Abstract
Nitric oxide (NO) is one of the most pleiotropic signaling molecules at systemic and cellular levels, participating in vascular tone regulation, cellular respiration, proliferation, apoptosis and gene expression. Indeed NO actively participates in trophoblast invasion, placental development and represents the main vasodilator in this tissue. Despite the large number of studies addressing the role of NO in the placenta, its participation in placental vascular development and the effect of altered levels of NO on placental function remains to be clarified. This review draws a time-line of the participation of NO throughout placental vascular development, from the differentiation of vascular precursors to the consolidation of vascular function are considered. The influence of NO on cell types involved in the origin of the placental vasculature and the expression and function of the nitric oxide synthases (NOS) throughout pregnancy are described. The developmental processes involved in the placental vascular bed are considered, such as the participation of NO in placental vasculogenesis and angiogenesis through VEGF and Angiopoietin signaling molecules. The role of NO in vascular function once the placental vascular tree has developed, in normal pregnancy as well as in pregnancy-related diseases, is then discussed.
Keywords: Placenta, Nitric oxide, Vasculogenesis, Angiogenesis, Vascular tone, Pregnancy diseases
1. Introduction
Placental vascular development represents a crucial process for adequate fetal development. In fact, pregnancy pathologies, such as, gestational diabetes mellitus (GDM), intrauterine growth restriction (IUGR) and pre-eclampsia (PE) are related with vascular dysfunction in the placental bed [1,2]. The etiology of this dysfunction remains to be fully understood [3,4] but even though these conditions have detrimental effects on the fetus in late gestation they seem to be influenced by early embryo development, and are exacerbated by environmental cues through gestation such as oxidative stress, local oxygen tension and metabolic disorders [5–7].
The placenta originates from the outer cell layer of the morula, called trophoblast, which proliferates after implantation, invades the decidua and differentiates into cytotrophoblast and syncytiotrophoblast, forming the primary villi. These villi are invaded by mesenchymal cells derived from the embryo (secondary villi) which through vasculogenesis generate vascular capillaries, forming the tertiary villi. These villi contunually undergo transformation and maturation during gestation and this includes (1) further differentiation of cytotrophoblast to syncytiotrophoblast, (2) branching angiogenesis and growth of the vascular tree, and (3) longitudinal growth of capillaries and maturation of vascular vessels [8,9]. Thus, placental vasculogenesis, angiogenesis and vascular function are interrelated processes that influence fetal growth throughout gestation.
Nitric oxide (NO) produced by the endothelial and inducible NO synthases (eNOS and iNOS, respectively) actively regulate embryo development, implantation and trophoblast invasion [10–12]. Furthermore, vascular tone in the placenta is controlled by several vasoactive mediators, of which NO is the most important [13]. On the other hand, vasculogenesis and angiogenesis depend on the expression of several signaling molecules, such as vascular endothelial growth factor (VEGF) and its receptors VEGFR-1 (Flt-1) and VEGFR-2 (Flk-1), transforming growth factor β-1 (TGF β-1), angiopoietin (Ang-) 1 and 2 [9,14], which exert their effects in part through NO synthesis. However, despite the evidence of the participation of NO in implantation and angiogenesis, both in the embryo and under physiologic adaptations, its role on vascular development in the placenta is not completely understood. Here we review direct and indirect data that relate NO synthesis with placental vascular development and function during gestation.
2. Expression of nitric oxide synthases in the placenta
During gestation NOS isoform expression is dynamically regulated in the placenta (Fig. 1), which show heterogeneous properties and distribution (Table 1). In fact, at least eNOS and iNOS have been found in diverse species since early stages of placental development [15–19]. The iNOS isoform is expressed mainly at the feto-maternal interface in the first stages of pregnancy [20]. Apparently, there is an increase in iNOS activity throughout pregnancy which peaks at mid gestation [21–24]. On the other hand, in human first trimester placenta, eNOS is expressed in syncytiotrophoblast, early endothelium within the primitive villous capillaries, intermediate and extravillous trophoblast [15,16], contributing to the total NO production at this stage [25]. As pregnancy continues there is an increase and redistribution of eNOS expression, mainly to syncytiotrophoblast and endothelial cells [16,17,26,27]. There is an up-regulation of eNOS expression in the endothelium of chorionic arteries during the second half of gestation, described in fetal sheep [28], which seems to be reduced in animal models of IUGR [19,29]. However, in human IUGR there is not agreement about the expression levels of eNOS [16,26,27,30]. Additionally, differences in eNOS levels do not explain by themselves the phenotypes observed in pregnancy diseases. To gain a more complete picture, it is necessary to determine how other molecules implicated in l-arginine metabolism, such as iNOS, arginases and reactive oxygen species, regulate NO synthesis and bioavailability. Thus, further studies addressing these aspects are required.
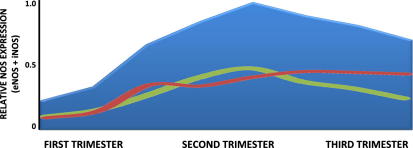
Fig. 1.
Schematic representation of NOS isoform expression in the placenta. Changes in total NOS (blue background), eNOS (red line) and iNOS (green line) expression in placenta throughout pregnancy. Graph shows NOS levels described for different species (i.e. human, mouse, porcine, rat and sheep) determined by enzymatic activity and/or protein expression. Data derived from Refs. [15–17, 19, 21–24, 184]. (For interpretation of the references to color in this figure legend, the reader is referred to the web version of this article.)
Table 1.
Kinetic parameters of recombinant human NOS (Refs. [185–189]) and placental NOS distribution (Ref.s [16,17,19,21–24,190]). EVT, extravillous trophoblast; ST, syncytiotrophoblast; EC, endothelial cell; SMC, smooth muscle cell; n.d., not described.
| eNOS | iNOS | nNOS | |
|---|---|---|---|
| Kinetic parameter | |||
| Vmax(nmol × min−1 × mg−1) | 170 | 800 | 425 |
| Km for l-arginine (μmol/l) | 2.5 | 22 | 0.8 |
| Km for O2 (μmol/l) | 4 | 130 | 350 |
| Placental distribution | |||
| Early gestation | EVT, ST | EVT, ST | n.d. |
| Mid gestation | ST, EC | ST | n.d. |
| Late gestation | EC | ST | SMC |
3. Nitric oxide and placental vasculogenesis
Vasculogenesis is the process by which vessels are formed from mesenchymal-derived hemangioblasts which differentiate into endothelial cells [8]. In general, initiation of vasculogenesis requires the expression of VEGF [31], the mitogenic effects of which are mediated by NO [32,33]. However, studies in NOS-knockout mice have shown that NOS deficiency does not prevent embryonic vascular development, although NO synthesis is required for adequate vascular structure and function [34,35]. Furthermore, expression of eNOS in embryonic vascular development represents a late hallmark of differentiation during vasculogenesis, which could be related to the emergence of cardiac activity [36] and its role is prominent during the consolidation and growth of the vascular system [37,38].
However, the site from which the vascular progenitors for placental and embryo vasculogenesis emerge is still debated. It is now broadly accepted that in the embryo vascular progenitors emerge from intra- and extra-embryonic mesodermal tissues [39], whilst in the placenta they arise from the extra-embryonic mesoderm [1]. Additionally, there is growing evidence for a crucial role of the yolk sac in embryo and placental vascular development [40]. Indeed, using Ncx-1 knockout mice which fail to initiate cardiac contraction Lux et al. [41] showed that all the hematopoietic progenitor cells emerge from the yolk sac. Furthermore, a study in mice yolk sac demonstrated that vasculogenesis at this level is initiated by NO [42]. These authors described the spatio-temporal expression pattern of iNOS and eNOS, which was related to vasculogenesis in the yolk sac. In the first stage, at 7 days of embryonic development (E7.0), iNOS-derived NO synthesized by endodermal cells induces the differentiation of adjacent extra-embryonic mesodermal cells to form a primary capillary plexus. After that, eNOS expression increases in the yolk sac mesodermal cells [36,42] accompanied by a decrease in iNOS expression in the endoderm [42]. Experimental inhibition of NOS activity at E6.5 completely arrests the development of the primary capillary plexus [42]. Altogether, these data suggest that NO could be crucial for placental vasculogenesis.
4. Nitric oxide and placental angiogenesis
Growth and consolidation of the placental vascular tree occurs by angiogenesis. In this process single vessels are formed by endothelial precursor cells (EPC) which differentiate into endothelial cells, and/or proliferate from endothelial cells. These vessels can grow in two ways, (1) non-branching angiogenesis, which implies an increase in the length of the villous vessels, and (2) branching angiogenesis, in which multiple short capillary loops are formed [8], increasing the vascular surface area. After these processes have taken place, the vessels mature and their structures stabilize. Additional maturation and specialization in the vascular system is influenced by environmental cues, such as blood flow, oxygen tension, oxidative stress which could be signaled by epigenetic mechanisms [43]. All these factors have been implicated in the development and function of the human placenta [5–7].
Participation of NO in angiogenesis is more clearly established than it is in vasculogenesis. Angiogenesis has been studied in vitro using endothelial cells from the human umbilical vein (HUVEC). Animals with experimentally-induced eNOS deficiency show defective vascular development throughout the vascular tree, which is mainly associated with decreased vessel maturation and disorganization [35,44]. Despite the initial evidence that showed an inhibitory role for NO in angiogenesis [45], further studies have demonstrated that exogenous NO [46,47] or over-expression of eNOS [48,49] induce proliferation of endothelial cells and angiogenesis. In contrast, inhibition of NOS [50,51] or deletion of the eNOS gene [52] are accompanied by deficient angiogenesis in the embryo and placenta. Additionally, NO induces proliferation in fetal endothelial cells coming from different vascular beds [53–55] and regulates the caliber of central vessels [56].
The main molecular mediators of angiogenesis, VEGF and angiopoietin [57] depend mainly on NO synthesis to induce new vessel formation. In endothelial cells VEGF induces eNOS-dependent NO synthesis through the activation of VEGFR-1 [58] and VEGFR-2 [59]. It has been shown that VEGF-induced angiogenesis requires NO synthesis [32] derived from eNOS activity [60–62]. Moreover, migration of endothelial cells and EPC is regulated by NO. VEGF-induced migration requires the activation of eNOS through PKCδ [33], Akt [63] and HSP90 [64]. Nitric oxide facilitates cell migration in angiogenesis, increasing the expression of adhesion molecules (i.e. integrin αvβ3) [65,66] and extracellular matrix metalloproteases (i.e. MT1-MMP, MMP-9 and MMP-13) allowing the invasion of endothelial cells and new vessel formation [67–69]. Angiopoietin activates eNOS via PI3K/Akt [70] and ERK1/2 [71] pathways, leading to proliferation and angiogenesis. Additionally, Ang-1 increases the expression of eNOS [72], whilst eNOS over-expression enhances the angiogenic response to Ang-1 [49]. Moreover, the Ang-1/eNOS pathway contributes to vessel maturation and stabilization [49,72]. In this context, capillary formation and maintenance is influenced by the expression of VE-cadherin, which is regulated by VEGF and Ang-1 [73,74]. It has been shown that NO induces the expression and function of VE-cadherin [75–77] modifying the stability and permeability of the endothelium.
