Abstract
Background
Apolipoprotein A1 (apoA1) is the major apolipoprotein constituent of the high-density lipoprotein (HDL) and is involved in reverse cholesterol transport. Variation in the apoA1 gene might influence the function of the protein and, thus, brain cholesterol metabolism, leading to an increased risk for Alzheimer's disease (AD).
Aim
In the current report, we investigated the role of the functional apoA1 polymorphism (−75 G/A) as a genetic risk factor for AD in a Tunisian population.
Methods
173 AD patients and 150 healthy controls were studied.
Results
No association was found between this genetic variation in apoA1 gene and the risk of AD. The presence of the (−75 G/A) A allele appeared, however, to be associated with lower levels of cerebrospinal fluid Aβ42 and HDL cholesterol levels in sera.
Conclusion
Our data support the observation that apoA1 polymorphism influences cholesterol metabolism and Aβ42 deposition in the brain.
Key Words: Alzheimer's disease, Apolipoprotein A1, HDL cholesterol, Polymorphisms
Introduction
Alzheimer's disease (AD) is the most common form of dementia in elderly people [1,2]. Estimates suggest that ∼10% of individuals over the age of 65 and almost half over the age of 85 have Alzheimer's dementia. As human life expectancy continues to rise, the total number of affected individuals is also expected to increase dramatically [3].
AD is a multifactorial disease but its etiology and pathophysiology are still not fully understood [4]. AD probably results from a complex interaction between aging [5], vascular risk factors [6,7], impaired status of micronutrients [8], and genetic factors [9]. Three genes have been identified as causative genes in familial AD: the amyloid precursor protein (APP), presenilin-1 and presenilin-2 [10]. In addition, the apolipoprotein E (apoE) ∊4 allele is the only recognized genetic risk factor for familial as well as sporadic AD [11,12]. Although many studies have reported associations between genes involved in cholesterol metabolism and AD, the functional connection between the cholesterol pathway and AD pathology has not been clearly resolved.
Recently, apolipoprotein A1 (apoA1) polymorphism was identified as a factor affecting brain cholesterol metabolism and angiogenesis, leading to an increased risk for AD [13]. Up to now, several SNPs have been identified in the apoA1 gene located on the long arm of chromosome 11. Among these, a common G/A substitution located at −75 bp upstream from the apoA1 transcription start site (rs670) and a C/T and G/A base substitution at position +83 bp (rs5069) or +84 bp (rs1799837) were reported to differentially affect apoA1 expression [14,15]. In view of this, Vollbach et al. [16] reported an increase in the risk of early-onset AD for rs670 A allele bearers, but did not find any impact of rs5069 and rs1799837 polymorphisms on risk of AD. In addition, in vitro, studies linked the amyloid-β (Aβ) aggregation to the reduction of apoA1 levels in the brain, hence promoting neurodegeneration [17]. Furthermore, apoA1 is associated with an earlier onset of neurofibrillary tangle formation and an increased neurofibrillary tangle load.
In this case-control study, we investigated whether the −75 G/A polymorphism of the apoA1 gene may be responsible for susceptibility to AD in a sample of patients that was already genotyped for apoE, bleomycin hydrolase, and vascular endothelial growth factor (VEGF) [18,19], and to assess its relationship with the severity of the disease as estimated by the Mini-Mental State Examination (MMSE) score.
Subjects and Methods
The patients, Tunisian Arab descendants who live in the center of Tunisia, were consecutively evaluated at the Department of Neurology of Sahloul University Hospital between January 2005 and August 2008. All participants underwent a complete clinical investigation, including medical history, neurological and neuropsychological examination, MMSE, laboratory tests and neuroimaging which consisted of magnetic resonance imaging (MRI). Our patients were assigned either to the AD or the control group according to clinical examination and brain imaging. MRI has shown a great reduction in medial temporal lobe and hippocampal volume of patients with AD as compared to controls. The MMSE for grading the cognitive state [20] was used in a validated Arabic version [21].
