Abstract
Self-care behaviors are crucial for following the complex regimen after lung transplantation, yet little is known about recipients’ levels of self-care agency (the capability and willingness to engage in self-care behaviors) and its correlates. We examined levels of self-care agency and recipient characteristics (socio-demographics, psychological distress, quality of relationship with primary lay caregiver, and health locus of control) in 111 recipients. Based on Perceived Self-Care Agency scores, recipients were assigned to either the low or high self-care agency comparison group. Characteristics were compared between groups to identify characteristics likely to be associated with lower self-care agency. Mean (S.D.) score for self-care agency (scale range 53–265) was 223.02 (22.46). Recipients with lowest self-care agency scores reported significantly poorer quality of caregiver relationships (p < .001) and greater psychological distress (p < .001). After controlling for psychological distress, the quality of the recipient-caregiver relationship remained significantly associated with self-care agency. Every one-point decrease in the quality of caregiver relationship increased the risk of low self-care agency by 12%. Recipients with poorer caregiver relationships and greater psychological distress may need additional support to perform the self-care behaviors expected after lung transplantation.
Keywords: LUNG TRANSPLANTATION, TRANSPLANT RECIPIENTS, SELF-CARE, CAREGIVERS, PSYCHOLOGICAL
INTRODUCTION
Lung transplantation is one of the few treatments known to improvehealth-related quality of life and prolong survival for persons with end-stage lung disease. To date, over 30,000 persons have undergone lung transplantation world-wide.1 While most lung recipients experience an early dramatic improvement in their underlying conditions, over time they are at greater risk of developing transplant-related complications such as allograft rejection and recurrent infection than other solid organ recipients.2 The extent to which recipients perform self-care behaviors such as: adhering to the prescribed medical regimen, performing self-monitoring, attending to subtle changes in one’s health status, interpreting the importance of signs and symptoms, communicating changes to a clinical provider in a timely manner, and adopting healthy behaviors, has been shown to be clinically important for promoting healthy outcomes and demonstrating stewardship of the scarce donor organs available for transplantation.3–6 Thus, to manage their illness and maximize transplant outcomes, lung recipients are expected to actively engage in a variety of self-care practices.
Self-care agency, defined as the acquired capability and willingness to perform behaviors on one’s own behalf to maintain health and well-being or manage disease and illness,7 has been identified as the primary mechanism responsible for the performance of self-care behaviors and improvements in health outcomes among patients with chronic conditions.8–13 Self-care agency levels are thought to be influenced by factors such as socio-demographic characteristics (including age,14 gender,8, 15 adequacy of family income8, 14, 16), psychological distress,8 marital status,17 quality of social and family relationships,8, 14, 18 and beliefs about the locus of control over health.7, 8, 15 Yet such relationships among lung recipients at the time of transplant have not been examined. A better understanding of the characteristics that are associated with lower self-care agency among lung recipients, and thus may influence their ability to engage in self-care behaviors, is important given the serious consequences of failing to prevent, detect, and treat transplant related complications. The goals of this study were to examine the level of self-care agency among lung transplant recipients and to explore potential differences between recipients with low and high self-care agency after transplantation.
MATERIALS AND METHODS
Sample
The sample was comprised of lung recipients participating in a research trial comparing methods of tracking health information at home after transplantation. All adults (aged 18+) who received lung transplants at the UPMC Health System-Presbyterian Campus between January 2009 and August 2010 and survived the Intensive Care Unit recovery period were eligible for inclusion with the following exceptions: (i) recipient of any prior transplant (to avoid history and experiential effects); (ii) a condition that precluded discharge from the hospital; or (iii) inability to participate in their own care or provide informed consent. Of the 160 eligible lung transplant recipients, 5 were unexpectedly discharged before they could be approached and 44 refused to participate. The final sample of 111 lung recipients did not differ from recipients who refused to participate on any socio-demographic characteristics; however the majority of recipients who refused to enroll in the study reportedly did so because of feeling overwhelmed by hospital routines and preparations for discharge.
Procedure
The University of Pittsburgh’s Institutional Review Board approved the study protocol. All recipients provided written informed consent. When hospital discharge was imminent, and recipients completed the routine pre-discharge educational program, instruments regarding self-care agency and recipient characteristics (socio-demographics, symptoms of psychological distress, quality of relationship with primary lay caregiver, and health locus of control beliefs) were administered as part of their baseline assessment for the clinical trial and thus available for analysis in this study.
