Abstract
Streptococcus pyogenes is a leading cause of pharyngeal infection, with an estimated 616 million cases per year. The human nasopharynx represents the major reservoir for all S. pyogenes infection, including severe invasive disease. To investigate bacterial and host factors that influence S. pyogenes infection, we have devised an improved murine model of nasopharyngeal colonization, with an optimized dosing volume to avoid fulminant infections and a sensitive host strain. In addition we have utilized a refined technique for longitudinal monitoring of bacterial burden that is non-invasive thereby reducing the numbers of animals required. The model was used to demonstrate that the two component regulatory system, CovR/S, is required for optimum infection and transmission from the nasopharynx. There is a fitness cost conferred by covR/S mutation that is specific to the nasopharynx. This may explain why S. pyogenes with altered covR/S have not become prevalent in community infections despite possessing a selective advantage in invasive infection.
Introduction
Streptococcus pyogenes is estimated to cause 616 million cases of pharyngeal infection per year, and 663,000 cases of invasive disease [1]. As the human nasopharynx represents the major reservoir for all types of S. pyogenes infection, it is essential to develop a better understanding of the factors that influence upper respiratory tract infection.
Despite their limitations, mice play an important role in infectious diseases research [2]. The mouse nasopharynx has structural similarities to the nasal turbinate system in humans [3], although mice lack tonsils [4]. Instead, mice possess nasal associated lymphoid tissue (NALT), which shares some similarity to the tonsils [5] and has been shown to be a target for infection by S. pyogenes [6]. Indeed, mice have been used by several groups to investigate S. pyogenes in the upper respiratory tract, although there is no consensus on which is the most appropriate strain, sex or age of animal to use [6], [7], [8], [9], [10]. Furthermore, the maximum dose volume posited for establishing infection by previous studies ranges from 5 µl, as determined by administration of colored dye [8], [11], 10 µl as determined by radioactive microspheres [10], [12], to 20 µl volumes [6]. This is an important consideration, as aspiration of the bacteria into the lungs has the potential to trigger a more invasive disease and systemic infection.
It is known that phenotypic differences can exist between nasopharyngeal and invasive S. pyogenes isolates, and these have been ascribed to altered activity or mutation of the streptococcal two component regulatory system, covR/S [13]. As a result of signalling from the sensor kinase, CovS, CovR represses a range of virulence factors concerned with resistance to phagocytosis, such as the capsule synthesis operon hasABC, the DNase, sda, and the CXC chemokine protease, SpyCEP [13], [14], [15], [16], [17]. Mutations in covR/S de-repress these virulence genes, conferring a selective advantage to S. pyogenes in mouse models of invasive infection, leading to greater mortality [15], [18]. However, the impact of such mutations on nasopharyngeal infection is unclear. Isolates of S. pyogenes with covS mutations bind less well to skin cells in vitro and in vivo than those without the mutation [19]. Furthermore, S. pyogenes with mutations in covS lack competitiveness in the saliva relative to wild type [20].
In this work, we set out to produce a longitudinally monitored murine model of nasopharyngeal infection, by examining the effect of mouse strain, age and sex on S. pyogenes carriage. We evaluated S. pyogenes pharyngitis isolates from patients rather than a previously-described mouse-pathogenic strain that lacks a functional copy of the multigene activator, mga [21], [22]. The improved nasopharyngeal infection model was used to evaluate the impact of the S. pyogenes CovR/S two component regulatory system on longevity and transmission of S. pyogenes upper respiratory tract infection.
Methods
Ethics Statement
In vivo experiments were performed in accordance with the Animals (scientific Procedures) Act 1986, subject to protocols set out in PPL 70/7379 that were approved by the Imperial College Ethical Review Process (ERP) panel and the UK Home Office.
Bacterial Strains
The bacterial strains used in this study are given in Table 1 [16], [23], [24]. Streptococcal strains were cultured in Todd Hewitt Yeast broth (THY) or on Columbia Blood Agar (CBA), while Luria Bertani (LB) medium was used for culturing C. rodentium ICC180. All strains were grown at 37°C. For animal experiments, S. pyogenes was grown without shaking with 5% CO2 overnight, centrifuged at 1864×g, (Sorvall RTH 750 Rotor), washed twice in phosphate buffered saline (PBS), and re-suspended in PBS to produce an inoculum of 1–7×108 colony forming units (cfu) per 5 µl. Numbers of viable bacteria within the inoculum were retrospectively assessed by plating of 10−6–10−8 dilutions of the inoculum onto agar.
Table 1. Bacterial strains used in this study.
| Strain Designation | Emm type | Species | Description | Ref. |
| H305 | emm1 | S. pyogenes | Scarlet fever reference strain | [23] |
| H343 | emm2 | S. pyogenes | Pharyngitis isolate | [16] |
| H292 | emm81 | S. pyogenes | Blood isolate | [16] |
| H347 | emm75 | S. pyogenes | Pharyngitis isolate | [16] |
| H494 | emm75 | S. pyogenes | Strain H347 with an inactivated covR/S operon | [16] |
| ICC180 | C. rodentium | Bioluminescent derivative of ICC169 | [24] |
Animals
Male and female 5–10 week old CD1, C57BL/6, A/J, BALB/c, FVB/n specific-pathogen free mice (Harlan, UK) were maintained in individually HEPA filtered cages with sterile bedding and free access to sterilized food and water. GLP Mini Fun Tunnels (Lillico), or Des. Res. Mini Mouse Houses (Lillico) were provided in each cage for environmental enrichment.
Intranasal Infection
Pilot experiments were conducted using ∼109 cfu in doses of 2.5 µl–20 µl bioluminescent C. rodentium ICC180 [24] to determine the correct dosing strategy to deliver bacteria to the murine nasopharynx without lung involvement. Bioluminescence (as photons s−1 cm−2 steridian [sr] −1) from living animals was performed as previously described [24] using an IVIS® 100 system (Perkin Elmer).
For streptococcal infection of the nasopharynx, 1–7×108 cfu of S. pyogenes was administered intranasally using a pipette to mice in a volume of 2.5 µl per nostril under 2–5% isoflurane anaesthesia. Mice were weighed daily; reduction by 20% of original weight was a defined humane endpoint.
