Abstract
Purpose
Planovalgus foot deformity is common in diplegic and quadriplegic patients. Surgery is the definitive treatment to restore the alignment of the talus, calcaneus, and navicular bones. We aimed, in the current study, to compare the effectiveness of subtalar fusion and calcaneal lengthening, and to assess the recurrence in ambulatory children with cerebral palsy.
Methods
This is a retrospective study of 78 patients (138 feet diagnosed with planovalgus deformity) who underwent surgical correction using subtalar fusion or calcaneal lengthening. Range of motion, radiographic indices, kinematic, and pedobarographic data were used to examine the deformity and the outcome of surgery. A repeated measures analysis of variance (ANOVA) was used to test the study hypothesis.
Results
Most of the patients were diplegic (87.2 %) and the mean age at surgery was 11.9 ± 2.9 years (range from 4.7 to 18.3 years), with a mean follow-up of 5 ± 4.4 years (range from 1 to 15.4 years). Sixty-three feet were treated with calcaneal lengthening, while 75 were treated with subtalar fusion. The feet treated with subtalar fusion were more severe preoperatively. However, both surgery groups showed improvement postoperatively. Among 12 cases of recurrence, medial column fusion was the main surgery performed to correct the deformity.
Conclusions
Surgery is effective in the treatment of planovalgus deformity in ambulatory children with cerebral palsy. Severe and rigid planovalgus feet can be treated effectively with subtalar fusion. Feet with milder deformity show good results, with calcaneal lengthening. Surgery provides good correction in young patients, but there is a higher recurrence rate.
Electronic supplementary material
The online version of this article (doi:10.1007/s11832-012-0413-3) contains supplementary material, which is available to authorized users.
Keywords: Pes planovalgus, Subtalar fusion, Calcaneal lengthening, Cerebral palsy
Introduction
Pes planovalgus is the most common foot deformity in all ages of children with cerebral palsy (CP) [1], specifically among diplegic and quadriplegic patients [2, 3]. In this deformity, the foot is in valgus, external rotation, and dorsiflexion relative to the talus. The equinus drives the calcaneus to displace posteriorly and rotates into valgus, causing the talar head to subluxate medially and inferiorly. The forefoot tends to abduct, leading to subluxation of the calcaneocuboid joint with dorsal subluxation of the cuneonavicular joint in the medial column. Consequently, the navicular and the head of the talus become the weight-bearing areas, which is often painful [4].
The radiographic evaluations consist of many angles; however, there are variations in these measurements. Gait analysis for ambulatory patients gives quantitative data, specifically, foot pressure, which measures the distribution of forces acting on the foot. From the pressure measurement, we can calculate the coronal plane pressure index (CPPI), which is the difference in pressure between the lateral and medial parts of the foot [5]. These measurements and calculations are useful to quantify the severity of the deformity and to assess outcome after treatment.
Surgical treatment is indicated when the patient no longer tolerates orthotics or when the deformity is so severe that it causes mechanical instability, impacting gait. Surgical options differ according to the severity of the deformity. Subtalar fusion [6, 7] and lateral calcaneal lengthening [6] are common procedures.
This current study aimed to assess the comparative effectiveness of calcaneal lengthening and subtalar fusion in correcting planovalgus deformity in ambulatory patients with CP, and to examine the complications as well as to assess the predisposing factors related to the recurrence of the deformity.
Materials and methods
After approval from the Institutional Review Board, we conducted a retrospective study to assess and compare lateral calcaneal lengthening versus subtalar fusion for the treatment of planovalgus foot deformity in ambulatory children with CP who were treated in our institution between 1994 and 2008. Two groups of patients were identified according to the initial surgical procedure (lateral calcaneal lengthening and subtalar fusion). All the associated surgical procedures were considered in the data collection.
Surgical technique
Subtalar fusion was an intra-articular fusion using allograft and screw fixation, and had been observed to be reliable and safe to correct planovalgus foot deformity in children with CP [7]. Subtalar fusion was performed with lateral exposure and removal of all the contents of the sinus tarsi, including the joint capsules of the posterior, middle, and anterior facets. This helps to mobilize the subtalar joint and to reduce the calcaneus to a normal anatomical position under the talus. Only the cartilage of the anterior facet is removed and through a separate medial incision, which exposes the talar neck. After that, a guide wire is driven across the anterior facet from anterior medial to plantar lateral. This should be transverse across the midfoot, since the center of rotation of the hind foot deformity is in the middle of the sinus tarsi, and it is important to be away from this center of rotation in order to gain good fixation. A cannulated screw is then driven across with good compression of the cancellous bone in the anterior facet, and the sinus tarsus is filled with allograft bone (Fig. 1). The calcaneal lengthening is performed with the same exposure, except we do not remove the soft tissue of the sinus tarsus. The calcaneal osteotomy is made midway between the posterior facet and the calcaneocuboid joint, without concern if it enters the middle facet. The osteotomy is then distracted and allograft bone is inserted and usually fixed with a two-hole semitubular plate (Fig. 2).
Fig. 1.
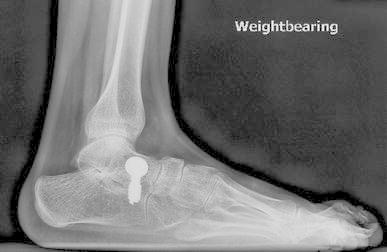
Subtalar fusion procedure. This radiograph shows mild residual forefoot supination which was judged intra-operatively to not be significant enough to correct
Fig. 2.
