smoker, drank alcohol infrequently and lived at home with his wife.
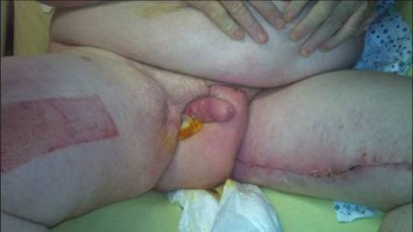
His scrotum was tender and erythematous, more so on the right, with cellulitis advancing superiorly along the anterior abdominal wall and posteriorly along the perineum. There were multiple black gangrenous patches on the right posterior aspect of the scrotum (figures 1 and 2).
Figure 1.
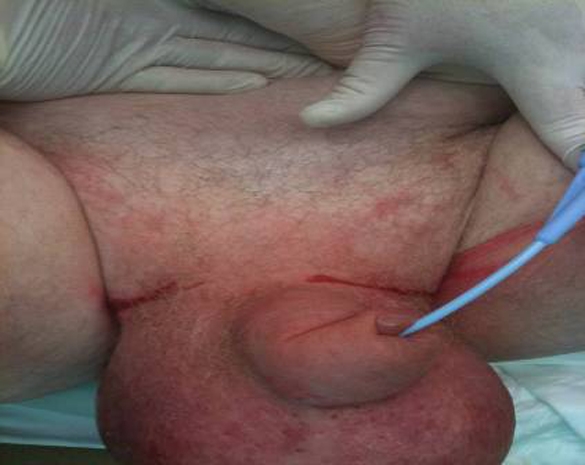
Pre operative images showing swollen, erythematous scrotum.
Figure 2.
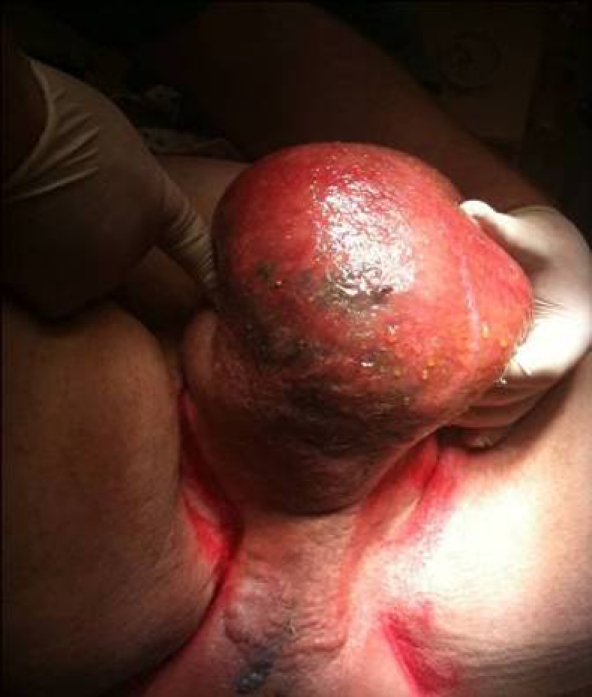
Black gangrenous patches on right posterior aspect of scrotum.
He was in septic shock, characterised by fever, warm peripheries, vasodilatation and hypotension, tachycardia and oliguria.
Investigations
Inflammatory markers were elevated: C-reactive protein of 283 mg/dl and a white cell count of 17 000×106. Blood urea nitrogen and serum creatinine were elevated at 12 mmol/litre and 198 micromol/litre, respectively. Arterial blood gas analysis revealed a metabolic acidosis with pH 7.18, pCO2 4.1 kPa, base deficit-9 and serum lactate 4 mEq/l in keeping with the diagnosis of septic shock.
Differential diagnosis
Differential diagnosis included cellulitis, balanitis, orchitis, epididymitis, torsion or a strangulated hernia. The diagnosis is mainly clinical and was made early by an experienced emergency department doctor.
Treatment
Initial resuscitation (commenced in the emergency department and continued in the intensive care unit) was with intravenous fluids (3 litres crystalloid, 1 litre colloid), vasopressor infusion (norepinephrine) and broad-spectrum antimicrobials; this was followed urgently by surgical exploration and debridement. Exploration revealed a devitalised gangrenous scrotum with abscess formation noted in the ischio-rectal spaces. This was debrided posteriorly to the wall of the rectum. The penis was de-gloved. Both testicles were spared and placed in the inguinal pouch (figure 3).
Figure 3.
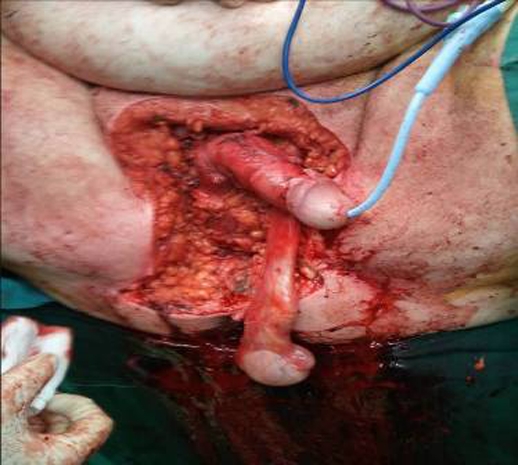
Post debridement. The penis is de-gloved. The right testes has been placed in the inguinal pouch.
