Abstract
Intraoperative anaphylactic shock is an unusual complication. Different causes can be involved. Surgery of hydatid cyst is rarely responsible. About a case report of anaphylactic shock due to hydatid cyst surgery, the authors discuss the mechanisms, principles of treatment, and prevention measures of this complication.
Keywords: Anaphylactic shock, hydatid cyst, prevention, surgery, treatment
INTRODUCTION
Anaphylaxis during anesthesia is uncommon. The effects of this complication range from mild urticaria to life-threatening circulatory shock. The estimated incidences of this complication vary between 1 in 5000 and 1 in 20,000[1] procedures with mortality from 3% to 6%.[2] All drugs and substances used during anesthesia and surgery may be implicated in these reactions. Muscle relaxants, antibiotics, and latex are most often involved.[3] Type of surgery is rarely involved. We report a case of anaphylactic shock during hydatid cyst surgery.
CASE REPORT
A 38-year-old woman was scheduled for elective surgery for a two liver hydatid cyst located in segment VII and VII diagnosed by computed tomography with a dimension of 5 × 6 × 5.5 cm. At the preoperative visit the patient measuring 176 cm and weighing 78 kg with a body mass index of 25.18 kg/m2. Her blood pressure was 132/67 mmHg, with a pulse rate of 82 beats/min. No personnel or familial history of allergy was documented. Preoperative examinations of the cardiovascular and respiratory systems were normal. Electrocardiography (ECG) and chest X-ray were unremarkable. Laboratory tests including alanine transaminase, aspartate transaminase, international normalized ratio, fibrinogen, urea, creatinine, and blood glucose concentrations were normal.
The day before surgery, a blood test with a request for a 2 pockets was made. After a premedication with hydroxyzine (75 mg), the patient was admitted in operative room where a standard monitoring including heart rate, arterial oxygen saturation (SpO2), and non invasive pression (NIP) has been installed. After a catheterization of a peripheral vein, an IV 2 g of cefazolin was administered without problems notably; the hemodynamic of patient remained stable. The initial parameters with a heart rate (HR) at 78 beats/min, NIP at 124/76 mmHg, and SpO2 at 99% have allowed induction of anesthesia with propofol (3 mg/kg), fentanyl (2.5 μg/ kg), and cisatracurium (0.15 mg/kg). Tracheal intubation with a normal tube was successful realized with a standard laryngoscope. The patient was connected to respirator and anesthesia was maintained with isoflurane (1%–1.5%) in a mixture of nitrous oxide and oxygen (50%:50%). With ventilation by a tidal volume of 480 mL, and rate of 13 breaths/min, SpO2 was 99%, capnography [endtidal CO2 (ETCO2)] was 38 mmHg and peak airway pressure (PAwP) was 21 cmH2O. Surgical incision was made after a bolus of fentanyl (50 μg). Five minutes after the opening of the second cyst (segment VIII), patient had presented hypotension (NIP: 65/34 mmHg), tachycardia (HR: 110 beats/min) without desaturation (SPO2: 98%). Surgical manipulations were stopped. Inhalator agent (isoflurane) was closed and oxygen fraction was increased to 100%. Pulmonary auscultation was normal and symmetric; in particular there was no wheeze. EtCO2 (39 mmHg) and airway pressure (20 cmH2O) had not changed. Monitoring did not notice any changes in ECG and no macroscopic evidence of infection was noted by surgeon. No cutaneous signs were noted on the face or neck. Blood loss was low (approximately ≈150 mL). Provisional diagnosis of anaphylactic shock was made. A second peripheral venous catheter (16 gauge), and arterial catheter were placed. Fluid resuscitation (saline 0.9%) 500 mL per 500 mL (with a total of 1500 mL) and IV boluses of ephedrine (30 mg total) allowed only a slight improvement (NIP: 69/43 mmHg). Epinephrine boluses (100 μg to a total of 300 μg) were administered and relayed by continuous infusion (0.08 μg/ kg/min) via a central venous catheter. This therapeutic has stabilized the hemodynamic status (NIP: 109/56 mmHg and HR: 90 beats/min) and so continue the surgery. A bolus of 200 mg of hydrocortisone was administered. No need for additional bolus of epinephrine or an increase in infusion rate were required for the rest of the surgery. After removing of surgical draping, presence of skin signs all over the body has attracted attention of the team [Figures 1 and 2]. Diagnosis of anaphylactic shock was then strongly suspected. Serum tryptase was not measured because of its nonavailability in our hospital. The patient was transferred to ICU. Postoperative course was unremarkable with extubation 1 h later and a withdrawal of drugs 3 h later. The patient was discharged home after 5 days of hospitalization.
