Abstract
Introduction
Obesity and associated metabolic disorders are a worldwide epidemic. Recent evidence suggests that the microbial community in the human intestine may play an important role in the pathogenesis of obesity. The aim of this study was to assess the differences in the composition of the intestinal microbiota between obese and normal weight Egyptian children and adults.
Material and methods
The study included 79 subjects among whom 51 were obese (23 children and 28 adults), and 28 were subjects of normal weight (17 children and 11 adults). Faecal samples were collected from all subjects. Total DNA was extracted from collected stool samples and submitted to conventional PCR for detection of Firmicutes and Bacteroidetes. All the studied group was subjected to clinical and anthropometric evaluation. Laboratory assessment of fasting glucose, high-sensitivity C-reactive protein (hsCRP) and lipid profile was performed.
Results
The proportions of the phyla Firmicutes and Bacteroidetes were statistically significantly increased in the obese group compared to the normal weight group (p < 0.001, p = 0.003 respectively). The study also found a statistically significant positive trend for higher hsCRP in subjects with positive Firmicutes (p = 0.004). However, no associations were found between positive Bacteroidetes and hsCRP.
Conclusions
The results of this study indicate that obesity in Egyptian children and adults is associated with compositional changes in faecal microbiota with increase in the phyla Firmicutes and Bacteroidetes. This could be considered when developing strategies to control obesity and its associated diseases by modifying the gut microbiota.
Keywords: obesity, gut microbiota, Firmicutes, Bacteroidetes, high-sensitivity C-reactive protein
Introduction
Obesity represents one of the five major health risks in modern societies with a frequency of more than 20% of the population in developed countries [1]. As a consequence of the expected dramatic increase in obesity prevalence rates, life expectancy may start to decrease for the first time in recent history due to numerous co-morbid disorders [2, 3].
The intestinal flora has been recently proposed as an environmental factor involved in the control of body weight and energy homeostasis [4-8]. The human intestine contains a large variety of microorganisms, consisting of at least 1014 bacterial cells and up to 500-1000 different species [9]. As a whole this represents overall more than 100 times the human genome [9, 10], and is called the “metagenome”. Thus, the intestinal flora can be considered as an “exteriorized organ” which contributes to our homeostasis with multiple, highly diversified functions. Studies have shown that the gut microbiota is dominated by 2 bacterial phyla, the gram-negative Bacteroidetes and the gram-positive, low GC% Firmicutes [11, 12], with other phyla represented at subdominant levels including the Actinobacteria, Fusobacteria and Verrucomicrobia phyla [11]. Within these phyla the dominant bacterial groups include the Clostridium coccoides-Eubacterium rectale group, Clostridium leptum group (Firmicutes), Bacteroides-Prevotella species (Bacteroidetes), Bifidobacterium and Atopobium genera (both Actinobacteria) [13]. Firmicutes are in the class Bacillus [14], which is rare in the human or mouse gut microbiota; none is a member of the Clostridium XIV class, which contains the most abundant representatives of this division in the distal guts of mice and humans. Hence, the physiological contributions of Firmicutes to the intestinal ecosystem, and to fuel partitioning, are unclear [14].
Diet-induced and genetically obese mice (ob/ob or db/db) showed a significant upregulation of expression of Toll-like receptors 1 to 9 in adipocytes and pre-adipocytes along with higher cytokine production upon stimulation [15]. In particular, it is known that Toll-like receptor 4 (TLR-4) can be activated by both lipopolysaccharide (LPS) and dietary saturated fatty acids inducing upregulation of common intracellular inflammatory pathways, such as JNK and NF-κB in adipocytes and macrophages, related to the induction of insulin resistance and increased adiposity [16]. Recently, metabolic endotoxaemia, characterized by an increase in serum LPS levels, has been demonstrated to be an inflammatory factor, causing body weight gain, insulin resistance, and diabetes in high-fat fed animal models [17-19].
