Abstract
Background
Despite being found with increasing frequency on esophageal biopsies, the clinical significance of lymphocytic esophagitis (LE) remains poorly understood.
Goals
The primary aim of our study was to characterize the clinical presentation and natural history of LE among adult patients.
Study
We retrospectively reviewed records for all 81 adult patients at the University of Michigan Medical Center who had a histopathological diagnosis of LE between January 1998 and November 2009. Patient demographics, clinical history, laboratory data, and imaging results from the time of diagnosis were obtained through review of computerized medical records. A telephone survey was conducted to collect natural history data.
Results
The number of LE diagnoses increased over time, with 81.5% (n=66) of patients being diagnosed in the last three years. The most frequent symptoms at the time of presentation were dysphagia (n=54), chest/abdominal pain (n=36), and heartburn (n=38). The majority (58.6%) of patients reported improvement in their initial gastrointestinal symptoms – most commonly associated with initiation of a proton pump inhibitor. Upon follow-up, most patients reported a good quality of life and satisfaction with their current health status.
Conclusions
Lymphocytic esophagitis is a new clinical entity with an increasing incidence. LE appears to have a benign natural history, with most patients reporting an improvement in symptoms and satisfaction with their health-related quality of life. Prospective studies are needed to better characterize the natural history and potential treatments for this clinical entity.
Keywords: Lymphocytic esophagitis, epidemiology, clinical presentation, natural history, quality of life
INTRODUCTION
Lymphocytic esophagitis (LE) is characterized by an increased number of intraepithelial lymphocytes without associated intraepithelial granulocytosis in esophageal tissue(1). Despite being identified with increasing frequency on esophageal biopsies, the clinical significance of this entity remains poorly understood.
Rubio and colleagues were the first to characterize the clinical presentation of LE(1). They compared 20 patients with LE (9 adult and 11 pediatric patients) to 61 patients with other forms of esophagitis characterized by an increase in both lymphocytes and granulocytes. Although they reported an association between LE and Crohns disease, this finding was primarily limited to the pediatric patients, with only 1 of the 9 adults with LE having inflammatory bowel disease (IBD).
A subsequent study by Purdy et al compared 42 patients with LE (34 adult and 8 pediatric patients) to 34 patients with esophageal biopsies for other reasons(2). They found a trend toward a higher rate of Crohn’s disease in patients with LE (12% vs. 3%, p=0.15) but this was not statistically significant. They otherwise found a trend toward higher rates of H. pylori gastritis (10% vs. 0%, p=0.06) but no differences in rates of GERD, dysphagia, or endoscopic findings.
These two studies have provided a starting point for further investigation of the clinical significance of LE but both were limited by a small sample size, particularly of adult patients. Furthermore, neither study examined the long-term natural history of LE or its response to therapies. Given the increasing recognition of LE, this is an area that deserves further attention. Therefore, the aim of our study was to characterize the clinical presentation and natural history of LE among adult patients.
MATERIALS AND METHODS
Patient Selection
We retrospectively reviewed records for all adult patients at the University of Michigan Medical Center who had a histopathological diagnosis of LE between January 1998 and November 2009. Patients were initially identified through review of all patients with esophageal biopsies over this time period, and only those that satisfied the criteria established by Rubio et al and Purdy et al were included (1). Specifically, the biopsies must have had a high number of intra-epithelial lymphocytes (at least greater than 20 lymphocytes) but no more than rare neutrophils and eosinophils. None of the patients had a sufficient number of eosinophils in their esophageal to meet the diagnostic criteria for eosinophilic esophagitis. This study was approved by the Institutional Review Board of the University of Michigan.
Data Collection
Patient demographics, clinical history, laboratory data, and imaging results from the time of diagnosis were obtained through review of computerized medical records. We recorded clinical symptoms at presentation, past medical history (including a history of inflammatory bowel disease, allergies, asthma, and GERD), and any medications the patient reported taking at the time. Laboratory data of interest included white blood cell count (WBC) and differential, platelet count, creatinine, albumin, aspartate aminotransferase (AST), alanine aminotransferase (ALT), bilirubin, and erythrocyte sedimentation rate (ESR). We recorded the endoscopic appearance of the esophagus, including the presence of erythema, esophagitis, strictures, rings, furrows, or ulcerations from the original endoscopy reports. Finally, findings from any imaging studies, including CT scans or barium studies, performed within 3 months of the index upper endoscopy were also recorded.
