Abstract
Objective
College matriculation begins a period of transition into adulthood, one that is marked by new freedoms and responsibilities. This transition also is marked by an escalation in heavy drinking and other drug use, and a variety of use-related negative consequences. Trauma and symptoms of posttraumatic stress disorder (PTSD) may affect alcohol and drug problems, and thus may be a point of intervention. Yet no studies have examined trauma, PTSD, and alcohol and drug problem associations during this developmental period. The present study provides such an examination.
Method
Matriculating college students (N=997) completed surveys in September (T1) and at five subsequent time points (T2-T6) over their first year of college. With latent growth analysis, trajectories of alcohol and drug-related consequences were modeled to examine how trauma (No Criterion A Trauma, Criterion A Only, No PTSD symptoms) and PTSD (partial or full) symptom status predicted these trajectories.
Results
Results showed substantial risk for alcohol- and other drug-related negative consequences that is conferred by the presence of PTSD at matriculation. Those with both partial and full PTSD started the year with more alcohol and drug consequences. These individuals showed a steeper decrease in consequences in the first semester, which leveled off as the year progressed. Both alcohol and drug consequences remained higher for those in the PTSD group throughout the academic year. Hyper-arousal symptoms showed unique effects on substance consequence trajectories. Risk patterns were consistent for both partial and full PTSD symptom presentations. Trajectories did not vary by gender.
Conclusions
Interventions that offer support and resources to students entering college with PTSD may help to ameliorate problem substance use and may ultimately facilitate a stronger transition into college and beyond.
Introduction
Of the 8 million college students in the U.S., as many as 25% meet DSM-IV criteria for an alcohol or other substance use disorder (Blanco et al., 2008; Dawson, Grant, Stinson, & Chou, 2004; Wu, Pilowsky, Schlenger, & Hasin, 2007). Many more engage in problem substance use which, though below diagnostic threshold, can lead to hazardous outcomes both acutely (e.g., sexually transmitted infections, interpersonal violence, intoxicated driving, overdose; Caldeira, Arria, O'Grady, Vincent, & Wish, 2008; O'Malley & Johnston, 2002; Rimza & Moses, 2005) and long-term (e.g., abuse or dependence; Arria, Vincent, & Caldeira, 2009; McCabe, West, & Wechsler, 2007; O'Neil, Parra, & Sher, 2001). Factors that contribute to substance misuse in college can be targeted in preventive interventions. Data now are emerging to suggest that trauma and posttraumatic stress are among these factors.
Trauma exposure among college students is unfortunately common (Marx & Sloan, 2003; Read, Ouimette, White, Colder, & Farrow, 2011; Scarpa et al., 2002). The traumas that college students experience are significant by any standard - including but not limited to sexual assault and other interpersonal violence, natural disasters, military trauma, life-threatening illness, and motor vehicle accidents (Read et al., 2011; Ullman & Filipas, 2005).
Research supports a dimensional model of psychological responses to trauma, with PTSD falling at the far end of the continuum (Broman-Fulks et al., 2006; Ruscio, Ruscio, & Keane, 2002). A substantial portion of trauma-exposed individuals do not meet full criteria for a PTSD diagnosis, but nonetheless experience significant trauma-associated distress (Mylle & Maes, 2004; Mendlowicz & Stein, 2000; Schnurr et al., 2000; Zlotnick et al., 2002). Whereas the prevalence of PTSD in college students is estimated to be around 9% (Read et al., 2011; Smyth, Hockemeyer, Heron, Wonderlich, & Pennebaker, 2008), rates of sub-syndromal PTSD are higher (30-35%; Lauterbach & Vrana, 2001; Smyth et al., 2008).
Theory and data suggest that PTSD and substance misuse may be etiologically linked, and in particular that trauma and PTSD may pose risk for the development of problem substance use. This literature is reviewed briefly below.
Substance Involvement Following Trauma and Traumatic Stress: Self-Medication
Prominent among theories posited to explain relations among trauma, PTSD, and substance involvement is the “Self-Medication” hypothesis (Khantzian, 2003). According to this framework, substance use occurs as an effort to manage distressing affect or symptoms associated with a trauma (Jacobsen, Southwick, & Kosten, 2001; Saladin et al., 1995).
Some empirical evidence supports the self-medication hypothesis with respect to traumatic stress and substance use (McFarlane et al., 2009; Ouimette, Coolhart, Funderburk, & Brown, 2007; Read, Brown, & Kahler, 2004; Stewart, Pihl, Conrod, & Dongier, 1998). Though studies in college populations have not examined self-medication of PTSD symptoms per se, data do show that students cite stress and negative affect as among the primary reasons for substance use (Flynn, 2000; Kassel, Jackson, & Unrod, 2000; O'Hare & Sherrer, 2000), and negative affect has been linked uniquely to substance consequences in this population, independent of consumption (Martens et al., 2008; Read et al., 2003; Simons, Gaher, Oliver, Bush, & Palmer, 2005).
Trauma effects vs. PTSD effects
Consistent with a self-medication formulation is the notion that individuals may use substances not so much in response to trauma alone, but as a result of psychological distress that follows the trauma. Data from older adult samples offer some support for this notion (Breslau & Davis, 1992; Epstein, Saunders, Kilpatrick, & Resnick, 1998; Lepore, 1997; Stewart & Conrod, 2003). Yet research with college samples has focused primarily on substance involvement following trauma exposure (e.g., Goldstein, Flett, & Wekerle, 2010; Klanecky, Harrington, & McChargue, 2008; McCauley, Ruggiero, Resnick, Conoscenti, & Kilpatrick, 2010) and with only a few exceptions (e.g., McDevitt-Murphy et al., 2010; Reed et al., 2007) has not typically examined the relative contribution of trauma exposure versus the contribution of symptoms resulting from such exposure.
Symptom cluster associations
According to the DSM, PTSD is comprised of three core symptom clusters, re-experiencing, avoidance/numbing, and hyper-arousal. Numerous studies have examined whether specific PTSD symptom clusters may be associated uniquely with substance outcomes, and have yielded disparate findings. The cluster of symptoms characterized by hyperarousal has been posited by some to be most strongly implicated in self-medication processes (see Stewart et al., 1998), yet empirical support for a specific effect of hyperarousal symptoms has been mixed. Though some work supports a unique link between these symptoms and substance outcomes (Shipherd et al., 2005 [illicit drug involvement only]; Stewart et al., 1999 [alcohol only]), other studies find either no effect for hyperarousal (Cook et al., 2009; McDevitt Murphy et al, 2010; Read et al., 2004; Shipherd et al., 2005 [alcohol use]) or an effect of hyper-arousal, but for other symptoms clusters as well (Jakupcak et al., 2010; McFall et al., 1992; Saladin et al., 1995; Stewart et al., 1999 [illicit drugs]Taft et al., 2007). No studies have tested these effects prospectively in a college sample.
Gender, PTSD, and Substance Involvement
Gender differences in PTSD, substance involvement, and the interaction between the two clinical phenomena have been noted. Women are at greater risk for PTSD following trauma exposure (e.g., Breslau et al., 1997, 2001; Kessler et al., 1995; Schnurr et al., 2002), even when controlling for type of trauma (Breslau, 2001). Further, across the lifespan, male gender is a risk factor for substance use and consequences (Lex, 1991; Spear, 2002; Thompson et al., 2009). At least one recent study has found gender differences in the mechanisms that may underlie co-occurring PTSD and alcohol involvement (Bornavalova, Ouimette, Crawford, & Levy, 2009). Together, existing research suggests that the effects of trauma and PTSD symptom status on alcohol and illicit drug trajectories could differ for men and women.
Summary
The first year of college is a time of excitement and possibility, as students take an important step toward independence. It is also a time of instability and transition, hallmark features of which are an increase in autonomy, a decrease in adult supervision, a shift in both quantity and quality of peer relationships (Arnett, 2000; 2005) and for many, an increase in substance use (Arria et al., 2008). As Sher and Rutledge (2007) note, the extant literature does not offer much in the way of examination of risk factors for substance misuse over this transitional period. Self-Medication theory would suggest that students with PTSD may rely on substances to help manage the many changes and challenges that they face during this transition as more familiar resources are absent or less available. Though an abundant literature has identified a link between PTSD and substance problems in older adult populations, PTSD as a risk factor for substance misuse in college students has been ignored.
The Present Study
The objective of the present study was to provide what is to our knowledge the first examination of the prospective relationship between trauma, posttraumatic stress symptoms, and substance-related consequences in students at the transition into college. We hypothesized that individuals with significant PTSD symptoms would show more problematic substance involvement across the first year of college.
In our investigation we modeled four discrete categories of trauma exposure and PTSD symptoms in order to contrast the prospective associations with substance outcomes across exposure and symptom levels. These levels were (1) No Criterion A exposure, (2) Criterion A exposure, but no significant PTSD symptoms, (3) Sub-threshold PTSD symptoms (Partial PTSD), and (4) Full PTSD. We hypothesized alcohol and drug consequence trajectories would differ by trauma and PTSD symptom status, with PTSD symptoms conferring greater risk relative to trauma exposure alone.
In more exploratory analysis, we also sought to understand the contribution of trauma and PTSD symptom characteristics to substance consequence trajectories. Thus, we examined whether unique effects of specific PTSD symptom clusters might be observed for alcohol and other drug consequence trajectories in our college sample. Given the mixed nature of extant findings, and the paucity of research in this area with college students, we did not forward a priori hypotheses. We also sought to examine the contribution of trauma severity to substance outcomes. Here again we forwarded no a priori hypotheses.
Finally, as gender differences have been observed both in posttraumatic stress and in substance involvement, we also evaluated whether the effects of posttraumatic stress on alcohol and other drug consequences were moderated by gender. We posited that the PTSD effects on alcohol/drug consequence trajectories would be stronger for women than for men.
Method
Participants
Participants (N=997; 65% female) were from a longitudinal study which began at college matriculation. Data analyzed in this study included six time points (see Figure 1) over the first year of college. At T1 (Sept), the average age was 18.12 (SD=0.45). Seventy three percent of participants self-identified as Anglo Caucasian (N = 723), 11% as Asian (N =113), 9% as Black (N =90), 3% as Hispanic/Latino (N = 33), less than 1% as American Indian/Alaskan (N=2), or Hawaiian/Pacific Islander (N =1), and 3% as multi-racial (N =31). Four participants did not report ethnicity. Eligibility, recruitment, and sample selection is described below.
