Abstract
Antineutrophil cytoplasm antibody (ANCA)–associated vasculitis (AAV) commonly results in glomerulonephritis, in which neutrophils and monocytes have important roles. The heterodimer calprotectin (S100A8/S100A9, mrp8/14) is a Toll-like receptor-4 ligand found in neutrophils and monocytes and is elevated in inflammatory conditions. By immunohistochemistry of renal biopsies, patients with focal or crescentic glomerular lesions were found to have the highest expression of calprotectin and those with sclerotic the least. Serum levels of calprotectin as measured by ELISA were elevated in patients with active AAV and the levels decreased but did not normalize during remission, suggesting subclinical inflammation. Calprotectin levels in patients with limited systemic disease increased following treatment withdrawal and were significantly elevated in patients who relapsed compared with those who did not. As assessed by flow cytometry, patients with AAV had higher monocyte and neutrophil cell surface calprotectin expression than healthy controls, but this was not associated with augmented mRNA expression in CD14+ monocytes or CD16+ neutrophils. Thus, serum calprotectin is a potential disease biomarker in patients with AAV, and may have a role in disease pathogenesis.
Keywords: ANCA, glomerulonephritis, immunology, macrophages, pathology, vasculitis
Antineutrophil cytoplasm antibody (ANCA)–associated vasculitis is characterized by small-vessel inflammation and immune reactivity against the neutrophil and monocyte components proteinase 3 (PR3) and myeloperoxidase (MPO). ANCA activate neutrophils and monocytes in vitro,1 and are capable of inducing disease in certain animal models.2, 3 ANCA titers do not closely follow disease activity, as patients in clinical remission frequently have persistent ANCA positivity, and serial measurements have been demonstrated to be of limited use during disease remission in guiding individualized patient treatment.4 A recently demonstrated transcriptional profiling of purified CD8+ T cells has identified a subset of genes associated with a poor prognosis, and is therefore a potential biomarker in ANCA–associated vasculitis (AAV).5 Glomerulonephritis, a common feature of AAV, is pauci-immune and characterized by infiltration of glomerular monocytes/macrophages and T cells.6 Importantly, the extent of glomerular inflammation on renal biopsy predicts renal outcome.7 The more inflamed the glomeruli, with predominance of crescents or focal necrosis, the better the renal outcome compared with mixed and sclerotic lesions, suggesting that these lesions respond the most to therapy. However, there are currently no noninvasive means of monitoring the activity of those proinflammatory glomerular-infiltrating leukocytes.
Calprotectin (S100A8/S100A9, MRP8/14) is a heterodimer complex of 2 intracellular calcium-binding proteins S100A8 (MRP 8) and S100A9 (MRP 14). These proteins are expressed by neutrophils, monocytes, and early differentiated macrophages.8, 9 Phagocytes have been demonstrated to release this complex after their interaction with activated, inflamed endothelium.10 Once secreted, the complex binds to activated endothelial cells via heparan sulfate proteogylcans,11, 12 and induces proinflammatory effects, such as increased secretion of IL8, upregulation of ICAM-1, and further recruitment of leukocytes. In addition, the interaction results in impairment of the endothelial monolayer integrity and induction of both caspase-dependent and caspase-independent cell death mechanisms resulting in both apoptosis and necrosis.13, 14 These characteristics make calprotectin a potentially important mediator of tissue damage in AAV, in which endothelial activation and vascular damage are prominent. A previous study demonstrated the formation of MRP8/MRP14 (calprotectin) complexes on glomerular infiltrating macrophages, which correlated with the severity of different forms of glomerulonephritis,15 whereas in renal vasculitis most activated macrophages express this complex and produce TNFα and IL 1.16 In addition, high serum calprotectin levels have been described in patients with systemic lupus erythematosus (SLE), rheumatoid arthritis, renal allograft rejection, juvenile idiopathic arthritis, and Kawasaki disease,17, 18, 19, 20, 21, 22 whereas increasing levels have been associated with relapse in juvenile-onset arthritis23 and decreasing levels with improvements in joint swelling in rheumatoid arthritis.24
In this study, we report on serum calprotectin levels, calprotectin surface expression on circulating leukocytes and in renal biopsies, and calprotectin (S100A8 and S100A9) gene expression in purified leukocyte subsets in patients with active AAV, AAV in remission, and healthy controls. We demonstrate that calprotectin is expressed on the surface of leukocytes and in the serum at higher basal levels in patients than in healthy controls, whereas disease activity is associated with increasing serum levels. Glomerular inflammation is characterized by infiltration with calprotectin-positive leukocytes, and the extent of glomerular inflammation is closely related to the degree of calprotectin expression. Overall, we find that calprotectin is a potential novel biomarker of disease activity in AAV, and the altered basal levels in patients suggest a potential role in disease etiology.
RESULTS
Renal biopsy immunohistochemistry
Immunohistochemistry (IHC) was performed on renal biopsies of 32 acute AAV patients. The patients were classified according to the Berden classification as follows: focal (n=4), crescentic (n=12), mixed (n=8), and sclerotic (n=4). In addition, there were four patients with no active lesions.