Figure 1.
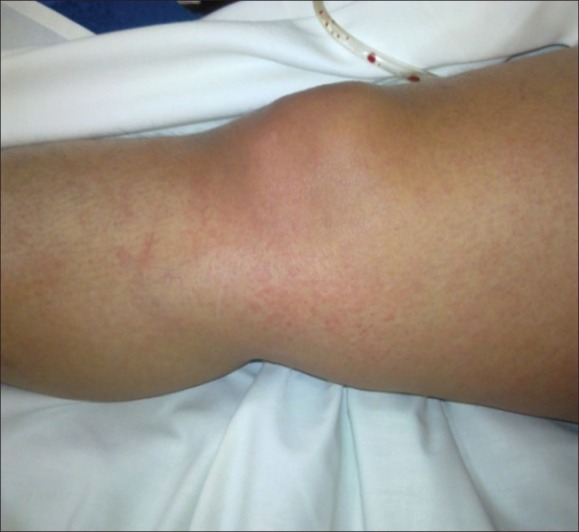
Cutaneous signs in the lower limb
Figure 2.
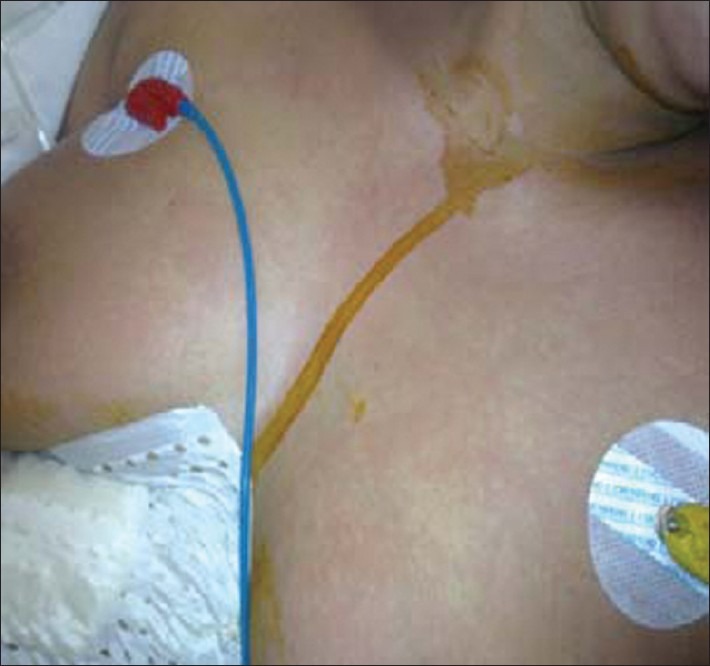
Cutaneous signs in the chest
DISCUSSION
Hydatid disease is a parasitic infestation caused by the larval form of Echinococcus. Surgical techniques are variable.[4] Most often this disease remains silent. Fortuitous discovery or from complications, such as anaphylactic shock following spontaneous[5] or ruptures have been described.[6,7] In intraoperative various factors can cause contamination by hydatid fluid with triggering anaphylactic reactions. The symptoms vary from mild urticaria to anaphylactic shock.[8] In the surgery of hydatid cyst, the incidence of this serious complication was variable.[9] The mechanism of these reactions is complex. In some cases, it is typically a hypersensitivity reaction type I associated with immunoglobulin E in response of a high plasma concentration of antigens Ecchinococcus.[10] Anaphylactic or anaphylactoid reactions may also be secondary to complement activation with liberation of anaphylatoxins.[11] The symptomatology is variable depending on the severity. During anesthesia cardiovascular signs, such hypotension, tachycardia, and arrhythmia predominate. Cutaneous symptoms, such as rash, flushing, and urticaria, are common in the neck, face, and especially on the anterior chest but these signs are often hidden by surgical draping. Occurrence of bronchospasm is less frequent and less sensitive, especially after general anesthesia. In incomplete presentations (only one symptom: hypotension, bronchospasm, so on) diagnosis of anaphylactic shock occurs after elimination of other causes: acute myocardial infarction, carcinoid syndrome, and hypovolemic shock.
