Abstract
Prime Time, a youth development intervention, aims to reduce multiple risk behaviors among adolescent girls seeking clinic services who are at high risk for pregnancy. The purpose of the current study was to examine whether Prime Time involvement produced changes in relational aggression, physical violence and related psychosocial and behavioral outcomes. Qualitative case exemplars illustrated social contexts of intervention participants with differing longitudinal patterns of relational aggression and physical violence. Data were from a randomized efficacy trial with 13–17 year old girls (n=253) meeting specified risk criteria. Intervention participants were involved in Prime Time and usual clinic services for 18 months, control participants received usual clinic services. Participants in the current study completed self-report surveys at baseline and 18 months following enrollment. Outcomes analyses revealed significantly lower levels of relational aggression perpetration in the intervention group versus controls. In contrast, Prime Time involvement did not result in significant reductions in physical violence. Exploratory dose-response analyses indicated that reductions in relational aggression may have been most pronounced among girls actively involved in Prime Time case management and peer leadership activities. Qualitative findings suggested that the intervention’s emphasis on modeling and building supportive relationships contributed to reductions in relational aggression. This study contributes to a very limited evidence base regarding effective approaches to preventing violence among high-risk adolescent girls. Findings suggest that offering youth development interventions through clinic settings hold promise in reducing violence risk among vulnerable youth.
Keywords: Aggression, Violence Prevention, Adolescent Girls, Vulnerable Populations, Randomized Trial
Introduction
Striking recent increases in aggression and violence among adolescent girls have captured the attention of scholars and public health practice audiences. From 1985 to 2007, the number of delinquency cases involving girls increased 101%; the number of cases involving boys increased only 30% during the same period (Puzzanchera et al. 2010). According to national crime statistics, from 1996 to 2005, the number of juvenile arrests for violent crimes increased 24% for girls, but decreased 4% for boys (FBI 2006). In a 2009 national survey, 23% of 9–12th grade girls reported being in one or more physical fights in the past year (CDC 2010). Among 9th and 12th graders in Minnesota, 13% of girls noted being kicked, bit, or hit by another student and 15% noted that they had hit or beat up someone in the past year (MDE 2007).
Physical violence involvement has important consequences for adolescent physical and mental health. Among 10–24 year olds, homicide is the 2nd leading cause of death (CDC 2010). In 2008, over 656,000 10–24 year olds were treated in emergency departments for violence-related injuries (CDC 2010). Youth involvement in physical violence has been associated with depression, distress, externalizing behaviors and pregnancy (Kirby and Lepore 2007; Buka et al. 2001). Physical violence within adolescent dating relationships, for example, has been linked to reproductive health outcomes including risk for pregnancy and sexually transmitted infections (Silverman et al. 2004). Given the co-occurrence of risk across multiple development domains, scholars and practitioners have argued for integrated prevention and intervention programs that target both violence involvement and reproductive health (Minnis et al. 2008).
In addition to physical violence, other forms of aggression are all-too-common among girls. Relational aggression is often considered a less direct form of aggression. Unlike physical violence, in which the goal may be to hurt or physically threaten someone, the goal of relational aggression is to damage the social standing or self-esteem of peers by using verbal rejection, rumor spreading, social ostracism, and gossip (Cairns et al. 1989). In a 2009 national survey, approximately 21% of female high school students reported being bullied on school property in the preceding 12 months (CDC 2010). Among 9th and 12th graders in Minnesota, 37% of girls reported that another student had made fun of them in a hurtful way in the past month; 41% reported making fun of another student (MDE 2007).
Similar to physical violence, relational aggression has been linked to poor health outcomes among youth. Victims of relational aggression are at increased risk for depression and suicidality (van der Wal et al. 2003), social and emotional adjustment difficulties, poor peer relationships, and loneliness (Crick and Grotpeter 1995). Perpetrators of relational aggression are at risk for physical violence, internalizing and externalizing behavior problems (Laird et al. 2001; Murray-Close et al. 2007) and substance use (Herrenkohl et al. 2009).
The prevalence of aggression and violence among adolescent girls and the multiple adverse outcomes related to these behaviors provide a compelling rationale for identifying effective preventative approaches. Youth Violence: A Report of the Surgeon General (DHHS 2001) calls for adoption of evidence-based public health approaches to preventing violence, including approaches that employ a dual strategy of addressing risks while building protective factors that buffer youth from violence involvement. To date, there is a startling dearth of evidence regarding effective approaches for preventing aggression and violence among girls (Zahn et al. 2008).
Sustained, multifaceted violence prevention efforts may be particularly important for youth at high risk for violence involvement including those living in neighborhoods characterized by high levels of poverty, residential mobility and violence (Limbos et al. 2007). Rather than aiming to ameliorate risk, preventive interventions grounded in a resilience paradigm emphasize developing internal assets and external resources among youth exposed to multiple environmental risks (Fergus and Zimmerman 2005). Such a focus is consistent with research regarding compensatory effects of assets and resources on cumulative risks for violent behavior. For example, among youth held back in school, good academic performance and strong family and school connections were protective against violence involvement and compensated for the negative effects of prior violence involvement (Borowsky et al. 2002). While many youth at high risk for violence involvement utilize clinic services, very little evidence exists on effective primary care services to prevent such outcomes (Borowsky et al. 2004).
Prime Time is a multi-component youth development intervention for adolescent girls at high risk for pregnancy. Designed for primary care clinics, this 18-month intervention aims to reduce precursors of teen pregnancy including sexual risk behaviors, violence involvement, and school disconnection. A randomized efficacy trial of the Prime Time intervention involved clinics in Minneapolis and St. Paul, Minnesota. In previous publications, we have demonstrated intervention effects on sexual risk behaviors at a 12-month interim intervention point and at the end of the intervention (18 months), with the intervention group reporting more consistent use of condoms, hormonal contraception and dual contraceptive methods than controls (Sieving et al. 2011a, 2012). In this paper, we examine another behavioral domain targeted by Prime Time -- namely relational aggression, physical violence, and related psychosocial and behavioral outcomes -- at the end of the intervention. Qualitative case exemplars are used to illustrate the social contexts of participants with differing longitudinal patterns of aggression and violence.
Methods
Participants
Study participants were at high risk for teen pregnancy. Specifically, our sample included sexually active girls ages 13–17 who met one or more of the following risk criteria: (1) clinic visit involving negative pregnancy test (Zabin et al. 1994); (2) clinic visit involving treatment for sexually transmitted infection (Orr et al. 2001); (3) young teens (ages 13–14; Kirby 2007); (4) aggressive and violent behaviors (Kirby 2007); (5) sexual risk behaviors (Kirby 2007); (6) behaviors indicating school disconnection (Kirby 2007). Recent sexual activity and risk criteria 3–6 (above) were assessed with a brief self-report screening tool (Sieving et al. 2011b). Girls who did not understand consent forms, were married, pregnant or had given birth were excluded. The study was approved by university and participating clinics’ institutional review boards.
Two community and two school-based primary care clinics served as study recruitment sites. In terms of usual services, community clinics reported that adolescents were most commonly seen for general medical concerns, while school-based clinics reported that youth were most commonly seen for reproductive health reasons and mental health concerns. Among high-risk girls similar to our study sample (i.e., never pregnant 13–19 year olds with a referent clinic visit involving a negative pregnancy test or STI treatment), a review of clinic charts (n=20 charts per clinic) revealed relatively frequent clinic visits. Usual clinic services for this high-risk group involved an average of 3.5–6.4 clinic visits per year.