Measures
Self-care agency
Recipients’ perceptions of their level of self-care agency were assessed using the Perception of Self-Care Agency (PSCA),19 a 53 item, Likert-type, self-report instrument with established psychometric properties. In prior studies, internal consistency reliability for the scale (Cronbach’s α) was 0.93, and test-retest reliability was 0.85.19 Construct validity was demonstrated by significant correlations between the PSCA and actual performance of self-care behaviors (r=.29=.76).20, 21 Examples of PSCA items include: I use information I get to help me take care of myself and I do not know exactly what I am aiming for when it comes to taking care of myself. Positively worded items are scored as (1 = never like me to 5 = always like me); negatively worded items were reversed coded, then summed, yielding a score ranging from 53 to 265; higher scores indicate a higher level of self-care agency. Cronbach’s α for the PSCA in the current sample was 0.95.
Socio-demographic characteristics
Demographic characteristics were determined using a Socio-Demographic Profile that included age, gender, race/ethnicity, education, adequacy of household income, and marital status.
Psychological distress
Symptoms of psychological distress were measured using the Anxiety and Depression Subscales of the Symptom Checklist 90-Revised (SCL-90-R).22 These self-report subscales measure the severity of anxiety and depression symptoms during the prior two weeks. Items are rated on a five-point Likert-type, scale (0 = not at all to 4 = extremely distressed). Subscale scores are computed by averaging items. Higher scores reflect higher levels of distress. Previously reported test-retest reliability coefficients ranged from .80 to .90.22 For the current analyses, the anxiety and depressive symptom sub-scale scores were used to identify which recipients reported clinically significant psychological distress (defined as any score exceeding one standard deviation above the gender-specific normative mean on either the anxiety or depression sub-scale). [Devito Dabbs, Dew et al 2003] Cronbach’s α for the anxiety and depression subscales in the current sample were .83 and .92, respectively.
Quality of relationship with primary lay caregiver
The Dyadic Adjustment Scale (DAS),23 was adapted to measure the quality of the recipients’ relationships with their primary lay caregivers. The DAS is a 15-item, self-report measure of the quality of the relationship with the adult whom the recipient identifies as most involved in his/her daily care. Higher scores reflect higher relationship quality. Although spouses (generally wives) usually fulfill this caregiver role, the scale also has been found to be applicable for assessing the supportive nature of non-spouse types of lung transplant recipient-caregiver dyads with Cronbach’s α = 0.94. 24 Cronbach’s α = 0.86 for the DAS in this current sample.
Health locus of control
The Multidimensional Health Locus of Control Scale25, 26 was used to assess the extent to which lung recipients believed that their health outcomes were, i) primarily their own responsibility (internality locus of control), ii) the responsibility of their health professionals (externality locus of control), or iii) primarily due to chance. Each of the 3 subscales is comprised of 6 items. Subscale scores range from 6–36 with higher scores reflecting stronger beliefs in internality, externality, or chance. Cronbach’s α in the current sample was 0.78.
Statistical Analysis
Descriptive statistics were used to score and examine distributions of self-care agency and recipient characteristics. Internal consistency of all instruments was determined. Differences in characteristics between recipients with lowest and higher self-care agency scores were determined using chi-square with Fisher’s Exact Test for dichotomous variables, independent-sample t-tests for normally distributed and Mann-Whitney U tests for non-normally distributed continuous variables. Characteristics with significant differences between groups were included as predictors in a logistic regression analysis with lower self-care agency as the outcome variable. Odds ratios (OR) with confidence intervals and parameter estimates were assessed. The Hosmer-Lemeshow (H-L) goodness of fit test 27 and the chi-square test for coefficients were used to check model fit. All statistical tests of significance were conducted using an alpha level of .05. SPSS version 20 (SPSS, Inc.) was the statistical software utilized in all data analyses.
RESULTS
Sample characteristics
The sample included 111 recipients, who were evenly split by gender, and predominantly white (90.1%) and currently married (73%), with a mean age of 55.98 ranging from 19–75 years (see Table 1). The majority of recipients reported that they completed some post-secondary education (93.7%) and were on disability support (50.5%) or retired (32.4%). Only 9% of recipients were employed and/or in school at the time of transplant, yet the majority (83.8%) affirmed that their current household income met their basic needs, such as food, housing, utilities, and health care. Patients were similar in gender, age, and ethnicity to the population of adult lung recipients transplanted in the U.S. during the same time period.9
Table 1.
