Abstract
The phosphatidylinositol-3-kinase/Akt (PI3K/Akt) pathway is constitutively activated in a substantial proportion of prostate tumors and is considered a key mechanism supporting progression toward an androgen-independent status, for which no effective therapy is available. Therefore, PI3K inhibitors, alone or in combination with other cytotoxic drugs, could potentially be used to treat cancer with a constitutive activated PI3K/Akt pathway. To selectively target advanced prostate tumors with a constitutive activated PI3K/Akt pathway, we generated a prostate cancer-specific PI3K inhibitor by coupling the chemically modified form of the quercetin analog LY294002 (HO-CH2-LY294002, compound 8) with the peptide Mu-LEHSSKLQL, in which the internal sequence HSSKLQ is a substrate for the prostate-specific antigen (PSA) protease. The result is a water-soluble and latent PI3K inhibitor prodrug (compound 11) which activation is dependent on PSA cleavage. Once activated, the L-O-CH2-LY294002 (compound 10) can specifically inhibit PI3K in PSA-secreting prostate cancer cells and induced apoptosis with a potency comparable to the original LY294002 compound.
Introduction
Prostate cancer remains the second leading cause of cancer-related death in men in the United States. Conventional treatments as surgery, radiation and androgen suppression are effective if prostate cancer is confined to the prostate. Unfortunately, many patients with advanced metastatic cancer treated with androgen ablation experience recurrence of androgen-independent cancer, with limited or transient response to other systemic chemotherapies.1,2 For this reason, there is an urgent need for new specific and targeted agents to treat androgen-independent prostate cancer. Several mechanisms have been proposed to explain why prostate cancer cells can grow in the absence or reduced presence of androgens. Recent reports suggest that the phosphatidylinositol 3-kinase/Akt (PI3K/Akt) pathway is one of the mechanisms that allow prostate cancer cells to maintain continued proliferation in a low-androgen environment.3
The PI3K pathway is a key signal-transduction pathway initiated by a receptor tyrosine kinases that recruit and activate the PI3K, resulting in an accumulation of phosphatidylinositol 3, 4, 5-triphosphate (PIP3) in plasma membrane. This lipid second messenger recruits Akt and the phosphoinositide dependent protein kinase 1 (PDK1) to the cell membrane, where Akt is phosphorylated by PDK1 at threonine 308. Activated Akt recruits the mammalian target of rapamycin (mTOR) that, acting with Rictor protein, forms the mTORC2 complex, which complete the activation of Akt by phosphorylation at serine 473. Fully activated Akt translocates to the cytoplasm and nucleus where it phosphorylates downstream substrates involved in angiogenesis, cell cycle progression, growth, migration, proliferation, and survival.4
Constitutive activation of the PI3K/Akt pathway in prostate cancer is often led by functional loss of the tumor suppressor PTEN (phosphatase and tensin homolog deleted on chromosome 10) that dephosphorylates PI3K substrates, or by activating mutations in the PI3 kinase itself that correlate with increased Akt phosphorylation, higher Gleason grade, advanced stage, and unfavorable prognosis.5,6 For these reasons, PI3K inhibitors have been considered as an adjuvant therapy for advanced prostate cancer, but unfortunately, despite promising effects in preclinical models, recent clinical trials did not show benefits in prostate cancer-affected patients treated with PI3K inhibitors (source www.ClinicalTrials.gov).
One possible approach for improving efficacy of PI3K inhibitors to treat prostate cancer patients may be to convert the PI3K inhibitor molecule into an inactive prodrug by attaching a specific prostate-specific antigen (PSA) cleavable peptide, increasing the delivery to tumor sites while minimizing systemic toxicity. PSA is a protease with chymotrypsin-like activity, and is involved in the hydrolytic processing of semenogelins, which are necessary for seminal fluid liquefaction. In patients with prostate cancer, systemic PSA concentration is high, but inactive in blood serum, as PSA is complexed with the α1-anti-chymotrypsin (PSA-ACT) or α2-macroglobulin.7,8 On the contrary, in the tumor environment, PSA is free (fPSA) and enzymatically active, able to activate cytotoxic prodrugs based on a PSA-cleavable peptidic sequence.9
In this work, we describe for the first time the synthesis and characterization of a prostate cancer-specific PI3K inhibitor prodrug based on the quercetin analog LY294002 activated by PSA cleavage. Based on previous reports on anti-cancer toxins converted to PSA-activated prodrugs, we linked the PI3K inhibitor LY294002 with the Mu-LEHSSKLQL peptide, containing the HSSKLQ sequence specific for PSA cleavage.8,10-12 The generated PI3K inhibitor prodrug-LY294002 (11) is water soluble and is specifically activated in the media conditioned by the prostate cancer cells C4-2 that secrete PSA. Upon activation, the PI3K inhibitor prodrug 11 showed consistent time-dependent and concentration-dependent inhibition of the PI3 kinase and induction of apoptosis. Specificity of the PI3K inhibitor prodrug 11 for PSA-secreting prostate cancer cells was confirmed using the BT-549 breast cancer cell line and glioblastoma-astrocytoma U-87 MG cells, which does not produce PSA: in these cells the PI3K pathway activity is not affected by 11. Consistent with the requirement of cleavage by PSA for drug activation, PI3K/Akt signaling in BT-549 breast cancer cells is inhibited if 11 is previously incubated in C4-2 conditioned medium or in presence of enzymatically active purified PSA.
Prostate tumor PSA-dependent inhibition of PI3K is expected to produce dual benefits for patients: by completely inhibiting the PI3K pathway at the tumor site and reducing side effects due to inhibition of PI3K in normal tissues, systemic exposure should be minimal, resulting only from the active drug being redistributed from the tumor.13,14
Design and Synthesis
PI3K Inhibitor Prodrug (Compound 11) Design
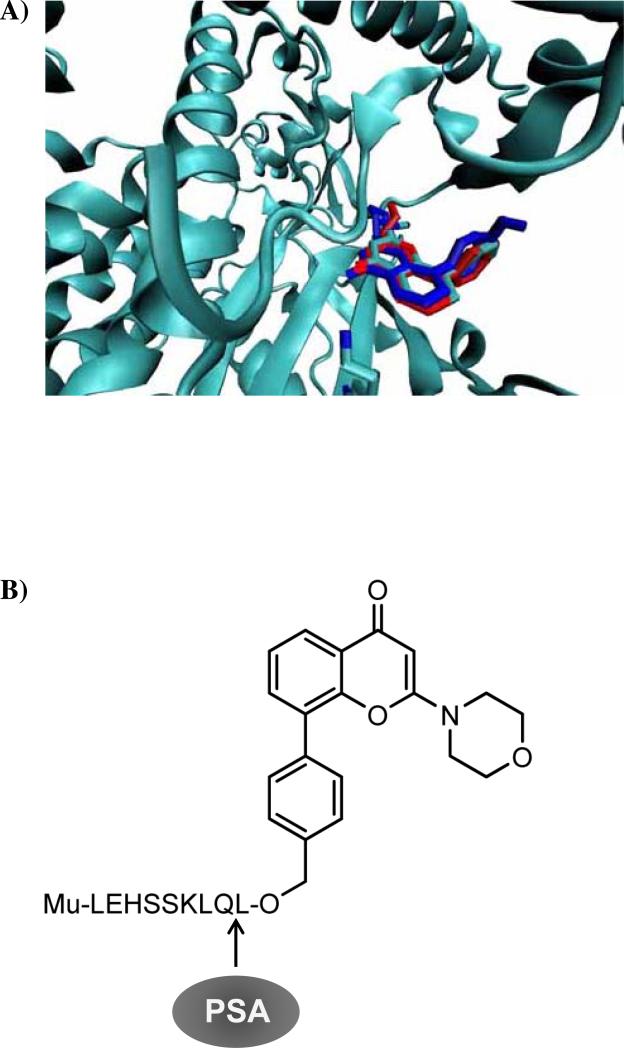
To generate a PI3K inhibitor prodrug activated by the prostate-specific antigen we choose the quercetin analog LY294002 (developed by Eli Lilly Company). The stability of this agent in aqueous solutions made it a reagent of choice for numerous tissue culture studies of PI3K signaling. To determine the position in the LY294002 structure where an inhibitory peptide could be attached, we conducted modeling studies of interactions between the ATP binding pocket of the PI3 kinase and LY294002. These modeling studies have been performed using an existing crystal structure of the PI3 kinase to which LY294002 has been bound as a template.15 AutoDock3 software with AutoDock Tools was used to generate the appropriate charge, solvent and Van der Waals parameters for LY294002 and the PI3 kinase.16 Electrostatic and Van der Waals potential grids for docking were generated based on these parameters and were centered at the center-of-geometry for LY294002 in the crystal structure; although LY294002 was removed before grid creation.
