Among the goals of surgically treating head and neck melanoma, the prevention of recurrence is foremost. Due to the proximity of the head and neck to vital structures such as the eyes, nose and mouth, it is incumbent on surgeons to achieve a balance between surgical requirements and the aesthetic needs of patients. Despite the many studies that have evaluated surgical outcomes, few, if any, have considered patient-based outcome measures. Previous studies have demonstrated that surgeon-based assessments suffer from poor interobserver agreement and poor test-retest reliability. Accordingly, the authors of this study used a visual analogue scale and an ordinal scale to measure a wide range of surgical outcomes from the patient perspective.
Keywords: Head and neck reconstruction, Local flap, Melanoma, Outcomes, Patient satisfaction
Abstract
BACKGROUND:
While studies have compared aesthetic outcomes following wide local excision of head and neck melanoma, none have evaluated this important outcome from the patient’s perspective. Indeed, one could argue that the psychosocial impact of head and neck melanoma excision and reconstruction is more accurately assessed by deriving patient-based as opposed to surgeon-based outcome measures.
OBJECTIVE:
To evaluate aesthetic outcomes following wide local excision of head and neck melanoma from the patient’s perspective.
METHODS:
Fifty-one patients who underwent excision of 57 head and neck melanomas followed by immediate closure by primary repair, skin grafting, local flap coverage or free tissue transfer were asked to complete a written survey at least six months after their surgery. A visual analogue scale (VAS) was used to assess the patient’s perception of appearance alteration, satisfaction with his or her appearance, and emotional impairment. An ordinal scale was used to evaluate several criteria of the reconstructive outcome (pain, itching, colour, scarring, stiffness, thickness and irregularity).
RESULTS:
Forty-two patients (82.4%) completed the survey. There were significant correlations between VAS scores reported for appearance alteration, satisfaction with outcome and emotional impairment (P=0.001). Patients who received skin grafts reported significantly unfavourable VAS scores compared with other methods of reconstruction (P=0.046). Moreover, skin grafts received significantly worse ordinal scale ratings for itching (P=0.043), colour (P=0.047), scarring (P=0.003) and stiffness (P=0.041) compared with other methods of reconstruction. Both skin grafts and free flaps were reported to have significantly less favourable thickness (P=0.012) and irregularity (P=0.036) than primary closure or local tissue transfer. There was no significant difference between patients undergoing primary closure with local tissue transfer (P>0.413). Other factors related to the patient’s VAS scores included location of the melanoma (P=0.033), size of defect (P=0.037) and recurrence of melanoma (P=0.042).
CONCLUSION:
The degree of emotional impairment following reconstruction of head and neck melanoma excision defects was correlated with the patient’s perception of appearance alteration. From the patient’s perspective, primary closure and local tissue transfer appeared to result in the highest aesthetic satisfaction.
Abstract
HISTORIQUE :
Des études ont comparé les résultats esthétiques après une importante excision locale d’un mélanome de la tête et du cou, mais aucune ne s’est attardée sur ce résultat important selon le point de vue du patient. Pourtant, on peut faire valoir que les répercussions psychosociales de l’excision d’un mélanome de la tête et du cou seront évaluées de manière plus exacte d’après les mesures de résultats du patient que du chirurgien.
OBJECTIF :
Évaluer les résultats esthétiques après l’excision importante d’un mélanome de la tête et du cou selon le point de vue du patient.
MÉTHODOLOGIE :
Cinquante et un patients qui ont subi une excision de 57 mélanomes de la tête et du cou suivie d’une fermeture immédiate par réparation primaire, par greffe cutanée, par recouvrement par un lambeau local ou par transfert de tissus libres ont été invités à répondre à un sondage écrit au moins six mois après l’opération. Une échelle analogique visuelle (ÉAV) a permis d’évaluer le point de vue du patient pour ce qui est de la modification de l’apparence, de la satisfaction envers l’apparence et de l’atteinte affective. Une échelle ordinale a servi à évaluer plusieurs critères des résultats de la reconstruction (douleur, démangeaison, couleur, cicatrice, épaisseur et irrégularité).