Intramuscular Infection
6×108 cfu S. pyogenes were administered to mice under isoflurane anaesthesia via injection with a 27 gauge needle into the right lateral thigh. Numbers of viable bacteria within the inoculum were assessed by retrospective plating of 10−6–10−8 dilutions. At 72 hours, the right thigh muscle and ipsilateral inguinal node were extracted, weighed and homogenized into PBS and then plated out onto CBA for bacterial enumeration.
Nasal Sampling
The level of shedding of S. pyogenes from the nasopharynx was assessed longitudinally using direct nasal sampling. The nares of each mouse were gently pressed onto the surface of a CBA plate ten times. Exhaled particulates were streaked out, and the plates were then incubated overnight at 37°C with 5% CO2 for bacterial enumeration. In preliminary experiments using naive, non-infected mice, α-hemolytic streptococci, staphylococci, pseudomonads and corynebacteria were recovered, but no β hemolytic Group A streptococci were found to naturally colonize the mouse nasopharyngeal tract.
For experiments where mice had been infected with S. pyogenes, β-hemolytic colonies were counted for each mouse and confirmed as S. pyogenes through Gram staining, catalase testing, oxidase testing, and Lancefield grouping. No other β-haemolytic bacteria were recovered from the mouse nasopharynx. Kaplan-Meier plots were created to analyse the duration of S. pyogenes shedding. Nasal samples were taken for 21 days post inoculation. Mice were determined to have stopped shedding upon the first instance of a nasal sample turning up negative.
In some studies, the nasopharynx was dissected and removed at fixed time points for microbiological culture. To ensure complete extraction of the nasopharynx, the skin and mandibles were removed to expose the cranium. This was then sectioned along the coronal plane at the bregma. The brain tissue within the cranium anterior to this incision was removed, exposing the posterior aspect of the nasal cavity, known as the cribriform plate. The orbits were removed from this tissue via sagittal incisions lateral to the pre-maxilla. The remaining tissue comprised the entire nasal cavity, and NALT. This was homogenized into PBS and serial dilutions plated onto CBA to quantify S. pyogenes from the whole nasopharynx.
Settle Plates
To detect the presence of airborne bacteria within cages of infected mice, CBA plates were placed in the upper rack of the individually HEPA filtered cages (n = 4 plates per cage) and exposed for defined time periods throughout each experiment. Plates then incubated overnight at 37°C and the numbers of S. pyogenes colonies, (identified by Gram staining, catalase testing, and Lancefield grouping) were enumerated.
Histopathology
The head of each mouse was removed at the atlanto-occipital joint and sagittally hemi-sected. One half was fixed in formalin and processed routinely to paraffin wax, while the other was homogenised and plated to assess S. pyogenes numbers in the nasopharynx. Paraffin sections were cut at 6 µm and stained with Haematoxylin and Eosin and Gram stains. The degree of nasal damage and inflammation was scored as : No significant abnormality (Intact nasal mucosa and absence of inflammation), Mild (Focal erosion of the mucosa with local neutrophil exocytosis across the affected epithelium), Moderate (Focal necrosis and ulceration of the mucosa with local neutrophilic exocytosis and surface neutrophilic exudation), Marked (Extensive necrosis and ulceration of the mucosa with widespread neutrophilic exocytosis and surface neutrophilic exudation) and Severe (Extensive necrosis and ulceration of the mucosa with widespread neutrophilic exocytosis and surface neutrophilic exudation and with extension of necrosis into underlying stroma). Slides were reviewed and scored by an experienced histopathologist (KS).
Statistics
For statistical analysis of Kaplan-Meier curves, the Mantel-Cox Logrank test was applied. For statistical analysis of colony count comparisons, a non-parametric Kruskal-Wallis test and Dunn’s post-test were used. P values less than 0.05 were defined as significant. Statistics were performed using Prism Graphpad version 5.02. Data are presented as median, ± interquartile range.
Results
Volume of Inoculum Determines Distribution within the Respiratory Tract
Bioluminescence imaging demonstrated that dose volumes of 20 µl volume delivered bacteria to the lungs, whereas this was not shown with lower volumes (Figure 1). Any dose volume above 10 µl was deposited in the trachea. Dose volumes of 5 µl and 2 µl did not distribute bacteria to the lungs. As the optimal dose volume for nasopharyngeal deposition without lung involvement or significant nasal clearance was 5 µl (2.5 µl per nostril), this was the volume used in subsequent experiments.
Figure 1. Bioluminescence imaging of bacterial distribution after intranasal inoculation with bioluminescent C.rodentium.

109 colony forming units (cfu) of bioluminescent C. rodentium were administered intranasally to 8 week old CD1 outbred female mice in 20 µl (n = 3), 10 µl (n = 2), 5 µl (n = 3) and 2.5 µl (n = 2) of PBS. Images were acquired using an IVIS spectrum system, and are displayed as images of peak bioluminescence, with variations in colour representing light intensity at a given location. Red represents the most intense light emission, while blue corresponds to the weakest signal. The colour bar indicates relative signal intensity (as photons s−1 cm2 sr−1). Two representative mice shown for each group.
Nasopharyngeal Shedding as a Method to Longitudinally Monitor S. pyogenes Infection in the Upper Respiratory Tract
To select an appropriate bacterial strain for development of the model, BALB/c mice were intranasally inoculated with four clinical S. pyogenes strains of different emm genotypes. An emm75 pharyngitis strain was found to have shed for the longest period using direct nasal sampling (Table 2) and was used in subsequent experiments. Importantly, a significant correlation was found between the numbers of colonies recovered from nasal shedding of S. pyogenes and bacterial numbers from dissected and homogenised nasal tissue on the same day (Figure 2, r2>0.95, n = 36). This longitudinal method of monitoring was therefore employed in subsequent experiments consistent with the principles of the 3Rs (Replacement, Refinement, and Reduction) by reducing the numbers of animals used.