After this assessment, 173 patients were classified as probable AD (99 females and 74 males; mean age 75 ± 1.87 years, n = 173) according to the criteria of the National Institute of Neurological and Communicative Disorders and Stroke – Alzheimer's Disease and Related Disorders Association (NINCDS-ADRDA) [22]. These patients were further classified according to their MMSE scores as follows: mild AD (MMSE ≥24), moderate AD (MMSE 11–23), and severe AD (MMSE ≤10).
The second group included 150 elderly subjects (79 females and 71 males; mean age 71 ± 1.78 years) that were selected as controls (MMSE >26) by experienced neurologists. These subjects were hospitalized for clinical suspicion of meningitis or polyneuropathy (acute or chronic). In both cases, a lumbar puncture was clinically indicated. Inclusion criteria were a normal renal or liver function (creatinine <120 μmol/l, ALT <45 IU/l, AST <40 IU/l). Exclusion criteria were the presence of an active neurological or psychiatric disease, memory complaints or other cognitive symptoms. The control subjects had a preserved general cognitive function and no family history of dementia. None of them complained of memory impairment at the time of examination. The control subjects were matched by age with the patients with dementia.
The Institution's Ethics Committee for studies in human subjects gave its approval for the study. A written informed consent to participate in this clinical research study was obtained from participants or from a relative (legal guardian).
Demographic details for all subjects were recorded, including age, gender, age at onset, MSSE score, duration of dementia, and plasma lipid and lipoprotein levels (table 1).
Table 1.
Demographic and clinical data by diagnostic groups
| Variable | Controls (n = 150) | AD (n = 173) | P |
|---|---|---|---|
| Women/men | 79/71 | 99/74 | NS |
| Age, years | 71 ± 1.78 | 75 ± 1.87 | NS |
| Age at onset, years | – | 71 ± 0.93 | – |
| Duration of AD, years | – | 3.1 ± 0.53 | – |
| Higher education, n (%) | 51 (34) | 37 (21) | – |
| MMSE | 28 ± 0.32 | 15 ± 1.8 | <0.001 |
| TC, mmol/l | 4.86 ± 1.11 | 4.58 ± 1.21 | NS |
| TG, mmol/l | 1.59 ± 0.76 | 1.19 ± 0.7 | <0.001 |
| LDL-C, mmol/l | 3.24 ± 0.91 | 3.47 ± 0.9 | NS |
| HDL-C, mmol/l | 1.23 ± 0.29 | 0.82 ± 0.22 | <0.001 |
| apoAl, g/l | 1.43 ± 0.2 | 1.18 ± 0.43 | <0.001 |
Data are expressed as means ± SD unless otherwise indicated. TC = Total cholesterol; TG = triglyc-erides.
Blood samples were obtained after an overnight fast. Plasma levels of total cholesterol, triglycerides, and high-density lipoprotein cholesterol (HDL-C) were measured by standardized enzymatic procedures, and apoA1 was measured using a turbidimetric assay on a Hitachi 912 analyzer. Low-density lipoprotein cholesterol (LDL-C) was calculated according to Friedewald's formula [23].
Cerebrospinal fluid (CSF) was obtained from 88 controls and 143 AD patients. The CSF was stored in polypropylene tubes at −80°C and analyzed after the clinical follow-up of the study had been completed. CSF t-tau and Aβ42 levels were determined using a commercially available sandwich enzyme-linked immunoabsorbant assay (Innotest hTAU-Ag, Innotest β-amyloid 42) from Innogenetics.
Total genomic DNA was isolated from peripheral blood leukocytes using genomic DNA purification kit (Promega). apoA1 genotype analysis was performed by PCR restriction fragment length polymorphism analysis using the primer 5′-AGGGACAGAGCTGATCCTTGAACTCTTAAG-3′, and 5′-TTAGGGGACACCTACCCGTCAGGAAGACGA-3′. The 180-bp amplified fragment was restricted with the enzyme MspI, and the DNA fragments were separated using 20% polyacrylamide gel electrophoresis. apoA1 genotype was determined by comparison with the combination of fragment sizes described by Vollbach et al. [16]. All subjects were genotyped for apoE using the methods described previously [24].
Statistics
Statistical analyses were performed by SPSS software for Windows (release 10.1). Allele frequencies were calculated by the gene counting method. Genotype and allele frequencies of apoA1 were compared between patients and controls using χ2 test. After adjusting for age, gender, and educational level, univariate logistic regression analysis was performed for apoA1 with AD by the apoE genotype. We used the statistical software Epinfo for power analysis. Statistical significance was set at p < 0.05.
