Abstract
Symptomatic thymomas are characterized by non-specific thoracic symptoms or symptoms related to associated para-thymic syndromes. We report the case of a 56-year old Caucasian male who was affected by invasive (Masaoka IVA) WHO mixed AB-B2 thymoma after the elimination through the sputum of a fragment of tumour vegetating in the left upper lobar bronchus. The patient received multimodal treatment consisting of neoadjuvant cisplatinum-based polychemiotherapy, radical surgical resection (‘en bloc’ thymectomy, thymomectomy and pulmonary left upper lobe exeresis and pleural implants resection) and subsequent mediastinal radiation therapy. At 18-month follow-up, the patient is alive and disease-free.
Keywords: Thymoma, Symptoms, Diagnosis, Surgery, Multimodal treatment
CASE REPORT
A 56-year old Caucasian male who was a past smoker presented to the emergency room of our hospital because of the recent elimination through cough of a solid tissue fragment and blood. The past history was negative for pulmonary, pleural or other diseases. He denied therapy assumption and informed that the episode was the first occurring and no other symptoms were associated. The tissue sample, even though not accurately stained, was immediately sent to our pathologist who diagnosed a fragment of lymphoid epithelial tissue on the frozen section. The patient was examined by our otorhinolaryngologist who excluded lesions of the adenoids, of tonsils and of the oral cavity. Then, the patient was submitted to chest X-ray, demonstrating a large anterior mediastinal mass invading the upper lobe of the lung. Computed tomography (CT) scan of the chest and abdomen with contrast medium confirmed an anterior mediastinal mass (6 cm diameter), partially calcified, with no homogeneous contrast enhancement, invading the upper pulmonary lobe of the lung and vegetating into the upper segmental bronchus (Fig. 1). Left parietal pleural implants were demonstrated. CT-positron emission tomography (CT–PET) of the whole body confirmed all the demonstrated lesions to be avid of 18F-deoxyglucose [maximum standardized uptake value (SUVmax), 4.2]. Flexible bronchoscopy demonstrated the vegetation of the tumour into the upper segmental bronchus on the left side whereas the lobar bronchus was free from the disease. On the basis of the described elements, our pathologist made a diagnosis of thymoma, but more material to define the subtype of the disease was requested. An anterior mediastinotomy was carried out, and a diagnosis of WHO B2 thymoma at stage IVA of the Masaoka classification was done [1, 2]. Cisplatin-based neoadjuvant polychemotherapy (four courses of ADOC scheme) was administered. At the end of the medical therapy, the patient was restaged with total-body CT scan and CT-PET, demonstrating a partial response. Surgery was planned. Thymectomy and mobilization of the thymoma from the anterior mediastinum was achieved through partial sternotomy, then ‘en bloc’ left upper lobectomy was carried out through an associated left postero-lateral thoracotomy; parietal pleural implants removal, two small deposits on the visceral pleura of the inferior pulmonary lobe by wedge resection and hilar and mediastinal lymph nodes dissection were carried out too. The diagnosis of WHO mixed AB-B2 thymoma invading the upper lobe of the left lung vegetating into the left upper bronchus without hilar and mediastinal lymph node metastasis, and parietal and visceral pleural implants were posed on surgical samples. Necrosis up to 50% of the volume due to the previous chemotherapy was demonstrated on surgical specimens. The post-operative stay was characterized by self-limiting bleeding requiring blood transfusions; the patient was discharged on day 7. Adjuvant external beam radiation therapy by a 6-MV linear accelerator was administered (56 Gy, daily fractions 1.8–2.2 Gy) on the entire mediastinum and previous tumour bed. At 18-month follow-up, the patient is still alive and disease-free.
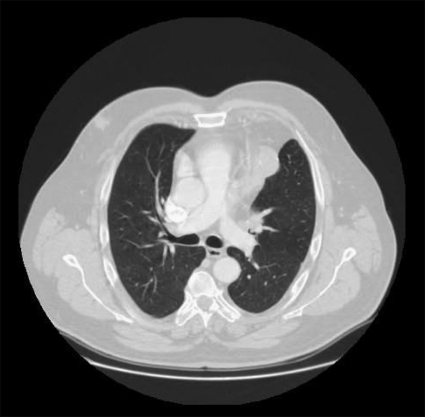
Figure 1:
CT scan of the chest, revealing the mediastinal tumour invading the upper lobe of the lung and vegetating into the bronchus justifying the symptom of ‘thymomaptysis’.
DISCUSSION
Thymomas are rare tumours and, in half of the cases, are asymptomatic and casually diagnosed after a routine chest X-ray [3]. When symptomatic, they are often associated with no specific symptoms such as thoracic pain, cough, dyspnoea or with symptoms related to para-thymic syndromes [3]. The literature reported <20 cases worldwide of thymomas with endobronchial growth, the majority of these but one being characterized by respiratory symptoms [4].