RÉSULTATS :
Quarante-deux patients (82,4 %) ont répondu au sondage. Il y avait une importante corrélation entre les indices de l’ÉAV relatifs à la modification de l’apparence et à la satisfaction des résultats et celui de l’atteinte affective (P=0,001). Les patients qui avaient subi une greffe de la peau ont déclaré des indices d’ÉAV particulièrement défavorables par rapport à d’autres modes de reconstruction (P=0,046). De plus, les greffes cutanées ont reçu des résultats beaucoup plus négatifs à l’échelle ordinale relativement aux démangeaisons (P=0,043), à la couleur (P=0,047), aux cicatrices (P=0,003) et à la raideur (P=0,041) par rapport à d’autres modes de reconstruction. Tant les greffes cutanées que les lambeaux libres donnaient des résultats considérablement moins favorables sur le plan de l’épaisseur (P=0,012) et de l’irrégularité (P=0,036) que la fermeture primaire ou le transfert local de tissus. Il n’y avait pas de différence significative entre les patients qui subissaient une fermeture primaire par transfert local de tissus (P>0,413). D’autres facteurs liés aux indices d’ÉAV des patients incluaient l’emplacement du mélanome (P=0,033), la dimension de l’anomalie (P=0,037) et la récurrence du mélanome (P=0,042).
CONCLUSION :
Le degré d’atteinte affective après la reconstruction d’anomalies causées par l’excision du mélanome de la tête et du cou était corrélé avec la perception qu’avait le patient des modifications à son apparence. Selon le point de vue du patient, la fermeture primaire et le transfert local de tissus semblaient s’associer à la plus grande satisfaction esthétique.
Head and neck melanoma poses challenges from both an oncological and a reconstructive perspective. First and foremost, these melanomas exhibit a higher rate of recurrence and poorer prognosis than melanomas in other locations (1). Furthermore, the proximity of head and neck melanomas to vital structures such as the eyes, nose and mouth requires that surgeons achieve a balance between adequate margins of excision and the functional and aesthetic needs of patients. With the increase in patient survival associated with better diagnostic and treatment protocols, attention to achieving these reconstructive goals has become increasingly important (2).
There are three main goals when surgically treating head and neck melanomas. First, and foremost, is the prevention of recurrence. This is best achieved by following the American Joint Commission on Cancer (AJCC) and National Comprehensive Cancer Network guidelines for margins of wide local excision, which vary from 0.5 cm to 2 cm depending on the thickness of nonmetastatic melanomas (3). The second goal is adequate coverage of soft tissue defects that are created by wide local excision. Several reconstructive techniques including primary closure, skin grafting, local tissue transfer and free flaps may be used in this setting without impacting recurrence rates (4). The third goal is selecting a method of soft tissue reconstruction that enables adequate restoration of function and optimizes aesthetic outcomes.
A few articles have reported on the preferred method of reconstruction to optimize aesthetic outcomes following wide local excision of head and neck melanomas. Primary closure is often sufficient for lesions <3 cm in diameter (5). Full thickness skin grafts were once the standard for larger defects, but they often left patients with disfiguring surface deformities and were replaced with more advanced reconstructive procedures (5,6). Currently, local tissue transfer is a common method of soft tissue reconstruction following excision of head and neck melanomas (4). Although only two articles have reported the outcomes of using local and free flaps in head and neck melanoma reconstruction, both described better functional and aesthetic outcomes than skin grafting in larger defects in which primary closure was not possible (4,6).
Anecdotal evidence largely supports the observation that plastic and reconstructive surgeons prefer local flap reconstruction over skin grafting whenever possible. The patient’s perspective on this matter, however, remains unknown. The intense psychosocial sequelae of extirpation and reconstruction of head and neck melanomas experienced by patients is important to evaluate from their perspective. Traditionally, subjective appearance evaluations are rarely solicited from patients due to the assumption that only expert evaluations provide a valid assessment of outcomes (7–9). It has been found, however, that the surgeon-based method of evaluation suffers from poor test-retest reliability and poor interobserver agreement (10). Interestingly, patient-based methods of evaluation are less affected by these factors (9–11).