Figure 1.
Schedule of Recruitment and Data Collection.
Procedure
Initial screening
To obtain the target longitudinal sample, college students at two mid-size public universities in the northeastern (Site A) and southeastern (Site B) parts of the United States screened for trauma and PTSD in the summer prior to matriculation. All students were sent an e-mail with a link to a secure online screening survey. An identical hard-copy packet was sent via postal mail. A return rate of 58% (3391/5885) was achieved, comparable to other studies using similar methodologies (e.g., Neighbors, Geisner, & Lee, 2008; Larimer, Turner, Mallet, & Geisner, 2004; Lewis et al., 2007). After deletion of cases with insufficient data to determine trauma and PTSD symptom status (see below), the final screening sample consisted of 3,014 students (59% female).
Longitudinal sample selection
To have sufficient representation of students with significant traumatic stress, we invited for participation all those who (1) reported at least one lifetime criterion A trauma and (2) endorsed at least one symptom from each of the three PTSD symptom clusters. Across sites, 649 participants met these criteria. An additional 585 students who did not meet trauma inclusion criteria were selected randomly for prospective follow-up.
E-mails and a link to the baseline survey (Time 1; T1) were sent to this selected sample (N = 1,234). At completion of the baseline survey, participants were sent a $20 gift card. Eighty-one percent (N=997) of those invited completed the baseline survey in September, and thus constituted the longitudinal sample. This sample was assessed five more times over the year. Across cohorts, the retention rate was 91.3%.
Measures
The present study is focused on a portion of the data from a larger longitudinal study. Measures used in the present study are described below. A schedule of these measures and the time points for which they are analyzed is provided in Figure 1.
Alcohol use
Participants were asked to indicate whether they had consumed any alcohol in the past month. Those participants who indicated that they had consumed alcohol at least once were asked to complete additional questions about their alcohol use. All participants were provided with a standard drink measurement chart to increase accuracy of reporting. Alcohol use was measured with items regarding typical quantity and frequency of alcohol consumption per week in a past one month interval (Wood, Read, Palfai and Stevenson, 2001). Quantity-frequency (QF) indices were created by multiplying item responses. This measure was used for descriptive purposes.
Alcohol-related consequences
Past month consequences associated with alcohol consumption were assessed with the 48-item Young Adult Alcohol Consequences Questionnaire (YAACQ; Read et al., 2006). Items assess a broad array of consequences that range in severity. Response options are rated dichotomously (yes-no) and thus the YAACQ yields a score that ranges from 0 to 48. The YAACQ has strong psychometric properties, including convergent validity and test-retest reliability (Read, Merrill, Kahler, & Strong, 2008). Participants who were not asked to complete these items (i.e. had no past month use) received a consequences score of 0. Cronbach's alpha for the total YAACQ score in this sample was .98.
Illicit substance use
Participants were asked to indicate whether they had used illicit drugs (i.e., cannabis, cocaine, stimulants, inhalants, sedatives or sleeping pills, hallucinogens, or opioids) in the past month (O'Malley & Johnson, 2002). Those participants who answered in the affirmative were asked to indicate the frequency with which they used each drug during the past month for a non-medical reason. Responses ranged from 0=never in the past month to 6=every day. This measure was used for descriptive purposes.
Illicit substance-related consequences
Participants who indicated that they had used substances in the past 30 days were asked to respond whether they had experienced a series of 24 substance-related consequences. Items were adapted from the YAACQ and the Brief YAACQ (Kahler, Strong, & Read, 2005), reworded to be relevant to drugs. Items were scored dichotomously and summed to create a total drug consequence score which could range from 0-24. Individuals who reported no use received a zero on this measure. Cronbach's alpha for the substance consequences scale in this sample was .98.
Big Five Inventory
To isolate the unique influences of PTSD, we controlled for negative affect in all models. We assessed baseline negative affect with the Neuroticism subscale (8 items) of the Big Five Inventory (BFI; John & Srivastava, 1999), a 44-item measure that assesses five personality dimensions: Openness, Conscientiousness, Extraversion, Agreeableness, and Neuroticism. Items consist of short phrases based on adjectives that assess prototypical features of each personality dimension, scored using a 5-point Likert scale. The Neuroticism subscale demonstrated good internal reliability (T1 alpha = .84). Possible scores ranged from 8 to 40.
Trauma Exposure
At matriculation, students were screened for criterion A trauma with items based on the Traumatic Life Events Questionnaire (Kubany et al., 2000). Seven items assessed exposure to: (1) accident/natural disaster/fire; (2) combat; (3) sudden unexpected death of a loved one; (4) life-threatening illness (to self or loved one); (5) physical assault; (6) sexual assault; or (7) other event that was life-threatening, caused serious injury, or extreme distress. A follow-up question assessed subjective responses (i.e., fear, helplessness, or horror) to each endorsed event.
In the longitudinal portion of the study, the Traumatic Life Events Questionnaire (TLEQ; Kubany et al., 2000, copyright © 2004 by Western Psychological Services. WPS, Format adapted by J. Read, SUNY at Buffalo) was used to assess trauma exposure. At Time 1, lifetime exposure was assessed. The TLEQ assesses a range of traumatic experiences consistent with the DSM IV-TR definition, including the subjective responses that comprise Criterion A.2. This measure has demonstrated good psychometric properties, and has been used with college students (Kubany et al., 2000). Scores yielded a count of lifetime traumas endorsed that were accompanied by fear, helplessness, or horror (i.e., Criterion A trauma). The number of trauma types that an individual has experienced has been used as an index of trauma severity (Bernat et al., 1998; Perkonigg et al., 2000) and has been shown to be among the strongest predictors of the development of PTSD. Accordingly, we used the TLEQ summed score (range = 0-22) to index trauma severity, with total scores representing the number of discrete types of trauma experienced.
Posttraumatic Stress Symptoms
PTSD was assessed using the PTSD Checklist-Civilian Version (PCL-C; Weathers, Huska, & Keane, 1991; Weathers, Litz, Herman, Huska, & Keane, 1993). This 17-item measure assesses Criteria B (re-experiencing), C (avoidance/numbing), and D (arousal) of the PTSD construct consistent with the DSM-IV, and has been shown to correspond strongly to gold-standard interview measures of PTSD (Andrykowski, Cordova, Studts, & Miller, 1998; Lang, Laffaye, Satz, Dresselhaus, & Stein, 2003). Participants rated on a 5-point scale (never to almost always) how much they had been bothered by each symptom in the past month. These idiographic traumas were programmed into the PCL instructions and participants were instructed to think about the particular traumatic event(s) that they endorsed while filling out the PCL-C (e.g., “You indicated that you have been in a fire and have experienced the sudden death of a loved one. For the next questions we would like you to think specifically about your response to that event…”). For those who did not report lifetime criterion A exposure, the computerized PCL prompted respondents to think about how they respond in general to stressful events that they have experienced.
Following Blanchard et al. (1996), empirically derived severity threshold cut-scores were created for all items on the PCL. This involved dichotomously scoring each item as either “1” or “0” based on the severity rating that the participant assigns on the 5-point Likert-type scale. Items rated as 3 or 4 (depending on the item, see Blanchard et al. 1996) or higher are scored as a “1”. All other ratings are scored as a “0”. Using this approach, each of the 17 items was dichotomously scored to reflect whether that symptom was “present” or “absent”. Thus, the possible range of scores on this measure is from 0-17. This scoring produces a clinically meaningful symptom count. Symptoms from criteria B, C, and D were summed to create a symptom count in each cluster. Possible subscale symptom scores ranged from 0-5 for re-experiencing (B), 0-7 for avoidance/numbing (C), and 0-5 for arousal (D).
Data Analytic Plan
After data cleaning, our first step was to examine frequencies of trauma, PTSD, and substance use variables. We also examined bivariate associations among model variables. Following this, latent growth models (LGMs) were used to test our primary aims because they provide an analytic framework to describe sample average trajectories as well as individual differences in growth and predictors of individual differences in growth (Curran & Muthén, 1999). Our central question was whether baseline trauma exposure and PTSD symptom status (Trauma and PTSD Group) predicted change in alcohol and drug consequences across the first year of college. Accordingly, we tested a series of unconditional growth models to determine the shape of growth in alcohol and drug consequences, and then tested conditional growth models with trauma and PTSD status as predictors of growth factors. To examine whether both alcohol and drug consequence trajectories differed for men and women, we estimated multiple group models and used nested chi-square tests to examine the equivalence of parameters across gender.
To examine differences in trajectories across trauma and PTSD symptom categories, we created three dummy coded variables based on four orthogonal groups (i.e., participants could only be included as a member of one PTSD symptom category). The groups were (1) No criterion A trauma, no significant PTSD symptoms (No Criterion A), (2) Criterion A exposure, but no significant PTSD symptoms (Criterion A Only), (3) Criterion A exposure and at least one symptom in each symptom cluster (Partial PTSD), and (4) Criterion A exposure and full PTSD symptoms -1 Re-Experiencing, 3 Avoidance, 2 Hyperarousal,– met (Full PTSD). Full PTSD was the reference group, and thus the dummy coded variables contrasted each of the remaining groups to the Full PTSD group. These dummy coded variables were created to allow us to examine the relative contribution of trauma exposure versus posttraumatic stress symptoms to alcohol and drug consequences. Site also was a covariate. In secondary analyses, we also examined the prospective influence of specific symptom clusters (re-experiencing, avoidance/numbing, hyper-arousal), and of trauma severity on consequences trajectories. To control for the possible contribution of general negative affect, symptoms of which might overlap with and thus confound the influence of PTSD symptoms, all models included baseline trait negative affect, measured by the BFI.