Results
In total of 173 patients with AD and 150 healthy controls were included in this study. The characteristics of the AD patients and control subjects are shown in table 1. The two groups were matched for gender (χ2 = 0.323; p = 0.11) and age (χ2 = 2.15; p = 0.73), with AD patients having a lower MMSE score together with lower serum apoA1, lower HDL-C levels, and higher triglyceride levels. Differences remained significant even when we took into account other parameters, such as age and sex, as covariants. In the AD patients, no significant differences in apoA1 concentrations between patients with one or two ∊4 alleles and those without the allele were found (data not shown; p = 0.72).
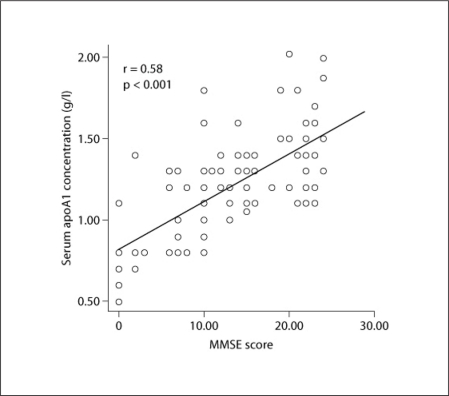
Our study demonstrated that apoA1 concentrations were highly correlated (p < 0.001) with the severity of AD, as reflected by the patients’ MMSE (fig. 1). This relationship was independent of all other parameters studied (age, gender, and apoE genotypes). Moreover, patients with fewer years of education appeared to have higher rates of AD (OR = 2.48, 95% CI 1.75–4.79; p = 0.007; adjusted for age: OR = 1.89, 95% CI 1.15–3.1; p = 0.004).
Fig. 1.
Relationship between serum apoA1 concentrations and MMSE score. The correlation coefficient and the significance level are shown.
Table 2 depicts the genotype distribution of apoA1 in AD patients and in the control group. Using the χ2 test, the distribution of the apoA1 −75 G/A genotypes in all patients with AD and healthy controls did not significantly deviate from that expected by Hardy-Weinberg equilibrium. The frequencies of the GG, GA, and AA genotypes in the control group and among AD patients were 67.4, 25.4, and 7.2% and 61.3, 32.3, and 6.4%, respectively, in the apoA1 −75 G/A SNP. As shown in table 2, there were no statistically significant differences in the AD group when compared to controls (Pearson's χ2 test, p < 0.05). According to the univariate logistic regression analysis, the −75 G/A allele of the apoA1 polymorphism was not associated with the risk of AD after adjusting for age, sex, and educational level (−75 G/A, presence of A allele: OR = 1.16, 95% CI 0.78–1.73; p = 0.43). Despite the presence of the apoE ∊4, the −75 G/A allele was not associated with AD after adjusting for age, sex, and educational level. The lack of an association observed could be linked to the low prevalence of the A allele.
Table 2.
Allele and genotype frequencies of the apoAl rs670 polymorphism
| apoAl polymorphism | AD group (n = 173) | Control group (n = 150) | Odds ratio (95% CI) | P |
|---|---|---|---|---|
| Allele frequency | ||||
| G | 268 (77.5%) | 240 (80%) | ||
| A | 78 (22.5%) | 60 (20%) | 1.16 (0.78–1.73) | 0.43 |
| Genotype distribution | ||||
| GG | 106 (61.3%) | 101 (67.4%) | 1 | |
| GA | 56 (32.4%) | 38 (25.4%) | 1.4 (0.84–2.37) | 0.16 |
| AA | 11 (6.4%) | 11 (7.2%) | 0.69 (0.27–1.78) | 0.4 |
| AA+GA | 67 | 49 | 1.3 (0.8–2.12) | 0.25 |
Investigation of the effect of the apoA1 polymorphism on apoA1 concentrations and HDL-C levels revealed that HDL-C levels were lower in AD patients who were carriers of at least one A allele of the apoA1 −75 G/A polymorphism than in carriers of the GG genotype (F = 7.1, d.f. = 1; p < 0.05). Similar differences across the apoA allele were seen with HDL-C within the control group. We did not find any effect of the apoA1 −75 G/A polymorphism on the apoA1 level within the AD group or the control group associated with the absence or presence of the allele (F = 0.341, d.f. = 1; p = 0.78).
