Abstract
The aim of this study was to evaluate psychometric properties and clinical correlates of the Weight Bias Internalization Scale (WBIS) in a sample of obese adolescents seeking bariatric surgery. Sixty five adolescents enrolled in a bariatric surgery program at a large, urban medical center completed psychiatric evaluations, self-report questionnaires including the WBIS and other measures of psychopathology and physical assessments. The WBIS had high internal consistency (Cronbach’s α = .92). As in previous research with adults, the one underlying factor structure was replicated and 10 of the original 11 items were retained. The scale had significant partial correlations with depression (r = .519), anxiety (r = .465), social and behavioral problems (r = .364), quality of life (r = −.480), and eating (r = .579), shape (r = .815), and weight concerns (r = .545), controlling for body mass index. However, WBIS scores did not predict current or past psychiatric diagnosis or treatment or past suicidal ideation. Overall, the WBIS had excellent psychometric properties in a sample of obese treatment-seeking adolescents and correlated significantly with levels of psychopathology. These findings suggest that the WBIS could be a useful tool for healthcare providers to assess internalized weight bias among treatment-seeking obese youth. Assessment of internalized weight bias among this clinical population has the potential to identify adolescents who may benefit from information on coping with weight stigma which in turn can augment weight loss efforts.
Keywords: Adolescents, Weight Bias, Stigma, Obesity, Bariatric Surgery
Public health concerns regarding the high prevalence of obesity among children and adults worldwide often stem from the health and financial costs associated with obesity’s medical sequelae. (1–3) However, obesity is also associated with a host of deleterious psychosocial consequences including psychiatric diagnoses, mood disturbances, binge eating and decreased self-esteem and quality of life. (3–6) While little is known about the mechanisms linking obesity with psychological problems, one possibility is that this relationship is partially explained by the experience of weight bias.
The incidence of weight-based discrimination has increased by 66% since 1995 (7), and is now on par with rates of racial discrimination.(8) Further, weight bias is more socially acceptable than other common forms of bias such as racism or sexism, and is observed in multiple domains, including employment, education, housing opportunities, health care, and portrayal in the media. (9) The widespread social acceptability of weight bias, as illustrated by its ubiquity in the media and lack of preventative legislation, (9) contributes to strong anti-fat attitudes expressed by non-overweight as well as overweight and obese people.(10) Such anti-fat attitudes have also been shown among overweight children (11) and weight bias directed towards obese children has increased over the last several decades, (12) with stigmatizing attitudes beginning as early as preschool.(13) In fact, Latner and Stunkard found that elementary-school aged youth would rather befriend an individual with various physical disabilities, such as facial disfigurement, than an obese peer.(12) Overweight and obese individuals report experiences of peer rejection and harassment in every phase of education, from elementary school through high school and college.(14)
Research demonstrates that youth who have experienced weight-based stigmatization and teasing have increased risk of depression, low self-esteem, body dissatisfaction, suicidality, unhealthy weight control behaviors, and disordered eating.(11) Importantly, many of these studies control for body mass index (BMI), indicating that the stigmatizing experience itself, rather than body weight, is contributing to these adverse psychological outcomes.
While many minorities or stigmatized groups tend to demonstrate ‘in-group’ preferences (15), the extant literature has found that overweight and obese individuals lack these favorable ‘in-group’ attitudes. In fact, overweight and obese persons endorse similarly high anti-fat attitudes as their normal weight counterparts.(10) The lack of favorable ‘in-group’ attitudes observed in overweight and obese individuals may be a result of the widespread social acceptability and prevalence of weight bias. This may partially explain why overweight individuals are especially likely to internalize negative weight-based stereotypes.(16,17)
While antifat attitudes are pervasive in American society, Durso and Latner (18) argue that various measures used to assess antifat attitudes among overweight and non-overweight individuals fail to distinguish between weight bias and the internalization of that bias. Therefore, Durso and Latner (18) developed the Weight Bias Internalization Scale (WBIS) to separate weight-based attributions made about “the other” from weight-based attributions made about “the self.” The authors suggest that attributions about one’s self, which reflect the internalization of weight bias, rather than just the presence of antifat attitudes, is an important contributing factor to negative psychological outcomes among overweight or obese individuals. The distinction between perceptions of the attitudes of others and attitudes toward one’s group is a critical one for understanding responses to stigma. With respect to racial and ethnic bias, for example, Crocker et al. found that whereas perceptions of others’ attitudes were not consistently related to well-being, members of racial and ethnic minority groups who personally held their group in lower esteem systematically experience lower levels of personal well being. (19)
In their initial study of the WBIS, Durso and Latner (18) demonstrated excellent reliability and validity of the scale based on an internet community sample of overweight and obese adults. In addition, the scale showed strong partial correlations with self-esteem, eating disturbances, depression, and anxiety while controlling for body mass index (BMI). Furthermore, they demonstrated that the WBIS was able to explain variance in measures of psychopathology and self-esteem beyond other measures of explicit antifat attitudes as well as BMI which were not found to be associated with those psychological measures.