Growth models were estimated in Mplus version 6.1 (Muthén & Muthén, 2010). The observed alcohol and drug consequence variables were skewed (values from 1.8-4.5), and thus robust maximum likelihood estimation was used to correct fit indices and standard errors for the effects of non-normality. Nested model tests were performed using robust maximum likelihood chi-square difference tests (Muthén & Muthén (2010). Separate models were estimated for alcohol and drug consequences. In addition to the model Χ2, we report the Comparative Fit Index (CFI), Tucker-Lewis Index (TLI), and Root Mean Square Error of Approximation (RMSEA). According to Hu and Bentler (1999), CFI >.95, TLI > .95, and RMSEA < .05 indicate a well-fitting model.
Management of missing data
All participants had complete data on outcome variables at Time 1. Eighty-one percent (n=810) of the sample completed all six time points; 90% (n=900) completed at least five time points. Three percent (n=23) completed two or fewer time points. At the item level, rates of missed/skipped items (including cases with a missing time point) were 9.9% (alcohol) and 9.2% (drug) consequences, respectively, over all 6 assessments.
To examine the potential influence of missing data, two dummy variables were created to indicate whether a participant had missing data on alcohol and drug consequence variables at any of the 5 longitudinal time points. We examined whether these dummy variables were related to model variables, or to trauma group. For alcohol and drug consequences, missing data was related to neuroticism, site and trauma group. Missing data on alcohol consequences was not related to T1 alcohol consequences, but presence of any missing data on substance consequences was related to T1 substance consequences. Missing data was unrelated to sex for both outcomes. Missing data did not differ across trauma/ PTSD symptom groups, for alcohol (F [3,993]=.22) or drug consequences (F[3, 993] = 2.3), ps >. 05). To gauge the influence of missing data, we calculated effect sizes for each association. Cohen's d (continuous variables) ranged from .16 to .35, and Craemer's Phi (dichotomous) coefficients ranged from .05 to .18 – all small effects (Cohen, 1988). Still, to minimize even a small impact, we used full-information robust maximum likelihood estimation, rather than listwise deletion in our analyses.
Results
Rates of Trauma, PTSD, Alcohol and Drug Involvement
Seventy-four percent of the sample (N=735) endorsed at least one criterion A trauma. Among those, the average number of traumas (trauma severity) was 3.09 (SD=2.19). Trauma types were diverse and included, but were not limited to, interpersonal traumas (e.g., unwanted sexual contact, 13%); physical assault by partner (7%), natural disasters (11%), sudden or unexpected death of someone close (65%), life-threatening illness or injury of other (47%) or self (5%), and motor vehicle accidents (11%). The average number of PTSD symptoms among those with a criterion A trauma was 4.60 (SD=4.06). Fifteen percent (N=152) of participants met criteria for full PTSD (criterion A trauma exposure and 1 B, 3 C, 2 D symptoms). An additional 15% (N= 151) met criteria for partial PTSD (trauma exposure and 1 PTSD symptom in each cluster).
At baseline, participants typically consumed 6.42 (SD=9.70) alcoholic drinks per week in the past month, drinking on an average of 1.43 occasions (SD=1.48) weekly. The average number of alcohol consequences in the month prior to baseline assessment was 5.34 (7.41). Thirty-nine percent (n=390) of our participants did not report any alcohol consequences at baseline and thus had a score of zero for this measure.
Across the six time points, rates of ever having used illicit substances were 30% (N=299) for cannabis, 7.1% (N=71) for amphetamines, 5.6% (N=56) for cocaine, 2.2% (N=22) for inhalants, 9.1% (N=91) for sedatives, 4.4% (N=44) for hallucinogens, and 6.2% (N=62) for opiates. Among those reporting drug use, the modal number of drugs used at any given time point was one. Seventy-nine percent (n=974) reported no drug consequences.
Group Differences on Demographics, TLEQ, PCL, and Substance Use-Related Consequences
As shown in Table 1, there were no group differences on age and ethnicity, however, there were gender differences on trauma and PTSD status. Group differences were also observed on neuroticism. These findings suggest that it is important to include gender and neuroticism when testing group differences in subsequent analysis. As expected, there were group differences on the TLEQ and PCL.
Table 1. Comparison of Trauma and PTSD Group Status on Demographics and Self-Report Measures.
| No Criterion A (n=263) |
Criterion A Only (n=431) |
Partial PTSD (n=151) |
Full PTSD (n=152) |
||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| n | % | n | % | n | % | n | % | χ2 | df | p | |
| Sex | |||||||||||
| Female | 114 | 43.3 | 303 | 70.3 | 117 | 77.5 | 115 | 75.7 | 77.59 | 3 | .00 |
| Ethnicity | |||||||||||
| Caucasian | 204 | 77.6 | 308 | 71.5 | 107 | 70.9 | 104 | 68.4 | 4.57 | 3 | .21 |
| Other | 59 | 22.4 | 122 | 28.3 | 42 | 27.8 | 47 | 30.9 | |||
| M | SD | M | SD | M | SD | M | SD | F | df | p | |
| Age | 18.13 | .39 | 18.11 | .48 | 18.05 | .24 | 18.17 | .57 | 2.052 | (3, 993) | .105 |
| # Criterion A Events (TLEQ) | 0 | 0 | 2.46 | 1.68 | 3.54 | 2.18 | 4.44 | 2.69 | 255.25 | (3, 993) | .000 |
| PTSD Symptom Count (from PCL w/Blanchard cutoffs) | 1.22 | 2.64 | 1.89 | 1.81 | 6.22 | 1.88 | 10.68 | 2.57 | 791.49 | (3, 993) | .000 |
| Neuroticism (BFI) | 2.64 | 0.77 | 3.07 | 0.80 | 3.32 | 0.86 | 3.54 | 0.75 | 48.36 | (3, 993) | .000 |
| Alcohol Problems Fall Semestera | 2.71 | 4.57 | 3.65 | 5.61 | 5.22 | 6.10 | 5.95 | 8.04 | 9.99 | (3, 991) | .000 |
| Alcohol Problems Spring Semesterb | 2.80 | 5.50 | 3.37 | 6.05 | 5.64 | 8.22 | 5.34 | 8.18 | 7.31 | (3, 912) | .000 |
| Drug Problems Fall Semestera | 0.48 | 1.82 | 0.59 | 1.65 | 1.17 | 2.69 | 1.38 | 2.80 | 8.59 | (3, 990) | .000 |
| Drug Problems Spring Semesterb | 0.36 | 1.68 | 0.51 | 1.92 | 1.27 | 2.94 | .95 | 2.50 | 7.00 | (3, 906) | .000 |
Note.
Average number of problems reported across the four fall semester assessments.
Average number of problems reported across the two spring semester assessments.
ANCOVAs were used to test trauma group differences on alcohol and drug-related consequences in the fall (averaged across the four fall assessments) and spring (averaged across the two spring assessments) semesters. Gender, neuroticism, and site were included so that we could test the unique effects of trauma group. As shown in Table 1, there were group differences in average number of alcohol and drug consequences in both semesters. Post-hoc comparisons using the Dunnett-Hsu adjustment for multiple comparisons with the Full PTSD group as the comparison group suggested that those with Full PTSD at matriculation reported more alcohol-related consequences in both the fall and spring semesters compared to the No Criterion A and the Criterion A only groups (ps < .05). However, no reliable differences were observed between the Full and Partial PTSD groups in either fall or spring semesters (ps > .50). Post-hoc comparisons showed a similar pattern for drug-related consequences. Those with Full PTSD at matriculation reported higher levels of drug-related consequences in the fall semester compared to the No Criterion A and the Criterion A Only groups (ps < .05). This Full PTSD Group also reported higher levels of drug-related consequences compared to the No Criterion A group (p<.05) and the Criterion A Only group (p<.07) in the spring semester, albeit the latter comparison fell short of conventional criteria for statistical significance. Differences between the Full and Partial PTSD groups on drug-related consequences were not statistically reliable in the fall or spring semester (ps >.45).
Trauma and PTSD Symptom Effects on Alcohol and Drug Consequence Trajectories
In a preliminary step, the shape of growth was tested for each construct. Growth models included intercept and slope factors. The factor loadings for the slope factors specified polynomial trends (linear, quadratic, and cubic), and the intercept was defined as the first (T1) assessment. We started with a model that specified an intercept and linear growth factor, and then added quadratic and cubic growth factors sequentially. For alcohol consequences the quadratic model was superior to the linear model (ΔΧ2(4)=40.84, p<.05). Adding a cubic growth factor resulted in non-convergence, suggesting over-fitting of the model. Accordingly, a model with a fixed cubic factor was estimated, and this model was superior to the quadratic model (ΔΧ2(1) =108.60, p<.05). The final model with random intercept, linear, and quadratic growth factors, and a fixed cubic growth factor fit the data well (Χ2(11)=41.89, p<.01, CFI=.98, TLI=.98, and RMSEA=.05). All growth factor means and variances were significantly different from zero (p<.05), and the model accounted for between 78% and 89% of the variability in the observed alcohol consequence variables. Similar results were found for drug consequences. The quadratic model was superior to the linear model (ΔΧ2(4)=23.96, p<.05). Adding a cubic growth factor resulted in non-convergence. A model with a fixed cubic growth factor was superior to the quadratic model (ΔΧ2(1)=22.31, p<.05). The final model with random intercept, linear, and quadratic growth factors, and a fixed cubic growth factor fit the data well (Χ2(11)=17.90, p>.05, CFI=.98, TLI=.97, and RMSEA=.02). All growth factor means and variances were significantly different from zero (p<.05), and the model accounted for between 71% and 90% of the observed variability in the drug consequence variables.