Additionally, NO donors induce proliferation in ovine placental endothelial cells via activation of MEK1/2 [54]. On the other hand, eNOS [36] and Akt [78] knockout mice show reduced placental development with decreased vascularization. Moreover, NO increases the levels of VEGF [46] and Ang-1 [79,80] in endothelium. All these data show that NO is not only an effector of angiogenic pathways, but an inducer and positive feedback signal for Ang-1- and VEGF-induced angiogenesis.
5. Placental angiogenesis in diseases of pregnancy
Placental dysfunction is present in some diseases of pregnancy (i.e. GDM, IUGR and PE) [1,2,81], and accompanied by abnormal expression of angiogenic mediators [82–86] and altered NO synthesis [2]. Interestingly Akt null mice fetuses present IUGR [37], detectable as early as E8.5 [38], a time at which the placental vascular development depends only on angiogenesis. In various models of IUGR the expression of eNOS and angiogenic factors is higher during the first half of pregnancy compared with normal fetuses [19,87–89]. However, by the end of gestation these levels fall below those seen in normal placentae [19,29,87,88] suggesting a possible failure of the compensatory mechanisms which normally sustain placental development and the consequently, fetal growth.
In contrast to IUGR, placentae from GDM pregnancies are larger than normal [90] showing decreased formation of terminal villi and increased numbers of intermediate villi in relation to gestational age [81]. Studies in rats have suggested that the increased growth and vascularization in GDM are associated with higher levels of MMP-2 and MMP-9, the activities of which are positively regulated by NO [91]. These data suggest that NO not only regulates endothelial cell proliferation and migration in the placenta, but participates in the stabilization of the new vessels.
However, there is no well established level of NO required for adequate placental angiogenesis. High NO levels can prevent angiogenesis [45,92,93], and its effect on cell survival and proliferation depends on its concentration [94]. This could explain in part why pregnancy diseases, such as IUGR and PE, show higher levels of placental NO [95–98] and nitrosative stress [99] without adequate placental vascularization.
6. Nitric oxide in placental vascular maturation
The adequate morphology and function of the vascular tree at different levels (i.e. arteries/veins, and conduit/resistance/exchange vessels) are modulated by environmental cues, such as, blood flow, oxygen levels, oxidative stress and epigenetic factors [43]. In addition, these signals have a functional relationship with the eNOS-derived NO. Shear stress induces the differentiation of human placenta-derived pluripotent cells to endothelial cells [100], and the specialization of endothelial progenitor cells to “arterial” endothelial cells [101]. In this context, the ability of new endothelial cells to generate vessels depends on the release of NO from pre-existing endothelial cells [102]. Additionally, shear stress is the main stimulus for NO release in placental vessels [103] and for angiogenesis via eNOS activation [104,105]. Indeed in the focal adhesion kinase (FAK – a critical shear stress sensor) knockout mouse there is impaired placental vascular development [106]. Thus, it can be proposed that the increase in placental blood flow during gestation [23,107] drives placental vascular maturation, in part, through NO synthesis.
Hypoxia is an important factor that regulates placental development and angiogenesis. In fact, a fine tuning of oxygen levels throughout pregnancy are required, being hypoxia associated with beneficial and detrimental effects on development [6]. It stimulates trophoblast invasion, differentiation, survival [6], angiogenesis [108,109] and vasculogenesis [108]. The angiogenic effect of hypoxia can occur via VEGF and eNOS, which are activated by hypoxia-inducible factor-α (HIF-α), a key transcription factor operating in hypoxia [108,109]. However, chronic hypoxia is associated with reduced fetal and placental development [110], and in the mouse embryo high levels of HIF-α induce defective chorionic villi and placental vascular development [111]. Prolonged hypoxia is also related with endothelial cell apoptosis via p53 [112] and nuclear factor κB (NF-κB) [113]. There is some uncertainty about the effect of hypoxia on eNOS expression and activity. Some reports have shown an induction of eNOS expression in hypoxia [114–116], whilst others suggest a down-regulation [117–119]. These differences could be explained, in part, by the different vascular beds, endothelial cell types (i.e. arteries [114,116] and veins [117–119]). Additionally, NO has a dual effect on HIF levels: short exposures to hypoxia (2 h) activates eNOS and increases HIF-1α [120,121], however, after 4 h of hypoxia NO increases the levels of prolyl hydroxylases (PHD), which under normal oxygen levels induce HIF-1α degradation [121,122]. Alternatively, NO-dependent activation of PHD can occur through a change in oxygen consumption [123] via inhibition of mitochondrial respiration [124]. Prolonged exposure to hypoxia is associated with decreased eNOS activity, endothelial cell apoptosis and deficient placental vascular development, indicating that placental angiogenesis is very sensitive to oxygen levels. This suggests that NO participates in responses to acute hypoxia via inducing HIF and contributes to a negative feedback process in chronic hypoxia.
During placental vascular maturation and development epigenetic mechanisms play a key role. The expression of genes implicated in trophoblast invasion are influenced by histone post-translational modifications (HPTM) [125], whilst placental growth and function are regulated by DNA methylation (imprinting) and HPTM [126–128]. Moreover, IUGR placentae show epigenetic modifications [129–131] which correlate with abnormal placental development. On the other hand, the first stages of vascular development are controlled mainly by genetic processes; however, endothelial specialization and vessel maturation are controlled by epigenetic mechanisms [43]. There is growing evidence that endothelial precursor cell differentiation, endothelial cell specialization, and shear stress- and hypoxia-induced responses are modulated by epigenetic mechanisms, such as, DNA methylation, HPTM and non-coding small RNA-mediated mechanisms [132,133]. Shear stress- and VEGF-induced differentiation of endothelial precursor cells activate histone deacetylase (HDAC) 1 and 3, increasing the expression of VEGFR-2 and eNOS [134]. HDAC inhibition reduces the VEGF-induced angiogenesis through down-regulation of VEGFR-1 and -2 expression [135], whilst histone methyl transferase activity is required for migration and vessel sprouting [136]. Additionally, hypoxia-induced angiogenesis requires HDAC1 activity, which decreases the expression of von Hippel-Lindau, increasing HIF-1α levels [137]. Interestingly, reduced angiogenesis induced by HDAC inhibition is not reversed by VEGF supplementation, but is restored by NO restitution with S-nitroso-N-acetylpenicillamine (SNAP) [138]. The promoter region of the eNOS gene shows a cell-specific pattern of epigenetic modifications [133]. There are subtle differences in the epigenetic markers between micro and macrovascular endothelial cells [139] arguing for a role for the differential expression of eNOS in different vascular beds. Altogether these data show that in endothelial cells eNOS expression is highly regulated by epigenetic mechanisms with important effects on angiogenesis. Additionally, there is growing evidence that NO exerts control on epigenetic mechanisms (reviewed in Illi et al. [140]).
7. Nitric oxide and placental vascular function
The placenta lacks adrenergic and cholinergic innervation [141], thus its vascular tone is regulated mainly by local factors derived from the endothelium and blood cells. Studies in the later 1980’s and early 1990’s show that the endothelium from chorionic and umbilical vessels releases NO [142,143]. Further studies demonstrated that in umbilical vessels the production of NO and its vasodilator effect is higher than that of prostacyclin I-2 [144,145]. Like other vascular beds, placental vessels express the molecular mediators of the classical NO-dependent pathway which includes the soluble guanylate cyclase (sGC) [146], cGMP-dependent protein kinase and cGMP-specific phosphodiesterases [147,148]. Nitric oxide exerts its effects via activation of the sGC [149] and modulation of potassium channel activity (BKCa) [150,151] (Fig. 2). The NO synthesis at this level can be induced by histamine [142], adenosine [143,152], ATP [143], calcitonin gene-related peptide (CGRP) [153,154], and shear stress [103,155]. The later is an important stimulus which activates eNOS through its phosphorylation at serine 1177 via ERK1/2 and Akt in placental endothelium [156] increasing its long term expression [157].
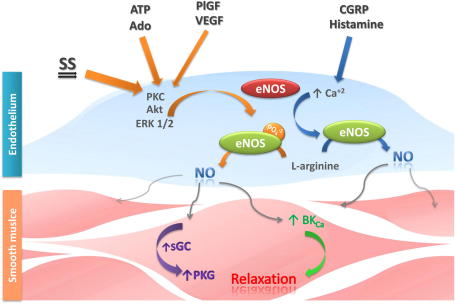
Fig. 2.
Nitric oxide-dependent vasodilation in the placenta. Vasodilator effects of NO in placental vessels can be induced via; a) activation of protein kinases (i.e. PKC, Akt and ERK1/2) by shear stress (SS), adenosine (Ado), ATP, VEGF or PlGF; and b) increasing intracellular calcium concentration induced by agonists (i.e. CGRP and histamine). Both pathways activate eNOS leading to NO production, which diffuses to the adjacent smooth muscle layer. Noteworthy, NO action on placental smooth muscle cells occurs either in a cGMP-dependent (PKG) and -independent (BKCa) fashion.
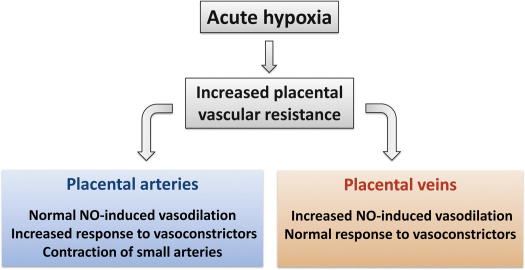
Oxygen level is the most important factor controlling placental vascular reactivity; hypoxia in vivo and ex vivo increases placental vascular tone. In isolated placental vessels low oxygen levels reduce the maximal response to vasodilator agents [158] and increase that to vasoconstrictors [158–160]. Studies in sheep have shown that NO synthesis plays a key role maintaining placental blood flow during acute episodes of hypoxemia [161]. In perfused human cotyledons NOS inhibition and hypoxia independently increase placental perfusion pressure to a similar degree, effects prevented by NO donors [162], suggesting that the effect of hypoxia is mediated in part via low NOS activity. The effect of hypoxia in placental vasculature depends on the vessels studied (Fig. 3). In isolated chorionic arteries hypoxia increases the maximal response to KCl and the thromboxaneA-2 mimetic U46619 [159,160]. However, the maximal response to the NO-donor SNP is unaffected by acute changes in the PO2 [160] in these vessels. In contrast, in chorionic and umbilical veins an acute reduction on PO2 has a positive effect on the vasodilator response to NO [160] and NOS activity [163], whilst there is no change in the response to vasoconstrictors [160]. The effect of PO2 on NO-induced responses in umbilical arteries has not been resolved; Lovren & Triggle [150] showed that the maximal vasodilator response and sensitivity to NO were reduced at low PO2 (<55 mmHg, slightly higher than normal fetal PO2, which is 25–30 mmHg) compared with higher oxygen levels (>300 mmHg); however Leung et al. [164] observed no changes in NO-induced vasodilation with changes in pO2. The study of the molecular mechanisms activated by hypoxia in placental endothelium has been carried out only in HUVEC. It has been demonstrated that HUVEC exposed to 24 h of hypoxia show a decrease in l-arginine transport and eNOS activity [117,118].