Table 2. Duration of shedding of different strains of S. pyogenes (7×108 cfu per 5 µl dose) in 8 week old male BALB/c mice after intranasal infection.
| Number of mice shedding S. pyogenes | |||
| Day 1 | Day 2 | Day 3 | |
| emm 1 | 0/7 | 0/7 | 0/7 |
| emm 2 | 1/7 | 1/7 | 1/7 |
| emm75 | 4/7 | 3/7 | 2/7 |
| emm 81 | 1/7 | 0/7 | 0/7 |
Figure 2. Correlation between S. pyogenes recovered from nasal shedding and from nasopharyngeal dissection.
Data are pooled from direct nasal samples taken on days 3, 7, and 14 from five week old female FVB/n mice during intranasal infection with emm75 S. pyogenes (1.3×108 cfu) were compared to bacterial numbers obtained on dissection on the same days. (r2>0.95, n = 36). Data shown from individual mice.
Longevity of Nasopharyngeal Shedding is Greater in FVB/n Mice
To determine the most appropriate mouse strain for model development, male mice of different host backgrounds were infected intranasally with emm75 S. pyogenes, and observed longitudinally for 72 h using direct nasal sampling. Data were used to create Kaplan Meier plots to analyse the duration of shedding for each strain of mouse (Figure 3 A). FVB/n mice carried S. pyogenes longer and shed significantly more S. pyogenes on the final day of the time course than all other strains tested (Figure 3 B). FVB/n mice carried S. pyogenes were therefore used for all future studies.
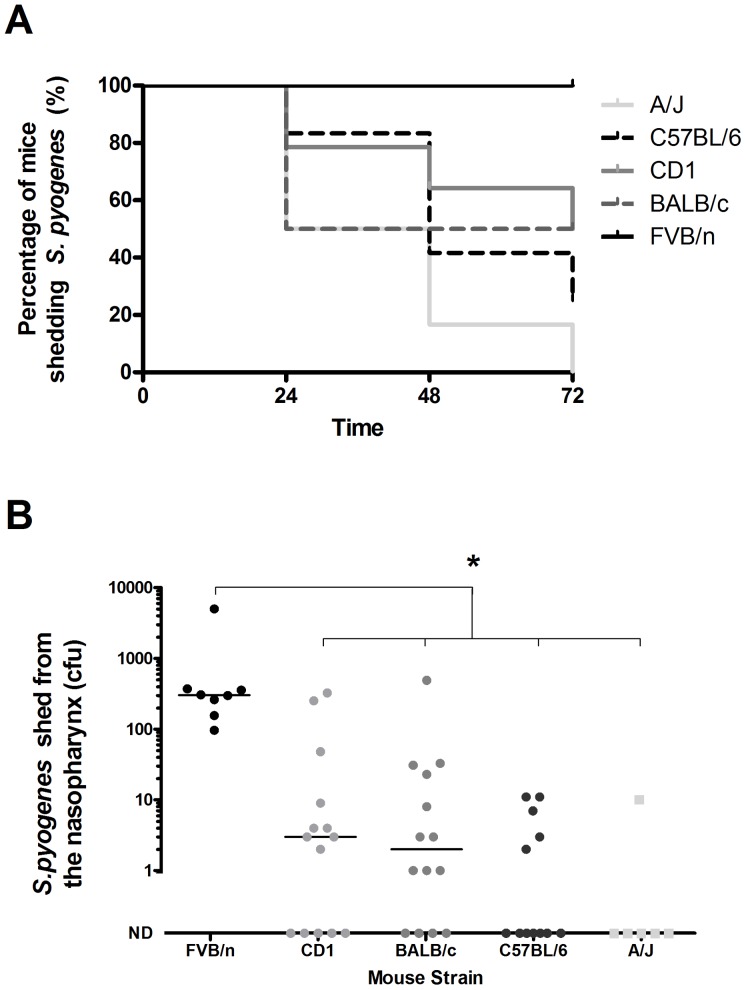
Figure 3. Comparison of nasopharyngeal shedding of S. pyogenes between different mouse strains.
Five week old male mice of different strain backgrounds were inoculated intranasally with emm75 S. pyogenes (1.5×108 cfu). Duration and quantity of shedding were determined from colonies recovered from direct nasal sampling of the mouse nasopharynx. (A) Kaplan-Meier plot showing percentage of mice shedding S. pyogenes in each group. (B) Bacterial counts shed by FVB/n (n = 8) CD1 (n = 14), BALB/c (n = 14), C57BL/6 (n = 12) and A/J (n = 6) at 72 hours. Individual points represent individual mice. (Kruskal Wallis with Dunns Post Test p<0.05). Bars indicate the median, ND = no detectable bacteria.
Gender has an Effect on the Nasopharyngeal Carriage of S. pyogenes that is Dependent on the Age of the Mice
To determine whether gender influenced S. pyogenes infection of the nasopharynx, peri pubertal (n = 10 per group, 5 per cage, 5 weeks of age) and post pubertal (n = 10 per group, 5 per cage, 10 weeks of age) male and female FVB/n mice were intranasally inoculated with S. pyogenes. There was no significant difference in infection duration between 5 week old males and females over a 21 day period (Figure 4, Logrank p>0.05), whereas 10 week old males shed S. pyogenes for significantly longer than 10 week old female mice (Figure 5, Logrank test p<0.05). However, the older males had to be housed separately to prevent intraspecific aggression and for this reason further experiments were conducted using female mice.