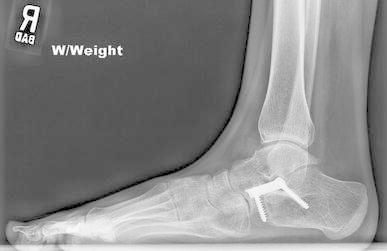
Lateral calcaneal lengthening procedure
The next step in both procedures is to carefully evaluate the foot and, if it does not come to neutral dorsiflexion with the knee fully extended, a gastrocnemius recession is performed, and if the ankle does not come to neutral with the knee flexed, an open Z-plasty lengthening of the tendon Achilles is performed. Next, a careful assessment of the midfoot is performed by putting pressure on the metatarsal heads. If there is forefoot supination, the navicular tuberosity is excised and the cuneonavicular joint is exposed. If this joint is hypermobile, a plantar medial-based wedge is resected and the fusion is fixed with a two-hole semitubular plate (Fig. 3). Usually, the tibialis anterior tendon is also transferred to the midfoot as part of the treatment of the forefoot supination. The tibialis posterior is advanced and sutured to the navicular. The foot is again tested and if there is instability with forefoot abduction, the calcaneocuboid joint is exposed on the lateral side with a decision made to carry out a fusion or further partial distal calcaneal turn-down osteotomy. A short leg cast was applied for 8 weeks and weight-bearing was allowed when the pain was tolerated. Orthoses were used if there was lack of ankle dorsiflexion–plantar flexion control or if there was a tendency of foot collapse.
Fig. 3.
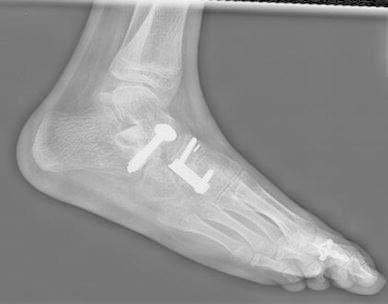
Subtalar fusion procedure with cuneonavicular joint fusion and proximal phalangeal osteotomy of the great toe. The radiograph is non-weight-bearing and shows residual forefoot supination. This is an important element of the deformity to correct and can be difficult to completely correct
Data collected
The medical records were examined and patients who had subtalar fusion or lateral calcaneal lengthening with available preoperative and postoperative gait analysis evaluations were included in this study. The data collected included: type of CP, height, weight, type of surgery, and reported foot pain. The body mass index (BMI) for each patient was calculated and compared with the Centers for Disease Control and Prevention (CDC) growth charts [8]. We divided the subjects into three BMI groups (underweight, normal, and overweight) [8]. We also evaluated and grouped individuals by the Gross Motor Function Classification System (GMFCS), depending on patients’ functional abilities, use of assistive devices, and quality of movement [9]. These data were collected from gait lab charts and gait videos. Two groups were identified, one for good ambulators (GMFCS I/II) and the other for those with lesser functional abilities (GMFCS III/IV).
Foot pressure (pedobarograph) was measured using the Tekscan High-Resolution Pressure Assessment System (Tekscan Inc., South Boston, MA) [10]. The foot was divided into five components, namely, medial midfoot (MMF), medial forefoot (MFF), lateral midfoot (LMF), lateral forefoot (LFF), and heel. The CPPI represents valgus–varus deviation [5]. The CPPI was calculated by subtracting the lateral foot pressure from the medial foot pressure and then dividing the result by the sum of the mid- and forefoot pressure ([MMF + MFF] − [LMF + LFF]/[MMF + MFF + LMF + LFF]) [10]. The normal range is −30 to 12, with values less than −30 indicating varus deviation of the foot. The data from gait records also included measures of passive ankle range of motion, stride length, and forward velocity.
The radiographic evaluation consisted of three angles [11], and non-weight-bearing radiographs were excluded from the study results:
Lateral talocalcaneal angle (on the lateral view, between the long axis of the talus and a line across the lower-most point of the anterior and the posterior part of the calcaneus);
Lateral calcaneal pitch (on the lateral view, between a line through the lower-most point of the posterior part of the calcaneus to the lower-most point of the anterior calcaneus and a line from the lower-most point of the posterior part of the calcaneus to the lower-most point of the fifth metatarsus);
Meary angle (on the lateral view, between the long axis of the talus and the first metatarsus).
All the parameters were available for preoperative and last follow-up (more than 1 year after surgery).
The outcomes were examined to compare the outcome of subtalar fusion and calcaneal lengthening based on the difference in study parameters between preoperative and the last available follow-up. Recurrence of the deformity was represented by patients who needed another surgery to correct foot deformity.
Statistical analysis
The data were examined for normality based on skewness and kurtosis. We examined the distribution of the categorical variables by using frequencies, percentages, and Chi-square test, whereas, an independent samples t-test was used for continuous variables (Mann–Whitney U-test was used for nonparametric data). To evaluate the overall outcome of surgery implying change over time in the study variables, we used a paired t-test (Wilcoxon rank-sum test was used for nonparametric variables). A repeated measures analysis of variance (ANOVA) test was used to compare changes over time between surgery groups. Further, univariable and multivariable logistic regression models were used to determine factors which may contribute to the recurrence. To build the multivariable model, we included only the potential predictors with a significance of less than 0.25 in the univariable model that were related to the indicated deformity [12]. The significance level was 0.05, which was adjusted to 0.01 when more than four factors were included in the multivariable model. The potential predictors were presented as odds ratios (ORs) and 95 % confidence intervals (CIs). All tests were two-tailed and analyses were performed using SPSS version 17.0 (Statistical Package for the Social Sciences, Chicago, IL).
