Abstract
Purpose
To examine the association between self-rated vision and distance visual acuity by race and other factors.
Design
Cross-sectional analysis within a longitudinal, population-based cohort study.
Participants and Controls
Two thousand five hundred and twenty individuals, aged 65 to 84, including 666 Black participants and 1854 White participants.
Methods
All participants reported their self-rated vision score. Binocular distance visual acuity was assessed. Based on the level of visual acuity and the self-reported vision score, participants were placed into concordant and discrepant groups.
Main Outcome Measures
Multinomial logistic regression models were used to examine the characteristics associated with concordant and discrepant groups.
Results
Black participants were more likely to be represented in the discordant group that reported good vision but had acuity worse than 20/40. In the multivariate analysis, a per year decrement in years of education received increased the odds of being in both discrepant groups, one that reported good vision but had a visual acuity worse than 20/40 (odds ratio, 1.21; P<0.0001) and the other discrepant group that reported bad vision but had a visual acuity of 20/40 or better (odds ratio, 1.04; P<0.0001). A per year decrement in years of education received also appeared to explain the excess risk of Black race in the discrepant group that reported good vision but had a visual acuity worse than 20/40.
Conclusions
Given the socioeconomically driven discrepancies in self-reported vision status, self-reported vision status should be used cautiously in surveillance surveys especially when assessing vision inequalities between socioeconomic groups.
Self-reported health data are widely used as an inexpensive measure of objective health status. However, self-reported measurements of health are not complete surrogates of objective health status.1 Rather, self-reported measurements may vary systematically with non-physiological factors even among persons with similar physiological impairment. Defining these characteristics is essential in determining the appropriate use of self-report data as a screening tool, in both clinical and research settings, and in national surveillance.
For example, racial differences in self-reported health have been observed in several patient populations.2–8 These racial differences persist among patients with similar physical impairment and after controlling for other factors.4–7 One hypothesis for these differences is that older Black adults are more pessimistic about health than their White counterparts, and therefore tend to evaluate health more negatively, even when their health status is similar.8 One interpretation of this finding is that self-reported health data may provide information with regard to health status and non-physiological factors, such as race and ethnicity, as opposed to serving as a direct measurement of health status alone. To our knowledge, “health pessimism” as it relates to vision has not been well described.
Further, the correlation between self-rated vision and objective measurements of vision is not well understood. Visual impairment is complex and dynamic. The potential for non-physiological factors to influence the accuracy of self-rated vision is great. Yet, self-rated vision is used on a number of national surveillance surveys often as a direct measure of vision status.9 Ultimately, this may lead to a mischaracterization of disparities in visual disability among different socioeconomic groups if there are differences in self-rated vision that are not correlated as well with an objective measure.
The goal of this study is to examine the association between self-rated vision and objective measurements of vision by race and other factors. We hypothesize that a racial discrepancy exists in the association between self-rated vision and objective measurements of vision, and that this discrepancy exists because, as is the tendency with self-reported health, Blacks will rate their vision lower although they may have similar levels of objectively measured visual impairment as compared to Whites in their similar cohort.
Methods
Subjects
The study sample consisted of 2520 individuals enrolled in the Salisbury Eye Evaluation (SEE) Study. The Johns Hopkins Institutional Review Board approved all protocols. Data collection began in 1993. All subjects gave written informed consent before participation. A detailed description of the sampling procedure has been described previously.10,11 Briefly, the sample was selected from the Health Care Financing Administration (HCFA) Medicare eligibility list and included only individuals between 65 and 84 years of age as of July 1, 1993 living in the Salisbury, MD metropolitan area. This sample included 100% of identified African American residents and a random age-stratified sample of 58% of identified white residents. No other ethnic groups were on the list. To be eligible for the study, the participant had to be able to travel to the clinic for vision tests and score greater than a 17 on the Mini-Mental Status Exam (MMSE).12 Eligible participants participated in a 2-hour in-home interview followed by a 4- to 5- hour clinic examination. Of those who were eligible, 65% participated. Details on the differences between participants and refusals has been described elsewhere.11
Self-Reported Health, Self-Rated Vision, and Baseline Variables
During the home interview, participants were asked how they would rate their current vision with glasses on, if they wore glasses, on a scale of 0=blindness to 10=excellent vision. The MMSE was also administered, as well as a standardized home questionnaire which included sections on years of education received, self-reported health status, self-reported vision function (Activities of Daily Vision Scale), and medical history including co-morbidities, food frequency, use of alcohol, and cigarette smoking.
