Introduction
Palmar radiocarpal dislocation is an extremely rare injury pattern. The largest reported series of radiocarpal dislocations included 27 cases, four of which were palmar, and the only pure palmar ligamentous dislocation in that series was lost to follow-up [1]. Another study [10] reviewed the existing literature on radiocarpal dislocation, summarized the findings of three previously reported palmar radiocarpal dislocations, and presented 3 months of follow-up of a single case. Other sporadic case reports [3, 5, 8] of palmar radiocarpal dislocation have been published, bringing the total available in the current literature to fewer than ten. Thus, the treatment of this injury has not been well defined. We herein present a case of palmar radiocarpal dislocation and a novel treatment method based on a recently described method of reconstruction of the extrinsic radiocarpal ligaments [6].
Case Report
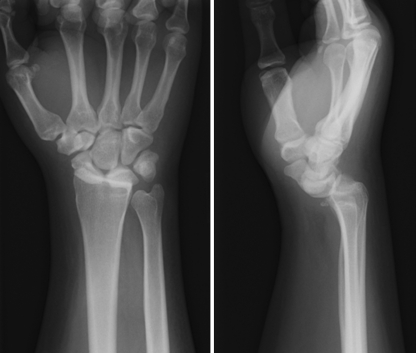
A 37-year-old male auto mechanic was involved in a motorcycle accident. He presented at our institution 2 weeks after the date of injury. An examination revealed a right wrist deformity without compromise of neurological function. Radiographs revealed a palmar radiocarpal dislocation (Fig. 1).
Fig. 1.
Radiocarpal dislocation can be seen
The next day, the patient underwent open reduction of the radiocarpal dislocation via palmar and dorsal exposures of the radiocarpal joint. An extended carpal tunnel release was performed from Kaplan’s cardinal line distally to 5 cm proximal to the distal flexion crease of the wrist. The palmar radiocarpal ligaments had been disrupted from the distal radius and already appeared attenuated. A separate 7-cm dorsal longitudinal incision was made over Lister tubercle. The dorsal wrist capsule had been avulsed as a sleeve from the distal radius. The carpus was inspected, and partial scapholunate ligament disruption was noted. Cartilage injury to the proximal lunate was present, but the majority of the articulating surfaces of the lunate facet and lunate remained undisrupted.
Repair of the extrinsic radiocarpal ligaments was achieved as follows: two 1.5-mm holes were drilled from palmar to dorsal to allow transosseous repair of the palmar and dorsal capsule and ligament complexes. Next, three .0625-in. Kirschner wires were advanced in a retrograde fashion, one in the lunate and two in the scaphoid fossae. Once the carpus was reduced, the wires were driven in an antegrade fashion across the carpus, maintaining appropriate reduction. Non-absorbable mono-filament sutures (2-0) were then used to secure the palmar and dorsal extrinsic ligaments to the distal radius by passing them through the previously made 1.5-mm holes.
Despite adequate reduction of the radiocarpal joint and transosseous repair of the extrinsic ligaments, concerns regarding the long-term sufficiency of the extrinsic ligaments remained. Therefore, reconstruction of the radioscaphocapitate ligament using the brachioradialis tendon according to the method presented by Maschke et al. [6] was completed. The brachioradialis tendon was harvested from its proximal muscle belly, and its distal insertion onto the radial styloid was left intact. It was then passed through the capitate via a 3.0-mm drill hole, from palmar to dorsal, to reconstruct the palmar radioscaphocapitate ligament. After tensioning, the brachioradialis tendon was secured within the capitate with the use of a bioabsorbable 4.0-mm interference screw (Arthrex, Naples, FL, USA). It was then passed proximally and anchored into the radius by using another 3.0-mm unicortical drill hole and interference screw to provide additional stability to the dorsal ligamentous repair (Fig. 2).
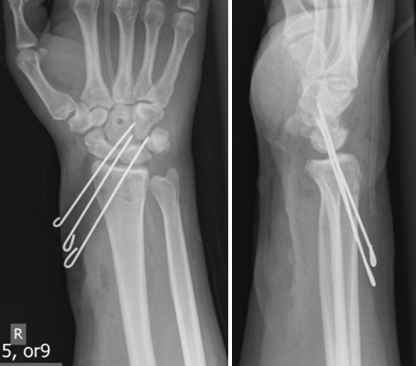
Fig. 2.