Trauma and PTSD effects on alcohol consequence trajectories
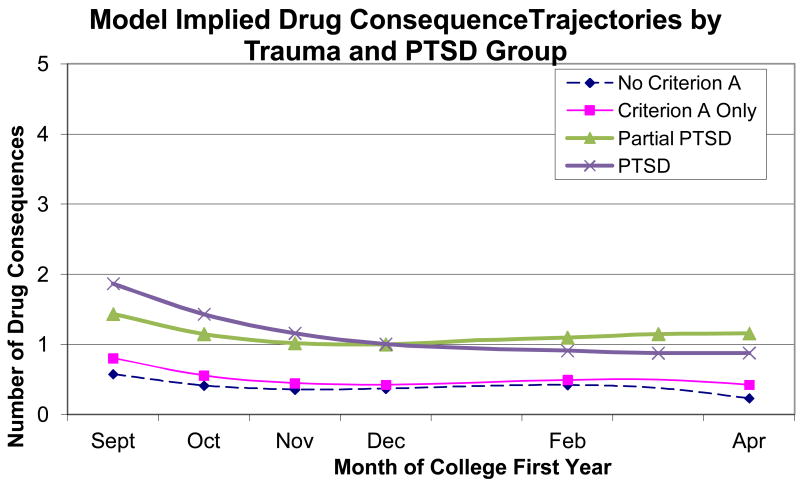
We then added the dummy coded PTSD group variables and control variables to estimate conditional growth models. Growth factors were regressed on control variables and models with and without paths from the dummy coded PTSD variables were compared to provide an omnibus test of the effect of PTSD on growth in alcohol consequences. The nested Χ2 test suggested a significant improvement in model fit when paths from the PTSD variables to the growth factors were added (ΔΧ2(9)=45.76, p<.05). The conditional model with paths from the PTSD variables fit the data well (Χ2(28)=71.25, p<.01, CFI=.98, TLI=.97, and RMSEA=.04) for alcohol consequences and the increment in R2 for the intercept, linear, and quadratic growth factors attributable to the PTSD paths was .05, .04, and .04, respectively. In addition to a significant intercept difference for site (northeastern site reporting higher levels of consequences, p < .01), we also observed significant baseline intercept effects for the trauma and PTSD contrasts. While there was no intercept difference between the Partial and Full PTSD groups, there were intercept differences between No Criterion A and Full PTSD, and between Criterion A Only and Full PTSD groups (ps < .05). The nature of these intercept effects was such that students who reported either no Criterion A or Criterion A only (i.e., trauma but no PTSD symptoms) reported fewer alcohol consequences at college matriculation (T1) than those in the Full PTSD group. Differences in both linear and quadratic trends also were observed. The linear trend was more negative for the Full PTSD compared to Criterion A Only (p<.05) group and marginally more negative compared to the No Criterion A group (p < .10), such that the Full PTSD group showed a steeper rate of decline in alcohol consequences at the beginning of the study. The quadratic trend was more positive for the Full PTSD group than for the No Criterion A group or the Criterion A Only group, suggesting a slight upward trend in alcohol consequences as the academic year ended for those with PTSD. A marginally significant difference was found between the Criterion A only and Full PTSD groups on the quadratic trend (p<.10), suggesting that the rate of decline in alcohol consequences at the beginning of the study was slower to level off for the Full PTSD group. The model implied trajectories for each group are plotted in Figure 2. The Full and Partial PTSD groups had very similar trajectories, starting college at the highest levels of consequences, and then showing a sharp decline during the fall semester. The No Criterion A and Criterion A Only groups started the college year with fewer alcohol consequences, and showed more modest declines during the fall semester.
Figure 2.
First Year College Alcohol Consequences Trajectories by Trauma and PTSD Symptom Status. Full PTSD was the contrast for these comparisons. All models controlled for negative emotionality.
Exploratory analysis of PTSD symptom cluster effects on alcohol consequence trajectories
Next, the dummy coded PTSD predictor variables were removed from the model and replaced with the PTSD symptom cluster (re-experiencing, avoidance/numbing, hyper-arousal) variables. This model conditioned on PTSD symptom clusters fit the data well (Χ2(31)=71.08, p<.01, CFI=.98, TLI=.98, and RMSEA=.04), and demonstrated that hyper-arousal, but not re-experiencing or numbing symptoms were associated with the growth factors. Hyperarousal symptoms predicted the intercept, and linear and quadratic trends (all ps <.05). As shown in Figure 3, high levels of hyperarousal symptoms were associated with high levels of negative drinking consequences in September, and a relatively rapid decline in consequences during the fall semester. However, negative drinking consequences showed a slight rise at the end of the spring semester for students with high levels of hyperarousal symptoms.
Figure 3.
First Year College Alcohol Consequences Trajectories by Level of Cluster C (Hyperarousal) Symptoms. All models controlled for negative emotionality.
Trauma and PTSD effects on other drug consequence trajectories
Comparison of conditional growth models for drug consequences with and without paths from the dummy coded PTSD group variables suggested a significant improvement in model fit when these paths were included (ΔΧ2(9)=31.46, p<.05). The conditional model with paths from the PTSD variables fit the data well (Χ2(28)=40.98, p>05, CFI=.99, TLI=.98, and RMSEA=.02), and increment in R2 for the intercept, linear, and quadratic growth factors attributable to the PTSD paths was .03, .01, and .01, respectively. As with the alcohol consequence model, significant baseline intercept effects were observed for the contrast between No Criterion A and Full PTSD, and between Criterion A Only and Full PTSD (ps < .05) groups. The nature of these intercept effects was that students with either no criterion A trauma or criterion A trauma only reported fewer drug consequences at college matriculation (T1) than those in the Full PTSD group. There was no intercept difference between the Partial and Full PTSD groups. Differences in linear growth were observed between the No Criterion A and Full PTSD groups (p<.05), such that the decline in drug consequences was steeper for the Full PTSD group at the beginning of the academic year. No differences between groups were observed for the quadratic trend. The model implied trajectories for each group are plotted in Figure 4, and suggest trends similar to those observed for alcohol consequences, albeit smaller. Again the Full and Partial PTSD groups had similar trajectories, starting at the highest levels of consequences, and showing a sharp decline in the fall semester. The No Criterion A and Criterion A Only groups started college with fewer consequences and showed more modest declines.
Figure 4.
First Year College Drug Consequences Trajectories by Trauma and PTSD Symptom Status. Full PTSD was the contrast for these comparisons. All models controlled for negative emotionality.
Exploratory analysis of PTSD symptom cluster effects on drug consequence trajectories
As we did for alcohol use consequences, the trauma group dummy coded predictor variables were removed from the model and replaced with the PTSD symptom cluster variables. Results suggested that the substance consequences growth model conditioned on PTSD symptom clusters fit the data well (Χ2 (31) =40.95, p<11, CFI=.99, TLI=.98, and RMSEA=.02). None of the symptom clusters, however, reliably predicted the growth factors (ps > .20).
Gender differences
Next, we examined potential gender differences in our models. Multiple group models were estimated and nested chi-square tests were used to test the equivalence of parameters across gender. Two sets of parameters were constrained to be equal across gender, including paths from the PTSD group variables and the means/intercepts of the latent growth factors, in separate nested tests. For both alcohol (ΔΧ2 (9) =10.78, ΔΧ2 (4) =1.75, ps>.05) and drug (ΔΧ2 (9) =4.07, ΔΧ2 (4) =10.78(9), p>.05) consequences, the nested models suggested no gender differences in causal paths from the PTSD group variables or the means/intercepts of the growth factors. Also, no gender differences were observed when paths from the PTSD symptom clusters were constrained for alcohol (ΔΧ2 (9) =9.07, p>.05) and drug (ΔΧ2 (9) =5.67, p>.05) consequences.
Trauma severity
In a final set of exploratory analyses, we considered the influence of trauma severity on substance consequence outcomes, using number of discrete trauma types derived from the TLEQ. To do this, we conducted our analyses (1) conditioning the alcohol and drug consequence trajectories on trauma severity, and then (2) including both PTSD status and trauma severity simultaneously in our models. In the first of these models, we found trauma severity to be significantly associated with both alcohol and drug intercept factors, but we observed no effects for trauma severity on either linear or quadratic slopes. Thus, our main analyses showed that PTSD predicted slopes, but our secondary analysis showed that trauma severity did not. To further explore the effects of trauma severity, we examined the conditional growth trajectories at 1 SD above the sample mean, a level equivalent to average levels of trauma severity in our PTSD group. For alcohol consequences, this trajectory suggested that high levels of trauma were associated with 6.5 consequences at the first assessment (one fewer consequence than that predicted for the PTSD group, 7.6, see Figure 2), and 4.9 consequences at the last assessment (equivalent to that predicted for the PTSD group, also 4.9, see Figure 2). For drug consequences, the model implied trajectory suggested that high levels of trauma were associated with 1.4 consequences at the first assessment (.5 fewer than that predicted for the PTSD group, see Figure 4), and .9 consequences at the last assessment (equivalent to that predicted for the PTSD group, also .9, see Figure 4). This general pattern suggests that PTSD status conferred higher risk at matriculation than did high levels of trauma severity, and this likely accounts for the observation that PTSD, but not trauma severity predicted declines in consequences.
In the second set of models, in which alcohol and drug consequence trajectories were conditioned on both the dummy coded PTSD variables and trauma severity, we observed trauma severity and PTSD group both to be significantly associated with alcohol and drug consequences intercept factors (ps < .05). Not surprisingly, with both of these highly correlated predictors in the model, there were no significant effects on either the linear or quadratic slope, suggesting that the shared variability in trauma severity and PTSD symptoms left little remaining unique variability for the prediction of these trajectories.1
Discussion
In this study, we provide what is to our knowledge the first examination of the prospective relationship between trauma and PTSD and substance involvement in young adults during their transition into college. Findings showed substantial risk for alcohol and other drug consequences that appears to be conferred by the presence of PTSD symptoms at matriculation. This association occurred above and beyond the influence of general trait negative emotionality, suggesting a unique effect of PTSD symptoms.
Our latent growth models show that risk for problem substance use is greatest for those with PTSD (and perhaps also for those with partial PTSD) at the beginning of the academic year. It can be noted from the figures that those in the Full PTSD group started college with almost twice as many consequences as those in the non-symptom groups – a clinically as well as statistically significant difference. Contrary to our expectations, this risk decreased over the course of the college year relative to those with only trauma exposure or no exposure at all. This likely is a function of the fact that those in these PTSD symptom groups began at higher consequence levels and thus had more room for diminution of consequences. Still, despite the declines that we observed, our ANCOVA analyses showed that differences between those with significant PTSD symptoms and those without persisted across the academic year.