To assess self-reported health status, participants were asked to rate their health as excellent, very good, good, fair, or poor. Co-morbidities included physician-diagnosed arthritis, broken hip, cardiovascular disease, hypertension, diabetes, emphysema, asthma, Parkinson’s disease, cancer, and stroke. Depression was assessed with the depression scale of the General Health Questionnaire as part of the clinical examination.
The clinical examination included self- reported measures of function assessed using the Activities of Daily Living (ADL) and Instrumental Activities of Daily Living (IADL) scales. It also included performance-based measures of function, risk factors questionnaires, questions on balance and falls, blood extraction for diabetic testing and levels of various micro nutrients, assessment of medical conditions, other than visual problems, that could affect function, an ophthalmologic exam, ocular photographs, dry eye testing, and visual function testing.
Visual Acuity
Detailed descriptions of the vision tests have been published elsewhere.10 Trained technicians using strict forced-choice testing procedures administered all vision tests.
Distance visual acuity was tested using the Early Treatment Diabetic Retinopathy Study (ETDRS) charts.13 The acuity charts were trans-illuminated with a light box (The Lighthouse New York, NY) that maintains chart luminance at 130 cd/m2. Acuity was measured monocularly and binocularly, with habitual refractive correction and best correction after subjective refraction. Visual acuity was scored as the total number of letters read correctly and converted to log10 minimum angle resolution (logMAR).14 Participants who failed to read any letters were arbitrarily assigned an acuity of 1.7 logMAR (20/1000).
Data Analysis
Based on the level of visual acuity and the self reported vision score, we created one concordant and two discordant groups as follows: 1) Concordant group: those with visual acuity 20/40 or better who graded their vision as 8 or more, and those with visual acuity worse than 20/40 who graded their vision as 7 or less; 2) Discordant group 1: those with visual acuity worse than 20/40 who graded their vision as 8 or more (impaired visual acuity reporting good vision); and 3) Discordant group 2: those with vision 20/40 or better who graded their vision as 7 or less (good visual acuity reporting impaired vision),.
Our hypothesis concerned racial differences, so we present baseline characteristics of the cohort by race; logistic regression models were used to test for age and gender adjusted significant differences between Blacks and Whites. Race specific Spearman correlation coefficient and corresponding 95% Confidence Intervals (CI) were calculated to estimate the strength of the association between the self-reported vision score and presenting binocular visual acuity.
We then modeled all relevant characteristics for the outcomes of being in the discordant groups. Age-adjusted multinomial logistic regression models were used. Odds ratios and 95% CI are presented using the concordant group as the reference category. The likelihood ratio test was used to test for significance of the global effect of individual covariates on the model. The multivariate model was built using a backward elimination strategy: we started with a model including all the variables that were significant at 0.15 level in the age –adjusted analysis. Among variables whose p-value was greater than 0.05, we removed from the model the one that had the highest p-value. We proceeded iteratively until all variables in the model had associated p-values of 0.05 or less.
Results
Among the SEE participants, Black participants were significantly more likely to be female and to have significantly less years of education (Table 1). White participants had an average of 11.8 years of education while Black participants had an average of 9.4 years of education, and less than 10% graduated from High School. Black and White participants did not significantly differ in age.
Table 1.
Baseline Characteristics of Participants by Race
| Baseline Characteristics | Whites N=1854 |
Blacks N=666 |
p-value |
|---|---|---|---|
| Demographics | |||
| Age in years (mean(sd)) | 73.6 (5.1) | 73.3 (5.1) | 0.19 |
| % Female | 56.4 | 61.9 | 0.011* |
| Years of education (mean(sd)) | 11.8 (3.1) | 9.4 (3.6) | <0.001** |
| Health Status | |||
| % Excellent | 12.4 | 5.4 | |
| % Very good | 27.1 | 18.9 | |
| % Good | 36.7 | 33.1 | <0.001** |
| % Fair | 20.6 | 37.9 | |
| % Poor | 3.1 | 4.7 | |
| Number of co-morbidities (mean(sd)) | 2.4 (1.6) | 2.3 (1.5) | 0.04** |
| % With depression symptoms | 8.4 | 12.4 | 0.002** |
| % Need help with ADL | 2.7 | 6.9 | <0.001** |
| % Need help with IADL | 11.0 | 15.8 | <0.001** |
| Vision status | |||
| Self Report of Vision [grade 0–10] (mean(sd)) | 7.7 (1.9) | 7.7 (2.2) | 0.48** |
| Presenting binocular visual acuity Mean LogMAR (sd) | 0.02 (0.19) | 0.07 (0.26) | <0.001** |
Age adjusted;
Age and gender adjusted. sd = standard deviation. ADL=activities of daily living. IADL=instrumental activities of daily living. LogMAR = logarithm of the minimum angle of resolution.