Results
There were 78 patients with 138 planovalgus feet [43 boys (55.1 %) and 35 girls (44.9 %)]. Sixty-eight patients were diplegic with 123 feet (87.2 %), two patients with two feet were hemiplegic (2.6 %), and eight patients were quadriplegic with 13 feet (10.3 %). There were 63 feet (45.7 %) managed with calcaneal lengthening and 75 feet (54.3 %) with subtalar fusion. Out of 13 feet of quadriplegic patients, 12 feet were treated with subtalar fusion. All patients were ambulatory; thirty-eight (48.7 %) were good ambulators, while 40 patients (51.3 %) were poor ambulators. The mean age at surgery for foot correction was 11.9 ± 4.9 years (range from 4.7 to 18.3 years), and the mean follow-up in years was 5 ± 4.4 (range from 1 to 15.4 years). Patients with GMFCS III/IV were more often treated with subtalar fusion, χ2 = 4.94, df = 1, p = 0.026 (Table 1).
Table 1.
Study characteristics stratified by the type of the initial surgery (138 feet)
| Variable | Calcaneal lengthening, n* (%) | Subtalar fusion, n* (%) | χ2 (df) | p |
|---|---|---|---|---|
| Sex | 1.75 (1) | 0.185 | ||
| Boys | 39 (61.9) | 38 (50.7) | ||
| Girls | 24 (38.1) | 37 (49.3) | ||
| CP type | 10.4 (2) | 0.005 | ||
| Hemiplegic | 2 (3.2) | 0 (0) | ||
| Diplegic | 60 (95.2) | 63 (84.0) | ||
| Quadriplegic | 1 (1.6) | 12 (16.0) | ||
| GMFCS | 4.9 (1) | 0.026 | ||
| 1 and 2 | 38 (60.3) | 31 (41.3) | ||
| 3 and 4 | 25 (39.7) | 44 (58.7) | ||
| Preoperative pain | 0.14 (1) | 0.71 | ||
| With pain | 16 (25.4) | 17 (22.7) | ||
| Without pain | 47 (74.6) | 58 (77.3) | ||
| Preoperative BMI | 4.05 (2) | 0.132 | ||
| Underweight | 8 (13.8) | 4 (5.5) | ||
| Normal | 36 (62.1) | 56 (76.7) | ||
| Overweight | 14 (24.1) | 13 (17.8) | ||
Chi-square with continuity correction; Fisher’s exact test was reported when the expected count <5
n number of feet, % percentage within the surgery group
χ2 Chi-square, df degrees of freedom, CP cerebral palsy, GMFCS Gross Motor Function Classification System, BMI body mass index
* Frequencies for the whole feet number
Preoperative findings
The preoperative medial midfoot pressure analysis represented significant differences (p < 0.0001), with the subtalar fusion group having more severe planovalgus preoperatively, while there were no significant differences in the CPPI (Table 2). Significant differences were also found in the preoperative talocalcaneal angle (p = 0.02), stride length (p = 0.0001), forward velocity (p = 0.001), and ankle dorsiflexion with knee flexion (p = 0.001) (Table 2).
Table 2.
Preoperative study parameters (gait, radiographic indices, and range of motion) of ambulatory CP patients (138 feet) who received calcaneal lengthening or subtalar fusion for foot deformity correction
| Variable | Calcaneal lengthening | Subtalar fusion | Normal range | p**‡ | ||
|---|---|---|---|---|---|---|
| Mean | SD | Mean | SD | |||
| CPPI | 45.3 | 25.1 | 50.9 | 23.9 | −30–12 | 0.20 |
| Heel impulse | 16.6 | 15.9 | 14.3 | 16.2 | 23.3–39.8 | 0.43 |
| MMF | 13.4* | 5–21.4* | 23.5* | 15.5–35.4* | 0–10.7 | 0.0001 |
| Stride length | 82.3* | 71.9–93.5* | 60.4* | 53.2–77.1* | 128–143 | 0.0001 |
| Forward velocity | 83.7* | 55.0–95.9* | 53.3* | 36.5–72.4* | 117–145 | 0.0001 |
| Plantar flexion | 36.46 | 13.17 | 37.08 | 13.3 | 20–30 | 0.78 |
| Dorsal flexion/knee extension | 1.48 | 7.7 | 4.4 | 10.9 | 0–10 | 0.07 |
| Dorsal flexion/knee flexion | 8* | 4–15* | 15* | 8–25* | 0–10 | 0.001 |
| Meary angle | 23.9 | 11.8 | 30.7 | 14.0 | 4–20 | 0.77 |
| Pitch angle | 8.2 | 5.6 | 8.6 | 6.2 | 21–27 | 0.10 |
| Talocalcaneal angle | 46.5 | 7.1 | 50.2 | 12.2 | 39–50 | 0.02 |
CP cerebral palsy, CPPI coronal plane pressure index
* Median and interquartile range was used because of the absence of normality
** Significant difference was calculated depending on the independent t-test or Mann–Whitney U-test
‡ p-value based on the equality of variance interpretation for parametric data
Operation-related findings
Twenty-six feet underwent foot-only surgery (15 cases of calcaneal lengthening, eight cases of subtalar fusion, and three cases of both calcaneal lengthening and subtalar fusion), while 112 feet were part of multilevel surgery to correct accompanied problems (Table 3).
Table 3.