Survey Development and Administration
We conducted a telephone survey to help establish the natural history of LE. For patients who could not be reached initially, we made three repeat attempts to contact them. The survey was administered by one author (S.C.), and responses were recorded on a standardized abstraction sheet. The survey was adapted from previously validated surveys when available (3). The survey was divided into four sections: clinical history, symptomatology, natural history, and quality of life. The clinical history section confirmed the patient’s past medical history, medications, allergies, alcohol and tobacco use, and any family history of esophageal diseases. The symptomatology section assessed the presence of any current or past esophageal symptoms including dysphagia, odynophagia, chest pain, heartburn, nausea, vomiting, or cough. The section regarding disease natural history included questions regarding any change in upper GI symptoms, any new medications, the number of ER visits, number of hospitalizations, and findings of any subsequent upper endoscopies. Finally, quality of life was assessed using questions adapted from the SF-12 (3). The Social Security Death File and the State of Michigan Death Records were utilized to ascertain date of deaths for patients we were unable to contact.
RESULTS
Patient Characteristics
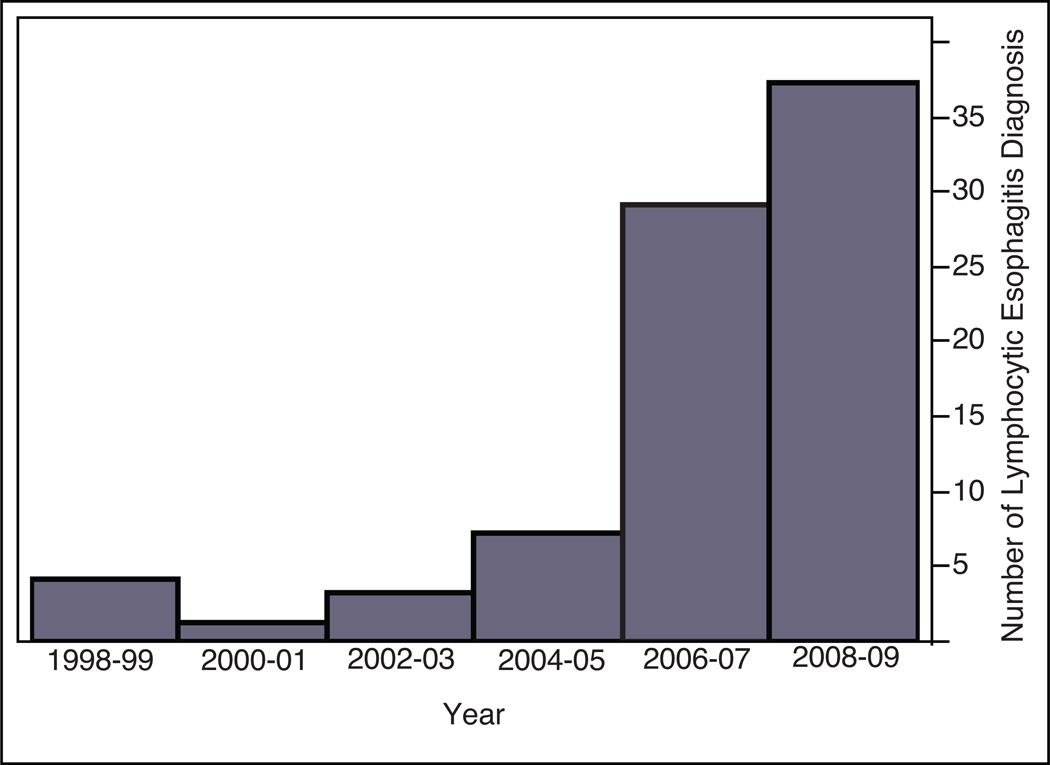
There were 81 patients diagnosed with LE between January 1998 and November 2009 (Table 1). The number of LE diagnoses increased over time, with five (6.2%) patients being diagnosed between 1998–2001, ten (12.3%) patients between 2002–2005, and 66 (81.5%) patients diagnosed between 2006–2009. The median age of the patients was 51 years (range 19–84), with the highest frequency in the 5th (24.7%)and 6th deciles (27.2%) of life. Eighty-six percent (n=69) of the patients were Caucasian and 54% (n=44) were female. The most common associated conditions were GERD (n=40), hypothyroidism (n=28), and inflammatory bowel disease (n=11). Seasonal or food allergies were reported in 13.6% (n=11) of patients and asthma in 14.8% (n=12) of patients, although most patients did not have a history of any allergic diseases. The median white blood cell count was 7.9 (range 2.7–13), with a median peripheral lymphocyte count of 1.9 (range 0.6–4.5). The majority of the patients appeared to have normal renal and liver function, with a median creatinine of 0.9 and a median bilirubin of 0.4.