The baseline characteristics of the races were compared using logistic models with race as the dependent variable, and each of the baseline characteristics as the independent variables. The Wald test was used to determine the level of significance adjusting for age alone or age and gender where specified.
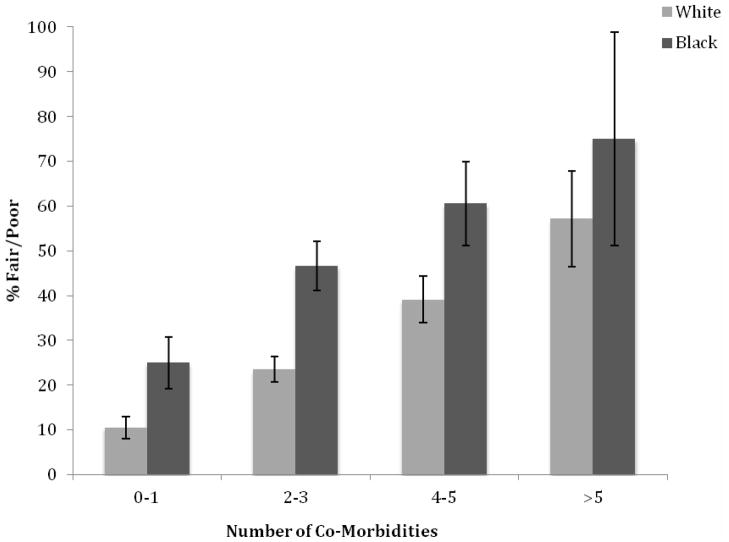
A significantly greater percentage of Black participants reported depressive symptoms and reported needing help with ADL and IADL when compared to White participants. Black participants were also significantly more likely to rate their health status as fair or poor and less likely to rate their health status as excellent, very good, or good. However, Black participants reported having significantly less co-morbidities than White participants. In fact, given a similar number of co-morbidities, a larger percentage of Black participants rated their health status as fair or poor when compared to White participants except when comparing participants with the highest number of co-morbidities (>5) (Figure 1).
Figure 1. Percentage of Participants who rated their Health Status as Fair or Poor by Number of Co-morbidities and Race.
For each co-morbidity level and each race, the proportion who reported fair to poor heath is presented, 95% confidence intervals around this proportion were estimated.
Black participants had significantly worse presenting visual acuity than White participants. Black participants had a mean presenting visual acuity of 0.07 logMAR (SD=of 0.26), while White participants had a mean presenting visual acuity of 0.02 logMAR (SD=0.19). However, Black and White participants did not significantly differ in how they rated their vision. Both Black and White participants had a mean self-rated vision score of 7.7 out of 10. The correlation between self-reported vision score and visual acuity was significantly stronger for White participants than it was for Black participants. The Spearman correlation coefficient was −0.29 for White participants (95% CI= −0.24 to −0.33) and −0.20 for Black participants (95% CI= −0.12 to −0.27).
Simple age-adjusted associations between these characteristics and discrepancies between self-reported visual status and visual acuity were examined by comparison with those who were concordant (Table 2). Older age and a per year decrement in years of education received were associated with increased odds of being in both discrepant groups compared to the concordant group. Being female, having symptoms of depression, having a per unit increase in number of co-morbidities, or needing help with IADL were associated with increased odds of being in the discrepant group that reported bad vision but had a visual acuity of 20/40 or better. Being Black increased the odds more than two fold of being in the discrepant group that reported good vision but had a visual acuity worse than 20/40.
Table 2.
