Abstract
Dengue infection is now known to present with wide spectrum of complications. Isolated cases of acute pancreatitis complicating dengue haemorrhagic fever have been reported in literature. Here the authors report a case of dengue haemorrhagic fever that develops acute pancreatitis and presented with acute onset of breathlessness, which then progressed to full-blown acute respiratory distress syndrome. To our knowledge, this is the first reported case of dengue haemorrhagic fever complicated with acute pancreatitis and acute respiratory distress syndrome.
Background
Dengue is an arboviral infection common in tropical countries including India. Dengue is transmitted by the bite of the Aedes mosquito infected with any one of the four dengue virus serotypes. Infection by different serotypes offers no cross protection and epidemics caused by multiple serotypes can occur. Physicians have now been perplexed with changing spectrum of complications seen in dengue infection, these need to be very well elucidated. Acute respiratory distress syndrome (ARDS) is a heterogeneous clinical syndrome comprising of respiratory distress, severe hypoxemia, diffuse radiographic infiltrates and decreased lung compliance that has a high mortality. Cases of ARDS complicating dengue virus infection have also been described in literature.1 Isolated cases of acute pancreatitis complicating dengue haemorrhagic fever have been reported in literature.2 Here we report a case of dengue haemorrhagic fever (DHF) who comes with abdominal pain, vomiting and respiratory distress for which further investigation is done and finally a diagnosis of ARDS with acute pancreatitis is confirmed.
Case presentation
A previously healthy, 38-year-old male was admitted with high grade fever for 10 days, breathlessness for 8 days and also had diffuse abdominal pain and multiple episodes of vomiting since 3 days. On examination, the patient was tachypnoeic; petechial rashes present over lower limbs and trunk; temperature 101.2°F; blood pressure 100/60 mm Hg; pulse rate 100/min; respiratory rate 40/min. Chest examination showed bilateral diffuse crackles. Cardiac examination was normal. Abdomen was distended, tender but bowel sounds were present and also did not have any organomegaly.
Investigations
Laboratory investigation showed decreased platelets count and negative malaria antigen by card test. However, dengue-specific IgM antibody was positive. Blood chemistry showed deranged renal function tests and serum lipase levels were raised. Serum aminotransferases, prothrombin time and partial thromboplastin time were normal. Arterial blood gas analysis showed type I respiratory failure (table 1). Bilateral infiltrates were present in chest x-ray (figure 1). Ultrasonography (USG) abdomen was done which suggest acute pancreatitis (figure 2). On day 7 when his renal function tests had allowed us, CT scan abdomen with contrast was done, findings of which were also suggestive of acute pancreatitis with modified CT severity index of VI/X (figure 3).