Fig. 3.
Effects of acute hypoxia in placental vasculature. Depicted in this figure is the vascular response of placental (umbilical and chorionic) vessels to an acute reduction in oxygen levels.
8. Placental vascular reactivity and nitric oxide synthesis in diseases of pregnancy
As previously discussed, in normal conditions NO is the main vasodilator in the placenta. For this reason several studies have characterized alteration in placental NO synthesis in an attempt to explain the vascular dysfunction observed in pregnancy diseases, such as IUGR, PE and GDM. Alterations in placental vascular reactivity in these conditions are associated with changes in vascular tree structure and vasoactive response pathways. In IUGR and IUGR/PE placentae the villous tree has longer capillaries with fewer branches [165] and lower caliber umbilical vessels [166,167] compared with normal placenta. However, there are no alterations in the maximal responses to vasoconstrictor agents in IUGR chorionic vessels [168,169]. In contrast, the response to NO-dependent vasodilator agents is decreased in IUGR and PE. IUGR chorionic arteries show a reduced vasodilator response to VEGF and PIGF [168], whilst in PE the response to CGRP is practically absent [170]. It is noteworthy that in these vessels the response to exogenous NO is not altered [171], however the amplitude and frequency of NO-dependent spontaneous tone oscillations are reduced in IUGR chorionic arteries and can be invoked in normal vessels by inhibiting NO synthesis [172]. As other metabolic pathways which use l-arginine, such arginases, could compete with eNOS in the placental endothelium, they may play a role under these circumstances. It has been shown that arginase-2 expression is increased in chorionic villi endothelium in PE [173]. Furthermore, we have recently demonstrated in HUVEC that arginase-2 levels and activity are up-regulated by hypoxia [174]; however the role of arginase activity in the control of placental vascular reactivity remains to be determined. These data suggest that vascular dysfunction in diseases of pregnancy is mainly due to changes in vessel structure and activation of NO-synthesis pathways by vasodilator agents rather than by altered responses to NO and vasoconstrictors.
The expression of NOS and NO-metabolites levels in placental endothelium in pregnancy pathologies cannot be easily correlated with the vascular dysfunction observed. Rutherford and colleagues [95] reported increased levels of NOS in chorionic villi of IUGR and PE placentae and these were decreased in umbilical vessels compared with normal placenta. Similarly, increased levels of NO-metabolites in umbilical cord blood [96] and placental tissue [98] of IUGR pregnancies have been reported. The source of this NO is still unclear. Initial studies carried out by Myatt and colleagues [26] found increased levels of eNOS in the endothelium of IUGR and PE placentae. However, other authors have found decreased levels of eNOS in these conditions [30,173] that can be correlated with the vascular dysfunction determined in vivo [30]. Additionally, in HUVEC from PE [175] and IUGR [118] pregnancies, decreased eNOS expression and activity can be observed. Apparently, HUVEC chronically exposed to hypoxia, as occurs in IUGR pregnancies, do not regulate the l-arginine/NO pathway in response to hypoxia and present a persistent hypoxia-like phenotype [117,118]. An explanation for the increased levels of NO-metabolites together with increased placental vascular resistance in IUGR and PE could be due to higher iNOS expression. Giannubilo and colleagues [30] found that eNOS protein levels negatively correlate with the pulsatility Index (PI) determined by Doppler ultrasound, whilst iNOS levels in IUGR placental endothelium show a positive correlation with PI. Additionally, normal HUVEC exposed to PE-derived umbilical plasma show higher iNOS expression [176]. Under these conditions increased levels of nitrosative stress have been described [99]. HUVEC exposed to oxidative stress down-regulate eNOS and up-regulate iNOS expression [177], effects which are increased by shear stress and lead to nitrosative stress and cell apoptosis [178]. Increased endothelial iNOS expression has been implicated in vascular dysfunction [179,180] and in animal models of diabetes [181,182], atherosclerosis [179] and aging [183]. Thus NO and NO-metabolite levels are not necessarily associated with improved placental endothelial function and further studies are required to determine the source of NO (i.e. eNOS or iNOS) in diseases of pregnancy characterized by placental vascular dysfunction.
Acknowledgements
FONDECYT 1080534 & 1110977 (PC); CONICYT-ACT-73 (PC); CONICYT-24100107 (BJK); British Heart Foundation (MAH).
References
- 1.Chaddha V., Viero S., Huppertz B., Kingdom J. Developmental biology of the placenta and the origins of placental insufficiency. Semin Fetal Neonatal Med. 2004;9:357–369. doi: 10.1016/j.siny.2004.03.006. [DOI] [PubMed] [Google Scholar]
- 2.Casanello P., Escudero C., Sobrevia L. Equilibrative nucleoside (ENTs) and cationic amino acid (CATs) transporters: implications in foetal endothelial dysfunction in human pregnancy diseases. Curr Vasc Pharmacol. 2007;5:69–84. doi: 10.2174/157016107779317198. [DOI] [PubMed] [Google Scholar]
- 3.Villar J., Carroli G., Wojdyla D., Abalos E., Giordano D., Ba’aqeel H., World Health Organization Antenatal Care Trial Research Group Preeclampsia, gestational hypertension and intrauterine growth restriction, related or independent conditions? Am J Obstet Gynecol. 2006;194:921–931. doi: 10.1016/j.ajog.2005.10.813. [DOI] [PubMed] [Google Scholar]
- 4.Escudero C., Sobrevia L. A hypothesis for preeclampsia: adenosine and inducible nitric oxide synthase in human placental microvascular endothelium. Placenta. 2008;29:469–483. doi: 10.1016/j.placenta.2008.02.008. [DOI] [PubMed] [Google Scholar]
- 5.Fowden A.L., Forhead A.J., Coan P.M., Burton G.J. The placenta and intrauterine programming. J Neuroendocrinol. 2008;20:439–450. doi: 10.1111/j.1365-2826.2008.01663.x. [DOI] [PubMed] [Google Scholar]
- 6.Burton G.J. Oxygen, the Janus gas; its effects on human placental development and function. J Anat. 2009;215:27–35. doi: 10.1111/j.1469-7580.2008.00978.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Dennery P.A. Oxidative stress in development: nature or nurture? Free Radic Biol Med. 2010;49:1147–1151. doi: 10.1016/j.freeradbiomed.2010.07.011. [DOI] [PubMed] [Google Scholar]
- 8.Demir R., Kayisli U.A., Cayli S., Huppertz B. Sequential steps during vasculogenesis and angiogenesis in the very early human placenta. Placenta. 2006;27:535–539. doi: 10.1016/j.placenta.2005.05.011. [DOI] [PubMed] [Google Scholar]
- 9.Herr F., Baal N., Widmer-Teske R., McKinnon T., Zygmunt M. How to study placental vascular development? Theriogenology. 2010;73:817–822. doi: 10.1016/j.theriogenology.2009.11.003. [DOI] [PubMed] [Google Scholar]
- 10.Kaufmann P., Black S., Huppertz B. Endovascular trophoblast invasion: implications for the pathogenesis of intrauterine growth retardation and preeclampsia. Biol Reprod. 2003;69:1–7. doi: 10.1095/biolreprod.102.014977. [DOI] [PubMed] [Google Scholar]
- 11.Ayling L.J., Whitley G.S., Aplin J.D., Cartwright J.E. Dimethylarginine dimethylaminohydrolase (DDAH) regulates trophoblast invasion and motility through effects on nitric oxide. Hum Reprod. 2006;21:2530–2537. doi: 10.1093/humrep/del111. [DOI] [PubMed] [Google Scholar]
- 12.Harris L.K., McCormick J., Cartwright J.E., Whitley G.S., Dash P.R. S-nitrosylation of proteins at the leading edge of migrating trophoblasts by inducible nitric oxide synthase promotes trophoblast invasion. Exp Cell Res. 2008;314:1765–1776. doi: 10.1016/j.yexcr.2008.02.010. [DOI] [PubMed] [Google Scholar]
- 13.Poston L., McCarthy A.L., Ritter J.M. Control of vascular resistance in the maternal and feto-placental arterial beds. Pharmacol Ther. 1995;65:215–239. doi: 10.1016/0163-7258(94)00064-a. [DOI] [PubMed] [Google Scholar]
- 14.Burton G.J., Charnock-Jones D.S., Jauniaux E. Regulation of vascular growth and function in the human placenta. Reproduction. 2009;138:895–902. doi: 10.1530/REP-09-0092. [DOI] [PubMed] [Google Scholar]
- 15.Ariel I., Hochberg A., Shochina M. Endothelial nitric oxide synthase immunoreactivity in early gestation and in trophoblastic disease. J Clin Pathol. 1998;51:427–431. doi: 10.1136/jcp.51.6.427. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Rossmanith W.G., Hoffmeister U., Wolfahrt S., Kleine B., McLean M., Jacobs R.A. Expression and functional analysis of endothelial nitric oxide synthase (eNOS) in human placenta. Mol Hum Reprod. 1999;5:487–494. doi: 10.1093/molehr/5.5.487. [DOI] [PubMed] [Google Scholar]
- 17.Dötsch J., Hogen N., Nyúl Z., Hänze J., Knerr I., Kirschbaum M. Increase of endothelial nitric oxide synthase and endothelin-1 mRNA expression in human placenta during gestation. Eur J Obstet Gynecol Reprod Biol. 2001;97:163–167. doi: 10.1016/s0301-2115(00)00532-7. [DOI] [PubMed] [Google Scholar]
- 18.Sengupta J., Dhawan L., Lalitkumar P.G., Ghosh D. Nitric oxide in blastocyst implantation in the rhesus monkey. Reproduction. 2005;130:321–332. doi: 10.1530/rep.1.00535. [DOI] [PubMed] [Google Scholar]
- 19.Ziebell B.T., Galan H.L., Anthony R.V., Regnault T.R., Parker T.A., Arroyo J.A. Ontogeny of endothelial nitric oxide synthase mRNA in an ovine model of fetal and placental growth restriction. Am J Obstet Gynecol. 2007;197:420. doi: 10.1016/j.ajog.2007.07.016. e1-5. [DOI] [PubMed] [Google Scholar]