Within the AD group, the A allele of apoA1 was associated with the CSF Aβ42 reduction (F = 1.26, d.f. = 1; p = 0.028). There was a significant CSF Aβ42 reduction in the AD patients with at least one copy of the A allele for apoA1 −75 G/A when compared with those AD patients without the allele [315 (270–410) vs. 419 (330–480); p = 0.033]. Contrarily, there were no significant differences in CSF t-tau protein levels within the AD group associated with the absence or presence of the allele (table 3).
Table 3.
CSF Aβ42, CSF t-tau, serum apoAl and HDL-C levels arranged by diagnosis and polymorphisms status (absent or present)
| AD group |
Control group |
|||||||
|---|---|---|---|---|---|---|---|---|
| n | total | A (+) | A (−) | n | total | A (+) | A (−) | |
| Aβ42, pg/ml | 143 | 410 (330–690)a | 315 (270–410)b | 419 (330–475) | 88 | 978 (790–1,055) | 890 (810–1,020)c | 960 (890–1,040) |
| t-tau, pg/ml | 143 | 445 (370–680)a | 460 (240–910) | 458 (315–880) | 88 | 280 (250–310) | 280 (175–410) | 265 (190–445) |
| HDL-C, mmol/l | 173 | 0.82 ± 0.22a | 0.70 ± 0.16b | 0.84 ± 0.24 | 150 | 1.23 ± 0.29 | 0.1 ± 0.22c | 1.27 ± 0.19 |
| apoAl, g/l | 173 | 1.18 ± 0.43a | 1.2±0.39 | 1.23 ± 0.19 | 150 | 1.43 ± 0.2 | 1.4 ± 0.17 | 1.39 ± 0.19 |
Values are medians and 25th to 75th percentiles in parentheses or means ± SD. Bonferroni-corrected p values:
Highly significant differences (p < 0.001): AD vs. control group.
Significant differences (p < 0.05): AD A (+) vs. AD A (−).
Significant differences (p < 0.05): control A (+) vs. control A (−).
Discussion
apoA1, a major apolipoprotein constituent of HDLs, is secreted into the bloodstream by the liver and intestine as a protein that is rapidly converted to mature apoA1. Different polymorphisms in apoA1 have been described, and influences on HDL and apoA1 plasma levels and on the risk of disorders such as coronary artery disease [25] or AD [16] have been detected. However, only few of these findings have been replicated, and it is unclear which polymorphism might act as the relevant functional one. According to a study by Juo et al. [26],the A allele of the −75 G/A gene may affect expression of apoA1, although it was not clear whether the observed effect was directly associated with the mutation or due to another mutant allele in linkage disequilibrium with the −75 G/A polymorphism. In this regard, while additional studies on a larger number of cases will be required to confirm and extend our findings, the present data suggest for the first time that this polymorphism has no influence on the expression of apoA1. Furthermore, this polymorphism was reported to be associated with changes in plasma HDL levels in particular in AD patients. HDL is the prominent lipoprotein in the human brain [27] and is involved in the regulation of Aβ protein metabolism and deposition in the brain [28]. Deficit in HDL-C could also affect memory through its influence on atherosclerotic disease and stroke [29] or subclinical vascular injury not reflected in the covariates examined. Other possible mechanisms linking low levels of HDL-C to neurodegenerative processes might involve its anti-inflammatory [30] or antioxidant [31] properties. In our current study, AD patients showed a significant decrease in HDL levels compared with controls. The subjects included in our study had a diet which was characterized by a low intake of meat, a high intake of vegetables and legumes, and no alcohol intake. None of the subjects were malnourished and the dietary habits of control subjects and patients were similar. Interestingly, our results showed also that the apoA1 −75 G/A polymorphism has a reducing effect on HDL-C levels in AD patients (–0.14 mmol/l). These findings prompted us, therefore, to evaluate with a case-control study whether this polymorphic variation may have an impact on the susceptibility to AD in a Tunisian population.