The first months of college are a time of particular risk for students regarding alcohol and other drug involvement (Schulenberg & Maggs, 2002; Sher & Rutledge, 2007; White, Labouvie, & Papadaratsakis, 2005). Though our data and others show that at least some of these consequences resolve naturalistically with time, these early consequences still can have significant acute and long-term implications for the individuals experiencing them. Findings here suggest that trauma exposure and PTSD in particular heighten risk for contribute to alcohol and other drug consequences during this period of vulnerability. Moreover, though our models suggest that consequences diminish at a faster rate during the fall semester for those with PTSD symptoms than for those without PTSD, they continue to remain significantly higher over the academic year. This points to a unique effect of PTSD over the most important year of transition into college.
In our models, Full PTSD was the contrast variable with which other trauma and PTSD groups were compared. Interestingly, though there were consistent differences in consequences between the non-trauma exposed and the Criterion A trauma only groups and the Full PTSD group in drug and alcohol consequence trajectories, there were no differences between Partial and Full PTSD groups. This suggests that the impact of sub-threshold PTSD symptoms on substance consequence outcomes is not substantially different from the impact of full PTSD. These findings offer further support for the clinical significance of PTSD syndromes that fall below a categorical threshold but that nonetheless impact functioning (Schutzwohl & Maercker, 1999; Mendlowicz & Stein, 2000; Stein, Walker, Hazen, & Forde, 1997; Zlotnick et al., 2002).
Findings from this study also shed light on another question that has been raised in the PTSD-substance comorbidity literature -that is, whether problem substance use emerges in response to exposure to a trauma event itself or as a result of continued psychological symptoms that follow the event (Epstein et al., 1998; Read et al., 2004, Stewart, 1996; Stewart & Conrod, 2003). We observed the strongest effects for PTSD symptoms – both partial and full PTSD – rather than criterion A trauma exposure alone. Though to a lesser extent, it also appeared that trauma severity (rather than just exposure) also influenced substance consequence outcomes. These findings corroborate what is to our knowledge the only other study to test the distinct effects of trauma versus PTSD prospectively in a young adult sample (Reed et al., 2007). These investigators found that posttraumatic stress symptoms, and not simply trauma exposure, were associated with risk for substance misuse one year later.
We found the Hyper-arousal cluster to show unique prediction of alcohol consequence trajectories, but no evidence of symptom cluster effects for drug trajectories. Though as noted, the research literature has yielded disparate outcomes, findings from the present study are consistent with some previous work (McFall, Mackey, & Donovan, 1992; Stewart et al., 1998; Shipherd et al., 2005; Taft et al., 2007) showing hyper-arousal symptoms to be significantly associated with alcohol consequences in particular. Perhaps the perceptual, physical, affective, and cognitive symptoms that comprise the hyper-arousal cluster may, when combined with the disinhibiting effects of alcohol, render students particularly vulnerable to externalizing and other problem behaviors (e.g., physical fights, sexual aggression, other risk behaviors).
Limitations and Future Directions
This study had a number of strengths, including a large sample drawn from two universities in different regions of the U.S., a high retention rate, prospective design, and frequent assessments over the first college year. Still there were some limitations and also several directions for future investigation. These are discussed below.
In the present study, we sought to understand the prospective effects of trauma and PTSD at college matriculation on alcohol and other drug involvement over the first year of college. We found support for the “Self-Medication” hypothesis, which suggests that individuals may use substances to ameliorate PTSD symptoms (Jacobsen et al., 2001; Khantzian, 2003; Saladin et al., 1995). The specific way in which college students may self-medicate is worth noting. Alcohol and drug use in college tends to occur in a fairly consistent pattern that is best represented by weekend use (Colder et al., 2006; Tremblay et al., 2010). Given these typical patterns in college samples, what is most likely is that to the extent that these students are self-medicating, this is occurring within the context of a strongly routinized substance use pattern. As such, rather than turning to alcohol or drugs every time a PTSD symptom is experienced, students with PTSD instead may be more likely to mismanage their consumption or themselves when drinking and drug use occasions occur. This is consistent with models of psychological functioning that conceptualize stress responses as a function of depletion of cognitive and other coping resources, which may then result in problem behavior in specific circumstances or environments (Bauer & Baumeister, 2011; Muraven & Baumeister, 2000).
Our findings in support of a self-medication process do not exclude other possible directions of association. For example, those who use substances heavily may be at greater risk for accidents, violence, or other types of trauma which may then result in greater post-traumatic stress symptoms (Chilcoat & Breslau,1998). Heavy substance use also may exacerbate PTSD symptoms (Saladin et al., 1995). Such “high risk” pathways were not tested here. We also did not examine the influence of additional traumas or worsening PTSD symptoms over the course of the year. The possibilities for future investigations of association are numerous, and point to exciting opportunities for further examination.
In this study, we sought to examine trauma, PTSD, and substance consequences at the time of college matriculation. Conducting over 1000 clinical interviews with newly incoming students in their first month of college was not feasible. Thus, we employed an online assessment. Our measures were chosen for their strong psychometric properties (Ruggiero et al., 2003; Pierce, Burke, Stoller, Neufeld, & Brooner, 2009), and prior work supports concurrent validity of the web-based trauma and PTSD measures used here with structured interviews (Read et al., 2009). Still, diagnostic interview remains the gold-standard assessment of clinical syndromes. Replication of these associations with interview data will build on the present findings.
Further, though the PCL has been used in many college samples (e.g., Adkins, Weathers, McDevitt-Murphy, & Daniels, 2008; Hoyt & Yeater, 2010; Read et al., 2011) and has been shown to correlate strongly with interview assessment of PTSD in college students (Adkins et al., 2008; Read et al., 2009; Ruggiero et al., 2003), the cut scores themselves have not been widely used in college samples. As such, it is possible that the scoring cutoffs recommended by Blanchard et al. (1996) may actually under-estimate PTSD in a sample where the base rates of PTSD are lower.
We did not find gender to moderate the effects of trauma and PTSD on substance consequence trajectories. Other factors may affect these processes and should be tested in future research. For example, socio-environmental influences such as peer group affiliation (heavy drinking peers, Greek involvement) and perceptions about normative substance use behavior exert a strong influence on the adoption and maintenance of substance behaviors in college (Borsari & Carey, 2001; Neighbors, Geisner, & Lee, 2008; Neighbors, Lee, Lewis, Fossos, & Larimer, 2007), and social support has been shown to be relevant to post-trauma adaptation (Charuvastra & Cloitre, 2008; Keane, Marshall, & Taft, 2006). As such, socio-environmental factors may be important moderators to test in future research. Other factors that could be relevant to PTSD-substance misuse include but are not limited to variables such as coping, re-victimization status, or alcohol and drug expectancies.
Future research also will add to the present work by examining a range of psychological distress beyond just posttraumatic distress. Though in our models we controlled for negative emotionality, we cannot from our data know how specific expressions of mood or anxiety (e.g., depression, generalized anxiety, phobias) may affect problem substance use, or how these may interact with PTSD to influence substance trajectories.
This study captures associations among trauma, PTSD, and substance use during a salient passage of young adulthood- the transition into college. Studies of these relations during other periods of vulnerability are needed. Schulenberg and Maggs (2002) note that substance use rates tend to increase during periods of transition. Though the transition into college has been identified as one distinct period of risk for escalation in substance use (see Del Boca et al., 2004), scant attention has been paid to substance use at other potentially important periods of change. Accordingly, an interesting direction for future research will be to examine whether the risk associated with PTSD symptoms persists beyond the first year of college, and perhaps most importantly, whether an effect is again observed during another important developmental transition – the transition out of college and into mature adulthood.
The present study has intervention implications. Risk for problem alcohol and other drug involvement was associated with baseline trauma and PTSD status. This risk was greatest at the point of matriculation, an identified period of vulnerability (Schulenberg & Maggs, 2002; Sher & Rutledge, 2007). Further, despite sharp declines over the first semester, greater alcohol and other drug consequences were observed for those with PTSD symptoms over the academic year. Accordingly, early identification of significant PTSD symptoms may deter problem substance use during the critical developmental transition into college, and could offset risk that persists over the first college year. This could include something as simple as screening and outreach for individuals who present to university counseling centers with PTSD symptoms, or as elaborate as developing integrated treatments for PTSD-substance abuse for college students. Several PTSD-Substance abuse interventions have been developed (Back, Dansky, Carroll, Foa, & Brady, 2001; Donovan, Padin, & Kowaliw, 2001; Najavits, 2002; Triffleman, Carroll, & Kellogg, 1999). Yet, none of these has been tested in a college population (Borsari, Read, & Campbell, 2008).
According to Curran, “There is a great need to link theoretical and statistical models in applied research… this is especially evident in developmental studies of substance use” (2000, pp.3). Here we present such a link. Our findings suggest that students experiencing PTSD symptoms as they matriculate into college are at greater risk for alcohol and other drug consequences during this time. Interventions offering support and resources to these students may ameliorate this risk, and may ultimately facilitate a better transition into college and beyond.
Acknowledgments
This work was supported by a grant from the National Institute on Drug Abuse (R01DA018993) to Dr. Jennifer P. Read.
We would like to thank Rachel Bachrach, Melissa Griffin, Leah Vermont, and Jeffrey Wardell for their helpful comments on earlier drafts of this manuscript. We also thank Dr. Sherry Farrow, Justin Swift, and the members of the UB Alcohol Research Lab for their many efforts to support data collection for this study. Finally, we thank the participants for sharing their experiences.
Footnotes
We also ran our conditional growth models with PTSD operationalized as a continuous variable (a sum of PTSD symptoms). Results for the alcohol consequence model suggested that high levels of PTSD symptoms were positively associated with the intercept (p<.05), negatively associated with the linear trend (p<.05), and marginally positively associated with the quadratic trend (p<.10). The nature of these effects mirrors what we found in our main analysis. That is, more severe forms of PTSD (e.g., Full PTSD or a high number of symptoms) are associated with high levels of negative alcohol consequences at the beginning of the study that decline steeply during the course of the first semester. Results for the drug consequence model were also consistent with our main analysis, such that high levels of PTSD symptoms were associated with high initial levels of drug consequences (p<.05), and PTSD symptoms were not associated with the slope factors. When trauma severity was added to these conditional models, the effects of the continuous the PTSD symptom variable on the slope factors was not statistically reliable for both alcohol and drug consequences. This again mirrors our main analysis suggesting that considering both trauma severity and PTSD symptoms simultaneously leaves little unique variance in the prediction of trajectories.