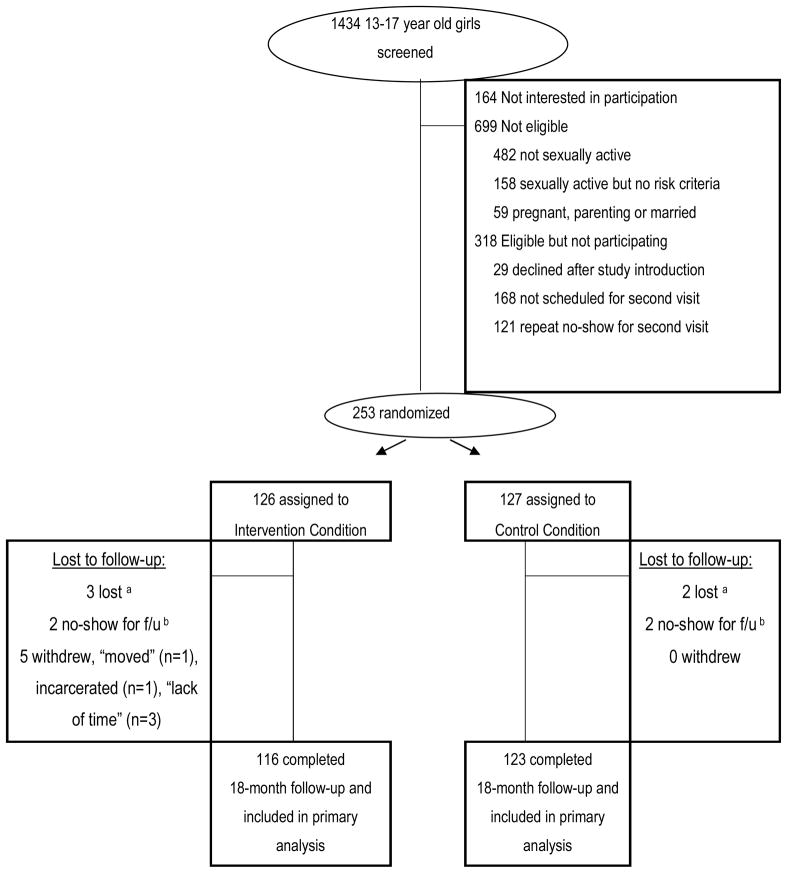
From April 2007 through October 2008, trained study staff screened 1434 girls at participating clinics (Figure 1). Of these, 571 sexually active girls who met one or more study risk criteria were invited to participate. Study enrollment involved two clinic visits, to minimize attrition (Henneken 1987) which is particularly problematic in high-risk, highly mobile youth populations (Sussman et al. 2002). At the first visit, study staff identified study-eligible girls and invited them to return for a second visit within two weeks. At the second visit, girls signed an informed consent statement, provided study baseline data and were randomized into study conditions. A total of 253 girls (44% of eligible) enrolled, a participation rate comparable to previous clinic-based intervention studies with high-risk youth (e.g., Shrier et al. 2001).
Figure 1. Flow of Prime Time Study Participants.
a Lost participants were those whom we were unable to locate.
b No-show participants were contacted and scheduled for a follow-up survey but did not complete the survey.
Demographic characteristics and risk behavior items on the screening tool (completed at the first visit) were used to compare participants (n=253) to eligible girls who did not enroll (n=318). The two groups were similar on multiple demographic and behavioral indicators (Sieving et al. 2011a). Participants were more likely than eligible non-participants to be living with one parent (64% vs. 52%; χ2 (2, N=545) =19.09, p=0.015). Furthermore, among eligible non-participants, intervention and control groups, there were no significant differences in the number of risk criteria endorsed on the screening tool (χ2 (10, N=571) =4.05, p=0.945). Across these three groups, the mean number of study risk criteria was 1.74.
Participants’ demographic characteristics, aggressive and violent behaviors at baseline are in Table 1. Intervention and control groups were equivalent on these descriptors. Baseline data indicated relatively high rates of aggression and violence in this sample compared to teen girls in Minnesota and the nation (e.g., Youth Risk Behavior Survey 2007 (CDC 2008); Minnesota Student Survey 2007 (MDE 2007)). For example, while 14.7% of Minnesota 9th and 12th grade girls noted hitting or beating someone up in the past 12 months, 43% of this sample noted hitting or beating someone up in a shorter time interval (6 months).
Table 1.
Baseline Characteristics of Prime Time Study Participants by Intervention Condition
| Intervention Group (n = 126) | Control Group (n = 127) | p-value* | |
|---|---|---|---|
|
|
|||
| Age, mean (se) | 15.7 (0.07) | 15.49 (0.21) | 0.334 |
| Race/Ethnicitya | 0.118 | ||
| American Indian/Native American | 3% | 2% | |
| Asian/Asian American/Pacific Islander | 10% | 13% | |
| Black/African/African American | 45% | 38% | |
| Hispanic /Latina | 17% | 8% | |
| White/European American | 6% | 16% | |
| Mixed/Multiple | 19% | 23% | |
| # Adults/guardians in homeb (n=252) | 0.152 | ||
| No adult guardian | 4% | 2% | |
| 1 adult guardian | 46% | 44% | |
| 2 adult guardians | 38% | 46% | |
| Other arrangements | 12% | 8% | |
| # Places lived, past 6 months | 0.811 | ||
| 1 place | 58% | 61% | |
| 2 or more places | 42% | 39% | |
| Receipt of public assistance, past yearc (n=252) | 0.343 | ||
| No | 43% | 51% | |
| Yes | 33% | 32% | |
| Unsure | 24% | 17% | |
| Currently enrolled in school (n=250) | 94% | 96% | 0.096 |
| History of school suspension (% Yes) (n=251) | 65% | 75% | 0.138 |
| Put someone down or called them names, past 30 days (n=250) | |||
| Never | 25% | 21% | 0.424 |
| 1–2 times | 42% | 37% | |
| 3 or more times | 33% | 42% | |
| Ignored or left someone out on purpose, past 30 days (n=250) | 0.509 | ||
| Never | 45% | 40% | |
| 1–2 times | 40% | 40% | |
| 3 or more times | 15% | 20% | |
| Hit or beat someone up, past 6 months (n=251) | 0.636 | ||
| Never | 60% | 55% | |
| 1–2 times | 32% | 35% | |
| 3 or more times | 8% | 10% | |
| Someone put you down or called you names, past 30 days (n=249) | 0.460 | ||
| Never | 23% | 25% | |
| 1–2 times | 48% | 40% | |
| 3 or more times | 29% | 35% | |
| Someone ignored or left you out on purpose, past 30 days (n=248) | 0.581 | ||
| Never | 47% | 45% | |
| 1–2 times | 37% | 32% | |
| 3 or more times | 16% | 23% | |
| Someone hit or beat you up, past 6 months (n=251) | 0.138 | ||
| Never | 75% | 69% | |
| 1–2 times | 22% | 22% | |
| 3 or more times | 3% | 9% | |
p-values associated with chi-square tests of differences between intervention and control groups. Analyses adjusted for within-clinic clustering
Mutually exclusive race categories; participants were allowed to select more than one category
May include biologic/adoptive mother, biologic/adoptive father, stepmother, stepfather, foster mother, foster father, grandmother, grandfather, other guardian
Public assistance includes welfare payments, M-FIP, public assistance, or food stamps
Intervention Components
The resilience paradigm (Resnick 2000), social cognitive theory (Bandura 1986) and findings from a Prime Time pilot study (Sieving et al. 2012) guided design of the Prime Time intervention. The intervention explicitly sought change in selected psychosocial and behavioral attributes linked to violence involvement and other targeted risk behaviors (Kirby 2007).
