Abstract
Objective
To estimate continuation rates, complications, and psychiatric hospitalizations among women with bipolar disorder using levonorgestrel-releasing or copper-containing (CuT380A) intrauterine devices (IUD), as compared with those using depot medroxyprogesterone acetate (DMPA) or sterilization for birth control.
Methods
Data for this cohort study were obtained from a nationwide health insurance claims database on an employed, commercially insured population. Women aged 18–44 with a prior diagnosis of bipolar disorder (n = 849), who were using the levonorgestrel intrauterine system, CuT380A, DMPA, or sterilization were evaluated. Outcomes included continuation rates over a 12-month interval, infectious and noninfectious complications, and hospitalizations for bipolar disorder or depression.
Results
Women using an IUD were more likely than those using DMPA to continue the method for at least 12 months (CuT380A, 86%; levonorgestrel intrauterine system, 87%). In comparison, only 31% of those who initiated DMPA received three more injections during the following year (p<0.0001). No significant differences were noted in infectious or noninfectious complications by contraceptive type. Finally, no differences were observed in the number of hospitalizations for bipolar disorder or depression among the four contraceptive groups.
Conclusions
More women with bipolar disorder continued using IUDs at one year than women using DMPA. The rates of complications and psychiatric hospitalizations were not different among women using an IUD, DMPA, or sterilization.
Introduction
Bipolar disorder spectrum occurs in 4.4%, or 9 million, of women in the US according to the first lifetime prevalence estimates from the 2007 National Comorbidity Survey Replication (NCS-R) (1). Age of onset ranges from 18 to 22 years, with women of childbearing age demonstrating the highest prevalence during a 12-month period: ages 18–29, 4.7%; ages 30–44, 3.5%) (2)(3). Women with bipolar disorder are at high risk for unintended pregnancies, as a result of multiple issues including sexual risk behavior associated with impulsivity of mania, not using contraception, or using ineffective contraception (4)(5)(6). They are also more likely to have had more than one partner (7)(8) and to engage in sex trading compared with the general U.S. population (4). Consistent with these high risk sexual behaviors, a survey of 136 women with bipolar disorder reported that only 58.8% were using contraception. The most common methods were oral contraceptives (OCP) (16.2%) and tubal ligation (16.3%). Other methods included condoms (12.8%), intrauterine contraception (4.4%) and partner vasectomy (2.8%) (5).
Recommending appropriate contraceptives for patients with bipolar disorder is challenging because of certain issues related to this population. First, many women with bipolar disorder may be treated with mood stabilizers including antiepileptics which can affect drug levels of OCP, thus, impairing contraceptive efficacy (9)(10)(11)(12). In addition, some evidence indicates that OCP may decrease levels of certain antieplileptics (11)(12). The second issue facing this population is non compliance, which would indicate long acting reversible contraceptives (LARC), such as an injectable depot medroxyprogesterone acetate (DMPA) and intrauterine devices (IUD), to be more desirable options than oral or barrier methods. However, because of high risk sexual behavior associated impulsivity, women with bipolar disorder may be at higher risk for sexually transmitted infections (13). As a result, some clinicians may not recommend IUDs to this population.
Another challenge in providing contraceptives to patients with bipolar disorder is the lack of published studies that evaluate complications of different methods in this population. The purpose of this study was to estimate complications in women with bipolar disorder who used an IUD compared with women who used DMPA or sterilization. Our hypothesis was that women using IUDs would have similar rates of complications compared with women using DMPA or sterilization. Specifically, we used medical claims data to investigate complications and psychiatric hospitalizations among women using levonorgestrel-releasing (LNG-IUS) and copper (CuT380A) IUDs compared with women using DMPA or sterilization.
Methods
Data for this cohort study were obtained from a nationwide U.S. health claims database, consisting of electronic health insurance claims from an employed, commercially insured population with dependents. A number of validation studies have documented use of these data for studies of health care utilization and outcomes (14)(15)(16). Medical claims from 2001 to 2006 were evaluated. All patient identifiers were removed prior to data being made available for research purposes. The University of Texas Medical Branch institutional review board granted an exemption for this protocol.