Appearance scales using subjective ratings are often used in measuring breast reconstruction outcomes, and are accepted as a relevant and meaningful tool in evaluating aesthetic results (12,13). The visual analogue scale (VAS), specifically, is useful for measuring cosmetic outcomes of wounds and evaluating the patient’s satisfaction and emotions (14–16). Similarly, ordinal scales are useful for evaluating certain subcriteria of wounds. These scales can be used to rate the pain, itching, colour, scarring, thickness and irregularity of wounds and, thus, provide more detailed information about the wound itself than the unimodal VAS (17).
In the present study, patients undergoing head and neck melanoma excisions followed by soft tissue reconstruction were asked to evaluate their reconstructive outcomes. A VAS was used to evaluate the patient’s perception of appearance alteration, satisfaction with their result and emotional impairment. An ordinal scale was used to evaluate several criteria of the wound. These results were compared with information gathered from a retrospective medical record review, which included the patient’s demographics, melanoma characteristics, treatment and prognosis.
METHODS
Patients
The present study was reviewed and approved by the Institutional Review Board of Northwestern University (Chicago, Illinois, USA).
Between 2001 and 2007, 51 patients with 57 cutaneous melanomas of the head and neck underwent wide local excision followed by immediate wound reconstruction at a single institution. A surgical oncologist performed the wide local excisions according to AJCC and National Comprehensive Cancer Network guidelines, with lesser margins occasionally determined by proximity to critical structures. Wound reconstructions were performed by a plastic and reconstructive surgeon, and were categorized as primary closure, full thickness skin graft, local tissue transfer or free tissue transfer. In 2008, after all patients were given the opportunity to complete a follow-up period of at least six months, a retrospective medical record review and patient survey were completed.
A prospective surgical database was used to gather information regarding patient demographics (age, sex); melanoma characteristics (primary versus recurrent status, Breslow thickness, Clark’s stage, AJCC stage, histological diagnosis, and presence or absence of ulceration and/or regression); primary melanoma treatment (size of surgical margins and need for sentinal lymph node biopsy, lymph node dissection or adjuvant therapies); wound reconstruction (location and size of final wound defect, method of reconstruction and related complications); and outcome (follow-up period, current health status, and evidence of local, regional or distant recurrence of melanoma).
Patient surveys included VAS and ordinal scales. Surveys were completed by mail or e-mail at a minimum of six months following the patient’s surgery. VAS were used to evaluate the patient’s perspective on degree of alteration of appearance, satisfaction with appearance and emotional impairment. This scale was measured in millimetre increments from the left end of the scale, which represented no alteration in appearance, highest satisfaction or no emotional impairment. Ordinal scales were used to evaluate the patient’s perspective on several criteria of their reconstructive outcomes including overall appearance, pain, itching, colour, stiffness, thickness and irregularity. The ordinal scale ranged from 1 to 10, with ‘1’ being the best rating and ‘10’ being the worst. The patient survey is presented in Figure 1.
Figure 1).
Patient survey. A copy of the survey completed by patients at least six months following their melanoma excision and soft tissue reconstruction. Visual analogue scales were used to evaluate the patient’s perception of appearance alteration, satisfaction with the outcome and emotional impact of their procedures. These scales were measured in millimetre increments from the left end of the scale. Ordinal scales were used to evaluate several subcategories of the reconstructive outcome including sensations of pain and itching, and perceived severity of scarring, stiffness, thickness and irregularity. An overall ordinal score was generated by averaging all scores from the subcategories. In total, 82.4% of patients completed and returned the survey
Responses from patient surveys and data gathered from medical records were compared and analyzed. Statistical analysis was performed using SPSS version 17.0 (IBM Corporation, USA). Correlations were evaluated using the Spearman rho coefficient. Multivariate analysis using Kruskal-Wallis and Fisher’s exact test were used where appropriate to evaluate differences between groups.