In surgery of hydatid cyst, causality of anaphylactic shock cannot be attributed to hydatid fluid that after eliminating the other causal drugs administered during surgery: Antibiotics, muscle relaxants, and so on. Otherwise, toxicity of scolicide product can cause cardiovascular events miming an aspect of anaphylaxis.
In our cases, anaphylactic shock was attributed to hydatid fluid due to the elimination of other causes and occurred at a distance of induction (time of injection of drugs). Nevertheless, the diagnosis of anaphylaxis should be established by various immunologic immunofluorescence reactions and immunoelectrophoresis hemagglutination.[12] In our center, these reactions were unavailable and not realized in our patient.
The treatment of anaphylactic shock during surgery is facilitated by the prior installation of monitoring, of vascular access and airway access if general anesthesia. This treatment consists of stopping administration of any medication, stopping momentary intervention, massive fluid resuscitation, and administration of vasopressor and corticosteroids. Fluid replacement should be assured by crystalloids. For vasopressor, epinephrine is the first-line treatment in most guidelines on perioperative management of anaphylaxis.[13–15] Glucocorticoids are often administered in acute phase of anaphylactic shock, although their effects are delayed several hours; a beneficial role has been suggested to prevent the recurrence of manifestations of anaphylaxis in the late phase.[16] Our patient has received a saline solution, corticosteroids, and epinephrine by bolus and infusion. Hemodynamic response was good and authorized to continue surgery.
Prevention of anaphylaxis of hydatid cyst is surgical; it is to avoid overdistension of the cyst by soft injecting of scolicide and gentle manipulation of the cyst. Other techniques have been described.[17,18] The choice of laparoscopy appears to be effective for the prevention, in the analysis of 5943 percutaneous treatment procedures on hepatic and nonhepatic echinococcal cysts, risk of anaphylactic reactions was low, with 0.03% of lethal anaphylaxis and 1.7% of reversible allergic reactions.[19] The choice of this technique was limited in complicated cyst. Medical prevention, including histamine H1, H2 receptor blockers, and corticosteroids, remains controversial. In a prospective study, the preoperative administration of H1 and H2 receptor blockers has mitigated the hemodynamic responses secondary of spillage of hydatid cyst.[20]
CONCLUSION
Hydatid cyst surgery is often simple. The occurrence of hemodynamic instability, apart from the bleeding and hypovolemia, should suggest the diagnosis of anaphylaxis and start the specific management. All prevent medical and surgical measures can be justified given of severity of anaphylaxis.
Footnotes
Source of Support: Nil
Conflict of Interest: None declared.
REFERENCES
- 1.Harboe T, Guttormsen AB, Irgens A, Dybendal T, Florvaag E. Anaphylaxis during anesthesia in Norway: A 6-year single-center follow-up study. Anesthesiology. 2005;102:897–903. doi: 10.1097/00000542-200505000-00006. [DOI] [PubMed] [Google Scholar]
- 2.Fisher MM, Baldo BA. The incidence and clinical features of anaphylactic reactions during anesthesia in Australia. Ann Fr Anesth Reanim. 1993;12:97–104. doi: 10.1016/s0750-7658(05)81016-0. [DOI] [PubMed] [Google Scholar]
- 3.Mertes PM, Alla F, Tréchot P, Auroy Y, Jougla E. Groupe d’Etudes des Réactions Anaphylactoïdes Peranesthésiques.Anaphylaxis during anesthesia in France: An 8-year national survey. J Allergy Clin Immunol. 2011;128:366–73. doi: 10.1016/j.jaci.2011.03.003. [DOI] [PubMed] [Google Scholar]
- 4.Brunetti E, Junghanss T. Update on cystic hydatid disease. Curr Opin Infect Dis. 2009;22:497–502. doi: 10.1097/QCO.0b013e328330331c. [DOI] [PubMed] [Google Scholar]