Characteristics Associated with Discrepancies in the Concordance of Self-Reported Vision Status and Visual Acuity (Age adjusted)
| Characteristics | Age adjusted OR (95% CI) | p-value | |
|---|---|---|---|
| Report Good Vision & VA worse than 20/40* | Report Bad Vision & VA 20/40 or better* | ||
| Age (per year increment) | 1.11 (1.05,1.17) | 1.04 (1.03,1.06) | <0.0001 |
| Blacks/Whites | 2.53 (1.37,4.69) | 1.11 (0.93,1.38) | 0.008 |
| Females/Males | 1.14 (0.61,2.13) | 1.24 (1.04,1.48) | 0.05 |
| With depression symptoms | 1.15 (0.40,3.31) | 1.53 (1.15,2.03) | 0.014 |
| Number of co-morbidities (per unit increment) | 1.09 (0.90,1.31) | 1.15 (1.09,2.22) | <0.0001 |
| Need help with IADL | 0.88 (0.34,2.32) | 1.59 (1.23,2.06) | <0.002 |
| Years of education (per year decrement) | 1.22 (1.12,1.33) | 1.04 (1.02,1.08) | <0.0001 |
Reference category: Report good vision: vision grades 8–10. OR=odds ratio. CI=confidence interval. IADL=instrumental activities of daily living.
The p-values presented are part of the type III analysis and correspond to the global effect of individual covariates in the multinomial logistic regression model.
Multivariate analysis, controlling for all significant characteristics associated with discrepancies, were examined by comparison with those who were concordant (Table 3). Again, older age and a per year decrement in years of education received was associated with increased odds of being in both discrepant groups compared to the concordant group. Being female, having a per unit increase in number of co-morbidities, or needing help with IADL were still associated with increased odds of being in the discrepant group that reported bad vision but had a visual acuity of 20/40 or better. There was no longer a statistically significant association between having symptoms of depression and being in either discrepant group when compared to the concordant group. Also, there was no longer a statistically significant association between race and being in the discrepant group that reported good vision despite a visual acuity of 20/40 or worse.. An interaction between race and education was explored and no statistically significant interaction was found.
Table 3.
Characteristics Associated with Discrepancies in the Concordance of Self-Reported Vision Status and Visual Acuity (Multivariate analysis)
| Characteristics | Multivariate analysis OR (95% CI) | p-value | |
|---|---|---|---|
| Report Good Vision & VA worse than 20/40* | Report Bad Vision & VA 20/40 or better* | ||
| Age (per year increment) | 1.10 (1.04,1.17) | 1.03 (1.02,1.05) | <0.0001 |
| Blacks/Whites | 1.65 (0.85, 3.20) | 1.05 (0.85,1.29) | 0.33 |
| Females/Males | 1.20 (0.64,2.26) | 1.24 (1.04,1.48) | 0.05 |
| Number of co-morbidities (per unit increment) | 1.10 (0.90,1.34) | 1.14 (1.07,1.20) | <0.0001 |
| Need help with IADL | 0.60 (0.22, 1.62) | 1.32 (1.02, 1.63) | 0.05 |
| Years of education (per year decrement) | 1.21 (1.10,1.32) | 1.04 (1.01,1.06) | <0.0001 |
Reference category: Report good vision: vision grades 8–10. OR=odds ratio. CI=confidence interval. IADL=instrumental activities of daily living.
The p-values presented are part of the type III analysis and correspond to the global effect of individual covariates in the multinomial logistic regression model.
A sensitivity test was performed by alternatively defining good vision as a vision grade of 6 or higher. The results were unchanged (data not shown).
Discussion
We had hypothesized that the construct of health pessimism, more prevalent in Blacks, would apply to self-rated vision when compared to standard measure of distance acuity. That is, given a similar level of visual impairment, Black participants would be more likely to rate their vision poorer than would the White participants. However, if anything, Black participants exhibited “vision optimism” rather than health pessimism. Although Black participants had worse mean presenting visual acuity than White participants, the mean self-rated vision grade for the two groups was the same. Further analysis demonstrated that the correlation between presenting visual acuity and self reported vision was significantly weaker among Black participants as compared to their White counterparts. However, in the multivariate analysis, less education appeared to attenuate the association between race and vision optimism. While Black participants were 65% more likely than White participants to be in the vision optimism group, the association was no longer significant once education was included in the model.
In part the attenuation may reflect the strong association between Black race and lower levels of education in this age group, which left few blacks in the group with higher education. However, clearly education is also an important predictor of being in either discrepant group. It is possible that whites with low education tend to be in the group who are vision pessimistic, and blacks with low education in the group with vision optimism. We tested for an interaction, recognizing we were underpowered, and did not find evidence of an interaction. This finding deserves further attention.
It is unlikely that education is the sole explanation for vision optimism among Black participants. If it were, we would have expected that Black participants would be over represented in both groups that were discrepant in the concordance of visual acuity and self-rated vision, as were those with low numbers of years of education. That Black participants were largely over represented only in the group that was vision optimistic could mean that other factors besides education may also be important in the vision optimism of Black participants.