Reviewing previous reports, it seems evident that the apoA1 (−75 G/A) A allele frequency demonstrates heterogeneity around the word [16,32,33]. In the present study, the −75 G/A variant was present at a frequency of 0.225 and 0.2 among AD and control subjects, respectively. This was comparable also to frequencies established for a French [32] and Italian population [33], but higher than the rates of 0.17–0.19 reported for a German population [16]. Although a previous study involving 500 healthy controls and 427 AD patients of Caucasian origin (UK and Germany) suggested an association between the rs670 A polymorphism and AD (age at onset <65 years; OR = 2.99, 95% CI 1.82–4.93; p < 0.001) [16], we were unable to reproduce these results in our population sample. Similar negative findings with respect to a direct association between potential genetic risk factor and disease have been reported previously [32]. The failure to replicate association in our population does not necessarily invalidate the previous results. It might be attributed to several factors, such as differences in the ethnic background and geographic characteristics of the studied populations. Also, differences in the inclusion and exclusion criteria may influence the study results, especially if subjects affected by some chronic diseases are not excluded from studies investigating genes involved in cholesterol metabolism. In addition, the absence of a statistically significant effect of the apoA1 polymorphism on the risk of AD in our sample can be attributed to low power because our sample had <80% power to detect an association with AD. Finally, it is not possible to exclude the role played by genes that are in relation with the apoA1 gene. In this condition, it is possible that one or more of these genes are in linkage disequilibrium with the apoA1 gene in some populations but not in others, thus influencing the results of these association studies.
The second point of our study was to assess the relationships between the presence of this polymorphism, the genotype found in both groups of patients, and the pathological CSF markers of the disease. To our knowledge, the contribution of apoA1 in neurological disorders and in AD patients has been evaluated in only a few of the autopsied brains, and most in vivo studies have been performed on plasma total. In the present study, one very important association was observed between CSF Aβ42 levels and the −75 G/A polymorphism of apoA1. A significant decrease was observed in the CSF Aβ42 levels among the AD patients with the −75 A allele of apoA1. The −75 A allele of apoA1 effect sizes were similar when comparing CSF Aβ42 levels of AD patients and control subjects. On the other hand, there were no significant differences in CSF t-tau levels between the AD subjects and the control group associated with the presence or absence of the −75 A allele of apoA1. We propose that the increase in apoA1 transcription for the A allele may affect the solubility of Aβ42 and/or its transport across the blood-brain barrier in AD. apoA1 could be involved in the pathology of AD in at least three ways. A first mechanism would entail the formation of amyloid-like fibrils. apoA1 has been shown to participate in the amylogenesis process by binding to Aβ [34] and to form amyloid-like fibrils in APP transgenic mice [8]. A second role of apoA1 with implications in the genesis of AD relates to neuron maintenance. apoA1 is one of the exchangeable apolipoproteins that are actively involved in the regeneration process of neuron cells occurring after injury [35]. Finally, the association between apoA1 and other proteins such as apoJ and apoE [36] could contribute to the pathogenesis of AD. Other pathological mechanisms are possible and would need to be further evaluated in future AD studies.
Regarding prognostic parameters, we have analyzed the correlations between the apoA1 levels and clinical characteristics of dementia including MMSE score in AD patients. Studies in the elderly have shown that high levels of serum apoA1 and HDL-C are associated with low total mortality and enhanced longevity [37,38]. Our results suggest that the AD patients with higher serum apoA1 concentrations have less cognitive impairment. This supports earlier findings by Merched et al. [15] showing that higher serum apoA1 concentrations are associated with a significant improvement in cognitive performance. Moreover, when patients were stratified according to their MMSE score, AD patients with a lower score had significantly decreased apoA1 levels. This finding may highlight the occurrence of some factors that may decrease the level or affinity of unknown molecular factors that affect synthesis and secretion of apoA1 in an allele-specific manner.
In summary, the present study does not support any impact of the apoA1 genetic polymorphism on AD in the Tunisian population and confirmed the relationship between apoA1 levels and MMSE score in AD patients. Further studies that identify the relevant functional apoA1 polymorphism are needed. These results will help to clarify the role of apoA1 polymorphisms in the regulation of cholesterol metabolism.