Concomitant foot correction procedures received by CP patients (138 feet) with the initial planovalgus foot correction surgery
| Foot surgery | Calcaneal lengthening | Subtalar fusion | χ2 | p | ||
|---|---|---|---|---|---|---|
| n | % | n | % | |||
| Foot-only procedure | 15 | 10.9 | 11 | 8.0 | – | – |
| Foot surgery as part of multilevel surgery | 48 | 34.8 | 64 | 46.4 | – | – |
| Foot procedures | ||||||
| Gastrocnemius recession | 39 | 61.9 | 42 | 56.0 | 0.49 | 0.48 |
| Achilles lengthening | 5 | 7.9 | 4 | 5.3 | 0.38 | 0.54 |
| Calcaneocuboid fusion | 0 | 0 | 16 | 21.3 | 15.2 | 0.0001 |
| Medial fusion | 2 | 3.2 | 21 | 28.0 | 15.2 | 0.0001 |
| Navicular tuberosity | 22 | 34.9 | 17 | 22.7 | 2.54 | 0.11 |
| Tibial osteotomy | 16 | 25.4 | 27 | 36.0 | 1.80 | 0.18 |
| Hallux operation | 26 | 41.3 | 16 | 21.3 | 6.43 | 0.011 |
| Other procedures | ||||||
| Hamstring lengthening | 41 | 65.1 | 51 | 68.0 | 0.13 | 0.72 |
| Rectus transfer | 18 | 28.6 | 33 | 44.0 | 3.50 | 0.06 |
| Adductor tenotomy** | 4 | 6.3 | 17 | 22.7 | 7.1 | 0.008 |
| Femoral osteotomy* | 11 | 17.5 | 18 | 24.0 | 0.88 | 0.35 |
| Patella maltracking surgery | 1 | 1.6 | 2 | 2.7 | –† | 1.0 |
| Ant. gluteus release | 0 | 0 | 1 | 1.3 | –† | 1.0 |
| Pelvic osteotomy | 1 | 1.6 | 1 | 1.3 | –† | 1.0 |
| Baclofen pump | 2 | 3.2 | 0 | 0 | –† | 0.207 |
n number of feet, % percentage within the surgery group, χ2 Chi-square, df degrees of freedom, CP cerebral palsy
* Femoral osteotomy also includes varus derotational osteotomy
** Adductors tenotomy includes also psoas lengthening
† Fisher’s exact test was reported when the expected count <5
Gastrocnemius recession and Achilles tendon lengthening were used in both subtalar fusion and calcaneal lengthening, while medial foot fusions and calcaneocuboid fusions were used more for feet corrected with subtalar fusion (Table 3). There were 15 patients treated with cuneonavicular fusion, six patients with talonavicular fusion, and one patient with talo-navicular-cuneiform fusion. Among patients who underwent talonavicular fusion, five patients also underwent calcaneocuboid fusion (triple arthrodesis). There were 20 patients with subtalar fusion who needed lateral calcaneal lengthening.
Pre- versus postoperative findings
There was a statistically significant change in the preoperative CPPI, MMF, and heel impulse in the whole sample, with remarkable improvement at last follow-up, p < 0.0001. Significant changes were also found for radiographic angles and ankle plantar flexion, while no difference was found for ankle dorsiflexion (supplemental material, Table S1). To examine whether or not the type of surgery had a significant effect on the outcome, we conducted repeated measures ANOVA with Bonferroni correction for multiple comparisons and found no significant effect of surgery type on the CPPI [F(1) = 0.043, p = 0.84] and on heel impulse (Table 4). Likewise, there was no significant effect of surgery on radiographic angles. However, there was a significant difference in the medial midfoot pressure (p = 0.0001). The mean preoperative MMF in the subtalar fusion group was higher than that in the calcaneal lengthening group, while both surgery groups had almost the same MMF pressure in the last follow-up. In addition, ankle dorsiflexion improvement over time was different between subtalar fusion and lateral calcaneal lengthening (Table 4).
Table 4.
The effects of calcaneal lengthening and subtalar fusion surgeries in CP children (138 feet) with planovalgus deformity
| Variable | Normal range | Calcaneal lengthening | Subtalar fusion | F | p‡ | ||
|---|---|---|---|---|---|---|---|
| Mean | SD | Mean | SD | ||||
| CPPI | 0.04 | 0.83 | |||||
| Preoperative | −30–12 | 45.3 | 25.1 | 50.9 | 23.9 | ||
| Last follow-up | 5.9 | 35.5 | 2.2 | 35.7 | |||
| Heel impulse | 0.75 | 0.39 | |||||
| Preoperative | 23.3–39.8 | 16.6 | 15.9 | 14.3 | 16.2 | ||
| Last follow-up | 29.3 | 20.4 | 27.2 | 17.8 | |||
| Medial midfoot (MMF) | 19.4 | 0.0001 | |||||
| Preoperative | 0–10.7 | 14.7 | 11.4 | 25.9 | 15.7 | ||
| Last follow-up | 5.3 | 5.6 | 8.2 | 7.6 | |||
| Lateral talocalcaneal angle | 0.55 | 0.46 | |||||
| Preoperative | 39–50 | 46.7 | 7.5 | 51.5 | 7.8 | ||
| Last follow-up | 41.7 | 7.7 | 40.1 | 7.9 | |||
| Pitch angle | 0.09 | 0.76 | |||||
| Preoperative | 21–27 | 6.8 | 4.1 | 9.4 | 5.9 | ||
| Last follow-up | 12.7 | 5.1 | 11.0 | 4.6 | |||
| Meary angle | 2.4 | 0.13 | |||||
| Preoperative | 4–20 | 23.7 | 12.1 | 30.3 | 11.7 | ||
| Last follow-up | 10.4 | 7.2 | 12.1 | 6.5 | |||
| Ankle plantar flexion | 0.6 | 4 | |||||
| Preoperative | 20–30 | 37.6 | 11.6 | 36.8 | 13.6 | ||
| Last follow-up | 29.9 | 11.9 | 27.9 | 14.4 | |||
| Ankle dorsal flexion with knee extension | 4.7 | 0.03 | |||||
| Preoperative | 0–10 | 1.5 | 7.8 | 4.4 | 10.3 | ||
| Last follow-up | 3.2 | 6.8 | 5 | 7.2 | |||
| Ankle dorsal flexion with knee flexion | 10.4 | 0.002 | |||||
| Preoperative | 0–10 | 9.5 | 8.9 | 15.5 | 11.8 | ||
| Last follow-up | 11.6 | 8.9 | 14.4 | 8.1 | |||
n number of feet, SD standard deviation, CPPI coronal plane pressure index
‡ p-value was calculated using repeated measures analysis of variance to compare the change between the surgery groups
There was a slight change in stride length and velocity at the last follow-up compared to preoperative status. There were 48 patients who had a slight increase of velocity (mean change was 16 cm/s); however, the overall change had the trend of reduction in velocity (Tables S1–S3 in the supplemental material).
