Abstract
The delay reverse sural neurofasciocutaneous flap is used to reconstruct soft tissue defects in the lower third of the leg to improve outcome in patients with associated comorbidities such as diabetes mellitus, hypertension, hypercholesterolaemia, smokers and ischaemic heart disease. The author reports the use of a delayed reverse sural flap as soft tissue cover for a calcaneal defect in a patient with associated comorbidities who has an ipsilateral Gred 3C (Gustilo) tibial fracture after vascular reconstruction.
Keywords: Lower-extremity reconstruction, Vascular injury, Sural flap, Delay procedure, Limb salvage
Case Report
This 46-year-old man sustained Grade 3C compound fracture of his right tibia with associated degloving injury of the ipsilateral heel pad in a motor-vehicle accident. He was a chronic smoker with diabetes, hypertension, hypercholesterolemia, and ischaemic heart disease.
An emergency wound exploration showed a nonflowing anterior tibial artery at the fracture site. An anterior tibial to dorsalis pedis artery bypass surgery was performed. The fracture was stabilized with an external fixator and the wounds was dressed.
He was referred to the plastic surgical unit 2 weeks later for coverage of the calcaneal defect. Examination showed an open wound exposing his right calcaneal bone. A right lower limb angiogram showed a patent bypass graft but evidence of “slow flow” in the right posterior tibial and peroneal arteries.
A delayed reverse sural fasciocutaneous flap was performed as described by Erdmann et al [1]. Elevation of the reverse sural flap measuring 10 cm × 8 cm was performed as the first stage. A sterile nonpowdered rubber glove was modified and placed between the elevated flap and its original bed (Fig. 1). The flap was then resutured back to its original location. Ten days later the flap was re-elevated and inserted to cover the exposed calcaneum. All remaining wounds were skin grafted. The wound healed and the external fixator was removed at 4 months post-trauma (Fig. 2).
Fig. 1.
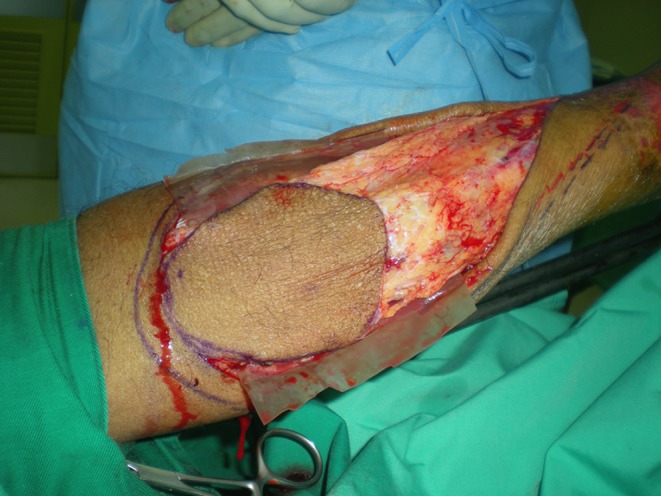
Picture showing a modified non-powdered rubber glove being placed between the flap and the gastrocnemius muscle underneath
Fig. 2.
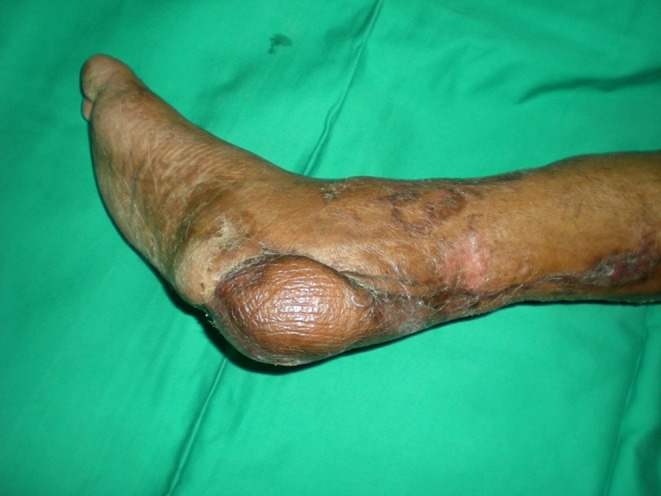
Picture showing the flap at four months, completely healed and the external fixator removed
Discussion
Reconstructive options for soft tissue defects in the lower third of the leg include the use of cutaneous, fasciocutaneous, muscle, and free flaps [2, 3]. Free flaps are superior to pedicle flaps because of their vascularity and flexibility. Their disadvantages are that they are lengthy procedure requiring a well-trained and equipped surgical team. Pedicle flaps can be done easily under regional anesthesia.