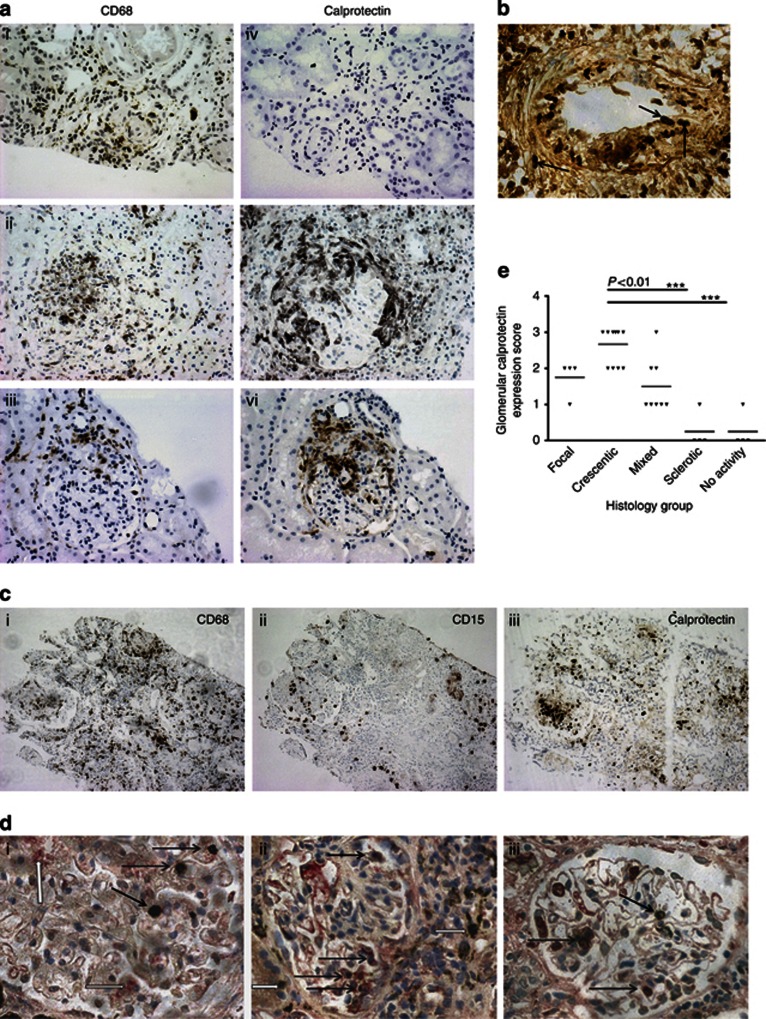
Calprotectin positivity was localized to active glomerular lesions, found within crescents or in areas of endocapillary proliferation (Figure 1a (v and vi)). Sclerotic lesions were generally negative for calprotectin expression (Figure 1a (iv)). There was a statistically significant difference between the levels of expression in the crescentic lesions compared with the sclerotic or inactive lesions (Figure 1e) (P<0.01, one-way analysis of variance (ANOVA)), whereas there was a trend to lower levels of expression with decreasing degrees of inflammation. Patients with globally sclerosed renal lesions did not demonstrate significant calprotectin staining despite the presence of CD68+ cells on the renal biopsy in 75% (3 out of 4) of the patients (Figure 1a (i and iv)). There were varying amounts of interstitial staining depending on the extent of active tubulointerstital nephritis, whereas there was particularly prominent calprotectin staining around active, necrotizing small vessels (Figure 1b). The recent AAV histological classification has been shown to predict long-term renal outcome, with best renal survival in focal lesions followed by crescentic lesions, and our data indicate that calprotectin expression effectively mirrors the histological findings, with the greatest staining in the crescentic lesions followed by focal lesions. Scarred glomeruli lack calprotectin expression, but may still contain CD68-positive macrophages, and are associated with poor long-term renal survival.
Figure 1.
Immunohistochemistry to demonstrate the presence of calprotectin positive cells in the renal biopsy of patients with antineutrophil cytoplasm antibody (ANCA)–associated vasculitis (AAV) glomerulonephritis. (a) Paired immunohistochemistry on renal biopsy specimens for CD68 (i–iii) and calprotectin (MRP8/14) (iv–vi) from sclerotic (sequential) sections from the same biopsy seen in (i, iv) crescentic, (ii, v) focal, and (iii, vi) glomerular lesions. Sclerosed glomeruli containing (i) CD68 macrophages but (iv) with an absence of calprotectin-positive cells. Within and around a crescent, there is a (ii) heavy CD68 macrophage infiltrate, (v) with prominent expression of calprotectin-positive cells in the crescentic lesion. Focal glomerulonephritis with the presence of (iii) CD68- and (vi) calprotectin-positive cells. (b) Immunohistochemistry for calprotectin showing prominent staining around a small vessel. Black arrows point to some of the infiltrating calprotectin-positive cells. (c) Immunohistochemistry for (i) monocyte/macrophages (CD68), (ii) neutrophils (CD15), and (iii) calprotectin (MRP8/14)-staining cells in serial sections of one renal biopsy from a patient with acute crescentic ANCA-associated glomerulonephritis demonstrating that most of the glomerular calprotectin staining appears to correlate with areas of CD68 staining. (d) Double staining of renal biopsies. (i) CD15 staining (brown) and calprotectin (red) demonstrating some double-positive cells (black arrows), and a population of cells positive for calprotectin but negative for CD15 (white arrows). (ii, iii) Biopsies of mixed and focal glomerulonephritis showing macrophage staining (brown) and calprotectin (red). These sections demonstrate different macrophage populations, with some cells staining for both markers (black arrows) and some interstitial macrophages not expressing calprotectin (white arrows in (ii)). (e) Graph demonstrates the glomerular calprotectin scoring of renal biopsies according to the Berden biopsy classification of focal, crescentric, mixed, and sclerotic glomerular lesions. Biopsies not demonstrating any current active AAV were also included.
The calprotectin staining pattern was predominantly glomerular, and in a similar glomerular distribution to that of CD68-positive macrophages (Figure 1c (i and iii)). Although some of the glomerular calprotectin-positive cells also were positive for the neutrophil marker CD15 (ii), more of the cells were positive for macrophage CD68 (i). Double staining was performed, which demonstrated some CD15-positive cells within the glomeruli (Figure 1d (i)), which were positive for calprotectin, with greater numbers of glomerular CD68-positive cells, many of which were calprotectin positive (Figure 1d (ii and iii)). By contrast, many interstitial macrophages were negative for calprotectin.
AAV patients demonstrate high calprotectin levels during acute disease, which diminishes during remission but does not normalize
Serum was obtained from AAV patients with acute disease (n=57) (32 patients from London, 25 patients from Cambridge), disease remission (n=57), and healthy controls. Twenty-six patients had sequential samples (acute and remission), with 17 patients having sequential samples measured within the first year from diagnosis. Table 1 shows the patient characteristics.