C-reactive protein (CRP) is an acute-phase protein that is a sensitive marker for systemic inflammation. Several inflammation-related diseases such as respiratory disease, rheumatoid arthritis, diabetes mellitus, and cardiovascular disease have been associated with elevated CRP concentrations. Moreover, recent studies have reported a positive relation between body mass index and CRP concentrations [20-22]. In obesity, an elevated CRP level concentration is explained by increased interleukin-6 expression in adipose tissue and its release into the peripheral circulation. The role of the gut microbiota in modulating plasma LPS levels, which triggers the inflammatory tone and the onset of obesity and type 2 diabetes, is under evaluation [23]. More studies are needed to unravel how changing gut microbiota impacts on the development of obesity and related metabolic alterations. The idea that gut microbial diversity is linked to obesity deserves exploration in humans, because it may yield new treatment strategies for this growing worldwide threat to our health.
The aim of this study was to assess the differences in the composition of the intestinal microbiota between obese and normal weight Egyptian children and adults by comparing the Firmicutes and Bacteroidetes frequency in the stool and its correlation with high-sensitivity C-reactive protein (hsCRP), as a marker of inflammation, and also the correlation with the amount of dietary fat and carbohydrate intake.
Material and methods
All subjects were recruited between September 2008 and December 2009 from outpatient clinics at the National Research Centre (NRC). Out of 120 subjects randomly chosen, only 79 were included in this study, among whom 51 were obese (23 children and 28 adults), and 28 were subjects of normal weight (17 children and 11 adults). Cases with hepatic disease, hypertension, asthma, infection, tumour, febrile conditions (or had febrile conditions within the previous 2 months), congestive heart failure, diseases affecting the gut microbiota, recent antibiotic intake and other acute inflammatory diseases were excluded from this study. Obesity in children and adults was considered as body mass index (BMI) ≥ 30 kg/m2 and overweight as BMI ≥ 25 kg/m2 and < 30 kg/m2 [24]. Corresponding normative data for Egyptian children and adolescents were used. Overweight was defined as between the 90th and 95th BMI percentiles and obesity as > 95th percentile in both children and adolescents.
A detailed medical and family history was obtained from all subjects and a complete physical examination was performed, including anthropometric parameters (height, weight), fatness indices (BMI, standard deviation score-BMI – SDS-BMI, and basal blood pressure).
Nutritional evaluation
Twenty-four-hour dietary recalls for three successive days were done for all cases and were evaluated according to the food pyramid guidelines. Food frequency questionnaires (FFQs) ask about the usual frequency of consumption of a list of foods mainly to evaluate fat and carbohydrate intake.
Stool samples were collected from all subjects and were diluted as 20% using sterile EDTA (50 mM), then all samples were purified from stool deprise by centrifugation at 5000 rpm for 10 min [25].
DNA extraction
DNA was extracted from diluted stool samples using Wizard Genomic DNA Purification Kit (Promega, Cat. No. A1120), according to the manufacturer’s instructions, and extracted DNA was stored at –20°C for detection of Bacteroidetes and Firmicutes by PCR [25, 26].
Polymerase chain reaction
Oligonucleotide primers
For amplification of selected DNA segments of Bacteroidetes and Firmicutes, two pairs of oligonucleotide primers were used as detected in stool samples using primers reported by Dick and Field, 2004 and Scupham et al., 2006, respectively [25, 27]. The primer sequences were: BactFA ACGCTAGCTACAGGCTTAACA (Forward) and BactR ACGCTACTTGGCTGGTTCA (Reverse), for Bacteroidetes, and FirmF GCGTGAGTGAAGAAGT (Forward) and FirmR CTACGCTCCCTTTACAC (Reverse) for Firmicutes.