References
- Adkins JW, Weathers FW, McDevitt-Murphy M, Daniels JB. Psychometric properties of seven self-report measures of posttraumatic stress disorder in college students with mixed civilian trauma exposure. Journal of Anxiety Disorders. 2008;22:1393–1402. doi: 10.1016/j.janxdis.2008.02.002. [DOI] [PubMed] [Google Scholar]
- Andrykowski M, Cordova M, Studts J, Miller T. Posttraurnatic Stress Disorder after treatment for breast cancer: Prevalence of diagnosis and use of the PTSD Checklist—civilian version (PCL-C) as a screening instrument. Journal of Consulting and Clinical Psychology. 1998;66:586–590. doi: 10.1037//0022-006x.66.3.586. [DOI] [PubMed] [Google Scholar]
- Arnett JJ. Emerging adulthood: A theory of development from the late teens through the twenties. American Psychologist. 2000;55:469–480. [PubMed] [Google Scholar]
- Arnett JJ. The developmental context of substance use in emerging adulthood. Journal of Drug Issues. 2005;42:235–253. [Google Scholar]
- Arria A, Caldeira K, O'Grady K, Vincent K, Fitzelle D, Johnson E, Wish E. Drug exposure opportunities and use patterns among college students: Results of a longitudinal prospective cohort study. Substance Abuse. 2008;29:19–38. doi: 10.1080/08897070802418451. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Arria A, Vincent KB, Caldeira KM. Measuring liability for substance use disorder among college students: Implications for screening and early intervention. The American Journal of Drug and Alcohol Abuse. 2009;35:233–241. doi: 10.1080/00952990903005957. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Back SE, Dansky BS, Carroll KM, Foa EB, Brady KT. Exposure therapy in the treatment of PTSD among cocaine-dependent individuals: Description of procedures. Journal of Substance Abuse Treatment. 2001;21:33–45. doi: 10.1016/s0740-5472(01)00181-7. [DOI] [PubMed] [Google Scholar]
- Bauer I, Baumeister RF. Self-regulatory strength. In: Vohs Kathleen D, Baumeister Roy F., editors. Handbook of self-regulation: Research, theory, and applications. 2nd. New York, NY, US: Guilford Press; 2011. pp. 64–82. [Google Scholar]
- Bernat JA, Ronfeldt HM, Calhoun KS, Arias I. Prevalence of traumatic events and peritraumatic predictors of posttraumatic stress symptoms in a nonclinical sample of college students. Journal of Traumatic Stress. 1998;11:645–664. doi: 10.1023/A:1024485130934. [DOI] [PubMed] [Google Scholar]
- Blanchard EB, Jones-Alexander J, Buckley TC, Forneris CA. Psychometric properties of the PTSD Checklist (PCL) Behavior Research and Therapy. 1996;34:669–673. doi: 10.1016/0005-7967(96)00033-2. [DOI] [PubMed] [Google Scholar]
- Blanco C, Okuda M, Wright C, Hasin DS, Grant BF, Shang-Min L, Olfson M. Mental health of college students and their non-college attending peers: Results from the national Epidemiologic Study on Alcohol and Related Conditions. Archives of General Psychiatry. 2008;65:1429–1437. doi: 10.1001/archpsyc.65.12.1429. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bornovalova MA, Ouimette P, Crawford AV, Levy R. Testing gender effects on the mechanisms explaining the association between posttraumatic stress symptoms and substance use frequency. Addictive Behaviors. 2009;34:685–692. doi: 10.1016/j.addbeh.2009.04.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Borsari B, Carey KB. Peer influences on college drinking: A review of the research. Journal of Substance Abuse. 2001;13/14:391–424. doi: 10.1016/s0899-3289(01)00098-0. [DOI] [PubMed] [Google Scholar]
- Borsari B, Read JP, Campbell J. Posttraumatic stress disorder and substance use disorders in college students: Implications for Counseling Centers. Journal of College Student Psychotherapy. 2008;22:61–85. doi: 10.1080/87568220801960720. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Breslau N. The epidemiology of posttraumatic stress disorder: What is the extent of the problem? Journal of Clinical Psychiatry. 2001;62:16–22. [PubMed] [Google Scholar]
- Breslau N, Davis GC. Posttraumatic stress disorder in an urban population of young adults: Risk factors for chronicity. American Journal of Psychiatry. 1992;149:671–675. doi: 10.1176/ajp.149.5.671. [DOI] [PubMed] [Google Scholar]
- Breslau N, Davis GC, Andreski P, Peterson EL, Schultz LR. Sex differences in posttraumatic stress disorder. Archives of General Psychiatry. 1997;54:1044–1048. doi: 10.1001/archpsyc.1997.01830230082012. [DOI] [PubMed] [Google Scholar]
- Broman-Fulks JJ, Ruggiero KJ, Green BA, Kilpatrick DG, Danielson C, Resnick HS, Saunders BE. Taxometric Investigation of PTSD: Data From Two Nationally Representative Samples. Behavior Therapy. 2006;37:364–380. doi: 10.1016/j.beth.2006.02.006. [DOI] [PubMed] [Google Scholar]
- Caldeira KM, Arria AM, O'Grady KE, Vincent KB, Wish ED. The occurrence of cannabis use disorders and other cannabis-related problems among first-year college students. Addictive Behaviors. 2008;33:397–411. doi: 10.1016/j.addbeh.2007.10.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Charuvastra A, Cloitre M. Social bonds and posttraumatic stress disorder. Annual Review of Psychology. 2008;59:301–328. doi: 10.1146/annurev.psych.58.110405.085650. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Chilcoat HD, Breslau N. Investigations of causal pathways between PTSD and drug use disorders. Addictive Behaviors. 1998;23:827–840. doi: 10.1016/s0306-4603(98)00069-0. [DOI] [PubMed] [Google Scholar]
- Cohen J. Statistical power analyses for the behavioral sciences. 2nd. Hillsdale, NJ: Lawrence Erlbaum Associates; 1988. [Google Scholar]
- Colder CR, Lloyd-Richardson EE, Flaherty BP, Hedeker D, Segawa E, Flay BR, The Tobacco Etiology Research Network The natural history of college smoking: Trajectories of daily smoking during the freshman year. Addictive Behaviors. 2006;31:2212–2222. doi: 10.1016/j.addbeh.2006.02.011. [DOI] [PubMed] [Google Scholar]
- Cook J, Jakupcak M, Rosenheck R, Fontana A, McFall M. Influence of PTSD symptom clusters on smoking status among help-seeking Iraq and Afghanistan veterans. Nicotine & Tobacco Research. 2009;11:1189–1195. doi: 10.1093/ntr/ntp123. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Curran PJ. A latent curve framework for the study of developmental trajectories in adolescent substance use. In: Rose JS, Chassin L, Presson CC, Sherman SJ, editors. Multivariate applications in substance use research. New Jersey: Erlbaum; 2000. pp. 1–33. [Google Scholar]
- Curran PJ, Muthen BO. The application of latent curve analysis to testing developmental theories in intervention research. American Journal of Community Psychology. 1999;27:567–590. doi: 10.1023/A:1022137429115. [DOI] [PubMed] [Google Scholar]
- Dawson DA, Grant BF, Stinson FS, Chou PS. Another look at heavy episodic drinking and alcohol use disorders among college and non-college youth. Journal of Studies on Alcohol. 2004;65:477–488. doi: 10.15288/jsa.2004.65.477. [DOI] [PubMed] [Google Scholar]
- Del Boca FK, Darkes J, Greenbaum PE, Goldman MS. Up close and personal: Temporal variability in the drinking of individual college students during their first year. Journal of Consulting and Clinical Psychology. 2004;72:155–164. doi: 10.1037/0022-006X.72.2.155. [DOI] [PubMed] [Google Scholar]
- Donovan B, Padin-Rivera E, Kowaliw S. “Transcend”: Initial outcomes from a posttraumatic stress disorder/substance abuse treatment program. Journal of Traumatic Stress. 2001;14:757–772. doi: 10.1023/A:1013094206154. [DOI] [PubMed] [Google Scholar]
- Epstein J, Saunders BE, Kilpatrick DG, Resnick HS. PTSD as a mediator between childhood rape and alcohol use in adult women. Child Abuse and Neglect. 1998;22:223–234. doi: 10.1016/s0145-2134(97)00133-6. [DOI] [PubMed] [Google Scholar]
- Flynn HA. Comparison of cross-sectional and daily reports in studying the relationship between depression and use of alcohol in response to stress in college students. Alcoholism: Clinical and Experimental Research. 2000;24:48–52. [PubMed] [Google Scholar]
- Goldstein AL, Flett GL, Wekerle C. Child maltreatment, alcohol use and drinking consequences among male and female college students: An examination of drinking motives as mediators. Addictive Behaviors. 2010;35:636–639. doi: 10.1016/j.addbeh.2010.02.002. [DOI] [PubMed] [Google Scholar]
- Hoyt T, Yeater EA. Comparison of posttraumatic stress disorder symptom structure models in Hispanic and White college students. Psychological Trauma: Theory, Research, Practice, and Policy. 2010;2:19–30. [Google Scholar]
- Hu L, Bentler PM. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Structural Equation Modeling. 1999;6:1–55. [Google Scholar]
- Jacobsen LK, Southwick SM, Kosten TR. Substance use disorders in patients with posttraumatic stress disorder: A review of the literature. American Journal of Psychiatry. 2001;158:1184–1190. doi: 10.1176/appi.ajp.158.8.1184. [DOI] [PubMed] [Google Scholar]
- Jakupcak M, Tull MT, McDermott M, Kaysen D, Hunt S, Simpson T. PTSD symptom clusters in relationship to alcohol misuse among Iraq and Afghanistan war veterans seeking post-deployment VA health care. Addictive Behaviors. 2010;35:840–843. doi: 10.1016/j.addbeh.2010.03.023. [DOI] [PubMed] [Google Scholar]