Based on functional abilities graded by the GMFCS, we found that six children were preoperatively in GMFCS III/IV, who were then classified in GMFCS I/II at the last follow-up. On the other hand, two children who were initially in GMFCS I/II experienced loss of their functional abilities and became GMFCS III/IV postoperatively.
Among the entire sample of patients, nine patients (12 feet) required further surgical procedure to correct a recurrent foot deformity. Eight feet were initially treated with subtalar fusion (they were GMFCS III/IV) and four with calcaneal lengthening (they were GMFCS I/II) (Table 5). The mean period of time between the first and the second surgeries was 4.6 ± 2.4 years (not shown in the table). Most of these feet (eight feet) were treated with medial fusion at the second procedure, and two feet were treated simultaneously with calcaneal lengthening and subtalar fusion (Table 5). Out of eight quadriplegic patients (13 feet) in the entire sample, two patients (two feet) underwent another surgery to correct foot deformity. There was no difference in the preoperative parameters between recurrence feet and the rest of the sample (see supplemental material, Table S4). Based on pedobarograph measurements before the second surgery in the recurrence feet, there was improvement in the CPPI compared to the initial evaluation; however, there was still valgus deviation, increase in medial midfoot pressure, and decrease in heel impulse (see supplemental material, Table S5).
Table 5.
Characteristics and surgery applied to recurrent feet
| ID | 1st Sx | 1st age | Sex | CP | 2nd age | Age difference | GMFCS | Pain | BMI | CCF | NO | MF | CL | SF |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | SF | 12.9 | 2 | 4 | 16.6 | 3.6 | 2 | 2 | – | * | * | * | ||
| 2.a | SF | 6.7 | 1 | 2 | 14.1 | 7.4 | 2 | 2 | 2 | * | ||||
| 2.b | SF | 6.7 | 1 | 2 | 14.1 | 7.4 | 2 | 2 | 2 | * | ||||
| 3.a | SF | 9.2 | 1 | 2 | 13.1 | 4.0 | 2 | 2 | 1 | * | * | * | ||
| 3.b | SF | 9.2 | 1 | 2 | 13.1 | 4.0 | 2 | 2 | 1 | * | * | |||
| 4 | CL | 7.3 | 2 | 2 | 10.7 | 3.4 | 1 | 2 | 2 | * | * | * | * | * |
| 5 | SF | 8.4 | 2 | 4 | 17.3 | 8.8 | 2 | 2 | 2 | * | ||||
| 6.a | SF | 11.7 | 1 | 2 | 15.7 | 4.0 | 2 | 1 | 2 | * | * | |||
| 6.b | SF | 11.7 | 1 | 2 | 15.7 | 4.0 | 2 | 1 | 2 | * | * | |||
| 7 | CL | 10 | 2 | 2 | 16.2 | 6.1 | 1 | 2 | 2 | * | ||||
| 8 | CL | 14.2 | 1 | 2 | 16.3 | 2.1 | 1 | 1 | – | * | ||||
| 9 | CL | 16.9 | 1 | 2 | 18.6 | 1.6 | 1 | 1 | 2 | * |
1st Sx first foot correction surgery, 1st age age at first surgery, 2nd age age at second surgery, Age difference the period of time since the first procedure, GMFCS Gross Motor Function Classification System (1 GMFCS I/II, 2 GMFCS III/IV, BMI body mass index (1 underweight, 2 normal), CCF calcaneocuboid fusion, NO navicular osteotomy, MF medial fusion, CL calcaneal lengthening, SF subtalar fusion, CP cerebral palsy
Pain was reported in 33 feet before surgery (16 feet in the calcaneal lengthening group and 17 feet in the subtalar fusion group). At the last follow-up, there were 35 feet with pain (23 feet treated with calcaneal lengthening and 12 feet treated with subtalar fusion). There was no case of infection in our patient sample, while there were 13 cases of hardware-related problems [four patients (six feet) were treated with calcaneal lengthening, two patients (four feet) were treated with subtalar fusion, and two patients (three feet) were treated with subtalar fusion and calcaneal lengthening].
The potential predictors of deformity recurrence among ambulatory children with CP treated with calcaneal lengthening or subtalar fusion were assessed using a univariable logistic regression model. With this model, we found that, for every one-unit increase in the preoperative CPPI, there was a 3 % increase in the odds of recurrence and need for further surgery; however, this finding was not very statistically stable, OR = 1.03, 95 % CI (0.99–1.06), p = 0.19 (not shown in the table). To further determine single potent predictors, we created a multivariable model using distinctive subgroups, namely, demographic, clinical, and pedobarographic measurements (Table 6). Age at the first surgery was a significant predictor of recurrence after adjustment for the BMI. Consequently, for every one-unit increase in age, there was a 22 % decreased risk of recurrence, OR = 0.78, 95 % CI (0.62–0.97), p = 0.03.
Table 6.