Table 1. Characteristics of the patients with serum calprotectin measurements.
| Acute, n=57 | Remission, n=57 (70 samples) | |
|---|---|---|
| Age | 61 (16–84) | 61 (16–85) |
| Gender | ||
| F | 30 | 23 |
| M | 27 | 34 |
| MPO-ANCA | 21 | 33 |
| PR3-ANCA | 30 | 20 |
| Both | 2 | 0 |
| ANCA negative | 4 | 4 |
| Median creatinine | 185 | 124 |
| Organ involvement | ||
| Renal and extrarenal | 42 | 48 |
| Extrarenal | 15 | 9 |
| Treatment at the time of sampling | Nil 35 | Nil 5 |
| RTX, CYP, P 3 | P and Aza 31 | |
| CYP, P 2 | P and CYP 10 | |
| MMF 1 | MMF 2 | |
| P/MP 10 | Aza 4 | |
| P, MTX 3 | P, RTX, CYP 1 | |
| P, AZA 1 | P and MMF 5 | |
| P, CYP 2 | P and MTX 3 | |
| P alone 2 | ||
| RTX and P 4 | ||
| RTX, P and Aza 2 | ||
| RTX, P and MMF 1 | ||
Abbreviations: ANCA, active antineutrophil cytoplasm antibody; AZA, azathioprine; CYP, cyclophosphamide; MMF, mycophenolate mofetil; MP, methylprednisolone; MPO, myeloperoxidase; MTX, methotrexate; P, prednisolone; PR3, proteinase 3; RTX, rituximab.
The median and ranges of calprotectin levels were as follows: healthy controls, 2836 ng/ml (range 1058–6175); acute AAV patients, 13,453 ng/ml (4769–40,000); and remission AAV patients, 8957 ng/ml (3860–25,083). There were significant differences between healthy control and both acute and remission AAV sera, as well as between acute and remission samples (one-way ANOVA P<0.001) (Figure 2a). In addition, there was a significant correlation between serum calprotectin levels and total neutrophil count (r=0.29; P<0.05). There was no correlation with blood monocyte count or serum creatinine. We also measured serum calprotectin in 59 patients maintained on chronic hemodialysis who demonstrated significantly lower levels of calprotectin than those patients with both active and inactive AAV (both P<0.001).
Figure 2.
Serum levels of calprotectin in patients with renal and non-renal anti-neutrophil cytoplasm antibody (ANCA)-associated vasculitis. (a) The level of serum calprotectin (ng/ml) in healthy controls (n=16) and in patients with active ANCA–associated vasculitis (AAV) (n=57) and in patients with AAV in disease remission (n=57). Patients with both active disease and in disease remission demonstrate significantly higher levels of calprotectin than healthy controls (P<0.001, one-way analysis of variance (ANOVA)). There is also a significant difference in levels between active disease and remission (P<0.001, one-way ANOVA). (b) Graph of 17 patients with serial calprotectin levels. The patient highlighted in red illustrates a patient with a relapse. (c) Corresponding ANCA titers of the patients in graph (b). (d) Graph demonstrating serum calprotectin levels in patients with early systemic non-renal involvement according to disease relapse after cessation of treatment at 12 months. (e) Receiver operating curves (ROCs) using serum calprotectin levels to predict relapse in patients with limited systemic disease using samples taken 1 month after treatment initiation. (f) ROC using serum calprotectin levels to predict relapse in patients with limited systemic disease using samples taken 6 months after treatment initiation. AUC, area under the curve.
Seventeen patients had serum calprotectin measured at more than one time point within the first year after diagnosis (Figure 2b). One patient had an increase in serum calprotectin at week 19, which correlated with a clinical relapse and requirement for escalated immunosuppression. In the patients who entered remission, there was a decrease in serum calprotectin levels from presentation to 4–6 months during remission (P<0.05). The ANCA titer decreased in all the patients (Figure 2c). There was no difference in calprotectin levels in those acute patients in whom prednisolone had already been initiated in the previous week compared with those who were yet to commence immunosuppression.
There were no sufficient recorded relapses in this cohort to investigate whether calprotectin may be a useful predictor of disease relapse. We therefore used serum samples taken from patients enrolled in the European Vasculitis Society (EUVAS) Nonrenal Wegener's Granulomatosis Treated Alternatively with Methotrexate (NORAM) trial. This trial included patients with limited systemic disease without renal involvement who were treated for 12 months with immunotherapy (either steroids and cyclophosphamide or steroids and methotrexate), and in whom high relapse rates were recorded. Patients had immunosuppression withdrawn at 12 months, unless relapse had occurred. Follow-up was continued for a total of 18 months.
Patients with relapsing-limited systemic disease demonstrate higher calprotectin levels than those in remission
Samples were unavailable from the NORAM patients before treatment initiation. However, samples from 27 patients were available for analysis (out of 100 patients recruited), which were taken at 1 month and 6 months of therapy when treatment was with tapering doses of prednisolone from 60 to 25 mg/day, as well as samples taken between 12 and 14 months, when immunosuppression had either been withdrawn or was continued/restarted in those patients who had already relapsed. Out of this group of 27 patients, 14 were relapsers and 13 were non-relapsers. The patients who did not relapse had treatment stopped at 12 months. Five of the relapsing patients relapsed before 12 months while on immunosuppression, and 9 patients relapsed after 12 months and restarted immunosuppression. Six of the late relapsers had calprotectin measured before the relapse and before reintroduction of immunosuppression.