- 20.Marinoni E., Di Iorio R., Lucchini C., Di Netta T., Letizia C., Cosmi E.V. Adrenomedullin and nitric oxide synthase at the maternal-decidual interface in early spontaneous abortion. J Reprod Med. 2004;49:153–161. [PubMed] [Google Scholar]
- 21.Baylis S.A., Strijbos P.J., Sandra A., Russell R.J., Rijhsinghani A., Charles I.G. Temporal expression of inducible nitric oxide synthase in mouse and human placenta. Mol Hum Reprod. 1999;5:277–286. doi: 10.1093/molehr/5.3.277. [DOI] [PubMed] [Google Scholar]
- 22.Takizawa T., Yoshikawa H., Yamada M., Morita H. Expression of nitric oxide synthase isoforms and detection of nitric oxide in rat placenta. Am J Physiol Cell Physiol. 2002;282:CC76762–CC76767. doi: 10.1152/ajpcell.00101.2001. [DOI] [PubMed] [Google Scholar]
- 23.Kwon H., Wu G., Meininger C.J., Bazer F.W., Spencer T.E. Developmental changes in nitric oxide synthesis in the ovine placenta. Biol Reprod. 2004;70:679–686. doi: 10.1095/biolreprod.103.023184. [DOI] [PubMed] [Google Scholar]
- 24.Suzuki T., Ikeda Y., Yoshikawa H., Tanaka K., Morita H., Yamamoto M. Gestational changes in production of NO and expression of NOS mRNA isoforms in the rat placenta. J Vet Med Sci. 2009;71:495–498. doi: 10.1292/jvms.71.495. [DOI] [PubMed] [Google Scholar]
- 25.Al-Hijji J., Andolf E., Laurini R., Batra S. Nitric oxide synthase activity in human trophoblast, term placenta and pregnant myometrium. Reprod Biol Endocrinol. 2003;1:51. doi: 10.1186/1477-7827-1-51. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Myatt L., Eis A.L., Brockman D.E., Kossenjans W., Greer I., Lyall F. Inducible (type II) nitric oxide synthase in human placental villous tissue of normotensive, pre-eclamptic and intrauterine growth-restricted pregnancies. Placenta. 1997;18:261–268. doi: 10.1016/s0143-4004(97)80060-4. [DOI] [PubMed] [Google Scholar]
- 27.Schiessl B., Mylonas I., Hantschmann P., Kuhn C., Schulze S., Kunze S. Expression of endothelial NO synthase, inducible NO synthase, and estrogen receptors alpha and beta in placental tissue of normal, preeclamptic, and intrauterine growth-restricted pregnancies. J Histochem Cytochem. 2005;53:1441–1449. doi: 10.1369/jhc.4A6480.2005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Sheppard C., Shaw C.E., Li Y., Bird I.M., Magness R.R. Endothelium-derived nitric oxide synthase protein expression in ovine placental arteries. Biol Reprod. 2001;64:1494–1499. doi: 10.1095/biolreprod64.5.1494. [DOI] [PubMed] [Google Scholar]
- 29.Galan H.L., Regnault T.R., Le Cras T.D., Tyson R.W., Anthony R.V., Wilkening R.B. Cotyledon and binucleate cell nitric oxide synthase expression in an ovine model of fetal growth restriction. J Appl Physiol. 2001;90:2420–2426. doi: 10.1152/jappl.2001.90.6.2420. [DOI] [PubMed] [Google Scholar]
- 30.Giannubilo S.R., Menegazzi M., Tedeschi E., Bezzeccheri V., Suzuki H., Tranquilli A.L. Doppler analysis and placental nitric oxide synthase expression during fetal growth restriction. J Matern Fetal Neonatal Med. 2008;21:617–622. doi: 10.1080/14767050802214774. [DOI] [PubMed] [Google Scholar]
- 31.Shalaby F., Rossant J., Yamaguchi T.P., Gertsenstein M., Wu X.F., Breitman M.L. Failure of blood-island formation and vasculogenesis in Flk-1-deficient mice. Nature. 1995;376:62–66. doi: 10.1038/376062a0. [DOI] [PubMed] [Google Scholar]
- 32.Parenti A., Morbidelli L., Cui X.L., Douglas J.G., Hood J.D., Granger H.J. Nitric oxide is an upstream signal of vascular endothelial growth factor-induced extracellular signal-regulated kinase1/2 activation in postcapillary endothelium. J Biol Chem. 1998;273:4220–4226. doi: 10.1074/jbc.273.7.4220. [DOI] [PubMed] [Google Scholar]
- 33.Shizukuda Y., Tang S., Yokota R., Ware J.A. Vascular endothelial growth factor–induced endothelial cell migration and proliferation depend on a nitric oxide–mediated decrease in protein kinase C activity. Circ Res. 1999;85:247–256. doi: 10.1161/01.res.85.3.247. [DOI] [PubMed] [Google Scholar]
- 34.Ortiz P.A., Garvin J.L. Cardiovascular and renal control in NOS-deficient mouse models. Am J Physiol Regul Integr Comp Physiol. 2003;284:R628–R638. doi: 10.1152/ajpregu.00401.2002. [DOI] [PubMed] [Google Scholar]
- 35.Tsutsui M., Shimokawa H., Otsuji Y., Ueta Y., Sasaguri Y., Yanagihara N. Nitric oxide synthases and cardiovascular diseases: insights from genetically modified mice. Circ J. 2009;73:986–993. doi: 10.1253/circj.cj-09-0208. [DOI] [PubMed] [Google Scholar]
- 36.Teichert A.M., Scott J.A., Robb G.B., Zhou Y.Q., Zhu S.N., Lem M. Endothelial nitric oxide synthase gene expression during murine embryogenesis: commencement of expression in the embryo occurs with the establishment of a unidirectional circulatory system. Circ Res. 2008;103:24–33. doi: 10.1161/CIRCRESAHA.107.168567. [DOI] [PubMed] [Google Scholar]
- 37.Hefler L.A., Reyes C.A., O’Brien W.E., Gregg A.R. Perinatal development of endothelial nitric oxide synthase-deficient mice. Biol Reprod. 2001;64:666–673. doi: 10.1095/biolreprod64.2.666. [DOI] [PubMed] [Google Scholar]
- 38.Pallares P., Gonzalez-Bulnes A. Intrauterine growth retardation in endothelial nitric oxide synthase-deficient mice is established from early stages of pregnancy. Biol Reprod. 2008;78:1002–1006. doi: 10.1095/biolreprod.107.066159. [DOI] [PubMed] [Google Scholar]
- 39.Jin S.W., Patterson C. The opening act: vasculogenesis and the origins of circulation. Arterioscler Thromb Vasc Biol. 2009;29:623–629. doi: 10.1161/ATVBAHA.107.161539. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Freyer C., Renfree M.B. The mammalian yolk sac placenta. J Exp Zool B Mol Dev Evol. 2009;312:545–554. doi: 10.1002/jez.b.21239. [DOI] [PubMed] [Google Scholar]
- 41.Lux C.T., Yoshimoto M., McGrath K., Conway S.J., Palis J., Yoder M.C. All primitive and definitive hematopoietic progenitor cells emerging before E10 in the mouse embryo are products of the yolk sac. Blood. 2008;111:3435–3438. doi: 10.1182/blood-2007-08-107086. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Nath A.K., Enciso J., Kuniyasu M., Hao X.Y., Madri J.A., Pinter E. Nitric oxide modulates murine yolk sac vasculogenesis and rescues glucose induced vasculopathy. Development. 2004;131:2485–2496. doi: 10.1242/dev.01131. [DOI] [PubMed] [Google Scholar]
- 43.Ribatti D., Nico B., Crivellato E. Morphological and molecular aspects of physiological vascular morphogenesis. Angiogenesis. 2009;12:101–111. doi: 10.1007/s10456-008-9125-1. [DOI] [PubMed] [Google Scholar]
- 44.Han R.N., Stewart D.J. Defective lung vascular development in endothelial nitric oxide synthase-deficient mice. Trends Cardiovasc Med. 2006;16:29–34. doi: 10.1016/j.tcm.2005.11.004. [DOI] [PubMed] [Google Scholar]
- 45.Pipili-Synetos E., Sakkoula E., Maragoudakis M.E. Nitric oxide is involved in the regulation of angiogenesis. Br J Pharmacol. 1993;108:855–857. doi: 10.1111/j.1476-5381.1993.tb13476.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Zhang R., Wang L., Zhang L., Chen J., Zhu Z., Zhang Z. Nitric oxide enhances angiogenesis via the synthesis of vascular endothelial growth factor and cGMP after stroke in the rat. Circ Res. 2003;92:308–313. doi: 10.1161/01.res.0000056757.93432.8c. [DOI] [PubMed] [Google Scholar]
- 47.Ridnour L.A., Isenberg J.S., Espey M.G., Thomas D.D., Roberts D.D., Wink D.A. Nitric oxide regulates angiogenesis through a functional switch involving thrombospondin-1. Proc Natl Acad Sci U S A. 2005;102:13147–13152. doi: 10.1073/pnas.0502979102. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Smith R.S., Jr., Lin K.F., Agata J., Chao L., Chao J. Human endothelial nitric oxide synthase gene delivery promotes angiogenesis in a rat model of hindlimb ischemia. Arterioscler Thromb Vasc Biol. 2002;22:1279–1285. doi: 10.1161/01.atv.0000026613.18742.67. [DOI] [PubMed] [Google Scholar]
- 49.Benest A.V., Stone O.A., Miller W.H., Glover C.P., Uney J.B., Baker A.H. Arteriolar genesis and angiogenesis induced by endothelial nitric oxide synthase overexpression results in a mature vasculature. Arterioscler Thromb Vasc Biol. 2008;28:1462–1468. doi: 10.1161/ATVBAHA.108.169375. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Jadeski L.C., Lala P.K. Nitric oxide synthase inhibition by N(G)-nitro-L-arginine methyl ester inhibits tumor-induced angiogenesis in mammary tumors. Am J Pathol. 1999;155:1381–1390. doi: 10.1016/S0002-9440(10)65240-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Kon K., Fujii S., Kosaka H., Fujiwara T. Nitric oxide synthase inhibition by N(G)-nitro-L-arginine methyl ester retards vascular sprouting in angiogenesis. Microvasc Res. 2003;65:2–8. doi: 10.1016/s0026-2862(02)00011-0. [DOI] [PubMed] [Google Scholar]
- 52.Zhao X., Lu X., Feng Q. Deficiency in endothelial nitric oxide synthase impairs myocardial angiogenesis. Am J Physiol Heart Circ Physiol. 2002;283:H2371–H2378. doi: 10.1152/ajpheart.00383.2002. [DOI] [PubMed] [Google Scholar]
- 53.Balasubramaniam V., Tang J.R., Maxey A., Plopper C.G., Abman S.H. Mild hypoxia impairs alveolarization in the endothelial nitric oxide synthase-deficient mouse. Am J Physiol Lung Cell Mol Physiol. 2003;284:L964–L971. doi: 10.1152/ajplung.00421.2002. [DOI] [PubMed] [Google Scholar]
- 54.Zheng J., Wen Y., Austin J.L., Chen D.B. Exogenous nitric oxide stimulates cell proliferation via activation of a mitogen-activated protein kinase pathway in ovine fetoplacental artery endothelial cells. Biol Reprod. 2006;74:375–378. doi: 10.1095/biolreprod.105.043190. [DOI] [PubMed] [Google Scholar]