Potential predictors for recurrence of planovalgus deformity among ambulatory CP patients treated with calcaneal lengthening or subtalar fusion
| Variable | ORa | 95 % CI | p |
|---|---|---|---|
| Demographic | |||
| Age at 1st surgery | 0.78 | 0.62–0.97 | 0.03 |
| BMI | |||
| Underweight | 1.47 | 0.24–8.84 | 0.67 |
| Normal | 1.0 | Referent | Referent |
| Overweight | –b | – | – |
| Clinical | |||
| GMFCS | |||
| Good ambulators | 1.0 | Referent | Referent |
| Poor ambulators | 3.07 | 0.78–12.07 | 0.11 |
| Ankle plantar flexion | 1.04 | 0.98–1.10 | 0.17 |
| Ankle dorsal flexion with knee extension | 1.04 | 0.98–1.10 | 0.18 |
| Radiographic | |||
| Pitch angle | 0.92 | 0.77–1.11 | 0.39 |
| Talocalcaneal angle | 0.96 | 0.89–1.04 | 0.37 |
| Pedobarograph | |||
| CPPI | 1.01 | 0.97–1.06 | 0.54 |
| LFF | 0.92 | 0.78–1.09 | 0.33 |
CP cerebral palsy, BMI body mass index, GMFCS Gross Motor Function Classification System, CPPI coronal plane pressure index
aOR implies the prevalence odds ratio, CI confidence interval
bOdds ratio could not be calculated because of the small number of cases
Although not shown in a table, potential predictors for recurrence were examined by the type of surgery using the same model. Forward velocity was a significant predictor of recurrence in the subtalar fusion group. For every one-unit increase in forward velocity, there was a 3 % decrease in the odds of recurrence, OR = 0.97, 95 % CI (0.94–0.99), p = 0.04. Age and BMI were also significant predictors in the univariable and multivariable models. However, the clinical and pedobarographic parameters did not significantly predict planovalgus recurrence in the subtalar fusion group, p > 0.05. Finally, we created a similar model in the calcaneal lengthening group but found no single predictor of recurrence, p > 0.05.
Discussion
Pes planovalgus in ambulatory children with CP is a common deformity. The primary treatment in milder cases and younger children involves the use of orthotics. However, as the child’s weight increases, the planovalgus deformity becomes a major contributor to stance phase instability due to lever arm dysfunction and the orthotics are no longer tolerated. The goal of surgical treatment is to enhance stance phase stability and to create a stable comfortable foot that may improve gait function. The aim of this study was to examine and compare two surgical techniques used in the treatment of planovalgus foot deformity in ambulatory children with CP, and also to determine the amount and maintenance of deformity correction and to examine factors that may lead to deformity recurrence.
The patients in this sample were all managed by two surgeons and the procedures were part of a multilevel reconstruction plan based on an individual surgical planning from three-dimensional gait analysis. The decision to perform subtalar fusion versus calcaneal lengthening in an individual patient was at the discretion of the surgeon, and there were no specific criteria from gait analysis or radiographs to make this decision. There was a recognized and acknowledged bias in favor of performing subtalar fusions on more severe planovalgus deformities and less functional ambulators (GMFCS III/IV). We also tended to use calcaneal lengthening more in patients who were good ambulators (GMFCS I/II) and for milder deformities. Figure 4 represents the surgical treatment algorithm of planovalgus foot deformity in ambulatory children with CP.
Fig. 4.

Surgical treatment algorithm of planovalgus foot deformity in ambulatory children with cerebral palsy (CP)
Based on our recognized bias, this study found that patients with subtalar fusion were more likely to be in the GMFCS III/IV group, and planovalgus deformity was worse based on increased MMF, shorter step length, and lower gait velocity compared to the calcaneal lengthening group.
Because the major reason for planovalgus foot correction is to improve the mechanical stiffness and weight-bearing function of the foot, the assessment of how the foot contacts the floor should be a major consideration in the outcome, with the goal being to normalize the foot–floor contact pattern. Foot pressure is altered in planovalgus deformity due to midfoot break and forefoot lateral deviation, and the pedobarograph is a sensitive measure for the severity of planovalgus [4]. There are other deformities which may also impact the pedobarographic pattern, such as foot progression angle. In the current study, there was no preoperative difference in the CPPI; however, the subtalar fusion group had higher preoperative medial midfoot pressure compared to the lateral calcaneal lengthening group. This could be explained by associated rotational deformities of the lower limbs, which might have affected the distribution of foot pressure represented by the CPPI. Forward velocity and stride length are kinematic data which are correlated to the severity of neurologic involvement in ambulatory patients with CP. Muscular contracture and the subsequent limited joint movement also tend to have greater involvement in slower walkers. All patients had short stride length and low forward velocity; however, patients in the subtalar fusion group were more involved with significant difference, indicating more impaired gait pattern. There was improvement after the indicated surgeries in the CPPI, heel impulse, and MMF, implying improved function of the foot as it interacts with the floor during gait. The degree of change was almost the same in both surgery groups in terms of the CPPI and heel impulse. However, the MMF showed a significant difference, as patients in the subtalar group had more severe midfoot break compared to the calcaneal lengthening group. Our findings confirm the results of previous studies, showing that subtalar fusion can successfully correct severe planovalgus deformity [13–15].
Radiographic indices reflect the relationship amongst the tarsal bones. The divergence of the talus and calcaneus on the lateral view appears as increased talocalcaneal angle, which is due to increased dorsiflexion of the calcaneus relative to the talus, with planter flexion of both the talus and calcaneus relative to the tibia. Talar plantar sag causes an increased Meary angle, which may also be seen as a midfoot break as well. The calcaneal pitch angle represents the plantar flexion of the calcaneus due to gastrocnemius contracture. Although there was a slight improvement in the calcaneal pitch angle at the last follow-up, it remained reduced, probably because of the recurrence of plantar flexor muscles contracture. In previous studies, the pitch angle was worse postoperatively in feet treated with extra-articular subtalar fusion compared with calcaneal lengthening, which might be due to the severe planovalgus deformity [13, 14].