Sample Characteristics and Differences in Characteristics between Recipients with Low and High Perceptions of Self-Care Agency (PSCA)
| Sample Characteristics (N = 112) | Between Group Comparisons | ||||||
|---|---|---|---|---|---|---|---|
| Mean | SD | % | Low a PSCA (n=30) | High PSCA (n=82) | Test statistic | p value | |
| Self-Care Agency, M (SD) | 223.02 | 22.46 | -- | 195.33 (11.97) | 233.16 (15.87) | 13.49 | <.001 |
| Age, M (SD) | 56.98 | 13.92 | -- | 60.00 (9.7) | 55.80 (12.2) | −1.4 b | 0.15 |
| Gender, % male | -- | -- | 55 | 70 | 61 | 3.148 d | 0.07 |
| Race, % White/European American | -- | -- | 90.1 | 90 | 90 | −.001 d | 1.00 |
| Education, % ≥ high school | -- | -- | 93.7 | 90 | 95 | .321 d | 0.38 |
| Employment Status, % disabled | -- | -- | 50.5 | 10 | 9 | .983 d | 0.73 |
| Household Income, % meets needs e | -- | -- | 83.8 | 74 | 74 | .001 d | 0.09 |
| Marital Status, % currently married | -- | -- | 73 | 70 | 86 | 3.094 d | 0.07 |
| Pre-transplant lung disease, % obstructive | -- | -- | 48.2 | 40 | 51 | 1.10 d | 0.29 |
| Type of transplant, % bilateral | -- | -- | 74.5 | 73 | 75 | .032 d | 0.86 |
| ICU stay (days), M (SD) | 10.29 | 12.56 | -- | 12.5 (13.01) | 9.46 (12.37) | 1.31 b | 0.261 |
| Hospital stay (days), M (SD) | 37.08 | 24.04 | -- | 43.36 (26.49) | 34.68 (24.21) | 1.65 b | 0.26 |
| Mechanical vent (days), % > 2 | -- | -- | 31.8 | 43 | 28 | 2.52 d | 0.11 |
| Discharge destination, % home | -- | -- | 88.2 | 86.7 | 88.8 | .091 d | .763 |
| Dyadic Adjustment Score, M (SD) | 76.06 | 9.57 | -- | 62.3 (7.8) | 68.4 (4.5) | 600.00 c | <.001 |
| SCL-90 Anxiety, M (SD) f | .78 | .60 | -- | 1.01 (.47) | .67 (.62) | 820.50 c | .002 |
| SCL-90 Depression, M (SD) f | .81 | .52 | -- | 1.03 (.35) | .70 (.55) | 711.00 c | <.001 |
| Any Psychological Distress, % | -- | -- | 70 | 96 | 69 | 9.695 d | <.001 |
| Locus of Control (Internality), M (SD) | 24.31 | 6.25 | -- | 24.2 (5.49) | 24.35 b (6.6) | .13 b | 0.89 |
| Locus of Control (Externality), M (SD) | 29.09 | 4.09 | -- | 16.4 (1.78) | 17.1 (1.7) | .175 b | 0.08 |
| Locus of Control (Chance), M (SD) | 19.03 | 7.59 | -- | 20.74 (7.7) | 18.23 (7.47) | − 1.62 b | 0.11 |
25th percentile score (207) was used to determine assignment to the low versus high PSCA group
Independent t-tests for normally distributed and
Mann Whitney U for non-normally distributed continuous variables or
chi-square with Fisher’s Exact Test for dichotomous variables, degrees of freedom (df) = 1.
N=110, one recipient refused to provide data regarding whether household income adequately met needs
Raw SCL-90 anxiety and depression subscale scores are reported here prior to converting to the dichotomous variable presence of any clinically significant psychological distress due to anxiety and/or depression
Self-care agency
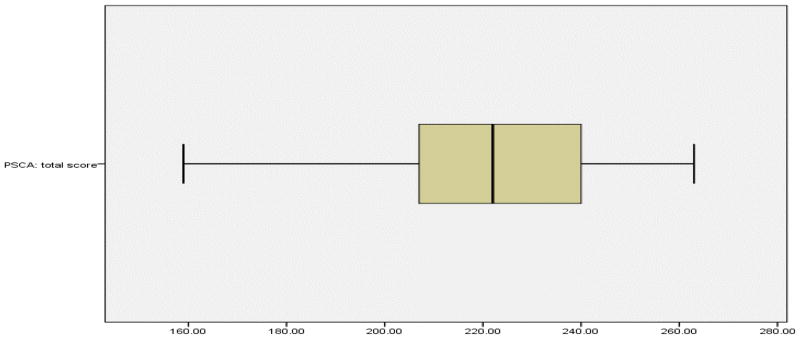
Most recipients reported high levels of self-care agency. Mean levels of PSCA were 223.02 (22.46), range 159–263 and the distribution of self-care agency scores was negatively skewed (see Figure 1: Box Plot of Self-Care Agency Scores, demonstrating scores per quartiles). The 25th percentile score (207) was used as the cut point between the low (n=30) and high (n=81) self-care agency groups.