- John OP, Srivastava S. The Big Five trait taxonomy: History, measurement, and theoretical perspectives. In: Pervin LA, John OP, editors. Handbook of personality. 2nd. Guilford; New York: 1999. pp. 102–138. [Google Scholar]
- Kassel JD, Jackson SI, Unrod M. Generalized expectancies for negative mood regulation and problem drinking among college students. Journal of Studies on Alcohol. 2000;61:332–340. doi: 10.15288/jsa.2000.61.332. [DOI] [PubMed] [Google Scholar]
- Keane TM, Marshall AD, Taft CT. Posttraumatic stress disorder: Etiology, Epidemiology, and Treatment Outcome. Annual Review of Clinical Psychology. 2006;2:161–197. doi: 10.1146/annurev.clinpsy.2.022305.095305. [DOI] [PubMed] [Google Scholar]
- Kessler RC, Sonnega A, Bromet E, Hughes M, Nelson CB. Posttraumatic stress disorder in the National Comorbidity Survey. Archives of General Psychiatry. 1995;52:1048–1060. doi: 10.1001/archpsyc.1995.03950240066012. [DOI] [PubMed] [Google Scholar]
- Khantzian EJ. The self-medication hypothesis revisited: The dually diagnosed patient. Primary Psychiatry. 2003;10:47–48. [Google Scholar]
- Klanecky AK, Harrington J, McChargue DE. Child sexual abuse, dissociation, and alcohol: Implications of chemical dissociation via blackouts among college women. The American Journal of Drug and Alcohol Abuse. 2008;34:277–284. doi: 10.1080/00952990802013441. [DOI] [PubMed] [Google Scholar]
- Klingemann H, Sobell MA, Sobell LC. Continuities and changes in self-change research. Addiction. 2010;105:1510–8. doi: 10.1111/j.1360-0443.2009.02770.x. [DOI] [PubMed] [Google Scholar]
- Kubany ES, Haynes SY, Leisen MB, Owens JA, Kaplan AS, Watson SB, Burns K. Development and preliminary validation of a brief broad-spectrum measure of trauma exposure: The Traumatic Life Events Questionnaire. Psychological Assessment. 2000;12:210–224. doi: 10.1037//1040-3590.12.2.210. [DOI] [PubMed] [Google Scholar]
- Lang A, Laffaye C, Satz L, Dresselhaus T, Stein M. Sensitivity and specificity of the PTSD Checklist in detecting PTSD in female veterans in primary care. Journal of Traumatic Stress. 2003;16:257–264. doi: 10.1023/A:1023796007788. [DOI] [PubMed] [Google Scholar]
- Larimer ME, Turner AP, Mallet KA, Geisner IM. Predicting drinking behavior and alcohol-related problems among fraternity and sorority members: Examining the role of descriptive and injunctive norms. Psychology of Addictive Behaviors. 2004;18:203–212. doi: 10.1037/0893-164X.18.3.203. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lauterbach D, Vrana S. The relationship among personality variables, exposure to traumatic events, and severity of posttraumatic stress symptoms. Journal of Traumatic Stress. 2001;14:29–43. [Google Scholar]
- Lewis MA, Neighbors C, Oster-Aaland L, Kirkeby BS, Larimer ME. Indicated prevention for incoming freshmen: Personalized normative feedback and high-risk drinking. Addictive Behaviors. 2007;32:2495–2508. doi: 10.1016/j.addbeh.2007.06.019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lepore SJ. Social-environmental influences on the chronic stress process. In: Gottleib BH, editor. Coping with chronic stress. New York: Plenum Press; 1997. pp. 133–160. [Google Scholar]
- Lex BW. Some gender differences in alcohol and polysubstance users. Health Psychology. 1991;10:121–132. doi: 10.1037//0278-6133.10.2.121. [DOI] [PubMed] [Google Scholar]
- Martens MP, Neighbors C, Lewis MA, Lee CM, Oster-Aaland L, Larimer ME. The roles of negative affect and coping motives in the relationship between alcohol use and alcohol-related problems among college students. Journal of Studies on Alcohol and Drugs. 2008;69:412–419. doi: 10.15288/jsad.2008.69.412. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Marx BP, Sloan DM. The role of emotion in the psychological functioning of adult survivors of childhood sexual abuse. Behavior Therapy. 2003;33:563–577. [Google Scholar]
- McCabe SE, West BT, Wechsler H. Trends and college-level characteristics associated with the non-medical use of prescription drugs among U.S. college students from 1993-2001. Addiction. 2007;102:455–465. doi: 10.1111/j.1360-0443.2006.01733.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McCauley J, Ruggiero KJ, Resnick HS, Conoscenti LM, Kilpatrick DG. Forcible, drug–facilitated, and incapacitated rape in relation to substance use problems: Results from a national sample of college women. Addictive Behaviors. 2009;34:458–462. doi: 10.1016/j.addbeh.2008.12.004. [DOI] [PubMed] [Google Scholar]
- McDevitt-Murphy ME, Murphy JG, Monahan CM, Flood AM, Weathers FW. Unique Patterns of Substance Misuse associated with PTSD, Depression, and Social Phobia. Journal of Dual Diagnosis. 2010;6:94–110. doi: 10.1080/15504261003701445. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McFall ME, Mackay PW, Donovan DM. Combat-related posttraumatic stress disorder and severity of substance abuse in Vietnam veterans. Journal of Studies on Alcohol. 1992;53:357–362. doi: 10.15288/jsa.1992.53.357. [DOI] [PubMed] [Google Scholar]
- McFarlane AC, Browne D, Bryant RA, O'Donnell M, Silove D, Creamer M, Horsley K. A longitudinal analysis of alcohol consumption and the risk of posttraumatic symptoms. Journal of Affective Disorders. 2009;118:166–172. doi: 10.1016/j.jad.2009.01.017. [DOI] [PubMed] [Google Scholar]
- Mendlowicz MV, Stein MB. Quality of life in individuals with anxiety disorders. American Journal of Psychiatry. 2000;157:669–682. doi: 10.1176/appi.ajp.157.5.669. [DOI] [PubMed] [Google Scholar]
- Miller ET, Neal DJ, Roberts LJ, Baer JS, Cressler JM, Marlatt GA. Test-retest reliability of alcohol measures: Is there a difference between internet-based assessment and traditional methods? Psychology of Addictive Behaviors. 2002;16:56–63. [PubMed] [Google Scholar]
- Muraven M, Baumeister RF. Self-regulation and depletion of limited resources: Does self-control resemble a muscle? Psychological Bulletin. 2000;126:247–259. doi: 10.1037/0033-2909.126.2.247. [DOI] [PubMed] [Google Scholar]
- Muthén L, Muthén B. Mplus: The comprehensive modeling program for applied researchers, version 6.1. Los Angeles, CA: 2010. [Google Scholar]
- Mylle J, Maes M. Partial posttraumatic stress disorder revisited. Journal of Affective Disorders. 2004;78:37–48. doi: 10.1016/s0165-0327(02)00218-5. [DOI] [PubMed] [Google Scholar]
- Najavits LM. Seeking Safety: A treatment manual for PTSD and substance abuse. New York: Guilford; 2002. [DOI] [PubMed] [Google Scholar]
- Najavits LM. Treatment and posttraumatic stress disorder and substance abuse: Clinical guidelines for implementing Seeking Safety therapy. Alcoholism Treatment Quarterly. 2004;22:43–62. [Google Scholar]
- Neighbors CL, Lee CM, Lewis MA, Fossos N, Larimer ME. Are social norms the best predictor of outcomes among heavy drinking college students? Journal of Studies on Alcohol and Drugs. 2007;68:556–565. doi: 10.15288/jsad.2007.68.556. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Neighbors CL, Geisner IM, Lee CM. Perceived marijuana norms and social expectancies among entering college student marijuana users. Psychology of Addictive Behaviors. 2008;22:433–438. doi: 10.1037/0893-164X.22.3.433. [DOI] [PubMed] [Google Scholar]
- O'Hare T, Sherrer MV. Co-occurring stress and substance abuse in college first offenders. Journal of Human Behavior in the Social Environment. 2000;3:29–44. [Google Scholar]
- O'Malley PM, Johnston LD. Epidemiology of alcohol and other drug use among American college students. Journal of Studies on Alcohol. 2002;(14):23–39. doi: 10.15288/jsas.2002.s14.23. [DOI] [PubMed] [Google Scholar]
- O'Neil SE, Parra GR, Sher KJ. Clinical relevance of heavy drinking during the college years: Cross-sectional and longitudinal perspectives. Psychology of Addictive Behaviors. 2001;13:350–359. doi: 10.1037//0893-164x.15.4.350. [DOI] [PubMed] [Google Scholar]
- Ouimette P, Coolhart D, Funderburk J, Brown PJ. Precipitants of first substance use in recently abstinent substance use disordered patients with PTSD. Addictive Behaviors. 2007;32:1719–1727. doi: 10.1016/j.addbeh.2006.11.020. [DOI] [PubMed] [Google Scholar]
- Peirce JM, Burke CK, Stoller KB, Neufeld KJ, Brooner RK. Assessing traumatic event exposure: Comparing the Traumatic Life Events Questionnaire to the Structured Clinical Interview for DSM-IV. Psychological Assessment. 2009;21:210–218. doi: 10.1037/a0015578. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Perkonigg A, Kessler RC, Storz S, Wittchen HU. Traumatic events and post-traumatic stress disorder in the community: Prevalence, risk factors and comorbidity. Acta Psychiatrica Scandinavica. 2000;101:46–59. doi: 10.1034/j.1600-0447.2000.101001046.x. [DOI] [PubMed] [Google Scholar]
- Read JP, Brown PJ, Kahler CW. Substance use and posttraumatic stress disorder: Symptom interplay and effects on outcome. Addictive Behaviors. 2004;29:1665–1672. doi: 10.1016/j.addbeh.2004.02.061. [DOI] [PubMed] [Google Scholar]
- Read JP, Farrow SM, Jaanimagi U, Ouimette PC. Assessing trauma and traumatic stress via the internet: Measurement equivalence and participant reactions. Traumatology. 2009;15:94–102. [Google Scholar]