PCR amplification
Polymerase chain reaction amplification was carried out in 50 µl reaction mixture containing 10 µl of DNA, 5 µl of 10 × PCR buffer, 4 µl of MgCl2 (25 mM), 0.5 µl (5 U/µl) of Go Taq Flexi DNA Polymerase (Promega Cat. No. M8301) [27], 1 µl of BactF upstream primer (50 pmol/µl), 1 µl of BactR downstream primer (50 pmol/µl), for Bacteroidetes detection or 1 µl of FirmF upstream primer (50 pmol/µl), and 1 µl of FirmR downstream primer (50 pmol/µl), for Firmicutes detection, and 4 µl of dNTPs (10 mM each), and 24.5 µl of DEPC-treated water. The PCR amplification profile was an initial denaturation step of 5 min at 95°C followed by 40 cycles of denaturation at 94°C for 45 s, annealing at 62°C for 45 s (for Bacteroidetes amplification), while the annealing was 58°C at 45 s (for Firmicutes amplification), and extension at 72°C for 1.5 min, with a final extension step of 10 min at 72°C. The PCR thermal cycling was done using a Biometra PCR system and the expected PCR product characteristic for Bacteroidetes was 396 bp and that characteristic for Firmicutes was 161 bp.
Gel electrophoresis
The amplified PCR products were electrophoresed through 1.5% agarose gel in Tris acetate/EDTA (TAE) buffer by using 100 V for 1 h, and the PCR product bands were visualized by staining with 0.01% ethidium bromide (0.5 µg/ml). Polymerase chain reaction product bands were visualized under UV light using a UV transilluminator and photos were taken using a gel documentation system [28].
Blood samples
Five ml of blood were drawn from the antecubital vein under aseptic precautions from fasting (for 12-14 h) subjects. After centrifugation serum was collected from each subject to evaluate inflammatory markers hs-CRP, lipid profile (total cholesterol, HDL cholesterol, LDL cholesterol, triglyceride). 1 – lipid analysis: Lipid assays in sera were determined by chemistry analyzer Olympus AU 400. 2 – the serum hs-CRP assay was based on the chemiluminescence technique. Determination of hs-CRP concentrations was performed with the Diagnostic Products Immulite 2000 analyzer (Block Scientific, Nutley, NJ); assay limits ranged from below 0.1 mg/l to above 10.0 mg/l.
Statistical analysis
Statistical analysis was performed using the software SPSS 12.0 (SPSS: Chicago, IL). Variables were expressed as mean ± standard deviation (SD). Mean values were compared among subjects using Student’s t test and ANOVA was used to compare variables between all groups. For comparing categorical data, χ2 test was performed. The exact test was used instead when the expected frequency was less than 5. Spearman’s correlation coefficient rho was used to correlate between non-normally distributed continuous variables. A probability value (p value) less than 0.05 was considered statistically significant.