Table 1.
Blood investigations done during the course of hospital stay
| Date | September 2011 | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| 05 | 06 | 07 | 08 | 09 | 10 | 12 | 15 | 17 | 20 | ||
| Parameters (reference ranges) | |||||||||||
| Haematocrit (35–44% for female) | 24.3 | 24.6 | 28.1 | 29.3 | 34.2 | 36 | 37 | 40 | 43 | ||
| Total WBC count (4000–11500 cells/cu.mm) | 7600 | 8830 | 8200 | 12 610 | 10 340 | 8900 | 9900 | 8800 | 7890 | ||
| Platelet count (1.5–4.5 lacs/cu.mm) | 0.15 | 0.07 | 0.09 | 0.18 | 0.54 | 0.69 | 1.2 | 1.4 | 1.6 | ||
| Random blood sugar (mg/dl) | 121 | 157 | |||||||||
| Serum sodium (135–148 meq/l) | 142 | 136 | |||||||||
| Serum potassium (3.5–5 meq/l) | 3.4 | 3.5 | 3.5 | 4.5 | 4.3 | ||||||
| Serum urea (15–43 mg%) | 162 | 178 | 98 | 69 | 58 | ||||||
| Serum creatinine (0.6–1.2 mg%) | 1.94 | 2.1 | 1.82 | 1.5 | 1.4 | ||||||
| PT (12–16 s) | 14 | ||||||||||
| INR (0.8–1.2) | 1.0 | ||||||||||
| aPTT (25–36 s) | 30 | ||||||||||
| Serum bilirubin (0.5–1.2 mg/dl) | 2.7 | ||||||||||
| SGPT (9–45 IU/l) | 35 | ||||||||||
| SALP | 289 | ||||||||||
| Serum amylase (20–85 U/l) | 750 | 67 | |||||||||
| Serum lipase (10–60 U/l) | 500 | 45 | |||||||||
| ABG | PO2 (80–100 mm Hg) | 82* | 100* | 92* | 136** | 158** | 138** | 130* | 70 | 75 | |
| PCO2 (35–45 mm Hg) | 20.8 | 21 | 21 | 28 | 30 | 31 | 34 | 35 | 37 | ||
| HCO3 (20–24 mmol/l) | 10.9 | 13 | 12.7 | 14.1 | 15.8 | 16.2 | 17.3 | 19.0 | 21.0 | ||
| SO2 (%) | 94.6 | 95 | 97 | 99 | 99 | 98 | 98 | 97 | 98 | ||
ABG, arterial blood gas; aPTT, activated partial thromboplastin time; INR, international normalised ratio; PT, prothrombin time; SALP, serum alkaline phosphatase; SGPT, serum glutamic pyruvic transaminase; WBC, white blood cell.
PO2 when patient on face mask (FiO2-40%)
PO2 when patient on face mask (FiO2-100%)
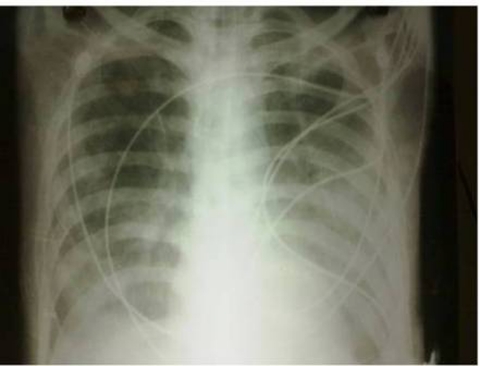
Figure 1.
Chest x-ray posterior-anterior view shows bilateral alveolar infiltrate in more than half of the lung fields.
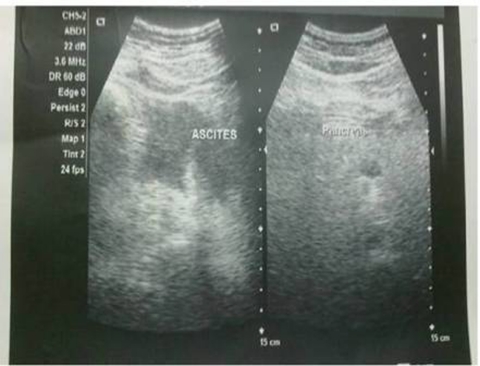
Figure 2.
Ultrasonography abdomen shows bulky heterogenous pancreas with free fluid in abdominal cavity suggestive of acute pancreatitis.
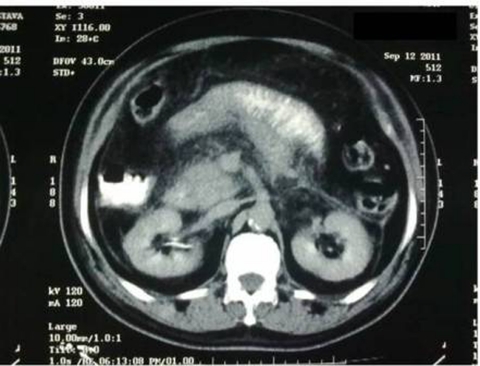
Figure 3.
CT scan abdomen shows bulky pancreas with post contrast enhancement. Few ill defined small non-enhancing hypodensities suggestive of necrosis are seen within pancreatic parenchyma.