Acknowledgment
This work was supported by a grant from Ministère de l'enseignement supérieur, de la recherche scientifique et de la technologie.
References
- 1.Blennow K, de Léon MJ, Zetterberg H. Alzheimer's disease. Lancet. 2006;368:387–403. doi: 10.1016/S0140-6736(06)69113-7. [DOI] [PubMed] [Google Scholar]
- 2.Ferri CP, Prince M, Brayne C, Brodaly H, Fratiglioni L, Ganguli M, et al. Global prevalence of dementia: a Delphi consensus study. Lancet. 2005;366:2112–2117. doi: 10.1016/S0140-6736(05)67889-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Evans DA, Funkenstein HH, Albert MS, Cook NR, Chown MJ, Hebert LE, Hennekens CH, Taylor JO. Prevalence of Alzheimer's disease in a community population of older persons. Higher than previously reported. JAMA. 1989;262:2551–2556. [PubMed] [Google Scholar]
- 4.Hardy J, Allsop D. Amyloid deposition as the central event in the aetiology of Alzheimer's disease. Trends Pharmacol Sci. 1991;12:383–388. doi: 10.1016/0165-6147(91)90609-v. [DOI] [PubMed] [Google Scholar]
- 5.Rubenstein E. Relationship of senescence of cerebrospinal fluid circulatory system to dementias of the aged. Lancet. 1998;351:283–285. doi: 10.1016/S0140-6736(97)09234-9. [DOI] [PubMed] [Google Scholar]
- 6.Cavalieri M, Enzinger C, Petrovic K, Fuerst AP, Homayoon N, Schmidt H, et al. Vascular dementia and Alzheimer's disease – are we in a dead-end road? Neurodegener Dis. 2010;7:122–126. doi: 10.1159/000285521. [DOI] [PubMed] [Google Scholar]
- 7.Dickstein DL, Walsh J, Brautigam H, Stockton SD, Jr, Gandy S, Hof PR. Role of vascular risk factors and vascular dysfunction in Alzheimer's disease. Mt Sinai J Med. 2010;77:82–102. doi: 10.1002/msj.20155. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Weir DG, Scott JM. Brain function in the elderly: role of vitamin B12 and folate. Br Med Bull. 1999;55:669–682. doi: 10.1258/0007142991902547. [DOI] [PubMed] [Google Scholar]
- 9.Corder EH, Saunders AM, Strittmatter WJ, Schechel DE, Gaskelle PC, Small GW, et al. Gene dose of apolipoprotein E type 4 allele and the risk of Alzheimer's disease in late onset families. Science. 1993;261:921–923. doi: 10.1126/science.8346443. [DOI] [PubMed] [Google Scholar]
- 10.Shibata N, Ohnuma T, Baba H, Arai H. No genetic association between polymorphisms of heme oxygenase 1 and 2 and Alzheimer's disease in a Japanese population. Dement Geriatr Cogn Disord. 2009;27:273–277. doi: 10.1159/000203891. [DOI] [PubMed] [Google Scholar]
- 11.Hardy J. A hundred years of Alzheimer's disease research. Neuron. 2006;52:3–13. doi: 10.1016/j.neuron.2006.09.016. [DOI] [PubMed] [Google Scholar]
- 12.Strittmattet WJ, Roses AD. Apolipoprotein E and Alzheimer disease. Proc Natl Acad Sic USA. 1995;92:25–27. doi: 10.1073/pnas.92.11.4725. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Paula-Lima AC, Tricerri MA, Brito-Moreira J, Bomfim TR, Oliveira FF, Magdesian MH, Grinberg LT, Panizzutti R, Ferreira ST. Human apolipoprotein A-I binds amyloid-beta and prevents Abeta-induced neurotoxicity. Int J Biochem Cell Biol. 2009;41:1361–1370. doi: 10.1016/j.biocel.2008.12.003. [DOI] [PubMed] [Google Scholar]
- 14.Ma YQ, Thomas GN, Tomlinson B. Association of two apolipoprotein A-I gene MspI polymorphisms with lipid and blood pressure levels. Int J Cardiol. 2005;102:309–314. doi: 10.1016/j.ijcard.2004.10.017. [DOI] [PubMed] [Google Scholar]