- 55.Gien J., Seedorf G.J., Balasubramaniam V., Markham N., Abman S.H. Intrauterine pulmonary hypertension impairs angiogenesis in vitro: role of vascular endothelial growth factor nitric oxide signaling. Am J Respir Crit Care Med. 2007;176:1146–1153. doi: 10.1164/rccm.200705-750OC. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Bustamante S.A., Pang Y., Romero S., Pierce M.R., Voelker C.A., Thompson J.H. Inducible nitric oxide synthase and the regulation of central vessel caliber in the fetal rat. Circulation. 1996;94:1948–1953. doi: 10.1161/01.cir.94.8.1948. [DOI] [PubMed] [Google Scholar]
- 57.Hamik A., Wang B., Jain M.K. Transcriptional regulators of angiogenesis. Arterioscler Thromb Vasc Biol. 2006;26:1936–1947. doi: 10.1161/01.ATV.0000232542.42968.e3. [DOI] [PubMed] [Google Scholar]
- 58.Bussolati B., Dunk C., Grohman M., Kontos C.D., Mason J., Ahmed A. Vascular endothelial growth factor receptor-1 modulates vascular endothelial growth factor-mediated angiogenesis via nitric oxide. Am J Pathol. 2001;159:993–1008. doi: 10.1016/S0002-9440(10)61775-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Kroll J., Waltenberger J. VEGF-A induces expression of eNOS and iNOS in endothelial cells via VEGF receptor-2 (KDR) Biochem Biophys Res Commun. 1998;252:743–746. doi: 10.1006/bbrc.1998.9719. [DOI] [PubMed] [Google Scholar]
- 60.Fukumura D., Gohongi T., Kadambi A., Izumi Y., Ang J., Yun C.O. Predominant role of endothelial nitric oxide synthase in vascular endothelial growth factor-induced angiogenesis and vascular permeability. Proc Natl Acad Sci U S A. 2001;98:2604–2609. doi: 10.1073/pnas.041359198. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Ahmad S., Hewett P.W., Wang P., Al-Ani B., Cudmore M., Fujisawa T. Direct evidence for endothelial vascular endothelial growth factor receptor-1 function in nitric oxide-mediated angiogenesis. Circ Res. 2006;99:715–722. doi: 10.1161/01.RES.0000243989.46006.b9. [DOI] [PubMed] [Google Scholar]
- 62.Cudmore M., Ahmad S., Al-Ani B., Hewett P., Ahmed S., Ahmed A. VEGF-E activates endothelial nitric oxide synthase to induce angiogenesis via cGMP and PKG-independent pathways. Biochem Biophys Res Commun. 2006;345:1275–1282. doi: 10.1016/j.bbrc.2006.04.031. [DOI] [PubMed] [Google Scholar]
- 63.Kawasaki K., Smith R.S., Jr., Hsieh C.M., Sun J., Chao J., Liao J.K. Activation of the phosphatidylinositol 3-kinase/protein kinase Akt pathway mediates nitric oxide-induced endothelial cell migration and angiogenesis. Mol Cell Biol. 2003;23:5726–5737. doi: 10.1128/MCB.23.16.5726-5737.2003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Miao R.Q., Fontana J., Fulton D., Lin M.I., Harrison K.D., Sessa W.C. Dominant-negative Hsp90 reduces VEGF-stimulated nitric oxide release and migration in endothelial cells. Arterioscler Thromb Vasc Biol. 2008;28:105–111. doi: 10.1161/ATVBAHA.107.155499. [DOI] [PubMed] [Google Scholar]
- 65.Murohara T., Witzenbichler B., Spyridopoulos I., Asahara T., Ding B., Sullivan A. Role of endothelial nitric oxide synthase in endothelial cell migration. Arterioscler Thromb Vasc Biol. 1999;19:1156–1161. doi: 10.1161/01.atv.19.5.1156. [DOI] [PubMed] [Google Scholar]
- 66.Lee P.C., Kibbe M.R., Schuchert M.J., Stolz D.B., Watkins S.C., Griffith B.P. Nitric oxide induces angiogenesis and upregulates alpha(v)beta(3) integrin expression on endothelial cells. Microvasc Res. 2000;60:269–280. doi: 10.1006/mvre.2000.2265. [DOI] [PubMed] [Google Scholar]
- 67.López-Rivera E., Lizarbe T.R., Martínez-Moreno M., López-Novoa J.M., Rodríguez-Barbero A., Rodrigo J. Matrix metalloproteinase 13 mediates nitric oxide activation of endothelial cell migration. Proc Natl Acad Sci U S A. 2005;102:3685–3690. doi: 10.1073/pnas.0408217102. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Genís L., Gonzalo P., Tutor A.S., Gálvez B.G., Martínez-Ruiz A., Zaragoza C. Functional interplay between endothelial nitric oxide synthase and membrane type 1 matrix metalloproteinase in migrating endothelial cells. Blood. 2007;110:2916–2923. doi: 10.1182/blood-2007-01-068080. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Lee C.Z., Xue Z., Hao Q., Yang G.Y., Young W.L. Nitric oxide in vascular endothelial growth factor-induced focal angiogenesis and matrix metalloproteinase-9 activity in the mouse brain. Stroke. 2009;40:2879–2881. doi: 10.1161/STROKEAHA.109.552059. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Chen J.X., Lawrence M.L., Cunningham G., Christman B.W., Meyrick B. HSP90 and Akt modulate Ang-1-induced angiogenesis via NO in coronary artery endothelium. J Appl Physiol. 2004;96:612–620. doi: 10.1152/japplphysiol.00728.2003. [DOI] [PubMed] [Google Scholar]
- 71.Urano T., Ito Y., Akao M., Sawa T., Miyata K., Tabata M. Angiopoietin-related growth factor enhances blood flow via activation of the ERK1/2-eNOS-NO pathway in a mouse hind-limb ischemia model. Arterioscler Thromb Vasc Biol. 2008;28:827–834. doi: 10.1161/ATVBAHA.107.149674. [DOI] [PubMed] [Google Scholar]
- 72.Chen J.X., Stinnett A. Ang-1 gene therapy inhibits hypoxia-inducible factor-1alpha (HIF-1alpha)-prolyl-4-hydroxylase-2, stabilizes HIF-1alpha expression, and normalizes immature vasculature in db/db mice. Diabetes. 2008;57:3335–3343. doi: 10.2337/db08-0503. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Dejana E., Tournier-Lasserve E., Weinstein B.M. The control of vascular integrity by endothelial cell junctions: molecular basis and pathological implications. Dev Cell. 2009;16:209–221. doi: 10.1016/j.devcel.2009.01.004. [DOI] [PubMed] [Google Scholar]
- 74.Gavard J. Breaking the VE-cadherin bonds. FEBS Lett. 2009;583:1–6. doi: 10.1016/j.febslet.2008.11.032. [DOI] [PubMed] [Google Scholar]
- 75.González D., Herrera B., Beltrán A., Otero K., Quintero G., Rojas A. Nitric oxide disrupts VE-cadherin complex in murine microvascular endothelial cells. Biochem Biophys Res Commun. 2003;304:113–118. doi: 10.1016/s0006-291x(03)00546-1. [DOI] [PubMed] [Google Scholar]
- 76.Chang C.C., Chang T.Y., Yu C.H., Tsai M.L. Induction of VE-cadherin in rat placental trophoblasts by VEGF through a NO-dependent pathway. Placenta. 2005;26:234–241. doi: 10.1016/j.placenta.2004.06.002. [DOI] [PubMed] [Google Scholar]
- 77.Hama S., Takeichi O., Fujisaki K., Tanabe N., Maeno M., Ochiai K. Nitric oxide attenuates vascular endothelial cadherin-mediated vascular integrity in human chronic inflammation. Clin Exp Immunol. 2008;154:384–390. doi: 10.1111/j.1365-2249.2008.03789.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Yang Z.Z., Tschopp O., Hemmings-Mieszczak M., Feng J., Brodbeck D., Perentes E. Protein kinase B alpha/Akt1 regulates placental development and fetal growth. J Biol Chem. 2003;278:32124–32131. doi: 10.1074/jbc.M302847200. [DOI] [PubMed] [Google Scholar]
- 79.Zacharek A., Chen J., Zhang C., Cui X., Roberts C., Jiang H. Nitric oxide regulates angiopoietin1/Tie2 expression after stroke. Neurosci Lett. 2006;404:28–32. doi: 10.1016/j.neulet.2006.05.027. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Cui X., Chen J., Zacharek A., Roberts C., Yang Y., Chopp M. Nitric oxide donor up-regulation of SDF1/CXCR4 and Ang1/Tie2 promotes neuroblast cell migration after stroke. J Neurosci Res. 2009;87:86–95. doi: 10.1002/jnr.21836. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Daskalakis G., Marinopoulos S., Krielesi V., Papapanagiotou A., Papantoniou N., Mesogitis S. Placental pathology in women with gestational diabetes. Acta Obstet Gynecol Scand. 2008;87:403–407. doi: 10.1080/00016340801908783. [DOI] [PubMed] [Google Scholar]
- 82.Ahmed A., Perkins J. Angiogenesis and intrauterine growth restriction. Baillieres Best Pract Res Clin Obstet Gynaecol. 2000;14:981–998. doi: 10.1053/beog.2000.0139. [DOI] [PubMed] [Google Scholar]
- 83.Helske S., Vuorela P., Carpén O., Hornig C., Weich H., Halmesmäki E. Expression of vascular endothelial growth factor receptors 1, 2 and 3 in placentas from normal and complicated pregnancies. Mol Hum Reprod. 2001;7:205–210. doi: 10.1093/molehr/7.2.205. [DOI] [PubMed] [Google Scholar]
- 84.Ahmad S., Ahmed A. Elevated placental soluble vascular endothelial growth factor receptor-1 inhibits angiogenesis in preeclampsia. Circ Res. 2004;95:884–891. doi: 10.1161/01.RES.0000147365.86159.f5. [DOI] [PubMed] [Google Scholar]
- 85.Chung J.Y., Song Y., Wang Y., Magness R.R., Zheng J. Differential expression of vascular endothelial growth factor (VEGF), endocrine gland derived-VEGF, and VEGF receptors in human placentas from normal and preeclamptic pregnancies. J Clin Endocrinol Metab. 2004;89:2484–2490. doi: 10.1210/jc.2003-031580. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86.Pietro L., Daher S., Rudge M.V., Calderon I.M., Damasceno D.C., Sinzato Y.K. Vascular endothelial growth factor (VEGF) and VEGF-receptor expression in placenta of hyperglycemic pregnant women. Placenta. 2010;31:770–778. doi: 10.1016/j.placenta.2010.07.003. [DOI] [PubMed] [Google Scholar]
- 87.Hagen A.S., Orbus R.J., Wilkening R.B., Regnault T.R., Anthony R.V. Placental expression of angiopoietin-1, angiopoietin-2 and tie-2 during placental development in an ovine model of placental insufficiency-fetal growth restriction. Pediatr Res. 2005;58:1228–1232. doi: 10.1203/01.pdr.0000185266.23265.87. [DOI] [PubMed] [Google Scholar]
- 88.Zhu M.J., Du M., Hess B.W., Means W.J., Nathanielsz P.W., Ford S.P. Maternal nutrient restriction upregulates growth signaling pathways in the cotyledonary artery of cow placentomes. Placenta. 2007;28:361–368. doi: 10.1016/j.placenta.2006.04.005. [DOI] [PubMed] [Google Scholar]