Figure 1.
Box Plot of Self-Care Agency Scores
Note: The dark line in the middle of the boxes is the median (223.5). Far ends of box indicate the 25th (207) and 75th (240) percentiles. T bars indicate minimum (159) and maximum (263) scores.
Characteristics of recipients
Characteristics were compared between recipients with lowest and higher self-care agency scores (see Table 1). There were no statistically significant differences between groups due to age, gender, race, education, employment status, adequacy of household income, marital status, pre-transplant diagnosis (obstructive versus non-obstructive), type of transplant (single versus bilateral), days of mechanical ventilation, ICU stay, overall hospital length of stay, discharge destination or health locus of control beliefs. Recipients with the lowest levels of self-care agency (scores less than or equal to 207), and thus at highest risk for difficulty performing self-care behaviors, were significantly more likely to have poorer quality relationships with lay caregivers (p < .001), and more distress due to anxiety (p = .002) and depression (p < .001).
Logistic regression
Characteristics with significant differences between groups, including the quality of the lay caregiver relationship and presence of anxiety and depression, were considered for the logistic regression analysis with lower self-care agency as the outcome variable. Anxiety and depression were highly correlated (r= −.77) 28 therefore, a composite variable of any clinically significant psychological distress (defined as presence or absence of clinically significant anxiety and/or depression) was created and entered in the model. Since we were interested in the group that had low scores on PSCA, they were coded as the reference group (low=1, high=0) for the two-predictor logistic model (see Table 2). The H-L test of goodness of fit (χ2 (8) = 12.341, p = .137) was not significant indicating that the model was an appropriate fit for the data. Additionally, the addition of the two predictors was an improvement over the null model (χ2 (2)= 27.362, p< .001). The results indicated that only the quality of the caregiver relationship remained a significant predictor (OR = 0.89, p=.001). The OR for the effect indicates that every one-point decrease in the quality of caregiver relationship measure increases the risk of low self-care agency by 12%.
Table 2.
Logistic Regression Coefficients
| B | SE | Wald | Sig. | df | β | 95% C.I. | for EXP(B) | |
|---|---|---|---|---|---|---|---|---|
| Lower | Upper | |||||||
| Constant | 9.327 | 2.89 | 10.420 | .001 | 1 | 11242.672 | ||
| Quality of caregiver relationship | −.154 | 0.450 | 11.879 | .001 | 1 | .857 | .785 | .936 |
| Any Psychological distress | −1.285 | .809 | 2.527 | .112 | 1 | .277 | .057 | 1.349 |
DISCUSSION
In this study we examined levels of self-care agency among lung transplant recipients, identified characteristics of recipients with lowest self-care agency, and explored potential correlates of self-care agency in order to better identify recipients who may be at risk for difficulty engaging in self-care behaviors after transplantation. We found that most recipients reported high levels of self-care agency. On average, recipients scored 223 (22.46) on the Perceptions of Self-Care Agency scale with potential scores ranging from a low of 53 to a high of 265. Lung recipients’ PSCA scores were higher than other patient populations, including patients whose mean self-care agency scores were 200.5 (22.8) on the day of discharge from the hospital after coronary artery bypass surgery, 29 and between 119–209 after treatment of mood disorders.17 Possible explanations for the high levels of self-care agency may include the fact that lung recipients already acquired the capability and willingness to engage in self-care behaviors while managing their pre-transplant underlying chronic lung diseases. Also the majority of recipients in this sample were relatively highly educated and affirmed that their household income met their needs, thereby reducing financial stressors and demands that may influence self-care agency. Another possible explanation is the timing of our assessment of self-care agency; we measured self-care agency prior to hospital discharge when recipients may be feeling overly confident about their ability to perform the self-care behaviors that are expected of them after transplant. It is also possible that participants in this study reported higher self-care agency because they were less anxious about their impending discharge and thus better able to master the skills necessary to perform self-care after transplant than other recipients who were unwilling to be studied because of feelings of being overwhelmed during their hospitalization.