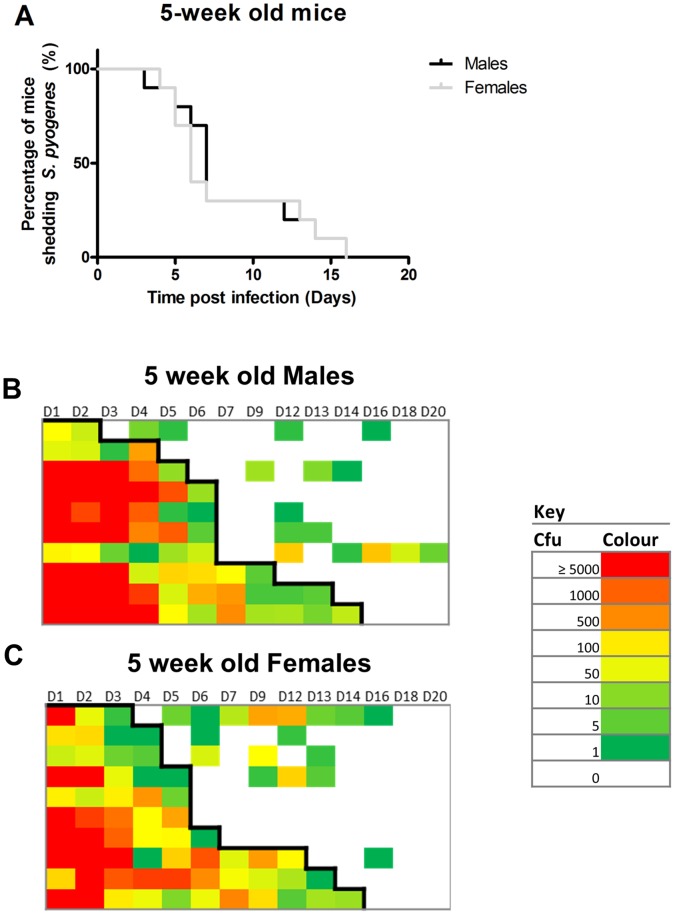
Figure 4. Sex differences in S .
pyogenes nasopharyngeal carriage and shedding intensity in 5 week old mice. Male and female FVB/n mice 5 weeks (A, p>0.05 Mantel–Cox Logrank test, n = 10) of age were infected intranasally with emm75 S. pyogenes (1.1×108 cfu) and sampled non-invasively through direct nasal sampling over 21 days. Shedding intensity maps display the data from direct nasal samples throughout the time course from the male mice (B) and the female mice (C). Rows indicate individual mice throughout the time course, colours indicate the numbers of S. pyogenes recovered from direct nasal samples with red indicating the highest recorded levels of carriage (≥5000 cfu) and green indicates the lowest levels of carriage (1 cfu) and blank blocks indicate no recovery of S. pyogenes. Black line indicates survival based on the first loss of carriage.
Figure 5. Sex differences in S.
pyogenes nasopharyngeal carriage and shedding intensity in 10 week old mice. Male and female FVB/n 10 weeks (A, p<0.05 Mantel–Cox Logrank test, n = 10) of age were infected intranasally with emm75 S. pyogenes (1.1×108 cfu) and sampled non-invasively through direct nasal sampling over 21 days. Male mice carried S. pyogenes for significantly longer than the female mice in this age group. Shedding intensity maps display the data from direct nasal samples throughout the time course from the male mice (B) and the female mice (C). Rows indicate individual mice throughout the time course, colours indicate the numbers of S. pyogenes recovered from direct nasal samples with red indicating the highest recorded levels of carriage (≥5000 cfu) and green indicates the lowest levels of carriage (1 cfu) and blank blocks indicate no recovery of S. pyogenes. Black line indicates survival based on the first loss of carriage.
ΔcovR/S Mutation is Detrimental to Long Term S. pyogenes Infection of the Nasopharynx
Two groups of FVB/n female mice (n = 20, 5 per cage) were infected intranasally with 5 µl of 108 cfu of emm75 S. pyogenes or an isogenic ΔcovR/S strain and observed over 21 days. Kaplan Meier analysis of daily nasal samples demonstrated that the ΔcovR/S strain was shed from the nasopharynx for a shorter length of time compared to its wild type counterpart. (Figure 6, Mantel Cox Logrank p<0.05).
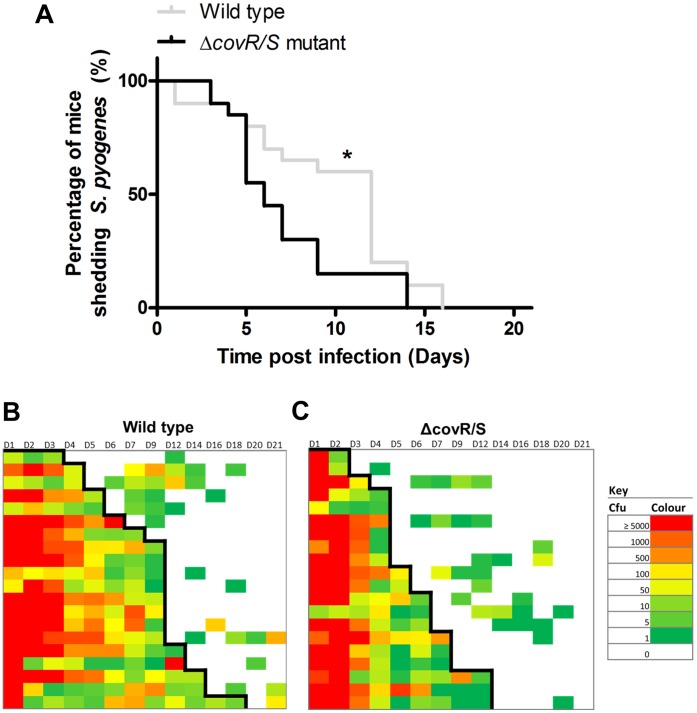
Figure 6. Nasopharyngeal infection is adversely affected by covR/S mutation.
Five week old female FVB/n mice were inoculated intranasally with either emm75 S. pyogenes, or ΔcovR/S S. pyogenes. To determine the duration of shedding, direct nasal samples were taken over a 21 day period. The wild type strain was shed over a significantly longer time period than the ΔcovR/S strain (A, 1.5×108 cfu per dose, n = 20 per group, Logrank Mantel Cox p<0.05). Shedding intensity maps display the data from direct nasal samples throughout the time course from the groups infected with the wild type emm75 strain (B) and the mice infected with the ΔcovR/S strain (C). Rows indicate individual mice throughout the time course, colours indicate the numbers of S. pyogenes recovered from direct nasal samples with red indicating the highest recorded levels of carriage (≥5000 cfu) and green indicates the lowest levels of carriage (1 cfu) and blank blocks indicate no recovery of S. pyogenes. Black line indicates survival based on the first loss of carriage.