To ensure both high resolution and sampling of a large region of protein for possible binding sites, the grids were generated at 0.375 Å resolution in a cube of 30×30×30 Å. LY294002 was redocked into the active site with 256 runs of AutoDock's Lamarckian genetic algorithm. Default parameters were used except in the number of runs (256), and the size of the initial pool (30000 initial dockings). Subsequent analysis showed that the LY294002 was docked with a similar poise as in the crystal structure with 4.0 μM predicted affinity, using AutoDock's estimator of binding affinity (Fig. 1A, in blue).16 Based on this analysis, a phenyl ring in LY294002 structure was identified to attach a CH2OH moiety, which subsequently was used to couple the Mu-LEHSSKLQL sequence, containing the PSA substrate peptide (Fig. 1B). Since PSA is predicted to cleave Mu-LEHSSKLQL peptide after glutamine (Q), it leaves leucine (L) attached to the phenyl ring of the LY294002 via the CH2OH moiety. The AutoDock modeling of interaction between this “activated prodrug” 10 and PI3K has shown that it can still fit into ATP binding site and, thus, is predicted to inhibit PI3K activity (Fig. 1A, in red).
Figure 1. Modeling of the interaction between LY294002 derivative and PI3 kinase ATP-binding site.
A) Ribbon diagram of an X-ray structure of the PI3K ATP-binding site (gray) with LY294002. An active site Lys in bonds is shown for reference. Modeled structurally similar docking poises for LY294002 (blue) and 10 (red) are shown for comparison.
B) The PI3K inhibitor prodrug (11) formula. Arrow points at predicted prostate-specific antigen cleavage site.
Synthesis of Compound 11
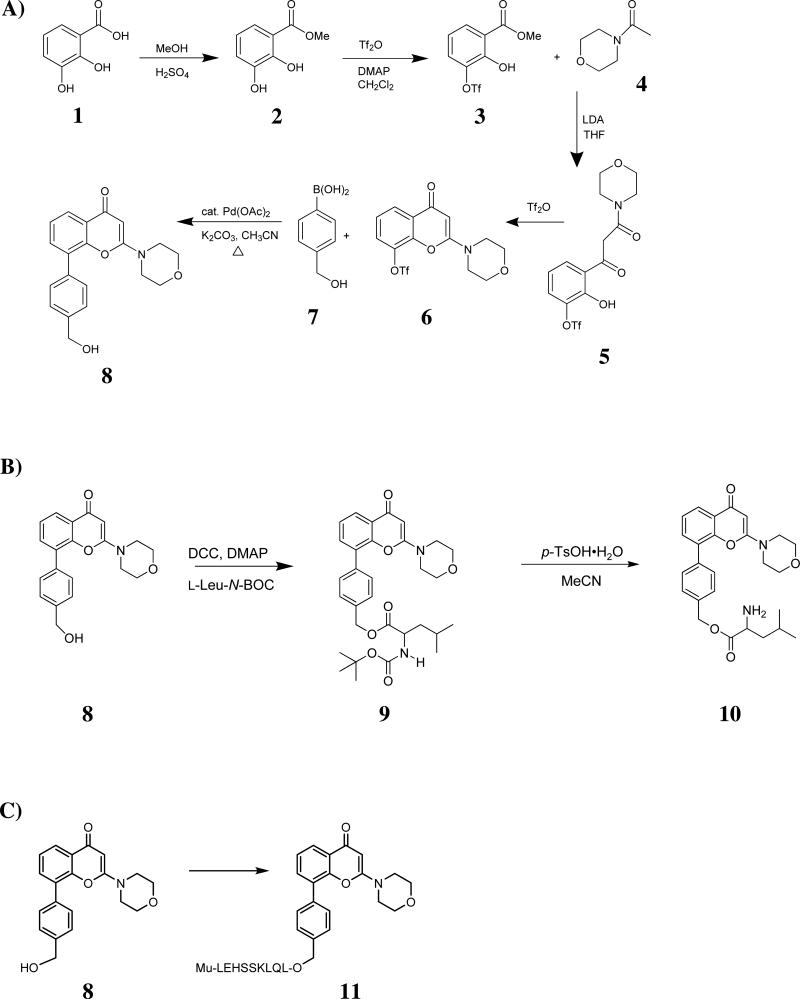
We synthesized 8-(4-(Hydroxymethyl)phenyl)-2-morpholino-4H-chromen-4-one (8), an analog of LY294002 containing a CH2OH functional group, which should not adversely affect the PI3K binding ability but will permit the attachment of PSA substrate peptides (Fig. 2A; numbers hereafter refer to sections in Figure 2). The synthesis of 8 was modeled after the synthetic strategy presented by Abbott and Thompson.17 Commercially available aromatic ester 2, 3- dihydroxybenzoic acid (1) was converted to methyl-2, 3-dihydroxybenzoate (2) by acid catalyzed addition of methanol. The least sterically hindered hydroxyl was then converted to a triflate by treatment with trifluoromethyl sulfonic anhydride to produce methyl-2-hydroxy-3-{[(trifluoromethyl)sulfonyl]oxy}benzoate (3). The enolate of N-acetyl morpholine (4) was then generated with lithium diisopropyl amide and condensed with the ester in 3 to produce 2-hydroxy-3-(3-morpholin-4-yl-3-oxopropanoyl)phenyl trifluoromethanesulfonate (5). 5 underwent cyclodehydration after being treated with triflic anhydride to give 2-morpholin-4-yl-4-oxo-4H-chromen-8-yl trifluoromethanesulfonate (6). 6 was then subjected to Suzuki coupling with commercially available 4-(hydroxymethyl)phenyl boronic acid (7) to produce 8. Once the LY294002 analog with the primary alcohol functional group (8) was prepared, it could be used to attach the leucine or the Mu-LEHSSKLQL-peptide (Fig 2B and 2C).
Figure 2. Synthesis of LY294002 analogues.
Once 8 was prepared (Part A), it was used to attach leucine, generating 10 (part B), or the Mu-LEHSSKLQ-peptide (part C), generating 11, the PI3K inhibitor prodrug.