In the NORAM patients' samples, calprotectin levels were significantly lower than in those with generalized (renal) disease even during remission (median levels limited disease at 1 month, 418 ng/ml (range 71–2167) compared with generalized disease remission 8957 ng/ml (3860–25,083) (P<0.0001). However, there was a significant increase in calprotectin levels after 12 months (median level at 14 months, 1689 ng/ml (384–6245), vs. 1 month, 418 ng/ml (range 71–2167)(P<0.0001, Mann–Whitney U test). The 14 patients who went on to relapse during the study (at a median of 13 months from entry, range 6–18 months) had significantly higher levels of calprotectin at the first two time points, while on treatment, than the 13 non-relapsing patients who were also on treatment at these time points (both P<0.005) (Figure 2d). At the final time point, there was a trend to higher values in the relapsers, but this did not reach statistical significance (P=0.055). These data indicate that failure to sufficiently suppress calprotectin levels, while on treatment, can predict subsequent relapse. Receiver operating curves comparing relapsers with non-relapsers demonstrated that at both 1 and 6 months there was a threshold that was associated with a significant risk of relapse: at 1 month a level >626 ng/ml was associated with a sensitivity of 78.6% and specificity of 92.3% and a likelihood ratio of 10.3, whereas at 6 months a level >454 ng/ml was associated with a sensitivity of 78.6% and specificity of 92.3%. Area under the curve at 1 month was 0.87, P=0.0009, whereas at 6 months it was 0.841, P=0.002 (Figure 2). This cohort of patients, unlike those with renal involvement, consisted predominantly of PR3-ANCA-positive patients (25 PR3-ANCA positive, 1 MPO-ANCA, and 1 ANCA negative), and the early samples were taken at a time when patients were established on significant immunotherapy.
Neutrophil and monocyte surface expression of calprotectin
Surface expression was investigated in a subset of healthy controls (n=7), active AAV (n=10), and remission AAV (n=18) patients. Twenty-three patients had renal disease, whereas five had extrarenal disease with no renal involvement. Fifteen were MPO-ANCA-positive and eight were PR3-ANCA-positive, whereas five were ANCA negative. Monocyte gates were determined on the flow cytometer by counterstaining with CD14, lymphocyte gates were determined by a CD3 counterstain, and neutrophil gates were identified by forward- and side-scatter characteristics (Figure 3). There was a greater proportion (% of gated cells) of neutrophils and monocytes with detectable extracellular expression of calprotectin in AAV patients during active disease and convalescence compared with healthy controls (percentage of neutrophils expressing calprotectin (median (range)): healthy controls, 0% (0–3.6%); acute AAV, 78.9% (14.7–98.1%); convalescence AAV, 6.8% (0–98.8%); active AAV compared with controls, P<0.001; and active AAV compared with convalescence AAV, P<0.05 (one-way ANOVA) (Figure 3d); percentage of monocytes expressing calprotectin (median (range)): healthy controls, 5.4% (0–16.9%); acute AAV, 50.5% (0–91.6%); and convalescence AAV, 5.6% (1–94.6%) (P=NS) (Figure 3e). We were unable to detect any surface calprotectin expression on CD3-positive cells. Among patients, the decrease in the proportion of monocytes expressing cell surface calprotectin between the acute and convalescent samples was large but did not reach statistical significance (Figure 3e). There was a statistically significant difference in calprotectin mean fluorescent intensity between acute patients and healthy controls for both neutrophil (P<0.001) (Figure 3f) and monocyte (P<0.01)(Figure 3g) cell surface expression. However, when we compared the levels of S100A8 and S100A9 mRNA extracted from purified patients' CD16-positive neutrophils and CD14-positive monocytes, from the Addenbrooke's hospital cohort, we found no correlation between serum calprotectin and mRNA expression. Moreover, there were no significant differences in mRNA expression between AAV patients and healthy controls (data not shown).
Figure 3.
Flow cytometry to demonstrate the cell surface expression of calprotectin on monocytes and neutrophils in patients with anti-neutrophil cytoplasm antibody (ANCA)-associated vasculitis. (a) Flow cytometry plot demonstrating the identification of the population of CD14-positive cells, neutrophils, and CD3-positive T lymphocytes. Monocytes were identified by anti-CD14 FITC antibody, neutrophils by forward and side scatter, and T cells by anti-CD3 PE antibody. (b, c) Graph to demonstrate calprotectin surface expression of (b) neutrophils and (c) CD14 cells in two individual patients (compared with isotype control). Shaded plot shows the FITC isotype control antibody, whereas other plots show the increase in calprotectin-positive cells in a patient with active AAV (blue) and an ANCA–associated vasculitis (AAV) remission patient (red). (d) Graph to demonstrate % gated neutrophils expressing extracellular calprotectin (% of positive cells based upon gating of the isotype control) (controls vs. AAV active P<0.001, AAV active vs. AAV inactive P<0.05, one-way ANOVA). (e) Graph showing % gated monocytes (CD14) expressing extracellular calprotectin, which follows a similar but nonsignificant trend to the neutrophils (P=NS) (d, e). Monocytes and neutrophils from active AAV (n=10) patients demonstrate the highest surface expression of calprotectin (controls n=7, inactive AAV n=18). (f) Mean fluorescent intensity (MFI) (calprotectin FITC antibody/isotype control antibody) of cells stained for calprotectin, comparing controls, active AAV, and inactive AAV. There was a significant increase in the MFI on neutrophils from acute patients compared with healthy controls (P<0.001). (g) MFI of calprotectin on monocytes demonstrating a significant increase in MFI between patients with active disease and healthy controls (P<0.01).
DISCUSSION
Glomerular monocyte/macrophage infiltration and neutrophil degranulation are key features of pauci-immune glomerulonephritis secondary to AAV, whereas circulating monocyte and neutrophil activation is found during active disease. A previous study has demonstrated glomerular macrophage expression of the heterodimer MRP8/14 (calprotectin, S100A8/A9) in patients with a variety of glomerulonephritidies,16 including patients with active AAV who demonstrated prominent expression in areas of necrotizing extracapillary damage. However, this heterodimer is reportedly absent from more chronic inflammatory lesions.25 We found glomerular infiltration of calprotectin-positive cells in the renal biopsies of patients with AAV. Prominent calprotectin expression was seen within active crescents and in areas of focal necrosis, but was absent in sclerotic or normal glomeruli. Calprotectin expression mirrored the histological lesions that predict better long-term renal outcome according to the recent Berden classification, with staining in the focal lesions and the greatest staining in crescentic lesions, whereas long-term outcome is best in focal glomerulonephritis followed by crescentic glomerulonephritis.