Table 1.
Baseline Patient Characteristics
| Variable | All patients (n=81) |
|---|---|
| Age | 51 (19–84) |
| Gender (% male) | 37 (45.7%) |
| Race (% Caucasian) | 69 (85.2%) |
| History of GERD | 40 (49.4%) |
| History of achalasia | 4 (4.9%) |
| History of allergies | 11 (13.6%) |
| History of asthma | 12 (14.8%) |
| History of eczema | 1 (1.2%) |
| History of IBD | 11 (13.6%) |
| History of hypothyroidism | 28 (34.6%) |
| History of alcohol use | 26 (32.1%) |
| History of tobacco use | 24 (29.6%) |
| WBC | 7.9 (2.7–13) |
| Peripheral lymphocyte count | 1.9 (0.6–4.5) |
Clinical Presentation
Data on clinical symptoms and presentation are found in Table 2. The most frequent symptom at the time of presentation was dysphagia (n=54), although chest/abdominal pain (n=36), heartburn (n=38), nausea (n=24) and odynophagia (n=10) were also frequently reported.
Table 2.
Clinical, Endoscopic and Imaging Findings in patients with Lymphocytic Esophagitis
| Variable | All patients (n=81) |
|---|---|
| Predominant Clinical Symptoms at Diagnosis | |
| Dysphagia | 54 (66.7%) |
| Heartburn | 38 (46.9%) |
| Abdominal/chest pain | 36 (44.4%) |
| Nausea/vomiting | 24 (29.6%) |
| Odynophagia | 10 (12.3%) |
| Esophageal Endoscopic Findings | |
| Normal | 24 (29.6%) |
| Rings | 16 (19.8%) |
| Esophagitis | 13 (16.0%) |
| Stricture | 7 (8.6%) |
| Erythema | 4 (4.9%) |
| Nodularity | 3 (3.7%) |
| Esophageal dilation performed | 24 (29.6%) |
The esophageal mucosa was regarded as being normal in 29.6% (n=24) of patients, although five of these patients appeared to have a hypertonic lower esophageal sphincter, dilated lower esophagus, or other findings to suggest abnormal esophageal motility. The most frequent endoscopic findings were esophageal rings (n=16), esophagitis (n=13), and esophageal strictures (n=7). Less common endoscopic findings included erythema (n=4), nodularity (n=3), plaques (n=2), furrows (n=1), and webs (n=1). Esophageal dilation was performed for dysphagia in 24 patients, of whom nine had esophageal rings, five had a documented stricture, five had retained food, and five had a normal-appearing esophagus.
Lymphocytic esophagitis was diagnosed by random esophageal biopsies in 91.4% (n=74) of patients, whereas it was found on biopsies directed at abnormal mucosa or a stricture in 7 patients. Of those with random biopsies, 18.9% (n=14) had biopsies taken from the distal and mid esophagus (as recommended to diagnose eosinophilic esophagitis), 31.1% (n=23) had biopsies taken from the distal or mid esophagus, and 50% (n=37) had random biopsies throughout the esophagus. The median number of esophageal biopsies was 4 pieces (range 1–18), with most (59.5%) patients having 2–4 biopsies.
Barium esophagram had been performed within three months of LE diagnosis in 21 patients. Findings confirmed achalasia in three patients, whereas another five patients had non-specific esophageal dysmotility, five patients had findings consistent with esophageal reflux, and three patients had a mild stricture not seen on upper endoscopy. Of the six patients with a CT scan within three months of diagnosis, three patients had esophageal wall thickening.