First we synthesized 4-(2-morpholino-4-oxo-4H-chromen-8-yl)benzyl-2-(tert-butoxycarbonylamino)-4-methylpentanoate (9), where 8 is directly attached to BOC-protected leucine. The BOC protecting group can be removed by p-TsOH when desired to produce 4-(2-morpholino-4-oxo-4H-chromen-8-yl) benzyl-2-amino-4-methylpentanoate (10). 10 represents what would remain after PSA has cleaved off the substrate peptide from the prodrug. The peptide Mu-LEHSSKLQL was attached to 8 by AnaSpec, Inc. (Fremont, CA), to yield Mu-LEHSSKLQL-8-(4-(Hydroxymethyl)phenyl)-2-morpholino-4H-chromen-4-one (11) as a white powder. Mass calculated as 1487.7 was found to be 1488.0 by LC-MS analysis, conducted at AnaSpec, Inc. (provided with the certificate of analysis).
Biological Results
Compound 10 Inhibits the PI3 Kinase
The androgen-independent prostate cancer C4-2 cells that secrete PSA were chosen for this study as a model of advanced and PSA-secreting prostate cancer and used for a preliminary experiment. In parallel, as a negative control, we used the breast cancer BT-549 cell line, which does not secrete PSA. Both cell lines are PTEN-deficient and show constitutive activation of the PI3K/Akt signaling pathway.
As reported, PSA is predicted to cleave 11 after the glutamine, leaving a leucine attached to the phenyl ring of the LY294002. We started by testing whether the “activated prodrug” 10 retained inhibitory properties toward PI3K inhibition, similarly to unmodified LY294002, as predicted by AutoDock modeling.
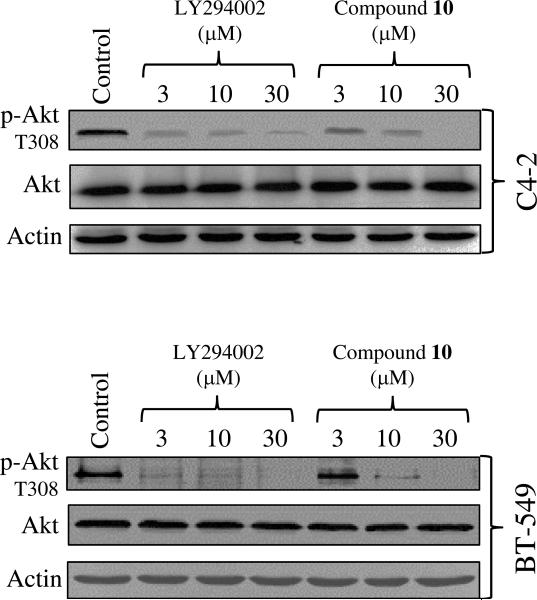
The activated prodrug 10 inhibited the PI3 kinase with a potency comparable to LY294002, resulting in a dose-dependent reduction of p-Akt T308 levels in both cell lines 30 min after administration (Fig. 3). Dose-response analysis shows that 30 μM of 10 completely inhibited Akt phosphorylation in both cell lines.
Figure 3. Compound 10 exerts similar PI3K inhibitory properties as LY294002.
At 30 min after the administration of the LY294002 or compound 10, the “activated prodrug”, dose-dependent decreases of p-Akt T308 were detected both in prostate cancer C4-2 and breast cancer BT-549 cells versus control (cells treated with DMSO). Similar results were obtained in three independent experiments.
Compound 11 Inhibits the PI3 Kinase in PSA-Secreting Prostate Cancer Cells
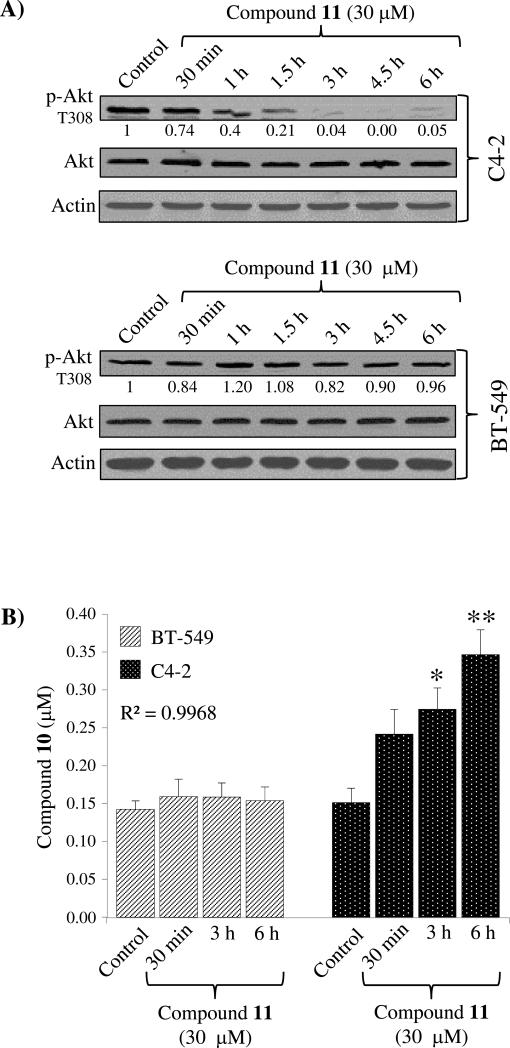
Effects of 11 were monitored in prostate cancer C4-2 and breast cancer BT-549 cells from 30 min to 6 h. A time-dependent reduction of p-Akt T308 levels was observed in prostate cancer C4-2 cells vs control (cells treated with DMSO). Notably, no significant differences in p-Akt T308 levels were detected in breast cancer BT-549 cells treated with 11 during this time period (Fig. 4A). To determine whether PI3 kinase inhibition is due to the cleavage of Mu-LEHSSKLQL peptide by PSA and conversion of 11 into 10, we monitored concentrations of 10 in the media conditioned by either prostate cancer C4-2 or breast cancer BT-549 cells. LC-ESI-MS analysis showed a significant increase of 10 in the media conditioned by prostate cancer C4-2 cells (that secrete PSA) at 30 min, 3 and 6 h after administration, whereas no significant increase was found in the media conditioned by breast cancer BT-549 cells compared to control (cells treated with PBS) (Fig. 4B). In addition, tPSA assay confirmed that during these time-points, PSA concentrations were significantly increased in prostate cancer C4-2 conditioned media, while no PSA was detected in breast cancer BT-549 conditioned media (Fig. 4C). These results suggest that PSA-peptide cleavage is required for activation of 11.
Figure 4. Compound 11 selectively inhibits PI3 kinase in PSA-secreting prostate cancer cells.
A) Prostate cancer C4-2 and breast cancer BT-549 cells were treated with 11 for indicated periods of time. Time-dependent reduction of p-Akt T308 was seen in prostate cancer C4-2 cells (left panel). No significant differences in p-Akt T308 levels were detected in breast cancer BT-549 cells treated with 11 in the same time-frame (right panel). A representative Western blot, out of three independent experiments, is shown. Control = cells treated with PBS.
B) LC-ESI-MS analysis of cell media treated with 11 showed significantly increased concentrations of 10 in the media conditioned by C4-2 cells, but no increase in BT-549 conditioned media. Results expressed as means ± SEM, n=3, *p<0.039 and **p<0.012 vs control, represented by BT-549 or C4-2 conditioned media.
C) Total PSA assay (tPSA) showing significant increase of secreted PSA in prostate cancer C4-2 cells in conditioned media. No PSA was detected in breast cancer BT-549 cells conditioned media. Results are expressed as means ± SEM, n=3, *p<1.1×10−5, **p<4.1×10−6 and ***p<3.26×10−5 vs control, represented by BT-549 or C4-2 media treated with 30 μM prodrug-LY294002.