Results
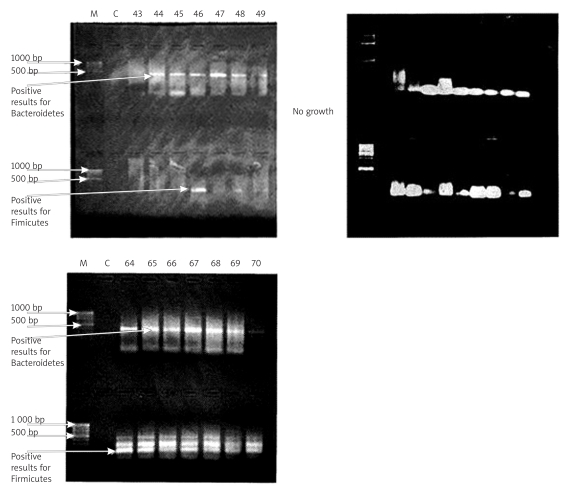
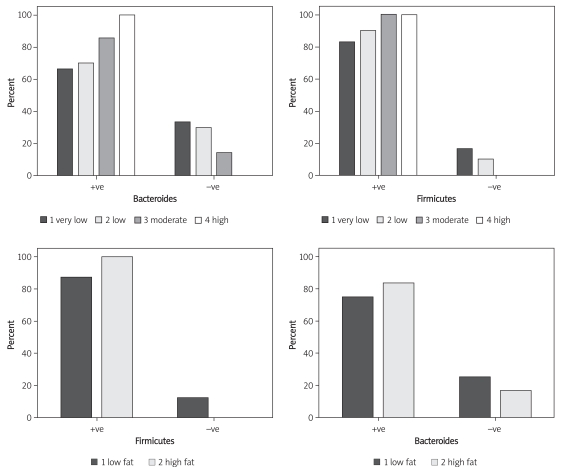
The results of PCR product bands for Bacteroidetes and Firmicutes by the gel documentation system of some cases are shown in Figure 1. Distribution of Bacteroidetes and Firmicutes was significantly increased in the obese group compared to the normal weight group (p = 0.003, p < 0.001 respectively) (Table I, II). Only 21 subjects had one positive bacteria (13 were positive for Firmicutes and 8 for Bacteroidetes). Table III shows the means and SDs of different variables and their statistical significance in both groups. Both cholesterol and hsCRP were significantly higher in obese individuals (p = 0.03, p = 0.05 respectively). Table IV shows the cross-tabulation between Firmicutes and Bacteroidetes in children and adults. Firmicutes showed a statistically significant increase in the adult group (p = 0.031). As regards the results of dietary analysis, subjects were divided into low and high fat intake. According to carbohydrate intake they were divided into four groups. The fourth group had the highest carbohydrate intake. We could not correlate changes in gut microbiota with fat or carbohydrate intake. Interestingly, the study found a trend for subjects with high fat intake to have positive Firmicutes, and those with the highest carbohydrate intake to have positive Bacteroidetes and Firmicutes (Figure 2). The study also showed a significant positive trend for higher hsCRP in subjects with positive Firmicutes (p = 0.004), as shown in Table V.
Figure 1.
Results of the PCR product bands for Bacteroidetes and Firmicutes by gel documentation system of some cases
Table I.
Distribution of Bacteroidetes and Firmicutes in obese and normal weight subjects
| Bacteroidetes | Total | Firmicutes | Total | ||||
|---|---|---|---|---|---|---|---|
| 1.00 | 2.00 | 1.00 | 2.00 | ||||
| Obesity | Count | 43 | 9 | 52 | 45 | 7 | 52 |
| % Within obesity | 82.7% | 17.3% | 100.0% | 86.5% | 13.5% | 100.0% | |
| Normal weight subjects | Count | 13 | 14 | 27 | 12 | 15 | 27 |
| % Within normal weight | 48.1% | 51.9% | 100.0% | 44.4% | 55.6% | 100.0% | |
Table II.
χ2 Tests for Bacteroidetes and Firmicutes in obese and normal weight subjects
| Asymp. sig. (2-sided) | Exact sig. (2-sided) | Exact sig. (1-sided) | Asymp. sig. (2-sided) | Exact sig. (2-sided) | Exact sig. (1-sided) | |
|---|---|---|---|---|---|---|
| Bacteroidetes | Firmicutes | |||||
| Pearson χ2 | 0.001 | < 0.001 | ||||
| Continuity correction | 0.003 | < 0.001 | ||||
| Likelihood ratio | 0.002 | < 0.001 | ||||
| Fisher’s exact test | 0.003 | 0.002 | < 0.001 | < 0.001 | ||
| Linear-by-linear association | 0.001 | < 0.001 | ||||
| N of valid cases | 0.001 | < 0.001 | ||||
Table III.