We considered the possibility that the reduced longevity of infection reflected a general fitness defect in the ΔcovR/S strain. However, following intramuscular infection of groups of mice with each strain, both the ΔcovR/S strain and wild-type strain survived equally well within the thigh muscle (n = 12 per group, 6 per cage, Figure 7 A). Furthermore the ΔcovR/S strain disseminated to the ipsilateral inguinal lymph node in greater numbers than the wild-type (Figure 7 B, p<0.05 Mann-Whitney), consistent with the predicted phenotype of a ΔcovR/S strain. Streptococci were detected in the liver (Figure 7 C) and in the spleen (Figure 7 D), but these differences were not significant.
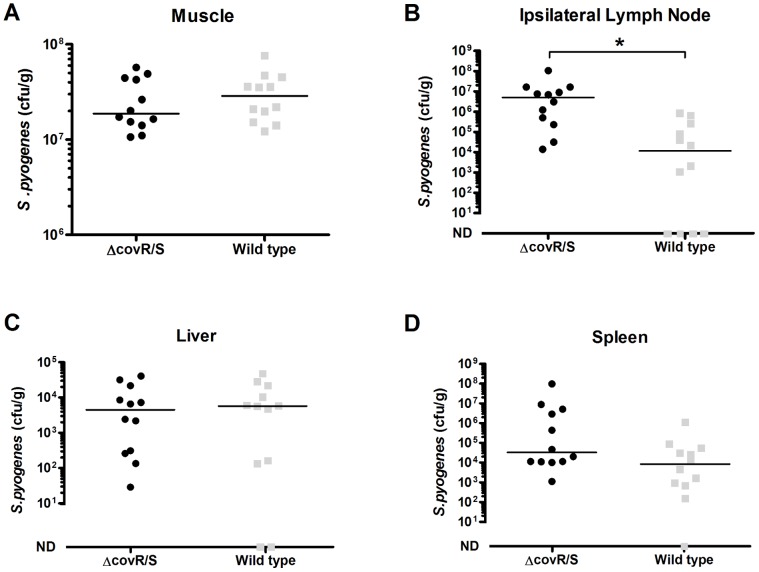
Figure 7. The effects of covR/S mutation on dissemination from an invasive intramuscular infection.
Five week old FVB/n female mice (n = 12) were infected intramuscularly in the right thigh with either wild type S. pyogenes or an isogenic ΔcovR/S strain (6×108 cfu per dose). After three days there was no significant difference in bacterial growth within the thigh (A, Mann Whitney U p>0.05), but there was a significant difference in bacterial numbers that had disseminated to the inguinal node (B, Mann Whitney U p<0.05). No significant difference in dissemination to the liver (C) and the spleen (D) was found between the wild type and the ΔcovR/S strains. Median indicated by a black line.
Intranasal Administration of S. pyogenes Results in a Suppurative Upper Respiratory Tract Infection that Resolves Over 21 Days
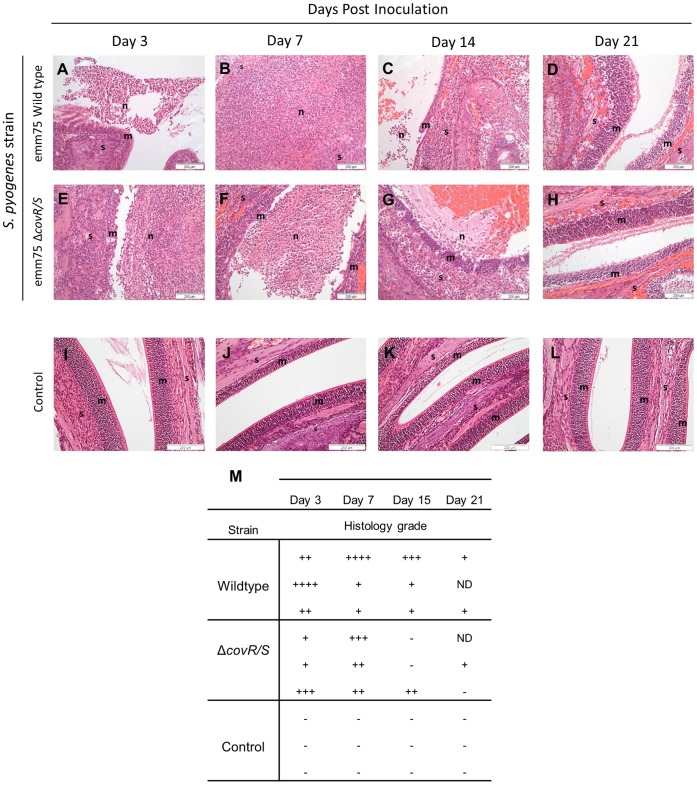
5 week old female FVB/n mice infected with emm75 S. pyogenes demonstrated inflammatory changes affecting the nasal cavity over the first week of infection (Figure 8, A–D), particularly in the caudal (ethmoturbinate) region. A moderate to marked suppurative rhinitis with complete erosion or ulceration of the nasal mucosa and neutrophilic exudate on the mucosal surface was observed. On days 3 and 7, mice occasionally demonstrated necrosis of underlying turbinate bone and extension of inflammation and infection across the cribriform plate, resulting in a localized meningoencephalitis affecting the olfactory bulbs (data not shown). However, by Day 21, the inflammatory damage to the nasal mucosa had resolved. The S. pyogenes ΔcovR/S strain elicited a similar inflammatory response (Figure 8, E–H), albeit over a slightly shorter time period. Mice demonstrated mild to marked suppurative rhinitis at days 3 and 7 that resolved by day 14. Both strains of S. pyogenes could be recovered from cultures of the nasopharynx from mice even after the inflammation resolved (Data not shown). Semi quantitative assessment of sections from mice infected with both the wild type and ΔcovR/S emm75 strains were undertaken in comparison with control sections from uninfected mice; this demonstrated that the observed inflammation decreased throughout the time course consistent with the lowering of the bacterial load (Figure 8 I–M).
Figure 8. Histopathological analysis of the caudal nasal cavity during long term nasal infection.