Girls were involved in intervention programming for 18 months. All programming was led by intervention research staff, who were case managers experienced in working with urban teens from diverse cultural backgrounds. Case managers completed an initial 4-week training focused on intervention principles, practice and feedback in implementing core intervention strategies. Case managers received weekly clinical supervision throughout the intervention, detailed elsewhere (Tanner et al. 2012). Each intervention component is summarized below and described more fully elsewhere (Sieving et al. 2011b).
Case Management
The overall goal of Prime Time case management was to establish a trusting relationship in which a teen and her case manager worked together to address attributes targeted by this intervention. Interviews with intervention staff indicated that within this vulnerable group there was considerable variability in girls’ initial interest and abilities to engage with case managers. Thus, case managers used distinct strategies to establish trusting relationships with girls who were easier or more difficult to engage (Tanner et al. 2012).
One-on-one visits focused on a set of core topics including emotional and social skills, and positive family, school and community involvement. Case managers helped girls develop positive relationships and access appropriate resources within family, school and community contexts. As a client-centered approach, the capacities, interests and needs of individual participants determined the topics and strategies employed during any particular visit. With each girl actively involved in case management, all core topics were addressed over a 6-month interval. Within a month of enrollment, case managers attempted an initial visit with each intervention participant. Monthly visits occurred for the duration of the 18-month intervention in community locations that were convenient for individual teens. Participants received $10 for each monthly visit. Case managers were available to teens as needed between scheduled monthly visits.
Peer Leadership Components
Designed to complement case management, youth leadership groups provided hands-on skill-building experiences. Peer educator training activities addressed basic skills to function constructively in a group. Service learning activities expanded on skills for pro-social group involvement acquired in peer educator training. All youth leadership group sessions were led by two case managers, held in convenient community locations, and involved 4–12 girls. Informal conversations were used to counsel individual girls who described using aggressive or violent behaviors outside of groups.
Peer Educator Training and Employment: Just in Time
The overall goal of Just In Time was to provide opportunities for positive peer, school and community involvement by actively engaging participants as peer health educators. Just In Time peer educator training employed a standard 15-session curriculum addressing communication skills, stress management skills, conflict management skills, expectations and skills for healthy relationships, social influences on sexual behaviors, sexual decision-making skills and contraception. Staff leading Just In Time groups intentionally focused on creating a group atmosphere which was safe, accepting, and valued sharing and listening. Session activities allowed teens to practice group decision-making, problem-solving, and conflict management skills. Weekly homework activities gave teens opportunities to discuss Just In Time topics with adult family members.
Starting with their first training session, girls were instructed to reach and teach others outside of their peer educator group. Girls received $5 for each documented contact, for up to 50 contacts during their 15-session training. After completing the Just In Time training curriculum, girls engaged in a group teaching practicum with an existing group of students. During this 7-session practicum, groups selected a topic, developed a lesson plan around that topic, taught a group session, adjusted the lesson plan as needed, and taught a second group session.
Service Learning: It’s Our Time
The overall goal of It’s Our Time was to expand girls’ emotional and social skills and their real-world experience in civic engagement and leadership. It’s Our Time groups followed a standard curriculum that included core elements of service learning: preparation, action, reflection and celebration. An initial It’s Our Time unit focused on building group cohesion and identifying participants’ leadership skills. In a second unit, groups explored community needs, assets, and potential service projects. A third unit consisted of implementing a group’s service project over 5–6 sessions (e.g., coat drive for homeless youth, domestic violence awareness campaign in local high school). Each implementation session included a group reflection highlighting the impact of service on recipients and on group members themselves. In a final session, groups celebrated their accomplishments.
Evaluation
All participants completed an audio computer-assisted self interview (A-CASI) survey at baseline and 18 months following enrollment. Research staff trained in A-CASI administration conducted evaluation visits, orienting girls to the computer survey with several non-sensitive practice items. Participants were paid $25 for completing each survey round.
Participants
Of 253 participants who completed baseline surveys, 94.5% (n=239) completed a survey at the end of the 18-month intervention period. Fourteen were lost to follow-up at the 18-month point, 10 of whom were in the intervention condition. There were no significant differences in baseline indicators (i.e., age, ethnicity, public assistance, relational aggression and physical violence) between intervention and control groups completing the 18-month survey. An attrition analysis yielded very few significant differences in baseline characteristics between girls lost to follow-up and those completing the 18-month survey. Compared to girls in the 18-month sample, those lost to follow-up were less likely to be in school at baseline (79% vs. 96%; p<0.01) and more likely to have been suspended from school (86% vs. 69%, p=0.05).
Outcome Measures
Four primary outcome measures were the focus of this analysis: relational aggression perpetration and victimization, physical violence perpetration and victimization. To assess relational aggression, a 30-day reference point was used. To assess physical violence, a 6-month reference was used. This time frame captures variability in behaviors that are episodic in nature (Sieving et al. 2005). Previous research has established the reliability of these measures among youth (Miller-Johnson et al. 2004; Resnick et al. 2004).
Relational aggression measures were adapted from the Multisite Violence Prevention Project (Miller-Johnson et al. 2004). A 6-item scale (α=0.65) assessed relational aggression perpetration in the past 30 days. Sample items included putting someone down or calling them names; leaving someone out on purpose; telling lies about someone. A 6-item scale (α=0.86) assessed relational aggression victimization. Victimization scale items paralleled perpetration items. For both scales, responses were dichotomized to yes or no. Scores ranged from 0 (no relational aggression) to 6 (all forms of aggression).
A 5-item scale (α=0.71), adapted from the National Longitudinal Study of Adolescent Health (Resnick et al. 2004), assessed physical violence perpetration in the past 6 months. Sample items included having been in a group fight; having used or threatened to use a weapon; having hit or beat up someone. Responses were dichotomized to yes or no. Scores ranged from 0 (no perpetration) to 5 (instigated all forms of violence). A 4-item scale (α=0.70) assessed being a victim of physical violence. Victimization items paralleled perpetration items, with the omission of the group fight item. Responses were dichotomized to yes or no. Scores ranged from 0 (no victimization) to 4 (victim of all forms of violence).
Psychosocial and behavioral attributes repeatedly associated with youths’ aggressive and violent behaviors (Borowsky et al. 2008; Resnick et al. 2004) and thus targeted for change by the intervention were also examined. Table 2 includes information on measures of social connectedness, skills for avoiding aggression and violence, and school-related behaviors.
Table 2.