Comparison between the obese and normal weight groups
| Obesity | Mean | Standard deviation | Sig. (2-tailed) | |
|---|---|---|---|---|
| FBS | 1 | 93.07 | 21.82 | 0.426 |
| 2 | 89.83 | 11.04 | 0.419 | |
| Cholesterol | 1 | 197.93 | 37.04 | 0.038 |
| 2 | 180.91 | 34.65 | 0.037 | |
| Triglyceride | 1 | 112.31 | 38.68 | 0.127 |
| 2 | 96.45 | 52.97 | 0.137 | |
| HDL | 1 | 41.11 | 8.16 | 0.624 |
| 2 | 42.10 | 9.83 | 0.629 | |
| LDL | 1 | 131.76 | 131.76 | 0.143 |
| 2 | 119.72 | 33.34 | 0.139 | |
| HsCRP | 1 | 6.43 | 10.31 | 0.053 |
| 2 | 2.35 | 3.31 | 0.036 | |
| BMI | 1 | 34.82 | 5.84 | 0.000 |
| 2 | 21.85 | 2.66 | 0.000 |
1 – obese group, 2 – normal weight group
FBS – fasting blood glucose, HDL – high density lipoprotein, LDL – low density lipoprotein, HsCRP – high-sensitivity C-reactive protein, BMI – body mass index,
p is significant < 0.05
Table IV.
Firmicutes and Bacteroidetes in children and adults
| Firmicutes | Total | Bacteroidetes | Total | |||||
|---|---|---|---|---|---|---|---|---|
| 1 (+ve) | 2 (-ve) | 1 (+ve) | 2 (-ve) | |||||
| Age group | 1 – children | Count | 22 | 18 | 40 | 27 | 13 | 13 |
| % Within age | 55.0% | 45.0% | 100.0% | 67.5% | 32.5% | 100.0% | ||
| 2 – adults | Count | 31 | 8 | 39 | 29 | 10 | 39 | |
| Adult | % Within age | 79.5% | 20.5% | 100.0% | 74.4% | 25.6% | 100.0% | |
Figure 2.
Relation between Firmicutes and Bacteroides and fat or carbohydrates intake
Table V.
HsCRP in positive and negative Firmicutes and Bacteroidetes subjects
| HsCRP | N | Mean [mg/l] | Standard deviation | Sig. (2-tailed) | |
|---|---|---|---|---|---|
| Firmicutes | -ve | 11 | 1.3745 | 1.12117 | 0.004 |
| +ve | 50 | 5.3426 | 4.91056 | ||
| Bacteroidetes | -ve | 14 | 4.0264 | 8.02824 | 0.759 |
| +ve | 47 | 4.8060 | 8.28610 |
Discussion
Obesity is now characterized by a cluster of several metabolic disorders, and by low grade inflammation. The evidence that the gut microbiota composition can be different between healthy and obese and type 2 diabetic patients has led to the study of this environmental factor as a key link between the pathophysiology of metabolic diseases and the gut microbiota. Techniques based on the PCR are commonly used and provide rapid qualitative information on the composition of the intestinal microbiota [29]. Qualitative changes of the gut microbiota according to gender and species are well known and there are wide interpersonal variations in gut microbiota as a result of host genetic and environmental factors (e.g. mother’s microbiota, birth place, diet, and living conditions). Our study revealed that the proportions of the phyla Firmicutes and Bacteroidetes were statistically significantly increased in the obese group compared to the normal weight group (p < 0.001, p = 0.003 respectively). Results obtained in both rodents and humans suggest that obesity is associated with an altered composition of gut microbiota. Turnbaugh et al. (2009) observed wide shifts of the two major phyla: obese are characterized by more Firmicutes versus lean individuals; some authors show a drop in Bacteroidetes upon obesity [30], whereas other authors show no change or even an increase of Bacteroidetes in overweight [30-33]. This highlights the danger of generalizing observations of changes in microbiota composition from one population to another.
To date, 73 genomes of members of Firmicutes have been fully or partially sequenced. Interestingly, hydrogen-producing members of the family Prevotellaceae within the Bacteroidetes phylum, as well as certain Firmicutes, were more prominent in microbiota of obese individuals. This is believed to accelerate fermentation of otherwise indigestible carbohydrates, thereby leading to increased acetate production and subsequently higher energy absorption [34]. A question remains open: are the changes in gut microbiota in overweight or obese individuals due to the obesity per se, or due to changes in nutritional habits in obese people?