Given that youth are particularly vulnerable to weight stigma (20), and disordered eating patterns and mood disturbances frequently emerge during adolescence (21–23), it is critical to explore the impact of internalized weight stigma on the psychological well-being of obese adolescents. To our knowledge, no studies have explored weight bias internalization using the WBIS in obese youth. Thus, the goal of the current study was to examine the psychometric properties and clinical correlates of internalized weight bias as measured by the WBIS in a sample of male and female adolescents seeking weight loss surgery. Based on Durso and Latner’s findings, (18) we hypothesized that the WBIS would exhibit good psychometric properties in a sample of severely obese youth and that internalized weight bias would be associated with greater levels of psychopathology. Specifically, we expected that higher scores on the WBIS would be associated with higher levels of depression, anxiety, general maladaptive behaviors and disordered eating behaviors and cognitions and lower quality of life. We also hypothesized that the WBIS would be positively associated with the presence of current or past psychiatric diagnoses, psychiatric treatment, and past serious suicidal ideation.
METHODS AND PROCEDURES
Participants
Participants were 65 severely obese adolescents enrolled in the Center for Adolescent Bariatric Surgery (CABS) program at the Morgan Stanley Children’s Hospital of New York Presbyterian at the Columbia University Medical Center (CUMC) between February 2006 and March 2008. Adolescents were eligible for bariatric surgery if they met the following criteria: 1) age between 14 and 18 years, 2) BMI > 40 kg/m2 or BMI > 35 kg/m2 with serious comorbid conditions (e.g., Type II diabetes, hyperlipidemia, sleep apnea); 3) long-standing severe obesity with documented attempts of weight loss for at least six months; 4) evidence of sufficient emotional maturity to comply with the study protocol; 5) appropriate contraception and not planning to become pregnant over the year following surgery; 6) absence of medical contraindications (e.g., anomalies of the gastrointestinal tract, prior gastric surgery, etc.); and 7) absence of self-induced vomiting.
Procedures
A more detailed description of the psychiatric evaluations conducted as part of the CABS program are reported elsewhere.(24) In brief, adolescent candidates and at least one parent completed a psychiatric evaluation prior to surgery that involved an interview with a psychologist or psychiatrist and completed self-report questionnaires. Written informed consent and assent were obtained prior to the evaluations and the CUMC Institutional Review Board approved this study.
Measures
Weight Bias Internalization Scale (WBIS)
(18) This 11 item self-report scale measures the degree to which a respondent believes that negative stereotypes about overweight and obese persons are applicable to him or her. Responses are measured on a 7-point Likert scale ranging from “strongly disagree” to “strongly agree.” Excellent reliability and validity of the scale was demonstrated in an internet community sample of overweight and obese participants.(18)
The Eating Disorder Examination Questionnaire (EDE-Q)
(25) This self-report questionnaire assesses the diagnostic criteria for eating disorders and other clinical symptoms. The EDE-Q captures the frequency of objective bulimic episodes (OBEs; experiencing a loss of control while consuming unusually large amounts of food), subjective bulimic episodes (SBEs; experiencing a loss of control without eating unusually large quantities of food), in addition to inappropriate compensatory behaviors (self-induced vomiting, laxative misuse, etc). The EDE-Q also generates four subscales: dietary restraint, eating concerns, weight concerns, and shape concerns. This questionnaire has adequate test-retest reliability, (26,27) good convergence with the interview-based version with various disordered-eating groups (28,29) and excellent reliability for assessing compensatory behaviors. (30)
The Beck Depression Inventory (BDI)
(31) This is a widely used, well-established measure to assess depressive symptoms and negative affect. Higher scores correspond to higher levels of depression and the scale has excellent reliability and validity.(32)
Multidimensional Anxiety Scale for Children (MASC)
(33) This 39 item self-report scale captures a range of anxiety symptoms among children and adolescents (age 8–19). The scale produces a total score and four main factors: Physical Symptoms, Social Anxiety, Harm Avoidance, and Separation Anxiety. It has demonstrated excellent internal reliability, satisfactory test-retest reliability and adequate validity.(33)
Child Behavior Checklist and Youth Self-Report (CBCL, YSR)
(34) These widely used measures capture the following eight constructs or syndromes among children and adolescents: Social Withdrawal, Somatic Complaints, Anxiety/Depression, Social Problems, Thought Problems, Attention Problems, Delinquent Behavior, and Aggressive Behavior. The CBCL is completed by the child’s parent and the YSR is completed by the child. The scale has excellent psychometric properties.(34)
Pediatric Quality of Life Inventory 4.0 (PEDS-QL)
(35) This scale, which includes child self-report and parent proxy-report scales, is a measure of health-related quality of life designed for children and adolescents ages 2 to 18. Four generic core scales (Physical, Emotional, Social and School) comprise the total 23 items which also yield an overall score. Good scale reliability and validity has been demonstrated in both healthy participants and those with acute or chronic conditions.(35)
Clinical Interview
Information about the age, gender, and race/ethnicity of participants was obtained by the psychiatrist or psychologist conducting the adolescent evaluation. In addition, current and past psychiatric diagnoses as well as psychological treatment history and past serious suicidal ideation were established by clinical interview.