In acute AAV, circulating monocytes and neutrophils are activated. We found that patients with AAV have elevated levels of cell surface calprotectin on both neutrophils and monocytes compared with healthy controls, with levels increasing further during active disease. In addition, serum levels of calprotectin reflect these cellular findings, with significantly higher levels in active disease compared with remission and those found in healthy controls. Interestingly, those patients in clinical remission still had persistently elevated serum calprotectin levels and leukocyte expression, suggesting that there is a degree of subclinical innate immune activation. These data are reminiscent of other findings in AAV remission, in which there is persistent monocyte IL-12 and interferon gamma production,26 with augmented indoleamine dioxygenase activation27 and elevated monocyte TLR expression.28 Importantly, levels of calprotectin diminished after therapy, but achieved lower degrees of suppression in those patients who went on to relapse. Analysis of receiver operating curve suggests that failure to suppress calprotectin at 1 or 6 months may be a useful predictor of future relapses, with a likelihood ratio of 10.3 at 1 month. This is significantly better than a rising ANCA titer, which has recently been estimated in meta-analysis to provide a likelihood ratio of 2.8 for disease relapse.4 However, as we did not have pretreatment levels, there remains a possibility that relapsers simply maintain higher levels of calprotectin. The levels at 1 month and 6 months were measured when patients were receiving immunosuppression, which may partially account for the much lower levels compared with those patients with renal involvement. These results are similar to those found in SLE.17, 18 The most elevated levels in SLE have been seen with arthritis and renal involvement, with a correlation between the serum concentration and Systemic Lupus Erythematosus Disease Activity Index, and no strong correlations between cell surface levels and serum levels.29 In addition, a recent study measuring S100A8/S100A9 (calprotectin) levels in patients with early osteoarthritis demonstrated significantly higher levels of S100A8/S100A9 in patients whose disease progressed compared with the group of non-progressors.30 Patients with severe sepsis also demonstrate elevated levels of calprotectin, although the levels are generally lower than those seen in vasculitis patients, with no apparent correlation between serum levels and severity on the infection.31
With regard to the source of serum calprotectin, we were not able to demonstrate intracellular or surface expression of the heterodimer in human umbilical vein endothelial cells at rest or after stimulation with lipopolysaccharide (data not shown), suggesting that most serum calprotectin is derived from circulating neutrophils and monocytes.
We were not able to demonstrate a correlation between the serum levels of calprotectin and the mRNA expression levels in CD14 and CD16 cells, nor did we find significant changes between patients and controls, suggesting that cellular expression and secretion of calprotectin are not proportional to the amount of the mRNA produced by the cell. However, both serum levels and cell surface calprotectin expression are augmented during disease activity, and in early systemic disease higher levels are associated with disease relapse. These findings suggest that serum calprotectin levels may help guide immunosuppression treatment and may be of more clinical utility than C-reactive protein, an acute-phase reactant, which is generally within the normal range in patients during remission and does not provide prognostic information. A previous study in patients with juvenile idiopathic arthritis treated with methotrexate demonstrated that higher levels of MRP8/14 were predictive of flares, and reflected underlying subclinical inflammation.23
Calprotectin (MRP8/14, S100A8/9), an example of a damage-associated molecular pattern and a marker of activation of innate immunity, has recently been demonstrated to have a role in autoimmunity and in induction of autoimmune T cells, exerting its action through TLR4.32 TLR4 expression has been demonstrated in the kidney and has been shown to contribute to renal injury in animal models.33 Furthermore, TLR4 expression on both bone marrow–derived cells and glomerular endothelial cells has been shown to have a role in neutrophil recruitment and renal injury in the experimental myeloperoxidase glomerulonephritis model.34
In another animal model, S100A8 was able to upregulate activatory FcγR in macrophages through binding TLR4.35 Recently, it has been demonstrated that neutrophil extracellular traps (NETs) contain calprotectin36 and that NETS are released by ANCA-stimulated neutrophils. The formation of NETS may have a role in triggering vasculitis and promoting the autoimmune response in patients with small-vessel vasculitis.37
Overall, we demonstrate that calprotectin is upregulated in patients with AAV and represents a marker of cellular immune activation and disease activity. Larger prospective trials of patients with generalized disease and long-term follow-up should enable us to further define its prognostic value in predicting disease relapse, with further investigations required to demonstrate whether calprotectin could be considered to have a role in vasculitis as a potential biomarker.
MATERIALS AND METHODS
The samples were obtained from patients after informed consent under local ethics committee approval (04/Q0406/25 Hammersmith and Queen Charlotte's & Chelsea Hospitals Research Ethics Committee, 05/Q0508/6 Royal Free Hospital Research Ethics Committee and 08/H0306/21 Cambidgeshire 3 Research Ethics Committee).
IHC on renal biopsies
IHC was performed on formalin-fixed paraffin-embedded sections using standard techniques staining for macrophages (anti-CD68) and calprotectin using the Dako Envision system-HRP (Ely, UK) (DAB (3,3-diaminobenzidine)). Antigen retrieval was performed using a 0.1% calcium chloride solution in 0.5 mℳ tris-buffered saline with 1% trypsin (pH 7.8) for 10 min at 37 °C. Primary antibodies used were mouse anti-human CD68 (Dako)(dilution 1:25) or mouse anti-human MRP8/14 (Bachem, Bubendorf, Switzerland) (dilution 1:50). Isotype control antibody was used as a negative control at the same dilution as the primary antibody. The primary antibodies were incubated at room temperature in a humidified chamber for 1 h. Peroxidase activity was detected with DAB. The slides were then rinsed in water and counterstained with filtered Harris' hematoxylin (Cell Path plc, Powys, UK); next, the slides were dehydrated and mounted with DePeX Gurr mounting medium, and coverslips were then placed. The slides were categorized according to the recently described Berden classification for AAV,7 and the quantification of calprotectin staining in both the glomerulus and the interstitium was graded 0 (no staining) to 3 (extensive staining) by blinded observers. Double staining was performed using anti-CD15 (Dako), anti-CD68 (Dako), and polyclonal anti-MRP8/14 (Immundiagnostik AG, Bensheim, Germany). Antigen retrieval was performed using the Leica epitope retrieval system for 30 min (anti-CD15) and 20 min (anti-CD68) and Leica enzyme for 10 min for anti-MRP8/14. The antibodies were incubated for 30 min at room temperature at the following dilutions: anti-CD15 and anti-CD68, 1:50; and anti-MRP8/14, 1:2000. The sections were developed using DAB for anti-CD15 and anti-CD68 and alkaline phosphatase for anti-MRP 8/14 using the Leica Bond polymer refine detection kits (Newcastle, UK). The Trio (Caliper Life Sciences, Hopkinton, MA) multispectral imaging system was used to assess the sections.