Based on general walking function assessed by the GMFCS, we found that some of the GMFCS III/IV patients became better as they moved to the GMFCS I/II group. These patients were primarily dependent on assistive devices preoperatively because of severe lever arm dysfunction and crouch, who became independent after surgery. Four patients were GMFCS I/II and they dropped a grade to GMFCS III/IV at the last follow-up. These patients used to walk preoperatively with significant instability but not using assistive devices, and later progressed to using assistive devices, so they were reclassified from GMFCS II to GMFCS III.
Midfoot break, collapsed longitudinal arch, and forefoot supination are all related to subluxation between tarsal bones and indicate the severity of valgus foot deformity [3, 4]. After reducing the relationship between the talus and the calcaneus, forefoot supination and abduction need to be addressed by performing talonavicular joint and/or cuneonavicular joint fusion, as well as calcaneocuboid joint fusion [4]. In this current study, medial foot fusions and calcaneocuboid fusion were used more often in subtalar fusion feet. The aim was to reduce the medial column by carrying out the correction at the apex of the deformity, which was at the navicular–cuneiform level or talonavicular joint.
Maintenance of deformity correction is the target of management for planovalgus foot. Recurrent foot deformity was considered as a significant failure when it required further surgery for pain with weight-bearing or lever arm disease causing mechanical instability during gait. There were nine patients (12 feet) who underwent additional foot surgery; most of them were poor ambulators with severe deformity treated initially with subtalar fusion. The number of quadriplegic patients in our study was small (eight patients with 13 feet), two of whom (two feet) had recurrent foot deformity. Although this is not statistically significant, it reflects the high risk of deformity recurrence in quadriplegic patients. The most commonly required second procedure was a midfoot fusion to stabilize the medial column of the foot. This also reflects the fact that our attention to correct the medial column in the early period of this study group was much less than in the later part of the study period. Medial column fusion is now a major part of our focus in both calcaneal lengthening and subtalar fusion, with the goal being to define the area of instability and provide the correction at that time. The assessment of failure in this context confirms the need to correct medial column instability that has been reported previously [16, 17].
There is no clear evidence to suggest that orthotics impact the natural history of planovalgus deformity [4]. Soft-tissue procedures were suggested to treat early valgus deformities in younger ages. Peroneal muscle lengthening was recommended for this aim and to prevent severe deformities [18], although overcorrection was reported [19]. Since the natural history is unclear, with many children improving without intervention, we do not feel that there is a benefit in soft-tissue procedures alone. Pain, mechanical malfunction, and severe foot deformity are indications for reconstruction surgery. Based on the outcome of this current study, age at the first surgery was a predictor for recurrence of the deformity, meaning that the younger the patient, the more risk there is for recurrence. One of the potential contributions of recurrence is the increase of muscle contracture with growth. Early surgical treatment may be less complicated due to less severe foot deformity; however, recurrence is more frequent. On the other hand, waiting until late childhood or adolescence may be recommended, recognizing that more severe deformity will likely be encountered. Moreover, we were not able to find other predictors of recurrence when examining the radiographic and pedobarographic parameters. Our inability might have resulted from the small number of recurrent cases, since only 12 feet required repeat surgery, and there were also a number of patients whose follow-up was less than the mean time for recurrence.
Children with CP have increased muscle tone and spasticity, which prevents them from having full (hip, knee) range of motion during gait, which results in reduced stride length and velocity. As mentioned before, patients treated by subtalar fusion were more severely involved than the calcaneal lengthening group. The primary goal of foot correction in CP patients with planovalgus deformity is to improve stance phase stability. In some children, improving stance stability does improve the velocity; however, in others, it may reduce the velocity, since the child is not in a falling gait posture.
When CP patients are starting to lose function, typically at the adolescent growth spurt, a full workup with full three-dimensional gait analysis is performed to assess all deformities that may impact the gait and to plan for the surgery. There is a group of children, though, who have only collapse of the foot that is causing the problem. Spastic patients with planovalgus foot deformity may have other related pathologies which require correction (hamstring lengthening, rectus transfer, tibial rotational osteotomy, or femoral derotational osteotomy). Each of these pathologies affects the pattern of the gait (crouched, intoeing, stiff knee) and were observed more often in the subtalar fusion group. It is very important to recognize that the results of most of the patients reported in this study were not isolated planovalgus foot corrections, but were single-stage multilevel correction of all the deformities identified by gait analysis. Multilevel surgery is efficient and gives improvement in gait abilities in children with CP [20]. This will prevent secondary deforming factors which had already contributed to the primary deformity.
In spite of the strength of this study, there were a few limitations. First, as a retrospective design, there is a possibility of information and selection bias. However, we rechecked the data on the parameters used in this study from the medical records. Second, as preexisting data, our study might have been influenced by unmeasured confounding factors, despite the use of a multivariable model. Additionally, there was a recognized bias in terms of patient selection for surgery, as patients with severe preoperative foot deformity and more severe disability had been treated with subtalar fusion; therefore, it was difficult to compare the relative effectiveness of subtalar fusion and calcaneal lengthening. Also, interpreting the last follow-up as being the final outcome of the initial surgery might be confounding, considering those patients with recurrence (the need for another correcting procedure). Finally, insufficient power affected the assessment of the predictors of recurrence, given that we studied a small sample of patients with recurrence (n = 12).