Body Mass Index
Height and weight were measured by a member of the CABS staff and were used to calculate body mass index generated by dividing weight over meters squared (kg/m2).
Statistical Analysis
All analyses were conducted using SPSS 18.0 (SPSS, Inc., Chicago, IL). First, item-total correlations and Cronbach’s alpha were calculated followed by a factor analysis to examine the reliability and factor structure of the WBIS in this sample of obese youth. Then Pearson correlations were performed to assess clinical correlates of the WBIS. Because little research has been conducted on the WBIS in an adolescent sample these analyses were considered exploratory and not corrected for multiple comparisons. Associations between the WBIS and variables that were highly skewed were examined with Kendall’s tau correlations. Independent samples one-way ANOVAs were also conducted to examine potential differences in WBIS scores between males and females and among different racial/ethnic groups. Finally, three logistic regression analyses were conducted to evaluate relationships between the WBIS while controlling for other key clinical variables and psychiatric diagnosis, treatment history and past suicidal ideation. An alpha level of less than 0.05 was used to evaluate statistical significance and all tests were two-tailed.
RESULTS
Participant Characteristics
A total of 65 adolescents completed the WBIS and all participants were included in the factor analysis. Eight of the 65 did not complete the other measures, so were excluded from other analyses. The sample of 57 participants was composed of 11 males (19.3%) and 46 females (80.7%). The racial/ethnic distribution of the sample was: 50.9% Caucasian, 31.6% Hispanic, 12.3% African American and 5.3% identifying as Other. The mean age was 15.65 ±1.08 years and the mean BMI was 46.92±7.86 kg/m2 (range 35.90–72.30 kg/m2). Twenty seven (41.5%) adolescents met criteria for at least one current or past psychiatric diagnosis, 40 (70.2%) reported ever receiving psychiatric treatment, and 10 (17.5%) endorsed past serious suicidal ideation. Fourteen (32.6%) of the adolescents completing the EDE-Q (N = 43) reported at least one OBE during the previous month. Ten (22.73%) of the adolescents (N = 44) reported at least one SBE in the previous month.
Scale Psychometric Properties:
Test Reliability
Cronbach’s α, reflecting the internal consistency of the 11 item WBIS, was .91. Applying the same criteria as Durso and Latner, (18) we removed any items that did not achieve an item-total correlation of ≥ .40. This led to the removal of the first question (“As an overweight person, I feel that I am just as competent as anyone);” all other item-total correlations were greater than .40 [range .497–.90].
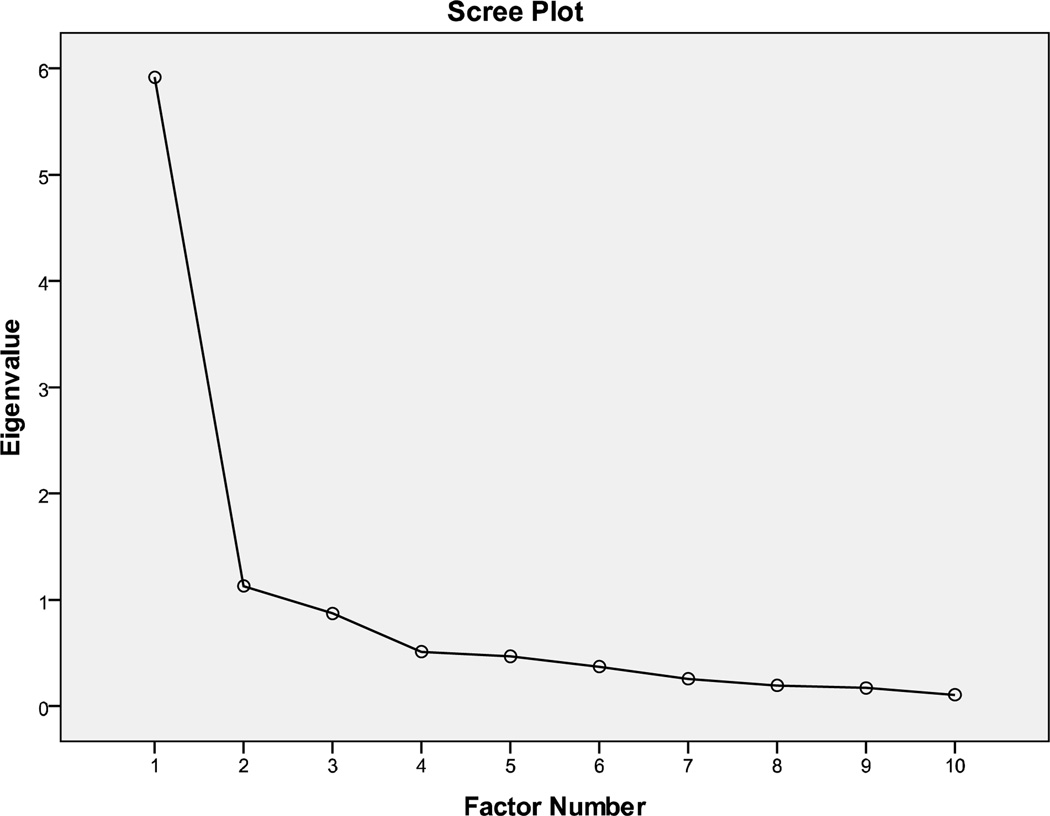