Subjects
AAV patients were identified through the vasculitis clinics at hospitals in London (Royal Free and Hammersmith Hospitals) and Cambridge (Addenbrooke's Hospital).5 All fulfilled the Chapel Hill Consensus criteria for diagnosis of either Granulomatosis with polyangiitis (GPA, formerly Wegener's granulomatosis) or microscopic polyangiitis. Disease activity was assessed clinically, biochemically, and histologically. Active disease at presentation was defined by symptoms consistent with vasculitis, an elevated Birmingham vasculitis activity score, and biochemical findings demonstrating an acute inflammatory response, without evidence of infection. Acute patients were either newly diagnosed, with positive autoantibody serology, or in the case of ANCA-negative patients, histological evidence of a pauci-immune glomerulonephritis, or were known patients undergoing disease relapse which was defined clinically as requiring an escalation in immunosuppression in order to control disease activity. Acute blood samples were obtained where possible before induction therapy initiation or shortly thereafter. Remission patients were assessed by experienced clinicians and had no symptoms related to active vasculitis, and had a Birmingham vasculitis activity score of 0. Healthy controls were volunteers from the individual units. In addition, serum samples stored from a cohort of patients with limited systemic AAV, from the NORAM trial38 conducted by the EUVAS, were also investigated.
Measurement of serum calprotectin levels
Serum was isolated from blood samples obtained from patients with active disease, as well as from patients in disease remission and from healthy controls. The serum from the patients in the NORAM trial was obtained from the EUVAS serum bank and consisted of samples from patients at 0–2 months from entry into the study and commencement of immunosuppressive treatment with initial active disease, at 5–7 months from entry when in remission on immunosuppressive treatment, and at 12–14 months from entry when a number of patients had relapsed. In these patients, immunosuppression was withdrawn at 12 months, with re-commencement of therapy in those patients who had relapsed. Serum was stored at −20 °C until analysis. Calprotectin levels were assessed by sandwich enzyme-linked immunosorbent assay (BMA Biomedicals, Augst, Switzerland) according to the manufacturers' instructions. Sample dilution was optimized and incubated overnight at 4 °C before analysis the following day.
Leukocyte cell surface calprotectin expression
Whole blood was collected from patients in EDTA and processed shortly after collection. The sample was centrifuged at 2400 r.p.m. for 5 min to remove plasma. Red-cell lysis was carried out for 10 min at room temperature, followed by two washing steps. Extracellular staining was performed with CD14 PE (BD Biosciences, Oxford, UK), CD3 PE (eBioscience, Hatfield, UK), and calprotectin FITC (Santa-Cruz Biotechnology, Santa Cruz, CA), as well as isotype control antibodies. The cells were incubated with the antibodies on ice for 30 min, followed by two washing steps. Cells were fixed in 2% paraformaldehyde before flow cytometry.
Separation of leukocyte subsets, extraction of RNA, and microarray hybridization
The protocol is described in detail in Lyons et al.39 Briefly, monocytes were obtained from density gradient–separated peripheral blood mononuclear cells by positive selection using CD14+ microbeads. Neutrophils were obtained from the red-cell pellet by positive selection using CD16+ microbeads after a red-cell lysis step. RNA was then extracted using RNEasy mini kits (Qiagen, Hilden, Germany) according to the manufacturer's instructions. Double-stranded cDNA was then prepared, labeled with Cy5- or Cy3-dCTP, and hybridized to custom-spotted ‘MEDIANTE' oligonucleotide microarrays prepared by the Centre for Microarray Resources, Department of Pathology, University of Cambridge using a two-color, dye-swap design. Spot intensities were extracted using the Koadarray v2.4 software (Stirling, UK), background-corrected and within-print-tip normalized. Preprocessing and subsequent differential expression analysis for S100A8 and S100A9 was performed using the limma package in R.39 The raw microarray data are available on ArrayExpress under accession E-MTAB-157.
Statistics
Statistical analysis was performed using GraphPad Prism 4.0 (GraphPad software, San Diego, CA). Nonparametrc tests of significance were carried out. A Mann–Whitney test was used when comparing two groups. When comparing three or more groups, a one-way ANOVA Kruskal–Wallis test with Dunn's multiple comparisons was used. For correlation data, a Spearman rank correlation test was applied. Receiver operating curve curves were calculated for relapsing and non-relapsing patients in the NORAM study. Results were significant when P<0.05.
Acknowledgments
RJP is supported by a MRC clinical training fellowship. This work was supported by the the Imperial College NIHR comprehensive Biomedical Research Center, the Wellcome Trust (Program Grant number 083650/Z/07/Z), the Cambridge National Institute of Health Research Biomedical Research Center, the UK Medical Research Council, the Evelyn Trust, and Kidney Research UK. KGCS is a Lister Prize Fellow. The Cambridge Institute for Medical Research is in receipt of a Wellcome Trust Strategic Award (079895). The EUVAS Serum Bank was established as part of the European Community Systemic Vasculitis Trial project (Contract nos. BMH1-CT93-1078 and CIPD-CT94-0307) and the Associated Vasculitis European Randomized Trial project (Contract nos. BMH4-CT97-2328 and IC20-CT97-0019) funded by the European Union. We are grateful to Prof Justin Mason, Imperial College London, who kindly provided the HUVEC.
All the authors declared no competing interests.