In conclusion, both calcaneal lengthening and subtalar fusion are effective in treating planovalgus deformity. Calcaneal lengthening is recommended in CP patients with good ambulatory function, since it preserves joint motion, while subtalar fusion is recommended in poor ambulatory CP patients who usually present with more severe deformities and provides long-term stability. There has to be careful consideration to complete midfoot correction, especially medial column correction, as this oversight was a major cause of recurrence. Foot reconstruction surgery is not recommended in younger patients, as it is related with high recurrence rates; however, a better outcome can be expected if the deformity is not as severe.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Acknowledgments
Conflict of interest
None.
Source of funding
No financial support was given for this study.
References
- 1.O’Connell PA, D’Souza L, Dudeney S, Stephens M. Foot deformities in children with cerebral palsy. J Pediatr Orthop. 1998;18:743–747. [PubMed] [Google Scholar]
- 2.Bennet GC, Rang M, Jones D. Varus and valgus deformities of the foot in cerebral palsy. Dev Med Child Neurol. 1982;24:499–503. doi: 10.1111/j.1469-8749.1982.tb13656.x. [DOI] [PubMed] [Google Scholar]
- 3.Herring JA. Section III: neuromuscular disorders. Chapter 25: disorders of the brain. In: Herring JA, editor. Tachdjian’s pediatric orthopedics. 4. Philadelphia: Saunders Elsevier; 2008. pp. 1275–1404. [Google Scholar]
- 4.Miller F. Knee, leg, and foot. In: Miller F, editor. Cerebral palsy. New York: Springer; 2005. pp. 667–804. [Google Scholar]
- 5.Miller F. Gait. In: Miller F, editor. Cerebral palsy. New York: Springer; 2005. pp. 251–386. [Google Scholar]
- 6.Miller F. Surgical techniques. In: Miller F, editor. Cerebral palsy. New York: Springer; 2005. pp. 865–1024. [Google Scholar]
- 7.Senaran H, Yilmaz G, Nagai MK, Thacker M, Dabney KW, Miller F. Subtalar fusion in cerebral palsy patients: results of a new technique using corticocancellous allograft. J Pediatr Orthop. 2011;31:205–210. doi: 10.1097/BPO.0b013e3182092988. [DOI] [PubMed] [Google Scholar]
- 8.Kuczmarski RJ, Ogden CL, Grummer-Strawn LM, Flegal KM, Guo SS, Wei R, Mei Z, Curtin LR, Roche AF, Johnson CL. CDC growth charts: United States. Adv Data. 2000;314:1–27. [PubMed] [Google Scholar]
- 9.Palisano R, Rosenbaum P, Walter S, Russell D, Wood E, Galuppi B. Development and reliability of a system to classify gross motor function in children with cerebral palsy. Dev Med Child Neurol. 1997;39:214–223. doi: 10.1111/j.1469-8749.1997.tb07414.x. [DOI] [PubMed] [Google Scholar]
- 10.Bowen TR, Miller F, Castagno P, Richards J, Lipton G. A method of dynamic foot-pressure measurement for the evaluation of pediatric orthopaedic foot deformities. J Pediatr Orthop. 1998;18:789–793. [PubMed] [Google Scholar]
- 11.Vanderwilde R, Staheli LT, Chew DE, Malagon V. Measurements on radiographs of the foot in normal infants and children. J Bone Joint Surg Am. 1988;70:407–415. [PubMed] [Google Scholar]
- 12.Hosmer DW, Lemeshow S. Applied logistic regression. 2. New York: Wiley; 2000. pp. 91–142. [Google Scholar]
- 13.Dogan A, Zorer G, Mumcuoglu EI, Akman EY. A comparison of two different techniques in the surgical treatment of flexible pes planovalgus: calcaneal lengthening and extra-articular subtalar arthrodesis. J Pediatr Orthop B. 2009;18:167–175. doi: 10.1097/BPB.0b013e32832c2f32. [DOI] [PubMed] [Google Scholar]
- 14.Yoon HK, Park KB, Roh JY, Park HW, Chi HJ, Kim HW. Extraarticular subtalar arthrodesis for pes planovalgus: an interim result of 50 feet in patients with spastic diplegia. Clin Orthop Surg. 2010;2:13–21. doi: 10.4055/cios.2010.2.1.13. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Park KB, Park HW, Lee KS, Joo SY, Kim HW. Changes in dynamic foot pressure after surgical treatment of valgus deformity of the hindfoot in cerebral palsy. J Bone Joint Surg Am. 2008;90:1712–1721. doi: 10.2106/JBJS.G.00792. [DOI] [PubMed] [Google Scholar]
- 16.Mosca VS. Calcaneal lengthening for valgus deformity of the hindfoot. Results in children who had severe, symptomatic flatfoot and skewfoot. J Bone Joint Surg Am. 1995;77:500–512. doi: 10.2106/00004623-199504000-00002. [DOI] [PubMed] [Google Scholar]
- 17.Turriago CA, Arbeláez MF, Becerra LC. Talonavicular joint arthrodesis for the treatment of pes planus valgus in older children and adolescents with cerebral palsy. J Child Orthop. 2009;3:179–183. doi: 10.1007/s11832-009-0168-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Nather A, Fulford GE, Stewart K. Treatment of valgus hindfoot in cerebral palsy by peroneus brevis lengthening. Dev Med Child Neurol. 1984;26:335–340. doi: 10.1111/j.1469-8749.1984.tb04450.x. [DOI] [PubMed] [Google Scholar]
- 19.Bleck EE. Orthopedic management in cerebral palsy. Oxford: MacKeith Press; 1987. [Google Scholar]
- 20.Gannotti ME, Gorton GE, 3rd, Nahorniak MT, Masso PD. Walking abilities of young adults with cerebral palsy: changes after multilevel surgery and adolescence. Gait Posture. 2010;32:46–52. doi: 10.1016/j.gaitpost.2010.03.002. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.


