Introduction
The incidence of gastrointestinal tract duplication cysts is 1:100,000, with only about 160 cases described in adults. They are rare anomalies, 25% of which occur in the esophagus [1]. They most commonly present in infancy and in childhood. In adults they may cause symptoms due to mass effect. When symptomatic, surgical excision is usually recommended as risk of complications, such as intracystic hemorrhage, cyst rupture, infection and very rarely malignant transformation, increase [2].
Case History
A 40 year old lady presented with history of suffering from dysphagia to solids for 6 months. She complained of progressive difficulty in swallowing solid food materials which tend to get stuck in the mid thorax. There was no history of loss of appetite, weight loss, chest pain, breathlessness or fever. An upper GI endoscopy showed narrowing of esophageal lumen by a mass compressing it from the outside. The mucosa over the mass was normal. CT scan of the chest showed a well defined soft tissue density lesion with minimal contrast enhancement arising from the lower thoracic esophagus with mass effect, suggestive of an esophageal leiomyoma. Endoscopic ultrasound again showed a solid submucosal tumor in the lower thoracic esophagus (Fig. 1).
Fig. 1.
Esophagoscopy showing submucosal lesion bulging into lumen 1
The patient was taken up for surgery. Transhiatal excision of the tumor was attempted. However, the mass which was cystic got ruptured inadvertently discharging thick brownish fluid. The wall of the cyst was then excised from the wall of the lower esophagus. After excision, the defect in the esophageal muscle was closed primarily. No mucosal injury was noted. Histopathological examination of the cyst wall showed evidence of two muscle layers; the epithelium, which was of pseudostratified columnar type, had eroded in most places (Fig. 2). The patient recovered well. Barium evaluation of the patient after 6 months showed a small diverticulum at the site of the excised cyst. However, the patient was asymptomatic with complete relief of her dysphagia.
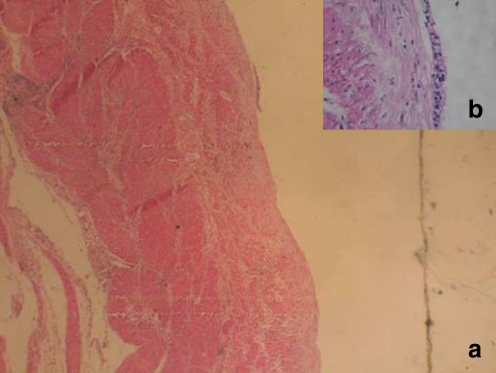
Fig. 2.
H & E stain of wall of the cyst showing the two muscle coats
Discussion
Foregut duplication cysts are rare congenital anomalies of enteric origin that are well-marginated, round, epithelium-lined lesions containing fluid. They are classified into bronchogenic cysts and esophageal duplication cysts [3]. The esophageal duplication cysts, the less common of the two types, are most frequently located in the right posterior mediastinum at the level of the distal third of the oesophagus [3, 4]. They become symptomatic in a rare adult, owing to compression of adjacent structures causing dysphagia, pain, or other symptoms. The rarity of this condition, sometimes, results in failure of diagnosis of this condition in the preoperative setting. On a CT or MRI, an oval or teardrop-shaped well circumscribed mass in close association with the esophageal wall is seen. This raises the suspicion of an exophytic or intramural benign esophageal tumor. Endoscopic ultrasonography has the best chance of accurate preoperative diagnosis, by demonstration of the cystic nature of the lesion. However, thick contents of the cyst can mimic a solid lesion, thus eluding an accurate preoperative diagnosis. The high protein density and high viscosity can result in elevation of the attenuation and/or signal intensity on CT and T1-weighted MR images, respectively. The CT density of the cyst can vary from typical water density (0 to 20 Hounsefield units) to high-density 80 to 90 Hounsefield units [5]. The hypoechogenicity of a cystic lesion could not be demonstrated in our lesion. Hence, the more common solid stromal tumor of the esophagus was diagnosed.
The standard surgical treatment uses a posterolateral thoracotomy or thoracoscopy. But the location of the cyst in the lower mediastinum also enables the transhiatal laparoscopic or laparotomy approach [3, 4]. Transluminal total endoscopic removal [1] and laparoscopic robotic-assisted transhiatal excision [6] have been reported in the literature with good results.
Esophageal duplication cysts are lined by squamous, columnar, cuboid, pseudostratified, or ciliated epithelium [6]. They are covered by two thick muscle layers which are in contiguity with the muscularis propria of the esophagus. Hence, after surgical excision of the cyst, repair of the defect in the esophageal wall by approximation of the muscle edges is mandatory to avoid long term complications of a pseudodiverticulum. It is also important to note that recurrence has been reported after incomplete excision of mediastinal cysts [7]. The preoperative diagnosis of a lower esophageal solid tumor that might be amenable to enucleation resulted in the selection of the transhiatal approach vis-à-vis a posterolateral thoracotomy in this case. The relatively poor exposure provided by this approach probably resulted in the incomplete muscle repair which caused a pseudodiverticulum in this patient.
In conclusion, esophageal duplication cysts can present in an adult mimicking a solid tumor clinically and radiologically. Hence it should be included in the differential diagnosis of a solid esophageal tumor, even though it is a rare condition, as management options differ for the two conditions.
Footnotes
Key Messages
Duplication cysts of the esophagus can become symptomatic in the rare adult. The thick fluid content of the cyst can sometimes masquerade it for a solid tumor of the esophagus. We report one such instance, when transhiatal exploration resulted in inadvertent rupture of the cyst.
References
- 1.Will U, Meyer F, Bosseckert H. Successful endoscopic treatment of an esophageal duplication cyst. Scand J Gastroenterol. 2005;40:995–999. doi: 10.1080/00365520510023125. [DOI] [PubMed] [Google Scholar]
- 2.Lee HS, Jeon HJ, Song CW, Lee SW, Choi JH, Kim CD, et al. Esophageal duplication cyst complicated with intramural hematoma–case report. J Korean Med Sci. 1994;9:188–196. doi: 10.3346/jkms.1994.9.2.188. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Cioffi U, Bonavina L, Simone M, et al. Presentation and surgical management of bronchogenic and esophageal duplication cysts in adults. Chest. 1998;113:1492–1496. doi: 10.1378/chest.113.6.1492. [DOI] [PubMed] [Google Scholar]
- 4.Procházka V, Kala Z, Novotný I, Hrobar P. Laparoscopic management of an infected oesophageal cyst. Rozhl Chir. 2005;84:526–528. [PubMed] [Google Scholar]
- 5.Yernault JC, Kuhn G, Dumortier P, Rocmans P, Ketelbant P, Vuyst P. "Solid" mediastinal bronchogenic cyst: mineralogic analysis. AJR Am J Roentgenol. 1986;146:73–74. doi: 10.2214/ajr.146.1.73. [DOI] [PubMed] [Google Scholar]
- 6.Ringley C, Bochkarev V, Oleynikov D. Esophageal duplication cyst–a guest case in robotic and computer-assisted surgery from the University of Nebraska Medical Center. MedGenMed. 2006;8:25. [PMC free article] [PubMed] [Google Scholar]
- 7.Al-Sadoon H, Wiseman N, Chernick V. Recurrent thoracic duplication cyst with associated mediastinal gas. Can Respir J. 1998;5:149–151. doi: 10.1155/1998/305489. [DOI] [PubMed] [Google Scholar]