Natural History
After a median follow-up of 3.3 years, 70 (86.4%) of the 81 patients were still alive. Surveys were conducted in 29 (41.4%) patients to obtain natural history data (Tables 3 and 4). Three-fourths of these patients (n=22) had an emergency room visit in the past five years, of which 41% (n=9) was related to a primary gastrointestinal complaint. The most common symptoms leading to ER presentation were dysphagia (n=4) and chest pain (n=2). Nearly 50% of patients (n=14) reported a hospitalization in the past five years, of which four were related to gastrointestinal symptoms (dysphagia, odynophagia, chest pain, and gastrointestinal bleeding).
Table 3.
Natural History of patients with Lymphocytic Esophagitis
| Variable | All patients (n=29) |
|---|---|
| Clinical Symptoms upon Follow-up | |
| Any GI symptoms | 28 (96.5%) |
| Dysphagia | 16 (55.2%) |
| Heartburn | 16 (55.2%) |
| Chest pain | 11 (37.9%) |
| Odynophagia | 10 (34.5%) |
| Nausea/vomiting | 9 (31.0%) |
| Emergency room visits in past 5 years | |
| Overall | 22 (75.9%) |
| Any GI symptoms | 9 (31.0%) |
| Dysphagia | 4 (13.8%) |
| Odynophagia | 1 (3.4%) |
| Nausea/vomiting | 1 (3.4%) |
| Chest pain | 2 (6.9%) |
| GI bleeding | 1 (3.4%) |
| Hospitalization in past 5 years | |
| Overall | 14 (48.3%) |
| Any GI symptoms | 4 (13.8%) |
| Dysphagia | 1 (3.4%) |
| Odynophagia | 1 (3.4%) |
| Chest pain | 1 (3.4%) |
| GI bleeding | 1 (3.4%) |
| Quality of Life | |
| Overall Health Status Poor Fair Good Very Good Excellent |
2 (6.9%) 7 (24.1%) 7 (24.1%) 11 (37.9%) 2 (6.9%) |
| GI symptoms interfere with daily activities in past month | 12 (41.4%) |
| Reported getting sick easier than others | 8 (27.6%) |
| Reported as healthy as others | 16 (55.2%) |
| Satisfaction with care for GI symptoms | 23 (79.3%) |
| Satisfied with current state of GI health | 19 (65.5%) |
Table 4.
Natural History of patients with Lymphocytic Esophagitis
| Symptom | Resolution (#) | Improvement (#) | No change(#) | Worsening (#) | Never (#) |
|---|---|---|---|---|---|
| Dysphagia | 3 | 10 | 5 | 2 | 8 |
| Odynophagia | 1 | 4 | 3 | 3 | 17 |
| Chest pain | 3 | 1 | 8 | 2 | 14 |
| Heart burn | 7 | 3 | 8 | 6 | 4 |
| Nausea/vomiting | 3 | 4 | 1 | 4 | 16 |
| Coughing | 5 | 0 | 6 | 3 | 14 |
Overall, 58.6% (n=17) of patients reported improvement in their initial gastrointestinal symptoms (Table 4). Patients reported their improvement was related to escalation of medical management in 70.6% (n=12) of cases – most commonly with a proton pump inhibitor (n=7). Three of the eleven patients with a history of IBD were started on an anti-TNF agent and reported improvement in their GI symptoms. The highest rates of symptomatic improvement were seen in patients with dysphagia and the lowest rates were seen in patients with chest pain. Of the 20 patients who initially presented with dysphagia, thirteen (65.0%) reported improvement or resolution of their dysphagia, five (25.0%) reported stable disease, and three (15%) patients reported progression of their dysphagia. Of those who improved, 5 patients had undergone esophageal dilation and 3 patients had been started on PPI therapy.
Follow-up upper endoscopy had been performed in 22 patients, of whom nine had documented LE on repeat biopsies. Nine patients had other forms of esophagitis, such as reflux and/or Candida esophagitis, and one patient had Crohns disease. Two patients had normal esophageal biopsies and one patient did not have any esophageal biopsies on follow-up upper endoscopy.
Quality of Life
The majority of patients reported that are satisfied with their health status, with 7 (24.1%) patients reporting a good quality of life and 13 (44.8%) patients reporting a very good or excellent quality of life (Table 3). Only 31% (n=9) of patients reported that they have a fair or poor quality of life. Over 50% (n=16) of patients reported they feel as healthy as other people, with only 28% (n=8) of patients thinking they are more susceptible to getting sick than other people. Over 60% of patients (n=19) reported being satisfied with the current state of their gastrointestinal health, and nearly 80% (n=23) reported being satisfied with the medical care they are receiving for their gastrointestinal symptoms.
