Abstract
AIM
To describe the results of vitrectomy and partial capsulectomy via anterior approach surgical technique in treatment of chronic postoperative endophthalmitis (CPE).
METHODS
Clinical records of 9 patients treated for CPE between 2006 and 2010 were reviewed retrospectively. All of these patients were treated with vitrectomy and partial capsulectomy via anterior approach.
RESULTS
Six of 9 patients were male. The average patients' age was (60±8.1) years. The average period between cataract extraction and onset of signs and symptoms was (3.6±1.3) weeks. The average presenting visual acuity was 0.3±0.1 and the average final post operative visual acuity was 0.7±0.2. The mean follow-up period was (28.1±8.9) weeks. In all patients, the inflammation subsided after surgery.
CONCLUSION
Our results suggest that anterior vitrectomy and partial capsulectomy via anterior approach may be considered as potentially useful and relatively less invasive technique to treat CPE.
Keywords: chronic postoperative endophthalmitis, anterior vitrectomy, partial capsulectomy
INTRODUCTION
Chronic postoperative endophthalmitis (CPE) is a rare complication of cataract surgery but has been well documented in several small series [1]-[5]. It is characterized by an indolent low-grade uveitis with latent onset, an initial response to topical steroids, and the frequent absence of more typical endophthalmitis signs and symptoms [6]. This endophthalmitis occur months or even years after the initial surgical event [1].
There is no generally accepted treatment protocol for CPE; thus, patients are treated by variety of methods; such as intravitreal antibiotics, total capsulectomy with removal of intraocular lens (IOL), pars plana vitrectomy (PPV) with partial capsulectomy, Nd-YAG capsulotomy with intravitreal antibiotics, lens capsular bag irrigation [7]. Here, we describe an effective surgical technique with good results in treatment of CPE.
SUBJECTS AND METHODS
Clinical records of patients treated for CPE between 2006 and 2010 were reviewed retrospectively. The procedure was carried out in 9 patients who presented with whitish precipitates in the capsular bag and anterior chamber inflammation and mild cells in the vitreous body 2-10 weeks following uncomplicated cataract surgery and IOL implantation into the capsular bag. These clinical symptoms were relatively mild and mainly seen in the anterior chamber [1]. Prior intravitreal ceftazidime (2mg/0.1mL) and intravitreal vancomycin (2mg/0.1mL) administration was not sufficient for the treatment of CPE in these patients.
Surgical technique
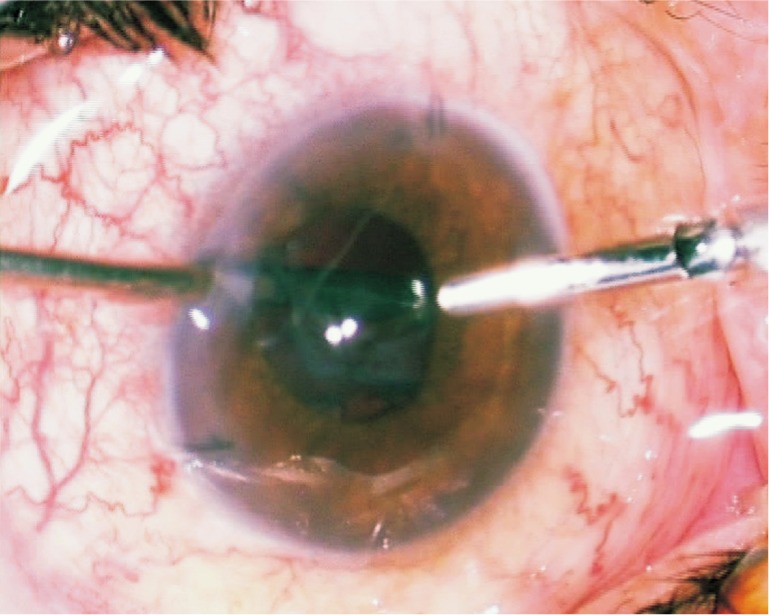
Limbal corneal paracentesis with a 20G microvitreoretinal blade were performed at 2 and 10 o'clock, and an anterior chamber tap was taken with an insulin syringe and an aspiration cannula. The aspirate of about 0.1mL containing cellular debris from the capsular bag was microbiologically evaluated. Next, an anterior chamber maintainer was introduced into the anterior chamber at inferior temporal meridian of the limbal cornea. In case of necessity, posterior synechiae and adhesions between the iris and the optics of the IOL were separated. The vitreous cutter was inserted under the IOL via limbal corneal paracentesis (Figure 1). Then, partial capsulectomy and anterior vitrectomy was performed. After the completion of the vitrectomy, lens capsular bag remnants were irrigated with 10mg/mL vancomycin and 20mg/mL ceftazidime. At the end of the procedure, the incisions were hydrated to ensure tight closure and the anterior chamber was filled. The IOLs were preserved in all cases. Standard antibiotic (moxifloxacin 0.5% q.i.d) and steroid (prednisolone acetate 1% q.i.d) drops were applied postoperatively.