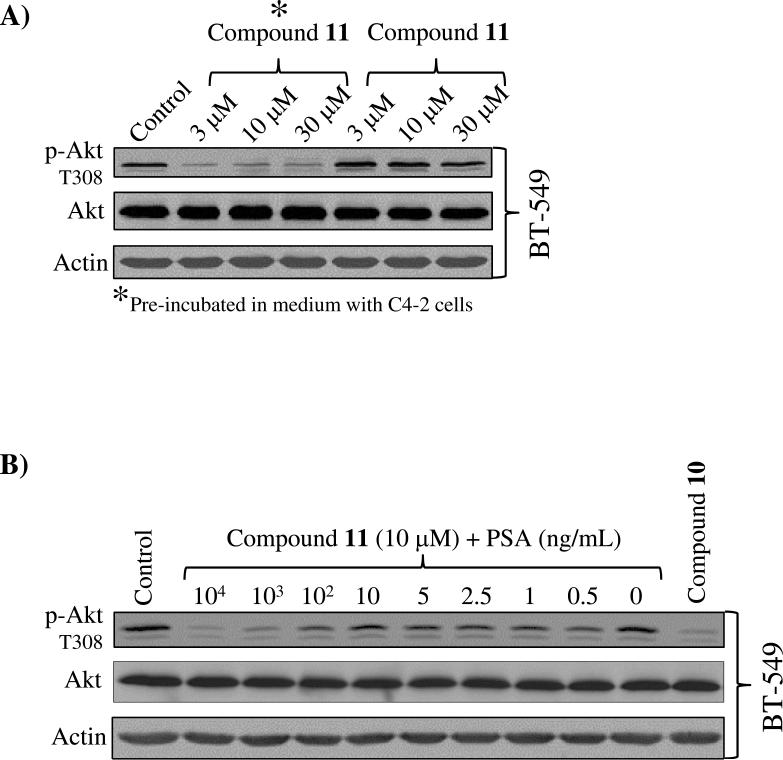
To further demonstrate that inhibition of the PI3K/Akt pathway by 11 depends on the presence of PSA in the media, we incubated 11 in the medium conditioned by prostate cancer C4-2 cells and then after an incubation of 6 h, we transferred the C4-2 conditioned media (containing also 11 activated by PSA cleavage) into Petri dishes containing breast cancer BT-549 cells. As shown in Figure 5A, addition of 11 previously incubated in the media conditioned by prostate cancer C4-2 cells significantly reduced p-Akt T308 levels in breast cancer BT-549 cells (which do not secrete PSA). In contrast, 11 incubated in the media conditioned by breast cancer BT-549 cells had no effects on p-Akt T308 levels. Finally, to confirm that inhibition of PI3K activity by 11 was due to peptide cleavage by PSA (and not by unrelated proteases secreted by prostate cancer C4-2 cells), 11 was incubated for 6 h at 37 °C with increasing concentrations of enzymatically active PSA purified from human semen. Addition of 11 (pre-incubated with PSA) to BT-549 cells for 30 min reduced p-Akt T308 levels in a PSA dose-dependent fashion (Fig. 5B). Notably, 11 without enzymatically active PSA had no effect on p-Akt T308 levels in BT-549 cells.
Figure 5. PSA converts compound 11 into an active PI3K inhibitor.
A) Addition of 11 (incubated for 6 h in media conditioned by prostate cancer C4-2 cells) resulted in significant reduction of p-Akt T308 in breast cancer BT-549 cells. (Control = cells treated with PBS).
B) Compound 11 incubated for 6 h with a range of concentrations (0-104 ng/mL) of active PSA and added to breast cancer BT-549 cells media for 30 min resulted in significant decrease of p-Akt T308, if compared to control (Control = cells treated with DMSO).
Similar results were obtained in three independent experiments.
To further demonstrate that activation of 11 is PSA-dependent, we extended the screening to hormone-sensitive prostate cancer LNCaP cells (that secrete PSA) and to glioblastoma-astrocytoma U-87 MG cells that do not secrete PSA (Fig. 6A and 6B). Consistent with earlier results, p-Akt T308 levels were reduced in LNCaP cells incubated with 11 and in C4-2 cells in a dose-dependent fashion (Fig. 6A). This effect was not seen in U-87 MG cells or in BT-549 cells (Fig. 6B), supporting the notion that secretion of PSA in the media (confirmed by tPSA assay) (Fig. 6C) is needed to cleave the Mu-LEHSSKLQL peptide.
Figure 6. Selective inhibition of PI3K in PSA-secreting prostate cancer cells by compound 11.
A) Incubation of prostate cancer LNCaP cells and C4-2 cells with 11 at 3 h resulted in a dose-dependent reduction of p-Akt T308 levels (Control = cells treated with PBS).
B) No significant reduction of p-Akt T308 levels was observed in glioblastoma-astrocytoma U-87 MG cells, or breast cancer BT-549 cells (Control = cells treated with PBS). Similar results were obtained in three independent experiments.
C) Total PSA (tPSA) assay confirms secretion of PSA in prostate cancer LNCaP and C4-2 cells media at 3 h (Control = cells media). As expected, breast cancer BT-549 and glioblastoma-astrocytoma U-87 MG cells did not secrete PSA.
Results are expressed as means ± SEM, n=3, #p<4.2×10−9 and *p<6.3×10−10 vs control.
Compound 11 Promotes Apoptosis in C4-2LucBAD Prostate Cancer Cells
As we have previously shown, LY294002 induces apoptosis in C42LucBAD cells that ectopically express BAD, a BH3-only pro-apoptotic protein of Bcl-2 family.18-21
Administration of 11 inhibited PI3K/Akt pathway and induced apoptosis in C42LucBAD cells, as evident from increased Caspase 3 activity and cleavage of caspase substrate PARP (Fig. 7). Somewhat lower levels of caspase activity induced by 11 are likely due to extra time needed for conversion of 11 into an active PI3K inhibitor. These experiments unequivocally demonstrate that 11 is converted by PSA cleavage into an active PI3K inhibitor that selectively blocks the PI3K/Akt pathway and induces apoptosis in PSA-secreting prostate cancer cells.
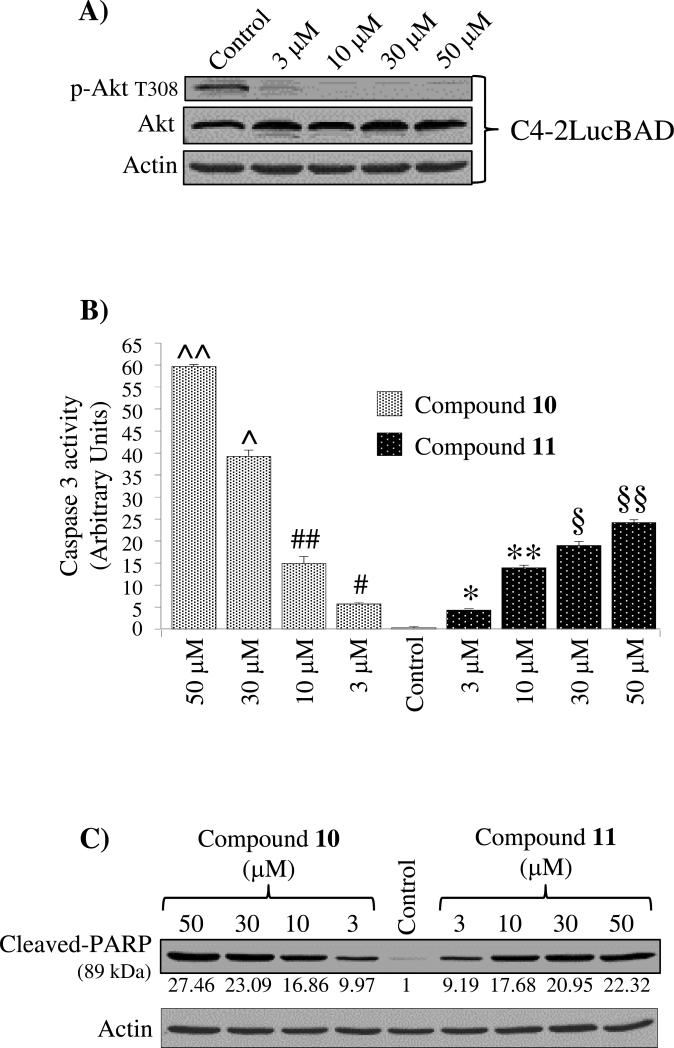
Figure 7. The compound 11 induces apoptosis in C4-2LucBAD cells.