He was ventilated for 12 h post operatively and septic shock resolved by 24 h post operatively. A colostomy was performed on day 3 to maintain a clean environment for subsequent healing and a vacuum assisted closure (VAC) dressing was applied over the debrided area. Antimicrobials were continued for 14 days. Scrotal reconstruction and grafting was performed on day 21 with a pedicled gracilis flap and split skin grafting (figure 4). He was discharged home on day 26.
Figure 4.
Post scrotal grafting and reconstruction with pedicled gracilis flap and split skin grafts.
Outcome and follow-up
The grafts and flap have healed well. He underwent successful elective reversal of colostomy at 5 months and he has had no significant complications since discharge.
Discussion
First described by Baurienne in 1764 and formally named by the French venerologist Jean Alfred Fournier in 1883, Fournier’s gangrene is a polymicrobial, synergistic necrotising fasciitis of the perineal, perianal, or genital areas.
Gangrene refers to the local necrosis of soft tissue due to disease or trauma; the necrotic tissue is usually colonised by bacteria. Gangrene is termed dry (usually non-infected) or wet (infected)/gas gangrene.2 Gas gangrene has been recognised for centuries. Hippocrates described it as infection that causes ‘flesh, gnew and bones to fall away in great quantity’.3 Gas gangrene progresses rapidly and has a high morality. Subdivisions include Clostridium cellulites, Clostridium myonecrosis and necrotising fasciitis. These represent part of a continuum of infections, from cutaneous to deep soft tissue, not all of which are due to clostridial species.
Necrotising fasciitis is a fulminant, rapidly progressive infection characterised by widespread tissue destruction and necrosis of fat and fascia with overlying secondary necrosis of skin. It is broadly classified into two types. Type I is a polymicrobial infection, usually with both aerobic and anaerobic organisms, while Type II generally describes a monomicrobial infection, commonly due to Group A streptococcus, or less commonly methicillin resistant staphylococcus aureus (MRSA).
Risk factors for development of Fournier’s gangrene include diabetes (the majority of infections occur in diabetic men), obesity, alcohol abuse and malnutrition, poor tissue perfusion, renal insufficiency, trauma and immunosuppression. There is an identifiable cause in about 95% of cases,4 broadly categorised as an infective process arising in the ano-rectum, urogenital tract or skin of the genitalia.5 Ano-rectal causes include infection in the perianal glands, colorectal injury, inflammatory bowel disease, diverticulitis or appendicitis. Urogenital causes are infective or due to trauma, often related to urethral stricture manipulation. Dermatological causes include hidradenitis suppurativa, ulceration due to scrotal pressure (often related to obesity) or scrotal or perineal trauma.
Fournier’s gangrene generally begins with a prodromal period (hours to days) of pruritus and discomfort of the genitalia or perineum, often followed by sudden onset of severe pain. The pain may later be replaced by anaesthesia as the gangrene progresses. The infection is usually centred at the fascial level, meaning the overlying skin may appear normal initially and the extent of the subdermal gangrene is not apparent. Progression through the fascial layers results in deep tissue necrosis and ultimately gangrenous skin changes. Products of anaerobic metabolism include hydrogen, hydrogen sulphide, nitrogen and nitrous oxide- all of which may be visible radiologically and account for the associated crepitus.
Pathognomonic findings histologically include necrosis of both superficial and deep fascial planes, fibrinoid coagulation of arterioles, acute inflammatory changes and identification of microorganisms. Microorganism virulence results from toxin or enzyme production that creates an environment conducive to rapid microbial multiplication. It is postulated that some organisms produce enzymes causing fibrinoid coagulation of nutrient vessels. This leads to thrombosis and hypoxia, allowing growth of anaerobes and microaerophilic organisms, which can produce enzymes (such as collagenase) that digest fascial barriers allowing further rapid spread of infection.
Macroscopically, fascial destruction is a hallmark of the disease and provides a marker of its extent. Generally, if the fascial plane can be separated easily from the surrounding tissue by blunt dissection it suggests that it is involved in the gangrenous process and that further debridement is required.
There is usually rapid development of severe toxaemia leading to a systemic inflammatory response syndrome, septic shock and progressive organ dysfunction. The inflammatory response to the cytokine storm is characterised by fever or hypothermia, leucocytosis or leucopaenia (or progression from one to the other characterised by >10% immature blast cells), tachycardia or bradycardia and tachypnoea. Septic shock is defined as hypotension (systolic blood pressure <90 mm Hg or >40mm Hg deviation from baseline) which leads to tissue hypoperfusion and organ dysfunction, manifest as lactic acidosis, oliguria, elevated blood urea nitrogen and acute alteration in mental status.