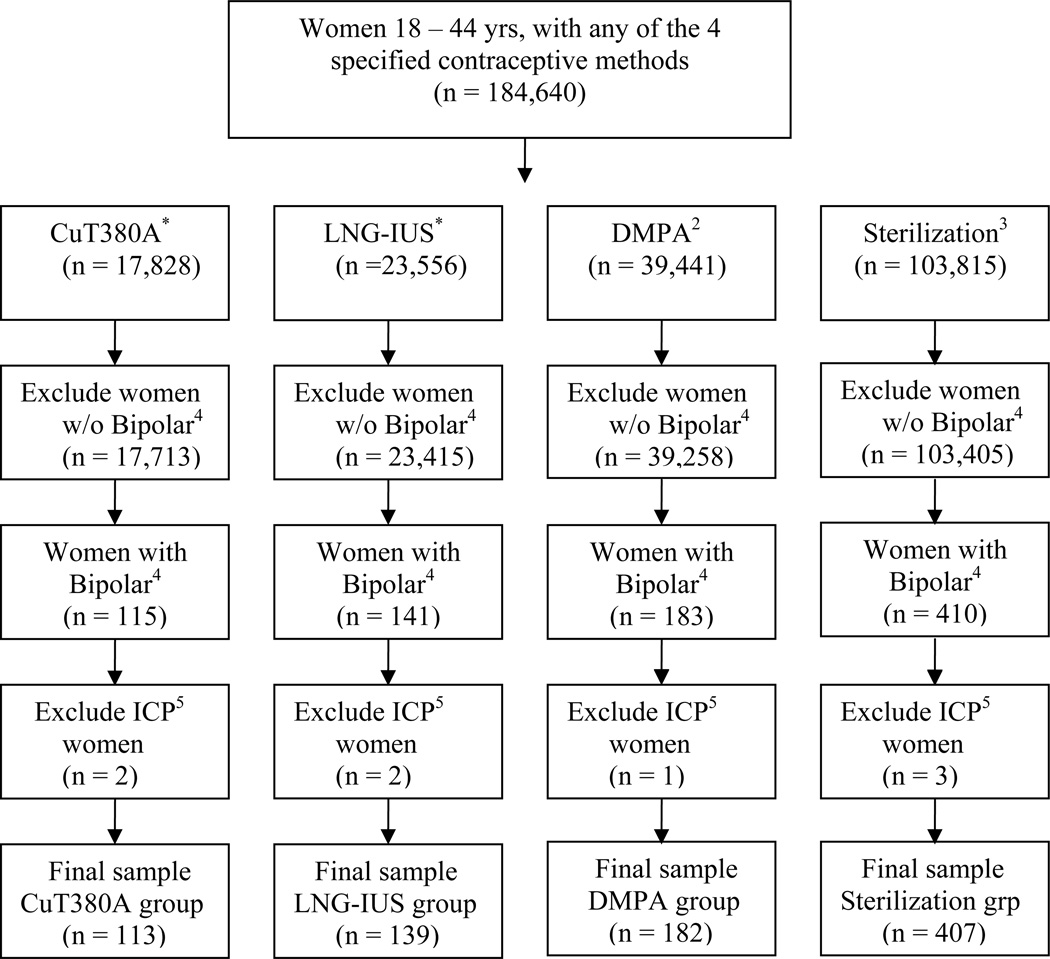
To examine the effects of using LARC among women with bipolar disorder, we first identified all women aged 18–44 years who received one of four different highly effective contraceptive methods: intrauterine contraception (CuT380A or LNG-IUS); depot medroxyprogesterone acetate injections (DMPA), or permanent sterilization, between 2001 and 2005, and had 12 months of continuous follow up. All DMPA users had received four injections within 12 months which is the recommended standard of care. (Figure 1). A total of 184,640 women were identified, of whom 849 were coded as having a diagnosis of bipolar disorder (BP-I, BP-II, or subthreshold BP) during the year prior to use of LARC. Eight of these women were excluded because they were immunocompromised and thus at increased risk of infection. Of the remaining 841 women diagnosed with bipolar disorder, 407 had undergone sterilization, 113 had used CuT380A, 139 had used the LNG-IUS, and 182 had received four injections of DMPA within 12 months. For women in each of the four contraceptive groups, age and the region of residence in US were described.
Figure 1.
Classification of women having a CuT380A or LNG-IUS inserted, receiving DMPA, or undergoing sterilization.