Postoperative radiographs obtained after closed reduction and percutaneous pinning of radiocarpal dislocation
The Kirschner wires remained in place for 6 weeks. After Kirschner wire removal in the office, the patient began occupational therapy for range-of-motion and strengthening exercises. Six months after surgery, the Disabilities of the Arm, Shoulder and Hand score was 6. At the 1-year follow-up visit, the range of motion of the injured wrist had a flexion–extension arc of 72% and a pronation–supination arc of 100% of the uninjured side. The patient’s grip strength at Jamar setting three was 42 kg on the right and 60 kg on the left. Radiographs obtained of the uninjured left side and injured right side are shown in Fig. 3, which includes flexion and extension views of the right side. The images show scapholunate widening on the right compared with the left, measured at 2.7 mm. However, no evidence of ulnar translocation was observed with preservation of the radiolunate angle, and the majority of the patient’s motion occurs at the midcarpal joint.
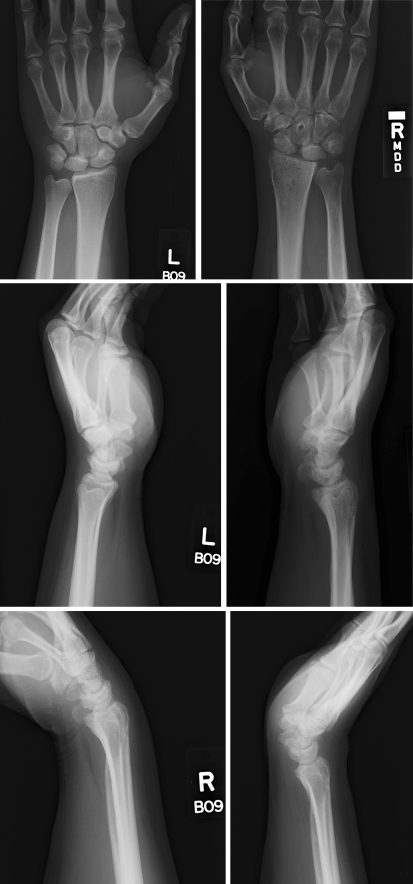
Fig. 3.
Postoperative radiographs obtained at the 1-year follow-up visit showing 2.7-mm scapholunate widening on the right, no evidence of ulnar translocation, and preservation of the radiolunate angle. It can be seen that the majority of the patient’s motion occurs at the midcarpal joint. Upper left, anteroposterior view of left side; upper right, anteroposterior view of right side; middle left, lateral view of left side; middle right, lateral view of right side; lower left, flexion view of the right (injured) side; lower right, extension view of the right (injured) side
Discussion
Palmar radiocarpal dislocations are rare injuries, often with devastating functional consequences [4, 7]. Insufficient ligamentous healing is considered to be the cause of the frequent complication of ulnar translocation of the carpus, defined as an increase in space between the radial styloid and scaphoid with displacement of the lunate over the distal ulna [2, 8, 9]. For this reason, closed reduction and casting have been abandoned.
Surgical treatment includes primary ligamentous repair [8, 9] combined with percutaneous pinning, with or without external fixation [3, 7]. Despite aggressive treatment, maintaining normal radiocarpal relationships can be difficult [7, 9]. When these methods fail, a salvage procedure such as radioscaphoid, radiolunate, or total wrist arthrodesis becomes necessary [3, 4, 7–9], prompting several authors to recommend some form of primary arthrodesis as the index procedure.
Dumontier et al. [1] noted important differences between radiocarpal dislocation involving a large radial styloid fragment and radiocarpal dislocation involving only a radial styloid avulsion fragment or pure ligamentous disruption. The latter type of dislocation lacks a bony scaffold for anatomic restoration of the radiocarpal ligaments, often resulting in inferior outcomes. This important distinction is supported by multiple other case reports in which, despite open repair, radiocarpal relationships were not maintained in pure ligamentous injuries [3, 7, 9].
Ligamentous reconstruction models have been described to reconstruct the palmar extrinsic ligaments. Rayhack et al. [9] described reconstructing the radiolunate ligament by using the extensor carpi ulnaris tendon; however, symptoms recurred with ulnar translocation and a salvage wrist arthrodesis was performed. Rayhack et al. also described using half of a distally based extensor carpi radialis brevis slip to reconstruct the radioscaphocapitate ligament by passing the tendon through a drill hole in the capitate dorsal to palmar and then obliquely palmar to dorsal via a drill hole in the radial styloid before suturing the tendon back on itself. Although the wrist motion was fair, with 30° of wrist extension, 20° of wrist flexion, 30% grip strength, and mild recurrent ulnar translation, the patient was unable to return to his job as a heavy equipment operator in the oil field.