To further assess whether the items were capturing the same unitary weight bias internalization construct, we performed an exploratory factor analysis using an OBLIQUE rotation on the new 10-item scale. This factor analysis yielded two potential factors with Eigenvalues > 1. Factor 1 explained 59.2% of the variance in scores (Eigenvalue = 5.917) while Factor 2 accounted for 11.3% of the variance (Eigenvalue = 1.130). However, inspection of the Scree plot, a preferred method of identifying the number of factors, suggested that only one factor should be retained (See Figure 1). (36) The factor correlation matrix indicated that the potential factors had a correlation of −.654, confirming the appropriateness of the OBLIQUE rotation over other common approaches such as VARIMAX. (36) All items had loadings of greater than .6 with the exception of item number eight which still had a moderately good loading of .448 and item number 9 which had a loading of .398; both items were retained (See Table 2 for Factor Loadings). This final scale, comprising ten items, had a Cronbach’s α of .92.
Figure 1.
Scree Plot for Exploratory Factor Analysis using OBLIQUE Rotation for the Weight Bias Internalization Scale; 1 Factor Retained
Table 2.
Correlations and partial correlations for the Weight Bias Internalization Scale and Study Measures
| Scale | Correlation | Partial Correlationsa |
|---|---|---|
| Age (yrs) | 0.169 | 0.169 |
| Beck Depression Inventory | 0.520** | 0.519** |
| Youth Self-Report Total | 0.366** | 0.364** |
| Child Behavior Checklist Total | 0.310* | 0.307* |
| Pediatric Quality of Life -Teen Self-Report | −0.483** | −0.480** |
| Multidimensional Anxiety Scale for Children | 0.467** | 0.465**> |
| Eating Disorder Examination-Questionnaire | ||
| Restraint Subscale | −0.081 | −0.106 |
| Eating Concerns Subscale | 0.581** | 0.579** |
| Shape Concerns Subscale | 0.813** | 0.815** |
| Weight Concerns Subscale | 0.570** | 0.545** |
| Body Mass Index (kg/m2) | 0.044 |
Controlling for Body Mass Index
Correlation significant at the 0.05 level
Correlation significant at the 0.01 level
Correlations with Psychopathology
The average WBIS score was 4.29±1.52 (range: 1.5–6.6) compared to a mean of 3.95±1.28 (range: 1.33–6.50) in the Durso and Latner study (18). The item means for the WBIS (see Table 1) in this adolescent sample were similar to those observed in Durso and Latner’s adult sample.(18) Table 2 presents correlations between the WBIS average scores and measures of psychopathology. Based on Pearson correlations, age, BMI and dietary restraint as measured by the EDE-Q were not associated with WBIS scores. The WBIS was significantly positively correlated with the BDI, CBCL, YSR, MASC and the eating, shape and weight concerns subscales of the EDE-Q. The WBIS was also negatively correlated with the PEDS-QL. Partial correlations, which controlled for BMI, replicated the findings from the first correlation analyses. Because the reported number of OBEs and SBEs were significantly skewed, Kendall’s tau correlations were performed to examine the relationship between frequency of OBEs, SBEs and the WBIS. These analyses revealed a significant positive relationship between the number of OBEs (τ = 0.325, p = .007) and the WBIS, but there was no relationship between the WBIS and the number of SBEs (τ = .229, p = .061).
Table 1.
