SUMMARY
Mitra and colleagues analyzed microRNA expression profiles of fibroblasts isolated from ovarian cancer patients, searching for dysregulated microRNAs in the stromal compartment of human cancer. They found that decreased miR-31 and miR-214 and increased miR-155 expression can reprogram normal fibroblasts into tumor-promoting cancer-associated fibroblasts. They identified CCL5, a pro-tumorigenic chemokine that is highly expressed in tumors, as a key target of miR-214, thus demonstrating that microRNA perturbation in the stromal microenvironment can affect tumor growth.
IN THE SPOTLIGHT
The tumor microenvironment, which includes cells such as macrophages, T cells, endothelial cells and fibroblasts, as well as extracellular matrix components, plays an important role during tumor evolution and metastasis (1, 2). Although these stromal cells are not themselves transformed, they are often induced by tumor cells to contribute to tumorigenesis, and are believed to adapt and continuously co-evolve with tumor epithelial cells to foster transformation, angiogenesis, growth and invasion (3, 4). These desmoplastic changes to the tumor stroma are observed in many cancer types, including breast, prostate, skin, pancreatic and ovarian cancers. As a result, these non-malignant tumor components have emerged as attractive therapeutic targets.
Fibroblasts are one of the principal constituents of the tissue microenvironment. In non-malignant tissues, fibroblasts are capable of adapting to tissue injury, and during wound healing, change their phenotype to become reactive. The reactive fibroblast, also known as a myofibroblast, shares properties with both fibroblasts and smooth muscle cells. In addition to wound healing, reactive fibroblasts are also found in malignant cancers and referred to as carcinoma-associated fibroblasts (CAFs), which differ from normal fibroblasts by their unusually high expression of smooth muscle actin (SMA) and their pro-tumorigenic properties (1, 5, 6). They secrete a repertoire of pro-inflammatory molecules, growth factors and proteinases including interleukins (e.g., IL-6), chemokines (e.g., CXCL12/SDF-1α), vascular endothelial and platelet-derived growth factors (e.g., VEGF and PDGFs), matrix metalloproteinases (MMPs) and extracellular matrix components (e.g., tenascin C, fibronectin and collagen type I) (7). These factors recruit other cell types to the primary tumor and even to future sites of metastatic colonization (8), and actively remodel the surrounding tumor microenvironment to facilitate growth, invasion and metastasis. Indeed, perturbation of fibroblast homeostasis by Pten deletion in the mammary gland accelerates the initiation, progression and malignant transformation of mammary epithelial tumors (9). This phenomenon is associated with extensive extracellular matrix remodeling, immune infiltration and angiogenesis, thus illustrating the powerful effects CAFs exert on the tumor microenvironment, which in turn affect tumor development.
The origin of CAFs and the mechanisms that regulate their development remain largely unknown. One model posits that CAFs are generated locally by inducing normal fibroblasts to take on CAF properties, which is mediated by soluble paracrine signals secreted by the tumor (6). One striking finding is that the CAF phenotype is stable and sustainable over multiple passages in vitro (5). Although the signals that govern the transition are not fully understood, recent evidence suggests that transforming growth factor-β (TGFβ) and IL-1β play important roles (6, 7). Other work has suggested that the epithelial-to-mesenchymal transition (EMT) can convert malignant epithelial cells into CAFs under certain conditions (7), although it remains controversial whether the genomes of CAFs are identical to those of the malignant cells. Another possibility is that CAFs originate from bone marrow-derived cells or mesenchymal stem cells, which differentiate in situ into CAFs. Support for each of these hypotheses can be found in the literature. However, several outstanding questions remain: what drives CAFs to acquire tumor-promoting functions? What genetic networks are activated in normal fibroblasts that convert them into CAFs? How is the CAF phenotype sustained over time, and is the phenotype reversible?
In this issue of Cancer Discovery, Mitra and colleagues (10) investigated the role of microRNAs (miRNAs) in regulating the CAF phenotype in human ovarian cancer. miRNAs are small non-coding RNA molecules that negatively regulate gene expression at the post-transcriptional level, and have recently been implicated in a number of developmental processes, including cell differentiation and reprogramming. While many studies have focused on miRNAs expressed by tumor cells, few studies have analyzed miRNAs expressed by CAFs. Mitra and colleagues sought to determine differences in the miRNA expression profiles of normal fibroblasts and CAFs. Accordingly, they isolated primary CAFs and adjacent normal fibroblasts from ovarian cancer patients, as well as generated induced human CAFs by co-culturing normal fibroblasts (isolated from human patients undergoing benign gynecologic surgery) with tumor cells, and performed microRNA array studies. Interestingly, several differentially expressed miRNAs emerged as interesting candidates to control the CAF phenotype.