A) Compound 11 induced a dose-dependent reduction of p-Akt T308 in C4-2LucBAD cells in 3 h (Control = cells treated with PBS).
B) Caspase 3 assay performed in C4-2LucBAD cells 6 h after the administration of 10 and 11. Results are expressed as means ± SEM, n=2, #p<0.0062, ##p<0.012, ^p<0.0015, ^^p<8.3×10−5 and *p<0.0055, **p<0.0022, §p<0.003, §§p<0.001, vs control (Control = cells treated with DMSO).
C) Samples from (B) were analyzed for the cleaved PARP (89 kDa), confirming activation of caspases effector after the administration of 10 or 11 (Control = cells treated with DMSO). Similar results were obtained in three independent experiments.
Discussion and Conclusions
In this paper, we have demonstrated for the first time the conversion of a non-tissue-specific PI3K inhibitor (LY294002) into an inactive and latent prodrug (11), which can be specifically activated by the PSA protease. Earlier publications have shown that various non-specific cytotoxic drugs, including thapsigargin, 5-fluorodeoxyuridine, and doxorubicin, could be converted into inactive prodrugs by attaching a PSA-cleavable substrate peptide; however, no publications have reported an attempt to convert a PI3 kinase inhibitor (or any kinase inhibitor) into latent prodrugs activated by PSA cleavage.22-24 Converting a PI3K inhibitor into a latent and prostate cancer-specific prodrug may allow an increased drug dosage, accomplishing complete inhibition of PI3K activity in prostate cancer cells while at the same time reducing systemic cytotoxic effects exerted by non-tissue specific PI3K inhibitors. Comparing to non-targeted PI3K inhibitors, a PI3K inhibitor prodrug is expected to be more effective against prostate tumors with a constitutively activated PI3K pathway, which become dependent on PI3K signaling for their growth and survival.25,26
Although this narrows the spectrum of potentially targeted tumors compared to “non-specific” cytotoxic drugs, there are several advantages of targeting the PI3K signaling pathway in prostate cancer. First, normal tissues do not require constitutive PI3K activity; thus, the presence of the PI3K inhibitor outside of tumor sites is not expected to produce substantial toxic side effects, as evident from phase I clinical trials with several non-targeted PI3K inhibitors.27,28 Second, as constitutively activated PI3K activity is connected with increased resistance to apoptosis in prostate cancer, a prostate cancer-selective PI3K inhibitor is expected to sensitize prostate tumors to other anti-cancer therapeutics.29,30 Third, as the PI3K inhibitor prodrug cannot enter into cells (and be metabolized) until “released” from inhibiting peptide, these agents should have an improved pharmacokinetic profile compared to unmodified PI3K inhibitor, as reported for SF1126, a LY294002 derivative coupled with a RGDS peptide.14 Also, unlike the original LY294002, which has poor water solubility and must be dissolved in dimethyl sulfoxide, the peptide-coupled prodrug-LY294002 here presented is water soluble and thus, could be easier formulated as an orally or intravenously delivered therapeutic.
Future experiments in mouse models of prostate cancer will examine pharmacokinetics, pharmacodynamics and anti-tumor effects of 11. Should these experiments demonstrate superior properties of 11 comparing to unmodified LY294002, it will justify modification of other PI3K inhibitors into PSA-activated prodrugs and clinical testing of these new prodrug-PI3K inhibitors in patients with advanced prostate cancer. Activating mutations of PI3K pathway are observed in almost all advanced prostate tumors; therefore introducing improved prostate-selective PI3K inhibitors into the clinic may benefit substantial number of prostate cancer patients.
Experimental Section
Chemical synthesis
8-(4-(Hydroxymethyl)phenyl)-2-morpholino-4H-chromen-4-one (8)
2-Morpholin-4-yl-4-oxo-4H-chromen-8-yl trifluoromethanesulfonate, 7 (100 mg, 0.263 mmol) was dissolved in 5:1 MeCN/EtOH (10 mL). K2CO3 (2.5 eq., 0.091 g, 0.658 mmol) was added and the solution was degassed with N2. 4-(Hydroxymethyl)phenylboronic acid (1.21 eq., 0.048 g, 0.318 mmol) and Pd(OAc)2 (0.1 eq., 0.006 g, 0.0263 mmol) were added and the solution refluxed overnight. The solution was cooled to room temperature, filtered through Celite®, washed with MeCN (10 mL), and dried with Na2SO4. The reaction mixture was condensed by rotary evaporation and purified on alumina using 95:5 ethyl acetate/ethanol as an eluent to give 8-(4-(hydroxymethyl)phenyl)-2-morpholino-4H-chromen-4-one as a pale yellow powder (0.062 g, 0.184 mmol, 67%): Rf 0.5 (95:5 ethyl acetate/ethanol). 1H NMR (300 MHz, CDCl3) δ 8.18 (dd, J = 1.7, 7.9 Hz, 1H), 7.50 (m, 6H), 5.52 (s, 1H), 4.80 (s, 2H), 3.74 (t, J = 4.8 Hz, 4H), 3.36 (t, J = 5.1 Hz, 4H). 13C NMR (75.47 MHz, CDCl3) δ 177.23, 162.57, 150.57, 140.93, 135.49, 133.56, 130.03, 129.46, 126.82, 125.05, 124.76, 123.35, 87.03, 65.88, 64.75, 44.74. HRMS [M+H]+ calculated for C20H19NO4, 338.1392; found, 338.1393.