Weight Bias Internalization Scale Items and Factor Loadings
| Item No. | Scale Item | Item Mean |
Item-total correlation |
Final scale item-total correlation |
Final Scale Factor Loading |
|---|---|---|---|---|---|
| 1 | As an overweight person, I feel that I am just as competent as anyone. | 3.11 | 0.344 | ||
| 2 | I am less attractive than most other people because of my weight | 4.62 | 0.699 | .699 | 0.741 |
| 3 | I feel anxious about being overweight because of what people might think of me | 4.6 | 0.770 | .770 | 0.753 |
| 4 | I wish I could drastically change my weight | 5.65 | 0.658 | .658 | 0.690 |
| 5 | Whenever I think a lot about being overweight, I feel depressed | 4.43 | 0.904 | .904 | 0.871 |
| 6 | I hate myself for being overweight | 3.46 | 0.854 | .854 | 0.703 |
| 7 | My weight is a major way that I judge my value as a person | 3.25 | 0.812 | .812 | 0.656 |
| 8 | I don't feel that I deserve to have a really fulfilling social life, as long as I'm overweight | 2.31 | 0.633 | .633 | 0.448 |
| 9 | I am OK being the weight that I am | 5.45 | 0.497 | .497 | 0.398 |
| 10 | Because I'm overweight, I don't feel like my true self | 4.62 | 0.809 | .809 | 0.834 |
| 11 | Because of my weight, I don't understand how anyone attractive would want to date me | 4.49 | 0.896 | .896 | 0.913 |
Two independent samples one-way ANOVAs did not detect any significant differences in WBIS scores between males and females (F(1,55) = .571, p = .453, η2 = .01). There were also no significant differences among the racial/ethnic groups (F(3,53) = 2.344, p = .083, η2 = .12), though the eta-squared effect size was large.
Logistic Regression Analyses
Results from the logistic regression analyses are presented in Table 3. All predictor variables included in the analyses were mean-centered. Three logistic regression analyses were performed to examine whether BMI, BDI, MASC and the WBIS were significant predictors of 1) current or past psychiatric diagnoses; 2) any psychiatric treatment; or 3) past serious suicidal ideation. Due to the moderate sample size and concerns about multicollinearity among the psychological variables, only the BDI and MASC were included as psychological predictors in the logistic regression models along with BMI and the WBIS because they were thought to be most strongly related to psychopathology. All response variables were coded 0 or 1 to reflect the presence or absence of the variable of interest. The BDI was the only psychological variable associated with a current or past psychiatric diagnosis. None of the other variables, including the WBIS, were significantly associated with any of the three response variables.
Table 3.
Odds Ratios, 95% Confidence Intervals and P Values for Logistic Regression Analyses
|
Independent Variable |
Psychiatric Diagnosis OR (95% CI) |
P |
Psychiatric Treatment OR (95% CI) |
P |
Past Suicidal Ideation OR (95% CI) |
P |
|---|---|---|---|---|---|---|
| BMI | 1.01 (0.94,1.09) | .799 | 1.10 (0.99,1.22) | .072 | 0.95 (0.85,1.05) | .320 |
| BDI | 1.14 (1.03,1.27) | .013* | 1.01 (0.93,1.11) | .773 | 1.03 (0.93,1.15) | .541 |
| MASC | 1.00 (0.94,1.07) | .943 | 1.00 (0.94,1.07) | .992 | 1.02 (0.94,1.10) | .713 |
| WBIS | 0.89 (0.54,1.46) | .638 | 0.98 (0.59,1.61) | .921 | 0.77 (0.43,1.39) | .385 |
Significant at p <0.05
BMI: Body Mass Index; BDI: Beck Depression Inventory; MASC: Multidimensional Anxiety Scale for Children; WBIS: Weight Bias Internalization 10-item Scale
DISCUSSION
This was the first study to examine the WBIS in a sample of severely obese adolescents seeking weight loss surgery. In this sample, the WBIS had high internal consistency and the same unitary factor structure identified by Durso and Latner (18) was replicated, though one additional item was removed from the scale creating a final 10-item version. In addition, similar item means were reported in this obese adolescent sample when compared to Durso and Latner’s adult overweight and obese sample.(18) We replicated Durso and Latner’s (18) finding that the WBIS scale is positively correlated with a variety of measures of psychopathology, but not correlated with BMI. Similar to Durso and Latner, (18) there was also a significant relationship between frequency of binge eating and the WBIS, but no relationship between SBEs, which indicate a loss of control while eating a subjectively large amount of food. In addition, the WBIS correlated highly with measures of eating concerns and shape and weight concerns and did not correlate with dietary restraint. We also expanded upon Durso and Latner’s (18) work by showing that the WBIS was positively related to a measure of social problems and maladaptive behaviors and inversely related to quality of life.