DISCUSSION
Lymphocytic esophagitis is a newly described histologic entity with an increasing number of diagnoses over the past several years. In our study of 81 adult patients, the largest cohort with LE reported to date, 80% of diagnoses occurred in the last three years. The most common symptom at the time of presentation was dysphagia, although a substantial portion of patients also had chest or abdominal pain, heartburn and nausea. The majority of patients had an improvement in their symptoms over time and reported satisfaction with their health status.
We found that the number of LE diagnoses have dramatically increased over time, with a majority of our patients being diagnosed in the last three years of the study period. This increase in the number of cases may represent a true increase in incidence or may simply be an artifact from the increased number of esophageal biopsies taken due to concerns of eosinophilic esophagitis, as well as an increased recognition of this entity by our pathologists. Although confirmation of an increasing incidence of LE in other centers is necessary, this finding in our study suggests that further attention should be paid to this potentially important clinical entity.
Compared to reports of eosinophilic esophagitis from the literature (4, 5), patients with LE had similar rates of dysphagia (66.7% vs 70.1%) but substantially lower rates of food impaction (6.2% vs. 12.3%). This was also recently reported in another cohort of 34 adult patients with LE, of whom 67.7% had dysphagia (6). Although our study highlights the likely association between LE and dysphagia, we are unable to establish a causal relationship given the observational nature of our study. Alternatively, the association between LE and dysphagia could be related to moderating factors, such as GERD, or mediating factors, such as stasis of esophageal contents.
Similar to patients with eosinophilic esophagitis, a substantial portion of patients had histologic evidence of LE despite having a normal endoscopic appearance (29.6% in our cohort vs. 24.8% in EE patients) (4). We also found similar rates of esophageal rings (19.8% vs. 18.8%) but substantially lower rates of esophageal strictures (8.6% vs. 16.3%) (4). Given the overlap in symptomatology and presentation with eosinophilic esophagitis, many patients with possible LE will already have random biopsies taken from the lower, mid and upper esophagus. However, our study suggests that since these clinical entities may differ, pathologists should look for and report any findings of LE, in addition to eosinophilic esophagitis.
Our study is also the first to report that natural history of patients with lymphocytic esopahagitis. After a median follow-up of 3.3 years, nearly 90% of patients were still alive. We found that most patients reported a good quality of life and satisfaction with their medical care. Furthermore, most patients had an improvement in their symptoms associated with an escalation in medical therapy, most commonly with a proton pump inhibitor (PPI). It is unclear if PPI therapy resulted in symptom improvement due to treatment of patients’ LE or if this was related to treatment of concomitant GERD. Although a few patients (with underlying IBD) had been treated with anti-TNF agents with a good response, available data do not support a causal relationship between LE and IBD. Trials of other agents, such as topical steroids, were not reported in our cohort but deserve further study.
Despite most patients having improvement in their symptoms, a subset of patients with LE still had high resource utilization on follow-up, with one-third having an ER visit for a GI complaint and nearly 20% having a recent hospitalization for GI symptoms. The variability in natural history of LE may be related to differential response rates to therapies, such as PPIs among these patients. Alternatively, it has been suggested that LE may also be a common non-specific pathway for several pathogenic stimuli and these patients may truly have different underlying diseases. Further prospective and case-control studies are necessary to establish a causal relationship between LE and clinical symptoms, better characterize the natural history of LE, and evaluate its response to therapies.
There were a high proportion of patients with Crohns disease in prior pediatric cohort studies of LE, with nearly 40% of children with LE having associated IBD in the study by Rubio et al (1). This finding has not been replicated in adults, with only 13.6% of our patients having IBD. Even lower rates of IBD (5.9%) were reported in a prior case series of 34 adult patients with LE from Caris Diagnostics (6).
Based on available data, including this study, it remains unclear whether LE is a true independent clinical entity or simply a marker of another disease process. Given it’s histologic resemblance to contact dermatitis, Purdy et al previously postulated that LE may be a common pathway for a response to a variety of pathogenic stimuli (2). Several conditions associated with LE in our study could potentially cause esophageal injury via stasis and/or regurgitation – dysphagia, GERD, achalasia, and esophageal dysmotility. Further large multi-center studies are necessary to determine if LE is an independent clinical entity, causing dysphagia and GERD symptoms, or if it is a non-specific response to multiple forms of esophageal injury.