It is not entirely clear why receiving less education would make an individual more likely to be generally discrepant in the concordance of self-reported vision status and visual acuity. It has been previously reported that the repercussions of health problems on self-rated health are worse in those who are more highly educated.18 Previous studies have also demonstrated that the expectations regarding health and quality of life were higher for those who have received more education and those with higher expectations about their quality of life were more frequently dissatisfied.19, 20 Similarly, one hypothesis to explain our findings is that the expectations for having good vision also increase with level of education. Those who have received less education have lower expectations regarding their vision, are more easily satisfied, and therefore are more likely to be vision optimistic. This, however, does not explain why those with less education are also more likely to be in the discrepant group that reports bad vision while having good visual acuity. Instead, it is known that in the most general sense, self-reported measurements can be seen as reflecting an individual’s objective health status as well as that individual’s health knowledge, attitudes, and beliefs.21 Education influences an individual’s health knowledge and more highly educated individuals are more aware of their health or vision problems in terms of current limitations and future risk.18 Therefore, a greater understanding of their own objective vision status may in part explain why those with more education are more likely to be in the group concordant for self reported and objectively measured vision and vice versa.
This finding of education and race and discordant groups deserves further attention, especially to understand why less years of education make individuals more likely to be generally discrepant in the concordance of self reported vision status and visual acuity. At present, it is not possible to determine in which discrepant group those with less education will fall.
In the SEE population, as in other population studies, we found evidence of differences in general rating of health. Black participants were more likely than White participants to rate their health as fair or poor rather than good, very good, or excellent. This was true even though White participants had significantly more co-morbidities. In fact, given a similar number of co-morbidities, a larger percentage of Black participants rated their health status as fair or poor except when comparing participants with the highest number of co-morbidities (>5). This observation is consistent with previous literature and other patient populations, and supports the finding of racial differences in health pessimism.2–8 In part, this finding may reflect under ascertainment of co-morbid conditions in the Black population, which while formally undiagnosed, would still manifest as symptoms and result in rating of poor health. Additionally, a larger percentage of Black participants reported symptoms of depression and needed help with ADLs and IADLs. These factors may contribute to why Black participants were found to be health pessimistic. Nonetheless, health pessimism is a significant finding, as prospective studies have found that, given similar objective health status, those who rate their health as poor have worse health in the future and have a significant increase in the risk of death.15–17
We chose to measure distance acuity for this study, because that is the measure most often used to assess eye health in populations. A potential limitation of the current study is that we did not assess near vision, which may well be associated with self-rated vision and therefore also explain some of the discrepancy between self-rated vision and distance visual acuity. Since near vision was not assessed, further study is warranted. Also, our study population did not include the “oldest” old, those over age 84 and can be generalized only to those from 65 to 84 years of age.
In conclusion, there is strong evidence of socioeconomic differences, racial and educational in particular, that effect the utility of using self-rating of vision as a proxy for measuring distance visual acuity. Black participants were vision optimistic when asked to rate their vision status, and this was in part explained by a lower mean years of education received among Black participants. Furthermore, a per year decrement in years of education received was associated with increased odds of being generally discrepant in the concordance of self-reported vision status and visual acuity. Given the socioeconomically driven discrepancies in self-reported vision status, self-reported vision status should be used cautiously in surveillance surveys especially when assessing vision inequalities between socioeconomic groups.
Acknowledgments
Financial Support: National Institute on Aging Grant AG02513. Dr. West is the recipient of a Senior Scientific Investigator award from Research to Prevent Blindness
Footnotes
Conflict of Interest: The author(s) have no proprietary or commercial interest in any materials discussed in this article
Meeting Presentation: The Association for Research in Vision and Ophthalmology Annual Meeting, May, 2011.