RESULTS
Fifty-one patients (20 female, 31 male) with a mean age of 54 years (range 16 to 96 years) underwent wide local excision of 57 (53 primary, four recurrent) head and neck cutaneous melanomas followed by immediate plastic and reconstructive surgery wound reconstruction. The distribution of melanomas was as follows: 21 cheek, 10 auricle, seven forehead, seven neck, five scalp, four nose and three eyelid (Table 1). Histological diagnosis included 18 superficial spreading, 17 nodular, 14 lentigo maligna and eight other or unknown. According to the Breslow depth classification, there were eight in situ lesions, 21 lesions <0.76 cm, eleven between 0.76 cm and 1.5 cm, 11 between 1.5 cm and 4.0 cm, and three >4.0 cm. According to AJCC criteria, eight lesions were stage 0, 29 were stage I, 14 were stage II and three were stage III. There were no stage IV lesions at the time of initial diagnosis. Wide local excision margins ranged from 0.5 cm to 2.0 cm. In addition to wide local excision, 22 patients received sentinal lymph node biopsies, seven received complete lymph node dissections, and one underwent a superficial parotidectomy in addition to wide local excision. Six patients underwent adjuvant therapy with radiation, chemotherapy, interleukin-2, interferon and/or vaccine therapy.
TABLE 1.
Location of head and neck cutaneous melanomas
| Location | Frequency, n (%) | Survey responses, n |
|---|---|---|
| Cheek | 21 (36.8) | 7 |
| Ear | 10 (17.5) | 4 |
| Eye | 3 (5.3) | 6 |
| Forehead | 7 (12.3) | 16 |
| Neck | 7 (12.3) | 8 |
| Nose | 4 (7) | 3 |
| Scalp | 5 (8.8) | 4 |
| Total | 57 | 48 |
Reconstructive methods were categorized into primary closure, full thickness skin graft, local tissue transfer or free tissue transfer. There were 25 primary closures, 15 full thickness skin grafts, 15 local flaps (six advancement, five transposition and four rotational) and two free flaps. The mean defect size was 18.43 cm2 (range 1 cm2 to 144 cm2), but differed depending on type of reconstruction (Table 2).
TABLE 2.
Method of reconstruction following excision of head and neck cutaneous melanomas
| Method of reconstruction | Frequency, n (%) | Defect size, cm2, mean ± SD | Survey responses, n |
|---|---|---|---|
| Primary | 25 (43.9) | 9.2±10.1 | 19 |
| Skin graft | 15 (26.3) | 20.4±17.4 | 13 |
| Local flap | 15 (26.3) | 21.9±38.3 | 13 |
| Advancement | 6 | ||
| Rotational | 4 | ||
| Transposition | 5 | ||
| Free flap | 2 (3.5) | 90.5±13.4 | 2 |
| Total | 57 | 47 |
Patients were followed for a mean of 26.9 months (range one to 72.6 months). There were four complications resulting from the wide local excision or reconstruction including neuropraxia (primary closure), significant scar contracture (skin graft), hematoma (free flap) and neurotmesis (free flap). There were 13 instances of recurrence, representing 22.8% of patients (three local, two regional lymph node and eight distant metastasis). There was no difference between methods of reconstruction and complications or incidence of recurrence.