Contrary to our hypotheses, the WBIS did not predict the presence of a current or past psychiatric diagnosis, receipt of psychiatric treatment or past serious suicidal ideation after controlling for BDI and MASC scores and BMI. However, with the exception of BDI predicting psychiatric diagnosis status, none of the other variables were associated with diagnosis, psychiatric treatment history or past suicidal ideation. The lack of a relationship between the psychological variables and suicidal ideation may reflect the discrepancy between assessing current psychological status and past suicidal ideation. It is also possible that pursuit of psychiatric treatment in this sample is more strongly driven by other factors like the parents and/or adolescents seeking possible explanations for severe obesity in the absence of significant psychiatric symptoms. Finally, it is possible that in anticipation of bariatric surgery, the reporting of psychological symptoms was dampened and may partially explain the lack of associations between the predictors and response variables.
This study is limited by a moderate sample size. However, the strong item factor loadings suggest the 5:1 item to factor ratio is reasonable, though replication of the factor structure in larger samples is needed.(36) While significant differences among racial/ethnic groups were not detected, a large effect size suggests that more research in larger, diverse samples is needed to adequately assess potential differences among racial/ethnic groups. While this study has several limitations, it also has a number of strengths. This is the first study to examine the WBIS in a racially/ethnically diverse obese adolescent treatment seeking sample. In addition, weight and height were obtained in person to calculate BMI, rather than relying on self-report and psychiatric disorders were assessed via clinical interview.
Future research should longitudinally follow adolescents receiving bariatric surgery to examine the relationship between internalized weight stigma and surgery outcome and assess how internalized weight stigma changes with weight loss. Similar to the results of the current study, another study of overweight and obese adults undergoing a behavioral weight loss program found that the WBIS was associated with depression, body dissatisfaction, and binge frequency at baseline. (37) Following 14 weeks of treatment, participants demonstrated decreased internalized weight bias; additionally, they reported decreased explicit anti-fat biases, depression, body image disturbance, and binge eating behaviors following the program, though the mechanisms explaining these changes are unknown and require further study in both adults and adolescents.
The current study in conjunction with existing research finds that internalized weight stigma is associated with elevated levels of psychopathology, but more work is needed to understand the ways in which the internalization of weight stigma influences behaviors and impacts long-term psychological and health outcomes among adolescents. Research suggests that adults who internalize weight bias and negative weight-based stereotypes are more likely to engage in binge-eating behaviors and are more likely to report coping with stigma by refusing to diet and consuming more food.(11) In fact, the experience of weight stigma has been shown to hinder weight loss efforts; it was associated with increased caloric intake, decreased exercise, and increased attrition in a sample of overweight and obese adults participating in a behavioral weight-loss trial.(38) However, when health care providers sensitively addressed the issue of weight stigma and appropriate coping mechanisms with overweight patients, weight loss efforts were bolstered and psychological distress was decreased. (39)
Therefore, greater efforts should be made to inform healthcare providers of the potential presence of weight bias internalization and its psychological correlates, such as depression and binge eating, among overweight and obese patients. As overweight and obese youth are particularly vulnerable to weight stigma, psychopathology, and disordered eating behaviors healthcare providers have a unique opportunity to assess and address weight bias internalization in treatment-seeking children and adolescents. The WBIS could be a helpful tool to quickly assess weight bias internalization in these clinical populations and identify patients who need support from healthcare providers to cope with weight stigma. Such efforts have the potential to increase weight loss and improve psychological health and functioning.
Acknowledgements
Christina Roberto is supported by the National Institute of Diabetes and Digestive and Kidney Diseases grant 1F31DK088523-01. Dr. Sysko is supported by National Institute of Diabetes and Digestive and Kidney Diseases grant K23DK088532.
The authors thank B. Timothy Walsh, MD, Michael J. Devlin, MD, Laura Durso, MA, Janet Latner, PhD, and members of the Center for Adolescent Bariatric Surgery team.
Footnotes
Disclosure
No authors report conflict of interest.