Photomicrographs demonstrating five week old female FVB/n mice infected with either the emm75 S. pyogenes (A–D) or the emm75 ΔcovR/S strain (E–H) (1.5×108 cfu per dose, n = 3 per group) were taken at days 3, 7, 14 and 21 after inoculation (Haemotoxylin & Eosin staining). n = Neutrophilic Exudate, m = Nasal mucosa, s = Nasal stroma. Scale bar as shown. Damage to the nasal mucosa with surface neutrophilic exudate was apparent at day 3 post inoculation with both strains (A & E). The nasal epithelia of mice in both groups were widely eroded or ulcerated by day 7 (B) than those infected with the ΔcovR/S strain (F). At day 14 the inflammation had begun to resolve in both strains (C & G). By day 21, mice in all groups had histologically normal mucosa (D & H). Control mice over the time course are shown in (I–L). Semi quantitative analysis of the histopathology was undertaken to determine the severity of infection and assigned a numerical designation for each time point (n = 3 mice per time point). − = No significant abnormality,+ = Mild,++ = Moderate,+++ = Marked,++++ = Severe and ND = Non diagnostic sections (M).
Transmission of S. pyogenes within a Mouse Cage is Dependent on the Proportion of Infected Donor Mice Present
Preliminary work showed that S. pyogenes shed by infected mice could lead to the infection of uninfected mice in the same cage. Transmissibility of S. pyogenes in the nasopharynx was formally investigated through introducing infected donor mice into cages of uninfected recipient mice (n = 8 per cage). The effect of varying the ratio of donor to recipient (D:R) mice present in a cage on transmission was evaluated.
Within 4 hours of donor introduction transmission occurred to all recipients. A higher D:R ratio resulted in greater counts of S. pyogenes cultured from recipient mice in those cages. Recipient mice in the cage with a D:R ratio of 4∶4 had significantly more bacteria in the nasopharynx compared to mice in the cage with a D:R ratio of 2∶6 (Figure 9 p<0.05).
Figure 9. Density of infected carriers determines the burden of transmitted infection.
Five week old female FVB/n donor mice infected intranasally with S. pyogenes (1.63×108 cfu per dose) were introduced into a cage of naïve recipient female mice. The Donor: Recipient (D:R) ratio was varied between 4∶4, 3∶5 and 2∶6 between cages. Recipient mice were sampled at 4, 24, 48, 72 and 96 hours after the infection and introduction of the donor mice to a cage. Data show counts from direct nasal sampling from recipient mice only. Donor mice had >5000 cfu recovered at all time points (not shown). The burden of transmitted infection was significantly higher in cages with a D:R ratio of 4∶4 compared with cages with a 2∶4 ratio. (AUC analysis, followed by Kruskal Wallis with Dunns Post test p<0.05). Lines indicate the median and the interquartile range.
ΔcovR/S Mutation is Detrimental to the Transmission of S. pyogenes in a Mouse Model
Mice were observed over the first three days of infection, when shedding of the wild-type and the ΔcovR/S strain were shown to be similar, to determine whether a mutation in covR/S affects transmission.
Female FVB/n mice infected with either the wild-type or the ΔcovR/S strains were introduced into cages at a D:R ratio of 3∶5. After inoculation, the infected mice were separated for six hours before being introduced to the recipients, to prevent passive inoculum transfer. Direct nasal samples were taken from recipient mice over three days after the introduction of the donor mice.
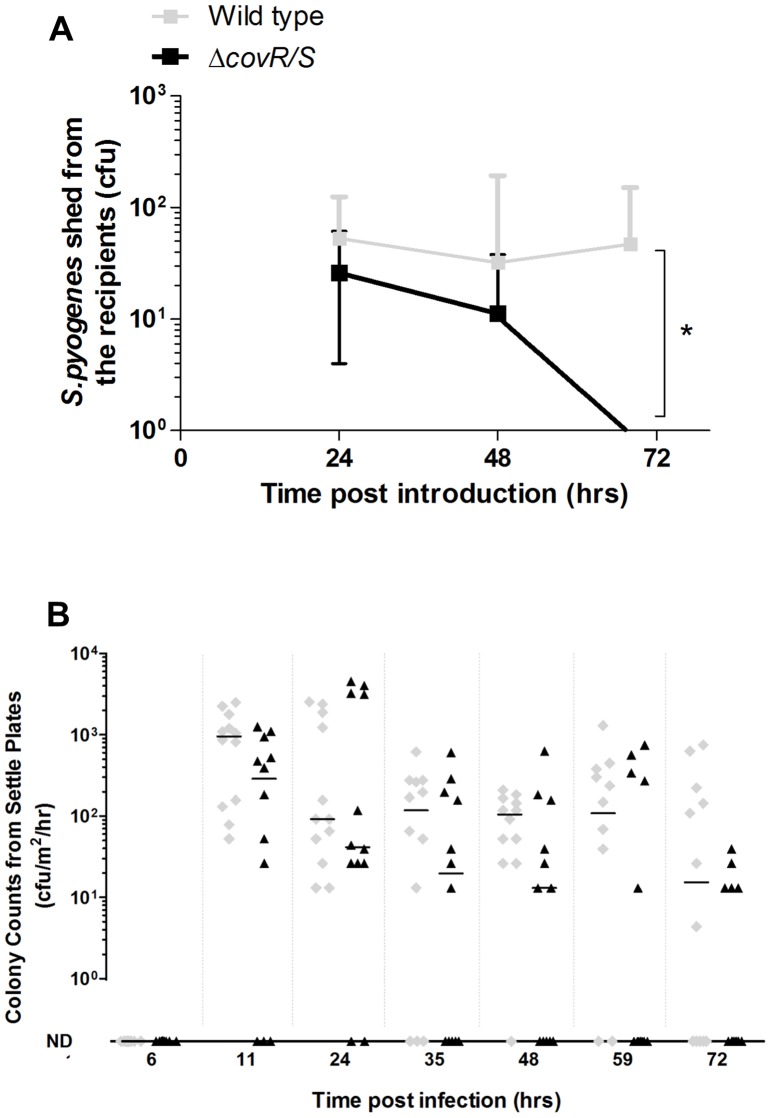
Recipient mice housed with donor mice carrying wild type S. pyogenes acquired significantly more bacteria over the time course than the recipient mice housed with donor mice carrying the ΔcovR/S strain (Figure 10 A, AUC analysis, with Mann Whitney U p<0.05).
Figure 10. Transmission of S. pyogenes is hampered by loss of covR/S regulation.