- 5.Boyano T, Moldenhauer F, Mira J, Joral A, Saiz F. Systemic anaphylaxis due to hepatic hydatid disease. J Investig Allergol Clin Immunol. 1994;4:158–9. [PubMed] [Google Scholar]
- 6.Shameem M, Akhtar J, Bhargava R, Ahmed Z, Khan NA, Baneen U. Ruptured pulmonary hydatid cyst with anaphylactic shock and pneumothorax. Respir Care. 2011;56:863–5. doi: 10.4187/respcare.00821. [DOI] [PubMed] [Google Scholar]
- 7.Tonnelet R, Jausset F, Tissier S, Laurent V. Spontaneous rupture of a hydatid cyst and anaphylactic shock] J Radiol. 2011;92:735–8. doi: 10.1016/j.jradio.2011.03.021. [DOI] [PubMed] [Google Scholar]
- 8.Vuitton DA. Echinococcosis and allergy. Clin Rev Allergy Immunol. 2004;26:93–104. doi: 10.1007/s12016-004-0004-2. [DOI] [PubMed] [Google Scholar]
- 9.Jakubowski MS, Barnard DE. Anaphylactic shock during operation for hydatid disease. Anesthesiology. 1971;34:197–9. doi: 10.1097/00000542-197102000-00029. [DOI] [PubMed] [Google Scholar]
- 10.Khoury G, Khoury SJ, Soueidi A, Nabbout G, Baraka A. Shock complicating laparoscopic treatment of hydatid cysts of the liver. Surg Endosc. 1998;12:452–4. doi: 10.1007/s004649900703. [DOI] [PubMed] [Google Scholar]
- 11.Perricone R, Fontana L, De Coralis C, Ottaviani P. Activation of alternative complement pathway by fluid from hydatid cysts. N Engl J Med. 1980;302:808–9. doi: 10.1056/nejm198004033021414. [DOI] [PubMed] [Google Scholar]
- 12.Simons FE, Ardusso LR, Bilò MB, El-Gamal YM, Ledford DK, Ring J, et al. World Allergy Organization.World Allergy Organization anaphylaxis guidelines: summary. J Allergy Clin Immunol. 2011;127:587–93.e1. doi: 10.1016/j.jaci.2011.01.038. 22. [DOI] [PubMed] [Google Scholar]
- 13.Kroigaard M, Garvey LH, Gillberg L. Scandinavian Clinical Practice Guidelines on the diagnosis, management and follow-up of anaphylaxis during anaesthesia. Acta Anaesthesiol Scand. 2007;51:655–70. doi: 10.1111/j.1399-6576.2007.01313.x. [DOI] [PubMed] [Google Scholar]
- 14.American Heart Association: Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Anaphylaxis: 10.6. Circulation. 2005;112:143–5. doi: 10.1161/CIRCULATIONAHA.105.166550. [DOI] [PubMed] [Google Scholar]
- 15.Longrois D, Lejus C, Constant I, Bruyère M, Mertes PM. Treatment of hypersensitivity reactions and anaphylactic shock occurring during anaesthesia] Ann Fr Anesth Reanim. 2011;30:312–22. doi: 10.1016/j.annfar.2010.12.010. [DOI] [PubMed] [Google Scholar]
- 16.Kloeck W, Cummins RO, Chamberlain D, Bossaert L, Callanan V, Carli P, et al. Special resuscitation situations: An advisory statement from the International Liaison Committee on Resuscitation. Circulation. 1997;95:2196–210. doi: 10.1161/01.cir.95.8.2196. [DOI] [PubMed] [Google Scholar]
- 17.Kosar A, Orki A, Haciibrahimoglu G, Kiral H, Arman B. Effect of capitonnage and cystotomy on outcome of childhood pulmonary hydatid cysts. J Thorac Cardiovasc Surg. 2006;132:560–4. doi: 10.1016/j.jtcvs.2006.05.032. [DOI] [PubMed] [Google Scholar]
- 18.Santini M, Fiorello A, Vicidomini G, Perrone A. A home-made device for safe intraoperative aspiration of pulmonary hydatid cysts. Interact Cardiovasc Thorac Surg. 2008;7:365–7. doi: 10.1510/icvts.2007.170621. [DOI] [PubMed] [Google Scholar]
- 19.Neumayr A, Troia G, de Bernardis C, Tamarozzi F, Goblirsch S, Piccoli L, et al. Justified concern or exaggerated fear: The risk of anaphylaxis in percutaneous treatment of cystic echinococcosis: A systematic literature review. PLoS Negl Trop Dis. 2011;5:e1154. doi: 10.1371/journal.pntd.0001154. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Kambam JR, Dymond R, Krestow M, Handte RE. Efficacy of histamine H1 and H2 receptor blockers in the anesthetic management during operation for hydatid cysts of liver and lungs. South Med J. 1988;81:1013–5. doi: 10.1097/00007611-198808000-00018. [DOI] [PubMed] [Google Scholar]