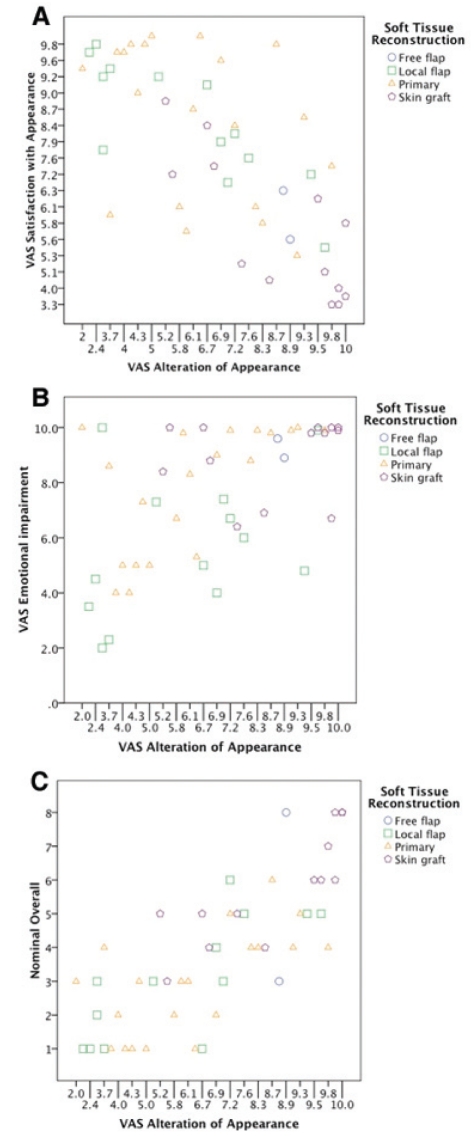
Forty-two patients (82.4%) completed the survey (Tables 1 and 2 summarize the number of survey responses according to location and method of reconstruction, respectively). Of those not completing the survey, three were deceased, five declined to participate and two could not be reached. Responses from the VAS were well correlated. The patients’ VAS scores for alteration of appearance were inversely correlated with their VAS scores for satisfaction with outcomes (Pearson correlation −0.702; P<0.01, Figure 2A) and directly correlated with their VAS scores for emotional impairment (Pearson correlation 0.542; P<0.05, Figure 2B). VAS scores for alteration of appearance were also directly correlated with the patients’ overall rating of their reconstructive outcomes on the ordinal scale (Spearman’s rho coefficient 0.789, P<0.001, Figure 2C).
Figure 2).
Correlation between alteration of appearance, satisfaction with outcomes, emotional impairment, and the overall nominal subcategory scale. There is a significant correlation between the way a patient perceives their alteration of appearance and satisfaction with their outcome (inverse correlation, Pearson coefficient −0.702, P<0.01) (A); emotional impairment (direct correlation, Pearson coefficient 0.542, P<0.05) (B); and overall ratings from the ordinal subcategory scale (direct correlation, Pearson coefficient 0.789, P<0.001) (C). VAS Visual analogue scale
The mean ± SD VAS score for alteration of appearance was 6.8±2.4. This score was significantly different depending on the location of melanoma, size of the defect and method of reconstruction. Melanomas located on the eyelid and nose received less favourable scores than those located on other parts of the head and neck (P<0.05 versus forehead or scalp, Figure 3A). Reconstruction with full thickness skin grafts received significantly worse scores than primary closure or local tissue transfer (P<0.05, Figure 3B). There was no significant difference between primary closure and local flaps. When comparing the size of defects of all head and neck melanomas, there was no statistically significant difference in VAS alteration of appearance scores (data not shown). When considering only cheek melanomas, however, there was a significant correlation between the defect size and the VAS alteration of appearance score (Spearman’s rho coefficient 0.525, P<0.05, Figure 3C).
Figure 3).
Factors affecting a patient’s perception of appearance alteration. Visual analogue scale (VAS) scores for alteration of appearance were significantly different depending on location of melanoma, method of reconstruction and size of defect. A Melanomas located on the eyelid and nose received less favourable scores than those located on other parts of the head and neck (P<0.05 versus forehead or scalp). B Reconstruction with full thickness skin grafts received significantly worse scores than primary closure or local tissue transfer (P<0.05). There was no significant difference between primary closure and local flaps. C There was a significant correlation between the defect size created by excision of cheek melanomas and the VAS alteration of appearance score (Spearman rho coefficient 0.525, P<0.05). Bar graphs are presented with a thick bar representing the mean, two solid purple bars representing the two interquartiles, and extension bars representing 95% CIs
Patients reported several differences between methods of reconstruction on the ordinal outcomes scale. Full thickness skin grafts were reported to be significantly “itchier” than the other reconstructive methods (P<0.05, Figure 4A). Scarring from skin grafts was also reported to be greater than scarring from primary closure and local tissue transfer (P<0.05), but not more than scarring resulting from free tissue transfer (Figure 4B). Skin grafts were reported to be stiffer than local tissue transfers (P<0.05), but not stiffer than primary closure or free flaps (Figure 4C). Skin grafts and free flaps were reported to be thicker and have more irregular contours than primary closure and local flaps (P<0.05, Figures 4D and 4E, respectively). As stated above, the patient’s overall perception of the reconstructive outcome on the ordinal scale was correlated to the VAS score (Figure 2C). There was no difference in pain reported between the different reconstructive techniques (data not shown). All other comparisons among reconstructive techniques were not statistically significant.