To demonstrate that these candidates played an important role in CAF induction, the authors used a combination of in vitro and in vivo assays to study the effects of miR-31, miR-214, and miR-155. They showed that transient perturbation of these three miRNAs was sufficient to convert normal ovarian fibroblasts into induced CAFs that promoted ovarian tumor growth and increased tumor cell invasiveness and migration. Conversely, they showed the reverse was also true, and that CAFs could be retro-converted into more normal fibroblasts by over-expressing the down-regulated miRNAs (miR-31 and miR-214), and knocking down the up-regulated miRNA (miR-155).
Using a screen for chemokines and cytokines, Mitra and colleagues identified a target of miR-214 to be CCL5 and showed that miR-214 inversely regulated CCL5. Importantly, the authors demonstrated that down-regulation of miR-214 increases CCL5 production, leading to increased tumor growth. An anti-CCL5 antibody blocked the effect of CAFs on tumor growth and cell migration. This work illustrates that miRNA dysregulation in CAFs, not epithelial tumor cells, is capable of affecting tumorigenesis and highlights the importance of microRNAs in controlling the tumor microenvironment.
One of the most notable aspects of the study is that the authors used primary ovarian fibroblasts from omental metastases of human patients to conduct their microarray study. The authors compared these fibroblasts to normal adjacent fibroblasts from the same patient, as well as ovarian fibroblasts from patients with benign gynecologic disease. In addition, they created induced CAFs by co-culturing the normal primary human fibroblasts with ovarian cancer cells. This is a key strength of the study, as it immediately validates the clinical relevance of the findings, and uses complementary strategies to isolate CAFs. In addition, the study sheds light on how the CAF phenotype is maintained by reversible epigenetic modifications, namely microRNA regulation. This gives us insight into how CAFs sustain their tumor-promoting properties, which may be a therapeutically targetable pathway. Finally, the study emphasizes the complexities of the crosstalk between the tumor and stromal compartments, adding miRNAs to the conversation.
However several missing links remain that will certainly be important to address in future studies. For example, what upstream tumor-derived signals promote and inhibit expression of these three microRNAs? In their experiments, the authors show that ovarian cancer cells are capable of inducing normal ovarian fibroblasts to become CAFs. Yet the nature of this signal is not explored, and it will be important to determine whether the signal is soluble or whether it depends on cell-cell interactions. While it is known that molecules such as TGFβ and IL-1β regulate CAF induction, it is unclear whether these three miRNAs are downstream of these signaling pathways.
In addition, what other sources of these signals might exist in vivo? It is an intriguing possibility that cells other than the carcinoma might also secrete factors that trigger fibroblasts to down-regulate miR-31 and miR-214 and up-regulate miR-155. This may establish multiple feed-forward loops to drive tumor progression and metastasis. It will be important to determine the upstream signals within the tumor microenvironment that regulate the expression of miR-31, miR-214 and miR-155.
Furthermore, although Mitra and colleagues nicely demonstrate that inhibition of CCL5 using a blocking antibody abrogates the tumor-promoting properties of miR-CAFs on ovarian cancer growth, it is not yet clear by what mechanism this effect occurs. In other words, how does CCL5 regulate ovarian cancer progression and metastasis? Other chemokines such as CXCL12/SDF-1α have been shown to increase tumor growth as well as recruit endothelial progenitor cells to stimulate tumor angiogenesis (5). Whether CCL5 promotes tumor progression through a non-cell autonomous mechanism by modification of the microenvironment in ovarian cancer remains to be determined.
Finally, the authors identified three miRNAs that are important in ovarian CAFs, yet have only elucidated one target of one miRNA. How do miR-31 and miR-155 function in CAF induction, and what downstream chemokines, cytokines or growth factors are involved? Do the targets of miR-31 and miR-155 interact with other cells in the microenvironment? miR-31 has recently shown to be anti-metastatic in mammary epithelial cancer cells by modulating integrin α5, radixin and RhoA (11). Whether these targets are operative in the CAF remain to be determined. These questions, and others that will stem from this exciting work, will be important to answer in the near future, and may provide important considerations and new strategies for therapeutic intervention.
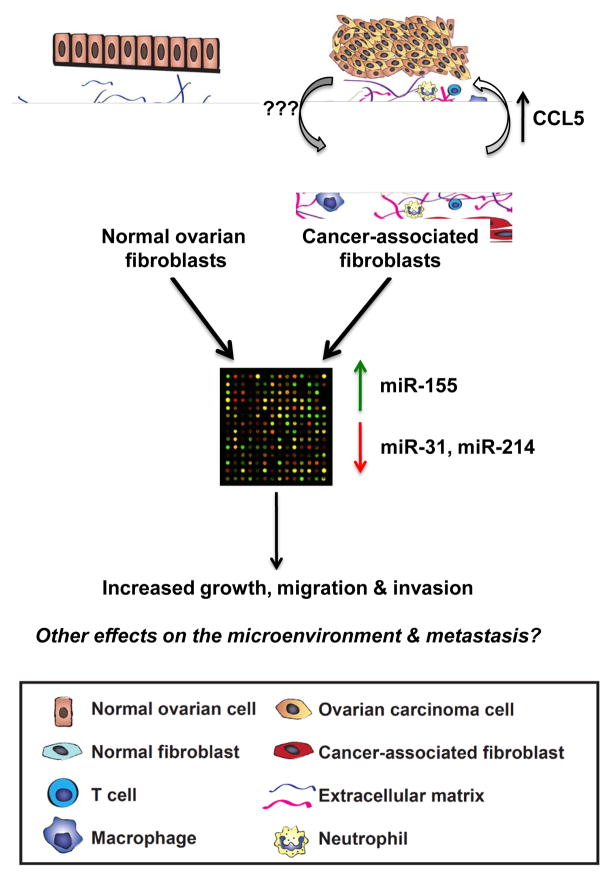
Figure 1.