Naïve five week old female FVB/n recipients co-mingled at a D:R ratio of 3∶5 with female FVB/n mice infected with either the emm75 wild type strain or it’s isogenic ΔcovR/S strain (5 ×108 cfu per dose) and sampled after the introduction of the donor mice. Donor mice had >5000 cfu recovered from direct nasal sampling throughout the experiment. The ΔcovR/S strain transmitted significantly less well to recipients compared to the wild type strain (A, n = 15 recipients per group, AUC analysis, followed by Mann-Whitney U test). Line indicates median, error bars indicate interquartile range. Settle plates exposed to the air in the cages revealed no significant differences in the bacteria deposited on the surface of the plates by mice infected with the strain, or the ΔcovR/S strain (B, n = 4 plates per cage, AUC analysis followed by Mann-Whitney U test p>0.05) Data is shown for individual animals with medians indicated by black line.
There was no statistically significant difference in the abundance of airborne S. pyogenes in the cages of mice infected with the wild-type compared with the cages of mice infected with the ΔcovR/S strain. (Figure 10 B, AUC analysis with Mann Whitney U p>0.05).
Discussion
To facilitate the investigation of bacterial and host factors that influence S. pyogenes in nasopharyngeal infection, an improved, new model of nasopharyngeal colonisation was devised, with an optimised dosing volume to avoid fulminant infections. A non-invasive method of longitudinal monitoring was developed that does not require culling of mice at multiple time points, thus reducing the numbers of animals used.
An emm75 strain of S. pyogenes was found in preliminary experiments to be carried better than other emm types by BALB/c mice, although previous studies have however found that the BALB/c strain is more resistant to infection than other strains [9]. A number of mouse strains were therefore tested in this study, of which the FVB/n was found to be the most susceptible to S. pyogenes intranasal infection. Emm types 1, 2, 3, 4, 6, 12, 22 and 89 were also successfully carried by FVB/n mice (data not shown), although in some cases causing a far more severe disease than the emm75 strain, making them unsuitable for long term infection studies.
We found that gender had an impact on susceptibility to carriage in post pubertal mice only. Data were consistent with other published work demonstrating an increase in susceptibility to infection in male mice [9], [25]. However, the intraspecific aggression expressed by males of this strain made them difficult to house in groups, and thus the older individuals were housed individually. In previous studies, housing mice singly has been demonstrated to increase immune responses [26], [27], [28], and would theoretically increase their resistance to infection.
Histological analysis during infection revealed that nasal shedding of S. pyogenes was associated with on-going inflammation that subsided in the second and third weeks of infection. Previous studies have demonstrated bacterial infection of the mouse NALT [6]. However this study focussed on the site of infection in the deeper nasal passages, which demonstrated a suppurative rhinitis. Studies have shown that S. pyogenes distributes to the ethmoid sinuses in humans during rhinosinusitis [29], [30].
The model was used to demonstrate that a functional covR/S is required for optimum infection and transmission from the nasopharynx. The failure of the ΔcovR/S strain to survive in the mouse nasopharynx was not due to a consistent fitness burden, since in invasive infection, the covR/S strain disseminated in significantly greater numbers than the wild type bacteria to the inguinal lymph node.
During preliminary experiments, we became aware that individual mice occasionally became re-infected after clearing the initial infection. To address transmission, and the factors that may influence this, co-mingling experiments were conducted. These demonstrated that transmission occurred as early as 4 hours post introduction, and the numbers of bacteria recovered from the nares of the recipients increased as the number of infected donor mice in the cage was increased. Importantly, such transmission events may not necessarily constitute a productive infection, as S. pyogenes did not reach the same abundance in recipient mice as observed in donor mice.
Co-mingling was then used to examine the impact of covR/S on transmission. Despite the fact that the infection burden (as measured by direct nasal sampling) was similar between the two donor groups in the first 72 h, recipients housed with donor mice carrying the ΔcovR/S were demonstrated to have a shorter shedding duration than the recipient mice housed with the donors carrying the wild type strain.
Furthermore, despite some differences between the experimental groups, settle plates placed in each cage revealed no significant difference in aerosolization between the two strains. This suggests that the impairment of the covR/S primarily affects the survival of S. pyogenes in the nasopharynx after the initial transmission event has taken place.
There is thus a fitness cost conferred by covR/S mutation specific to the nasopharynx that may explain why such bacteria have not become prevalent in community S. pyogenes pharyngitis despite being advantageous in invasive infection.
The model described represents a refinement of previous systems to study upper respiratory tract infection by S. pyogenes; the model is non-invasive and allows longitudinal monitoring of bacterial infection, using the same mice throughout the study. Such a model will facilitate research which might otherwise require prohibitively large numbers of animals and could be of importance in future evaluation of vaccines, antimicrobials, as well as the factors that influence transmission.
