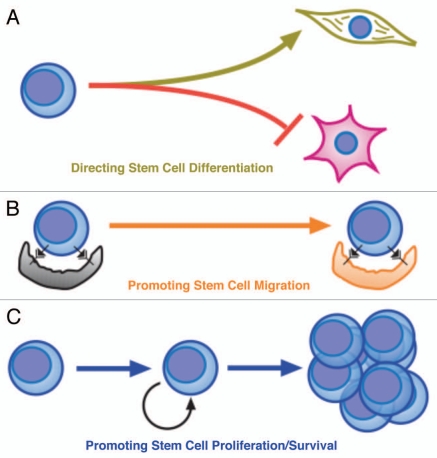
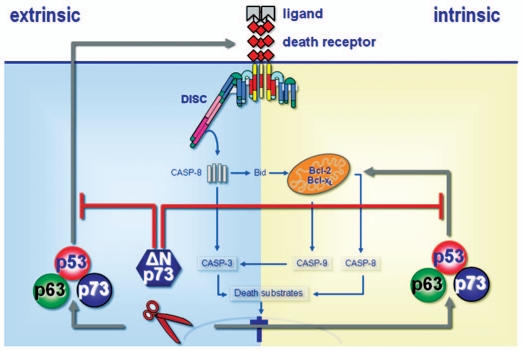
Several studies recently unveiled the involvement of the Polycomb group (PcG) proteins, most notably Bmi-1 and EZH2, in the occurrence of various human cancers and maintenance of the invasive phenotype. The PcG proteins are typically involved in the transcriptional silencing of their target genes through epigenetic mechanisms resulting in chromatin compaction. As part of the polycomb repressive complex (PRC) 2, EZH2 trimethylates histone 3 at lysine 27 (H3K27), allowing for the recruitment and assembly of the PRC1 proteins at the regulatory chromatin of the target genes.1 Bmi-1 is a component of the PRC1 required for monoubiquitination of histone 2A (uH2A), which would further promote chromatin compaction and gene silencing. Genome-wide screening revealed nearly 700 genes enriched with uH2A near the transcription start sites, and this correlated well with Bmi-1 enrichment,2 suggesting wide array of molecular pathways under transcriptional repression by Bmi-1. Oncogenic effects seen with the elevated levels of Bmi-1 and EZH2 stem from the transcriptional silencing of tumor suppressors, such as p16INK4A and p57KIP2, among other unknown PcG target genes. Bmi-1 also plays a critical role in maintaining the self-renewal capacity of normal and malignant cancer stem cells (CSCs).3 Recent advances in cancer research revealed importance of CSCs in the perpetuity of the disease due to their unique characteristics, such as enhanced malignant phenotype and resistance to the death signaling by irradiation or chemotherapeutic agents. To that end, effective anti-cancer therapy necessitates selective targeting of the CSCs, which may be accomplished by inhibiting Bmi-1 and EZH2. Success of this approach has been reported in recent articles in which Bmi-1 or EZH2 was targeted by RNAi to result in cell proliferation arrest and loss of self-renewal of cancer cell lines.4,5 However, there has been a notable gap between the principle of this novel anti-cancer approach and its clinical application due to lack of appropriate means to target the PcG proteins.
The article by Bommi et al.6 demonstrated that Bmi-1 expression can be targeted by exposure of cultured cells to sodium butyrate (NaB), a histone deacetylase inhibitor (HDACI).6 This finding is significant because it provides a novel mechanism underlying the anti-cancer effects of HDACIs. To date, the therapeutic benefits HDACIs have been demonstrated in many hematologic malignancies and few solid tumors when they are used as a single agent or in combination with demethylating agent. Several mechanisms have been proposed to involve (1) activating the DNA damage and growth arrest responses through ATM; (2) dowregulating thymidylate synthase, a target of a chemotherapeutic agent 5-fluorouracil; and (3) disrupting the chaperon function of hsp90 by protein acetylation, resulting in the reduced levels of its oncogenic client proteins.7 As shown in the current study, inhibition of the PcG proteins by NaB led to the induction of the growth inhibitory genes, such as p21WAF1 and p57KIP2, and cell death response via premature senescence or apoptosis in the breast cancer cell lines. The authors elegantly demonstrated the transcriptional repression of Bmi-1 by NaB through a mechanism independent of c-Myc, which was previously shown to be necessary for Bmi-1 expression. The time-course experiment also showed that Bmi-1 down-regulation by NaB is indirect, and suggests an unknown factor that mediates the inhibitory effects of the HDACI. Due to the involvement of Bmi-1 in self-renewal and maintenance of CSCs, this study revealed a possibility that HDACIs may target CSCs to elicit their anticancer effect.
Although the relationship between histone acetylation and stem cell phenotype is not well established, a recent study by Lee et al. showed that HDACIs interfere with stem cell function.8 HDACI exposure to human mesenchymal stem cells (hMSCs) isolated from the adipose tissues led to premature senescence by induction of p21WAF1 and loss of pluripotency. Another study by Jung et al. demonstrated that accelerated aging of hMSCs by HDACI treatment was due to downregulation of PcG proteins, namely Bmi-1, EZH2, and SUZ12, while treatment of cells to a histone acetyltransferase (HAT) inhibitor delayed the senescent phenotype.9 These findings plus the current study of Bommie et al. raise the possibility that the therapeutic efficacy of HDACI against cancer lies on its inhibitory effects on CSCs through targeting the PcG expression. Further research is needed to unveil this connection.
References
- 1.Simon JA, et al. Nat Rev Mol Cell Biol. 2009;10:697–708. doi: 10.1038/nrm2763. [DOI] [PubMed] [Google Scholar]
- 2.Kallin EM, et al. PLoS Genet. 2009;5:e1000506. doi: 10.1371/journal.pgen.1000506. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Liu S, et al. Cancer Res. 2006;66:6063–6071. doi: 10.1158/0008-5472.CAN-06-0054. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Godlewski J, et al. Cancer Res. 2008;68:9125–9130. doi: 10.1158/0008-5472.CAN-08-2629. [DOI] [PubMed] [Google Scholar]
- 5.Zhang YB, et al. Eur J Cancer Care. 2010;46:1640–1649. doi: 10.1016/j.ejca.2010.02.003. [DOI] [PubMed] [Google Scholar]
- 6.Bommi PV, et al. Cell Cycle. 2010;9:2663–2673. doi: 10.4161/cc.9.13.12147. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Glaser KB. Biochem Pharmacol. 2007;74:659–671. doi: 10.1016/j.bcp.2007.04.007. [DOI] [PubMed] [Google Scholar]
- 8.Lee S, et al. Cell Prolif. 2009;42:711–720. doi: 10.1111/j.1365-2184.2009.00633.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Jung JW, et al. Cell Mol Life Sci. 2010;67:1165–1166. doi: 10.1007/s00018-009-0242-9. [DOI] [PMC free article] [PubMed] [Google Scholar]