To explore the roles of diet on intestinal microbial ecology, dietary records were analysed for carbohydrate and fat contents. We could not correlate changes in gut microbiota with fat or carbohydrate intake. Interestingly, the study showed a trend for subjects with high fat intake to have positive Firmicutes, and those with the highest carbohydrate intake to have positive Bacteroidetes and Firmicutes. Other studies have correlated changes in gut microbiota with carbohydrate intake [35]. Data obtained in animals suggest that a high-fat diet – and not the obese state per se – can modulate microbiota composition towards an increase in Firmicutes and a proportional decrease in Bacteroidetes [36]. This highlights the likelihood of external factors such as diet, and potentially host factors, in modulating the microbiota.
Another point remains to be elucidated: could we attribute the low grade inflammatory process observed in obese subjects to changes in the gut bacteria? Our study showed that hsCRP was significantly higher in obese individuals (p = 0.05). The study also showed a significant positive trend for higher hsCRP in subjects with positive Firmicutes (p = 0.004). The role of the gut microbiota in modulation of plasma lipopolysaccharide (LPS) levels, which triggers the inflammatory tone and the onset of obesity, might be possible. Cani et al. (2007) have shown that subcutaneous infusion of LPS can cause weight gain and insulin resistance in mice without altering energy intake [37]. In accordance with this, mice lacking Toll-like receptor 4 (TLR4), which recognizes LPS, are resistant to diet-induced obesity and insulin resistance [38].
In conclusion, our data support the key idea that the gut microbiota can contribute to the pathophysiology of obesity. This could be considered when developing strategies to control obesity and its associated diseases by modifying the gut microbiota.
References
- 1.World Health Organization. The world health report 2002. Reducing risks, promoting healthy life. WHO, Geneva. 2002.
- 2.Olshansky SJ, Passaro DJ, Hershow RC, et al. A potential decline in life expectancy in the United States in the 21st century. N Engl J Med. 2005;352:1138–45. doi: 10.1056/NEJMsr043743. [DOI] [PubMed] [Google Scholar]
- 3.Vishal S, Faheem A, Chul W, et al. Impact of morbid obesity on pulmonary function. Arch Med Sci. 2008;4:66–70. [Google Scholar]
- 4.Flint HJ, Bayer EA, Lamed R, White BA. Polysaccharide utilization by gut bacteria potential for new insights from genomic analysis. Nature Rev Microbiol. 2008;6:121–31. doi: 10.1038/nrmicro1817. [DOI] [PubMed] [Google Scholar]
- 5.Gordon S. Microbial ecology: human gut microbes associated with obesity. Nature. 2006;444:1022–23. doi: 10.1038/4441022a. [DOI] [PubMed] [Google Scholar]
- 6.Turnbaugh PJ, Ley RE, Mahowald MA, Magrini V, Mardis ER, Gordon JI. An obesity associated gut microbiome with increased capacity for energy harvest. Nature. 2006;444:1027–31. doi: 10.1038/nature05414. [DOI] [PubMed] [Google Scholar]
- 7.Backhed F, Manchester JK, Semenkovich CF, Gordon JI. Mechanisms underlying the resistance to diet-induced obesity in germ-free mice. Proc Natl Acad Sci USA. 2007;104:979–84. doi: 10.1073/pnas.0605374104. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Backhed F, Ley RE, Sonnenburg JL, Peterson DA, Gordon JI. Host-bacterial mutualism in the human intestine. Science. 2005;30:1915–20. doi: 10.1126/science.1104816. [DOI] [PubMed] [Google Scholar]