Recipients with the lowest levels of self-care agency (25th percentile), and thus at highest risk for difficulty performing self-care behaviors, were significantly more likely to have poorer quality relationships with lay caregivers and more psychological distress than recipients with higher self-care agency. Differences in self-care agency due to recipient characteristics (age, gender, race, education, employment, marital status, and household income) were not significant and consistent with previous studies that reported only small effects between socio-demographic characteristics and self-care behaviors.30 Exceptions were that poorer quality of lay caregiver relationship and greater psychiatric distress differed between low and high self-care agency.
The quality of the recipients’ relationship with their primary lay caregivers had an important impact on level of self-care agency. These results are consistent with other reports, including synthesized evidence from meta-analyses, that suggest that social support from family and friends were predictors of better adherence to the medical regimen, a major aspect of self-care.31, 32 In the setting of lung transplantation, the quality of the lay caregiver relationship is vital to the well-being, psychological functioning, and adherence of transplant recipients particularly because lung recipients are expected to follow more complex medical regimens and experience more post-transplant complications than do other types of solid organ transplant recipients.33–39 Moreover, the quality of caregiver relationship remained important for self-care agency after the presence of clinically significant psychological distress was controlled.
Although we anticipated that psychological status at baseline would be influenced by the stress of the postoperative recovery and impending discharge, examining psychological distress at this point enabled us to describe how variations in psychological distress related to self-care agency. The presence of any clinically significant psychological distress (due to either anxiety and/or depression) was an important correlate of self-care agency. This finding is particularly meaningful when one considers the fact that our sample may not have included the most distressed lung recipients such as those who felt too overwhelmed to participate in this study. Psychological distress is known to negatively affect transplant recipients’ self-concept, motivation, sleep quality, ability to problem-solve, concentrate, and cope effectively 40 all prerequisites for recipients to be actively engaged in their care and perform self-care behaviors. Therefore, it is not surprising that persons with higher levels of anxiety or depressive symptoms reported lower self-care agency, highlighting the importance of assessing for and intervening to reduce psychological distress among lung transplant recipients.
Although one might expect recipients with higher levels of self-care agency to hold health control beliefs of internality (i.e., belief that health outcomes were primarily their own responsibility), and recipients with lower levels of self-care agency to hold health control beliefs of externality (i.e., belief that of their health professionals were responsible for health outcomes) or chance (i.e., belief that health outcomes were up to chance), we found no differences in health locus of control beliefs between recipients with low and high levels of self-care agency, nor was there an inverse correlation between self-care agency and holding health control beliefs of externality as one might expect. Recipients in this study with beliefs that their health outcomes were primarily due to chance, reported lower levels of self-care agency. While this finding was surprising, and not reported previously, it makes sense that recipients who believe that chance alone influences their health outcomes might be less likely to recognize the importance of acting as agents of their own self-care.
Limitations
This research has several limitations. First, the study was conducted with lung recipients from a single transplant program which could affect the generalizability of our findings; however as noted, characteristics of our sample were similar to other recipients who underwent lung transplantation in the U.S. Second, we measured self-care agency, an important predictor of a person’s ability to be actively involved in their care, but possession of self-care agency may not reflect the actual performance of self-care behaviors. Third, we assessed levels of self-care agency at only one time point, prior to discharge, to identify recipients who may be at risk for difficulty performing self-care behaviors after transplant, but there is evidence to suggest that individuals’ confidence in their ability to manage an illness in the future may be inflated compared to their actual ability to independently perform the appropriate self-care behaviors. In addition, self-care agency, like self-care behaviors, may wane over time and fluctuate with changes in recipients’ conditions. Lastly, recipients who agreed to participate in this study appeared to be less overwhelmed by hospital routines and preparations for discharge than recipients who refused to be studied. Therefore, it is likely that refusers may represent recipients with greater psychological distress and thus lower levels of self-care agency.
Despite these limitations, an important correlate of self-care agency—the presence of clinically significant psychological distress was identified, and even after controlling for this factor, the quality of relationship with primary lay caregiver raised recipients’ risk for lower levels of self-care agency and the potential for reduced engagement in self-care activities.
Implications
Knowing characteristics of recipients who are likely to have lower levels of self-care agency may help clinicians to identify those who need additional assistance and support to perform self-care behaviors after discharge. Some of the predictors of self-care agency are modifiable, therefore interventions should be designed to strengthen the quality of relationships with lay caregivers and reduce psychological distress in order to increase recipients’ active involvement and performance of self-care behaviors.