Figure 4).
Subcategorical evaluation of reconstructive outcomes. Outcomes from the various methods of reconstruction were evaluated using ordinal scales. A Full thickness skin grafts were reported to be significantly “itchier” than the other reconstructive methods (P<0.05). B Scarring from skin grafts was also reported to be greater than scarring from primary closure and local tissue transfer (P<0.05), but not more than scarring resulting from free tissue transfer. C Skin grafts were reported to be stiffer than local tissue transfers (P<0.05), but not stiffer than primary closure or free flaps. Skin grafts and free flaps were reported to be (D) thicker and (E) have more irregular contours than primary closure and local flaps. All other comparisons among reconstructive techniques were not statistically significant. Bar graphs are presented with a thick bar representing the mean, two solid purple bars representing the two interquartiles, two extension bars representing 95% CIs, and numbered dots representing outliers that were included in the statistical analysis
Recurrence was the only other factor to significantly affect VAS scores for emotional impairment (Figure 5, P<0.05); however, recurrence did not affect the patients’ VAS scores for alteration of appearance and satisfaction with appearance (data not shown). There was no difference between VAS scores and sex, age, Breslow depth, AJCC stage, performance of sentinel lymph node biopsy or lymph node dissection, histological diagnosis, presence of ulceration or regression, adjuvant treatment or surgical complications (data not shown).
Figure 5).
Emotional impact of recurrence. (Yes: recurrent diagnosis of melanoma; No: no recurrent diagnosis) Recurrent diagnosis with melanoma significantly affected patients’ visual analogue scale (VAS) scores for emotional impairment (P<0.05), but did not affect VAS scores for alteration of appearance and satisfaction with appearance (data not shown). Bar graphs are presented with a thick bar representing the mean, two solid purple bars representing the two interquartiles, two extension bars representing 95% confidence intervals, and numbered dots representing outliers that were included in the statistical analysis
DISCUSSION
Several important conclusions can be drawn from the present study. First, the emotional impact of soft tissue reconstruction following excision of head and neck melanomas was correlated to the degree to which patients perceive their appearance has been altered and by their satisfaction with the reconstructive outcome. Second, from the perspective of the patient, primary closure and local tissue transfer yielded the highest aesthetic satisfaction. Third, the degree of emotional impairment is also related to the location of melanoma on the head and neck, the size of the defect following wide local excision and incidence of recurrence.
The results of the present study indicate that patients share similar viewpoints to plastic surgeons when selecting a method of soft tissue reconstruction following excision of head and neck melanomas. Primary closure is the ideal method of reconstruction and should be used when defects are of proper size. When primary closure is inadequate, local tissue transfer offers a straightforward alternative that does not adversely affect local recurrence or increase patient morbidity (4). Skin grafts, on the other hand, tend to produce unfavourable outcomes. In the present study, patients reported less favourable skin color matching, poor stiffness, increased thickness and worse contour irregularities of skin grafts compared with local tissue transfers. Given the small number of free flaps in this series, it is difficult to comment on the patient’s viewpoint on this method of reconstruction.
Other factors correlating to VAS scores included the location of melanoma, size of the defect and incidence of recurrence. Eyelid and nose melanomas had a greater emotional impact on patients than those located on other parts of the head and neck. We presume this is true because the nose and eyelid are a major visual focus of attention for patients (18). The size of the defect also correlated with the patient’s VAS scores, but only after stratifying our results to solely the cheek location. We believe stratification by location is relevant because similar size defects of the eyelid and cheek are likely to have a different impact on patients. Furthermore, we chose the cheek because it represented the largest number and greatest variety of reconstructive cases in this series.