- 89.Blomberg L.A., Schreier L.L., Guthrie H.D., Sample G.L., Vallet J., Caperna T. The effect of intrauterine growth retardation on the expression of developmental factors in porcine placenta subsequent to the initiation of placentation. Placenta. 2010;31:549–552. doi: 10.1016/j.placenta.2010.03.005. [DOI] [PubMed] [Google Scholar]
- 90.Kucuk M., Doymaz F. Placental weight and placental weight-to-birth weight ratio are increased in diet- and exercise-treated gestational diabetes mellitus subjects but not in subjects with one abnormal value on 100-g oral glucose tolerance test. J Diabetes Complications. 2009;23:25–31. doi: 10.1016/j.jdiacomp.2007.04.002. [DOI] [PubMed] [Google Scholar]
- 91.Pustovrh M.C., Jawerbaum A., White V., Capobianco E., Higa R., Martínez N. The role of nitric oxide on matrix metalloproteinase 2 (MMP2) and MMP9 in placenta and fetus from diabetic rats. Reproduction. 2007;134:605–613. doi: 10.1530/REP-06-0267. [DOI] [PubMed] [Google Scholar]
- 92.Sakkoula E., Pipili-Synetos E., Maragoudakis M.E. Involvement of nitric oxide in the inhibition of angiogenesis by interleukin-2. Br J Pharmacol. 1997;122:793–795. doi: 10.1038/sj.bjp.0701436. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93.Ouyang N., Williams J.L., Rigas B. NO-donating aspirin inhibits angiogenesis by suppressing VEGF expression in HT-29 human colon cancer mouse xenografts. Carcinogenesis. 2008;29:1794–1798. doi: 10.1093/carcin/bgn127. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 94.Thomas D.D., Ridnour L.A., Isenberg J.S., Flores-Santana W., Switzer C.H., Donzelli S. The chemical biology of nitric oxide: implications in cellular signaling. Free Radic Biol Med. 2008;45:18–31. doi: 10.1016/j.freeradbiomed.2008.03.020. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95.Rutherford R.A., McCarthy A., Sullivan M.H., Elder M.G., Polak J.M., Wharton J. Nitric oxide synthase in human placenta and umbilical cord from normal, intrauterine growth-retarded and pre-eclamptic pregnancies. Br J Pharmacol. 1995;116:3099–3109. doi: 10.1111/j.1476-5381.1995.tb15111.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96.Lyall F., Greer I.A., Young A., Myatt L. Nitric oxide concentrations are increased in the feto-placental circulation in intrauterine growth restriction. Placenta. 1996;17:165–168. doi: 10.1016/s0143-4004(96)80009-9. [DOI] [PubMed] [Google Scholar]
- 97.von Mandach U., Lauth D., Huch R. Maternal and fetal nitric oxide production in normal and abnormal pregnancy. J Matern Fetal Neonatal Med. 2003;13:22–27. doi: 10.1080/jmf.13.1.22.27. [DOI] [PubMed] [Google Scholar]
- 98.Tikvica A., Kusan Jukić M., Pintarić I., Medić M., Hudicek-Martincić G., Kosec V. Nitric oxide synthesis in placenta is increased in intrauterine growth restriction and fetal hypoxia. Coll Antropol. 2008;32:565–570. [PubMed] [Google Scholar]
- 99.Myatt L. Reactive oxygen and nitrogen species and functional adaptation of the placenta. Placenta. 2010;31:S66–S69. doi: 10.1016/j.placenta.2009.12.021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.Wu C.C., Chao Y.C., Chen C.N., Chien S., Chen Y.C., Chien C.C. Synergism of biochemical and mechanical stimuli in the differentiation of human placenta-derived multipotent cells into endothelial cells. J Biomech. 2008;41:813–821. doi: 10.1016/j.jbiomech.2007.11.008. [DOI] [PubMed] [Google Scholar]
- 101.Obi S., Yamamoto K., Shimizu N., Kumagaya S., Masumura T., Sokabe T. Fluid shear stress induces arterial differentiation of endothelial progenitor cells. J Appl Physiol. 2009;106:203–211. doi: 10.1152/japplphysiol.00197.2008. [DOI] [PubMed] [Google Scholar]
- 102.You D., Waeckel L., Ebrahimian T.G., Blanc-Brude O., Foubert P., Barateau V. Increase in vascular permeability and vasodilation are critical for proangiogenic effects of stem cell therapy. Circulation. 2006;114:328–338. doi: 10.1161/CIRCULATIONAHA.105.589937. [DOI] [PubMed] [Google Scholar]
- 103.Wieczorek K.M., Brewer A.S., Myatt L. Shear stress may stimulate release and action of nitric oxide in the human fetal-placental vasculature. Am J Obstet Gynecol. 1995;173:708–713. doi: 10.1016/0002-9378(95)90327-5. [DOI] [PubMed] [Google Scholar]
- 104.Baum O., Da Silva-Azevedo L., Willerding G., Wöckel A., Planitzer G., Gossrau R. Endothelial NOS is main mediator for shear stress-dependent angiogenesis in skeletal muscle after prazosin administration. Am J Physiol Heart Circ Physiol. 2004;287:H2300–H2308. doi: 10.1152/ajpheart.00065.2004. [DOI] [PubMed] [Google Scholar]
- 105.Cai W.J., Kocsis E., Luo X., Schaper W., Schaper J. Expression of endothelial nitric oxide synthase in the vascular wall during arteriogenesis. Mol Cell Biochem. 2004;264:193–200. doi: 10.1023/b:mcbi.0000044388.27953.a0. [DOI] [PubMed] [Google Scholar]
- 106.Shen T.L., Park A.Y., Alcaraz A., Peng X., Jang I., Koni P. Conditional knockout of focal adhesion kinase in endothelial cells reveals its role in angiogenesis and vascular development in late embryogenesis. J Cell Biol. 2005;169:941–952. doi: 10.1083/jcb.200411155. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 107.Sutton M.S., Theard M.A., Bhatia S.J., Plappert T., Saltzman D.H., Doubilet P. Changes in placental blood flow in the normal human fetus with gestational age. Pediatr Res. 1990;28:383–387. doi: 10.1203/00006450-199010000-00016. [DOI] [PubMed] [Google Scholar]
- 108.Ohneda O., Nagano M., Fujii-Kuriyama Y. Role of hypoxia-inducible factor-2alpha in endothelial development and hematopoiesis. Methods Enzymol. 2007;435:199–218. doi: 10.1016/S0076-6879(07)35011-8. [DOI] [PubMed] [Google Scholar]
- 109.Fong G.H. Mechanisms of adaptive angiogenesis to tissue hypoxia. Angiogenesis. 2008;11:121–140. doi: 10.1007/s10456-008-9107-3. [DOI] [PubMed] [Google Scholar]
- 110.Hendrix N., Berghella V. Non-placental causes of intrauterine growth restriction. Semin Perinatol. 2008;32:161–165. doi: 10.1053/j.semperi.2008.02.004. [DOI] [PubMed] [Google Scholar]
- 111.Takeda K., Ho V.C., Takeda H., Duan L.J., Nagy A., Fong G.H. Placental but not heart defects are associated with elevated hypoxia-inducible factor alpha levels in mice lacking prolyl hydroxylase domain protein 2. Mol Cell Biol. 2006;26:8336–8346. doi: 10.1128/MCB.00425-06. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 112.Stempien-Otero A., Karsan A., Cornejo C.J., Xiang H., Eunson T., Morrison R.S. Mechanisms of hypoxia-induced endothelial cell death. Role of p53 in apoptosis. J Biol Chem. 1999;274:8039–8045. doi: 10.1074/jbc.274.12.8039. [DOI] [PubMed] [Google Scholar]
- 113.Matsushita H., Morishita R., Nata T., Aoki M., Nakagami H., Taniyama Y. Hypoxia-induced endothelial apoptosis through nuclear factor-kappaB (NF-kappaB)-mediated bcl-2 suppression: in vivo evidence of the importance of NF-kappaB in endothelial cell regulation. Circ Res. 2000;86:974–981. doi: 10.1161/01.res.86.9.974. [DOI] [PubMed] [Google Scholar]
- 114.Arnet U.A., McMillan A., Dinerman J.L., Ballermann B., Lowenstein C.J. Regulation of endothelial nitric-oxide synthase during hypoxia. J Biol Chem. 1996;271:15069–15073. doi: 10.1074/jbc.271.25.15069. [DOI] [PubMed] [Google Scholar]
- 115.Coulet F., Nadaud S., Agrapart M., Soubrier F. Identification of hypoxia-response element in the human endothelial nitric-oxide synthase gene promoter. J Biol Chem. 2003;278:46230–46234. doi: 10.1074/jbc.M305420200. [DOI] [PubMed] [Google Scholar]
- 116.Dong Y., Thompson L.P. Differential expression of endothelial nitric oxide synthase in coronary and cardiac tissue in hypoxic fetal guinea pig hearts. J Soc Gynecol Investig. 2006;13:483–490. doi: 10.1016/j.jsgi.2006.06.005. [DOI] [PubMed] [Google Scholar]
- 117.Casanello P., Torres A., Sanhueza F., González M., Farías M., Gallardo V. Equilibrative nucleoside transporter 1 expression is downregulated by hypoxia in human umbilical vein endothelium. Circ Res. 2005;97:16–24. doi: 10.1161/01.RES.0000172568.49367.f8. [DOI] [PubMed] [Google Scholar]
- 118.Casanello P., Krause B., Torres E., Gallardo V., González M., Prieto C. Reduced l-arginine transport and nitric oxide synthesis in human umbilical vein endothelial cells from intrauterine growth restriction pregnancies is not further altered by hypoxia. Placenta. 2009;30:625–633. doi: 10.1016/j.placenta.2009.04.010. [DOI] [PubMed] [Google Scholar]
- 119.Fish J.E., Yan M.S., Matouk C.C., St Bernard R., Ho J.J., Gavryushova A. Hypoxic repression of endothelial nitric-oxide synthase transcription is coupled with eviction of promoter histones. J Biol Chem. 2010;285:810–826. doi: 10.1074/jbc.M109.067868. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 120.Kasuno K., Takabuchi S., Fukuda K., Kizaka-Kondoh S., Yodoi J., Adachi T. Nitric oxide induces hypoxia-inducible factor 1 activation that is dependent on MAPK and phosphatidylinositol 3-kinase signaling. J Biol Chem. 2004;279:2550–2558. doi: 10.1074/jbc.M308197200. [DOI] [PubMed] [Google Scholar]
- 121.Berchner-Pfannschmidt U., Yamac H., Trinidad B., Fandrey J. Nitric oxide modulates oxygen sensing by hypoxia-inducible factor 1-dependent induction of prolyl hydroxylase 2. J Biol Chem. 2007;282:1788–1796. doi: 10.1074/jbc.M607065200. [DOI] [PubMed] [Google Scholar]
- 122.Berchner-Pfannschmidt U., Tug S., Trinidad B., Oehme F., Yamac H., Wotzlaw C. Nuclear oxygen sensing: induction of endogenous prolyl-hydroxylase 2 activity by hypoxia and nitric oxide. J Biol Chem. 2008;283:31745–31753. doi: 10.1074/jbc.M804390200. [DOI] [PubMed] [Google Scholar]