- Women with a LNG-IUS insertion were identified as those who had (a) HCPCS codes of S4981 or J7302, and any of the following CPT or ICD-9 codes: 58300, 69.7, V25.1 and V25.42. Women with a CuT380A insertion were identified as those who had HCPCS code of J7300, and any of the following: CPT code of 88300 or ICD-9-CM codes of 69.7, V25.1 and V25.42.
- A woman was classified in the DMPA group if she received 4 injections in a 12-month period. The HCPCS code of J1055 was used to identify DMPA injection.
- The codes for sterilization included: CPT codes of 58565, 58600, 58605, 58611, 58615, 58670, 58671, and ICD-9-CM codes of 66.2, 66.3, V25.2.
- The diagnosis codes for bipolar disorder (BPD-I, BPD-II, BPD-Not Otherwise Specified (NOS)/subthreshold) include 296.0-296.8 except for codes 296.2 and 296.3. We included only those diagnoses by a mental health professional.
- The diagnosis codes for women who were immunocompromised (ICP) include: 042, 043, 044, 279.0-279.3.
Outcomes examined for each of the four contraceptive groups included rates of contraceptive continuation over a 12-month interval, infectious and noninfectious complications, and rates of hospitalization for bipolar disorder. Because 40% of bipolar patients, particularly women, are diagnosed initially with unipolar depression, we also included hospitalizations for depression (17)(18). Efficacy of the four methods has been well-established and was not examined in this study. In instances where an IUD was discontinued within the first year of use, these complications were evaluated only for the duration of use. Infectious outcomes included gonoccal infections, inflammatory diseases of the female reproductive tract, and cervicitis/endocervitis. Non infectious complications included pain associated with female genital organs (dyspareunia, dysmenorrhea, or premenstrual tension syndrome), disorders of menstruation (absences of menstruation, scanty or infrequent menstruation, excessive or frequent menstruation, irregular menstrual cycles, metrorrhagia, postcoital bleeding, dysfunctional or functional uterine hemorrhage, or unspecified), accidental puncture or laceration, and mechanical complications of intrauterine devices. Due to the vague nature for the last code, all claims within one year of this diagnosis were reviewed. In addition, the ectopic pregnancy rate was examined for each group. Chi-square tests were used to compare categorical variables and one way ANOVA to compare continuous variables (19). The exact Pearson chi-square was used to compare the rates of hospitalizations for bipolar disorder and depression among the contraceptive groups.
Results
Sterilization (48.4%) was the most common method of long acting birth control selected by women diagnosed with bipolar disorder, followed by DMPA (21.6%), LNG-IUS (16.5%) and CuT380A (13.4%). Women undergoing sterilization were significantly older than those using the three reversible contraceptive methods examined. No significant differences were observed in the type of birth control used across geographic regions among these women with bipolar disorder (Table 1).
Table 1.
Characteristics of women using each contraceptive method.
| CuT380A | LNG-IUS | DMPA | Sterilization | P-Value | |
|---|---|---|---|---|---|
| Total, N (%) | 113(13.4) | 139(16.5) | 182(21.6) | 407(48.4) | -- |
| Age (Mean±SD) | 30.0±6.6 | 31.2±6.4 | 30.0±7.5 | 33.3±5.7 | <0.0001 |
| Region, N(%) | -- | -- | -- | -- | 0.33 |
| Northeast | 14 (12.4) | 13 (9.4) | 64 (35.2) | 27 (6.6) | -- |
| Midwest | 38 (33.6) | 43 (30.9) | 16 (8.8) | 144 (35.4) | -- |
| South | 52 (46.0) | 68 (48.9) | 76 (41.8) | 177 (43.5) | -- |
| West | 9 (8.0) | 15 (10.8) | 26 (14.3) | 59 (14.5) | -- |
CuT380A, copper intrauterine device; LNG-IUS, levonorgestrel intrauterine system; DMPA, depot medroxyprogesterone acetate.
When the three LARC methods (CuT380A, LNG-IUS, and DMPA) were compared, a significant difference was observed in continuation rates. (Table 2). Among women who received a CuT380A or LNG-IUS, 86% and 87% respectively were still using the method 12 months later. In comparison, only 31% of those who received a DMPA injection during the study interval received three more injections during the following year (p<0.0001). With regard to the effect of these contraceptive methods on bipolar disorder, no significant differences were observed in the number of hospitalizations for bipolar disorder or depression among the four contraceptive groups. (Table 3).