4-(2-Morpholino-4-oxo-4H-chromen-8-yl)benzyl-2-(tert-butoxycarbonylamino)-4-methylpentanoate (9)
8-(4-(Hydroxymethyl)phenyl)-2-morpholino-4H-chromen-4-one, 8 (0.259 g, 0.766 mmol) was dissolved in DCM (20 mL). N-α-tert-Butoxycarbonyl-l-leucine (2 eq., 0.354 g, 1.532 mmol), DCC (2 eq., 0.316 g, 1.532 mmol) and DMAP (1 eq., 0.094 g, 0.766 mmol) were added and the solution was stirred at room temperature overnight. DCM (90 mL) was added and the solution was washed with cold 1M HCl (80 mL), NaHCO3 (60 mL) and brine (60 mL). Organic fractions were dried with Na2SO4 and the reaction mixture was condensed by rotary evaporation and purified on alumina using ethyl acetate as an eluent to give 4-(2-morpholino-4-oxo-4H-chromen-8-yl)benzyl-2-(tert-butoxycarbonylamino)-4-methylpentanoate as a clear oil (0.161 g, 0.293 mmol, 38%): Rf 0.6 (100% ethyl acetate). 1H NMR (300 MHz, CDCl3) δ 8.16 (dd, J = 1.8, 7.8 Hz, 1H), 7.56 – 7.37 (m, 6H), 5.52 (s, 1H), 5.22 (s, 2H), 4.96 (d, J = 8.6 Hz, 1H), 4.37 (m, 1H), 3.73 (t, J = 4.4 Hz, 4H), 3.34 (t, J = 4.9 Hz, 4H), 2.03 (m, 2H), 1.62 (m, 1H), 1.43 (s, 9H), 0.92 (dd, J = 1.1, 6.5 Hz, 6H). 13C NMR (75.47 MHz, CDCl3) δ 177.10, 173.37, 162.48, 155.39, 150.47, 136.25, 135.38, 133.47, 129.50, 127.94, 125.18, 124.75, 123.31, 87.02, 79.90, 66.34, 65.84, 52.13, 44.66, 41.58, 28.25, 24.75, 22.81, 21.82. HRMS [M+Na]+ calculated for C31H38N2O7, 573.2577; found, 573.2643.
4-(2-Morpholino-4-oxo-4H-chromen-8-yl) benzyl-2-amino-4-methylpentanoate (10)
4-(2-Morpholino-4-oxo-4H-chromen-8-yl) benzyl-2-(tert-butoxycarbonylamino)-4-methylpentanoate, 9 (0.070 g, 0.127 mmol) was dissolved in MeCN (15 mL). p-TsOH•H2O (2 eq., 0.044 g, 0.254 mmol) was added and the solution stirred at room temperature for 42 h. p-TsOH•H2O (1 eq., 0.022 g, 0.127 mmol) was added and the solution stirred for an additional 23 h. The reaction mixture was condensed by rotary evaporation. The solid residue was dissolved in cold H2O (6 mL) and ethyl acetate (10 mL) was added. The aqueous layer was separated and saturated NaHCO3 (5 mL) was added. An aqueous layer was extracted with ethyl acetate (3×10 mL). Organic fractions were dried with Na2SO4 and solvent was removed by rotary evaporation to give 4-(2-morpholino-4-oxo-4H-chromen-8-yl)benzyl 2-amino-4-methylpentanoate as a white solid (0.033 g, 0.073 mmol, 58%). 1H NMR (300 MHz, CDCl3) δ 8.16 (dd, J = 1.6, 7.8 Hz, 1H), 7.46 (m, 6H), 5.52 (s, 1H), 5.22 (s, 2H), 3.71 (t, J = 4.8 Hz, 4H), 3.57 (m, 1H), 3.34 (t, J = 5.0 Hz, 4H), 1.91 (m, 2H), 1.62 (m, 1H), 0.91 (t, J = 6.5 Hz, 6H). 13C NMR (75.47 MHz, CDCl3) δ 177.53, 176.60, 162.93, 150.93, 136.78, 136.04, 133.91, 130.12, 130.00, 128.52, 125.66, 125.21, 123.77, 87.50, 66.55, 66.29, 45.13, 44.48, 29.17, 25.19. HRMS [M+H]+ calculated for C26H30N2O5, 451.2233; found, 451.2302.
Purity of compounds was measured by LC-ESI-MS analysis using an Accela Open 1200 UHPLC coupled to a LTQ XL Orbitrap mass spectrometer (Thermo Fisher Scientific, Waltham, MA), resulting to be ≥95%. Purity of 11 resulted >95% after LC-ESI-MS analysis, was conducted at AnaSpec, Inc., and provided with the certificate of analysis.
Cell Cultures
The hormone-responsive prostate cancer LNCaP and breast cancer BT-549 cell lines were purchased from ATCC (Manassas, VA). The androgen-independent prostate cancer LNCaP subline C4-2 and the glioblastoma-astrocytoma U-87 MG cells were generous gifts from Dr. Leland Chung (Cedars-Sinai Medical Center, Los Angeles, CA) and Dr. Frank Furnari (University of California, San Diego, CA), respectively.
All cells were maintained in a humidified atmosphere (5% CO2) at 37 °C, using RPMI 1640 (C4-2, C4-2LucBAD and BT-549), T-Medium (LNCaP), and DMEM (U-87 MG) supplemented with 10% FBS (5% for LNCaP). BT-549 medium was also supplemented with 0.023 U/mL of insulin. All tissue culture reagents were purchased from Invitrogen (Carlsbad, CA).
Experimental set-up
If not otherwise indicated, cells were seeded at 4×105/6 cm Petri dish and kept in culture for 48 h to reach about 80% confluence before starting any experiments. Cells were kept in a serum-free media condition (LNCaP cells were kept in medium supplemented with 2.5% FBS). C4-2LucBAD cells were kept in serum-free medium for 18 h to increase PSA concentration.
Total PSA electrochemiluminescence immunoassay
Total PSA was assayed with a Cobas Elecsys Total PSA according to manufacturer protocol, using a Roche Elecsys 2010 Chemistry Analyzer (Roche, Basel, Switzerland). Each sample was assayed in triplicate.
Western Blotting
Media were removed and cells washed gently twice times using cold phosphate buffered saline (PBS) on ice. Lysates were generated using cold 20 mM HEPES, 150 mM NaCl, 1 mM EDTA, 0.5% Na+Deoxycholate, 1% Nonidet P-40, 1 mM DTT pH 7.4 buffer containing protease inhibitors (10 μg/mL aprotinin, 10 μg/mL leupeptin, 10 μg/mL pepstatin, 1 mM benzamidine, 1 mM PMSF) and phosphatase inhibitors (1 mM NaVO4, 50 mM β-glycerophosphate, 40 mM p-nitrophenylphosphate, 40 mM NaF and 1 μg/mL microcystin). All reagents were purchased from Sigma-Aldrich (St. Louis, MO). Cell lysates were clarified by centrifugation at 15000 rpm for 15 min at 4 °C, and the supernatant collected and protein content measured by a Bradford assay (Bio-Rad Laboratories, Hercules, CA) according to the manufacturer's directions. Proteins were separated on SDS-PAGE on 12% gels and transferred onto a 0.45 μm nitrocellulose membrane (PerkinElmer, Waltham, MA). Western blotting was performed with the Odyssey CLx Infrared Imaging System (Li-Cor Biosciences, Lincoln, NE), according to the manufacturer's instructions. Rabbit polyclonal anti-p-Akt Thr308, anti-Akt and anti-Cleaved PARP (Asp214) were purchased from Cell Signaling Technology (Beverly, MA). Mouse monoclonal anti-β-Actin was purchased from Sigma-Aldrich. Secondary goat anti-mouse IRDye 680 and goat-anti rabbit IRDye 800 were both purchased from Li-Cor Biosciences. Protein bands were quantified using ImageJ software (National Institutes of Health, USA).
Caspase 3 Assay
Apoptosis in whole cell populations was assessed by monitoring Caspase 3 activity with the specific fluorogenic substrate Ac-DEVD-7-amido-4-trifluoromethylcoumarin (Bachem, Torrance, CA), as previously reported 30. On ice, adherent and floating cells were collected and lysed using a cold lysis buffer (1% Nonidet P-40, 150 mM NaCl, 20 mM HEPES, 1 mM EDTA, 1 mM DTT, and 5 μg/mL aprotinin, leupeptin, and pepstatin, respectively). Fluorescence was recorded each 15 min for 1 h using a VersaFluor (BioRad, Hercules, CA). Caspase 3 activity was expressed in arbitrary units and calculated using Excel 2010 (Microsoft Corporation, Redmond, WA).