Measurement Information for Related Psychosocial and Behavioral Outcomes
| Construct | # Items | Sample Items | Response Format | Reliability |
|---|---|---|---|---|
|
Social Connectedness
| ||||
| Family connectedness | 5 | My family cares about me. I feel close to my family. |
4-point response (0 = not at all; 3 = a lot) | α=0.90 |
| School connectedness | 9 | I feel like I belong at my school. My teachers respect me. |
4-point response (0=never or seldom; 3=very often) | α=0.85 |
|
| ||||
|
Skills
| ||||
| Fight avoidance skills | 5 | To avoid a fight, I would… …try to get my friends to calm down. …talk with an adult. |
2-point response (0=No, 1=Yes) | α=0.70 |
| Stress management skillsa | 8 | I get angry easily. When I get angry, I act without thinking. |
4-point response (0=never or seldom; 3=very often) | α=0.86 |
|
| ||||
|
School-Related Behaviors
| ||||
| Suspended or expelled from school, past 6 months | 2 | In the last 6 months, have you… …been suspended from school? …been expelled from school? |
2-point response (0=No, 1=Yes) b | NA |
| In college or technical school | 1 | Are you in technical school or college now? | 2-point response (0=No, 1=Yes) c | NA |
From Bar-On Emotional Quotient Inventory:Youth Version (Bar-On 2006).
Measure dichotomized, contrasting participants who reported suspension or expulsion with others.
Measure dichotomized, contrasting participants who reported currently being enrolled in college or technical school with others.
Process Measures
To assess participant exposure and fidelity to each intervention component, case managers completed a brief checklist of attendance and topics at each case management visit and peer leadership session. To identify contextual factors and intervention processes associated with changes in study outcomes, case managers completed an intervention summary for every participant after six months of intervention involvement and updated this summary at each teen’s 12- and 18-month intervention points. This summary utilized a standard format including (1) a psychosocial assessment using HEADSSS, a universally-accepted adolescent clinical screening tool (Goldenring and Rosen 2004) (Home/Family Involvement; Education and Employment; Activities with Friends; Drug Use; Sexual Behavior/Contraceptive Use; Suicidality/Emotional Health; Safety/Violence Involvement); and (2) observations related to changes in the teen’s aggressive and violent behaviors and intervention strategies that the case manager perceived to support positive behavior change.
Analysis Methods
Endpoint Analysis of 18-Month Outcomes
Using an intent-to-treat design in which participants were analyzed in their originally assigned study condition, 18-month outcomes were assessed through traditional endpoint analysis. Each outcome was regressed upon study condition (intervention vs. control) and its corresponding baseline measure, with the exception of college/technical school enrollment. We utilized a complete-case strategy to deal with missing data because of a low rate of missingness (<10%, Cohen and Cohen 1983), due to high sample retention over time and low item non-response. Valid sample sizes for each outcome are included in Table 3.
Table 3.
Effects of Prime Time Intervention on Behavioral and Psychosocial Outcomes at 18 Months, Adjusted for Baseline Values
| Variable | Sample Size | Intervention Mean Score or % | Control Mean Score or % | Adjusted RR, OR or Mean Difference (95%CI) | P-Value | d+ |
|---|---|---|---|---|---|---|
| Aggressive and Violent Behavior Outcomes | ||||||
| Relational aggression perpetration, past 30 days++,a | 235 | 1.70 | 1.90 | aRR=0.90 (0.82, 0.98) | 0.02 | 0.28 |
| Relational aggression victimization, past 30 days++,a | 236 | 2.27 | 2.38 | aRR=0.95 (0.89, 1.02) | 0.16 | |
| Physical violence perpetration, past 6 months++,b | 235 | 1.07 | 1.00 | aRR=1.08 (0.83, 1.41) | 0.57 | |
| Physical violence victimization, past 6 months++,c | 235 | 0.89 | 0.97 | aRR=0.91 (0.77, 1.07) | 0.26 | |
| Related Psychosocial and Behavioral Outcomes | ||||||
| Family connectedness++,d | 235 | 2.13 | 1.96 | 0.18 (0.07, 0.28) | 0.00 | 0.63 |
| School connectedness++,&,d | 206 | 2.16 | 2.18 | −0.02 (−0.15, 0.12) | 0.78 | |
| Fight avoidance skills++,e | 237 | 3.76 | 3.65 | 0.11 (−0.52, 0.74) | 0.74 | |
| Stress management skills ++,d | 234 | 1.77 | 1.72 | 0.05 (−0.09, 0.20) | 0.46 | |
| Suspended or expelled, past 6 months++,^,& | 205 | 17.96% | 16.24% | aOR=1.16 (0.75, 1.78) | 0.49 | |
| Currently in college or technical school +++, ^, && | 60 | 58.82% | 38.46% | aOR=2.25 (1.30, 3.93) | 0.00 | 0.52 |
Effect sizes computed using Cohen’s d with pooled standard deviation (Cohen & Cohen, 1983)) are noted for outcomes with significant differences between groups.
Regression model adjusted for baseline measure of outcome, within-clinic clustering.
Regression model adjusted for within-clinic clustering.
Logistic regression used with this dichotomous outcome.
Model excludes participants who were not in school at 12-month and 18-month follow-up points.
Model includes only participants who had graduated from high school or received a GED.
Count ranged from 0 (low) to 6 (high).
Count ranged from 0 (low) to 5 (high).
Count ranged from 0 (low) to 4 (high).
Scores ranged from 0 (low) to 3 (high).
Scores ranged from 0 (low) to 5 (high).
Regression models were estimated using generalized estimating equations (GEEs) in SAS Version 9.2. This estimation strategy allows for modeling of both normally and non-normally distributed variables and adjustment of standard errors for correlations between girls enrolled from the same clinic (Ballinger 2004; Liang and Zeger 1986). Intracluster coefficients for outcome measures ranged from 0.00 to 0.07. Model estimates are interpreted as odds or means applicable to an “average” participant in this group of high-risk adolescents, as GEE models are “marginal” or “population averaged models” (Liang and Zeger 1986).
Dose Analysis
Because intervention participants engaged in different levels of case management and peer leadership groups, we also conducted exploratory analyses to assess whether different outcomes were associated with different levels of exposure (dose-response) (Birnbaum et al. 2002). The main independent variable in the dose-response analyses was a categorical measure of intervention exposure: 0 = no exposure (control group; n=123); 1 = minimal exposure (<6 case management visits, <7 peer educator sessions; n=17); 2 = case management only (≥6 case management visits, <7 peer educator sessions; n=24); and 3 = case management + peer leadership (≥6 case management visits, ≥7 peer educator sessions; n=75). The decision to dichotomize case management and peer leadership as noted above was based on the number of visits/sessions considered to constitute substantial involvement in each. Substantial exposure to case management was defined as ≥6 case management visits, as process data revealed that all core case management topics were addressed with every girl completing ≥6 visits. Substantial exposure to peer leadership was defined as attending ≥7 sessions in our 22-session peer educator program, which allowed sufficient time for girls to function successfully in a group.
Using the control group as the reference, the impact of three differing levels of exposure to the intervention on 18-month outcomes was evaluated through GEE models, similar to endpoint analyses. A Bonferroni correction was applied to reduce the likelihood of Type I error due to multiple comparisons to the control group (i.e., 0.05/3 comparisons for each outcome=0.02). Due to small sample sizes in two of the exposure groups, we consider these analyses to be exploratory.