Differential diagnosis
Complicated malaria.
Treatment
Supportive treatment in the form of antipyretic, intravenous fluid and oxygen inhalation was started and two units of platelets were transfused to patient. The patient’s condition was worsened and next day, his breathlessness was also increased and eventually he developed acute lung injury and was put on mechanical ventilation. The patient was weaned off from ventilator on day 7 and was treated conservatively. An opinion from gastrosurgery department was also sought that remains the same in the favour of continuing conservative treatment.
Outcome and follow-up
The patient did well and recovered fully and gets discharged on 15th day. At the first follow-up made after a week, he did not have any complains.
Discussion
Dengue infection has wide array of atypical manifestations.3 It has now no longer been presented only as spectrum from classical dengue fever to potentially fatal form of DHF or dengue shock syndrome (DSS). ARDS is an acute hypoxaemic respiratory failure due to non-cardiogenic pulmonary oedema caused by increased permeability of the alveolar capillary barrier. It is precipitated by various conditions that range from direct injury (eg, aspiration, diffuse infection) to indirect injury (eg, sepsis, non-thoracic trauma). Many infectious agents have been implicated to trigger ARDS, ranging from bacteria, fungi, parasites and viruses too.
Acute pancreatitis is an uncommon complication of DHF. Pathophysiology behind the involvement of the pancreas in dengue infection is not exactly known but possible mechanism may be due to direct viral invasion or hypotension in DHF. However, there are no convincing reports where histological confirmation of dengue virus has been done.
In this patient, illness started with fever and petechial rashes and during the course of illness he had pain abdomen, vomiting and breathlessness. Since the patient was residing in a dengue endemic area, clinical scenario (petechial rashes) and lab investigations (severe thrombocytopenia and positive IgM antibodies for dengue virus infection) were suggesting a diagnosis of DHF. Although, cases of dengue infection causing ARDS have been reported, it is not a well known cause of ARDS. Here, the diagnosis of ARDS was made on the basis of chest x-ray findings and the PaO2/FiO2 ratio, in accordance with the American-European consensus conference on ARDS guidelines.4
Acute pancreatitis was suspected in our patients because of history of vomiting and abdominal pain, and later on got confirmed (>3 times raised serum lipase, findings of USG and CT scan abdomen). It is a well-known fact that acute pancreatitis can also cause ARDS. Therefore, in our patient, ARDS might also be developed due to ongoing pancreatitis or might be the result of DHF.
Learning points.
-
▶
This case description highlights the fatal and unusual complications of dengue hemorrhagic fever.
-
▶
Acute pancreatitis can be a complication of DHF, it should be kept in mind when patient of DHF come with abdominal pain and vomiting.
-
▶
Adherence to conservative and supportive measures that should have been taken according to situation may result into a successful outcome.
-
▶
The spectrum of dengue infection and its complications needs further validation.
Footnotes
Competing interests None.
Patient consent Obtained.
References
- 1.Sen MK, Ojha UC, Chakrabarti S, et al. Dengue hemorrhagic fever (DHF) presenting with ARDS. Indian J Chest Dis Allied Sci 1999;41:115–9 [PubMed] [Google Scholar]
- 2.Derycke T, Levy P, Genelle B, et al. [Acute pancreatitis secondary to dengue]. Gastroenterol Clin Biol 2005;29:85–6 [DOI] [PubMed] [Google Scholar]
- 3.Gulati S, Maheshwari A. Atypical manifestations of dengue. Trop Med Int Health 2007;12:1087–95 [DOI] [PubMed] [Google Scholar]
- 4.Bernard GR, Artigas A, Brigham KL, et al. The American-European Consensus Conference on ARDS. Definitions, mechanisms, relevant outcomes, and clinical trial coordination. Am J Respir Crit Care Med 1994;149(3 Pt 1):818–24 [DOI] [PubMed] [Google Scholar]