The reverse sural neurofasciocutaneous flap is widely used to reconstruct soft tissue defects in this area [2, 3]. The anatomical basis of this flap was explained by Masquelet et al. [4]. However, partial necrosis is common in patients with associated comorbidities: elderly, peripheral vascular disease, diabetes, and heavy smoker. Baumeister et al found a complication rate up to 36 % in patients from this group [5].
A delay procedure will improve blood flow to the flap through a mechanism of increased vessel size, reorientation, and increased number of vessels [6]. A delay procedure will open up “choke vessels,” increasing perfusion to the most distal part of the flap preventing necrosis [7].
Another area where the delay reverse sural flap can be helpful is in treating soft tissue defects in the lower leg in patients with concomitant vascular injury. These injuries are treated by either amputation or a free flap after initial vascular reconstruction [8]. This procedure requires resources that might not be available in most hospitals. Patients with associated comorbid factors might also not be suitable candidates. The delay reverse sural flap can be performed relatively quickly and under regional anesthesia. The only disadvantage is the need for a two-stage surgery. However, certain clinical situations may necessitate a two-stage or perhaps even more surgery anyway, for example, in a severely traumatized or infected wound.
This preliminary case report suggests that a delayed reverse sural flap can be an option for soft tissue cover in the lower third of the leg for a patient with comorbidities and associated vascular trauma.
Acknowledgments
Disclaimer
The author does not have any conflict of interest related to this article nor did he receive any financial support.
References
- 1.Erdmann D, Gottlieb N, Humphrey JS, et al. Sural flap delay procedure: a preliminary report. Ann Plast Surg. 2005;54:562–565. doi: 10.1097/01.sap.0000154873.08087.d5. [DOI] [PubMed] [Google Scholar]
- 2.Costa-Ferreira A, Reis J, Pinho C, et al. The distally based island superficial sural artery flap: clinical experience with 36 flaps. Ann Plast Surg. 2001;46:308–313. doi: 10.1097/00000637-200103000-00018. [DOI] [PubMed] [Google Scholar]
- 3.Jeng S, Wei F. Distally based sural island flap for foot and ankle reconstruction. Plast Reconstr Surg. 1997;99:744–750. doi: 10.1097/00006534-199703000-00022. [DOI] [PubMed] [Google Scholar]
- 4.Masquelet AC, Romana MC, Wolf G. Skin island flaps supplied by the vascular axis of the sensitive superficial nerves: anatomic study and clinical experience. Plast Reconstr Surg. 1992;89:1115–1121. doi: 10.1097/00006534-199206000-00018. [DOI] [PubMed] [Google Scholar]
- 5.Baumeister SP, Spierer R, Erdmann D, et al. A realistic complication analysis of 70 sural artery flaps in a multi-morbid patient group. Plast Reconstr Surg. 2003;112:129–140. doi: 10.1097/01.PRS.0000066167.68966.66. [DOI] [PubMed] [Google Scholar]
- 6.Fisher J, Gingrass MK. Basic principles of skin flaps. In: Georgiade GS, Riefkohl R, Levin LS, editors. Plastic, maxillofacial and reconstructive surgery. Baltimore: Williams and Wilkins; 1997. pp. 22–24. [Google Scholar]
- 7.Dhar SC, Taylar GI. The delay phenomenon: the story unfolds. Plast Reconstr Surg. 1999;104:2079–2091. doi: 10.1097/00006534-199912000-00021. [DOI] [PubMed] [Google Scholar]
- 8.Bishara SA, Maher MH, Ahmad MT, et al. Early microvascular reconstruction of Gustilo type III-C lower extremity wound: case report. Scan J Plast Reconstr Surg Hand Surg. 1997;31(4):351–355. doi: 10.3109/02844319709008983. [DOI] [PubMed] [Google Scholar]