Qualitative Analysis
Intervention summaries, written by case managers, provided a qualitative description of participants’ social contexts as related to relational aggression and physical violence. Using a descriptive content analysis approach, each participant’s summary was read in its entirety (i.e., entries at 6, 12, and 18-month intervention points); then, one of the investigators used open coding strategies to identify types and sources of aggression and violence, and developed a coding template. Next, two researchers used the coding template to independently categorize the episodes of violence in intervention summaries. Reliability between coders was high. A third researcher with extensive qualitative experience resolved one disagreement between coders.
Data from participant surveys were used to categorize groups of girls to include those who: (1) reported decreases in relationally aggressive behaviors over time and (2) maintained high levels of relational aggression over time. Parallel groups were created for patterns of physical violence. Next, patterns in behavior and psychosocial contexts within and across groups were identified. In particular, we aimed to identify contextual factors that may have influenced change, or lack of change, in aggressive and violent behaviors. Case exemplars exhibiting patterns of (1) relational aggression and (2) physical violence were selected to illustrate the influence of social contexts on these behaviors among girls with high levels of case management and peer leadership group involvement. Because we were interested in independent experiences of different forms of aggression, separate exemplars were selected to illustrate relational aggression and physical violence.
Results
Intervention Participation
Participation in case management and peer educator training and practicum sessions was high. The median number of case management visits among girls in the intervention condition was 12; 79% of girls participated in ≥6 case management visits during the 18-month intervention. Additionally, 60% of participants completed ≥7 peer educator sessions; among those who reached this threshold, the median number of peer educator sessions attended was 18. Among girls actively involved in case management (i.e., ≥6 visits), 73% attended ≥7 peer educator sessions. The median number of peer educator contacts made by participants attending one or more peer educator training sessions was 46.
In contrast, participation in service learning was low; 29.4% of the intervention group completed ≥5 service learning sessions. Process data indicated that barriers included teens taking on part-time jobs, starting college or technical school, or being otherwise unable to commit to ongoing group involvement.
Eighteen Month Outcomes
Relational Aggression
Table 3 compares intervention and control groups on study outcomes. Intervention participants reported instigating fewer relationally aggressive behaviors in the past 30 days than did control participants. There were no intervention-control differences in relational aggression victimization at this follow-up point.
Dose-response analysis (available on request) suggested differences in relational aggression perpetration by intervention exposure. The control group reported instigating significantly more relationally aggressive behaviors than the case management + peer leadership group (p<.001). Dose-response analysis also indicated differences relational aggression victimization by intervention exposure. The control group was significantly more likely to have been a victim than the case management + peer leadership group (p=.04), and significantly less likely to have been a victim than the minimal exposure group (p=.01).
Relational Aggression Exemplar
The following exemplar, using a pseudonym, illustrates psychosocial contexts of an intervention participant who noted high levels of relational aggression at baseline and low levels of aggressive behaviors at the 18-month follow-up point. This exemplar is similar to others whose self-reports reflected linear decreases in relational aggression over time.
When she began the Prime Time intervention, Carlisha was a ward of the state and had recently left foster care to live with her mother who had serious mental illness. Carlisha’s family was living on social security and child support payments along with income from an older sister. Carlisha and her mother had poor communication. Carlisha didn’t want to be in school and often ran away from home to stay with an older boyfriend. Her case manager, however, documented dramatic change in Carlisha’s life during her involvement in the intervention. Since engaging in Prime Time, Carlisha reported not fighting in school, chose not to have a boyfriend or use drugs, adopted healthier sexual behaviors, and chose to stay in school. Many improvements occurred during the first six months of Carlisha’s involvement in Prime Time. During her final 12 months of involvement, Carlisha continued to demonstrate positive behaviors and progress towards her personal goals. She reported using birth control regularly and quitting smoking; her communication with her mother improved. She also noted looking forward to college, something she hadn’t spoken of previously. Her case manager attributed many positive changes in Carlisha’s life to her Prime Time group involvement, re-engagement in school, and support from her case manager along with a teacher at school and her older sister.
Physical Violence
There were no overall intervention-control group differences in physical violence perpetration or victimization at this follow-up point (Table 3). Dose-response analysis (available on request) suggested differences in violence perpetration by intervention exposure. Control participants reported significantly less violence perpetration than the minimal exposure group (p<.001). Dose-response analysis indicated no differences in violence victimization by intervention exposure.
Physical Violence Exemplar
The following exemplar, using a pseudonym, illustrates psychosocial contexts of an intervention participant who noted high levels of physical violence at baseline and at 18-month follow-up despite active involvement in case management and peer leadership activities. This exemplar is similar to others whose self-reports reflected maintaining high levels of violence over time.
Throughout the time she was involved in Prime Time, Maria lived in a public housing unit with her mother who received public assistance for a disability. Maria was often home for prolonged periods of time without adult supervision. An older sister, who periodically lived with Maria and her mother, was incarcerated for possession of methamphetamines during Maria’s first six months of involvement with Prime Time. As Maria began the intervention, she was struggling with alcohol and marijuana use. She was also two years behind in school credits. At 12 months, her case manager reported that Maria was caught using marijuana at school and sentenced to mandatory drug treatment. Upon completing drug treatment, she told her case manager that she had no plans to quit using marijuana and alcohol as drugs helped her cope with her home life; she noted that everyone in her family used drugs. Twelve months into the intervention, she no longer attended school because of her drug use and need to sleep most of the day. She reported that it was difficult to stay focused on school or not use drugs because her friends used drugs a lot of the time. Violence was pervasive in Maria’s community. Throughout the intervention, Maria told her case manager that she regularly witnessed violent situations in the public housing unit in which she lived. As the 18-month intervention ended, Maria was in a violent relationship with an older man whom she had recently received a protection order against for verbally threatening her. She was not optimistic that the order would be effective as he lived across the street from her. Her case manager characterized Maria as being “very enmeshed” in a life of drug use and environmental chaos, a life that Maria felt she would never get out of. Maria also thought that her family expected her not to succeed in life.
Related Psychosocial & Behavioral Outcomes
Table 3 also includes psychosocial and behavioral outcomes related to aggressive behavior and physical violence. Intervention participants reported higher levels of family connectedness than did control participants (p<.001). Among the small subgroup who had graduated from high school or received a GED 18 months following study enrollment, intervention participants were more likely than controls to be enrolled in college or technical school (p<.001). No between-group differences were found in measures of school connectedness, stress management skills, fight avoidance skills, or recent school suspension or expulsion.
Dose-response analysis (available upon request) suggested differences in some psychosocial and behavioral outcomes. Significant differences in family connectedness by intervention exposure were noted, with the control group reporting significantly lower levels of family connectedness than case management + peer leadership group (p=.00). Among those who had completed high school or equivalent, control group girls were significantly less likely to be enrolled in college or technical school than the case management + peer leadership group (p=.01). No differences between intervention dose groups in stress management skills, fight avoidance skills or recent school suspension/expulsion were noted.