The incidence of recurrence had the greatest impact on emotional impairment when compared with all other factors examined in the present study. In fact, 12 of the 13 patients experiencing recurrence reported VAS scores for emotional impairment of 9 and greater. The observation that the patients’ VAS scores for appearance alteration and for satisfaction with outcome were not affected by recurrence suggests that emotional impairment following recurrence is less a function of reconstructive outcomes and more a function of the psychological impact of recurrence. More than one-half of patients who were diagnosed with recurrence in this study had stage IV disease, which itself is expected to have a large emotional impact on patients. And congruent to other studies, our series showed that the method of reconstruction did not appear to have an effect on recurrence (4).
Traditionally, the approach to evaluating subjective measures involves assessments by experts and not patients. This is based on the belief that experts can evaluate distinct components of reconstructive outcomes that are aesthetically desirable, offering other surgeons with specific and technical feedback. Our study would suggest that the patient’s opinion of his or her appearance is also an important factor to consider when evaluating aesthetic outcomes. The use of patient-based subjective evaluation scales is gaining popularity in plastic and reconstructive surgery and has provided surgeons with a valid method of assessing outcomes, especially following breast reconstruction (10–12). Of these scales, the VAS is often used to evaluate subjective feelings and satisfaction (15,16). The VAS has been used in several clinical scenarios including pain assessments and effectiveness of prescription medications (19,20). Advantages of the VAS include its high reproducibility, simplicity and intuitive use for patients, and its sensitivity to differences as small as 1 mm (21). Therefore, we believe the VAS was the best tool for assessing patient satisfaction and the emotional impact of head and neck melanoma reconstruction. The ordinal scale has different advantages. This scale allows subjects to rank outcomes (ordinal data) and is useful in evaluating subcategories of an outcome. The results of ordinal subcategory scales have been shown to have the greatest potential reliability because they explicitly specify the criteria that one wishes the evaluate (10). Therefore, we believe the ordinal scale was the best tool to evaluate specific attributes of the reconstructive outcome such as colour match, scarring and thickness.
Limitations of the present study merit discussion. First, the number of patients in this case series was small, limiting the study’s power and ability to draw statistically significant conclusions. For example, only two patients received free flaps in the present study. Although they both reported thickness and contour irregularities, it is difficult to conclude that these results are significant. Furthermore, our conclusion that local tissue transfer is superior to skin grafting is a generalization that does not account for location or defect size. Specific locations and sizes of wounds may benefit greatly from skin grafting.
CONCLUSION
The degree of emotional impairment following the reconstruction of head and neck melanoma extirpative defects correlates with the patient’s perception of appearance alteration. More importantly, from the patient’s perspective, primary closure and local tissue transfer are the preferred methods of reconstruction, while skin grafts are the least favoured.
Footnotes
DISCLOSURE: The authors have no financial interest in any of the products or techniques mentioned in this article. Also, there is no commercial association with any company related to this study.
REFERENCES
- 1.Fisher SR, O’Brien CJ. Head and neck melanoma. In: Balch CM, Houghton AN, Sober AJ, Hoong S, editors. Cutaneous Melanoma. St Louis: Quality Medical Publishing, Inc; 1998. pp. 163–71. [Google Scholar]
- 2.Brown TJ, Nelson BR. Malignant melanoma: A clinical review. Cutis. 1999;63:275–8. 281–4. [PubMed] [Google Scholar]
- 3.Coit DG. NCCN Practice Guidelines in Oncology- v.2.2009: Melanoma. National Comprehensive Cancer Network. < www.nccn.org> Last accessed February 19, 2009.