Summary of the experimental strategy and key findings in Mitra et al. (10). The authors isolated cancer-associated fibroblasts (CAFs) and adjacent normal fibroblasts from ovarian cancer patients, and looked for differentially expressed microRNAs using microarrays. They found increased expression of miR-155 and decreased expression of miR-214 and miR-31 in CAFs. Perturbation of these microRNAs was sufficient to generate induced CAFs from normal fibroblasts. One key target of miR-214 was CCL5, which provided tumor-promoting signals back to the carcinoma cells. The tumor-derived signals that regulate expression of these microRNAs remain to be determined, as well as effects on other components of the tumor microenvironment.
Acknowledgments
GRANT SUPPORT
This work was supported in part by funds from the National Cancer Institute (R01 CA129523 to Z.W.), a Department of Defense Predoctoral Fellowship (W81XWH-10-1-0168 to J.C.), and the UCSF Medical Scientist Training Program (J.C.).
Footnotes
DISCLOSURE OF POTENTIAL CONFLICTS OF INTEREST
No potential conflicts of interests were disclosed.
References
- 1.Egeblad M, Littlepage LE, Werb Z. The fibroblastic coconspirator in cancer progression. Cold Spring Harb Symp Quant Biol. 2005;70:383–8. doi: 10.1101/sqb.2005.70.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Hanahan D, Coussens LM. Accessories to the crime: functions of cells recruited to the tumor microenvironment. Cancer Cell. 2012;21:309–22. doi: 10.1016/j.ccr.2012.02.022. [DOI] [PubMed] [Google Scholar]
- 3.Allinen M, Beroukhim R, Cai L, Brennan C, Lahti-Domenici J, Huang H, et al. Molecular characterization of the tumor microenvironment in breast cancer. Cancer Cell. 2004;6:17–32. doi: 10.1016/j.ccr.2004.06.010. [DOI] [PubMed] [Google Scholar]
- 4.Olumi AF, Grossfeld GD, Hayward SW, Carroll PR, Tlsty TD, Cunha GR. Carcinoma-associated fibroblasts direct tumor progression of initiated human prostatic epithelium. Cancer Res. 1999;59:5002–11. doi: 10.1186/bcr138. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Orimo A, Gupta PB, Sgroi DC, Arenzana-Seisdedos F, Delaunay T, Naeem R, et al. Stromal fibroblasts present in invasive human breast carcinomas promote tumor growth and angiogenesis through elevated SDF-1/CXCL12 secretion. Cell. 2005;121:335–48. doi: 10.1016/j.cell.2005.02.034. [DOI] [PubMed] [Google Scholar]
- 6.Erez N, Truitt M, Olson P, Arron ST, Hanahan D. Cancer-associated fibroblasts are activated in incipient neoplasia to orchestrate iumor-promoting inflammation in an NF-kappaB-dependent manner. Cancer Cell. 2010;17:135–47. doi: 10.1016/j.ccr.2009.12.041. [DOI] [PubMed] [Google Scholar]
- 7.Kalluri R, Zeisberg M. Fibroblasts in cancer. Nat Rev Cancer. 2006;6:392–401. doi: 10.1038/nrc1877. [DOI] [PubMed] [Google Scholar]
- 8.Psaila B, Lyden D. The metastatic niche: adapting the foreign soil. Nat Rev Cancer. 2009;9:285–93. doi: 10.1038/nrc2621. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Trimboli AJ, Cantemir-Stone CZ, Li F, Wallace JA, Merchant A, Creasap N, et al. Pten in stromal fibroblasts suppresses mammary epithelial tumours. Nature. 2009;461:1084–91. doi: 10.1038/nature08486. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Mitra AK, Zillhardt M, Hua Y, Tiwari P, Murmann AE, Peter ME, et al. MicroRNAs reprogram normal fibroblasts into cancer associated fibroblasts in ovarian cancer. Cancer Discov. 2012 doi: 10.1158/2159-8290.CD-12-0206. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Valastyan S, Benaich N, Chang A, Reinhardt F, Weinberg RA. Concomitant suppression of three target genes can explain the impact of a microRNA on metastasis. Genes Dev. 2009;23:2592–7. doi: 10.1101/gad.1832709. [DOI] [PMC free article] [PubMed] [Google Scholar] [Retracted]