References
- 1.Ogden CL, Flegal KM, Carroll MD, Johnson CL. Prevalence and trends in overweight among US children and adolescents, 1999–2000. JAMA. 2002;288:1772–1773. doi: 10.1001/jama.288.14.1728. [DOI] [PubMed] [Google Scholar]
- 2.Ogden CL, Carroll MD, Flegal KM. High body mass index for age among US children and adolescents, 2003–2006. JAMA. 2008;299:2401–2405. doi: 10.1001/jama.299.20.2401. [DOI] [PubMed] [Google Scholar]
- 3.Dietz WH. Health consequences of obesity in youth: childhood predictors of adult disease. Pediatrics. 1998;101:1175–1182. [PubMed] [Google Scholar]
- 4.Isnard P, Michel G, Frelut ML, et al. Binge eating and psychopathology in severely obese adolescents. Int J Eat Disord. 2003;34:235–243. doi: 10.1002/eat.10178. [DOI] [PubMed] [Google Scholar]
- 5.Schwimmer JB, Burwinkle TM, Varni JW. Health-related quality of life of severely obese children and adolescents. JAMA. 2003;289:1813–1819. doi: 10.1001/jama.289.14.1813. [DOI] [PubMed] [Google Scholar]
- 6.Quantin L, Cortese S, Falissard B, Musher-Eizenman D, Guedeney A, Frelut ML, Mouren MC. Bulimic behaviours and psychopathology in obese adolescents and in their parents. Int J Pediatr Obes. 2010 doi: 10.3109/17477160903571987. in press. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Andreyeva T, Puhl RM, Brownell KD. Changes in perceived weight discrimination among Americans: 1995–1996 through 2004–2006. Obesity. 2008;16:1129–1134. doi: 10.1038/oby.2008.35. [DOI] [PubMed] [Google Scholar]
- 8.Puhl RM, Andreyeva T, Brownell KD. Perceptions of weight discrimination: prevalence and comparison to race and gender discrimination in America. Int J Obes. 2008;32:992–1000. doi: 10.1038/ijo.2008.22. [DOI] [PubMed] [Google Scholar]
- 9.Puhl RM, Heuer CA. The stigma of obesity: A review and update. Obesity. 2009;17:941–964. doi: 10.1038/oby.2008.636. [DOI] [PubMed] [Google Scholar]
- 10.Puhl RM, Moss-Racusin CA, Schwartz MB. Internalization of Weight Bias: Implications for Binge Eating and Emotional Well-being. Obesity. 2007;15:19–23. doi: 10.1038/oby.2007.521. [DOI] [PubMed] [Google Scholar]
- 11.Puhl RM, Latner J. Stigma, obesity, and the health of the nation’s children. Psychol Bull. 2007;133:557–580. doi: 10.1037/0033-2909.133.4.557. [DOI] [PubMed] [Google Scholar]
- 12.Latner JD, Stunkard AJ. Getting Worse: The Stigmatization of Obese Children. Obes Res. 2003;11:452–456. doi: 10.1038/oby.2003.61. [DOI] [PubMed] [Google Scholar]
- 13.Musher-Eizenman DR, Holub SC, Miller AB, Goldstein SE, Edwards-Leeper L. Body size stigmatization in preschool children: The role of control attributions. J Pediatr Psychol. 2004;29:613–620. doi: 10.1093/jpepsy/jsh063. [DOI] [PubMed] [Google Scholar]
- 14.Puhl R, Brownell KD. Bias, discrimination, and obesity. Obes Res. 2001;9:788–805. doi: 10.1038/oby.2001.108. [DOI] [PubMed] [Google Scholar]
- 15.Brewer M. In-group bias in the minimal intergroup situation: A cognitive motivational analysis. Pyschol Bull. 1979;86:307–324. [Google Scholar]
- 16.Wang SS, Brownell KD, Wadden TA. The influence of the stigma of obesity on overweight individuals. Int J Obes. 2004;28:1333–1337. doi: 10.1038/sj.ijo.0802730. [DOI] [PubMed] [Google Scholar]
- 17.Puhl RM, Moss-Racusin CA, Schwartz MB. Internalization of weight bias: Implications for binge eating and emotional well-being. Obesity. 2007;15:19–23. doi: 10.1038/oby.2007.521. [DOI] [PubMed] [Google Scholar]
- 18.Durso L, Latner J. Understanding self-directed stigma: development of the weight bias internalization scale. Int J Obesity. 16:S80–S86. doi: 10.1038/oby.2008.448. [DOI] [PubMed] [Google Scholar]
- 19.Crocker J, Luhtanen R, Blaine B, Broadnax S. Collective self-esteem and psychological well-being among White, Black, and Asian college students. Pers Soc Psychol Bull. 1994;20:503–513. [Google Scholar]
- 20.Maclean L, Edwards N, Garrard M, Sims-Jones N, Clinton K, Ashley L. Obesity, stigma and public health planning. Health Promot Int. 2009;24:88–93. doi: 10.1093/heapro/dan041. [DOI] [PubMed] [Google Scholar]
- 21.Lewinsohn P, Striegel-Moore R, Seeley J. Epidemiology and natural course of eating disorders in young women from adolescence to adulthood. J Am Acad Child Adolesc Psychiatry. 2000;39:1284–1292. doi: 10.1097/00004583-200010000-00016. [DOI] [PubMed] [Google Scholar]