LC-ESI-MS analysis
LC-ESI-MS analysis was performed using an Accela Open 1200 UHPLC coupled to a LTQ XL Orbitrap mass spectrometer (Thermo Fisher Scientific, Waltham, MA). Separation was accomplished using a ZORBAX Eclipse XDB-C18 (1.8 μm, 2.1 × 50 mm) analytical column with a ZORBAX extend C18 Narrow Bore Guard column (5 μm, 2.1 × 12.5 mm) (Agilent Technologies, Santa Clara, CA). The following mobile phases were used for the separation: Solvent A, water/0.1% formic acid, and solvent B, methanol/0.1% formic acid. The gradient used for separation was 95% to 5% solvent A over 10 min at a flow rate of 250 μL/min. Using the mass of 496.2569 ± 0.005, optimized positive mode ESI conditions were found as follows: sheath and aux gas were 60 and 4 arbitrary units, respectively, spray voltage 4 kV, capillary temperature and voltage were 325 °C and 49 V, and the tube lens was 115 V. Full scan high-resolution mass spectra were collect at 60,000 Hz from 150 to 2000 m/z. The full scan data for standard curve samples and unknowns were processed with Xcalibur software to determine concentrations (Thermo Fisher Scientific, Waltham, MA).
C4-2 conditioned medium assay
C4-2 and BT-549 cells were cultured as described above. 11 was added to the medium with C4-2 cells and incubated for 6 h at 37 °C in a humidified atmosphere (5% CO2) in serum-free medium. Medium was then collected and added to BT-549 cells for 3 h. Inhibition of PI3 kinase pathway was followed by monitoring the p-Akt T308 levels by Western blotting.
Cleavage of Compound 11 with purified PSA
Compound 11 was incubated in 50 mM Tris-HCl, 0.1 M NaCl, pH 7.8 buffer for 6 h at 37 °C with purified active human PSA (Merck, Darmstadt, Germany) and then added to BT-549 cells for 30 min, cultured as previously described. Inhibition of PI3 kinase was followed by monitoring p-Akt T308 levels by Western blotting.
Statistical Analysis
Probability (p) values were calculated using the ANOVA one-way test; p values ≤ 0.05 were considered statistically significant. The results are expressed as means ± SEM, n=3.
Acknowledgment
We thank Dr. Marcus W. Wright (Wake Forest University, Dept. of Chemistry) for LC-ESI-MS analysis and Ms. Tina Snider (Dept. of Urology, Wake Forest Baptist Health), for performing ECLIA tPSA assays and Karen Kline for editing. This work was supported by WFU Cross-Campus Collaborative Research Program and R01CA118329 to G.K.
Abbreviations List
- BAD
Bcl-2-associated death promoter
- Bcl-2
B-cell lymphoma 2
- Bcl-XL
B-cell lymphoma extra-large
- DCC
N,N’-dicyclohexylcarbodiimide
- DCM
dichloromethane
- DMAP
4-dimethylaminopyridine
- DMSO
dimethyl sulfoxide
- DTT
dithiothritol
- PARP
Poly(ADP-Ribose) Polymerase
- PBS
phosphate buffer saline
- PI3K
Phosphatidylinositol-3-kinase
- PSA
Prostate-Specific Antigen
- PTEN
Phosphatase and tensin homolog deleted on chromosome 10
Footnotes
The authors declare no competing financial interest.
References
- 1.Wang X, Ma D, Olson WC, Heston WD. In vitro and in vivo responses of advanced prostate tumors to PSMA ADC, an auristatin-conjugated antibody to prostate-specific membrane antigen. Mol Cancer Ther. 2011;10:1728–1739. doi: 10.1158/1535-7163.MCT-11-0191. [DOI] [PubMed] [Google Scholar]
- 2.Sarker D, Reid AHM, Yap TA, de Bono JS. Targeting the PI3K/AKT pathway for the treatment of prostate cancer. Clin Cancer Res. 2009;15:4799–4805. doi: 10.1158/1078-0432.CCR-08-0125. [DOI] [PubMed] [Google Scholar]
- 3.Cohen MB, Rokhlin OW. Mechanisms of prostate cancer cell survival after inhibition of AR expression. J Cell Biochem. 2009;106:363–371. doi: 10.1002/jcb.22022. [DOI] [PubMed] [Google Scholar]
- 4.Morgan TM, Koreckij TD, Corey E. Targeted therapy for advanced prostate cancer: inhibition of the PI3K/Akt/mTOR pathway. Curr Cancer Drug Targets. 2009;9:237–249. doi: 10.2174/156800909787580999. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Mazzoletti M, Bortolin F, Brunelli L, Pastorelli R, Di Giandomenico S, Erba E, Ubezio P, Broggini M. Combination of PI3K/mTOR inhibitors: antitumor activity and molecular correlates. Cancer Res. 2011;71:4573–4584. doi: 10.1158/0008-5472.CAN-10-4322. [DOI] [PubMed] [Google Scholar]
- 6.Erlich RB, Kherrouche Z, Rickwood D, Endo-Munoz L, Cameron S, Dahler A, Hazar-Rethinam M, de Long LM, Wooley K, Guminski A, Saunders NA. Preclinical evaluation of dual PI3K-mTOR inhibitors and histone deacetylase inhibitors in head and neck squamous cell carcinoma. Br J Cancer. 2012;106:107–115. doi: 10.1038/bjc.2011.495. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Bjork T, Lilja H, Christensson A. The prognostic value of different forms of prostate specific antigen and their ratios in patients with prostate cancer. BJUInt. 1999;84:1021–1027. doi: 10.1046/j.1464-410x.1999.00345.x. [DOI] [PubMed] [Google Scholar]
- 8.LeBeau AM, Singh P, Isaacs JT, Denmeade SR. Prostate-specific antigen is a “chymotrypsin-like” serine protease with unique P1 substrate specificity. Biochemistry. 2009;48:3490–3496. doi: 10.1021/bi9001858. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Evans-Axelsson S, Ulmert D, Orbom A, Peterson P, Nilsson O, Wennerberg J, Strand J, Wingardh K, Olsson T, Hagman Z, Tolmachev V, Bjartell A, Lilja H, Strand SE. Targeting free prostate-specific antigen for in vivo imaging of prostate cancer using a monoclonal antibody specific for unique epitopes accessible on free prostate-specific antigen alone. Cancer Biother Radiopharm. 2012;27:243–251. doi: 10.1089/cbr.2011.1088. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Coombs GS, Bergstrom RC, Pellequer JL, Baker SI, Navre M, Smith MM, Tainer JA, Madison EL, Corey DR. Substrate specificity of prostate-specific antigen (PSA). Chem Biol. 1998;5:475–488. doi: 10.1016/s1074-5521(98)90004-7. [DOI] [PubMed] [Google Scholar]