While lower levels of self-care agency may increase recipients’ risk for fully engaging in their care, the possession of self-care agency alone does not guarantee that recipients will be fully equipped to perform self-care behaviors. High levels of self-care agency do not preclude the need to ‘tool’ recipients to perform self-care behaviors. Therefore recipients’ ability to actually perform self-care behaviors should be monitored closely. Furthermore, it is important to continually assess recipients’ self-care behaviors over time because vulnerability for nonadherence to self-care increases in times of medical stability,3, 41 and interventions to promote self-care are likely to be most effective when recipients are experiencing health threats, time when they are motivated to reduce their risks and improve their well-being.32, 42 Further study is needed to assess the pattern of self-care agency over time and its influence on the actual performance of self-care behaviors after lung transplantation.
SUMMARY.
This original research study examines levels and correlates of self-care agency, defined as the capability and willingness of lung recipients to engage in self-care behaviors, among 111 lung transplant recipients in order to identify recipients who may be at risk for lower self-care agency and thus difficulty performing self-care behaviors after hospital discharge. There were no statistically significant differences between groups with low versus high self-care agency due to age, gender, race, education, employment status, adequacy of household income, marital status, or health locus of control beliefs. Recipients with the lowest levels of self-care agency (25th percentile), and thus at highest risk for difficulty performing self-care behaviors, were significantly more likely to have poorer quality relationships with lay caregivers (p < .001), and more distress due to anxiety (p = .002) and depression (p < .001). After controlling for the presence of psychological distress, the quality of the recipient-caregiver relationship remained significantly associated with self-care agency.
Acknowledgments
Study funded by a grant NR010711 (DeVito Dabbs, PI) from the National Institute of Nursing Research.
Footnotes
AUTHORS’ CONTRIBUTIONS:
Annette DeVito Dabbs, RN, Ph.D, FAAN: Concept/design, Data analysis/interpretation, Drafting article, Critical revision of article, Approval of article, Statistics, Funding secured by.
Lauren Terhorst, Ph.D: Statistics, data analysis/interpretation
Mi-Kyung Song RN, Ph.D: Concept/design, Data analysis/interpretation, Drafting article, Critical revision of article, Approval of article
Diana A. Shellmer Ph.D: Data analysis/interpretation, Drafting article, Critical revision of article, Approval of article
Jill Aubrecht RN, MSN, MBA: Data analysis/interpretation, Critical revision of article, Approval of article, Data collection
Mary Connolly RN, BSN: Data analysis/interpretation, Critical revision of article, Approval of article, Data collection
Mary Amanda Dew, Ph.D: Concept/design, Data analysis/interpretation, Drafting article, Critical revision of article, Approval of article, Statistics
References
- 1.Christie JDLB, Edwards LB, Kucheryavaya AY, Aurora P, Dobbels F, Kirk R, Rahmel AOJ, Hertz MI. The Registry of the International Society for Heart and Lung Transplantation: Twenty-seventh official adult-lung and heart-lung report-2010. J Heart & Lung Transplantation. 2010;29:1104–1118. doi: 10.1016/j.healun.2010.08.004. [DOI] [PubMed] [Google Scholar]
- 2.Korom SBA, Weder W. Immunosuppressive therapy in lung transplantation: state of the art. European J Cardio-Thorac Surg. 2009;35:1045–1055. doi: 10.1016/j.ejcts.2009.02.035. [DOI] [PubMed] [Google Scholar]
- 3.DeVito Dabbs A, Hoffman L, Swigart V, et al. Using Conceptual Triangulation to Develop an Integrated Model of the Symptom Experience of Acute Rejection after Lung Tranplantation. Advances in Nursing Science. 2004;27:138–149. doi: 10.1097/00012272-200404000-00007. [DOI] [PubMed] [Google Scholar]