- 15.Merched A, Xia Y, Visviskis S, Serot JM, Siest G. Decreased HDL cholesterol and serum apolipoprotein A1 concentrations are highly correlated with the severity of Alzheimer's disease. Neurobiol Aging. 2000;21:27–30. doi: 10.1016/s0197-4580(99)00103-7. [DOI] [PubMed] [Google Scholar]
- 16.Vollbach H, Heun R, Morris CM, Edwardson JA, McKeith IG, Jessen Schulz FA, Maier W, Kolsch H. ApoA1 polymorphism influences risk for early-onset nonfamilial AD. Ann Neurol. 2005;58:436–441. doi: 10.1002/ana.20593. [DOI] [PubMed] [Google Scholar]
- 17.Wisniewski T, Golabek AA, Kida E, Wisniewski KE, Frangione B. Conformational mimicry in Alzheimer's disease. Role of apolipoproteins in amyloidogenesis. Am J Pathol. 1995;147:238–244. [PMC free article] [PubMed] [Google Scholar]
- 18.Smach MA, Charfeddine B, Lammouchi T, Harrabi I, Ben Othman L, Dridi H, Bennamou S, Limem K. CSF beta-amyloid 1–42 and tau in Tunisian patients with Alzheimer's disease: the effect of APOE epsilon4 allele. Neurosci Lett. 2008;440:145–149. doi: 10.1016/j.neulet.2008.05.076. [DOI] [PubMed] [Google Scholar]
- 19.Smach MA, Charfeddine B, Othman LB, Lammouchi T, Ltaief A, Nafati S, Dridi H, Bennamou S, Limem K. −1154G/A and −2578C/A polymorphisms of the vascular endothelial growth factor gene in Tunisian Alzheimer patients in relation to beta amyloid (1–42) and total tau protein. Neurosci Lett. 2010;472:139–142. doi: 10.1016/j.neulet.2010.01.073. [DOI] [PubMed] [Google Scholar]
- 20.Folstein MF, Folstein SE, McHugh PR. ‘Mini-Mental State’. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12:198–198. doi: 10.1016/0022-3956(75)90026-6. [DOI] [PubMed] [Google Scholar]
- 21.Bellaj T: Dysfonctionnement de la mémoire de travail dans la maladie d'Alzheimer. Thèse de Doctorat. Faculté des Sciences Humaines et Sociales de Tunis, 1999.
- 22.McKann G, Drachman DA, Folstein M, Katzman R, Price DL, Stadlan EM. Clinical diagnosis of Alzheimer's disease – report of the NINCDS-ADRDA work group under the auspices of Department of Health and Human Services Task Force on Alzheimer's Disease. Neurology. 1984;34:939–944. doi: 10.1212/wnl.34.7.939. [DOI] [PubMed] [Google Scholar]
- 23.Friedward WT, Levy RI, Fredrickson DS. Estimation of the concentration of low-density lipoprotein cholesterol in plasma, without use of the preparative ultracentrifuge. Clin Chem. 1972;18:402–499. [PubMed] [Google Scholar]
- 24.Wenham PR, Price WH, Blandell G. Apolipoprotein E genotyping by one-stage PCR. Lancet. 1991;337:1158–1159. doi: 10.1016/0140-6736(91)92823-k. [DOI] [PubMed] [Google Scholar]
- 25.Kamboh MI, Aston CE, Nestlerode CM, McAllister AE, Hamman RF. Haplotype analysis of two Apo1/MspI polymorphisms in relation to plasma levels of apoA-I and HDL-cholesterol. Atherosclerosis. 1996;127:255–262. doi: 10.1016/s0021-9150(96)05966-7. [DOI] [PubMed] [Google Scholar]
- 26.Juo SH, Wyszynski DF, Beaty TH, Huang HY, Bailey-Wilson JE. Mild association between the A/G polymorphism in the promoter of the apolipoprotein A-I gene and apolipoprotein A-I levels: a meta-analysis. Am J Med Genet. 1999;82:235–241. [PubMed] [Google Scholar]