- 11.LeBeau AM, Banerjee SR, Pomper MG, Mease RC, Denmeade SR. Optimization of peptide-based inhibitors of prostate-specific antigen (PSA) as targeted imaging agents for prostate cancer. Bioorg Med Chem. 2009;17:4888–4893. doi: 10.1016/j.bmc.2009.06.012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Vlahos CJ, Matter WF, Brown RF, Traynor-Kaplan AE, Heyworth PG, Prossnitz ER, Ye RD, Marder P, Schelm JA, Rothfuss KJ, Serlin BS, Simpson PJ. Investigation of neutrophil signal transduction using a specific inhibitor of phosphatidylinositol 3-kinase. J Immunol. 1995;154:2413–2422. [PubMed] [Google Scholar]
- 13.Holmes D. PI3K pathway inhibitors approach junction. Nat Rev Drug Discov. 2011;10:563–564. doi: 10.1038/nrd3527. [DOI] [PubMed] [Google Scholar]
- 14.Garlich JR, De P, Dey N, Su JD, Peng X, Miller A, Murali R, Lu Y, Mills GB, Kundra V, Shu HK, Peng Q, Durden DL. A vascular targeted pan phosphoinositide 3-kinase inhibitor prodrug, SF1126, with antitumor and antiangiogenic activity. Cancer Res. 2008;68:206–215. doi: 10.1158/0008-5472.CAN-07-0669. [DOI] [PubMed] [Google Scholar]
- 15.Gharbi SI, Zvelebil MJ, Shuttleworth SJ, Hancox T, Saghir N, Timms JF, Waterfield MD. Exploring the specificity of the PI3K family inhibitor LY294002. Biochem J. 2007;404:15–21. doi: 10.1042/BJ20061489. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Morris GM, Goodsell DS, Halliday RS, Huey R, Hart WE, Belew RK, Olson AJ. Automated Docking Using a Lamarckian Genetic Algorithm and and Empirical Binding Free Energy Function J. Computational Chemistry. 1998:1639–1662. [Google Scholar]
- 17.B. Abbott PT. Synthetic Studies of the Phosphatidylinositol 3-Kinase Inhibitor LY294002 and Related Analogues. Aust. J. Chem. 2003;56:1099–1106. [Google Scholar]
- 18.Zha J, Harada H, Yang E, Jockel J, Korsmeyer SJ. Serine phosphorylation of death agonist BAD in response to survival factor results in binding to 14-3-3 not BCL-X(L). Cell. 1996;87:619–628. doi: 10.1016/s0092-8674(00)81382-3. [DOI] [PubMed] [Google Scholar]
- 19.Datta SR, Dudek H, Tao X, Masters S, Fu H, Gotoh Y, Greenberg ME. Akt phosphorylation of BAD couples survival signals to the cell-intrinsic death machinery. Cell. 1997;91:231–241. doi: 10.1016/s0092-8674(00)80405-5. [DOI] [PubMed] [Google Scholar]
- 20.del Peso L, Gonzalez-Garcia M, Page C, Herrera R, Nunez G. Interleukin-3-induced phosphorylation of BAD through the protein kinase Akt. Science. 1997;278:687–689. doi: 10.1126/science.278.5338.687. [DOI] [PubMed] [Google Scholar]
- 21.Sastry KSR, Karpova Y, Kulik G. Epidermal growth factor protects prostate cancer cells from apoptosis by inducing BAD phosphorylation via redundant signaling pathways. J Biol Chem. 2006;281:27367–27377. doi: 10.1074/jbc.M511485200. [DOI] [PubMed] [Google Scholar]
- 22.Khan SR, Denmeade SR. In vivo activity of a PSA-activated doxorubicin prodrug against PSA-producing human prostate cancer xenografts. Prostate. 2000;45:80–83. doi: 10.1002/1097-0045(20000915)45:1<80::aid-pros10>3.0.co;2-q. [DOI] [PubMed] [Google Scholar]
- 23.Brady SF, Pawluczyk JM, Lumma PK, Feng DM, Wai JM, Jones R, DeFeo-Jones D, Wong BK, Miller-Stein C, Lin JH, Oliff A, Freidinger RM, Garsky VM. Design and synthesis of a pro-drug of vinblastine targeted at treatment of prostate cancer with enhanced efficacy and reduced systemic toxicity. J Med Chem. 2002;45:4706–4715. doi: 10.1021/jm020139f. [DOI] [PubMed] [Google Scholar]
- 24.Denmeade SR, Jakobsen CM, Janssen S, Khan SR, Garrett ES, Lilja H, Christensen SB, Isaacs JT. Prostate-specific antigen-activated thapsigargin prodrug as targeted therapy for prostate cancer. J Natl Cancer Inst. 2003;95:990–1000. doi: 10.1093/jnci/95.13.990. [DOI] [PubMed] [Google Scholar]
- 25.Rudner J, Ruiner CE, Handrick R, Eibl HJ, Belka C, Jendrossek V. The Akt-inhibitor Erufosine induces apoptotic cell death in prostate cancer cells and increases the short term effects of ionizing radiation. Radiat Oncol. 2010;5:108. doi: 10.1186/1748-717X-5-108. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Ellwood-Yen K, Keilhack H, Kunii K, Dolinski B, Connor Y, Hu K, Nagashima K, O'Hare E, Erkul Y, Di Bacco A, Gargano D, Shomer NH, Angagaw M, Leccese E, Andrade P, Hurd M, Shin MK, Vogt TF, Northrup A, Bobkova EV, Kasibhatla S, Bronson RT, Scott ML, Draetta G, Richon V, Kohl N, Blume-Jensen P, Andersen JN, Kraus M. PDK1 attenuation fails to prevent tumor formation in PTEN-deficient transgenic mouse models. Cancer Res. 2011;71:3052–3065. doi: 10.1158/0008-5472.CAN-10-2282. [DOI] [PubMed] [Google Scholar]
- 27.Yuan J, Mehta PP, Yin MJ, Sun S, Zou A, Chen J, Rafidi K, Feng Z, Nickel J, Engebretsen J, Hallin J, Blasina A, Zhang E, Nguyen L, Sun M, Vogt PK, McHarg A, Cheng H, Christensen JG, Kan JL, Bagrodia S. PF-04691502, a potent and selective oral inhibitor of PI3K and mTOR kinases with antitumor activity. Mol Cancer Ther. 2011;10:2189–2199. doi: 10.1158/1535-7163.MCT-11-0185. [DOI] [PubMed] [Google Scholar]
- 28.Brachmann SM, Hofmann I, Schnell C, Fritsch C, Wee S, Lane H, Wang S, Garcia-Echeverria C, Maira SM. Specific apoptosis induction by the dual PI3K/mTor inhibitor NVP-BEZ235 in HER2 amplified and PIK3CA mutant breast cancer cells. Proc Natl Acad Sci U S A. 2009;106:22299–22304. doi: 10.1073/pnas.0905152106. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Wallin JJ, Edgar KA, Guan J, Berry M, Prior WW, Lee L, Lesnick JD, Lewis C, Nonomiya J, Pang J, Salphati L, Olivero AG, Sutherlin DP, O'Brien C, Spoerke JM, Patel S, Lensun L, Kassees R, Ross L, Lackner MR, Sampath D, Belvin M, Friedman LS. GDC-0980 is a novel class I PI3K/mTOR kinase inhibitor with robust activity in cancer models driven by the PI3K pathway. Mol Cancer Ther. 2011;10:2426–2436. doi: 10.1158/1535-7163.MCT-11-0446. [DOI] [PubMed] [Google Scholar]
- 30.Sastry KSR, Karpova Y, Prokopovich S, Smith AJ, Essau B, Gersappe A, Carson JP, Weber MJ, Register TC, Chen YQ, Penn RB, Kulik G. Epinephrine protects cancer cells from apoptosis via activation of cAMP-dependent protein kinase and BAD phosphorylation. J Biol Chem. 2007;282:14094–14100. doi: 10.1074/jbc.M611370200. [DOI] [PubMed] [Google Scholar]