Funding Statement
This work was supported by the Biotechnology and Biological Sciences Research Council via the Centre for Integrative Mammalian Physiology and Pharmacology [DDDH.PS0618] and the National Centres for Replacement, Refinement and Reduction of Animals in Research. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
References
- 1. Carapetis JR, Steer AC, Mulholland EK, Weber M (2005) The global burden of group A streptococcal diseases. Lancet Infect Dis 5: 685–694. [DOI] [PubMed] [Google Scholar]
- 2. Wiles S, Hanage WP, Frankel G, Robertson BD (2006) Modelling infectious disease–time to think outside the box? Nature Rev Microbiol 4: 307–312. [DOI] [PubMed] [Google Scholar]
- 3. Hillenius WJ (1992) The evolution of nasal turbinates and mammalian endothermy. Paleobiology 18: 17–29. [Google Scholar]
- 4. Slípka J (1988) Palatine tonsils–their evolution and ontogeny. Acta Oto-Laryngol 454: 18–22. [PubMed] [Google Scholar]
- 5. Wu HY, Nguyen H, Russell MW (1997) Nasal lymphoid tissue (NALT) as a mucosal immune inductive site. Scand J Immunol 46: 506–513. [DOI] [PubMed] [Google Scholar]
- 6. Park HS, Francis KP, Yu J, Cleary PP (2003) Membranous cells in nasal-associated lymphoid tissue: a portal of entry for the respiratory mucosal pathogen group A streptococcus. J Immunol 171: 2532–2537. [DOI] [PubMed] [Google Scholar]
- 7. Mannam P, Jones KF, Geller BL (2004) Mucosal vaccine made from live, recombinant Lactococcus lactis protects mice against pharyngeal infection with Streptococcus pyogenes . Infect Immun 72: 3444–3450. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. Jordan RT, Ohno S (1958) Comparative pathological changes in AKR mice following intranasal instillation of tumor cells and streptococci. Cancer Res 18: 47–50. [Google Scholar]
- 9. Medina E, Goldmann O, Rohde M, Lengeling A, Chhatwal GS (2001) Genetic control of susceptibility to group A streptococcal infection in mice. J Infect Dis 184: 846–852. [DOI] [PubMed] [Google Scholar]
- 10.Husmann LK, Dillehay DL, Jennings VM, Scott JR (1996) Streptococcus pyogenes infection in mice. Microb Pathogenesis: 213–224. [DOI] [PubMed] [Google Scholar]
- 11. Bronze MS, McKinsey DS, Beachey EH, Dale JB (1988) Protective immunity evoked by locally administered group A streptococcal vaccines in mice. J Immunol 141: 2767–2770. [PubMed] [Google Scholar]
- 12. Eyles JE, Spiers ID, Williamson ED, Alpar HO (2001) Tissue distribution of radioactivity following intranasal administration of radioactive microspheres. J Pharm Pharmacol 53: 601–607. [DOI] [PubMed] [Google Scholar]
- 13. Sumby P, Whitney AR, Graviss EA, DeLeo FR, Musser JM (2006) Genome-Wide Analysis of Group A Streptococci Reveals a Mutation That Modulates Global Phenotype and Disease Specificity. PLoS Pathog 2: 0041–0049. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Graham MR, Smoot LM, Migliaccio CA, Virtaneva K, Sturdevant DE, et al. (2002) Virulence control in group A Streptococcus by a two-component gene regulatory system: global expression profiling and in vivo infection modeling. Proc Natl Ac Sci U S A 99: 13855–13860. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Kansal RG, Datta V, Aziz RK, Abdeltawab NF, Rowe S, et al. (2010) Dissection of the molecular basis for hypervirulence of an in vivo-selected phenotype of the widely disseminated M1T1 strain of group A Streptococcus bacteria. J Infect Dis 201: 855–865. [DOI] [PubMed] [Google Scholar]
- 16. Turner CE, Kurupati P, Jones MD, Edwards RJ, Sriskandan S (2009) Emerging role of the interleukin-8 cleaving enzyme SpyCEP in clinical Streptococcus pyogenes infection. J Infect Dis 200: 555–563. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Walker MJ, Hollands A, Sanderson-Smith ML, Cole JN, Kirk JK, et al. (2007) DNase Sda1 provides selection pressure for a switch to invasive group A streptococcal infection. Nature Med 13: 981–985. [DOI] [PubMed] [Google Scholar]
- 18. Engleberg NC, Heath A, Miller A, Rivera Starr C, DiRita VJ (2001) Spontaneous mutations in the CsrRS two-component regulatory system of Streptococcus pyogenes result in enhanced virulence in a murine model of skin and soft tissue infection. J Infect Dis 183: 1043–1054. [DOI] [PubMed] [Google Scholar]
- 19. Hollands A, Pence MA, Timmer AM, Osvath SR, Turnbull L, et al. (2010) Genetic switch to hypervirulence reduces colonization phenotypes of the globally disseminated group A Streptococcus M1T1 clone. J Infect Dis 202: 11–19. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Treviño J, Perez N, Ramirez-Peña E, Liu Z, Shelburne SA, et al. (2009) CovS simultaneously activates and inhibits the CovR-mediated repression of distinct subsets of group A Streptococcus virulence factor-encoding genes. Infect Immun 77: 3141–3149. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Hook EW, Wagner RR, Lancefield RC (1960) An epizootic in Swiss mice caused by a group A streptococcus, newly designated type 50. Am J Epidemiol 72: 111–119. [DOI] [PubMed] [Google Scholar]
- 22. Yung DL, McIver KS, Scott JR, Hollingshead SK (1999) Attenuated expression of the mga virulence regulon in an M serotype 50 mouse-virulent group A streptococcal strain. Infect Immun 67: 6691–6694. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23. Sriskandan S, Unnikrishnan M, Krausz T, Cohen J (1999) Molecular analysis of the role of streptococcal pyrogenic exotoxin A (SPEA ) in invasive soft-tissue infection resulting from Streptococcus pyogenes. Mol Microb 33: 778–790. [DOI] [PubMed] [Google Scholar]
- 24. Wiles S, Clare S, Harker J, Huett A, Young D, et al. (2004) Organ specificity, colonization and clearance dynamics in vivo following oral challenges with the murine pathogen Citrobacter rodentium . Cell Microbiol 6: 963–972. [DOI] [PubMed] [Google Scholar]
- 25. Willoughby DS, Watson DW (1964) Host-parasite relationships among group A streptococci II. Influence of sex on the susceptibility of inbred mice toward streptococcal infection. J Bacteriol 87: 1457–1461. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26. Shanks N, Renton C (1994) Influence of Change From Grouped to Individual Housing on a T-Cell-Dependent Immune Response in Mice?: Antagonism by Diazepam. Pharmacol Biochem Behav 47: 497–502. [DOI] [PubMed] [Google Scholar]
- 27. Grewal IS, Heilig M, Miller A, Genetics M (1997) Environmental regulation of T-cell function in mice?: group housing of males affects accessory cell function. Immunology 90: 165–168. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28. Rabin BS, Lyte M, Hamill E (1987) The influence of mouse strain and housing on the immune response. J Neuroimmunol 17: 11–16. [DOI] [PubMed] [Google Scholar]
- 29. Brook I (2011) Microbiology of sinusitis. Proc Am Thorac Soc 8: 90–100. [DOI] [PubMed] [Google Scholar]
- 30. Ozcan M, Unal A, Aksaray S, Yalcin F, Akdeniz T (2002) Correlation of middle meatus and ethmoid sinus microbiology in patients with chronic sinusitis. Rhinology 40: 24–27. [PubMed] [Google Scholar]