References
- Falk RJ, Terrell RS, Charles LA, et al. Anti-neutrophil cytoplasmic autoantibodies induce neutrophils to degranulate and produce oxygen radicals in vitro. Proc Nat Acad Sci USA. 1990;87:4115–4119. doi: 10.1073/pnas.87.11.4115. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Xiao H, Heeringa P, Hu P, et al. Antineutrophil cytoplasmic autoantibodies specific for myeloperoxidase cause glomerulonephritis and vasculitis in mice. J Clin Invest. 2002;110:955–963. doi: 10.1172/JCI15918. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Little MA, Smyth CL, Yadav R, et al. Antineutrophil cytoplasm antibodies directed against myeloperoxidase augment leukocyte-microvascular interactions in vivo. Blood. 2005;106:2050–2058. doi: 10.1182/blood-2005-03-0921. [DOI] [PubMed] [Google Scholar]
- Tomasson G, Grayson PC, Mahr AD, et al. Value of ANCA measurements during remission to predict a relapse of ANCA-associated vasculitis—a meta-analysis. Rheumatology. 2012;51:100–109. doi: 10.1093/rheumatology/ker280. [DOI] [PMC free article] [PubMed] [Google Scholar]
- McKinney EF, Lyons PA, Carr EJ, et al. A CD8+ T cell transcription signature predicts prognosis in autoimmune disease. Nat Med. 2010;16:586–591. doi: 10.1038/nm.2130. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ruth AJ, Kitching AR, Kwan RY, et al. Anti-neutrophil cytoplasmic antibodies and effector CD4+ cells play nonredundant roles in anti-myeloperoxidase crescentic glomerulonephritis. J Am Soc Nephrol. 2006;17:1940–1949. doi: 10.1681/ASN.2006020108. [DOI] [PubMed] [Google Scholar]
- Berden AE, Ferrario F, Hagen EC, et al. Histopathologic classification of ANCA-associated glomerulonephritis. J Am Soc Nephrol. 2010;21:1628–1636. doi: 10.1681/ASN.2010050477. [DOI] [PubMed] [Google Scholar]
- Edgeworth J, Freemont P, Hogg N. Ionomycin-regulated phosphorylation of the myeloid calcium-binding protein p14. Nature. 1989;342:189–192. doi: 10.1038/342189a0. [DOI] [PubMed] [Google Scholar]
- Nacken W, Roth J, Sorg C, et al. S100A9/S100A8: Myeloid representatives of the S100 protein family as prominent players in innate immunity. Microsc Res Tech. 2003;60:569–580. doi: 10.1002/jemt.10299. [DOI] [PubMed] [Google Scholar]
- Frosch M, Strey A, Vogl T, et al. Myeloid-related proteins 8 and 14 are specifically secreted during interaction of phagocytes and activated endothelium and are useful markers for monitoring disease activity in pauciarticular-onset juvenile rheumatoid arthritis. Arthritis Rheum. 2000;43:628–637. doi: 10.1002/1529-0131(200003)43:3<628::AID-ANR20>3.0.CO;2-X. [DOI] [PubMed] [Google Scholar]
- Robinson MJ, Tessier P, Poulsom R, et al. The S100 family heterodimer, MRP-8/14, binds with high affinity to heparin and heparan sulfate glycosaminoglycans on endothelial cells. J Biol Chem. 2002;277:3658–3665. doi: 10.1074/jbc.M102950200. [DOI] [PubMed] [Google Scholar]
- Srikrishna G, Panneerselvam K, Westphal V, et al. Two proteins modulating transendothelial migration of leukocytes recognize novel carboxylated glycans on endothelial cells. J Immunol. 2001;166:4678–4688. doi: 10.4049/jimmunol.166.7.4678. [DOI] [PubMed] [Google Scholar]
- Viemann D, Strey A, Janning A, et al. Myeloid-related proteins 8 and 14 induce a specific inflammatory response in human microvascular endothelial cells. Blood. 2005;105:2955–2962. doi: 10.1182/blood-2004-07-2520. [DOI] [PubMed] [Google Scholar]
- Viemann D, Barczyk K, Vogl T, et al. MRP8/MRP14 impairs endothelial integrity and induces a caspase-dependent and -independent cell death program. Blood. 2007;109:2453–2460. doi: 10.1182/blood-2006-08-040444. [DOI] [PubMed] [Google Scholar]
- Frosch M, Vogl T, Waldherr R, et al. Expression of MRP8 and MRP14 by macrophages is a marker for severe forms of glomerulonephritis. J Leukoc Biol. 2004;75:198–206. doi: 10.1189/jlb.0203076. [DOI] [PubMed] [Google Scholar]
- Rastaldi MP, Ferrario F, Crippa A, et al. Glomerular monocyte-macrophage features in ANCA-positive renal vasculitis and cryoglobulinemic nephritis. J Am Soc Nephrol. 2000;11:2036–2043. doi: 10.1681/ASN.V11112036. [DOI] [PubMed] [Google Scholar]
- Haga HJ, Brun JG, Berntzen HB, et al. Calprotectin in patients with systemic lupus erythematosus: relation to clinical and laboratory parameters of disease activity. Lupus. 1993;2:47–50. doi: 10.1177/096120339300200108. [DOI] [PubMed] [Google Scholar]
- Soyfoo MS, Roth J, Vogl T, et al. Phagocyte-specific S100A8/A9 protein levels during disease exacerbations and infections in systemic lupus erythematosus. J Rheumatol. 2009;36:2190–2194. doi: 10.3899/jrheum.081302. [DOI] [PubMed] [Google Scholar]
- De Rycke L, Baeten D, Foell D, et al. Differential expression and response to anti-TNFalpha treatment of infiltrating versus resident tissue macrophage subsets in autoimmune arthritis. J Pathol. 2005;206:17–27. doi: 10.1002/path.1758. [DOI] [PubMed] [Google Scholar]
- Burkhardt K, Radespiel-Troger M, Rupprecht HD, et al. An increase in myeloid-related protein serum levels precedes acute renal allograft rejection. J Am Soc Nephrol. 2001;12:1947–1957. doi: 10.1681/ASN.V1291947. [DOI] [PubMed] [Google Scholar]