Although this is the largest cohort of patients with LE, our study had several limitations. It was performed in a single, tertiary-care institution, which can introduce a selection bias because of referral patterns and therefore make the results less generalizable. Our results also require confirmation in other centers to rule out the possibility that our findings may be an artifact of increased recognition of this entity by our pathologists or an increased number of esophageal biopsies taken over time. Additionally, our study may under-sample asymptomatic patients with lymphocytic esopahagitis as they would be less likely to have an upper endoscopy and/or esophageal biopsies. Third, we were only able to collect natural history data on one-third of our cohort, although this response rate is similar to other patient survey studies in the literature. Furthermore, as stated above, our study was unable to determine if LE is a true independent clinical entity or a non-specific response to multiple forms of esophageal injury. Finally, the retrospective nature of this study can lead to missing or inaccurate data, particularly with regard to clinical presentation. We attempted to adjust for this limitation by confirming initial symptoms and clinical history during the survey portion of our study. Overall, we feel that the limitations of our study are outweighed by its notable strengths, including the fact that this is the largest cohort of adult patients with LE reported to date, the first to report its increasing frequency, and the first study to describe the natural history of LE.
In conclusion, lymphocytic esophagitis is a newly described clinical entity with an increasing number of diagnoses over time. Patients with LE have similar rates of dysphagia as those seen in eosinophilic esophagitis but do not typically present with food impaction. Although LE is associated with high resource utilization including frequent ER visits and hospitalizations, it appears to have a benign natural history, with low mortality rates and high rates of symptomatic improvement. Given the increasing frequency of LE diagnoses, further prospective studies are needed to better characterize its natural history and potential treatments for this clinical entity.
Figure 1.
Incidence of Lymphocytic Esophagitis
Acknowledgments
Declaration of Funding Sources: Dr. Singal’s research is supported by grant KL2 RR024983-04 and UL1 RR024982. Dr. Elmunzer’s and Dr. Waljee’s research is supported by grant UL1RR024986 from the National Center for Research Resources (NCRR). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NCRR, or the National Institutes of Health.
Footnotes
Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
Conflicts of Interest: None of the authors have any financial interests or conflicts of interest with the subject matter discussed in this manuscript.
Author Contributions: All of the listed authors have made substantial contributions to the conception and design of the study, acquisition of data and/or analysis and interpretation of the data, drafting of the manuscript, and final approval of the version to be submitted.
REFERENCES
- 1.Rubio CA, Sjodahl K, Lagergren J. Lymphocytic esophagitis: a histologic subset of chronic esophagitis. Am J Clin Pathol. 2006 Mar;125(3):432–437. [PubMed] [Google Scholar]
- 2.Purdy JK, Appelman HD, Golembeski CP, McKenna BJ. Lymphocytic esophagitis: a chronic or recurring pattern of esophagitis resembling allergic contact dermatitis. Am J Clin Pathol. 2008 Oct;130(4):508–513. doi: 10.1309/D3PCF6D6YYMQRX9A. [DOI] [PubMed] [Google Scholar]
- 3.Ware J, Jr., Kosinski M, Keller SD. A 12-Item Short-Form Health Survey: construction of scales and preliminary tests of reliability and validity. Med Care. 1996 Mar;34(3):220–233. doi: 10.1097/00005650-199603000-00003. [DOI] [PubMed] [Google Scholar]
- 4.Muller S, Puhl S, Vieth M, Stolte M. Analysis of symptoms and endoscopic findings in 117 patients with histological diagnoses of eosinophilic esophagitis. Endoscopy. 2007 Apr;39(4):339–344. doi: 10.1055/s-2007-966216. [DOI] [PubMed] [Google Scholar]
- 5.Straumann A, Spichtin HP, Grize L, Bucher KA, Beglinger C, Simon HU. Natural history of primary eosinophilic esophagitis: a follow-up of 30 adult patients for up to 11.5 years. Gastroenterology. 2003 Dec;125(6):1660–1669. doi: 10.1053/j.gastro.2003.09.024. [DOI] [PubMed] [Google Scholar]
- 6.Haque S, Genta RM. Lymphocytic Esophagitis: A Real Condition in Search of Clinicopathologic Criteria. New Orleans: Digestive Disease Weekly; 2010. [Google Scholar]