Figure 1. The vitreous cutter was inserted under the IOL via limbal corneal paracentesis.
RESULTS
In the current study, 7 patients presented with a white intracapsular plaque and the remaining 2 patients had chronic inflammation. All patients demonstrated conjunctival injection with minimal vitreous inflammation, and majority had keratic precipitates. Hypopyon was not present in any of patients. Intraocular pressures were in normal limits in all patients.
Demographic data and presenting clinical features of patients are presented in Table 1. Six of 9 patients were male. The average patients' age was (60±8.1) years. The average period between cataract extraction and onset of signs and symptoms was (3.6±1.3) weeks. The average presenting visual acuity was 0.3±0.1 and the average final post operative visual acuity was 0.7±0.2. The main follow-up period was (28.1±8.9) weeks.
Table 1. Demographic data and presenting clinical features of patients.
| Age(a)/ sex | Time from cataract extraction to inflammation (weeks) | Preop VA | Postop VA | Fundus |
| 1.56/M | 2 | 0.4 | 0.8 | Unaffected |
| 2.54/M | 4 | 0.3 | 0.7 | Unaffected |
| 3.61/F | 2 | 0.1 | 0.5 | CME |
| 4.67/F | 3 | 0.3 | 0.8 | Unaffected |
| 5.43/M | 4 | 0.4 | 1.0 | Unaffected |
| 6.70/F | 6 | 0.2 | 0.5 | AMD |
| 7.63/M | 4 | 0.5 | 0.8 | Unaffected |
| 8.61/M | 3 | 0.4 | 0.6 | CME |
| 9.65/M | 5 | 0.2 | 0.7 | Drusen |
AMD: Age-related macular degeneration; CME: Cystoid macular oedema; VA: Visual acuity.
In all patients, the inflammation subsided after anterior vitrectomy and partial capsulectomy via anterior approach. The visual acuity improved markedly in all patients. None of the patients required further surgery. During the follow-up, cystoid macular edema continued in two patients. No further complications such as retinal detachment, IOL dislocation, bullous keratopathy or glaucoma were recorded in the follow-up period. The microbiologic examinations revealed a positive finding in only one of nine patients. In this case, Stafilococus epidermidis, sensitive to vancomycin was cultured.
DISCUSSION
Chronic postoperative endophthalmitis is an important cause of chronic, recurrent inflammation in pseudophakic eyes caused by organisms sequestered between the IOL and posterior capsular bag at the equator [4]. Propionibacterium acnes is the most commonly isolated organism, with others such as Acinetobacter calcoaceticus, Torulopsis candida, Corynebacterium minutissimum, Alcaligens xylosoxidans being reported occasionally [4]. The binding of bacteria on the surface of the IOL during implantation is known to play a main role in the pathogenesis of the disease [8]. Scanning electron microscopy has been used to demonstrate bacterial adherence to the IOL in studies of pseudophakic endophthalmitis [9].
A white inflammatory lesion within the peripheral capsular bag has been associated with CPE, along with severe conjunctival injection, keratic precipitates and vitritis [10]. However, in a number of patients, the inflammatory response seems quite clearly restricted to the anterior segment, with only mild vitreous opacification, corresponding to grade 1 cellular infiltration in the vitreous [11]. To minimize the surgical procedure and thus further trauma to the eye such patients were selectively chosen for the present study.
Management of CPE can be difficult for several reasons. The intraocular inflammation may resemble sterile postoperative inflammation during its early stages and may be suppressed temporarily with topical steroids. Because many of these infections occur in cases when the posterior capsule is intact, the organisms are able to grow in an anaerobic environment, isolated from host defenses [10]. Because the organisms become sequestered within the capsular bag, adequate drug levels may not be present for sufficient time to kill the organism even after injection of antibiotics into the capsular bag [6].