Table 2.
12-mo continuation rates and frequency of infectious and noninfectious complications
| CuT380A | LNG-IUS | DMPA | Sterilization | P-Value | |||||
|---|---|---|---|---|---|---|---|---|---|
| N | % | N | % | N | % | N | % | ||
| CONTINUATION RATES | 113 | 86 | 139 | 87 | 182 | 31 | 407 | 100 | <.0001 |
|
COMPLICATIONS Menstrual Disorders |
-- | -- | -- | -- | -- | -- | -- | -- | -- |
| Absence of menstruation | 4 | 3.54 | 7 | 5.04 | 8 | 4.40 | 12 | 2.95 | 0.65 |
| Scanty menstruation | 0 | 0.00 | 0 | 0.00 | 0 | 0.00 | 1 | 0.25 | 1.00 |
| Excessive menstruation | 6 | 5.31 | 5 | 3.60 | 5 | 2.75 | 26 | 6.39 | 0.67 |
| Irregular menses | 6 | 5.31 | 6 | 4.32 | 3 | 1.65 | 19 | 4.67 | 0.31 |
| Metrorrhagia | 4 | 3.54 | 5 | 3.60 | 3 | 1.65 | 7 | 1.72 | 0.43 |
| Postcoital bleeding | 0 | 0.00 | 1 | 0.72 | 0 | 0.00 | 0 | 0.00 | 0.30 |
| Other dysfunctional uterine hemorrhage | 7 | 6.19 | 3 | 2.16 | 7 | 3.85 | 23 | 5.65 | 0.30 |
| Unspecified | 1 | 0.88 | 0 | 0.00 | 2 | 1.10 | 4 | 0.98 | 0.79 |
| Pain related to genital organs | -- | -- | -- | -- | -- | -- | -- | -- | -- |
| Dyspareunia | 2 | 1.77 | 5 | 3.60 | 1 | 0.55 | 6 | 1.47 | 0.19 |
| Dysmenorrhea | 6 | 5.31 | 4 | 2.88 | 5 | 2.75 | 20 | 4.91 | 0.49 |
| Premenstrual tension syndromes | 0 | 0.00 | 0 | 0.00 | 2 | 1.10 | 3 | 0.74 | 0.60 |
| Infectious Complications | -- | -- | -- | -- | -- | -- | -- | -- | -- |
| Inflammatory diseases of the fallopian tubes | 0 | 0.00 | 1 | 0.72 | 0 | 0.00 | 2 | 0.49 | 0.66 |
| Inflammatory disease of the uterus | 2 | 1.77 | 0 | 0.00 | 0 | 0.00 | 7 | 1.72 | 0.12 |
| Cervicitis | 2 | 1.77 | 5 | 3.60 | 2 | 1.10 | 12 | 2.95 | 0.42 |
CuT380A, copper intrauterine device; LNG-IUS, levonorgestrel intrauterine system; DMPA, depot medroxyprogesterone acetate.
Table 3.
Frequency of hospitalizations for BPD or depression
| Hospitalizations | CuT380A | LNG-IUS | DMPA | Sterilization | ||||
|---|---|---|---|---|---|---|---|---|
| N | % | N | % | N | % | N | % | |
| Bipolar disorder | 6 | 5.31 | 5 | 3.60 | 11 | 6.04 | 23 | 5.65 |
| Depression | 1 | 0.88 | 1 | 0.72 | 4 | 2.20 | 13 | 3.19 |
BPD, bipolar disorder; CuT380A, copper intrauterine device; LNG-IUS, levonorgestrel intrauterine system; DMPA, depot medroxyprogesterone acetate.
The exact Pearson chi-square test was used.
Overall, we did not observe any differences by contraceptive type in infectious or noninfectious complications. (Table 2). Cervicitis was the most common infectious complication across all contraceptive groups (1.8% CuT380A, 3.6% LNG-IUS, 1.1% DMPA and 3.0% sterilization) while dysmenorrhea was the most common non infectious complication (5.3% CuT380A, 2.9% LNG-IUS, 2.8% DMPA and 4.9% sterilization). Three IUD users (two CuT380A and one LNG-IUS) were coded for “mechanical complication of an IUD.” Due to the vague description of this code, the trajectories for these three cases were reviewed in detail. One woman with a CuT380A was coded with this diagnosis two days after insertion followed by an emergency room encounter for pain associated with female genital organs four days later. Four days after the emergency room encounter, the CuT380A was removed. This sequence of events suggests that the mechanical complication may have been a partial expulsion. The other two patients did not have any testing or procedures related to their mechanical complication, so the exact nature of the complication could not be determined.