- 27.Olesen OF, Dago L. High density lipoprotein inhibits assembly of amyloid beta-peptides into fibrils. Biochem Biophys Res Commun. 2000;270:62–66. doi: 10.1006/bbrc.2000.2372. [DOI] [PubMed] [Google Scholar]
- 28.Reiss AB, Siller KA, Rahman MM, Chan ES, Ghiso J, de Leon MJ. Cholesterol in neurologic disorders of the elderly: stroke and Alzheimer's disease. Neurobiol Aging. 2004;25:977–989. doi: 10.1016/j.neurobiolaging.2003.11.009. [DOI] [PubMed] [Google Scholar]
- 29.Sacco RL, Benson RT, Kargman DE, Boden-Albala B, Tuck C, Lin IF, Cheng JF, Paik MC, Shea S, Berglund L. High-density lipoprotein cholesterol and ischemic stroke in the elderly: the Northern Manhattan Stroke Study. JAMA. 2001;285:2729–2735. doi: 10.1001/jama.285.21.2729. [DOI] [PubMed] [Google Scholar]
- 30.Cockerill GW, Huehns TY, Weerasinghe A, Stocker C, Lerch PG, Miller NE, Haskard DO. Elevation of plasma high-density lipoprotein concentration reduces interleukin-1-induced expression of E-selectin in an in vivo model of acute inflammation. Circulation. 2001;103:108–112. doi: 10.1161/01.cir.103.1.108. [DOI] [PubMed] [Google Scholar]
- 31.Paterno R, Ruocco A, Postiglione A, Hubsch A, Andresen I, Lang MG. Reconstituted high-density lipoprotein exhibits neuroprotection in two rat models of stroke. Cerebrovasc Dis. 2004;17:204–211. doi: 10.1159/000075792. [DOI] [PubMed] [Google Scholar]
- 32.Helbecque N, Codron V, Cottel D, Amouyel P. An apolipoprotein A-I gene promoter polymorphism associated with cognitive decline, but not with Alzheimer's disease. Dement Geriatr Cogn Disord. 2008;25:97–102. doi: 10.1159/000112176. [DOI] [PubMed] [Google Scholar]
- 33.Orlacchio A, Babalini C, Varlese M, Patrono C, Borreca A, Esposito Z, Sancesario G, Orlacchio A, Kawarai T, Bernardi G. Association study of the APOA1 gene in an Italian population with Alzheimer's disease. Alzheimer's Dementia. 2008;4:T593. [Google Scholar]
- 34.Koudinov A, Matsubara E, Frangione B, Ghiso J. The soluble form of Alzheimer's amyloid beta protein is complexed to high density lipoprotein 3 and very high density lipoprotein in normal human plasma. Biochem Biophys Res Commun. 1994;205:1164–1171. doi: 10.1006/bbrc.1994.2788. [DOI] [PubMed] [Google Scholar]
- 35.Boyles JK, Zoellner CD, Anderson LJ, Kosik LM, Pitas RE, Weisgraber KH, Hui DY, Mahley RW, Gebicke-Haerter PJ, Ignatius MJ, et al. A role for apolipoprotein E, apolipoprotein A-I, and low density lipoprotein receptors in cholesterol transport during regeneration and remyelination of the rat sciatic nerve. J Clin Invest. 1989;83:1015–1031. doi: 10.1172/JCI113943. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Stuart WD, Krol B, Jenkins SH, Harmony JA. Structure and stability of apolipoprotein J-containing high-density lipoproteins. Biochemistry. 1992;31:8552–8559. doi: 10.1021/bi00151a024. [DOI] [PubMed] [Google Scholar]
- 37.Van den Kommer TN, Dik MG, Comijis HC, Fassbender K, Lutjohann D, Jonker C. Total cholesterol and oxysterols: early markers for cognitive decline in elderly? Neurobiol Aging. 2009;30:534–545. doi: 10.1016/j.neurobiolaging.2007.08.005. [DOI] [PubMed] [Google Scholar]
- 38.VanVliet P, Van de Water W, de Craen AJM, Westendrop RGJ. The influence of age on the association between cholesterol and cognitive function. Exp Gerontol. 2009;44:112–122. doi: 10.1016/j.exger.2008.05.004. [DOI] [PubMed] [Google Scholar]