- 9.Xu J, Mahowald MA, Ley RE, et al. Evolution of symbiotic bacteria in the distal human intestine. PLoS Biol. 2007;5:e156. doi: 10.1371/journal.pbio.0050156. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Xu J, Gordon JI. Inaugural article Honor thy symbionts. Proc Natl Acad Sci USA. 2003;100:10452–9. doi: 10.1073/pnas.1734063100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Eckburg PB, Bik EM, Bernstein CN, et al. Diversity of the human intestinal microbial flora. Science. 2005;308:1635–38. doi: 10.1126/science.1110591. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Lay C, Doré J, Rigottier-Gois L. Separation of bacteria of the Clostridium leptum subgroup from the human colonic microbiota by fluorescence-activated cell sorting or groupspecific PCR using 16S rRNA gene oligonucleotides. FEMS Microbiol Ecol. 2007;60:513–20. doi: 10.1111/j.1574-6941.2007.00312.x. [DOI] [PubMed] [Google Scholar]
- 13.Zoetendal E, Vaughan E, de Vos W. The microbial world within us. Mol Microbiol. 2006;59:1639–50. doi: 10.1111/j.1365-2958.2006.05056.x. [DOI] [PubMed] [Google Scholar]
- 14.Ley RE, Bäckhed F, Peter T, Lozupone CA, Knightand RD. Obesity alters gut microbial ecology. PNAS. 2005;102:11070–5. doi: 10.1073/pnas.0504978102. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Batra A, Pietsch J, Fedke I, et al. Leptin-dependent Toll like receptor expression and responsiveness in preadipocytes and adipocytes. Am J Pathol. 2007;170:1931–41. doi: 10.2353/ajpath.2007.060699. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Tsukumo DM, Carvalho-Filho MA, Carvalheira JBC, et al. Loss-of-function mutation in Toll-like receptor 4 prevents diet-induced obesity and insulin resistance. Diabetes. 2007;56:1986–98. doi: 10.2337/db06-1595. [DOI] [PubMed] [Google Scholar]
- 17.Cani PD, Neyrinck AM, Fava F, et al. Selective increases of bifidobacteria in gut microflora improve high-fat-diet induced diabetes in mice through a mechanism associated with endotoxaemia. Diabetologia. 2007;50:2374–83. doi: 10.1007/s00125-007-0791-0. [DOI] [PubMed] [Google Scholar]
- 18.Siebler J, Galle PR, Weber MM. The gut-liver-axis endotoxemia inflammation insulin resistance and NASH. J Hepatol. 2008;48:1032–34. doi: 10.1016/j.jhep.2008.03.007. [DOI] [PubMed] [Google Scholar]
- 19.Cani PD, Bibiloni R, Knauf C, et al. Changes in gut microbiota control metabolic endotoxemia-induced inflammation in high-fat diet-induced obesity and diabetes in mice. Diabetes. 2008;57:1470–81. doi: 10.2337/db07-1403. [DOI] [PubMed] [Google Scholar]
- 20.Rubins HB, Robins SJ, Collins D, et al. Gemfibrozil for the secondary prevention of coronary heart disease in men with low levels of high-density lipoprotein cholesterol. Veterans Affairs High-Density Lipoprotein Cholesterol Intervention Trial Study Group. N Engl J Med. 1999;341:410. doi: 10.1056/NEJM199908053410604. [DOI] [PubMed] [Google Scholar]
- 21.van Guldener C, Stam F, Stehouwer CD. Homocysteine metabolism in renal failure. Kidney Int. 2001;59:S234. doi: 10.1046/j.1523-1755.2001.59780234.x. [DOI] [PubMed] [Google Scholar]
- 22.Bostom AG, Bausserman L, Jacques PF, et al. Cystatin C as a determinant of fasting plasma total homocysteine levels in coronary artery disease patients with normal serum creatinine. Arterioscler Thromb Vasc Biol. 1999;19:2241. doi: 10.1161/01.atv.19.9.2241. [DOI] [PubMed] [Google Scholar]