To our knowledge, this is the first case reported in the literature of a thymoma diagnosed after spontaneous elimination through the cough of a fragment of the tumour. Because of the rarity of the symptom, in a first time we focused on lesions of other lymphoid organs of the oral cavity and nose.
At the CT scan, the mediastinal tumour was demonstrated to directly invade the lung parenchyma up to the segmental bronchus of the culmen and to vegetate into it growing as a polypoid lesion; the endobronchial component of the tumour spontaneously broke and was eliminated with the cough.
After a long experience in thymoma surgery, we have never encountered a case such as this one [5].
In the past, other authors tried to confirm the diagnosis of thymoma with bronchoscopic biopsy and had frequent response of normal mucosa or necrotic tissue [4].
Consequently, we preferred to have confirmation of the subtype of the disease through an open mediastinal large biopsy and then the diagnosis of WHO B2 thymoma was posed. Even though some calcifications were demonstrated at CT scan, we were suspecting more aggressive subtype of thymic tumour such as a WHO B3 or a thymic carcinoma. Probably, considering the presence of tumour calcification, the local extension and the B2 subtype, this was the case of a long-lasting asymptomatic disease which slowly grew up to invade the bronchus and finally revealed itself with the first episode of ‘thymomaptysis’. Because of the demonstrated chemo-sensitivity of thymomas, we submitted our patient to four courses of ADOC scheme obtaining a partial response. The sequent surgical intervention was carried out with the aim of complete resection of all the resectable disease with the maximum respect of the residual function. The deep invasion of the lung parenchyma should have caused the dissemination to the lobar, hilar and mediastinal lymph nodes. These lymph nodal stations are not typical for mediastinal invasive thymic tumours but in the specific case we carried out an hilar–mediastinal lymph nodal sampling to evaluate the possible local dissemination of the tumour such as a lung cancer. The absence of lymph nodal dissemination and the presence of pleural implants determined the pathological WHO staging pT4N0Mx [1] which is correspondent to the Masaoka stage IVA [2]. Adjuvant radiation therapy was carried out to minimize the potential of mediastinal recurrence [6]. Even if the follow-up period may be considered short for a WHO-mixed AB-B2 thymoma, we think the absence of demonstrated disease after 18 months in a Masaoka stage IVA tumour should be considered as a good intermediate result.
Long-term follow-up will be attempted in order to evaluate the possibility of an aerogenous pulmonary dissemination due to the previous endobronchial growth.
Conflict of interest: none declared.
REFERENCES
- 1.Harris CC. In: World Health Organization Classification of Tumors. Pathology, Genetics of Tumors of the Lung, Pleura, Thymus and Heart. Travis WD, Brambilla E, Mueller-Hermelink HK, editors; Lyon: IARC Press; 2004. [Google Scholar]
- 2.Masaoka A, Monden Y, Nakahara K, Tanioka T. Follow-up study of thymomas with special reference to their clinical stages. Cancer. 1981;48:2485–92. doi: 10.1002/1097-0142(19811201)48:11<2485::aid-cncr2820481123>3.0.co;2-r. doi:10.1002/1097-0142(19811201)48:11<2485::AID-CNCR2820481123>3.0.CO;2-R. [DOI] [PubMed] [Google Scholar]
- 3.Detterbeck FC, Parsons AM. Thymic tumours. Ann Thorac Surg. 2004;77:1860–9. doi: 10.1016/j.athoracsur.2003.10.001. doi:10.1016/j.athoracsur.2003.10.001. [DOI] [PubMed] [Google Scholar]
- 4.Sakuraba M, Sagara Y, Tamura A, Park Z, Hebisawa A, Komatsu H. A case of invasive thymoma with endobronchial growth. Ann Thorac Cardiovasc Surg. 2005;11:114–6. [PubMed] [Google Scholar]
- 5.Rena O, Papalia E, Maggi G, Oliaro A, Ruffini E, Filosso PL, et al. World Health Organization classification: an independent prognostic factor in resected thymomas. Lung Cancer. 2005;50:59–66. doi: 10.1016/j.lungcan.2005.05.009. doi:10.1016/j.lungcan.2005.05.009. [DOI] [PubMed] [Google Scholar]
- 6.Ogawa K, Uno T, Toita T, Onishi H, Yoshida H, Kakinobana Y, et al. Postoperative radiotherapy for patients with completely resected thymoma: a multiistitutional, retrospective review of 103 patients. Cancer. 2002;94:1405–13. doi: 10.1002/cncr.10373. doi:10.1002/cncr.10373. [DOI] [PubMed] [Google Scholar]