- 123.Hagen T., Taylor C.T., Lam F., Moncada S. Redistribution of intracellular oxygen in hypoxia by nitric oxide: effect on HIF1alpha. Science. 2003;302:1975–1978. doi: 10.1126/science.1088805. [DOI] [PubMed] [Google Scholar]
- 124.Cooper C.E., Giulivi C. Nitric oxide regulation of mitochondrial oxygen consumption II: molecular mechanism and tissue physiology. Am J Physiol Cell Physiol. 2007;292:C1993–C2003. doi: 10.1152/ajpcell.00310.2006. [DOI] [PubMed] [Google Scholar]
- 125.Dokras A., Coffin J., Field L., Frakes A., Lee H., Madan A. Epigenetic regulation of maspin expression in the human placenta. Mol Hum Reprod. 2006;12:611–617. doi: 10.1093/molehr/gal074. [DOI] [PubMed] [Google Scholar]
- 126.Fowden A.L., Sibley C., Reik W., Constancia M. Imprinted genes, placental development and fetal growth. Horm Res. 2006;65:50–58. doi: 10.1159/000091506. [DOI] [PubMed] [Google Scholar]
- 127.McMinn J., Wei M., Sadovsky Y., Thaker H.M., Tycko B. Imprinting of PEG1/MEST isoform 2 in human placenta. Placenta. 2006;27:119–126. doi: 10.1016/j.placenta.2004.12.003. [DOI] [PubMed] [Google Scholar]
- 128.Kimura A.P., Sizova D., Handwerger S., Cooke N.E., Liebhaber S.A. Epigenetic activation of the human growth hormone gene cluster during placental cytotrophoblast differentiation. Mol Cell Biol. 2007;27:6555–6568. doi: 10.1128/MCB.00273-07. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 129.McMinn J., Wei M., Schupf N., Cusmai J., Johnson E.B., Smith A.C. Unbalanced placental expression of imprinted genes in human intrauterine growth restriction. Placenta. 2006;27:540–549. doi: 10.1016/j.placenta.2005.07.004. [DOI] [PubMed] [Google Scholar]
- 130.Chelbi S.T., Mondon F., Jammes H., Buffat C., Mignot T.M., Tost J. Expressional and epigenetic alterations of placental serine protease inhibitors: SERPINA3 is a potential marker of preeclampsia. Hypertension. 2007;49:76–83. doi: 10.1161/01.HYP.0000250831.52876.cb. [DOI] [PubMed] [Google Scholar]
- 131.Guo L., Choufani S., Ferreira J., Smith A., Chitayat D., Shuman C. Altered gene expression and methylation of the human chromosome 11 imprinted region in small for gestational age (SGA) placentae. Dev Biol. 2008;320:79–91. doi: 10.1016/j.ydbio.2008.04.025. [DOI] [PubMed] [Google Scholar]
- 132.Krause B., Sobrevia L., Casanello P. Epigenetics: new concepts of old phenomena in vascular physiology. Curr Vasc Pharmacol. 2009;7:513–520. doi: 10.2174/157016109789043883. [DOI] [PubMed] [Google Scholar]
- 133.Shirodkar A.V., Marsden P.A. Epigenetics in cardiovascular disease. Curr Opin Cardiol. 2011;26:209–215. doi: 10.1097/HCO.0b013e328345986e. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 134.Zeng L., Xiao Q., Margariti A., Zhang Z., Zampetaki A., Patel S. HDAC3 is crucial in shear- and VEGF-induced stem cell differentiation toward endothelial cells. J Cell Biol. 2006;174:1059–1069. doi: 10.1083/jcb.200605113. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 135.Deroanne C.F., Bonjean K., Servotte S., Devy L., Colige A., Clausse N. Histone deacetylases inhibitors as anti-angiogenic agents altering vascular endothelial growth factor signaling. Oncogene. 2002;21:427–436. doi: 10.1038/sj.onc.1205108. [DOI] [PubMed] [Google Scholar]
- 136.Diehl F., Rössig L., Zeiher A.M., Dimmeler S., Urbich C. The histone methyltransferase MLL is an upstream regulator of endothelial-cell sprout formation. Blood. 2007;109:1472–1478. doi: 10.1182/blood-2006-08-039651. [DOI] [PubMed] [Google Scholar]
- 137.Kim M.S., Kwon H.J., Lee Y.M., Baek J.H., Jang J.E., Lee S.W. Histone deacetylases induce angiogenesis by negative regulation of tumor suppressor genes. Nat Med. 2001;7:437–443. doi: 10.1038/86507. [DOI] [PubMed] [Google Scholar]
- 138.Rössig L., Li H., Fisslthaler B., Urbich C., Fleming I., Förstermann U. Inhibitors of histone deacetylation downregulate the expression of endothelial nitric oxide synthase and compromise endothelial cell function in vasorelaxation and angiogenesis. Circ Res. 2002;91:837–844. doi: 10.1161/01.res.0000037983.07158.b1. [DOI] [PubMed] [Google Scholar]
- 139.Fish J.E., Matouk C.C., Rachlis A., Lin S., Tai S.C., D’Abreo C. The expression of endothelial nitric-oxide synthase is controlled by a cell-specific histone code. J Biol Chem. 2005;280:24824–24838. doi: 10.1074/jbc.M502115200. [DOI] [PubMed] [Google Scholar]
- 140.Illi B., Colussi C., Grasselli A., Farsetti A., Capogrossi M.C., Gaetano C. NO sparks off chromatin: tales of a multifaceted epigenetic regulator. Pharmacol Ther. 2009;123:344–352. doi: 10.1016/j.pharmthera.2009.05.003. [DOI] [PubMed] [Google Scholar]
- 141.Reilly R.D., Russell P.T. Neurohistochemical evidence supporting an absence of adrenergic and cholinergic innervation in the human placenta and umbilical cord. Anat Rec. 1977;188:277–286. doi: 10.1002/ar.1091880302. [DOI] [PubMed] [Google Scholar]
- 142.Van de Voorde J., Vanderstichele H., Leusen I. Release of endothelium-derived relaxing factor from human umbilical vessels. Circ Res. 1987;60:517–522. doi: 10.1161/01.res.60.4.517. [DOI] [PubMed] [Google Scholar]
- 143.Read M.A., Boura A.L., Walters W.A. Vascular actions of purines in the foetal circulation of the human placenta. Br J Pharmacol. 1993;110:454–460. doi: 10.1111/j.1476-5381.1993.tb13832.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 144.Chaudhuri G., Cuevas J., Buga G.M., Ignarro L.J. NO is more important than PGI2 in maintaining low vascular tone in feto-placental vessels. Am J Physiol Heart Circ Physiol. 1993;265:H2036–H2043. doi: 10.1152/ajpheart.1993.265.6.H2036. [DOI] [PubMed] [Google Scholar]
- 145.Izumi H., Makino Y., Mohtai H., Shirakawa K., Garfield R.E. Comparison of nitric oxide and prostacyclin in endothelium-dependent vasorelaxation of human umbilical artery at midgestation. Am J Obstet Gynecol. 1996;175:375–381. doi: 10.1016/s0002-9378(96)70149-7. [DOI] [PubMed] [Google Scholar]
- 146.Bamberger A.M., Koglin M., Kempfert J., Löning T., Scholz H., Behrends S. Expression and tissue localization of soluble guanylyl cyclase in the human placenta using novel antibodies directed against the alpha(2) subunit. J Clin Endocrinol Metab. 2001;86:909–912. doi: 10.1210/jcem.86.2.7409. [DOI] [PubMed] [Google Scholar]
- 147.Santos-Silva A.J., Cairrão E., Morgado M., Alvarez E., Verde I. PDE4 and PDE5 regulate cyclic nucleotides relaxing effects in human umbilical arteries. Eur J Pharmacol. 2008;582:102–109. doi: 10.1016/j.ejphar.2007.12.017. [DOI] [PubMed] [Google Scholar]
- 148.Maharaj C.H., O’Toole D., Lynch T., Carney J., Jarman J., Higgins B.D. Effects and mechanisms of action of sildenafil citrate in human chorionic arteries. Reprod Biol Endocrinol. 2009;7:34. doi: 10.1186/1477-7827-7-34. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 149.Sand A.E., Andersson E., Fried G. Effects of nitric oxide donors and inhibitors of nitric oxide signalling on endothelin- and serotonin-induced contractions in human placental arteries. Acta Physiol Scand. 2002;174:217–223. doi: 10.1046/j.1365-201x.2002.00939.x. [DOI] [PubMed] [Google Scholar]
- 150.Lovren F., Triggle C. Nitric oxide and sodium nitroprusside-induced relaxation of the human umbilical artery. Br J Pharmacol. 2000;131:521–529. doi: 10.1038/sj.bjp.0703588. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 151.Sand A., Andersson E., Fried G. Nitric oxide donors mediate vasodilation in human placental arteries partly through a direct effect on potassium channels. Placenta. 2006;27:181–190. doi: 10.1016/j.placenta.2004.12.013. [DOI] [PubMed] [Google Scholar]
- 152.Sobrevia L., Yudilevich D.L., Mann G.E. Activation of A2-purinoceptors by adenosine stimulates L-arginine transport (system y+) and nitric oxide synthesis in human fetal endothelial cells. J Physiol. 1997;499:135–140. doi: 10.1113/jphysiol.1997.sp021916. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 153.Dong Y.L., Vegiraju S., Chauhan M., Gangula P.R., Hankins G.D., Goodrum L. Involvement of calcitonin gene-related peptide in control of human fetoplacental vascular tone. Am J Physiol Heart Circ Physiol. 2004;286:H230–H239. doi: 10.1152/ajpheart.00140.2003. [DOI] [PubMed] [Google Scholar]
- 154.Thakor A.S., Giussani D.A. Role of nitric oxide in mediating in vivo vascular responses to calcitonin gene-related peptide in essential and peripheral circulations in the fetus. Circulation. 2005;112:2510–2516. doi: 10.1161/CIRCULATIONAHA.105.562546. [DOI] [PubMed] [Google Scholar]
- 155.Sprague B., Chesler N.C., Magness R.R. Shear stress regulation of nitric oxide production in uterine and placental artery endothelial cells: experimental studies and hemodynamic models of shear stresses on endothelial cells. Int J Dev Biol. 2010;54:331–339. doi: 10.1387/ijdb.082832bs. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 156.Li Y., Zheng J., Bird I.M., Magness R.R. Mechanisms of shear stress-induced endothelial nitric-oxide synthase phosphorylation and expression in ovine fetoplacental artery endothelial cells. Biol Reprod. 2004;70:785–796. doi: 10.1095/biolreprod.103.022293. [DOI] [PubMed] [Google Scholar]
- 157.Li Y., Zheng J., Bird I.M., Magness R.R. Effects of pulsatile shear stress on nitric oxide production and endothelial cell nitric oxide synthase expression by ovine fetoplacental artery endothelial cells. Biol Reprod. 2003;69:1053–1059. doi: 10.1095/biolreprod.102.013474. [DOI] [PubMed] [Google Scholar]