Furthermore, no significant difference was observed in the number of ectopic pregnancies that occurred in each group (p = 0.14). One patient was coded with this diagnosis two weeks after her LNG-IUS insertion while another had an ectopic pregnancy seven months after insertion of a CuT380A. Both underwent a laparoscopic procedure to treat the ectopic pregnancy. No patients in the sterilization or DMPA groups had a claim for the diagnosis or treatment of an ectopic pregnancy during the 12 months of follow-up.
Discussion
This study examined complications associated with sterilization and three types of LARC among women previously diagnosed with bipolar disorder. We observed that rates of infectious and non infectious complications were low among this population of women using sterilization and different types of LARC. Further, hospitalizations due to bipolar disorder or depression did not differ between women using different types of contraception.
Similar to the general population, IUD continuation rates were higher than DMPA after one year of use. In fact, over 80% of women who selected either LNG-IUS or CuT380A continued their chosen method for at least 12 months. This is in agreement with other studies on women without a history of mental illness (10)(20). In contrast, only 31% of women who began DMPA received 4 injections in a 12-month period. This continuation rate is much lower than reported rates that demonstrate approximately 50% of women who initiate DMPA continue this method for at least one year (10) (21)(22)(23)(24)(25).
When we re-examined results of 14 international clinical studies conducted by the World Health Organization, we found that although the average continuation rate at one year was 51% for DMPA, the rate ranged from 25% to 67% on individual investigations (25). Similarly, some studies in US women have reported 12-month continuation rates on DMPA ranging from 21.3% to 28.6% (26)(27)(28). In line with our findings, another study generated from a different U.S. insurance claims database indicates that nearly 60% of new DMPA users did not receive a second injection at 3 months (29)(30). Perhaps differences in study settings, such as international versus U.S. populations, and formal clinical research studies versus actual use as documented in medical claims data, have contributed to the wide range of continuation rates reported for DMPA. Also, a copayment was required of the women reflected in the medical claims database. In addition, they would not have received financial incentives nor extended supportive counseling that are usually provided to research participants in DMPA studies.
Use of a large claims database allowed us to examine usage of four different types of contraception and related complications among reproductive-aged women diagnosed with bipolar disorder, thus, providing new insights into the importance of choosing LARC for these women. However, there are several limitations to this study which could have affected our conclusions. First, the population consisted of women with commercial health insurance, so our findings may not be applicable to those who do not have this level of coverage. Also, claims data is generated from past patient encounters, precluding randomization of women to different methods of contraception. Because we detected few complications, we may not have had the statistical power to detect differences. In addition, women may not seek medical help for minor side effects associated with contraceptive use. Thus, some complications are likely underreported in this data. However, we would anticipate that major complications were reported and coded. Medical charts were not available for review, so we were not able to determine reasons for contraceptive discontinuation. Future studies should address these issues to help provide more information in addressing the contraceptive needs of women with bipolar disorder.
Despite these limitations, we have demonstrated that women with bipolar disorder who desire a reversible contraceptive method are appropriate candidates for LARC. Furthermore, women with this disorder are more likely to continue using IUDs than DMPA for at least one year for contraception. Although findings from claims data possess certain limitations, mined information can provide a valuable snapshot of actual treatment practices and outcomes within a defined population. Bipolar disorder and associated medication challenges are sometimes poorly understood by Ob/Gyns. Likewise, the contraceptive needs of women with the disorder may not be adequately addressed by those in psychiatry. Our study provides relevant information for improved clinical decision-making by Ob/Gyns whose patients include women with bipolar disorder.
Acknowledgments
Federal support for this study was provided by the Eunice Kennedy Shriver National Institute of Child Health & Human Development (NICHD) as follows: Mid-Career Investigator Award (K24HD04365, Berenson); National Research Service Award institutional training grant for postdoctoral fellows (T32HD055163, Asem).