Discussion
This study examined the effects of the Prime Time intervention on relational aggression, physical violence, and related psychosocial and behavioral outcomes among adolescents at high risk for early pregnancy. Findings demonstrate that a large proportion of vulnerable adolescent girls seeking clinic services will engage in youth development programming, with sizable percentages of participants completing substantial numbers of case management visits and peer educator sessions. This level of involvement appears to have yielded desired changes in relational aggression. At the close of the 18-month intervention, girls in the intervention group were significantly less likely to have instigated relationally aggressive behaviors in the past 30 days, compared to the control group. The magnitude of this effect (d=0.28) is comparable to the mean effect size for school-based programs targeting aggressive behavior among at-risk students (d=0.29) (Wilson and Lipsey 2007). Exploratory dose-response findings suggest that reductions in relational aggression perpetration and victimization may have been most pronounced among girls who were actively involved in case management + peer leadership activities. In contrast, Prime Time involvement did not appear to result in reductions in physical violence. Of the intervention dose groups, the minimal exposure group tended to maintain the highest levels of violence perpetration. Among related psychosocial and behavioral outcomes, the intervention group reported higher levels of family connectedness and greater likelihood of enrolling in college or technical school than controls. Although exploratory, dose-response findings suggest that both of these outcomes were most pronounced in the case management + peer leadership dose group. At this follow-up point, Prime Time involvement did not appear to be linked to changes in school connectedness, social-emotional skills or school suspension.
The intervention’s intentional focus on supportive relationships with adults, peers and family members may have contributed to reductions in relational aggression perpetration. Previous research indicates that caring, consistent relationships with pro-social adults and supportive peer relationships buffer girls from involvement in aggressive behaviors (Zahn et al. 2008). Similarly, mentoring interventions that include an emphasis on emotional support have been linked to reductions in youth aggression (Tolan et al. 2008). As illustrated in the case exemplar of Carlisha, ongoing support from a case manager, another consistent pro-social adult and an older sister, along with positive experiences as a member of a Prime Time peer leadership group, appeared to contribute to reductions in relational aggression. The emphasis on supportive relationships is illustrated by the case management practice of building and maintaining a trusting youth-adult relationship over an 18-month period (Tanner et al. 2012). Peer leadership group practices also emphasized supportive relationships. For example, rather than expelling a teen for inappropriate behavior, case managers facilitated a process in which the teen and the group talked about how people were affected and agreed on actions to repair the harm. Peer leadership group activities were structured to give girls ample opportunity to form and maintain positive relationships with other girls. A focus on maintaining supportive relationships with peers may be particularly important for our target group, as prior research suggests that it is common for these girls to have experienced substantial disruptions in peer relationships (Caines et al. 2004).
In contrast to effects on relational aggression, Prime Time appeared to have minimal effects on girls’ involvement in physical violence. As illustrated in the case exemplar of Maria, violence was pervasive in these girls’ social contexts (Secor-Turner et al. 2013). Girls routinely observed others modeling violence in response to stressful situations; thus, it was normative for girls to incorporate similar responses into their repertoires. Further, the intervention did not appear to affect fight avoidance skills, stress management skills, school connectedness or school suspension, known correlates of physical violence in this sample and other high-risk groups (Borowsky et al. 2008; Polan et al. 2012). Relatively few intervention activities addressed cognitions, skills and behaviors specific to physical violence. The intervention could be more effective in preventing physical violence among girls from high-risk social contexts by incorporating activities that explicitly convey social expectations for non-violence (Borowsky et al. 2008), expand girls’ stress tolerance and impulse control skills (Polan et al. 2012), build their repertoire of non-violent responses to potentially violent situations (Wilson and Lipsey 2007) and enhance their pro-social involvement with teachers and school (Resnick et al. 2004).
Exploratory dose-response analyses found that girls in the minimal exposure group (n=17) reported more physical violence perpetration and relational aggression victimization than the control group. Despite repeated attempts, we were unsuccessful in engaging this group of girls in regular intervention activities. These girls tended to be facing extremely chaotic life circumstances (e.g., abuse, parent deported) or dealing with severe behavioral and/or mental health issues compounded by poor family functioning (Tanner et al. 2012). Due to such circumstances, infrequent case management visits focused on immediate crisis management rather than on intervention topics. High levels of self-reported aggression and violence were likely a reflection of normative violence in these girls’ social contexts (Secor-Turner et al. 2013).
Of measured psychosocial and behavioral outcomes, the intervention had a substantial impact on family connectedness. This outcome appeared to be most pronounced in the case management + peer leadership group. Both case management and peer educator group activities had an intentional focus on pro-social family engagement. It may be that case managers’ individualized coaching combined with homework activities from peer educator sessions triggered girls’ efforts to engage with family members and build supportive family relationships. Prior longitudinal research suggests that high levels of connectedness to family acts as a powerful protective buffer against girls’ involvement in violence (Resnick et al. 2004).
Worthy of note is a preliminary finding among participants who had completed high school at the 18-month follow-up survey point. Compared to the control group, a significantly higher proportion of the intervention group was enrolled in college or technical school. This outcome was most pronounced in the case management + peer leadership dose group. It may be that case managers’ explicit focus on exploring girls’ interests and goals following high school (through activities such as local college tours with girls who expressed interest), in combination with peer leadership group activities in which girls explored school and career options, gave participants the types of support needed to translate post-secondary education aspirations into reality. Involvement in post-secondary education has been associated with reduced risk for patterns of serious violence during emerging adulthood (Kosterman et al. 2005).
Several methodological limitations exist. First, data were collected using self-report surveys subject to response bias. However, using self-reports is standard practice for intervention studies addressing adolescent aggressive and violent behaviors (Wilson and Lipsey 2007); prior research supports the reliability of youths’ reports of aggressive and violent behaviors (Brenner et al. 2002) particularly with the use of A-CASI methods (Turner et al. 1998). Second, our study lacks measures assessing relational elements of the intervention. Such measures would allow for formal mediation analyses examining whether intervention involvement led to reductions in aggressive behaviors via improvements in supportive relationships. Third, our findings may not be generalizable to high-risk adolescent girls who do not access clinic services. Fourth, because analyses were conducted using participants with data at both baseline and 18-month surveys, there is a small chance for biased results due to missing data. These limitations are balanced by methodologic strengths. First, the finding that participants and eligible non-participants were similar on a range of indicators suggests that results are generalizable to a population of high-risk adolescent girls seeking clinic services. Second, minimal loss to follow-up at the 18-month survey along with only isolated differences between girls in the 18-month sample and those lost to follow-up increases our confidence in the validity of findings, as does the very low rate of item non-response.
This study addresses a dearth of evidence regarding effective approaches to preventing violence among girls (Zahn et al. 2008). Reductions in relational aggression perpetration were seen among high-risk adolescent girls involved in an intervention with an intentional focus on building supportive relationships with adults, peers and family members. The magnitude of this intervention effect was comparable to the mean effect size of school-based programs targeting students at high risk for aggressive behavior (Wilson and Lipsey 2007). Changes appeared to be most prominent among girls involved in a combination of case management and peer leadership intervention activities, providing preliminary support for multi-component approaches that address diverse psychosocial issues confronting high-risk youth while offering opportunities and supports for youth leadership. Formal mediation analyses are needed to identify the extent to which intervention effects on relational aggression were mediated through measured psychosocial and behavioral attributes. Further research is also needed on intervention refinements aimed at reducing physical violence. Relational aggression was the most prevalent form of violence among this high-risk group at baseline; findings suggest that a relationally-based intervention offered through primary care clinics reaches this audience and is effective in preventing a damaging form of youth violence.