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
References
- 1.Singh-Manoux A, Martikainen P, Ferrie J, et al. What does self rated health measure? Results from the British Whitehall II and French Gazel cohort studies. J Epidemiol Community Health. 2006;60:364–72. doi: 10.1136/jech.2005.039883. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Boyington JE, Howard DL, Holmes DN. Self-rated health, activities of daily living, and mobility limitations among black and white stroke survivors. J Aging Health. 2008;20:920–39. doi: 10.1177/0898264308324643. [DOI] [PubMed] [Google Scholar]
- 3.Thomas SB, Sansing VV, Davis A, et al. BARI 2D Study Group. Racial differences in the association between self-rated health status and objective clinical measures among participants in the BARI 2D trial. Am J Pub Health. 2010;100(suppl):S269–76. doi: 10.2105/AJPH.2009.176180. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Boardman JD. Health pessimism among black and white adults: the role of interpersonal and institutional maltreatment. Soc Sci Med. 2004;59:2523–33. doi: 10.1016/j.socscimed.2004.04.014. [DOI] [PubMed] [Google Scholar]
- 5.Borrell LN, Crawford ND. Race, ethnicity, and self-rated health status in the Behavioral Risk Factor Surveillance System survey. Hisp J Behav Sci. 2006;28:387–403. [Google Scholar]
- 6.Borrell LN, Dallo FJ. Self-rated health and race among Hispanic and non-Hispanic adults. J Immigr Minor Health. 2008;3:229–38. doi: 10.1007/s10903-007-9074-6. [DOI] [PubMed] [Google Scholar]
- 7.Spencer SM, Schulz R, Rooks RN, et al. Racial differences in self-rated health at similar levels of physical functioning: an examination of health pessimism in the health, aging, and body composition study. J Gerontol B Psych Sci Soc Sci. 2009;64:87–94. doi: 10.1093/geronb/gbn007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Ferraro KF. Are black older adults health-pessimistic? J Health Soc Behav. 1993;34:201–14. [PubMed] [Google Scholar]
- 9.Enhancing Public Health Surveillance of Visual Impairment and Eye Health in the United States. Atlanta, GA: Centers for Disease Control and Prevention; 2010. [Accessed June 25, 2011]. pp. 27–43. Available at: http://www.cdc.gov/visionhealth/pdf/surveillance_background.pdf. [Google Scholar]
- 10.Rubin GS, West SK, Munoz B, et al. SEE Project Team. A comprehensive assessment of visual impairment in a population of older Americans: the SEE Study. Invest Ophthalmol Vis Sci. 1997;38:557–68. [PubMed] [Google Scholar]
- 11.Munoz B, West S, Rubin GS, et al. SEE Project Team. Who participates in population based studies of visual impairment? The Salisbury Eye Evaluation Project experience. Ann Epidemiol. 1999;9:53–9. doi: 10.1016/s1047-2797(98)00026-x. [DOI] [PubMed] [Google Scholar]
- 12.Folstein MF, Folstein SE, McHugh PR. “Mini-mental state:” a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12:189–98. doi: 10.1016/0022-3956(75)90026-6. [DOI] [PubMed] [Google Scholar]
- 13.Ferris FL, III, Kassoff A, Bresnick GH, Bailey I. New visual acuity charts for clinical research. Am J Ophthalmol. 1982;94:91–6. [PubMed] [Google Scholar]
- 14.Bailey IL, Bullimore MA, Raasch TW, Taylor HR. Clinical grading and the effects of scaling. Invest Ophthalmol Vis Sci. 1991;32:422–32. [PubMed] [Google Scholar]
- 15.Idler EL, Benyamini Y. Self-rated health and mortality: a review of twenty-seven community studies. J Health Soc Behav. 1997;38:21–37. [PubMed] [Google Scholar]
- 16.Ferraro KF, Farmer MM, Wybraniec JA. Health trajectories: long-term dynamics among black and white adults. J Health Soc Behav. 1997;38:38–54. [PubMed] [Google Scholar]
- 17.Lyness JM, King DA, Conwell Y, et al. Self-rated health, depression, and one-year health outcomes in older primary care patients. Am J Geriatr Psychiatry. 2004;12:110–3. [PubMed] [Google Scholar]
- 18.Delpierre C, Lauwers-Cances V, Datta GD, et al. Using self-rated health for analysing social inequalities in health: a risk for underestimating the gap between socioeconomic groups? J Epidemiol Community Health. 2009;63:426–32. doi: 10.1136/jech.2008.080085. [DOI] [PubMed] [Google Scholar]
- 19.Brouwer WB, van Exel NJ. Expectations regarding length and health related quality of life: some empirical findings. Soc Sci Med. 2005;61:1083–94. doi: 10.1016/j.socscimed.2005.01.008. [DOI] [PubMed] [Google Scholar]
- 20.Ross CE, Van Willigen M. Education and the subjective quality of life. J Health Soc Behav. 1997;38:275–97. [PubMed] [Google Scholar]
- 21.Bailis DS, Segall A, Chipperfield JG. Two views of self-rated general health status. Soc Sci Med. 2003;56:203–17. doi: 10.1016/s0277-9536(02)00020-5. [DOI] [PubMed] [Google Scholar]