- 22.Lewinsohn PM, Clarke GN, Seeley JR, Rohde P. Major depression in community adolescents: Age at onset, episode duration, and time to Recurrence. J Am Acad Child Adolesc Psychiatry. 1994;33:809–818. doi: 10.1097/00004583-199407000-00006. [DOI] [PubMed] [Google Scholar]
- 23.Mussell MP, Peterson CB, Weller CL, Crosby RD, de Zwaan M, Mitchell JE. Differences in body image and depression among obese women with and without binge eating disorder. Obes Res. 1996;4:431–439. doi: 10.1002/j.1550-8528.1996.tb00251.x. [DOI] [PubMed] [Google Scholar]
- 24.Sysko R, Finkelson EB, Devlin MJ, Walsh BT. Psychiatric disorders, family functioning, eating pathology, and quality of life among adolescent bariatric surgery candidates. under review. [Google Scholar]
- 25.Fairburn CG, Beglin SJ. Assessment of eating disorders: interview or self-report questionnaire? Int J Eat Disord. 1994;16:363–370. [PubMed] [Google Scholar]
- 26.Reas DL, Grilo CM, Masheb RM. Reliability of the Eating Disorder Examination-Questionnaire in patients with binge eating disorder. Behav Res Ther. 2006;44:43–51. doi: 10.1016/j.brat.2005.01.004. [DOI] [PubMed] [Google Scholar]
- 27.Luce KH, Crowther JH. The reliability of the Eating Disorder Examination-Self-Report Questionnaire Version (EDE-Q) Int J Eat Disord. 1999;25:349–351. doi: 10.1002/(sici)1098-108x(199904)25:3<349::aid-eat15>3.0.co;2-m. [DOI] [PubMed] [Google Scholar]
- 28.Grilo CM, Masheb RM, Wilson GT. A comparison of different methods for assessing the features of eating disorders in patients with binge eating disorder. J Consult Clin Psychol. 2001;69:317–322. doi: 10.1037//0022-006x.69.2.317. [DOI] [PubMed] [Google Scholar]
- 29.Mond JM, Hay PJ, Rodgers B, Owen C, Beumont PJ. Validity of the Eating Disorder Examination Questionnaire (EDE-Q) in screening for eating disorders in community samples. Behav Res Ther. 2004;42:551–567. doi: 10.1016/S0005-7967(03)00161-X. [DOI] [PubMed] [Google Scholar]
- 30.Mond J, Hay P, Rodgers B, Owen C. Self-report versus interview assessment of purging in a community sample of women. Eur Eat Disord Rev. 2007;15:403–409. doi: 10.1002/erv.792. [DOI] [PubMed] [Google Scholar]
- 31.Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J. An inventory for measuring depression. Arch Gen Psychiatry. 1961;4:561–571. doi: 10.1001/archpsyc.1961.01710120031004. [DOI] [PubMed] [Google Scholar]
- 32.Beck AT, Steer R, Garbin MG. Psychometric properties of the Beck Depression Inventory - 25 years of evaluation. Clin Psychol Rev. 1988;8:77–100. [Google Scholar]
- 33.March JS, Parker JD, Sullivan K, Stallings P, Conners K. The multidimensional anxiety scale for children (MASC): factor structure, reliability, and validity. J Am Acad Child Adolesc Psychiatry. 1997;36:554–565. doi: 10.1097/00004583-199704000-00019. [DOI] [PubMed] [Google Scholar]
- 34.Achenbach TM, Rescorla LA. Manual for ASEBA School-Age Forms & Profiles. Burlington, VT: University of Vermont, Research Center for Children, Youth, & Families; 2001. 2001. [Google Scholar]
- 35.Varni JW, Seid M, Rode CA. The PedsQL: Measurement model for the Pediatric Quality of Life Inventory. Med Care. 1999;37:126–139. doi: 10.1097/00005650-199902000-00003. [DOI] [PubMed] [Google Scholar]
- 36.Costello A, Osborne J. Best practices in exploratory factor analysis: Four recommendations for getting the most from your analysis. Practical Assessment, Research & Evaluation. 2005;10:1–9. [Google Scholar]
- 37.Carels RA, Wott CB, Young KM, Gumble A, Koball A, Oehlhof MW. Implicit, explicit, and internalized weight bias and psychosocial maladjustment among treatment-seeking adults. Eating Behav. 2010;11:180–185. doi: 10.1016/j.eatbeh.2010.03.002. [DOI] [PubMed] [Google Scholar]
- 38.Carels RA, Young KM, Wott CB, Harper J, Gumble A, Oehlof MW, Clayton AM. Weight bias and weight loss treatment outcomes in treatment-seeking adults. Ann Behav Med. 2009;37:350–355. doi: 10.1007/s12160-009-9109-4. 2009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Lillis J, Hayes SC, Bunting K, Masuda A. Teaching acceptance and mindfulness to improve the lives of the obese: a preliminary test of a theoretical model. Ann Behav Med. 2009;37:58–69. doi: 10.1007/s12160-009-9083-x. [DOI] [PubMed] [Google Scholar]