- 4.DeVito Dabbs A. Are symptom reports useful for differentiating between acute pulmonary complications after lung transplantation? Heart & Lung, Journal of Critical Care. 2004;33:372–380. doi: 10.1016/j.hrtlng.2004.05.001. [DOI] [PubMed] [Google Scholar]
- 5.Dew MA, DiMartini AF, De Vito Dabbs A, et al. Rates and risk factors for nonadherence to the medical regimen after adult solid organ transplantation. Transplantation. 2007;83:858–873. doi: 10.1097/01.tp.0000258599.65257.a6. [DOI] [PubMed] [Google Scholar]
- 6.Van Muylem A, Knoop C, Estenne M. Early Detection of Chronic Pulmonary Allograft Dysfunction by Exhaled Biomarkers. American Journal of Respiratory and Critical Care Medicine. 2007;175:731–736. doi: 10.1164/rccm.200609-1301OC. [DOI] [PubMed] [Google Scholar]
- 7.Orem DE. Nursing concepts of Practice. 2. St Louis: MO Mosby; 1991. [Google Scholar]
- 8.Callaghan D. Basic conditioning factors’ influences on adolescents’ health behaviors, self-efficacy and self-care. Issues of Comprehensive Pediatric Nursing. 2006;29:191–204. doi: 10.1080/01460860601087156. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.OOSADR. Department of Health and Human Services, Health Resources and Services Administration, Healthcare Systems Bureau, Division of Transplantation. 2011. [Accessed 1/15/2012]. 2010. [Google Scholar]
- 10.Lorig KSD, Ritter P, Laurent D, Hobbs M. Effect of a self-management program on patients with chronic disease. Eff Clin Pract. 2001;4:256–262. [PubMed] [Google Scholar]
- 11.Riesch S, Haucj R. The Exercise of Self-Care Agency: An Analysis of Construct and Discriminant Validity. Research in Nursing & Health. 1988;11:245–255. doi: 10.1002/nur.4770110406. [DOI] [PubMed] [Google Scholar]
- 12.Sousa VDHS, Miller EH, Carroll MA. Measrues of diabetes self-care agency, diabetes self-efficacy and diabetes self-managment for insulin-treated individuals with type 2 diabetes. Journal of Clinical Nursing. 2008:18. doi: 10.1111/j.1365-2702.2008.02729.x. [DOI] [PubMed] [Google Scholar]
- 13.Wagner EH, Austin BT, Davis C, et al. Improving chronic illness care: translating evidence into action. Health Affairs. 2001;20:64–78. doi: 10.1377/hlthaff.20.6.64. [DOI] [PubMed] [Google Scholar]
- 14.Orem DE. Nursing, Concepts of Practice. 6. St. Louis: Mosby; 2001. [Google Scholar]
- 15.Gaut DKRN. Assessment of self-care agency in chronically ill adolescents. J Adolesc Health Care. 1998;9:55–60. doi: 10.1016/0197-0070(88)90019-8. [DOI] [PubMed] [Google Scholar]
- 16.Baker LDMJ. Predictors of self-care in adolescents with cystic fibrosis: A test of Orem’s theories of self-care and self-care deficit. J Pediatr Nurs. 2008;23:37–48. doi: 10.1016/j.pedn.2007.07.008. [DOI] [PubMed] [Google Scholar]
- 17.Cutler C. Disseration Abstracts International The Sciences and Engineering. 1998. The relationship of self-care agency, self efficacy and social support to post-hospitalization adjustment of patiens with a mood disorder; p. 59. [Google Scholar]
- 18.Faulkner MCI. Family influences on self-care, quality of life and metabollic control in school aged children with Type I diabetes. J Pediatr Nurs. 2007:27. doi: 10.1016/j.pedn.2006.02.008. [DOI] [PubMed] [Google Scholar]
- 19.Hanson B, Bickel L. Development and testing on perception of self-care agency. In: Riehl-Sisca J, editor. The Science and Art of Self-Care. Norwalk, Connecticut: Appleton-Century-Crofts; 1985. pp. 271–278. [Google Scholar]
- 20.Cleveland S. Perceived Self-Care Agency: A Lisrel Factor Analysis of Bickels and Hanson’s Questionnaire {Letter to the Editor} Nurs Res. 1989;38:59. [PubMed] [Google Scholar]
- 21.Weaver M. Perceived Self-Care Agency: A lisrel factor analysis of Bickel and Hanson’s Questionnaire. Nurs Res. 1987;36:381–387. [PubMed] [Google Scholar]
- 22.Derogatis L. SCL-90-R: Symptom Checklist 90-Revised: Administration, scoring, and procedures manual. Towson, MD: Clinical Psychometrics Research; 1994. [Google Scholar]
- 23.Spanier GB. Measuring Dyadic Adjustment: New scales for assessing the quality of marriage and similar dyads. Journal of Marriage & Family. 1976:38. [Google Scholar]