More recently, Maschke et al. [6] described a cadaveric model for reconstructing the radioscaphocapitate using the brachioradialis tendon. The study showed prevention of ulnar translation when using the brachioradialis tendon with its insertion maintained on the radial styloid and passing it palmar to dorsal through a drill hole in the center of the capitate before anchoring it to the dorsal rim of the distal radius. This model offers several biomechanical advantages. First, retaining the brachioradialis tendon’s origin from the radial styloid and then passing it distally through the capitate allow for simulation of the radioscaphocapitate ligament’s near-anatomic origin from the radial styloid and its course as it inserts onto the capitate. Additionally, this model eliminates one of the points of potential insertion site failure of a free graft and has minimal donor site deficit.
In the present case, a young male auto mechanic presented with a 2-week-old radiocarpal dislocation involving his dominant wrist. Limited or total wrist arthrodesis was not considered a viable treatment option by the patient or the treating surgeon. Therefore, open treatment was undertaken, and the palmar and dorsal ligamentous structures were found to be attenuated and not deemed to be sufficient to provide a satisfactory result. Thus, the brachioradialis tendon was used to reconstruct the radioscaphocapitate ligament and to reinforce the dorsal capsular repair. Although the range of motion on the injured side was approximately 50% of that on the contralateral side, the patient returned to his previous occupation, reported no pain, and scored remarkably well on follow-up Disabilities of the Arm, Shoulder and Hand assessment.
In conclusion, we submit that reconstruction of an attenuated radioscaphocapitate ligament with the brachioradialis tendon is a reasonable alternative to wrist arthrodesis. The method provided satisfactory results in our case.
Acknowledgment
The authors thank the senior editor and writer Dori Kelly, MA, University of Maryland School of Medicine, for assistance with the manuscript.
References
- 1.Dumontier C, Meyer zu Reckendorf G, Sautet A, et al. Radiocarpal dislocations: classification and proposal for treatment: a review of twenty-seven cases. J Bone Joint Surg Am. 2001;83:212–218. doi: 10.2106/00004623-200102000-00008. [DOI] [PubMed] [Google Scholar]
- 2.Fehring T, Milek MA. Isolated volar dislocation of the radiocarpal joint: a case report. J Bone Joint Surg Am. 1984;66:464–466. [PubMed] [Google Scholar]
- 3.Freeland AE, Ferguson CA, McCraney WO. Palmar radiocarpal dislocation resulting in ulnar radiocarpal translocation and multidirectional instability. Orthopedics. 2006;29:604–608. doi: 10.3928/01477447-20060701-08. [DOI] [PubMed] [Google Scholar]
- 4.Grabow RJ, Catalano L., III Carpal dislocations. Hand Clin. 2006;22:485–500. doi: 10.1016/j.hcl.2006.07.004. [DOI] [PubMed] [Google Scholar]
- 5.Howard RF, Slawski DP, Gilula LA. Isolated palmar radiocarpal dislocation and ulnar translocation: a case report and review of the literature. J Hand Surg Am. 1997;22:78–82. doi: 10.1016/S0363-5023(05)80183-2. [DOI] [PubMed] [Google Scholar]
- 6.Maschke SD, Means KR, Jr, Parks BG, et al. A radiocarpal ligament reconstruction using brachioradialis for secondary ulnar translation of the carpus following radiocarpal dislocation: a cadaver study. J Hand Surg Am. 2010;35:256–261. doi: 10.1016/j.jhsa.2009.10.011. [DOI] [PubMed] [Google Scholar]
- 7.Mourikis A, Rebello G, Villafuerte J, et al. Radiocarpal dislocations: review of the literature with case presentations and a proposed treatment algorithm. Orthopedics. 2008;31:386–392. doi: 10.3928/01477447-20080401-24. [DOI] [PubMed] [Google Scholar]
- 8.Penny WH, III, Greene TL. Volar radiocarpal dislocation with ulnar translocation. J Orthop Trauma. 1988;2:322–326. doi: 10.1097/00005131-198802040-00009. [DOI] [PubMed] [Google Scholar]
- 9.Rayhack JM, Linscheid RL, Dobyns JH, et al. Posttraumatic ulnar translation of the carpus. J Hand Surg Am. 1987;12:180–189. doi: 10.1016/s0363-5023(87)80268-x. [DOI] [PubMed] [Google Scholar]
- 10.Thomsen S, Falstie-Jensen S. Palmar dislocation of the radiocarpal joint. J Hand Surg Am. 1989;14:627–630. doi: 10.1016/0363-5023(89)90179-2. [DOI] [PubMed] [Google Scholar]