Together with previous research demonstrating reductions in sexual risk behaviors among Prime Time participants (Sieving et al. 2011a, 2012), findings from the current study suggest that sustained involvement in a youth development intervention offered through clinics holds promise in preventing multiple risk behaviors among a group of youth most vulnerable to poor health outcomes including early pregnancy. Vulnerable youth comprise a critical subset of the adolescent population who typically do not receive health services addressing their complex multi-system needs (Irwin et al. 2009), contributing to enduring inequities in violence, pregnancy and birth rates. While innovative multifaceted models of preventive services for this population exist, evidence regarding outcomes, costs and downstream benefits of such approaches is limited (NRC/IOM 2009). In this era of health care reform, continued research examining the efficacy, effectiveness, and cost-benefits of preventive services for vulnerable youth is critical to guiding changes in the organization and delivery of health services that meet the needs of this important population.
Acknowledgments
This project is supported with funds from the National Institute of Nursing Research (5R01-NR008778) and from the Centers for Disease Control and Prevention (U48-DP001939). The views presented do not necessarily reflect those of the funders. The Prime Time study would not have been possible without the cooperation and contributions of the young women, clinics and research staff involved with this project. We also thank Amy Gower for her review of drafts of this manuscript and Jenna Baumgartner for her excellent editorial assistance with manuscript preparation.
References
- Ballinger G. Using generalized estimating equations for longitudinal data analysis. Organizational Research Methods. 2004;7:127–150. [Google Scholar]
- Bandura A. Social foundations of thought and action: A social cognitive theory. Englewood Cliffs, NJ: Prentice–Hall; 1986. [Google Scholar]
- Bar-On R. The Bar-On model of emotional-social intelligence. Psicothema. 2006;18(Suppl):13–25. [PubMed] [Google Scholar]
- Birnbaum A, Lytle L, Story M, Perry C, Murray D. Are differences in exposure to a multicomponent school-based intervention associated with varying dietary outcomes in adolescents? Health Education Behavior. 2002;29:427–443. doi: 10.1177/109019810202900404. [DOI] [PubMed] [Google Scholar]
- Borowsky I, Ireland M, Resnick M. Violence risk and protective factors among youth held back in school. Ambulatory Pediatrics. 2002;2:475–484. doi: 10.1367/1539-4409(2002)002<0475:vrapfa>2.0.co;2. [DOI] [PubMed] [Google Scholar]
- Borowsky I, Mozayeny S, Stuenkel K, Ireland M. Effects of a primary care-based intervention on violent behavior and injury in children. Pediatrics. 2004;114:e392–e399. doi: 10.1542/peds.2004-0693. [DOI] [PubMed] [Google Scholar]
- Borowsky I, Widome R, Resnick M. Youth and violence. In: Hennenhougen K, Quah S, editors. International encyclopedia of public health. San Diego, CA: Academic Press; 2008. pp. 675–684. [Google Scholar]
- Brener N, Kann L, McManus T, Kinchen S, Sundberg E. Reliability of the 1999 Youth Risk Behavior Survey Questionnaire. Journal of Adolescent Health. 2002;31:336–342. doi: 10.1016/s1054-139x(02)00339-7. [DOI] [PubMed] [Google Scholar]
- Buka S, Stichick T, Birdthistle I, Earls F. Youth exposed to violence: Prevalence, risks, and consequences. American Journal of Orthopsychiatry. 2001;71:298–310. doi: 10.1037/0002-9432.71.3.298. [DOI] [PubMed] [Google Scholar]
- Caines K, Sieving R, Resnick M. Realities, rituals, and rhythms: Mentoring high-risk sexually active girls. Journal of Adolescent Health. 2004;34(2):150–151. [Google Scholar]
- Cairns R, Cairns B, Neckerman H, Ferguson L, Gariepy J. Growth and aggression: Childhood to early adolescence. Developmental Psychology. 1989;25:320–330. [Google Scholar]
- Centers for Disease Control and Prevention. Youth risk behavior surveillance-United States, 2007. Morbidity and Mortality Weekly Report. 2008;57(SS–4) [PubMed] [Google Scholar]
- Centers for Disease Control and Prevention. Youth risk behavior surveillance – United States, 2009. Morbidity and Mortality Weekly Report. 2010;59(SS–5) [PubMed] [Google Scholar]
- Cohen J, Cohen P. Applied multiple regression/correlation analysis for the behavioral sciences. 2. Hillsdale, NJ: Lawrence Erlbaum; 1983. [Google Scholar]
- Crick N, Grotpeter J. Relational aggression, gender, and social-psychological adjustment. Child Development. 1995;66:710–722. doi: 10.1111/j.1467-8624.1995.tb00900.x. [DOI] [PubMed] [Google Scholar]
- Department of Health and Human Services. Youth violence: A report of the surgeon general. 2001 Retrieved 7/19/11, from http://www.surgeongeneral.gov/library/youthviolence/
- Federal Bureau of Investigation. Crime in the United States, 2005: Uniform crime reports. Washington, DC: U.S. Department of Justice, FBI; 2006. [Google Scholar]
- Fergus S, Zimmerman M. Adolescent resilience: A framework for understanding healthy development in the face of risk. Annual Review of Public Health. 2005;26:399–419. doi: 10.1146/annurev.publhealth.26.021304.144357. [DOI] [PubMed] [Google Scholar]
- Goldenring J, Rosen D. Getting into adolescent HEADSSS. Contemporary Pediatrics. 2004;21:64. [Google Scholar]
- Henneken C. Epidemiology in medicine. Boston, MA: Little Brown and Company; 1987. [Google Scholar]
- Herrenkohl T, Catalano R, Hemphill S, Tomborou J. Longitudinal examination of physical and relational aggression as precursors to adolescent problem behaviors. Violence and Victims. 2009;24:3–19. doi: 10.1891/0886-6708.24.1.3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Irwin C, Adams S, Park M, Newacheck P. Preventive care for adolescents: Few get visits and fewer get services. Pediatrics. 2009;123:e565–e572. doi: 10.1542/peds.2008-2601. [DOI] [PubMed] [Google Scholar]
- Kirby D. Emerging answers: Research on programs to reduce teen pregnancy and sexually transmitted diseases. Washington, DC: National Campaign to Prevent Teen Pregnancy; 2007. [Google Scholar]
- Kirby D, Lepore G. Risk and protective factors affecting teen sexual behavior, pregnancy, childbearing and sexually transmitted disease. Scotts Valley, CA: ETR Associates; 2007. [Google Scholar]
- Kosterman R, Hawkins JD, Abbott R, Hill K, Herrenkohl T, Catalano R. Measures of positive adult behavior and their relationship to crime and substance use. Prevention Science. 2005;6:21–33. doi: 10.1007/s11121-005-1250-0. [DOI] [PubMed] [Google Scholar]
- Laird R, Jordan K, Dodge K, Pettit G, Bates J. Peer rejection in childhood involvement with antisocial peers in early adolescence, and the development of externalizing behavior problems. Development and Psychopathology. 2001;13:337–354. doi: 10.1017/s0954579401002085. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Liang K, Zeger S. Longitudinal analysis with generalized linear models. Biometrika. 1986;73:13–22. [Google Scholar]