- Frosch M, Ahlmann M, Vogl T, et al. The myeloid-related proteins 8 and 14 complex, a novel ligand of toll-like receptor 4, and interleukin-1beta form a positive feedback mechanism in systemic-onset juvenile idiopathic arthritis. Arthritis Rheum. 2009;60:883–891. doi: 10.1002/art.24349. [DOI] [PubMed] [Google Scholar]
- Hirono K, Foell D, Xing Y, et al. Expression of myeloid-related protein-8 and -14 in patients with acute Kawasaki disease. J Am Coll Cardiol. 2006;48:1257–1264. doi: 10.1016/j.jacc.2006.02.077. [DOI] [PubMed] [Google Scholar]
- Foell D, Wulffraat N, Wedderburn LR, et al. Methotrexate withdrawal at 6 vs. 12 months in juvenile idiopathic arthritis in remission: a randomized clinical trial. JAMA. 2010;303:1266–1273. doi: 10.1001/jama.2010.375. [DOI] [PubMed] [Google Scholar]
- Andres Cerezo L, Mann H, Pecha O, et al. Decreases in serum levels of S100A8/9 (calprotectin) correlate with improvements in total swollen joint count in patients with recent-onset rheumatoid arthritis. Arthritis Res Ther. 2011;13:R122. doi: 10.1186/ar3426. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bhardwaj RS, Zotz C, Zwadlo-Klarwasser G, et al. The calcium-binding proteins MRP8 and MRP14 form a membrane-associated heterodimer in a subset of monocytes/macrophages present in acute but absent in chronic inflammatory lesions. Eur J Immunol. 1992;22:1891–1897. doi: 10.1002/eji.1830220732. [DOI] [PubMed] [Google Scholar]
- Hruskova Z, Rihova Z, Mareckova H, et al. Intracellular cytokine production in ANCA-associated vasculitis: low levels of interleukin-10 in remission are associated with a higher relapse rate in the long-term follow-up. Arch Med Res. 2009;40:276–284. doi: 10.1016/j.arcmed.2009.04.001. [DOI] [PubMed] [Google Scholar]
- Chavele KM, Shukla D, Keteepe-Arachi T, et al. Regulation of myeloperoxidase-specific T cell responses during disease remission in antineutrophil cytoplasmic antibody-associated vasculitis: the role of Treg cells and tryptophan degradation. Arthritis Rheum. 2010;62:1539–1548. doi: 10.1002/art.27403. [DOI] [PubMed] [Google Scholar]
- Tadema H, Abdulahad WH, Stegeman CA, et al. Increased expression of Toll-like receptors by monocytes and natural killer cells in ANCA-associated vasculitis. PloS one. 2011;6:e24315. doi: 10.1371/journal.pone.0024315. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lood C, Stenstrom M, Tyden H, et al. Protein synthesis of the pro-inflammatory S100A8/A9 complex in plasmacytoid dendritic cells and cell surface S100A8/A9 on leukocyte subpopulations in systemic lupus erythematosus. Arthritis Res Ther. 2011;13:R60. doi: 10.1186/ar3314. [DOI] [PMC free article] [PubMed] [Google Scholar]
- van Lent P, Blom A, Schelbergen R, et al. Active involvement of "alarmins" S100A8 and S100A9 in regulation of synovial activation and joint destruction during mouse and human osteoarthritis. Arthritis Rheum. 2012;64:1466–1476. doi: 10.1002/art.34315. [DOI] [PubMed] [Google Scholar]
- van Zoelen MA, Vogl T, Foell D, et al. Expression and role of myeloid-related protein-14 in clinical and experimental sepsis. Am J Respir Crit Care Med. 2009;180:1098–1106. doi: 10.1164/rccm.200810-1552OC. [DOI] [PubMed] [Google Scholar]
- Loser K, Vogl T, Voskort M, et al. The Toll-like receptor 4 ligands Mrp8 and Mrp14 are crucial in the development of autoreactive CD8+ T cells. Nat Med. 2010;16:713–717. doi: 10.1038/nm.2150. [DOI] [PubMed] [Google Scholar]
- Brown HJ, Lock HR, Wolfs TG, et al. Toll-like receptor 4 ligation on intrinsic renal cells contributes to the induction of antibody-mediated glomerulonephritis via CXCL1 and CXCL2. J Am Soc Nephrol. 2007;18:1732–1739. doi: 10.1681/ASN.2006060634. [DOI] [PubMed] [Google Scholar]
- Summers SA, van der Veen BS, O'Sullivan KM, et al. Intrinsic renal cell and leukocyte-derived TLR4 aggravate experimental anti-MPO glomerulonephritis. Kidney Int. 2010;78:1263–1274. doi: 10.1038/ki.2010.327. [DOI] [PubMed] [Google Scholar]
- van Lent PL, Grevers LC, Schelbergen R, et al. S100A8 causes a shift toward expression of activatory Fcgamma receptors on macrophages via toll-like receptor 4 and regulates Fcgamma receptor expression in synovium during chronic experimental arthritis. Arthritis Rheum. 2010;62:3353–3364. doi: 10.1002/art.27654. [DOI] [PubMed] [Google Scholar]
- Urban CF, Ermert D, Schmid M, et al. Neutrophil extracellular traps contain calprotectin, a cytosolic protein complex involved in host defense against Candida albicans. Plos Pathog. 2009;5:e1000639. doi: 10.1371/journal.ppat.1000639. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kessenbrock K, Krumbholz M, Schonermarck U, et al. Netting neutrophils in autoimmune small-vessel vasculitis. Nat Med. 2009;15:623–625. doi: 10.1038/nm.1959. [DOI] [PMC free article] [PubMed] [Google Scholar]
- De Groot K, Rasmussen N, Bacon PA, et al. Randomized trial of cyclophosphamide versus methotrexate for induction of remission in early systemic antineutrophil cytoplasmic antibody-associated vasculitis. Arthritis Rheum. 2005;52:2461–2469. doi: 10.1002/art.21142. [DOI] [PubMed] [Google Scholar]
- Lyons PA, Koukoulaki M, Hatton A, et al. Microarray analysis of human leucocyte subsets: the advantages of positive selection and rapid purification. BMC genomics. 2007;8:64. doi: 10.1186/1471-2164-8-64. [DOI] [PMC free article] [PubMed] [Google Scholar]