- 4.Bogle M, Kelly P, Shenaq J, Friedman J, Evans G. The role of soft tissue reconstruction after melanoma resection in the head and neck. Head Neck. 2001;23:8–15. [PubMed] [Google Scholar]
- 5.Eshima I. The role of plastic surgery in the treatment of malignant melanoma. Surg Clin North Am. 1996;76:1331–42. doi: 10.1016/s0039-6109(05)70518-1. [DOI] [PubMed] [Google Scholar]
- 6.Lent WM, Ariyan S. Flap reconstruction following wide local excision for primary malignant melanoma of the head and neck region. Ann Plast Surg. 1994;33:23–7. doi: 10.1097/00000637-199407000-00005. [DOI] [PubMed] [Google Scholar]
- 7.Asplund O, Nilsson B. Interobserver variation and cosmetic result of submuscular breast reconstruction. Scand J Plast Reconstr Surg. 1984;18:215–20. doi: 10.3109/02844318409052840. [DOI] [PubMed] [Google Scholar]
- 8.Kroll SS, Baldwin B. A comparison of outcomes using three different methods of breast reconstruction. Plast Reconstr Surg. 1992;90:455–62. doi: 10.1097/00006534-199209000-00015. [DOI] [PubMed] [Google Scholar]
- 9.Veiga DF, Neto MS, Garcia EB, et al. Evaluations of the aesthetic results and patient satisfaction with the late pedicled TRAM flap breast reconstruction. Ann Plast Surg. 2002;48:515–20. doi: 10.1097/00000637-200205000-00012. [DOI] [PubMed] [Google Scholar]
- 10.Lowery JC, Wilkins EG, Kuzon WM, Davis JA. Evaluations of aesthetic results in breast reconstruction: An analysis of reliability. Ann Plast Surg. 1996;36:601–6. doi: 10.1097/00000637-199606000-00007. [DOI] [PubMed] [Google Scholar]
- 11.Cohen M, Evanoff B, George LT, Brandt KE. A subjective scale for evaluating the appearance outcome of autologous breast reconstruction. Plast Reconstr Surg. 2005;116:440–9. doi: 10.1097/01.prs.0000173214.05854.e4. [DOI] [PubMed] [Google Scholar]
- 12.Kroll SS. Evaluations of aesthetic results in breast reconstruction: An analysis of reliability (discussion) Ann Plast Surg. 1996;36:607. doi: 10.1097/00000637-199606000-00007. [DOI] [PubMed] [Google Scholar]
- 13.Al-Ghazal SK, Blamey RW. Cosmetic assessment of breast-conserving surgery for primary breast cancer. Breast. 1999;8:162–8. doi: 10.1054/brst.1999.0017. [DOI] [PubMed] [Google Scholar]
- 14.Quinn JV, Drzewiecki AE, Steill IG, Elmslie TJ. Appearance scales to measure the cosmetic outcomes of healed lacerations. Am J Emerg Med. 1995;13:229–31. doi: 10.1016/0735-6757(95)90100-0. [DOI] [PubMed] [Google Scholar]
- 15.Aitken RC. Measurement of feelings using visual analog scales. Proc Roy Soc Med. 1969;62:989–93. doi: 10.1177/003591576906201005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Hayes MHJ, Paterson DG. Experimental development of the graphic rating method. Psychol Bull. 1921;18:98–9. [Google Scholar]
- 17.Singer AJ, Arora B, Dagum A, Valentine S, Hollander JE. Development and validation of a novel evaluation scale. Plast Reconstr Surg. 2007;120:1892–7. doi: 10.1097/01.prs.0000287275.15511.10. [DOI] [PubMed] [Google Scholar]
- 18.Alsarraf R, Larrabee WF, Jr, Anderson S, Murakami CS, Johnson CM., Jr Measuring cosmetic facial plastic surgery outcomes: A pilot study. Arch Facial Plast Surg. 2001;3:198–201. doi: 10.1001/archfaci.3.3.198. [DOI] [PubMed] [Google Scholar]
- 19.Huskisson EC. Visual analogue scales. In: Melzack R, editor. Pain Measurement and Assessment. New York: Raven Press; 1983. pp. 33–7. [Google Scholar]
- 20.Nicholson AN. Visual analogue scales and drug effects in man. Br J Clin Pharm. 1978;6:3–4. doi: 10.1111/j.1365-2125.1978.tb01673.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Dixon JS, Bird HA. Reproducibility along a 10 cm vertical visual analogue scale. Ann Rheum Dis. 1981;40:87–9. doi: 10.1136/ard.40.1.87. [DOI] [PMC free article] [PubMed] [Google Scholar]