- Read JP, Kahler CW, Strong D, Colder CR. Development and preliminary validation of the Young Adult Alcohol Consequences Questionnaire. Journal of Studies on Alcohol. 2006;67:169–178. doi: 10.15288/jsa.2006.67.169. [DOI] [PubMed] [Google Scholar]
- Read JP, Merrill JE, Kahler CW, Strong DS. Predicting functional outcomes among college drinkers: Reliability and predictive validity of the Young Adult Alcohol Consequences Questionnaire. Addictive Behaviors. 2008;32:2597–2610. doi: 10.1016/j.addbeh.2007.06.021. [DOI] [PubMed] [Google Scholar]
- Read JP, Ouimette P, White J, Colder C, Farrow S. Rates of DSM IV-TR trauma exposure and posttraumatic stress disorder among newly matriculated college students. Trauma: Theory, Research, and Practice. 2011;3:148–156. doi: 10.1037/a0021260. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Reed PL, Anthony JC, Breslau N. Incidence of drug problems in young adults exposed to trauma and posttraumatic stress disorder: do early life experiences and predispositions matter? Archives of General Psychiatry. 2007;64:1435–42. doi: 10.1001/archpsyc.64.12.1435. [DOI] [PubMed] [Google Scholar]
- Rimsza ME, Moses KS. Substance abuse on the college campus. Pediatric Clinics of North America. 2005;52:307–319. doi: 10.1016/j.pcl.2004.10.008. [DOI] [PubMed] [Google Scholar]
- Ruggiero KJ, Del Ben K, Scotti JR, Rabalais AE. Psychometric properties of the PTSD Checklist- Civilian Version. Journal of Traumatic Stress. 2003;16:495–502. doi: 10.1023/A:1025714729117. [DOI] [PubMed] [Google Scholar]
- Ruscio AM, Ruscio J, Keane TM. The Latent Structure of Posttraumatic Stress Disorder: A Taxometric Investigation of Reactions to Extreme Stress. Journal of Abnormal Psychology. 2002;111:290–301. [PubMed] [Google Scholar]
- Saladin ME, Brady KT, Dansky BS, Kilpatrick DG. Understanding comorbidity between PTSD and substance use disorders: Two preliminary investigations. Addictive Behaviors. 1995;20:643–655. doi: 10.1016/0306-4603(95)00024-7. [DOI] [PubMed] [Google Scholar]
- Scarpa A, Fikretoglu D, Bowser F, Hurley JD, Pappert CA, Romero N, Van Voorhees E. Community violence exposure in university students: A replication and extension. Journal of Interpersonal Violence. 2002;17:253–272. [Google Scholar]
- Schnurr PP, Ford JD, Friedman MJ, Green BL, Dain BJ, Sengupta A. Predictors and outcomes of posttraumatic stress disorder in World War II veterans exposed to mustard gas. Journal of Consulting and Clinical Psychology. 2000;68:258–268. [PubMed] [Google Scholar]
- Schnurr PP, Friedman MJ, Vernardy NC. Research on posttraumatic stress disorder: Epidemiology, pathophysiology, and assessment. Psychotherapy in Practice. 2002;58:877–889. doi: 10.1002/jclp.10064. [DOI] [PubMed] [Google Scholar]
- Schulenberg JE, Maggs JL. A developmental perspective on alcohol use and heavy drinking during adolescence and the transition to young adulthood. Journal of Studies on Alcohol. 2002;114:54–70. doi: 10.15288/jsas.2002.s14.54. [DOI] [PubMed] [Google Scholar]
- Schutzwohl M, Maercker A. Effects of varying diagnostic criteria for posttraumatic stress disorder are endorsing the concept of partial PTSD. Journal of Traumatic-Stress. 1999;12:155–165. doi: 10.1023/A:1024706702133. [DOI] [PubMed] [Google Scholar]
- Sher KJ, Rutledge PC. Heavy drinking across the transition to college: Predicting first-semester heavy drinking from pre-college variables. Addictive Behaviors. 2007;32:819–835. doi: 10.1016/j.addbeh.2006.06.024. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Shipherd J, Stafford JC, Tanner LR. Predicting alcohol and drug abuse in Persian Gulf War Veterans: What role do PTSD symptoms play? Addictive Behaviors. 2005;30:595–599. doi: 10.1016/j.addbeh.2004.07.004. [DOI] [PubMed] [Google Scholar]
- Simons JS, Gaher RM, Oliver M, Bush JA, Palmer MA. An Experience Sampling Study of Associations between Affect and Alcohol Use and Problems among College Students. Journal of Studies on Alcohol. 2005;66:459–469. doi: 10.15288/jsa.2005.66.459. [DOI] [PubMed] [Google Scholar]
- Smyth JM, Hockemeyer JR, Heron KE, Wonderlich SA, Pennebaker JW. Prevalence, type, disclosure, and severity of adverse life events in college students. Journal of American College Health. 2008;57:69–76. doi: 10.3200/JACH.57.1.69-76. [DOI] [PubMed] [Google Scholar]
- Spear L. Alcohol's effects on adolescents. Women and Alcohol: An Update. 2002;24:287–291. [PMC free article] [PubMed] [Google Scholar]
- Stein MB, Walker JR, Hazen AL, Forde DR. Full and partial posttraumatic stress disorder: Findings from a community survey. American Journal of Psychiatry. 1997;154:1114–1119. doi: 10.1176/ajp.154.8.1114. [DOI] [PubMed] [Google Scholar]
- Stewart SH. Alcohol abuse in individuals exposed to trauma: A critical review. Psychological Bulletin. 1996;120:83–112. doi: 10.1037/0033-2909.120.1.83. [DOI] [PubMed] [Google Scholar]
- Stewart SH, Conrod PJ. Psychosocial models of functional associations between posttraumatic stress disorder and substance use disorder. In: Ouimette PC, Brown PJ, editors. Trauma and substance abuse: Causes, consequences, and treatment of comorbid disorders. Washington, DC: APA; 2003. pp. 29–56. [Google Scholar]
- Stewart SH, Conrod PJ, Pihl RO, Dongier M. Relations between posttraumatic stress symptoms dimensions and substance dependence in a community-recruited sample of substance abusing women. Psychology of Addictive Behaviors. 1999;13:78–88. [Google Scholar]
- Stewart SH, Pihl RO, Conrod PJ, Dongier M. Functional associations among trauma, PTSD, and substance-related disorders. Addictive Behaviors. 1998;23:797–812. doi: 10.1016/s0306-4603(98)00070-7. [DOI] [PubMed] [Google Scholar]
- Substance Abuse and Mental Health Services Administration. Results from the 2005 National Survey on Drug Use and Health: National findings (Office of Applied Studies, NSDUH Series H-30, DHHS Publication No. SMA 06-4194) 2006 Retrieved July 23, 2010, from http://www.oas.samhsa.gov/NSDUH/2k5nsduh/tabs/2k5Tabs.pdf.
- Taft CT, Kaloupek DG, Schumm JA, Marshall AD, Panuzio J, King DW, Keane TM. Posttraumatic stress disorder symptoms, physiological reactivity, alcohol problems, and aggression among military veterans. Journal of Abnormal Psychology. 2007;116:498–507. doi: 10.1037/0021-843X.116.3.498. [DOI] [PubMed] [Google Scholar]
- Thompson M, Spitler H, McCoy T, Marra L, Sutfin E, Rhodes S, et al. The moderating role of gender in the prospective associations between expectancies and alcohol–related negative consequences among college students. Substance Use & Misuse. 2009;44:934–942. doi: 10.1080/10826080802490659. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tremblay PF, Graham K, Wells S, Harris R, Pulford R, Roberts SE. When do first-year college students drink most during the academic year? An internet-based study of daily and weekly drinking. Journal of American College Health. 2010;58:401–411. doi: 10.1080/07448480903540465. [DOI] [PubMed] [Google Scholar]
- Triffleman E, Carroll K, Kellogg S. Substance dependence posttraumatic stress disorder therapy: An integrated cognitive-behavioral approach. Journal of Substance Abuse Treatment. 1999;17:3–14. doi: 10.1016/s0740-5472(98)00067-1. [DOI] [PubMed] [Google Scholar]
- Ullman J, Filipas HH. Gender differences in social reactions to abuse disclosures, post-abuse coping, and PTSD of child sexual abuse survivors. Child Abuse and Neglect. 2005;29:767–782. doi: 10.1016/j.chiabu.2005.01.005. [DOI] [PubMed] [Google Scholar]
- Vriends N, Becker ES, Meyer A, Williams S, Lutz R, Margraf J. Recovery from social phobia in the community and its predictors: Data from a longitudinal epidemiological study. Journal of Anxiety Disorders. 2007;21:320–337. doi: 10.1016/j.janxdis.2006.06.005. [DOI] [PubMed] [Google Scholar]
- Weathers FW, Huska JA, Keane TM. The PTSD Checklist- Civilian Version (PCL-C) 1991. Available from F.W. Weathers, National Center for PTSD, Boston VAMC, 150 S. Huntington Ave., Boston, MA, 02130. [Google Scholar]
- Weathers FW, Litz BT, Herman DS, Huska JA, Keane TM. The PTSD Checklist (PCL): Reliability, validity, and diagnostic utility. Paper presented at the meeting of the International Society for Traumatic Stress Studies; San Antonio, TX. Oct, 1993. [Google Scholar]
- White HR, Labouvie EW, Papadaratsakis V. Changes in substance use during the transition to adulthood: A comparison of college students and their non-college age peers. Journal of Drug Issues. 2005;35:281–304. [Google Scholar]
- Wood MD, Read JP, Palfai TP, Stevenson JF. Social influence processes and college student drinking: The mediational role of alcohol outcome expectations. Journal of Studies on Alcohol. 2001;62:32–43. doi: 10.15288/jsa.2001.62.32. [DOI] [PubMed] [Google Scholar]
- Wu L, Pilowsky DJ, Schlenger WE, Hasin D. Alcohol use disorders and the use of treatment services among college-age young adults. Psychiatric Services. 2007;58:192–200. doi: 10.1176/appi.ps.58.2.192. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zlotnick C, Franklin CL, Zimmerman M. Does “subthreshold” posttraumatic stress disorder have any clinical relevance? Comprehensive Psychiatry. 2002;43:413–419. doi: 10.1053/comp.2002.35900. [DOI] [PubMed] [Google Scholar]