- 23.Cani PD, Delzenne NM, Amar J, Burcelin R. Role of gut microflora in the development of obesity and insulin resistance following high-fat diet feeding. Pathologie Biologie. 2008;56:305–9. doi: 10.1016/j.patbio.2007.09.008. [DOI] [PubMed] [Google Scholar]
- 24.Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Organization. Technical Report Series. 2000;894:250–3. [PubMed] [Google Scholar]
- 25.Alexandra JS, Laura LP, Bo Wei, et al. Abundant and diverse fungal microbiota in the murine intestine. Appl Environ Microbiol. 2006;72:793–801. doi: 10.1128/AEM.72.1.793-801.2006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Jonathan B, James B. Abundant and diverse fungal microbiota in the murine intestine. Appl Environ Microbiol. 2006;1:793–801. doi: 10.1128/AEM.72.1.793-801.2006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Dick LK, Field KG. Rapid estimation of numbers of fecal Bacteroidetes by use of a quantitative PCR assay for 16S rRNA genes. Appl Environ Microbiol. 2004;70:5695–7. doi: 10.1128/AEM.70.9.5695-5697.2004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Bernhard AE, Field KG. Identification of nonpoint sources of fecal pollution in coastal waters by using host-specific 16S ribosomal DNA genetic markers from fecal anaerobes. Appl Environ Microbiol. 2000;66:1587–94. doi: 10.1128/aem.66.4.1587-1594.2000. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Huijsdens XW, Linskens RK, Mak M, et al. Quantification of bacteria adherent to gastrointestinal mucosa by real-time PCR. J Clin Microbiol. 2002;40:4423–7. doi: 10.1128/JCM.40.12.4423-4427.2002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Turnbaugh PJ, Micah H, Tanya Y, et al. A core gut microbiome in obese and lean twins. Nature. 2008;457:480–4. doi: 10.1038/nature07540. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Carmen C, Muriel D, Erika I, et al. Intestinal integrity and Akkermansia muciniphila a Mucin-degrading member of the intestinal microbiota present in infants adults and the elderly. Appl Envir Microbiol. 2007;73:7767–70. doi: 10.1128/AEM.01477-07. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Duncan SH, Lobley GE, Holtrop G, et al. Human colonic microbiota associated with diet, obesity and weight loss. Int J Obes. 2008;32:1720–4. doi: 10.1038/ijo.2008.155. [DOI] [PubMed] [Google Scholar]
- 33.Ley RE, Turnbaugh PJ, Jeffrey SK, Gordon I. Microbial ecology human gut microbes associated with obesity. Nature. 2006;444:1022–3. doi: 10.1038/4441022a. [DOI] [PubMed] [Google Scholar]
- 34.Zhang H, DiBaise JK, Zuccolo A. Human gut microbiota in obesity and after gastric bypass. Proc Natl Acad Sci U S A. 2009;106:2365–70. doi: 10.1073/pnas.0812600106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Ley RE. Obesity and the human microbiome. Curr Opin Gastroenterol. 2010;26:5–11. doi: 10.1097/MOG.0b013e328333d751. [DOI] [PubMed] [Google Scholar]
- 36.Hildebrandt MA, Hoffman C, Sherrill-Mix SA, et al. High fat diet determines the composition of the murine gut microbiome independently of obesity. Gastroenterology. 2009;137:1716–24. doi: 10.1053/j.gastro.2009.08.042. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Cani PD, Amar J, Iglesias MA, et al. Metabolic endotoxemia initiates obesity and insulin resistance. Diabetes. 2007;56:1761–72. doi: 10.2337/db06-1491. [DOI] [PubMed] [Google Scholar]
- 38.Tsukumo D, Carvalho-Filho M, Carvalheira J, et al. Loss-of-function mutation in Toll-like receptor 4 prevents diet-induced obesity and insulin resistance. Diabetes. 2007;56:1886–98. doi: 10.2337/db06-1595. [DOI] [PubMed] [Google Scholar]