- Limbos M, Chlan L, Warf C, Schneir A, Iverson E, Shekelle P, et al. Effectiveness of interventions to prevent youth violence: A systematic review. American Journal of Preventive Medicine. 2007;33:65–74. doi: 10.1016/j.amepre.2007.02.045. [DOI] [PubMed] [Google Scholar]
- Miller-Johnson S, Sullivan T, Simon T. Evaluating the impact of interventions in the Multisite Violence Prevention Study: Samples, procedures, and measures. American Journal of Preventive Medicine. 2004;26:48–61. doi: 10.1016/j.amepre.2003.09.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Minnesota Department of Education. Minnesota Student Survey 2007. Roseville, MN: 2007. http://education.state.mn.us/MDE/Learning_Support/Safe_and_Healthy_Learners/Minnesota_Student_Survey/Statewide_Tables/index.html. [Google Scholar]
- Minnis A, Moore J, Doherty I, Rodas C, Auerswald C, Shiboski S, et al. Gang exposure and pregnancy among female adolescents in San Francisco: Evidence for integrating reproductive health and violence prevention efforts. American Journal of Epidemiology. 2008;167:1102–1109. doi: 10.1093/aje/kwn011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Murray-Close D, Ostrov J, Crick N. A short-term longitudinal study of growth of relational aggression during middle childhood: Associations with gender, friendship intimacy, and internalizing problems. Development and Psychopathology. 2007;19:187–203. doi: 10.1017/S0954579407070101. [DOI] [PubMed] [Google Scholar]
- National Research Council and Institute of Medicine. Adolescent health services: Missing opportunities. Washington, DC: The National Academies Press; 2009. [PubMed] [Google Scholar]
- Orr D, Johnston K, Brizendine E, Katz B, Fortenberry D. Subsequent sexually transmitted infection in urban adolescents. Archives of Pediatrics and Adolescent Medicine. 2001;155:947–953. doi: 10.1001/archpedi.155.8.947. [DOI] [PubMed] [Google Scholar]
- Polan J, Sieving R, Pettingell S, Bearinger L, McMorris B. Relationships between adolescent girls’ social-emotional intelligence and their involvement in relational aggression and physical fighting. Journal of Adolescent Health. 2012;50:S81–S82. [Google Scholar]
- Puzzanchera C, Adams B, Sickmund M. Juvenile court statistics 2006–2007. Pittsburgh, PA: National Center for Juvenile Justice; 2010. [Google Scholar]
- Resnick M. Protective factors, resiliency and healthy youth development. Adolescent Medicine State of the Art Reviews. 2000;11:157–164. [PubMed] [Google Scholar]
- Resnick M, Ireland M, Borowsky I. Youth violence perpetration: What protects? What predicts? Findings from the National Longitudinal Study of Adolescent Health. Journal of Adolescent Health. 2004;35:424.e1–424e10. doi: 10.1016/j.jadohealth.2004.01.011. [DOI] [PubMed] [Google Scholar]
- Shrier L, Ancheta R, Goodman E, Chiou V, Lyden M. Randomized controlled trial of a safer sex intervention for high-risk adolescent girls. Archives of Pediatrics & Adolescent Medicine. 2001;155:73–79. doi: 10.1001/archpedi.155.1.73. [DOI] [PubMed] [Google Scholar]
- Secor-Turner M, Garwick A, Seppelt A, Sieving R. Characteristics of violence among adolescent girls at high risk for pregnancy. Journal of Pediatric Health Care. 2013 doi: 10.1016/j.pedhc.2013.03.002. under review. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sieving R, Bernat D, Resnick M, Oliphant J, Pettingell S, Plowman S, et al. A clinic-based youth development program to reduce sexual risk behaviors among adolescent girls: Prime Time pilot study. Health Promotion Practice. 2012;13:462–471. doi: 10.1177/1524839910386011. [DOI] [PubMed] [Google Scholar]
- Sieving R, Hellerstedt W, McNeely C, Fee R, Resnick M. Reliability of contraceptive use and sexual behavior self-reports among adolescent girls. Journal of Sex Research. 2005;42:159–166. doi: 10.1080/00224490509552269. [DOI] [PubMed] [Google Scholar]
- Sieving R, McMorris B, Beckman K, Pettingell S, Secor-Turner M, Kugler K, et al. Prime Time: 12-month sexual health outcomes of a clinic-based intervention to prevent pregnancy risk behaviors. Journal of Adolescent Health. 2011a;49:172–179. doi: 10.1016/j.jadohealth.2010.12.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Sieving R, Resnick M, Garwick A, Bearinger L, Beckman K, et al. A youth development approach to teen pregnancy prevention. American Journal of Health Behavior. 2011b;35:346–358. doi: 10.5993/ajhb.35.3.8. [DOI] [PubMed] [Google Scholar]
- Silverman J, Raj A, Clements K. Dating violence and associated sexual risk and pregnancy among adolescent girls in the United States. Pediatrics. 2004;114:e220–e225. doi: 10.1542/peds.114.2.e220. [DOI] [PubMed] [Google Scholar]
- Sussman S, Dent C, Stacy A. Project Towards No Drug Use: A review of the findings and future directions. American Journal of Health Behavior. 2002;26:354–365. doi: 10.5993/ajhb.26.5.4. [DOI] [PubMed] [Google Scholar]
- Tanner A, Secor-Turner M, Garwick A, Sieving R, Rush K. Engaging vulnerable adolescents in the Prime Time program to reduce unintended pregnancy: Perspectives of case managers. Journal of Pediatric Health Care. 2012;26:254–265. doi: 10.1016/j.pedhc.2010.10.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tolan P, Henry D, Schoeny M, Bass A. Campbell Systematic Reviews. Vol. 16. Oslo, Norway: The Campbell Collaboration; 2008. Mentoring interventions to affect juvenile delinquency and associated problems. [Google Scholar]
- Turner C, Ku L, Rogers S, Lindberg L, Pleck J, Sonenstein F. Adolescent sexual behavior, drug use and violence: Increased reporting with computer survey technology. Science. 1998;280:867–873. doi: 10.1126/science.280.5365.867. [DOI] [PubMed] [Google Scholar]
- van der Wal M, de Wit C, Hirasing R. Psychosocial health among young victims and offenders of direct and indirect bullying. Pediatrics. 2003;111:1312–1317. doi: 10.1542/peds.111.6.1312. [DOI] [PubMed] [Google Scholar]
- Wilson S, Lipsey M. School-based interventions for aggressive and disruptive behavior: Update of a meta-analysis. American Journal of Preventive Medicine. 2007;33(2S):S130–S143. doi: 10.1016/j.amepre.2007.04.011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Zabin L, Sedivy V, Emerson M. Subsequent risk of childbearing among adolescents with a negative pregnancy test. Family Planning Perspectives. 1994;26:212–217. [Google Scholar]
- Zahn M, Hawkins S, Chiancone J, Whitworth A. Girls study group: Charting the way to delinquency prevention for girls. Washington: Office of Juvenile Justice and Delinquency Prevention; 2008. Retrieved from www.ojp.usdoj.gov/ojjdp. [Google Scholar]