No true consensus exists regarding the most appropriate treatment method for CPE; thus, patients are treated by variety of methods [6]. The choice of initial therapy may influence the recurrences of inflammation but does not appear to significantly affect the final visual acuity [12]. Two important retrospective studies, by Clark et al [10] and Aldave et al [6] demonstrated that the injection of intravitreal antibiotics alone is associated with a very high rate of endophthalmitis recurrence. Antibiotics were injected either directly into the capsular bag or injected simultaneously into the aqueous and vitreous in a “two compartment” approach [6]. Schlichtenbrede et al [11] suggested that capsular bag irrigation with an antibiotic enriched irrigation solution resulted in a cessation of the intraocular inflammation in all patients with CPE following uncomplicated routinely performed cataract surgery.
Rojo et al [13] treated the patients with symptoms of CPE after extracapsular cataract extraction, with an IOL following a protocol that included: YAG capsulotomy, vitreal aspiration and intravitreal injection of antibiotics. In all cases the inflammatory process decreased, and a noticeable improvement of visual acuity was achieved. No recurrent cases were observed. They stated that the initial capsulotomy allows the destruction of the infection reservoir in order to eradicate the agent. Clark et al [10] reported that treatment strategies consisting intraocular antibiotic injection alone or vitrectomy without capsulectomy were associated with persistent intraocular inflammation. PPV and partial capsulectomy without IOL exchange is another initial treatment strategy. PPV, total capsulectomy, and the removal or exchange of the IOL is also an effective treatment. It can be performed as initial therapy or is a successful strategy in patients with recurrent intraocular inflammation [6],[10].
In this study, overall visual outcomes were favorable and comparable to the previous reports of chronic endophthalmitis. This method was effective to control the CPE in 9 of 9 patients. In the majority of the patients, visual acuity improved markedly. With this less invasive procedure, a rapid resolution of the inflammatory response was achieved. Initial surgical approach by anterior vitrectomy with partial capsulectomy may offer theoretical advantages over PPV only or PPV with total capsulectomy and IOL removal. This treatment strategy allows removal of localized infectious sources while leaving enough capsular support for the IOL. It also provides less surgical manipulation and avoids the potentially more serious complications of IOL exchange or removal. In addition, this approach allows earlier visual rehabilitation and eliminates the need for aphakic correction. Any cataract surgeon will be able to perform this method without help from the vitreoretinal colleague. The procedure may therefore, be considered as a potentially useful first-line approach in the treatment of CPE.
On the other hand, our method has some shortcomings. The presented case series is a retrospective study, thus all limitations of subjectivity or comparability which hamper non-randomized and non-prospective trials apply. The number of patients was relatively small. The patients in this study were presented with whitish precipitates in the capsular bag and anterior chamber inflammation and mild cells in the vitreous body. These findings mainly represented low-grade (or chronic) postoperative endophthalmitis. Therefore, we think that our results cannot be generalized to acute fulminant post cataract surgery endophthalmitis. In undilated pupils or pupils with posterior synechiae it may be difficult to perform this method. Overall careful patient selection seems to be the most important factor for successful anterior vitrectomy and partial capsulectomy.
Microbiologic examinations in our study revealed a positive finding in only one of nine patients. In this case, Stafilococus epidermidis, sensitive to vancomycin was cultured. On the other hand P. acnes is the most commonly isolated organism in the CPEs. The diagnosis of P. acnes infection in endophthalmitis can be difficult because the culture results from the aqueous humor are usually negative due to the slow growth rate of P acnes and also possibly due to the sequestered state of the organisms in the remaining capsular bag [14]. Its generation time for doubling is 5.1 hours, compared with 24 minutes for S. aureus. As a result, the average time to positive culture is often between 8 and 10 days, which is longer than the 5 days most laboratories hold bacterial cultures [14]. Polymerase chain reaction (PCR) has been shown to be a more sensitive method than culturing to detect intraocular P. acnes infection in aqueous and vitreous samples from cases of delayed-onset endophthalmitis [15]. Since we could not get positive culture results for P. acnes, we might have done PCR analysis of the samples, instead of culturing them. In conclusion our results suggest that anterior vitrectomy and partial capsulectomy via anterior approach may be considered as potentially useful and relatively less invasive technique to treat CPE. It may avoid removal of the IOL and thus prevents the need for visual rehabilitation, and may also decrease the surgical risks of more complex procedures.