The content is solely the responsibility of the authors and does not necessarily represent the official views of the NICHD nor the National Institutes of Health.
Footnotes
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
Financial Disclosure: The authors did not report any potential conflicts of interest.
Presented at the North American Forum on Family Planning, Oct 22 – 24, 2011. Washington DC.
References
- 1.Merikangas KR, Akiskal HS, Angst J, Greenberg PE, Hirschfeld RM, Petukhova M, et al. Lifetime and 12-month prevalence of bipolar spectrum disorder in the National Comorbidity Survey replication. Arch Gen Psychiatry. 2007;64:543–552. doi: 10.1001/archpsyc.64.5.543. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Kessler RC, Merikangas KR, Wang PS. Prevalence, comorbidity, and service utilization for mood disorders in the United States at the beginning of the twenty-first century. Annu Rev Clin Psychol. 2007;3:137–158. doi: 10.1146/annurev.clinpsy.3.022806.091444. [DOI] [PubMed] [Google Scholar]
- 3.National Comorbidity Survey Replication (NCS-R) [Accessed 05/24/2011];12-month prevalence estimates. 2007 Table 2. Available at http://www.hcp.med.harvard.edu/ncs/
- 4.Meade CS, Graff FS, Griffin ML, Weiss RD. HIV risk behavior among patients with co-occurring bipolar and substance use disorders: associations with mania and drug abuse. Drug Alcohol Depend. 2008;92:296–300. doi: 10.1016/j.drugalcdep.2007.07.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Magalhães PV, Kapczinski F, Kauer-Sant'Anna M. Use of contraceptive methods among women treated for bipolar disorder. Arch Womens Ment Health. 2009;12:183–185. doi: 10.1007/s00737-009-0060-y. [DOI] [PubMed] [Google Scholar]
- 6.Curtis V. Women are not the same as men: specific clinical issues for female patients with bipolar disorder. Bipolar Disord. 2005;7 Suppl 1:16–24. doi: 10.1111/j.1399-5618.2005.00190.x. [DOI] [PubMed] [Google Scholar]
- 7.Coverdale JH, McCullough LB, Chervenak FA. Sexually transmitted diseases and unwanted pregnancies in chronically ill psychiatric patients. Med J Aust. 1997;166:231–232. [PubMed] [Google Scholar]
- 8.Coverdale JH, Turbott SH, Roberts H. Family planning needs and STD risk behaviours of female psychiatric out-patients. Br J Psychiatry. 1997;171:69–72. doi: 10.1192/bjp.171.1.69. [DOI] [PubMed] [Google Scholar]
- 9.Crawford P. Interactions between antiepileptic drugs and hormonal contraception. CNS Drugs. 2002;16:263–272. doi: 10.2165/00023210-200216040-00005. [DOI] [PubMed] [Google Scholar]
- 10.Centers for Disease Control and Prevention (CDC) U S. Medical Eligibility Criteria for Contraceptive Use, 2010. MMWR Recomm Rep. 2010;59(RR-4):1–86. [PubMed]
- 11.Dutton C, Foldvary-Schaefer N. Contraception in women with epilepsy: pharmacokinetic interactions, contraceptive options, and management. Int Rev Neurobiol. 2008;83:113–134. doi: 10.1016/S0074-7742(08)00006-8. [DOI] [PubMed] [Google Scholar]
- 12.Gaffield ME, Culwell KR, Lee CR. The use of hormonal contraception among women taking anticonvulsant therapy. Contraception. 2011;83:16–29. doi: 10.1016/j.contraception.2010.06.013. [DOI] [PubMed] [Google Scholar]
- 13.Carey MP, Carey KB, Maisto SA, Schroder KE, Vanable PA, Gordon CM. HIV risk behavior among psychiatric outpatients: association with psychiatric disorder, substance use disorder, and gender. J Nerv Ment Dis. 2004;192:289–296. doi: 10.1097/01.nmd.0000120888.45094.38. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Lanza LL, Dreyer NA, Schultz NJ, Walker AM. Use of insurance claims in epidemiologic research: identification of peptic ulcers, GI bleeding, pancreatitis, hepatitis, and renal disease. Pharmacoepidemiol Drug Saf. 1995;4:239–248. [Google Scholar]