- 158.Read M.A., Boura A.L., Walters W.A. Effects of variation in oxygen tension on responses of the human fetoplacental vasculature to vasoactive agents in vitro. Placenta. 1995;16:667–678. doi: 10.1016/0143-4004(95)90011-x. [DOI] [PubMed] [Google Scholar]
- 159.Wareing M., Crocker I.P., Warren A.Y., Taggart M.J., Baker P.N. Characterization of small arteries isolated from the human placental chorionic plate. Placenta. 2002;23:400–409. doi: 10.1053/plac.2002.0825. [DOI] [PubMed] [Google Scholar]
- 160.Wareing M., Greenwood S.L., Baker P.N. Reactivity of human placental chorionic plate vessels is modified by level of oxygenation: differences between arteries and veins. Placenta. 2006;27:42–48. doi: 10.1016/j.placenta.2004.11.008. [DOI] [PubMed] [Google Scholar]
- 161.Coumans A.B., Garnier Y., Supçun S., Jensen A., Hasaart T.H., Berger R. The role of nitric oxide on fetal cardiovascular control during normoxia and acute hypoxia in 0.75 gestation sheep. J Soc Gynecol Investig. 2003;10:275–282. doi: 10.1016/s1071-5576(03)00085-6. [DOI] [PubMed] [Google Scholar]
- 162.Byrne B.M., Howard R.B., Morrow R.J., Whiteley K.J., Adamson S.L. Role of the L-arginine nitric oxide pathway in hypoxic fetoplacental vasoconstriction. Placenta. 1997;18:627–634. doi: 10.1016/s0143-4004(97)90003-5. [DOI] [PubMed] [Google Scholar]
- 163.Mildenberger E., Biesel B., Siegel G., Versmold H.T. Nitric oxide and endothelin in oxygen-dependent regulation of vascular tone of human umbilical vein. Am J Physiol Heart Circ Physiol. 2003;285:H1730–H1737. doi: 10.1152/ajpheart.00938.2002. [DOI] [PubMed] [Google Scholar]
- 164.Leung S.W., Quan A., Lao T.T., Man R.Y. Efficacy of different vasodilators on human umbilical arterial smooth muscle under normal and reduced oxygen conditions. Early Hum Dev. 2006;82:457–462. doi: 10.1016/j.earlhumdev.2005.11.009. [DOI] [PubMed] [Google Scholar]
- 165.Krebs C., Macara L.M., Leiser R., Bowman A.W., Greer I.A., Kingdom J.C. Intrauterine growth restriction with absent end-diastolic flow velocity in the umbilical artery is associated with maldevelopment of the placental terminal villous tree. Am J Obstet Gynecol. 1996;175:1534–1542. doi: 10.1016/s0002-9378(96)70103-5. [DOI] [PubMed] [Google Scholar]
- 166.Bruch J.F., Sibony O., Benali K., Challier J.C., Blot P., Nessmann C. Computerized microscope morphometry of umbilical vessels from pregnancies with intrauterine growth retardation and abnormal umbilical artery Doppler. Hum Pathol. 1997;28:1139–1145. doi: 10.1016/s0046-8177(97)90251-3. [DOI] [PubMed] [Google Scholar]
- 167.Raio L., Ghezzi F., Di Naro E., Duwe D.G., Cromi A., Schneider H. Umbilical cord morphologic characteristics and umbilical artery Doppler parameters in intrauterine growth-restricted fetuses. J Ultrasound Med. 2003;22:1341–1347. doi: 10.7863/jum.2003.22.12.1341. [DOI] [PubMed] [Google Scholar]
- 168.Szukiewicz D., Szewczyk G., Watroba M., Kurowska E., Maslinski S. Isolated placental vessel response to vascular endothelial growth factor and placenta growth factor in normal and growth-restricted pregnancy. Gynecol Obstet Invest. 2005;59:102–107. doi: 10.1159/000082622. [DOI] [PubMed] [Google Scholar]
- 169.Wareing M., Greenwood S.L., Fyfe G.K., Baker P.N. Reactivity of human placental chorionic plate vessels from pregnancies complicated by intrauterine growth restriction (IUGR) Biol Reprod. 2006;75:518–523. doi: 10.1095/biolreprod.106.051607. [DOI] [PubMed] [Google Scholar]
- 170.Dong Y.L., Green K.E., Vegiragu S., Hankins G.D., Martin E., Chauhan M. Evidence for decreased calcitonin gene-related peptide (CGRP) receptors and compromised responsiveness to CGRP of fetoplacental vessels in preeclamptic pregnancies. J Clin Endocrinol Metab. 2005;90:2336–2343. doi: 10.1210/jc.2004-1481. [DOI] [PubMed] [Google Scholar]
- 171.Mills T.A., Wareing M., Bugg G.J., Greenwood S.L., Baker P.N. Chorionic plate artery function and Doppler indices in normal pregnancy and intrauterine growth restriction. Eur J Clin Invest. 2005;35:758–764. doi: 10.1111/j.1365-2362.2005.01577.x. [DOI] [PubMed] [Google Scholar]
- 172.Sweeney M., Wareing M., Mills T.A., Baker P.N., Taggart M.J. Characterisation of tone oscillations in placental and myometrial arteries from normal pregnancies and those complicated by pre-eclampsia and growth restriction. Placenta. 2008;29:356–365. doi: 10.1016/j.placenta.2008.01.007. [DOI] [PubMed] [Google Scholar]
- 173.Noris M., Todeschini M., Cassis P., Pasta F., Cappellini A., Bonazzola S. L-arginine depletion in preeclampsia orients nitric oxide synthase toward oxidant species. Hypertension. 2004;43:614–622. doi: 10.1161/01.HYP.0000116220.39793.c9. [DOI] [PubMed] [Google Scholar]
- 174.Prieto C.P., Krause B., Sobrevia L., Casanello P. Hypoxia-reduced eNOS activity could be explained by higher arginase II activity and cellular redistribution in human umbilical vein endothelial cells. Reprod Sci. 2010;17:298A. doi: 10.1016/j.placenta.2011.09.003. [DOI] [PubMed] [Google Scholar]
- 175.Wang Y., Gu Y., Zhang Y., Lewis D.F. Evidence of endothelial dysfunction in preeclampsia: decreased endothelial nitric oxide synthase expression is associated with increased cell permeability in endothelial cells from preeclampsia. Am J Obstet Gynecol. 2004;190:817–824. doi: 10.1016/j.ajog.2003.09.049. [DOI] [PubMed] [Google Scholar]
- 176.Wang X., Wang J., Trudinger B. Gene expression of nitric oxide synthase by human umbilical vein endothelial cells: the effect of fetal plasma from pregnancy with umbilical placental vascular disease. BJOG. 2003;110:53–58. [PubMed] [Google Scholar]
- 177.Jacobi J., Kristal B., Chezar J., Shaul S.M., Sela S. Exogenous superoxide mediates pro-oxidative, proinflammatory, and procoagulatory changes in primary endothelial cell cultures. Free Radic Biol Med. 2005;39:1238–1248. doi: 10.1016/j.freeradbiomed.2005.06.010. [DOI] [PubMed] [Google Scholar]
- 178.Mattiussi S., Lazzari C., Truffa S., Antonini A., Soddu S., Capogrossi M.C. Homeodomain interacting protein kinase 2 activation compromises endothelial cell response to laminar flow: protective role of p21(waf1, cip1, sdi1) PLoS One. 2009;4:e6603. doi: 10.1371/journal.pone.0006603. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 179.Hayashi T., Sumi D., Juliet P.A., Matsui-Hirai H., Asai-Tanaka Y., Kano H. Gene transfer of endothelial NO synthase, but not eNOS plus inducible NOS, regressed atherosclerosis in rabbits. Cardiovasc Res. 2004;61:339–351. doi: 10.1016/j.cardiores.2003.09.027. [DOI] [PubMed] [Google Scholar]
- 180.Gunnett C.A., Lund D.D., McDowell A.K., Faraci F.M., Heistad D.D. Mechanisms of inducible nitric oxide synthase-mediated vascular dysfunction. Arterioscler Thromb Vasc Biol. 2005;25:1617–1622. doi: 10.1161/01.ATV.0000172626.00296.ba. [DOI] [PubMed] [Google Scholar]
- 181.Nagareddy P.R., Xia Z., McNeill J.H., MacLeod K.M. Increased expression of iNOS is associated with endothelial dysfunction and impaired pressor responsiveness in streptozotocin-induced diabetes. Am J Physiol Heart Circ Physiol. 2005;289:H2144–H2152. doi: 10.1152/ajpheart.00591.2005. [DOI] [PubMed] [Google Scholar]
- 182.Tanaka J., Qiang L., Banks A.S., Welch C.L., Matsumoto M., Kitamura T. Foxo1 links hyperglycemia to LDL oxidation and endothelial nitric oxide synthase dysfunction in vascular endothelial cells. Diabetes. 2009;58:2344–2354. doi: 10.2337/db09-0167. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 183.Kim J.H., Bugaj L.J., Oh Y.J., Bivalacqua T.J., Ryoo S., Soucy K.G. Arginase inhibition restores NOS coupling and reverses endothelial dysfunction and vascular stiffness in old rats. J Appl Physiol. 2009;107:1249–1257. doi: 10.1152/japplphysiol.91393.2008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 184.Zheng J., Li Y., Weiss A.R., Bird I.M., Magness R.R. Expression of endothelial and inducible nitric oxide synthases and nitric oxide production in ovine placental and uterine tissues during late pregnancy. Placenta. 2000;21:516–524. doi: 10.1053/plac.1999.0504. [DOI] [PubMed] [Google Scholar]
- 185.Rodríguez-Crespo I., Ortiz de Montellano P.R. Human endothelial nitric oxide synthase: expression in Escherichia coli, coexpression with calmodulin, and characterization. Arch Biochem Biophys. 1996;336:151–156. doi: 10.1006/abbi.1996.0543. [DOI] [PubMed] [Google Scholar]
- 186.Gerber N.C., Nishida C.R., Ortiz de Montellano P.R. Characterization of human liver inducible nitric oxide synthase expressed in Escherichia coli. Arch Biochem Biophys. 1997;343:249–253. doi: 10.1006/abbi.1997.0187. [DOI] [PubMed] [Google Scholar]
- 187.Abu-Soud H.M., Ichimori K., Presta A., Stuehr D.J. Electron transfer, oxygen binding, and nitric oxide feedback inhibition in endothelial nitric-oxide synthase. J Biol Chem. 2000;275:17349–17355. doi: 10.1074/jbc.M000050200. [DOI] [PubMed] [Google Scholar]
- 188.Abu-Soud H.M., Ichimori K., Nakazawa H., Stuehr D.J. Regulation of inducible nitric oxide synthase by self-generated NO. Biochemistry. 2001;40:6876–6881. doi: 10.1021/bi010066m. [DOI] [PubMed] [Google Scholar]
- 189.Santolini J., Meade A.L., Stuehr D.J. Differences in three kinetic parameters underpin the unique catalytic profiles of nitric-oxide synthases I, II, and III. J Biol Chem. 2001;276:48887–48898. doi: 10.1074/jbc.M108666200. [DOI] [PubMed] [Google Scholar]
- 190.Schönfelder G., Fuhr N., Hadzidiakos D., John M., Hopp H., Paul M. Preeclampsia is associated with loss of neuronal nitric oxide synthase expression in vascular smooth muscle cells of the human umbilical cord. Histopathology. 2004;44:116–128. doi: 10.1111/j.1365-2559.2004.01806.x. [DOI] [PubMed] [Google Scholar]