REFERENCES
- 1.Rogers NK, Fox PD, Noble BA, Kerr K, Inglis T. Agressive management of an epidemic of chronic pseudophakic endophthalmitis: results and literature survey. Br J Ophthalmol. 1994;78(2):115–119. doi: 10.1136/bjo.78.2.115. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Horster S, Bader L, Seybold U, Eschler I, Riedel KG, Bogner JR. Stenotrophomonas maltophilia induced post-cataract-surgery endophthalmitis: Outbreak investigation and clinical courses of 26 patients. Infection. 2009;37(2):117–122. doi: 10.1007/s15010-008-8150-8. [DOI] [PubMed] [Google Scholar]
- 3.Haimann MH, Weiss H, Miller JA. Delayed onset pseudophakic endophthalmitis. Am J Ophthalmol. 1991;111(5):656–657. doi: 10.1016/s0002-9394(14)73722-5. [DOI] [PubMed] [Google Scholar]
- 4.Gopal L, Nagpal A, Verma A. Direct aspiration of capsular bag material in a case of sequestered endophthalmitis. Indian J Ophthalmol. 2008;56(2):155–157. doi: 10.4103/0301-4738.39125. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Buggage RR, Shen DF, Chan CC, Callanan DG. Propionibacterium acnes endophthalmitis diagnosed by microdissection and PCR. Br J Ophthalmol. 2003;87(9):1190–1191. doi: 10.1136/bjo.87.9.1190. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Aldave AJ, Stein JD, Deramo VA, Shah GK, Fischer DH, Maguire JI. Treatment strategies for postoperative propionibacterium acnes endophthalmitis. Ophthalmology. 1999;106(2):2395–2401. doi: 10.1016/S0161-6420(99)90546-8. [DOI] [PubMed] [Google Scholar]
- 7.Yam JC, Kwok AK. Update of the management of postoperative endophthalmitis. Hong Kong Med J. 2004;10(5):337–343. [PubMed] [Google Scholar]
- 8.Lai JY, Chen KH, Lin YC, Hsu WM, Lee SM. Propionibacterium acnes DNA from an explanted intraocular lens detected by polymerase chain reaction in a case of chronic pseudophakic endophthalmitis. J Cataract Refract Surg. 2006;32(3):522–525. doi: 10.1016/j.jcrs.2005.12.071. [DOI] [PubMed] [Google Scholar]
- 9.Busin M, Cusumano A, Spitznas M. Intraocular lens removal from eyes with chronic low-grade endophthalmitis. J Cataract Refract Surg. 1995;21(6):679–684. doi: 10.1016/s0886-3350(13)80566-4. [DOI] [PubMed] [Google Scholar]
- 10.Clark WL, Kaiser PK, Flynn HW, Belfort A, Miller D, Meisler DM. Treatment strategies and visual acuity outcomes in chronic postoperative Propionibacterium acnes endophthalmitis. Ophthalmology. 1999;106(9):1665–1671. doi: 10.1016/S0161-6420(99)90348-2. [DOI] [PubMed] [Google Scholar]
- 11.Schlichtenbrede FC, Spandau UH, Harder B, Jonas JB. Lens capsular bag irrigation for low-grade endophthalmitis. Graefes Arch Clin Exp Ophthalmol. 2009;247(9):1273–1276. doi: 10.1007/s00417-009-1085-7. [DOI] [PubMed] [Google Scholar]
- 12.Song S, Ahn JK, Lee GH, Park YG. An epidemic of chronic pseudophakic endophthalmitis due to Ochrobacterium anthropi: clinical findings and management of nine consecutive cases. Ocul Immunol Inflamm. 2007;15(6):429–434. doi: 10.1080/09273940701798546. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Rojo A, Ferrer E, Torrón C, Villuendas MC, Ruiz O, Pablo L, Honrubia FM. Nd-YAG capsulotomy and intravitreal antibiotics as treatment of chronic endophthalmitis. Arch Soc Esp Oftalmol. 2000;75(2):109–116. [PubMed] [Google Scholar]
- 14.Hall GS, Pratt-Rippin K, Meisler DM, Washington JA, Roussel TJ, Miller D. Growth curve for Propionibacterium acnes. Curr Eye Res. 1994;13(6):465–466. doi: 10.3109/02713689408999875. [DOI] [PubMed] [Google Scholar]
- 15.Lohmann CP, Linde HJ, Reischl U. Improved detection of microorganisms by polymerase chain reaction in delayed endophthalmitis after cataract surgery. Ophthalmology. 2000;107(6):1047–1051. doi: 10.1016/s0161-6420(00)00083-x. [DOI] [PubMed] [Google Scholar]