- 15.Enger C, Cali C, Walker AM. Serious ventricular arrhythmias among users of cisapride and other QT-prolonging agents in the United States. Pharmacoepidemiol Drug Saf. 2002;11:477–486. doi: 10.1002/pds.725. [DOI] [PubMed] [Google Scholar]
- 16.Johannes CB, Koro CE, Quin SG, Cutone JA, Seeger JD. The risk of coronary heart disease in type 2 diabetic patients exposed to thiazolidinediones compare to metformin and sulfonylurea therapy. Pharmacoepidemiol Drug Saf. 2007;16:504–512. doi: 10.1002/pds.1356. [DOI] [PubMed] [Google Scholar]
- 17.McElroy SL. Bipolar disorders: special diagnostic and treatment considerations in women. CNS Spectr. 2004;9:5–18. doi: 10.1017/s1092852900002327. [DOI] [PubMed] [Google Scholar]
- 18.Saunders KEA, Goodwin GM. The course of bipolar disorder. Adv Psychiatr Treat. 2010:318–328. [Google Scholar]
- 19.Agresti A. An Introduction to Categorical Data Analysis. 2nd Ed. New York: John Wiley & Sons; 2007. [Google Scholar]
- 20.Peipert JF, Zhao Q, Allsworth JE, Petrosky E, Madden T, Eisenberg D, Secura G. Continuation and satisfaction of reversible contraception. Obstet Gynecol. 2011;117:1105–1113. doi: 10.1097/AOG.0b013e31821188ad. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Paul C, Skegg DC, Williams S. Depot medroxyprogesterone acetate. Patterns of use and reasons for discontinuation. Contraception. 1997;56:209–214. doi: 10.1016/s0010-7824(97)00140-6. [DOI] [PubMed] [Google Scholar]
- 22.Hubacher D, Goco N, Gonzalez B, Taylor D. Factors affecting continuation rates of DMPA. Contraception. 1999 Dec;60(6):345–351. doi: 10.1016/s0010-7824(99)00104-3. [DOI] [PubMed] [Google Scholar]
- 23.Berenson AB, Odom SD, Breitkopf CR, Rahman M. Physiologic and psychologic symptoms associated with use of injectable contraception and 20 microg oral contraceptive pills. Am J Obstet Gynecol. 2008;199 doi: 10.1016/j.ajog.2008.04.048. 351.e1-12. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Vaughan B, Trussell J, Kost K, Singh S, Jones R. Discontinuation and resumption of contraceptive use: results from the 2002 National Survey of Family Growth. Contraception. 2008;78:271–283. doi: 10.1016/j.contraception.2008.05.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Draper BH, Morroni C, Hoffman M, Smit J, Beksinska M, Hapgood J, Van der Merwe L. Depot medroxyprogesterone versus norethisterone oenanthate for long-acting progestogenic contraception. Cochrane Database Syst Rev. 2006;3:CD005214. doi: 10.1002/14651858.CD005214.pub2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Westfall JM, Main DS, Barnard L. Continuation rates among injectable contraceptive users. Fam Plann Perspect. 1996;28:275–277. [PubMed] [Google Scholar]
- 27.Sangi-Haghpeykar H, Poindexter AN, 3rd, Bateman L, Ditmore JR. Experiences of injectable contraceptive users in an urban setting. Obstet Gynecol. 1996;88:227–233. doi: 10.1016/0029-7844(96)00194-9. [DOI] [PubMed] [Google Scholar]
- 28.Raine TR, Foster-Rosales A, Upadhyay UD, Boyer CB, Brown BA, Sokoloff A, Harper CC. One-year contraceptive continuation and pregnancy in adolescent girls and women initiating hormonal contraceptives. Obstet Gynecol. 2011;117:363–371. doi: 10.1097/AOG.0b013e31820563d3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Halpern V, Lopez LM, Grimes DA, Gallo MF. Strategies to improve adherence and acceptability of hormonal methods of contraception. Cochrane Database Syst Rev. 2011;4:CD004317. doi: 10.1002/14651858.CD004317.pub3. [DOI] [PubMed] [Google Scholar]
- 30.Murphy PA, Brixner D. Hormonal contraceptive discontinuation patterns according to formulation: investigation of associations in an administrative claims database. Contraception. 2008;77:257–263. doi: 10.1016/j.contraception.2008.01.002. [DOI] [PubMed] [Google Scholar]