Patient Management
Resuscitation and reversal of septic shock, antimicrobials and aggressive surgical debridement form the mainstay of treatment; urinary or faecal diversion is used later to prevent contamination and allow healing.6 7
-
▶
Initial resuscitation is an emergency and should follow an A, B, C approach. Septic shock is characterised by vasodilatation and capillary leak. Coupled with a degree of septic cardiomyopathy and micro-thrombosis this leads to tissue hypoperfusion, which is compounded by impaired oxygen uptake and utilisation, due to tissue oedema and mitochondrial dysfunction. Therapy is aimed at improving tissue oxygen delivery and uptake, as per the Surving Sepsis Guidelines.8 Supplemental oxygen is administered. Intravascular volume is restored with crystalloid or colloid. End points of resuscitation include urinary output (>0.5 ml/kg/h), central venous pressure (>12 mm Hg) and a reduction in serum lactate. Inotropic and vasopressor support should be commenced to augment cardiac output and treat vasoplegia, once circulating volume is restored. Dobutamine (inotrope at dose range 0–20 mcg/kg/min if heart rate allows) and norepinephrine (vasopressor at dose range of 5–10 mcg/kg/min) are the agents most commonly used. Packed red cell transfusion (to Hb >9 g/dl) to improve oxygen delivery is appropriate if there is evidence of ongoing tissue hypoperfusion.
-
▶
Broad-spectrum intravenous antimicrobial therapy should be commenced immediately following blood sampling for culture and sensitivity. Agents used should have gram positive, gram negative and anaerobic cover. Typically a broad-spectrum penicillin is combined with an imidazole (metronidazole) and an aminoglycoside. Anti MRSA cover with vancomycin or linezolid should be considered if there is a history of or risk factors for MRSA. Clindamycin which has excellent tissue penetration and is effective against gram positive and anaerobic agents may also be used. Antimicrobial therapy is rationalised when tissue and blood culture results are available.
-
▶
Following initial stabilisation and resuscitation urgent surgical exploration and radical debridement should be carried out, to remove all necrotic tissue and any marginally perfused tissue, dissecting through all the fascial planes. If a blunt probe slides through the fascial planes effortlessly, it indicates necrotising fasciitis. Debridement is continued until all remaining tissues are adherent and viable. This can pose a problem if the necrosis is extensive. Multiple repeat exploration and debridement may be required. Faecal diversion is often employed to maintain a clean environment for healing. VAC dressings are useful once adequate surgical debridement has been achieved. They allow fewer dressing changes, less pain, fewer skipped meals, and greater mobility.
-
▶
Renal replacement therapy may be required if acute tubular necrosis develops despite adequate volume restoration and renal perfusion pressure. This is usually delayed until after surgical debridement. Haemodynamic instability means continuous veno-venous haemo-diafiltration is most often used. Anticoagulation with prostacyclin rather than with heparin is preferred as there is less bleeding (important in the post operative period). Co-agulopathy and thrombocytopaenia due to sepsis are corrected as appropriate. Ventilatory support may be required for respiratory failure from acute respiratory distress syndrome secondary to systemic sepsis.
Learning points.
-
▶
Early diagnosis and treatment is essential to reduce mortality in this rare but life-threatening disease.
-
▶
Reversal of shock, broad-spectrum antimicrobial therapy and aggressive surgical debridement are the cornerstones of treatment.
-
▶
Faecal diversion, VAC dressings and reconstructive plastic surgery are important considerations when the infective process has been arrested.
Acknowledgments
Dr Aidan Sharkey, Consultant Anaesthetist, University College Hospital, Galway.
Footnotes
Competing interests None.
Patient consent Obtained.
References
- 1.Pawłowski W, Wroński M, Krasnodebski IW. [Fournier’s gangrene]. Pol Merkur Lekarski 2004;17:85–7 [PubMed] [Google Scholar]
- 2.Henry M, Thompsen J. Clinical Surgery. First edition Edinburgh: WB Saunders; 2002:113, 126. [Google Scholar]
- 3.Cameron JL. Current Surgical Therapy. Eight edition Philadelphia, PA: Elsevier Mosby; 2004:1079–85 [Google Scholar]
- 4.Smith GL, Bunker CB, Dinneen MD. Fournier’s gangrene. Br J Urol 1998;81:347–55 [DOI] [PubMed] [Google Scholar]
- 5.Clayton MD, Fowler JE, Jr, Sharifi R, et al. Causes, presentation and survival of fifty-seven patients with necrotizing fasciitis of the male genitalia. Surg Gynecol Obstet 1990;170:49–55 [PubMed] [Google Scholar]
- 6.Eke N. Fournier’s gangrene: a review of 1726 cases. Br J Surg 2000;87:718–28 [DOI] [PubMed] [Google Scholar]
- 7.Endorf FW, Supple KG, Gamelli RL. The evolving characteristics and care of necrotizing soft-tissue infections. Burns 2005;31:269–73 [DOI] [PubMed] [Google Scholar]
- 8.Dellinger RP, Levy MM, Carlet JM, et al. Surviving sepsis campaign: international guidelines for management of severe sepsis and septic shock. Crit Care Med 2008;36:296–327 [DOI] [PubMed] [Google Scholar]