- 24.DeVito Dabbs AJ, Dew MA, Myers B, et al. Evaluation of a hand-held, computer-based intervention to promote early self-care behaviors after lung transplant. Clin Transplant. 2009;23:537–545. doi: 10.1111/j.1399-0012.2009.00992.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Wallston KA, Walltson BS, DeVellis R. Development of Multidimensional Health Locus of Control (MHLC) Scale. Health Education Monographs. 1978;6:160–170. doi: 10.1177/109019817800600107. [DOI] [PubMed] [Google Scholar]
- 26.Wallston BS, KAW Locus of control and health: A review of the literature. Health Education Monographs. 1978;6:106–117. doi: 10.1177/109019817800600102. [DOI] [PubMed] [Google Scholar]
- 27.Hosmer DW, Lemeshow S. Applied Logistic Regression. 2. New York: Wiley and Sons; 2000. [Google Scholar]
- 28.Bewick V, Cheek L, Ball J. Statistics review 14: Logistic regression. Critical Care. 2005;9:112–118. doi: 10.1186/cc3045. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Cebeci FC. SS Discharge training and counseling increase self-care ability and reduce post-discharge problems in CABD patients. Journal of Clinical Nursing. 2007;29:412–420. doi: 10.1111/j.1365-2702.2007.01952.x. [DOI] [PubMed] [Google Scholar]
- 30.DiMatteo MR. Variations in Patients’ Adherence to Medical Recommendations: A Quantitative Review of 50 Years of Research. Medical Care. 2004;42:200–209. doi: 10.1097/01.mlr.0000114908.90348.f9. [DOI] [PubMed] [Google Scholar]
- 31.Dew MA, DiMartini AF, De Vito Dabbs AJ, et al. Adherence to the medical regimen during the first two years after lung transplantation. Transplantation. 2008;85:193–202. doi: 10.1097/TP.0b013e318160135f. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.DiMatteo M, Haskard KB, Williams SL. Health Beliefs, Disease Severity, and Patient Adherence, A Meta-Analysis. Medical Care. 2007;45:521–528. doi: 10.1097/MLR.0b013e318032937e. [DOI] [PubMed] [Google Scholar]
- 33.Chaparro C, Scavuzzo M, Winton T, et al. Status of lung transplant recipients surviving beyond five years. Journal of Heart and Lung Transplantation. 1997;16:511–516. [PubMed] [Google Scholar]
- 34.Gross C, Savik K, Bolman R, et al. Long-term health status and quality of life outcomes of lung transplant recipients. Chest. 1995;108:1587–1593. doi: 10.1378/chest.108.6.1587. [DOI] [PubMed] [Google Scholar]
- 35.Gross CR, Raghu G. The cost of lung transplantation and the quality of life post-transplant. Clinics in Chest Medicine. 1997;18:391–403. doi: 10.1016/s0272-5231(05)70387-7. [DOI] [PubMed] [Google Scholar]
- 36.Limbos MM, Joyce DP, Chan CKN, et al. Psychological Functioning and Quality of Life in Lung Transplant Candidates and Recipients. Chest. 1997;112:1165–1174. doi: 10.1378/chest.112.5.1165. [DOI] [PubMed] [Google Scholar]
- 37.MacNaughton K, Rodrigue J, Cicale M, et al. Health-related quality of life and symptom frequency before and after lung transplantation. Clinical Transplantation. 1998;12:320–323. [PubMed] [Google Scholar]
- 38.Rodrigue JR, Baz MA, Kanasky WF, et al. Does lung transplantation improve health-related quality of life? The University of Florida experience. Journal of Heart and Lung Transplantation. 2005;24:755–763. doi: 10.1016/j.healun.2004.04.012. [DOI] [PubMed] [Google Scholar]
- 39.TenVergert EM, Essink-Bot M-L, Geertsma A, et al. The Effect of Lung Transplantation on Health-Related Quality of Life: A Longitudinal Study. Chest. 1998;113:358–364. doi: 10.1378/chest.113.2.358. [DOI] [PubMed] [Google Scholar]
- 40.Dew MA, DiMartini A. Psychological Disorders and Distress After Adult Cardiothoracic Transplantation. Journal of Cardiovascular Nursing. 2005;20:s51–66. doi: 10.1097/00005082-200509001-00007. [DOI] [PubMed] [Google Scholar]
- 41.Riegel BCB, Glaser D. Development and testing of a clinical tool measuring self-management of heart failure. Heart Lung. 2000;29:4–12. doi: 10.1016/s0147-9563(00)90033-5. [DOI] [PubMed] [Google Scholar]
- 42.Coleman MTN, KS Supporting self-management in patients with chronic illness. Am Fam Physician. 2005;72:1503–1510. [PubMed] [Google Scholar]